Abstract
Purpose
Amorphous solid dispersions (ASDs) have been widely used in the pharmaceutical industry for solubility enhancementof poorly water-soluble drugs. The physical stability, however, remainsone of the most challenging issues for the formulation development.Many factors can affect the physical stability via different mechanisms, and therefore an in-depth understanding on these factors isrequired.
Methods
In this review, we intend to summarize the physical stability of ASDsfrom a physicochemical perspective whereby factors that can influence the physical stability areclassified into thermodynamic, kinetic and environmental aspects.
Results
The drug-polymer miscibility and solubility are consideredas the main thermodynamicfactors which may determine the spontaneity of the occurrence of the physical instabilityof ASDs. Glass-transition temperature,molecular mobility, manufacturing process,physical stabilityof amorphous drugs, and drug-polymerinteractionsareconsideredas the kinetic factors which areassociated with the kinetic stability of ASDs on aging. Storage conditions including temperature and humidity could significantly affect the thermodynamicand kineticstabilityof ASDs.
Conclusion
When designing amorphous solid dispersions, it isrecommended that these thermodynamic, kinetic and environmental aspects should be completely investigatedand compared to establish rationale formulations for amorphous solid dispersions with high physical stability.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Amorphous solid dispersion (ASD) has been used as a classic drug delivery system for poorly water-soluble drugs for decades (1,2,3,4,5,6,7). Fundamentally it relies on the concept of dispersing drug molecules into polymeric carriers via pharmaceutical processes to form a homogeneous amorphous system. Within such dispersion system, drugs exist in the state of separated molecules, and thus the lattice energy that has to be overcome during dissolution could be completely avoided, and hence the dissolution rate can be enhanced (8,9,10,11). The application of ASDs has been successful as proved by ASD based medicines approved by FDA as shown in Table I (9).
Despite the successful commercialization of ASD based medicines, the main hurdle of using such system, the physical stability, remains substantially challenging for formulation scientists (12,13,14,15). Up to date, there have been many studies concerning the physical stability of ASDs since the concept was first introduced in 1961 (1). It has been reported that a number of factors, such as glass transition temperature (Tg) of amorphous drugs and polymers, molecular mobility of drugs, drug-polymer miscibility, solid solubility of drugs in the polymers, physical stability of amorphous drugs alone, fragility index of amorphous drugs, drug-polymer interaction, molecular weight of drugs, recrystallization temperature of amorphous drugs, storage environment (temperature and humidity) and preparation process, were related to and may significantly affect the physical stability of ASDs (16,17,18,19,20,21,22,23,24). Formulation design for ASDs are therefore guided under these factors. For instance, ASDs are recommended to be formulated with the drug loadings below the drug-polymer solubility (25). Meanwhile, it is also suggested that polymers with high glass transition temperatures should be used as the polymeric carriers for ASDs to enhance the physical stability of ASDs (26). When developing ASD formulations, such diverse suggestions may eventually raise the question as to selecting the polymers with high Tg or selecting the polymers that can offer high drug-polymer solubility. The two recommendations are certainly both correct, but they actually come from thermodynamic and kinetic concerns, respectively, which would influence the physical stability of ASDs by completely different mechanisms. The above mentioned stability-related factors that can thermodynamically or kinetically determine the physical stability, however, may not have been clearly distinguished (27,28,29,30). Therefore, under the great contributions that have already been made by previous studies, an overview on the physical stability of ASDs from the physicochemical perspective may further assist formulation design for ASDs (31,32). In this paper, we intend to review the physical stability of ASDs from the physicochemical perspective by classifying the physical stability-related factors into thermodynamic, kinetic and environmental aspects. Basically, ASDs can be considered as systems to be stored in the environment. Thermodynamics and kinetics of the physical stability of ASDs would therefore be influenced by the environment (temperature and humidity). The physical stability-related factors could accordingly be classified and summarized into thermodynamic and kinetic aspects. Thermodynamic factors are associated with the thermodynamic stability of ASDs, which can determine the spontaneity of the occurrence of the physical instability, such as phase separation or recrystallization (28). Kinetic factors are associated with the kinetic stability, which can be used to estimate or describe the rate of phase separation or recrystallization of ASDs, and hence understanding the kinetic factors could be useful to predict the shelf lives for ASD based medicines (33). Moreover, environmental aspect, referring to temperature and humidity, is exterior aspect that could only influence the physical stability of ASDs via affecting the thermodynamic and kinetic related factors.
The classification of the stability-related factors into different physicochemical aspects could be a novel and more fundamental way for understanding the physical stability of ASDs. Such classification could assist formulation scientists to group the numerous physical stability-related factors, which may simplify the application of these factors. Additionally in this review, not only all factors associated with the physical stability of ASDs are classified into different aspects, but also the classic theories or calculating models for these factors are introduced and discussed. It is expected that through this review, the strategy for developing ASDs might be clear and the process of formulation screening for ASDs could be shortened.
Thermodynamics of the Physical Stability of Amorphous Solid Dispersions
Thermodynamic viewpoint on the physical stability of ASDs are mainly derived from the concepts of liquid systems, in which miscibility and solubility are applied to describe mixing solutions and dissolving solids into solvents (34). Considering the preparation of ASDs as dissolving solvates in solvents, ASDs can therefore be thermodynamically stable if the drug loading of the ASD is below the solid solubility of the drug in the polymer (34). Unlike solubility, miscibility is the concept for describing the mixing proportions of two liquids to form single-phase solutions at certain temperature and pressure i.e. mixing water and phenol (33,35). Similarly, amorphous drugs and amorphous polymers could be considered as two liquids, and thus at certain temperature and pressure, thermodynamically stable ASDs could be formed if the drug to polymer ratio in the system is within the single-phase region as illustrated in Fig. 1 (34,36). Up to date, the prediction or calculation of miscibility and solid solubility has been carried out via theoretical models and experiments, and the details of these approaches are discussed in the following sections.
Miscibility Between Drug and Polymer
Prediction of drug-polymer miscibility is a useful tool for screening polymeric carriers and determining the drug loadings in formulation development of ASDs. The commonly reported approaches for predicting the drug-polymer miscibility include solubility parameter approach, molecular modelling and Tg evaluation of solid dispersions (37,38,39,40).
Solubility Parameter
Solubility parameter is defined as the square root of the cohesive energy density that is consumed to separate unit volume of molecules from condensed phase to infinite distance (41). The drugs and polymers with similar solubility parameters are considered to be miscible based on the concept of “likes dissolve likes” (42). Group contribution method is usually employed to calculate the solubility parameters of compounds with complex structure and high molecular weight (43). In this method, the compound with complex chemical structure could be divided into several small functional groups, and the solubility parameters of these small groups can be determined by evaporation method, and hence the solubility parameter of the intact compound can be calculated (42). For instance, in Fedors solubility parameter, chemicals are simply divided into small groups, and the solubility parameter is calculated by
where δ represents solubility parameter, Σ Ecoh represents the sum of cohesive energy of each group and Σ V represents the sum of the molar volume of each group (44). An example of group contribution method is given in this review to ease the understanding of this method, and fenofibrate is used as the model drug. As seen in the chemical structure of fenofebrate (Table II), the drug molecule is composed of several chemical groups, such as methyl group and carbonyl groups. Therefore, the intact structure could be divided into small chemical groups as listed in Table II. The cohesive energy and molar volume of these small groups can be achieved by direct determination using evaporation method or from published results. The solubility parameter of fenofibrate could accordingly be calculated by Eq. (1).
In addition to Fedors method, other group contribution approaches were also reported to be used to calculate the solubility parameter (45,46,47). For example, in Hansen solubility parameter method, total solubility parameter of chemicals are contributed by three components including dispersion force, hydrogen bonding and polar (electrostatic) force, as described in Eq. (2) (35,45):
where δd2, δp2, and δh2 are the dispersion, polar and hydrogen bonding components of solubility parameters, respectively. Although the approaches of predicting solubility parameters are different, the calculated results of the same chemicals by different methods do not vary significantly, and therefore the miscibility results between drugs and polymers predicted using different solubility parameter methods are similar (43).
It was reported that, chemicals with a Δδ value (the difference of solubility parameter values between the drug and the polymer) less than 7.0 MPa0.5 were considered to be miscible whereas chemicals with a Δδ value larger than 7.0 MPa0.5 were considered to be immiscible, and the smaller the Δδ value, the higher the miscibility (43,48). This rule was reported to be useful for early stage formulation screening when developing ASD products (43). In one study, the researchers calculated the Δδ value between itraconazole and different polymers including Soluplus®, Eudragit® E PO and PVPVA64. The results showed that Eudragit® E PO had the highest Δδ value amongst the three polymers, and hence melt extrudates using Soluplus® and PVPVA64 presented better physical stability than the ASDs composed of Eudragit® E PO and itroconazole (38). The predicted results via solubility parameter for guiding the formulation development of ASDs, however, may not be reliable in some cases (49). For instance, it was reported that a binary system consisting of Vitamin E TPGS and Eudragit® E PO with a small Δδ value (0.8 MPa0.5) was immiscible. In contrast, another binary system composed of Eudragit® E PO and tartaric acid was miscible and exhibited better physical stability despite of the large Δδ value (19.8 MPa0.5) (49).
