Abstract
Purpose
Patients with brain cancer and painful symptoms of the disease experience heavy pressure and negative inner experiences, leading to a sense of stigma. Therefore, this study assessed the level of stigma in patients with brain cancer and analyzed the risk factors for stigma to analyze the underlying relationships among depression, social support, low self-esteem, and stigma.
Methods
Patients completed the Social Impact Scale, Self-rating Depression Scale, Rosenberg Self-Esteem Scale, Herth Hope Index, Social Support Rating Scale, and Self-Perceived Burden Scale. Multiple linear regression analysis was used to identify factors independently associated with stigma. Parallel mediation analysis was used to evaluate the mediating role of the relationship between psychoemotional factors and stigma.
Results
A multivariate linear regression analysis demonstrated significant associations between age (β = − 0.189, P = 0.002), treatment (β = 0.184, P = 0.003), self-esteem (β = − 0.128, P = 0.046), depression (β = 0.273, P < 0.001), hope (β = − 0.217, P = 0.003), and self-perceived burden (β = 0.260, P < 0.001) with brain cancer. It was observed that the social support received by brain cancer patients directly impacted their stigma (total effect, − 0.851, P = 0.001). Additionally, this relationship was influenced by depression and self-esteem through two distinct pathways.
Conclusion
Increased stigma among brain cancer patients was found to be associated with severe depression, feelings of inferiority, diminished hope, and a heavy perceived burden. The structural equation modeling (SEM) revealed that social support negatively influenced stigma through depression and self-esteem. It is imperative to grasp patients’ inner needs, implement psychological interventions, and cultivate a cancer-friendly social environment to prevent stigmatization and discrimination based on their patient status.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Brain cancer constitutes a prevalent disease of the nervous system, accounting for approximately 40–50% of intracranial tumors. Brain cancer is ranked ninth in the incidence spectrum of cancer and exhibits annual fluctuations in prevalence [1, 2]. Patients with brain cancer experience both physical symptoms and psychological distress, which are influenced by the pathological characteristics of the disease, the tumor’s location, and its size. These include abnormal changes in neurological and cognitive functioning, as well as alterations in personality and behavior [3], leading to significant physical and mental stress. Those with brain cancer and painful symptoms endure substantial pressure and adverse psychological experiences, which contribute to a sense of stigma [4,5,6]. Public misconceptions about brain cancer lead to beliefs that such patients may display psychiatric and behavioral abnormalities, potentially posing safety risks. Consequently, the societal response often involves estrangement, exclusion, and even discrimination, further intensifying the patient’s feelings of shame [4, 7, 8].
Research on cancer stigma has verified that cancer is a highly stigmatized illness [4]. Sociologist Goffman described stigma as an attribute that discredits an individual, making them feel distinct from others and reducing their status to that of a tainted individual [9]. The “modified labeling theory” (MLT), proposed by Link, outlines stigma through its components—labeling, stereotyping, separation, status loss, and discrimination. Knapp et al. discuss the classic theory of stigma, highlighting the perceived threat of “cancer” status as a primary cause of stigma [6]. Researchers agree on the strong link between social discrimination, patients’ self-perception, and stigma development. Stigma arises from both internal and external factors, with its intermittent or persistent presence adversely affecting patients’ social roles, mental health, disease diagnosis, and quality of life.
The stigma research includes three primary disease categories: infectious diseases like AIDS, appearance and psychology-related conditions such as obesity and schizophrenia [10], and illnesses like cancer [5, 11]. This study focuses on the stigma experienced by brain cancer patients, which is part of the broader theoretical framework of cancer-related stigma. Drawing from stigma theory, we posit that the stigma surrounding brain cancer patients arises from multifaceted factors. Firstly, there is stigma stemming from dysfunction and disability. Brain cancer patients often experience motor, speech, and neurological impairments leading to temporary or sustained disability, fostering a sense of stigma. Secondly, concerns about body image contribute to stigma [12]. Thirdly, discrimination during societal and workplace reintegration may erode social roles, resulting in social isolation [4, 13]. This underscores that the stigma felt by brain cancer patients originates from various causes, many of which are unavoidable.
Although many studies have examined stigma among cancer patients, few have focused on those with brain cancer [5, 14, 15]. Baksi et al. surveyed 124 patients with primary malignant brain tumors, finding high levels of perceived stigma. The study showed that with increasing age and hope levels, the experience of negative discrimination decreased. However, patients currently undergoing radiotherapy reported increased experiences of discrimination [4]. Similarly, Acquaye et al. and Stergiou-Kita et al. found that patients with brain cancer often suffer from low hope and increased stigma levels, adversely affecting their attendance, treatment, and prognosis [16, 17]. Research on the stigma of cancer patients in China has primarily focused on lung, cervical, and breast cancer, with less attention given to nervous system diseases [5, 18]. Prior research has shown that stigma can reduce self-esteem in patients with brain cancer, placing a significant psychological burden on them and potentially delaying diagnosis, reducing treatment compliance, and adversely affecting their prognosis and quality of life [4]. Thus, understanding the current state of stigma in brain cancer patients and its influencing factors is crucial for improving their quality of life in China.
