Abstract
Chronic cerebral hypoperfusion (CCH) contributes to the Alzheimer’s-like pathogenesis, but the relationship between CCH and the occurrence of Alzheimer’s disease (AD) remains obscure. The aim is to elucidate the potential pathophysiological mechanism in the field of amyloid-beta (Aβ) pathology induced by CCH. A rat model of CCH has been developed with permanent bilateral occlusion of common carotid arteries (BCCAO). The cognitive function of rats was tested by the Morris water maze. The levels of Aβ (Aβ40 and Aβ42) and soluble amyloid precursor protein (sAPP: sAPPα and sAPPβ) were determined by enzyme linked immunosorbent assay. The expression of beta-site amyloid precursor protein cleaving enzyme 1 (BACE1), presenilin1 (PS1), nicastrin (NCT), anterior pharynx-defective 1alpha (Aph-1α) and presenilin enhancer 2 (Pen-2), sAPPα and sAPPβ were detected by Western blotting. Morris water maze test showed that CCH induced decline in learning and memory related to Aβ levels in the hippocampus. The levels of sAPPα, ADAM10 and ADAM17 in the hippocampus of CCH rats were higher than the control ones (P < 0.05); the levels of sAPPβ, BACE and BACE1 increased more than the control ones (P < 0.05). CCH intervention (1-week or 4-week) markedly increased the expression of PS1, Aph-1α and Pen-2 in the hippocampus of rats, but had no effect on NCT. CCH contributed to cognitive impairment and altered the amyloidogenic and non-amyloidogenic pathway of APP processing by boosting the activity of β-secretase/γ-secretase and α-secretase respectively. The non-amyloidogenic pathway can’t overcome the damage role of the amyloidogenic pathway in the process of chronic cerebral hypoperfusion which promotes amyloid-beta pathogenesis.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Alzheimer’s disease (AD) is an age-related neurodegenerative disorder that is the most common cause of dementia among older adults. Multiple pathogenic hypotheses have been put forward, including amyloid the theory of extracellular amyloid-beta peptide (Aβ) deposition [1], intracellular accumulation of hyperphosphorylated tau protein (formation of neurofibrillary tangles) [2, 3], cholinergic hypothesis [4], neuroinflammation and oxidative stress [5, 6]. It is well known that the Aβ hypothesis is the most classical pathological feature among them [7, 8]. Aβ generation and deposition represents the triggering role in the pathogenesis of AD [9].
Aβ generated from amyloid precursor protein (APP) by sequential actions of two proteolytic enzymes (β-secretase and γ-secretase) [7]. β-secretase indicates the beta-amyloid precursor protein cleavage enzyme (BACE) which mainly includes BACE1 and BACE2 [10, 11]. BACE1 is responsible for the chief function of β-secretase for processing APP [12, 13]. γ-secretase is an enzyme complex and its main components include the amino- and carboxy-terminal fragments of presenilin 1 (PS1), a highly glycosylated form of nicastrin (NCT), anterior pharynx-defective 1alpha (Aph-1α), and presenilin enhancer 2 (Pen-2) [12, 14]. γ-secretase plays a critical role in the Aβ generation [12, 14].
Studies have implicated that impaired cerebral blood flow is correlated with cognitive impairment and chronic neurodegenerative process [15, 16]. It has been reported that cerebral blood flow can better represent perfusion abnormalities in predementia stages of AD than cerebral blood volume [17]. Chronic cerebral hypoperfusion (CCH) is a common impaired cerebral blood supply that promotes the synthesis of Aβ [18]. Even CCH may act as a severity marker of AD and a biomarker of preclinical AD [19, 20]. Previously, we found that CCH results in cognitive impairment and the occurrence of Alzheimer’s-like pathogenesis mediated by upregulation of BACE1 and Aβ in the hippocampus [12]. However, the role of CCH in Aβ pathology remains unclear. The purpose of this study is to investigate whether CCH is involved in regulating the activity of γ-secretase. This study found that CCH enhanced both the non-amyloidogenic and amyloidogenic pathway. CCH contributed to cognitive impairment related to Aβ levels. CCH promoted the amyloidogenic pathway through increasing the activity of both β-secretase and γ-secretase. The general neuro-pathological presentation induced by CCH-insult may be attributed to the imbalance between the non-amyloidogenic and amyloidogenic pathway. The cognitive damage may be the results that the pathological role of the amyloidogenic pathway overrides the non-amyloidogenic pathway in the process of CCH-condition. This study elucidates the potential mechanisms that CCH results in cognitive impairment and the amyloidogenic pathway of APP processing by boosting the activity of both β-secretase and γ-secretase.