The reason for the discrepancy between the predicted miscibility and the real-time physical stability may be attributed to the interaction between the two types of compounds. Chemical entities are very likely to have high miscibility if interactions i.e. hydrogen bonding or acid-base interaction can be formed between drugs and polymers (50). When strong interactions between chemicals occurs, the solubility parameter approach would be less accurate in predicting miscibility between drugs and polymers (50). Therefore, while applying solubility parameter to develop formulations, it is recommended to initially assess the potential interactions between components by using technologies such as infrared spectroscopy or solid state NMR (51,52,53).
Evaluation of Glass Transition Temperatures of Solid Dispersions
Another approach of assessing the drug-polymer miscibility relies on the application of MTDSC (modulated temperature differential scanning calorimetry) in testing the prepared ASDs (54). An amorphous solid dispersion with a single Tg that has a value in between the Tg values of the amorphous drug and the polymer is considered to be a homogeneous system, and the drug and the polymer are miscible in the system (39,55). As can be seen in Fig. 2, solid dispersion composed of felodipine and PVP-VA64 with 30% w/w drug loading shows the Tg value in between the Tg values of amorphous felodipine and PVP-VA64, and consequently the drug and the polymer in the solid dispersion are miscible. This approach is a direct indicator for the drug and the polymer being miscible in ASDs, and it is often served as the primary tool when investigating the miscibility between the drug and the polymer in ASDs (56).
Molecular Modelling Prediction on Miscibility Between Drug and Polymer
Molecular modelling prediction is a method that employs quantum mechanical calculations combining with commercial software, i.e. Gaussian 09, to characterize the potential interactions between drugs and polymers (57,58). It is well known that interactions, such as hydrogen bonding between drugs and polymers, play important role in the miscibility between drugs and polymers (28). In molecular modelling method, dimeric structure of polymer and monomeric structure of drug are constructed by software, i.e. GaussView (59). The possibility of hydrogen bonding formation between drugs and polymers are assessed by calculating the binding energies from placing the drug molecule within the proximity of the dimeric structure of the polymer (40,60). If the binding energy level is comparable to the normal hydrogen bonding level, it is likely that H-bond might be formed between the drug and the polymer (61,62). Therefore, through molecular modelling, drug-polymer miscibility could be predicted before preparation into ASDs. A typical research by Douroumis et al. reported the study of investigating into the miscibility between model drugs (such as propranolol HCl) and commercial polymers (such as Eudragit® L100 and Kollidon VA64) (40). It was concluded that some of the predicted drug-polymer interactions were in agreement with DSC studies and molecular modelling could be broadly applied when solubility parameter method or Flory-Huggins method had limitations (40). This method, although being useful for formulation development of ASDs, requires certain knowledge on quantum mechanical calculation.
Determination of Solid Solubility of Drug in Polymer
Melting Point Depression Approach
Melting point depression method was derived from Flory-Huggins lattice theory that was originally employed to assess the thermodynamics of polymer solutions (63,64). The method was further developed and modified to be applied in determining the solid solubility of drugs in polymers (65). The method requires a series DSC (differential scanning calorimetry) tests at low heating rate on drug-polymer physical mixtures with different ratios (66). Upon heating on a physical mixture of a crystalline drug and an amorphous polymer to equilibrium state, the solid–liquid chemical potential (calculated as partial differential of the free energy from Flory-Huggins model) change of the crystalline drug should be equivalent to the chemical potential change of the crystalline drug in liquid state and in the amorphous polymer phase (67). Such decreased chemical potential of the crystalline drug would cause a depression of melting point of the crystalline drug. Combined with Flory-Huggins model, the following relationship could be established (65,68):
where TmixM is the melting temperature of the crystalline drug in the presence of the amorphous polymer, TpureM isthe standard melting point of the pure drug, ΔHfus is the heat fusion of the crystalline drug, m is the ratio of molar volume of polymer to that of the drug, and χ is the interaction parameter between the drug and the polymer. The interaction parameter (χ) can be achieved by the regression analysis using Eq. (3).
With the achieved interaction parameter (χ) value, combining Flory-Huggins lattice theory and the calculation of thermodynamic solubility, melting point depression method can be employed to predict the solid solubility of drugs in polymers using the following equations:
where S is the solubility of the compound at temperature T, ΔHfus is the enthalpy of fusion of the compound. At a certain temperature, Eq. (4) can be rewritten into:
where T2 and T1 represents TmixM and TpureM in Eq. (3), respectively. Therefore, according to Eq. (3) and Eq. (5), the solid solubility of drug in polymer, Sdrug, can be calculated by:
where Sdrug represents the solubility of drug in polymer at the temperature where solubility parameter is calculated, and in the melting point depression approach this temperature is the depressed meting point at standard atmospheric pressure (63,65,69).
Melting point depression method has been used to assist the formulation development of ASDs in optimizing the ratios of drug to polymer and screening polymer candidates (70,71). Recently, a report from Tian et al. successfully applied Flory-Huggins lattice theory to draw a phase diagram for felodipine and three polymers to determine the maximum drug loading for each polymer (72). Inaccurate prediction by melting point depression method, however, was also reported (73). For instance, Yang et al. reported that felodipine-Eudragit® E PO dispersions with the estimated solid solubility of approximately 31% (w/w) showed significantly higher physical stability under different storage conditions than carbamazepine-Eudragit® E PO dispersions with the estimated solubility of 46% (w/w) (73). These results suggests that there could be limitations when using melting point depression method to calculate the solid solubility of drugs in polymers. Flory-Huggins lattice theory does not take into account the effect of molecular interactions, i.e. dipole-dipole interactions (64,74). In addition, the calculation of the interaction parameter, χ, is dependent on temperature, drug to polymer ratio and polymer molecular weight, and these factors varies significantly between different drugs and polymers (64,75). The assumptions and restrictions from the method may lead to unexpected results of physical stability of ASDs. It is therefore recommended that when using melting point depression method to develop ASD formulations, short-time physical stability studies under stressed conditions may be conducted to confirm the applicable drug loading.
Perturbed-Chain Statistical Associating Fluid Theory
Perturbed-chain statistical associating fluid theory (PC-SAFT) is a thermodynamic model in which each API molecule is considered as a chain of spherical segments, and it can interact with other segments via different types of interactions (76,77,78). Unlike Flory-Huggins lattice method, in PC-SAFT approach, it involves almost all effective interactions between drugs and polymers, including repulsive interactions, van der Waals attractions, hydrogen bonding, and dipole-dipole interactions and charges (79). Due to the involvement of many aspects, PC-SAFT is more complex than Flory-Huggins method (melting point depression method). The advantage of PC-SAFT lies in the fact that all parameters in PC-SAFT have physical meanings and are not dependent on other variables. Besides, PC-SAFT parameters has been calculated for more than 400 compounds covering the fields of gases, solvate molecules and polymers (80).
The application of PC-SAFT approach in predicting drug/polymer solubility and miscibility is briefly summarised in this review. Thermodynamically, when a system composed of API and polymer reaches equilibrium, the solubility of the API in the polymer could be written by:
where \( {x}_{API}^L \) is the solubility of API (mole fraction), \( {Y}_{API}^L \) is the activity coefficient of the API in the liquid API/polymer phase, R is the universal gas constant, T is the temperature in Kelvin, \( {T}_{API}^{SL} \),\( {\varDelta h}_{API}^{SL} \), and \( {\varDelta Cp}_{API}^{SL} \) are the melting temperature, the heat fusion and the difference in the solid and the liquid heat capacities of the API, respectively. It can be seen that values such as\( {T}_{API}^{SL} \), \( {\varDelta h}_{API}^{SL} \), and \( {\varDelta Cp}_{API}^{SL} \) could be easily determined by DSC. Consequently, if the activity coefficient value, \( {Y}_{API}^L \), could be achieved, the solid solubility of the drug in the polymer should be able to be calculated using Eq.(7). The PC-SAFT approach is mainly applied for the calculation of the activity coefficient. In PC-SAFT, all molecules are treated as chains consisting of spherical segments with a certain value of diameter (Fig. 3). These chains could interact with each other. The number of segments (msegi), the diameter of the segment (σi), and the interaction energy between two segments (ui) are used to account for the interactions occurred between drug molecules and polymer molecules. In PC-SAFT, the residual of Helmholtz energy of a drug-polymer system is contributed by three types of energies including hard-chain contribution, van der Waals attraction and association, and can be calculated as the sum of repulsion of molecules. The repulsive interaction is the collective interactions that could be obtained by using msegi, σi, and ui. The activity coefficient is linked with the residual of Helmholtz energy via a few equations (details of these equations is discussed in Sadowski’s publications). Therefore, with the known values of msegi, σi, and ui, the value of \( {Y}_{API}^L \) could be achieved, and hence the solid solubility of the drug in the polymer can be estimated.
The molecule of indomethacin described in PC-SAFT chain model composed of segments (grey sphere) and association sites (75).
