Abstract
Objectives
Periodontopathogens induce immunoinflammatory responses characterized by the release of inflammatory mediators, e.g., interleukin (IL)-1β, IL-6, and IL-8. Ghrelin (GHRL) is an appetite hormone which mediates its effect via the functional receptor GHS-R1a. This study was to examine the effect of an inflammatory insult on GHS-R1a in human periodontal cells.
Materials and methods
Periodontal ligament (PDL) cells and gingival fibroblasts (HGFs) were exposed to IL-1β in the presence and absence of GHRL. Cells were also pre-incubated with specific inhibitors of NF-κB or MEK1/MEK2 signaling. Gene expression of GHS-R1a and proinflammatory mediators was assessed by real-time PCR, GHS-R1 protein level by immunocytochemistry, and NF-κB nuclear translocation by immunofluorescence.
Results
IL-1β increased significantly the GHS-R1a expression in both cell types in a dose-dependent manner. The stimulatory effect of IL-1β involved the NF-κB and MAPK pathways. Exposure of cells to IL-1β also resulted in an increased production of GHS-R1 protein in both cell types. Furthermore, GHRL counteracted significantly the stimulatory actions of IL-1β on IL-6 and IL-8 in PDL cells.
Conclusions
This study demonstrates for the first time that IL-1β upregulates the functional ghrelin receptor in periodontal fibroblastic cells. Moreover, these results further support the assumption that the GHRL/GHS-R system exerts anti-inflammatory effects. Therefore, the upregulation of ghrelin receptor in periodontal cells in response to an inflammatory stimulus may represent a negative feedback mechanism to attenuate the initial inflammatory process in periodontal diseases.
Clinical relevance
The anti-inflammatory GHRL/GHS-R system may serve as a promising target for the prevention and therapy of periodontal diseases.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Periodontitis is a highly prevalent chronic inflammatory disease caused by pathogenic microorganisms of the subgingival biofilm in combination with other risk factors, such as genetic predisposition, smoking, and certain systemic diseases and conditions. Periodontitis is characterized by the destruction of the tooth-supporting tissues comprising gingiva, periodontal ligament (PDL), cementum, and alveolar bone [1].
According to the current understanding of the pathogenesis of periodontitis, subgingival microorganisms, their components, and products initiate a local immunoinflammatory host response. In response to the pathogenic bacteria, both professional and accessory immunoinflammatory cells release a variety of inflammatory mediators and proteases, such as interleukin (IL)-1β, IL-6, IL-8, cyclooxygenase-2 (COX2), and chemokine CC motif ligand 2 (CCL2), which mediate matrix degradation and alveolar bone resorption [2, 3].
Periodontitis, even though not fatal, has a negative impact on the quality of life and systemic health [4, 5]. A plethora of studies have convincingly demonstrated an association of periodontitis with systemic diseases, such as coronary heart disease, cerebrovascular infarction, diabetes mellitus, obesity, and metabolic syndrome [6,7,8,9]. However, the pathomechanisms underlying these perio-systemic associations are as yet only partially understood.
In this context, due to its link to obesity and the immune system, the actions of ghrelin (growth hormone secretagogue receptor ligand (GHRL)) in periodontal health and diseases have recently become a hot topic of interest [10, 11]. GHRL was first identified as a peptide appetite hormone secreted mainly by gastrointestinal cells and regulates many critical biological processes in the human body, such as food intake, metabolism, inflammation, sleep, and memory [12,13,14]. The effects of GHRL are mediated by the growth hormone secretagogue receptor (GHS-R), which is a G-protein-coupled receptor highly expressed in brain but also detectable in some peripheral tissues [15, 16]. Two transcript variants of GHS-R have been identified: type 1a and 1b. Upon binding of GHRL to GHS-R1a, a profound change in receptor conformation occurs, which leads to a diversity of physiological responses. Whereas GHS-R1a is biologically active, the GHS-R1b does not mediate any known effect [15, 16].
To date, few studies have been dedicated to the role of GHRL in periodontal homeostasis and diseases. Whereas GHRL levels in gingival crevicular fluid (GCF) have been shown to be lower in periodontitis patients as compared to healthy subjects [17], serum levels of GHRL seem to be increased in periodontally diseased patients [18]. In addition, GHRL has been detected in saliva as well as in cells and tissues of the tooth germ, such as the inner enamel epithelium, mesenchymal cells, ameloblasts, odontoblasts, and Hertwig’s epithelial root sheath [19,20,21]. Recently, we have found that the periodontopathogen Fusobacterium nucleatum caused an initial upregulation and subsequent downregulation of GHS-R1a in PDL cells [22]. Furthermore, in a rat experimental periodontitis model, the GHS-R1a expression was higher at sites of periodontitis as compared to healthy sites during the early stage of periodontitis [22]. However, our understanding of the role of the GHRL/GHS-R system in periodontal inflammation is still limited. The main objective of this in vitro investigation was to examine the effect of an inflammatory insult on the GHS-R1a expression in human PDL cells and gingival fibroblasts (HGFs).