Materials and Methods
Animal Model
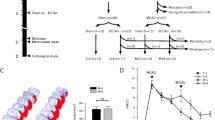
Sprague Dawley (SD) rats (female, weighting 250–300 g) were obtained from the Animal Experimental Center of Hubei University of Medicine (Shiyan, Hubei province, China). All uses of experimental animals were conducted with protocols that were approved by the Institutional Animal Care and Use Committee of Hubei University of Medicine. Ten-month-old SD rats were housed in individual cages at constant temperature (25 °C) under with a 12/12 h light/dark cycle and with free access to food and water. All rats were habituated to the hanging cage for 5 days before the experiments. A rat model of chronic cerebral hypoperfusion (CCH) has been developed with permanent bilateral occlusion of common carotid arteries (BCCAO). Rats were randomly divided into three groups. The 1-week CCH group rats (n = 10) and 4-week CCH group rats (n = 10) were subjected to permanent bilateral occlusion of both common carotid arteries after 5 days adaptation, and the control rats (n = 10) underwent the same surgery procedure without vessel occlusion. The BCCAO was performed by permanent vessel double ligation under general anesthesia with 10% chloral hydrate (350 mg/kg) intraperitoneally and allowed to breathe spontaneously throughout the surgical procedure. A midline incision was done to expose both common carotid arteries. The artery was gently isolated from the carotid sheath and vagus nerve and both common carotid arteries was ligated with non-absorbable 6–0 black silk suture. The rats were sent back into their cages with free access to water and food after the midline incision was closed.
Morris Water Maze Task
Morris water maze (MWM) was performed extensively in the study of the neurobiology and neuropharmacology of spatial learning and memory. The procedure of the MWM test was recorded with Morris Image System (Shanghai DOiT Industrial Co., Ltd.). The MWM test was performed in a circular white pool (a diameter of 180 cm and a height of 60 cm) with white milk water and at a fixed range of water temperature (20 ± 1 °C). The pool was divided into four quadrants (Quadrant A, B, C and D), and the escape platform was placed at Quadrant A as the target quadrant, which was hidden 2 cm below the water surface in this study. This MWM test includes place navigation and spatial probe carried in the Basic Research Center of Hubei University of Medicine. The MWM test was finished according to these previous studies [12, 21, 22] and the manufacturer’s instructions for use of Morris water maze. Five trials were created with an inter-trial interval of 60 s. The trail length was 120 s.
ELISA for Aβ
The rats were deeply anesthetized with 4% chloral hydrate intraperitoneally (400 mg/kg) 48 h after MWM test. The blood was collected from the orbital sinus by removing the eyeball from socket with a pair of tissue forceps. The harvested hippocampus tissues were dissected and homogenized with T-PER buffer (Biosource International, Inc., USA) in the presence of protease inhibitors (Biosource International, Inc., USA). The 100 mg hippocampus tissue was rinsed with 1 × PBS, homogenized in 1 ml of 1 × PBS and stored overnight at −20 °C. After two freeze–thaw cycles were performed to break the cell membranes, the homogenates were centrifuged for 5 min at 5000×g, 2–8 °C. The supernate was removed and assayed immediately. The colorimetric enzyme-linked immunosorbent assay (ELISA) kits were used to determine the concentrations of Aβ (Aβ40 and Aβ42: Abcam, Cambridge, UK) and sAPP (sAPPα and sAPPβ: Cusabio Biotech Co., Ltd, USA) according to the manufacturer’s instructions and previous studies [23]. The optical density (OD) at 450 nm of each well was read using a microplate reader immediately. The concentration of Aβ (Aβ40 and Aβ42) and sAPP (sAPPα and sAPPβ) in the samples was then determined by comparing the OD of the samples to the standard curve. The sensitivity in this assay is 1.0 pg/ml.
Western Blotting
The hippocampus tissues were homogenized in the presence of protease inhibitors and incubated on ice for 30 min. After the homogenate samples was centrifuged at 5000×g for 30 min at 4 °C to generate their supernatant fractions, the supernatant was collected and used for Western blotting arrays. The procedure of Western blotting was executed according to the manufacturer’s instructions and previous studies [24, 25]. The equal protein was loaded for all samples, including the control. The sAPPα (1:500), BACE (1:100), BACE1(1:300), NCT(1:1000), PS1(1:200), Aph-1α (1:300) and Pen-2 (1:1000) antibodies were purchased from Abcam, Cambridge, UK. The optical densities (OD) of the specific bands were scanned and measured by image analysis software (HPIAS 2000, Tongji Qianping Company, Wuhan, China).
Statistical Analysis
Quantitative data were expressed as the mean ± SEM. Statistical analysis was carried out with GraphPad Prism 6. For statistical evaluation of intergroup differences, one-way analyses of variance (ANOVA) were employed. A two-tailed t test was used for two group comparisons. Differences were considered significantly at P < 0.05.
Results
Morris Water Maze (MWM) Test
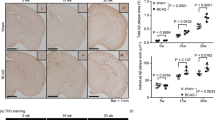
To investigate the potential effect of CCH on cognitive deficit in learning and memory, the functions of learning and memory of rats were measured with the MWM test. Rats were subjected to MWM test 1 week or 4 weeks after BCCAO. In MWM, the spatial learning of rats is tested with the hidden-platform acquisition test (navigation), and spatial memory is investigated with the probe trial test. The escape latency which rats find the hidden-platform time in the water maze was more increased in CCH-insulted rats (1 week or 4 weeks) than control ones in Day 4, 5, 6 and 7 (P < 0.01) (Fig. 1a, b), implicating that the BCCAO rats had cognitive impairment in spatial learning. In the probe trials, the platform was removed, and the rats were placed into the non-target quadrants (Quadrant B, C and D) respectively and allowed to swim freely for 120 s. The BCCAO rats was significantly lower than the littermate control in the time spent in the target quadrant (Quadrant A: removed-platform one) and the number of times crossing the target quadrant during the last probe trial (P < 0.01) (Fig. 1c, d), implicating that the BCCAO rats had cognitive impairment in spatial learning and memory.
