Abstract
Objective
To determine whether peroxisome proliferator-activated receptor (PPAR) γ ligands improve survival of patients with septic shock we treated a mouse model of sepsis [apolipoprotein (Apo) E) knockout mice] with pioglitazone, a PPAR-γ ligand. ApoE knockout mice have a high mortality rate due to sepsis because the endotoxin is not cleared.
Design and setting
Prospective study in a university laboratory.
Subjects
We assorted 87 male ApoE knockout mice and 60 wild-type C57/B6 mice randomly into three groups (sepsis, pretreatment, posttreatment).
Interventions
Cecal ligation and puncture (CLP) was carried out in the sepsis and treatment groups. Mice were injected with pioglitazone (5 mg/kg per day) on the day before CLP or 6 h after surgery.
Measurements and results
Both pre- and post-CLP treatment with pioglitazone improved survival of ApoE knockout and wild-type mice. Serum levels of cytokines and chemokines and myeloperoxidase activity in lung and liver were suppressed in the pioglitazone-treated group. Pioglitazone also suppressed monocyte adhesion to vascular endothelium under flow conditions.
Conclusions
Pioglitazone improved survival of ApoE knockout mice after onset of septic shock through suppression of inflammatory responses.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Severe sepsis and septic shock are the second common causes of death in the intensive care unit. Despite significant advances in intensive care therapy and antibiotics the mortality rate due to severe sepsis has not decreased significantly over the past 10 years [1]. In fact, the number of patients suffering from severe sepsis has increased. Sepsis is a complex clinical syndrome that results from a damaging host response to microbial infection due to dysregulation of the innate immune system. Sepsis is characterized by excessive production of cytokines such as tumor necrosis factor (TNF) α and interleukin (IL) 6. Many anti-inflammatory drugs have been tested for the treatment of severe sepsis. Some have improved the survival rate of animal models when administered after onset of sepsis. These drugs include antagonists of high-mobility group box 1 [2], statins [3], soluble Flt-1 [4], adrenomedullin [5], and β-glucan [6].
It was recently reported that lipid metabolism has a strong relationship to the progression of severe sepsis [7, 8]. Some lipoproteins have been shown to inhibit inflammation in vivo and in vitro [9]. Moreover, an apolipoprotein (Apo) E polymorphism also has a close association with the risk and mortality of severe sepsis [10]. ApoE is a ligand for the low-density lipoprotein (LDL) receptor and plays a significant role in lipid metabolism, and ApoE knockout (ApoE–/–) mice show hyperlipidemia. It was reported recently that ApoE–/– mice are highly susceptible to endotoxinemia [11]. This can be explained by the fact that under normal circumstances ApoE binds and neutralizes endotoxins. Interestingly, administration of ApoE to ApoE–/– mice suppresses inflammation and improves the rate of survival of mice with sepsis [12]. On the basis of these facts we hypothesized that ApoE–/– mice could be a model system for high mortality in response to sepsis.
Peroxisome proliferator-activated receptor (PPAR) γ is a member of the nuclear receptor superfamily and is expressed in various cells, including monocyte-macrophages, T cells, endothelial cells (ECs), and other cells involved in the progression of sepsis. PPAR-γ ligands have anti-inflammatory effects and improve outcomes in various situations such as transplantation-associated arteriosclerosis [13], rheumatoid arthritis [14], allergic reaction [15], and inflammatory bowel disease [16]. Recent studies have shown that administration of ciglitazone, a thiazolidinedione and PPAR-γ ligand, 1 h after cecal ligation and puncture (CLP) suppresses inflammation and improves survival in a rat model of sepsis [17]. The statins improve survival rate through their pleiotropic effects, such as inhibition of monocytes–endothelial cell interaction and anti-inflammatory activity.
There are reports that the PPAR ligands have the same anti-inflammatory effects as statins. Therefore in the present study we investigated whether pioglitazone, a member of the thiazolidinediones and PPAR-γ ligand, improves the survival of septic ApoE–/– and wild-type (WT) mice 6 h after CLP.
