Abstract
Purpose
Despite advancements in laparoscopic ventral hernia repair (LVHR) using the intraperitoneal onlay mesh technique (sIPOM), recurrence remains a common postoperative complication. The objective of this systematic review and meta-analysis is to compare the efficacy of defect closure (IPOM-plus) versus non-closure in ventral and incisional hernia repair. The aim is to determine which technique yields better outcomes in terms of reducing recurrence and complication rates.
Methods
A comprehensive literature review was conducted in the PubMed, Web of Science, Cochrane Library, Embase, and ClinicalTrials.gov databases from their inception until October 1, 2022, to identify all online English publications that compared the outcomes of laparoscopic ventral hernia repair with and without fascia closure.
Results
Three randomized controlled trials (RCTs) and eleven cohort studies involving 1585 patients met the inclusion criteria. The IPOM-plus technique was found to reduce the recurrence of hernias (OR = 0.51, 95% CI [0.35, 0.76], p < 0.01), seroma (OR = 0.48, 95% CI [0.32, 0.71], p < 0.01), and mesh bulging (OR = 0.08, 95% CI [0.01, 0.42], p < 0.01). Subgroup analysis revealed that body mass index (BMI) (OR = 0.43, 95% CI [0.29, 0.65], p < 0.0001), type of article (OR = 0.51, 95% CI [0.35, 0.76], p = 0.0008 < 0.01), geographical location (OR = 0.54, 95% CI [0.36, 0.82], p = 0.004 < 0.01), follow-up time (OR = 0.50, 95% CI [0.34, 0.73], p = 0.0004 < 0.01) had a significant influence on the postoperative recurrence of the IPOM-plus technique.
Conclusion
The IPOM-plus technique has been shown to greatly reduce the occurrence of recurrence, seroma, and mesh bulging. Overall, the IPOM-plus technique is considered a safe and effective procedure. However, additional randomized controlled studies with extended follow-up periods are necessary to further evaluate the IPOM-plus technique.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Ventral and incisional hernia repair is a common surgical procedure, with up to two million patients worldwide undergoing the procedure every year [1]. The cumulative incidence of incisional hernia may be as high as 28% following open abdominal surgery [2], making it the most common complication following laparotomy and the most common indication for reoperation, triple that of bowel obstruction [3]. In the United States alone, over 250,000 ventral/incisional hernia repairs are performed per year, and this number is expected to increase with the rising number of major abdominal surgeries and aging populations [4]. The burden of ventral/incisional hernia and its recurrences on the healthcare system and economy is substantial [5]. Various surgical approaches to ventral and incisional hernia repair have been developed, including open ventral and incisional hernia (OVIHR) repair using a prosthetic mesh, which involves fascial release to permit myofascial advancement and reconstruction of the linea alba, creating large spaces within the abdominal wall [6]. Minimally invasive surgical techniques, such as laparoscopic ventral hernia and incisional repair (LVHIR), have also been continuously developed. Since its introduction by Karl Leblanc [7], LVIHR has gained increasing acceptance due to its shorter hospital stay, less postoperative pain, and earlier recovery compared to OVIHR. LVIHR is now considered the preferred treatment option for abdominal and incisional hernias by most hernia surgical experts [1, 8]. For ventral/incisional hernia repair, the mesh could be placed in various layers, including inlay, onlay, retrumscular, preperitoneal and intraperitoneal [9].
Intraperitoneal laparoscopic ventral hernia repair is widely accepted and was once the gold standard. IPOM still holds the dominant position in the absence of sufficient evidence [10]. However, two problems have plagued surgeons. The first problem is that intraperitoneal mesh placement may lead to intestinal adhesions. This issue has been improved in recent years with further developments in material science and production process science. The introduction of composite mesh has reduced the incidence of intestinal adhesions [11]. The second problem is recurrence, and IPOM-plus has attracted interest in addressing this issue. A meta-analysis was recently published comparing sIPOM with IPOM-plus [12], and it was concluded that there was no difference between the two techniques in terms of postoperative recurrence. However, it should be noted that this meta-analysis only included three trials, and its conclusion was biased due to the inclusion of an irrelevant study [13]. Additionally, an important randomized controlled trial study [14] was not included in the analysis. Therefore, an updated meta-analysis on this topic is necessary. Our aim is to provide an evidence-based foundation for the selection of surgical techniques and the development of individualized clinical treatment strategies for patients with ventral hernia.
