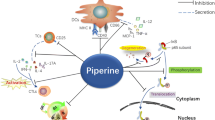
Abstract
Oral lichen planus (OLP) is a T-cell-mediated inflammatory autoimmune disease, whose pathogenesis includes both antigen-specific and non-specific mechanisms. Antigen-specific mechanisms in OLP consist of antigen presentation, lymphocyte activation, proliferation and migration as well as keratinocyte apoptosis mediated by CD8+ cytotoxic T-cells, whereas non-specific mechanisms include mast cell degranulation and matrix metalloproteinase (MMP) activation in OLP lesions. Deficient antigen-specific transforming growth factor-β (TGF-β)-mediated immunosuppression may also contribute to the pathogenesis of OLP. In addition, OLP is considered to be a potentially malignant disorder with a malignant transformation rate of 0–5.3%. Green tea, especially epigallocatechin-3-gallate, possesses anti-inflammatory and chemopreventive properties. It can inhibit antigen presentation, T-cell activation, proliferation and migration, keratinocyte apoptosis, nuclear factor-kappaB (NF-кB) activation and MMP-9 activity, as well as regulated on activation, normal T-cell expressed and secreted (RANTES) expression, and can modulate the imbalance between TGF-β and interferon-γ signaling, all of which are involved in the pathogenesis of OLP. Thus, our hypothesis is that green tea consumption may decrease OLP incidence and provide a neoteric, nontoxic and inexpensive therapeutic strategy for OLP. Furthermore, green tea might be a possible agent for preventing malignancies in OLP.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Oral lichen planus (OLP) is a common T-cell-mediated inflammatory autoimmune disease with the features of disease chronicity, adult onset, female predilection, depressed immune suppressor activity and the presence of auto-cytotoxic T-cell clones in lichen planus lesions [1]. OLP is characterized by T-cell accumulation in the superficial lamina propria, basement membrane disruption, intra-epithelial T-cell migration and keratinocyte apoptosis, resulting from both antigen-specific and non-specific mechanisms [2]. Antigen-specific mechanisms in OLP consist of antigen presentation, lymphocyte activation, proliferation and migration as well as keratinocyte apoptosis mediated by CD8+ cytotoxic T cells, whereas non-specific mechanisms include mast cell degranulation and matrix metalloproteinase (MMP) activation in OLP lesions [2]. Moreover, deficient antigen-specific transforming growth factor (TGF-β)-mediated immunosuppression may contribute to the pathogenesis of OLP [3]. OLP is considered to be a potentially malignant disorder and carcinogenesis in OLP may be modulated by the integrative signal from various tumor inhibitors and promoters [2, 4].
Green tea, a popular, tasty and inexpensive beverage, is consumed throughout the world and has been suggested to have many potential health benefits. Green tea is a rich source of the polyphenols known as catechins, including epicatechin (EC), epicatechin-3-gallate (ECG), epigallocatechin (EGC) and epigallocatechin-3-gallate (EGCG) [5]. EGCG is the most biologically active catechin in green tea and accounts for 50–80% of the total tea catechins [6]. It has been investigated in recent years because of its anti-inflammatory and immunomodulatory activities [7, 8]. Findings indicated that EGCG supplementation may be beneficial to those with abnormally excessive T-cell function such as in autoimmune and inflammatory disorders [9]. Evidence has also suggested that green tea could be therapeutically beneficial for autoimmune disease such as osteoarthritis, rheumatoid arthritis, autoimmune diabetes, Sjögren’s syndrome and lupus erythematosus [10–13]. However, research on the connection between green tea consumption and OLP is still inconclusive. In addition, present therapies for OLP are far from satisfactory because of various side effects [14]. Thus, we speculate that green tea consumption, through its anti-inflammatory and immunomodulatory activities, may affect OLP at multiple levels.
Based on the anti-inflammatory and chemopreventive properties of green tea, we here surmise that green tea consumption may have a potential to manage OLP by modulating antigen-specific and non-specific mechanisms involved in the pathogenesis of OLP. In addition, green tea consumption may prevent OLP from malignant transformation.
