Abstract
Purpose
Cancer cells often elicit a higher glycolytic rate than normal cells, supporting the development of glycolysis inhibitors as therapeutic agents. 2-Deoxyglucose (2-DG) is used in this context due to its ability to compete with glucose. However, many studies do not take into account that 2-DG inhibits not only glycolysis but also N-glycosylation. Since there are limited publications on 2-DG mechanism of action in breast cancer, we studied its effects in breast cancer cell lines to determine the part played by glycolysis inhibition and N-linked glycosylation interference.
Methods and Results
2-Deoxyglucose behaved as an anticancer agent with a similar efficiency on cell number decrease between the hormone-dependent MCF-7 and hormone-independent MDA-MB-231 breast cancer cells. It also interfered with the N-linked glycosylation process in both cell lines as illustrated by the migration profile of the lysosomal-associated membrane protein 2 and calumenin. These results are reinforced by the appearance of an abnormal Man7GlcNAc2 structure both on lipid-linked oligosaccharides and N-linked glycoproteins of 2-DG incubated MDA-MB-231 cells. Besides, 2-DG-induced a transient endoplasmic reticulum stress that was more sustained in MDA-MB-231 cells. Both changes were abrogated by mannose. 2-DG, even in the presence of mannose, decreased glycolysis in both cell lines. Mannose partially reversed the effects of 2-DG on cell numbers with N-linked glycosylation interference accounting for 37 and 47% of 2-DG anti-cancerous effects in MDA-MB-231 and MCF-7 cells, respectively.
Conclusion
N-linked glycosylation interference and glycolysis disruption both contribute to the anticancer properties of 2-DG in breast cancer cells.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
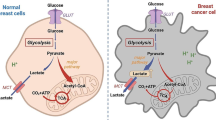
Most cancer cells elicit a high rate of glycolysis even under normal oxygen concentrations, called the Warburg effect [1]. This metabolic property is clinically exploited by positron emission tomography imaging with 2-[18F]fluoro-2-deoxy-d-glucose [2]. This altered metabolism responds to requirements of rapid proliferating tumor cells such as rapid ATP generation, stimulated biosynthesis of macromolecules and maintenance of cellular redox homeostasis [3].
Up-regulation of glycolysis was reported to promote invasive tumor growth and to contribute to drug resistance in cancer therapy [4, 5]. Hence, consequent efforts have been initiated to develop anticancer treatments targeting tumor glycolysis [6]. Among them, 2-deoxy-d-glucose (2-DG) emerged as an interesting candidate. This sugar analog displayed anticancer activity in numerous in vitro and in vivo studies and improved the chemosensitivity and radiosensitivity of cancer cells [7].
2-Deoxyglucose is a glucose analog, in which the hydroxyl group at the second carbon atom was substituted by hydrogen. Competition with glucose occurs at different levels in the glycolytic pathway. 2-DG firstly decreases the cellular glucose uptake suggesting a competition between both sugars [8]. 2-DG and glucose are then phosphorylated by hexokinase, but 2-DG-6-phosphate cannot be further metabolized through the glycolysis, resulting in its cellular accumulation. As a consequence, phosphoglucoisomerase and hexokinase are respectively competitively and non-competitively inhibited by 2-DG-6-phosphate [9, 10].
Due to the structural similarity of glucose with mannose, 2-DG also competes with mannose for the process of N-linked glycosylation of proteins in the endoplasmic reticulum (ER). It is converted in the nucleoside-disphosphate derivative GDP-2-DG, before being incorporated in lipid-linked oligosaccharides precursors [11, 12]. The resulting intermediates cannot be further extended by the addition of mannosyl residues, leading to a disruption of glycosylation of proteins [11]. Consequently, misfolded N-glycoproteins accumulate in the ER leading to ER stress and the activation of the unfolded protein response (UPR) [13]. This interference with the N-linked glycosylation process can be reversed by addition of exogenous mannose [13].
Despite numerous studies, the relative contribution of glycolysis inhibition and N-linked glycosylation interference in the anticancer effects of 2-DG has not been systematically evaluated. Moreover, there are limited publications on 2-DG mechanism of action in breast cancer [7]. Then, we studied its effects in breast cancer cell lines to determine the part played by glycolysis inhibition and N-linked glycosylation interference.
Materials and methods
Cell culture and treatments
MDA-MB-231 and MCF-7 human breast cancer cell lines were obtained from American Type Culture Collection (Manassas, VA, USA). They were grown at 37 °C under 5% CO2 in Roswell Park Memorial Institute (RPMI) 1640 medium (Gibco®, Thermo Fisher Scientific, Villebon-sur-Yvette, France) for MDA-MB-231 and Dulbecco’s Modified Eagle Medium (DMEM, Gibco®) for MCF-7, supplemented with 2 mM l-glutamine (Sigma-Aldrich, Saint-Quentin Fallavier, France) and 10% fetal bovine serum (Sigma-Aldrich). 24 h after seeding, cells were treated for various times with 2-DG (Sigma-Aldrich) and/or mannose (Sigma-Aldrich) at the indicated concentrations.
