Abstract
Background
Oral lichen planus (OLP) is a T-cell-mediated inflammatory disease with a risk of malignant transformation. Although the etiology of OLP is still uncertain, growing evidence suggests that oral microbiota, antigen-specific, and non-specific mechanisms are involved in the pathogenesis of OLP. Antigen-specific mechanisms include antigen presentation, T-cell activation, nuclear factor-kappa B signaling pathway, and cytokine secretion, while non-specific mechanisms consist of matrix metalloproteinases (MMP)-9 upregulation, psychological pressure, oxidative damage, aberrant expression of microRNAs (miRNAs), and autophagy. Till now, there is no cure for OLP, and the main purpose of OLP therapy is symptomatic control.
Finding
Seafood and its derivative omega-3 polyunsaturated fatty acids (n-3 PUFAs) can suppress antigen presentation, T-cell activation, and nuclear factor-kappa B signaling pathway, modulate the overexpressed inflammatory cytokines, inhibit the expression of MMP-9, as well as regulate the expression of miRNAs and autophagy. And they are possible agents for ameliorating psychological disorder and oxidative damage. Moreover, n-3 PUFAs supplementation has a beneficial effect on preventing tumorigenesis.
Conclusion
n-3 PUFAs consumption may provide a non-toxic, inexpensive administration for OLP.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
OLP is a chronic immune and inflammatory disease mainly affecting the oral mucosa [1, 2]. The prevalence of OLP in general adult population is 0.5–2% with a female predisposition and children can also be involved [2, 3]. OLP carries a potential risk of malignancy, with an oral squamous cell carcinoma transformation rate of 0.9–1.1% [4]. OLP classically affects the buccal mucosa, gingiva, and tongue, exhibiting a bilateral and symmetrical pattern [2, 5]. There are six clinical subtypes of OLP: reticular, plaque-like, atrophic, erosive, papular, and bullous [5, 6]. The dysbiosis of subgingival microbiota mainly result in periodontitis [7]. Similarly, the imbalance between protective and harmful bacteria in oral mucosa is associated with the pathogenesis of OLP [8]. On one hand, pathological features show dense subepithelial lymphocytes infiltration and intraepithelial CD8+ cytotoxic T lymphocytes (CTLs) targeting the basal keratinocytes (Fig. 1) [1, 2, 9, 10]. Our group revealed that T helper (Th) 1-type immune response plays a prominent role in the pathogenesis of OLP. The expression of T-bet was related to different clinical features of OLP [11]. Th17 cells with the secretion of interleukin (IL)-17 highlighted its role in the development of different types of OLP [12]. On the other hand, MMP activation, psychological disorder, and oxidative damage are correlated with the exacerbation of OLP [2, 5, 10, 13, 14]. Currently, a permanent cure is not available and corticosteroids are well known as the first-line treatment for OLP. To some degree, long-term use of corticosteroids has side effects, ranging from acne to damage on most major organ systems such as musculoskeletal, gastrointestinal, and cardiovascular system [15]. Thus, it is crucial to find a novel and relatively safe substance for OLP.
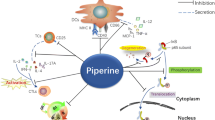
n-3 PUFAs act on the immune cells of OLP. n-3 PUFAs could inhibit the expression of ICAM-1, LFA-1, MHC II, and CD80 on DCs, and suppress the expression of CD28 on Th cells, interfering the interaction between dendritic cells and Th cells and further restraining the activation of cytotoxic T cells which kill the basal keratinocytes. n-3 PUFAs also could inhibit the development of Th1 and Th17 through down-regulating the production of IL-2, TNF-α, IFN-γ, and IL-17
Omega-3 polyunsaturated fatty acids (n-3 PUFAs) are extracted from transgenic plants, fungi, and other microorganisms but mostly fatty fish [16, 17]. n-3 PUFAs and their derivatives, especially eicosapentaenoic acid (EPA) and docosahexaenoic acid (DHA), were reported to exert anti-inflammatory and immunomodulatory effects through multiple mechanisms [18]. Oral cavity is colonized with microbiomes and changes of these bacteria lead to oral diseases. Usage of DHA with low-dose aspirin influenced the periodontitis which is initiated by bacteria [7]. The T-cell activation can be suppressed by n-3 PUFAs through the modulation of plasma membrane microdomains [19, 20]. Consumption of n-3 PUFAs is a crucial determinant of inflammatory and immune processes. Omega-3 fatty acids could inhibit the polarization of splenic CD4+ T cells into the inflammatory Th1 and Th17-cell subset [21,22,23]. Data suggested that n-3 PUFAs would be beneficial to inflammation and autoimmune diseases such as rheumatoid arthritis, Crohn’s disease, ulcerative colitis, psoriasis, lupus erythematosus, and multiple sclerosis [24,25,26,27,28]. Of note, omega-3 fatty acids had a psychological-protective role due to their regulatory effects on hypothalamic–pituitary–adrenocortical (HPA) axis [29]. EPA and DHA were able to reduce salivary cortisol in healthy adults and defend against the increased oxidative stress [30, 31]. n-3 PUFAs are considered as safety seafood in many aspects [32].
Based on these facts, we speculate that n-3 PUFAs may have a therapeutic potency for OLP through antigen-specific and non-specific mechanisms involved in the pathogenesis of OLP.
Status of Omega-3 polyunsaturated fatty acids in oral microbial community
As the entry part of the gastrointestinal tract, oral cavity and its microorganisms are essential to OLP. Streptococcus was decreased and gingivitis bacteria exhibited positive correlations with the levels of infiltrated CD3+, CD4+, and CD8+ cells in OLP lesions [8]. Fusobacterium, Leptotrichia, and Lautropia were abundant in the buccal mucosa of OLP [33]. Fusobacterium nucleatum and Treponema denticola damaged the physical barrier of epithelial cells [34]. Saliva samples of OLP patients were different in the oral microbiota compared to control group, which were recommended as one of the diagnostic tools for OLP [35]. An 1-year clinical trial showed that oral microbial composition was individual, and the balance between health and disease was influenced by oral microorganism of bacteria and fungi, especially Malassezia [36]. 30% of OLP patients suffered oral candidiasis after corticosteroid therapy [37]. These studies emphasized the primary role of oral microbiota in the pathogenesis of OLP.
During a 3-month pilot trial, daily DHA consumption suppressed the Porphyromonas gingivalis growth and decreased the expression of local inflammatory markers [7, 38]. n-3 PUFAs as functional foods can be considered as prebiotics, because it shows capability of increasing anti-inflammatory molecules, like short-chain fatty acids [39]. On the other hand, n-3 PUFAs are beneficial to preventing chronic inflammatory disease such as inflammatory bowel disease and modulating the microbiota between intestinal wall integrity and host immune cells [16]. 4 g of mixed DHA/EPA supplement (as capsules and functional drink) for 8 week trail increased the amount of Bifidobacterium, Oscillospira, Roseburia, and Lachnospira species, while decreased that of Coprococcus and Faecalibacterium species in human intestinal microbiota [40]. Although the accurate mechanisms that n-3 PUFAs regulate the oral microbial community are unknown, n-3 PUFAs may affect oral microbial diversity.
