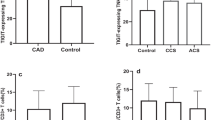
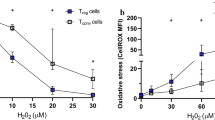
Abstract
In acute coronary syndrome (ACS), T cell abnormalities are associated to a worse outcome. Loss of inhibitory activity of CD31, an Ig-like adhesion molecule, on peripheral leukocytes has been found to enhance atherosclerosis in experimental models. In this study, we examined the expression of CD31 on T cells, and its role on TCR signaling in 35 patients with non-ST elevation ACS, in 35 patients with stable angina (SA), and in 35 controls. Furthermore, 10 ACS and 10 SA patients were re-analyzed at 1-year follow-up. Flow-cytometry analysis showed that in ACS patients, CD31 expression was reduced on total CD4+ and CD4+CD28null (P < 0.001, ACS vs. SA), on naïve (P < 0.001, ACS vs. SA) and on central-memory and effector-memory CD4+ T cells (P < 0.05, ACS vs. SA and controls). The immunomodulatory effect of CD31 on TCR signaling of CD4+ and CD4+CD28null T cells, was lower in ACS than SA patients (P < 0.05, for both comparisons). At 1-year follow-up, CD31 expression and function increased in ACS becoming similar to that found in SA. CD31 recruitment in the immunological synapse was lower in ACS than controls (P = 0.012). Moreover, CD31 modulated MAPK signaling and reduced the expression of T bet and Rorγ-t, necessary for Th1 and Th17 differentiation. Finally, we studied TCR signaling in CD31+ naïve and primed T cell subsets observing a different pattern of protein phosphorylation. A CD31-mediated regulatory pathway is enhanced in SA and temporarily downregulated in ACS. As CD31 modulates both T cell activation, by increasing the threshold for TCR stimulation, and T cell differentiation, it might represent a novel molecular target to treat T cell abnormalities in ACS.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Atherosclerosis is an inflammatory disease that involves both innate and adaptive immunity. Atherosclerotic lesions contain abundant immune cells including T cells, dendritic cells and macrophages that take part in initiation, progression and destabilization of the atherosclerotic plaque [16, 22].
Helper T cells (CD4+ lymphocyte) are the key players of adaptive immunity. Following T cell receptor (TCR) activation by antigen presenting cells, T cells differentiate into functionally polarized helper T cells such as Th1, Th2, Th17 and regulatory T cells. In addition to cytokine environment, the generation of different T cell subsets is modulated by TCR-mediated signal strength and antigen dosage [29]. In acute coronary syndrome (ACS), T cell subpopulations are dysregulated [3, 7, 12, 23–25, 28] and TCR signaling is altered leading to hyperreactivity [34]. Moreover, T cells of patients with ACS showed a differential MAPK activation [17].
CD31 is a member of the immunoglobulin (Ig) superfamily of cell adhesion molecules. It is expressed on most cells of the hematopoietic lineage including platelets, monocytes, neutrophils and T cells and plays an important role in inflammatory response through the modulation of leukocyte activation, cytokine production and the maintenance of vascular barrier integrity [2, 26, 27, 31, 32, 34, 38]. CD31 is involved in TCR-signaling immunomodulation by reducing Zap70 phosphorylation through the action of protein tyrosine phosphatases [26, 27]. Loss of CD31 Ig-like domains 1 to 5 prevents homophilic binding interaction and the consequent activation of CD31 ITIM/SHP2 inhibitory pathway, finally leading to uncontrolled T cell activation [11, 27]. CD31 signaling is triggered by homophilic and heterophilic binding interactions with different ligands [34]. In primed/memory CD4+ T cells, CD31 signaling, also triggered by cell polarization and subsequent clustering on the same cell membrane, attenuates the chemokine-induced signaling pathways, further contributing to regulation of effector T cell immunity [20]. In naive CD4+ T cells, CD31 identifies two distinct cell subsets with different roles in peripheral blood homeostasis and immune competence maintenance [19, 21]. Experimental studies have shown that loss of CD31 signaling in T cells promotes atherosclerosis and its complications [2, 4, 15].
As CD4+ T cells of ACS patients exhibit TCR hyperreactivity [35] and CD31 increases the threshold for TCR activation [26, 32], we decided to investigate the expression of CD31 on circulating T cells of ACS patients as compared with stable angina (SA) patients and subjects at intermediate risk for cardiovascular diseases (controls). We extended our analysis to CD4+CD28null T cell subpopulation, a subset of long-lived directly cytotoxic CD4+ T lymphocytes that produce a large amount of the pro-inflammatory cytokine interferon-γ (IFN-γ) [23]. We have previously shown that circulating CD4+CD28null T cell frequency is associated with a worse outcome of ACS, particularly in diabetic patients [12, 23]. Also, altered co-stimulatory pathways of CD4+CD28null T cells have recently been described in ACS [8].
To further investigate the role of CD31 in ACS, we assessed the expression of CD31 in naïve and memory T cell compartments; we studied CD31 recruitment in an ex vivo model of immunological synapse between autologous monocyte-derived dendritic cells and T cells, and we assessed the effects of CD31 triggering on MAPK signaling in naïve and primed helper T cells.
Methods
For a detailed description of all methods, see Supplementary material online.
Population
We enrolled 35 patients admitted to our Coronary Care Unit with a diagnosis of non-ST elevation myocardial infarction (NSTEMI). NSTEMI was defined as detection of rise and fall of cardiac troponin T (cTnT) and at least one of the following: angina, ST segment depression or T wave inversion. We also enrolled 35 patients with chronic stable angina (SA) admitted to our cardiovascular ward to undergo coronary angiography because of severe symptoms (CCS class III or IV) and/or high-risk abnormalities on non-invasive testing, and 35 individuals aged >50 years at intermediate risk for cardiovascular diseases, without previous history and/or current symptoms or signs of ischemic heart disease (controls). The first 25 individuals in each group were consecutively enrolled from January 2012 to June 2012. After the end of the study, ten additional patients in each group were consecutively enrolled to better match the groups for gender and statin use and to assess the effects of CD31 on MAPK signaling in naïve and memory helper T cells.
