Abstract
Background
Laparoscopic ventral hernia repair (LVHR) has been increasing in popularity over the years. Seroma formation is a common complication of LVHR. The aim of this study is to review the current evidence on seroma prevention strategies following LVHR.
Methods
A systematic search of PubMed, Embase (1946—13 February 2019) and Medline (1946—13 February 2019) databases was conducted using terms which include “seroma”, “hernia, ventral” and “laparoscopy”. All studies are comparative retrospective or prospective human adult studies in peer-reviewed journals describing at least one intra-operative intervention designed to decrease the rate of seroma formation in laparoscopic ventral hernia repair.
Results
The database searches identified 3762 citations, and 21 studies were included for final analysis.
Five studies compared the different methods of mesh fixation, nine studies compared primary defect closure (PFC) and bridged repair, two studies compared the effect of different types of meshes, two studies looked into the use of electrical cauterization, one study compared single- site laparoscopy with conventional laparoscopy, one study looked into the use of fibrin sealant and one study compared transabdominal preperitoneal placement of mesh with conventional repair. PFC appears to be the most promising with large studies showing a low rate of seroma formation with additional benefits of decreasing wound infection and recurrence rate. Cauterisation of hernia sac and injection of fibrin sealant also show promising results but are mainly derived from small studies. Other strategies did not demonstrate benefit.
Conclusion
Currently, primary fascial closure appears to be the most promising strategy available to decrease seroma formation after LVHR based on the results of large studies. Other promising strategies that decrease dead space such as cauterisation of the sac and fibrin sealant injection will require further multicentre trials to confirm benefit before an increase in operative time and cost can be justified for their routine use.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Laparoscopic hernia repair was first described by LeBlanc and Booth in 1993 [1] and has since been increasing in popularity due to faster recovery time, reduction in perioperative morbidity, reduced need of analgesic drugs and significant reduction in hernia recurrence rate compared to the open approach [2]. Incisional hernia is reported to occur in up to 28% of patients post-abdominal operations and primary ventral hernia can be found in about 5% of the general population [3, 4]. Due to the high volume of cases, reducing complications and recurrences of ventral hernia repair can have a major impact on health care, as studies have reported that every 1% reduction in hernia recurrence would result in a US $32 million yearly savings in procedural costs alone [3].
Mesh repairs of ventral hernias result in lower rate of recurrence but comes with wound complications such as clinically significant seroma formation requiring intervention in 3–17% of laparoscopic ventral hernia repair cases [4,5,6]. Seroma is defined as a collection of fluid detected in the subcutaneous space through clinical or radiographical investigation and is most common following surgery that involves extensive tissue dissection resulting in a “dead space” [7]. While clinically significant seroma is reported in up to 17% of hernia repairs, studies have reported that the rate of seroma detection approaches 100% when diagnosed based on radiological criteria alone [8]. This is clinically relevant as all seroma can lead to postoperative wound infection and potentially increase recurrence rate.
Seroma formation results in patient dissatisfaction, poor aesthetic outcome and serious surgical site infections [9]. Therefore, many surgeons are exploring perioperative strategies that aid to minimize the rate of seroma occurrence. These interventions include suture or tack for mesh fixation and use of electrical cauterization [10,11,12,13,14]. Massey has performed a systematic review to evaluate adjuncts to reduce seroma formation in open incisional hernia repairs but there are no studies to our knowledge that compares strategies employed in laparoscopic ventral hernia repairs [15]. There is no conclusive evidence to date that describes which adjunct employed during hernia repair is the most effective to prevent seroma formation.
The primary aim of this systematic review aims to evaluate intra-operative strategies that can reduce seroma formation in laparoscopic ventral hernia repairs.
Methods
An electronic search of PubMed, Embase (1974—13 February 2019) and Medline (1946—13 February 2019) was performed independently by HC and LJD. The search terms used were medical subject headings (MeSH); “seroma”, “exudates and transudates”, “hernia, abdominal”, “hernia, ventral”, “laparoscopy”, “Laparoscopic Surgery”, “laparoscopic ventral hernia repair”, “herniorrhaphy”, “hernioplasty” and “hernia/surgery”.
All citations identified by our search strategy were reviewed independently by HC and LJD. Bibliographic references were searched to identify relevant studies that were not found by electronic search. The sequential review of title, abstract and then full text were performed independently by both authors on Covidence. Discrepancies were addressed with discussion until consensus was achieved. The authors were not blinded to the source of the document or authorship for the purpose of data extraction. The analysis was prepared in accordance with the preferred reporting of systematic reviews and meta-analyses (PRISMA) statement [16].
Inclusion and exclusion criteria
The abstracts of the identified articles were reviewed independently by HC and LJD for prospective eligibility. Full-text articles were retrieved and checked against the inclusion and exclusion criteria in Table 1. The appropriateness of the full-text articles was determined by the reviewers independently and by discussion in case of inconsistency.
Outcome measure
The primary outcome measure was seroma formation. Secondary outcome measure was recurrence of the hernia.
