Abstract
Introduction
The implementation of 3D-navigation in the operating theater is reported to be complex, time consuming, and radiation intense. This prospective single-center cohort study was performed to objectify these assumptions by determining navigation-related learning curves in lumbar single-level posterior fusion procedures using 3D-fluoroscopy for real-time image-guided pedicle screw (PS) insertions.
Materials and methods
From August 2011 through July 2016, a total of 320 navigated PSs were inserted during 80 lumbar single-level posterior fusion procedures by a single surgeon without any prior experience in image-guided surgery. PS misplacements, navigation-related pre- and intraoperative time demand, and procedural 3D-radiation dose (dose-length-product, DLP) were prospectively recorded and congregated in 16 subgroups of five consecutive procedures to evaluate improving PS insertion accuracy, decreasing navigation-related time demand, and reduction of 3D-radiation dose.
Results
After PS insertion and intraoperative O-arm control scanning, 11 PS modifications were performed sporadically without showing “learning curve dependencies” (PS insertion accuracies in subgroups 96.6 ± 6.3%). Average navigation-related pre-surgical time from patient positioning on the operating table to skin incision decreased from 61 ± 6 min (subgroup 1) to 28 ± 2 min (subgroup 16, p < 0.00001). Average 3D-radiation dose per surgery declined from 919 ± 225 mGycm (subgroup 1) to 66 ± 4 mGycm (subgroup 16, p < 0.0001).
Conclusions
In newly inaugurated O-arm based image-guidance, lumbar PS insertions can be performed at constantly high accuracy, even without prior experience in navigated techniques. Navigation-related time demand decreases considerably due to accelerating workflow preceding skin incision. Procedural 3D-radiation dose is reducible to a fraction (13.2%) of a lumbar diagnostic non-contrast-enhanced computed tomography scan’s radiation dose.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Originating from spinal plate osteosynthesis, pedicle screw (PS)-based posterior stabilization systems have been successfully applied for an array of indications after the prototype “fixateur interne” had been presented in 1984 [1, 2]. During more than three decades of wide-spread use all over the world, PS insertion procedures have become increasingly sophisticated, when computer navigation started to interlace with the original surgical approach. These first steps in image-guided spine surgery were arduous and technically complex, so that acceptance was low among spine surgeons. But the idea of increased procedural safety at low radiation doses even in anatomically challenging spinal regions forced both, industry and therapists, into a rapid evolution of innovative computer navigation techniques. Although still being time consuming and technically demanding, advantages of today’s navigated procedures cannot be neglected. Non-navigated PS insertion techniques show malposition rates beyond the 10%-threshold [3,4,5,6,7,8], and reoperation rates of about 5% [9], even in the hands of experienced surgeons. In navigated procedures, however, reoperation rates are reported to be 0% [10,11,12], with PS placement accuracies commonly surpassing those of non-navigated techniques [3,4,5,6, 11].
Among the diversity of computer-assisted surgical devices on the market, O-arm navigation has evolved as very promising appliance concerning imaging quality and accuracy [7, 13, 14]. Nevertheless, these modern technical aids are expensive and usually not reimbursed by health care systems. Critics furthermore emphasize higher irradiation doses for patients and personnel during computer-assisted spinal procedures, and complain about time-consuming navigational steps that prolong surgeries. But these issues are not immutable problems that have to be tolerated, when computer-assisted surgery is implemented in the operating room. They are rather subjected to learning processes ending up in maximized accuracy and safety for the patient at acceptable time demand and irradiation dose.
This prospective study was performed to investigate learning curve effects on accuracy, navigation-associated time demand, and radiation dose in O-arm based navigation-assisted PS instrumentation procedures. To limit confounding factors that might arise from the number of instrumented vertebrae, anatomical peculiarities of various spinal sections, or different experience levels of participating surgeons, observations are restricted to lumbar single-level posterior fusion procedures performed during a 5-year period by a single surgeon who had never used image guidance before.