Crystal violet staining assay
MDA-MB-231 (2 × 104 cells) and MCF-7 (1.5 × 104 cells) cells were seeded in 96-well plates. Cells were fixed and stained for 20 min with 0.2% crystal violet (Sigma-Aldrich) in 2% ethanol, as previously described [14]. Cell number was determined by absorbance at 595 nm with a VICTOR™ X3 multilabel plate reader (PerkinElmer, Courtaboeuf, France). The concentration of 2-DG leading to a decrease of 50% of the cell number (IC50) was determined.
Western immunoblotting
MDA-MB-231 (8.0 × 105 cells) and MCF-7 (6.5 × 105 cells) cells were seeded in 60 mm-diameter culture dishes. Western blot experiments were performed as described previously [14]. The rabbit monoclonal antibodies anti-BiP (B1770, United States Biological, Euromedex, Souffelweyersheim, France) and anti-PERK (clone C33E10, 3192, Cell Signaling Technology, Ozyme, Saint-Quentin en Yvelines, France), the mouse monoclonal anti-LAMP2 (sc-18822, Santa Cruz Biotechology, Heidelberg, Germany), the rabbit polyclonal anti-calumenin (HPA006018, Sigma-Aldrich), and the goat polyclonal antibody anti-Actin (sc-1615, Santa Cruz Biotechnology) were diluted at 1:1000. The immunostaining was observed with a ChemiDoc™ XRS imaging system (Bio-Rad Laboratories). For PERK electrophoretic mobility shift detection, blots were developed on X-ray films (Amersham, GE Healthcare Life sciences).
Metabolic labeling
MDA-MB-231 cells treated for 30 h or not with 2-DG (5 mM) were then metabolically labeled for 2 h with 150 µCi of (2-3H)mannose. The lipid-linked oligosaccharides (LLO) and the N-linked glycoproteins (N-GP) were extracted and processed as described elsewhere [15].
Semi-quantitative reverse transcription-polymerase chain reaction (RT-PCR)
MDA-MB-231 (1.8 × 105 cells) and MCF-7 cells (1.6 × 105 cells) were seeded in 12-well plates. Total RNA was extracted using TRIzol® Reagent (Invitrogen, Thermo Fisher Scientific) according to the manufacturer’s instructions. Total RNA concentration was determined with a spectrophotometer (NanoDrop 2000c, Thermo Fisher Scientific). The cDNAs were synthetized and further amplified by PCR as previously described [14]. The primers sequences were : XBP-1 (NM_005080) forward 5′-TTACGAGAGAAAACTCATGGC-3′, reverse 5′-GGGTCCAAGTTGTCCAGAATGC-3′, PCR products length 282/256 base pairs (bp); RPLP0 (NM_053275; ribosomal protein, large, P0) forward 5′-ACAACCCAGCTCTGGAGAAA-3′, reverse 5′-TCGTTTGTACCCGTTGATGA-3′, PCR product length 530 bp. 25 µL of the PCR product were mixed with loading buffer (5 µL) and 15 µL of the mixture were submitted to electrophoresis (in a 3% agarose gel in case of XBP-1 analysis and a 1% agarose gel for RPLP0) at 100 V. The gel was stained with ethidium bromide, viewed and photographed on a UV-transilluminator (GelDoc 2000, Bio-Rad Laboratories).
Immunocytochemistry
MDA-MB-231 (1.8 × 105) and MCF-7 (1.6 × 105) cells were seeded on glass coverslips in 12-well plates. Cells were fixed and subjected to protein immunodetection and hoechst counterstaining, as previously described [14]. The mouse monoclonal antibody anti-CHOP (SC-7351, Santa Cruz Biotechnology) was diluted at 1:100. Fluorescence labeling was observed under an Eclipse 80i microscope (Nikon, Champigny-sur-Marne, France). Images were collected using LuciaG 4.81 software (Nikon).
Measurement of lactate production
Cell culture media were collected for each condition and lactate concentration was measured using an YSI 2950 Biochemistry Analyzer (YSI Life Sciences, Yellow Springs, OH, USA). Production of lactate was calculated by subtracting the blank value (medium without cultured cells) from the lactate concentration measured for each condition. The values were normalized to cell number evaluated by crystal violet staining assay.
Statistical analysis
The results were depicted as mean ± standard error of the mean (s.e.m) of at least three independent experiments. Statistical analyses were performed using one-way analysis of variance (ANOVA) followed by the Bonferroni post-test for multiple comparisons (GraphPad InStat software, San Diego, CA, USA). Differences in which P-value was less than 0.05 were statistically significant.
Results
2-DG treatment exhibits anticancer effects on MDA-MB-231 and MCF-7 cells
To assess the anti-proliferative properties of 2-DG on breast cancer cells, the hormone-independent MDA-MB-231 and hormone-dependent MCF-7 breast cancer cell lines were treated for 48 h with increasing concentrations of 2-DG. Crystal violet staining revealed that 2-DG-induced a significant dose-dependent decrease of cell number for both cell lines (Fig. 1). The concentration leading to a 50% decrease in cell number (IC50) was 4.2 ± 0.5 and 3.1 ± 0.5 mM in MDA-MB-231 and MCF-7 cells, respectively. Thus, both the hormone-dependent and hormone-independent breast cancer cell lines were sensitive to 2-DG.