Definitions
Seroma
Fluid deposition in the subcutaneous space detected by clinical or radiographical assessment. There is no standard definition of clinical assessment so the need for intervention to treat seroma is the most commonly used method.
Recurrence
Clinical or radiological evidence of a recurrent hernia detected during the follow-up period.
Method of mesh fixation
A variety of strategies have been demonstrated to fix the mesh to close the hernia defect. The methods include use of glue, tacks and sutures.
Primary defect closure and bridged repair
Primary defect closure describes the approximation of the fascial defect before the placement of the mesh. Bridged repair is when a piece of mesh is placed intraperitoneally in an underlay position to achieve circumferential overlap of the fascial defect [17].
Primary defect closure is performed with the primary approximation of the fascial edges of the hernia defect with sutures before placing the mesh. Three trocars are used for the procedure, one as a central optical trocar and two for lysis of adhesions, defect closure and mesh positioning. This is followed by the lysis of the adhesions to the abdominal wall surrounding the hernia. The defect is then either closed with a needle and laparoscopic needle driver, an Endo Stitch (Covidien) suturing device or closed percutaneously using a suture passer. After the defect closure, an appropriately sized intraperitoneal mesh is placed to overlap the margins of the defect by 5–7 cm [18, 19].
Types of mesh
Different types of mesh for fixation are available for laparoscopic repair of ventral hernias. The characteristic of an ideal mesh should prevent adhesions and promote fibrous ingrowth [20]. The commonly used types of mesh include composite mesh with monofilament polyester textile on one side and a hydrophilic absorbable collagen film on one side (Parietex) and non-coated synthetic polyvinylidene fluoride and polypropylene mesh (DynaMesh-IPOM) [[17]]. Other choices of mesh include a nitinol frame on the mesh to keep the mesh well positioned against the abdominal wall and reduce the incidence of mesh shrinkage [21].
Electrical cauterization
Cauterization of the hernia sac destroys the serosal surface of the hernial subcutaneous cavity and creates adhesions immediately in the burned sac close to the dead space [22].
Single-incision laparoscopy
Single-port laparoscopy has been introduced to minimize abdominal wall trauma by performing the hernia repair through a minimal single fascia incision [23].
Fibrin sealant
This describes the percutaneous application of a heterologous fibrin sealant with the intention of collapsing the dead space where the seroma settles [24].
Preperitoneal placement of mesh
The placement of mesh in the preperitoneal/retromuscular space instead of the standard intraperitoneal location to avoid direct contact of mesh with abdominal contents [25].
Data extraction and quality assessment
The rate of seroma formation in percentage and p value and the recurrence rate were extracted. The number of patients for intervention and control, study design, difference in baseline characteristic and length of follow-up were also recorded for each study. A p value ≤ 0.05 is considered statistically significant.
Observational studies were assessed using the Methodological Index for Non-Randomised Studies (MINORS) criteria to evaluate the methodologic quality and potential of bias of the articles selected for this review and the single randomized trial was assessed using the Cochrane collaboration’s risk of bias tool at study level.
Results
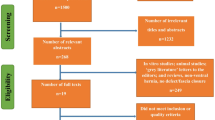
The database searches identified 3762 citations. After removing duplicates and screening titles, 1545 were included for review and after application of inclusion/exclusion criteria, 97 full texts were assessed and 21 were included for final analysis. The PRISMA statement of search results is shown (Fig. 1).
13 were retrospective cohort studies: two on method of mesh fixation with a total of 560 patients, eight on primary fascial closure and bridged repair with a total of 2707 patients, two on electrical cauterization with a total of 174 patients and one on types of mesh with a total of 82 patients.
Five were prospective comparative studies: one on method of mesh fixation with a total of 60 patients, one on fibrin sealant with a total of 50 patients, one on single-site laparoscopy with a total of 34 patients, one on unidirectional barbed sutures with a total of 57 patients and one on preperitoneal placement of mesh with a total of 279 patients.
Three were randomized controlled trials, two of which compared the method of mesh fixation with a total of 182 patients and one compared the type of mesh with different methods of mesh fixation with a total of 92 patients.
A summary of the patient demographics and study design differences is shown in Tables 2, 3, 4, 5, 6, 7 and 8. The studies varied in the assessment method of seroma and follow-up period. All the studies included recurrence data.
Method of mesh fixation
Five studies reported seroma outcomes using purely different methods of mesh fixation with a total of 802 patients. Two studies compared tacker fixation with suture fixation with a total of 166 patients. Kitamura et al. showed seroma formation as 6% in the tack group and 14% in the suture group while Bansal et al. showed seroma formation as 12.8% in the tack group and 20% in the suture group [12, 26].
One study compared glue fixation with tacker fixation with a total of 60 patients. Ambore et al. [27] found a 0% rate of seroma formation in the group with glue fixation of the mesh and 13.3% rate of seroma formation in the group with tacker fixation of the mesh.
