Abstract
We aimed to examine the correlation of T-cell immunoglobulin and ITIM domain (TIGIT)-expressing CD3 + CD56 + cells (TNKS) with coronary artery disease (CAD), atherosclerotic lesion progression, and inflammatory environment. A total of 199 subjects, including 98 patients with acute coronary syndrome (ACS), 52 patients with chronic coronary syndrome (CCS), and 49 control subjects, were recruited in the study. The TIGIT-expressing TNKS were quantified by flow cytometric analysis; the severity of coronary artery lesions was evaluated by the Gensini score. Whole blood cells were stimulated with interleukin-2 (IL-2), interleukin-7 (IL-7), and interleukin-15 (IL-15) in presence or absence of STAT, PI3K, and P38 MAPK inhibitors, respectively. The TIGIT-expressing TNKS was significantly increased in patients with CAD, ACS, and CCS compared to the control group (P < 0.05). The TIGIT-expressing TNKS were independent predictors of CAD, ACS and CCS (P < 0.05). The TIGIT-expressing TNKS were positively associated with Gensini score (P < 0.05). The TIGIT-expressing TNKS was positively correlated with age, and being male (P < 0.05). The inflammatory microenviroment with increased IL-2, IL-7, and IL-15 contributed to upregulation of TIGIT expression in TNKS. PI3K and P38 MAPK inhibitors could inhibit the upregulation of TIGIT expression in TNKS induced by IL-2, IL-7, and IL-15. The TIGIT-expressing TNKS may be involved in common pathogenesis of ACS and CCS, and atherosclerotic lesion progression. Meanwhile, the increased TIGIT-expressing TNKS might be associated with a proatherogenic microenvironment or inflammatory microenvironment. PI3K and P38 MAPK signaling pathways were involved in the regulation of TIGIT expression.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
INTRODUCTION
Coronary artery disease (CAD), including acute coronary syndrome (ACS) and chronic coronary syndrome (CCS), is a commonly diagnosed disease worldwide and also a disease caused by multiple factors [1, 2]. CAD, which is a major cause of high morbidity and mortality rates, is associated with global burden of disease [1, 2]. The complex mechanisms underlying CAD warrants a detailed study of CAD pathogenesis. Innate and adaptive immune responses participate in the pathogenesis of atherosclerosis [3]. Both T cells and T-cell subsets and natural killer (NK) cells were observed in atherosclerotic lesions in humans or mice, these cells produce cytokines such as interferon-ү (IFN-γ), tumor necrosis factor-α (TNF-α), and interleukin-2 (IL-2), which are important inflammatory mediators associated with atherosclerosis [4, 5].
CD3+CD56+ cells (TNKS) consist of αβT, γδT, mucosal-associated invariant T (MAIT) cells, and a few invariant T (iNKT) cells [6]. Moreover, TNKS include a part of CD4+ cells and CD8+ cells [6, 7]. TNKS express CD3 T-cell and NK-cell markers. Therefore, TNKS shares some functional characteristics with T and NK cells, including NK cytotoxicity, T-cell-mediated immunity in a MHC- or CD1d-restricted manner, and secretion of cytokines such as IFN-γ and TNF-α [8]. TNKS constitute approximately 50% of T lymphocytes in the human liver [9, 10]. However, the proportions of TNKS in peripheral blood was much lower than that in liver [9, 10]. Although the number of TNKS is less in peripheral blood, they are an indispensable part of T cells. TNKS have been described in many diseases such as autoimmune diseases, allergy, primary hepatocellular carcinoma, and type 1 diabetes [6, 7, 11, 12]. Several studies have also reported the association of the subsets of TNKS with CAD [13, 14], suggesting that TNKS participates in CAD pathogenesis.
T-cell immunoglobulin and ITIM domain (TIGIT), a new member of the CD28 family, is an immunosuppressive checkpoint molecule [15,16,17,18,19]. The expression of TIGIT on immune cells such as T cells and NK cells is associated with a negative immune response [17–19]. TIGIT is elaborated in many diseases such as cancer [19], atopic dermatitis [20], autoimmune thyroiditis [21], and is associated with disease severity [20,21,22]. Upregulation of TIGIT expression mitigated disease severity in a mouse model of rheumatoid arthritis [22]. Previous study demonstrated that TIGIT expression on CD4+T cells in patients with human immunodeficiency virus is associated with the development of coronary artery calcium [23], suggesting that TIGIT expression on some immune cells may also be involved in atherosclerosis.
However, to date, the role of TIGIT-expressing TNKS in patients with CAD, ACS, or CCS has not been reported. Therefore, in this study, we aimed to investigate the correlation of TIGIT-expressing TNKS with CAD, atherosclerotic lesion progression, and the effect of inflammatory microenvironment on TIGIT expression in TNKS.
PATIENTS AND METHODS
Patients
This study involved consecutive 199 participants willing to participate in the study from the Affiliated Hospital of Guizhou Medical University, including 150 patients with CAD and 49 control subjects between May 2021 and August 2022. The patients with CAD (mean age 61.67 ± 11.95 years) were separated into two subgroups: ACS group (n = 98) (mean age 61.35 ± 12.43 years) including patients with acute ST-segment elevation ACS and non-ST-segment elevation ACS, the chronic coronary syndrome (CCS) group (n = 52) (mean age 62.27 ± 11.09 years). The patients with ACS and CCS were diagnosed based on a combination of clinical presentations, risk factors for CAD, electrocardiogram alterations, and cardiac troponin T levels [24,25,26]. The inclusion criteria for ACS patients are acute chest discomfort at rest or on minimal exertion with the presence of electrocardiogram alteration and/or a corresponding alteration of troponin T [24, 25]. The inclusion criteria for CCS are patients with stable exertional chest discomfort and/or dyspnoea, asymptomatic or mild symptomatic patients with the hostory of CAD during periodic follow-up, and asymptomatic or atypical symptomatic CAD patients detected by screening [26]. Finally, the patients with ACS and CCS have at least one main coronary artery stenosis of ≥ 50% luminal diameter. In addition, 49 control subjects (mean age 57.96 ± 12.41 years) without abnormal coronary angiogram and the history of atherosclerotic cardiovascular disease were included in the study. The patients with a history of acquired immune deficiency syndrome, serious infections, and past medical histories of severe liver and kidney insufficiency, neoplastic diseases, aortic dissection, mental disturbance, serious chronic inflammatory and immune diseases, or taking immunosuppressants, were excluded from the study. In addition, the patients with advanced heart failure were also excluded.
