Abstract
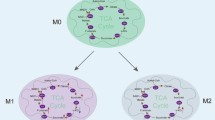
Macrophages are myeloid immune cells, present in virtually all tissues which exhibit considerable functional plasticity and diversity. Macrophages are often subdivided into two distinct subsets described as classically activated (M1) and alternatively activated (M2) macrophages. It has recently emerged that metabolites regulate the polarization and function of macrophages by altering metabolic pathways. These metabolites often cannot freely pass the cell membrane and are therefore transported by the corresponding metabolite transporters. Here, we reviewed how glucose, glutamate, lactate, fatty acid, and amino acid transporters are involved in the regulation of macrophage polarization. Understanding the interactions among metabolites, metabolite transporters, and macrophage function under physiological and pathological conditions may provide further insights for novel drug targets for the treatment of macrophage-associated diseases.
Graphical abstract
In Brief
Recent studies have shown that the polarization and function of macrophages are regulated by metabolites, most of which cannot pass freely through biofilms. Therefore, metabolite transporters required for the uptake of metabolites have emerged seen as important regulators of macrophage polarization and may represent novel drug targets for the treatment of macrophage-associated diseases. Here, we summarize the role of metabolite transporters as regulators of macrophage polarization.

Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Macrophages are a key component of the innate immune system and represent critical players in host defense and tissue homeostasis (Lavin et al. 2015). To carry out these diverse functions appropriately, macrophages exhibit a high functional plasticity and adopt different metabolic states. The two “extremes” of these states are defined as classically activated (M1) and alternatively activated macrophages (M2) (Mulder et al. 2021; Van Dyken and Locksley 2013). M1 and M2 macrophages exert different functions, with M1 (pro-inflammatory) macrophages being generally involving in fighting infections, pathogens, and tumors, while M2 (anti-inflammatory) macrophages exhibit potent capacity for phagocytosis and are thought to repair inflammation-related damage (Udalova et al. 2016). More recent data have suggested that an imbalance of macrophage polarization is present in atherosclerosis, asthma, metabolic disorders and obesity, rheumatoid arthritis (RA), and fibrotic diseases (Murray and Wynn 2011).
It has previously been shown that macrophage polarization is dependent on metabolic reprogramming and alterations in cellular metabolism (O'Neill and Pearce 2016). During the transition from resting state to activation, macrophages require a considerable amount of nutrients to provide energy (Newton et al. 2016). In the last decade, several studies have assessed how the immune metabolism affects macrophage polarization. It is now generally accepted that energy is generated via aerobic glycolysis and the pentose phosphate pathway (PPP) in M1 macrophages, while M2 macrophages mainly rely on oxidative phosphorylation (OXPHOS) and fatty acid oxidation (FAO) (Stunault et al. 2018).
There is now mounting evidence that suggests that cellular metabolites can also alter metabolic pathways. In particular active metabolites are known to mediate essential physiological functions of cells and are the key to cell survival. In addition, they can also influence the cellular microenvironment directly by modifying production and/or consumption of other metabolites (Hotamisligil 2017; Pålsson-McDermott and Diskin 2018). Tabas et al. reported that metabolic pathways of macrophages can be altered following ingestion of metabolites derived from other cells via efferocytosis (Tabas and Bornfeldt 2020). Most metabolites cannot pass freely through the cell membrane and therefore dedicated transporters are required (Hsu and Dzhagalov 2019). Membrane-bound metabolite transporters can mediate the absorption of nutrients and xenobiotics into the cells, thus providing energy for cells (Lin et al. 2015). In this review, we provide an overview of how metabolite transporters impact on macrophage polarization and how metabolite transporters may represent novel drug targets for the treatment of macrophage-associated diseases in the future.
Role of metabolite transporters in macrophage polarization
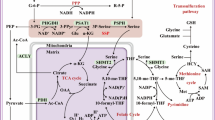
Macrophage activation is accompanied by rapid changes in nutrient flux to meet the energy requirements for immune activation. Previous studies have demonstrated that M1 macrophages do not rely on the citric acid (TCA) cycle to produce ATP but instead generate energy via glycolysis and PPP, while M2 macrophages rely on OXPHOS as well as FAO and undergo the TCA cycle (El Kasmi and Stenmark 2015). Accordingly, metabolic reprogramming in macrophages is not only important to supply the anabolic metabolism with substrates and ATP, but also regulates gene transcription and cell signaling events, and ultimately shapes cell polarization phenotypes. Interestingly, the regulation of cell metabolism and macrophage polarization is jointly realized through metabolite transporters (Hediger et al. 2013). In macrophages, metabolites are transported across the membrane by solute carriers (SLCs), including absorption and outflow of intracellular sugars, amino acids, and nucleotides (Perland and Fredriksson 2017). In addition, SLCs can also transport neurotransmitters and inorganic/metal ions, among other metabolites and nutrients (Zhu et al. 2015). Cells with incorrect transporter expressions may lack anabolic substrates or accumulate metabolites, leading to altered polarization (Fig. 1).
The impact of metabolite transporters on macrophage polarization. Glucose transporter 1 (GLUT1) overexpression, promoting glucose uptake and glycolysis, leads to an M1 phenotype in macrophages which results in the production of large amounts of lactate and transport by monocarboxylate transporters (MCTS). In addition, pyruvate converted from glucose can enter the TCA cycle, where NADH is produced for use in the electron transport chain (ETC). Citrate in the TCA cycle is used for the synthesis of fatty acids (FA), cholesterol, and prostaglandins (PGs). Cholesterol is released into the extracellular space by ATP-binding cassette superfamily (ABC) A1 and ABCG1 transport, which promotes M2 macrophage polarization and reduces the risk of atherosclerosis, while FA taken up by fatty acid transporter 1 (FATP1) transport can also be oxidized to produce NADH. However, overexpression of FATP1 downregulates M1 markers including inducible nitric oxide synthase (iNOS), tumor necrosis factor α (TNF-α), and interleukin-1β (IL-1β) and IL-6. Notably, amino acids (AAs) (transported by l-amino acid transporters 1, LAT1) and glutamate (transported by XCT, SLC7A11) are important to the TCA cycle, and upregulation of LAT1 and XCT promotes M1 macrophage polarization
Glucose transporters and macrophage polarization
Glucose is a large polar molecule which cannot traverse the cellular lipid membrane via diffusion. It is the most important energy source of cells and is transported into cells via glucose transporters, after which it can be converted to ATP by glycolysis or OXPHOS to maintain the energy requirements for survival and growth (Hui et al. 2017). Glucose transporters can be subdivided into two types, including sodium-dependent glucose transporters (SGLTs) and diffusible glucose transporters (GLUTs) (Jurcovicova 2014). At present, the physiological significance of SGLTs is unknown.
The best characterized glucose transporters in macrophages are GLUT1 and GLUT3. GLUT1, also known as solute carrier family 2, facilitated glucose transporter member 1, or SLC2A1, is a critical regulator of glucose metabolism in macrophages (Freemerman et al. 2014), and overexpression of GLUT1 has been shown to promote glucose uptake, resulting in a proinflammatory macrophage phenotype (Freemerman et al. 2014). Furthermore, GLUT1-deficient bone marrow–derived macrophages (BMDMs) exhibited reduced release of pro-inflammatory metabolites such as succinate and showed an increased M2-related biomarkers and anti-inflammatory metabolites such as ornithine and polyamines (Freemerman et al. 2019). Of note, recent studies have shown that glucose uptake and utilization during GLUT1-mediated aerobic glycolysis contribute to efferocytosis (Morioka et al. 2018), i.e., the energy-intensive process of apoptotic cell removal (Doran et al. 2020; Verdone et al. 2015). Generally speaking, macrophages have been shown to promote the resolution of inflammation and tissue repair through efferocytosis (Poon et al. 2014). Interestingly, GLUT1-deficient BMDMs displayed decreased efferocytosis in vitro (Morioka et al. 2018). Further studies revealed that efferocytosis promotes metabolic gene programming of glucose uptake and subsequent glycolysis in phagocytes, downregulating genes associated with OXPHOS and FAO in macrophages (Kelly and O'Neill 2015; Morioka et al. 2018). Collectively, the GLUT1-mediated glycolytic metabolism may be involved in M2 polarization of macrophages, although efferocytic macrophages are more M2-like (Kelly and O'Neill 2015).