Materials and methods
Culture and treatment of PDL cells and HGFs
This project was approved by the Ethics Committee of the University of Bonn (#043/11). Tissue samples and teeth were collected, after informed consent was obtained. PDL cells were derived from periodontally healthy teeth extracted for orthodontic reasons from six donors (three males/three females), and HGFs were obtained from healthy gingiva of six individuals (four males/two females), who had to undergo wisdom tooth extraction. PDL cells and HGFs were grown in Dulbecco’s minimal essential medium (DMEM; Invitrogen, Karlsruhe, Germany) supplemented with 10% fetal bovine serum (FBS; Invitrogen), 100 U/ml penicillin, and 100 μg/ml streptomycin (Invitrogen) at 37 °C in a humidified atmosphere of 5% CO2. Cells were used between third and fifth passages, seeded (5.0 × 104 cells/well) on tissue culture plates (Corning, NY, USA), and grown to 80% confluence for experiments. The FBS concentration was reduced to 1% 1 day prior to the experiments. Medium was changed every second day. Human recombinant IL-1β (PromoKine, Heidelberg, Germany), which has been shown to be increased in gingival tissues and GCF at inflamed periodontal sites, was used to mimic inflammatory conditions in vitro [23,24,25]. In order to ensure that data were comparable with existing studies, HGFs and PDL cells were typically exposed to an IL-1β concentration of 1 ng/ml in our experiments [26,27,28]. However, to examine a possible dose dependency of the IL-1β actions on the GHS-R1a expression, a range of IL-1β concentrations from 0.2 to 5.0 ng/ml were used. In a subset of experiments, PDL cells and HGFs were also pre-incubated with GHRL (20 nM, human n-octanoylated GHRL; Pepta Nova, Sandhausen, Germany) 45 min prior to the IL-1β treatment to evaluate potential anti-inflammatory effects of the GHRL/GHS-R system. The same or similar GHRL concentrations were also used by other investigators and proved to be effective in our previous experiments [22, 29,30,31]. In order to unravel the intracellular signaling pathways involved in the potential regulatory effects of IL-1β on GHS-R1a, HGFs and PDL cells were pre-incubated with ammonium pyrrolidine dithiocarbamate (PDTC; 10 μM; Calbiochem, San Diego, CA, USA), a selective inhibitor of the NF-κB signaling pathway, and U0126 (10 μM; Calbiochem), a highly selective inhibitor of MEK1/MEK2, two important components of MAPK signaling pathway, 1 h prior to the IL-1β treatment. All experiments were performed in triplicates and repeated at least twice.
Real-time polymerase chain reaction
Total RNA from PDL cells and HGFs was extracted using the RNeasy Mini Kit (Qiagen, Hilden, Germany) according to the manufacturer’s protocol. RNA concentrations were measured by the NanoDrop ND-2000 spectrophotometer (Thermo Fisher Scientific, Wilmington, DE, USA), and reverse transcription of 500 ng of total RNA was performed using the iScript™ Select cDNA Synthesis Kit (Bio-Rad Laboratories, Munich, Germany) at 42 °C for 90 min, followed by 85 °C for 5 min according to the manufacturer’s instruction. The gene expressions of GHS-R1, COX2, CCL2, IL-6, and IL-8 were analyzed by quantitative real-time PCR using specific primers (QuantiTect Primer Assay, Qiagen), SYBR Green QPCR Master Mix (Bio-Rad), and the iCycler iQ™ Real-Time PCR Detection System (Bio-Rad). Amplification was carried out under the following conditions: initial denaturation at 95 °C for 5 min, followed by 40 cycles of denaturation at 95 °C for 10 s, and combined annealing/extension at 60 °C for 30 s. Data were analyzed using the comparative threshold cycle (CT) method with glyceraldehyde-3-phosphate dehydrogenase (GAPDH) as the housekeeping gene.
Immunocytochemistry for GHS-R detection
PDL cells and HGFs were cultured on plastic coverslips (Thermo Fisher Scientific) of 13-mm diameter in 24-well plates in the presence or absence of IL-1β for 1 and 2 days. Then, the cell monolayers were fixed in 4% paraformaldehyde (Sigma-Aldrich, Munich, Germany) at pH 7.4 and at room temperature (RT) for 10 min and permeabilized in 0.1% Triton X-100 (Sigma-Aldrich) for 5 min, followed by blocking with serum block (Dako, Hamburg, Germany) for 20 min. Next, the cells were labeled using rabbit polyclonal primary antibody to GHS-R (Abcam, Cambridge, UK, 1:500) in a humid chamber at 4 °C overnight and then incubated with goat anti-rabbit IgG HRP secondary antibody (Dako) for 45 min. In between each step, cells were rinsed with PBS (Invitrogen). Cells were mounted with DePeX (SERVA Electrophoresis, Heidelberg, Germany), and GHS-R protein levels were examined with an Axioskop 2 microscope (20×, Carl Zeiss, Germany). An AxioCam MRc camera and the AxioVision 4.7 software (Carl Zeiss) were used to capture and analyze the images. Untreated cells served as a control.