Effect of green tea consumption on antigen-specific mechanisms in OLP
Inhibition of antigen presentation
In antigen-specific mechanisms of OLP, antigen presentation as the first step can activate T cells and trigger a subsequent autoimmune reaction [15]. To stimulate a T-cell response, dendritic cells (DCs) and presumably Langerhans cells (LCs) must undergo a process of terminal differentiation called maturation [2]. After maturation, antigen-presenting cells (APCs) endocytose apoptotic basal keratinocytes, activate self-reactive CD4+ T cells and then promote autoimmune reactions against basal keratinocytes [1]. EGCG, at 4–10 times higher doses than its daily intake from green tea (2.5 mmol/L), can inhibit the differentiation, terminal maturation and antigen-presenting function of DCs, and induce their apoptosis, possibly by increased production of interleukin (IL)-10 [7, 16]. Accordingly, we propose that treatment of OLP may profit from the inhibitory effects of EGCG on DCs.
Effects of EGCG on T cells
Subsequently, T-cell activation, proliferation, migration and keratinocyte apoptosis mediated by CD8+ cytotoxic T cells involve in antigen-specific mechanisms of OLP. In OLP, most lymphocytes in the lamina propria are CD4+ T cells, while the majority of lymphocytes within the epithelium and adjacent to damaged basal keratinocytes are activated CD8+ T cells [3]. Helper CD4+ T cells may be activated by antigen associated with major histocompatibility complex (MHC) II presented by Langerhans cells or keratinocytes, and secrete T-helper-1 (Th1) cytokines such as IL-2 and interferon-γ (IFN-γ) which bind their respective receptors on CD8+ T cells [2, 17]. With the combination of antigen associated with MHC I on basal keratinocytes and Th1 cytokines, cytotoxic CD8+ T cells are activated and trigger basal keratinocyte apoptosis, possibly via secreted tumour necrosis factor-α (TNF-α), resulting in the clinical and histological appearance of OLP [2, 3, 18]. Notably, studies showed that both in-vivo and in-vitro supplementation with EGCG at physiologically relevant concentrations of 2.5–10 μM can reduce T-cell proliferation [19]. One possibility is that EGCG may reduce expression of IL-2R in T cells rather than decrease IL-2 synthesis to impair IL-2/IL-2R signaling, which may in turn, through corresponding downstream pathways, affect cell cycle regulatory proteins and lead to inhibition of cell cycle division and progression [19]. Another possibility is that EGCG may function as a proteasome inhibitor to suppress T-cell activation and proliferation [20, 21]. In addition, green tea catechin, especially EGCG, can decrease adhesive and migratory properties of CD8+ T cells to sites of inflammation by downregulating CD11b expression on CD8+ T cells [22]. Therefore, EGCG supplementation may be beneficial for OLP by inhibiting T-cell activation and proliferation as well as modulating the migration of CD8+ T cells to sites of inflammation.
Influence of EGCG on NF-кB signaling pathway
EGCG has been shown to inhibit nuclear factor-kappaB (NF-кB) activation in intestinal epithelial cells, respiratory epithelial cells, endothelial cells and mast cells [23–26]. Our previous study indicated that there was strong nuclear expression of p65, which may represent NF-кB activation, both in epithelial keratinocytes and infiltrated lymphocytes in OLP but not in normal oral mucosa [27]. EGCG has been reported to inhibit NF-кB activation through inhibition of p65 phosphorylation [24]. Similarly, higher NF-κB nuclear expression was demonstrated in oral LP than in cutaneous LP and was associated with significantly increased numbers of cytotoxic lymphocytes within the infiltrate [28]. Increased NF-κB activity might correlate with the severity of OLP and contribute to the long-lasting course and relapse of OLP [28]. NF-κB, a master switch or control point for the expression of a large number of proinflammatory genes, can induce the production of several proinflammatory cytokines such as TNF-α, IL-1β, IL-2 and IL-6, chemokines (IL-8), and adhesion molecules such as intercellular adhesion molecule-1 (ICAM-1), which can ultimately cause a dysregulated inflammatory cascade that results in significant autoinjury to the host [29]. It is indicated that pro-inflammatory NF-κB-dependent cytokines, including TNF-α, IL-1α, IL-6 and IL-8, may be elevated to various degrees in serum, oral keratinocytes, tissue-infiltrated mononuclear cells and various oral fluids (i.e., whole saliva, saline rinse and tissue transudate) in patients with OLP [30]. To sum up, all data confirm that increased NF-κB and NF-κB-dependent inflammation contribute to the outcome of OLP and strongly support the concept of therapeutic strategies targeting the NF-κB pathway, thereby limiting the inherent redundancy of the inflammatory cascade. For example, EGCG potently inhibits production of TNF-α by inhibition of NF-κB activation to protect keratinocytes in OLP from TNF-α-induced apoptosis, whereas EGCG may decrease ICAM-1 by inhibition of NF-κB activation to reduce tissue infiltration of T cells in OLP [1, 31]. Thus, green tea polyphenols, especially EGCG, potentially become a novel therapeutic strategy for OLP by inhibiting NF-κB activation and subsequent production of proinflammatory cytokines, chemokines and adhesion molecules in OLP.