Patients enrolled in the SA group had symptoms of stable effort angina lasting more than 12 months, angiographically confirmed coronary artery disease, no previous ACS and no overt ischemic episodes during the previous 48 h.
Controls were screened in our ouT patients clinic among subjects at intermediate risk for cardiovascular diseases to match them as better as possible for risk factors with ACS and SA patients. Controls never had symptoms of ischemic heart disease. To exclude inter-current signs of ischemic heart disease, a complete cardiovascular screening was performed, including a standard 12-lead EKG, a treadmill EKG stress test, an echocardiogram, and an Echo-color Doppler of carotid arteries. Controls had normal standard 12-lead EKG, negative treadmill EKG stress test, and no significant IMT on Echo-color Doppler of carotid arteries; although the majority of patients had no regional wall motion abnormalities on echocardiogram, some of them had an ejection fraction below 55 %. Three controls had atrial fibrillation, three had mild aortic stenosis, five mild mitral valve regurgitation, and eight diastolic dysfunction because of hypertension.
Exclusion criteria were: (1) age >80 years; (2) evidence of inflammatory or infectious diseases, malignancies, immunologic or hematological disorders; (3) allergic disorders; (4) ejection fraction <40 %; (5) treatment with anti-inflammatory drugs other than low-dose aspirin. Demographic data, classical cardiovascular risk factors, history of previous ACS, previous coronary revascularization procedures, ventricular function and medical treatment, were evaluated. All ACS and SA patients underwent coronary angiography; in ACS coronary angiography was performed within 72 h after admission; in-hospital revascularization procedures were recorded. After 1-year follow-up, ten ACS who did not experience any recurrence of acute coronary events and ten SA patients free of any symptom matched for age, gender and treatment were re-assessed.
All patients gave their written informed consent. The Ethics Committee of the Catholic University of Rome approved the study. The study has been performed in accordance with the ethical standards laid down in the 1964 Declaration of Helsinki and its later amendments.
Blood sampling
Venous blood samples were taken at the time of patient enrollment. In ACS, venous blood samples were collected within 24 h from symptom onset (mean ± SD, 12.9 ± 7.5 h).
Immunophenotypic analysis
Flow-cytometry analysis was used to measure CD31 and transcription factors expression in helper and naïve T cells (for details see Supplementary material online).
Phosphoflow analysis
PBMCs were starved overnight, stimulated with anti-CD3/CD28 mAb or with anti-CD3/CD28 plus anti-CD31 mAb. They were then fixed, permeabilized, stained and analyzed by flow cytometry to measure phosphorylation levels of Zap70 and MAPKs (p38 and ERK) (for details see Supplementary material online).
Cell co-cultures and immunofluorescence microscopy
CD4+ T cells and monocytes for co-culture experiments were purified from PBMCs by sorting with CD4+ and CD14+ magnetic beads, respectively. Isolated CD4+ T cells from patients were stained and incubated with Staphylococcus Enterotoxin B (SEB)-loaded monocyte-derived dendritic cells for 10 min, fixed and stained for anti-CD3 and anti-CD31 mAb and analyzed by immunofluorescence microscopy to assess CD3 and CD31 migration in the immunological synapse (for details see Supplementary material online).
Statistical analysis
Continuous variables were normally distributed as assessed by Shapiro–Wilk test and described as mean and standard error. One-way ANOVA for repeated measures, with Bonferroni correction, was used for multiple pairwise comparisons and paired-samples t test to compare the means of two related-samples within groups. Proportions were compared using the Chi square test. A two-tailed P value <0.05 was considered statistically significant. Statistical analysis was performed with GraphPad Prism version 5.00 for Windows, (GraphPad Software, San Diego, CA, USA) and SPSS 18.0 software (SPSS Inc., Chicago, IL, USA). No power calculation could be performed because of lack of previous studies in this setting. Thus, the enrollment of 35 patients in each group was arbitrary.
Results
Characteristics of study population are reported in Table 1.
CD31 expression on CD4+ T cell subsets
As shown in Fig. 1 and Table 2, CD31 expression on total CD4+ T cells, assessed in all patients, and on CD4+CD28null T cells, assessed in 25 consecutively enrolled patients per group, was significantly higher in SA patients than in both ACS patients and controls (P < 0.001, for both comparisons) (Fig. 1; Table 2).
Flow-cytometric analysis of CD31 expression on T cell subsets. CD31 expression on total CD4+ T cells and on CD4+CD28null T cells was significantly higher in SA patients than both ACS and controls. Cumulative data from 35 ACS, 35 SA and 35 controls for total CD4+ T cells and 25 ACS, 25 SA and 25 controls for CD4+CD28null T cells are presented as single dot plots and mean ± SEM of CD31 MFI. CD31 expression on CD4+ naïve T cells was significantly higher in SA patients than both ACS and controls. ACS patients showed the lowest CD31 expression on CD4+ naïve T cells, central-memory and effector-memory T cells. Cumulative data from 25 ACS patients, 25 SA patients, and 25 controls are presented as single dot plots and mean ± SEM of CD31 MFI. For complete gating strategy see Supplemental Figure-S1. MFI median fluorescence intensity
CD31 expression on CD4+ naïve and “primed” T cells was assessed in 25 consecutively enrolled patients per group. SA patients showed the highest CD31 expression and ACS patients the lowest CD31 expression on CD4+CD45RA+CD45RO−CCR7+ (“naïve” T cells) (P < 0.001 SA vs. ACS and controls; P = 0.064 ACS vs. controls). Moreover, when we analyzed CD31 expression on “primed” T cells (CD45RA−CD45RO+), ACS patients showed the lowest CD31 expression both on CD4+CD45RA−CD45RO+CCR7+ (central-memory T cells) (P = 0.004 and P = 0.005 ACS vs. SA and controls, respectively) and on CD4+CD45RA−CD45RO+CCR7− (effector-memory T cells) (P < 0.001 and P = 0.002 ACS vs. SA and controls, respectively) (Fig. 1; Table 2).
CD31 inhibition of TCR-induced Zap70 phosphorylation
Zap70 have several residues of phosphorylation with different function [36], thus we analyzed the effects of CD31 at the Tyr319 site (a positive regulator of Zap70 function) and Tyr292 site (a negative regulator of Zap70 function). CD4+ T cells and CD4+CD28null T cells (assessed in those patients with CD28null ≥2 %) were stimulated with anti-CD3/CD28, with or without anti-CD31 cross link, for 5′.