Materials and methods
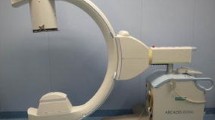
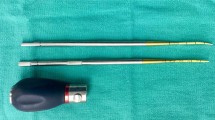
All navigated lumbar single-level posterior fusion procedures conducted by the author from August 2011 through July 2016 were included in this study. Procedures were standardized according to a pre-established study protocol utilizing navigation unit plus O-arm (StealthStation S7 Surgical Navigation System, O-arm®, Surgical Imaging System, Medtronic Sofamor Danek, Memphis, TN, USA). Prior to surgery, patients gave written informed consent after having received information about the use of O-arm and navigation unit for 3D-image-guided PS instrumentation and post-instrumentation screw position control. During surgery, patients were under general anesthesia in prone position on a radiolucent carbon fiber-operating table. The O-arm was adjusted to the surgical site for two imaging (anteroposterior and lateral view) and one parking position. These three standard settings were digitally stored for reliable reproduction of 2D-fluoroscopy and 3D-imaging during surgery. After skin disinfection and sterile draping of patient and O-arm, surgery started with skin incision, sub-periosteal preparation of spinous processes and vertebral arcs, and navigation reference clamp fixation to a spinous process in the caudad end of the surgical field. During the initial scan for navigational data acquisition, patients were not ventilated to prevent poor image quality due to trunk movements. Scan data were transformed for multiplanar reformations and transferred to the navigation unit. With the combination of navigation work station, infra-red camera, special surgical navigated tools (blunt probe, awl), and image-guidance software, real-time tool tracking was possible on the navigation unit’s monitor in 2D-sectional images (coronal, transaxial, sagittal orientation) after navigated tools had been referenced. PS beds were prepared using a navigated awl and probe. With the navigated probe, screw diameters and lengths were determined by calibrated virtual display on the StealthStation monitor. For PS application, a non-navigated screwdriver was used after non-navigated thread cutting.
Evaluation of PS insertion accuracy
For controlling PS positions, a second 3D-fluoroscopy scan was performed after spinal instrumentation to visualize screw positions in the three two-dimensional views (transaxial, sagittal, and coronal orientation). Initial scan parameters could optionally be changed. Screw positions were modified in case of insufficient vertebral anchorage jeopardizing the instrumentation’s stability (due to extrapedicular/extravertebral screw positions or suboptimal insertion depth), or if anatomical structures (facet joints, neural structures in the spinal or nerve root canal, retroperitoneal vessels) were at risk of harmful violation. These screw modifications were recorded post-surgically and categorized into major (concerning a screw’s vertebral starting point, its trajectory, or replacement due to suboptimal screw size) and minor modifications (mere alterations of a screw’s vertebral insertion depth after control scanning) for accuracy evaluation. Only in case of major modifications, another 3D-fluoroscopic control scan was conducted.
Evaluation of navigation-associated time demand
In image-guided surgery, several procedural steps are additionally performed, or conducted in a modified way compared to the conventional surgical approach. For determining navigation-associated time requirements, durations of navigation-associated pre-skin-incision periods (including prone positioning of anesthetized patients, O-arm adjustment, finding imaging and parking gantry-positions, skin disinfection, and sterile draping of patient and O-arm) and post-skin-incision periods (i.e., navigation-related interruptions of the actual surgical workflow, including 3D-fluoroscopy scanning, dataset processing for visualization, plus the time the surgical team needed for leaving and re-entering the room during scans) were separately recorded and evaluated as total, pre-, and post-skin-incisional navigation-associated time demands.
Evaluation of radiation dose
For every 3D-fluoroscopy scan (initial and control scans), a standard or high-density (HD) scan mode had to be selected affecting image resolution, radiation dose, and scanning time (120 kVp, 156.4–596.0 mAs, 13, respectively, 25 s). Four different preset 3D-radiation dose programs could additionally be chosen, e.g., adapted to the patient’s body mass index (Table 1). The cylindrical scan field with 16 cm length could be shortened in cephalad-caudad direction to cover only a limited number of segments (collimated scan). Radiation dose of 3D fluoroscopy (dose-length-product, DLP) was calculated by the O-arm software and recorded for evaluation, post-operatively.
Statistical analysis and evaluation of learning curves
Comparative data were summarized in consecutive subgroups of five patients. Values were expressed as mean and standard deviation of the mean. Student’s t test was used for comparison of continuous, and Fisher’s exact test for categorical variables. Significance was set at p < 0.05. Learning curve effects were assumed, if average data in consecutive subgroups showed decreasing values for “malposition rate”, “navigation-associated time requirement”, or “radiation dose”, with significant differences between the first and last subgroup. Analyses were conducted with SPSS 15.0.1 for Windows (SPSS Inc, Chicago, IL).
For this observational study, the STROBE statement was followed.