Huang et al.’s study corroborated the close relationship between the stigma experienced by cancer patients and various factors such as depression, self-perceived burden, social support, self-esteem, and hope levels [5]. A prior study by our group also measured stigma in patients with growth hormone–type pituitary tumors, revealing high stigma levels and identifying anxiety, inferiority-type personality, and body image concerns as risk factors [19]. Further, anxiety was found to mediate the relationship between stigma and depression [15]. Zamanian et al. suggested that social support and coping strategies could mediate the impact of stigma on patients’ quality of survival [20]. A mediation effect model indicated that body image mediated the relationship between stigmatization and depressive symptoms [21]. Lebel et al.’s study found that illness intrusiveness in significant life domains partially mediated the psychosocial impact of stigma on both subjective well-being and distress [22]. Structural equation modeling was used to propose the possible effects of stigma on anxiety and then the possible effects of anxiety on depression among patients with head and neck cancer [15]. Structural equation modeling was used to propose the possible effects of stigma on anxiety and then the possible effects of anxiety on depression among patients with head and neck cancer [23].
Through the literature review, we found that Baksi et al.’s article is highly worth our study. While Baksi et al.’s study [4] tended to analyze stigma in a comprehensive way, including three aspects: positive experienced discrimination, negative experienced discrimination, and anticipated discrimination, our study will analyze stigma in these four aspects: social rejection, financial insecurity, internalized shame, and social isolation. Such varying perspectives potentially enrich the findings and complement previous research conclusions. Moreover, existing studies have confirmed a mechanism of action between psychological factors such as anxiety, depression, and stigma in different groups of tumor patients, although the pathways between these factors have not been fully explored in brain tumor patients [15, 20]. This study, therefore, constructed a mediation model with stigma as the dependent variable to further clarify the influence of psychological factors on stigma. The analysis of mediating effects revealed causal relationships between variables and underlying mechanisms, which are crucial for developing interventions focused on improving aspects of psychological health.
Hence, this investigation evaluated stigma among brain cancer patients via questionnaires, while incorporating psychological assessments for depression and low self-esteem to explore the connection between stigma and negative emotions, alongside identifying stigma risk factors. Furthermore, we proposed a hypothesis positing a significant correlation between brain cancer patients’ stigma and psychological aspects like depression and low self-esteem, intending to elucidate the mediation effect between these variables.
Methods
Participants
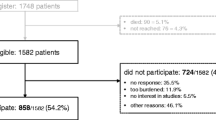
The study procedure received approval from the Ethics Committee of the Affiliated Hospital of Nantong University (2021-K051) and strictly adhered to the principles of confidentiality, non-harm, and informed consent in accordance with the Declaration of Helsinki. Patients were informed about the study’s content, purpose, and significance and provided voluntary consent to participate. All participants met the following inclusion criteria: (1) diagnosis of brain cancer confirmed through imaging and pathology or by neurosurgeons, (2) awareness of brain cancer, and (3) age ≥ 18 years. Exclusion criteria comprised the following: (1) concurrent diagnosis of another cancer or brain tumor metastasis; (2) severe hepatic, hematological, cardiovascular, renal, or other conditions that impeded questionnaire completion due to physical weakness; and (3) psychiatric disorders (presence of ICD-10 psychiatric diagnoses) or cognitive impairment (MMSE ≤ 17 for illiterate individuals, ≤ 20 for participants with elementary school education, and ≤ 24 for those with middle school education and above) hindering questionnaire completion. A total of 135 brain cancer patients from the Department of Neurosurgery were invited to participate between June 2021 and December 2022.
Assessment tools
The questionnaire design integrated insights from pertinent literature and recommendations from clinical experts to gather both general and disease-specific information from patients. This included data such as age at diagnosis, gender, occupation, religion, treatment approach, and chronic health conditions. Chronic diseases documented were those with confirmed diagnoses, such as gout, hypertension, diabetes, stroke, coronary artery disease, and chronic pulmonary conditions. Additionally, the Karnofsky Performance Scale (KPS) score was evaluated and documented prior to the patient’s hospital discharge, while tumor pathology was graded according to WHO classifications II to IV.
Social Impact Scale (SIS)
The scale, initially developed by Fife and Wright [23] in 2000 based on Link’s “Modified Labeling Theory” (MLT) of stigma, was translated into traditional Chinese by Pan Aiwan in Taiwan Province of China [24]. Due to cultural variations within China, we culturally adapted and revised the scale. The reliability analysis of the revised scale met statistical standards, and it was subsequently published in prominent journals in China. Thus, this study employed the revised scale, comprising four dimensions: internalized shame (4 items) includes item such as “I feel I need to keep my illness a secret”, social isolation (6 items) includes item such as “Changes in my appearance have affected my social relationship,” social rejection (9 items) includes item such as “I feel others avoid me because of my illness,” and financial insecurity (3 items) includes item such as “I have experienced financial hardship that has affected my relationship with others.” Among them, social rejection and financial insecurity represent experienced stigma, with scores ranging from 12 to 48, and internalized shame and social isolation represent the internalized experience of being stigmatized, with scores ranging from 10 to 40. Responses were scored on a 4-point Likert scale ranging from 1 (strongly disagree) to 4 (strongly agree), with higher scores indicating greater stigma levels. The Cronbach α coefficient for this scale in our study was 0.933.
