Abstract
Objective
To report a single center’s experience evaluating the efficacy and safety of computed tomography–guided radiofrequency ablation for the treatment of osteoid osteoma in children.
Materials and methods
Institutional database research identified 33 symptomatic patients (≤ 18 years of age; male/female ratio: 21/12, mean age 13.09 ± 3.66) with osteoid osteoma who were treated by CT-guided RFA. Technical and clinical success as well as complication rates were recorded. The duration of the procedure, the number of computed tomography scans and the results of the biopsy were assessed. Pain, prior, the following morning and 1 week, 1/6/12 months after the procedure were compared by means of a numeric visual scale (NVS) questionnaire.
Results
Mean lesion size was 8.28 ± 4.24 mm. Mean follow-up was 23.33 ± 17.61 months (range 12–62). Mean pain score prior to radiofrequency ablation was 9.06 ± 0.80 NVS units. On week 1 and 1/6/12 months, all patients were pain-free reporting 0 NVS units (p < 0.05). The mean procedure time was 54 min (range 51–59) and a mean of 7 CT scans were performed during the ablation session. RF electrode was successfully placed in the center of the nidus in all cases. In our study, none of our patient experienced recurrence of the pain, nor complications.
Conclusion
The present study demonstrates that percutaneous CT-guided radiofrequency ablation constitutes a safe and effective technique for osteoid osteoma treatment in children.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Osteoid osteoma is a benign bone tumor that usually affects young males and typically causes pain which often worsens at night and is significantly relieved by non-steroid anti-inflammatory drugs (NSAID) [1]. Imaging with computed tomography is well established in the diagnosis of osteoid osteoma and easily depicts the tumor᾽s nidus which measures less than 2 cm in diameter and is characterized by varying degree of peripheral mineralization [2]. Surgical approaches aim for open removal of the nidus, while percutaneous therapies are less invasive and cause less discomfort, lower the likelihood of complications as well as recovery time post-procedure [3,4,5].
Percutaneous thermal ablation of osteoid osteoma is the gold-standard therapy at the moment; the first ever case report was described by Rosenthal in 1992 [5]. There are copious data demonstrating the long-term efficacy and safety of percutaneous radiofrequency or laser ablation; additionally, in the literature, there are case series for microwave ablation and cryoablation for the treatment of osteoid osteoma [6,7,8,9,10,11,12,13,14,15,16]. All these techniques are minimally invasive with percutaneous approach and minimal damage to surrounding tissues governed by similar rates of success (95–97%), recurrence (2–5%), failure to treat (< 2%), and complications (< 2%) [6,7,8,9,10,11,12,13,14,15,16]. Furthermore, MR-guided high intensity focused ultrasound is an absolutely non-invasive technique which can be used for pain reduction in the treatment of osteoid osteoma [17, 18].
There is much more in minimally invasive techniques for children than working with smaller patients including among others the need for sedation or general anesthesia and sizing of the devices. As far as ablation of osteoid osteoma is concerned in children, general anesthesia is necessary in the vast majority of the cases while exposure to ionizing radiation is another area of concern [19]. CT dose–optimizing strategies in children include application of protocols specific for age, body size, and composition [20]. Although the amount of literature focusing upon percutaneous treatment of osteoid osteoma is extensive, there are fewer studies focusing solely upon pediatric population [21,22,23,24,25,26,27,28].
The purpose of the present study is to report a single center’s experience and to evaluate the efficacy and safety of CT-guided radiofrequency ablation for treatment of osteoid osteoma in children.
Materials and methods
Patient selection and evaluation
This is a retrospective single center study; time period of data collection was from 1/1/2010 until 31/12/2019. Institutional database research identified 33 patients with osteoid osteoma who were treated by CT-guided radiofrequency ablation. Inclusion criteria included symptomatic patients (< 18 years of age) with clinical and radiological findings compatible with osteoid osteoma. Involved bones included femur (n = 12), humerus (n = 1), acetabulum (n = 2), calcaneus (n = 1), tibia (n = 8), phalangophalangeal joint (n = 1), fibula (n = 2), talus (n = 3), spine (n = 2), and fibula (n = 1). The demographics, location, and size of lesions are listed in Table 1. Mean patient age was 13.09 ± 3.66 (range 5–18) and male/female ratio was 21/12. Each patient underwent laboratory tests (including routine blood count test as well as renal function and coagulation tests) at least 24 h prior to the percutaneous ablation session. Exclusion criteria included parents’ or legal guardians’ denial to consent, uncontrollable INR, systematic or local infection.