Muysoms et al. [28] conducted the study among 76 patients and reported a 3.0% rate of seroma formation in the group with mesh fixation using double row of spiral tackers and a 0% rate of seroma formation in the group with mesh fixation using transfascial sutures combined with one row of spiral tackers.
Lastly, Caruso et al. [11] conducted the study among 500 patients and reported the seroma formation rate in the group with mesh fixation using EMS stapler as 3.4% and the group with mesh fixation using tacks as 4.6%.
Primary defect closure and bridged repair
Nine retrospective studies compared seroma outcomes in patients who underwent primary fascial closure and patients who underwent bridged repair with a total of 6526 patients. Martin-del-Campo et al. [18] reported 0.4% rate of seroma formation in the group who underwent defect closure compared to 11.5% rate of seroma formation in the group with underwent bridged repair. Papageorge et al. [17] reported 10% rate of seroma formation in the group with primary fascial closure and 11% in the group with bridged repair. Karipineni et al. [29] reported 2.5% in the group with defect closure and 0% in the group without defect closure. Light et al. [30] reported 5.4% seroma formation in the group with fascial closure and 13.2% in the group without fascial closure. Wennergren et al. [31] reported 8.3% in the group with primary fascial closure and 14.1% in the group with bridged repair. Nguygen et al. [32] reported 0% in the group with primary closure and 6.9% in the group without defect repair. Clapp et al. [6] reported 5.6% rate of seroma formation in the group with transcutaneous closure of defects compared to 27.8% in the group that underwent standard repair. Zeichen et al. [19] reported 11.4% in the group which underwent closure of hernia defect and 4.3% in the group without closure of hernia defect. Sharma et al. [33] reported 0% rate of seroma formation in the group with defect closure and 13.7% in the group which did not undergo defect closure.
Electrical cauterization
Two retrospective studies reported seroma formation after electrical cauterization of the hernia sac was applied with a total of 174 patients. Prassas et al. [13] reported 0% rate of seroma after electrical cauterization and 25% rate of seroma formation in the controlled group. Tysimoyiannis et al. [14] reported 1.9% rate of seroma after electrical cauterization and 25% rate in the control. Both studies were statistically significant in the intervention impact on seroma outcome with the reported p value ≤ 0.05.
Types of mesh
Two studies compared the rate of seroma formation using different types of mesh with a total of 174 patients. Grubnik et al. [21] reported in their randomized controlled trial a 16.3% rate of seroma formation in tacker fixation of expanded polytetrafluoroethylene mesh (ePTFE) and 2.0% rate of seroma formation in suture fixation of ePTFE mesh with a nitinol frame that keeps the mesh flat and firmly positioned against the abdominal wall while reducing the incidence of mesh shrinkage. Tandon et al. [34] reported in their study that the rate of seroma formation in the group which used Parietex composite mesh was 6.4% while the group which used Dynamesh which had a rate of 0% of formation of seroma.
Single-site laparoscopy
There is one prospective comparative study comparing seroma formation in single-site laparoscopy and standard laparoscopy with a total of 34 patients. The rates of seroma formation are 13.3% in the single-site laparoscopy group and 10.5% in the standard laparoscopy group [35].
Fibrin sealant
There is one prospective comparative study on the use of fibrin sealant in preventing seroma formation with a total of 50 patients. Tissucol Duo was injected percutaneously in the space between the prosthesis and the hernia sac once the pneumoperitoneum was evacuated. The amount of fibrin sealant applied was 1 ml for every 16 cm2 of prosthesis. The rates of seroma were high in both the fibrin sealant and control groups in this study at three different time points on CT scan, varying from 64% at 7 days to 12% at 3 months in the fibrin sealant group and 92% at 7 days to 24% at 3 months in the non-fibrin sealant group [24].
Preperitoneal placement of mesh
There is one comparative study comparing the rates of seroma formation when the mesh is placed in preperitoneal position instead of intraperitoneally with a total of 279 patients included in the study. Prasad et al. [25] reports the rate of seroma formation at 5.8% in the transabdominal preperitoneal group compared to 8.5% in the intraperitoneal group.
Study quality
The 13 retrospective studies and 5 prospective comparative studies were assessed according to the MINORS criteria [36]. Most of the studies score high on the MINORS criteria (median 19, range 8 to 24).
The three randomized controlled trial were assessed according to the Cochrane risk of bias tool. In both Grubnik and Bansal’s studies [21, 26], the source of bias may arise from the lack of information on whether the participants were blinded of their intervention and whether the assessors were blinded of the intervention during the measurement of outcome. In Muysoms et al.’s study [28], the source of bias arises from the lack of blinding to both the patient and assessor about the treatment arm.
There was frequent variation in the patient’s baseline characteristics between the intervention and control group.