Self-rating Depression Scale (SDS)
The scale is utilized to evaluate individuals’ depression levels, comprising 20 items, such as “I feel down-hearted and blue,” aimed at comprehending the patient’s specific life performance. Responses are measured using a 4-point Likert scale. The scores from each item are totaled and then multiplied by 1.25 to derive the final assessment score. In China, a score falling between 53 and 62 indicates mild depression, while scores ranging from 63 to 72 indicate moderate depression. Scores above 72 are indicative of severe depression, with higher scores reflecting more pronounced depression [25]. The Cronbach α coefficient for this scale in our study was 0.854.
The Rosenberg Self-Esteem Scale (RSES)
The scale comprises 10 items, such as “On the whole, I am satisfied with myself,” and is utilized to measure an individual’s self-esteem level. Total scores range from 10 to 40, with lower scores indicating a tendency towards inferiority complex personality traits, while higher scores suggest elevated levels of self-esteem. In China, a total score below 10 indicates an inferiority personality, scores between 10 and 20 suggest an inclination towards inferiority, scores from 21 to 30 indicate relatively high self-esteem, and scores falling between 31 and 40 indicate high self-esteem [26]. The Cronbach α coefficient for this scale in our study was 0.907.
Herth Hope Index (HHI)
The HHI scale was originally developed by Hert, including items such as “I have a faith that gives me comfort.” The 12 items are scored on a 4-point Likert scale, with a total possible score of 12 ~ 48 points. A score of 12 ~ 23 points indicates a low level of inner hope, 24 ~ 35 points indicates a medium level of hope, and 36 ~ 48 points indicates a high level of hope; the higher the score is, the greater the level of hope of the individual [27]. The Cronbach α coefficient for this scale in our study was 0.894.
Social Support Rating Scale (SSRS)
The SSRS includes three dimensions: support utilization, subjective support, and objective support, including items such as “How many close friends do you have who could use support and help.” Scores on this scale range from 11 to 66, where higher scores indicate greater perceived social support [28]. In our study, the Cronbach α coefficient for this scale was 0.676.
Self-Perceived Burden Scale (SPBS)
The SPBS includes 10 items, such as “Difficulty in accepting need to rely on others,” rated on a scale of 1 to 5, ranging from “never” to “always,” to measure the subject’s perception of burden. The total score, ranging from 10 to 50, is obtained by summing these scores, with higher scores indicating increased self-perceived burden [29]. In our study, Cronbach’s α coefficient for this scale was 0.899.
Karnofsky Performance Status Scale (KPS)
It is mainly used to assess functional capability to carry out normal daily activities.With a total score of 0 ~ 100, patients with a score of more than 80 are usually considered to be independent, with good self-care ability; with a score of 50 ~ 70, patients are considered to be frail, needing the assistance of others but able to partially realize self-care; with a score of less than 50, patients are considered to be dependent, with difficulty in realizing self-care in their lives [30].
Data collection and quality control
In this study, standardized protocols were followed to guide patients in understanding the questionnaire instructions. The survey was administered a day before the patients’ hospital discharge. Patients completed the questionnaire independently, with timely clarification provided for any uncertainties. For patients with low education levels or visual impairments unable to complete the questionnaire alone, the researcher offered assistance. Throughout the data collection phase, two researchers double-checked each question’s completion, addressing any errors or omissions with the patients. Data entry was carried out by two investigators after confirming accuracy and subsequently reviewed by one investigator to ensure completeness and correctness.
Statistical analysis
Data analysis was conducted using IBM SPSS 26.0 and AMOS 26.0, with graph plotting performed using GraphPad Prism 9.5.1. (a) Descriptive analysis: The normality of data distribution was assessed using the Kolmogorov‒Smirnov test, which combined skewness and kurtosis results. General data, disease-related data, and psychometric scale scores of brain cancer patients were described using mean ± standard deviation (X̅ ± SD) for normally distributed data and median (25th and 75th percentiles) for non-normally distributed data. (b) Univariate analysis of variance: Spearman’s correlation was employed to examine the relationship between stigma level and scores of various psychological scales. The Mann–Whitney U test and Kruskal–Wallis H test were utilized to compare stigma total scores and dimension scores among different brain cancer patient groups. (c) Multifactorial analysis: Variables found statistically significant (P < 0.05, two-sided) in univariate analysis were included in a multiple linear regression model to identify factors influencing stigma in brain cancer patients. (d) Parallel mediation analysis: The mediating role of psychoemotional factors in the relationship with stigma was evaluated. A total of 2000 bootstrap samples were implemented for percentile bootstrap confidence intervals, with a confidence level set at 95%.
Results
Patient characteristics and results of univariate analysis on the factors of stigma in patients with brain cancer
Table 1 presents the demographic and clinical characteristics of 135 brain cancer patients. The mean age of the patients was 58.32 years (SD = 12.94, range = 20 ~ 78). Among them, 57.04% were male, 91.85% were married, and 77.78% were currently employed. The average time since diagnosis was 10.65 months. None of the participants had comorbid infectious diseases such as AIDS. Dizziness and headache were the primary symptoms in 69.63% of patients. Tumor locations included 40% in the frontal lobe, 28.15% in the temporal lobe, and 31.85% in other brain regions like parietal and occipital lobes. Tumor diameters ranged from 1.5 to 6.8 cm. Most patients received a pathological diagnosis of glioma (65.19%). The WHO grade at resection determined the tumor’s WHO grade [31]. The WHO grade IV brain cancer was used for 43.00% of the patients, the WHO grades II–III were used for 57.00%, and 51.85% of the patients had a KPS score greater than 80, indicating good physical functioning. The results of the univariate analysis of variance showed that age (Z = − 3.686, P < 0.001), recurrence (Z = − 3.068, P = 0.002), treatment (Z = 21.788, P < 0.001), course of disease (Z = − 3.038, P < 0.001), and characteristics (Z = 14.724, P < 0.001) had effects on stigma.