The PC-SAFT approach has been applied in a few studies regarding the relationship between the predicted drug-polymer solubility and the physical stability of corresponding ASDs (75,81,82,83). In these studies, various polymeric carriers, such as PVP, PVPVA 64, HPMCAS, and PLGA were formulated with typical BCS II drugs (i.e. ibuprofen) into ACSs. The results showed that, under stressed humidity, formulations with the drug loadings below the drug-polymer solubility by PC-SAFT approach showed excellent physical stability. The consistency between the results from real-time physical stability and the predicted drug-polymer solubility verifies the PC-SAFT approach, demonstrating its effectiveness in estimating the solubility of drug in polymer.
Observation of Drug Dissolution in Polymer
The drug-polymer solubility could also be investigated visually by using polarized hot-stage microscopy (84,85). In this method, the physical mixtures with different ratios of crystalline drug and polymer are subjected to direct heating process on hot stage microscope. Birefringence from crystalline drug could be observed when temperature is below the melting point of the drug. At the temperature above the melting point of the drug and the Tg of the polymer, if birefringence disappears and a single liquid phase without boundary appears, the drug is considered to be dissolved in the polymer. Through testing a series of drug-polymer physical mixtures, the drug-polymer solubility may be obtained. This method that relies on observation, however, could only provide an approximation of drug-polymer solubility. Besides, inaccurate estimation on the drug-polymer solubility by this method may occur, due to the bubbles left by the melted drugs, which could be recognised as drug-polymer boundaries.
Thermal Approaches
Enthalpy Approach
The application of enthalpy approach to predict the solubility of drug in polymer is based on the principle that the fraction of the drug dissolved in polymer make no contribution to the melting endotherm associated with the dispersed drug fraction (86). Accordingly, linear regression could be applied to estimate the relationship between the experimental values of melting enthalpy (dependent variables) and the drug concentrations (independent variables) in drug-polymer physical mixture (62). The solubility of the drug in the polymer, could be calculated as the x-intercept from the regression equation. In order to obtain an accurate drug-polymer solubility by this method, a fast heating rate (circa 400°C/min) has to be used to minimize the dissolution of the drug into the polymer while being heated, and hence the contribution from the exothermic drug dissolution to the melting endotherm can be reduced (87). It has been found that the faster the heating rate, the more accurate estimation of the drug solubility in polymer (87,88). With conventional DSC equipment, however, it is difficult to completely avoid the dissolution of the drug into the polymer on heating. This is because the maximum heating rate by conventional DSC may be less than 100°C/min, resulting in an inaccurate prediction (89).
Qi et al. modified the enthalpy approach and established a novel model to predict the solubility of drug in polymer (90). In that paper, it was assumed that the melting endotherm consisted of the energy associated with the drug dissolution in polymer and the energy of the drug melting. In that paper, the dissolution behavior of drug into polymer was dependent on the drug fraction in the drug-polymer physical mixture. According to the drug fractions, the drug-polymer mixing behaviors were divided into three areas: drug loading below the solubility of drug in polymer, polymer loading below the solubility of polymer in melted drug and the intermittent drug loading (Fig. 4) (90). The two x values at the corresponding interception points on the curve were the drug solubility in polymer (PA) and the polymer solubility in molten drug (PB), respectively. When predicting the solid solubility, this approach only involved the melting enthalpy and dissolution enthalpy of drugs, and the thermal test was nearly at equilibrium state due to the extremely slow heating rate used (90). Therefore the achieved solid solubility results could be considered as the thermodynamic solubility of the drug in the polymer. This approach, similar to the melting point depression method, however, may have its intrinsic limitation whereby the predicted solid solubility is only obtained at the temperature close to the melting point of the drug. Therefore there may be physical stability issues if the ASDs are designed based on the solubility predicted by such approach, since the solubility may decrease with decreasing temperature, leading to super-saturated systems at room temperature.
Three possible regions of drug-polymer mixing behavior (90).
Thermal Acceleration Approach
Mahieu et al. reported another approach to estimate the drug solubility in polymer using thermal method (91). In this method, a super-saturated solid dispersion system consisting of indomethacin and PVP K12 was prepared using milling method. The solid dispersion was heated at 120°C in DSC for two hours to completely demix the drug from the solid dispersion, and then followed by re-scanning in DSC from room temperature to detect the Tg. An increased Tg value was detected in the milled samples compared with the Tg value in the fresh and untreated sample. Via Gordon-Taylor equation, the drug concentration in the heat-treated sample can be estimated using the Tg value from DSC re-scanning, and this drug concentration was considered as the solubility of indomethacin in PVP K12. The fundamental concept of this method lies in the fact that demixing of super-saturated ASDs occurs much faster than completely dissolving crystalline drugs into polymers (as illustrated in Fig. 5). Moreover, heat treatment at high temperature to ASDs can accelerate phase separation or recrystallization in ASDs and hence the fraction of super-saturated drug in ASDs can recrystallize out in short time. The remaining amount of drug in ASDs could therefore be considered as the dissolved drug in the polymer. The authors provide a practical approach for the determination of solid solubility in ASDs, and the method does not involve much assumption or complex calculation. Some restrictions, however, may also apply to this method. For instance, although milling method can be used to prepare solid dispersion consisting of drug and PVP, it may not be a general manufacturing process for preparing super-saturated ASDs containing other drug-polymer compositions, and hence limiting the broad application of this method (92).
Time evolutions of glass transition temperature of a drug/polymer mixture when reaching equilibrated state on annealing (redrawn figure from the paper by Mahieu et al.) (91).
Kinetics of the Physical Stability of Amorphous Solid Dispersions
As mentioned above, although formulations with drug loadings above the drug solid solubility in polymers are thermodynamically instable, it is very likely that such formulations can be physically stable over a period of time. If this physically stable time period is longer than the common shelf life of a pharmaceutical product, the super-saturated ASD based products, can still be used clinically. Consequently, it is essential to understand the kinetic stability of ASDs as well as the factors that are associated with phase separation and recrystallization. It has been reported that factors including glass transition temperature of amorphous drugs and ASDs, molecular mobility of amorphous drugs, manufacturing process, physical stability of amorphous drugs and interactions between drugs and polymers, were linked with the kinetics of the physical stability of ASDs (18,93,94,95,96,97,98). These kinetic related factors are discussed in the following sections.
Glass Transition Temperature
The super-cooling method has been one of the most widely used methods for the preparation of amorphous material from its crystalline form (19,21,99,100). The relationship between the thermodynamic properties, such as enthalpy (H) or specific volume (V), and the temperature during the super-cooling process is shown in Fig. 6. For crystalline material at temperature below the melting point (Tm), the enthalpy increases slightly with increasing temperature (100). On increasing the temperature above the Tm, a discontinuous increase in both enthalpy (H) and specific volume (V) at Tm is observed, representing a first-order phase transition from crystalline state to liquid (99). As the melt suffers a rapid cooling process, the enthalpy (H) declines along the extrapolated liquid line, and the melt is formed into super-cooled liquid. As the super-cooled liquid is further cooled to the temperature below the Tg of the material, a break point could be observed at Tg, and the system is transformed into glass state with a significantly increased viscosity (99).
Schematic depiction of the change in enthalpy (H) with temperature for a material undergoing super-cooling process (redrawn figure from the paper by Craig et al.) (99).
At the temperature below Tg, amorphous materials tend to approach the equilibrium (crystal) by releasing the extra enthalpy or configurational entropy, the process of which is defined as structural relaxation (101). During relaxation, amorphous materials could recrystallize at different rates depending on the storage temperature (101). Therefore, discrepancy between the glass transition temperature and the storage temperature can significantly affect the recrystallization rate of amorphous materials and hence increasing the Tg may improve the physical stability of ASDs due to the reduced recrystallization rate (102,103).
Preparing ASDs using polymeric carriers with high Tgs can increase the Tg of ASD to a higher value in comparison to the Tg of pure amorphous drug. The Tg of the system can be predicted using Gordon-Taylor equation (104):
where Tg1, Tg2 and Tgmix represent the Tg (in Kelvin temperature) of compound 1, 2 and the mixture, respectively, w1 and w2 represent the weight fractions of compound 1 and 2, respectively, and K represent a constant. K can be calculated by:
where ρ1 and ρ2 represent the true density of compound 1 and 2, respectively (104). Tg is highly associated with the mole cular mobility of amorphous materials (this is discussed later in the paper), and the increased Tg value (compared with pure amorphous drug) can substantially reduce the molecular mobility of drugs in systems, resulting in a reduced recrystallization rate (105).
Molecular Mobility of Amorphous Drugs
As mentioned above, at the storage temperature lower than Tg, structural relaxation occurs in amorphous materials in the form of releasing extra enthalpy and configurational entropy. The time consumed by structural relaxation is defined as relaxation time. Molecular mobility is reciprocal to the relaxation time. The relaxation time, τ, can be calculated using the Adam-Gibbs model:
where τ0 is a constant, C is a material dependent constant, T is the absolute temperature, and Sc is the configurational entropy (106). Equation (10) can be rewritten into Adam-Gibbs-Vogel equation:
where D is the strength parameter, T0 is the temperature at which molecular mobility is zero, and Tf is the fictive temperature that can usually be replaced by the Tg value of the material as reported in literature (101,107,108).