Effects of EGCG on non-specific mechanisms in OLP
Inhibition of MMP-9 and RANTES expression
Non-specific T cells in OLP may contribute to disease pathogenesis by secreting matrix metalloproteinase-9 (MMP-9) and regulated on activation, normal T cell expressed and secreted (RANTES) [2]. MMPs are a family of zinc-containing endo-proteinases whose main function is the proteolytic degradation of connective tissue matrix proteins. The gelatinases (MMP-2 and -9) cleave type IV collagen and the stromelysins (MMP-3 and -10) cleave collagen IV and laminin. MMPs or proMMPs can form complexes with tissue inhibitor metalloproteinases (TIMPs) which are involved in regulating MMP proteolysis [32]. Since MMPs play an essential role in immune cell migration into inflammatory sites, tumor spread and connective tissue destruction, an imbalance in their expression or activity may have important consequences in various pathologies such as rheumatoid arthritis, multiple sclerosis and the development of cancers [11, 33, 34]. A previous study indicated that relative overexpression of MMP-9 (compared with TIMP-1) may cause T-cell migration and basement membrane disruption which further facilitate intra-epithelial CD8+ cytotoxic T-cell migration in OLP [32]. T-cell-derived MMP-9 may therefore play a central role in disease pathogenesis and novel therapies may include blocking MMP-9 activity in OLP. Demeule et al. indicated that EGCG was the most potent inhibitor of MMP-2, MMP-9 and MMP-12, followed by ECG [35]. EGCG has also been shown to inhibit MMP-9 activity and MMP-9 expression [34]. Studies have documented that EGCG not only decreased the level of MMP production but also increased the expression of TIMP-1 in vitro [36]. RANTES secreted by OLP lesional T cells may attract mast cells into the developing OLP lesion and subsequently stimulate mast cell degranulation, which would release TNF-α and chymase, in turn upregulating OLP lesional T-cell RANTES secretion. EGCG has been shown to downregulate IL-1β-induced RANTES [37]. Overall, consumption of green tea or EGCG may inhibit the expression of MMP-9 and RANTES involved in the non-specific mechanisms of OLP and this may have a therapeutic benefit for OLP.
Modulation of the imbalance between TGF-β and IFN-γ signaling
Weak expression of TGF-β1 has been found in OLP and its chronicity may be due, in part, to a defect in the TGF-β1 immunosuppressive pathway [1]. TGF-β1 activity is mediated via the TGF-β II receptor, with subsequent phosphorylation of the TGF-β I receptor [2]. In addition, local overproduction of IFN-γ by Th1 CD4+ T cells in OLP lesions would downregulate the immunosuppressive effect of TGF-β1 and upregulate keratinocyte MHC class II expression and CD8+ cytotoxic T-cell activity [1]. Recently, EGCG was shown to exert a stimulatory effect on expressions of TGF-β1, TGF-β I receptor, TGF-β2, and TGF-β II receptor in the presence of IL-1 in mice [38]. It is found that EGCG interrupts TGF-β signaling in activated hepatic stellate cells by suppressing gene expression of TGF-β I receptor and TGF-β II receptor [39]. EGCG also can reduce IFN-γ production [9]. This suggests that EGCG has the potential to treat OLP by upregulating TGF-β1 expression associated with its receptors and downregulating IFN-γ production, which promotes the balance between TGF-β and IFN-γ signaling.
Potential of green tea consumption to prevent malignancies in OLP
OLP carries a malignant potential, and its malignant transformation rate is 0–5.3% [40]. The integrated signal from various tumor inhibitors and promoters may determine the sensitivity of oral keratinocytes to exogenous mutagens and may regulate tumor growth and metastasis following cancer formation in OLP. Some direct evidence was reported on the role of green tea in the protection of oral pre-cancerous mucosa lesions [41]. EGCG was also found to inhibit the migration and invasion of human oral cancer cells by inhibiting the activation of MMP-2, MMP-9 and urokinase plasminogen activator (uPA) in a dose-dependent manner [34]. Dietary supplements of tea may serve that purpose in vivo, although 10 cups (120 ml/cup) of green tea daily supplemented with green tea tablets have been recommended to the general population for the prevention of cancer [42]. Overall, green tea might be a possible agent for preventing malignancies in OLP.
