Abstract
Background
Osteoid osteoma is a benign osteoblastic tumor with a nidus of <20 mm in maximum diameter. There are several treatment options, all of them aiming either to resect or to eliminate the nidus.
Purpose
To report and to describe the benefits of treating non-spinal osteoid osteoma by percutaneous computed tomography-guided resection, according to our experience.
Study design
Retrospective case series
Methods
Between 1992 and 2008, 54 patients with non-spinal osteoid osteoma underwent primary treatment with percutaneous CT-guided resection. In all cases, the materials obtained were processed for pathology and microbiology.
Results
Fifty-four patients with a mean age of 22.7 years (range 10–47), of whom 46 were males (85.2 %) and 8 were females (14.8 %). The lesion size ranged between 5 and 15 mm with an average size of 6.9 mm. The resection was considered complete by the CT study in all 54 cases. Of all the specimens sent to pathology, the histological diagnosis was achieved in 41 (75.9 %). Cure was obtained in 50 patients (92.6 %) and the other four patients required a second surgery using the same technique, after which all of them achieved clinical and radiological improvement (100 %).
Conclusion
Percutaneous computed tomography-guided resection of non-spinal osteoid osteomas provides good results, similar to other surgical techniques, with the advantages of being a simple, mini invasive, safe and economic procedure without the need for specific materials. Level of evidence, IV.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Osteoid osteoma is a benign osteoblastic tumor first described in 1930 [1] by Bergstrand and was not until 1935 [2] when was first to be recognized as a unique entity by Jaffe. Usually, osteoid osteomas are smaller than 20 mm, characterized by an osteoid-rich nidus and vascular connective tissue. The nidus is well demarcated and surrounded by sclerotic bone [3]. The diagnosis is mainly clinical, with the most constant symptom of nocturnal-predominant pain [4]. The clinical presentation, along with additional radiographic examinations, is useful for diagnosis. Current treatment strategies include intralesional resection by curettage or trephine, laser photocoagulation or radiofrequency ablation [4–6]. We present our experience with computed tomography (CT)-guided percutaneous resection as a treatment for non-spinal osteoid osteomas in 54 patients.
Materials and methods
We retrospectively studied 54 patients with non-spinal osteoid osteomas who underwent primary treatment with CT-guided percutaneous resection at our institution (level I trauma centre) between 1992 and 2008. The diagnosis was based on medical history, X-ray, CT scan, MRI and bone scintigraphy. Inclusion criteria were: clinical and radiological diagnosis of osteoid osteoma and first surgery being performed in our hospital.
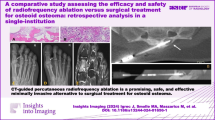
All procedures were performed under general anaesthesia, spinal anaesthesia or axillary block with sedation. Antibiotic prophylaxis used was cefazolin (as per hospital protocol). All procedures were performed in the CT room, with patients placed supine or prone according to the lesion location. CT scan with interval cuts of 2.5 mm to find the nidus was used, measuring depth from the skin surface and marking adequate coordinates. After this, a Kirschner wire (K-wire) was inserted from the cortex until the center of nidus under CT guidance and removal of the lesion with 5–10 mm in diameter drill bit or trephine through this K-wire was performed. Excision was considered complete according to immediate CT-imaging conformation (Fig. 1). All fragments obtained were processed for pathology and microbiology. At the end, CT confirmed complete excision of the lesion (Fig. 2). Skin surface was closed with sutures.
We recorded all the complications associated with the procedure.
Postoperatively, patients who had affected lower limbs were allowed partial weight bearing for 2 or 3 weeks. Follow-up was based on clinical as well as in radiological controls in the 2nd and 6th weeks postoperatively and then at 3, 6 and 12 months. Good results were defined as symptom disappearance and recurrence as their persistence after percutaneous resection.
Statistical analysis
Statistical analysis was performed using SPSS (SPSS 20.0 Student Version for Windows). Descriptive statistics were used to present the results. There was no external funding source in the investigation.
Results
Of the 54 patients included in the study group, 46 were males (85.2 %) and 8 were females (14.8 %), with average age of 22.7 years (range 10–47). In our series, where the male-to-female ratio was 5.75:1. The average time from the onset of symptoms to diagnosis was 18 months (range from 3 to 30 months). All patients had characteristic clinical and imaging criteria. The locations of the osteoid osteomas were: femur (n = 28, 51.9 %), tibia (n = 15, 27.7 %), humerus (n = 5, 9.3 %), fibula (n = 2, 3.7 %), talus (n = 2, 3.7 %) and ulnar (n = 2, 3.7 %). Thus, in half of the cases the lesion was located in the femur. The lesion size (CT measurement) ranged between 5 and 15 mm with an average size of 6.9 mm.