Methods
Animals
The study used 10- to 12-week-old male C57BL/6 mice from Japan Clea and male C57BL/6 ApoE–/– mice from Prof. S. Ishibashi (Jichi Medical School, Tochigi, Japan). Animals were maintained at least 1 week in our animal facility and weighed 25–35 g. The present study conformed to the Guide for the Care and Use of Laboratory Animals of Tokyo Medical and Dental University.
CLP model
Mice were anesthetized with a mixture of ketamine (60 mg/kg) and xylazine (10 mg/kg) given intraperitoneally. The cecum was exposed through an abdominal incision and subjected to ligation of the distal half followed by two punctures with a 21-gauge needle. A small amount of stool was expelled into the peritoneal cavity, and the incision was closed. After the surgery 0.5 ml 0.9% NaCl was administered by subcutaneous injection twice each day for volume restoration. Pioglitazone (Takeda Pharmaceutical, Tokyo, Japan) was dissolved with 0.5% methylcellulose and administered by intraperitoneal injection. One group of mice (n = 20) received pioglitazone 18 h and 6 h before surgery and received twice injections each day (total 5 mg/kg per day) until 7 days after CLP; this group was called the Pre-Pio group. The other group of mice (n = 20) received pioglitazone 6 h after surgery and received injections twice each day (total 5 mg/kg per day); this group was called the Post-Pio group. Control group mice (n = 20) received 0.5% methylcellulose only. The daily dose of 5 mg/kg pioglitazone used in the present study is parallel to the dose used for therapy in humans and used in many studies [13, 18, 19]. Six mice in each CLP (vehicle, preadministration, and postadministration) and sham-operated (vehicle, preadministration, and postadministration) group were used in the following experiments. Three mice in each CLP and sham-operated group were used for histopathology. In total, 87 ApoE–/– mice and 60 C57BL/6 mice were subjected to CLP, and 27 ApoE–/– mice were used as sham controls.
Hemodynamic measurements
Blood pressure (BP) was measured in six mice each group by a noninvasive method (BP-98A, Softron, Tokyo, Japan). Mice were placed in a warm, dark sack, and BP was measured in the tail as described previously [20].
Measurement of cytokines and chemokines by enzyme-linked immunosorbent assay
The blood samples obtained and heparinized 18 h after CLP were centrifuged at 5,000 rpm for 5 min to separate the plasma. Serum IL-6, TNF-α, IL-10, and monocyte chemoattractant protein (MCP) 1 levels in ApoE–/– mice (n = 6, each group) 18 h after CLP were measured with an enzyme-linked immunosorbent assay (ELISA) kit (BioSource International, Camarillo, CA, USA) according to the manufacturer's instructions. The levels exceeded the upper measurement limits of the kits, and therefore we diluted each serum 100-fold and repeated the assay.
Measurement of liver function
Blood aspartate transaminase (AST) and alanine transaminase (ALT) levels were determined by MDH-UV method and Hitachi 7350 (Hitachi, Tokyo, Japan) in the same serum samples used for ELISA.
Measurement of myeloperoxidase activity in lung and liver
Myeloperoxidase (MPO) activity in ApoE–/– mice (n = 6) 18 h after surgery was determined as described previously [21]. Briefly, tissues were weighed and washed with 0.9% NaCl immediately after excision. Tissues were homogenized in a potassium phosphate buffer containing 0.5% hexadecyltrimethylammonium bromide (Sigma, St. Louis, MO, USA). Homogenates were reacted with a 50-mM phosphate buffer (pH 6.0) containing 0.167 mg/ml o-dianisidine hydrochloride (Sigma) and 0.0005% hydrogen peroxide (Wako, Osaka, Japan). The change in absorbance at 460 nm was measured with a microplate reader (Ultramark, Bio-Rad, Hercules, CA, USA), and the results are expressed as units of MPO/100 mg tissues. One unit of MPO was defined as that degrades 1 μmol peroxidase/min at 25°.
