Abstract
Background
During esophagectomy, laparoscopy can be used together with thoracoscopy, but it is not known whether a combined thoracoscopic–laparoscopic procedure is associated with fewer postoperative complications than open esophagectomy, and without compromising oncological outcome.
Methods
This was a longitudinal cohort study that included 185 esophageal cancer patients, including 72 who underwent combined thoracoscopic–laparoscopic esophagectomy (TLE), 34 who underwent thoracoscopic esophagectomy (TE), and 79 who underwent open esophagectomy (OE) between January 2002 and May 2010. The main outcome measures were postoperative respiratory and overall complications. The secondary outcome was 2-year relapse-free survival (RFS).
Results
Respiratory complications occurred in 9 patients who underwent TLE, 13 who underwent TE, and 31 who underwent OE. TLE was associated with fewer respiratory complications (TLE vs. OE: odds ratio [OR], 0.22; 95% confidence interval [CI], 0.09–0.53 and TE vs. OE: OR, 0.71; 95% CI 0.29–1.76). Overall complications occurred in 34 patients who underwent TLE, 20 who underwent TE, and 54 who underwent OE. TLE was associated with fewer overall complications (TLE vs. OE: OR, 0.47; 95% CI 0.23–0.94 and TE vs. OE: OR, 0.51; 95% CI 0.21–1.25). The 2-year RFS rates were similar among the three groups: 71.6% for TLE, 57.7% for TE, and 58.3% for OE (TLE vs. OE: hazard ratio, 0.65; 95% CI 0.35–1.20 and TE vs. OE: hazard ratio, 0.91; 95% CI 0.45–1.82).
Conclusion
Unlike TE, TLE was associated with fewer postoperative complications than was OE, with no compromise of 2-year RFS. A randomized controlled trial with longer follow-up is needed.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
In patients with esophageal cancer, minimally invasive esophagectomy (MIE) can be used to reduce surgical invasiveness, gain a better operative field, and lessen perioperative complications. MIE is believed to entail less blood loss and shorter hospital stays than conventional open esophagectomy (OE). The superiority of MIE over OE with regard to postoperative complications has been suggested by several meta-analyses [1–3] and comparative studies [4–7]. However, it is not clear whether MIE provides these benefits without compromising oncological outcome.
Furthermore, there is no consensus regarding the optimal method for MIE. The techniques used can be thoracoscopic, laparoscopic, or both, and the combined technique has been directly compared with the others only rarely [6, 8, 9]. Specifically, the additional benefit of laparoscopy is unclear.
We therefore studied whether incorporating laparoscopy into MIE for esophageal cancer could reduce the postoperative respiratory and overall complications without compromising 2-year relapse-free survival.
Patients and methods
Preoperative patient assessment and definition of procedures
This longitudinal cohort study was done at the Department of Surgery, Kyoto University Hospital, with data collected over more than 8 years. It was approved by the ethics committee at Kyoto University. All patients had detailed preoperative risk assessments based on clinical presentation, chest radiography, electrocardiography, and pulmonary function tests. Preoperative tumor staging was based on physical examination, radiologic examination (computed tomography and/or magnetic resonance imaging), upper gastrointestinal series, ultrasonography, and endoscopy.
We used three procedures: combined thoracoscopic–laparoscopic esophagectomy (TLE), thoracoscopic esophagectomy (TE), and open esophagectomy (OE). Through August 2005, all esophagectomies at our hospital were done with an open transthoracic approach (OE). In September 2005, we started using thoracoscopic procedures (TLE or TE) and have continued using these techniques. The indications for OE changed with the introduction of thoracoscopic procedures, and they differ from the indications for TLE or TE. Before thoracoscopic procedures were introduced, OE was indicated in patients with T1–T3 (TNM classification, 6th ed.) and technically resectable T4 tumors (those with invasion of adjacent structures) irrespective of lymph node metastasis, previous chemoradiation therapy, or previous esophageal resection. Starting in September 2005, TLE or TE was indicated only in those with T1–T3 tumors. OE was indicated only in the remaining patients: those with previous chemoradiation therapy, previous esophageal resection, or T4 tumor. Irrespective of the type of thoracic procedure, the surgeon’s preference determined whether a patient underwent laparotomy or laparoscopy.