Morris water maze (MWM) for behavioral test. The escape latency which rats found the hidden-platform time increased in CCH-insulted rats (1 week or 4 weeks) in Day 4, 5, 6 and 7 (F(2, 15) = 2.360, df = 15, P < 0.0001) (a: P = 0.0036, 1-week CCH vs. control normal rats; b: P = 0.0029, 4-week CCH vs. control normal rats). In the probe trials, the BCCAO rats was significantly lower than the control in the time spent in the target quadrant and the number of times crossing the target quadrant (P < 0.01) [c: F(2, 15) = 1.875, df = 15, P < 0.0001; d: F(2, 15) = 0.912, df = 15, P < 0.0001]. Values represented as mean ± SEM (n = 6). ##P < 0.01, versus control normal rats
Upregulation of Aβ in the Hippocampus of CCH Rats
The Aβ levels in the serum and hippocampal tissues of rats were investigated with colorimetric ELISA method. As shown in Fig. 2a, the Aβ42 levels in the hippocampal tissues were increased in the CCH-intervened rats compared to the control rats. The Aβ40 levels were also markedly elevated in the CCH-intervened rats compared to the control rats. These results indicate that CCH enhanced the expression of Aβ in the hippocampus of rats.
Aβ 40/42 ELISA assay and the correlation analysis between the Aβ levels of hippocampus and the variables of MWM task. The Aβ42 and Aβ40 levels were increased in the CCH-intervened rats compared to the control rats (a) (##P < 0.01). There was no difference in serum Aβ levels between control and CCH rats (b). The levels of Aβ40 and 42 were positively correlated with the escape latency (Aβ40: r = 0.8234, P < 0.0001; Aβ42: r = 0.9571, P < 0.0001) (c, d). The levels of Aβ40 and 42 were negatively correlated with the time staying in the target quadrant which is the removed-platform quadrant (Aβ40: r = −0.8119, P < 0.0001; Aβ42: r = −0.8322, P < 0.0001) (e, f), and times acrossing the target quadrant (Aβ40: r = −0.7192, P = 0.0009; Aβ42: r = −0.7884, P = 0.0001) (g, h). Data are expressed as the mean ± SED. Aβ amyloid beta, CCH chronic cerebral hypoperfusion, CI confidence interval
However, there was no difference in serum Aβ levels between control and CCH rats (Fig. 2b). Furthermore, the correlation was analyzed between the Aβ levels of hippocampus and the variables of MWM task. As shown in Fig. 2c and d, the levels of Aβ40 and 42 were positively correlated with the escape latency (Aβ40: r = 0.8234, P < 0.0001; Aβ42: r = 0.9571, P < 0.0001), suggesting that the upregulation of Aβ enhanced the impairment of spatial learning. Figure 2e–h interpreted the relation between the Aβ levels and the trial probe task. These analysis demonstrated the negative correlation between the Aβ levels and the variables of the trial probe task: time staying in the target quadrant which is the removed-platform quadrant (Aβ40: r = −0.8119, P < 0.0001; Aβ42: r = −0.8322, P < 0.0001), and times acrossing the target quadrant (Aβ40: r = −0.7192, P = 0.0009; Aβ42: r = −0.7884, P = 0.0001). The negative correlation implicated that the upregulation of Aβ contributed to the impairment of memory.
CCH Enhanced the Expression of α-Secretase in the Hippocampus of Rats
Aβ is produced by the proteolytic cleavage of amyloid precursor protein (APP). APP cleavage mainly includes two distinct pathways: the non-amyloidogenic pathway and the amyloidogenic pathway (Fig. 3a). The non-amyloidogenic pathway involves the sequential cleavage of APP by α-secretase and γ-secretase to generate N-terminal ectodomain (sAPPα) and p3 peptide. ADAM10 and ADAM17 have been identified as the two main α-secretases.
The effects of CCH on α-secretase. The process of APP cleavage mainly includes the following two pathways: the non-amyloidogenic pathway and the amyloidogenic pathway (a). Relative amounts of ADAM10 and ADAM17 were expressed as the densitometry OD ratio to β-actin (mean ± SED) for Western blotting. The sAPPα, ADAM10 and ADAM17 levels in the CCH-treated rats were significantly higher than the control rats (P < 0.05) (b). The ELISA test showed that the levels of sAPPα in the hippocampus of CCH rats significantly increased, compared with the control ones (P < 0.05) (c). ADAM a disintegrin and metalloprotease domain, CCH chronic cerebral hypoperfusion, OD optical density
To further explore the role of CCH in the Aβ production, the α-secretase (ADAM10 and ADAM17) and sAPPα were measured in this study. As shown in Fig. 3b and c, the levels of sAPPα, ADAM10 and ADAM17 in the hippocampus of CCH rats significantly increased, compared with the control ones (P < 0.05).