Discussion
Laparoscopic ventral hernia repair is being performed more commonly with about 20–27% of ventral hernia repairs performed laparoscopically [37]. Massey et al. first performed a review on the adjuncts to reduce seroma in open incisional hernia repair and we believe that as LVHR becomes increasingly popular, it would be imperative to study the factors contributing to seroma formation in laparoscopic repair as well. Our systematic review with a total of 21 studies identified is the first in the literature as far as we are aware that examines the interventions contributing to seroma prevention after LVHR.
Seroma formation is a common complication after LVHR with incidence ranging from 3 to 100% depending on whether clinical or radiological criteria are used to define seroma. This is important as seromas can be detected through radiological imaging in almost all patients after a LVHR and is generally regarded as an expected outcome [38]. Morales-Conde 2012 [39] proposes the adoption of a seroma classification to categorize seromas into clinically insignificant, asymptomatic collections to those with complications such as infection so as to allow data to be interpreted and compared more meaningfully across studies.
In our review, we identified the recurring themes and strategies in seroma prevention and propose a logical recommendation based on the current available literature and limitations on this topic below.
Primary fascial closure of defect
The necessity of primary fascial closure (PFC) of the hernia defect in laparoscopic ventral hernia repair (LVHR) continues to be controversial. A large series single-institution trial by Chelala et al. in 2015 demonstrated a significantly low seroma formation rate at 2.56% based on CT scan within 3 months along with many purported benefits associated with the use of PFC including low rate of recurrences and reduction in overall morbidity [40]. This is further supported by a recent meta-analysis in 2016 by Tandon et al. which found PFC in LVHR to be associated with fewer recurrences, mesh eventration and/or bulging as well as a lower incidence of seroma formation [41]. However, our study has found five new studies in addition to the meta-analysis by Tandon. Four of the studies did not associate PFC with lower incidences of seroma formation while one study found statistically lower seroma formation rate [17, 18, 29, 30, 32]. This highlights that emerging new studies with conflicting results continue to add on to the existing debate regarding this intervention.
Nevertheless, most large analysis supports the use of PFC in reducing seroma formation. The purported benefits of this intervention could lie in the reduction of effective dead space between the mesh and overlying tissue [17]. Proponents of PFC also cite its importance through the restoration of abdominal wall function which is achieved by the realignment of the abdominal muscle and fascial layers which restores normal anatomy. There is also decreased incidence of infection after seroma formation as the mesh is physically separated from the skin by the abdominal wall muscle and fascia [19]. However, the downside of performing routine PFC will be that it is time consuming, has a learning curve and fascia may be under tension for larger defects.
Our recommendation would be similar to the 2010 Ventral Hernia Working Group that recommends PFC in both open and laparoscopic ventral hernia repair [4]. This given the context of several large studies having demonstrated a low seroma formation after PFC as well as other benefits of decreased surgical site infection and hernia recurrence would make PFC ideal in centres with available technical expertise.
Cauterization of hernia sac
Our systematic review found that in the small number of studies published thus far, the intra-operative manoeuvre of cauterizing the hernia sac appears to be associated with lower rates of seroma formation. The Society of American Gastrointestinal and Endoscopic Surgeons (SAGES) currently provides a weak recommendation for the routine cauterization of the hernia sac in reducing seroma formation, largely based on Tsimonyiannis’s 2001 prospective study on 51 patients [22]. We have only found two new retrospective studies to further support SAGES’s weak recommendation. The pathophysiological basis of such a manoeuvre is well described by Prassas et al. who postulate that the inflammatory response is mitigated by destroying the mesothelial cells (which produce cytokines and chemokines to form an inflammatory exudate) and eliminates dead space by forming adhesion between the mesh and cauterized surface [13]. The obliteration of dead space to reduce seroma formation is an important theme for several other different intra-operative manoeuvres such as PFC in LVHR as well as quilting sutures in abdominoplasties and mastectomy [42].
Currently, the evidence for routine sac cauterisation is weak and based on small studies. We recommend interpretation of the results with caution. Nevertheless, cauterization of the hernia sac is a relatively intuitive and safe intra-operative manoeuvre with no added cost that may prove promising if future multicentre studies can confirm its benefit.
Mesh types
There remains a lot of controversy on the indications of using a synthetic versus biologic mesh. The sheer volume of different types of meshes available on the market can be overwhelming, with subtypes within each different mesh groups. The categories of mesh types can be largely classified into synthetic and biologic mesh. There remains little high-quality evidence to suggest the choice of mesh in LVHR and this largely depends on its institutional availability, costs as well as the surgeon’s preference. Older studies conducted that used ePTFE (expanded tetrafluoroethylene)-based meshes for hernia repair have found high rates of seroma, postulated to be due to the low porosity of the material that prevented adequate drainage of fluid [43, 44]. Our systematic review found two studies comparing different mesh types and their risk of developing seromas, but in these studies’ seroma formation was measured as secondary outcomes. There also exists much variability in surgical techniques, mesh positions as well as surgeon’s experience which can all influence the patient’s seroma formation incidence independent of the mesh alone. This makes it extremely difficult to directly compare these studies and conclude that a certain mesh type is superior due to the numerous confounders.