Materials and methods
Inclusion and exclusion criteria
The Systematic review was performed following consultation of the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) [15] guidelines according to a predefined protocol. Registered with PROSPERO and obtained registration number: CRD42022377383.
The research question and eligibility criteria were defined using the PICO criteria. The study inclusion criteria were limited to English-language studies that compared closure versus non-closure techniques in laparoscopic repair of ventral or incisional hernias and included randomized controlled trials and cohort studies. Observational studies without a control group, case series or reports, conference abstracts, editorials, and protocols were excluded. Studies involving patients younger than 18 years of age were also excluded.
Search strategy
The search strategy utilized the following terms: "laparoscopic incisional hernia repair ", "laparoscopic ventral hernia repair", "IPOM-plus", "IPOM", "ventral hernia", "incisional hernia", "fascial defect closure", and "primary closure". The search was conducted on PubMed, Web of Science, Cochrane Library, Embase, and Controlled Trials Reg (http://www.controlled-trials.com), without any country restrictions. The search terms were combined using the Boolean AND/OR operators. The last literature search was performed on 1/10/2022. The search strategy on PubMed was as follows: ((Laparoscopy [Mesh]) AND ("Hernia, ventral" [Mesh] OR "Hernia, umbilical" [Mesh] OR "Incisional Hernia" [Mesh])) AND (Fascial) OR (Fascial closure) OR (defect closure) OR (primary closure) OR (without defect closure)OR (non-closure defect)). This search strategy was also applied to the other four databases.
Study selection
The initially identified studies underwent a screening process for duplicates. The titles and abstracts of the remaining studies were then screened to determine if they met the inclusion or exclusion criteria. Once a potential trial was identified, the full article was read to verify its validity and extract data. Additionally, the references of the included trials were searched to identify any additional relevant studies.
Data extraction
Data extraction and entry were performed independently by two team members. Any disagreements were resolved by discussion until a consensus was reached, or by consulting a third author. The following data were extracted: (1) general characteristics of the literature, including author names, publication year, and study type. (2) Patient demographics, including age, gender, BMI, sample size, and hernia size. (3) Postoperative complications, with the primary outcome being postoperative hernia recurrence. Secondary outcomes included the development of chronic pain, seroma, mesh bulging, and SSI. Seroma was defined as serous fluid retention between the mesh and the anterior abdominal wall, and chronic pain as pain or discomfort in the hernia repair region lasting more than 6 months. For studies on the same topic with different follow-up times, we selected high-quality literature for inclusion in the analysis. Incomplete data were corrected where possible by contacting the respective authors.
Quality assessment
The studies were evaluated for quality by two reviewers to ensure they meet the inclusion criteria, and any disagreements were resolved by consulting with the corresponding authors. The Cochrane Risk of Bias Assessment Tool [16] was used to assess the quality of RCTs, and the results were expressed as low risk, high risk, or unclear. For non-RCTs, the Newcastle–Ottawa Scale [16] (NOS) was used, and the results were expressed as a score out of 10, with studies scoring ≥ 7 considered high-quality, and those scoring ≥ 5 considered medium-quality.
Statistical analysis
Statistical analysis was performed by the statistical software Review Manager Version 5.3 (Cochrane Collaboration, Oxford, UK). Forest plots displayed the relative strength of the treatment effects graphically. The Odds ratio (OR) was calculated for binary data. The 95% confidence interval (CI) was reported for each analyzed value. Heterogeneity was explored with the chi-square test, with the significance set at p < 0.05. Similarly, I2 values were calculated to test for heterogeneity, with a value of 50% or less was considered to be low heterogeneity. This study did not force the median, minimum, maximum, first and third quartiles in the literature to be transformed into sample means and standard deviations, and this transformation would undoubtedly lead to some errors.
Results
Study selection and identification
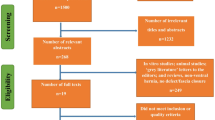
A total of 1845 studies were initially reviewed, and after the stratified screening, 3 randomized controlled trials [14, 18, 19] and 11 cohort studies [20,21,22,23,24,25,26,27,28,29,30], which met the inclusion criteria and included 1585 patients, were finally selected. The process and results of the literature screening are presented in Fig. 1.
