Abstract
Objective
This prospective study aimed to predict the adequacy of free quadriceps tendon (QT) autograft length using simple anthropometric measures.
Materials and methods
One hundred and eighty-four consecutive patients who underwent knee high-resolution MRI were enrolled in this study. The QT and native anterior cruciate ligament (ACL) length were measured using the oblique sagittal section. The adequate free QT length was calculated using the native ACL length and 30 mm for femoral and tibial tunnels in each patient. A QT shorter than the calculated length was considered inadequate. Age, sex, height, weight, body mass index, thigh circumference, and activity score were used to predict the adequacy of QT length with regression analysis.
Results
There were 92 men and 92 women with a mean age of 34.1 ± 8.0 years (range 18–45). The mean QT and ACL lengths were 69.0 ± 8.8 mm (range 48.1–90.3 mm) and 35.6 ± 2.5 mm (range 29.2–42.6 mm), respectively. The QT and the ACL lengths were longer in men (p < 0.001 for both). Twenty-three men and 39 women (total: 62, 33.7%) had inadequate QT length for a free QT autograft, and 6 patients (3 males, 3 females, 3.3%) had inadequate QT length with the bone block technique. There was a weak positive correlation between QT length and height (p < 0.001), weight (p < 0.001), and activity score (p = 0.007). Height was the only independent variable that predicted the QT length adequacy (r2 = 0.051, p = 0.009) but ROC analysis showed that height did not have an ability to detect a subject with an inadequate QT length (AUC: 0.384, 95% CI 0.300–0.468).
Conclusions
Free QT autografts may be inadequate in one-third of the patients, while a QT autograft with a bone block is almost always sufficient. Inadequate free QT autograft is more common in women. Although QT length correlated with height, it cannot be used as an accurate diagnostic tool to identify patients with an inadequate QT autograft. Preoperative measurement of the ACL and QT lengths by MRI might be beneficial to decide whether QT is usable, especially when harvesting without a bone block.
Level of evidence
Level II, diagnostic, prospective cohort study.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
The effect of optimal graft selection on clinical outcomes and subsequent graft failure remains controversial in anterior cruciate ligament reconstruction (ACLR). Several grafts may be used in primary ACLR, including quadruple hamstring tendons, bone–patellar tendon–bone (BPTB), the quadriceps tendon (QT), allografts and synthetic grafts [1, 2]. Each of these graft options has its own advantage and disadvantages. Current evidence indicates that synthetic grafts and allografts have poor clinical outcomes and a higher complication rate compared to autografts [3,4,5]. Thus, many surgeons prefer autografts even in revision cases as the first graft choice.
The most popular grafts used in primary ACLR are the hamstring tendons and BPTB [1,2,3,4,5,6]. However, these grafts also have various disadvantages. BPTB graft increases the risk of patellar fracture, residual anterior knee pain, kneeling difficulty, patellar tendon rupture, and knee flexion contracture [2, 7]. Similarly, hamstring tendon harvesting may cause iatrogenic saphenous nerve injuries, hamstring muscle weakness, tunnel widening, a high residual laxity rate, and re-rupture, particularly with small-sized grafts less than 7 mm [2, 8, 9].
Conversely, QT autografts offer several advantages over hamstring and BPTB tendon autografts, such as a higher cross-sectional area and biomechanical properties similar to those of the native anterior cruciate ligament ACL [10,11,12]. The QT tendon harvesting technique was first described by Marshall et al. in 1979 [13]. However, this technique necessitated extensive incision, and the initial clinical results were not favorable. In the late 1990s, Fulkerson revised the technique and described a minimally invasive QT harvesting method with less donor site morbidity [14]. Subsequently, QT autografts gained popularity. It is suspected that using QT autografts will become widespread and override other options in standard practice [15,16,17]. Recent studies also demonstrated that the QT autograft is not inferior to other graft alternatives in terms of functional outcomes [1, 6, 18].