CCH Upregulated the Level of β-Secretase in the Hippocampus of Rats
The amyloidogenic pathway produces neurotoxic Aβ peptides by the sequential cleavage of APP by β-secretase (BACE) and γ-secretase. This process generates N-terminal ectodomain (sAPPβ) and Aβ peptides. The beta-amyloid precursor protein cleavage enzyme 1 (BACE1) has been identified as the leading function in Aβ production. To further clarify the role of CCH in the Aβ production, this study investigated the change in the levels of BACE and BACE1 in the hippocampus.
As shown in Fig. 4a, the levels of BACE and BACE1 in the hippocampus of CCH rats were significantly higher than the control ones (P < 0.05). Figure 4b demonstrated that the levels of sAPPβ in the hippocampus of CCH rats were significantly upregulated, compared to the control ones (P < 0.05).
The effects of CCH on β-secretase. Relative amounts of BACE and BACE1 were expressed as the densitometry OD ratio to β-actin (mean ± SED) for Western blotting. The BACE and BACE1 levels in the hippocampus of CCH-treated rats were higher than the control ones (P < 0.05) (a). The ELISA test showed that the levels of sAPPβ in the hippocampus of CCH rats significantly elevated, compared to the control ones (P < 0.05) (b). BACE1 the beta-amyloid precursor protein cleavage enzyme 1, CCH chronic cerebral hypoperfusion, OD optical density
CCH Accentuated the Activity of γ-Secretase Complex
CCH contributed to behavioral deficits by up-regulating Aβ, and it had effects on BACE1 which is the primary contributor to Aβ generation. It is well known that the production of Aβ is from a sequential cleavage by β-secretase and γ-secretase. γ-secretase is a protease complex which has at least four components: the amino- and carboxy-terminal fragments of presenilin 1 (PS1), a highly glycosylated form of nicastrin (NCT), anterior pharynx-defective 1alpha (Aph-1α), and presenilin enhancer 2 (Pen-2). Therefore, the four components of γ-secretase complex were investigated the role of CCH on the Aβ production. As shown in Fig. 5, CCH intervention (1-week or 4-week) markedly increased the expression of PS1, Aph-1α and Pen-2 in the hippocampus of rats, but had no effect on NCT, suggesting the enhancing role of CCH in the activity of γ-secretase complex in the hippocampus.
Effects of CCH on the activity of γ-secretase complex. The activity of γ-secretase complex was determined by Western blotting. The expression of PS1, Aph-1α and Pen-2 in CCH-intervented (1-week or 4-week) rats was markedly higher in the hippocampus (##P < 0.01), but had no effect on NCT, compared with the control rats. The protein levels of NCT, PS1, Aph-1α and Pen-2 are expressed as the densitometry ratio of NCT, PS1, Aph-1α and Pen-2 to β-actin. Values represented as mean ± SEM (n = 10). Aph-1α anterior pharynx-defective 1alpha, CCH chronic cerebral hypoperfusion, Ctr control, NCT nicastrin, OD optical density, Pen-2 presenilin enhancer 2, PS1 presenilin1
Discussion
Reduced cerebral blood flow and cerebral ischemia play an important role in the regulation of amyloid-beta (Aβ) production. Chronic cerebral hypoperfusion (CCH) is an etiological factor for Alzheimer’s disease (AD) besides the causes of vascular dementia. The aim of this study was to investigate the effects of CCH on the Aβ production. Our study showed that CCH not only enhanced the activity of the non-amyloidogenic pathway but reinforced the activity of the amyloidogenic pathway as well. In addition, CCH contributed to the cognitive dysfunction related to the Aβ over-expression.
Compelling experiments to mimic CCH-induced cerebral ischemia have been designed by permanent or reversible occlusion of more than one major vessel supplying the brain in animals [26,27,28]. There is accumulating evidence that bilateral common carotid artery occlusion (BCCAO), known as ischemic preconditioning or ischemic tolerance, is an adequate CCH stimulus to induce chronic cerebral ischemia [29,30,31]. Studies of rats with BCCAO have demonstrated that BCCAO-induced CCH has been often used as an animal model for vascular cognitive impairment and dementia, involving in hippocampus-dependent memory impairment and a series of neuropathologies (e.g. cerebral microvessel, white matter and gray matter damage) associated with CCH [31,32,33]. In this study, we found that BCCAO rats had the resulting impairment of spatial learning and memory investigated by MWM testing, and confirmed the causative relationship between CCH and cognitive impairment. A variety of studies have indicated that Aβ, a major component of senile plaques in AD, has been implicated in cognitive impairment [12, 34,35,36,37]. Our study suggested that the upregulation of Aβ in the CCH-condition enhanced the impairment of spatial learning and memory, and reaffirmed the evidence that CCH is associated with cognitive impairment correlated to the Aβ expression.
The non-amyloidogenic pathway of APP processing indicates a sequential cleavage of APP by α-secretase (ADAM-10 and ADAM-17) and γ-secretase to generate sAPPα, p3 and C-terminal fragment that is also known as APP intracellular domain (AICD) [38,39,40]. The non-amyloidogenic α-secretase cleavage of APP promotes the release of sAPPα [41, 42]. In this study, the sAPPα and two enzymes of α-secretase (ADAM10 and ADAM17) were investigated. These results showed that the levels of sAPPα, ADAM10 and ADAM17 in the hippocampus of CCH-rats were all up-regulated, suggesting the enhancing role of CCH in the non-amyloidogenic pathway. The non-amyloidogenic pathway prohibits Aβ production since cleavage of APP by α-secretase occurs within the Aβ domain [38, 41]. Therefore, it seems that the process of CCH-condition activated the non-amyloidogenic pathway which acts as a beneficial neurotrophic effect. The general neuro-pathological presentation suffering from CCH-insult may be due to the imbalance between the non-amyloidogenic pathway and amyloidogenic pathway. The cognitive damage may be the results that the non-amyloidogenic pathway can’t overcome the damage role of the amyloidogenic pathway in the process of CCH-condition.