Psychological characteristics and stigma scores
Table 2 summarizes the psychological characteristics of brain cancer patients. Scale score results revealed that some patients exhibited poor psychological status. The median stigma score among brain cancer patients was 62.00 (55.00, 71.00), indicating severe feelings of stigma, with scores ranging from 40 to 88. Among the four stigma dimensions, social isolation had the highest mean average item score (3.10 points). A comparison of mean average item scores for the four dimensions revealed that social isolation was more severe than social rejection, with a statistically significant difference (P = 0.003) (Fig. 1). Moreover, 22.22% of patients experienced severe depression, 45.93% displayed an inclination towards inferiority, and 48.15% had low hope in life. Univariate analysis of variance results indicated that depression (Z = 36.673, P < 0.001), self-esteem (Z = 16.163, P < 0.001), hope (Z = − 6.043, P < 0.001), social support (r = − 0.345, P < 0.001), and self-perceived burden (r = 0.358, P < 0.001) significantly influenced stigma.
Multivariate linear regression model of the factors associated with stigma in brain cancer patients
Table 3 presents the results of the multiple linear regression analysis investigating potential predictors of stigma in brain cancer patients. The validity of the model was initially tested, with the variance inflation factor (VIF) ranging from 1.081 to 1.526, indicating no multicollinearity among the variables. Additionally, the Durbin-Watson value of 1.851 suggested that the residuals were independent of each other. Together, these six factors accounted for 54.70% of the stigma experienced by brain cancer patients. Age (β = − 0.189, P = 0.002), treatment method (β = 0.184, P = 0.003), self-esteem (β = − 0.128, P = 0.046), depression (β = 0.273, P < 0.001), hope (β = − 0.217, P = 0.003), and self-perceived burden (β = 0.260, P < 0.001) were found to be significantly associated with brain cancer stigma. These results suggest that individuals aged less than 60 years, experiencing severe depression, displaying inferiority tendencies, having low hope, perceiving heavy burdens, and undergoing different treatment methods are influencing factors for stigma in brain cancer patients. Additionally, a false discovery rate (FDR) correction based on R Studio was performed to minimize false-positive results. After FDR adjustment, the six factors of stigma remained significant.
Structural equation modeling (SEM) of stigma, social support, depression, and self-esteem
Table 4 The correlation analysis results of the psychological characteristics of brain cancer patients are presented in Table 4. The stigma score exhibited significant correlations with depression (r = 0.529, P < 0.01), self-esteem (r = − 0.350, P < 0.01), and social support (r = − 0.345, P < 0.01).
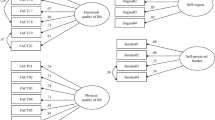
SEM confirmed the mediating effect relationship between stigma, social support, depression, and self-esteem, and the model summary of the structural equation was as follows: χ2/df = 1.246, RMSEA = 0.043, GFI = 0.995, AGFI = 0.954, CFI = 0.997, and TLI = 0.983. The pathway analysis results revealed that the social support of brain cancer patients had a direct influence on their stigma (total effect, − 0.851, P = 0.001). Depression and self-esteem mediated this relationship through two distinct pathways. Comparing the indirect effects of these two pathways, the results indicated no difference in the magnitude of the mediating effect of depression and self-esteem on stigma (Table 5, Fig. 2).
Discussion
In this study, the median stigma score among brain cancer patients was 62.00 (55.00, 71.00), suggesting comparable or potentially more severe stigma levels than those observed in other cancer patients [5, 32]. Multiple linear regression analysis identified age under 60, severe depression, inclination towards inferiority, low hope, and heavy perceived burden as risk factors for stigma. Furthermore, the pathway analysis results indicated that social support directly influenced brain cancer patients’ stigma (total effect, − 0.851, P = 0.001), with depression and self-esteem mediating this relationship through distinct pathways.
In our analysis of the patients’ scores across the four dimensions of stigma, we observed that stigma among patients primarily manifested in social isolation. Within the traditional Chinese cultural context, the pessimistic and negative psychosocial feelings resulting from brain cancer contribute significantly to the stigma experienced by patients. Consequently, brain cancer patients often perceive themselves as belonging to marginalized groups, view themselves as having little value, and fear societal discrimination, which exacerbates feelings of isolation and segregation [33]. Our study also indicated that social isolation was more pronounced than social rejection, with a statistically significant difference (P = 0.003). Considering these findings, it can be inferred that the internalized experience of stigma may have a more profound impact on a patient’s psychological well-being, as patients harbor fears of discrimination due to their illness.This observation suggests that healthcare professionals should prioritize addressing negative psychological emotions, such as fear, in brain cancer patients. Implementing psychotherapy and psychosocial care interventions could help mitigate the internalized experience of stigma among these individuals.