Procedures were performed under general anaesthesia in 30 patients, spinal anaesthesia in 19 patients and peripheral nerve block in 5 cases. The resection was considered complete by the CT study in all 54 cases. All specimens were sent for anatomopathologic study, getting a histologic diagnosis in 41 cases (75.9 %) while in the remaining 15 cases the material collected was insufficient and did not reach definitive histologic diagnosis. Cultures were negative in all the cases. The average length of the procedure was 68 min (range 58–87 min). In general, patients were hospitalized for the first night. None of them required blood transfusion. Postoperatively 47 patients, who had affected lower extremities, were limited to partial weight-bearing for 2 or 3 weeks.
After the resection procedure, 50 patients (92.6 %) were free of clinical symptoms and there was no radiographic evidence of local recurrence at the last follow-up visit. The remaining four patients who were also pain free initially recurred with symptoms between 2 and 7 months postoperative. These four patients had radiographic confirmation of a recurrent osteoid osteoma. These patients were submitted to a second CT-guided percutaneous resection that achieved symptom resolution in all of them. Radiographic follow-up did not show any recurrences either. The mean follow-up for all the patients was 22 months (range 6–28 months). During this time, no additional recurrences were recorded.
Two patients (3.7 %) presented as a minor complication a mild postoperative haematoma in the affected area, solved with conservative treatment. We did not have any cases of post-resection fracture, osteomyelitis, technical problems or other complications.
Discussion
It is well known that osteoid osteoma is a small and benign osteogenic tumor [4–7]. Current treatment options focused on percutaneous techniques include intralesional curettage, trephine resection, RFA and laser photocoagulation that search for short hospital stays and rapid recovery without sacrificing results.
The key for obtaining a good result is the proper nidus localization and its complete resection. Thus, it is very important to combine these percutaneous techniques with CT guidance because incomplete resection is the most common cause of recurrence [8].
We present the longest series of percutaneous CT-guided excision of osteoid osteoma published in the literature so far. In addition, we obtained good results after the first procedure in 50 out of 54 patients. However, the four patients with recurrence of the injury improved with a second procedure of the same surgical technique (percutaneous CT-guided resection). Even though all patients had a post procedural CT that confirmed correct lesion location and resection, it is still an intralesional oncologic procedure not exempt from risk of recurrence. All of them improved and even today, after an average of 22 months of follow-up, they continue symptom free. Our results show that the rate of patients healed after the first procedure, recurrences, histological diagnosis and complications) are comparable with other articles published in the literature performing the same procedure, as it can be seen in Table 1 [4, 5, 7–12].
The recent studies published about the treatment of osteoid osteoma using ablation by radiofrequency (RFA) reported similar rates of good results as shown in Tables 1, 2 and 3 [1, 4–14]. Also, the rates of major complications are similar using both techniques. So the main differences between these two surgical techniques are: first, we can obtain histological confirmation of the diagnosis with the percutaneous CT-guided resection, in the majority of the patients (75.9 % in our series). Some authors [6, 13, 14] used the combined technique (biopsy prior to radiofrequency ablation CT-guided), and these papers reported an average rate of histological confirmation of 55 % (range 17–100 %). Second, percutaneous CT-guided resection costs less because the material needed is reusable and it can be found in any department of orthopedic surgery and traumatology, while the material used for radiofrequency ablation is single use and with a higher cost (Table 3). Therefore, we think that despite the high cost of combined technique, its results did not show a substantial improvement compared to percutaneous CT-guided resection.
We have reported two minor complications in our patient cohort, both of them solved with conservative treatment. These facts can also been seen in Table 3, together with papers reports about percutaneous CT-guided resection in the last 17 years, in which most of the complications have been minor ones and have been solved without any secondary procedure. Of the four major complications reported, three are described in the same study [5] (2 fractures and a focal chronic osteomyelitis). The fourth one was a technical problem [8], so the surgeons decided to change the operative technique to an open procedure. This was the one and only technical problem described in the literature so far (Table 3).