Immunofluorescence for nuclear factor-κB p65 detection
Cells cultured on plastic coverslips (Thermo Fisher Scientific) were exposed or not to IL-1β for 60 min. Afterwards, the cells were fixed and permeabilized, as mentioned above, and blocked with nonfat dry milk (Bio-Rad) for 1 h. Next, the cells were incubated with rabbit anti-nuclear factor-κB p65 (E498) primary antibody (Cell Signaling Technology, Danvers, MA, USA; 1:100) at room temperature for 90 min, rinsed with PBS, and then incubated with CY3-conjugated goat anti-rabbit IgG secondary antibody (Abcam; 1:1000) at room temperature for 45 min. Finally, the location of NF-κB p65 within the cells was studied with the ZOE™ Fluorescent Cell Imager (Bio-Rad) with a 20× objective. The images were captured with an integrated digital 5-MP CMOS camera.
Statistical analysis
Statistical analysis of the data was performed using the IBM SPSS Statistics software (version 22, IBM SPSS, Chicago, IL, USA). Quantitative data are presented as mean and standard error of the mean (SEM). To test for statistically significant differences between the groups, the t test, Mann-Whitney U test, and ANOVA followed by the post hoc Dunnett’s and Tukey’s tests were used. The level of significance was set at p < 0.05.
Results
Regulation of GHS-R1a by IL-1β in human PDL cells and HGFs
First, we sought to examine whether GHS-R1a is regulated by IL-1β in PDL cells. As shown in Fig. 1a, IL-1β (1 ng/ml) caused a significant upregulation of the GHS-R1a expression at 1 day, which was even further increased at 2 days, as analyzed by real-time PCR. Additional experiments revealed that the stimulatory effect of IL-1β on the GHS-R1a expression was dose dependent. The highest IL-1β concentration resulted in the strongest upregulation of GHS-R1a at 1 day (Fig. 1b). The stimulatory action of IL-1β on the GHS-R1a expression in PDL cells was also observed at protein level, as analyzed by immunocytochemistry. A stronger immunoreaction was found in IL-1β-treated PDL cells as compared to untreated control cells at 1 day (Fig. 1c).
a GHS-R1a expression in PDL cells either exposed or not to IL-1β (1 ng/ml) for 1 and 2 days, as analyzed by real-time PCR. Mean ± SEM (n = 18). *Significant (p < 0.05) difference between groups. b GHS-R1a expression in PDL cells in response to various concentrations of IL-1β (0.2, 1, 5 ng/ml) at 1 day. Unstimulated cells were used as control. Mean ± SEM (n = 9). *Significantly (p < 0.05) different from control. c GHS-R1a protein in PDL cells either exposed or not to IL-1β (1 ng/ml) for 1 day, as visualized by immunocytochemistry. Representative images from one out of three experiments are presented
Next, we studied the influence of IL-1β on GHS-R1a in HGFs. Again, IL-1β exerted a stimulatory effect on the GHS-R1a expression, which was significant at 1 day but not at 2 days (Fig. 2a). Moreover, the IL-1β actions on GHS-R1a expression in HGFs were also dose dependent, as depicted in Fig. 2b. Interestingly, the highest GHS-R1a upregulation was found when HGFs were stimulated with 1 ng/ml of IL-1β (Fig. 2b). Like in PDL cells, IL-1β treatment also resulted in an increased immunoreaction for GHS-R1a protein in HGFs, as evidenced by immunocytochemistry (Fig. 2c).
a GHS-R1a expression in HGFs either exposed or not to IL-1β (1 ng/ml) for 1 and 2 days, as analyzed by real-time PCR. Mean ± SEM (n = 18). *Significant (p < 0.05) difference between groups. b GHS-R1a expression in HGFs in response to various concentrations of IL-1β (0.2, 1, 5 ng/ml) at 1 day. Unstimulated cells were used as control. Mean ± SEM (n = 9). *Significantly (p < 0.05) different from control. c GHS-R1a protein in HGFs cells either exposed or not to IL-1β (1 ng/ml) for 1 day, as visualized by immunocytochemistry. Representative images from one out of three experiments are presented
Molecular pathways involved in the regulation of GHS-R1a by IL-1β
We then sought to unravel signaling pathways involved in the actions of IL-1β on GHS-R1a. As expected, treatment of PDL cells with IL-1β triggered the NF-κB (p65) pathway, with a maximal NF-κB nuclear translocation at 60 min, as visualized by immunofluorescence microscopy (Fig. 3a). PDL cells were also pre-incubated with specific inhibitors of NF-κB (PDTC) and MEK1/MEK2 (U0126). Both inhibitors reduced significantly the IL-1β-induced GHS-R1a upregulation in PDL cells at 1 day (Fig. 3b).