GLUT3 is the most abundant glucose transporter in the brain and has a higher affinity for glucose than other glucose transporters (Jurcovicova 2014). GLUT3 is considered to be an independent prognostic marker associated with the expression of inflammatory gene and is thought to induce macrophage activation in part through lactate regulation of C-X‐C motif-chemokine ligand 8 (CXCL8) (Tsai et al. 2021). GLUT6, a low-affinity glucose transporter, can also be expressed in macrophages (Navale and Paranjape 2016). GLUT6 protein was significantly upregulated in LPS-induced inflammatory macrophages, while naive macrophages and IL-4-induced anti-inflammatory macrophages do not express (Caruana et al. 2019). Interestingly, although GLUT6 has been shown to be significantly upregulated in M1 macrophages, glucose uptake or the glycolytic metabolism of M1 macrophage is not altered in GLUT6-knockout mice (Maedera et al. 2019).
Glutamine transporters and macrophage polarization
In addition to the glucose metabolism, macrophages employ glutaminolysis to meet their energetic and biosynthetic demands (Pearce and Pearce 2013). Glutamine is converted to glutamate by deamination and glutamate is then transformed to α-ketoglutarate (α-KG). α-KG is an anti-inflammatory metabolite that not only prevents M1 polarization by inhibiting the activation of IκB kinase-β (IKK-β), but also enhances M2 polarization of macrophages via the α-KG-Jumonji domain-containing 3 (Jmjd3) pathway (Liu et al. 2017). However, not all of the cellular glutamine is used for metabolism. Recent studies have shown following knockdown of glutaminase, the key enzyme converting glutamine to glutamate, glutamine enters the TCA cycle and hexosamine pathways, thereby promoting the anti-inflammatory polarization of macrophages in response to IL-4 stimulation. Conversely, LPS-stimulated inflammatory macrophages do not require glutamate (Jha et al. 2015), and instead, glutamine is transported out of the cell in exchange for essential amino acids (EAAs) that directly activate mTORC1 to promote protein translation and cell growth (Wise and Thompson 2010).
As glutamate is water-soluble, in order to enter the cell, it must be transported across the plasma membrane which is enabled by a variety of transporters. Glutamine transporters are subdivided into in four main families: SLC1, SLC6, SLC7, and SLC38 (Bhutia and Ganapathy 2016). Several glutamate transporter systems have been identified, including Na ( +)-dependent excitatory amino acid transporters (EAATs), the Xc– transport system, and the XAG system (Grewer and Rauen 2005; Noda et al. 1999). Both EAATS and XAG transport systems are Na ( +)-dependent, while the anionic amino acid exchange Xc– transport system is Na ( +)-independent. The main component of the Xc– transport system, XCT (SLC7A11), is induced by LPS in macrophages (Kobayashi et al. 2018), and the Xc– transport system is highly specific for l-glutamate and l-cystine(La Bella et al. 2007). It has been reported that LPS induces the activity of cystine transport mediated by system Xc– and upregulates the expression of cystine/glutamine transporter XCT/SLC7A11, promoting the conversion of cystine to cysteine and finally enabling the synthesis of glutathione (GSH) in mouse peritoneal macrophages (Sato et al. 1995; Bannai et al. 1991). In line with this, recent studies have demonstrated that increased activity of the XCT upregulates GSH levels, protecting cells from oxidative stress damage and maintaining the mercaptan redox state in macrophages (Song et al. 2020). Also, GSH promotes M1 polarization and enhances the immune activity through the potential ROS scavenging (Kwon et al. 2019). A high extracellular glutamate concentration inhibits cystine uptake via XCT, which in turn blocks GSH synthesis and induces oxidative stress–mediated cell death (Guo et al. 2021).
Lactate transporters and macrophage polarization
During glycolysis, one glucose molecule is converted to pyruvate two molecules, which are in turn converted to lactate by the cytoplasmic lactate dehydrogenase (LDH) (Rogatzki et al. 2015). Lactate is a pro-inflammatory signaling molecule, lactate promoting inflammation by increasing the expression of inflammatory genes and enhancing LPS-induced TLR4 and NF-κB signaling (Samuvel et al. 2009). In line with this, lactate has been shown to increase the activity of LPS-stimulated monocyte matrix metalloproteinases and release of IL-1β in obesity and type 1 diabetes (Nareika et al. 2005). Shime et al. found that lactate enhanced the expression of antigen-dependent IL-17A during co-culture of CD4( +) T cells and BMDM (Shime et al. 2008). However, although lactate is primarily thought of as a pathological metabolite marker, recent studies have demonstrated that lactate can also act as a modulator of immune cell metabolism capable of reducing inflammation and representing a negative feedback signal high level of glycolysis, thereby alleviating the excessive inflammatory responses of pro-inflammatory immune cells (Hoque et al. 2014; Ratter et al. 2018). Zhang et al. found that in the late phases of inflammatory macrophage polarization, lactate could induce expression of genes involved in wound healing, such as arginase-1 (Arg1), via histone lactylation (Zhang et al. 2019a). Moreover, there is a fast-growing body evidence demonstrating that lactate produced by tumor cells can influence M2 polarization of macrophages in the tumor microenvironment (TME) (Spencer and Stanton 2019). For example, in human head and neck squamous cell carcinoma, lactate promotes the induction of an M2-like macrophage polarization by inhibiting LDH and GLUT1 expression, as well as the resulting increased secretion of vascular endothelial growth factor, via induction of hypoxia inducible factor-1α (HIF-1α) (Colegio et al. 2014; Ohashi et al. 2017). Importantly, efferocytic phagocytes have been shown to promote an anti-inflammatory phenotype in surrounding non-engulfing naive macrophages toward via lactate transporter-mediated lactate release, as well as anti-inflammatory factors, such as IL-10, released in the tissue microenvironment during efferocytosis (Han et al. 2016).
The effects of lactate on macrophages are predominantly mediated by proton-bound monocarboxylate transporters (MCTs) (Moreira et al. 2009). The MCT family, or solute carrier family 16 (SLC16), comprises 14 members, of which only the first four have been proven to be involved in the transport of lactate, including SLC16A1 (MCT1), SLC16A3 (MCT4), SLC16A7 (MCT2), and SLC16A8 (MCT3) (Halestrap 2013; Halestrap and Meredith 2004). In mammalian cells, these 4 subtypes exhibit functions related to the uptake and flux of lactate across the membrane (Halestrap and Meredith 2004). Previous work showed that macrophages have a higher expression of MCT1 and MCT4 than MCT2 (Imai et al. 2019). In high lactate microenvironments, MCT1 and MCT2 enable cellular lactate uptake, while MCT4 mediates lactate output (Contreras-Baeza et al. 2019; Diehl et al. 2018). MCT2 has been shown to have a higher affinity to lactate than MCT1 (Halestrap and Meredith 2004).
Crucially, MCTs are important regulators of glycolysis. Liang et al. found that MCT1 promoted classical microglial activation and MCT1 knockout reduced the rate of glycolysis as well as the expression of LPS-induced inflammatory markers, including inducible nitric oxide synthase (iNOS), interleukin-1β (IL-1β), and IL-6 (Kong et al. 2019). MCT4 contributes to the maintenance of the expression of glycolytic and pro-inflammatory mediators in TLR4 agonist activated macrophages (Tan et al. 2015).
Fatty acid transporters and macrophage polarization
In mammals, there are two key sources of fatty acids (FAs): food and endogenous synthesis (i.e., de novo synthesis). The OXPHOS of FAs produces large amounts of ATP and represents an important energy source of M2 macrophages (Malandrino et al. 2015). Recent work showed that LPS increases fatty acid synthesis (FAS) in macrophages and promotes inflammation (Posokhova et al. 2008). However, enhanced FAO in macrophages not only reduces the accumulation of lipids, but also reduces the production of inflammatory cytokines regulating macrophage inflammation (Malandrino et al. 2015). As described above, in addition to recognition and clearance of apoptotic cells (ACs), efferocytosis induces the production of anti-inflammatory and tissue-restorative cytokines. A recent study has moreover shown that following an injury, IL-10 is upregulated during macrophage efferocytosis. This upregulation was not associated with glycolysis; instead, it was related to an increased FAO and the ETC of apoptotic cells, leading to M2 macrophage polarization and promoting tissue repair (Zhang et al. 2019b).