As shown in Fig. 2a, CD31 triggering inhibited the phosphorylation of both Tyr319 and Tyr292. ACS patients showed a higher phospho-Zap70 Tyr319/Tyr292 ratio in untreated and TCR-stimulated total CD4+ T cells (P < 0.001 ACS vs. SA and controls), as well as in CD31-stimulated total CD4+ T cells (P = 0.002 ACS vs. SA). We also observed a greater Zap70 activation in CD31-stimulated CD4+CD28null T cells of ACS patients as compared with SA (P = 0.003) (Fig. 2b). Finally, we calculated the percentage of phospho-Zap70 inhibition (at the activating site Tyr-319) by CD31. As shown in Fig. 2c and Table 2, the inhibitory effect of CD31 on TCR-induced Zap70 phosphorylation in CD4+ T cells was greater in SA than in ACS and controls (P = 0.030 and P = 0.019, respectively). Similarly, in CD4+CD28null T cells the inhibition of TCR-induced Zap70 phosphorylation after CD31 triggering was greater in SA as compared with ACS and controls (P = 0.048 and P = 0.011, respectively).
CD31 triggering inhibits early TCR signaling. PBMCs were activated in vitro with αCD3/αCD28 for TCR stimulation in combination or not with αCD31. Cells were harvested after 5 min of stimulation and phosphorylation of ZAP70 (Y-319) and ZAP70 (Y-292) was assessed by flow cytometry in CD4+ and CD4+CD28null T cell gate. a CD31 triggering inhibits ZAP70 phosphorylation both at the activating and at the inhibitory residue (Tyr-319 and Ty3-292, respectively). Representative histograms of unstimulated T cells (blue histogram), TCR activated T cells (red histogram) and TCR/CD31 activated T cells (green histogram) and isotype control (grey histogram) are shown in CD4+ T cell gate. b ACS patients showed higher ZAP70 phosphorylation ratio (Tyr-319/292) both in untreated and in TCR-stimulated CD4+ T cells as compared with SA and controls and higher ZAP70 phosphorylation ratio (Tyr-319/292) in CD31-stimulated CD4+ T cells and CD4+CD28null T cells with respect to SA patients. c CD31 inhibition of Zap70 phosphorylation in CD4+ and CD4+CD28null T cells was significantly higher in SA patients than both ACS and controls. CD31 inhibition of Zap70 phosphorylation was calculated as described in supplemental materials. Data are presented as single dot plots and mean ± SEM. d CD31 expression on total CD4+ T cells strongly correlates with inhibition of Zap70 phosphorylation. Data obtained by ten ACS, ten SA, and ten controls independent experiments for total CD4+ T cells and seven ACS, seven SA, and six controls for CD4+CD28null T cells
CD31 expression on CD4+ T cells was significantly correlated with TCR immune modulation (P < 0.001, r = 0.664) (Fig. 2d).
CD31 expression and signaling in ACS and SA at 1-year follow-up
Figure 3a shows CD31 expression on CD4+ T cell subsets of ACS and SA patients at baseline and 1 year after hospitalization. In ACS, all CD4+ T cell subsets showed a significant increase in CD31 expression at 1-year follow-up as compared with baseline (P = 0.001 for total CD4+ T cells; P = 0.028 for CD4+CD28null T cells; P = 0.002 for naïve T cells; P < 0.001 for central-memory and effector-memory T cells), becoming similar to that found in SA patients. No changes were observed in SA patients.
CD31 expression and signaling in ACS and SA after 1-year of follow-up. a After 1-year follow-up, in a stable phase of the disease, all CD4+ T cell subsets of ACS patients showed a significant increase in CD31 expression as compared with baseline, becoming similar to that found in SA. Cumulative data from ten ACS patients and ten SA patients are presented as single dot plots and mean ± SEM of CD31 MFI. *P = ns, ACS follow-up vs. SA follow-up. MFI median fluorescence intensity. b PBMCs were activated in vitro as described in Fig. 2. One year after hospitalization, in a stable phase of the disease, total CD4+ T cells and CD4+CD28null T cells of ACS patients showed a significantly increased CD31 inhibition of Zap70 phosphorylation with respect to baseline, becoming similar to that found in SA. Cumulative data from five ACS patients and five SA patients are presented as single dot plots and mean ± SEM of CD31 MFI. *P = ns, ACS follow-up vs. SA follow-up. MFI median fluorescence intensity
Frequency of total CD4+ T cells, CD4+CD28null T cells, naïve, central-memory and effector-memory T cells was similar at 1 year of follow-up as compared with baseline in both ACS and SA patients (data not shown).
In ACS, the recovery of CD31 expression paralleled the increased inhibitory effects in Zap70 phosphorylation both on total CD4+ T cells and CD4+CD28null T cells (P = 0.021 and P = 0.045, respectively), becoming similar to that found in SA (Fig. 3b). No changes were observed in SA patients.
CD31 accumulation in the immunologic synapse
To assess if CD31 is implicated in immunological synapse during antigen presentation, we used an ex vivo model of autologous SEB-loaded monocyte-derived dendritic cells (MDDCs). At the time of antigen presentation, CD3 and CD31 are redistributed to the MDDCs/CD4+ T cell conjugate contact region in the immunological synapse (Fig. 4a). TCR/CD3 expression in the immunologic synapse, assessed in five consecutively enrolled patients per group, was greater in ACS patients as compared with controls (P = 0.032) (Fig. 4b; Table 2). More importantly, CD31 accumulation in the immunologic synapse on CD4+ T cells was lower in ACS as compared with controls (P = 0.012) (Fig. 4c; Table 2). Flow-cytometry analysis of MDDCs showed no differences in CD80 and CD31 expression among groups (Table 2).