Histology and immunohistochemistry
Lungs and livers from ApoE–/– mice were dissected 18 h after surgery. Lung tissues were inflated with formalin at a pressure of 20 cmH2O. Tissues were fixed in formalin for 3 days and then embedded in paraffin. Tissues were sectioned at a thickness of 5 μm and stained with hematoxylin and eosin. Liver tissues were frozen in liquid nitrogen. Frozen sections (5 μm) were fixed in acetone for 10 min at 4°. Sections were washed with phosphate-buffered saline and then incubated with anti-CD11b rat antibody (1:400, BD Biosciences, NJ, USA) overnight at 4°. Sections were then incubated with biotinylated secondary antibody for 30 min at room temperature. Immunocompleted slides were visualized with avidin-biotin-horseradish peroxidase complex (Nichirei, Tokyo, Japan) according to the manufacturer's protocol and then counterstained with hematoxylin.
Monocyte adhesion assay
The monocyte/macrophage cell line THP-1 was obtained from Riken Bioresource Center (Tsukuba, Ibaragi, Japan) and grown in RPMI 1640 medium supplemented with 10% fetal calf serum (Life Technologies Oriental, Tokyo, Japan). Human umbilical vein ECs (HUVECs) were isolated from normal-term umbilical cords and cultured as described previously [22]. The protocols for the adhesion assay under static flow and flow conditions were described previously [22]. Briefly, for the flow assays HUVEC monolayers were stimulated with 10 ng/ml TNF-α (Genzyme, Boston, MA, USA) for 4 h on coverslips and then positioned in a flow chamber mounted on an inverted microscope (IX70, Olympus, Tokyo, Japan). THP-1 cells (1 × 106/ml) were preincubated with pioglitazone (2 and 20 μM) for 12 h and drawn through the chamber at a wall shear stress of 1.0 dyne/cm2 for 10 min. Those dose of pioglitazone were used previously in many experiments [13, 23]. The entire perfusion period was recorded on video. The number of rolling and adherent THP-1 cells present on HUVEC monolayers was counted in ten randomly selected 20 × microscope fields.
Statistical analysis
All data are expressed as mean ± SEM. Kaplan–Meier analysis was used to evaluate mice survival, and the Mann–Whitney U test was used to examine differences in survival between two groups. Analysis of variance with Dunnett's post-hoc test for comparisons between groups ELISA and MPO assay results. Differences at p < 0.05 were considered statistically significant. All statistical analyses were performed with JMP 5.1 software (SAS, Cary, NC, USA).
Results
Pioglitazone improved survival and BP in an experimental model of sepsis
After undergoing CLP the mice displayed signs of severe sepsis, including reduced mobility, apathy, and falling BP. Both ApoE–/– and WT mice treated with pioglitazone either on the day prior to CLP or 6 h showed significantly better survival rates than control mice (Fig. 1; p < 0.05). In contrast, ApoE–/– mice deceased within 36 h after CLP. Pioglitazone treatment also prevented the drop in mean BP in ApoE–/– mice (Fig. 2; p < 0.05). Mean BP was lower in sham-operated mice given pioglitazone than in mice given vehicle; however, this drop was not statistically significant 18 h after CLP (data not shown).