The amyloidogenic pathway of APP processing provides the results in neurotoxic Aβ generation, the releases of sAPPβ and AICD [43, 44]. The production and accumulation of Aβ from APP by the sequential cleavage of β-secretase and γ-secretase, has been well recognized as the initial causative events in AD. Previous study by our group found the over-expression of β-secretase (BACE1) and Aβ in the hippocampus of BCCAO rats increased [12]. Level of BACE1 and Aβ had a positive correlation with degree of cognitive impairment in BCCAO rats [12]. Hence, over-expression of BACE1 and Aβ from CCH was a potential vascular pathogenesis of AD. This study further evidenced the hypothesis that CCH makes a remarkable contribution to Aβ generation and releases of sAPPβ via enhancing the activity of β-secretase (ABCE and BACE1). It has also been certified the determinative role of γ-secretase in the Aβ pathogenesis [45, 46]. It seems that inhibiting the activity of γ-secretase is a promising therapeutics target. This study demonstrated that CCH activated the main three components of γ-secretase complex (PS1, Aph-1α and Pen-2). Taken together, CCH makes a remarkable contribution to Aβ generation because CCH not only enhanced the activity of β-secretase but increased the activity of γ-secretase as well.
The γ-secretase complex, a membrane protein complex, at least includes four components: presenilin1 (PS1), nicastrin (NCT), anterior pharynx-defective 1alpha (Aph-1α) and presenilin enhancer 2 (Pen-2) [47]. The γ-secretase complex catalyzes the intramembrane proteolysis of Notch, APP and other substrates as a key step in the pathogenesis of AD. This study demonstrated that CCH significantly highered the expression of PS1, Aph-1α and Pen-2 in the hippocampus of rats, but had no effect on NCT. The primary role of NCT is maintaining the stability of the γ-secretase complex and regulating intracellular protein trafficking [48]. Hence, it seems that CCH has no influence on the functional stability and intracellular protein trafficking of γ-secretase.
A variety of mechanisms have been reported that CCH may affect AD pathogenesis [49,50,51,52]. Cerebral hypoperfusion and glucose hypometabolism are key pathophysiological modulators that promote the Alzheimer’s-like neurodegeneration with impaired microvascular function (dysfunction of neurovascular unit, cerebrovascular remodeling damage and disruption of neurovascular trophic coupling) [50, 53,54,55]. CCH impairs white matter integrity and lesions in AD and leads to cognitive impairment [36, 56]. Substantial studies have demonstrated that reduced cerebral blood flow and CCH plays an important role in the Aβ pathogenesis [12, 51, 57], and even mild CCH ignites peripheral Aβ to enter into brain and promote its aggregation [57, 58]. Although CCH makes a remarkable contribution to Aβ generation via activating β-secretase, it remains elusive that what’s the relation between CCH and activity of the γ-secretase complex. The purpose of the present study was to investigate whether CCH would affect the activity of the γ-secretase complex in an Alzheimer’s mouse model. Our study demonstrated that CCH promotes Aβ generation because CCH enhances both the activity of β-secretase and γ-secretase. Moreover, the process of CCH activates the non-amyloidogenic pathway which acts as a beneficial neurotrophic effect. Therefore, the general neuro-pathological presentation suffering from CCH-insult may be due to the imbalance between the non-amyloidogenic and amyloidogenic pathway. The cognitive damage may be the results that the pathological role of the amyloidogenic pathway is more than over the non-amyloidogenic pathway in the process of CCH-condition. This study offers the possible mechanisms that CCH contributes to cognitive impairment and the amyloidogenic pathway of APP processing by enhancing both the activity of β-secretase and γ-secretase. These results provided a novel molecular mechanism by which cerebral risk factors contributed to Aβ pathology in the development of AD. These findings also provide a possible mechanistic linkage between AD and vascular factors.