Molecular mobility is linked with the recrystallization rate of amorphous materials, and hence it can affect the kinetics of phase separation and recrystallization of ASDs. Basically, there are two types of relaxations for amorphous materials, i.e. β- relaxation (local molecular mobility) and α-relaxation (global molecular mobility), which are defined at temperatures lower and higher than the Tg of the amorphous material, respectively (19). At the temperature below Tg, β-relaxation, characterized by the spinning of atoms in single molecule, is the major relaxation for small molecules. For polymeric molecules, β-relaxation refers to the vibration of polymer side chains (109,110). At the temperature above Tg, α-relaxation, characterized by the mobilization of intact molecule, is the dominant relaxation for both amorphous small molecules and polymers (β-relaxation still take place at this temperature) (109,110). It has been reported that α-relaxation and β-relaxation both contributed to the relaxation enthalpy of amorphous indomethacin that stored at room temperature for a certain time period (18,19). In addition, relaxations of drug and polymer in ASDs both make contributions to the physical instability of ASDs on aging (18,19,111,112,113). Amongst these studies, a profound research by Hancock first suggested a “Tg-50 K” rule for storing ASDs, which was achieved via the calculation of molecular mobility (18). In this study, molecular mobility of amorphous drug (indomethacin), polymer (PVP) and amorphous sugar (sucrose) were studied at different storage temperatures (18). It was found that no molecular mobility was detected for each material at the temperature 50 K lower than the individual Tg of each material, and excellent physical stability of amorphous materials was presented by all materials for over a period of years. Such results led to the classic theory that the storage temperature for ASDs should be at least 50 K lower than the Tg of the ASD to minimize molecular mobility of drug moleculesand to enhance the physical stability (18,34). Although the recommended “rule” of “Tg-50 K” is not universal for the storage of ASDs, it indeed demonstrates the correlation between the molecular mobility and the recrystallization rate of amorphous materials. This finding enlightens the formulation development of ASDs that the reduction of molecular mobility can substantially enhance the physical stability of ASDs (114).
Physical Stability of Amorphous Drugs
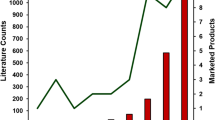
Several studies have reported that the physical stability of amorphous drugs alone also could affect the physical stability of ASDs (73,93,115). For instance, in a study regarding the “glass forming ability” of marketed amorphous drugs, instead of using experimental method i.e. DSC, the researchers applied in silico method to classify the marketed amorphous drugs into different categories based on the chemical space (115). The authors finally suggested that when developing ASD formulations, Class I drugs that had a high recrystallization tendency should be avoided to decrease the formulation risk (115). Similarly, Ng et al. prepared several drug-polymer ASDs containing different drugs including carbamazepine, felodipine, celecoxib and fenofibrate by spin coating method (93). It was confirmed that the more physically stable the amorphous drugs alone, the more physically stable the corresponding ASDs (93). In another paper, carbamazepine, felodipine, celecoxib and fenofibrate were formulated with Eudragit® EPO using hot melt extrusion (73). Amorphous drugs alone with higher physical stability also showed better physical stability of ASDs composed of these drugs (73). In the above two studies, typical preparation processes for solid dispersions including solvent evaporation (spin coating) and melting (hot melt extrusion) approaches were both employed. These results indicate that the physical stability of amorphous drugs alone is consistent with the physical stability of ASDs and is independent of preparation processes.
Although the mechanism of such consistency has not been completely understood, it is likely that kinetic stability of ASDs are dependent on or strongly influenced by the kinetic stability of amorphous drugs alone. Compared with physically stable amorphous drugs, physically instable amorphous drugs intrinsically has a higher recrystallization rate which could only be reduced to a limited level even after being formulated with polymeric carriers. Whereas physically stable amorphous drugs in nature has a slow recrystallization rate that can be further slowed down when being formulated with polymers, leading to higher physical stability of ASDs. The mechanism of the physical stability of amorphous drugs alone, however, has not been fully disclosed, and it may be linked with various properties such as molecular weight, glass forming ability and recrystallization temperature of amorphous drugs as reported in the literature (116,117,118).
Manufacturing Process
As reported in literature, ASDs of the same components but prepared by different processes can present different physical stability (119,120,121). For example, in the paper by Yang et al., felodipine-Eudragit® E PO solid dispersion systems were prepared by hot melt extrusion and spin coating, respectively (98). The spin coated ASDs with drug loadings up to 90% (w/w) only showed low level surface recrystallization after 12 months aging under 75% RH at room temperature. In contrast, hot melt extruded ASDs with 50% and 70% drug loading (aged under the same condition) showed high level surface recrystallization after 6 months as confirmed by SEM and AFM studies (98). Similarly, in the study by Weuts et al., etravirine was prepared into ASDs with HPMC by both film casting and spray drying methods, and the spray dried samples showed higher physical stability than the corresponding film casted samples (119).
Such phenomenon has occurred in other studies, the underpinning mechanism, however, has not been disclosed yet (120,122). It is likely that different preparation processes may generate different super-saturation levels for ASDs. Therefore, kinetically, ASDs with low super-saturation level would exhibit better physical stability (123). This was reported in the study, where super-saturation levels of ASDs prepared by hot melt extrusion were assessed using milling method (Fig. 7) (123). The mechanism of this approach was based on the theory that milling can accelerate phase separation of super-saturated ASDs. In the paper, super-saturated ASDs were prepared by hot melt extrusion, and the extrudates were milled using ball milling for 5 min. It was found that 70% (w/w) extrudates without milling only showed low level phase separation and crystallization, and even after being aged under 75% RH at room temperature for 10 months, the crystallinity of the sample was still under 2.5% (w/w) (estimated using MTDSC). On the contrary, freshly prepared and milled 70% (w/w) extrudates showed high level phase separation and recrystallization, approximately 25% (w/w). In addition, 50% (w/w) milled extrudates also showed phase separation and recrystallization (the crystallinity was circa 5% w/w) after being aged under the same condition for 2 months. By subtracting the amount of recrystallized drug in 50% and 70% (w/w) milled extrudates, the remained drugs in both systems were the physically stable drugs. Surprisingly, the amount of the thermodynamically stable drugs in both systems (50% and 70% w/w) were close, circa 45% (w/w), and this value was higher than the predicted solubility values using three theoretical models (123). Furthermore, crystallinity in both milled systems did not increase on further aging under 75% RH at room temperature up to 6 months. These results indicate that manufacturing process may be capable to reduce super-saturation levels for ASDs, which might create an “apparent” drug-polymer solubility that is higher than the thermodynamic solubility. Therefore, this increased “apparent” drug-polymer solubility can guarantee the physical state of ASDs for a certain time length. Results from this research are also useful for the formulation scientists while developing ASD medicines: when the formulation show poor physical stability, it could be potentially helpful to move to another processing technique.
Illustration of the measurement of process related solid solubility in hot melt extrudates using milling method (123).
Interactions Between Drug and Polymer
Drug-polymer interaction in ASDs has been suggested as one of the key factors contributing to the physical stability of ASDs (69,124). The mechanism of the physical stability enhancement via drug-polymer interaction is mainly attributed to two reasons. Firstly, the drug-polymer interactions, such as hydrogen bonding and acid-base interaction, can reduce the molecular mobility of drugs in ASDs, leading to an enhanced physical stability of ASDs (8,101,125). Secondly, the drug-polymer interactions have been reported to be associated with the drug-polymer miscibility and the drug solubility in polymer (65). In this review, we consider the drug-polymer interaction as the kinetic factor due to the reason that the restriction on molecular mobility via drug-polymer interactions may be the dominant mechanism for the enhanced physical stability (126).
One of the common drug-polymer interactions is hydrogen bonding that is likely to be formed amongst the amine groups (proton donors), carbonyl groups (proton acceptors), and hydroxyl groups (proton donors and accepters). Drugs and polymers containing the above groups tend to form hydrogen bonding in ASDs, which can be characterized using solid state NMR and FT-IR (22,127,128).
Acid-base interaction is another drug-polymer interaction which is also responsible for the enhanced physical stability of ADSs in some case studies (129,130). Similar to the mechanism of hydrogen bonding, acid-base interaction can slow down the phase separation and recrystallization rate by reducing the molecular mobility. However, this interaction may not be generalized when developing ASD formulations, since the acid-base interaction is dependent on the chemical properties of drugs and polymers.
Despite of the effect on reducing molecular mobility, hydrogen bonding may not always be favorable for kinetic stability when using hydrophilic carriers i.e. PVP or PVPVA64 in ASDs (93,131,132). Aged upon exposure to high humidity, ASDs prepared with hydrophilic polymers are likely to absorb moisture (93,133). As illustrated in Fig. 8, the hydrogen bonding between drug and polymer can be disrupted by the moisture absorption since water molecules can act as both strong hydrogen bonding donor and acceptor (93). Consequently, in these systems, phase separation followed by recrystallization is prone to occur. For instance, Qi et al. found that phase separation was detected in felodipine-PVP ASDs within 24 h aged under high humidity (23). Therefore, the formulation strategy of using hydrogen bonding acceptor polymers should be applied carefully, and short time physical stability study under stressed humidity is highly recommended for formulation screening.