FAs are insoluble in water and therefore have to be imported into the mitochondria by members of the fatty acid transporter (FATP) family. The FATP family is composed of six isoforms, with FATP1 (SLC27A1) representing the most important subtype capable of mediating macrophage polarization (Nishiyama et al. 2018). FATP1 is an acyl-CoA synthase that inhibits macrophage inflammation by regulating lipid mediators and oxidative stress (Zhao et al. 2017), and it has been shown that the glucose metabolism is increased in FATP1 knockout mice, resulting in a pro-inflammatory macrophage proinflammatory (Johnson et al. 2016). Conversely, FATP1 overexpression has been shown to reduce glycolysis and decrease the production of iNOS, tumor necrosis factor-α (TNF-α), IL-6, and IL-1β, thereby alleviating M1 macrophage–mediated inflammation (Johnson et al. 2016). Taken together, FATP1 acts as an important regulator of inflammatory signaling in macrophages.
Amino acid transporters and macrophage polarization
Amino acids (AAs) are the main components for protein synthesis and thereby constitute essential nutrients for all living cells. The cellular catabolism of AAs can be used for the production of ATP or act as a source of citric acid for the synthesis of fatty acids; it can also be used to maintain the immune activity of macrophages (Pålsson-McDermott and Diskin 2018). Early evidence suggested that macrophages may inhibit tumor growth by Arg consumption and subsequent production of nitric oxide (NO), which prevents the repolarization of M1 to M2 macrophages (Currie 1978; Mills 1991). Moreover, as mentioned earlier, the clearance of ACs, during which macrophages take up arginine and ornithine, promotes injury regression (Arandjelovic and Ravichandran 2015). Macrophages metabolize arginine and ornithine to putrescine via Arg1 and ornithine decarboxylase (ODC), which introduces sustained efferocytosis and thereby inhibits inflammation and promotes tissue repair (Yurdagul et al. 2020). In addition, it has been recently reported that ODC inhibits M1 activation and macrophage antimicrobial activity via histone and chromatin modifications (Hardbower et al. 2017). Das et al. (2010) found that a variety of pathogens compete with iNOS for arginine and prevent NO production by an increased in Arg expression. In general, the AA metabolism during macrophage efferocytosis may provide novel therapeutic strategies for intervention in over-responsive or persistent inflammation. Importantly, current studies suggest that the AA metabolism is closely related to amino acid transporters (AATs).
AATs are membrane-bound transport proteins, most of which belong to the group of SLCs and are involved in nutrient uptake, cell signaling pathways, and the cell redox balance (Broer and Palacin 2011). Eleven members of the SLC family have been shown to represent AATs, including SLC1, SLC3, SLC6, SLC7, SLC15, SLC17, SLC18, SLC25, SLC32, SLC36, and SLC38 (Schweikhard and Ziegler 2012). The SLC7 family is further divided into two subfamilies, l-amino acid transporters (LATs) and cationic amino acid transporters (CATs) (Fotiadis et al. 2013). It has been shown that SLC7A5 (LAT1, l-amino acid transporter 1) is a key solute transporter in macrophages, and has the been shown to be expressed higher in M1 than in M2 macrophages (Martinez et al. 2006). Increased LAT1 expression mediates leucine influx and enhances mTORC1-induced glycolysis, thereby elevating the production of pro-inflammatory IL-1β in macrophages (Yoon et al. 2018). Conversely, macrophage downregulation of LAT1 significantly decreased levels of IL-1β (Yoon et al. 2018). Interestingly, the expression of LAT1 in peripheral blood monocytes of RA patients has been shown to be significantly higher than that in healthy controls (Yoon et al. 2018). Thus, LAT1 can serve as an important indicator of inflammatory macrophages.
The other subfamily of SLC7 transporters, the cationic amino acid transporters 1–4 (CAT1-4), is responsible for the transport of extracellular l-Arg into cells (Bronte and Zanovello 2005). CAT2 is a key protein regulating the uptake of l-Arg by macrophages, and its expression is elevated in activated macrophages in vitro (Barry et al. 2011). Moreover, the synthesis of NO mediated by iNOS in M1 macrophages is dependent on CAT2 (Nicholson et al. 2001).
Cholesterol transporters and macrophage polarization
Cholesterol is the most abundant steroid compound in the body. It is not only an essential structural component of cell membranes, but is also the raw material for the synthesis of bile acids and steroids (Narwal et al. 2019). However, a cellular accumulation of cholesterol may cause hypercholesterolemia and lead to atherosclerosis (Groh et al. 2018). Cholesterol exits macrophages predominantly via ATP-binding cassette superfamily (ABCs) transporters which regulate intracellular cholesterol homeostasis, including ABCA1 and ABCG1 (Klaassen and Aleksunes 2010; Phillips 2014). Approximately two-third of the cellular cholesterol efflux are regulated by ABCA1 (Phillips 2014). Significantly, recent studies have shown that activation of central regulators of lipid homeostasis, liver X receptors (LXRs) LXRα and LXRβ, upregulates the expression of ABCA1 and ABCG1, thereby stimulating cholesterol efflux from macrophages and promoting M2 macrophage polarization and reducing the atherosclerosis risk (Venkateswaran et al. 2000; Janowski et al. 1999; Schwartz et al. 2000). On the other hand, Sag et al. found that ABCG1-deficient macrophages transition from M2 polarization to anti-tumoral M1 macrophages and exhibited an increased NF-κB activation in vitro (Sag et al. 2015).
The significance of metabolite transport for macrophage polarization and cellular communication
Metabolites can not only interact with the environment to coordinate cellular metabolism but also act as signaling molecules modifying gene expression and can thereby play an important role in cell survival, differentiation, and function (Curi et al. 2017). As a consequence, the transport of metabolites is critical for both the regulation of macrophage polarization and the communication between macrophages and other cells (Fig. 2).
Significance of metabolite transport in macrophage polarization and communication with other cells. Prostaglandin E2 (PGE2) secreted by macrophages is transported to the extracellular space by OATP2A1/SLCO2A1 and binds to EP4 receptor expressed on neutrophils, inhibiting inflammation. In addition, the pro-inflammatory mediator succinate is produced and released by M1 macrophages. Succinate binds to the specific succinate receptor 1 (SUCNR1)/GPR91 on NSCs and induces expression of succinate transporters SLC13A3 and SLC13A5, thereby increasing extracellular succinate uptake and reducing inflammation. Notably, lactate derived from tumor cells and endothelial cells is taken up by macrophages via MCTs, promoting M2 polarization
Prostaglandin E2 (PGE2) is an effective immune regulator that can be secreted by macrophages and is transported into the extracellular space via OATP2A1/SLCO2A1 (Shimada et al. 2015), and it has been reported that the amount of PGE2 secreted from macrophages is significantly reduced in LPS-activated macrophages deficient for OATP2A1 compared to controls (Shimada et al. 2015). Interestingly, although PGE2 is generally considered a pro-inflammatory factor, it has also been shown to exhibit certain anti-inflammatory properties (Scher and Pillinger 2009). For instance, under inflammatory conditions, PGE2 released into the extracellular space by OATP2A1 binds to neutrophil EP4 receptors and removes neutrophils from inflammatory tissues, inhibiting inflammation (Loynes et al. 2018; Yamane et al. 2000).
Succinate, produced and released by M1 macrophages, is a highly pro-inflammatory mediator that results in upregulation of IL-1β and induces a glycolytic metabolism in macrophages via stabilization and activation of HIF-1α (Murphy and O'Neill 2018; Tannahill et al. 2013). Succinate is released into the extracellular space and binds to the G-protein-coupled receptor (GPR) 91, which is highly expressed on dendritic cells (DCs), acting synergistically with TLRs (Rubic et al. 2008). Recently, it was found that the release of succinate by classically activated macrophages activate specific succinate receptor 1 (SUCNR1)/GPR91 on NSCs, inducing the expression of succinate transporters SLC13A3 and SLC13A5 on NSCs (Gonzalez et al. 2016; Peruzzotti-Jametti et al. 2018). These transporters increase the uptake of extracellular succinate and thereby reduce succinate-mediated inflammation. In line with this, LPS-induced macrophages were shown to be reprogrammed toward an OXPHOS M2 phenotype when co-cultured with NSCs (Peruzzotti-Jametti et al. 2018).