Despite these apparent advantages, QT autografts are not without complications or risks. One problem is that the tendon length might be inadequate, particularly when harvested as a free tendon autograft [19, 20]. Anatomical studies report that the QT length might be as short as 37.6 mm, far shorter than required for a proper ACLR [21]. Preoperative magnetic resonance imaging (MRI) can be used to measure QT length, but a standard MRI examination does not display the entire length of QT because the field of view (FOV) is usually only between 14 and 18 cm. Preoperative information about the QT autograft adequacy is useful in preventing intraoperative problems. A few studies previously have investigated the relationship between QT length and anthropometric measures. Although these studies reported a significant positive correlation between the person's height and QT length, no diagnostic threshold was determined [19, 20, 22].
It is hypothesized that simple anthropometric measures such as height, weight, and thigh circumference may be used to estimate free QT autograft adequacy. Therefore, the purpose of this study was to investigate the relationship between anthropometric measures and the QT length to provide a practical diagnostic guide into identify patients with inadequate free QT autograft lengths.
Materials and methods
Patients and study design
Patients who presented to the orthopedic outpatient clinic with knee symptoms and were referred to the radiology department for a knee MRI between December 2020 and February 2021 were enrolled in this prospective study. Skeletally mature patients between 18 and 45 years of age with a full range of knee motion and who required dominant-sided knee MRI were included. Patients with ACL rupture, QT pathologies, and patellofemoral disorders, patients with a history of previous knee surgery, and neuromuscular and chronic inflammatory diseases were excluded. The institutional review board approved the study protocol (approval date/issue: 09.12.2020/26-5), and the study was conducted in accordance with the Declaration of Helsinki and later amendments. All participants provided written informed consent for participation.
MRI protocol
The MRI examination was performed using a 16-channel knee coil with a 1.5-Tesla MRI device (GE Healthcare, Signa, Milwaukee, WI, USA). The imaging protocol included axial coronal and sagittal fat-saturated, proton-density-weighted (TR/TE: 3500/20, matrix: 320 × 192, FOV: 16 × 16, slice thickness: 4 mm); sagittal fast spin-echo, T1-weighted (TR/TE: 650/25, matrix: 320 × 192, FOV: 16 × 16, slice thickness: 4 mm). In addition to standard knee MRI, a high-resolution axial fast spin-echo, T1-weighted image was obtained (TR/TE: 550/20–21, matrix: 512 × 256, FOV: 32.6 × 21.2, slice thickness: 0.5 mm). The FOV (32 cm) in the additional examination included the tibial tubercle to the rectus femoris muscle belly to visualize the full length of the QT.
MRI measurements
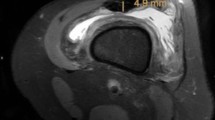
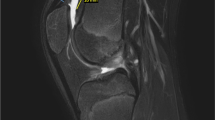
Since the QT follows an oblique course proximally and laterally, an oblique sagittal section was obtained by performing multiplanar reformation (MPR) over the high-resolution axial T1-weighted sections to determine the correct QT length. On the sagittal oblique T1-weighted images, the QT length was measured between the patella’s superior pole (patellar insertion site) and the musculotendinous junction of the rectus femoris muscle (Fig. 1). To measure the ACL length, oblique sagittal reformatted images parallel to the longitudinal axis of the ACL were created. The ACL length was measured between the midpoints of femoral and tibial attachment sites (Fig. 2).
Two independent observers measured all variables once on the workstation (Advantage Windows 4.2, GE Healthcare). Both observers were radiologists with more than 10 years of experience in musculoskeletal radiology. Interobserver reliability was calculated using the interclass correlation coefficient (ICC) and 95% confidence interval (CI). ICCs of 0.81–1.00, 0.61–0.80, 0.41–0.60, 0.21–0.40, and 0.00–0.20 were interpreted as excellent, good, moderate, fair, and poor, respectively [23]. Both measurements showed excellent agreement; ICC ranged between 0.952 and 0.997 (Table 1), and the mean was used for the analysis.