Results
From August 2011 to July 2016, 80 patients underwent lumbar single-level posterior fusion using spinal 3D-fluoroscopy-based navigation. Baseline conditions and underlying diagnoses are given in Table 2 (see also Electronic Supplementary Material). Intraoperative data acquisition for navigation was successfully performed in all cases. A total of 320 PSs (diameters 5.5–8.5 mm, lengths 45–65 mm) were inserted in vertebral levels L1–L6 (Fig. 1). The number of control scans was 83 in 80 surgeries.
Accuracy
Eleven screws were modified (3.4%) to address suboptimal insertion depth (minor modifications, n = 8), or to remedy impending violation of anatomical structures [major modifications, n = 3, performed for screw penetration into a nerve root canal (n = 1), extravertebral screw position (n = 1), or medial pedicle wall encroachment (n = 1)] indicating an overall accuracy of 96.6% (Fig. 2). All major modifications were performed in the L5-level. Excluding minor modifications from calculations, the mean accuracy in subgroups was 99.1 ± 2.6%.
Pedicle screw insertion accuracy during 80 image-guided lumbar single-level posterior fusion procedures in 16 subgroups of five patients, each. Individual accuracies of every single procedure, mean values and standard deviation of subgroups are listed under columns. Values are given in percent. SD standard deviation
Navigation-associated time demand
The average pre-surgical preparation time from patient positioning to skin incision significantly decreased from 61 ± 6 min in the first to 28 ± 2 min in the last subgroup of five patients (Fig. 3, p < 0.00001). Navigation-related procedural interruptions for initial and post-instrumentation 3D-fluoroscopy took 2.8 ± 0.3 min in the overall collective without significant differences between subgroups (p = 1.0).
Decreasing average navigation-associated preparation time during 80 image-guided lumbar single-level posterior fusion procedures in 16 subgroups of five patients, each. Individual preparation time of every single procedure, mean values and standard deviation of subgroups are listed under columns. Unit of values is minutes. SD standard deviation
Radiation dose
The first 17 individuals were operated on with an average 3D-radiation dose of 1014 ± 241 mGycm. They all had at least one HD scan, either for initial data acquisition, for PS control, or for both modalities. After 26 procedures, standard scans were performed, exclusively. This was the preferred scan mode in the overall collective (84.7%), providing high resolution imaging and high accuracy in lumbar spinal navigation. After the introduction of collimated scans, 3D-radiation dose considerably decreased to an average of 66 ± 4 mGycm in the last subgroup (Fig. 4, p < 0.0001).
Reduction of 3D-radiation dose during 80 image-guided lumbar single-level posterior fusion procedures displayed as average dose-length-products (DLP) in 16 subgroups of five consecutive procedures. Individual total 3D-radiation dose (DLP) of single surgeries, mean DLP and standard deviation of subgroups are listed under columns. Unit of values is mGycm. DLP Dose-length-product, mGycm milligray-centimeter, SD standard deviation
Learning curves (Table 3)
During the study period, accuracy was constantly high without notable learning curve effects (p = 1.0, Fig. 5a).
a, b, c In 80 image-guided lumbar single-level posterior fusion procedures, pedicle screw insertion accuracy was constant without detectable learning curve effects (a). A linear decrease in navigation-associated preparation time was found (b). For the total intraoperative 3D-radiation dose, an asymptotic convergence approximating the 50 mGycm baseline could be detected (c). DLP Dose-length-product, mGycm milligray-centimeter
A linear decrease in navigation-related time demand was detected revealing a learning curve effect for navigation-associated pre-surgical preparation time (p < 0.00001, Fig. 5b), but not for navigation-related interruptions during surgeries (p = 1.0).
An asymptotic decrease of procedural 3D-radiation doses from nearly 1400 mGycm to less than 70 mGycm (p < 0.0001, Fig. 5c) delineated the learning curve in radiation control.
Discussion
Investigations were restricted to posterior single-level fusion procedures of the lumbar spine to keep the study collective as homogenous as possible. All surgeries were performed by the author in the same medical center. These prerequisite helped to exclude heterogeneities resulting from anatomical peculiarities of different spinal sections, from differences in various surgeons’ skills, and from alternating surgical teams.
Numerous studies have documented the advantages of navigation for thoracic and lumbosacral PS insertions [3,4,5,6, 11, 13, 15,16,17,18,19]. Hence, most of today’s spine surgeons still hold on to non-navigated techniques for reasons such as tradition, acceptable accuracy of established techniques, lower costs, less time consumption [15, 20], less technical problems [15] and less radiation exposure than in computer-assisted surgery.