Percutaneous radiofrequency ablation
All patients and their parents were informed about the technique itself as well as possible benefits and complications and signed a relevant written informed consent form prior to the procedure. According to the Division of Infectious Diseases (under the Department of Internal Medicine) of our Hospital, each patient was administered with a dose of ceftriaxone 45–60 min before the RFA. Radiofrequency ablation was always performed in an inpatient setting under general anesthesia. Computed tomography guidance with sequential scanning (120 kV peak, 240 mAs wavelength, and 0.9 mm slice thickness) was used for planning, targeting, and intra-procedural modification during the ablation session. Under local sterility, radiofrequency ablation was performed with percutaneous approach in all cases. Post the initial CT scan, skin entry point was selected. A bone trocar (Bonopty Bone Biopsy System 14G, Apriomed, Uppsala, Sweden or OnControl bone marrow biopsy system 11G OBM, Arrow OnControl, Teleflex, Shavano Park, TX, USA) was inserted in the lesion of interest and its approach was evaluated with sequential CT scans. Once in the correct location, coaxially the bone biopsy needle was inserted for sampling (Fig. 1). A 15-cm long, 17-gauge radiofrequency electrode with a 1-cm single active tip (RF AMICA probe, Hospital Service S.P.A. Rome/Italy) was then introduced into the osteoid osteoma ‘s nidus through the coaxial system; the trocar was withdrawn until being outside the expected ablation zone and ablation session was performed at 90 °C for 6 min (Fig. 2). Computed tomography assessed any potential immediate complications at the end of the ablation treatment. Patients remained in the hospital overnight and pain medication was injected (IV paracetamol depended on age and weight) for post-RFA pain relief. Pain management represents a major concern during the hours following after the procedure and should be managed accordingly; collaboration with an anesthesiologist is critical for the optimal management of the patient after the procedure. All patients were discharged the next day, with advice to avoid excessive stressful weight bearing and prolonged strenuous activity for the next 2–3 weeks.
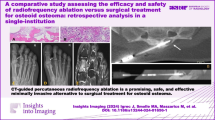
A 12-year-old female patient with osteoid osteoma of the right femur. A CT axial scan illustrating the nidus of the osteoid osteoma in subcortical location at the right femoral neck. B CT axial scan—once the bone trocar is inside the nidus coaxially the biopsy needle is inserted for sampling. C CT axial scan—once the bone sample is taken, biopsy needle is removed and coaxially the radiofrequency electrode is inserted; trocar is removed from the expected ablation zone. D CT axial scan—post ablation CT scan evaluating lack of immediate complications—notice the access route through the nidus
A 7-year-old male patient with osteoid osteoma of the right talus. A CT axial scan illustrating the nidus of the osteoid osteoma in subcortical location at the right talus. B CT axial scan—post biopsy the radiofrequency electrode is coaxially inserted; trocar is removed from the expected ablation zone. C CT axial scan—post ablation CT scan evaluating lack of immediate complications—notice the access route through the nidus
Outcome measures
Technical success was defined as the ability of nidus localization with CT scan and confirmation of RF electrode placement in the center with multiplanar reconstruction (MPR). Clinical success was defined as relief of pain caused by osteoid osteoma without any need of receiving analgesic after the first week post the procedure. Recurrence was defined as the reappearance of symptoms at any time during the follow-up period.
Procedure time (time from the moment patient was placed on CT table until the moment he/she was taken to recovery room), amount of scans (from the scanogram taken until the last scan post ablation with trocar and electrode removed), and the results of biopsy were recorded. Pain and mobility were recorded prior (maximum 1 week before the ablation), and the morning post radiofrequency ablation procedure with clinical evaluation and an inventory containing a numeric visual scale (NVS). In the same inventory, questions were included concerning the pain itself and its influence upon patient’s activity (sleep, walking) and mobility impairment.
Follow-up lasted for 1 year and consisted of clinical visit (general, clinical and neurological condition, pain reduction, and mobility improvement according to NVS scale) at week 1 with phone calls at 1, 6, and 12 months. Questions asked during the follow-up period concerned the pain reduction and mobility improvement and whether the procedure had decreased or entirely resolved the symptoms they were treated for. Immediate complications were evaluated in the post ablation CT scan and by clinical evaluation the morning after. Delayed complications were considered absent if no symptoms were reported on the follow-up phone call at 1st and 6th month.