a NF-κB (p65) nuclear translocation in PDL cells exposed to IL-1β (1 ng/ml) over 60 min, as examined by immunofluorescence microscopy. Representative images from one out of three experiments are presented. b GHS-R1a expression in PDL cells treated with IL-1β (1 ng/ml) in the presence and absence of a MEK inhibitor (U0126, 10 μM) or an NF-κB inhibitor (PDTC, 10 μM) at 1 day. Mean ± SEM (n = 6). *Significant (p < 0.05) difference between groups
Like in PDL cells, IL-1β also caused a maximal NF-κB nuclear translocation in HGFs at 60 min (Fig. 4a). Furthermore, pre-incubation with both specific inhibitors also reduced significantly the stimulatory effect of IL-1β on GHS-R1a in HGFs at 1 day (Fig. 4b).
a NF-κB (p65) nuclear translocation in HGFs exposed to IL-1β (1 ng/ml) over 60 min, as examined by immunofluorescence microscopy. Representative images from one out of three experiments are presented. b GHS-R1a expression in HGFs treated with IL-1β (1 ng/ml) in the presence and absence of a MEK inhibitor (U0126, 10 μM) or an NF-κB inhibitor (PDTC, 10 μM) at 1 day. Mean ± SEM (n = 6). *Significant (p < 0.05) difference between groups
Regulation of IL-1β actions on inflammatory mediators by GHRL
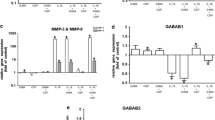
Finally, we aimed to study the effects of GHRL on inflammatory mediators associated with periodontitis. In PDL cells, IL-1β caused a significant upregulation of COX2, CCL2, IL-6, and IL-8 expressions at 1 day, as expected (Fig. 5a–d). However, pre-incubation of PDL cells with GHRL counteracted the stimulatory actions of IL-1β on these inflammatory molecules. Although the inhibitory effect of GHRL was only slight for COX2 and CCL2, it was significant for IL-6 and IL-8 at 1 day (Fig. 5a–d). These inhibitory GHRL effects were also observed in HGFs (data not shown).
Discussion
The results of the present in vitro study show for the first time that the functional ghrelin receptor is upregulated by IL-1β in PDL cells and HGFs. Moreover, our data provide further support for the assumption that the GHRL/GHS-R system can exert anti-inflammatory effects. Therefore, the upregulation of the GHS-R in periodontal fibroblastic cells in response to an inflammatory stimulus may represent a negative feedback mechanism to attenuate the initial inflammatory process in periodontal diseases.
GHRL regulates many critical biological processes in the human body, such as food intake, metabolism, inflammation, sleep, and memory [12,13,14]. These effects are mediated by its functional receptor, i.e., GHS-R1a, which is a G-protein-coupled receptor expressed in brain and some peripheral tissues [15, 16]. Interestingly, GHRL and its receptors have also been detected in parotid, sublingual, and submandibular glands as well as in oral epithelial cells and fibroblasts [21, 29, 32]. Furthermore, few studies focused on the role of GHRL in periodontitis. Reduced GCF levels and increased serum levels of GHRL were found in patients suffering from periodontitis as compared to periodontally healthy individuals [17, 18]. Although our current knowledge on the GHRL/GHS-R1 system in periodontitis is still very limited, the aforementioned investigations suggest a critical role for GHRL and its functional receptor in periodontal tissues.
In order to better understand the involvement of GHRL in the pathophysiology of periodontitis, it is important to disclose the GHS-R1a regulation in periodontal cells, such as PDL cells and HGFs, under inflammatory conditions. In the present study, the GHS-R1a expression was significantly increased in the presence of IL-1β, which was used to mimic an inflammatory environment in vitro. Further experiments revealed that the IL-1β actions on GHS-R1a were dose dependent and also observed at protein level. Although both cell types showed a significant initial upregulation of GHS-R1a at 1 day, a further increase in the GHS-R1a expression was only observed in PDL cells. In addition, the cell response to IL-1β was also stronger in PDL cells, as compared with HGFs, at transcriptional level. One explanation for the shorter and weaker cell response of HGFs to IL-1β might be that these cells are located anatomically closer to the periodontopathogenic microorganisms and, thereby, the inflammatory process than PDL cells. HGFs might be less sensitive in order to cope sufficiently with high concentrations of bacterial and inflammatory stressors. Another reason for the differences in the GHS-R1a expression between PDL cells and HGFs could be that PDL cells and HGFs were not derived from the same individuals. Therefore, different genetic and epigenetic backgrounds of the donors might also be a potential cause for the observed differences in the GHS-R1a regulation. If other reasons, such as different functions of HGFs and PDL cells, could have been responsible for the observed differences in the GHS-R1a, regulation among both cell types has yet to be elucidated. Interestingly, the IL-1β-induced upregulation of GHS-R1a involved the NF-κB and MAPK signaling pathways. Periodontal disease can develop and progress, if the bacteria-induced inflammation is excessive and/or prolonged. Therefore, the upregulation of GHS-R1a by IL-1β, as observed in the present study, may represent a negative feedback mechanism to attenuate the initial inflammatory process, thereby protecting the periodontal tissues from matrix degradation and bone resorption.