This study’s intention was to evaluate the gravity of some of these arguments by determining the impact of learning curve effects on accuracy, navigation-associated time requirements, and radiation exposure when a surgeon starts to perform navigated PS instrumentations.
In lumbar PS applications, O-arm image-guided PS insertion accuracy was constantly high (96.6 ± 6.3%) without showing dependencies on learning curve effects. This seems to be advantageous compared to non-navigated PS insertion techniques that were reported to have malposition rates of more than 10%, even in experienced hands [3,4,5,6,7,8]. During the first 104 navigated PS insertions, not even minor screw modifications (e.g., slight corrections of screw insertion depths) had to be performed. Sclafani et al. compared the accuracy of O-arm navigated versus C-arm navigated PSs in cadaveric adult torsos and similarly found constantly high accuracy rates with distinct learning curve effects for insertion time in O-arm navigation [21]. Our overall modification rate including minor modifications was 3.4%, which is comparable to our data on modification rates in 1547 navigated PSs of spinal levels T10-S1 [22]. All major modifications (n = 3) concerned the L5-level (100%, trajectory errors). In 1651 navigated thoracolumbosacral PSs, Rivkin et al. similarly found misplacements predominantly in the L5-level, but identified them as anterolateral (“tip out”) perforations (insertion depth errors) [23].
Contrarily to an absence of accuracy improvement, a linear decrease of pre-surgical navigation-associated time demand could be detected in the current study from 61 ± 6 min in the first group of five patients to a threshold of 28 min on average after 65 navigated procedures (Table 3), which is 45.9% of the initial duration (p < 0.00001). In a recent study, we analogously determined this time span in 100 non-navigated C-arm-based spinal surgeries under identical conditions (same anesthesiologists, same operating room personnel, same surgeon) and found an average duration of 30.6 ± 8.3 min [24]. Adding navigation-related procedural interruptions (2.8 ± 0.3 min) to the final average preparation-time result of 28 ± 2 min, similar durations are obtained in navigated and non-navigated procedures (30.8 versus 30.6 min). This shows that a relevant time-loss during navigational steps in image-guided lumbar single-level PS instrumentation procedures can be compensated with the experience of a limited number of cases, although navigation-related workflow initially is considerably time consuming. Of course, we also gained experience using O-arm image-guidance in posterior spinal fusion procedures of more than one level and in sections different from the lumbar spine, which helped to improve our handling with this new kind of equipment. In the author’s overall history of navigated spinal PS instrumentations, a pre-surgical duration of less than 30 min was reached for the first time after 141 procedures, showing a similar, but slower pace of the overall learning curve. Various studies could furthermore identify a decrease in operative time using navigated techniques for posterior spinal fusion [25,26,27]. These facts question higher time requirements in navigated surgeries compared to non-navigated procedures after having surmounted the learning curve, and accentuate the potential of training effects.
Most considerable learning curve results were observed in radiation control. As 2D-fluoroscopy was only used for finding imaging positions and documenting final surgical results, learning curve considerations had been confined to 3D-radiation dose data. Between the first and last subgroup of five cases, 3D-radiation dose could be reduced from an average procedural DLP of 919 ± 225 to 66 ± 4 mGycm (Table 3), which is 7.2% of the initial average DLP (p < 0.0001) and 13.2% of the DLP recommended for a diagnostic lumbar non-contrast-enhanced CT scan [24]. These improvements result from considerations concerning basic requirements for acceptable image quality. Initially, HD scans were performed with preference to attain maximum image resolution for navigation. As accuracy was not a problem at all, standard scans were increasingly performed, instead. This implicated a 34.5% dose reduction per scan. Another factor concerned preset dose programs that provided standardized device settings for body size categories “S”, “M”, “L”, and “XL”. Bigger individuals were to be scanned at higher energetic radiation levels to obtain a resolution clear enough to work with. As we stepwise reduced the mAs (milliampere second)-product by switching preset O-arm programs to settings stored for smaller individuals, we did not find considerable deterioration in resolution, but a radiation dose reduction of 20.0–37.5% per step. Relevant image resolution deterioration resulted as soon as X-ray tube voltage was additionally reduced. A study on saving radiation exposure during O-arm scans similarly showed that radiation dose can be reduced 5–13 times by scanning at lowered peak kilovoltage- and mAs-product-levels without relevant negative impact on image quality regarding information required for spinal navigation [28]. The third approach to decrease radiation dose was a radical scan field collimation to the two vertebrae to be instrumented with PSs. This modification to the initial procedure was the most effective step to control patients’ radiation exposure. By restricting the scan field length to two instead of usually five vertebrae, theoretically 60% of 3D-radiation dose can be saved. The latest modification was to perform O-arm scans with preset programs for body regions different from the “lumbar spine/pelvis” section (120 kV, 128–600 mAs, 25–100 mA), e.g., “head” programs (120 kV, 100–240 mAs, 20–40 mA). This was conducted in combination with all the aforementioned modifications only in the 14th group of five patients. However, relevant positive effects on 3D-radiation dose control were not noted with this proceeding, thus we decided to return to the “lumbar spine/pelvis protocol”.