References
Mutsuga M, Chambers JK, Uchida K, Tei M, Makibuchi T, Mizorogi T, Takashima A, Nakayama H (2012) Binding of curcumin to senile plaques and cerebral amyloid angiopathy in the aged brain of various animals and to neurofibrillary tangles in Alzheimer’s brain. J Vet Med Sci 74(1):51–57
Shin J, Lee SY, Kim SH, Kim YB, Cho SJ (2008) Multitracer PET imaging of amyloid plaques and neurofibrillary tangles in Alzheimer’s disease. Neuroimage 43(2):236–244
Gamblin TC, Chen F, Zambrano A, Abraha A, Lagalwar S, Guillozet AL, Lu M, Fu Y, Garcia-Sierra F, LaPointe N et al (2003) Caspase cleavage of tau: linking amyloid and neurofibrillary tangles in Alzheimer’s disease. Proc Natl Acad Sci USA 100(17):10032–10037
Deibel SH, Weishaupt N, Regis AM, Hong NS, Keeley RJ, Balog RJ, Bye CM, Himmler SM, Whitehead SN, McDonald RJ (2016) Subtle learning and memory impairment in an idiopathic rat model of Alzheimer’s disease utilizing cholinergic depletions and beta-amyloid. Brain Res 1646:12–24
Soodi M, Saeidnia S, Sharifzadeh M, Hajimehdipoor H, Dashti A, Sepand MR, Moradi S (2016) Satureja bachtiarica ameliorate beta-amyloid induced memory impairment, oxidative stress and cholinergic deficit in animal model of Alzheimer’s disease. Metab Brain Dis 31(2):395–404
Suganthy N, Malar DS, Devi KP (2016) Rhizophora mucronata attenuates beta-amyloid induced cognitive dysfunction, oxidative stress and cholinergic deficit in Alzheimer’s disease animal model. Metab Brain Dis 31(4):937–949
Selkoe DJ, Hardy J (2016) The amyloid hypothesis of Alzheimer’s disease at 25 years. EMBO Mol Med 8(6):595–608
Tamaoka A (2013) [The pathophysiology of Alzheimer’s disease with special reference to “amyloid cascade hypothesis”]. Rinsho Byori 61(11):1060–1069
Barage SH, Sonawane KD (2015) Amyloid cascade hypothesis: pathogenesis and therapeutic strategies in Alzheimer’s disease. Neuropeptides 52:1–18
Solans A, Estivill X, de La Luna S (2000) A new aspartyl protease on 21q22.3, BACE2, is highly similar to Alzheimer’s amyloid precursor protein beta-secretase. Cytogenet Cell Genet 89(3–4):177–184
Sadleir KR, Kandalepas PC, Buggia-Prevot V, Nicholson DA, Thinakaran G, Vassar R (2016) Presynaptic dystrophic neurites surrounding amyloid plaques are sites of microtubule disruption, BACE1 elevation, and increased Abeta generation in Alzheimer’s disease. Acta Neuropathol 132(2):235–256
Zhiyou C, Yong Y, Shanquan S, Jun Z, Liangguo H, Ling Y, Jieying L (2009) Upregulation of BACE1 and beta-amyloid protein mediated by chronic cerebral hypoperfusion contributes to cognitive impairment and pathogenesis of Alzheimer’s disease. Neurochem Res 34(7):1226–1235
Maloney B, Lahiri DK (2011) The Alzheimer’s amyloid beta-peptide (Abeta) binds a specific DNA Abeta-interacting domain (AbetaID) in the APP, BACE1, and APOE promoters in a sequence-specific manner: characterizing a new regulatory motif. Gene 488(1–2):1–12
Xu TH, Yan Y, Kang Y, Jiang Y, Melcher K, Xu HE (2016) Alzheimer’s disease-associated mutations increase amyloid precursor protein resistance to gamma-secretase cleavage and the Abeta42/Abeta40 ratio. Cell Discov 2:16026
Zhang N, Gordon ML, Goldberg TE (2017) Cerebral blood flow measured by arterial spin labeling MRI at resting state in normal aging and Alzheimer’s disease. Neurosci Biobehav Rev 72:168–175
Hanaoka T, Kimura N, Aso Y, Takemaru M, Kimura Y, Ishibashi M, Matsubara E (2016) Relationship between white matter lesions and regional cerebral blood flow changes during longitudinal follow up in Alzheimer’s disease. Geriatr Gerontol Int 16(7):836–842
Lacalle-Aurioles M, Mateos-Perez JM, Guzman-De-Villoria JA, Olazaran J, Cruz-Orduna I, Aleman-Gomez Y, Martino ME, Desco M (2014) Cerebral blood flow is an earlier indicator of perfusion abnormalities than cerebral blood volume in Alzheimer’s disease. J Cereb Blood Flow Metab 34(4):654–659
Toda N, Okamura T (2016) Cigarette smoking impairs nitric oxide-mediated cerebral blood flow increase: implications for Alzheimer’s disease. J Pharmacol Sci 131(4):223–232
Leeuwis AE, Benedictus MR, Kuijer JP, Binnewijzend MA, Hooghiemstra AM, Verfaillie SC, Koene T, Scheltens P, Barkhof F, Prins ND et al (2017) Lower cerebral blood flow is associated with impairment in multiple cognitive domains in Alzheimer’s disease. Alzheimers Dement 131(5):531–540
Hays CC, Zlatar ZZ, Wierenga CE (2016) The utility of cerebral blood flow as a biomarker of preclinical Alzheimer’s disease. Cell Mol Neurobiol 36(2):167–179