As mentioned above, lactate is an active metabolite capable of inducing metabolic reprogramming and modifying the phenotype and function of macrophages. An increasing body of literature demonstrates increased levels of lactate secreted by tumor cells into the tumor microenvironment influence macrophage polarization as part of the Warburg effect (Domingo-Vidal et al. 2019; Stone et al. 2019). Zhang et al. (2020) recently found that endothelial cells release lactate via MCT4 and macrophages take it up via MCT1, after which it induces an anti-inflammatory phenotype and promotes muscle regeneration. Conversely, Stone et al. demonstrated that the conversion of cervical TAM to the M1 phenotype can be promoted by blocking either lactate synthesis or transport in cervical tumor cells (Stone et al. 2019).
Metabolite transporters as drug targets
Recent data indicate that 50% of SLC family members are related to human diseases (Cesar-Razquin et al. 2015). Significantly, there is accumulating evidence suggesting that metabolite transporters are involved in the etiology of a variety of metabolic and autoimmune diseases linked to macrophages due to their involvement in the transport of various metabolites, such as glucose, AAs, vitamins, neurotransmitters, and inorganic/metal ions (Borst and Elferink 2002; Zhang et al. 2019c). Based on the importance of metabolic requirements for macrophage polarization, metabolite transporters have become attractive targets for the regulation of macrophage polarization and the immune response (Table 1).
A prime example is the FA transporter GPR84, which is highly expressed in LPS-stimulated macrophages and is currently being investigated as a potential target for the treatment of fibrosis and metabolic diseases (Yin et al. 2020). PBI-4547, a GPR84 antagonist, has been shown to significantly increase the glucose and lipid metabolism and thereby reduce non-alcoholic fatty liver disease (NAFLD) scores (Simard et al. 2020). Another GPR84 antagonist, PBI-4050, has also been shown to reduce the expression of fibrotic and inflammatory markers and prevents the activation of fibroblast into pro-fibrotic myofibroblasts as well as inflammatory macrophage activation (Grouix et al. 2018). PBI-4050 has now entered phase II clinical trials as a lead drug candidate (Khalil et al. 2019).
ATP-binding cassette transporter A1 (ABCA1) is involved in the cellular cholesterol export and is highly expressed in liver- and other tissue-resident macrophages (Lawn et al. 2001). It has become an important new target for the removal of cholesterol from arterial macrophages and the treatment of atherosclerotic cardiovascular disease (CVD) (Oram and Vaughan 2006). ABCA1 is regulated by the expression and activity of liver X receptor α (LXRα) and peroxisome proliferator activated receptor γ (PPARγ) (Soumian et al. 2005). Previously, PPARγ agonists like the glitazones used in type 2 diabetes and LXR agonists (TO901317 and GW3965) have been shown to ameliorate atherosclerosis via upregulation transcription of ABCA1 and induction of cholesterol extravasation from macrophages in mouse models (Cabrero et al. 2003; Miao et al. 2004; Oram and Heinecke 2005; Joseph et al. 2002). Due to limitations of first-generation LXR agonists, the development and production of LXR agonists that effectively and selectively induce ABCA1 and other cholesterol transporters remains a major challenge (Repa et al. 2000).
In addition to the abovementioned therapeutic functions, metabolite transporters also represent potential cancer targets. The TME has been suggested to play a crucial role in carcinogenesis (Korniluk et al. 2017). Of note, a growing number of studies have shown that TAMs in the TME are involved in tumor progression and metastasis, and may therefore represent attractive therapeutic targets (Singh et al. 2017; Xu et al. 2018). Colegio et al. reported that the uptake of tumor-derived lactate by TAMS in the TME is mediated by MCT1, which promotes an M2 polarization (Colegio et al. 2014). AR-C155858 is a novel class of MCT1 inhibitor developed by AstraZeneca which inhibits the uptake of lactate, thereby inhibiting glycolysis (Guan et al. 2018). Taken together, the abovementioned findings emphasize the potential of metabolite transporters as immunoregulatory and cancer therapeutic targets.
Conclusions
Metabolite transporters are involved in modifying macrophage polarization. This review summarized the roles of metabolic transporters in macrophage polarization and macrophage-associated diseases. As evident from the presented literature, the immunometabolism is key for determining immunophenotypes and responses. The regulation of metabolite transporters has emerged as an attractive target for the manipulation of macrophage phenotypes and functions. Unfortunately, many SLC transporters currently lack crystallographic data and are known as orphan transporters, whose endogenous functions and substrates are unknown. It is likely that future studies will investigate these orphan SLCs. With a further understanding of metabolite transporters, more detailed knowledge of the pathogenesis and prevention of diseases associated with an imbalance of macrophage polarization will emerge and provide insights for new therapeutic targets.
Availability of data and materials
Literature and figures are available upon request.
Abbreviations
- PPP:
-
Pentose phosphate metabolism pathways
- OXPHOS:
-
Oxidative phosphorylation
- FAO:
-
Fatty acid oxidation
- SLCs:
-
Solute carriers
- GLUT1:
-
Glucose transporter 1
- MCTs:
-
Monocarboxylate transporters
- ETC:
-
Electron transport chain
- PGs:
-
Prostaglandins
- ABC:
-
ATP-binding cassette superfamily
- FA:
-
Fatty acids
- FATP1:
-
Fatty acid transporter 1
- iNOS:
-
Inducible nitric oxide synthase
- HIF-1α:
-
Hypoxia-inducible factor-1α
- TNF-α:
-
Tumor necrosis factor α
- IL-1β:
-
Interleukin-1β
- NO:
-
Nitric oxide
- Arg1:
-
Arginase-1
- ODC:
-
Ornithine decarboxylase
- AAs:
-
Amino acids
- LAT1:
-
L-Amino acid transporters 1
- EAAs:
-
Essential amino acids
- SGLTs:
-
Sodium-dependent glucose transporters
- α-KG:
-
α-Ketoglutarate
- IKK-β:
-
IκB kinase-β
- EAATs:
-
Excitatory amino acid transporters
- GSH:
-
Glutathione
- TME:
-
Tumor microenvironment
- LDHA:
-
Lactate dehydrogenase
- PGE2:
-
Prostaglandin E2
- GPR91:
-
G-protein-coupled receptor 91
- CVD:
-
Cardiovascular disease
References
Arandjelovic S, Ravichandran KS (2015) Phagocytosis of apoptotic cells in homeostasis. Nat Immunol 16(9):907–917. https://doi.org/10.1038/ni.3253
Bannai S, Sato H, Ishii T, Taketani S (1991) Enhancement of glutathione levels in mouse peritoneal macrophages by sodium arsenite, cadmium chloride and glucose glucose oxidase. Biochim Biophys Acta 1092(2):1175–179. https://doi.org/10.1016/0167-4889(91)90153-o
Barry DP, Asim M, Scull BP et al (2011) Cationic amino acid transporter 2 enhances innate immunity during Helicobacter pylori infection. PLoS One 6(12):e29046. https://doi.org/10.1371/journal.pone.0029046
Bhutia YD, Ganapathy V (2016) Glutamine transporters in mammalian cells and their functions in physiology and cancer. Biochim Biophys Acta 1863(10):2531–2539. https://doi.org/10.1016/j.bbamcr.2015.12.017