Eligible patients for the analyses
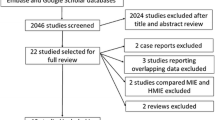
We reviewed the records of 243 patients who had histologically proven primary esophageal cancer and who underwent first esophagectomy between January 2002 and May 2010. To reduce imbalances in patients’ clinical characteristics between procedures, only data of patients with T1–T3 tumors, which is also the indication for TLE or TE, were eligible for the analyses. By that criterion 195 patients were eligible and the remaining 48 were excluded. Ten patients who underwent thoracotomy–laparoscopy also were excluded, and thus the remaining total was 185. The TLE group comprised 72 patients, the TE group 34, and the OE group 79 (Fig. 1).
The data were analyzed by intention-to-treat, i.e., any patient who required conversion from TLE to OE or TE because of intraoperative trauma was considered to belong to the TLE group.
Surgical procedure
The thoracoscopic approach was defined as thoracoscopic mobilization of the esophagus and regional lymphadenectomy without the use of minithoracotomy, as reported previously [10, 11]. For thoracoscopic mobilization, patients were placed in the left lateral decubitus position or the prone position. The regional lymph nodes removed were the mediastinal (paraesophageal, paratracheal, subcarinal, supradiaphragmatic, and para–recurrent-laryngeal-nerve) and perigastric nodes. In patients with an upper esophageal tumor or metastases to the para–recurrent-laryngeal-nerve lymph nodes, the cervical lymph nodes were also removed.
Subsequently, patients were placed in the supine position for the gastric mobilization to obtain complete en bloc resection with upper abdominal lymph nodes. The abdominal procedure was done either by laparoscopic (endoscopic or hand-assisted endoscopic) surgery, or by open laparotomy. In the laparoscopic approach, after the first port was inserted through the umbilicus and CO2 pneumoperitoneum at 8 mmHg was established, four operating ports were placed. The greater omentum, gastrosplenic ligament, and short gastric vessels were cut. The esophagus was dissected all around at the level of the hiatus and mobilized with preservation of the right gastroepiploic vessels. Then, laparotomy within 5 cm was done to remove the specimen. In the open approach, an upper abdominal midline incision was made. An incision was made on the left side of the neck, and then the prepared stomach was pulled up via the posterior mediastinal route, an intrathoracic route, or a retrosternal route, and a colon conduit was created through the antethoracic or retrosternal route.
The thoracotomy approach comprised open transthoracic esophageal mobilization using a three-incision technique as previously reported [12]. A right posterolateral thoracotomy was done, followed by laparoscopy or laparotomy for esophageal dissection and abdominal lymphadenectomy. Reconstruction was similar to that done with the thoracoscopic approach.
No patients underwent pyloroplasty, and no feeding jejunostomy tubes were placed.
Perioperative management
The procedures were done under a combination of epidural and general anesthesia. A double-lumen endotracheal tube was used for single-lung ventilation. At the beginning of the operation, 125 mg of methylprednisolone was administered intravenously to attenuate intraoperative surgical stress responses and to prevent postoperative complications [13]. Immediately after the operation, all patients were routinely admitted to the ICU and placed on mechanical ventilation overnight. The management of all the patients was in the same environment using intensive care, and the same principles of care were applied. After extubation on the next day, patients received respiratory physiotherapy to aid expectoration of any retained secretions. Bronchoscopic suction was done when necessary. For postoperative analgesia, epidural analgesia was preferred.
Histopathologic assessment
The pathological classifications of the primary tumor, the degree of lymph node involvement, and the presence of organ metastases were defined according to the TNM classification (6th ed.), and R classification was used to describe the extent of residual disease after esophagectomy (R0: no residual tumor, R1: microscopic residual tumor, R2: macroscopic residual tumor) [14].
Outcomes
The main outcomes of interest were respiratory and overall complications that occurred within 30 days of the operation. The secondary outcome was 2-year relapse-free survival (RFS). Respiratory complications were selected from complications higher than grade 2 according to the National Cancer Institute Common Terminology Criteria for Adverse Events (NCI-CTCAE) version 3.0 (adult respiratory distress syndrome, pneumonia, pleural effusion, atelectasis, bronchopulmonary hemorrhage, cough, hiccups, aspiration, pneumothorax, and respiratory tract fistulae [Supplementary Material 1]) because these were considered to be clinically important. Cases of pleural effusion and pneumothorax were included only if they appeared after withdrawal of the thoracic drainage tube. Cases of atelectasis were included only if they were confirmed by chest radiography or bronchoscopy.
