Abstract
Despite the well-established link between parental depressive symptoms and children’s internalizing symptoms, studies that divide transmission into gender-specific components remain scarce. Therefore, the present study focused on gender-specific associations between internalizing symptoms of parents and children over the course of early school age, a key stage where gender-specific roles are increasingly adopted. Participants were 272 children (49.6% girls) oversampled for internalizing symptoms. Parents completed questionnaires twice during early school age (mean age time 1 = 7.4 years; SD = 0.24; mean age time 2 = 8.5 years; SD = 0.28). Mothers and fathers separately reported on their own depressive symptoms and their child’s internalizing symptoms. Latent multiple group analyses indicated gender-independent stability as well as gender-specific relations between parental and child outcomes. Maternal depressive symptoms were concurrently associated with symptoms of girls and boys, while paternal symptoms were concurrently associated only with symptoms of boys, but not of girls. Moreover, the associations between children and the parent of the same gender became more relevant over time, suggesting a growing identification with the same-gender model, particularly for fathers and boys. In regard to prospective effects, girls’ internalizing symptoms at age 7 predicted paternal depressive symptoms 1 year later. In a rigorous longitudinal design, this study underscores the importance of gender specificity in the associations of internalizing symptoms between children and their mothers and fathers after controlling for symptom stability over time. The study also raises the interesting possibility that girls’ internalizing symptoms elicit similar symptoms in their fathers.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
A wealth of studies testifies to the importance of intergenerational transmission of internalizing symptoms from parents to offspring [32]. However, the complex and individual interplay of internalizing symptoms in families remains incompletely understood. To date, the vast majority of studies has focused on associations between mother and child or combined reports from both parents to study parent–offspring transmission [58]. By contrast, studies accounting for both mother– and father–offspring associations as well as the role of child gender remain scarce [31]. In a comprehensive review, Connell and Goodman [11] stressed the need for research on the transmission for girls and boys due to a lack of gender-specific research. The current study addresses this pressing need by focusing on gender-specific transmission between parental depressive symptoms and children’s internalizing symptoms over the course of early school age.
Genetic, but also environmental, factors (e.g. parenting influences, role modelling) may contribute to the familial transmission of internalizing symptoms [4, 20]. In dismantling familial transmission into its gender-specific components, our study may be viewed in the light of work addressing the differential socialization of girls and boys [54] as well as the specific roles of mothers and fathers in parenting [45]. Paquette suggests that different parenting dimensions form children’s attachment to mothers and fathers: mothers act as “primary caregiver” in calming and comforting the child, whereas fathers act as “primary playmate” in engaging in exciting and playful activities with their child [45]. In this context, between the mother and child attachment relationship and the father and child activation relationship can be distinguished [45]. The differential parenting roles underscore the importance of taking into account both the father–child dyad and the mother–child dyad when examining intergenerational transmission.
Moreover, the mechanisms of the gender-specific symptom transmission in the family might be understood against the backdrop of gender cognition theory. A central tenet of the developmental theories on gender cognition concerns the gender identity development of children, which promotes increasing integration of stereotypes of the same gender into their self-image [56]. Children progress through different stages regarding their knowledge of gender identity. At the age of about 2–3 years, most children succeed in assigning themselves to the category “girls” or “boys”. However, the children’s categorization is based primarily on physical characteristics as well as stereotype clothing and behavioural patterns. At the age of about 4–5 years, they realize that their basic gender identity does not change over time. Finally, they reach the stage of gender constancy at the age of about 6–7 years: the children now understand that their gender is irreversible, not only in terms of time but also across situations, regardless of changes in surface qualities such as hair length, clothing, and behaviour [8, 36]. Once they reach the last stage, Kohlberg postulated that children are highly motivated to imitate gender stereotypes to reduce cognitive dissonance and build high self-esteem [36].
In other words, as awareness of gender identity and constancy grows, children are thought to increasingly strive for gender-congruent behaviour [22, 36]. This emerging goal of gender congruency therefore potentially entails an important role for same-gender effects in parent–offspring transmission of symptoms. Moreover, regarding the socialization of girls and boys, social learning theory proposes that children adjust their behaviour more strongly to a same-gender model because of greater similarity to themselves [8]. Learning from a same-gender model may also help the child to gain safety and guidance on what behaviours are expected, effective and useful in different situations, depending on one’s own gender [17].
Gender-specific transmission of internalizing symptoms
The effects of maternal depressive symptoms on child internalizing symptoms are well established and seem higher than for fathers, especially in early and middle childhood [11]. This pattern might be due to the mothers’ unique position in child development, including their common role as “primary caregiver” [45, 51], but also prenatal influence [27], or the higher prevalence of depression in women [37]. At the same time, the relative lack of research on paternal influences makes these patterns difficult to interpret [46]. The few studies on father–offspring transmission indicate, however, that paternal depressive symptoms may be uniquely associated with their child’s internalizing symptoms as well [5, 31].
In line with theory about same-gender effects, several studies have shown that maternal depressive symptoms are more strongly related to internalizing symptoms in girls than in boys, while paternal depressive symptoms are more strongly related to maladjustment such as low prosocial behaviour in boys than in girls [15, 25]. The influences in same-gender dyads may also be reciprocal, because parents tend to more strongly identify with a child of the same gender [11]. Following Coyne’s [13] interpersonal model, depressive behaviours (e.g. social withdrawal) may contribute to symptom maintenance by prompting negative reactions from others, which enhance the depressed persons’ negative mood in terms of cyclic mutual maladjustment. Some researchers suggest that parents may react with frustration, stress, or self-blame to children’s internalizing symptoms. Moreover, parents may also question their parenting skills, which in turn might add to an elevated risk for prospective parental depressive symptoms [29]. Potentially, these processes may also become amplified in same-gender relative to opposite-gender dyads.