Pioglitazone (Pio) administration improves survival of both ApoE–/– (ApoE KO) and wild-type (WT) mice: survival curves. WT mice: daily preadministration of 5 mg/kg pioglitazone (filled squares), daily postadministration of 5 mg/kg pioglitazone mice (filled triangles), and control (filled diamonds); * p < 0.05 vs. control; n = 20 in each group. ApoE–/– mice: daily preadministration of 5 mg/kg pioglitazone (open circles), daily postadministration of 5 mg/kg pioglitazone mice (filled circles), and control (×); # p < 0.05 vs. control; n = 20 in each group
Pioglitazone (Pio) restores mean BP in CLP ApoE–/– mice. Mean BP progression in mice treated with 5 mg/kg pioglitazone per day for 1 day before CLP (filled squares), for 6 h after CLP (filled triangles), and injected with control vehicle alone (filled diamonds); * p < 0.05 vs. control; n = 6, each group
Pioglitazone suppressed the systemic release of inflammatory cytokines and chemokines in ApoE–/– mice
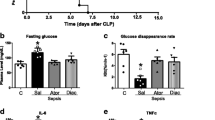
Serum levels of TNF-α, IL-6, IL-10, and MCP-1 in ApoE–/– mice (n = 6) 18 h after CLP were measured. As expected, CLP significantly increased levels of all proteins examined. Treatment with pioglitazone significantly decreased plasma levels of proinflammatory cytokines TNF-α and IL-6, anti-inflammatory cytokine IL-10, and proinflammatory chemokine MCP-1 (Fig. 3). Serum levels of TNF-α, IL-6, IL-10, and MCP-1 were measured six times for each of the three animal groups (preadministration, postadministration, and control).
Pioglitazone (Pio) treatment significantly decreases plasma cytokine levels in ApoE–/– mice. Plasma levels of TNF-α, IL-6, IL-10, and MCP-1 18 h after CLP. Levels of all cytokines in mice treated with 5 mg/kg pioglitazone per day 1 day before CLP were reduced significantly. TNF-α, IL-6, and MCP-1 levels were reduced significantly in mice that received postsurgical pioglitazone; ** p < 0.01, * p < 0.05 vs. control; n = 6, each group
Pioglitazone suppressed inflammation of the organs in ApoE–/– mice
We next examined whether pioglitazone suppresses inflammation in the lungs and liver of septic mice. Increased MPO activity is correlated with neutrophil invasion of the organs. MPO activity was reduced significantly in lungs and liver from animals treated with pioglitazone (Fig. 4a). Lung MPO activity (IU/100 mg tissue) in mice treated with pioglitazone prior to surgery, after surgery, and not treated (n = 6) was 74.7 ± 5.1, 82.3 ± 5.0, and 111.6 ± 4.4, respectively. Liver MPO activity values were 2.1 ± 0.3, 3.1 ± 0.2, and 4.1 ± 0.3, respectively. Next we checked blood AST and ALT levels as an indication of liver damage (Fig. 4b). The AST (IU/l) in mice (n = 6, each group) treated with pioglitazone prior to surgery, after surgery, and with vehicle were 545.0 ± 100.1, 693.8 ± 44.6, and 966.8 ± 56.6, while the ALT (IU/l, n = 6) values were 133.0 ± 10.9, 162.3 ± 12.5, and 252.2 ± 19.7. Immunohistochemistry revealed that pioglitazone treatment suppressed invasion of CD11b+ cells into the liver (Fig. 4c). Morphological analysis indicated that pioglitazone treatment inhibited leukocyte infiltration into the interstitial space and alveolar wall (data not shown).
a MPO activity 18 h after CLP. MPO activity in both lung and liver of mice treated with pioglitazone (Pio) before CLP was reduced significantly. MPO activity in mice treated with pioglitazone after CLP was also reduced; ** p < 0.01, * p < 0.05 vs. control; n = 6, each group. b Serum AST and ALT levels of mice treated with pioglitazone were also reduced in mice treated with pioglitazone; ** p < 0.01, * p < 0.05 vs. control; n = 6, each group. c Representative immunohistochemical staining of CD11b in liver 18 h after CLP. Invasion by CD11b+ cells was significantly lower in mice treated with pioglitazone than in control mice; original magnification × 400
Pioglitazone suppressed monocytes adhesion to ECs
To clarify the mechanisms of the protective effects of pioglitazone on the organs we studied the interaction of monocytes with ECs. We examined the effect of pioglitazone on adhesion of monocytic THP-1 cells to TNF-α activated HUVECs under flow conditions at a laminar shear stress level of 1.0 dyne/cm2. THP-1 cells were pretreated with 2 and 20 μM pioglitazone for 12 h prior to the adhesion assay. As shown in Fig. 5, the numbers of adhered and rolling THP-1 cells were significantly lower after pioglitazone treatment.