As such we are unable to recommend any particular type of mesh to be used in LVHR that may particularly decrease seroma formation, but it is probably worthy to note that PTFE meshes may potentially increase rates of seroma due to its inherent mesh property.
Mesh fixation methods
Fixation of meshes to the abdominal wall is an important step in LVHR. However, there exists controversy over the type of fixation method. Mesh fixation methods can be widely categorized into tacks and sutures, both in absorbable and nonabsorbable (permanent) forms. Meshes can be secured purely with tacks, sutures or a combination of both. Mesh fixation to the abdominal wall must be able to withstand shear forces created by the abdominal musculature such that it will not break loose and cause mesh migration within the abdomen. There have been various studies including a meta-analysis evaluating for the optimal fixation technique. However, no single-mesh fixation method has proven to be the superior option. In a systematic review and meta-analysis by Baker et al., the authors report that suture fixation was associated with a lower hernia recurrence rate compared to permanent tacks after directly comparing three randomized controlled trials [45]. There still exists conflicting evidence in hernia recurrence as well as postoperative pain in individuals receiving suture versus tack fixation [10, 26, 46, 47].
There are many series published using these fixation methods but there appears to be a lack of review studies specifically looking at seroma incidence [45, 48]. Our systematic review found a total of five studies, two of which are randomized control trials and they generally do not find any fixation method to be more superior to the other in terms of seroma incidence. Muysoms 2013 et al. compared mesh fixation with double rows of permanent tacks versus transfascial sutures with a single row of tacks and reported that transfascial sutures caused more postoperative pain at 3 months [28]. Furthermore, although absorbable tacks do not have any significantly greater adverse outcomes, they are also associated with increased healthcare cost and no apparent benefit in primary outcomes such as postoperative pain and patient satisfaction [49].
It is important to note that the primary outcome of these studies looked into hernia recurrence rate, postoperative quality of life and the incidence of abdominal wall pain with seroma formation being a secondary outcome [12, 26, 28]. As such, we do not recommend any particular type of mesh fixation and suggests interpreting the data with caution as none of these studies is powered to detect primary difference in seroma formation and any positive findings may likely be an incidental secondary finding rather than a true effect from the type of fixation.
Mesh placement location
There is a growing interest in alternative mesh placement locations in LVHR. The intraperitoneal onlay mesh (IPOM) technique is widely used in clinical practice and is the equivalent of the underlay method in open ventral hernia repair. In a meta-analysis by Holihan 2017 et al., the authors reported that LVHR with the underlay mesh placement, i.e. IPOM, was associated with the lowest incidence of surgical site infections [50]. Although it has been associated with postoperative complications due to the intraperitoneal placement of the mesh, they appear to be uncommon [25].
Our systematic review found one comparative study on transabdominal preperitoneal (TAPP) versus IPOM. The transabdominal preperitoneal (TAPP) technique in LVHR is more commonly employed in the surgical correction of inguinal hernias. In the study, the TAPP approach was associated with longer operative time (96.7 versus 87.4 min) and decreased costs [25]. There were no statistically significant differences in other outcomes, namely seroma formation.
We do not recommend using the TAPP technique in LVHR to decrease seroma formation as this technique increases the operative time without clear advantage.
Single-site laparoscopy
Our study identified one prospective comparative study on the use of single-incision versus conventional laparoscopy. There is inconclusive evidence to recommend such a surgical procedure due to the paucity of such studies and the intrinsic challenges in performing single-site laparoscopy compared to standard laparoscopy, as acknowledged by the authors in this study.
Fibrin sealant
Our study identified one prospective comparative study on the use of injection of fibrin sealant into the hernia sac to reduce seroma incidence via the reduction of dead space. Although there is a statistically significant reduction of seroma with the use of fibrin sealant, this remains an isolated study and use of fibrin sealant is also associated with increased cost. Until future studies confirm its benefit, we are currently unable to recommend its usage based on a single study.
Hernia sac excision
Although there we are unable to identify any specific study looking at the effect of hernia sac excision, we are aware that some surgeons routinely excise the sac in an attempt to decrease seroma formation. This may be the subject of future research.
Limitations
We recognize the lack of a standardized definition and follow-up protocol for seroma detection and the high risk of bias in most of these studies as a limitation of our review. Meta-analysis of available studies is difficult due to heterogeneity in areas of operative protocol, mesh types, mesh location as well as fixation methods. This makes valid comparisons extremely challenging.
Nevertheless, we hope to present a comprehensive summary of the vast body of literature on this topic and stimulate future research that clarifies some of the current controversies and validate promising strategies that are currently being utilized to decrease seroma formation after LVHR.
Conclusion
Currently, primary fascial closure appears to be the most promising strategy available to decrease seroma formation after LVHR based on the results of large studies. Other promising strategies that decrease dead space such as cauterisation of the sac and fibrin sealant will require further multicentre trials to confirm its benefit before an increase in operative time and cost can be justified for their routine use.