In accordance with these views, previous studies show that children’s internalizing symptoms in early and middle childhood were associated with later maternal depressive symptoms [18, 30]. Conversely, research on paternal intergenerational transmission have hitherto yielded inconsistent findings with unique support for reciprocal associations between fathers and daughters [19], fathers and sons [55], and no support for reciprocal associations, respectively [29]. In addition, the extant literature about reciprocal effects between paternal depressive symptoms and psychopathology in their children has focused exclusively on transmission during adolescence.
Research gaps at early school age
While parental psychopathology has been established as a key risk factor for children’s internalizing symptoms [58], little is known about gender-specific transmission of internalizing symptoms, especially at early school age (i.e. age 6–10). This gap is particularly notable given that the peak age of onset of most childhood anxiety disorders has been estimated to lie in this age band in recent work [12]. Moreover, children of early school age show prevalence rates of about 12.3–14.3% for anxiety, and 10.7% for relevant depressive symptoms [50]. Thus, examining childhood internalizing problems is essential given their high prevalence rates [50], high social impairment [3], stability through subsequent developmental periods [34], and high risk of recurrence [24].
Further, as outlined above, children at early school age become increasingly aware of their own gender constancy [8]. This circumstance influences the way in which they perceive themselves and their environment and can be accompanied by more positive evaluation of persons of the same gender than the opposite gender, potentially in the service of stabilizing their self-image [33]. Accordingly, the investigation of gender-specific transmission seems to be of special importance at this age.
Aims of the current study
The current study aims to describe individual, gender-specific transmission between parental depressive symptoms and children’s internalizing symptoms over the course of early school age. These associations were assessed concurrently and longitudinally modelling bidirectional effects between child and parent.
In the light of previous findings, we expected for both, longitudinal and cross-sectional relations that maternal depressive symptoms would be more strongly associated with both girls’ and boys’ internalizing symptoms than paternal depressive symptoms [11]. In contrast, based on the notion of same-gender transmission [8, 11], we expected for both longitudinal and cross-sectional associations paternal depressive symptoms to have stronger links to boys’ internalizing symptoms than to girls’ internalizing symptoms.
Method
Study design and participants
Families participated in a longitudinal study on trajectories of internalizing symptoms in children from preschool age onwards conducted at the Department of Child and Adolescent Psychiatry, Psychotherapy, and Psychosomatics at the University of Leipzig, in Germany. During recruitment, children were screened and oversampled for internalizing symptoms by using the Strengths and Difficulties Questionnaire (SDQ 4–16) [23]. Following the results of the SDQ 4–16, we invited families of children with internalizing symptoms (sum score ≥ 4 on the SDQ subscale emotional symptoms) and families with healthy children (all SDQ problem scales in normal range) to further visits in our project office. For more details of recruitment, also see the studies of von Klitzing et al. and Klein et al. [35, 57].
This study reports on a sample of 272 families (n = 135 girls, 49.6%), who were invited for two visits, and completed questionnaires at early elementary school age (time 1: Mage = 7.4 years; SD = 0.24), and 1 year later (time 2: Mage = 8.5 years; SD = 0.28). Based on the recruitment strategy, the sample represents an at-risk sample with n = 74 children (27.2%) with internalizing symptoms in borderline or abnormal range at early elementary school age (n = 34 girls, 45.9%). The educational level of parents was divided into three categories: 6.2% of mothers and 8.7% of fathers had a low educational level (including basic education), 51.2% of mothers and 44.6% of fathers had an intermediate educational level (secondary school certificate or high-school diploma), and 42.6% of mothers and 46.7% of fathers had a high educational level (bachelor or higher degree).
There were no gender differences with respect to age at time 1 [t(266) = 0.39, p = 0.69] and time 2 [t(246) = 0.41, p = 0.68], maternal education [U(117, 125) = 6445.0, z = − 1.80, p = 0.07], paternal education [U(108, 121) = 5954.5, z = − 1.29, p = 0.20], and internalizing symptoms at baseline [time 1: t(262) = − 0.73, p = 0.46; for more details see Table 1]. Further, girls’ and boys’ family characteristics were comparable regarding the residential situation [χ2(3, N = 260) = 1.82, p = 0.61]: 73.3% of girls and 76.0% of boys lived with both parents, 23.7% of girls and 23.3% of boys lived with a single parent (mostly with the mother, 96.7%), and 3.0% of girls and 0.7% of boys lived in shared physical custody arrangements.
Parental written consent and child assent were obtained prior to participation. The institutional review board of the Medical Faculty of the University of Leipzig, in Germany approved the study.
Measures
At both waves of data collection, mothers and fathers reported on their own and their children’s mental health. To assess maternal and paternal depressive symptoms, mothers and fathers completed the Depression Scale of the Patient Health Questionnaire (PHQ-9) [38]. The PHQ-9 uses diagnostic criteria from the DSM-IV and is a widely accepted, valid, reliable, and efficient diagnostic tool to screen for the presence and severity of depressive symptoms [40]. For example, the parents were asked if they had felt “down, depressed or hopeless” or had “little interest or pleasure in doing things” over the last 2 weeks. The scale comprises nine items scoring from 0 to 3 (0 = not at all, 1 = several days, 2 = more than half the days, 3 = nearly every day), with higher scores illustrating higher severity. In the current study, the internal consistency of the depression scale was α = 0.86 for mothers and α = 0.77–0.78 for fathers across the two waves of data collection. Maternal and paternal depressive symptoms at time 1 and 2 were represented by latent factors derived from the PHQ-9 using parcels.Footnote 1 The use of parcels has several advantages: a better goodness of fit [1] and a higher reliability [39] compared to item-level models. We created three parcels for each latent parental variable by random assignment, as described by Little et al. [39]. We used the same three parcels as indicators for mothers’ and fathers’ depressive symptoms. Each of the three parcels represents the mean score of three items from the PHQ-9.