Pioglitazone reduces adhesion and rolling of THP-1 cells on HUVECs under physiological flow conditions. Black bars Adhesion; gray bars number of rolling cells/HPF. THP-1 cells were treated with 2 or 20 μM pioglitazone for 12 h and then passed over HUVECs activated with TNF-α; ** p < 0.01, * p < 0.05 vs. control vehicle only
Discussion
Sepsis is a complex clinical syndrome that results from a harmful host response to infection. Sepsis progresses without the initial, appropriate host responses to inflammation. In the presence of endotoxin white blood cells such as monocytes and neutrophils become activated and produce proinflammatory cytokines. Excessive production of these proinflammatory cytokines causes irreversible multiorgan failure. There is an urgent need to identify substances that improve survival of patients with modulating the immune response under such conditions.
We used ApoE–/– mice subjected to CLP to demonstrate that pioglitazone improves survival under conditions of severe sepsis through suppression of inflammatory responses. Ours is the first study showing that administration of a PPAR-γ ligand, pioglitazone, after onset of severe sepsis improves survival in a clinically relevant model of sepsis [24]. It was previously reported that PPAR-γ ligands, ciglitazone, and 15-deoxy-Δ12,14-prostaglandin J2 reduced systemic inflammation and improved survival in animal model [17], indicating that PPAR-γ ligands are effective treatment for severe sepsis. Zingarelli B et al. [17] found that BP in rats had fallen significantly 4 h after CLP procedure in their study. We therefore administered pioglitazone at 6 h after the drop in BP. We also found that administration of pioglitazone before CLP improved survival of WT mice, as reported previously. In a separate study the administration of the phytochemical curcumin 5 h after CLP suppressed inflammatory responses and improved survival through activation of PPAR-γ. These effects were abolished by administration of a PPAR-γ antagonist [25]. PPAR-γ ligands improve the survival rate in various models of shock including hemorrhagic shock [26], zymosan-induced nonseptic shock [27], and endotoxin shock [28]. Moreover, a recent report clarified that the acute anti-inflammatory effects of statins were mediated by PPAR-α, an isotype of PPAR expressed by macrophages and ECs during progression of sepsis [29]. The PPAR-α ligand improved severe sepsis in a rabbit model of shock [30]. These reports support our finding that pioglitazone has strong anti-inflammatory effects and improves survival of mice with severe sepsis.
It was reported previously that many PPAR-γ ligands, including pioglitazone, suppress inflammation through suppression of mitogen-activated protein kinase (MAPK) and nuclear factor (NF) κB activation by lipopolysaccharide in monocytes/macrophages. We also checked the suppressive effects of pioglitazone on MAPK and NF-κB stimulated by LPS in THP-1 cells (data not shown). Suppression of cytokines and chemokines may occur through these MAPK and NF-κB pathways. However, there are many reports that anti-inflammatory treatment increases IL-10 expression, and IL-10 is thought to be a marker of good positive change effect. We did not observe an increase in IL-10 ApoE–/– mice. A previous report indicated that serum IL-10 levels differ in mild vs. moderate and severe cases, whereas IL-6 levels differ between each group [31]. We believe that IL-10 caused the ApoE–/– mice to have such severe inflammation, and that the IL-10 level was not affected. It was recently reported that serum cytokine levels sometimes vary from survival and other inflammatory indices [32].
The present study also shows that pioglitazone inhibits adhesion of monocytes to ECs similarly to statins [3, 22]. This suppression may decrease invasion of white blood cells into organs such as lung and liver and may attenuate lung injury [33]. This would explain the decreased MPO activity observed in lungs and liver of pioglitazone-treated mice. PPAR-γ was initially described as an insulin sensitizer; however, it has many functions in other cells and situations. The PPAR-γ ligand pioglitazone improves EC function [34] and suppresses neointimal formation after stent implantation [35], even in nondiabetic patients.