Different recruitment of CD3 and CD31 in the immunologic synapse in ACS patients. CD4+ T cells from patients with ACS, SA, and controls (5 each) were stained with αCD3 (green), αCD31 (red) and DAPI (blue) and stimulated with autologous SEB-loaded monocyte-derived dendritic cells (MDDCs) for 10 min. a Representative image of CD4+ T cell/MDDC conjugates with maximum fluorescence intensity of CD31 in the contact site. b, c Enhanced recruitment of CD3 and reduced recruitment of CD31 in the immunological synapse of ACS patients as compared with SA and controls
CD31 differentially modulates ERK and p38 mitogen-activated protein kinase (MAPK) activation and inhibits the master regulators of Th1 and Th17 differentiation
To evaluate CD31 effects downstream of TCR activation, we assessed the levels of p38 and ERK phosphorylation after CD31 stimulation in CD4+ T cells from five consecutively enrolled patients per group. TCR stimulation induces distinct MAPK pathways in naïve and primed T cells [1], thus we assessed the effects of CD31 signaling in these T cell subsets.
As shown in Fig. 5a, b, CD31 triggering reduced p38 and increased ERK phosphorylation both in naïve and in primed T cells, although the effect of CD31 stimulation was more pronounced in naïve T cells.
CD31 modulates ERK and p38 phosphorylation. PBMCs were activated in vitro with αCD3/αCD28 for TCR stimulation in combination or not with αCD31. Cells were harvested after 5 min of stimulation; and phosphorylation of p38 (a) and ERK (b) was assessed by flow cytometry in naïve and primed CD4+ T cell gate. CD31 triggering inhibits p38 phosphorylation and increased ERK phosphorylation. Representative histograms of unstimulated cells (blue histogram), TCR activated cells (red histogram), TCR/CD31 activated cells (green histogram) are shown. a Naïve T cells of ACS patients showed the highest p38 phosphorylation as compared with SA and controls in untreated, TCR-stimulated and CD31 stimulated cells. CD31 inhibition of p38 phosphorylation (expressed as described in Supplemental material) was significantly higher in naïve T cells of SA patients than both ACS and controls. No differences were observed in primed T cells. b No differences were observed in ERK phosphorylation in naïve T cells among the three groups of study. Naïve T cells of SA patients showed an increased CD31-induced ERK phosphorylation (expressed as described in Supplemental material) as compared with ACS patients. Primed T cells from ACS patients showed a reduced ERK phosphorylation with respect to SA in untreated, TCR-stimulated and CD31 stimulated cells. Data obtained by five ACS, five SA, and five controls independent experiments and presented as mean ± SEM. For complete gating strategy see Supplemental Figure-S1. MFI median fluorescence intensity
Naïve T cells from ACS (defined as CD45RA+CD45RO−) showed a greater p38 phosphorylation in all setting of analysis (untreated, αCD3/CD28 stimulated, αCD3/CD28/CD31 stimulated) as compared with SA and controls (all P < 0.05). Moreover, naïve T cells from SA patients showed a higher percentage of p38 inhibition by CD31 triggering as compared with ACS and controls (P = 0.034 and P = 0.041, respectively) (Fig. 5a). There were no differences among the three groups in primed T cells (Fig. 5a).
As shown in Fig. 5b, primed T cells of ACS patients (defined as CD45RA−CD45RO+) showed a reduced ERK phosphorylation in all setting of analysis (untreated, αCD3/CD28 stimulated, αCD3/CD28/CD31 stimulated) as compared with SA (all P < 0.05), while naïve T cells from SA patients showed increased percentage of ERK activation by CD31 triggering as compared with ACS (P = 0.019).
Since MAPK pathways are implicated in helper T cell differentiation [6, 36], we also evaluated the expression of the lineage-specifying transcription factors T bet and Rorγ-t, necessary for Th1 and Th17 differentiation, respectively. As shown in Fig. 6, the expression of both transcription factors was reduced in CD4+ naïve T cells stimulated by αCD3/CD28/CD31 as compared with cells stimulated by αCD3/CD28. ACS patients showed a higher T bet expression after 72 h of TCR stimulation with (P = 0.001 and P = 0.007 ACS vs. SA and controls, respectively) or without CD31 cross link (P = 0.041 and P = 0.008 ACS vs. SA and controls, respectively) (Fig. 6a).
CD31 modulates the lineage-specifying transcription factors T bet and Rorγ-t. Isolated naïve CD4+ T cells were stimulated with αCD3/αCD28 (red histogram) in combination or not with αCD31 (green histogram) for 3 days and stained for T bet and Rorγ-t. CD31 stimulation reduced the expression of both transcription factors. a ACS patients showed increased T bet expression in naïve CD4+ T cells stimulated with αCD3/αCD28 and αCD3/αCD28 plus αCD31 as compared with SA and controls. b ACS patients showed increased Rorγ-t expression in naïve CD4+ T cells stimulated with αCD3/αCD28 and αCD3/αCD28 plus αCD31 as compared with controls. Data obtained by five ACS, five SA, and five controls independent experiments and presented as mean ± SEM
Similarly, ACS patients showed a higher Rorγ-t expression as compared with controls after TCR stimulation with and without CD31 cross link (P = 0.004 and P = 0.005, respectively) (Fig. 6b).
CD31+ naïve and primed T cells have distinct TCR signaling pathways
CD31+ naïve T cells have recently been identified as a distinct subset of CD4+ naïve T cells [19, 21]. In five controls, we studied the TCR signaling in CD31+ and CD31− naïve and primed T cells. After TCR stimulation, CD31+ naïve T cells showed a reduced Zap70 phosphorylation at its activating residue Tyr-319 as compared with CD31+ primed T cells (P = 0.003); similarly, CD31− naïve T cells showed a reduced Zap70 (Tyr-319) phosphorylation as compared with CD31− primed T cells (P = 0.014) (Fig. 7a). In contrast, Zap70 phosphorylation at its inhibitory residue Tyr-292 was higher in CD31+ naïve T cells as compared with CD31+ primed T cells (P = 0.019) (Fig. 7b). No differences were observed between CD31+ and CD31− naïve T cells.