Recently, we studied the expression of the GHS-R in periodontal cells under microbial conditions [22]. Interestingly, the periodontopathogen F. nucleatum caused an initial upregulation and subsequent downregulation of GHS-R1a in periodontal cells. Moreover, in rat experimental periodontitis, the GHS-R1a expression at periodontitis sites was enhanced during the early stage of periodontitis, but decreased afterwards, when compared with healthy sites [22]. These findings indicating an initial GHS-R1a upregulation under microbial conditions concur very well with the results from the present study, which revealed an GHS-R1a increase under inflammatory conditions. If this likely protective feedback mechanism also gets lost, when the involved cells are exposed to inflammatory mediators for longer time periods, has yet to be clarified in further studies. The fact that the stimulatory effect of IL-1β on GHS-R1a was not detectable at 2 days in HGFs may point in this direction.
Since the actions of the GHRL/GHS-R1 system depend on the availability of both ligand and its receptor, we also studied the effects of IL-1β on GHRL in PDL cells and HGFs. However, the constitutive and IL-1β-stimulated GHRL expressions were negligible in these cells (data not shown), suggesting that GHS-R1 is the main target in these cells under inflammatory conditions.
The present investigation also demonstrated that the expressions of COX2, CCL2, IL-6, and IL-8 are increased under inflammatory conditions. These proinflammatory and chemotactic mediators are increased at periodontitis sites in comparison with periodontally healthy sites [33, 34]. Moreover, these findings are in line with other studies, which have demonstrated elevated levels of these cytokines in response to IL-1β [35, 36]. Remarkably, pre-incubation with GHRL abrogated the IL-1β-induced upregulation of IL-6 and IL-8 in PDL cells, which underlines the anti-inflammatory role of GHRL in the periodontium. The finding that GHRL can cause a downregulation of proinflammatory cytokine expressions has also been observed in other studies [37,38,39,40]. For example, it has been shown that GHRL counteracts the stimulatory effects of lipopolysaccharide (LPS) on the IL-6 and IL-8 releases from mouse dopaminergic neurons and human oral epithelial cells, respectively [32, 41]. Similarly, GHRL inhibited the endotoxin-induced IL-8 synthesis in rats [42]. Several studies have demonstrated that the anti-inflammatory actions of GHRL involve the NF-κB pathway [43, 44]. The aforementioned studies support our findings which suggest a critical role for GHRL in controlling periodontal inflammation. In our experiments, we mainly focused on “classical” inflammatory mediators which are known to play a pivotal role in the initiation and progression of periodontitis. Nevertheless, other proinflammatory mediators, such as IL-17, and anti-inflammatory cytokines, such as IL-10 and IL-1ra, are also critical. Further studies should also address their regulation by GHRL under inflammatory and microbial conditions. Local or systemic application of GHRL in animal models of experimental periodontitis could further clarify the anti-inflammatory and protective role of GHRL. Moreover, experimental periodontitis models in GHS-R knockout and wild-type mice will help to better understand the GHRL/GHS-R system in periodontal diseases. Whether periodontal treatment causes alterations in the GHRL/GHS-R system locally and/or systemically is another exciting area of future periodontal research.
As described above, in this in vitro study, IL-1β was used to simulate periodontal inflammation, because this proinflammatory cytokine is increased in gingival tissues and GCF at inflamed periodontal sites, induces the production and release of other inflammatory and chemotactic mediators that amplify the periodontal inflammatory response, leads to the production of matrix-degrading enzymes, and stimulates bone resorption [23,24,25, 45,46,47]. However, periodontitis is a complex inflammatory and bacterial disease. Other inflammatory mediators, such as TNF-α and prostaglandins, are also key players in the aetiopathogenesis of periodontitis and participate in the inflammatory and degradative processes. In addition, these inflammatory mediators do not act alone but exert their detrimental effects on periodontal tissues in combination with periodontal bacteria, their components, and products. Further studies should therefore also focus on the actions of other inflammatory mediators, either alone or combined with bacteria, on the GHRL/GHS-R system in periodontal cells.