Clinical Data Collection
Data on demographic characteristics (age, sex, height, and weight), drug use, and medical history were obtained during hospitalization. Body mass index (BMI) was calculated by dividing the individual’s weight (kilograms) by the square of height (meters). The levels of total cholesterol (TC), high density lipoprotein cholesterol (HDL-C) were determined with a commercially available assay kit: Cholesterol Gen.2 (CHOL2) (SEKISUI MEDICAL CO., LTD, Japan), and Cholestest N HDL(Roche, Germany), respectively. The lipid levels were measured by an automatic biochemical analyzer (Roche, Germany).
Coronary Angiography Analysis
Two interventional cardiologists carried out coronary angiography through the radial or femoral access. Iodinated contrast medium is used during coronary angiography procedures. Standard multi-angle views of coronary artery were obtained to gain a better presentation of the coronary artery lesions. Based on views of the coronary angiography, the severity of coronary artery stenosis was examined by the Gensini score. The Gensini score was calculated according to the location of coronary artery stenosis and the degree of luminal stenosis. Reductions of no more than 25%, 26–50%, 51–75%, 76–90%, 91–99%, and 100% corresponded to the scores of 1, 2, 4, 8, 16, and 32, respectively. The corresponding segment score of stenosis was multiplied by a factor of the location of coronary artery stenosis as follows: 5 points for the left main coronary artery; 2.5 points for the proximal left anterior descending coronary artery (LAD) or left circumflex artery (LCX); 1.5 points for the middle segment of LAD; and 1 point for the distal LAD, first diagonal branch, the right coronary artery, posterior descending branch, obtuse marginal branch or the distal LCX, and 0.5 point for other segments [27].
Flow Cytometric Analysis
Heparin-anticoagulated blood specimens were collected and incubated with antibodies against CD3, CD56, and TIGIT at room temperature for 20 min. Then, the specimens were incubated with a red blood cell lysis buffer for 5 min in the dark, followed by washing once. Flow cytometric analysis was performed using the flow cytometer (BD celesta) equipped with BD FACS Diva software. The antibodies against CD3 and CD56 were purchased from BD Biosciences, and the antibody against TIGIT was purchased from BioLegend.
Cell Cultures and Cellular Stimulation
Heparin-anticoagulated whole blood was diluted 1/1 in RPMI 1640 culture medium (gibco). Diluted whole blood were treated with 50 ng/ml IL-2 (novoprotein), 50 ng/ml interleukin-7 (IL-7) (Sino Biological), and 50 ng/ml interleukin-15 (IL-15) (Sino Biological), and then incubated at 37 °C and 5% CO2 for 24 h. The whole blood cells were collected, and stained with antibodies against CD3, CD56, and TIGIT at room temperature for 20 min. The cells were analyzed with flow cytometer (BD celesta). TIGIT level in CD3 + CD56 + T cells was quantified using mean fluorescence intensity (MFI) to assess their changes in response to inflammatory cytokines.
Signaling Pathway Analysis
For signaling pathway studies, the diluted whole blood was cultured with IL-2 (50 ng/ml, novoprotein), IL-7 (50 ng/ml, Sino Biological), IL-15 (50 ng/ml, Sino Biological) for 30 h in the presence of PI3K inhibitor (LY 294002, 20uM, Selleck), P38 MAPK inhibitor (SB203580, 20uM, Selleck), or STAT inhibitor (SH-4–54, 20uM, Selleck), respectively. The cells were analyzed by flow cytometer.
Statistical Analysis
Normally distributed variables were expressed as mean ± standard deviation (SD), the independent samples t-test was used to compare the differences between the two groups, and comparison of normally distributed variables among three or more groups was carried out by one-way ANOVA, followed by LSD’s test. Non-normally distributed continuous variables were expressed as median with the interquartile range (IQR), and the Mann–Whitney U test was used to compare variables between the two groups. Comparisons of non-normally distributed variables among three or more groups were determined by the Kruskal–Wallis test. Categorical variables were expressed as percentages and compared using the Chi-square test or Fisher’s exact test. The association of TIGIT-expressing TNKS with CAD, ACS, or CCS was identified by logistic regression analyses in which the forward likelihood ratio method was used to select variables entering the model. Spearman’s correlation analysis was performed to examine the correlation between TIGIT-expressing TNKS and other variables such as age, Gensini score. Multiple stepwise regression analyses were performed to assess the independent correlation between TIGIT-expressing TNKS and age, sex, and Gensini score. Statistical analyses were performed using SPSS 26.0. Values with a two-sided P-value of < 0.05 were considered statistically significant.
RESULTS
Patients Characteristics
The basic characteristics of the study patients are given in Table I. Patients with CAD have a higher prevalence of hypertension and diabetes mellitus, compared to control group (P < 0.05). The proportion of male was higher in ACS group than in control group (P < 0.05). The proportion of smoking was also higher in ACS group than in control and CCS groups (P < 0.05). Compared to the patients with ACS and control, the patients with CCS showed obviously lower total cholesterol (TC) levels (P < 0.05). The HDL-C level was lower in the ACS group than in control group (P < 0.05). Compared to the patients with ACS and control, prehospital use of statins, antiplatelet, angiotensin converting enzyme inhibitors/angiotensin receptor blockers (ACEI/ARB) and β-blockers was more common in patients with CCS (P < 0.05). However, no statistically significant differences in age, BMI, and calcium antagonists use were observed among ACS group, CCS group, and control group (all P > 0.05) (Table 1).
The Abundance of TIGIT-Expressing TNKS, and TNKS in Patients with CAD, CCS, and ACS
As shown in Fig. 1, the abundance of TIGIT-expressing TNKS was obviously increased in patients with CAD, ACS, and CCS compared to the control group (Fig. 1a, b). However, the abundance of TIGIT-expressing TNKS was comparable between patients with ACS and those with CCS (P > 0.05) (Fig. 1b). Furthermore, the abundance of TNKS was similar between the patients with CAD and control group (Fig. 1c), and among these patients with ACS, CCS, and control group (Fig. 1d).