Calculation of sufficient free QT autograft length
Previous studies advocated that at least a 15 mm tendon is required in the bone tunnels for secure graft fixation and subsequent healing [19, 24, 25]. The minimum required QT autograft length was calculated by adding the native ACL length and 30 mm for the bone tunnels (15 mm for the tibial tunnel, 15 mm for the femoral tunnel). If the measured QT length was shorter than the calculated autograft length, the subject was assigned to the insufficient free tendon autograft group. If the length was equal or longer, the subject was assigned to the sufficient group (Fig. 3).
Anthropometric measurements
Anthropometric measurements included height, weight, and thigh circumference. Thigh circumference was measured at 10 cm above the superior pole of the patella while the patient was standing by the senior author using the same tape measure for standardization. Body mass index (BMI) was calculated by dividing weight (kg) by height squared (m2). The Tegner activity scale was used to grade the patients’ work and sporting activities.
Statistical analysis
Descriptive statistics for categorical variables were presented as frequencies and percentages, and continuous variables were presented as mean ± standard deviation and range. The Kolmogorov–Smirnov test was used for testing normality. Comparative analysis between independent groups was performed using the Student t test, Mann–Whitney U test, and Chi-square tests. Correlation between variables was assessed using Pearson’s and Spearman’s correlation tests. Multivariate logistic regression was used to identify independent risk factors associated with insufficient QT length. Odds ratio (OR) and 95% CI were used to quantify the associations with risk. Receiver-operating characteristic (ROC) curve analysis was used to assess the diagnostic performance of each variable. The sensitivity, specificity, cutoff value, and area under the ROC curve (AUC) were analyzed. A value of p < 0.05 was accepted as statistically significant.
Results
One hundred and eighty-four patients (92 male and 92 females, all ethnically Caucasian) with a mean age of 34.1 ± 8.0 years (range 18–45) were included in the analysis. Male subjects were younger (p = 0.012), taller (p < 0.001), heavier (p < 0.001), and more active (p < 0.001) than female subjects, but the BMI (p = 0.328) and thigh circumference (p = 0.072) were similar between sexes. The mean QT length was 69.0 ± 8.8 mm (range 48.1–90.3 mm), and the mean ACL length was 35.6 ± 2.5 mm (range 29.2–42.6 mm). The QT length and the ACL length were significantly longer in male subjects than in females (p < 0.001 for both). Patient demographics and anthropometric characteristics are shown in Table 2.
There was a weak positive correlation between QT length and height (p < 0.001), weight (p < 0.001), and activity score (p = 0.007), but there was no correlation with the other variables. Similarly, ACL length was positively correlated with height (p < 0.001), weight (p < 0.001), and activity score (p = 0.007). However, QT and ACL lengths did not correlate with each other (p = 0.118). The correlation coefficients are listed in Table 3.
According to the adequacy calculation, 23 males and 39 females (total: 62, 33.7%) had inadequate QT length for a free QT autograft. Females had insufficient QT length more frequently than males (p = 0.009). The sufficient QT length was significantly longer, ranging from 62.1 to 90.3 mm (mean 73.5 ± 6.4 mm), compared to the insufficient length, ranging from 48.1 to 68.3 mm (60.0 ± 5.0 mm) (p < 0.001). Subjects with sufficient QT length were taller (p < 0.001), but other variables showed no significant difference (Table 4). If the QT graft was harvested with a bone block (adding 15 mm), only 6 patients (3 males, 3 females, 3.3%) would remain who still have insufficient graft size.
Age, sex, height, weight, body mass index, thigh circumference, activity score, and ACL length were set as explanatory variables to create a regression model that predicts QT length. Testing for multicollinearity with variance inflation factor (VIF) among explanatory variables showed that weight (VIF = 103.9), height (VIF = 39.0), and BMI (VIF = 89.5) were significantly correlated; thus, weight (highest VIF) was excluded from the regression model to increase the precision of the estimate coefficients and the statistical power. After excluding weight, both tolerance and VIF values were acceptable (Tolerance > 0.20, VIF < 4) for the rest of the variables.