In our experiments, PDL cells and HGFs were used, as these cells are most frequently found in the periodontium. These fibroblastic cells play a critical role in periodontal homeostasis, destruction, and regeneration. The results of our study revealed that the GHS-R1a regulation of the cells was similar. However, periodontitis is also characterized by alveolar bone destruction, and bone cells are therefore as important as fibroblastic cells. It is known that GHRL regulates the differentiation and function of osteoblasts. In this context, GHRL also interacts with leptin, whose levels are altered in obesity and periodontitis [48]. Moreover, GHRL has also been demonstrated to protect osteoblasts against oxidative stress and apoptosis [49, 50]. Therefore, studying the role of GHRL and its functional receptor in periodontal bone and cementum under inflammatory and microbial conditions is essential. Future studies should also involve co-culture models of different periodontal cells and animal studies, which will clarify if the observed beneficial effects of GHRL on periodontal cells can also be found in a more complex environment.
Conclusions
This in vitro study demonstrates for the first time that IL-1β upregulates the functional ghrelin receptor in PDL cells and HGFs. Moreover, these results further support the assumption that the GHRL/GHS-R system exerts anti-inflammatory effects. The upregulation of the ghrelin receptor in periodontal fibroblastic cells in response to an inflammatory stimulus may serve as a protective feedback mechanism to attenuate the initial inflammatory process in periodontitis.
References
Slots J (2017) Periodontitis: facts, fallacies and the future. Periodontol 75:7–23
Silva N, Abusleme L, Bravo D, Dutzan N, Garcia-Sesnich J, Vernal R, Hernández M, Gamonal J (2015) Host response mechanisms in periodontal diseases. J Appl Oral Sci 23:329–355
Yucel-Lindberg T, Båge T (2013) Inflammatory mediators in the pathogenesis of periodontitis. Expert Rev Mol Med 15:e7
Ferreira MC, Dias-Pereira AC, Branco-de-Almeida LS, Martins CC, Paiva SM (2017) Impact of periodontal disease on quality of life: a systematic review. J Periodontal Res 52:651–665
Beikler T, Flemmig TF (2011) Oral biofilm-associated diseases: trends and implications for quality of life, systemic health and expenditures. Periodontol 55:87–103
Nascimento GG, Leite FR, Do LG, Peres KG, Correa MB, Demarco FF, Peres MA (2015) Is weight gain associated with the incidence of periodontitis? A systematic review and meta-analysis. J Clin Periodontol 42:495–505
Orlandi M, Suvan J, Petrie A, Donos N, Masi S, Hingorani A, Deanfield J, D’Aiuto F (2014) Association between periodontal disease and its treatment, flow-mediated dilatation and carotid intima-media thickness: a systematic review and meta-analysis. Atherosclerosis 236:39–46
Nibali L, Tatarakis N, Needleman I, Tu YK, D'Aiuto F, Rizzo M, Donos N (2013) Clinical review: association between metabolic syndrome and periodontitis: a systematic review and meta-analysis. J Clin Endocrinol Metab 98:913–920
Chávarry NG, Vettore MV, Sansone C, Sheiham A (2009) The relationship between diabetes mellitus and destructive periodontal disease: a meta-analysis. Oral Health Prev Dent 7:107–127
Churm R, Davies JS, Stephens JW, Prior SL (2017) Ghrelin function in human obesity and type 2 diabetes: a concise review. Obes Rev 18:140–148
Baatar D, Patel K, Taub DD (2011) The effects of ghrelin on inflammation and the immune system. Mol Cell Endocrinol 340:44–58
Müller TD, Nogueiras R, Andermann ML, Andrews ZB, Anker SD, Argente J, Batterham RL, Benoit SC, Bowers CY, Broglio F, Casanueva FF, D'Alessio D, Depoortere I, Geliebter A, Ghigo E, Cole PA, Cowley M, Cummings DE, Dagher A, Diano S, Dickson SL, Diéguez C, Granata R, Grill HJ, Grove K, Habegger KM, Heppner K, Heiman ML, Holsen L, Holst B, Inui A, Jansson JO, Kirchner H, Korbonits M, Laferrère B, LeRoux CW, Lopez M, Morin S, Nakazato M, Nass R, Perez-Tilve D, Pfluger PT, Schwartz TW, Seeley RJ, Sleeman M, Sun Y, Sussel L, Tong J, Thorner MO, van der Lely AJ, van der Ploeg LH, Zigman JM, Kojima M, Kangawa K, Smith RG, Horvath T, Tschöp MH (2015) Ghrelin. Mol Metab 4:437–460
