Abstract
Background
Anorectal malignant melanoma (ARMM) is a rare disease accounting for less than 1% of primary anorectal malignancies. Here we first present a case of early primary anorectal malignant melanoma completely resected by endoscopic submucosal dissection (ESD).
Methods and results
A 43-year-old woman visited our hospital because of suspected anal melanoma found by routine colonoscopy in her local hospital. Following series of tests including CT, MRI, and whole-body PET-CT did not show any evidence of metastasis. The lesion was removed by the method of ESD in en bloc and no delayed bleeding or perforation occurred. The result of histopathologic examinations confirmed to be malignant melanoma. No recurrence or distant metastases were found during follow-up time (the latest follow-up was 2 years after ESD).
Conclusion
The present case showed endoscopic submucosal dissection that can be an effective and safe alternative treating early primary anorectal malignant melanoma.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Anorectal malignant melanoma (ARMM) is a rare disease accounting for less than 1% of primary anorectal malignancies [1]. Because it is often misdiagnosed for hemorrhoids and difficult to be correctly diagnosed especially in the early stage, anorectal malignant melanoma is thought to have a poor prognosis. The documented 5-year survival rate is 10% and a median survival of 24 months [2]; almost all patients die of metastases. There is still no standard therapy for the treatment of ARMM, and radical surgery is often used as the main method. Until now, there are only two reported cases of ARMM removed by endoscopic mucosal resection (EMR) with a survival time longer than 5 years [3]. Here we first present a case of early primary anorectal malignant melanoma completely resected by endoscopic submucosal dissection (ESD).
Case report
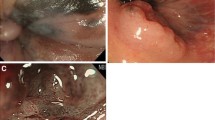
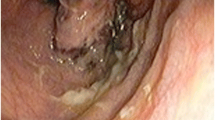
A 43-year-old woman visited our hospital because of suspected anal melanoma found by routine colonoscopy in her local hospital. She was admitted for further examination. No abnormality was found in either physical examination or routine blood tests. Colonoscopy revealed a dark black and longitudinally protrude lesion in the anal, about 1 cm in diameter (Fig. 1). Magnifying chromoendoscopy demonstrated that the surface of the lesion was smooth without ulceration, filled with black objects in submucosa. Following series of tests including CT, MRI, and whole-body PET-CT did not show any evidence of metastasis. The patient as a college teacher refused radical surgery due to fear of reducing her quality of life. Considering the higher curative resection and lower recurrence rate comparing with EMR [4], we performed ESD for her after plenary preoperative preparation. ESD was performed by Dr. Meidong Xu in a surgical operation room. The whole procedure cost about 20 min and was similar to ESD for other lesions in the rectum. The lesion was removed in en bloc and no delayed bleeding or perforation occurred (Fig. 2). The resected specimen was 1.5 cm in diameter (Fig. 3). The result of histopathologic examinations confirmed to be malignant melanoma showing large number of pigment-rich larger tumor cells arranged in nest; they were overt or spindle-shaped and confined to the mucosa (Fig. 4). The tumor was 1 mm in thickness with negative margins. Immunohistochemical staining showed tumor cells were positive for A103, and weakly positive for HMB-45.
The patient was discharged after two days and did not receive any additional treatment. Follow-up including CT-scan and colonoscopy was arranged every 3–6 months, and no recurrence or distant metastases were found by the latest follow-up (2 years after ESD) (Fig. 5).
Discussion
Melanoma in the site of anorectum is very rare but lethal, accounting for 0.4–1.6% of all malignant melanomas [5]. Diagnosis is often quite challenging due to its vague presentation. It was often poorly understood and difficult to be rightly diagnosed especially when the lesion was superficial. Due to delayed diagnosis and the aggressive nature of ARMM, 37% of the patients already had distant or regional metastasis at the time of diagnosis [6]. In the present case, melanoma in the anal was fortunately recognized and suspected by an experienced endoscopist outside our hospital.