Overall complications were, in addition to the respiratory complications described above, cardiac or liver dysfunction or failure, stroke, intestinal fistulae, anastomotic leakage, chylothorax, perforation of the conduit, anastomotic stenosis, ileus, wound infection, intraoperative trauma, intraoperative bleeding, and palsy of the recurrent laryngeal nerve (Supplementary Material 1). Information on these complications, and on death within 30 days of the operation, was extracted from medical records by two reviewers (Y. Kinjo and Y. Kataoka) who worked independently and were blinded to the surgical procedures.
Two-year RFS was ascertained only for the patients with R0. The duration used was the duration from the date of the surgery until the date of either death (due to any cause) or of the first recurrence confirmed by diagnostic imaging.
Statistics and survival analysis
Continuous variables were expressed as mean ± SD when normally distributed or as median and range when non-normally distributed. The three groups were compared with one-way ANOVA, Kruskal–Wallis test, or χ2 test, as appropriate. Logistic-regression models were used to compare the occurrence of postoperative complications between the groups. RFS curves were estimated by the Kaplan–Meier method, and differences between them were compared with the log-rank test. The Cox proportional-hazard model was used to compare the RFS among the three groups. Variables with a P < 0.20 in the bivariate analyses were included in the multivariate analyses. All P values < 0.05 were considered statistically significant. All analyses were done with STATA statistical software, ver. 11.0 (Stata Corp., College Station, TX, USA).
Results
Patient characteristics and surgical outcomes
The clinical and pathologic characteristics of the patients are given in Table 1. There were no significant differences in age, sex, body mass index, smoking history, or FEV1%. The prevalence of a history of neoadjuvant chemotherapy varied between groups: TLE > TE > OE. The mean preoperative serum albumin and the proportion of patients with squamous cell carcinoma were higher in the TLE group. There was no significant difference in pathological TNM staging between the groups.
The details of the surgical procedures are given in Table 2. There was no significant difference in the field of lymphadenectomy. No patient in the TLE or the TE group had intrathoracic anastomosis. Use of stomach conduit and use of hand-sewing were more common in the TLE group. For the thoracoscopic procedure, the prone position was used in 16 patients: 13 (18%) in the TLE group and 3 (9%) in the TE group.
The intraoperative and postoperative surgical outcomes are given in Table 3. The thoracic procedure took more time in the TLE group than in the TE and OE groups (308 vs. 264 vs. 268 min, P < 0.001), but TLE was done with less loss of blood (320 vs. 536 vs. 680 g, P < 0.001). The postoperative hospital stay, duration of epidural anesthesia, and length of oxygen therapy were shorter in the TLE group. There were no differences in residual tumor or in the duration of ICU stay.
Respiratory and overall complications
Respiratory complications occurred in 9 patients (13%) in the TLE group, 13 patients (38%) in the TE group, and 31 patients (39%) in the OE group (Table 3). Overall complications occurred in 34 patients (47%), 20 patients (58%), and 54 patients (68%), respectively. The proportions of patients who required reoperation were similar. One patient in the TLE group, three in the TE group, and three in the OE group had reoperations due to anastomotic leakage, and one patient in the TLE group had a reoperation due to a chylothorax. All patients in all groups survived longer than 30 days after the operation.
The details of postoperative complications within 30 days are given in Table 4. A total of 14 respiratory adverse events occurred in the TLE group, 21 occurred in the TE group, and 36 occurred in the OE group. For overall adverse events, the totals were 50, 42, and 81, respectively.
In the bivariate analyses, respiratory complications were associated with age, ASA-PS, history of smoking, pathological T stage, colon conduit, and with having undergone OE rather than TLE (Table 5). Respiratory complications were not associated with having undergone OE rather than TE. In the multivariate analyses, respiratory complications were associated with having undergone OE rather than TLE (adjusted odds ratio [AOR] = 0.22; 95% confidence interval [CI] 0.09–0.53; P = 0.001).