Distinct TCR-signaling pathways in CD31+ T cell subpopulations. PBMCs were activated with αCD3/αCD28 for 5′ and the phosphoprotein levels were assessed by phosphoflow in naïve CD31+, naïve CD31−, primed CD31+ and primed CD31− T cell subpopulations. a Naïve CD31+ T cells showed reduced Zap70 phosphorylation (at activating site Tyr-319) as compared with primed CD31+ T cells; similarly, naïve CD31− T cells had reduced Zap70 phosphorylation as compared with primed CD31− T cells. b Naïve CD31+ T cells showed increased Zap70 phosphorylation at inhibitory site Tyr-292 with respect to primed CD31+ T cells. c Naïve CD31+ T cells showed increased ERK phosphorylation as compared with naïve CD31− and primed CD31+ T cells. d Primed CD31+ T cells showed reduced p38 phosphorylation as compared with primed CD31− T cells. Data obtained by five controls independent experiments and presented as mean ± SEM of fold increase with respect to untreated sample. Paired t test was used to statistical analysis
The study of MAPK signaling revealed increased ERK phosphorylation in CD31+ naïve T cells as compared with CD31− naïve T cells (P = 0.007), and increased ERK phosphorylation in CD31+ naïve T cells as compared with CD31+ primed T cells (P = 0.015) (Fig. 7c). Finally as shown in Fig. 7d, CD31+ primed T cells showed reduced p38 phosphorylation as compared with CD31− primed T cells (P = 0.036). Overall, CD31+ naïve T cells revealed distinct Zap70 and MAPK phosphorylation patterns.
Discussion
Innate and adaptive immunity act in a complex network finely tuned by several feedback loops calibrating the immune response to avoid inappropriate leukocyte activation. In this contest, CD31 plays an important immunoregulatory role by setting the threshold for T cell activation [11, 26, 27, 32] which may be relevant in several inflammatory diseases [13, 14, 37]. Recently, an impaired CD3+/CD31+ ratio and a reduced frequency of CD31+ Treg have been reported in ACS, suggesting that CD31 might be involved in regulatory T cell defects in patients with ACS [18, 41].
In the current study, the expression of CD31 on CD4+ T cell subsets was higher in SA patients as compared with ACS and controls. Consistently with its higher expression, the inhibitory effect of CD31 on TCR-induced Zap70 phosphorylation was greater in SA than in ACS and controls. Moreover, CD31 accumulation on CD4+ T cells in the immunologic synapse was reduced in patients with ACS as compared with that observed in controls. Notably, CD31 expression and function increased in ACS during follow-up becoming similar to that observed in SA patients. Here we also make the novel observation that CD31 interferes with MAPK signaling pathways in CD4+ naïve T cells, thus reducing the expression of lineage markers T bet and Rorγ-t necessary for Th1 and Th17 differentiation, respectively. These effects are prevalent in SA and reduced in ACS patients. Moreover, CD31+ and CD31− naïve and memory subpopulations have distinct Zap70 and MAPK phosphorylation patterns.
These findings suggest an enhanced CD31-mediated protective mechanism operating in SA patients, which is transiently downregulated in ACS patients during the acute phase of the disease. Our data are in agreement with experimental studies correlating CD31 loss on the surface of circulating T cells with the occurrence of atherothrombosis in mice and with the development of abdominal aortic aneurysm in patients [2, 4]. Hence, CD31 might represent a novel molecular target to treat the TCR-signaling alteration observed in ACS.
Several studies have highlighted the importance of innate and adaptive immunity in ACS [3, 7, 12, 17, 23–25, 28, 30, 35, 39]. The origin of the altered T cell response in ACS is still a matter of debate. T cell response can be directed to restricted antigens within the culprit lesions; [5, 33, 40] yet, the putative antigenic stimuli evoked in ACS can also be found in patients with chronic atherosclerotic disease [5]. Alternatively, the causes of the abnormal immune response observed in ACS might reside in a defective regulation of T cell compartment. We have observed that a large subset of ACS patients presents a unique adaptive immunity system signature, associated to a worse outcome and characterized by inadequate regulatory T cell response to effector T cell expansion [25]. Moreover, CD4+ T cells of ACS patients have abnormalities in the TCR-signaling machinery [35], and altered MAPKs phosphorylation [17] that leads to inappropriate T cell activation.
The first step in lymphocyte activation is the TCR binding with specific peptides presented by APCs. Once TCR engages its ligand, Zap70 is recruited thus initiating several signaling cascades that lead to the activation of different transcription factors and ultimately regulate T cell development, activation and effector functions. A previous study showed that TCR signaling is altered in ACS. In this study, CD4+ T cells exhibited enhanced accumulation of TCR/CD3 complexes in the immunological synapse and a defective Tyr-505 lymphocyte-specific protein tyrosine kinase phosphorylation which increases Zap70 activity [35]. The sustained TCR activation results in increased lymphocyte effector functions that could contribute to destabilize atherosclerotic plaque integrity through multiple damaging pathways. Furthermore, the altered TCR signal activation might affect the direction of T helper polarization [29].
In the present study, we expand these previous findings by dissecting out the role of CD31 in T cell dysregulation observed in ACS. The immunoregulatory functions of CD31 in T cells are now well recognized. During cell–cell interaction, homophilic CD31 engagement triggers inhibitory signaling that downmodulates lymphocyte activation by inhibition of Zap70 phosphorylation [26, 27] which is involved in helper T cell differentiation [6, 36]. In this study we have found that in SA patients, CD31 expression on T cells is upregulated as compared with controls and this is associated with enhanced CD31 inhibitory signaling. We have also observed that CD31 expression is transiently reduced at the time of the acute event in patients with ACS as compared with SA. Moreover in ACS patients, CD31 recruitment in the immunological synapse was reduced while CD3 recruitment was increased with respect to controls, thus confirming and extending previous studies regarding the alteration of TCR signaling within the immunological synapse of ACS patients [35]. We also showed that CD31 signaling modulates the overall expression of lineage-specifying transcription factors for pro-inflammatory Th1 and Th17, also through modulation of the MAPK pathways (Fig. 7). Finally, the study of the TCR signaling in CD31+ and CD31− T cell subsets revealed a different phosphorylation pattern of the protein involved in T cell activation, highlighting the differences between the CD31+ and CD31− subpopulations of both naïve and primed CD4+ T cells, at least in response to TCR stimulation. Our evidences might help further studies to gain new insights into the role of CD31 in immune response.