2-DG induces a decrease in cell number. MDA-MB-231 (a) and MCF-7 (b) cells were treated for 48 h with increasing concentrations of 2-DG. Control cells were not treated. Cell number was evaluated by a crystal violet staining assay and the IC50 were determined. Results are depicted as mean ± SEM of at least three independent counts performed in triplicate. Significant differences with control cells are indicated (**P < 0.01; ***P < 0.001)
2-DG triggers transient ER stress in breast cancer cells
To determine whether 2-DG treatment induces ER stress in MDA-MB-231 and MCF-7 breast cancer cells, we followed several key players of the UPR : (i) the phosphorylation of the pancreatic endoplasmic reticulum kinase-like endoplasmic reticulum kinase (PERK), (ii) the cleavage of the inositol requiring enzyme 1 (IRE1)-dependent X-box-binding protein-1 (XBP-1) mRNA, and (iii) the expression of the immunoglobulin heavy chain binding protein (BiP), a luminal ER chaperone [16]. We used concentrations above the obtained IC50 values of 2-DG, 5 and 4 mM for MDA-MB-231 and MCF-7 cells, respectively.
In MDA-MB-231 cells, we observed an early and transient increase of PERK phosphorylation, as demonstrated by its transient mobility shift (Fig. 2a). This shift in molecular weight was evident after 6 h of treatment with 2-DG and then progressively disappeared up to 72 h. RT-PCR analysis also revealed a transient cleavage of XBP-1 mRNA in 2-DG-treated cells (Fig. 2b). Indeed, both spliced and unspliced forms of XBP-1 mRNA were only observed after 6 h of exposure to 2-DG. The spliced form was not yet detectable after 1 h and was no more present after 24 h. Regarding the chaperone BiP, its expression increased in response to 2-DG with a maximum of induction after 24 h and was maintained up to 72 h (Fig. 2a). In MCF-7 cells, 6 h after addition of 2-DG, PERK displayed a high electrophoretic shift which then gradually decreased (Fig. 2a). No evident splicing of XBP-1 mRNA was detected after exposure to 2-DG (Fig. 2b). The expression of BiP was enhanced with a maximum after 24 h of exposure to 2-DG and decreased after 48 h (Fig. 2a). Control untreated cells did not exhibit any of these modifications.
2-DG triggers a transient ER stress. MDA-MB-231 and MCF-7 cells were treated for indicated times with 2-DG (5 and 4 mM, respectively) or were not treated (Control, Ctrl). Cells were harvested for protein (a, c) or RNA (b) analysis. a PERK phosphorylation and BiP expression were detected by western blotting. Actin was used as a loading control. Protein MW (kDa) are indicated on the right. b XBP-1 mRNA expression was studied by RT-PCR. The 282 bp-long and 256 bp-long PCR products correspond to the unspliced and spliced forms of XBP-1 mRNA, respectively. The housekeeping gene RPLP0 was used as an internal control. c CHOP expression was analyzed by immunofluorescence. Cells were fixed and subjected to CHOP immunodetection. Cells were counterstained with Hoechst dye and the merged pictures were presented for each condition. Bar represents 10 µm
We also studied the transcription factor CEBP homologous protein (CHOP), a mediator of apoptosis whose expression is induced when the UPR is not sufficient to rescue ER functions. MDA-MB-231 and MCF-7 cells were treated for 24 and 48 h with 2-DG. In MDA-MB-231 cells, immunocytochemistry analysis revealed the induction of CHOP after 24 h of treatment, with both cytoplasmic and nuclear localizations (Fig. 2c). CHOP was still detected after 48 h but the immunostaining intensity was lower. Interestingly, in MCF-7 cells, CHOP protein expression was not induced after 2-DG treatment (Fig. 2c).
Altogether these results demonstrate that 2-DG triggers a transient ER stress, more pronounced in MDA-MB-231 cells than in MCF-7 cells.
2-DG treatment disrupts the N-linked glycosylation pathway in breast cancer cells
Based on these results, we then further wanted to determine whether the induction of ER stress observed in 2-DG-treated cells could arise from the disruption of the N-linked protein glycosylation process. To tackle this point, the steady-state glycosylation status of LAMP2, an extensively N-glycosylated lysosomal resident protein, and calumenin, a single N-linked glycosylated ER protein, were followed in MCF-7 and MDA-MB-231 cells exposed to 2-DG treatment for 24 or 48 h. As presented on western blots (Fig. 3), while a subtle change in the LAMP2 mobility arguing for slight heterogeneity in glycosylation could be observed after 24 h of 2-DG treatment, a stronger increase in LAMP2 gel mobility was observed after 48 h of 2-DG treatment for both cell lines. Moreover, our results also show that 2-DG treatment only affects the steady-state level of LAMP2 in MDA-MB-231 treated cells. Remarkably, when mannose was added to the cell culture, the observed altered gel mobility of LAMP2 was completely suppressed in 2-DG-treated cells. This was clearly the case for both MDA-MB-231 and MCF7 cells. The stability of LAMP2 is rescued in 2-DG-treated MDA-MB-231 cells likely due to the restoration of the N-linked glycosylation pathway. Calumenin also presented a gel mobility shift in 2-DG-treated MDA-MB-231, completely reversed by addition of mannose, whereas no shift was observed in MCF-7 cells (Fig. 3).