Borst P, Elferink RO (2002) Mammalian ABC transporters in health and disease. Annu Rev Biochem 71:537–592. https://doi.org/10.1146/annurev.biochem.71.102301.093055
Broer S, Palacin M (2011) The role of amino acid transporters in inherited and acquired diseases. Biochem J 436(2):193–211. https://doi.org/10.1042/BJ20101912
Bronte V, Zanovello P (2005) Regulation of immune responses by L-arginine metabolism. Nat Rev Immunol 5(8):641–654. https://doi.org/10.1038/nri1668
Cabrero A, Cubero M, Llaverias G et al (2003) Differential effects of peroxisome proliferator-activated receptor activators on the mRNA levels of genes involved in lipid metabolism in primary human monocyte-derived macrophages. Metabolism 52(5):652–657. https://doi.org/10.1053/meta.2003.50100
Caruana BT, Byrne FL, Knights AJ, Quinlan KGR, Hoehn KL (2019) Characterization of glucose transporter 6 in lipopolysaccharide-induced bone marrow-derived macrophage function. J Immunol 202(6):1826–1832. https://doi.org/10.4049/jimmunol.1801063
Cesar-Razquin A, Snijder B, Frappier-Brinton T et al (2015) A call for systematic research on solute carriers. Cell 162(3):478–487. https://doi.org/10.1016/j.cell.2015.07.022
Chen LH, Zhang Q, Xie X, Nan FJ (2020) Modulation of the G-protein-coupled receptor 84 (GPR84) by agonists and antagonists. J Med Chem 63(24):15399–15409. https://doi.org/10.1021/acs.jmedchem.0c01378
Colegio OR, Chu NQ, Szabo AL et al (2014) Functional polarization of tumour-associated macrophages by tumour-derived lactic acid. Nature 513(7519):559–563. https://doi.org/10.1038/nature13490
Contreras-Baeza Y, Sandoval PY, Alarcon R et al (2019) Monocarboxylate transporter 4 (MCT4) is a high affinity transporter capable of exporting lactate in high-lactate microenvironments. J Biol Chem 294(52):20135–20147. https://doi.org/10.1074/jbc.RA119.009093
Curi R, de Siqueira MR, de Campos Crispin LA, Norata GD, Sampaio SC, Newsholme P (2017) A past and present overview of macrophage metabolism and functional outcomes. Clin Sci (Lond) 131(12):1329–1342. https://doi.org/10.1042/CS20170220
Currie GA (1978) Activated macrophages kill tumour cells by releasing arginase. Nature 273(5665):758–759. https://doi.org/10.1038/273758a0
Das P, Lahiri A, Lahiri A, Chakravortty D (2010) Modulation of the arginase pathway in the context of microbial pathogenesis: a metabolic enzyme moonlighting as an immune modulator. PLoS Pathog 6(6):e1000899. https://doi.org/10.1371/journal.ppat.1000899
Diehl K, Dinges LA, Helm O et al (2018) Nuclear factor E2-related factor-2 has a differential impact on MCT1 and MCT4 lactate carrier expression in colonic epithelial cells: a condition favoring metabolic symbiosis between colorectal cancer and stromal cells. Oncogene 37(1):39–51. https://doi.org/10.1038/onc.2017.299
Domingo-Vidal M, Whitaker-Menezes D, Martos-Rus C et al (2019) Cigarette smoke induces metabolic reprogramming of the tumor stroma in head and neck squamous cell carcinoma. Mol Cancer Res 17(9):1893–1909. https://doi.org/10.1158/1541-7786.MCR-18-1191
Doran AC, Yurdagul A Jr, Tabas I (2020) Efferocytosis in health and disease. Nat Rev Immunol 20(4):254–267. https://doi.org/10.1038/s41577-019-0240-6
El Kasmi KC, Stenmark KR (2015) Contribution of metabolic reprogramming to macrophage plasticity and function. Semin Immunol 27(4):267–275. https://doi.org/10.1016/j.smim.2015.09.001
Fotiadis D, Kanai Y, Palacin M (2013) The SLC3 and SLC7 families of amino acid transporters. Mol Aspects Med 34(2–3):139–158. https://doi.org/10.1016/j.mam.2012.10.007
Freemerman AJ, Johnson AR, Sacks GN et al (2014) Metabolic reprogramming of macrophages: glucose transporter 1 (GLUT1)-mediated glucose metabolism drives a proinflammatory phenotype. J Biol Chem 289(11):7884–7896. https://doi.org/10.1074/jbc.M113.522037
Freemerman AJ, Zhao L, Pingili AK et al (2019) Myeloid Slc2a1-deficient murine model revealed macrophage activation and metabolic phenotype are fueled by GLUT1. J Immunol 202(4):1265–1286. https://doi.org/10.4049/jimmunol.1800002
Gonzalez R, Hamblin MH, Lee J-P (2016) Neural stem cell transplantation and CNS diseases. CNS Neurol Disord Drug Targets 15(8):881–886. https://doi.org/10.2174/1871527315666160815164247
Grewer C, Rauen T (2005) Electrogenic glutamate transporters in the CNS: molecular mechanism, pre-steady-state kinetics, and their impact on synaptic signaling. J Membr Biol 203(1):1–20. https://doi.org/10.1007/s00232-004-0731-6
Groh L, Keating ST, Joosten LAB, Netea MG, Riksen NP (2018) Monocyte and macrophage immunometabolism in atherosclerosis. Semin Immunopathol 40(2):203–214. https://doi.org/10.1007/s00281-017-0656-7
Grouix B, Sarra-Bournet F, Leduc M et al (2018) PBI-4050 reduces stellate cell activation and liver fibrosis through modulation of intracellular ATP levels and the liver kinase B1/AMP-activated protein kinase/mammalian target of rapamycin pathway. J Pharmacol Exp Ther 367(1):71–81. https://doi.org/10.1124/jpet.118.250068
Guan X, Bryniarski MA, Morris ME (2018) In vitro and in vivo efficacy of the monocarboxylate transporter 1 inhibitor AR-C155858 in the murine 4T1 breast cancer tumor model. AAPS J 21(1):3. https://doi.org/10.1208/s12248-018-0261-2
Guo W, Li K, Sun B et al (2021) Dysregulated glutamate transporter SLC1A1 propels cystine uptake via Xc(-) for glutathione synthesis in lung cancer. Cancer Res 81(3):552–566. https://doi.org/10.1158/0008-5472.CAN-20-0617
Halestrap AP (2013) The SLC16 gene family - structure, role and regulation in health and disease. Mol Aspects Med 34(2–3):337–349. https://doi.org/10.1016/j.mam.2012.05.003
Halestrap AP, Meredith D (2004) The SLC16 gene family-from monocarboxylate transporters (MCTs) to aromatic amino acid transporters and beyond. Pflugers Arch 447(5):619–628. https://doi.org/10.1007/s00424-003-1067-2
Han CZ, Juncadella IJ, Kinchen JM et al (2016) Macrophages redirect phagocytosis by non-professional phagocytes and influence inflammation. Nature 539(7630):570–574. https://doi.org/10.1038/nature20141
Hardbower DM, Asim M, Luis PB et al (2017) Ornithine decarboxylase regulates M1 macrophage activation and mucosal inflammation via histone modifications. Proc Natl Acad Sci U S A 114(5):E751–E760. https://doi.org/10.1073/pnas.1614958114
Hediger MA, Clemencon B, Burrier RE, Bruford EA (2013) The ABCs of membrane transporters in health and disease (SLC series): introduction. Mol Aspects Med 34(2–3):95–107. https://doi.org/10.1016/j.mam.2012.12.009
Hoque R, Farooq A, Ghani A, Gorelick F, Mehal WZ (2014) Lactate reduces liver and pancreatic injury in Toll-like receptor- and inflammasome-mediated inflammation via GPR81-mediated suppression of innate immunity. Gastroenterology 146(7):1763–1774. https://doi.org/10.1053/j.gastro.2014.03.014
Hotamisligil GS (2017) Foundations of immunometabolism and implications for metabolic health and disease. Immunity 47(3):406–420. https://doi.org/10.1016/j.immuni.2017.08.009
Hsu C-L, Dzhagalov IL (2019) Metabolite transporters—the gatekeepers for T cell metabolism. Immunometabolism 1:e190012. https://doi.org/10.20900/immunometab20190012