References
LeBlanc KA, Booth WV (1993) Laparoscopic repair of incisional abdominal hernias using expanded polytetrafluoroethylene: preliminary findings. Surg Laparosc Endosc 3(1):39–41
Sauerland S, Walgenbach M, Habermalz B, Seiler CM, Miserez M (2011) Laparoscopic versus open surgical techniques for ventral or incisional hernia repair. Cochrane Database of Syst Rev. https://doi.org/10.1002/14651858.CD007781.pub2
Poulose BK, Shelton J, Phillips S, Moore D, Nealon W, Penson D, Beck W, Holzman MD (2012) Epidemiology and cost of ventral hernia repair: making the case for hernia research. Hernia J Hernias Abdom Wall Surg 16(2):179–183. https://doi.org/10.1007/s10029-011-0879-9
Breuing K, Butler CE, Ferzoco S, Franz M, Hultman CS, Kilbridge JF, Rosen M, Silverman RP, Vargo D (2010) Incisional ventral hernias: review of the literature and recommendations regarding the grading and technique of repair. Surgery 148(3):544–558. https://doi.org/10.1016/j.surg.2010.01.008
Lund S, Farley D (2018) A decade of experience with laparoscopic ventral hernia repairs. Am J Surg. https://doi.org/10.1016/j.amjsurg.2018.10.008
Clapp ML, Hicks SC, Awad SS, Liang MK (2013) Trans-cutaneous Closure of Central Defects (TCCD) in laparoscopic ventral hernia repairs (LVHR). World J Surg 37(1):42–51. https://doi.org/10.1007/s00268-012-1810-y
Clemens MW, Butler CE (2019) Ventral abdominal hernia repair: technique—external oblique release. In: The SAGES manual of hernia surgery. Springer, Berlin, pp 217–236
Bedi AP, Bhatti T, Amin A, Zuberi J (2007) Laparoscopic incisional and ventral hernia repair. J Minim Access Surg 3(3):83–90. https://doi.org/10.4103/0972-9941.37190
Kaafarani HM, Hur K, Hirter A, Kim LT, Thomas A, Berger DH, Reda D, Itani KM (2009) Seroma in ventral incisional herniorrhaphy: incidence, predictors and outcome. Am J Surg 198(5):639–644. https://doi.org/10.1016/j.amjsurg.2009.07.019
Bansal VK, Misra MC, Kumar S, Keerthi Rao Y, Singhal P, Goswami A, Guleria S, Arora MK, Chhabra A (2011) A prospective randomized study comparing suture mesh fixation versus tacker mesh fixation for laparoscopic repair of incisional and ventral hernias. Surg Endosc Other Interv Tech 25(5):1431–1438
Caruso F, Ciccarese F, Cesana G, Uccelli M, Castello G, Olmi S (2017) Massive incisional hernia repair with parietex: monocentric analysis on 500 cases treated with a laparoscopic approach. J Laparoendosc Adv Surg Techn Part A 27(4):388–392. https://doi.org/10.1089/lap.2016.0623
Kitamura RK, Choi J, Lynn E, Divino CM (2013) Suture versus tack fixation of mesh in laparoscopic umbilical hernia repair. JSLS J Soc Laparoendosc Surgeons 17(4):560–564. https://doi.org/10.4293/108680813X13693422520044
Prassas D, Schumacher FJ (2018) Electric cauterization of the hernia sac in laparoscopic ventral hernia repair reduces the incidence of postoperative seroma: a propensity score-matched analysis. Hernia J Hernias Abdom Wall Surg 22(5):747–750. https://doi.org/10.1007/s10029-018-1790-4
Tsimoyiannis EC, Tsimogiannis KE, Pappas-Gogos G, Nikas K, Karfis E, Sioziou H (2008) Seroma and recurrence in laparoscopic ventral hernioplasty. JSLS J Soc Laparoendosc Surgeons 12(1):51–57
Massey LH, Pathak S, Bhargava A, Smart NJ, Daniels IR (2018) The use of adjuncts to reduce seroma in open incisional hernia repair: a systematic review. Hernia J Hernias Abdom Wall Surg 22(2):273–283. https://doi.org/10.1007/s10029-017-1690-z
Moher D, Liberati A, Tetzlaff J, Altman DG (2009) Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. PLoS Med 6(7):e1000097. https://doi.org/10.1371/journal.pmed.1000097
Papageorge CM, Funk LM, Poulose BK, Phillips S, Rosen MJ, Greenberg JA (2017) Primary fascial closure during laparoscopic ventral hernia repair does not reduce 30-day wound complications. Surg Endosc 31(11):4551–4557. https://doi.org/10.1007/s00464-017-5515-z
Martin-Del-Campo LA, Miller HJ, Elliott HL, Novitsky YW (2018) Laparoscopic ventral hernia repair with and without defect closure: comparative analysis of a single-institution experience with 783 patients. Hernia J Hernias Abdom Wall Surg 22(6):1061–1065. https://doi.org/10.1007/s10029-018-1812-2