Mannose prevents the 2-DG-induced alteration of N-linked protein glycosylation. MDA-MB-231 and MCF-7 cells were treated or not (Ctrl) with 2-DG (5 and 4 mM, respectively) in the presence (+) or absence (−) of mannose (Man, 1 mM). Western blot analysis was then performed using anti-LAMP2, anti-calumenin, and anti-actin antibodies. Actin was used as a loading control. Protein MW (kDa) is indicated on the right
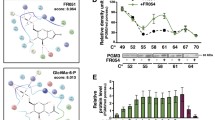
In order to assess the ER N-glycosylation defect, metabolic labeling with (2-3H) mannose was performed in MDA-MB-231 cells treated or not with 2-DG. Lipid-linked oligosaccharides (LLO) and N-linked glycoproteins (N-GP) were extracted and analyzed by HPLC. The results show that 2-DG treatment affects the ER N-glycosylation process with the appearance of an abnormal Man7GlcNAc2 structure both on LLO and N-GP of 2-DG incubated MDA-MB-231 cells (Fig. 4). Altogether these results demonstrate that (i) 2-DG treatment disrupts the N-linked glycosylation pathway and (ii) the mannose supplementation prevents the action of 2-DG on this pathway.
MDA-MB-231 cells treated or not (Ctrl) with 2-DG (5 mM) were incubated with [2-3H]mannose for 2 h. After sequential extraction, LLO and N-GP were analyzed by HPLC as described in Materials and Methods. G1-3M9Gn2 indicates oligomannosides containing one, two, or three Glc, nine Man, and two GlcNAc residues. M7Gn2, M8Gn2, and M9Gn2 indicate oligomannosides containing seven, eight, or nine Man and two GlcNAc residues, respectively
The 2-DG-induced disruption of the N-linked glycosylation pathway leads to ER stress in breast cancer cells
In order to assess whether ER stress induced by 2-DG treatment was a consequence of the alteration of the N-linked glycosylation of proteins, cells were exposed to 2-DG in the presence or absence of mannose to follow the expression of ER stress markers. In both cell lines, the presence of mannose prevented the phosphorylation of PERK and the induction of BiP expression, usually observed in response to 2-DG treatment (Fig. 5a). Similarly, in MDA-MB-231 cells, the cleavage of XBP-1 mRNA observed after 6 h of treatment with 2-DG was absent in the presence of mannose (Fig. 5b). The increase in the expression of CHOP induced by a 24 h 2-DG treatment of MDA-MB-231 cells was also highly reduced in the presence of mannose (Fig. 5c). Due to the absence of XBP-1 mRNA cleavage and CHOP expression in 2-DG-treated MCF-7 cells, the impact of competition with mannose was not studied in this cell line. Thus, addition of exogenous mannose tends to suppress the effects of 2-DG on N-linked glycosylation pathway and ER stress.
Mannose prevents 2-DG-induced ER stress. MDA-MB-231 and MCF-7 cells were treated or not (Control, Ctrl) for indicated times with 2-DG (5 and 4 mM, respectively) in the presence (+) or absence (−) of mannose (Man, 1 mM). Cells were harvested for protein (a, c) or RNA (b) analysis. a Western blot analysis was performed using anti-PERK and anti-BiP antibodies. Actin was used as a loading control. Protein MW (kDa) is indicated on the right. b RT-PCR analysis was carried out using specific primers to detect XBP-1 mRNA expression. The 282 bp-long and 256 bp-long PCR products correspond respectively to the unspliced and spliced forms of XBP-1 mRNA. The housekeeping gene RPLP0 was used as a control. c MDA-MB-231 cells were fixed and CHOP protein was immunodetected. Cells were additionally counterstained with Hoechst dye and the merged photos were presented for each condition. Bar represents 10 µm
2-DG still induces the inhibition of glycolysis in the presence of mannose
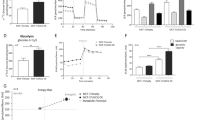
MDA-MB-231 and MCF-7 cells were treated for 48 h with 2-DG and the production of lactate was measured as an indicator of the glycolytic activity. After addition of 2-DG, we observed a 2.3-fold and 3.3-fold decrease in lactate production in MDA-MB-231 (Fig. 6a) and MCF-7 cells (Fig. 6b), respectively. Production of lactate was thus significantly reduced in 2-DG-treated cells. Nevertheless, addition of mannose did not impact the induced 2-DG decrease of lactate production in MDA-MB-231 and MCF-7 cells (Fig. 6). These results demonstrate that addition of mannose only suppresses the observed ER stress related to 2-DG-induced inhibition of N-linked glycosylation but does not affect the 2-DG-induced inhibition of glycolysis.
2-DG reduces lactate production, even in the presence of mannose. MDA-MB-231 (a) and MCF-7 (b) cells were treated or not for 48 h with 2-DG (5 and 4 mM, respectively), in the presence (+) or absence (−) of mannose (Man, 1 mM). Lactate concentration in culture medium was assessed using a biochemistry analyser and cell number was evaluated by a crystal violet staining assay. Production of lactate per cell was then calculated for each condition. Results are depicted as mean ± SEM of three independent experiments. **P < 0.01 compared with control cells. ***P < 0.001 compared with control cells. Not significant (ns) between conditions with or without mannose
Both inhibition of glycolysis and N-linked glycosylation contribute to 2-DG anticancer activity
To characterize the relative contribution of glycosylation and glycolysis inhibition in the anticancer effects of 2-DG, MDA-MB-231 and MCF-7 cells were treated for 48 h with 2-DG in the presence or absence of mannose and cell number was evaluated by a crystal violet staining assay. First, addition of mannose alone did not modify the cell number compared to control conditions (Fig. 7). A 70% decrease in the MDA-MB-231 cell number was observed following 2-DG treatment (Fig. 7a). In the presence of mannose, this decrease was limited to 44%. Thus in MDA-MB-231 cells, mannose supplementation only reduced the anticancer effect of 2-DG by 37% (1–44%/70%). In MCF-7 cells, a 42% reduction in the number of 2-DG-treated cells was detected (Fig. 7b). In the presence of mannose, cell number was only diminished by 22%. Thus in MCF-7 cells, mannose reduced the anticancer effect of 2-DG by 47% (1–22%/42%). Interference with N-linked glycosylation of proteins thus appeared to contribute partially to the anticancer effects of 2-DG in these breast cancer cells.