Environmental Effects on the Physical Stability of Amorphous Solid Dispersions
Unlike thermodynamic and kinetic aspects that can directly affect the physical stability of ASDs, environmental aspect is indirect influence that could only affect the physical stability of ASDs via affecting the thermodynamic and kinetic factors. Seeing ASDs as systems stored in the normal environment, accordingly the environmental factors are composed of temperature and humidity (134,135,136).
As discussed above, molecular mobility of amorphous materials is associated with temperature in an exponential relationship (18). According to the relationship of Eq. (10) and Eq. (11), the increase of temperature may cause orders of magnitude increase of molecular mobility, leading to a substantially accelerated rate of phase separation and recrystallization of ASDs. Humidity can influence the physical stability through the absorbed water molecules in ASDs. The physical stability can therefore be reduced by moisture uptake through the plasticizing effect and potential of destroying drug-polymer hydrogen bonding, offered by the water molecules (137,138,139). Recently in a research, a novel mechanism of water induced physical instability of ASD was introduced, and in the research, poloxamer 188 was applied as the polymeric carrier in the ASD (16). It was found that physical instability of the ASD was attributed to the drug recrystallization process within absorbed water. Poloxamer 188 was highly hygroscopic and hence a high level water absorption in the system was established to the extent that drugs were found to be dissolved in the absorbed water. Therefore, on aging the ASD started losing water progressively, leading to the recrystallization of the dissolved drugs.
Despite the fact that both factors can affect the physical stability of ASDs, the dominant environment factor, however, has not been revealed yet. The selection of the main physical stability related environmental factor is vitally important, because this would determine the storage condition for ASDs. A report by Tian et al. studied the effect of temperature and humidity on the physical stability of hot melt extruded cinnarizine and Soluplus® (72). Samples were stored at 40°C and 60°C under dry condition, and at 25°C under the humidity of 75% RH and 94% RH, respectively. It was found that humidity and temperature showed similar effect on the physical stability of cinnarizine-Soluplus® system with 20% (w/w) drug loading, but with increased drug loading, samples stored under high humidity presented poorer physical stability. In another study regarding the effect of temperature and humidity, the authors used four model drugs including felodipine, carbamazepine, celecoxib and fenofibrate, to formulate with Eudragit® E PO using hot melt extrusion (73). Melt extrudates were stored under controlled temperature and humidity, and it was found that samples aged under high humidity (75% RH, 25°C) showed higher level crystallization than samples aged at high temperature (0% RH, 40°C). These results can be applied to the ASDs of all four model drugs with both low (10% w/w) and high (70% w/w) drug loadings (73).
From the results of the two reported studies, it may be unacceptable to make the conclusion that humidity has more significant influence on the physical stability of ASDs than temperature. This is because the effect of temperatures was not completely eliminated in both studies. At room temperature (25°C), the contribution from molecular mobility of drugs to the physical instability in ASDs cannot be neglected. These studies, however, still provide useful information that moisture proof should be significantly taken into consideration when developing formulations of ASDs.
In the study regarding the physical stability of ASDs, a polymer blend ASD system was developed to enhance the physical stability of ASDs against stressed humidity (140). The authors took advantage of immiscible polymer blend system to purposely design a phase separated solid dispersion. The hypothesis was that when hydrophobic acid-soluble polymer (i.e. Eudragit® E PO), hydrophilic polymer (i.e. PVP-VA64) and drugs were extruded together, phase separation would occur due to the two types of polymers being immiscible (140). Moreover, asymmetry drug distribution in the system could be generated. This was because hydrophilic polymers that can form hydrogen bonding with the drugs were able to dissolve more drug molecules than the hydrophobic polymers. Therefore, after co-extrusion of the polymer blend and the drug, a phase separated solid dispersion was formed, having a micro-structure similar to “emulsion”. In the solid state “emulsion”, hydrophobic polymers containing small amount of drugs could be the continuous phase (outer phase) and the hydrophilic polymers containing large amount of drugs could be the separated phase. Via the “emulsion” structure, such polymer blend system could effectively block the moisture penetration into the solid dispersions as the outer or continuous phase was completely hydrophobic (the design is illustrated in Fig. 9). Therefore the physical stability of the solid dispersions could be enhanced. Unlike the conventional formulation strategy of using homogeneous solid dispersions, this study provides an insightful formulation strategy of using immiscible for ASDs to improve the physical stability. It is highly likely that, by optimising the ratio of hydrophobic polymers and hydrophilic polymers, the solid “emulsion” ASDs as illustrated in Fig. 9 could be achieved (140).
Mechanism of the improved physical stability against stressed humidity by polymer blend solid dispersions (modified figure from the paper by Qi et al.) (140).
Conclusion
In this review, the physical stability of ASDs are discussed and summarized from a physicochemical perspective and factors that can affect the physical stability are accordingly divided into thermodynamic, kinetic and environmental aspects. The formulation development of ASDs, therefore, may be conducted by following such perspective. For instance, given a specific drug, one may try to screen the polymeric carriers that have the highest drug solubility using theoretical models. Subsequently, the formulation scientists may further use different preparation process to formulate the drug into ASDs and compare the physical stability of different formulations. If possible, the influence of manufacturing process on the super-saturation levels of ASDs should be assessed to approximate the maximum drug loading that can be used. Meanwhile, the physical stability of the amorphous drug alone and other physical characterisation of the amorphous drug should be investigated to predict the kinetics of the physical stability of ASDs. If given a group of drugs to be developed into ASDs, the comparison of physical stability of amorphous drugs alone is recommended to be carried out to estimate the physical stability of ASDs composed of these drugs, and hence screening the suitable drug candidates. Finally, when designing the packing, moisture proof materials should be applied to avoid the moisture uptake by ASDs.
Abbreviations
- API:
-
Active pharmaceutical ingredient
- ASD:
-
Amorphous solid dispersion
- DSC:
-
Differential scanning calorimetry
- FDA:
-
Food and drug administration
- FT-IR:
-
Fourier transform infrared spectroscopy
- HPMCAS:
-
Hydroxypropyl cellulose acetate succinate
- MTDSC:
-
Modulated temperature differential scanning calorimetry
- NMR:
-
Nuclear magnetic resonance spectroscopy
- PC-SAFT:
-
Perturbed-chain statistical associating fluid theory
- PEG:
-
Polyethylene glycol
- PLGA:
-
Poly lactic-co-glycolic acid
- PVP:
-
Polyvinylpyrrolidone
- PVP K12:
-
Polyvinylpyrrolidone (Mw = 3500)
- PVPVA64:
-
Vinylpyrrolidone-vinyl acetate copolymer[60:40]
- Tg :
-
Glass transition temperature
- Vitamin E TPGS :
-
D-α-tocopheryl polyethylene glycol succinate
References
Sekiguchi K, Obi N. Studies on absorption of eutectic mixture. I. A comparison of the behavior of eutectic mixture of sulfathiazole and that of ordinary sulfathiazole in man. Chem Pharm Bull. 1961;9(11):866–72.
Goldberg AH, Gibaldi M, Kanig JL, Mayersohn M. Increasing dissolution rates and gastrointestinal absorption of drugs via solid solutions and eutectic mixtures. Iv. Chloramphenicol--urea system. J Pharm Sci. 1966;55(6):581–3.
Suzuki H, Yakushiji K, Matsunaga S, Yamauchi Y, Seto Y, Sato H, et al. Amorphous solid dispersion of meloxicam enhanced oral absorption in rats with impaired gastric motility. J Pharm Sci. 2018;107(1):446–52.
Ohyagi N, Ueda K, Higashi K, Yamamoto K, Kawakami K, Moribe K. Synergetic role of hypromellose and methacrylic acid copolymer in the dissolution improvement of amorphous solid dispersions. J Pharm Sci. 2017;106(4):1042–50.
Weerapol Y, Limmatvapirat S, Nunthanid J, Konthong S, Suttiruengwong S, Sriamornsak P. Development and characterization of nifedipine-amino methacrylate copolymer solid dispersion powders with various adsorbents. Asian J Pharm Sci. 2017;12(4):335–43.
Weerapol Y, Tubtimsri S, Jansakul C, Sriamornsak P. Improved dissolution of kaempferia parviflora extract for oral administration by preparing solid dispersion via solvent evaporation. Asian J Pharm Sci. 2017;12(2):124–33.
Amidon GL, Lennernäs H, Shah VP, Crison JRA. theoretical basis for a biopharmaceutic drug classification: the correlation of in vitro drug product dissolution and in vivo bioavailability. Pharm Res. 1995;12(3):413–20.
Yu L. Amorphous pharmaceutical solids: Preparation, characterization and stabilization. Adv Drug Deliv Rev. 2001;48(1):27–42.
Vasconcelos T, Marques S, das Neves J, Sarmento B. Amorphous solid dispersions: rational selection of a manufacturing process. Adv Drug Deliv Rev. 2016;100:85–101.
Singh A, Mooter GVD. Spray drying formulation of amorphous solid dispersions. Adv Drug Deliv Rev. 2016;100:27–50.