Hui S, Ghergurovich JM, Morscher RJ et al (2017) Glucose feeds the TCA cycle via circulating lactate. Nature 551(7678):115–118. https://doi.org/10.1038/nature24057
Imai H, Yoshimura K, Miyamoto Y et al (2019) Roles of monocarboxylate transporter subtypes in promotion and suppression of osteoclast differentiation and survival on bone. Sci Rep 9(1):15608. https://doi.org/10.1038/s41598-019-52128-2
Janowski BA, Grogan MJ, Jones SA, Wisely GB, Kliewer SA, Corey EJ, Mangelsdorf DJ (1999) Structural requirements of ligands for the oxysterol liver X receptors LXRalpha and LXRbeta. Proc Natl Acad Sci U S A:266–271. https://doi.org/10.1073/pnas.96.1.266
Jha AK, Huang Stanley C-C, Sergushichev A et al (2015) Network integration of parallel metabolic and transcriptional data reveals metabolic modules that regulate macrophage polarization. Immunity 42(3):419–430. https://doi.org/10.1016/j.immuni.2015.02.005
Johnson AR, Qin Y, Cozzo AJ et al (2016) Metabolic reprogramming through fatty acid transport protein 1 (FATP1) regulates macrophage inflammatory potential and adipose inflammation. Mol Metab 5(7):506–526. https://doi.org/10.1016/j.molmet.2016.04.005
Joseph SB, McKilligin E, Pei L, Watson MA, Collins AR, Laffitte BA, Chen M, Noh G, Goodman J, Hagger GN, Tran J, Tippin TK, Wang X, Lusis AJ, Hsueh WA, Law RE, Collins JL, Willson TM, Tontonoz P (2002) Synthetic LXR ligand inhibits the development of atherosclerosis in mice. Proceedings of the National Academy of Sciences 99(11):7604–7609. https://doi.org/10.1073/pnas.112059299
Jurcovicova J (2014) Glucose transport in brain - effect of inflammation. Endocr Regul 48(1):35–48. https://doi.org/10.4149/endo_2014_01_35
Kelly B, O’Neill LA (2015) Metabolic reprogramming in macrophages and dendritic cells in innate immunity. Cell Res 25(7):771–784. https://doi.org/10.1038/cr.2015.68
Khalil N, Manganas H, Ryerson CJ et al (2019) Phase 2 clinical trial of PBI-4050 in patients with idiopathic pulmonary fibrosis. Eur Respir J 53(3). https://doi.org/10.1183/13993003.00663-2018
Klaassen CD, Aleksunes LM (2010) Xenobiotic, bile acid, and cholesterol transporters: function and regulation. Pharmacol Rev 62(1):1–96. https://doi.org/10.1124/pr.109.002014
Kobayashi S, Hamashima S, Homma T et al (2018) Cystine/glutamate transporter, system xc(-), is involved in nitric oxide production in mouse peritoneal macrophages. Nitric Oxide 78:32–40. https://doi.org/10.1016/j.niox.2018.05.005
Kong L, Wang Z, Liang X, Wang Y, Gao L, Ma C (2019) Monocarboxylate transporter 1 promotes classical microglial activation and pro-inflammatory effect via 6-phosphofructo-2-kinase/fructose-2, 6-biphosphatase 3. J Neuroinflamm 16(1). https://doi.org/10.1186/s12974-019-1648-4
Korniluk A, Koper O, Kemona H, Dymicka-Piekarska V (2017) From inflammation to cancer. Ir J Med Sci 186(1):57–62. https://doi.org/10.1007/s11845-016-1464-0
Kwon DH, Lee H, Park C et al. (2019) Glutathione induced immune-stimulatory activity by promoting M1-Like macrophages polarization via potential Ros scavenging capacity. Antioxidants (Basel) 8(9). https://doi.org/10.3390/antiox8090413
La Bella V, Valentino F, Piccoli T, Piccoli F (2007) Expression and developmental regulation of the cystine/glutamate exchanger (xc-) in the rat. Neurochem Res 32(6):1081–1090. https://doi.org/10.1007/s11064-006-9277-6
Lavin Y, Mortha A, Rahman A, Merad M (2015) Regulation of macrophage development and function in peripheral tissues. Nat Rev Immunol 15(12):731–744. https://doi.org/10.1038/nri3920
Lawn RM, Wade DP, Couse TL, Wilcox JN (2001) Localization of human ATP-binding cassette transporter 1 (ABC1) in normal and atherosclerotic tissues. Arterioscler Thromb Vasc Biol 21(3):378–385. https://doi.org/10.1161/01.atv.21.3.378
Lee TM, Chang NC, Lin SZ (2017) Dapagliflozin, a selective SGLT2 Inhibitor, attenuated cardiac fibrosis by regulating the macrophage polarization via STAT3 signaling in infarcted rat hearts. Free Radic Biol Med 104:298–310. https://doi.org/10.1016/j.freeradbiomed.2017.01.035
Leite DF, Echevarria-Lima J, Ferreira SC, Calixto JB, Rumjanek VM (2007) ABCC transporter inhibition reduces zymosan-induced peritonitis. J Leukoc Biol 82(3):630–637. https://doi.org/10.1189/jlb.0107042
Lin L, Yee SW, Kim RB, Giacomini KM (2015) SLC transporters as therapeutic targets: emerging opportunities. Nat Rev Drug Discov 14(8):543–560. https://doi.org/10.1038/nrd4626
Liu P-S, Wang H, Li X et al (2017) α-ketoglutarate orchestrates macrophage activation through metabolic and epigenetic reprogramming. Nat Immunol 18(9):985–994. https://doi.org/10.1038/ni.3796
Loynes CA, Lee JA, Robertson AL, MJG Steel et al (2018) PGE 2 production at sites of tissue injury promotes an anti-inflammatory neutrophil phenotype and determines the outcome of inflammation resolution in vivo. Sci Adv 4(9):eaar8320. https://doi.org/10.1126/sciadv.aar8320
Maedera S, Mizuno T, Ishiguro H, Ito T, Soga T, Kusuhara H (2019) GLUT6 is a lysosomal transporter that is regulated by inflammatory stimuli and modulates glycolysis in macrophages. FEBS Lett 593(2):195–208. https://doi.org/10.1002/1873-3468.13298
Malandrino MI, Fucho R, Weber M et al (2015) Enhanced fatty acid oxidation in adipocytes and macrophages reduces lipid-induced triglyceride accumulation and inflammation. Am J Physiol Endocrinol Metab 308(9):E756–E769. https://doi.org/10.1152/ajpendo.00362.2014
Martinez FO, Gordon S, Locati M, Mantovani A (2006) Transcriptional profiling of the human monocyte-to-macrophage differentiation and polarization: new molecules and patterns of gene expression. J Immunol 177(10):7303–7311. https://doi.org/10.4049/jimmunol.177.10.7303
Miao B, Zondlo S, Gibbs S et al (2004) Raising HDL cholesterol without inducing hepatic steatosis and hypertriglyceridemia by a selective LXR modulator. J Lipid Res 45(8):1410–1417. https://doi.org/10.1194/jlr.M300450-JLR200
Mills CD (1991) Molecular basis of suppressor macrophages. Arginine metabolism via the nitric oxide synthetase pathway. J Immunol 146:2719–2723
Moreira TJTP, Pierre K, Maekawa F et al (2009) Enhanced cerebral expression of MCT1 and MCT2 in a rat ischemia model occurs in activated microglial cells. J Cereb Blood Flow Metab 29(7):1273–1283. https://doi.org/10.1038/jcbfm.2009.50
Morioka S, Perry JSA, Raymond MH et al (2018) Efferocytosis induces a novel SLC program to promote glucose uptake and lactate release. Nature 563(7733):714–718. https://doi.org/10.1038/s41586-018-0735-5
Mulder K, Patel AA, Kong WT et al (2021) Cross-tissue single-cell landscape of human monocytes and macrophages in health and disease. Immunity 54(8):1883-1900 e5. https://doi.org/10.1016/j.immuni.2021.07.007
Murphy MP, O’Neill LAJ (2018) Krebs cycle reimagined: the emerging roles of succinate and itaconate as signal transducers. Cell 174(4):780–784. https://doi.org/10.1016/j.cell.2018.07.030
Murray PJ, Wynn TA (2011) Protective and pathogenic functions of macrophage subsets. Nat Rev Immunol 11(11):723–737. https://doi.org/10.1038/nri3073
Nareika A, He L, Game BA et al (2005) Sodium lactate increases LPS-stimulated MMP and cytokine expression in U937 histiocytes by enhancing AP-1 and NF-κB transcriptional activities. Am J Physiol Endocrinol Metab 289(4):E534–E542. https://doi.org/10.1152/ajpendo.00462.2004