Conclusion
In conclusion, green tea, especially EGCG, is likely to be a suitable therapeutic candidate for OLP, as a result of its inhibition of antigen presentation, T-cell activation, proliferation and migration, keratinocyte apoptosis, NF-кB activation and MMP-9 activity as well as RANTES expression and its modulation of the imbalance between TGF-β and IFN-γ signaling. Furthermore, green tea might be a possible agent for preventing malignancies in OLP. Green tea consumption in general has not displayed any acute or chronic toxic effects, and in fact is health promoting [43]. EGCG has been showed to have markedly anti-allergic, anti-diabetic, anti-obesity, anti-cardiovascular disease, anti-bacterial, anti-viral, anti-periodontal gum diseases and anti-cariogenic/cariostatic effects [12, 44–49]. However, harmful effects of green tea overconsumption could be due to two main factors: caffeine content and the presence of aluminum [50]. Overconsumption of green tea may cause nervousness, sleep disorder, vomiting, headaches and tachycardia, but green tea presents low toxicity and high tolerance in human subjects, even when given in doses of EGCG as high as 1,600 mg [50]. It seems likely that much higher doses than the daily intake of EGCG from green tea are necessary for the immunosuppressive effects of EGCG to develop. Thus, pharmaceutical formulations of green tea would be necessary to achieve these plasma levels and caution should be taken in consuming large amounts of green tea. In any case, oral green tea consumption could provide a neoteric, nontoxic and inexpensive therapeutic strategy for OLP.
References
Roopashree MR, Gondhalekar RV, Shashikanth MC, George J, Thippeswamy SH, Shukla A. Pathogenesis of oral lichen planus––a review. J Oral Pathol Med. 2010;39:729–34.
Sugerman PB, Savage NW, Walsh LJ, Zhao ZZ, Zhou XJ, Khan A, et al. The pathogenesis of oral lichen planus. Crit Rev Oral Biol Med. 2002;13:350–65.
Lodi G, Scully C, Carrozzo M, Griffiths M, Sugerman PB, Thongprasom K. Current controversies in oral lichen planus: report on an international consensus meeting. Part 1. Viral infections and etiopathogenesis. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2005;100:40–51.
Warnakulasuriya S, Johnson NW, van der Waal I. Nomenclature and classification of potentially malignant disorders of the oral mucosa. J Oral Pathol Med. 2007;36:575–80.
Cabrera C, Artacho R, Gimenez R. Beneficial effects of green tea––a review. J Am Coll Nutr. 2006;25:79–99.
Yang CS, Maliakal P, Meng X. Inhibition of carcinogenesis by tea. Annu Rev Pharmacol Toxicol. 2002;42:25–54.
Yoneyama S, Kawai K, Tsuno NH, Okaji Y, Asakage M, Tsuchiya T, et al. Epigallocatechin gallate affects human dendritic cell differentiation and maturation. J Allergy Clin Immunol. 2008;121:209–14.
Kawai K, Tsuno NH, Kitayama J, Okaji Y, Yazawa K, Asakage M, et al. Epigallocatechin gallate induces apoptosis of monocytes. J Allergy Clin Immunol. 2005;115:186–91.
Wu D, Guo Z, Ren Z, Guo W, Meydani SN. Green tea EGCG suppresses T cell proliferation through impairment of IL-2/IL-2 receptor signaling. Free Radic Biol Med. 2009;47:636–43.
Varilek GW, Yang F, Lee EY, deVilliers WJ, Zhong J, Oz HS, et al. Green tea polyphenol extract attenuates inflammation in interleukin-2-deficient mice, a model of autoimmunity. J Nutr. 2001;131:2034–9.
Ahmed S. Green tea polyphenol epigallocatechin 3-gallate in arthritis: progress and promise. Arthritis Res Ther. 2010;12:208.
Fu Z, Zhen W, Yuskavage J, Liu D. Epigallocatechin gallate delays the onset of type 1 diabetes in spontaneous non-obese diabetic mice. Br J Nutr. 2011;105:1218–25.
Hsu S, Dickinson D. A new approach to managing oral manifestations of Sjogren’s syndrome and skin manifestations of lupus. J Biochem Mol Biol. 2006;39:229–39.
Carrozzo M, Thorpe R. Oral lichen planus: a review. Minerva Stomatol. 2009;58:519–37.