Bowers CY (2012) History to the discovery of ghrelin. Methods Enzymol 514:3–32
Fetissov SO, Laviano A, Kalra S, Inui A (2010) Update on ghrelin. Int J Pept 2010:963501
Callaghan B, Furness JB (2014) Novel and conventional receptors for ghrelin, desacyl-ghrelin, and pharmacologically related compounds. Pharmacol Rev 66:984–1001
Laviano A, Molfino A, Rianda S, Rossi Fanelli F (2012) The growth hormone secretagogue receptor (Ghs-R). Curr Pharm 18:4749–4754
Mohamed HG, Idris SB, Mustafa M, Ahmed MF, Åstrøm AN, Mustafa K, Ibrahim SO (2015) Impact of chronic periodontitis on levels of glucoregulatory biomarkers in gingival crevicular fluid of adults with and without type 2 diabetes. PLoS One 10:e0127660
Yılmaz G, Kırzıoğlu FY, Doğuç DK, Koçak H, Orhan H (2014) Ghrelin levels in chronic periodontitis patients. Odontology 102:59–67
Liu B, Han X, Feng W, Cui J, Hasegawa T, Amizuka N, Xu X, Li M (2016) Altered distribution of ghrelin protein in mice molar development. Arch Oral Biol 65:82–86
Aydin S, Ozercan IH, Geckil H, Dagli F, Aydin S, Kumru S, Kilic N, Sahin I, Ozercan MR (2007) Ghrelin is present in teeth. J Biochem Mol Biol 40:368–372
Gröschl M, Topf HG, Bohlender J, Zenk J, Klussmann S, Dötsch J, Rascher W, Rauh M (2005) Identification of ghrelin in human saliva: production by the salivary glands and potential role in proliferation of oral keratinocytes. Clin Chem 51:997–1006
Nokhbehsaim M, Damanaki A, Nogueira AVB, Eick S, Memmert S, Zhou X, Nanayakkara S, Götz W, Cirelli JA, Jäger A, Deschner J (2017) Regulation of ghrelin receptor by periodontal bacteria in vitro and in vivo. Mediat Inflamm 2017:4916971
Mathur A, Michalowicz B, Castillo M, Aeppli D (1996) Interleukin-1 alpha, interleukin-8 and interferon-alpha levels in gingival crevicular fluid. J Periodontal Res 31:489–495
Hou LT, Liu CM, Chang WK (1994) Increased interleukin-1 beta levels in gingival crevicular fluid of Chinese periodontal patients. J Formos Med Assoc 93:99–103
Hönig J, Rordorf-Adam C, Siegmund C, Wiedemann W, Erard F (1989) Increased interleukin-1 beta (IL-1 beta) concentration in gingival tissue from periodontitis patients. J Periodontal Res 24:362–367
Nokhbehsaim M, Deschner B, Winter J, Bourauel C, Jäger A, Jepsen S, Deschner J (2012) Anti-inflammatory effects of EMD in the presence of biomechanical loading and interleukin-1β in vitro. Clin Oral Investig 16:275–283
Nokhbehsaim M, Deschner B, Winter J, Bourauel C, Rath B, Jäger A, Jepsen S, Deschner J (2011) Interactions of regenerative, inflammatory and biomechanical signals on bone morphogenetic protein-2 in periodontal ligament cells. J Periodontal Res 46:374–381
Nokhbehsaim M, Winter J, Rath B, Jäger A, Jepsen S, Deschner J (2011) Effects of enamel matrix derivative on periodontal wound healing in an inflammatory environment in vitro. J Clin Periodontol 38:479–490
Kraus D, Reckenbeil J, Wenghoefer M, Stark H, Frentzen M, Allam JP, Novak N, Frede S, Götz W, Probstmeier R, Meyer R, Winter J (2016) Ghrelin promotes oral tumor cell proliferation by modifying GLUT1 expression. Cell Mol Life Sci 73:1287–1299
Frascarelli S, Ghelardoni S, Ronca-Testoni S, Zucchi R (2003) Effect of ghrelin and synthetic growth hormone secretagogues in normal and ischemic rat heart. Basic Res Cardiol 98:401–405
Syed M, Cozart M, Haney AC, Akhter N, Odle AK, Allensworth-James M, Crane C, Syed FM, Childs GV (2013) Ghrelin restoration of function in vitro in somatotropes from male mice lacking the Janus kinase (JAK)-binding site of the leptin receptor. Endocrinology 154:1565–1576
Ohta K, Laborde NJ, Kajiya M, Shin J, Zhu T, Thondukolam AK, Min C, Kamata N, Karimbux NY, Stashenko P, Kawai T (2011) Expression and possible immune-regulatory function of ghrelin in oral epithelium. J Dent Res 90:1286–1292
Stadler AF, Angst PD, Arce RM, Gomes SC, Oppermann RV, Susin C (2016) Gingival crevicular fluid levels of cytokines/chemokines in chronic periodontitis: a meta-analysis. J Clin Periodontol 43:727–745