A stepwise backward logistic regression analysis revealed that height was the only independent variable that predicted adequacy of QT graft (r2 = 0.051, p = 0.009) (Table 5). Age, sex, weight, thigh circumference, and the activity score failed to show an association. A calibration plot was used to assess the accuracy of the predictive model, and it indicated that the model fit the quadratic data well (Fig. 4). ROC analysis showed that height could not detect a subject with an inadequate QT length (AUC: 0.384, 95% CI 0.300–0.468). The ROC curve diagram is presented in Fig. 5. A power calculation was performed to eliminate type II error in the logistic regression, and a post hoc power analysis using G*Power software (Version 3.1.9.6) showed a regression model power of 94.1%.
Discussion
This study attempted to predict the adequacy of free QT autograft length using simple anthropometric measures, namely age, sex, weight, BMI, thigh circumference, and activity score. The findings of this study showed that the height of the subject positively correlated with QT length, and regression analysis showed that it was an independent predictor of graft length adequacy. However, the discriminatory capacity was too weak to use as a diagnostic tool to identify patients with inadequate free QT autograft. The weak diagnostic capacity may be related to calculating the required tendon length using the subject’s native ACL length. The QT length increases as the height of the subjects increases; however, the native ACL length also increases with height. Thus, a short QT might still be adequate for a particular short subject with a short native ACL. Conversely, even if the free QT autograft in a tall person is long, inadequacy may arise because the native ACL is also long in the same person.
This study also found that the QT length was insufficient for a free QT autograft in approximately one-third of subjects. Almost half of the female subjects (42%), and a quarter of the male subjects (25%) had inadequate QT length. However, the inadequacy rate dropped to 3.3% if the tendon was harvested with a 15 mm bone block. Thus, surgeons who prefer free QT autografts should keep in mind that the tendon length may be short, particularly in female patients. The bone block harvesting technique described by Blauth increases the QT autograft length by 15 mm and an adequate graft can be achieved in almost all patients [26]. However, a notable complication of this technique is patellar fracture [27]. Fu et al. reported 3.5% intraoperative and 8.8% postoperative patellar fractures in a series of 67 patients who underwent QT autograft with bone block [28]. Apart from the bone block technique, the length of the QT autograft might also be extended by the elevation of periosteal flap (2 cm strip) from the surface of the patella. The periosteal part of the graft is folded in the middle and it provides approximately 1 cm of additional length [29].
The findings of the current study conflict with relevant studies in the literature. Xerogeanes et al. measured the QT length using three-dimensional MRI in 60 patients and found a moderate correlation between QT length and height [30]. They reported that 90% of patients had grafts longer than 70 mm, and 96% of patients had grafts > 60 mm. However, males and females were on average taller in this study than that in ours. They reported that the free QT graft was not below 60 mm in any subject taller than 167 cm. In contrast, 24 out of 66 patients with inadequate free QT grafts were taller than 167 cm in our study. Ukogewa et al. measured the QT length in 51 patients who underwent total knee prosthesis and found a positive correlation between height and QT length [20]. The QT was longer than 80 mm in 48 out of 51 patients, and it was less than 75 mm in only three female patients shorter than 160 cm. However, in both studies, the ACL length was not considered. Similarly, many authors suggested that a 65–70 mm tendon length is sufficient for an all-inside ACLR [31, 32]. However, we believe that these dogmatic values do not have meaning without knowing the native ACL size. The ACL length is subject to variations according to gender and height of the subject. In a recent systematic review, the mean ACL length ranged between 26.0 and 38.2 mm in 16 different studies [33]. In our study, the native ACL length was between 28.5 and 42.6 mm; subsequently a sufficient tendon length ranged between 58.5 mm and 72.6 mm.