Effects of 2-DG on cell number are attenuated in the presence of mannose. MDA-MB-231 (a) and MCF-7 (b) cells were treated or not for 48 h with 2-DG (5 and 4 mM, respectively) in the presence (+) or absence (−) of mannose (Man, 1 mM). Cell number was determined by a crystal violet staining assay. Results are depicted as mean ± SEM of three independent counts performed in triplicate. ***P < 0.001 compared with control cells. #P < 0.05 between conditions with or without mannose. ###P < 0.001 between conditions with or without mannose
Discussion
It has been demonstrated that 2-DG, a known glycolysis inhibitor, reduces energy production in several types of cancer cells [7]. However, 2-DG treatment affects several other intracellular activities and its mode of action is complex. In the present work, we studied two breast cancer cell lines in order to determine the part played by glycolysis inhibition and N-linked glycosylation interference, respectively, in the anticancer effects of 2-DG.
First, we characterized the effects of 2-DG on breast cancer cells by analyzing cell number. Our results showed that both MDA-MB-231 and MCF-7 cells were affected by 2-DG. The measured IC50 (3.1 and 4.2 mM for MCF-7 and MDA-MB-231 cells, respectively) after 48 h of 2-DG treatment were in the millimolar range and in accordance with previously reported values (from 4.2 mM to 10 mM) [17,18,19,20]. Differences in sensitivity to 2-DG between breast cancer cell lines have already been reported by Aft et al., with SKBR-3 being the most sensitive one [21]. These differences in sensitivity could be the result of differences in the kinetics of 2-DG uptake. The differences among the studies could be explained by the method used to monitor cell number and by the treatment duration. The culture medium used for cell growth and its glucose concentration could also enter into account [22].
In the present work, using a real-time (2-3H)mannose metabolic labeling, we show that 2-DG alters the ER N-glycosylation process in MDA-MB-231 cells, reinforcing the data obtained by Kurtoglu et al. [13]. 2-DG affects the LLO structures with the appearance of shorter LLO structures that can still be transferred onto newly synthesized glycoproteins, although less efficiently than the Glc3Man9GlcNAc2-PP-Dol. As such, the consequence is the lack of N-glycan structures on certain N-glycosylation sites and the presence of abnormal N-glycan structures transferred onto newly synthesized glycoproteins. 2-DG treatment appears much lighter compared to a treatment with tunicamycin, a strong inhibitor of the N-glycosylation process, which prevents the formation of GlcNAc-PP-dolichol/LLO [23]. Several findings illustrate the importance of glycosylation in tumor growth and malignant transformation but also in the modulation of the responsiveness of cancer cells to treatments [23]. Indeed, in gastrointestinal tumors, 2-DG-induced the reduction of the glycosylation of the proto-oncogene KIT accompanied by inhibition of its phosphorylation and membrane expression [24]. Besides, maintenance of the breast cancer SKBR-3 cells in tunicamycin-containing medium increased their sensitivity to herceptin and doxorubicin [25]. These data clearly highlight a potential interest for glycosylation inhibitors in breast cancer treatment.
Competition with mannose completely prevents the 2-DG effects on both N-glycosylation process and ER stress activation. These data strongly suggest that ER stress due to the accumulation of unfolded proteins is the consequence of an ER N-linked protein glycosylation pathway alteration observed in MDA-MB-231 and MCF-7 cells. These results strengthen a set of data obtained in different type of cell lines, including MDA-MB-231 and SKBR-3 breast cancer cells [13, 20, 26,27,28,29]. We further demonstrated that ER stress was transient in both cell lines and XBP-1 mRNA splicing absent in MCF-7 cells. This could be explained by a lower impact of 2-DG on the N-linked glycosylation process in MCF-7 cells, as shown on LAMP2 and calumenin molecular shifting. Moreover, such a difference of sensitivity between the two cell lines is in agreement with other studies. Indeed, thiazolidinediones derivatives (Δ2-TGZ and TZD18) and the indole-3-carbinol cyclic tetrameric derivative CTet were reported to induce a more extended splicing of XBP-1 mRNA in MDA-MB-231 cells compared to MCF-7 cells [14, 30, 31]. At this time, it is difficult to determine if these differences are a consequence of their different molecular marker expression profile (estrogen receptor).