This study examined various factors influencing stigma in brain cancer patients from diverse perspectives. From a sociodemographic standpoint, being under 60 years old emerged as a risk factor of stigma, consistent with previous research [4]. Malignant brain tumors often afflict young and middle-aged individuals, many of whom have active careers and multiple social roles [2]. Transitioning to the status of cancer patients not only burdens them financially but also exposes them to potential discrimination in the workplace. Moreover, losing these social roles may lead to a perceived loss of personal value, contributing to feelings of uselessness, isolation, and increased stigma. Regarding clinical characteristics, the severity of stigma varied among different treatment modalities, with patients undergoing surgery reporting lower levels of stigma. These findings align with prior studies, including those by scholars such as Baksi et al., who found that brain cancer patients undergoing chemotherapy experience the most severe stigma [4, 34]. This may be attributed to the adverse effects of chemotherapy and radiotherapy, such as hair loss and dermatitis, which can negatively impact the patient’s appearance and self-image, fostering an inferiority complex and reducing social engagement, thereby exacerbating feelings of social isolation.
The lack of hope for life among brain cancer patients is a significant concern. Consistent with Baksi et al.’s findings [4], our study revealed that lower levels of hope were associated with higher levels of stigma in brain cancer patients. Hope serves as a positive psychological belief and intrinsic motivation, enabling patients to confront treatment and recovery with optimism, thereby resisting the negative pessimism induced by illness. It plays a crucial role in maintaining a positive mental health state and has been demonstrated to motivate patients to maintain a positive mood and aid in physical recovery [35]. Research indicates that patients and their families generally prefer healthcare communication that provides an authentic prognosis, which can foster hope [36]. Thus, healthcare professionals should offer transparent explanations about disease progression to alleviate unnecessary worries and fears and help patients develop a correct understanding of their condition to maintain hope for life. Moreover, music interventions, comprising music therapy provided by trained music therapists and music medicine, involving listening to prerecorded music administered by healthcare professionals, have been shown to effectively enhance hope levels in cancer patients [37]. Therefore, implementing music interventions in brain cancer patients could potentially reduce stigma.
Patients experiencing high self-perceived burdens often encounter greater stigma. Culturally ingrained beliefs regarding family and filial piety in Chinese brain cancer patients may contribute to this burden [38]. Some patients may fear rejection from others due to visible physical changes, mobility limitations, and the financial strain of the illness. Additionally, the ongoing need for caregiving may lead to feelings of low self-esteem and guilt, further exacerbating their social isolation and negative emotions in interpersonal interactions, ultimately intensifying the sense of stigma. Qualitative studies have shown that cancer patients prioritize their families’ well-being over their own health when considering the ramifications of their disease [39]. This dynamic undoubtedly adds to the patient’s burden and amplifies internal suffering. Drawing from previous research findings, the expressive writing approach may offer an effective psychotherapeutic strategy to help brain cancer patients alleviate feelings of burden and stigma [40].
The outcomes of the self-esteem questionnaire in this cohort revealed that nearly half of the patients experienced feelings of inferiority, representing a risk factor for stigma in brain cancer patients. Malignant brain tumors often induce functional limitations, disability, and changes in appearance, fostering a sense of denial, worthlessness, and inferiority in affected individuals. As these sentiments intensify, patients may perceive a decline in their self-worth and grapple with escalating self-doubt. Learning from insights gleaned in prior research, it may be prudent to prioritize strategies aimed at mitigating discrimination and alleviating feelings of inferiority [41, 42].
Aligned with prior studies emphasizing negative emotions, depression emerged as a key risk factor for stigma among brain cancer patients in this study [43]. Within our sample, a significant majority (67.41%) experienced mild to moderate depression. According to cognitive-behavioral theory, individuals with severe depressive symptoms may develop emotional disturbances characterized by extreme thoughts and increased sensitivity to their surroundings [44]. Both depression and stigma represent negative states of mind, potentially interacting to create a detrimental cycle. Brain cancer patients confront substantial physical and psychological burdens during treatment, making them vulnerable to depression and subsequent negative emotions, potentially fostering perceptions of discrimination and rejection. Building upon previous studies [15, 20], our study hypothesized a potential mediating effect between various psychoemotional factors and stigma among brain cancer patients. Through SEM analysis, we constructed meaningful models with depression and self-esteem as mediating variables and social support as the X-variable. Our model suggested that social support negatively predicted stigma through depression and self-esteem pathways, with comparable effect values between the two. Overall, our findings propose a plausible causal model indicating that brain cancer patients’ perceptions of inadequate social support may trigger depression and low self-esteem, subsequently contributing to stigma development. This novel perspective suggests that interventions targeting the adverse effects of stigmatization should prioritize improving social support and addressing depression and low self-esteem, rather than solely focusing on stigma itself.