Only one study supports our findings. Yamasaki et al. calculated the required tendon length by leaving a 30 mm margin for the femoral and tibial tunnels and reported that 37% of the patients had inadequate free QT [19]. Similarly, in our study, the tendon length was inadequate in 33% of the patients. The Yamasaki study was conducted in an Asian population, and the authors suggested that the tendon length might be shorter due to ethnic differences. Two cadaver studies have been conducted in Asian populations. In both, the average tendon length ranged from 60 to 65 mm [21, 34]. However, in studies conducted in Caucasian races, the tendon lengths were reported to be longer (70–99 mm) [10, 20, 29, 35, 36]. These findings suggest that the QT lengths may differ by ethnicity.
This study has both strengths and limitations. First, MRI was used for the measurements, which may not be an accurate technique compared to direct dissection measurements. However, a high correlation was detected in a previous study between the MRI measurements and the harvested QT length with a 0.1 mm precision [19]. The mean of the two ratings derived by the experienced radiologists was used to reduce measurement errors. The FOV was also wider than a standard knee MRI to visualize the entire QT length. Moreover, the QT and ACL lengths were measured through MPR since they follow an oblique course, and standard sagittal sections might underestimate the true longitudinal dimensions [37]. The current study focused on the QT length and did not evaluate the thickness and volume, which are also critical issues for the adequacy. But it is well known that the QT thickness and strength are quite sufficient and larger than other autograft options, as shown in several previous studies [22, 38,39,40,41,42]. To our knowledge, this study had the largest number of patients, and the high statistical power strengthened the results.
In conclusion, free QT autograft may be inadequate for one-third of the patients, but a QT autograft with a bone block is almost always sufficient. Inadequate free QT autografts are more common in women than men. Although the QT length correlated with height, it cannot be used as an accurate diagnostic tool to identify subjects with an inadequate QT autograft. Measuring the ACL and QT lengths by MRI might eliminate the problems during the surgery, if a free QT graft is chosen, especially in female patients.
Abbreviations
- ACL:
-
Anterior cruciate ligament
- ACLR:
-
Anterior cruciate ligament reconstruction
- AUC:
-
Area under the curve
- BMI:
-
Body mass index
- BPTB:
-
Bone–patellar tendon–bone
- CI:
-
Confidence interval
- FOV:
-
Field of view
- ICC:
-
Interclass correlation coefficient
- MPR:
-
Multiplanar reconstruction
- MRI:
-
Magnetic resonance imaging
- ROC:
-
Receiver-operating characteristics
- QT:
-
Quadriceps tendon
- TE:
-
Echo time
- TR:
-
Repetition time
- VIF:
-
Variance inflation factor
References
Duchman KR, Lynch TS, Spindler KP (2017) Graft selection in anterior cruciate ligament surgery: who gets what and why? Clin Sports Med 36(1):25–33. https://doi.org/10.1016/j.csm.2016.08.013
Lin KM, Boyle C, Marom N, Marx RG (2020) Graft selection in anterior cruciate ligament reconstruction. Sports Med Arthrosc Rev 28(2):41–48. https://doi.org/10.1097/JSA.0000000000000265
Goetz G, de Villiers C, Sadoghi P, Geiger-Gritsch S (2020) Allograft for anterior cruciate ligament reconstruction (ACLR): a systematic review and meta-analysis of long-term comparative effectiveness and safety. Results of a health technology assessment. Arthrosc Sports Med Rehabil 2(6):e873–e891. https://doi.org/10.1016/j.asmr.2020.07.003