Children’s internalizing symptoms were assessed using the emotional symptoms subscale of the Strengths and Difficulties Questionnaire (SDQ 4–16) [23]. Mothers and fathers reported on children’s anxiety, sadness, as well as psychosomatic complaints (5 items) in the last 6 months using a 3-point scale (0 = not true, 1 = somewhat true, 2 = certainly true), resulting in a sum score between 0 and 10. Previous research demonstrated adequate validity and reliability for the subscale [33]. The internal consistency in this sample was α = 0.72–0.74 for mothers and α = 0.68–0.70 for fathers across the two waves of data collection. The correlations between mothers’ and fathers’ scores on the entire subscale were moderate to high (r = 0.51–0.62, p < 0.01 at time 1 and 2 for girls; and r = 0.45–0.52, p < 0.01 at time 1 and 2 for boys). Children’s internalizing symptoms at time 1 and 2 were represented by latent factors derived from both, maternal and paternal sum scores on the SDQ emotional symptoms subscale as separate indicators.
Analyses
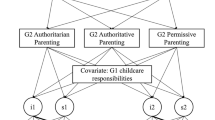
We used Mplus 7.2 [44] to estimate a latent autoregressive cross-lagged model with multiple groups (Fig. 1). The multiple group modelling allows a direct and empirical comparison across groups (girls and boys). Thus, the model enables the examination of gender-specific prospective bidirectional associations between parental depressive symptoms and children’s internalizing symptoms across early school age (cross-lagged paths), while controlling for correlations within each wave of data collection (cross-sectional paths) and the stability of each construct (autoregressive paths from time 1 to time 2). The goodness of fit of the models was evaluated using the Comparative Fit Index (CFI), the Tucker–Lewis Index (TLI), the Root Mean Square Error of Approximation (RMSEA), and the Standardized Root Mean Squared Residual (SRMR). The minimal requirements for adequate structural equation model fit comprise CFI and TLI values larger than 0.90, and RMSEA and SRMR values smaller than 0.10 [53, 59].
Latent autoregressive cross-lagged model with multiple groups and standardized parameters. The model only displays the significant paths of girls and boys. SDQ emo = SDQ emotional symptoms subscale reported by mothers and fathers. Standard errors are shown in parentheses and item parcels have been omitted for illustrative purposes. *p < 0.05; **p < 0.01; ***p < 0.001
Full information maximum likelihood (FIML) estimation was used to handle missing data. We ensured that missing data patterns were unconfounded with the child’s residential situation [single-parent vs. two-parent household; χ2(3, N = 260) = 3.97, p = 0.27].
As a final check for path differences of girls and boys, we used the Chi-square Difference Calculator (CDC) [14] and compared unconstrained models with path coefficients freely estimated across gender groups (less restrictive model, LRM) with constrained models that forced the path estimate to take on the same value for boys and girls (more restrictive model, MRM). If the more restrictive model did not result in a significantly worse model fit over the less restrictive model, the parameter was considered to be equal across gender. As the Chi-square statistic tends to be affected by large sample sizes, the goodness of model fit was determined by the Akaike Information Criterion (AIC). The CDC allows comparing the AIC of both models. The model with a significantly lower AIC was chosen as the better-fitting model [53].
Results
Descriptive statistics
Table 1 shows the descriptive statistics and intercorrelations for all study variables. Children’s internalizing symptoms are presented as mean scores of the maternal and paternal ratings on the SDQ emotional symptoms subscale because of good concordance between the informants.
Boys and girls did not differ in their level of internalizing symptoms (parental report) at time 1 (p = 0.46), and time 2 (p = 0.99). At both waves of data collection, mothers of girls [t(127) = 13.23, p < 0.001 at time 1, t(117) = 11.74, p < 0.001 at time 2] and boys [t(131) = 12.29, p < 0.001 at time 1, t(125) = 12.00, p < 0.001 at time 2] reported more own depressive symptoms than fathers. Moreover, at time 2, mothers of boys reported more own depressive symptoms than mothers of girls (p < 0.05), while there were no differences between girls and boys for the level of paternal depressive symptoms (p = 0.18 for time 1 and p = 0.80 for time 2) and maternal depressive symptoms at time 1 (p = 0.08).
Structural equation model
Model fit
The model constrained factor loadings and intercepts to be equal across groups and waves of data collection (scalar invariance). The final latent autoregressive cross-lagged model with multiple groups showed acceptable fit to the data (CFI = 0.95; TLI = 0.94; RMSEA = 0.06; SRMR = 0.09). The multiple group model enabled including both genders in the same analysis. Figure 1 shows the gender-specific significant path coefficients.
Autoregressive results
Autoregressive paths represent the stability of each construct from time 1 to time 2. In both gender groups, all autoregressive effects over the two waves were statistically significant (see Fig. 1). Internalizing symptoms at time 1 were associated with internalizing symptoms at time 2 in the group of girls (β = 0.82, p < 0.001) and boys (β = 0.86, p < 0.001). Parental depressive symptoms at time 1 were associated with parental depressive symptoms at time 2 in the groups of mothers (β = 0.65, p < 0.001) and fathers (β = 0.77, p < 0.001) of girls, and in the groups of mothers (β = 0.53, p < 0.001) and fathers (β = 0.57, p < 0.001) of boys. Summarized, we found high symptom stability for girls and boys as well as mothers and fathers.