Taken together these findings suggest that CD31 might have a role in containing the immune response in patients with SA, while in patients with ACS the protective function of CD31 is reduced during the acute phase of the disease, thus leading to the uncontrolled lymphocyte activation and helper T cell dysregulation observed in previous studies. CD31 expression on CD4+ T cells of ACS patients and its immunomodulatory effect increased 1 year after the acute event, becoming substantially similar to that of SA patients. It is tempting to speculate that CD31 overexpansion might be a counter-regulatory mechanism which limits the detrimental effects of atherogenic stimuli in SA. However, T cell phenotype and function in peripheral blood not necessarily reflect what happens in the microenvironment of the unstable atherosclerotic plaque. We have not had the opportunity to collect coronary plaque specimens in ACS and SA patients, thus losing information on the role of CD31 on T cell locally resident in unstable plaques (Fig. 8).
Schematic representation of CD31-mediated regulatory pathway in CD4+ T cells. TCR recruitment by APC initiates a cascade of phosphorylation events which activate different downstream molecules and transcription factors. In ACS patients, TCR signaling is altered and lead to lymphocyte hyperreactivity. CD31 inhibits TCR-induced Zap70 phosphorylation and the subsequent downstream p38 MAPK activation; this pathway is involved in Th1 and Th17 differentiation (green arrows). In parallel, CD31 recruits and activates SH2-domain-containing protein tyrosine phosphatases that enhances ERK activation; this pathway acts as negative regulator of Th17 differentiation (red arrows). Thus, CD31 triggering modulates T cell activation by setting the threshold for TCR stimulation and reduces the expression of the lineage markers T bet and Rorγ- t, necessary for Th1 and Th17 differentiation. This protective mechanism was less efficient in ACS patients, in whom CD31 signaling and its recruitment in the immunological synapse are reduced. The lower CD31-mediated regulatory activity might explain the enhanced TCR signaling and the unpaired balance of lymphocyte subsets in these patients
There are no reports on the role of CD4+CD28null CD31+ subpopulation. In contrast, CD8+CD28null CD31+ T cells are considered senescent T cells with a role in inflammatory diseases [9]. Ligation of CD31, independently of TCR stimulation, induces tyrosine phosphorylation and production of interferon-γ and interleukin-10. CD31-driven IL-10 production indicates regulatory activity of CD8+CD28null CD31+ T cells [9]. In our study, CD31 expression on CD4+CD28null T cells is higher in SA than in ACS patients. Figure 2b, c shows how CD4+CD28null T cells respond to CD31 stimulation. SA patients showed lower ZAP70 phosphorylation ratio (Tyr-319/292) in CD31-stimulated CD4+CD28null T cells with respect to ACS patients. Moreover, CD31 inhibition of Zap70 phosphorylation in CD4+CD28null T cells was higher in SA than in ACS patients. Thus, we can speculate that CD4+CD28null CD31+ T cells might represent senescent T cells with an anti-inflammatory phenotype. Further studies, appropriately designed, are mandatory to investigate the role of CD4+CD28null CD31+ T cells in coronary artery disease.
Limitations
Our study has some limitations. It is an observational prospective analysis, including a limited number of patients. No power calculation could be performed because of the lack of previous studies in this setting; thus, the enrollment of 35 patients in each group was arbitrary. After 1-year follow-up, to avoid confounders related to the acute phase, we re-assessed only ACS who did not experience recurrence of acute coronary events and SA patients free of symptom matched for age, gender and treatment; thus, a small number of ACS and SA patients were re-assessed. ACS, SA patients and controls were matched for age and sex, but not for risk factors; however, no significant differences were observed to this regard between ACS and SA patients. Furthermore controls used less often aspirin and statin than SA and ACS patients. Nevertheless, controls were partly patients with cardiovascular diseases, although without previous history and/or current symptoms or signs of ischemic heart disease, and did not represent healthy probands. These limitations imply two dominant methodologic issues that cannot be eluded. First, several variables other than the coronary disease state might explain the differences observed across these three small populations. Secondly, it is impossible in this type of study to determine a cause–effect relationship. To this regard, we cannot exclude that loss of CD31 on T cells might be part of the general stress response in the acute setting of ACS. We cannot completely exclude that the reduced inhibitory effect of CD31 in ACS might simply be a marker of the general phenomenon of T cell receptor complex abnormality in these patients. Only a rescue experiment in which CD31 is restored would be ideal to prove that the observed reduced inhibitory effect of CD31 in T cells of ACS is specific. Finally, it would be of interest to analyze isolated T cells out of the coronary lesions. Thus, our study is more hypothesis-generating than hypothesis-testing.
Conclusion
In spite of these limitations, our study adds novel pieces of information to the important role of adaptive immunity alteration in coronary artery disease by suggesting that enhancement of CD31 signaling protects against plaque instability through modulation of TCR activation and through modulation of CD4+ naïve T cell differentiation in Th1 and Th17 subsets. Our findings provide evidence for a protective role of CD31 against both the helper T cell dysregulation and the lymphocyte hyperreactivity observed during ACS. Our study highlights the clinical relevance of CD31 in atherosclerotic complications identifying this molecule as a potential candidate in the treatment of CAD. Indeed, it has recently been shown that a synthetic CD31-derived peptide, able to engage a truncated extracellular CD31 fragment expressed by T cells that apparently lack CD31, has an immunosuppressive effect in vivo through restoration of the CD31 inhibitory pathway [10]. This peptide prevents the inflammatory responses underlying atherosclerosis complications and aortic aneurysms development in an experimental model [10].
Therefore, CD31-mediated regulatory pathway might represent a novel therapeutic target in the subset of ACS patients in whom an inflammatory outburst is the likely cause of coronary instability [5].