Comparison of TIGIT-expressing TNKS, TNKS between the patients with CAD and its subgroups and control group. a, b The abundance of TIGIT-expressing TNKS. c, d The abundance of TNKS. (**Indicates P < 0.01). Abbreviations: TNKS, CD3 + CD56 + cells; CAD, coronary artery disease; ACS, acute coronary syndrome; CCS, chronic coronary syndrome
TIGIT-Expressing TNKS Are Associated with CAD and Its Subgroups
The CAD, ACS, and CCS were considered as a dependent variable, respectively. Results of the univariate analysis showed that TIGIT-expressing TNKS were positively correlated with CAD (odds ratio [OR] = 1.039, 95% confidence interval [CI] = 1.017–1.061, P < 0.001), ACS (OR = 1.038, 95% CI = 1.015–1.061, P = 0.001), CCS (OR = 1.041, 95% CI = 1.015–1.068, P = 0.002), respectively (Table 2). The TIGIT-expressing TNKS, age, sex, BMI, hypertension, diabetes mellitus, lipids, smoking were considered as independent variables. The results of multiple logistic regression analyses showed a significant positive correlation of TIGIT-expressing TNKS with CAD, ACS, and CCS (Table 2).
Correlation of TIGIT-Expressing TNKS with Severity of Coronary Artery Lesions
We investigated the correlation of TIGIT-expressing TNKS with coronary lesions. The Gensini score of 170 patients was calculated to quantify the severity of coronary artery lesion burden after excluding patients with a history of revascularization. Results of spearman’s correlation analysis showed that TIGIT-expressing TNKS were positively associated with the Gensini score (r = 0.277, P < 0.001). We also performed multiple regression analysis. The independent variables included TIGIT-expressing TNKS, age, BMI, sex, smoking, hypertension, diabetes mellitus, lipids, prehospital use of antiplatelets and statins. Gensini score was considered the dependent variable, after adjustment for the above potential covariates, results of multiple stepwise regression analysis showed that TIGIT-expressing TNKS were positively correlated with the Gensini score (standardization coefficient β = 0.282, P < 0.001).
Correlation of TIGIT-Expressing TNKS with Age and Sex
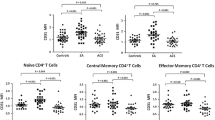
Next, we investigated the correlation of TIGIT-expressing TNKS with the conventional risk factors for CAD and found that TIGIT-expressing TNKS were positively correlated with age (r = 0.293, P < 0.01) (Fig. 2a). The TIGIT-expressing TNKS were markedly higher in patients aged ≥ 65 years than in patients aged < 65 years (P < 0.01) (Fig. 2b). Moreover, the TIGIT-expressing TNKS was higher in men than in women (p < 0.05) (Fig. 2c). We also investigated the correlation of TIGIT-expressing TNKS with hypertension, diabetes mellitus, and smoking, and the results showed that TIGIT-expressing TNKS were not associated with the history of hypertension, diabetes mellitus, and smoking (all P > 0.05). In addition, we performed a multiple stepwise regression analysis, independent variable included age, sex, BMI, hypertension, diabetes mellitus, smoking, lipids, prehospital use of antiplatelets and statins. After adjustment for the above potential variables, the results showed that age (standardization coefficient β = 0.300, P < 0.01) and being male (standardization coefficient β = 0.194, P < 0.05) were independently associated with TIGIT-expressing TNKS.
The correlation of TIGIT-expressing TNKS with age and sex. a The TIGIT-expressing TNKS were correlated with age (r = 0.293, P < 0.01). b Differences in the abundance of TIGIT-expressing TNKS in patients aged ≥ 65 years and those aged < 65 years. c Differences in the abundance of TIGIT-expressing TNKS between male and female. d The synergistic effects of age and sex on TIGIT-expressing TNKS. (**indicates P < 0.01; *indicates P < 0.05). Abbreviations: TNKS, CD3 + CD56 + cells.
The Synergistic Effects of Age and Being Male on TIGIT-Expressing TNKS
Furthermore, we investigated the synergistic effects of age and being male on TIGIT-expressing TNKS. All participants were divided into the following four groups: group 1: male aged ≥ 65 years, group 2: female aged ≥ 65 years, group 3: male aged < 65 years, and group 4: female < 65 years. The TIGIT-expressing TNKS was significantly increased in group 1 compared to that in groups 2, 3, and 4. However, no statistically significant differences in the abundance of TIGIT-expressing TNKS were observed among groups 2, 3, and 4 (Fig. 2d). Thus, both age and sex have a synergistic effect on the upregulation of TIGIT-expressing TNKS.
The Microenvironment with Increased IL-2, IL-7, and IL-15 Upregulated Expression of TIGIT in TNKS
Periperal whole blood sample from 6 patients with CAD were divided into stimulated group and control group. We stimulated whole blood cells in the stimulated group with IL-2, IL-7, and IL-15. The control group was treated with equal amounts of culture medium. The TIGIT expression in TNKS was increased in stimulated group compared with control group after 24 h of stimulation (Fig. 3).
Signaling Pathway for the Regulation of TIGIT Expression
To examine the signaling pathways involved in the regulation of TIGIT expression. Periperal whole blood sample from 9 patients with CAD were cultured with specific inhibitors of the signaling pathways, including PI3K, P38 MAPK, and STAT. As shown in Fig. 4, compared to culture medium group, the TIGIT expression was markedly increased in cytokines and STAT inhibitor groups (P < 0.05). However, the TIGIT expression was comparable between culture medium and PI3K inhibitor groups (P > 0.05). Similar results were also found between culture medium and P38 MAPK groups (P > 0.05). The results showed that PI3K and P38 MAPK inhibitors could inhibit the upregulation of TIGIT expression induced by an inflammatory environment with increased IL-2, IL-7, and IL-15.