The induction of ER stress could be protective for the cells [7]. In the case of the 2-DG treatment performed in our study, the results of our competition experiments using mannose disagree with a protective role of ER stress since mannose, a compound that prevents this process, reverses 2-DG cytotoxicity. Such a reversion of ER stress and UPR in the presence of mannose has never been described for these two cell lines but was previously observed in other cell types [13, 28, 29]. If ER stress is not protective and the cell cannot overcome this process, the up-regulation of CHOP could lead to the activation of an UPR-specific apoptotic pathway [32]. Indeed, we confirm that 2-DG induces CHOP expression in MDA-MB-231, but surprisingly we were not able to detect CHOP protein in MCF-7 cells. This absence could be explained by the partial ER stress response observed in MCF-7 cells. This data strongly suggest that CHOP protein may not be the mediator of the 2-DG-induced cytotoxic effect associated with the N-glycosylation alteration in MCF-7 cells. This absence of link between apoptosis and ER stress has been previously illustrated in MCF-7 and LNCaP cells treated with thiazolidinediones [18, 33]. In contrast, in lymphoma and rhabdomyosarcoma cells, 2-DG induces an UPR-mediated mitochondrial apoptosis involving CHOP and ATF-4 [29, 34, 35]. This discrepancy could be dependent on the cellular context.
Then, we analyzed the effects of 2-DG on glycolysis. We observed in both MCF-7 and MDA-MB-231 cells exposed to 2-DG for 48 h that lactate production was greatly reduced. This result is in agreement with other studies performed in MCF-7 in which the inhibiting effect of 2-DG on glycolysis were appreciated by ATP measurement [17, 19, 36]. In the presence of mannose, ER stress and UPR did not occur but the decrease in lactate production was still observed in 2-DG-treated cells indicating that mannose did not interfere with glycolysis inhibition, supporting previous data [37]. Since in absence of ER stress and UPR, cell number was still affected by 2-DG, it indicates that inhibition of glycolysis is involved in the anticancer effect of 2-DG in our two cell lines and that N-glycosylation inhibition does not act alone. This is consistent with results obtained in T cell lymphoma cell lines [34] whereas inhibition of N-linked glycosylation has been reported as the predominant mechanism leading to 2-DG’s cytotoxicity in other studies [13, 24, 28, 29, 35]. We used 2-DG at concentrations slightly higher than the IC50 we measured. It could be interesting to complete this work by an analysis of the effect of lower doses. Indeed, a hierarchy of 2-DG’s activity could exist where at low concentrations it interferes with N-linked glycosylation but at moderate concentrations glycolysis is also inhibited [38]. This could be due to the 50 times lower concentration of mannose as compared to glucose found not only in culture medium but also in human blood [26].
To conclude, our data reveal that both protein N-glycosylation and glycolysis inhibitions contribute to the anticancer effect of 2-DG in MDA-MB-231 and MCF-7 breast cancer cells. Thus, 2-DG has really to be considered both as a glycolytic and as a glycosylation inhibitor. The right association and clinical applications of this agent has still to be defined but at this time, increasing our knowledge about its mode of action is crucial.
Abbreviations
- 2-DG:
-
2-Deoxyglucose
- BiP:
-
Binding immunoglobulin protein
- CHOP:
-
Transcription factor CEBP homologous protein
- ER:
-
Endoplasmic reticulum
- Glc:
-
Glucose
- GlcNAc:
-
N-Acetylglucosamine
- IC50 :
-
Half maximal inhibitory concentration
- IRE1:
-
Inositol requiring enzyme 1
- LAMP2:
-
Lysosomal-associated membrane protein 2
- LLO:
-
Lipid-linked oligosaccharides
- Man:
-
Mannose
- N-GP:
-
N-linked glycoproteins
- PERK:
-
Pancreatic endoplasmic reticulum kinase-like endoplasmic reticulum kinase
- UPR:
-
Unfolded protein response
- XBP-1:
-
X-box-binding protein-1
References
Koppenol WH, Bounds PL, Dang CV (2011) Otto Warburg’s contributions to current concepts of cancer metabolism. Nat Rev Cancer 11(5):325–337. https://doi.org/10.1038/nrc3038
Gambhir SS (2002) Molecular imaging of cancer with positron emission tomography. Nat Rev Cancer 2(9):683–693. https://doi.org/10.1038/nrc882
Cairns RA, Harris IS, Mak TW (2011) Regulation of cancer cell metabolism. Nat Rev Cancer 11(2):85–95. https://doi.org/10.1038/nrc2981