Hancock BC, Parks M. What is the true solubility advantage for amorphous pharmaceuticals? Pharm Res. 2000;17(4):397–404.
DeBoyace K, Wildfong PLD. The application of modeling and prediction to the formation and stability of amorphous solid dispersions. J Pharm Sci. 2018;107(1):57–74.
Khougaz K, Clas SD. Crystallization inhibition in solid dispersions of mk-0591 and poly(vinylpyrrolidone) polymers. J Pharm Sci. 2000;89(10):1325–34.
Crowley MM, Zhang F, Koleng JJ, McGinity JW. Stability of polyethylene oxide in matrix tablets prepared by hot-melt extrusion. Biomaterials. 2002;23(21):4241–8.
Chiou D, Langrish TAG. Crystallization of amorphous components in spray-dried powders. Dry Technol. 2007;25(9):1427–35.
Wu Q, Kennedy MT, Nagapudi K, Kiang YH. Humidity induced phase transformation of poloxamer 188 and its effect on physical stability of amorphous solid dispersion of amg 579, a pde10a inhibitor. Int J Pharm. 2017;521(1–2):1–7.
Zhu DA, Zografi G, Gao P, Gong Y, Zhang GG. Modeling physical stability of amorphous solids based on temperature and moisture stresses. J Pharm Sci. 2016;105(9):2932–9.
Hancock BC, Shamblin SL, Zografi G. Molecular mobility of amorphous pharmaceutical solids below their glass transition temperatures. Pharm Res. 1995;12(6):799.
Hancock BC, Zograf G. Characteristics and significance of the amorphous state in pharmaceutical systems. J Pharm Sci. 1997;86(1):1–12.
Andronis V, Zografi G. The molecular mobility of supercooled amorphous indomethacin as a function of temperature and relative humidity. Pharm Res. 1998;15(6):835–42.
Saiter JM, Grenet J, Dargent E, Saiter A, Delbreilh L. Glass transition temperature and value of the relaxation time at tg in vitreous polymers. Macromol Symp. 2007;258(1):152–61.
Huang J, Wigent RJ, Schwartz JB. Drug-polymer interaction and its significance on the physical stability of nifedipine amorphous dispersion in microparticles of an ammonio methacrylate copolymer and ethylcellulose binary blend. J Pharm Sci. 2008;97(1):251–62.
Qi S, Moffat JG, Yang Z. Early stage phase separation in pharmaceutical solid dispersion thin films under high humidity: Improved spatial understanding using probe-based thermal and spectroscopic nanocharacterization methods. Mol Pharm. 2013;10(3):918–30.
Singh A, Bharati A, Frederiks P, Verkinderen O, Goderis B, Cardinaels R, et al. Effect of compression on the molecular arrangement of itraconazole–soluplus solid dispersions: Induction of liquid crystals or exacerbation of phase separation? Mol Pharm. 2016;13(6):1879.
Knopp MM, Tajber L, Tian Y, Olesen NE, Jones DS, Kozyra A, et al. Comparative study of different methods for the prediction of drug–polymer solubility. Mol Pharm. 2015;12(9):3408–19.
Huang Y, Dai WG. Fundamental aspects of solid dispersion technology for poorly soluble drugs. Acta Pharm Sin B. 2014;4(1):18–25.
Meng F, Gala U, Chauhan H. Classification of solid dispersions: Correlation to (i) stability and solubility (ii) preparation and characterization techniques. Drug Dev Ind Pharm. 2015;41(9):1401–15.
Janssens S, GVd M. Review: Physical chemistry of solid dispersions. J Pharm Pharmacol. 2009;61(12):1571–86.
Listed N. The use of amorphous solid dispersions: A formulation strategy to overcome poor solubility and dissolution rate. Drug Discov Today. 2012;9(2):e71.
Vo LN, Park C, Lee BJ. Current trends and future perspectives of solid dispersions containing poorly water-soluble drugs. Eur J Pharm Biopharm. 2013;85(3):799–813.
Van Duong T, Van den Mooter G. The role of the carrier in the formulation of pharmaceutical solid dispersions. Part i: crystalline and semi-crystalline carriers. Expert Opin Drug Del. 2016;13(11):1583–94.
Van Duong T, Van den Mooter G. The role of the carrier in the formulation of pharmaceutical solid dispersions. Part ii: Amorphous carriers. Expert Opin Drug Del. 2016;13(12):1681–94.
Purohit HS, Taylor LS. Phase separation kinetics in amorphous solid dispersions upon exposure to water. Mol Pharm. 2015;12(5):1623–35.
Qian F, Huang J, Hussain MA. Drug-polymer solubility and miscibility: stability consideration and practical challenges in amorphous solid dispersion development. J Pharm Sci. 2010;99(7):2941–7.
Knopp MM, Olesen NE, Holm P, Langguth P, Holm R, Rades T. Influence of polymer molecular weight on drug–polymer solubility: a comparison between experimentally determined solubility in pvp and prediction derived from solubility in monomer. J Pharm Sci. 2015;104(9):2905–12.
Paudel A, Van Humbeeck J, Van den Mooter G. Theoretical and experimental investigation on the solid solubility and miscibility of naproxen in poly(vinylpyrrolidone). Mol Pharm. 2010;7(4):1133–48.
Jog R, Gokhale R, Burgess DJ. Solid state drug-polymer miscibility studies using the model drug abt-102. Int J Pharm. 2016;509(1–2):285–95.
Piccinni P, Tian YW, McNaughton A, Fraser J, Brown S, Jones DS, et al. Solubility parameter-based screening methods for early-stage formulation development of itraconazole amorphous solid dispersions. J Pharm Pharmacol. 2016;68(5):705–20.
Li N, Taylor LS. Nanoscale infrared, thermal, and mechanical characterization of telaprevir-polymer miscibility in amorphous solid dispersions prepared by solvent evaporation. Mol Pharm. 2016;13(3):1123–36.
Maniruzzaman M, Pang J, Morgan DJ, Douroumis D. Molecular modeling as a predictive tool for the development of solid dispersions. Mol Pharm. 2015;12(4):1040–9.
Fedors RF. A method for estimating both the solubility parameters and molar volumes of liquids. Polym Eng Sci. 1974;14(2):147–54.
Sunwoo C, Eisen H. Solubility parameter of selected sulfonamides. J Pharm Sci. 1971;60(2):238–44.
Greenhalgh DJ, Williams AC, Timmins P, York P. Solubility parameters as predictors of miscibility in solid dispersions. J Pharm Sci. 1999;88(11):1182–90.
Albers J, Matthee K, Knop K, Kleinebudde P. Evaluation of predictive models for stable solid solution formation. J Pharm Sci. 2011;100(2):667–80.
Hansen CM. The universality of the solubility parameter. Ind Eng Chem Prod Res Dev. 1969;8(1):2–11.
Yani Y, Kanaujia P, Chow PS, Tan RBH. Effect of api-polymer miscibility and interaction on the stabilization of amorphous solid dispersion: a molecular simulation study. Ind Eng Chem Res. 2017;56(44):12698–707.
Liu J, Cao F, Zhang C, Ping Q. Use of polymer combinations in the preparation of solid dispersions of a thermally unstable drug by hot-melt extrusion. Acta Pharm Sin B. 2013;3(4):263–72.
Meng F, Dave V, Chauhan H. Qualitative and quantitative methods to determine miscibility in amorphous drug–polymer systems. Eur J Pharm Sci. 2015;77:106–11.
Yoo SU, Krill SL, Wang Z, Telang C. Miscibility/stability considerations in binary solid dispersion systems composed of functional excipients towards the design of multi-component amorphous systems. J Pharm Sci. 2009;98(12):4711–23.
Barton AFM. Solubility parameters. Chem Rev. 1975;75(6):731–53.
Bugay DE. Characterization of the solid-state: spectroscopic techniques. Adv Drug Deliv Rev. 2001;48(1):43–65.
Ewing AV, Clarke GS, Kazarian SG. Stability of indomethacin with relevance to the release from amorphous solid dispersions studied with atr-ftir spectroscopic imaging. Eur J Pharm Sci. 2014;60(1449):64–71.
Paudel A, Geppi M, Mooter GVD. Structural and dynamic properties of amorphous solid dispersions: The role of solid-state nuclear magnetic resonance spectroscopy and relaxometry. J Pharm Sci. 2014;103(9):2635–62.
Li J, Zhao J, Tao L, Wang J, Waknis V, Pan D, et al. The effect of polymeric excipients on the physical properties and performance of amorphous dispersions: Part i, free volume and glass transition. Pharm Res. 2015;32(2):500–15.
Penumetcha SS, Gutta LN, Dhanala H, Yamili S, Challa S, Rudraraju S, et al. Hot melt extruded aprepitant-soluplus® solid dispersion: preformulation considerations, stability and in-vitro study. Drug Dev Ind Pharm. 2016;42(10):1609–20.
Baird JA, Taylor LS. Evaluation of amorphous solid dispersion properties using thermal analysis techniques. Adv Drug Deliv Rev. 2012;64(5):396.