We also found that pioglitazone treatment improves survival of both septic ApoE–/– mice and WT mice. ApoE has received a great deal of attention in the fields of neurology, endocrinology, and cardiology where it is believed to have direct links to some diseases. ApoE is a ligand of the LDL receptor and plays an essential role in lipid metabolism and atherosclerosis progression. In addition, an ApoE polymorphism is a significant predictor of Alzheimer's disease occurrence. Furthermore, an ApoE polymorphism is linked to the incidence of severe sepsis [10]. ApoE also modulates the type I inflammatory responses; a recent study indicated that cytokine levels in ApoE–/– mice cytokine are higher than those in WT mice [9]. In addition, ApoE regulates clearance of apoptotic bodies involved in systemic inflammation [36]. ApoE has multiple functions in progression of inflammatory responses. For these reasons the CLP model with ApoE–/– mice can reproduce one type of severe sepsis in human beings. Our findings suggest that treatment with PPAR-γ agonist may be a strategy to treat severe sepsis.
References
Vincent JL, Abraham E (2006) The last 100 years of sepsis. Am J Respir Crit Care Med 173:256–263
Yang H, Ochani M, Jianhua L, Qiang X, Tanovic M, Harris HE, Susarla SM, Ulloa L, Wang H, Diramio R, Czura CJ, Wang H, Roth J, Warren HS, Fink MP, Fenton MJ, Andersson U, Tracy KJ (2004) Reversing established sepsis with antagonists of endogenous high-mobility group box 1. Proc Natl Acad Sci U S A 101:296–301
Merx MW, Liehn EA, Graf J, Sandt A, Schaltenbrand M, Schrader J, Hanrath P, Weber C (2005) Treatment after onset of sepsis in a murine model improves survival. Circulation 112:117–124
Yano K, Liaw PC, Mullington JM, Shih SC, Okada H, Bodyak N, Kang PM, Toltl L, Belikoff B, Buras J, Simms BT, Mizgerd JP, Carmeliet P, Karumanchi SA, Aird WC (2006) Vascular endothelial growth factor is an important determinant of sepsis morbidity and mortality. J Exp Med 203:1447–1458
Temmesfeld-Wollbruck B, Brell B, David I, Dorenberg M, Adolphs J, Schmeck B, Suttorp N, Hippenstiel S (2007) Adrenomedullin reduces vascular hyperpermeability and improves survival in rat septic shock. Intensive Care Med 33:703–710
Babayigit H, Kucuk C, Sozuer E, Yazici C, Kose K, Akgun H (2005) Protective effects of β glucan on lung injury after cecal ligation and puncture in rats. Intensive Care Med 31:865–870
Murch O, Collin M, Hinds CJ, Thiemermann C (2007) Lipoproteins in inflammation and sepsis. I. Basic science. Intensive Care Med 33:13–24
Wendel M, Paul R, Heller AR (2007) Lipoproteins in inflammation and sepsis. II. Clinical aspects. Intensive Care Med 33:25–35
Ali K, Middleton M, Pure E, Rader DJ (2005) Apolipoprotein E suppresses the type II inflammatory response in vivo. Circ Res 97:922–927
Moretti EW, Morris RW, Podgoreanu M, Schwinn DA, Newman MF, Bennett E, Moulin VG, Mba UU, Laskowitz DT, for the Perioperative Genetics nd Safety Outcomes Study (PEGASYS) Investigative Team (2005) APOE polymorphism is associated with risk of severe sepsis in surgical patients. Crit Care Med 33:2521–2526
Bont N, Netea MG, Demacker PNM, Verschueren I, Kullberg BJ, Dijk KW, Meer JWM, Stalenhoef AFH (1999) Apolipoprotein E knock-out mice highly susceptible to endotoxinemia and Klebsiella pneumoniae infection. J Lipid Res 40:680–685