Zeichen MS, Lujan HJ, Mata WN, Maciel VH, Lee D, Jorge I, Plasencia G, Gomez E, Hernandez AM (2013) Closure versus non-closure of hernia defect during laparoscopic ventral hernia repair with mesh. Hernia J Hernias Abdom Wall Surg 17(5):589–596
Elango S, Perumalsamy S, Ramachandran K, Vadodaria K (2017) Mesh materials and hernia repair. BioMedicine 7(3):16–16. https://doi.org/10.1051/bmdcn/2017070316
Grubnik VV, Grubnik AV, Vorotyntseva KO (2014) Laparoscopic repair of incisional and ventral hernias with the new type of meshes: randomized control trial. Wideochirurgia I Inne Techniki Maloinwazyjne 9(2):145–151
Tsimoyiannis EC, Siakas P, Glantzounis G, Koulas S, Mavridou P, Gossios KI (2001) Seroma in laparoscopic ventral hernioplasty. Surg Laparosc Endosc Percutan Tech 11(5):317–321
Bower CE, Love KM (2011) Single incision laparoscopic ventral hernia repair. JSLS J Soc Laparoendosc Surgeons 15(2):165–168. https://doi.org/10.4293/108680811x13071180406475
Morales-Conde S, Suarez-Artacho G, Socas M, Barranco A (2013) Influence of fibrin sealant in preventing postoperative seroma and normalizing the abdominal wall after laparoscopic repair of ventral hernia. Surg Endosc 27(9):3214–3219. https://doi.org/10.1007/s00464-013-2894-7
Prasad P, Tantia O, Patle NM, Khanna S, Sen B (2011) Laparoscopic ventral hernia repair: a comparative study of transabdominal preperitoneal versus intraperitoneal onlay mesh repair. J Laparoendosc Adv Surg Tech Part A 21(6):477–483. https://doi.org/10.1089/lap.2010.0572
Bansal VK, Misra MC, Babu D, Singhal P, Rao K, Sagar R, Kumar S, Rajeshwari S, Rewari V (2012) Comparison of long-term outcome and quality of life after laparoscopic repair of incisional and ventral hernias with suture fixation with and without tacks: a prospective, randomized, controlled study. Surg Endosc 26(12):3476–3485. https://doi.org/10.1007/s00464-012-2390-5
Ambore VK, More JP, Bhandarwar AH, Gandhi SS, Patel CB, Taori R (2017) Comparative study of tacker vs glue fixation of mesh in laparoscopic intraperitoneal onlay mesh repair of ventral hernias. World J Laparosc Surg 10(3):87–90
Muysoms F, Vander Mijnsbrugge G, Pletinckx P, Boldo E, Jacobs I, Michiels M, Ceulemans R (2013) Randomized clinical trial of mesh fixation with "double crown" versus "sutures and tackers" in laparoscopic ventral hernia repair. Hernia J Hernias Abdom Wall Surg 17(5):603–612
Karipineni F, Joshi P, Parsikia A, Dhir T, Joshi ART (2016) Laparoscopic-assisted ventral hernia repair: primary fascial repair with polyester mesh versus polyester mesh alone. Am Surg 82(3):236–242
Light D, Bawa S (2016) Trans-fascial closure in laparoscopic ventral hernia repair. Surg Endosc 30(12):5228–5231. https://doi.org/10.1007/s00464-016-4868-z
Wennergren JE, Askenasy EP, Greenberg JA, Holihan J, Keith J, Liang MK, Martindale RG, Trott S, Plymale M, Roth JS (2016) Laparoscopic ventral hernia repair with primary fascial closure versus bridged repair: a risk-adjusted comparative study. Surg Endosc 30(8):3231–3238. https://doi.org/10.1007/s00464-015-4644-5
Nguyen D, Szomstein S, Ordonez A, Dip F, Rajan M, Menzo EL, Rosenthal RJ (2016) Unidirectional barbed sutures as a novel technique for laparoscopic ventral hernia repair. Surg Endosc 30(2):764–769
Sharma D, Jindal V, Pathania OP, Thomas S (2010) Novel technique for closure of defect in laparoscopic ventral hernia repair. J Minim Access Surg 6(3):86–88. https://doi.org/10.4103/0972-9941.68580
Tandon A, Shahzad K, Pathak S, Oommen CM, Nunes QM, Smart N (2016) Parietex™ Composite mesh versus DynaMesh®-IPOM for laparoscopic incisional and ventral hernia repair: a retrospective cohort study. Ann R Coll Surgeons Engl 98(8):568–573. https://doi.org/10.1308/rcsann.2016.0292
Gronvold LB, Spasojevic M, Nesgaard JM, Ignjatovic D (2012) Single-incision laparoscopic versus conventional laparoscopic ventral hernia repair: a comparison of short-term surgical results. Surg Laparosc Endosc Percutan Tech 22(4):354–357. https://doi.org/10.1097/SLE.0b013e318257cefc
Slim K, Nini E, Forestier D, Kwiatkowski F, Panis Y, Chipponi J (2003) Methodological index for non-randomized studies (minors): development and validation of a new instrument. ANZ J Surg 73(9):712–716