Yang W, Huang X, Wang S, Wang H, Huang W, Shao Z (2020) The long-term outcomes of different grafts in anterior cruciate ligament reconstruction: a network meta-analysis. J Orthop Translat 26:16–30. https://doi.org/10.1016/j.jot.2020.03.008
Yang XG, Wang F, He X, Feng JT, Hu YC, Zhang H, Yang L, Hua K (2020) Network meta-analysis of knee outcomes following anterior cruciate ligament reconstruction with various types of tendon grafts. Int Orthop 44(2):365–380. https://doi.org/10.1007/s00264-019-04417-8
Mehran N, Moutzouros VB, Bedi A (2015) A review of current graft options for anterior cruciate ligament reconstruction. JBJS Rev 3(11):01874474-201511000–00003. https://doi.org/10.2106/JBJS.RVW.O.00009
Busam ML, Provencher MT, Bach BR Jr (2008) Complications of anterior cruciate ligament reconstruction with bone-patellar tendon-bone constructs: care and prevention. Am J Sports Med 36(2):379–394. https://doi.org/10.1177/0363546507313498
Hardy A, Casabianca L, Andrieu K, Baverel L, Noailles T, Junior French Arthroscopy Society (2017) Complications following harvesting of patellar tendon or hamstring tendon grafts for anterior cruciate ligament reconstruction: systematic review of literature. Orthop Traumatol Surg Res 103(8S):S245–S248. https://doi.org/10.1016/j.otsr.2017.09.002
Figueroa F, Figueroa D, Espregueira-Mendes J (2018) Hamstring autograft size importance in anterior cruciate ligament repair surgery. EFORT Open Rev 3(3):93–97. https://doi.org/10.1302/2058-5241.3.170038
Harris NL, Smith DA, Lamoreaux L, Purnell M (1997) Central quadriceps tendon for anterior cruciate ligament reconstruction. Part I: morphometric and biomechanical evaluation. Am J Sports Med 25(1):23–28. https://doi.org/10.1177/036354659702500105
Stäubli HU, Schatzmann L, Brunner P, Rincón L, Nolte LP (1999) Mechanical tensile properties of the quadriceps tendon and patellar ligament in young adults. Am J Sports Med 27(1):27–34. https://doi.org/10.1177/03635465990270011301
Offerhaus C, Albers M, Nagai K, Arner JW, Höher J, Musahl V, Fu FH (2018) Individualized anterior cruciate ligament graft matching: in vivo comparison of cross-sectional areas of hamstring, patellar, and quadriceps tendon grafts and ACL insertion area. Am J Sports Med 46(11):2646–2652. https://doi.org/10.1177/0363546518786032
Marshall JL, Warren RF, Wickiewicz TL, Reider B (1979) The anterior cruciate ligament: a technique of repair and reconstruction. Clin Orthop Relat Res. https://doi.org/10.1097/00003086-197909000-00014
Fulkerson JP, McKeon BP, Donahue BJ, Tarinelli DJ (1998) The central quadriceps tendon as a versatile graft alternative in anterior cruciate ligament reconstruction: techniques and recent observations. Tech Orthop 13:367–374
Middleton KK, Hamilton T, Irrgang JJ, Karlsson J, Harner CD, Fu FH (2014) Anatomic anterior cruciate ligament (ACL) reconstruction: a global perspective. Part 1. Knee Surg Sports Traumatol Arthrosc 22(7):1467–1482
Lubowitz JH (2016) Editorial commentary: quadriceps tendon autograft use for anterior cruciate ligament reconstruction predicted to increase. Arthroscopy 32(1):76–77
Winkler PW, Vivacqua T, Thomassen S, Lovse L, Lesniak BP, Getgood AMJ, Musahl V (2021) Quadriceps tendon autograft is becoming increasingly popular in revision ACL reconstruction. Knee Surg Sports Traumatol Arthrosc. https://doi.org/10.1007/s00167-021-06478-y (Epub ahead of print)
Riaz O, Aqil A, Mannan A, Hossain F, Ali M, Chakrabarty G, Radcliffe G (2018) Quadriceps tendon-bone or patellar tendon-bone autografts when reconstructing the anterior cruciate ligament: a meta-analysis. Clin J Sport Med 28(3):316–324. https://doi.org/10.1097/JSM.0000000000000451