The TIGIT expresssion in CD3 + CD56 + T cells after 30 h of treatment with different reagents. Blood cells were treated with culture medium, cytokines, cytokines in presence of STAT, PI3K, and P38 MAPK inhibitors, respectively. Cytokines included IL-2, IL-7, IL-15. Abbreviations: MFI, mean fluorescence intensity. (**Indicates P < 0.05, *Indicates P > 0.05).
DISCUSSION
In the present study, we demonstrated that the abundance of TIGIT-expressing TNKS was increased in CAD, ACS, and CCS. Increasing evidence has demonstrated that TIGIT expression on immune cells varied with different disease microenvironments. For example, TIGIT expression on CD4+T cells is upregulated in atopic dermatitis [20], and systemic lupus erythematosus (SLE) [28], and downregulated in psoriasis [29]. Moreover, TIGIT expression on CD8+ T cells is unaltered in atopic dermatitis [20], and downregulated in SLE [28]. The above studies indicate that TIGIT expression on immune cells varies in a clinical context-dependent manner.
It is widely accepted that TIGIT, an immune checkpoint molecule, is a negative costimulatory molecule [17, 30]. TIGIT can inhibit T-cell functions, including activation, IFN-γ secretion, and proliferation. Mao et al. found that TIGIT+CD4 T cells had lower IFN-γ production and proliferation rate compared to TIGIT−CD4 T cells in both healthy individuals and patients with SLE [28]. Guillerey et al. reported that IFN-γ and TNF-α production and proliferation rate of CD8 T cells were lower in TIGIT+CD8 T cells than in TIGIT−CD8 T cells in multiple myeloma [31]. In NK cells, low TIGIT expression was shown to be associated with higher IFN-γ production and cytotoxicity [15]. These findings strongly indicate that TIGIT expression on the above-mentioned immune cells negatively regulates the activity of immune cells [32, 33]. Inflammatory immunity is involved in the pathogenesis of atherosclerosis and CAD. Given that there were elevated concentrations of IL-2, IL-7, and IL-15 in patients with CAD [34,35,36]. In this study, we examined whether the combination of IL-2, IL-7, and IL-15 could influence the TIGIT expression in TNKS. Interestingly, the increased abundance of TIGIT-expressing TNKS was found after 24 h of inflammatory stimulation (Fig. 3), suggesting that increased abundance of TIGIT-expressing TNKS may be regulated, at least in part, through the inflammatory stimulation pathway in CAD. Similar to the increase in N-terminal-pro-B-type natriuretic peptide (NT-proBNP) levels in patients with cardiac failure, the increase in the abundance of TIGIT-expressing TNKS may be a physiopathologic response to the CAD microenvironment. Accordingly, the increased abundance of TIGIT-expressing TNKS may reflect the ongoing TNKS activation in the CAD microenvironment [37]. A recent study showed that the expression of the inhibitory receptor LILRB1 in TNKS was increased and that the expression of the inhibitory receptor NKG2A and NKG2C in TNKS was unaltered in patients with CAD compared to patients without CAD, which indicated that increased inhibitory receptor LILRB1 expression may be associated with the pathogenesis of CAD [38]. Similar to LIRBI, TIGIT was also inhibitory receptor. In this study, an increased abundance of TIGIT-expressing TNKS was seen in patients with CAD, ACS, and CCS. We also demonstrated that the increased abundance of TIGIT-expressing TNKS was an independent predictor of CAD, ACS, and CCS. These findings indicated that TIGIT-expressing TNKS might be involved in common pathogenesis of ACS and CCS. However, in CAD subgroup analysis, we did not observe any differences in the abundance of TIGIT-expressing TNKS between patients with ACS and those with CCS (Fig. 1b), suggesting that TIGIT-expressing TNKS might be not associated with the onset of ACS or destabilization of plaque.
Furthermore, we showed that the increased TIGIT-expressing TNKS was associated with the Gensini score reflecting the severity of coronary artery lesions, suggesting that the increased TIGIT expression might participate in the atherosclerotic lesion progression, in line with the literature [23]. TIGIT, an immune-inhibitory checkpoint molecule, can exert negative immune response [17, 30]. Therefore, activating the signaling pathway of TIGIT on TNKS may inhibit the progression of atherosclerosis. Targeting TIGIT-expressing TNKS may be a novel therapeutic option for CAD. Further animal study in vivo is necessary to confirm the hypothesis.
Age is another important risk factor for atherosclerosis, which is an age-related disease [39, 40]. Lu et al. examined the association of age with the development of carotid plaques using carotid magnetic resonance imaging and found that the development of carotid plaques progressed significantly in older patients compared to younger patients. Moreover, they showed that age was still correlated with carotid plaque progression after adjusting for clinical variables [41]. Huang et al. investigated the risk factors of progression of carotid intima-media thickness (IMT) and plaque using an ultrasound imaging system and revealed that age was an independent risk factor of IMT and carotid plaque development [42]. Using coronary computed tomography angiography, Conte et al. demonstrated that the total plaque volume was increased in patients aged ≥ 65 years old compared to patients aged < 65 years [43]. Furthermore, old age was associated with chronic inflammation [44, 45]. Moreover, the risk of CAD significantly increased with age [46].
Men are also at a higher risk of developing atherosclerosis than women, and a higher atherosclerotic plaque burden is found in men [47]. Huang et al. revealed that men were more prone to plaque progression than women [42]. Moreover, Taqueti et al. showed that a higher degree of obstructive CAD prevalence was observed in men than in women [48]. Liu et al. found that aging could promote atherosclerosis progression, especially in male mice [49], which indicated that older age and being male had a synergistic effect on atherosclerosis. Furthermore, a study found that plaques from carotid artery samples in men had higher levels of inflammatory macrophage than women [50]. Another study used 18F-FDG positron emission computed tomography, reflecting inflammation of atherosclerotic lesions, and found that men had more extensive inflammatory response levels in plaques of the carotid and iliofemoral arteries than women [51].
Therefore, both older age and being male may be associated with a proatherogenic and proinflammatory microenvironment. In the present study, we found that the abundance of TIGIT-expression TNKS was positively correlated with age and being male and that they synergized to augment the level of TIGIT-expressing TNKS (Fig. 2). Collectively, our findings demonstrated the close relationship between TIGIT-expression TNKS and age and being male, suggesting the increased abundance of TIGIT-expressing TNKS may be associated with a proatherogenic and proinflammatory microenvironment. This was further confirmed by the finding in response to cytokines in Fig. 3.