Li M, Zhang P, Wei HJ, Li MH, Zou W, Li X, Gu HF, Tang XQ (2017) Hydrogen sulfide ameliorates homocysteine-induced cognitive dysfunction by inhibition of reactive aldehydes involving upregulation of ALDH2. Int J Neuropsychopharmacol 20(4):305–315
Zhao Y, Gu JH, Dai CL, Liu Q, Iqbal K, Liu F, Gong CX (2014) Chronic cerebral hypoperfusion causes decrease of O-GlcNAcylation, hyperphosphorylation of tau and behavioral deficits in mice. Front Aging Neurosci 6:10
He J, Qiao JP, Zhu S, Xue M, Chen W, Wang X, Tempier A, Huang Q, Kong J, Li XM (2013) Serum beta-amyloid peptide levels spike in the early stage of Alzheimer-like plaque pathology in an APP/PS1 double transgenic mouse model. Curr Alzheimer Res 10(9):979–986
Neumann S, Schobel S, Jager S, Trautwein A, Haass C, Pietrzik CU, Lichtenthaler SF (2006) Amyloid precursor-like protein 1 influences endocytosis and proteolytic processing of the amyloid precursor protein. J Biol Chem 281(11):7583–7594
Singh I, Sagare AP, Coma M, Perlmutter D, Gelein R, Bell RD, Deane RJ, Zhong E, Parisi M, Ciszewski J et al (2013) Low levels of copper disrupt brain amyloid-beta homeostasis by altering its production and clearance. Proc Natl Acad Sci USA 110(36):14771–14776
Liang CC, Lin YH, Liu HL, Lee TH (2015) Bladder dysfunction induced by cerebral hypoperfusion after bilateral common carotid artery occlusion in rats. Neurourol Urodyn 34(6):586–591
Schiavon AP, Soares LM, Bonato JM, Milani H, Guimaraes FS, Weffort de Oliveira RM (2014) Protective effects of cannabidiol against hippocampal cell death and cognitive impairment induced by bilateral common carotid artery occlusion in mice. Neurotox Res 26(4):307–316
Huang Y, Fan S, Li J, Wang YL (2014) Bilateral common carotid artery occlusion in the rat as a model of retinal ischaemia. Neuroophthalmology 38(4):180–188
Speetzen LJ, Endres M, Kunz A (2013) Bilateral common carotid artery occlusion as an adequate preconditioning stimulus to induce early ischemic tolerance to focal cerebral ischemia. J Vis Exp 75:4387
Surapaneni S, Prakash T, Ansari M, Manjunath P, Kotresha D, Goli D (2016) Study on cerebroprotective actions of Clerodendron glandulosumleaves extract against long term bilateral common carotid artery occlusion in rats. Biomed Pharmacother 80:87–94
Kim DH, Choi BR, Jeon WK, Han JS (2016) Impairment of intradimensional shift in an attentional set-shifting task in rats with chronic bilateral common carotid artery occlusion. Behav Brain Res 296:169–176
Wang X, Lin F, Gao Y, Lei H (2015) Bilateral common carotid artery occlusion induced brain lesions in rats: a longitudinal diffusion tensor imaging study. Magn Reson Imaging 33(5):551–558
Fukuoka T, Hayashi T, Hirayama M, Maruyama H, Tanahashi N (2014) Cilostazol inhibits platelet-endothelial cell interaction in murine microvessels after transient bilateral common carotid artery occlusion. J Stroke Cerebrovasc Dis 23(5):1056–1061
Han H, Qian Q, Yu Y, Zhao D, Sun G (2015) Lamotrigine attenuates cerebral ischemia-induced cognitive impairment and decreases beta-amyloid and phosphorylated tau in the hippocampus in rats. Neuroreport 26(12):723–727
Song B, Ao Q, Niu Y, Shen Q, Zuo H, Zhang X, Gong Y (2013) Amyloid beta-peptide worsens cognitive impairment following cerebral ischemia-reperfusion injury. Neural Regen Res 8(26):2449–2457
Lee JS, Im DS, An YS, Hong JM, Gwag BJ, Joo IS (2011) Chronic cerebral hypoperfusion in a mouse model of Alzheimer’s disease: an additional contributing factor of cognitive impairment. Neurosci Lett 489(2):84–88
Reijmer YD, van Veluw SJ, Greenberg SM (2016) Ischemic brain injury in cerebral amyloid angiopathy. J Cereb Blood Flow Metab 36(1):40–54
Kojro E, Fahrenholz F (2005) The non-amyloidogenic pathway: structure and function of alpha-secretases. Subcell Biochem 38:105–127
Filippov MA, Dityatev A (2012) Matrix metalloproteinase-9 and non-amyloidogenic pathway of amyloid precursor protein processing. J Neurochem 121(2):181–183
Naslund J, Jensen M, Tjernberg LO, Thyberg J, Terenius L, Nordstedt C (1994) The metabolic pathway generating p3, an A beta-peptide fragment, is probably non-amyloidogenic. Biochem Biophys Res Commun 204(2):780–787
Bandyopadhyay S, Goldstein LE, Lahiri DK, Rogers JT (2007) Role of the APP non-amyloidogenic signaling pathway and targeting alpha-secretase as an alternative drug target for treatment of Alzheimer’s disease. Curr Med Chem 14(27):2848–2864
Bandyopadhyay S, Hartley DM, Cahill CM, Lahiri DK, Chattopadhyay N, Rogers JT (2006) Interleukin-1alpha stimulates non-amyloidogenic pathway by alpha-secretase (ADAM-10 and ADAM-17) cleavage of APP in human astrocytic cells involving p38 MAP kinase. J Neurosci Res 84(1):106–118