Characteristics of included studies
This meta-analysis included a total of 1585 patients, with 721 undergoing IPOM-plus and 864 undergoing sIPOM. 13 studies were identified for recurrence rates [18,19,20,21,22,23,24,25,26,27,28,29,30], 13 studies for seroma [14, 18, 19, 21,22,23,24,25,26,27,28,29,30], 10 studies for SSI [14, 18, 21,22,23,24,25,26, 29, 30], 7 studies for chronic pain [18, 19, 24, 26,27,28, 30], and 3 studies for mesh bulging [21, 28, 31]. The basic characteristics of the included studies were summarized and presented in Table 1.
Quality assessment of included studies
The Cochrane Risk of Bias Assessment Tool was used to evaluate three randomized controlled trials (RCTs) [14, 18, 19]. The 'Risk of bias' graph (Fig. 2)and the 'Risk of bias' summary table (Fig. 3)provide an overview of the 'Risk of bias' assessment, all of which mentioned randomization and were registered at ClinicalTrials.gov with individual registration numbers. One RCT detailed the randomization process, which involved creating a separate randomization list by computer for each participating center. Three of the RCTs were multicenter studies [14, 18, 19]. Additionally, eleven cohort studies [20,21,22,23,24,25,26,27,28,29,30] were evaluated using the Newcastle–Ottawa Scale. Five were evaluated as high quality (scores ≥ 7) [20, 21, 25, 28, 29], and six were evaluated as moderate quality (scores ≥ 5). Table 2 shows the results of the quality evaluation for the cohort studies.
Meta-analysis results
Recurrence rate
13 studies [18,19,20,21,22,23,24,25,26,27,28,29,30] (2 RCTs [18, 19] and 11 cohort studies [20,21,22,23,24,25,26,27,28,29,30]) reported recurrence data, which included a total of 1401 patients. There was no statistically significant heterogeneity among the studies (I2 = 24% < 50% p = 0.20 > 0.01). The clinical heterogeneity was acceptable, and a fixed-effects model was used for the analysis. The results showed that the recurrence rate after IPOM-plus was 6.66% (42/631), and the recurrence rate after sIPOM was 11.43% (88/770). IPOM-plus reduced the recurrence rate by 3.28% compared to sIPOM. Furthermore, IPOM-plus significantly reduced the postoperative recurrence rate with a statistically significant difference (OR = 0.51, 95% CI [0.35, 0.76], p < 0.01) (Fig. 4).
Seroma
There were 13 studies [14, 18, 19, 21,22,23,24,25,26,27,28,29,30] that reported on the incidence of seroma, including 3 RCTs [14, 18, 19] and 10 cohort studies [21,22,23,24,25,26,27,28,29,30], with a total of 1395 patients included. there was no statistically significant heterogeneity among the studies (I2 = 0% < 50% p = 0.47 > 0.01). A fixed-effects model was chosen for the analysis, which showed that the incidence of seroma after IPOM-plus was 6.99% (46/658), and the incidence of seroma after sIPOM was 12.07% (89/737). IPOM-plus reduced the incidence of seroma after sIPOM by 3.08%, and there was a statistically significant difference in the incidence of postoperative seroma between IPOM-plus and sIPOM (OR = 0.48, 95% CI [0.32, 0.71], p < 0.01) (Fig. 5).
Surgical site infection (SSI)
There were 10 studies [14, 18, 21,22,23,24,25,26, 29, 30] that reported on the incidence of SSI, including 2 RCTs [14, 18] and 8 cohort studies [21,22,23,24,25,26, 29, 30], with a total of 1218 patients included. There was no statistically significant heterogeneity among the studies (I2 = 0% < 50% p = 0.92 > 0.01). A fixed-effects model was chosen for the analysis, which showed that the incidence of incision site infection after IPOM-plus was 5.11% (30/587), and the incidence of incision site infection after sIPOM was 5.86% (37/631). There was no statistically significant difference between sIPOM and IPOM-plus in terms of the incidence of incision site infection (OR = 0.82, 95% CI [0.49, 1.38], p = 0.46 > 0.05) (Fig. 6).