Cross-sectional results
Cross-sectional paths represent correlations within each wave of data collection. Maternal depressive symptoms were associated with girls’ (time 1: r = 0.65, p < 0.001; time 2: r = 0.34, p < 0.05) and boys’ (time 1: r = 0.42, p < 0.001; time 2: r = 0.41, p < 0.05) internalizing symptoms within each wave. However, significant cross-sectional associations between paternal depressive symptoms and children’s internalizing symptoms emerged only for boys (time 1: r = 0.35, p < 0.05; time 2: r = 0.52, p < 0.01) and not for girls (time 1: r = 0.25, p = 0.16; time 2: r = 0.38, p = 0.12). Using the CDC we found a better model fit (a lower AIC) for the less restrictive model (AICLRM = 2264.0) than for the more restrictive model (AICMRM = 2265.6) at time 1, but not at time 2 (AICLRM = 2125.5 vs. AICMRM = 2124.3), indicating significant gender differences for the association between paternal depressive symptoms and child internalizing symptoms at time 1, but not at time 2.
For the comparison of the associations between mother and child versus father and child, the less restrictive model showed a better model fit (a lower AIC) for girls at both waves (time 1: AICLRM = 3088.8 vs. AICMRM = 3090.9; time 2: AICLRM = 2783.9 vs. AICMRM = 2787.0) and for boys at time 1 (AICLRM = 3088.8 vs. AICMRM = 3090.9), while the more restrictive model was preferred for boys at time 2 (AICLRM = 2783.9 vs. AICMRM = 2782.2). In other words, associations between maternal depressive symptoms and children’s internalizing symptoms differed significantly from the associations between paternal depressive symptoms and children’s internalizing symptoms, with the exception of the associations of mothers’ and fathers’ depressive symptoms with boys’ internalizing symptoms at time 2.
Further, maternal depressive symptoms were significantly associated with paternal depressive symptoms, but only in the group of girls (time 1: r = 0.36, p < 0.001; time 2: r = 0.37, p < 0.05) and not in the group of boys (time 1: r = 0.04, p = 0.79; time 2: r = 0.24, p = 0.12). Using the CDC we found a better model fit (a lower AIC) for the less restrictive model at time 1 (AICLRM = 1229.3 vs. AICMRM = 1230.7) and time 2 (AICLRM = 965.0 vs. AICMRM = 974.8), indicating significant gender differences for girls and boys regarding these associations.
In sum, cross-sectional associations with mothers’ depressive symptoms were significant for girls and boys at both waves. Cross-sectional associations with fathers’ depressive symptoms were only significant for boys, but not for girls. A comparison of children’s associations with mothers’ and fathers’ depressive symptoms revealed that the associations between girls and mothers were in general stronger than those between girls and fathers, while we found this effect for boys only at time 1, but not at time 2. Additionally, there were significant associations between depressive symptoms of mothers and fathers of girls, but not between mothers and fathers of boys.
Cross-lagged results
Cross-lagged paths represent the prospective bidirectional associations between children’s internalizing symptoms and parental depressive symptoms across the two waves of data collection. There were no significant cross-lagged effects for parental depressive symptoms at time 1 and children’s internalizing symptoms at time 2 (β = 0.008, p = 0.94 for mothers and girls; β = − 0.11, p = 0.30 for mothers and boys; β = − 0.002, p = 0.99 for fathers and girls; β = − 0.06, p = 0.65 for fathers and boys). The cross-lagged effect between girls’ internalizing symptoms at time 1 and parental depressive symptoms at time 2 was statistically significant for fathers (β = 0.26, p < 0.01), but not for mothers (β = 0.17, p = 0.18). However, there was no cross-lagged effect between boys’ internalizing symptoms at time 1 and parental depressive symptoms at time 2 (β = 0.05, p = 0.75 for mothers, β = 0.14, p = 0.33 for fathers). The results of the CDC indeed suggested a better model fit for the less restrictive model (AICLRM = 2173.5) than for the more restrictive model (AICMRM = 2176.9) regarding the cross-lagged effect between children’s symptoms at time 1 and paternal symptoms at time 2, indicating significant differences for girls and boys. In short, we only found a significant prospective association between girls internalizing symptoms at time 1 and fathers’ depressive symptoms at time 2.
Discussion
The current longitudinal study provides new insights and evidence for gender-specific associations between parental depressive symptoms and children’s internalizing symptoms at early school age. We confirmed our predictions regarding the general importance of maternal depressive symptoms for boys and girls, and the specific importance of paternal depressive symptoms for boys at this age. Our latent structural equation model showed significant concurrent associations between maternal depressive symptoms and both girls’ and boys’ internalizing symptoms. For fathers, we found significant concurrent associations with boys’ internalizing symptoms at early school age, but not with girls’ internalizing symptoms. Notably, a key limitation of the study was the use of parents as informant for their own symptoms and those of their offspring. However, this limitation does not detract from the gender-specific pattern of our results (see below).
In line with our first hypothesis, maternal depressive symptoms were more strongly related to girls’ and boys’ internalizing symptoms than paternal depressive symptoms during the early elementary school period. In accordance with attachment theory, one possible explanation for this pattern may be the mother’s role as primary caregiver, reflecting a default mode of transmission unrelated to gender [6]. Also, Paquette refers to the mother–child relationship as attachment relationship in contrast to the father–child activation relationship [45]. The interaction with the mother serves as kind of prototype and leads to the development of internal working models of the self and the attachment figure, which, in turn, influence the child’s behaviour and thinking [6]. What type of internal working model they construct is therefore of special importance. Especially in the early years, mothers spend more time in close proximity to their children than fathers [9, 11]. Thus, assuming more close and frequent interactions between mothers and their early school-aged children, girls and boys at this age could be more exposed to maladaptive behaviours, cognitions, and affects of depressive mothers than fathers [11]. Given the cross-sectional nature of these data, it is also conceivable that depressive symptoms mainly of mothers co-occur with children’s internalizing symptoms, because children’s problems give rise to distress, helplessness and/or feelings of guilt among mothers, culminating in maternal depressive symptoms [29].