Gatenby RA, Gillies RJ (2004) Why do cancers have high aerobic glycolysis? Nat Rev Cancer 4(11):891–899. https://doi.org/10.1038/nrc1478
Zhao Y, Butler EB, Tan M (2013) Targeting cellular metabolism to improve cancer therapeutics. Cell Death Dis 4:e532. https://doi.org/10.1038/cddis.2013.60
Porporato PE, Dhup S, Dadhich RK, Copetti T, Sonveaux P (2011) Anticancer targets in the glycolytic metabolism of tumors: a comprehensive review. Front Pharmacol 2:49. https://doi.org/10.3389/fphar.2011.00049
Kuntz S, Mazerbourg S, Boisbrun M, Cerella C, Diederich M, Grillier-Vuissoz I, Flament S (2014) Energy restriction mimetic agents to target cancer cells: comparison between 2-deoxyglucose and thiazolidinediones. Biochem Pharmacol 92(1):102–111. https://doi.org/10.1016/j.bcp.2014.07.021
Nakada HI, Wick AN (1956) The effect of 2-deoxyglucose on the metabolism of glucose, fructose, and galactose by rat diaphragm. J Biol Chem 222(2):671–676
Chen W, Gueron M (1992) The inhibition of bovine heart hexokinase by 2-deoxy-d-glucose-6-phosphate: characterization by 31P NMR and metabolic implications. Biochimie 74(9–10):867–873
Wick AN, Drury DR, Nakada HI, Wolfe JB (1957) Localization of the primary metabolic block produced by 2-deoxyglucose. J Biol Chem 224(2):963–969
Datema R, Schwarz RT (1978) Formation of 2-deoxyglucose-containing lipid-linked oligosaccharides. Interference with glycosylation of glycoproteins. Eur J Biochem 90(3):505–516
Schmidt MF, Schwarz RT, Scholtissek C (1974) Nucleoside-diphosphate derivatives of 2-deoxy-d-glucose in animal cells. Eur J Biochem 49(1):237–247
Kurtoglu M, Gao N, Shang J, Maher JC, Lehrman MA, Wangpaichitr M, Savaraj N, Lane AN, Lampidis TJ (2007) Under normoxia, 2-deoxy-d-glucose elicits cell death in select tumor types not by inhibition of glycolysis but by interfering with N-linked glycosylation. Mol Cancer Ther 6(11):3049–3058. https://doi.org/10.1158/1535-7163.MCT-07-0310
Berthe A, Flament S, Grandemange S, Zaffino M, Boisbrun M, Mazerbourg S (2016) Delta2-Troglitazone promotes cytostatic rather than pro-apoptotic effects in breast cancer cells cultured in high serum conditions. Cell Cycle 15(24):3402–3412. https://doi.org/10.1080/15384101.2016.1245248
Peanne R, Vanbeselaere J, Vicogne D, Mir AM, Biot C, Matthijs G, Guerardel Y, Foulquier F (2013) Assessing ER and Golgi N-glycosylation process using metabolic labeling in mammalian cultured cells. Methods Cell Biol 118:157–176. https://doi.org/10.1016/B978-0-12-417164-0.00010-0
Bravo R, Parra V, Gatica D, Rodriguez AE, Torrealba N, Paredes F, Wang ZV, Zorzano A, Hill JA, Jaimovich E, Quest AF, Lavandero S (2013) Endoplasmic reticulum and the unfolded protein response: dynamics and metabolic integration. Int Rev Cell Mol Biol 301:215–290. https://doi.org/10.1016/b978-0-12-407704-1.00005-1
Tagg SL, Foster PA, Leese MP, Potter BV, Reed MJ, Purohit A, Newman SP (2008) 2-Methoxyoestradiol-3,17-O,O-bis-sulphamate and 2-deoxy-d-glucose in combination: a potential treatment for breast and prostate cancer. Br J Cancer 99(11):1842–1848. https://doi.org/10.1038/sj.bjc.6604752
Wei S, Kulp SK, Chen CS (2010) Energy restriction as an antitumor target of thiazolidinediones. J Biol Chem 285(13):9780–9791. https://doi.org/10.1074/jbc.M109.065466
Zhu Z, Jiang W, McGinley JN, Thompson HJ (2005) 2-Deoxyglucose as an energy restriction mimetic agent: effects on mammary carcinogenesis and on mammary tumor cell growth in vitro. Cancer Res 65(15):7023–7030. https://doi.org/10.1158/0008-5472.CAN-05-0453
Huang YY, Liu H, Li Y, Pu LJ, Jiang CC, Xu JC, Jiang ZW (2013) Down-regulation of RIP1 by 2-deoxy-d-glucose sensitizes breast cancer cells to TRAIL-induced apoptosis. Eur J Pharmacol 705(1–3):26–34. https://doi.org/10.1016/j.ejphar.2013.02.005
Aft RL, Zhang FW, Gius D (2002) Evaluation of 2-deoxy-d-glucose as a chemotherapeutic agent: mechanism of cell death. Br J Cancer 87(7):805–812. https://doi.org/10.1038/sj.bjc.6600547
Kaplan O, Navon G, Lyon RC, Faustino PJ, Straka EJ, Cohen JS (1990) Effects of 2-deoxyglucose on drug-sensitive and drug-resistant human breast cancer cells: toxicity and magnetic resonance spectroscopy studies of metabolism. Cancer Res 50(3):544–551
Vasconcelos-Dos-Santos A, Oliveira IA, Lucena MC, Mantuano NR, Whelan SA, Dias WB, Todeschini AR (2015) Biosynthetic machinery involved in aberrant glycosylation: promising targets for developing of drugs against cancer. Front Oncol 5:138. https://doi.org/10.3389/fonc.2015.00138