Gupta J, Nunes C, Vyas S, Jonnalagadda S. Prediction of solubility parameters and miscibility of pharmaceutical compounds by molecular dynamics simulations. J Phys Chem B. 2011;115(9):2014–23.
M M DJM, AP M JP, MJ S DD. Drug-polymer intermolecular interactions in hot-melt extruded solid dispersions. Int J Pharm. 2013;443(1–2):199.
Papantonopoulos SA. In silico modelling of drug-polymer interactions for pharmaceutical formulations. J R Soc Interface. 2010;7 Suppl 4(Suppl_4):S423.
Ouyang D. Investigating the molecular structures of solid dispersions by the simulated annealing method. Chem Phys Lett. 2012;554(554):177–84.
Li N, Gilpin CJ, Taylor LS. Understanding the impact of water on the miscibility and microstructure of amorphous solid dispersions: an afm–lcr and tem–edx study. Mol Pharm. 2017;14(5):1691–705.
Baghel S, Cathcart H, O'Reilly NJ. Polymeric amorphous solid dispersions: A review of amorphization, crystallization, stabilization, solid-state characterization, and aqueous solubilization of biopharmaceutical classification system class ii drugs. J Pharm Sci. 2016;47(42):2527–44.
Nishi T, Wang TT. Melting point depression and kinetic effects of cooling on crystallization in poly(vinylidene fluoride)-poly(methyl methacrylate) mixtures. Macromolecules. 2006;8(6):909–15.
Flory PJ. Principles of polymer chemistry. Ithaca: Cornell University Press; 1953.
Marsac PJ, Shamblin SL, Taylor LS. Theoretical and practical approaches for prediction of drug-polymer miscibility and solubility. Pharm Res. 2006;23(10):2417–26.
Pina MF, Zhao M, Pinto JF, Sousa JJ, Craig DQ. The influence of drug physical state on the dissolution enhancement of solid dispersions prepared via hot-melt extrusion: a case study using olanzapine. J Pharm Sci. 2014;103(4):1214–23.
Nishi T, Wang TT. Melting point depression and kinetic effects of cooling on crystallization in poly(vinylidene fluoride)-poly(methyl methacrylate) mixtures. Macromolecules. 1975;8(6):909–15.
Yi T, Wan J, Xu H, Yang X. A new solid self-microemulsifying formulation prepared by spray-drying to improve the oral bioavailability of poorly water soluble drugs. Eur J Pharm Biopharm. 2008;70(2):439–44.
Rumondor ACF, Ivanisevic I, Bates S, Alonzo DE, Taylor LS. Evaluation of drug-polymer miscibility in amorphous solid dispersion systems. Pharm Res. 2009;26(11):2523–34.
Verma S, Rudraraju VS. A systematic approach to design and prepare solid dispersions of poorly water-soluble drug. AAPS PharmSciTech. 2014;15(3):641–57.
Thakral S, Thakral NK. Prediction of drug-polymer miscibility through the use of solubility parameter based flory-huggins interaction parameter and the experimental validation: peg as model polymer. J Pharm Sci. 2013;102(7):2254–63.
Tian YW, Jones DS, Andrews GP. An investigation into the role of polymeric carriers on crystal growth within amorphous solid dispersion systems. Mol Pharm. 2015;12(4):1180–92.
Yang Z, Nollenberger K, Albers J, Craig D, Qi S. Molecular indicators of surface and bulk instability of hot melt extruded amorphous solid dispersions. Pharm Res. 2015;32(4):1210–28.
Zhao Y, Inbar P, Chokshi HP, Malick AW, Choi DS. Prediction of the thermal phase diagram of amorphous solid dispersions by flory-huggins theory. J Pharm Sci. 2011;100(8):3196–207.
Prudic A, Ji Y, Sadowski G. Thermodynamic phase behavior of api/polymer solid dispersions. Mol Pharm. 2014;11(7):2294–304.
Schäfer E, Sadowski G. Liquid–liquid equilibria of systems with linear aldehydes. experimental data and modeling with pcp-saft. Ind Eng Chem Res. 2012;51(44):14525–34.
Gross J, Sadowski G. Application of the perturbed-chain saft equation of state to associating systems. Ind Eng Chem Res. 2002;41(22):5510–5.
Prudic A, Lesniak AK, Ji Y, Sadowski G. Thermodynamic phase behaviour of indomethacin/plga formulations. Eur J Pharm Biopharm. 2015;93:88–94.
Gross J, Spuhl O, Tumakaka F, Sadowski G. Modeling copolymer systems using the perturbed-chain saft equation of state. Ind Eng Chem Res. 2003;42(6):1266–74.
Kouskoumvekaki IA, von Solms N, Lindvig T, Michelsen ML, Kontogeorgis GM. Novel method for estimating pure-component parameters for polymers: application to the pc-saft equation of state. Ind Eng Chem Res. 2004;43(11):2830–8.
Luebbert C, Sadowski G. Moisture-induced phase separation and recrystallization in amorphous solid dispersions. Int J Pharm. 2017;532(1):635–46.
Prudic A, Ji Y, Luebbert C, Sadowski G. Influence of humidity on the phase behavior of api/polymer formulations. Eur J Pharm Biopharm. 2015;94:352–62.
Luebbert C, Huxoll F, Sadowski G. Amorphous-amorphous phase separation in api/polymer formulations. Molecules. 2017;22(2)
Yang M, Wang P, Huang CY, Ku MS, Liu HJ, Gogos C. Solid dispersion of acetaminophen and poly(ethylene oxide) prepared by hot-melt mixing. Int J Pharm. 2010;395(1–2):53–61.
Maru SM, de Matas M, Kelly A, Paradkar A. Characterization of thermal and rheological properties of zidovidine, lamivudine and plasticizer blends with ethyl cellulose to assess their suitability for hot melt extrusion. Eur J Pharm Sci. 2011;44(4):471–8.
Amharar Y, Curtin V, Gallagher KH, Healy AM. Solubility of crystalline organic compounds in high and low molecular weight amorphous matrices above and below the glass transition by zero enthalpy extrapolation. Int J Pharm. 2014;472(1–2):241–7.
Gramaglia D, Conway BR, Kett VL, Malcolm RK, Batchelor HK. High speed dsc (hyper-dsc) as a tool to measure the solubility of a drug within a solid or semi-solid matrix. Int J Pharm. 2005;301:1–2):1-5.
Ford JL, Mann TE. Fast-scan dsc and its role in pharmaceutical physical form characterisation and selection. Adv Drug Deliv Rev. 2012;64(5):422–30.
Jones DS, Tian Y, Abu-Diak O, Andrews GP. Pharmaceutical applications of dynamic mechanical thermal analysis. Adv Drug Deliv Rev. 2012;248(5):440–8.
Qi S, Belton P, Nollenberger K, Clayden N, Reading M, Craig DQM. Characterisation and prediction of phase separation in hot-melt extruded solid dispersions: a thermal, microscopic and nmr relaxometry study. Pharm Res. 2010;27(9):1869–83.
Mahieu A, Willart JF, Dudognon E, Danede F, Descamps M. A new protocol to determine the solubility of drugs into polymer matrixes. Mol Pharm. 2013;10(2):560–6.
Al-Obaidi H, Lawrence MJ, Shah S, Moghul H, Al-Saden N, Bari F. Effect of drug-polymer interactions on the aqueous solubility of milled solid dispersions. Int J Pharm. 2013;446(1–2):100–5.
Ng YC, Yang ZY, McAuley WJ, Qi S. Stabilisation of amorphous drugs under high humidity using pharmaceutical thin films. Eur J Pharm Biopharm. 2013;84(3):555–65.
Yoshioka M, Hancock BC, Zografi G. Crystallization of indomethacin from the amorphous state below and above its glass-transition temperature. J Pharm Sci. 1994;83(12):1700–5.
Duddu SP, DalMonte PR. Effect of glass transition temperature on the stability of lyophilized formulations containing a chimeric therapeutic monoclonal antibody. Pharm Res. 1997;14(5):591–5.
Bergese P, Colombo I, Gervasoni D, Depero LE. Melting of nanostructured drugs embedded into a polymeric matrix. J Phys Chem B. 2004;108(40):15488–93.
Z A AP. G VdM. Can compression induce demixing in amorphous solid dispersions? A case study of naproxen-pvp k25. Eur J Pharm Biopharm. 2012;81(1):207.
Yang ZY, Nollenberger K, Albers J, Moffat J, Craig D, Qi S. The effect of processing on the surface physical stability of amorphous solid dispersions. Eur J Pharm Biopharm. 2014;88(3):897–908.
Craig DQM, Royall PG, Kett VL, Hopton ML. The relevance of the amorphous state to pharmaceutical dosage forms: glassy drugs and freeze dried systems. Int J Pharm. 1999;179(2):179–207.
Hilden LR, Morris KR. Physics of amorphous solids. J Pharm Sci. 2004;93(1):3–12.
Aso Y, Yoshioka S, Kojima S. Molecular mobility-based estimation of the crystallization rates of amorphous nifedipine and phenobarbital in poly(vinylpyrrolidone) solid dispersions. J Pharm Sci. 2004;93(2):384–91.