Sugerman PB, Savage NW, Zhou X, Walsh LJ, Bigby M. Oral lichen planus. Clin Dermatol. 2000;18:533–9.
Ullmann U, Haller J, Decourt JP, Girault N, Girault J, Richard-Caudron AS, et al. A single ascending dose study of epigallocatechin gallate in healthy volunteers. J Int Med Res. 2003;31:88–101.
Farhi D, Dupin N. Pathophysiology, etiologic factors, and clinical management of oral lichen planus, part I: facts and controversies. Clin Dermatol. 2010;28:100–8.
Sugerman PB, Satterwhite K, Bigby M. Auto-cytotoxic T cell clones in lichen planus. Br J Dermatol. 2000;142:449–56.
Pae M, Ren Z, Meydani M, Shang F, Meydani SN, Wu D. Epigallocatechin-3-gallate directly suppresses T cell proliferation through impaired IL-2 utilization and cell cycle progression. J Nutr. 2010;140:1509–15.
Nam S, Smith DM, Dou QP. Ester bond-containing tea polyphenols potently inhibit proteasome activity in vitro and in vivo. J Biol Chem. 2001;276:13322–30.
Berges C, Haberstock H, Fuchs D, Miltz M, Sadeghi M, Opelz G, et al. Proteasome inhibition suppresses essential immune functions of human CD4+ T cells. Immunology. 2008;124:234–46.
Kawai K, Tsuno NH, Kitayama J, Okaji Y, Yazawa K, Asakage M, et al. Epigallocatechin gallate attenuates adhesion and migration of CD8+ T cells by binding to CD11b. J Allergy Clin Immunol. 2004;113:1211–7.
Yang F, Oz HS, Barve S, deVilliers WJ, McClain CJ, Varilek CW. The green tea polyphenol (−)-epigallocatechin-3-gallate blocks nuclear factor-kappa B activation by inhibiting I kappa B kinase activity in the intestinal epithelial cell line IEC-6. Mol Pharmacol. 2001;60:528–33.
Wheeler DS, Catravas JD, Odoms K, Denenberg A, Malhotra V, Wong HR. Epigallocatechin-3-gallate, a green tea-derived polyphenol, inhibits IL-1 beta-dependent proinflammatory signal transduction in cultured respiratory epithelial cells. J Nutr. 2004;134:1039–44.
Hong MH, Kim MH, Chang HJ, Kim NH, Shin BA, Ahn BW, et al. (−)-Epigallocatechin-3-gallate inhibits monocyte chemotactic protein-1 expression in endothelial cells via blocking NF-kappaB signaling. Life Sci. 2007;80:1957–65.
Shin HY, Kim SH, Jeong HJ, Kim SY, Shin TY, Um JY, et al. Epigallocatechin-3-gallate inhibits secretion of TNF-alpha, IL-6 and IL-8 through the attenuation of ERK and NF-kappaB in HMC-1 cells. Int Arch Allergy Immunol. 2007;142:335–44.
Zhou G, Xia K, Du GF, Chen XM, Xu XY, Lu R, et al. Activation of nuclear factor-kappa B correlates with tumor necrosis factor-alpha in oral lichen planus: a clinicopathologic study in atrophic-erosive and reticular form. J Oral Pathol Med. 2009;38:559–64.
Santoro A, Majorana A, Bardellini E, Festa S, Sapelli P, Facchetti F. NF-kappaB expression in oral and cutaneous lichen planus. J Pathol. 2003;201:466–72.
Barnes PJ, Karin M. Nuclear factor-κB: a pivotal transcription factor in chronic inflammatory diseases. N Engl J Med. 1997;336:1066–71.
Rhodus NL, Cheng B, Myers S, Bowles W, Ho V, Ondrey F. A comparison of the pro-inflammatory, NF-kappaB-dependent cytokines: TNF-alpha, IL-1-alpha, IL-6, and IL-8 in different oral fluids from oral lichen planus patients. Clin Immunol. 2005;114:278–83.
Yang F, de Villiers WJ, McClain CJ, Varilek GW. Green tea polyphenols block endotoxin-induced tumor necrosis factor-production and lethality in a murine model. J Nutr. 1998;128:2334–40.
Zhou XJ, Sugerman PB, Savage NW, Walsh LJ. Matrix metalloproteinases and their inhibitors in oral lichen planus. J Cutan Pathol. 2001;28:72–82.