It is worth noting that social support comprises several facets; on the one hand, it is recommended that the family, friends, and healthcare professionals of the patient be encouraged to enhance their care and support, which should be readily accessible to the patient [45]. Regarding the social environment, it is advisable to conduct public awareness and educational campaigns to increase the general public’s understanding of the disease. In China, public-facing health science initiatives (including videos and live streaming) conducted by healthcare professionals have proven to be effective. Through the dissemination of knowledge about brain cancer via online media, the public can be informed about the symptoms and treatment processes of brain cancer, which helps reduce misconceptions about the patients and promotes the formation of a patient-friendly social support system. This is conducive to decreasing the exclusion and isolation of patients within the social environment. A new psychological intervention named “Coping Internalized Stigma Program’ (PAREI) has been shown to be effective in treating stigma in patients with mental illness [46], suggesting that healthcare professionals need to draw on new treatments in order to develop multidisciplinary psychological intervention programs [47]. Cancer self-help groups (CSHGs) have demonstrated effectiveness in improving the psychological well-being of cancer patients, suggesting the potential value of adopting or exploring interventions to mitigate the stigma associated with the disease [48]. Additionally, scholars have conducted extensive research on the social experiences of brain tumor patients. Previous studies, utilizing both qualitative and quantitative methodologies and drawing upon scientific theories such as social identity theory and social network buffering, have highlighted the significance of maintaining social connections for brain tumor patients. These studies have indicated that stronger social connections can mitigate the negative psychological impacts of the disease, such as depression and anxiety [49,50,51]. From a social-environmental perspective, it is imperative not to leave brain tumor patients isolated. Therefore, healthcare professionals and individuals around patients should actively encourage participation in community activities, potentially facilitating the formation of new social connections and fostering a profound sense of resilience and mutual support.
Study limitations
Certainly, there are several limitations to acknowledge in this study. Firstly, while the SSRS is widely recognized and compliant with measurement standards, the Cronbach alpha observed in our sample was relatively low, possibly due to the limited sample size. Secondly, the grouping of “Course of disease” lacked a sufficient categorical basis, and although it did not impact on the findings, it is hoped that a more rigorous basis for grouping can be found in our later studies.Thirdly, SEM may exhibit less stability with small samples (60–120), and the minimum sample size primarily depends on the model’s complexity, effect size, and degrees of freedom. Future endeavors will entail expanding the sample size and constructing a more robust mediation effect model. However, exploring the causal relationships underlying stigma, self-esteem, social support, and depression among brain cancer patients remains largely unexplored. Thus, longitudinal follow-up research and qualitative inquiries are essential to substantiate causality, while considering relevant confounding variables. Moreover, the discussion on social support in this study was somewhat one-sided. It would be valuable to explore the distinctions between “general’ social support (from friends/family) and support from individuals facing similar health conditions. This broader perspective may yield more clinically meaningful insights. Lastly, stigma is a persistent negative psychological state that can undermine stability. Extending the duration of patient follow-up, examining stigma in patients during recovery, and exploring online interventions such as internet applications are avenues worth exploring.
Conclusion
Our results hold significant implications. Increased stigma among brain cancer patients is associated with severe depression, feelings of inferiority, low hope, and a heavy perceived burden. The SEM analysis demonstrated that social support was inversely associated with stigma through its effects on depression and self-esteem. Understanding the intrinsic needs of patients, delivering psychological interventions, and cultivating a cancer-supportive social environment are essential measures to mitigate the risk of stigmatization and discrimination due to their patient status.
Data availability
No datasets were generated or analyzed during the current study.
References
Global Burden of Disease Cancer C, Kocarnik JM, Compton K et al (2022) Cancer. Incidence, mortality, years of life lost, years lived with disability, and disability-adjusted life years for 29 cancer groups from 2010 to 2019: a systematic analysis for the Global Burden of Disease Study 2019. JAMA Oncol 8:420–444
Miller KD, Ostrom QT, Kruchko C, Patil N, Tihan T, Cioffi G, Fuchs HE, Waite KA, Jemal A, Siegel RL (2021) Barnholtz-Sloan JS (2021) Brain and other central nervous system tumor statistics. CA Cancer J Clin 71:381–406
Weyer-Jamora C, Brie MS, Luks TL, Smith EM, Hervey-Jumper SL, Taylor JW (2021) Postacute cognitive rehabilitation for adult brain tumor patients. Neurosurgery 89:945–953