Influence of n-3 PUFAs on antigen-specific mechanisms of OLP
Effects of n-3 PUFAs on antigen-presenting cells
Dendritic cells (DCs) are necessary and sufficient for the activation of naive T cells [41]. In OLP lesions, DCs primarily Langerhans cells (LCs) are significantly increased in the epithelial–stromal junction where epithelial damage predominantly occurs [42]. These cells have the principal function of capturing pathogens and presenting antigens to T cells, which leads to the primary immune response [10]. Lymphocyte function-associated antigen 1 (LFA-1) is involved in the process of mediated killing, and LFA-1/intercellular adhesion molecule 1 (ICAM-1) interactions have been shown to stimulate signaling pathways that influence T-cell differentiation [43]. When DCs recapture an antigen, the antigen is presented by major histocompatibility class II (MHC II) through an endosomal cellular pathway, triggering a secondary immune response which may explain the appearance of the clinical signs of OLP [10, 44]. DCs are involved in the pathogenesis of antigen-specific mechanisms of OLP.
Dietary intake of n-3 PUFAs inhibits the expression of MHC class II molecules and adhesion molecules ICAM-1 and LFA-1 on human peripheral blood monocytes [45,46,47]. A n-3 PUFAs-rich diet downregulates cell-mediated immune responses. It is possible that one of the mechanisms is the inhibitory function on antigen-presenting cells [45]. Treatment with omega-3 fatty acids gave rise to a significant reduction in DCs proportion when compared to control groups [48]. n-3 PUFAs diminished the antigen presentation activity of rat DCs via reducing the level of MHC II molecule [49]. The key aspects (CD11c+, CD80) of DC surface expression are suppressed by n-3 PUFAs [50]. Therefore, n-3 PUFAs are beneficial to OLP in the antigen presentation aspect (Fig. 1).
Influence of n-3 PUFAs on T cells
When CD4+ T helper cells and CD8+ CTLs binding to MHC II and MHC I molecules, respectively, T cells are activated in OLP lesions [10]. Most of CD4+ T cells infiltrated in the lamina propria; on the contrary, the majority of intraepithelial lymphocytes in OLP are composed almost exclusively of CD8+ CTLs [2, 10]. MHC class II antigen-presenting cells in OLP express high levels of CD40, CD80, and secrete IL-12 which are confirmed to promote a Th1 CD4+ T-cell response with IL-2 and interferon (IFN)-γ secretion [10, 51,52,53]. CD28 is the receptor for CD80 and is one of the expressed molecules that provide signals required for T-cell activation and survival [54]. CD8+ CTLs are involved in disease pathogenesis, and activated CD8+ T cells trigger keratinocyte apoptosis in OLP [55]. The proportion of Th17 cells in patients with OLP was significantly higher than that in controls; furthermore, Th17 cells in atrophic-erosive OLP were elevated when compared with that in reticular OLP [12]. Our previous studies observed a higher T-bet mRNA level and T-bet/GATA-3 mRNA ratios, along with a significantly high expression of programmed cell death receptor-1 and programmed death ligand-1 in OLP patients [11, 56]. T-bet mRNA gives rise to IFN-γ which is the most critical mediators of Th1 [57]. It also manifested the dominance of Th1 CD4+ T lymphocytes in the inflammatory environment, which may stimulate the activities of CD8+ CTLs in OLP [11, 56, 57]. This demonstrates that T-cell immunologic dysregulation plays a central role in the pathogenesis of OLP.
It is worth noting that T-cell proliferation was inhibited through a dietary with highly purified EPA and DHA in a mouse model [58]. n-3 PUFAs suppressed IL-2 secretion and IL-2 receptor α chain mRNA transcription [58, 59]. DHA reduced the production of IL-2 via modifying the important phospholipid-derived intracellular second messengers (e.g., phospholipase Cγ, diacylglycerol, and ceramide) of T cells [58]. n-3 PUFAs were reported to interfere with Ca2+ signaling and suppress mitochondrial translocation to the immunologic synapse, which is crucial in T-cell activation [19, 20]. CD28 and CD80 coreceptors are among the mechanisms by which n-3 PUFAs directly suppress T-cell activation [58,59,60]. Dietary n-3 PUFAs are incorporated into cellular membranes and phospholipids, consequently, affecting lipid metabolism [60,61,62]. n-3 PUFAs have regulatory effects on the suppression of Th1 and Th17 development (Fig. 1) [21, 63, 64].
Inhibition of n-3 PUFAs on the NF-κB signaling pathway
Our previous research revealed an elevation of NF-κB which can be regulated by p65 (a subunit of NF-κB) in the nuclei of infiltrated lymphocytes in OLP [65]. NF-κB signaling pathway is triggered by the Toll-like receptors via proinflammatory factors such as tumor necrosis factor (TNF)-α. The transcriptional downstream of NF-κB is promoted after the phosphorylation of IκBα protein. An overexpression of NF-κB leads to the chronic inflammatory process in OLP [66, 67]. Studies have shown that the expression of NF-κB is inhibited by n-3 PUFAs in the colonic mucosa, arterial endothelial cells, hepatocytes, and kidney [68,69,70]. In general, NF-κB is downregulated through the consumption of n-3 PUFAs in two different manners (Fig. 2): a decline in the activity of the NF-κB subunit p65/RelA by inhibiting phosphorylation, such as p65/RelA serine 536 phosphorylation (p-p65 (S536)) [71]; a high level of inhibition on NF-κB DNA-binding activity and NF-κB p65 subunit nuclear translocation which were observed in rats. Additionally, the mice with SLE were fed with n-3 PUFAs-DHA, which increased the most median life span to 658 days [72]. 4 weeks of feeding with a high ratio of omega-3 fatty acids mice resulted in the attenuation in p65 expression and nuclear localization, leading to the downregulation of NF-κB [73].
Interactions between n-3 PUFAs and NF-κB signaling pathway. NF-κB signaling pathway triggered by TNF-α is promoted after the phosphorylation of IκBα protein. n-3 PUFAs are able to reduce the NF-κB pathway in two ways: inhibiting the phosphorylation of p65, or decreasing the binding activity of NF-κB with DNA and thus impeding the NF-κB p65 subunit nuclear translocation
Effects of n-3 PUFAs on cytokines
Abnormal secretion of cytokines, such as TNF-α, IFN-γ, IL-2, IL-6, and IL-17, is evident in the inflammatory-related cytokines involved in OLP [57]. In addition to TNF-α, increased IFN-γ, IL-6, and IL-17 are identified in the serum and lesions of OLP, respectively, indicating an imbalance in Th1 and Th17 cytokine profiles in OLP [56, 57]. n-3 PUFAs have a privilege effect on the inflammation led by Th1 and Th17. IL-17 is an important proinflammatory cytokine associated with the pathogenesis of OLP [12, 74]. n-3 PUFAs directly affect the development of Th17 cells by reducing expression of the Th17-cell signature cytokine IL-17A and transcription factor RORγt, implicating a n-3 PUFA-dependent, anti-inflammatory mechanism of action via the suppression of the development of this inflammatory T-cell subset [23]. A clinical trial showed the efficacy of 4 g omega-3 fatty acids on TNF-α, IL-6, and nitric oxide catabolites levels, which were decreased by involving competitive inhibition of arachidonic acid. n-3 PUFAs also inhibited the migratory activity of leucocytes via alteration of cytoskeletal components [75,76,77]. n-3 PUFAs may influence OLP by modulating TNF-α, IFN-γ, IL-6, and IL-17.