Oosten MV, Rensen PCN, Amersfoort ESV, Eck MV, Dam AMV, Breve JJP, Vogel T, Panet A, Berkel TJCV (2001) Apolipoprotein E protects against bacterial lipopolysaccharide-induced lethality. J Biol Chem 276:8820–8824
Kosuge H, Haraguchi G, Koga N, Maejima Y, Suzuki JI, Isobe M (2006) Pioglitazone prevents acute and chronic cardiac allograft rejection. Circulation 113:2613–2622
Shiojiri T, Wada K, Nakajima A, Katayama K, Shibuya A, Kudo C, Kadowaki T, Mayumi T, Yura Y, Kamisaki Y (2002) PPARγ ligands inhibit nitrotyrosine formation and inflammatory mediator expressions in adjuvant-induced rheumatoid arthritis mice. Eur J Pharmacol 448:231–238
Woerly G, Honda K, Loyens M, Papin JP, Auwerx J, Staels B, Capron M, Dombrowicz D (2003) Peroxisome proliferator-activated receptors α and γ down-regulate allergic inflammation and eosinophil activation. J Exp Med 198:411–421
Katayama K, Wada K, Nakajima A, Mizuguchi H, Hayakawa T, Nakagawa S, Kadowaki T, Nagai R, Kamisaki Y, Blumberg RS, Mayumi (2003) A novel PPARγ gene therapy to control inflammation associated with inflammatory bowel disease in a murine model. Gastroenterology 124:1315–1324
Zingarelli B, Sheehan M, Hake PW, O'Connor M, Denenberg A, Cook JA (2003) Peroxisome proliferator activator receptor-γ ligands, 15-deoxy-Δ12:14-prostaglandin J2 and ciglitazone, reduce systemic inflammation in polymicrobial sepsis by modulation of signal transduction pathways. J Immunol 171:6827–6837
Joner M, Farb A, Cheng Q, Finn AV, Acampado E, Burke AP, Skorija K, Creighton W, Kolodgie FD, Gold HK, Virmani R (2007) Pioglitazone inhibits in-stent restenosis in atherosclerotic rabbits by targeting transforming growth factor-beta and MCP-1. Arterioscler Thromb Vasc Biol 27:182–189
Frantz S, Hu K, Widder J, Bayer B, Witzel CC, Schmidt I, Galuppo P, Strotmann J, Ertl G, Bauersachs J (2004) Peroxisome proliferator activated-receptor agonism and left ventricular remodeling in mice with chronic myocardial infarction. Br J Pharmacol 141:9–14
Suzuki JI, Ogawa M, Futamatsu H, Kosuge H, Tanaka H, Isobe M (2006) A cyclooxygenase-2 inhibitor alters Th1/Th2 cytokine balance and suppresses autoimmune myocarditis in rats. J Mol Cell Cardiol 40:688–695
Onai Y, Suzuki JI, Kakuta T, Maejima Y, Haraguchi G, Fukasawa H, Muto S, Itai A, Isobe M (2004) Inhibition of IκB phosphorylation in cardiomyocyte attenuates myocardial ischemia/reperfusion injury. Cardiovasc Res 63:51–59
Yoshida M, Sawada T, Ishii H, Gerszten RE, Rosenzweig A, Gimbrone MA, Yasukochi Y, Numano F (2001) HMG-CoA reductase inhibitor modulates monocyte-endothelial cell interaction under physiological flow conditions in vitro. Arterioscler Thromb Vasc Biol 21:1165–1171
Ogawa D, Nomiyama T, Nakamachi T, Heywood EB, Stone JF, Berger JP, Law RE, Bruemmer D (2006) Activation of peroxisome proliferator-activated receptorγ suppresses telomerase activity in vascular smooth muscle cells. Circ Res 98:e50–e59
Rittirsch D, Hoesel LM, Ward PA (2007) The disconnect between animal models of sepsis and human sepsis. J Leukoc Biol 81:137–143
Siddiqui AM, Cui X, Wu R, Dong W, Zhou M, Hu M, Simms H, Wang P (2006) The anti-inflammatory effect of curcumin in an experimental model of sepsis is mediated by up-regulation of peroxisome proliferators-activated receptor-γ. Crit Care Med 34:1874–1882