Postoperative chronic pain
There were 7 studies on chronic pain [18, 19, 24, 26,27,28, 30], 2 of which were RCTs [18, 19] and 5 were cohort studies [24, 26,27,28, 30], including a total of 538 patients. There was no statistically significant heterogeneity among the studies (I2 = 0% < 50%, p = 0.83 > 0.01). A fixed-effects model was selected. The results showed that the incidence of chronic pain after IPOM-plus was 7.14% (19/266), and the incidence of chronic pain after sIPOM was 9.93% (27/272). There was no statistically significant difference in the incidence of chronic pain after sIPOM compared with IPOM-plus (OR = 0.92, 95% CI [0.48, 1.76], p = 0.80 > 0.05) (Fig. 7).
Mesh bulging
Three cohort studies [21, 28, 30] investigated mesh bulging, involving a total of 228 patients. There was no statistically significant heterogeneity among the studies (I2 = 0% < 50%, p = 0.82 > 0.01), and a fixed-effects model was chosen. None of the cases had mesh bulge after IPOM-plus, while the incidence of bulging after sIPOM was 12.40% (15/121). IPOM-plus significantly reduced the incidence of postoperative mesh buging with a statistically significant difference (OR = 0.08, 95% CI [0.01, 0.42], p < 0.01) (Fig. 8).
Subgroup analysis
Subgroup analysis by BMI based on recurrence
Two groups were included in the analysis: BMI ≥ 30 kg/m2 and BMI < 30 kg/m2, comprising 8 studies with 935 patients in the BMI ≥ 30 kg/m2 group and 3 studies with 229 patients in the BMI < 30 kg/m2 group. A total of 11 studies with 1164 patients were included in the meta-analysis. There was no statistically significant heterogeneity among the studies (I2 = 12% < 50%, p = 0.88 > 0.01). The clinical heterogeneity was acceptable, and a fixed-effects model was chosen. The results indicated that IPOM-plus significantly reduced the postoperative recurrence rate in patients with BMI ≥ 30 kg/m2 with a statistically significant difference [OR = 0.50, 95% CI [0.31, 0.79], p = 0.003 < 0.05]; For patients with a BMI < 30 kg/m2, there was also statistically significant difference between IPOM-plus and sIPOM (OR = 0.27, 95% CI [0.11, 0.67], p = 0.004 < 0.01). Overall, patients' BMI had a significant impact on the postoperative recurrence rate, with a statistically significant difference [OR = 0.43, 95% CI [0.29, 0.65], p < 0.0001] (Fig. 9).
Subgroup analysis by article type based on recurrence
Recurrence was analyzed based on the type of articles: RCT and non-RCT (NRCT) groups. The RCT group comprised 2 studies with 196 patients, while the NRCT group comprised 11 studies with 1205 patients. After pooling, a total of 13 studies with 1401 patients were included. There was no statistically significant heterogeneity among the studies (I2 = 24% < 50%, p = 0.20 > 0.05). Clinical heterogeneity was acceptable, and a fixed-effects model was selected. The results of the NRCT group showed that IPOM-plus significantly reduced the postoperative recurrence rate in patients with NRCT, with a statistically significant difference [OR = 0.46, 95% CI [0.30, 0.72], p = 0.0006 < 0.05]; in the randomized controlled trial (RCT) group, the observed difference between IPOM-plus and IPOM was not statistically significant (OR = 0.77, 95% CI [0.33, 1.82], p = 0.56 > 0.05). Overall, the quality of the literature included in the study had a significant impact on the postoperative recurrence rate, with a statistically significant difference [OR = 0.51, 95% CI [0.35, 0.76], p = 0.0008 < 0.01] (Fig. 10).
Subgroup analysis by geographical location based on recurrence
Three groups were studied: American, European, and Asian, including 7 studies with 903 patients in the American group, 2 studies with 194 patients in the European group, and 3 studies with 231 patients in the Asian group. After pooling, a total of 12 studies with 1328 patients were included. There was no significant heterogeneity among the studies (I2 = 27% < 50%, p = 0.18 > 0.05). Clinical heterogeneity was acceptable, and a fixed-effects model was used. The results showed that IPOM-plus significantly reduced the postoperative recurrence rate for patients in Asia [OR = 0.25, 95% CI [0.07, 0.91], p = 0.04 < 0.05] and for patients in Europe [OR = 0.28, 95% CI [0.09, 0.84], p = 0.02 < 0.05]; There was no statistically significant difference observed between IPOM-plus and IPOM for patients in the Americas. (OR = 0.71, 95% CI [0.44, 1.14], p = 0.16 > 0.05). Overall, there was a significant difference in postoperative recurrence rates among patients from different geographical locations [OR = 0.54, 95% CI [0.36, 0.82], p = 0.004 < 0.01] (Fig. 11).