Vorst AL, Kaoutzanis C, Carbonell AM, Franz MG (2015) Evolution and advances in laparoscopic ventral and incisional hernia repair. World J Gastrointest Surg 7(11):293–305. https://doi.org/10.4240/wjgs.v7.i11.293
Earle D, Roth JS, Saber A, Haggerty S, Bradley JF, Fanelli R, Price R, Richardson WS, Stefanidis D (2016) SAGES guidelines for laparoscopic ventral hernia repair. Surg Endosc 30(8):3163–3183
Morales-Conde S (2012) A new classification for seroma after laparoscopic ventral hernia repair. Hernia J Hernias Abdom Wall Surg 16(3):261–267. https://doi.org/10.1007/s10029-012-0911-8
Chelala E, Baraké H, Estievenart J, Dessily M, Charara F, Allé JL (2015) Long-term outcomes of 1326 laparoscopic incisional and ventral hernia repair with the routine suturing concept: a single institution experience. Hernia J Hernias Abdom Wall Surg 20(1):101–110. https://doi.org/10.1007/s10029-015-1397-y
Tandon A, Pathak S, Lyons NJ, Nunes QM, Daniels IR, Smart NJ (2016) Meta-analysis of closure of the fascial defect during laparoscopic incisional and ventral hernia repair. Br J Surg 103(12):1598–1607. https://doi.org/10.1002/bjs.10268
Ouldamer L, Bonastre J, Brunet-Houdard S, Body G, Giraudeau B, Caille A (2016) Dead space closure with quilting suture versus conventional closure with drainage for the prevention of seroma after mastectomy for breast cancer (QUISERMAS): protocol for a multicentre randomised controlled trial. BMJ Open 6(4):e009903. https://doi.org/10.1136/bmjopen-2015-009903
Utrera Gonzalez A, de la Portilla de Juan F, Carranza Albarran G (1999) Large incisional hernia repair using intraperitoneal placement of expanded polytetrafluoroethylene. Am J Surg 177(4):291–293. https://doi.org/10.1016/s0002-9610(99)00041-0
Susmallian S, Gewurtz G, Ezri T, Charuzi I (2001) Seroma after laparoscopic repair of hernia with PTFE patch: is it really a complication? Hernia J Hernias Abdom Wall Surg 5(3):139–141
Baker JJ, Oberg S, Andresen K, Klausen TW, Rosenberg J (2018) Systematic review and network meta-analysis of methods of mesh fixation during laparoscopic ventral hernia repair. Br J Surg 105(1):37–47. https://doi.org/10.1002/bjs.10720
Wassenaar E, Schoenmaeckers E, Raymakers J, van der Palen J, Rakic S (2010) Mesh-fixation method and pain and quality of life after laparoscopic ventral or incisional hernia repair: a randomized trial of three fixation techniques. Surg Endosc 24(6):1296–1302. https://doi.org/10.1007/s00464-009-0763-1
Beldi G, Wagner M, Bruegger LE, Kurmann A, Candinas D (2011) Mesh shrinkage and pain in laparoscopic ventral hernia repair: a randomized clinical trial comparing suture versus tack mesh fixation. Surg Endosc 25(3):749–755. https://doi.org/10.1007/s00464-010-1246-0
Reynvoet E, Deschepper E, Rogiers X, Troisi R, Berrevoet F (2014) Laparoscopic ventral hernia repair: is there an optimal mesh fixation technique? A systematic review. Langenbecks Arch Surg 399(1):55–63. https://doi.org/10.1007/s00423-013-1126-x
Bansal VK, Asuri K, Panaiyadiyan S, Kumar S, Subramaniam R, Ramachandran R, Sagar R, Misra MC (2016) Comparison of absorbable versus nonabsorbable tackers in terms of long-term outcomes, chronic pain, and quality of life after laparoscopic incisional hernia repair: a randomized study. Surg Laparosc Endosc Percutaneous Tech 26(6):476–483
Holihan JL, Hannon C, Goodenough C, Flores-Gonzalez JR, Itani KM, Olavarria O, Mo J, Ko TC, Kao LS, Liang MK (2017) Ventral hernia repair: a meta-analysis of randomized controlled trials. Surg Infect 18(6):647–658. https://doi.org/10.1089/sur.2017.029
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
All authors declare no conflict of interest.
Ethical approval
This study design conformed to ethical standards.
Human and animal rights
This article does not contain any studies with human participants or animals performed by any of the authors.
Informed consent
There were no individual participants included in this study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
He, C., Lu, J., Ong, M.W. et al. Seroma prevention strategies in laparoscopic ventral hernia repair: a systematic review. Hernia 24, 717–731 (2020). https://doi.org/10.1007/s10029-019-02098-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10029-019-02098-1