Collin M, Abdelrahman M, Thiemermann C (2004) Endogenous ligands of PPAR-γ reduce the liver injury in haemorrhagic shock. Eur J Pharmacol 486:233–235
Cuzzocrea S, Pisano B, Dugo L, Ianaro A, Patel NSA, Paola RD, Genovese T, Chatterjee PK, Fulia F, Cuzzocrea E, Rosa MD, Caputi AP, Thiemermann C (2004) Rosiglitazone, a ligand of the peroxisome proliferator-activated receptor-γ, reduces the development of nonseptic shock induced by zymosan in mice. Crit Care Med 32:457–466
Collin M, Patel NSA, Dugo L, Thiemermann C (2004) Role of peroxisome proliferator-activated receptor-γ in the protection afforded by 15-deoxyΔ12:14 prostaglandin J2 against the multiple organ failure caused by endotoxin. Crit Care Med 32:826–831
Paumelle R, Blanquart C, Briand O, Barbier O, Duhem C, Woerly G, Percevault F, Fruchart JC, Dombrowicz D, Glineur C, Staels B (2006) Acute antiinflammatory properties of statins involve peroxisome proliferator-activated receptor-α via inhibition of the protein kinase C signaling pathway. Circ Res 98:361–369
Wiel E, Lebuffe G, Robin E, Gasan G, Corseaux D, Tavernier B, Jude B, Bordet R, Vallet B (2005) Pretreatment with peroxisome proliferator-activated receptorα agonist fenofibrate protects endothelium in rabbit Escherichia coli endotoxin-induced shock. Intensive Care Med 31:1269–1279
Walley KR, Lukacs NW, Standiford TJ, Strieter RM, Kunkel SL (1996) Balance of inflammatory cytokines related to severity and mortality of murine sepsis. Infect Immun 64:4733–4738
Li Y, Li X, Haley M, Fitz Y, Gerstenberger E, Banks SM, Eichacker PQ, Cui X (2006) DTPA Fe (III) decreases cytokines and hypotension but worsens survival with Escherichia coli sepsis in rats. Intensive Care Med 32:1263–1270
Eyal FG, Hamm CR, Parker JC (2007) Reduction in alveolar macrophages attenuates acute ventilator lung injury in rats. Intensive Care Med 33:1212–1218
Campia U, Matuskey LA, Panza JA (2006) Peroxisome proliferator-activated receptor-γ activation with pioglitazone improves endothelium-dependent dilation in nondiabetic patients with major cardiovascular risk factors. Circulation 113:867–875
Marx N, Whorle J, Nusser T, Walcher D, Rinker A, Hombach V, Koenig W, Hoher M (2005) Pioglitazone reduces neointima volume after coronary stent implamtation. Circulation 112:2792–2798
Grainger DJ, Reckless J, McKilligin E (2004) Apolipoprotein E modulates clearance of apoptic bodies in vitro and in vivo, resulting in a systemic proinflammatory state in apolipoprotein E-deficient mice. J Immunol 173:6366–6375
Acknowledgements
We thank Michiyo Deushi and Noriko Tamura for excellent technical assistance. We also appreciate Dr. Julie Trudel's kind advice.
Author information
Authors and Affiliations
Corresponding author
Additional information
This study was supported by grants-in-aid from the Japanese Ministry of Education, Culture, Sports, Science, and Technology.
Electronic supplementary material
Rights and permissions
About this article
Cite this article
Haraguchi, G., Kosuge, H., Maejima, Y. et al. Pioglitazone reduces systematic inflammation and improves mortality in apolipoprotein E knockout mice with sepsis. Intensive Care Med 34, 1304–1312 (2008). https://doi.org/10.1007/s00134-008-1024-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00134-008-1024-9