Subgroup analysis by Follow-up time based on recurrence
Subgroup analysis of recurrence was carried out in three periods: ≤ 6 months, 6–12 months, and ≥ 12 months, including 2 studies with 242 patients in the ≤ 6 months group, 3 studies with 433 patients in the 6–12 months group, and 7 studies with 706patients in the ≥ 12 months. As shown in Fig. 12. The results indicated that IPOM-plus significantly reduced the postoperative recurrence rate in the three periods, and follow-up time may be a source of heterogeneity. [OR = 0.50, 95% CI [0.34, 0.73], p = 0.0004 < 0.01] (Fig. 12).
Sensitivity analysis
A sensitivity analysis of the recurrence of outcome indicators with heterogeneity was performed by excluding studies with large differences, and it was found that the study of Wennergren JE [29] had a large effect on heterogeneity, and the I2 decreased from 24 to 0% after excluding this study, suggesting that the study of Wennergren JE may be the source of heterogeneity, but the results did not change, indicating that the conclusions obtained were more robust.
Publication bias assessment
A funnel plot test was conducted to assess publication bias based on recurrence plotting, which revealed two significant outliers in the study of Bernardi [18] and Wennergren [29]. After removing this study, all included studies were within the 95% confidence interval. However, based on visualization, it was observed that some of the included studies were not symmetrical about the vertical axis, indicating the presence of some publication bias in this meta-analysis (Fig. 13).
Discussion
In the early days of IPOM, most scholars believed that ventral hernias should be repaired "tension-free" like inguinal hernias, without closure of the hernial defect [31, 32]. The rationale behind this was that forcibly closing the hernia defect would increase intra-abdominal pressure and cause a pulling sensation at the surgical site after the operation, leading to chronic pain in the late stage. Furthermore, high-tension sutures may cut the abdominal wall, causing secondary injury. However, a large number of recent studies have challenged this perception and shown that closing the hernia defect can reduce the incidence of mesh bulging and chronic pain [19, 28, 33]. As a result, most scholars have shifted their approach from the earlier concept of "tension-free repair" to the current concept of "restoring the function of the abdominal wall" [34]. In particular, the hernia defect in the central zone, where the white line is the convergence of the abdominal wall stresses, is reconstructed to restore the original function of the abdominal wall. Placing the rectus abdominis in a physiological position improves functional status, cosmetic satisfaction, and ultimately quality of life [24], which led to the invention of IPOM-plus technology. However, the question of whether closing the hernia defect can achieve long-term benefit or not is a matter of great debate. Lambrecht [35] published a randomized controlled study in 2015 with a mean follow-up of up to 38 months, which concluded that closing the hernia defect increased the overall rate of complications instead of providing long-term benefits. Additionally, the high recurrence rate for extremely obese patients with large fascial defect hernias is yet to be resolved. A recent review [36] concluded that the relative merits of the two techniques remain unclear.
Summary of main results
In this meta-analysis and review, we pooled 14 studies (3 RCTs, 11 cohort studies), including 1585 patients, and found that laparoscopic repair of ventral and incisional hernias with fascial defect closure significantly reduced postoperative recurrence, mesh bulging and seroma formation. There was no difference between the two techniques for other postoperative complications, such as postoperative chronic pain and surgical site infection. However, we observed a significant reduction in the incidence of mesh bulging and postoperative seroma formation with fascial defect closure, and the low interstudy heterogeneity (I2 = 0%) in the analysis suggests that the findings regarding these outcomes may be reliable. The results of our subgroup analysis indicated that patients' BMI, study type, geographic location and follow-up time were potential sources of heterogeneity and all had an impact on postoperative recurrence.