Baksi A, Arda Surucu H, Genc H (2021) Hope, Sociodemographic and clinical characteristics as predictors of stigma-related negative discrimination experiences of patients with primary malignant brain tumor. J Neurosci Nurs 53:81–86
Huang Z, Yu T, Wu S, Hu A (2021) Correlates of stigma for patients with cancer: a systematic review and meta-analysis. Support Care Cancer 29:1195–1203
Knapp S, Marziliano A, Moyer A (2014) Identity threat and stigma in cancer patients Health Psychol Open 1:2055102914552281
Kelly D, Casey M, Beattie McKenna F, McCarthy M, Kiely P, Twomey F, Glynn L et al (2021) Identifying the gaps in Irish cancer care: patient, public and providers’ perspectives. Health Policy 125:1482–1488
Rigney M, Rapsomaniki E, Carter-Harris L, King JC (2021) A 10-year cross-sectional analysis of public, oncologist, and patient attitudes about lung cancer and associated stigma. J Thorac Oncol 16:151–155
Stergiou-Kita M, Pritlove C, Kirsh B (2016) The “Big C”-stigma, cancer, and workplace discrimination. J Cancer Surviv 10:1035–1050
Rubino F, Puhl RM, Cummings DE, Eckel RH, Ryan DH, Mechanick JI, Nadglowski J, Ramos Salas X, Schauer PR, Twenefour D, Apovian CM, Aronne LJ, Batterham RL, Berthoud HR, Boza C, Busetto L, Dicker D, De Groot M, Eisenberg D, Flint SW, Huang TT, Kaplan LM, Kirwan JP, Korner J, Kyle TK, Laferrere B, le Roux CW, McIver L, Mingrone G, Nece P, Reid TJ, Rogers AM, Rosenbaum M, Seeley RJ, Torres AJ, Dixon JB (2020) Joint international consensus statement for ending stigma of obesity. Nat Med 26:485–497
Lei H, Tian X, Jin YF, Tang L, Chen WQ, Jimenez-Herrera MF (2021) The chain mediating role of social support and stigma in the relationship between mindfulness and psychological distress among Chinese lung cancer patients. Support Care Cancer 29:6761–6770
Zhang X, Li Y, Zhong Y, Wang Z (2022) Variables associated with body image concerns in acromegaly patients: a cross-sectional study Front Psychol 13:733864
Shim S, Kang D, Bae KR, Lee WY, Nam SJ, Sohn TS, Jeong BC, Sinn DH, Kweon SS, Shim YM, Cho J (2021) Association between cancer stigma and job loss among cancer survivors. Psychooncology 30:1347–1355
Ostroff JS, Riley KE, Shen MJ, Atkinson TM, Williamson TJ, Hamann HA (2019) Lung cancer stigma and depression: validation of the Lung Cancer Stigma Inventory. Psychooncology 28:1011–1017
Tseng WT, Lee Y, Hung CF et al (2022) Stigma, depression, and anxiety among patients with head and neck cancer. Support Care Cancer 30:1529–1537
Acquaye AA, Lin L, Vera-Bolanos E, Gilbert MR, Armstrong TS (2016) Hope and mood changes throughout the primary brain tumor illness trajectory. Neuro Oncol 18:119–125
Stergiou-Kita M, Qie X, Yau HK, Lindsay S (2017) Stigma and work discrimination among cancer survivors: a scoping review and recommendations: stigmatisation et discrimination au travail des survivants du cancer : Examen de la portee et recommandations. Can J Occup Ther 84:178–188
Tang WZ, Yusuf A, Jia K, Iskandar YHP, Mangantig E, Mo XS, Wei TF, Cheng SL (2022) Correlates of stigma for patients with breast cancer: a systematic review and meta-analysis. Support Care Cancer 31:55
Li Y, Zhang X, Zhang J, Zhang D, Wang Y, Zhu Y, Xu X (2022) Stigma and unhealthy psychological characteristics in patients with acromegaly: a cross-sectional study and identification of the associated factors. Acta Neurochir (Wien) 164:2069–2081
Zamanian H, Amini-Tehrani M, Jalali Z et al (2022) Stigma and quality of life in women with breast cancer: mediation and moderation model of social support, sense of coherence, and coping strategies. Front Psychol 13:657992
Esser P, Mehnert A, Johansen C, Hornemann B, Dietz A, Ernst J (2018) Body image mediates the effect of cancer-related stigmatization on depression: a new target for intervention. Psychooncology 27:193–198
Lebel S, Castonguay M, Mackness G, Irish J, Bezjak A, Devins GM (2013) The psychosocial impact of stigma in people with head and neck or lung cancer. Psychooncology 22:140–152
Fife BL, Wright ER (2000) The dimensionality of stigma: a comparison of its impact on the self of persons with HIV/AIDS and cancer. J Health Soc Behav 41:50–67
Pan AW, Chung L, Fife BL, Hsiung PC (2007) Evaluation of the psychometrics of the Social Impact Scale: a measure of stigmatization. Int J Rehabil Res 30:235–238
Babore A, Bramanti SM, Lombardi L, Stuppia L, Trumello C, Antonucci I, Cavallo A (2019) The role of depression and emotion regulation on parenting stress in a sample of mothers with cancer. Support Care Cancer 27:1271–1277
Hong Y, Yuhan L, Youhui G, Zhanying W, Shili Z, Xiaoting H, Wenhua Y (2022) Death anxiety among advanced cancer patients: a cross-sectional survey. Support Care Cancer 30:3531–3539
Liu M, Liu L, Zhang S, Li T, Ma F, Liu Y (2022) Fear of cancer recurrence and hope level in patients receiving surgery for non-small cell lung cancer: a study on the mediating role of social support. Support Care Cancer 30:9453–9460
Wang L, Luo J, Li Y et al (2022) Social support, anxiety, and depression in patients with prostate cancer: complete mediation of self-efficacy. Support Care Cancer 30:6851–6856
Ting CY, Teh GC, Yu KL, Alias H, Tan HM, Wong LP (2020) Self-perceived burden and its associations with health-related quality of life among urologic cancer patients. Eur J Cancer Care (Engl) 29:e13248
Zhang D, Wang J, Gu X et al (2022) Prevalence, correlates, and impact of sleep disturbance in Chinese meningioma patients. Support Care Cancer 30:1231–1241