Narwal V, Deswal R, Batra B et al (2019) Cholesterol biosensors: a review. Steroids 143:6–17. https://doi.org/10.1016/j.steroids.2018.12.003
Navale AM, Paranjape AN (2016) Glucose transporters: physiological and pathological roles. Biophys Rev 8(1):5–9. https://doi.org/10.1007/s12551-015-0186-2
Newton R, Priyadharshini B, Turka LA (2016) Immunometabolism of regulatory T cells. Nat Immunol 17(6):618–625. https://doi.org/10.1038/ni.3466
Nicholson B, Manner CK, Kleeman J, MacLeod CL (2001) Sustained nitric oxide production in macrophages requires the arginine transporter CAT2. J Biol Chem 276(19):15881–15885. https://doi.org/10.1074/jbc.M010030200
Nishiyama K, Fujita T, Fujimoto Y, Nakajima H, Takeuchi T, Azuma YT (2018) Fatty acid transport protein 1 enhances the macrophage inflammatory response by coupling with ceramide and c-Jun N-terminal kinase signaling. Int Immunopharmacol 55:205–215. https://doi.org/10.1016/j.intimp.2017.12.003
Noda M, Nakanishi H, Akaike N (1999) Glutamate release from microglia via glutamate transporter is enhanced by amyloid-beta peptide. Pergamon:1465–1474. https://doi.org/10.1016/s0306-4522(99)00036-6
Ohashi T, Aoki M, Tomita H et al (2017) M2-like macrophage polarization in high lactic acid-producing head and neck cancer. Cancer Sci 108(6):1128–1134. https://doi.org/10.1111/cas.13244
O’Neill LA, Pearce EJ (2016) Immunometabolism governs dendritic cell and macrophage function. J Exp Med 213(1):15–23. https://doi.org/10.1084/jem.20151570
Oram JF, Heinecke JW (2005) ATP-binding cassette transporter A1: a cell cholesterol exporter that protects against cardiovascular disease. Physiol Rev 85(4):1343–1372. https://doi.org/10.1152/physrev.00005.2005
Oram JF, Vaughan AM (2006) ATP-Binding cassette cholesterol transporters and cardiovascular disease. Circ Res 99(10):1031–1043. https://doi.org/10.1161/01.RES.0000250171.54048.5c
Pålsson-McDermott EM, Diskin C (2018) Metabolic modulation in macrophage effector function. Front Immunol 9:270. https://doi.org/10.3389/fimmu.2018.00270
Pearce EL, Pearce EJ (2013) Metabolic pathways in immune cell activation and quiescence. Immunity 38(4):633–643. https://doi.org/10.1016/j.immuni.2013.04.005
Perland E, Fredriksson R (2017) Classification systems of secondary active transporters. Trends Pharmacol Sci 38(3):305–315. https://doi.org/10.1016/j.tips.2016.11.008
Peruzzotti-Jametti L, Bernstock JD, Vicario N et al (2018) Macrophage-derived extracellular succinate licenses neural stem cells to suppress chronic neuroinflammation. Cell Stem Cell 22(3):355-368 e13. https://doi.org/10.1016/j.stem.2018.01.020
Phillips MC (2014) Molecular mechanisms of cellular cholesterol efflux. J Biol Chem 289(35):24020–24029. https://doi.org/10.1074/jbc.R114.583658
Poon IK, Lucas CD, Rossi AG, Ravichandran KS (2014) Apoptotic cell clearance: basic biology and therapeutic potential. Nat Rev Immunol 14(3):166–180. https://doi.org/10.1038/nri3607
Posokhova EN, Khoshchenko OM, Chasovskikh MI, Pivovarova EN, Dushkin MI (2008) Lipid synthesis in macrophages during inflammation in vivo: effect of agonists of peroxisome proliferator activated receptors alpha and gamma and of retinoid X receptors. Biochemistry (Mosc) 73(3):296–304. https://doi.org/10.1134/s0006297908030097
Ratter JM, Rooijackers HMM, Hooiveld GJ et al (2018) In vitro and in vivo effects of lactate on metabolism and cytokine production of human primary PBMCs and monocytes. Front Immunol 9:2564. https://doi.org/10.3389/fimmu.2018.02564
Repa JJ, Liang G, Ou J et al (2000) Regulation of mouse sterol regulatory element-binding protein-1c gene (SREBP-1c) by oxysterol receptors, Lxralpha and LXRbeta. Genes Dev 14(22):2819–2830. https://doi.org/10.1101/gad.844900
Rogatzki MJ, Ferguson BS, Goodwin ML, Gladden LB (2015) Lactate is always the end product of glycolysis. Front Neurosci 9:22. https://doi.org/10.3389/fnins.2015.00022
Rubic T, Lametschwandtner G, Jost S et al (2008) Triggering the succinate receptor GPR91 on dendritic cells enhances immunity. Nat Immunol 9(11):1261–1269. https://doi.org/10.1038/ni.1657
Sag D, Cekic C, Wu R, Linden J, Hedrick CC (2015) The cholesterol transporter ABCG1 links cholesterol homeostasis and tumour immunity. Nat Commun 6:6354. https://doi.org/10.1038/ncomms7354
Samuvel DJ, Sundararaj KP, Nareika A, Lopes-Virella MF, Huang Y (2009) Lactate boosts TLR4 signaling and NF-kappaB pathway-mediated gene transcription in macrophages via monocarboxylate transporters and MD-2 up-regulation. J Immunol 182(4):2476–2484. https://doi.org/10.4049/jimmunol.0802059
Sato H, K Fujiwara, J Sagara, S Bannai (1995) Induction of cystine transport activity in mouse peritoneal macrophages by bacterial lipopolysaccharide. Biochem J 310(Pt 2):547–551. https://doi.org/10.1042/bj3100547
Scher JU, Pillinger MH (2009) The anti-inflammatory effects of prostaglandins. J Investig Med 57(6):703–708. https://doi.org/10.2310/JIM.0b013e31819aaa76
Schwartz K, Lawn RM, Wade DP (2000) ABC1 gene expression and ApoA-I-mediated cholesterol efflux are regulated by LXR. Biochem Biophys Res Commun 274(3):794–802. https://doi.org/10.1006/bbrc.2000.3243
Schweikhard ES, Ziegler CM (2012) Amino acid secondary transporters: toward a common transport mechanism. Curr Top Membr 70:1–28. https://doi.org/10.1016/B978-0-12-394316-3.00001-6
Shimada H, Nakamura Y, Nakanishi T, Tamai I (2015) OATP2A1/SLCO2A1-mediated prostaglandin E2 loading into intracellular acidic compartments of macrophages contributes to exocytotic secretion. Biochem Pharmacol 98(4):629–638. https://doi.org/10.1016/j.bcp.2015.10.009
Shime H, Yabu M, Akazawa T, Kodama K, Matsumoto M, Seya T, Inoue N (2008) Tumor-secreted lactic acid promotes IL-23/IL-17 proinflammatory pathway. J Immunol 180(11):7175–7183. https://doi.org/10.4049/jimmunol.180.11.7175
Simard JC, Thibodeau JF, Leduc M et al (2020) Fatty acid mimetic PBI-4547 restores metabolic homeostasis via GPR84 in mice with non-alcoholic fatty liver disease. Sci Rep 10(1):12778. https://doi.org/10.1038/s41598-020-69675-8
Singh Y, Pawar VK, Meher JG et al (2017) Targeting tumor associated macrophages (TAMs) via nanocarriers. J Control Release 254:92–106. https://doi.org/10.1016/j.jconrel.2017.03.395
Song W, Li D, Tao L, Luo Q, Chen L (2020) Solute carrier transporters: the metabolic gatekeepers of immune cells. Acta Pharm Sin B 10(1):61–78. https://doi.org/10.1016/j.apsb.2019.12.006
Soumian S, Albrecht C, Davies AH, Gibbs RGJ (2005) ABCA1 and atherosclerosis. Vasc Med 10(2):109–119. https://doi.org/10.1191/1358863x05vm593ra
Spencer NY, Stanton RC (2019) The Warburg effect, lactate, and nearly a century of trying to cure cancer. Semin Nephrol 39(4):380–393. https://doi.org/10.1016/j.semnephrol.2019.04.007
Stone SC, Rossetti RAM, Alvarez KLF et al (2019) Lactate secreted by cervical cancer cells modulates macrophage phenotype. J Leukoc Biol 105(5):1041–1054. https://doi.org/10.1002/JLB.3A0718-274RR
Stunault MI, Bories G, Guinamard RR, Ivanov S (2018) Metabolism plays a key role during macrophage activation. Mediators Inflamm 2018:2426138. https://doi.org/10.1155/2018/2426138