Principal findings and other studies
The results of this meta-analysis showed that the IPOM-plus technique significantly reduces postoperative recurrence, which is the primary outcome measure of long-term success of the surgery and is a major concern for scholars. Recent discussions have highlighted the effectiveness of primary laparoscopic repair with mesh placement for the management of ventral and incisional hernia, as evidenced by low recurrence rates [20, 37]. A meta-analysis conducted by Holihan et al. [38]. also concluded that primary fascial closure in open ventral hernia repair is associated with fewer surgical site occurrences and recurrences than bridged repair, which is generally consistent with our findings. The IPOM-plus technique may reduce postoperative recurrence because, firstly, closure of the hernia defect reestablishes the integrity of the abdominal wall, enabling it to bear forces evenly in all directions. If the hernia defect is not closed, the defect is more likely to bulge and eventually cause hernia recurrence while bearing the same forces. Secondly, hernia defect closure allows for a greater mesh overlap at the time of repair, resulting in a reduction in recurrence rates [20].
The results of this meta-analysis indicate that the IPOM-plus technique significantly reduces the incidence of postoperative seroma compared to sIPOM. A meta-analysis [39] also concluded that IPOM-plus had significantly lower rates of seroma formation compared to sIPOM, which is consistent with our findings. The IPOM-plus technique may reduce the formation of postoperative seroma because the hernia sac is not dissected out, and the hernia space is isolated from the abdominal cavity by the mesh. However, the reported incidence of seroma varies widely in the literature, ranging from 0.5 to 78% [40]. A study by Perrone et al. [41] concluded that the most common complication after laparoscopic ventral and incisional hernia repair was seroma, which can cause discomfort, pain, infections and negatively affect the aesthetic outcome for patients. Regardless, our findings suggest that closure of the fascial defect may reduce the formation of postoperative seroma.
The findings of this meta-analysis indicate that the IPOM-plus technique significantly reduces postoperative mesh bulging. Mesh bulging can be easily misdiagnosed as a hernia recurrence, leading to an overestimation of recurrence rates and making it clinically challenging to differentiate between the two. The mechanism underlying mesh bulging involves the protrusion of the central nonfunctioning portion of the abdominal wall into the hernia sac due to intraabdominal pressure, as described by Laplace's law. This results in the patient feeling a noticeable bulge in the area. This underscores the importance of using high-resolution imaging techniques such as computed tomography (CT) or magnetic resonance imaging to establish an accurate diagnosis [42]. These imaging techniques can reveal the mesh and help clinicians determine whether the patient has a recurrence or a bulge caused by mesh protrusion. In a study by Clapp et al. [30], the incidence of mesh bulging was significantly higher after IPOM compared to IPOM-plus. The study also concluded that IPOM-plus can effectively control both mesh bulging and recurrence. This is consistent with the results of our study.
In relation to postoperative chronic pain and surgical site infection, this meta-analysis discovered that IPOM-plus did not decrease the incidence of these complications compared to sIPOM. It is well-known that IPOM-plus contradicts the concept of tenselessness, which could result in a higher incidence of postoperative chronic pain compared to sIPOM, as reported by previous studies [28]. However, the current meta-analysis did not reach a definitive conclusion on this matter. We speculate that the subjective perception of pain varies among patients, making it challenging to objectively evaluate chronic pain in the included literature. Some studies have suggested that the lower incidence of postoperative surgical site infections with IPOM-plus compared to sIPOM may be due to the lower incidence of postoperative seroma with IPOM-plus, which in turn results in a lower incidence of secondary infections associated with seroma. While this study did find a lower incidence of postoperative seroma with IPOM-plus, it did not find a corresponding lower incidence of postoperative surgical site infections with IPOM-plus, as shown in the previous analysis.
In 2016, Tandon et al. conducted a meta-analysis [39] of 16 studies with 3638 patients, concluding that laparoscopic ventral hernia repair reduces seroma formation and adverse hernia-site events. In 2022, Tryliskyy et al. [12] pooled three studies, including 259 patients, and found that both closure and non-closure techniques have an equal safety profile and do not differ in the risk of recurrence, seroma formation, or risks of clinical or radiological eventration. However, our present meta-analysis produced different results. Tandon et al. included seven observational studies without a control group, which could significantly affect the quality of the study and the pooled results. Tryliskyy et al. [12] only included three randomized controlled trials with a small number of patients and literature. Moreover, In Tryliskyy's research study, the comparison between IPOM and IPOM-plus did not reflect a true comparison, as one study by Ali et al. added an extra step to the surgical operation on the peritoneum, which is not typically performed during IPOM [13]. In contrast, our meta-analysis included 3 randomized controlled trials and 11 cohort studies, which involved a larger number of patients and higher quality literature. Therefore, our results are more precise and comprehensive than those of the previous studies. We believe that our conclusions are more robust and reliable.