References
Roy-Camille R, Saillant G, Mazel C (1986) Plating of thoracic, thoracolumbar, and lumbar injuries with pedicle screw plates. Orthop Clin North Am 17:147–159
Dick W, Kluger P, Magerl F, Woersdörfer O, Zäch G (1985) A new device for internal fixation of thoracolumbar and lumbar spine fractures: the ‘fixateur interne’. Paraplegia 23(4):225–232
Merloz P, Tonetti J, Pittet L, Coulomb M, Lavalleé S, Sautot P (1998) Pedicle screw placement using image guided techniques. Clin Orthop Relat Res 354:39–48
Merloz P, Troccaz J, Vouaillat H, Vasile C, Tonetti J, Eid A, Plaweski S (2007) Fluoroscopy-based navigation system in spine surgery. Proc Inst Mech Eng H 221(7):813–820. https://doi.org/10.1243/09544119JEIM268
Kosmopoulos V, Schizas C (2007) Pedicle screw placement accuracy: a metaanalysis. Spine 32:E111–E120. https://doi.org/10.1097/01.brs.0000254048.79024.8b
Laine T, Lund T, Ylikoski M, Lohikoski J, Schlenzka D (2000) Accuracy of pedicle screw insertion with and without computer assistance: a randomized controlled clinical study in 100 consecutive patients. Eur Spine J 9:235–240
Shin MH, Hur JW, Ryu KS, Park CK (2015) Prospective comparison study between the fluoroscopy-guided and navigation coupled with O-arm-guided pedicle screw placement in the thoracic and lumbosacral spines. J Spinal Disord Tech 28(6):E347–E351. https://doi.org/10.1097/BSD.0b013e31829047a7
Waschke A, Walter J, Duenisch P, Reichart R, Kalff R, Ewald C (2013) CT-navigation versus fluoroscopy-guided placement of pedicle screws at the thoracolumbar spine: single center experience of 4500 screws. Eur Spine J 22:654–660. https://doi.org/10.1007/s00586-012-2509-3
Zdichavsky M, Blauth M, Knop C, Lotz J, Krettek C, Bastian L (2004) Accuracy of pedicle screw placement in thoracic spine fractures. Part II: A retrospective analysis of 278 pedicle screws using computed tomographic scans. Eur J Trauma 30:241–247
Zausinger S, Scheder B, Uhl E, Heigl T, Morhard D, Tonn JC (2009) Intraoperative computed tomography with integrated navigation system in spinal stabilizations. Spine 34(26):2919–2926. https://doi.org/10.1097/BRS.0b013e3181b77b19
Amiot LP, Lang K, Putzier M, Zippel H, Labelle H (2000) Comparative results between conventional and computer-assisted pedicle screw installation in the thoracic, lumbar, and sacral spine. Spine 25(5):606–614
Mathew JE, Mok K, Goulet B (2013) Pedicle violation and navigational errors in pedicle screw insertion using the intraoperative O-arm: a preliminary report. Int J Spine Surg 7:e88–e94. https://doi.org/10.1016/j.ijsp.2013.06.002
Tian NF, Xu HZ (2009) Image-guided pedicle screw insertion accuracy: a meta-analysis. Int Orthop 33:895–903. https://doi.org/10.1007/s00264-009-0792-3
Van de Kelft E, Costa F, Van der Planken D, Schils F (2012) A prospective multicenter registry on the accuracy of pedicle screw placement in the thoracic, lumbar, and sacral levels with the use of the O-arm imaging system and StealthStation Navigation. Spine 37(25):E1580–E1587. https://doi.org/10.1097/BRS.0b013e318271b1fa
Laine T, Schlenzka D, Mäkitalo K, Tallroth K, Nolte LP, Visarius H (1997) Improved accuracy of pedicle screw insertion with computer-assisted surgery. A prospective clinical trial of 30 patients. Spine 22:1254–1258
Slomczykowski M, Roberto M, Schneeberger P, Ozdoba C, Vock P (1999) Radiation dose for pedicle screw insertion. Fluoroscopic method versus computer-assisted surgery. Spine 24:975–982
Schnake KJ, König B, Berth U, Schröder RJ, Kandziora F, Stöckle U, Raschke M, Haas NP (2004) Accuracy of CT-based navigation of pedicle screws in the thoracic spine compared with conventional technique. Unfallchirurg 107:104–112. https://doi.org/10.1007/s00113-003-0720-8