Results
Access to the nidus was feasible in all cases (33/33). Radiofrequency electrode was coaxially inserted within the nidus and ablation was successfully performed in all lesions (technical success rate 100%). Ancillary procedures (including hydrodissection with Dextrose 5%, temperature monitoring with thermocouples and neurophysiologic monitoring) were performed in 3 patients. Hydrodissection with Dextrose 5%, temperature monitoring with thermocouples, and neurophysiologic monitoring were applied during ablation in a patient with osteoid osteoma of the peroneal bone located right next to the common peroneal nerve. In 2 patients with spinal osteoid osteomas gas (n = 1) and hydrodissection with Dextrose 5% (n = 1), along with thermocouples and neurophysiologic monitoring were applied during ablation. Histological verification of osteoid osteoma was performed in 22/33 cases in which, part or the whole nidus was extracted determining thus the osteoid osteoma diagnosis; in 11/33 cases, there was no nidus, nor any signs of malignancy in the sample.
Treated lesions had a mean diameter of 8.28 ± 4.24 mm. Mean follow-up was 23.33 ± 17.61 months (range 3–62). Mean pain score prior to RF was 9.06 ± 0.80 NVS units (range 8–10). This baseline score was reduced to a mean value of 0 on week 1, 1/6/12 months when all patients were pain-free (p < 0.05). This significant pain decrease remained stable throughout the follow-up. Median procedure time (including anesthesia, trocar placement, biopsy ablation, and post-procedural scan evaluation) was 54 min (range 51–59) while a median of 7 CT scans was necessary for controlling correct trocar, biopsy needle, and electrode placement within the nidus. Overall mobility improved in 33/33 patients. No clinically significant complications were noted in our study population.
Discussion
The present study adds to the growing number of case series (Table 2) showing that percutaneous radiofrequency ablation of osteoid osteoma in children is an efficacious and safe technique in terms of achieving symptoms’ control. Garge et al. applied CT-guided radiofrequency ablation in 30 pediatric patients reporting 100% technical and secondary clinical success with 0% recurrence and 3.3% complication rate; similarly, Ghanem et al. in 23 patients reported 100% technical and secondary clinical success with 0% recurrence and complication rate [26, 28]. Other reported complications in literature case series include two incidents of hyperthermia and a case of partial osteonecrosis of the ankle [21, 25]. Especially for osteoid osteoma ablation in the spine neurophysiological monitoring may be a valuable protective measure that requires minimal additional time and provides feedback on the state of the spinal cord and nerves at risk during the procedure; in addition, gas or hydrodissection creates a protective barrier increasing the distance between ablation zone and sensitive nerve structures [29, 30]. In the present study, neither recurrences nor complications were observed whilst technical and clinical success was 100% with no need for secondary intervention.
Hage et al. reported similar safety and efficacy rates of osteoid osteoma radiofrequency ablation in pediatric and adult patients [31]. When compared to open surgery, percutaneous CT-guided ablation is less invasive, easily repeatable, governed by lower morbidity, and lower cost with high rates of technical and clinical success rates [5, 9, 15, 32,33,34,35]. Wu et al. compared the results of surgical treatment and percutaneous radiofrequency with laser ablation of osteoid osteoma in pediatric population, concluding that the percutaneous approach is equally effective with the surgical one, with lesser morbidity and complications [27].
CT guidance offers excellent spatial resolution and field of view allowing detailed access route planning to reduce injury risk and achieve correct placement of the radiofrequency electrode minimizing thermal damage in adjacent to the target structures. Ionizing radiation of CT-guided percutaneous ablation is a burdening factor for pediatric population; specific low-dose protocols available in most if not all CT vendors can contribute in dose reduction. Cone beam CT with fluoroscopic overlay when compared to conventional CT guidance seems to be governed by significantly lower effective radiation dose at increased, however, total room utilization time [36]. MRI guidance could be an alternative method of guidance or could substitute CT-guided percutaneous treatment of osteoid osteoma, especially in pediatric population; despite the need for compatible electrodes, increased duration and limited availability, successful thermal monitoring, superior soft tissue resolution, and multiplanar navigation capabilities are features that are advantageous for interventional guidance [12, 15, 37, 38]. In the present study apart from radiation protective lead parts on the patient, all CT scans were performed with age- and weight-specific special pediatric protocols and tube current reduction factors as provided by the vendor.
Limitations of the present study include its retrospective design and the small number of participants. Furthermore, there is lack of comparison to a group of patients undergoing alternative (conservative, surgical, or another type of ablation) approaches in treatment of osteoid osteoma.
In conclusion according to the results of the present study, percutaneous CT-guided ablation constitutes a safe and effective technique for osteoid osteoma treatment in children with significant pain relief and minimal complication rates.
References
Lee EH, Shafi M, Hui JH. Osteoid osteoma: a current review. J Pediatr Orthop. 2006;26(5):695–700.
Chai JW, Hong SH, Choi JY, Koh YH, Lee JW, Choi JA, et al. Radiologic diagnosis of osteoid osteoma: from simple to challenging findings. Radiographics. 2010;30(3):737–49.