Effects of n-3 PUFAs on non-specific mechanisms in OLP
Influencing on MMPs via n-3 PUFAs in OLP
Matrix metalloproteinases (MMPs) containing more than 20 members are a family of zinc-containing endo-proteinases with the primary proteolytic function of connective tissue matrix proteins and basement membrane components [78, 79]. A balance can be achieved through the interaction between tissue inhibitors of metalloproteinases (TIMPs) and MMPs, because MMPs are reduced by tissue inhibitors of TIMPs through a stable, inactive enzyme-inhibitor complex with MMPs or pro-MMPs [2]. There is tissue destruction in the pathology of OLP due to an imbalance between MMPs and TIMPs which is found in the pathology of OLP. T cells release MMP-9 activators which assist in the activation of pro-MMP-9, resulting in basement membrane disruption in OLP [2, 10]. Increased MMP expression and an imbalance between MMPs and TIMPs play a pivotal role in the pathogenesis of OLP. Studies have shown an inhibitory effect of n-3 PUFAs on MMP-9 in multiple sclerosis and dystrophic cardiomyopathy [80, 81]. n-3 PUFAs significantly decrease immune cell-secreted MMP-9 levels in vivo [82, 83]. Shinto et al. [80] confirmed that EPA and DHA decreased MMP-9 protein levels and MMP-9 activity, and significantly suppressed human T-cell migration in vitro. n-3 PUFAs modulate the cardiac and skeletal muscle environment towards an anti-inflammatory influence by affecting proinflammatory mediators, including MMP-9 and TIMP-1 [81].
n-3 PUFAs have anti-oxidative effects on OLP
Oxidative stress plays an essential role in the pathogenesis of several inflammatory and autoimmune diseases [84, 85]. In OLP serum, the level of malondialdehyde, a fundamental representative of oxidative stress, was significantly enhance, and the total antioxidant capacity was markedly declined [86], indicating the pathogenic role of oxidative stress in OLP. And reactive oxygen species (ROS), pro-oxidative free radicals, have been found participated in both the OLP pathogenesis and carcinogenesis [14, 85, 87]. It is evident that ROS damages cellular components via free amino acids, protein peroxidation of nucleic acids, and lipoproteins, disrupting cellular processes such as DNA repair and apoptosis [88]. Managing antioxidants in patients with OLP is useful to elaborate on a treatment strategy and to monitor OLP itself. Increased antioxidant genes might be an adaptive reaction against increased oxidative stress. Besides, a diet rich in n-3 PUFAs alters gene expression profiles to defend against excess peroxisome proliferator-activated receptor alpha (PPARα) activation and ROS production [14, 30]. Cells isolated from rats’ diet with n-3 PUFAs exhibited higher proportions of the n-3 PUFAs in their membrane phospholipids and were shown to be less sensitive to the effects of ROS. Anti-oxidative enzyme gene expression was enhanced after dietary supplemented with omega-3 fatty acids [30, 89].
Ameliorating psychological pressure by n-3 PUFAs in OLP
Psychological or mental disorders have a high correlation with OLP [90]. The HPA axis is involved in functional illnesses, such as anxiety disorder, insomnia, and major depressive disorder through regulating the expression of adrenocorticotropin [91]. Cortisol is one of the important substances and exhibits high serum and salivary levels in OLP patients [90, 92]. Sleep disturbances are considered a symptom of mood disorders which are associated with the initiation and relapse of OLP [90]. There is concrete evidence that n-3 PUFAs, notably DHA and EPA, have a stress-protective role, due to their inhibitory effects on stress-elicited adrenal activation through the central nervous system. n-3 PUFAs directly affect the adrenal glands [29, 93, 94]. A randomized trial showed that after treatment with n-3 PUFAs for 6 weeks, there was a decrease in salivary cortisol [31]. Consumption of oily fish rich in omega-3 consumption improved the sleep quality and showed an inverse association with the Pittsburgh sleep quality index [95].
n-3 PUFAs have positive effects on OLP via miRNAs and autophagy
MiRNAs are small non-coding RNA molecules containing about 18-25 nucleotides. MiRNAs function in RNA silencing and post-transcriptional regulation of gene expression [96]. Our previous studies showed that circulating miR-34a-5p and miR-130b-3p were upregulated, while miR-301b-3p and miR-125a were downregulated in OLP. Besides, miR-34a-5p was positively correlated with the severity of OLP [53, 97]. MiR-34a-5p was modulated in OLP progression through the PI3K/Akt signaling pathway. MiR-146a was higher in local lesion with OLP [98]. Several miRNAs, such as miR-let-7 family, are regulated by EPA, leading to the reductions in NF-κB, Toll-like receptor 4, and proinflammatory cytokines in the mouse liver [99]. n-3 PUFAs regulated immune homeostasis in an inflammation rat model through inflammatory pathways by targeting miR-19b-3p, -146b-5p, and -183-5p [100].
Autophagy is a catabolic process that mediates cellular degradation and recycling. Meanwhile, autophagy is an vital pathway for maintaining homeostasis and is connected with human oral diseases [101]. Dietary n-3 PUFAs reduce atherosclerosis inflammation by activating macrophage autophagy and attenuating intracellular ROS [102]. Above all, n-3 PUFAs might downregulate inflammation and help maintain homeostasis on OLP through miRNAs and autophagy.
Preventing malignancy in OLP
The World Health Organization (WHO) identified OLP as an oral potentially malignant disorder (OPMD), which rates approximately 1.1% [4, 103]. Researchers have been attempting to address the malignant transformation of OLP. Biomarkers that can predict malignant transformation have been validated in OLP lesions, such as the increased P53 and MMP-9, and the decreased caspase-3 [104]. Mignogna et al. reported the possible role of macrophages, mast cells, lymphocytes, and fibroblasts which contribute to the process of carcinogenesis in OLP via secreting cytokines, MMPs, and CCL5 molecules. Besides, overexpressed MMPs can cause DNA damage, bypassing p53 tumor suppression function [105]. We also reviewed OLP as one of the OPMD showed a higher expression of p53 and 8-nitroguanine [106].
It is illuminating that n-3 PUFAs have the ability to increase the expression of p53 and modulate Bcl-2 to induce apoptosis of cancer cells [107,108,109,110,111]. The high content of n-3 PUFAs with a decrease in n-6/n-3 PUFA ratio induces apoptosis by p53, Bcl-2, caspase-7, and caspase-3 in cancer cells [109,110,111]. During a 7,12-dimethylbenz(α)anthracene-induced mammary carcinogenesis rats’ model, omega-3 fatty acids have the potential to limit mammary tumorigenesis in vivo by inducing apoptosis and suppressing the growth of the tumor cells [110]. Moreover, n-3 PUFA intake conferred additional benefits and lowered the risk of colorectal cancer-specific mortality to patients with colorectal cancer [112].
Safety of n-3 PUFAs
There is a good image of n-3 PUFAs in public. Fish oil is considered as nutritious supplement for inflammatory bowel disease, cardiovascular, and many other inflammatory diseases. Public health advice is different across countries. European Food Safety Authority suggests that a consumption of 250 mg per day of EPA and DHA appears to be sufficient for healthy subjects, while the American Heart Association (AHA) is more positive [113]. AHA recommends 720 mg per day of EPA and DHA supplements for adults from dietary supplements than from foods (410 mg per day) [114]. Excessive usage of n-3 PUFAs leads to potential risks. Overdose of EPA and DHA may affect platelet activation and significantly reduce platelet aggregation which leads to side effect for wound healing [115]. Public concerns about the low doses of chemical pollutant mixtures (organochlorine pesticides, methylmercury, dioxins, and dibenzofurans) contained in seafood [32]. To minimize the risk of pollutant, it would be necessary to control the quality of seafood products. More importantly, clinicians should balance the potential benefits of n-3 PUFAs supplementation against the potential risks when recommending n-3 PUFAs.