Rajasekaran S, Vidyadhara S, Ramesh P, Shetty AP (2007) Randomized clinical study to compare the accuracy of navigated and non-navigated thoracic pedicle screws in deformity correction surgeries. Spine 32(2):E56–E64. https://doi.org/10.1097/01.brs.0000252094.64857.ab
Tang J, Zhu Z, Sui T, Kong D, Cao X (2014) Position and complications of pedicle screw insertion with or without image-navigation techniques in the thoracolumbar spine: a meta-analysis of comparative studies. J Biomed Res 28(3):228–239. https://doi.org/10.7555/JBR.28.20130159
Oertel MF, Hobart J, Stein M, Schreiber V, Scharbrodt W (2011) Clinical and methodological precision of spinal navigation assisted by 3D intraoperative O-arm radiographic imaging. J Neurosurg Spine 14:532–536. https://doi.org/10.3171/2010.10.SPINE091032
Sclafani JA, Regev GJ, Webb J, Garfin SR, Kim CW (2011) Use of a quantitative pedicle screw accuracy system to assess new technology: initial studies on O-arm navigation and its effect on the learning curve of percutaneous pedicle screw insertion. SAS J 5(3):57–62. https://doi.org/10.1016/j.esas.2011.04.001
Balling H, Blattert TR (2017) Rate and mode of screw misplacements after 3D-fluoroscopy navigation-assisted insertion and 3D-imaging control of 1547 pedicle screws in spinal levels T10-S1 related to vertebrae and spinal sections. Eur Spine J 26(11):2898–2905. https://doi.org/10.1007/s00586-017-5108-5
Rivkin MA, Yocom SS (2014) Thoracolumbar instrumentation with CT-guided navigation (O-arm) in 270 consecutive patients: accuracy rates and lessons learned. Neurosurg Focus 36(3):E7. https://doi.org/10.3171/2014.1.FOCUS13499
Balling H (2017) Time demand and radiation dose in 3D-fluoroscopy based navigation-assisted 3D-fluoroscopy-controlled pedicle screw instrumentations. Spine. https://doi.org/10.1097/BRS.0000000000002422 (Epub ahead of print)
Sasso RC, Garrido BJ (2007) Computer-assisted spinal navigation versus serial radiography and operative time for posterior spinal fusion at L5-S1. J Spinal Disord Tech 20(2):118–122. https://doi.org/10.1097/01.bsd.0000211263.13250.b1
Houten JK, Nasser R, Baxi N (2012) Clinical assessment of percutaneous lumbar pedicle screw placement using theO-arm multidimensional surgical imaging system. Neurosurgery 70(4):990–995. https://doi.org/10.1227/NEU.0b013e318237a829
Yang BP, Wahl MM, Idler CS (2012) Percutaneous lumbar pedicle screw placement aided by computer-assisted fluoroscopy-based navigation: perioperative results of a prospective, comparative, multicenter study. Spine 37(24):2055–2060. https://doi.org/10.1097/BRS.0b013e31825c05cd
Abul-Kasim K, Söderberg M, Selariu E, Gunnarsson M, Kherad M, Ohlin A (2012) Optimization of radiation exposure and image quality of the cone-beam O-arm intraoperative imaging system in spinal surgery. J Spinal Disord Tech 25(1):52–58. https://doi.org/10.1097/BSD.0b013e318211fdea
Funding
This study was not funded by an organization.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The author declares that he has no conflict of interest. The author declares that he has full control of all primary data and that he allows the journal to review his data if requested.
Research involving human participants
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards. This article does not contain any studies with animals performed by any of the authors.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Ethical approval
The devices (O-arm, StealthStation S7) are FDA-approved or approved by corresponding national agency for this indication.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Balling, H. Learning curve analysis of 3D-fluoroscopy image-guided pedicle screw insertions in lumbar single-level fusion procedures. Arch Orthop Trauma Surg 138, 1501–1509 (2018). https://doi.org/10.1007/s00402-018-2994-x
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00402-018-2994-x