Though there are various treatment modalities of AMM, including surgical excision, been standardized due to low incidence and lack of evidence. If the melanoma is confined at the anorectal area, abdominoperineal resection (APR) or wide local excision (WLE) is the common option. However, which is the better approach is still a controversial issue. APR is traditionally preferred because it can control lymphatic spread. However, according to the limited retrospective studies, there was no difference in 5-year survival rates between the patients who underwent APR and WLE [7,9,9]. Even it was reported that WLE with successful R0 resection could show better survival than APR. [10] Endoscopic resection was a local resection method. As referring to the method of endoscopic resection, ESD is known to achieve a higher en bloc and R0 resection rate but lower local recurrence rate for the treatment of colorectal tumors compared with EMR [11]. Local recurrence occurred four times in the reported case removed by endoscopic mucosal resection (EMR) alone [12]. In the present case, also no other treatment was involved and no recurrence or metastasis was discovered during 2 years follow-up. Some previous studies proved that both the depth and the size of tumor have a significant effect on the survival rate [7, 13, 14], and thickness less than 2 mm is the major factor for determining long-term survival. In our case, the tumor was about only 1 mm in depth and 3 mm in width without any positive margin based on the pathological finding; a good prognosis with long-term survival is expected.
References
Weinstock MA (1993) Epidemiology and prognosis of anorectal melanoma. Gastroenterology 104:174–178
Solaz Moreno E, Vallalta Morales M, Silla Búrdalo G, Cervera Miguel JI, Díaz Beveridge R, Rayón Martín JM (2005) Primary melanoma of the rectum: an infrequent neoplasia with an atypical presentation. Clin Transl Oncol 7:171–173
Park JH, Lee JR, Yoon HS, Jung TY, Lee EJ, Lim JG, Ko SY, Wang JH, Lee JD, Kim HY (2015) Primary anorectal malignant melanoma treated with endoscopic mucosal resection. Intest Res 13(2):170–174
Fujiya M, Tanaka K, Dokoshi T (2015 Mar) Efficacy and adverse events of EMR and endoscopic submucosal dissection for the treatment of colon neoplasms: a meta-analysis of studies comparing EMR and endoscopic submucosal dissection. Gastrointest Endosc 81(3):583–595
Goldman S, Glimelius B, Pahlman L (1990) Anorectal malignant melanoma in Sweden. Report of 49 patients. Dis Colon Rectum 33:874–877
Taylor JP, Stem M, Yu D (2019) Treatment strategies and survival trends for anorectal melanoma: is it time for a change? World J Surg 43(7):1809–1819
Brady MS, Kavolius JP, Quan SH (1995) Anorectal melanoma. A 64-year experience at Memorial Sloan-Kettering Cancer Center. Dis Colon Rectum 38:146–151
Thibault C, Sagar P, Nivatvongs S, Ilstrup DM, Wolff BG (1997) Anorectal melanoma-- an incurable disease? Dis Colon Rectum 40:661–668
Ross M, Pezzi C, Pezzi T, Meurer D, Hickey R, Balch C (1990) Patterns of failure in anorectal melanoma. A guide to surgical therapy. Arch Surg 125:313–316
Nilsson PJ, Ragnarsson-Olding BK (2010) Importance of clear resection margins in anorectal malignant melanoma. Br J Surg 97:98–103
Wang J, Zhang XH, Ge J, Yang CM, Liu JY, Zhao SL (2014) Endoscopic submucosal dissection vs endoscopic mucosal resection for colorectal tumors: a meta-analysis. World J Gastroenterol 20(25):8282–8287
Tanaka S, Ohta T, Fujimoto T, Makino Y, Murakami I (2008) Endoscopic mucosal resection of primary anorectal malignant melanoma: a case report. Acta Med Okayama 62:421–424
Pessaux P, Pocard M, Elias D, Duvillard P, Avril MF, Zimmerman P, Lasser P (2004) Surgical management of primary anorectal melanoma. Br J Surg 91:1183–1187
Che X, Zhao DB, Wu YK, Wang CF, Cai JQ, Shao YF, Zhao P (2011) Anorectal malignant melanomas: retrospective experience with surgical management. World J Gastroenterol 17:534–539
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
The authors declare that there are no conflicts of interest.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Lian, J., Xu, A., Chu, Y. et al. Early primary anorectal malignant melanoma treated with endoscopic submucosal dissection: a case report. Int J Colorectal Dis 35, 959–961 (2020). https://doi.org/10.1007/s00384-020-03546-6
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00384-020-03546-6