Besides, the literature reported that the common ү chain cytokine IL-2, IL-7, and IL-15 had the impact on the JAK-STAT, PI3K, and MAPK signaling pathways [52,53,54]. We found that PI3K and P38 MAPK inhibitors could inhibit the upregulation of TIGIT expression in TNKS induced by IL-2, IL-7, and IL-15, indicating that PI3K and MAPK signaling pathways were involved in regulation of TIGIT expression in TNKS.
There are certain limitations to our study. Firstly, this is a single-center study in southwest China. Secondly, besides IL-2, IL-7, and IL- 15, patients with CAD have many other cytokines associated with pathogenesis of CAD or atherosclerosis. Whether they also could influence the TIGIT expression in TNKS remains to be further studied. Moreover, the role of TIGIT-expressing TNKS was not demonstrated in vivo. Finally, we could not determine the causal relationship between TIGIT-expressing TNKS and CAD due to the cross-sectional nature of this study.
CONCLUSIONS
In summary, we demonstrated for the first time that the increase in the abundance of TIGIT-expressing TNKS was significantly associated with the presence of CAD, ACS, or CCS, and the severity of coronary artery lesions. The results indicated that TIGIT-expressing TNKS were involved in the common pathogenesis of ACS and CCS, and the progression of atherosclerotic lesions. Meanwhile, the positive correlation of increased TIGIT-expressing TNKS with age and being male suggested that TIGIT-expressing TNKS were associated with the proatherogenic microenvironment. The inflammatory micorenvironment with increased IL-2, IL-7, and IL-15 contributed to upregulation of TIGIT expression in TNKS. PI3K and P38 MARK signaling pathways were involved in the regulation of TIGIT expression. The precise role of TIGIT-expressing TNKS in atherosclerosis will be further elucidated in our ongoing studies.
Data Availability
The data presented in this study are available on reasonable request from the corresponding author.
References
Faria, A., A.C. Caldas, and I. Laher. 2022. Is noise exposure a risk factor for cardiovascular diseases? A literature review. Heart Mind 6:226-31. https://doi.org/10.4103/hm.hm_48_22.
Safiri, S., N. Karamzad, K. Singh, K. Carson-Chahhoud, C. Adams, S.A. Nejadghaderi, A. Almasi-Hashiani, M.J.M. Sullman, M.A. Mansournia, N.L. Bragazzi, J.S. Kaufman, G.S. Collins, and A.A. Kolahi. 2022. Burden of ischemic heart disease and its attributable risk factors in 204 countries and territories, 1990–2019. European journal of preventive cardiology 29 (2): 420–431. https://doi.org/10.1093/eurjpc/zwab213.
Hong, L.Z., Q. Xue, and H. Shao. 2021. Inflammatory markers related to innate and adaptive immunity in atherosclerosis: Implications for disease prediction and prospective therapeutics. Journal of inflammation research 14: 379–392. https://doi.org/10.2147/JIR.S294809.
Saigusa, R., H. Winkels, and K. Ley. 2020. T cell subsets and functions in atherosclerosis. Nature reviews. Cardiology 17 (7): 387–401. https://doi.org/10.1038/s41569-020-0352-5.
Kumrić, M., T.T. Kurir, J.A. Borovac, and J. Božić. 2020. The role of natural killer (NK) cells in acute coronary syndrome: A comprehensive review. Biomolecules 10 (11): 1514. https://doi.org/10.3390/biom10111514.
Tao, L., S. Wang, G. Kang, S. Jiang, W. Yin, L. Zong, J. Li, and X. Wang. 2021. PD-1 blockade improves the anti-tumor potency of exhausted CD3+CD56+ NKT-like cells in patients with primary hepatocellular carcinoma. Oncoimmunology 10 (1): 2002068. https://doi.org/10.1080/2162402X.2021.2002068.
Terrazzano, G., S. Bruzzaniti, V. Rubino, M. Santopaolo, A.T. Palatucci, A. Giovazzino, C. La Rocca, P. de Candia, A. Puca, F. Perna, C. Procaccini, V. De Rosa, C. Porcellini, S. De Simone, V. Fattorusso, A. Porcellini, E. Mozzillo, R. Troncone, A. Franzese, J. Ludvigsson, … M. Galgani. 2020. T1D progression is associated with loss of CD3+CD56+ regulatory T cells that control CD8+ T cell effector functions. Nature Metabolism 2 (2): 142–152. https://doi.org/10.1038/s42255-020-0173-1.
Kelly-Rogers, J., L. Madrigal-Estebas, T. O’connor, and D.G. Doherty. 2006. Activation-induced expression of CD56 by T cells is associated with a reprogramming of cytolytic activity and cytokine secretion profile in vitro. Human immunology 67 (11): 863–873. https://doi.org/10.1016/j.humimm.2006.08.292.
Doherty, D.G., and C. O’farrelly. 2000. Innate and adaptive lymphoid cells in the human liver. Immunological reviews 174: 5–20. https://doi.org/10.1034/j.1600-0528.2002.017416.x.
Doherty, D.G. 2016. Immunity, tolerance and autoimmunity in the liver: A comprehensive review. Journal of autoimmunity 66: 60–75. https://doi.org/10.1016/j.jaut.2015.08.020.
Romero-Olmedo, A.J., A.R. Schulz, M. Huber, C.U. Brehm, H.D. Chang, C.M. Chiarolla, T. Bopp, C. Skevaki, F. Berberich-Siebelt, A. Radbruch, H.E. Mei, and M. Lohoff. 2021. Deep phenotypical characterization of human CD3+ CD56+ T cells by mass cytometry. European journal of immunology 51 (3): 672–681. https://doi.org/10.1002/eji.202048941.
Zhao, L., W. Xu, Z. Chen, H. Zhang, S. Zhang, C. Lian, J. Sun, H. Chen, and F. Zhang. 2021. Aberrant distribution of CD3+CD56+ NKT-like cells in patients with primary Sjögren’s syndrome. Clinical and Experimental Rheumatology 39 (1): 98–104. https://doi.org/10.55563/clinexprheumatol/uzzz6d.