Grimm MO, Regner L, Mett J, Stahlmann CP, Schorr P, Nelke C, Streidenberger O, Stoetzel H, Winkler J, Zaidan SR et al (2016) Tocotrienol affects oxidative stress, cholesterol homeostasis and the amyloidogenic pathway in neuroblastoma cells: consequences for Alzheimer’s disease. Int J Mol Sci 17(11):1809
Fisher CL, Resnick RJ, De S, Acevedo LA, Lu KP, Schroeder FC, Nicholson LK (2017) Cyclic cis-locked phospho-dipeptides reduce entry of AbetaPP into amyloidogenic processing pathway. J Alzheimers Dis 55(1):391–410
Sachse CC, Kim YH, Agsten M, Huth T, Alzheimer C, Kovacs DM, Kim DY (2013) BACE1 and presenilin/gamma-secretase regulate proteolytic processing of KCNE1 and 2, auxiliary subunits of voltage-gated potassium channels. FASEB J 27(6):2458–2467
Hogl S, Kuhn PH, Colombo A, Lichtenthaler SF (2011) Determination of the proteolytic cleavage sites of the amyloid precursor-like protein 2 by the proteases ADAM10, BACE1 and gamma-secretase. PLoS ONE 6(6):e21337
Kimberly WT, LaVoie MJ, Ostaszewski BL, Ye W, Wolfe MS, Selkoe DJ (2003) Gamma-secretase is a membrane protein complex comprised of presenilin, nicastrin, Aph-1, and Pen-2. Proc Natl Acad Sci USA 100(11):6382–6387
Zhang YW, Luo WJ, Wang H, Lin P, Vetrivel KS, Liao F, Li F, Wong PC, Farquhar MG, Thinakaran G et al (2005) Nicastrin is critical for stability and trafficking but not association of other presenilin/gamma-secretase components. J Biol Chem 280(17):17020–17026
Huang KL, Lin KJ, Ho MY, Chang YJ, Chang CH, Wey SP, Hsieh CJ, Yen TC, Hsiao IT, Lee TH (2012) Amyloid deposition after cerebral hypoperfusion: evidenced on [(18)F]AV-45 positron emission tomography. J Neurol Sci 319(1–2):124–129
Daulatzai MA (2017) Cerebral hypoperfusion and glucose hypometabolism: key pathophysiological modulators promote neurodegeneration, cognitive impairment, and Alzheimer’s disease. J Neurosci Res 95(4):943–972
Liang W, Zhang W, Zhao S, Li Q, Liang H, Ceng R (2015) Altered expression of neurofilament 200 and amyloid-beta peptide (1–40) in a rat model of chronic cerebral hypoperfusion. Neurol Sci 36(5):707–712
Pimentel-Coelho PM, Michaud JP, Rivest S (2013) Effects of mild chronic cerebral hypoperfusion and early amyloid pathology on spatial learning and the cellular innate immune response in mice. Neurobiol Aging 34(3):679–693
Zhai Y, Yamashita T, Nakano Y, Sun Z, Shang J, Feng T, Morihara R, Fukui Y, Ohta Y, Hishikawa N (2016) et al Chronic cerebral hypoperfusion accelerates Alzheimer’s disease pathology with cerebrovascular remodeling in a novel mouse model. J Alzheimers Dis 53(3):893–905
Shang J, Yamashita T, Zhai Y, Nakano Y, Morihara R, Fukui Y, Hishikawa N, Ohta Y, Abe K (2016) Strong impact of chronic cerebral hypoperfusion on neurovascular unit, cerebrovascular remodeling, and neurovascular trophic coupling in Alzheimer’s disease model mouse. J Alzheimers Dis 52(1):113–126
Okamoto Y, Yamamoto T, Kalaria RN, Senzaki H, Maki T, Hase Y, Kitamura A, Washida K, Yamada M, Ito H (2012) et al Cerebral hypoperfusion accelerates cerebral amyloid angiopathy and promotes cortical microinfarcts. Acta Neuropathol 123(3):381–394
Zhai Y, Yamashita T, Nakano Y, Sun Z, Morihara R, Fukui Y, Ohta Y, Hishikawa N, Abe K (2016) Disruption of white matter integrity by chronic cerebral hypoperfusion in Alzheimer’s disease mouse model. J Alzheimers Dis 52(4):1311–1319
ElAli A, Theriault P, Prefontaine P, Rivest S (2013) Mild chronic cerebral hypoperfusion induces neurovascular dysfunction, triggering peripheral beta-amyloid brain entry and aggregation. Acta Neuropathol Commun 1:75
Bennett SA, Pappas BA, Stevens WD, Davidson CM, Fortin T, Chen J (2000) Cleavage of amyloid precursor protein elicited by chronic cerebral hypoperfusion. Neurobiol Aging 21(2):207–214
Acknowledgements
This work was supported by grants from by the Natural Science Foundation of Hubei Province (2015CFB260), and the Hubei Province Health and Family Planning Scientific Research Project (WJ2015MB219) and the Shiyan Natural Science Foundation (15K70) and Chongqing General Hospital to Dr Zhiyou Cai.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of interest
All authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Cai, Z., Liu, Z., Xiao, M. et al. Chronic Cerebral Hypoperfusion Promotes Amyloid-Beta Pathogenesis via Activating β/γ-Secretases. Neurochem Res 42, 3446–3455 (2017). https://doi.org/10.1007/s11064-017-2391-9
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11064-017-2391-9