Yamasaki S, Hashimoto Y, Han C, Nishino K, Hidaka N, Nakamura H (2020) Patients with a quadriceps tendon shorter than 60 mm require a patellar bone plug autograft in anterior cruciate ligament reconstruction. Knee Surg Sports Traumatol Arthrosc. https://doi.org/10.1007/s00167-020-06261-5 (Epub ahead of print)
Ugwuoke A, Syed F, El-Kawy S (2020) Predicting adequacy of free quadriceps tendon autograft, for primary and revision ACL reconstruction, from patients’ physical parameters. Knee Surg Sports Traumatol Arthrosc 28(2):448–453. https://doi.org/10.1007/s00167-019-05640-x
Tanpowpong T, Tanasansomboon T, Huanmanop T, Thamyongkit S, Jaruprat P, Inkaratana T (2019) Anatomical study of quadriceps tendon for anterior cruciate ligament reconstruction. Asian Biomed (Res Rev News) 13(5):179–183. https://doi.org/10.1515/abm-2019-0058
Zakko P, van Eck CF, Guenther D, Irrgang JJ, Fu FH (2017) Can we predict the size of frequently used autografts in ACL reconstruction? Knee Surg Sports Traumatol Arthrosc 25(12):3704–3710. https://doi.org/10.1007/s00167-015-3695-4
Koo TK, Li MY (2016) A guideline of selecting and reporting intraclass correlation coefficients for reliability research. J Chiropr Med 15(2):155–163
Zantop T, Ferretti M, Bell KM, Brucker PU, Gilbertson L, Fu FH (2008) Effect of tunnel-graft length on the biomechanics of anterior cruciate ligament-reconstructed knees: intra-articular study in a goat model. Am J Sports Med 36(11):2158–2166. https://doi.org/10.1177/0363546508320572
Qi L, Chang C, Jian L, Xin T, Gang Z (2011) Effect of varying the length of soft-tissue grafts in the tibial tunnel in a canine anterior cruciate ligament reconstruction model. Arthroscopy 27(6):825–833. https://doi.org/10.1016/j.arthro.2011.01.016
Blauth W (1984) Die zweizügelige Ersatzplastik des vorderen Kreuzbandes aus der Quadricepssehne [2-strip substitution-plasty of the anterior cruciate ligament with the quadriceps tendon]. Unfallheilkunde 87(2):45–51
Slone HS, Romine SE, Premkumar A, Xerogeanes JW (2015) Quadriceps tendon autograft for anterior cruciate ligament reconstruction: a comprehensive review of current literature and systematic review of clinical results. Arthroscopy 31(3):541–554. https://doi.org/10.1016/j.arthro.2014.11.010
Fu FH, Rabuck SJ, West RV, Tashman S, Irrgang JJ (2019) Patellar fractures after the harvest of a quadriceps tendon autograft with a bone block: a case series. Orthop J Sports Med 7(3):2325967119829051. https://doi.org/10.1177/2325967119829051
Fink C, Herbort M, Abermann E, Hoser C (2014) Minimally invasive harvest of a quadriceps tendon graft with or without a bone block. Arthrosc Tech 3(4):e509–e513. https://doi.org/10.1016/j.eats.2014.06.003
Xerogeanes JW, Mitchell PM, Karasev PA, Kolesov IA, Romine SE (2014) Anatomic and morphological evaluation of the quadriceps tendon using 3-dimensional magnetic resonance imaging reconstruction: applications for anterior cruciate ligament autograft choice and procurement. Am J Sports Med 41(10):2392–2399. https://doi.org/10.1177/0363546513496626
Slone HS, Ashford WB, Xerogeanes JW (2016) Minimally invasive quadriceps tendon harvest and graft preparation for all-inside anterior cruciate ligament reconstruction. Arthrosc Tech 5(5):e1049–e1056. https://doi.org/10.1016/j.eats.2016.05.012
Crall TS, Gilmer BB (2015) Anatomic all-inside anterior cruciate ligament reconstruction using quadriceps tendon autograft. Arthrosc Tech 4(6):e841–e845. https://doi.org/10.1016/j.eats.2015.08.004