Kurup AN, Callstrom MR. Expanding role of percutaneous ablative and consolidative treatments for musculoskeletal tumours. Clin Radiol. 2017;72(8):645–56.
Sluga M, Windhager R, Pfeiffer M, Dominkus M, Kotz R. Peripheral osteoid osteoma Is there still a place for traditional surgery? J Bone Joint Surg Br. 2002;84(2):249–51.
Rosenthal DI, Alexander A, Rosenberg AE, Springfield D. Ablation of osteoid osteomas with a percutaneously placed electrode: a new procedure. Radiology. 1992;183(1):29–33.
Motamedi D, Learch TJ, Ishimitsu DN, Motamedi K, Katz MD, Brien EW, et al. Thermal ablation of osteoid osteoma: overview and step-by-step guide. Radiographics. 2009;29(7):2127–41.
Prud’homme C, Nueffer JP, Runge M, Dubut J, Kastler B, Aubry S. Prospective pilot study of CT-guided microwave ablation in the treatment of osteoid osteomas. Skeletal Radiol. 2017;46(3):315–23.
Filippiadis DK, Velonakis G, Kostantos C, Kouloulias V, Brountzos E, Kelekis N, et al. Computed tomography-guided radiofrequency ablation of intra-articular osteoid osteoma: a single centre’s experience. Int J Hyperthermia. 2017;33(6):670–4.
Rosenthal DI, Hornicek FJ, Torriani M, Gebhardt MC, Mankin HJ. Osteoid osteoma: percutaneous treatment with radiofrequency energy. Radiology. 2003;229(1):171–5.
Tsoumakidou G, Thénint MA, Garnon J, Buy X, Steib JP, Gangi A. Percutaneous image-guided laser photocoagulation of spinal osteoid osteoma: a single-institution series. Radiology. 2016;278(3):936–43.
Woertler K, Vestring T, Boettner F, Winkelmann W, Heindel W, Lindner N. Osteoid osteoma: CT-guided percutaneous radiofrequency ablation and follow-up in 47 patients. J Vasc Interv Radiol. 2001;12(6):717–22.
Gebauer B, Tunn PU, Gaffke G, Melcher I, Felix R, Stroszczynski C. Osteoid osteoma: experience with laser- and radiofrequency-induced ablation. Cardiovasc Interv Radiol. 2006;29(2):210–5.
Gangi A, Dietemann JL, Gasser B, Mortazavi R, Brunner P, Mourou MY, et al. Interstitial laser photocoagulation of osteoid osteomas with use of CT guidance. Radiology. 1997;203(3):843–8.
Witt JD, Hall-Craggs MA, Ripley P, Cobb JP, Bown SG. Interstitial laser photocoagulation for the treatment of osteoid osteoma. J Bone Joint Surg Br. 2000;82(8):1125–8.
Coupal TM, Mallinson PI, Munk PL, Liu D, Clarkson P, Ouellette H. CT-guided percutaneous cryoablation for osteoid osteoma: initial experience in adults. AJR Am J Roentgenol. 2014;202(5):1136–9.
Basile A, Failla G, Reforgiato A, Scavone G, Mundo E, Messina M, et al. The use of microwaves ablation in the treatment of epiphyseal osteoid osteomas. Cardiovasc Intervent Radiol. 2014;37(3):737–42.
Arrigoni F, Napoli A, Bazzocchi A, Zugaro L, Scipione R, Bruno F, et al. Magnetic-resonance-guided focused ultrasound treatment of non-spinal osteoid osteoma in children: multicentre experience. Pediatr Radiol. 2019;49(9):1209–16.
Masciocchi C, Zugaro L, Arrigoni F, Gravina GL, Mariani S, La Marra A, et al. Radiofrequency ablation versus magnetic resonance guided focused ultrasound surgery for minimally invasive treatment of osteoid osteoma: a propensity score matching study. Eur Radiol. 2016;26(8):2472–81.
Burrill J, Manraj S, Heran KS. Nonvascular pediatric interventional radiology. Can Assoc Radiol J. 2012;63(3):S49–58.
Al Mahrooqi KMS, Ng CKC, Sun Z. Pediatric computed tomography dose optimization strategies: a literature review. J Med Imaging Radiat Sci. 2015;46(2):241–9.
Donkol RH, Al-Nammi A, Moghazi K. Efficacy of percutaneous radiofrequency ablation of osteoid osteoma in children. Pediatr Radiol. 2008;38(2):180–5.