In the bivariate analyses, having at least one of the overall complications was associated with ASA-PS, history of smoking, pathological T stage, colon conduit, and with having undergone OE rather than TLE (Table 6). In the multivariate analyses, having undergone TLE was associated with a lower adjusted odds of having one or more of the overall complications (AOR = 0.47; 95% CI 0.23–0.94; P = 0.034).
Relapse-free survival
The median follow-up time was 26 months (range = 3–63) in the TLE group, 24 months (4–51) in the TE group, and 50 months (3–95) in the OE group. The 2-year RFS rates were 71.6%, 57.7%, and 58.3%, respectively. The RFS curve for TLE group was slightly higher than the curves for the other groups (Fig. 2; TLE vs. OE: P = 0.079; TE vs. OE: P = 0.845 by log-rank test). When compared with OE, neither TLE nor TE was associated with longer RFS (Table 7).
Discussion
Both TE and TLE were associated with acceptable midterm oncological outcomes, but only the TLE group had lower odds of postoperative respiratory and overall complications than the OE group. In comparison to OE, laparoscopy might result in more rapid recovery of bowel function, easier postoperative ambulation, and thus also easier expectoration of respiratory secretions. This is consistent with post-gastrectomy findings that laparoscopy results in less impaired pulmonary function [15] and fewer pulmonary complications [16] than do open procedures. In addition, thoracoscopic surgery can minimize damage to the chest wall, which will preserve lung and chest-wall compliance. It can also provide a better operative field and easier identification of the mediastinal structures, for more precise dissection.
Use of the prone position during thoracoscopy may promote hemostasis [10] and decrease lung injury. The mediastinum is exposed because bloody exudate flows out from the chest cavity by gravity, and thus does not conceal the operative field. The lung collapses because of the positive pressure pneumothorax, so lung retraction is not necessary. The overall result is less blood loss and fewer respiratory complications. The finding that TE alone was not associated with fewer postoperative complications indicates that the combination of laparoscopic and thoracoscopic surgery may synergistically reduce postoperative pain and restriction to breathing, resulting in fewer respiratory complications.
Three previous studies have compared the results of TLE, TE, and OE. The present results are consistent with the report in which the percentage of patients with postoperative pulmonary complications was significantly lower in the TLE group (6.7%) than in the other two groups (20% for TE, 30% for OE) [8]. The other two studies did not show such a benefit of TLE [6, 9]. This inconsistency between studies may be related to study designs: First, we used a relatively broad definition of “respiratory complication.” Second, the previous reports did not give details of the clinicopathological characteristics of the patients who underwent the three procedures, and likely confounders for respiratory complication such as age, history of smoking, and ASA-PS were not considered [17–19]. In contrast, our analyses included adjustments for likely confounders, which should provide stronger evidence of the superiority of TLE in terms of postoperative complications.
The patients who underwent TLE were less likely to have overall complications (Table 6) than were those who underwent OE (both bivariate and multivariate analyses). The only exception was palsy of the recurrent laryngeal nerve, which was more common in the TLE group than in the other groups. All cases of this complication were CTCAE grade 2, which required testing and follow-up but were not aggravated. In this context we note that the prone position was more frequently used during TLE than during TE. The prone position provides better visual control than does the left decubitus position. When patients are in the prone position the lymph nodes are more clearly seen, and therefore the nodes might have been more aggressively dissected from the recurrent nerve, which could account for the higher incidence of recurrent laryngeal nerve palsy in TLE group. This does not mitigate the advantage of TLE, but of course more attention should be given to the dissection of lymph nodes around the recurrent laryngeal nerve to minimize the risk of injury.
The advantages of TLE were not accompanied by any compromise in 2-year RFS. The Kaplan–Meier curve for RFS after TLE was the best of the three curves, although that might have been due to there being slightly more patients with N0-stage tumors in the TLE group. The survival advantage for TLE that was seen in the bivariate analysis was attenuated after adjustment for likely confounders. Thus, with regard to oncological outcome, we consider TLE and OE to be comparable, and we note that decisions to use the newer technique (TLE) therefore do not require any compromise with regard to that outcome. We are aware of no previous comparative studies in which RFS was evaluated. In two previous studies there were no differences in overall survival between TLE and OE [8, 9], although the numbers of patients in the TLE groups of those studies were relatively small (19 and 30 patients), so reasonable comparisons between techniques are difficult. The next question is whether TLE affects long-term survival, and this question requires further follow-up.