Conclusion
n-3 PUFAs have the properties of inhibiting antigen presentation, T-cell activity, and NF-κB signaling pathway, reducing the production of MMP-9, alleviating psychological disorders oxidative, maintaining miRNAs and autophagy, and preventing malignancy (Fig. 3). In addition, n-3 PUFAs modulate the number of different bacteria in oral cavity and are potential adjunctive management for OLP. Nevertheless, studies about n-3 PUFAs in OLP are still void. To translate theoretical assumption to clinical application, basic experimental studies are needed to figure out what the potential effects of n-3 PUFAs on OLP are in vitro and in vivo. Meanwhile, multi-center randomized blinded controlled trials are necessary to provide evidence-based data of the optimized usage and dosage of n-3 PUFAs for the management of OLP. Given all these possessions of n-3 PUFAs, it is possible to take n-3 PUFAs as a candidate for OLP management. In conclusion, n-3 PUFAs might be a safe, inexpensive, and non-conventional adjunctive therapy for OLP.
Abbreviations
- CTLs:
-
Cytotoxic T lymphocytes
- DCs:
-
Dendritic cells
- DHA:
-
Docosahexaenoic acid
- EPA:
-
Eicosapentaenoic acid
- HPA:
-
Hypothalamic–pituitary–adrenocortical
- ICAM-1:
-
Intercellular adhesion molecule 1
- INF-γ:
-
Interferon-γ
- IL:
-
Interleukin
- LFA-1:
-
Lymphocyte function-associated antigen 1
- LCs:
-
Langerhans cells
- miRNAs:
-
microRNAs
- MHC II:
-
Major histocompatibility class II
- MMPs:
-
Matrix metalloproteinases
- NF-κB:
-
Nuclear factor-kappa B
- n-3 PUFAs:
-
omega-3 Polyunsaturated fatty acids
- OLP:
-
Oral lichen planus
- OPMD:
-
Oral potentially malignant disorder
- PPARα:
-
Peroxisome proliferator-activated receptor alpha
- ROS:
-
Reactive oxygen species
- Th:
-
T helper
- TIMPs:
-
Tissue inhibitors of metalloproteinases
- TNF-α:
-
Tumor necrosis factor-α
References
Carrozzo M, Porter S, Mercadante V, Fedele S. Oral lichen planus: A disease or a spectrum of tissue reactions? Types, causes, diagnostic algorhythms, prognosis, management strategies. Periodontol 2000. 2019;80(1):105–25. https://doi.org/10.1111/prd.12260.
Alrashdan MS, Cirillo N, McCullough M. Oral lichen planus: a literature review and update. Arch Dermatol Res. 2016;308(8):539–51. https://doi.org/10.1007/s00403-016-1667-2.
Khandelwal V, Nayak PA, Nayak UA, Gupta A. Oral lichen planus in a young Indian child. BMJ Case Rep. 2013. https://doi.org/10.1136/bcr-2013-010516.
Aghbari SMH, Abushouk AI, Attia A, Elmaraezy A, Menshawy A, Ahmed MS, et al. Malignant transformation of oral lichen planus and oral lichenoid lesions: a meta-analysis of 20095 patient data. Oral Oncol. 2017;68:92–102. https://doi.org/10.1016/j.oraloncology.2017.03.012.
Gupta S, Jawanda M. Oral Lichen Planus: an update on etiology, pathogenesis, clinical presentation, diagnosis and management. Indian J Dermatol. 2015;60(3):222–9. https://doi.org/10.4103/0019-5154.156315.
Olson MA, Rogers RS, Bruce AJ. Oral lichen planus. Clin Dermatol. 2016;34(4):495–504. https://doi.org/10.1016/j.clindermatol.2016.02.023.
Naqvi AZ, Mu L, Hasturk H, Van Dyke TE, Mukamal KJ, Goodson JM. Impact of docosahexaenoic acid therapy on subgingival plaque microbiota. J Periodontol. 2017;88(9):887–95. https://doi.org/10.1902/jop.2017.160398.
Choi YS, Kim Y, Yoon HJ, Baek KJ, Alam J, Park HK, et al. The presence of bacteria within tissue provides insights into the pathogenesis of oral lichen planus. Sci Rep. 2016;6:29186–99. https://doi.org/10.1038/srep29186.
Kurago ZB. Etiology and pathogenesis of oral lichen planus: an overview. Oral Surg Oral Med Oral Pathol Oral Radiol. 2016;122(1):72–80. https://doi.org/10.1016/j.oooo.2016.03.011.
Roopashree MR, Gondhalekar RV, Shashikanth MC, George J, Thippeswamy SH, Shukla A. Pathogenesis of oral lichen planus—a review. J Oral Pathol Med. 2010;39(10):729–34. https://doi.org/10.1111/j.1600-0714.2010.00946.x.
Lu R, Zhou G, Du GF, Xu XY, Yang JG, Hu JY. Expression of T-bet and GATA-3 in peripheral blood mononuclear cells of patients with oral lichen planus. Arch Oral Biol. 2011;56:499–505. https://doi.org/10.1016/j.archoralbio.2010.11.006.
Xie SX, Ding L, Xiong ZG, Zhu SR. Implications of Th1 and Th17 Cells in pathogenesis of oral lichen planus. J Huazhong Univ Sci Technol. 2012;32(3):451–7. https://doi.org/10.1007/s11596-012-0078-7.
Pippi R, Romeo U, Santoro M, Del Vecchio A, Scully C, Petti S. Psychological disorders and oral lichen planus: matched case-control study and literature review. Oral Dis. 2016;22(3):226–34. https://doi.org/10.1111/odi.12423.
Darczuk D, Krzysciak W, Kaczmarzyk T, Vyhouskaya P, Kesek B, Galecka-Wanatowicz D, et al. Salivary oxidative status in patients with oral lichen planus. J Physiol Pharmacol. 2016;67(6):885–94.
Oray M, Abu Samra K, Ebrahimiadib N, Meese H, Foster CS. Long-term side effects of glucocorticoids. Expert Opin Drug Saf. 2016;15(4):457–65. https://doi.org/10.1517/14740338.2016.1140743.
Parolini C. Effects of fish n-3 PUFAs on intestinal microbiota and immune system. Mar Drugs. 2019;17(6):374–401. https://doi.org/10.3390/md17060374.
Adarme-Vega TC, Lim DKY, Timmins M, Vernen F, Li Y, Schenk PM. Microalgal biofactories: a promising approach towards sustainable omega-3 fatty acid production. Microb Cell Fact. 2012;11(1):96–106. https://doi.org/10.1186/1475-2859-11-96.
Calder PC. Mechanisms of action of (n-3) fatty acids. J Nutr. 2012;142(3):592S–9S. https://doi.org/10.3945/jn.111.155259.
Hou TY, Monk JM, Fan YY, Barhoumi R, Chen YQ, Rivera GM, et al. n-3 polyunsaturated fatty acids suppress phosphatidylinositol 4,5-bisphosphate-dependent actin remodelling during CD4 + T-cell activation. Biochem J. 2012;443(1):27–37. https://doi.org/10.1042/BJ20111589.