Tabas I, Bornfeldt KE (2020) Intracellular and intercellular aspects of macrophage immunometabolism in atherosclerosis. Circ Res 126(9):1209–1227. https://doi.org/10.1161/circresaha.119.315939
Tan Z, Xie N, Banerjee S et al (2015) The monocarboxylate transporter 4 is required for glycolytic reprogramming and inflammatory response in macrophages. J Biol Chem 290(1):46–55. https://doi.org/10.1074/jbc.M114.603589
Tannahill GM, Curtis AM, Adamik J et al (2013) Succinate is an inflammatory signal that induces IL-1beta through HIF-1alpha. Nature 496(7444):238–242. https://doi.org/10.1038/nature11986
Tsai TH, Yang CC, Kou TC et al (2021) Overexpression of GLUT3 promotes metastasis of triple-negative breast cancer by modulating the inflammatory tumor microenvironment. J Cell Physiol. https://doi.org/10.1002/jcp.30189
Udalova IA, Mantovani A, Feldmann M (2016) Macrophage heterogeneity in the context of rheumatoid arthritis. Nat Rev Rheumatol 12(8):472–485. https://doi.org/10.1038/nrrheum.2016.91
Van Dyken SJ, Locksley RM (2013) Interleukin-4- and interleukin-13-mediated alternatively activated macrophages: roles in homeostasis and disease. Annu Rev Immunol 31:317–343. https://doi.org/10.1146/annurev-immunol-032712-095906
Venkateswaran A, Repa JJ, Lobaccaro JM, Bronson A, Mangelsdorf DJ, Edwards PA (2000) Human white murine ABC8 mRNA levels are highly induced in lipid-loaded macrophages. A transcriptional role for specific oxysterols. J Biol Chem:14700–1470. https://doi.org/10.1074/jbc.275.19.14700
Verdone JE, Zarif JC, Pienta KJ (2015) Aerobic glycolysis, motility, and cytoskeletal remodeling. Cell Cycle 14(2):169–170. https://doi.org/10.1080/15384101.2014.995493
Wang L, Pavlou S, Du X, Bhuckory M, Xu H, Chen M (2019) Glucose transporter 1 critically controls microglial activation through facilitating glycolysis. Mol Neurodegener 14(1):2. https://doi.org/10.1186/s13024-019-0305-9
Wise DR, Thompson CB (2010) Glutamine addiction: a new therapeutic target in cancer. Trends Biochem Sci 35(8):427–433. https://doi.org/10.1016/j.tibs.2010.05.003
Wu Q, Zhang Y, Zhang Y et al (2020) Riluzole improves functional recovery after acute spinal cord injury in rats and may be associated with changes in spinal microglia/macrophages polarization. Neurosci Lett 723:134829. https://doi.org/10.1016/j.neulet.2020.134829
Xu L, Ota T (2018) Emerging roles of SGLT2 inhibitors in obesity and insulin resistance: Focus on fat browning and macrophage polarization. Adipocyte 7(2):121–128. https://doi.org/10.1080/21623945.2017.1413516
Xu F, Cui WQ, Wei Y et al (2018) Astragaloside IV inhibits lung cancer progression and metastasis by modulating macrophage polarization through AMPK signaling. J Exp Clin Cancer Res 37(1):207. https://doi.org/10.1186/s13046-018-0878-0
Yamane H, Sugimoto Y, Tanaka S, Ichikawa A (2000) Prostaglandin E(2) receptors, EP2 and EP4, differentially modulate TNF-alpha and IL-6 production induced by lipopolysaccharide in mouse peritoneal neutrophils. Biochem Biophys Res Commun 278(1):224–228. https://doi.org/10.1006/bbrc.2000.3779
Yin C, Cheng L, Pan J et al (2020) Regulatory role of Gpr84 in the switch of alveolar macrophages from CD11b(lo) to CD11b(hi) status during lung injury process. Mucosal Immunol 13(6):892–907. https://doi.org/10.1038/s41385-020-0321-7
Yoon BR, Oh YJ, Kang SW, Lee EB, Lee WW (2018) Role of SLC7A5 in metabolic reprogramming of human monocyte/macrophage immune responses. Front Immunol 9:53. https://doi.org/10.3389/fimmu.2018.00053
Yurdagul A Jr, Subramanian M, Wang X et al (2020) Macrophage metabolism of apoptotic cell-derived arginine promotes continual efferocytosis and resolution of injury. Cell Metab 31(3):518-533 e10. https://doi.org/10.1016/j.cmet.2020.01.001
Zhang D, Tang Z, Huang H et al (2019a) Metabolic regulation of gene expression by histone lactylation. Nature 574(7779):575–580. https://doi.org/10.1038/s41586-019-1678-1
Zhang S, Weinberg S, DeBerge M et al (2019b) Efferocytosis fuels requirements of fatty acid oxidation and the electron transport chain to polarize macrophages for tissue repair. Cell Metab 29(2):443-456 e5. https://doi.org/10.1016/j.cmet.2018.12.004
Zhang Y, Zhang Y, Sun K, Meng Z, Chen L (2019c) The SLC transporter in nutrient and metabolic sensing, regulation, and drug development. J Mol Cell Biol 11(1):1–13. https://doi.org/10.1093/jmcb/mjy052
Zhang J, Muri J, Fitzgerald G et al (2020) Endothelial lactate controls muscle regeneration from ischemia by inducing M2-like macrophage polarization. Cell Metab 31(6):1136-1153 e7. https://doi.org/10.1016/j.cmet.2020.05.004
Zhao L, Cozzo AJ, Johnson AR et al (2017) Lack of myeloid Fatp1 increases atherosclerotic lesion size in Ldlr(-/-) mice. Atherosclerosis 266:182–189. https://doi.org/10.1016/j.atherosclerosis.2017.10.009
Zhu L, Zhao Q, Yang T, Ding W, Zhao Y (2015) Cellular metabolism and macrophage functional polarization. Int Rev Immunol 34(1):82–100. https://doi.org/10.3109/08830185.2014.969421
Acknowledgements
The work of the author’s laboratory is supported by Anhui Biochemical and Pharmaceutical Engineering Research Center.
Funding
This work was supported by grants from the National Natural Science Foundation of China (81703529), the Anhui Province Postdoctoral Research Activity Funding Project (2018B251), the Innovation and Entrepreneurship Project Plan of National Undergraduate Support Project of China (201910367036, 202010367037), the Innovative Drug Innovation Team of Bengbu Medical College (BYKC201904), the Innovative re-search project plan of Postgraduate Support Project of Bengbu Medical College (Byycx20036), the 512 Talent Training Program of Bengbu Medical College (by51202203), and the Collaboration Scientific and technological project of Bengbu and Bengbu Medical College (BYLK201819).
Author information
Authors and Affiliations
Contributions
J. C. designed and conducted the literature review and drafted the manuscript. W. C., S. Z., and Y. Y. conducted the literature review. F. W. designed and conceptualized the manuscript. All authors read and approved the manuscript.
Corresponding author
Ethics declarations
Ethical approval
Not applicable.
Consent to participate
Not applicable.
Consent for publication
Not applicable.
Competing interests
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Highlights
• Metabolic reprogramming and changes in cell metabolism are required for macrophage polarization and activation.
• Metabolites participate in modification of macrophage polarization by altering metabolic pathways.
• Metabolite transporters regulate macrophage polarization by mediating the input/output of metabolites which cannot freely pass through the cell membrane.
• Metabolite transporters may represent novel drug targets for the treatment of macrophage-associated diseases.
The author confirm that no paper mill was used.
Rights and permissions
About this article
Cite this article
Cheng, J., Cai, W., Zong, S. et al. Metabolite transporters as regulators of macrophage polarization. Naunyn-Schmiedeberg's Arch Pharmacol 395, 13–25 (2022). https://doi.org/10.1007/s00210-021-02173-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00210-021-02173-4