Roudaut G, Simatos D, Champion D, Contreras-Lopez E, Meste ML. Molecular mobility around the glass transition temperature: a mini review. Innovative Food Sci Emerg Technol. 2004;5(2):127–34.
Mehta M, Kothari K, Ragoonanan V, Suryanarayanan R. Effect of water on molecular mobility and physical stability of amorphous pharmaceuticals. Mol Pharm. 2016;13(4):1339–46.
Gordon JM, Rouse GB, Gibbs JH, Jr WMR. The composition dependence of glass transition properties. J Chem Phys. 1977;66(11):4971–6.
Alhalaweh A, Alzghoul A, Mahlin D, Bergström CA. Physical stability of drugs after storage above and below the glass transition temperature: relationship to glass-forming ability. Int J Pharm. 2015;495(1):312–7.
Hodge IM. Effects of annealing and prior history on enthalpy relaxation in glassy polymers. 6. Adam-gibbs formulation of nonlinearity. Macromolecules. 1987;20(11):2897–908.
Claudy P, Jabrane S, Létoffé JM. Annealing of a glycerol glass: Enthalpy, fictive temperature and glass transition temperature change with annealing parameters. Thermochim Acta. 1997;293(293):1–11.
Badrinarayanan P, Zheng W, Li QX, Simon SL. The glass transition temperature versus the fictive temperature. J Non-Cryst Solids. 2007;353(26):2603–12.
Bohmer R, Ngai KL, Angell CA, Plazek DJ. Nonexponential relaxations in strong and fragile glass formers. J Chem Phys. 1993;99(5):4201–9.
Craig DQM, Barsnes M, Royall PG, Kett VL. An evaluation of the use of modulated temperature dsc as a means of assessing the relaxation behaviour of amorphous lactose. Pharm Res. 2000;17(6):696–700.
Viciosa MT, Ramos JJM, Diogo HP. The slow relaxation dynamics in the amorphous pharmaceutical drugs cimetidine, nizatidine, and famotidine. J Pharm Sci. 2016;105(12):3573–84.
Tripathi P, Romanini M, Tamarit JL, Macovez R. Collective relaxation dynamics and crystallization kinetics of the amorphous biclotymol antiseptic. Int J Pharm. 2015;495(1):420–7.
Shete G, Khomane KS, Bansal AK. Molecular relaxation behavior and isothermal crystallization above glass transition temperature of amorphous hesperetin. J Pharm Sci. 2014;103(1):167–78.
Alem N, Beezer AE, Gaisford S. Quantifying the rates of relaxation of binary mixtures of amorphous pharmaceuticals with isothermal calorimetry. Int J Pharm. 2010;399(1–2):12–8.
Wyttenbach N, Kuentz M. Glass-forming ability of compounds in marketed amorphous drug products. Eur J Pharm Biopharm. 2017;112:204–8.
Edueng K, Mahlin D, Larsson P, Bergstrom CAS. Mechanism-based selection of stabilization strategy for amorphous formulations: insights into crystallization pathways. J Control Release. 2017;256:193–202.
Mahlin D, Bergstrom CA. Early drug development predictions of glass-forming ability and physical stability of drugs. Eur J Pharm Sci. 2013;49(2):323–32.
Hellrup J, Alderborn G, Mahlin D. Inhibition of recrystallization of amorphous lactose in nanocomposites formed by spray-drying. J Pharm Sci. 2015;104(11):3760–9.
Weuts I, Van Dycke F, Voorspoels J, De Cort S, Stokbroekx S, Leemans R, et al. Physicochemical properties of the amorphous drug, cast films, and spray dried powders to predict formulation probability of success for solid dispersions: Etravirine. J Pharm Sci. 2011;100(1):260–74.
Karmwar P, Graeser K, Gordon KC, Strachan CJ, Rades T. Investigation of properties and recrystallisation behaviour of amorphous indomethacin samples prepared by different methods. Int J Pharm. 2011;417(1–2):94–100.
Joe JH, Lee WM, Park YJ, Joe KH, Oh DH, Seo YG, et al. Effect of the solid-dispersion method on the solubility and crystalline property of tacrolimus. Int J Pharm. 2010;395(1):161–6.
Benes M, Pekarek T, Beranek J, Havlicek J, Krejcik L, Simek M, et al. Methods for the preparation of amorphous solid dispersions - a comparative study. J Drug Deliv Sci Tec. 2017;38:125–34.
Yang ZY, Nollenberger K, Albers J, Qi S. Molecular implications of drug-polymer solubility in understanding the destabilization of solid dispersions by milling. Mol Pharm. 2014;11(7):2453–65.
Li J, Fan N, Wang X, Li C, Sun M, Wang J, et al. Interfacial interaction track of amorphous solid dispersions established by water-soluble polymer and indometacin. Eur J Pharm Sci. 2017;106:244–53.
Ueda H, Aikawa S, Kashima Y, Kikuchi J, Ida Y, Tanino T, et al. Anti-plasticizing effect of amorphous indomethacin induced by specific intermolecular interactions with pva copolymer. J Pharm Sci. 2014;103(9):2829–38.
Wang B, Wang D, Zhao S, Huang X, Zhang J, Lv Y, et al. Evaluate the ability of pvp to inhibit crystallization of amorphous solid dispersions by density functional theory and experimental verify. Eur J Pharm Sci. 2017;96:45–52.
Tobyn M, Brown J, Dennis AB, Fakes M, Gao Q, Gamble J, et al. Amorphous drug-pvp dispersions: application of theoretical, thermal and spectroscopic analytical techniques to the study of a molecule with intermolecular bonds in both the crystalline and pure amorphous state. J Pharm Sci. 2009;98(9):3456–68.
Tang XC, Pikal MJ, Taylor LS. A spectroscopic investigation of hydrogen bond patterns in crystalline and amorphous phases in dihydropyridine calcium channel blockers. Pharm Res. 2002;19(4):477–83.
Telang C, Mujumdar S, Mathew M. Improved physical stability of amorphous state through acid base interactions. J Pharm Sci. 2009;98(6):2149–59.
Song Y, Zemlyanov D, Chen X, Su Z, Nie H, Lubach JW, et al. Acid-base interactions in amorphous solid dispersions of lumefantrine prepared by spray-drying and hot-melt extrusion using x-ray photoelectron spectroscopy. Int J Pharm. 2016;514(2):456–64.
Mahlin D, Berggren J, Alderborn G, Engstrom S. Moisture-induced surface crystallization of spray-dried amorphous lactose particles studied by atomic force microscopy. J Pharm Sci. 2004;93(1):29–37.
Lehmkemper K, Kyeremateng SO, Heinzerling O, Degenhardt M, Sadowski G. Long-term physical stability of pvp- and pvpva-amorphous solid dispersions. Mol Pharm. 2017;14(1):157–71.
Konno H, Taylor LS. Influence of different polymers on the crystallization tendency of molecularly dispersed amorphous felodipine. J Pharm Sci. 2006;95(12):2692–705.
Wlodarski K, Sawicki W, Kozyra A, Tajber L. Physical stability of solid dispersions with respect to thermodynamic solubility of tadalafil in pvp-va. Eur J Pharm Biopharm. 2015;96:237–46.
Li WJ, Buckton G. Using dvs-nir to assess the water sorption behaviour and stability of a griseofulvin/pvp k30 solid dispersion. Int J Pharm. 2015;495(2):999–1004.
Choi JS. Enhanced stability and solubility of ph-dependent drug, telmisartan achieved by solid dispersion. J Drug Deliv Sci Tec. 2017;37:194–203.
Lamm MS, Simpson A, Mcnevin M, Frankenfeld C, Nay R, Variankaval N. Probing the effect of drug loading and humidity on the mechanical properties of solid dispersions with nanoindentation: antiplasticization of a polymer by a drug molecule. Mol Pharm. 2012;9(11):3396.
Lehmkemper K, Kyeremateng SO, Bartels M, Degenhardt M, Sadowski G. Physical stability of api/polymer-blend amorphous solid dispersions. Eur J Pharm Biopharm. 2018;124:147–57.
Rumondor AC, Stanford LA, Taylor LS. Effects of polymer type and storage relative humidity on the kinetics of felodipine crystallization from amorphous solid dispersions. Pharm Res. 2009;26(12):2599.
Yang Z, Nollenberger K, Albers J, Craig D, Qi S. Microstructure of an immiscible polymer blend and its stabilization effect on amorphous solid dispersions. Mol Pharm. 2013;10(7):2767–80.
ACKNOWLEDGMENTS AND DISCLOSURES
The authors would like to thank Dr. Sheng Qi at University of East Anglia for the previous discussion. This work is supported by the National Natural Science Foundation of China [Grant numbers 81,603,059]; “Jiangsu Shuangchuang” Program; and Top-notch Academic Programs Project of Jiangsu Higher Education Institutions [Grant numbers PPZY2015B146].
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Lin, X., Hu, Y., Liu, L. et al. Physical Stability of Amorphous Solid Dispersions: a Physicochemical Perspective with Thermodynamic, Kinetic and Environmental Aspects. Pharm Res 35, 125 (2018). https://doi.org/10.1007/s11095-018-2408-3
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s11095-018-2408-3