As children progressed through elementary school, the unique role of maternal depression for girls remained constant, while, for boys, depressive symptoms of fathers became comparable in importance to those of mothers. Thus, for girls, our assumption of stronger concurrent same-gender than opposite-gender effects held throughout the elementary school period. For boys, initial significant opposite-gender effects were followed by subsequent opposite-gender coupled with same-gender effects, as we found a striking pattern of comparable effects of maternal and paternal depressive symptoms for boys at second wave. We believe this to be a sign of growing paternal influence as boys mature [5, 11]. In accordance with the social learning theory and Kohlberg’s assumptions about gender constancy, the pattern of findings may illustrate the identification process with the same-gender model as children grow older and develop their own gender-specific self-concept [8, 36, 47]. Especially at early school age, children prefer interactions with peers of the same gender [41]. Children may benefit substantially from identifying with the parent of the same gender to behave more confidently in different social contexts, such as school [17]. Such identification may mean that the parent of the same gender can now also become a potentially negative source of influence in cases of parental psychopathology.
Contrary to our expectations, there were no significant prospective same-gender effects for parental depressive symptoms on children’s internalizing symptoms, or vice versa. This finding is in contrast to other longitudinal studies, which found significant prospective same-gender effects for girls [18] and boys [55]. The transition to school could be a potential explanation for the lack of prospective effects of parental symptoms on child symptoms as children tackle the task of school entry, and their role models may now also encompass teachers and peers [48]. In addition, children are more confronted with their own psychological problems due to the numerous changes on an individual, interactional and contextual level. Internalizing symptoms represent a relevant risk factor in fulfilling the new development tasks [42]. For example, the motivation and concentration problems associated with internalizing symptoms can lead to deficits in school performance. Furthermore, social withdrawal behaviour can make it difficult to make new friendships. Failures in dealing with the numerous changes and new development tasks can in turn favour the maintenance of the internalizing symptoms [42], which would also explain the high symptom stability in children.
Moreover, our finding might also be a result of the chosen approach that controlled for symptom stability and thus, might have led to a more conservative estimate of interpersonal effects in our sample as our data suggest a high intrapersonal stability of internalizing symptoms over the course of early school age, as well as in adulthood. In other words, since the very high degree of symptom stability (especially in children) already explained a large proportion of statistical variance, there remained little variance to be explained for other prospective variables resulting in a dominance of cross-sectional findings.
Ge et al. [19] examined mutual influences in parent and adolescent psychological distress (e.g. depression) over a longer time period and found results similar to those of our study showing no significant cross-lagged effects between same-gender, but significant effects between opposite-gender family dyads. They proposed that these findings may reflect difficulties in relations between children and parents of the opposite gender vis-à-vis the same gender. The latter assumption might be in line with the finding that mothers of boys reported higher levels of depressive symptoms than mothers of girls. Perhaps, parents also respond to symptoms of children of the opposite gender with more stress and depressive symptoms, such as helplessness because they feel unable to embody an adequate role model.
Likewise, we also found an unexpected prospective opposite-gender effect for girls. Girls’ internalizing symptoms at first wave predicted paternal depressive symptoms 1 year later. While most studies confirmed same-gender effects for symptom transmission [29], Ge et al. [19] also found that girls’ emotional distress at eighth grade predicted later paternal distress. Against former beliefs that fathers seem to be less affected by their child’s functioning due to their lower involvement in childcare [60], or are more resilient when exposed to others’ symptoms [29], the fathers of our sample seem to be influenced by their daughters’ emotional well-being. Resembling our finding, Polenick et al. [49] found that fathers’ self-rated health depended on the positivity of the relationship with their daughters. Thus, fathers reported more depressive symptoms when they had a negative father–daughter relationship [49].
Some underlying mechanisms could be responsible for the specific finding of the gender-specific associations between girls and fathers: previous research for example showed that fathers, in particular, interact gender specifically with their children [7, 10]. They seem to behave more sociably and less intrusively in interaction with daughters than sons [2, 7]. Fathers also pay more attention to sad and anxious expressions of daughters, while they attend more to anger and disharmonious expressions of sons [10]. In keeping with these findings, it might be that fathers are more prone to perceive and affectively respond to their daughters’—in contrast to their sons’—internalizing symptoms, and as a consequence react with own depressive behaviour.
Additionally, we found significant associations of mothers’ and fathers’ depressive symptoms at both waves, but only for girls and not for boys. The cumulative exposure to maternal and paternal depressive symptoms is associated with significant adverse consequences: the presence of two parents with depressive symptoms might put girls at increased risk for internalizing symptoms through genetic and environmental factors (e.g. marital conflict, less parental warmth) [15, 25]. For example, a previous study of Mezulis et al. showed that paternal depression exacerbated the effect of maternal depression on children’s internalizing symptoms [43]. While a healthy parent could protect the child by providing a positive role model and by compensating for the dysfunctional behaviour of the depressed parent, it can be assumed that in a family with two parents with depressive symptoms there is a lack of compensation [24, 25].