Jabir, N.R., C.K. Firoz, F. Ahmed, M.A. Kamal, S. Hindawi, G.A. Damanhouri, H.A. Almehdar, and S. Tabrez. 2017. Reduction in CD16/CD56 and CD16/CD3/CD56 natural killer cells in coronary artery disease. Immunological investigations 46 (5): 526–535. https://doi.org/10.1080/08820139.2017.1306866.
Bergström, I., K. Backteman, A. Lundberg, J. Ernerudh, and L. Jonasson. 2012. Persistent accumulation of interferon-γ-producing CD8+CD56+ T cells in blood from patients with coronary artery disease. Atherosclerosis 224 (2): 515–520. https://doi.org/10.1016/j.atherosclerosis.2012.07.033.
Wang, F., H. Hou, S. Wu, Q. Tang, W. Liu, M. Huang, B. Yin, J. Huang, L. Mao, Y. Lu, and Z. Sun. 2015. TIGIT expression levels on human NK cells correlate with functional heterogeneity among healthy individuals. European journal of immunology 45 (10): 2886–2897. https://doi.org/10.1002/eji.201545480.
Lee, D.J. 2020. The relationship between TIGIT+ regulatory T cells and autoimmune disease. International Immunopharmacology 83: 106378. https://doi.org/10.1016/j.intimp.2020.106378.
Anderson, A.C., N. Joller, and V.K. Kuchroo. 2016. Lag-3, Tim-3, and TIGIT: Co-inhibitory receptors with specialized functions in immune regulation. Immunity 44 (5): 989–1004. https://doi.org/10.1016/j.immuni.2016.05.001.
Harjunpää, H., and C. Guillerey. 2020. TIGIT as an emerging immune checkpoint. Clinical and experimental immunology 200 (2): 108–119. https://doi.org/10.1111/cei.13407.
Chauvin, J.M., and H.M. Zarour. 2020. TIGIT in cancer immunotherapy. Journal for Immunotherapy of Cancer 8(2): e000957. https://doi.org/10.1136/jitc-2020-000957.
Kurita, M., Y. Yoshihara, Y. Ishiuji, M. Chihara, T. Ishiji, A. Asahina, and K. Yanaba. 2019. Expression of T-cell immunoglobulin and immunoreceptor tyrosine-based inhibitory motif domain on CD4+ T cells in patients with atopic dermatitis. The Journal of dermatology 46 (1): 37–42. https://doi.org/10.1111/1346-8138.14696.
Štefanić, M., S. Tokić, M. Suver-Stević,and L. Glavaš-Obrovac. 2019. Expression of TIGIT and FCRL3 is Altered in T cells from patients with distinct patterns of chronic autoimmune thyroiditis. Experimental and Clinical Endocrinology & Diabetes : Official Journal, German Society of Endocrinology [and] German Diabetes Association 127 (5): 281–288. https://doi.org/10.1055/a-0597-8948.
Zhao, W., Y. Dong, C. Wu, Y. Ma, Y. Jin, and Y. Ji. 2016. TIGIT overexpression diminishes the function of CD4 T cells and ameliorates the severity of rheumatoid arthritis in mouse models. Experimental cell research 340 (1): 132–138. https://doi.org/10.1016/j.yexcr.2015.12.002.
Bowler, S., G.M. Chew, M. Budoff, D. Chow, B.I. Mitchell, M.L. DʼAntoni, C. Siriwardhana, L.C. Ndhlovu, and C. Shikuma. 2019. PD-1+ and TIGIT+ CD4 T cells are associated with coronary artery calcium progression in HIV-infected treated adults. Journal of Acquired Immune Deficiency Syndromes (1999) 81 (1): e21–e23. https://doi.org/10.1097/QAI.0000000000002001.
Ibanez, B., James, S., Agewall, S., Antunes, M. J., Bucciarelli-Ducci, C., Bueno, H., Caforio, A. L. P., Crea, F., Goudevenos, J. A., Halvorsen, S., Hindricks, G., Kastrati, A., Lenzen, M. J., Prescott, E., Roffi, M., Valgimigli, M., Varenhorst, C., Vranckx, P., Widimský, P., & ESC Scientific Document Group. 2018. 2017 ESC Guidelines for the management of acute myocardial infarction in patients presenting with ST-segment elevation: The task force for the management of acute myocardial infarction in patients presenting with ST-segment elevation of the European Society of Cardiology (ESC). European heart journal 39 (2): 119–177. https://doi.org/10.1093/eurheartj/ehx393.
Collet, J. P., Thiele, H., Barbato, E., Barthélémy, O., Bauersachs, J., Bhatt, D. L., Dendale, P., Dorobantu, M., Edvardsen, T., Folliguet, T., Gale, C. P., Gilard, M., Jobs, A., Jüni, P., Lambrinou, E., Lewis, B. S., Mehilli, J., Meliga, E., Merkely, B., Mueller, C., … ESC Scientific Document Group. 2021. 2020 ESC guidelines for the management of acute coronary syndromes in patients presenting without persistent ST-segment elevation. European heart journal 42 (14): 1289–1367. https://doi.org/10.1093/eurheartj/ehaa575.
Knuuti, J., Wijns, W., Saraste, A., Capodanno, D., Barbato, E., Funck-Brentano, C., Prescott, E., Storey, R. F., Deaton, C., Cuisset, T., Agewall, S., Dickstein, K., Edvardsen, T., Escaned, J., Gersh, B. J., Svitil, P., Gilard, M., Hasdai, D., Hatala, R., Mahfoud, F., … ESC Scientific Document Group. 2020. 2019 ESC guidelines for the diagnosis and management of chronic coronary syndromes. European heart journal 41 (3): 407–477. https://doi.org/10.1093/eurheartj/ehz425.
Gensini, G.G. 1983. A more meaningful scoring system for determining the severity of coronary heart disease. The American journal of cardiology 51 (3): 606. https://doi.org/10.1016/s0002-9149(83)80105-2.