Gamonal J, Acevedo A, Bascones A, Jorge O, Silva A (2000) Levels of interleukin-1 beta, -8, and -10 and RANTES in gingival crevicular fluid and cell populations in adult periodontitis patients and the effect of periodontal treatment. J Periodontol 71:1535–1545
Hosokawa Y, Hosokawa I, Shindo S, Ozaki K, Matsuo T (2015) Calcitriol suppressed inflammatory reactions in IL-1β-stimulated human periodontal ligament cells. Inflammation 38:2252–2258
Iwayama T, Yanagita M, Mori K, Sawada K, Ozasa M, Kubota M, Miki K, Kojima Y, Takedachi M, Kitamura M, Shimabukuro Y, Hashikawa T, Murakami S (2012) Adiponectin regulates functions of gingival fibroblasts and periodontal ligament cells. J Periodontal Res 47:563–571
Oztas B, Sahin D, Kir H, Eraldemir FC, Musul M, Kuskay S, Ates N (2017) The effect of leptin, ghrelin, and neuropeptide-Y on serum Tnf-Α, Il-1β, Il-6, Fgf-2, galanin levels and oxidative stress in an experimental generalized convulsive seizure model. Neuropeptides 61:31–37
Tsubouchi H, Yanagi S, Miura A, Matsumoto N, Kangawa K, Nakazato M (2014) Ghrelin relieves cancer cachexia associated with the development of lung adenocarcinoma in mice. Eur J Pharmacol 743:1–10
Theil MM, Miyake S, Mizuno M, Tomi C, Croxford JL, Hosoda H, Theil J, von Hörsten S, Yokote H, Chiba A, Lin Y, Oki S, Akamizu T, Kangawa K, Yamamura T (2009) Suppression of experimental autoimmune encephalomyelitis by ghrelin. J Immunol 183:2859–2866
Zhou X, Xue C (2009) Ghrelin inhibits the development of acute pancreatitis and nuclear factor kappaB activation in pancreas and liver. Pancreas 38:752–757
Beynon AL, Brown MR, Wright R, Rees MI, Sheldon IM, Davies JS (2013) Ghrelin inhibits LPS-induced release of IL-6 from mouse dopaminergic neurons. J Neuroinflammation 10:40
Li WG, Gavrila D, Liu X, Wang L, Gunnlaugsson S, Stoll LL, McCormick M, Sigmund CD, Tang C, Weintraub NL (2004) Ghrelin inhibits proinflammatory responses and nuclear factor-kappaB activation in human endothelial cells. Circulation 109:2221–2226
Wang H, Yang T, Shen Y, Wan C, Li X, Li D, Liu Y, Wang T, Xu D, Wen F, Ying B (2016) Ghrelin inhibits interleukin-6 production induced by cigarette smoke extract in the bronchial epithelial cell via NF-κB pathway. Inflammation 39:190–198
Deng B, Fang F, Yang T, Yu Z, Zhang B, Xie X (2015) Ghrelin inhibits AngII-induced expression of TNF-α, IL-8, MCP-1 in human umbilical vein endothelial cells. Int J Clin Exp Med 8:579–588
Deo V, Bhongade ML (2010) Pathogenesis of periodontitis: role of cytokines in host response. Dent Today 29:60–62, 64–66; quiz 68-69
Graves DT, Cochran D (2003) The contribution of interleukin-1 and tumor necrosis factor to periodontal tissue destruction. J Periodontol 74:391–401
Birkedal-Hansen H (1993) Role of cytokines and inflammatory mediators in tissue destruction. J Periodontal Res 28:500–510
Delhanty PJ, van der Eerden BC, van Leeuwen JP (2014) Ghrelin and bone. Biofactors 40:41–48
Dieci E, Casati L, Pagani F, Celotti F, Sibilia V (2014) Acylated and unacylated ghrelin protect MC3T3-E1 cells against tert-butyl hydroperoxide-induced oxidative injury: pharmacological characterization of ghrelin receptor and possible epigenetic involvement. Amino Acids 46:1715–1725
Liang QH, Liu Y, Wu SS, Cui RR, Yuan LQ, Liao EY (2013) Ghrelin inhibits the apoptosis of MC3T3-E1 cells through ERK and AKT signaling pathway. Toxicol Appl Pharmacol 272:591–597
Acknowledgements
The authors would like to thank Prof. Heiko Spallek, Ms. Ramona Menden, and Ms. Silke van Dyck for their valuable support. This study was supported by the Medical Faculty of the University of Bonn and the University of Sydney.
Funding
This study was supported by the Medical Faculty of the University of Bonn and the University of Sydney.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards. This article does not contain any studies with animals performed by any of the authors.
Rights and permissions
About this article
Cite this article
Nokhbehsaim, M., Memmert, S., Damanaki, A. et al. Effect of interleukin-1β on ghrelin receptor in periodontal cells. Clin Oral Invest 23, 113–122 (2019). https://doi.org/10.1007/s00784-018-2417-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00784-018-2417-y