Finally, our findings must be viewed in the light of a potential shared informant bias. Given that parents reported on their own symptoms and those of children, it is conceivable that our associations between parent and child symptoms are at least partly attributable to the use of the same informants. However, it is difficult to account for our gender-specific and differential findings, especially the growing importance of fathers for boys. Further, a shared informant bias presumably refers to a state-dependent perception of the reporter (e.g. parents with current depressive symptoms perceive more internalizing symptoms in the children), but the high stability of symptoms, especially in children, indicates that parents did not merely report on transient child states. Lastly, we chose mothers and fathers as informants because parents may be more vigilant of their children’s internalizing symptoms compared to other informants from outside the family [11]. In previous studies, the validity of parental ratings on children’s internalizing symptoms could also be confirmed through a good agreement with diagnoses from clinicians [21], self-reports, and objective observations [28].
Limitations
A number of limitations of this study deserve attention. First, our specific at-risk sample makes it difficult to generalize the results for community samples or children of different age. Second, it might be argued that proximity of our waves of data collection led to an underestimation of potential interpersonal prospective effects, owing to the high level of intrapersonal stability in such a short time period. However, the opposite may also be true, i.e. to disentangle the directionality of concurrent effects, research may need to sample emotional symptoms of parents and children at very close time intervals. Broadly speaking, we faced a trade-off, given the need for a longitudinal study that examines precisely the first years of school, because early school age is a developmental period of crucial importance for gender congruency and same-gender preferences [8, 22]. Moreover, many advantages emanate from examination of a single developmental period given that similar competencies and developmental tasks are central.
Third, we used a between-family design, which compares families with boys to families with girls. Inevitably, it follows that gender differences could also be caused by other underlying group differences. Therefore, future studies should make more of an effort to examine gender differences within families.
Fourth, there is a risk for potential informant biases resulting in under- or overreporting of children’s internalizing symptoms. Since internalizing symptoms are less visible than externalizing symptoms, it is assumed that informants tend to underreport symptoms [16]. However, previous research showed that especially raters from outside the family (e.g. teachers) seem to underestimate children’s internalizing symptoms, whereas parents seem to be more sensitive to their children’s emotional inner life [11].
In contrast to the assumptions of underreporting, the depression distortion hypothesis presumes that raters with own depressive symptoms tend to overreport for depressive symptoms of others in contrast to healthy raters [52]. Even though the depression distortion hypothesis does lack empirical support [16], we must consider an overreporting bias for children’s internalizing symptoms because parents reported on their own and their children’s symptoms (shared informant bias). More specifically, the mothers of our sample reported a higher level of own depressive symptoms than fathers and thus seem to be at specific risk for overreporting. However, despite the higher level of maternal depressive symptoms, the descriptive results revealed an adequate concordance between mothers’ and fathers’ ratings of children’s symptoms, which speaks against a maternal informant bias. Further, to reduce potential informant biases, the latent factor of children’s internalizing symptoms was represented by the reports of mothers and fathers.
A final limitation relates to the absence of measures capturing underlying mechanisms in the gender-specific intergenerational transmission. Hence, there is a need for studies that identify potential moderators or mediators (e.g. parenting and child behaviour) regarding the specific transmission processes. Despite these limitations, our study has multiple, notable strengths that help extend the field: large sample size, longitudinal design, inclusion of mothers and fathers as informants, and specification of transmission for girls and boys.
Conclusions
The present study makes an important contribution to the body of research on the gender-specific interplay of parent and child internalizing symptoms by examining these associations in a longitudinal design focusing specifically on early school age. We found differential associations between fathers and daughters and fathers and sons, while the associations between mothers and their children seem to be more gender unspecific at this age.
This implies that clinical practice should be more attentive to potential gender-specific influences within the family when applying psychotherapeutic approaches that address the family as a whole. For example, if possible, therapists should aim to include both mothers and fathers in therapy to maximize effectiveness [26]. Especially for boys, paternal involvement seems to be of particular importance. The contribution of the parent of the same gender might assist children in developing positive role models that may influence their self-concept and thus their emotional well-being.
Moreover, the high symptom stability in both parents and children of early school age underscores the risk for chronicity of internalizing symptoms across different generations. Thus, internalizing symptoms of both parents and children must be taken seriously. Therefore, further implications for clinical practice should include early screenings for internalizing symptoms to facilitate the detection and intervention at early school age, and an expansion of low-threshold preventive interventions for families with parental depression. Finally, multipliers such as teachers, after-school care assistants, and primary care providers should be involved in concerted efforts to treat and prevent internalizing symptoms and disorders at early school age.
Notes
A parcel is an indicator of the latent factor that is defined as the mean (or sum) of two or more individual items [39].