Cone SG, Howe D, Fisher MB (2019) Size and shape of the human anterior cruciate ligament and the impact of sex and skeletal growth: a systematic review. JBJS Rev 7(6):e8. https://doi.org/10.2106/JBJS.RVW.18.00145
Hijazi MM, Khan MA, Altaf FMN, Ahmed MR, Alkhushi AG, Sakran AMEA (2015) Quadriceps tendon and patellar ligament; a morphometric study. Professional Med J 22(9):1192–1195. https://doi.org/10.17957/TPMJ/15.2759
Krebs N, Yaish A, O’Neill N (2019) Anatomic evaluation of the quadriceps tendon in cadaveric specimens: application for anterior cruciate ligament reconstruction graft choice. Spartan Med Res J 4(1):7961
Lippe J, Armstrong A, Fulkerson JP (2012) Anatomic guidelines for harvesting a quadriceps free tendon autograft for anterior cruciate ligament reconstruction. Arthroscopy 28(7):980–984. https://doi.org/10.1016/j.arthro.2012.01.002
Staeubli HU, Bollmann C, Kreutz R, Becker W, Rauschning W (1999) Quantification of intact quadriceps tendon, quadriceps tendon insertion, and suprapatellar fat pad: MR arthrography, anatomy, and cryosections in the sagittal plane. AJR Am J Roentgenol 173(3):691–698. https://doi.org/10.2214/ajr.173.3.10470905
Kupczik F, Schiavon MEG, Sbrissia B, Fávaro RC, Valério R (2013) ACL ideal graft: MRI correlation between ACL and hamstrings. PT and QT Rev Bras Ortop 48(5):441–447. https://doi.org/10.1016/j.rboe.2012.11.002
Camarda L, Grassedonio E, Albano D, Galia M, Midiri M, D’Arienzo M (2018) MRI evaluation to predict tendon size for knee ligament reconstruction. Muscles Ligaments Tendons J 7(3):478–484. https://doi.org/10.11138/mltj/2017.7.3.478
Dargel J, Schmidt-Wiethoff R, Schneider T, Brüggemann GP, Koebke J (2006) Biomechanical testing of quadriceps tendon-patellar bone grafts: an alternative graft source for press-fit anterior cruciate ligament reconstruction? Arch Orthop Trauma Surg 126(4):265–270. https://doi.org/10.1007/s00402-005-0048-7
Barié A, Sprinckstub T, Huber J, Jaber A (2020) Quadriceps tendon vs. patellar tendon autograft for ACL reconstruction using a hardware-free press-fit fixation technique: comparable stability, function and return-to-sport level but less donor site morbidity in athletes after 10 years. Arch Orthop Trauma Surg 140(10):1465–1474. https://doi.org/10.1007/s00402-020-03508-1
Horstmann H, Petri M, Tegtbur U, Felmet G, Krettek C, Jagodzinski M (2021) Quadriceps and hamstring tendon autografts in ACL reconstruction yield comparably good results in a prospective, randomized controlled trial. Arch Orthop Trauma Surg. https://doi.org/10.1007/s00402-021-03862-8
Acknowledgements
We would like to thank Editage (www.editage.com) for English language editing.
Funding
No funds have been received for this study.
Author information
Authors and Affiliations
Contributions
Study conception and design: OK, YY, and TE; acquisition of data: FY, TE, ET, and YY; analysis and interpretation of data: LS, YY, FY, and OK; drafting of the manuscript: YY, TE, OK, LS, and FY; critical revision: OK, YY, TE, LS, and FY (initials of authors’ names).
Corresponding author
Ethics declarations
Conflict of interest
The authors have no conflict of interest to declare.
Ethical approval
Institutional Review Board approved the study protocol (Date/Issue: 09.12.2020/26-5).
Informed consent
Written informed consent was provided by the participants.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Yuksel, Y., Kose, O., Torun, E. et al. Estimating the adequacy of the free quadriceps tendon autograft length using anthropometric measures in anterior cruciate ligament reconstruction. Arch Orthop Trauma Surg 142, 2001–2010 (2022). https://doi.org/10.1007/s00402-021-04197-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00402-021-04197-0