Moser T, Giacomelli MC, Clavert JM, Buy X, Dietemann JL, Gangi A. Image-guided laser ablation of osteoid osteoma in pediatric patients. J Pediatr Orthop. 2008;28(2):265–70.
Whitmore MJ, Hawkins CM, Prologo JD, Marshall KW, Fabregas JA, Yim DB, et al. Cryoablation of osteoid osteoma in the pediatric and adolescent population. J Vasc Interv Radiol. 2016;27(2):232–7.
Wu B, Xiao YY, Zhang X, Zhao L, Carrino JA. CT-guided percutaneous cryoablation of osteoid osteoma in children: an initial study. Skeletal Radiol. 2011;40(10):1303–10.
Aschero A, Gorincour G, Glard Y, Desvignes C, Paris M, Bourlière-Najean B, et al. Percutaneous treatment of osteoid osteoma by laser thermocoagulation under computed tomography guidance in pediatric patients. Eur Radiol. 2009;19(3):679–86.
Garge S, Keshava SN, Moses V, Chiramel GK, Ahmed M, Mammen S, et al. Radiofrequency ablation of osteoid osteoma in common and technically challenging locations in pediatric population. Indian J Radiol Imaging. 2017;27(1):88–91.
Wu H, Lu C, Chen M. Evaluation of minimally invasive laser ablation in children with osteoid osteoma. Oncol Lett. 2017;13(1):155–8.
Ghanem I, Collet LM, Kharrat K, Samaha E, Deramon H, Mertl P, et al. Percutaneous radiofrequency coagulation of osteoid osteoma in children and adolescents. J Pediatr Orthop B. 2003;12(4):244–52.
Nöel MA, Segura MJ, Sierre S, Francheri Wilson IA, Tello CA, et al. Neurophysiological Monitoring in radiofrequency ablation of spinal osteoid osteoma with a progressive time and temperature protocol in children. Spine Deform. 2017;5(5):351–9.
Filippiadis D, Mavrogenis A, Spiliopoulos S, Palialexis K, Brountzos E, Kelekis A. Percutaneous computed tomography-guided radiofrequency ablation of a spinal osteoid osteoma abutting the dura: a case report and review of the literature. Eur J Orthop Surg Traumatol. 2021 Mar 12. doi: https://doi.org/10.1007/s00590-021-02922-4. Online ahead of print.
Hage AN, Chick JFB, Gemmete JJ, Grove JJ, Srinivasa RN. Percutaneous radiofrequency ablation for the treatment of osteoid osteoma in children and adults: a comparative analysis in 92 patients. Cardiovasc Intervent Radiol. 2018;41(9):1384–90.
Goldberg SN, Gazelle GS, Mueller PR. Thermal ablation therapy for focal malignancy: a unified approach to underlying principles, techniques, and diagnostic imaging guidance. AJR Am J Roentgenol. 2000;174(2):323–31.
Dupuy DE, Goldberg SN. Image-guided radiofrequency tumor ablation: challenges and opportunities–part II. J Vasc Interv Radiol. 2001;12(10):1135–48.
Cioni R, Armillotta N, Bargellini I, Zampa V, Cappelli C, Vagli P, et al. CT-guided radiofrequency ablation of osteoid osteoma: long-term results. Eur Radiol. 2004;14(7):1203–8.
Sung KS, Seo JG, Shim JS, Lee YS. Computed-tomography-guided percutaneous radiofrequency thermoablation for the treatment of osteoid osteoma-2 to 5 years follow-up. Int Orthop. 2009;33(1):215–8.
Perry BC, Monroe EJ, McKay T, Kanal KM, Shivaram G. Pediatric percutaneous osteoid osteoma ablation: cone-beam CT with fluoroscopic overlay versus conventional CT guidance. Cardiovasc Intervent Radiol. 2017;40(10):1593–9.
Tuncali K, Morrison PR, Winalski CS, Carrino JA, Shankar S, Ready JE, et al. MRI-guided percutaneous cryotherapy for soft-tissue and bone metastases: initial experience. AJR Am J Roentgenol. 2007;189(1):232–9.
Kaul D, Bonhomme O, Schwabe P, Gebauer B and Streitparth F. Osteoid osteoma with a multicentric nidus: interstitial laser ablation under MRI guidance. Case Rep Orthop 2013; 254825.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
Approval from the Institutional Review Board was obtained and in keeping with the policies for a retrospective review, informed consent was not required.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Filippiadis, D., Stefanou, D., Mazioti, A. et al. Computed tomography guided radiofrequency ablation of osteoid osteoma in children: a single center’s experience. Skeletal Radiol 51, 855–861 (2022). https://doi.org/10.1007/s00256-021-03904-7
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00256-021-03904-7