On the other hand, in series where radiofrequency alone was used without or with a previous biopsy, a similar number of complications with an equal magnitude of them, both minor and major, have been described. Even more, all major complications described in the revised series [1, 6, 13, 14] have occurred in procedures that have used a core-drill for biopsy prior to RFA, which allows to reach a histological diagnosis as in percutaneous CT-guided resection and has high rates of good results with the first surgical procedure. Probably all these are related to the longer operating time, and that is a technically demanding procedure with a prolonged learning curve.
We presented the largest series of percutaneous treatment of non-spinal osteoma osteoid by CT-guided resection in the literature so far, as well as the good clinical and a low complication rate. These results are equal to the published results using RFA. We have presented this study to recommend the percutaneous computed tomography-guided resection procedure for non-spinal osteoid osteoma because it is simple, safe and does not require expensive and specific materials as compared to other techniques.
References
Papathanassiou ZG, Petsas T, Papachristou D, Megas P (2011) Radiofrequency ablation of osteoid osteomas: 5 years’ experience. Acta Orthop Belg 77(6):827–833
Jaffe HL (1953) Osteoid- osteoma. Proc R Soc Med. 46(12):1007–1012
Marić D, Djan I, Petković L, Vidosavljević M, Sopta J, Marić D (2011) Osteoid osteoma: fluoroscopic guided percutaneous excision technique—our experience. J Pediatr Orthop B 20(1):46–49
Sierre S, Innocenti S, Lipsich J, Lanfranchi L, Questa H, Moguillansky S (2006) Percutaneous treatment of osteoid osteoma by CT-guided drilling resection in pediatric patients. Pediatr Radiol 36(2):115–118
Sans N, Galy-Fourcade D, Assoun J, Jarlaud T, Chiavassa H, Bonnevialle P, Railhac N, Giron J, Morera-Maupomé H, Railhac JJ (1999) Osteoid osteoma: CT-guided percutaneous resection and follow-up in 38 patients. Radiology 212(3):687–692
Rimondi E, Mavrogenis AF, Rossi G, Ciminari R, Malaguti C, Tranfaglia C, Vanel D, Ruggieri P (2012) Radiofrequency ablation for non-pinal osteoid osteomas in 557 patients. Eur Radiol 22(1):181–188
Fenichel I, Garniack A, Morag B, Palti R, Salai M (2006) Percutaneous CT-guided curettage of osteoid osteoma with histological confirmation: a retrospective study and review of the literature. Int Orthop 30(2):139–142
Bühler M, Binkert C, Exner GU (2001) Osteoid osteoma: technique of computed tomography-controlled percutaneous resection using standard equipment available in most orthopaedic operating rooms. Arch Orthop Trauma Surg 121(8):458–461
Katz K, Kornreich L, David R, Horev G, Soudry M (2000) Osteoid osteoma: resection with CT guidance. Isr Med Assoc J 2(2):151–153
Parlier-Cuau C, Champsaur P, Nizard R, Hamze B, Laredo JD (1998) Percutaneous removal of osteoid osteoma. Radiol Clin North Am 36(3):559–566
Towbin R, Kaye R, Meza MP, Pollock AN, Yaw K, Moreland M (1995) Osteoid osteoma: percutaneous excision using a CT-guided coaxial technique. AJR Am J Roentgenol 164(4):945–949
Xu JQ, Zhang WB, Shen CW, Ding XY, Lu Y (2005) CT-guided percutaneous removal of osteoid osteoma. Zhonghua Wai Ke Za Zhi 43(16):1063–1065
Hoffmann RT, Jakobs TF, Kubisch CH, Trumm CG, Weber C, Duerr HR, Helmberger TK, Reiser MF (2010) Radiofrequency ablation in the treatment of osteoid osteoma-5-year experience. Eur J Radiol 73(2):374–379
Neumann D, Berka H, Dorn U, Neureiter D, Thaler C (2012) Follow-up of thirty-three computed-tomography-guided percutaneous radiofrequency thermoablations of osteoid osteoma. Int Orthop 36(4):811–815
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Reverte-Vinaixa, M.M., Velez, R., Alvarez, S. et al. Percutaneous computed tomography-guided resection of non-spinal osteoid osteomas in 54 patients and review of the literature. Arch Orthop Trauma Surg 133, 449–455 (2013). https://doi.org/10.1007/s00402-013-1686-9
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00402-013-1686-9