Yog R, Barhoumi R, McMurray DN, Chapkin RS. n-3 polyunsaturated fatty acids suppress mitochondrial translocation to the immunologic synapse and modulate calcium signaling in T cells. J Immunol. 2010;184(10):5865–73. https://doi.org/10.4049/jimmunol.0904102.
Shoda H, Yanai R, Yoshimura T, Nagai T, Kimura K, Sobrin L, et al. Dietary omega-3 fatty acids suppress experimental autoimmune uveitis in association with inhibition of Th1 and Th17 cell function. PLoS One. 2015;10(9):e0138241. https://doi.org/10.1371/journal.pone.0138241.
Zhang P, Kim W, Zhou L, Wang N, Ly LH, McMurray DN, et al. Dietary fish oil inhibits antigen-specific murine Th1 cell development by suppression of clonal expansion. J Nutr. 2006;136:2391–8. https://doi.org/10.1093/jn/136.9.2391.
Monk JM, Hou TY, Turk HF, McMurray DN, Chapkin RS. n3 PUFAs reduce mouse CD4 + T-cell ex vivo polarization into Th17 cells. J Nutr. 2013;143(9):1501–8. https://doi.org/10.3945/jn.113.178178.
Gioxari A, Kaliora AC, Marantidou F, Panagiotakos DP. Intake of u-3 polyunsaturated fatty acids in patients with rheumatoid arthritis: a systematic review and meta-analysis. Nutrition. 2018;45:114–24. https://doi.org/10.1016/j.nut.2017.06.023.
Scaioli E, Liverani E, Belluzzi A. The Imbalance between n-6/n-3 polyunsaturated fatty acids and inflammatory bowel disease: a comprehensive review and future therapeutic perspectives. Int J Mol Sci. 2017;18(12):2619–42. https://doi.org/10.3390/ijms18122619.
Clark CCT, Taghizadeh M, Nahavandi M, Jafarnejad S. Efficacy of omega-3 supplementation in patients with psoriasis: a meta-analysis of randomized controlled trials. Clin Rheumatol. 2019;38(4):977–88. https://doi.org/10.1007/s10067-019-04456-x.
Arriens C, Hynan LS, Lerman RH, Karp DR, Mohan C. Placebo-controlled randomized clinical trial of fish oil’s impact on fatigue, quality of life, and disease activity in systemic lupus erythematosus. Nutr J. 2015;14:82–93. https://doi.org/10.1186/s12937-015-0068-2.
Kouchaki E, Afarini M, Abolhassani J, Mirhosseini N, Bahmani F, Masoud SA, et al. High-dose omega-3 fatty acid plus vitamin D3 supplementation affects clinical symptoms and metabolic status of patients with multiple sclerosis: a randomized controlled clinical trial. J Nutr. 2018;148(8):1380–6. https://doi.org/10.1093/jn/nxy116.
Barbadoro P, Annino I, Ponzio E, Romanelli RM, D’Errico MM, Prospero E, et al. Fish oil supplementation reduces cortisol basal levels and perceived stress: a randomized, placebo-controlled trial in abstinent alcoholics. Mol Nutr Food Res. 2013;57(6):1110–4. https://doi.org/10.1002/mnfr.201200676.
Jahangiri A, Leifert WR, Kind KL, McMurchie EJ. Dietary fish oil alters cardiomyocyte Ca2 + dynamics and antioxidant status. Free Radic Biol Med. 2006;40(9):1592–602. https://doi.org/10.1016/j.freeradbiomed.2005.12.026.
Noreen EE, Sass MJ, Crowe ML, Pabon VA, Brandauer J, Averill LK. Effects of supplemental fish oil on resting metabolic rate, body composition, and salivary cortisol in healthy adults. J Int Soc Sports Nutr. 2010;7:31–8. https://doi.org/10.1186/1550-2783-7-31.
Gammone MA, Riccioni G, Dorazio GPAN. Omega-3 polyunsaturated fatty acids: benefits and endpoints in sport. Nutrients. 2019;11:46–62. https://doi.org/10.3390/nu11010046.
He Y, Gong D, Shi C, Shao F, Shi J, Fei J. Dysbiosis of oral buccal mucosa microbiota in patients with oral lichen planus. Oral Dis. 2017;23(5):674–82. https://doi.org/10.1111/odi.12657.
Ji S, Shin JE, Kim YC, Choi Y. Intracellular degradation of fusobacterium nucleatum in human gingival epithelial cells. Mol Cells. 2010;30:519–26. https://doi.org/10.1007/s10059-010-0142-8.
Carvalho M, Cavalieri D, Do Nascimento S, Lourenco TGB, Ramos DVR, Pasqualin DDC, et al. Cytokines levels and salivary microbiome play a potential role in oral lichen planus diagnosis. Sci Rep. 2019;9(1):18137–47. https://doi.org/10.1038/s41598-019-54615-y.
Kragelund C, Keller MK. The oral microbiome in oral lichen planus during a 1-year randomized clinical trial. Oral Dis. 2019;25(1):327–38. https://doi.org/10.1111/odi.12961.
dos Pereira TS, de Silva-Alves JF, Gomes CC, do Nascimento AR, Stoianoff MA, Gomez RS. Kinetics of oral colonization by Candida spp. during topical corticotherapy for oral lichen planus. J Oral Pathol Med. 2014;43:570–5. https://doi.org/10.1111/jop.12174.
Naqvi AZ, Hasturk H, Mu L, Phillips RS, Davis RB, Halem S, et al. Docosahexaenoic acid and periodontitis in adults: a randomized controlled trial. J Dent Res. 2014;93(8):767–73. https://doi.org/10.1177/0022034514541125.
Kim M, Qie Y, Kim JPACH. Gut microbial metabolites fuel host antibody responses. Cell Host Microbe. 2016;20(2):202–14. https://doi.org/10.1016/j.chom.2016.07.001.
Watson H, Mitra S, Croden FC, Taylor M, Wood HM, Perry SL, et al. A randomised trial of the effect of omega-3 polyunsaturated fatty acid supplements on the human intestinal microbiota. Gut. 2018;67(11):1974–83. https://doi.org/10.1136/gutjnl-2017-314968.
Kambayashi T, Laufer TM. Atypical MHC class II-expressing antigen-presenting cells: can anything replace a dendritic cell? Nat Rev Immunol. 2014;14(11):719–30. https://doi.org/10.1038/nri3754.
Santoro A, Majorana A, Roversi L, Gentili F, Marrelli S, Vermi W, et al. Recruitment of dendritic cells in oral lichen planus. J Pathol. 2005;205(4):426–34. https://doi.org/10.1002/path.1699.
Verma NK, Kelleher D. Not just an adhesion molecule: LFA-1 contact tunes the T lymphocyte program. J Immunol. 2017;199(4):1213–21. https://doi.org/10.4049/jimmunol.1700495.
Payeras MR, Cherubini K, Figueiredo MA, Salum FG. Oral lichen planus: focus on etiopathogenesis. Arch Oral Biol. 2013;58(9):1057–69. https://doi.org/10.1016/j.archoralbio.2013.04.004.
Hughes DA, Pinder AC, Piper Z, Johnson IT, Lund EK. Fish oil supplementation inhibits the expression of major histocompatibility complex class II molecules and adhesion molecules on human monocytes. Am J Clin Nutr. 1996;63:267–72. https://doi.org/10.1093/ajcn/63.2.267.