Louis DN, Perry A, Reifenberger G, von Deimling A, Figarella-Branger D, Cavenee WK, Ohgaki H, Wiestler OD, Kleihues P (2016) Ellison DW (2016) The. World Health Organization classification of tumors of the central nervous system: a summary Acta Neuropathol 131:803–820
Yang N, Cao Y, Li X, Li S, Yan H, Geng Q (2018) Mediating effects of patients’ stigma and self-efficacy on relationships between doctors’ empathy abilities and patients’ cellular immunity in male breast cancer patients. Med Sci Monit 24:3978–3986
Deng C, Lu Q, Yang L, Wu R, Liu Y, Li L, Chen S, Wei S, Wang Y, Huang Y, Fu L, Yue Z (2019) Factors associated with stigma in community-dwelling stroke survivors in China: a cross-sectional study. J Neurol Sci 407:116459
Paltun B, Bolukbas N (2021) Turkish version of the cancer stigma scale: validity and reliability study. Psychol Health Med 26:37–48
Steffen LE, Vowles KE, Smith BW, Gan GN, Edelman MJ (2018) Daily diary study of hope, stigma, and functioning in lung cancer patients. Health Psychol 37:218–227
Feldman DB, Corn BW (2023) Hope and cancer Curr Opin Psychol 49:101506
Bradt J, Dileo C, Myers-Coffman K, Biondo J (2021) Music interventions for improving psychological and physical outcomes in people with cancer. Cochrane Database Syst Rev 10(10):CD006911
Yeung NCY, Lu Q, Mak WWS (2019) Self-perceived burden mediates the relationship between self-stigma and quality of life among Chinese American breast cancer survivors. Support Care Cancer 27:3337–3345
Warmoth K, Cheung B, You J, Yeung NCY, Lu Q (2017) Exploring the social needs and challenges of Chinese American immigrant breast cancer survivors: a qualitative study using an expressive writing approach. Int J Behav Med 24:827–835
Wang L, Geng X, Ji L et al (2020) Treatment decision-making, family influences, and cultural influences of Chinese breast cancer survivors: a qualitative study using an expressive writing method. Support Care Cancer 28:3259–3266
Shah BB, Nieweglowski K, Corrigan PW (2022) Perceptions of difference and disdain on the self-stigma of mental illness. J Ment Health 31:22–28
Yuan JM, Zhang JE, Zheng MC, Bu XQ (2018) Stigma and its influencing factors among Chinese patients with stoma. Psychooncology 27:1565–1571
Lewis J, Mackenzie L (2022) Cognitive changes after breast cancer: a scoping review to identify problems encountered by women when returning to work. Disabil Rehabil 44:5310–5328
Clark DA, Beck AT (2010) Cognitive theory and therapy of anxiety and depression: convergence with neurobiological findings. Trends Cogn Sci 14:418–424
Ruiz-Rodriguez I, Hombrados-Mendieta I, Melguizo-Garin A, Martos-Mendez MJ (2022) The importance of social support, optimism and resilience on the quality of life of cancer patients. Front Psychol 13:833176
Diaz-Mandado O, Perianez JA (2021) An effective psychological intervention in reducing internalized stigma and improving recovery outcomes in people with severe mental illness. Psychiatry Res 295:113635
Mikal JP, Beckstrand MJ, Parks E, Oyenuga M, Odebunmi T, Okedele O, Uchino B, Horvath K (2020) Online social support among breast cancer patients: longitudinal changes to Facebook use following breast cancer diagnosis and transition off therapy. J Cancer Surviv 14:322–330
Jablotschkin M, Binkowski L, MarkovitsHoopii R, Weis J (2022) Benefits and challenges of cancer peer support groups: a systematic review of qualitative studies. Eur J Cancer Care (Engl) 31:e13700
Cubis L, Ownsworth T, Pinkham MB, Chambers S (2018) The social trajectory of brain tumor: a qualitative metasynthesis. Disabil Rehabil 40:1857–1869
Cubis L, Ownsworth T, Pinkham MB, Foote M, Green H, Chambers S (2023) “Hey, I’m still here!”: maintaining, managing and rebuilding social connections after brain tumour. Neuropsychol Rehabil 33:454–479
Cubis L, Ownsworth T, Pinkham MB, Foote M, Legg M, Chambers S (2019) The importance of staying connected: mediating and moderating effects of social group memberships on psychological well-being after brain tumor. Psychooncology 28:1537–1543
Acknowledgements
We would like to thank all the brain cancer survivors participating in this study for their willingness to reveal their experiences with frankness.
Funding
This study was supported by Science and technology Project of Nantong City, China, Grant Number: MS2023024.MS2023025.
Author information
Authors and Affiliations
Contributions
LYQ, ZJJ, and HJL wrote the main manuscript text and CX and YXN prepared the figures. FYY and ZYQ prepared the tables. ZXM and XXQ have contributed to the study design and preparation of the manuscript. All authors reviewed the manuscript.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Conflict of interest
The authors declare that they have no conflicts of interest.
Ethics statement
This study was performed in line with the principles of the Declaration of Helsinki. This study was approved by the local Hospital’s Ethics Committee (No. 2021-K051).
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Yanqing Li, Jiajia Zhang, and Jiali Hu are the first authors.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Li, Y., Zhang, J., Hu, J. et al. Stigma and related influencing factors in brain cancer patients: a cross-sectional study and parallel mediation analysis. Support Care Cancer 32, 522 (2024). https://doi.org/10.1007/s00520-024-08731-9
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00520-024-08731-9