References
Adachi K, Davis MM (2011) T cell receptor ligation induces distinct signaling pathways in naive vs. antigen-experienced T cells. Proc Natl Acad Sci 108:1549–1554. doi:10.1073/pnas.1017340108
Caligiuri G, Groyer E, Khallou-Laschet J, Al Haj Zen A, Sainz J, Urbain D, Gaston AT, Lemitre M, Nicoletti A, Lafont A (2005) Reduced immunoregulatory CD31+ T cells in the blood of atherosclerotic mice with plaque thrombosis. Arterioscler Thromb Vasc Biol 25:1659–1664. doi:10.1161/01.ATV.0000172660.24580.b4
Caligiuri G, Paulsson G, Nicoletti A, Maseri A, Hansson GK (2000) Evidence for antigen-driven T cell response in unstable angina. Circulation 102:1114–1119. doi:10.1161/01.CIR.102.10.1114
Caligiuri G, Rossignol P, Julia P, Groyer E, Mouradian D, Urbain D, Misra N, Ollivier V, Sapoval M, Boutouyrie P, Kaveri SV, Nicoletti A, Lafont A (2006) Reduced immunoregulatory CD31+ T cells in patients with atherosclerotic abdominal aortic aneurysm. Arterioscler Thromb Vasc Biol 26:618–623. doi:10.1161/01.ATV.0000200380.73876.d9
Crea F, Liuzzo G (2013) Pathogenesis of acute coronary syndromes. J Am Coll Cardiol 61:1–11. doi:10.1016/j.jacc.2012.07.064
Cui G, Qin X, Zhang Y, Gong Z, Ge B, Zang YQ (2009) Berberine differentially modulates the activities of ERK, p38 MAPK, and JNK to suppress Th17 and Th1 T cell differentiation in type 1 diabetic mice. J Biol Chem 284:28420–28429. doi:10.1074/jbc.M109.012674
De Palma R, Del Galdo F, Abbate G, Chiariello M, Calabró R, Forte L, Cimmino G, Papa MF, Russo MG, Ambrosio G, Giombolini C, Tritto I, Notaristefano S, Berrino L, Rossi F, Golino P (2006) Patients with acute coronary syndrome show oligoclonal T cell recruitment within unstable plaque: evidence for a local, intracoronary immunologic mechanism. Circulation 113:640–646. doi:10.1161/CIRCULATIONAHA.105.537712
Dumitriu IE, Baruah P, Finlayson CJ, Loftus IM, Antunes RF, Lim P, Bunce N, Kaski JC (2012) High levels of costimulatory receptors OX40 and 4-1BB characterize CD4+ CD28null T cells in patients with acute coronary syndrome. Circ Res 110:857–869. doi:10.1161/CIRCRESAHA.111.261933
Dvergsten JA, Mueller RG, Griffin P, Abedin S, Pishko A, Michel JJ, Rosenkranz ME, Reed AM, Kietz DA, Vallejo AN (2013) Premature cell senescence and T cell receptor-independent activation of CD8+ T cells in juvenile idiopathic arthritis. Arthritis Rheum 65:2201–2210. doi:10.1002/art.38015
Fornasa G, Clement M, Groyer E, Gaston AT, Khallou-Laschet J, Morvan M, Guedj K, Kaveri SV, Tedgui A, Michel JB, Nicoletti A, Caligiuri G (2012) A CD31-derived peptide prevents angiotensin II-induced atherosclerosis progression and aneurysm formation. Cardiovasc Res 94:30–37. doi:10.1093/cvr/cvs076
Fornasa G, Groyer E, Clement M, Dimitrov J, Compain C, Gaston AT, Varthaman A, Khallou-Laschet J, Newman DK, Graff-Dubois S, Nicoletti A, Caligiuri G (2010) TCR stimulation drives cleavage and shedding of the ITIM receptor CD31. J Immunol 184:5485–5492. doi:10.4049/jimmunol.0902219
Giubilato S, Liuzzo G, Brugaletta S, Pitocco D, Graziani F, Smaldone C, Montone RA, Pazzano V, Pedicino D, Biasucci LM, Ghirlanda G, Crea F (2011) Expansion of CD4+ CD28null T lymphocytes in diabetic patients: exploring new pathogenetic mechanisms of increased cardiovascular risk in diabetes mellitus. Eur Heart J 32:1214–1226. doi:10.1093/eurheartj/ehq499
Goel R, Schrank BR, Arora S, Boylan B, Fleming B, Miura H, Newman PJ, Molthen RC, Newman DK (2008) Site-specific effects of PECAM-1 on atherosclerosis in LDL receptor-deficient mice. Arterioscler Thromb Vasc Biol 28:1996–2002. doi:10.1161/ATVBAHA.108.172270
Graesser D, Solowiej A, Bruckner M, Osterweil E, Juedes A, Davis S, Ruddle NH, Engelhardt B, Madri JA (2002) Altered vascular permeability and early onset of experimental autoimmune encephalomyelitis in PECAM-1-deficient mice. J Clin Invest 109:383–392. doi:10.1172/JCI13595
Groyer E, Nicoletti A, AiT Oufella H, Khallou-Laschet J, Varthaman A, Gaston AT, Thaunat O, Kaveri SV, Blatny R, Stockinger H, Mallat Z, Caligiuri G (2007) Atheroprotective effect of CD31 receptor globulin through enrichment of circulating regulatory T cells. J Am Coll Cardiol 50:344–350. doi:10.1016/j.jacc.2007.04.040
Hansson GK, Hermansson A (2011) The immune system in atherosclerosis. Nat Immunol 12:204–212. doi:10.1038/ni.2001
Indolfi C, Gasparri C, Vicinanza C, De Serio D, Boncompagni D, Mongiardo A, Spaccarotella C, Agosti V, Torella D, Curcio A (2011) Mitogen-activated protein kinases activation in T lymphocytes of patients with acute coronary syndromes. Basic Res Cardiol 106:667–679. doi:10.1007/s00395-011-0172-1
Kakizaki M, Nobori K, Watanabe H, Iino K, Ishida M, Ito H (2013) Increased circulating CD3+/CD31+ T cells in patients with acute coronary syndrome. Heart Vessels 28:566–569. doi:10.1007/s00380-012-0284-z
Kimmig S, Przybylski GK, Schmidt CA, Laurisch K, Möwes B, Radbruch A, Thiel A (2002) Two subsets of naive T helper cells with distinct T cell receptor excision circle content in human adult peripheral blood. J Exp Med 18:789–794. doi:10.1084/jem.20011756
Kishore M, Ma L, Cornish G, Nourshargh S, Marelli-Berg FM (2012) Primed T cell responses to chemokines are regulated by the immunoglobulin-like molecule CD3. PLoS ONE 7:e39433. doi:10.1371/journal.pone.0039433