Hughes DA, Pinder AC. n-3 Polyunsaturated fatty acids inhibit the antigen-presenting function of human monocytes. Am J Clin Nutr. 2000;71(suppl):357S–60S. https://doi.org/10.1093/ajcn/71.1.357s.
Kong W, Yen JH, Vassiliou E, Adhikary S, Toscano MG, Ganea D. Docosahexaenoic acid prevents dendritic cell maturation and in vitro and in vivo expression of the IL-12 cytokine family. Lipids Health Dis. 2010;9:12–22. https://doi.org/10.1186/1476-511X-9-12.
Renuka A, Agnihotri N, Bhatnagar A. Differential ratios of fish/corn oil ameliorated the colon carcinoma in rat by altering intestinal intraepithelial CD8(+) T lymphocytes, dendritic cells population and modulating the intracellular cytokines. Biomed Pharmacother. 2018;98:600–8. https://doi.org/10.1016/j.biopha.2017.12.041.
Sanderson P, MacPherson GG, Jenkins CH, Calder PC. Dietary fish oil diminishes the antigen presentation activity of rat dendritic cells. J Leukoc Biol. 1997;62:771–7. https://doi.org/10.1002/jlb.62.6.771.
Teague H, Rockett BD, Harris M, Brown DA, Shaikh SR. Dendritic cell activation, phagocytosis and CD69 expression on cognate T cells are suppressed by n-3 long-chain polyunsaturated fatty acids. Immunology. 2013;139(3):386–94. https://doi.org/10.1111/imm.12088.
Sugerman PB, Savage NW, Zhou X, Walsh LJ, Bigby M. Oral lichen planus. Clin Dermatol. 2000;18:533–9. https://doi.org/10.1016/s0738-081x(00)00142-5.
Marshall A, Celentano A, Cirillo N, Mirams M, McCullough M, Porter S. Immune receptors CD40 and CD86 in oral keratinocytes and implications for oral lichen planus. J Oral Sci. 2017;59(3):373–82. https://doi.org/10.2334/josnusd.16-0334.
Hu JY, Zhang J, Ma JZ, Liang XY, Chen GY, Lu R, et al. MicroRNA-155-IFN-gamma feedback loop in CD4(+)T cells of erosive type oral lichen planus. Sci Rep. 2015;5:16935–45. https://doi.org/10.1038/srep16935.
Evans EJ, Esnouf RM, Manso-Sancho R, Gilbert RJ, James JR, Yu C, et al. Crystal structure of a soluble CD28-Fab complex. Nat Immunol. 2005;6(3):271–9. https://doi.org/10.1038/ni1170.
Sugerman PB, Satterwhite K, Bigby M. Autocytotoxic T-cell clones in lichen planus. Br J Dermatol. 2000;142:449–56. https://doi.org/10.1046/j.1365-2133.2000.03355.x.
Zhou G, Zhang J, Ren XW, Hu JY, Du GF, Xu XY. Increased B7-H1 expression on peripheral blood T cells in oral lichen planus correlated with disease severity. J Clin Immunol. 2012;32(4):794–801. https://doi.org/10.1007/s10875-012-9683-2.
Lu R, Zhang J, Sun W, Du G, Zhou G. Inflammation-related cytokines in oral lichen planus: an overview. J Oral Pathol Med. 2015;44(1):1–14. https://doi.org/10.1111/jop.12142.
McMurray DN, Jolly CA, Chapkin RS. Effects of dietary n-3 fatty acids on T cell activation and T cell receptor-mediated signaling in a murine model. J Infect Dis. 2000;182(Suppl 1):S103–7. https://doi.org/10.1086/315909.
Berra A, Tau J, Zapata G, Chiaradia P. Effects of pUFAs in a mouse model of HSV-1 chorioretinitis. Ocul Immunol Inflamm. 2017;25(6):844–54. https://doi.org/10.1080/09273948.2016.1184287.
Arrington JL, Mcmurray DN, Switzer KC, Fan Y-Y, Chapkin RS. Docosahexaenoic acid suppresses function of the CD28 costimulatory membrane receptor in primary murine and Jurkat T cells. J Nutr. 2000;2000:1147–53. https://doi.org/10.1093/jn/131.4.1147.
Chang YF, Hou YC, Pai MH, Yeh SL, Liu JJ. Effects of ω-3 polyunsaturated fatty acids on the homeostasis of CD4 + T cells and lung injury in mice with polymicrobial sepsis. JPEN J Parenter Enteral Nutr. 2017;41(5):805–14. https://doi.org/10.1177/0148607115597670.
Owen AJ, Peter-Przyborowska BA, Hoy AJ, McLennan PL. Dietary fish oil dose- and time-response effects on cardiac phospholipid fatty acid composition. Lipids. 2004;39(10):955–61. https://doi.org/10.1007/s11745-004-1317-0.
Kong WM, Yen JH, Ganea D. Docosahexaenoic acid prevents dendritic cell maturation, inhibits antigen-specific Th1/Th17 differentiation and suppresses experimental autoimmune encephalomyelitis. Brain Behav Immun. 2011;25(5):872–82. https://doi.org/10.1016/j.bbi.2010.09.012.
Jia Q, Ivanov I, Zlatev ZZ, Alaniz RC, Weeks BR, Callaway ES, et al. Dietary fish oil and curcumin combine to modulate colonic cytokinetics and gene expression in dextran sodium sulphate-treated mice. Br J Nutr. 2011;106(4):519–29. https://doi.org/10.1017/S0007114511000390.
Zhou G, Xia K, Du GF, Chen XM, Xu XY, Lu R, et al. Activation of nuclear factor-kappa B correlates with tumor necrosis factor-alpha in oral lichen planus: a clinicopathologic study in atrophic-erosive and reticular form. J Oral Pathol Med. 2009;38(7):559–64. https://doi.org/10.1111/j.1600-0714.2009.00779.x.
Santoro A, Majorana A, Bardellini E, Festa S, Sapelli P, Facchetti F. NF-kappaB expression in oral and cutaneous lichen planus. J Pathol. 2003;201(3):466–72. https://doi.org/10.1002/path.1423.
Rusanen P, Marttila E, Uittamo J, Hagstrom J, Salo T, Rautemaa-Richardson R. TLR1-10, NF-kappaB and p53 expression is increased in oral lichenoid disease. PLoS One. 2017;12(7):e0181361. https://doi.org/10.1371/journal.pone.0181361.
Mbodji K, Charpentier C, Guerin C, Querec C, Bole-Feysot C, Aziz M, et al. Adjunct therapy of n-3 fatty acids to 5-ASA ameliorates inflammatory score and decreases NF-kappaB in rats with TNBS-induced colitis. J Nutr Biochem. 2013;24(4):700–5. https://doi.org/10.1016/j.jnutbio.2012.03.022.
Jia D, Heng LJ, Yang RH, Gao GD. Fish oil improves learning impairments of diabetic rats by blocking PI3K/AKT/nuclear factor-κB-mediated inflammatory pathways. Neuroscience. 2014;258:228–37. https://doi.org/10.1016/j.neuroscience.2013.11.016.
Jangale NM, Devarshi PP, Dubal AA, Ghule AE, Koppikar SJ, Bodhankar SL, et al. Dietary flaxseed oil and fish oil modulates expression of antioxidant and inflammatory genes with alleviation of protein glycation status and inflammation in liver of streptozotocin-nicotinamide induced diabetic rats. Food Chem. 2013;141(1):187–95. https://doi.org/10.1016/j.foodchem.2013.03.001.