There are several limitations to our study. First, the 30-day mortality and in-hospital mortality were zero in this study and could not be used as main outcomes. We presume that the major reason for this was that patients were not included if they had undergone chemoradiation therapy or had a T4 tumor. Second, there were several imbalances in important clinical characteristics between the groups. For example, no patients in the TLE group underwent reconstruction with a colon conduit, which might have resulted in confounding. We tried to adjust for these imbalances by using multivariate analyses, but there could be residual confounding. However, in previous studies the type of reconstruction conduit (colon vs. stomach) did not affect the safety of esophagectomy [20, 21]. Third, our main outcomes are susceptible to bias. To minimize bias regarding the ascertainment of the main outcomes, the data reviewers were blinded to the surgical procedures. Finally, the duration of follow-up was limited. Still, the majority of recurrences develop within 1 year, and more than 90% of them develop by the third year after surgery [22, 23]. Thus, we believe that our follow-up period was long enough for comparing RFS among the groups.
We conclude that in patients with esophageal cancer, TLE, but not TE, was associated with fewer postoperative complications than OE, with no compromise of midterm RFS. These findings support the hypothesis that the combination of thoracoscopy with laparoscopy has a benefit greater than that of thoracoscopy alone. A randomized controlled trial with longer follow-up is needed.
Abbreviations
- ASA-PS:
-
American Society of Anesthesiologists Physical Status classification
- CI:
-
Confidence interval
- CTCAE:
-
Common Terminology Criteria for Adverse Events
- FEV1%:
-
Forced expiratory volume in 1 s as a percentage of the forced vital capacity
- MIE:
-
Minimally invasive esophagectomy
- OE:
-
Open esophagectomy
- OR:
-
Odds ratio
- RFS:
-
Relapse-free survival
- TNM:
-
Tumor Node Metastasis classification
References
Sgourakis G, Gockel I, Radtke A, Musholt TJ, Timm S, Rink A, Tsiamis A, Karaliotas C, Lang H (2010) Minimally invasive versus open esophagectomy: meta-analysis of outcomes. Dig Dis Sci 55:3031–3040
Nagpal K, Ahmed K, Vats A, Yakoub D, James D, Ashrafian H, Darzi A, Moorthy K, Athanasiou T (2010) Is minimally invasive surgery beneficial in the management of esophageal cancer? A meta-analysis. Surg Endosc 24:1621–1629
Biere SS, Cuesta MA, van der Peet DL (2009) Minimally invasive versus open esophagectomy for cancer: a systematic review and meta-analysis. Minerva Chir 64:121–133
Hamouda AH, Forshaw MJ, Tsigritis K, Jones GE, Noorani AS, Rohatgi A, Botha AJ (2010) Perioperative outcomes after transition from conventional to minimally invasive Ivor-Lewis esophagectomy in a specialized center. Surg Endosc 24:865–869
Pham TH, Perry KA, Dolan JP, Schipper P, Sukumar M, Sheppard BC, Hunter JG (2010) Comparison of perioperative outcomes after combined thoracoscopic-laparoscopic esophagectomy and open Ivor-Lewis esophagectomy. Am J Surg 199:594–598
Safranek PM, Cubitt J, Booth MI, Dehn TC (2010) Review of open and minimal access approaches to oesophagectomy for cancer. Br J Surg 97:1845–1853
Zingg U, McQuinn A, DiValentino D, Esterman AJ, Bessell JR, Thompson SK, Jamieson GG, Watson DI (2009) Minimally invasive versus open esophagectomy for patients with esophageal cancer. Ann Thorac Surg 87:911–919
Lee JM, Cheng JW, Lin MT, Huang PM, Chen JS, Lee YC (2011) Is there any benefit to incorporating a laparoscopic procedure into minimally invasive esophagectomy? the impact on perioperative results in patients with esophageal cancer. World J Surg 35(4):790–797
Smithers BM, Gotley DC, Martin I, Thomas JM (2007) Comparison of the outcomes between open and minimally invasive esophagectomy. Ann Surg 245:232–240