References
Bandalos DL (2002) The effects of item parceling on goodness-of-fit and parameter estimate bias in structural equation modeling. Struct Equ Model 9:78–102
Barnett MA, Deng M, Mills-Koonce WR, Willoughby M, Cox M (2008) Interdependence of parenting of mothers and fathers of infants. J Fam Psychol 22:561–573
Becker A, Rothenberger A, Sohn A, BELLA Study Group (2015) Six years ahead: a longitudinal analysis regarding course and predictive value of the Strengths and Difficulties Questionnaire (SDQ) in children and adolescents. Eur Child Adolesc Psychiatry 24:715–725
Bögels SM, Perotti EC (2011) Does father know best? A formal model of the paternal influence on childhood social anxiety. J Child Fam Stud 20:171–181
Bögels SM, Phares V (2008) Fathers’ role in the etiology, prevention and treatment of child anxiety: a review and new model. Clin Psychol Rev 28:539–558
Bretherton I (1992) The origins of attachment theory: John Bowlby and Mary Ainsworth. Dev Psychol 28(5):759–775
Bronstein P (1984) Differences in mothers’ and fathers’ behaviors toward children: a cross-cultural comparison. Dev Psychol 20:995–1003
Bussey K, Bandura A (1999) Social cognitive theory of gender development and differentiation. Psychol Rev 106:676–713
Cabrera NJ, Fitzgerald HE, Bradley RH, Roggman L (2014) The ecology of father–child relationships: an expanded model. J Fam Theory Rev 6:336–354
Chaplin TM, Cole PM, Zahn-Waxler C (2005) Parental socialization of emotion expression: gender differences and relations to child adjustment. Emotion 5:80–88
Connell AM, Goodman SH (2002) The association between psychopathology in fathers versus mothers and children’s internalizing and externalizing behavior problems: a meta-analysis. Psychol Bull 128:746–773
Costello EJ, Egger HL, Copeland W, Erkanli A, Angold A (2011) The developmental epidemiology of anxiety disorders: phenomenology, prevalence, and comorbidity. In: Silverman WK, Field AP (eds) Anxiety disorders in children and adolescents: research, assessment and intervention. Cambridge University Press, Cambridge, pp 56–75
Coyne JC (1976) Depression and the response of others. J Abnorm Psychol 85:186–193
Crayen C (2010) Chi square distributions calculator version 3 [computer software]. University of Berlin, Berlin
Cummings EM, Keller PS, Davies PT (2005) Towards a family process model of maternal and paternal depressive symptoms: exploring multiple relations with child and family functioning. J Child Psychol Psychiatry 46:479–489
De Los Reyes A, Augenstein TM, Wang M, Thomas SA, Drabick DA, Burgers DE, Rabinowitz J (2015) The validity of the multi-informant approach to assessing child and adolescent mental health. Psychol Bull 141:858–900
Eckes T, Trautner HM (2000) The developmental social psychology of gender. Erlbaum, Mahwah
Elgar FJ, Curtis LJ, McGrath PJ, Waschbusch DA, Stewart SH (2003) Antecedent-consequence conditions in maternal mood and child adjustment: a four-year cross-lagged study. J Clin Child Adolesc Psychol 32:362–374
Ge X, Conger RD, Lorenz FO, Shanahan M, Elder GH (1995) Mutual influences in parent and adolescent psychological distress. Dev Psychol 31:406–419
Gibb BE, Uhrlass DJ, Grassia M, Benas JS, McGeary J (2009) Children’s inferential styles, 5-HTTLPR genotype, and maternal expressed emotion-criticism: an integrated model for the intergenerational transmission of depression. J Abnorm Psychol 118:734–745
Grills AE, Ollendick TH (2003) Multiple informant agreement and the anxiety disorders interview schedule for parents and children. J Am Acad Child Adolesc Psychiatry 42:30–40
Golombok S, Rust J, Zervoulis K, Croudace T, Golding J, Hines M (2008) Developmental trajectories of sex-typed behavior in boys and girls: a longitudinal general population study of children aged 2.5–8 years. Child Dev 79:1583–1593
Goodman R (1999) The extended version of the Strengths and Difficulties Questionnaire as a guide to child psychiatric caseness and consequent burden. J Child Psychol Psychiatry 40:791–799
Goodman SH, Gotlib IH (2002) Children of depressed parents: Mechanisms of risk and implications for treatment. Am Psychol Assoc, Washington
Goodman SH, Rouse MH, Connell AM, Broth MR, Hall CM, Heyward D (2011) Maternal depression and child psychopathology: a meta-analytic review. Clin Child Fam Psychol Rev 14:1–27
Göttken T, White LO, Klein AM, von Klitzing K (2014) Short-term psychoanalytic child therapy for anxious children: a pilot study. Psychotherapy 51:148–158
Grote NK, Bridge JA, Gavin AR, Melville JL, Iyengar S, Katon WJ (2010) A meta-analysis of depression during pregnancy and the risk of preterm birth, low birth weight, and intrauterine growth restriction. Arch Gen Psychiatry 67:1012–1024
Hinshaw SP, Han SS, Erhardt D, Huber A (1992) Internalizing and externalizing behavior problems in preschool children: correspondence among parent and teacher ratings and behavior observations. J Clin Child Psychol 21:143–150
Hughes EK, Gullone E (2010) Reciprocal relationships between parent and adolescent internalizing symptoms. J Fam Psychol 24:115–124
Jaffee SR, Poulton R (2006) Reciprocal effects of mothers’ depression and children’s problem behaviors from middle childhood to early adolescence. In: Huston CA, Ripke MN, McCord J (eds) Developmental contexts in middle childhood: bridges to adolescence and adulthood. Cambridge University Press, New York, pp 107–129
Kane P, Garber J (2004) The relations among depression in fathers, children’s psychopathology, and father–child conflict: a meta-analysis. Clin Psychol Rev 24:339–360
Klasen F, Otto C, Kriston L, Patalay P, Schlack R, Ravens-Sieberer U, Bella Study Group (2015) Risk and protective factors for the development of depressive symptoms in children and adolescents: results of the longitudinal BELLA study. Eur Child Adolesc Psychiatry 24:695–703
Klein AM, Otto Y, Fuchs S, Zenger M, von Klitzing K (2013) Psychometric properties of the parent-rated SDQ in preschoolers. Eur J Psychol Assess 29:96–104
Klein AM, Otto Y, Fuchs S, Reibiger I, von Klitzing K (2015) A prospective study of behavioral and emotional symptoms in preschoolers. Eur Child Adolesc Psychiatry 24:291–299