Mao, L., H. Hou, S. Wu, Y. Zhou, J. Wang, J. Yu, X. Wu, Y. Lu, L. Mao, M.J. Bosco, F. Wang, and Z. Sun. 2017. TIGIT signalling pathway negatively regulates CD4+ T-cell responses in systemic lupus erythematosus. Immunology 151 (3): 280–290. https://doi.org/10.1111/imm.12715.
Wang, F.F., Y. Wang, L. Wang, T.S. Wang, and Y.P. Bai. 2018. TIGIT expression levels on CD4+ T cells are correlated with disease severity in patients with psoriasis. Clinical and experimental dermatology 43 (6): 675–682. https://doi.org/10.1111/ced.13414.
Grabie, N., A.H. Lichtman, and R. Padera. 2019. T cell checkpoint regulators in the heart. Cardiovascular research 115 (5): 869–877. https://doi.org/10.1093/cvr/cvz025.
Guillerey, C., H. Harjunpää, N. Carrié, S. Kassem, T. Teo, K. Miles, S. Krumeich, M. Weulersse, M. Cuisinier, K. Stannard, Y. Yu, S.A. Minnie, G.R. Hill, W.C. Dougall, H. Avet-Loiseau, M.W.L. Teng, K. Nakamura, L. Martinet, and M.J. Smyth. 2018. TIGIT immune checkpoint blockade restores CD8+ T-cell immunity against multiple myeloma. Blood 132 (16): 1689–1694. https://doi.org/10.1182/blood-2018-01-825265.
Yu, X., K. Harden, L.C. Gonzalez, M. Francesco, E. Chiang, B. Irving, I. Tom, S. Ivelja, C.J. Refino, H. Clark, D. Eaton, and J.L. Grogan. 2009. The surface protein TIGIT suppresses T cell activation by promoting the generation of mature immunoregulatory dendritic cells. Nature immunology 10 (1): 48–57. https://doi.org/10.1038/ni.1674.
Joller, N., J.P. Hafler, B. Brynedal, N. Kassam, S. Spoerl, S.D. Levin, A.H. Sharpe, and V.K. Kuchroo. 2011. Cutting edge: TIGIT has T cell-intrinsic inhibitory functions. Journal of Immunology (Baltimore, Md. : 1950) 186 (3): 1338–1342. https://doi.org/10.4049/jimmunol.1003081.
Ding, R., W. Gao, D.H. Ostrodci, Z. He, Y. Song, L. Ma, C. Liang, and Z. Wu. 2013. Effect of interleukin-2 level and genetic variants on coronary artery disease. Inflammation 36 (6): 1225–1231. https://doi.org/10.1007/s10753-013-9659-2.
Dozio, E., A.E. Malavazos, E. Vianello, S. Briganti, G. Dogliotti, F. Bandera, F. Giacomazzi, S. Castelvecchio, L. Menicanti, A. Sigrüener, G. Schmitz, and M.M. Corsi Romanelli. 2014. Interleukin-15 and soluble interleukin-15 receptor α in coronary artery disease patients: association with epicardial fat and indices of adipose tissue distribution. PloS One 9 (3): e90960. https://doi.org/10.1371/journal.pone.0090960.
Damås, J.K., T. Waehre, A. Yndestad, K. Otterdal, A. Hognestad, N.O. Solum, L. Gullestad, S.S. Frøland, and P. Aukrust. 2003. Interleukin-7-mediated inflammation in unstable angina: Possible role of chemokines and platelets. Circulation 107 (21): 2670–2676. https://doi.org/10.1161/01.CIR.0000070542.18001.87.
Fuertes Marraco, S.A., N.J. Neubert, G. Verdeil, and D.E. Speiser. 2015. Inhibitory Receptors Beyond T Cell Exhaustion. Frontiers in immunology 6: 310. https://doi.org/10.3389/fimmu.2015.00310.
Romo, N., M. Fitó, M. Gumá, J. Sala, C. García, R. Ramos, A. Muntasell, R. Masiá, J. Bruguera, I. Subirana, J. Vila, E. De Groot, R. Elosua, J. Marrugat, and M. López-Botet. 2011. Association of atherosclerosis with expression of the LILRB1 receptor by human NK and T-cells supports the infectious burden hypothesis. Arteriosclerosis, thrombosis, and vascular biology 31 (10): 2314–2321. https://doi.org/10.1161/ATVBAHA.111.233288.
Tyrrell, D.J., and D.R. Goldstein. 2021. Ageing and atherosclerosis: Vascular intrinsic and extrinsic factors and potential role of IL-6. Nature reviews. Cardiology 18 (1): 58–68. https://doi.org/10.1038/s41569-020-0431-7.
Chen, M.A., M. Kawakubo, P.M. Colletti, D. Xu, L. Labree Dustin, R. Detrano, S.P. Azen, N.D. Wong, and X.Q. Zhao. 2013. Effect of age on aortic atherosclerosis. Journal of geriatric cardiology : JGC 10 (2): 135–140. https://doi.org/10.3969/j.issn.1671-5411.2013.02.005.
Lu, M., P. Peng, H. Qiao, Y. Cui, L. Ma, B. Cui, J. Cai, and X. Zhao. 2019. Association between age and progression of carotid artery atherosclerosis: A serial high resolution magnetic resonance imaging study. The international journal of cardiovascular imaging 35 (7): 1287–1295. https://doi.org/10.1007/s10554-019-01538-4.
Huang, L.C., R.T. Lin, C.F. Chen, C.H. Chen, S.H. Juo, and H.F. Lin. 2016. Predictors of carotid intima-media thickness and plaque progression in a Chinese population. Journal of atherosclerosis and thrombosis 23 (8): 940–949. https://doi.org/10.5551/jat.32177.
Conte, E., A. Dwivedi, S. Mushtaq, G. Pontone, F.Y. Lin, E.J. Hollenberg, S.E. Lee, J. Bax, F. Cademartiri, K. Chinnaiyan, B.J.W. Chow, R.C. Cury, G. Feuchtner, M. Hadamitzky, Y.J. Kim, A. Baggiano, J. Leipsic, E. Maffei, H. Marques, F. Plank, … D. Andreini. 2021. Age- and sex-related features of atherosclerosis from coronary computed tomography angiography in patients prior to acute coronary syndrome: results from the ICONIC study. European Heart Journal Cardiovascular Imaging 22 (1): 24–33. https://doi.org/10.1093/ehjci/jeaa210.