Mühlenberg T, Grunewald S, Treckmann J, Podleska L, Schuler M, Fletcher JA, Bauer S (2015) Inhibition of KIT-glycosylation by 2-deoxyglucose abrogates KIT-signaling and combination with ABT-263 synergistically induces apoptosis in gastrointestinal stromal tumor. PLoS ONE 10(3):e0120531. https://doi.org/10.1371/journal.pone.0120531
Peiris D, Spector AF, Lomax-Browne H, Azimi T, Ramesh B, Loizidou M, Welch H, Dwek MV (2017) Cellular glycosylation affects herceptin binding and sensitivity of breast cancer cells to doxorubicin and growth factors. Sci Rep 7:43006. https://doi.org/10.1038/srep43006
Liu H, Kurtoglu M, Cao Y, Xi H, Kumar R, Axten JM, Lampidis TJ (2013) Conversion of 2-deoxyglucose-induced growth inhibition to cell death in normoxic tumor cells. Cancer Chemother Pharmacol 72(1):251–262. https://doi.org/10.1007/s00280-013-2193-y
Ramirez-Peinado S, Leon-Annicchiarico CL, Galindo-Moreno J, Iurlaro R, Caro-Maldonado A, Prehn JH, Ryan KM, Munoz-Pinedo C (2013) Glucose-starved cells do not engage in prosurvival autophagy. J Biol Chem 288(42):30387–30398. https://doi.org/10.1074/jbc.M113.490581
Merchan JR, Kovacs K, Railsback JW, Kurtoglu M, Jing Y, Pina Y, Gao N, Murray TG, Lehrman MA, Lampidis TJ (2010) Antiangiogenic activity of 2-deoxy-d-glucose. PLoS ONE 5(10):e13699. https://doi.org/10.1371/journal.pone.0013699
Ramirez-Peinado S, Alcazar-Limones F, Lagares-Tena L, El Mjiyad N, Caro-Maldonado A, Tirado OM, Munoz-Pinedo C (2011) 2-Deoxyglucose induces Noxa-dependent apoptosis in alveolar rhabdomyosarcoma. Cancer Res 71(21):6796–6806. https://doi.org/10.1158/0008-5472.CAN-11-0759
Galluzzi L, De Santi M, Crinelli R, De Marco C, Zaffaroni N, Duranti A, Brandi G, Magnani M (2012) Induction of endoplasmic reticulum stress response by the indole-3-carbinol cyclic tetrameric derivative CTet in human breast cancer cell lines. PLoS ONE 7(8):e43249. https://doi.org/10.1371/journal.pone.0043249
Zang C, Liu H, Bertz J, Possinger K, Koeffler HP, Elstner E, Eucker J (2009) Induction of endoplasmic reticulum stress response by TZD18, a novel dual ligand for peroxisome proliferator-activated receptor alpha/gamma, in human breast cancer cells. Mol Cancer Ther 8(8):2296–2307. https://doi.org/10.1158/1535-7163.mct-09-0347
Zinszner H, Kuroda M, Wang X, Batchvarova N, Lightfoot RT, Remotti H, Stevens JL, Ron D (1998) CHOP is implicated in programmed cell death in response to impaired function of the endoplasmic reticulum. Genes Dev 12(7):982–995
Colin-Cassin C, Yao X, Cerella C, Chbicheb S, Kuntz S, Mazerbourg S, Boisbrun M, Chapleur Y, Diederich M, Flament S, Grillier-Vuissoz I (2015) PPARγ-inactive ∆2-troglitazone independently triggers ER stress and apoptosis in breast cancer cells. Mol Carcinog 54(5):393–404. https://doi.org/10.1002/mc.22109
Zagorodna O, Martin SM, Rutkowski DT, Kuwana T, Spitz DR, Knudson CM (2012) 2-Deoxyglucose-induced toxicity is regulated by Bcl-2 family members and is enhanced by antagonizing Bcl-2 in lymphoma cell lines. Oncogene 31(22):2738–2749. https://doi.org/10.1038/onc.2011.454
Leon-Annicchiarico CL, Ramirez-Peinado S, Dominguez-Villanueva D, Gonsberg A, Lampidis TJ, Munoz-Pinedo C (2015) ATF4 mediates necrosis induced by glucose deprivation and apoptosis induced by 2-deoxyglucose in the same cells. FEBS J 282(18):3647–3658. https://doi.org/10.1111/febs.13369
Cheng G, Zielonka J, Dranka BP, McAllister D, Mackinnon AC Jr, Joseph J, Kalyanaraman B (2012) Mitochondria-targeted drugs synergize with 2-deoxyglucose to trigger breast cancer cell death. Cancer Res 72(10):2634–2644. https://doi.org/10.1158/0008-5472.CAN-11-3928
Xi H, Kurtoglu M, Liu H, Wangpaichitr M, You M, Liu X, Savaraj N, Lampidis TJ (2011) 2-Deoxy-d-glucose activates autophagy via endoplasmic reticulum stress rather than ATP depletion. Cancer Chemother Pharmacol 67(4):899–910. https://doi.org/10.1007/s00280-010-1391-0
Xi H, Kurtoglu M, Lampidis TJ (2014) The wonders of 2-deoxy-d-glucose. IUBMB Life 66(2):110–121. https://doi.org/10.1002/iub.1251
Funding
This project was funded by University of Lorraine and Région of Lorraine. Audrey Berthe and Claire Muller were recipient of a PhD grant of the “Ministère de l’Enseignement Supérieur et de la Recherche”.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Rights and permissions
About this article
Cite this article
Berthe, A., Zaffino, M., Muller, C. et al. Protein N-glycosylation alteration and glycolysis inhibition both contribute to the antiproliferative action of 2-deoxyglucose in breast cancer cells. Breast Cancer Res Treat 171, 581–591 (2018). https://doi.org/10.1007/s10549-018-4874-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10549-018-4874-z