Enguita M, Razquin N, Pamplona R, Quiroga J, Prieto J, Fortes P. The cirrhotic liver is depleted of docosahexaenoic acid (DHA), a key modulator of NF-kappaB and TGFbeta pathways in hepatic stellate cells. Cell Death Dis. 2019;10(1):14–27. https://doi.org/10.1038/s41419-018-1243-0.
Halade GV, Rahman MM, Bhattacharya A, Barnes JL, Chandrasekar B, Fernandes G. Docosahexaenoic acid-enriched fish oil attenuates kidney disease and prolongs median and maximal life span of autoimmune lupus-prone mice. J Immunol. 2010;184(9):5280–6. https://doi.org/10.4049/jimmunol.0903282.
Zuniga J, Cancino M, Medina F, Varela P, Vargas R, Tapia G, et al. N-3 PUFA supplementation triggers PPAR-alpha activation and PPAR-alpha/NF-kappaB interaction: anti-inflammatory implications in liver ischemia-reperfusion injury. PLoS One. 2011;6(12):e28502. https://doi.org/10.1371/journal.pone.0028502.
Maruyama T, Kono K, Mizukami Y, Kawaguchi Y, Mimura K, Watanabe M, et al. Distribution of Th17 cells and FoxP3(+) regulatory T cells in tumor-infiltrating lymphocytes, tumor-draining lymph nodes and peripheral blood lymphocytes in patients with gastric cancer. Cancer Sci. 2010;101(9):1947–54. https://doi.org/10.1111/j.1349-7006.2010.01624.x.
Gallai V, Sarchielli P, Trequattrini A, Franceschini M, Floridi A, Firenze C, et al. Cytokine secretion and eicosanoid production in the peripheral blood mononuclear cells of MS patients undergoing dietary supplementation with n-3 polyunsaturated fatty acids. J Neuroimmunol. 1995;56:143–53. https://doi.org/10.1016/0165-5728(94)00140-j.
Trebble T, Arden NK, Stroud MA, Wootton SA, Burdge GC, Miles EA, et al. Inhibition of tumour necrosis factor-α and interleukin 6 production by mononuclear cells following dietary fish-oil supplementation in healthy men and response to antioxidant co-supplementation. Br J Nutr. 2003;90(2):405–12. https://doi.org/10.1079/bjn2003892.
Ramirez-Ramirez V, Macias-Islas MA, Ortiz GG, Pacheco-Moises F, Torres-Sanchez ED, Sorto-Gomez TE, et al. Efficacy of fish oil on serum of TNF alpha, IL-1 beta, and IL-6 oxidative stress markers in multiple sclerosis treated with interferon beta-1b. Oxid Med Cell Longev. 2013;2013:709493–501. https://doi.org/10.1155/2013/709493.
Zhou XJ, Sugerman PB, Savage NW, Walsh LJ. Matrix metalloproteinases and their inhibitors in oral lichen planus. J Cutan Pathol. 2001;28:72–82. https://doi.org/10.1034/j.1600-0560.2001.280203.x.
Maciejczyk M, Pietrzykowska A, Zalewska A, Knas M, Daniszewska I. The Significance of matrix metalloproteinases in oral diseases. Adv Clin Exp Med. 2016;25(2):383–90. https://doi.org/10.17219/acem/30428.
Shinto L, Marracci G, Bumgarner L, Yadav V. The effects of omega-3 Fatty acids on matrix metalloproteinase-9 production and cell migration in human immune cells: implications for multiple sclerosis. Autoimmune Dis. 2011;2011:134592–8. https://doi.org/10.4061/2011/134592.
Fogagnolo Mauricio A, Pereira JA, Santo Neto H, Marques MJ. Effects of fish oil containing eicosapentaenoic acid and docosahexaenoic acid on dystrophic mdx mice hearts at later stages of dystrophy. Nutrition. 2016;32(7–8):855–62. https://doi.org/10.1016/j.nut.2016.01.015.
Shinto L, Marracci G, Baldauf-Wagner S, Strehlow A, Yadav V, Stuber L, et al. Omega-3 fatty acid supplementation decreases matrix metalloproteinase-9 production in relapsing-remitting multiple sclerosis. Prostag Leukotr Ess. 2009;80(2–3):131–6. https://doi.org/10.1016/j.plefa.2008.12.001.
Rad M, Hashemipoor MA, Mojtahedi A, Zarei MR, Chamani G, Kakoei S, et al. Correlation between clinical and histopathologic diagnoses of oral lichen planus based on modified WHO diagnostic criteria. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2009;107(6):796–800. https://doi.org/10.1016/j.tripleo.2009.02.020.
Baek J, Lee MG. Oxidative stress and antioxidant strategies in dermatology. Redox Rep. 2016;21(4):164–9. https://doi.org/10.1179/1351000215Y.0000000015.
Lightfoot YL, Blanco LP, Kaplan MJ. Metabolic abnormalities and oxidative stress in lupus. Curr Opin Rheumatol. 2017;29(5):442–9. https://doi.org/10.1097/BOR.0000000000000413.
Hashemy SI, Gharaei S, Vasigh S, Kargozar S, Alirezaei B, Keyhani FJ, et al. Oxidative stress factors and C-reactive protein in patients with oral lichen planus before and 2 weeks after treatment. J Oral Pathol Med. 2016;45(1):35–40. https://doi.org/10.1111/jop.12326.
Battinoa M, Greabub M, Totanb A, Bullonc P, Bucurd A, Tovarue S, et al. Oxidative stress markers in oral lichen planus. BioFactors. 2008;33:301–10. https://doi.org/10.1002/biof.5520330406.
Upadhyay RB, Carnelio S, Shenoy RP, Gyawali P, Mukherjee M. Oxidative stress and antioxidant defense in oral lichen planus and oral lichenoid reaction. Scand J Clin Lab Invest. 2010;70(4):225–8. https://doi.org/10.3109/00365511003602455.
Hong MY, Hoh E, Kang B, DeHamer R, Kim JY, Lumibao J. Fish oil contaminated with persistent organic pollutants induces colonic aberrant crypt foci formation and reduces antioxidant enzyme gene expression in rats. J Nutr. 2017;147(8):1524–30. https://doi.org/10.3945/jn.117.251082.
Lopez-Jornet P, Cayuela CA, Tvarijonaviciute A, Parra-Perez F, Escribano D, Ceron J. Oral lichen planus: salival biomarkers cortisol, immunoglobulin A, adiponectin. J Oral Pathol Med. 2016;45(3):211–7. https://doi.org/10.1111/jop.12345.
Kim JE, Cho BK, Cho DH, Park HJ. Expression of hypothalamic-pituitary-adrenal axis in common skin diseases: evidence of its association with stress-related disease activity. Acta Derm Venereol. 2013;93(4):387–93. https://doi.org/10.2340/00015555-1557.
Nadendla LK. Association of salivary vortisol and anxiety levels in lichen planus patients. J Clin Diagnostic Res. 2014;8(12):ZC01–3. https://doi.org/10.7860/jcdr/2014/8058.5225.
Liu XF, Wei ZY, Bai CL, Ding XB, Li X, Su GH, et al. Insights into the function of n-3 PUFAs in fat-1 transgenic cattle. J Lipid Res. 2017;58(8):1524–35. https://doi.org/10.1194/jlr.M072983.