Klein AM et al (2017) Latent trajectories of internalizing symptoms from preschool to school age: a multilevel multi-informant study in a high-risk sample (under review)
Kohlberg L (1966) A cognitive-developmental analysis of children’s sex-role concepts and attitudes. In: Maccoby E (ed) The development of sex differences. Stanford University Press, Stanford, pp 82–173
Kramer MD, Krueger RF, Hicks BM (2008) The role of internalizing and externalizing liability factors in accounting for gender differences in the prevalence of common psychopathological syndromes. Psychol Med 38:51–61
Kroenke K, Spitzer RL, Williams JB (2001) The Phq-9. J Gen Intern Med 16:606–613
Little TD, Cunningham WA, Shahar G, Widaman KF (2002) To parcel or not to parcel: exploring the question, weighing the merits. Struct Equ Model 9:151–173
Löwe B, Kroenke K, Herzog W, Gräfe K (2004) Measuring depression outcome with a brief self-report instrument: sensitivity to change of the Patient Health Questionnaire (PHQ-9). J Affect Disord 81:61–66
Martin CL, Fabes RA, Hanish LD (2014) Gendered-peer relationships in educational contexts. In: Liben L, Bigler R (eds) Advances in child development and behavior. Academic Press, Burlington, pp 151–187
Masten AS, Roisman GI, Long JD, Burt KB, Obradović J, Riley JR, Boelcke-Stennes K, Tellegen A (2005) Developmental cascades: linking academic achievement and externalizing and internalizing symptoms over 20 years. Dev Psychol 41:733–746
Mezulis AH, Hyde JS, Clarke R (2004) Father involvement moderates the effect of maternal depression during a child’s infancy on child behavior problems in kindergarten. J Fam Psychol 18:575–588
Muthén LK, Muthén BO (1998–2012) Mplus user’s guide. Muthén & Muthén, Los Angeles
Paquette D (2004) Theorizing the father–child relationship: mechanisms and developmental outcomes. Hum Dev 47:193–219
Parent J, Forehand R, Pomerantz H, Peisch V, Seehuus M (2017) Father participation in child psychopathology research. J Abnorm Child Psychol 45:1259–1270
Patterson MM (2012) Self-perceived gender typicality, gender-typed attributes, and gender stereotype endorsement in elementary-school-aged children. Sex Roles 67:422–434
Pianta RC, Stuhlman MW (2004) Teacher–child relationships and children’s success in the first years of school. School Psychol Rev 33:444–458
Polenick CA, DePasquale N, Eggebeen DJ, Zarit SH, Fingerman KL (2016) Relationship quality between older fathers and middle-aged children: associations with both parties’ subjective well-being. J Gerontol B Psychol Sci Soc Sci. https://doi.org/10.1093/geronb/gbw094
Ravens-Sieberer U, Wille N, Erhart M et al (2008) Prevalence of mental health problems among children and adolescents in Germany: results of the BELLA study within the National Health Interview and Examination Survey. Eur Child Adolesc Psychiatry 17:22–33
Reck C, Nonnenmacher N, Zietlow AL (2016) Intergenerational transmission of internalizing behavior: the role of maternal psychopathology, child responsiveness and maternal attachment style insecurity. Psychopathology 49:277–284
Richters JE (1992) Depressed mothers as informants about their children: a critical review of the evidence for distortion. Psychol Bull 112:485–499
Schermelleh-Engel K, Moosbrugger H, Müller H (2003) Evaluating the fit of structural equation models: tests of significance and descriptive goodness-of-fit measures. Methods Psychol Res Online 8:23–74
Stockard J (2006) Gender socialization. In: Chafetz JS (ed) Handbook of the sociology of gender. Springer, New York, pp 215–227
Thomas AM, Forehand R (1991) The relationship between paternal depressive mood and early adolescent functioning. J Fam Psychol 4:260–271
Tobin DD, Menon M, Menon M, Spatta BC, Hodges EV, Perry DG (2010) The intrapsychics of gender: a model of self-socialization. Psychol Rev 117:601–622
von Klitzing K, White LO, Otto Y, Fuchs S, Egger HL, Klein AM (2014) Depressive comorbidity in preschool anxiety disorder. J Child Psychol Psychiatry 55:1107–1116
Weissman MM, Wickramaratne P, Gameroff MJ, Warner V, Pilowsky D, Kohad RG, Verdeli H, Skipper J, Talati A (2016) Offspring of depressed parents: 30 years later. Am J Psychiatry 173:1024–1032
Whiteside-Mansell L, Corwyn RF (2003) Mean and covariance structures analyses: an examination of the Rosenberg Self-Esteem Scale among adolescents and adults. Educ Psychol Measur 63:163–173
Zahn-Waxler C (2000) The early development of empathy, guilt, and internalization of distress: Implications for gender differences in internalizing and externalizing problems. In: Davidson R (ed) Wisconsin symposium on emotion: anxiety, depression and emotion. Oxford University Press, Oxford, pp 222–265
Acknowledgements
This study was supported by Grants of the German Research Foundation (DFG) to Kai von Klitzing and Annette M. Klein (Grants KL 2315/1-1, KL2315/1-2 and KL2338/1-2), and the German Federal Ministry of Education and Research (Grant 01KR1201A). The authors would like to thank the Public Health Department of the City of Leipzig for cooperating in this study, as well as all families for taking part.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Research involving human participants and/or animals
The presented study was approved by the institutional review board of the Medical Faculty of the University of Leipzig and has been performed in accordance with the ethical standards laid down in the 1964 Declaration of Helsinki and its later amendments or comparable ethical standards.
Informed consent
Participation in the study was voluntary and all parents gave written informed consent prior to the inclusion in the study. Moreover, the child’s oral assent was obtained.
Conflict of interest
On behalf of all authors, the corresponding author states that there is no conflict of interest.
Rights and permissions
About this article
Cite this article
Andreas, A., White, L.O., Sierau, S. et al. Like mother like daughter, like father like son? Intergenerational transmission of internalizing symptoms at early school age: a longitudinal study. Eur Child Adolesc Psychiatry 27, 985–995 (2018). https://doi.org/10.1007/s00787-017-1103-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00787-017-1103-y