Noshiro H, Iwasaki H, Kobayashi K, Uchiyama A, Miyasaka Y, Masatsugu T, Koike K, Miyazaki K (2010) Lymphadenectomy along the left recurrent laryngeal nerve by a minimally invasive esophagectomy in the prone position for thoracic esophageal cancer. Surg Endosc 24:2965–2973
Itami A, Watanabe G, Tanaka E, Nakayama S, Fujimoto A, Kondo M, Nakau M, Okabe H, Satoh S, Sakai Y (2008) Multimedia article. Upper mediastinal lymph node dissection for esophageal cancer through a thoracoscopic approach. Surg Endosc 22:2741
Swanson SJ, Batirel HF, Bueno R, Jaklitsch MT, Lukanich JM, Allred E, Mentzer SJ, Sugarbaker DJ (2001) Transthoracic esophagectomy with radical mediastinal and abdominal lymph node dissection and cervical esophagogastrostomy for esophageal carcinoma. Ann Thorac Surg 72:1918–1924 discussion 1924-1915
Sato N, Koeda K, Ikeda K, Kimura Y, Aoki K, Iwaya T, Akiyama Y, Ishida K, Saito K, Endo S (2002) Randomized study of the benefits of preoperative corticosteroid administration on the postoperative morbidity and cytokine response in patients undergoing surgery for esophageal cancer. Ann Surg 236:184–190
Sobin LH, Wittekind C (2002) TNM classification of malignant tumours (UICC), 6th edn. Wiley-Liss, New York
Kitano S, Shiraishi N, Fujii K, Yasuda K, Inomata M, Adachi Y (2002) A randomized controlled trial comparing open vs laparoscopy-assisted distal gastrectomy for the treatment of early gastric cancer: an interim report. Surgery 131:S306–S311
Lee JH, Han HS (2005) A prospective randomized study comparing open vs laparoscopy-assisted distal gastrectomy in early gastric cancer: early results. Surg Endosc 19:168–173
Zingg U, Smithers BM, Gotley DC, Smith G, Aly A, Clough A, Esterman AJ, Jamieson GG, Watson DI (2011) Factors associated with postoperative pulmonary morbidity after esophagectomy for cancer. Ann Surg Oncol 18(5):1460–1468
Law S, Wong KH, Kwok KF, Chu KM, Wong J (2004) Predictive factors for postoperative pulmonary complications and mortality after esophagectomy for cancer. Ann Surg 240:791–800
Nagawa H, Kobori O, Muto T (1994) Prediction of pulmonary complications after transthoracic oesophagectomy. Br J Surg 81:860–862
Markar SR, Karthikesalingam A, Vyas S, Hashemi M, Winslet M (2011) Hand-sewn versus stapled oesophago-gastric anastomosis: systematic review and meta-analysis. J Gastrointest Surg 15(5):876–884
Mine S, Udagawa H, Tsutsumi K, Kinoshita Y, Ueno M, Ehara K, Haruta S (2009) Colon interposition after esophagectomy with extended lymphadenectomy for esophageal cancer. Ann Thorac Surg 88:1647–1653
Abate E, De Meester SR, Zehetner J, Oezcelik A, Ayazi S, Costales J, Banki F, Lipham JC, Hagen JA, De Meester TR (2010) Recurrence after esophagectomy for adenocarcinoma: defining optimal follow-up intervals and testing. J Am Coll Surg 210:428–435
Kunisaki C, Makino H, Takagawa R, Yamamoto N, Nagano Y, Fujii S, Kosaka T, Ono HA, Otsuka Y, Akiyama H, Ichikawa Y, Shimada H (2008) Surgical outcomes in esophageal cancer patients with tumor recurrence after curative esophagectomy. J Gastrointest Surg 12:802–810
Disclosures
Yousuke Kinjo, Noriaki Kurita, Fumiaki Nakamura, Hiroshi Okabe, Eiji Tanaka, Yoshiki Kataoka, Atsushi Itami, Yoshiharu Sakai, and Shunichi Fukuhara have no conflicts of interest or financial ties to disclose.
Author information
Authors and Affiliations
Corresponding author
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Kinjo, Y., Kurita, N., Nakamura, F. et al. Effectiveness of combined thoracoscopic–laparoscopic esophagectomy: comparison of postoperative complications and midterm oncological outcomes in patients with esophageal cancer. Surg Endosc 26, 381–390 (2012). https://doi.org/10.1007/s00464-011-1883-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-011-1883-y