Rea, I.M., D.S. Gibson, V. Mcgilligan, S.E. Mcnerlan, H.D. Alexander, and O.A. Ross. 2018. Age and age-related diseases: Role of inflammation triggers and cytokines. Frontiers in immunology 9: 586. https://doi.org/10.3389/fimmu.2018.00586.
De Almeida, A.J.P.O., M.S. De Almeida Rezende, S.H. Dantas, S. De Lima Silva, J.C.P.L. De Oliveira, and De Lourdes Assunção Araújo De Azevedo, F., Alves, R. M. F. R., De Menezes, G. M. S., Dos Santos, P. F., Gonçalves, T. A. F., Schini-Kerth, V. B., & De Medeiros, I. A. 2020. Unveiling the role of inflammation and oxidative stress on age-related cardiovascular diseases. Oxidative medicine and cellular longevity 2020: 1954398. https://doi.org/10.1155/2020/1954398.
Idris, I., R. Deepa, D.J. Fernando, and V. Mohan. 2008. Relation between age and coronary heart disease (CHD) risk in Asian Indian patients with diabetes: A cross-sectional and prospective cohort study. Diabetes research and clinical practice 81 (2): 243–249. https://doi.org/10.1016/j.diabres.2008.04.006.
Man, J.J., J.A. Beckman, and I.Z. Jaffe. 2020. Sex as a biological variable in atherosclerosis. Circulation research 126 (9): 1297–1319. https://doi.org/10.1161/CIRCRESAHA.120.315930.
Taqueti, V.R., L.J. Shaw, N.R. Cook, V.L. Murthy, N.R. Shah, C.R. Foster, J. Hainer, R. Blankstein, S. Dorbala, and M.F. Di Carli. 2017. Excess cardiovascular risk in women relative to men referred for coronary angiography is associated with severely impaired coronary flow reserve, not obstructive disease. Circulation 135 (6): 566–577. https://doi.org/10.1161/CIRCULATIONAHA.116.023266.
Liu, M., W. Zhang, X. Li, J. Han, Y. Chen, and Y. Duan. 2016. Impact of age and sex on the development of atherosclerosis and expression of the related genes in apoE deficient mice. Biochemical and biophysical research communications 469 (3): 456–462. https://doi.org/10.1016/j.bbrc.2015.11.064.
Yuan, X.M., L.J. Ward, C. Forssell, N. Siraj, and W. Li. 2018. Carotid atheroma from men has significantly higher levels of inflammation and iron metabolism enabled by macrophages. Stroke 49 (2): 419–425. https://doi.org/10.1161/STROKEAHA.117.018724.
Kaneko, K., T. Kawasaki, S. Masunari, T. Yoshida, and J. Omagari. 2013. Determinants of extraaortic arterial 18F-FDG accumulation in asymptomatic cohorts: Sex differences in the association with cardiovascular risk factors and coronary artery stenosis. Journal of nuclear medicine: Official publication, Society of Nuclear Medicine 54 (4): 564–570. https://doi.org/10.2967/jnumed.112.111930.
Read, K.A., M.D. Powell, P.W. Mcdonald, and K.J. Oestreich. 2016. IL-2, IL-7, and IL-15: Multistage regulators of CD4(+) T helper cell differentiation. Experimental hematology 44 (9): 799–808. https://doi.org/10.1016/j.exphem.2016.06.003.
Coppola, C., B. Hopkins, S. Huhn, Z. Du, Z. Huang, and W.J. Kelly. 2020. Investigation of the impact from IL-2, IL-7, and IL-15 on the growth and signaling of activated CD4+ T cells. International journal of molecular sciences 21 (21): 7814. https://doi.org/10.3390/ijms21217814.
Osinalde, N., V. Sanchez-Quiles, V. Akimov, B. Guerra, B. Blagoev, and I. Kratchmarova. 2015. Simultaneous dissection and comparison of IL-2 and IL-15 signaling pathways by global quantitative phosphoproteomics. Proteomics 15 (2–3): 520–531. https://doi.org/10.1002/pmic.201400194.
Funding
This work was supported in part by grants from the National Natural Science Foundation of China (Nos. 82160086 and 81960047), China Postdoctoral Science Foundation(2022MD723769), the Science and Technology Fund of Guizhou Province (No. qiankehepingtairencai-GCC[2022]040-1, qiankehezhicheng[2019]2800, qiankehejichu-ZK[2022]zhongdian043, qiankehechengguo-LC[2022]013), the Health and Family Planning Commission of Guizhou Province (qianweijianhan[2021]160), Provincial Key Medical Subject Construction Project of Health Commission of Guizhou Province and the National Key Medical Subject Construction Project of National Health Commission of China, Health Commission of Guizhou Province (gzwkj2021-357).
Author information
Authors and Affiliations
Contributions
Conceptualization, X.L.X., Z.H.L, W.L.; methodology, X.L.X., H.Y.Z; software, X.L.X.; validation, X.L.X., H.Y.Z., Z.G.D., G.W.H.; formal analysis, X.L.X., Y.Z.J.,L,N.; investigation, X.L.X., Z.H.L., L.N., Z.G.D.; resources, W.L.; data curation, Y.Z.J., X.L.X.,Z.G.D., G.W.H.; writing—original draft preparation, X.L.X.; writing—review and editing, X.L.X., Z.H.L., W.L.; supervision, H.Y.Z.; project administration, W.L.; funding acquisition, W.L., Z.H.L. All authors reviewed the manuscript.
Corresponding authors
Ethics declarations
Ethics Approval
This study was performed in accordance with the Declaration of Helsinki. This study was approved by the Ethics Committee of the Affiliated Hospital of Guizhou Medical University. Informed consent was obtained from all participants.
Competing Interests
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Xiong, X., Duan, Z., Zhou, H. et al. The Increased TIGIT-Expressing CD3+CD56+ Cells Are Associated with Coronary Artery Disease and Its Inflammatory Environment. Inflammation 46, 2024–2036 (2023). https://doi.org/10.1007/s10753-023-01859-6
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10753-023-01859-6