Benesová Y, Vasku A, Novotná H, Litzman J, Stourac P, Beránek M, et al. Matrix metalloproteinase-9 and matrix metalloproteinase-2 as biomarkers of various courses in multiple sclerosis. Mult Scler. 2009;15:316–22.
Ho YC, Yang SF, Peng CY, Chou MY, Chang YC. Epigallocatechin-3-gallate inhibits the invasion of human oral cancer cells and decreases the productions of matrix metalloproteinases and urokinase-plasminogen activator. J Oral Pathol Med. 2007;36:588–93.
Demeule M, Brossard M, Pagé M, Gingras D, Béliveau R. Matrix metalloproteinase inhibition by green tea catechins. Biochim Biophys Acta. 2000;1478:51–60.
Lee JH, Chung JH, Cho KH. The effects of epigallocatechin-3-gallate on extracellular matrix metabolism. J Dermatol Sci. 2005;40:195–204.
Ahmed S, Pakozdi A, Koch AE. Regulation of interleukin-1beta-induced chemokine production and matrix metalloproteinase 2 activation by epigallocatechin-3-gallate in rheumatoid arthritis synovial fibroblasts. Arthritis Rheum. 2006;54:2393–401.
Andriamanalijaona R, Kypriotou M, Baugé C, Renard E, Legendre F, Raoudi M, et al. Comparative effects of 2 antioxidants, selenomethionine and epigallocatechin-gallate, on catabolic and anabolic gene expression of articular chondrocytes. J Rheumatol. 2005;32:1958–67.
Yumei F, Zhou Y, Zheng S, Chen A. The antifibrogenic effect of (-)-epigallocatechin gallate results from the induction of de novo synthesis of glutathione in passaged rat hepatic stellate cells. Lab Invest. 2006;86:697–709.
Lodi G, Scully C, Carrozzo M, Griffiths M, Sugerman PB, Thongprasom K. Current controversies in oral lichen planus; report of an international consensus meeting––Part 2. Management and malignant transformation. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2005;100:164–78.
Li N, Sun Z, Han C, Chen J. The chemopreventive effects of tea on human oral precancerous mucosa lesions. Proc Soc Exp Biol Med. 1999;220:218–24.
Fujiki H, Suganuma M, Imai K, Nakachi K. Green tea: cancer preventive beverage and/or drug. Cancer Lett. 2002;188:9–13.
Schwarz B, Bischof HP, Kunze M. Coffee, tea, and lifestyle. Prev Med. 1994;23:377–84.
Maeda-Yamamoto M, Ema K, Shibuichi I. In vitro and in vivo anti-allergic effects of ‘benifuuki’ green tea containing O-methylated catechin and ginger extract enhancement. Cytotechnology. 2007;55:135–42.
Basu A, Sanchez K, Leyva MJ, Wu M, Betts NM, Aston CE, et al. Green tea supplementation affects body weight, lipids, and lipid peroxidation in obese subjects with metabolic syndrome. J Am Coll Nutr. 2010;29:31–40.
Hernández Figueroa TT, Rodríguez-Rodríguez E, Sánchez-Muniz FJ. The green tea, a good choice for cardiovascular disease prevention? Arch Latinoam Nutr. 2004;54:380–94
Friedman M. Overview of antibacterial, antitoxin, antiviral, and antifungal activities of tea flavonoids and teas. Mol Nutr Food Res. 2007;51:116–34.
Yu H, Oho T, Tagomori S, Morioka T. Anticariogenic effects of green tea. Fukuoka Igaku Zasshi. 1992;83:174–80.
Yun JH, Pang EK, Kim CS, Yoo YJ, Cho KS, Chai JK, et al. Inhibitory effects of green tea polyphenol (–)-epigallocatechin gallate on the expression of matrix metalloproteinase-9 and on the formation of osteoclasts. J Periodontal Res. 2004;39:300–7.
Singh R, Akhtar N, Haqqi TM. Green tea polyphenol epigallocatechin-3-gallate: inflammation and arthritis. Life Sci. 2010;86:907–18.
Acknowledgments
This work was supported by a Grant (No. 30973311, No. 81170972) from the National Natural Science Foundation of China.
Author information
Authors and Affiliations
Corresponding author
Additional information
Responsible Editor: Michael Parnham.
Rights and permissions
About this article
Cite this article
Zhang, J., Zhou, G. Green tea consumption: an alternative approach to managing oral lichen planus. Inflamm. Res. 61, 535–539 (2012). https://doi.org/10.1007/s00011-012-0440-z
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00011-012-0440-z