Kohler S, Thiel A (2009) Life after the thymus: CD31+ and CD31− human naive CD4+ T cell subsets. Blood 113(4):769–774. doi:10.1182/blood-2008-02-139154
Lahoute C, Herbin O, Mallat Z, Tedgui A (2011) Adaptive immunity in atherosclerosis: mechanisms and future therapeutic targets. Nat Rev Cardiol 8:348–358. doi:10.1038/nrcardio.2011.62
Liuzzo G, Biasucci LM, Trotta G, Brugaletta S, Pinnelli M, Digianuario G, Rizzello V, Rebuzzi AG, Rumi C, Maseri A, Crea F (2007) Unusual CD4+ CD28null T lymphocytes and recurrence of acute coronary events. J Am Coll Cardiol 50:1450–1458. doi:10.1016/j.jacc.2007.06.040
Liuzzo G, Goronzy JJ, Yang H, Kopecky SL, Holmes DR, Frye RL, Weyand CM (2000) Monoclonal T cell proliferation and plaque instability in acute coronary syndromes. Circulation 101:2883–2888. doi:10.1161/01.CIR.101.25.2883
Liuzzo G, Montone RA, Gabriele M, Pedicino D, Giglio AF, Trotta F, Galiffa VA, Previtero M, Severino A, Biasucci LM, Crea F (2013) Identification of unique adaptive immune system signature in acute coronary syndromes. Int J Cardiol 168:564–567. doi:10.1016/j.ijcard.2013.01.009
Ma L, Mauro C, Cornish GH, Chai JG, Coe D, Fu H, Patton D, Okkenhaug K, Franzoso G, Dyson J, Nourshargh S, Marelli-Berg FM (2010) Ig gene-like molecule CD31 plays a non redundant role in the regulation of T cell immunity and tolerance. Proc Natl Acad Sci USA 107:19461–19466. doi:10.1073/pnas.1011748107
Marelli-Berg FM, Clement M, Mauro C, Caligiuri G (2013) An immunologist’s guide to CD31 function in T cells. J Cell Sci 126:2343–2352. doi:10.1242/jcs.124099
Mor A, Luboshits G, Planer D, Keren G, George J (2006) Altered status of CD4(+) CD25(+) regulatory T cells in patients with acute coronary syndromes. Eur Heart J 27:2530–2537. doi:10.1093/eurheartj/ehl222
Nakayama T, Yamashita M (2010) The TCR-mediated signaling pathways that control the direction of helper T cell differentiation. Semin Immunol 22:303–309. doi:10.1016/j.smim.2010.04.010
Narducci ML, Grasselli A, Biasucci LM, Farsetti A, Mulè A, Liuzzo G, La Torre G, Niccoli G, Mongiardo R, Pontecorvi A, Crea F (2007) High telomerase activity in neutrophils from unstable coronary plaques. J Am Coll Cardiol 50:2369–2374. doi:10.1016/j.jacc.2007.08.048
Newman PJ (1999) Switched at birth: a new family for PECAM-1. J Clin Invest 103:5–9. doi:10.1172/JCI5928
Newton-Nash DK, Newman PJ (1999) A new role for plateleT endothelial cell adhesion molecule-1 (CD31): inhibition of TCR-mediated signal transduction. J Immunol 163:682–688
Pedicino D, Giglio AF, Galiffa VA, Cialdella P, Trotta F, Graziani F, Liuzzo G (2012) Infections, immunity and atherosclerosis: pathogenic mechanisms and unsolved questions. Int J Cardiol 166:572–583. doi:10.1016/j.ijcard.2012.05.098
Privratsky JR, Newman DK, Newman PJ (2010) PECAM-1: conflicts of interest in inflammation. Life Sci 87:69–82. doi:10.1016/j.lfs.2010.06.001
Pryshchep S, Goronzy JJ, Parashar S, Weyand CM (2010) Insufficient deactivation of the protein tyrosine kinase lck amplifies T cell responsiveness in acute coronary syndrome. Circ Res 106:769–778. doi:10.1161/CIRCRESAHA.109.206052
Rincón M, Enslen H, Raingeaud J, Recht M, Zapton T, Su MS, Penix LA, Davis RJ, Flavell RA (1998) Interferon-gamma expression by Th1 effector T cells mediated by the p38 MAP kinase signaling pathway. EMBO J 17:2817–2829. doi:10.1093/emboj/17.10.2817
Wong MX, Hayball JD, Hogarth PM, Jackson DE (2005) The inhibitory co-receptor, PECAM-1 provides a protective effect in suppression of collagen-induced arthritis. J Clin Immunol 25:19–28. doi:10.1007/s10875-005-0354-7
Woodfin A, Voisin MB, Nourshargh S (2007) PECAM-1: a multi-functional molecule in inflammation and vascular biology. Arterioscler Thromb Vasc Biol 27:2514–2523. doi:10.1161/ATVBAHA.107.151456
Yonekawa K, Neidhart M, Altwegg LA, Wyss CA, Corti R, Vogl T, Grigorian M, Gay S, Lüscher TF, Maier W (2011) Myeloid related proteins activate Toll-like receptor 4 in human acute coronary syndromes. Atherosclerosis. 218:486–492. doi:10.1016/j.atherosclerosis.2011.06.020
Zal B, Kaski JC, Arno G, Akiyu JP, Xu Q, Cole D, Whelan M, Russell N, Madrigal JA, Dodi IA, Baboonian C (2004) HeaT shock protein 60-reactive CD4+ CD28null T cells in patients with acute coronary syndromes. Circulation 109:1230–1235. doi:10.1161/01.CIR.0000118476.29352.2A
Zhang WC, Wang J, Shu YW, Tang TT, Zhu ZF, Xia N, Nie SF, Liu J, Zhou SF, Li JJ, Xiao H, Yuan J, Liao MY, Cheng LX, Liao YH, Cheng X (2012) Impaired thymic export and increased apoptosis account for regulatory T cell defects in patients with non-ST segment elevation acute coronary syndrome. J Biol Chem 287:34157–34166. doi:10.1074/jbc.M112.382978
Conflict of interest
On behalf of all the authors, the corresponding author states that there is no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Additional information
G. Liuzzo and F. Crea contributed equally.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Flego, D., Severino, A., Trotta, F. et al. Altered CD31 expression and activity in helper T cells of acute coronary syndrome patients. Basic Res Cardiol 109, 448 (2014). https://doi.org/10.1007/s00395-014-0448-3
Received:
Revised:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00395-014-0448-3