Xie X, Wang X, Mick GJ, Kabarowski JH, Wilson LS, Barnes S, et al. Effect of n-3 and n-6 polyunsaturated fatty acids on microsomal P450 steroidogenic enzyme activities and in vitro cortisol production in adrenal tissue from yorkshire boars. Endocrinology. 2016;157(4):1512–21. https://doi.org/10.1210/en.2015-1831.
Del Brutto OH, Mera RM, Ha JE, Gillman J, Zambrano M, Castillo PR. Dietary fish intake and sleep quality: a population-based study. Sleep Med. 2016;17:126–8. https://doi.org/10.1016/j.sleep.2015.09.021.
Bartel DP. MicroRNAs: genomics, biogenesis, mechanism, and function. Cell. 2004;116:281–97. https://doi.org/10.1016/s0092-8674(04)00045-5.
Peng Q, Zhang J, Zhou G. Differentially circulating exosomal microRNAs expression profiling in oral lichen planus. Am J Transl Res. 2018;10(9):2848–58.
Yang JG, Sun YR, Chen GY, Liang XY, Zhang J, Zhou G. Different expression of MicroRNA-146a in peripheral blood CD4(+) T cells and lesions of oral lichen planus. Inflammation. 2016;39(2):860–6. https://doi.org/10.1007/s10753-016-0316-4.
Albracht-Schulte K, Gonzalez S, Jackson A, Wilson S, Ramalingam L, Kalupahana NS, et al. Eicosapentaenoic acid improves hepatic metabolism and reduces inflammation independent of obesity in high-fat-fed mice and in HepG2 cells. Nutrients. 2019;11(3):599–616. https://doi.org/10.3390/nu11030599.
Zheng Z, Ge Y, Zhang J, Xue M, Li Q, Lin D, et al. PUFA diets alter the microRNA expression profiles in an inflammation rat model. Mol Med Rep. 2015;11(6):4149–57. https://doi.org/10.3892/mmr.2015.3318.
Tan YQ, Zhang J, Zhou G. Autophagy and its implication in human oral diseases. Autophagy. 2017;13(2):225–36. https://doi.org/10.1080/15548627.2016.1234563.
Shen L, Yang Y, Ou T, Key CCC, Tong SH, Sequeira RC, et al. Dietary PUFAs attenuate NLRP3 inflammasome activation via enhancing macrophage autophagy. J Lipid Res. 2017;58(9):1808–21. https://doi.org/10.1194/jlr.m075879.
Liu Y, Messadi DV, Wu H, Hu S. Oral lichen planus is a unique disease model for studying chronic inflammation and oral cancer. Med Hypotheses. 2010;75(6):492–4. https://doi.org/10.1016/j.mehy.2010.07.002.
Tampa M, Caruntu C, Mitran M, Mitran C, Sarbu I, Rusu LC, et al. Markers of oral lichen planus malignant transformation. Dis Markers. 2018;2018:1959506. https://doi.org/10.1155/2018/1959506.
Mignogna MD, Fedele S, Lo Russo L, Lo Muzio L, Bucci E. Immune activation and chronic inflammation as the cause of malignancy in oral lichen planus: is there any evidence? Oral Oncol. 2004;40(2):120–30. https://doi.org/10.1016/j.oraloncology.2003.08.001.
Peng Q, Zhang J, Ye X, Zhou G. Tumor-like microenvironment in oral lichen planus: evidence of malignant transformation? Expert Rev Clin Immunol. 2017;13(6):635–43. https://doi.org/10.1080/1744666X.2017.1295852.
Tabatabaei SH, Sheikhha MH, Karbasi MHA, Zarmehi S, Hoseini M. Evaluation of polymorphism of P53 protein codon 72 in oral lichen planus by PCR technique. J Dent Res Dent Clin Dent Prospects. 2018;12(4):245–51. https://doi.org/10.15171/joddd.2018.038.
Laniosz V, Torgerson RR, Ramos-Rodriguez AJ, Ma JE, Mara KC, Weaver AL, et al. Incidence of squamous cell carcinoma in oral lichen planus: a 25-year population-based study. Int J Dermatol. 2019;58(3):296–301. https://doi.org/10.1111/ijd.14215.
Borghetti G, Yamaguchi AA, Aikawa J, Yamazaki RK, de Brito GA, Fernandes LC. Fish oil administration mediates apoptosis of Walker 256 tumor cells by modulation of p53, Bcl-2, caspase-7 and caspase-3 protein expression. Lipids Health Dis. 2015;14:94–9. https://doi.org/10.1186/s12944-015-0098-y.
Manna S, Chakraborty T, Ghosh B, Chatterjee M, Panda A, Srivastava S, et al. Dietary fish oil associated with increased apoptosis and modulated expression of Bax and Bcl-2 during 7,12-dimethylbenz(alpha)anthracene-induced mammary carcinogenesis in rats. Prostag Leukotr Ess. 2008;79(1–2):5–14. https://doi.org/10.1016/j.plefa.2008.05.005.
Eltweri AM, Howells LM, Thomas AL, Dennison AR, Bowrey DJ. Effects of Omegaven(R), EPA, DHA and oxaliplatin on oesophageal adenocarcinoma cell lines growth, cytokine and cell signal biomarkers expression. Lipids Health Dis. 2018;17(1):19–28. https://doi.org/10.1186/s12944-018-0664-1.
Song M, Zhang X, Meyerhardt JA, Giovannucci EL, Ogino S, Fuchs CS, et al. Marine omega-3 polyunsaturated fatty acid intake and survival after colorectal cancer diagnosis. Gut. 2017;66(10):1790–6. https://doi.org/10.1136/gutjnl-2016-311990.
European Food Safety Authority. Scientific opinion on dietary reference values for fats, including saturated fatty acids, polyunsaturated fatty acids, monounsaturated fatty acids, trans fatty acids, and cholesterol. EFSA J. 2010;8(3):1461–568. https://doi.org/10.2903/j.efsa.2010.1461.
Papanikolaou Y, Brooks J, Reider C, Fulgoni VLUS. adults are not meeting recommended levels for fish and omega-3 fatty acid intake: results of an analysis using observational data from NHANES 2003–2008. Nutr J. 2014;13:31–7. https://doi.org/10.1186/1475-2891-13-31.
Wensing AGCL, Mensink RP, Hornstra G. Effects of dietary n-3 polyunsaturated fatty acids from plant and marine origin on platelet aggregation in healthy elderly subjects. Br J Nutr. 1999;82(3):183–91. https://doi.org/10.1017/s0007114599001361.
Acknowledgements
Our group and the laboratory members have made contributions to this review and they all deserve our acknowledgement. Duo-Na Xia came up with the idea, wrote and edited the manuscript, and designed and executed all the figures. Gang Zhou has contributed to the conception, discussion, and critical review of the manuscript. Ya-Qin Tan and Jing-Ya Yang have contributed to the discussion and especially to the thoughtful suggestion part. This work was supported by grants from National Natural Science Foundation of China (No. 81771080, No. 81970949) to Professor Zhou Gang.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
No potential conflicts of interest were disclosed.
Additional information
Responsible Editor: John Di Battista.
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Xia, DN., Tan, YQ., Yang, JY. et al. Omega-3 polyunsaturated fatty acids: a promising approach for the management of oral lichen planus. Inflamm. Res. 69, 989–999 (2020). https://doi.org/10.1007/s00011-020-01388-0
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00011-020-01388-0