Subgroup analysis and interpretation
We conducted a subgroup analysis based on hernia defect size, BMI, geographic location, study type and follow-up time to explore the factors that may affect the outcome of laparoscopic ventral hernia repair (LVHR), with recurrence being the main outcome indicator. However, the diversity of hernia defect data expression prevented a meta-analysis of hernia defects. A published study analyzed whether hernia size affects postoperative recurrence [29]. A subgroup analysis was performed, stratifying by hernia defect width (< 3, 3–6 and > 6 cm), and it was concluded that there was no statistically significant difference between the different hernia widths and postoperative recurrence between the two techniques [29]. In the subgroup analysis based on BMI, our meta-analysis found that increased recurrence rate after LVHR in patients with BMI ≥ 30 kg/m2. This finding is consistent with a meta-analysis published in 2021[43] that concluded that patients with a higher BMI had a greater chance of recurrence following LVHR. Another retrospective study, which included 26,268 patients, supports the association between BMI and increased recurrence rate following LVHR [44]. This could be explained by the fact that intra-abdominal pressure and abdominal wall tension are directly related to the abdominal wall radius, which is increased in obese patients, leading to an enlargement of the hernia defect [45]. Moreover, excess intra-abdominal fat can hinder visualization during laparoscopic surgery, resulting in increased surgical complexity and duration [46].
Regarding the subgroup analysis based on geographic location, type of literature and follow-up time, our results showed significant differences in the recurrence rates between studies conducted in different regions. This could be attributed to variations in economic, health, and technical proficiency among medical staff in different regions. However, we were surprised to find that IPOM-plus performed in Europe and Asia significantly reduced the postoperative recurrence rate compared to IPOM-plus performed in the Americas (mainly in the United States), where the difference was not statistically significant. This finding is not consistent with our initial perception and requires further investigation. It's important to exercise caution when interpreting the results of subgroup analyses. Our findings suggest that the quality of the literature may significantly impact the meta-analysis results. RCT studies are typically considered more reliable and homogeneous than non-RCT studies. as reported by Pawlak et al. [47], the onset of all cases of recurrence was within the first 6 months postoperatively, This study suggests that follow-up time may have an effect on recurrence, which is consistent with the results of our subgroup analysis, and that follow-up time may be a possible source of outcome heterogeneity.
Our funnel plot test for publication bias, based on the plotting of relapse rates, identified an outlier—the study by Wennergren [29], which reported a significantly higher recurrence rate of 18.37% among the included population. Notably, the number of recurrences in this study accounted for 31.86% of all recurrences in the included population. Upon closer examination of this study, we found that a higher proportion of patients had comorbidities, such as diabetes mellitus (21.43% or 42/196) and ASA class III/IV (44.90% or 88/196), as well as unhealthy lifestyle habits, such as smoking (31.63% or 62/196). Patients with underlying diseases or unhealthy lifestyle habits are known to be at a higher risk of postoperative recurrence.
Strengths and limitations
This study has several significant strengths, making it the most comprehensive and largest study to date. Firstly, it includes large data from multiple RCTs and cohort studies and provides a uniform definition of key outcome indicators. Additionally, there is less heterogeneity among the included literature, with a heterogeneity test for seroma, SSI, postoperative chronic pain, and mesh bulging at 0%, and the heterogeneity test for recurrence less than 50%. Secondly, the quality of the included literature was high, making the credibility of the meta-analysis results high. This study includes three RCTs and five high-quality Cohort Studies. Lastly, a subgroup analysis of the main outcome indicator (recurrence) was performed to further clarify the factors affecting recurrence. However, this study also has some limitations. Firstly, only a small number of RCTs were included in the literature reviewed. Out of the 14 publications included, only 3 were RCTs, and one of these did not report the primary outcome indicator (recurrence). Secondly, the duration of follow-up varied widely, which may have impacted the outcome indicators. The longest period in the included literature was 44 months, and the shortest was 1 month, making it difficult to explore the recurrence rate after hernia repair as it depends on the follow-up period [47]. To minimize the effect of follow-up time on the results, our meta-analysis excluded a study with a 1-month follow-up because it did not report recurrence rates, in addition, we performed a subgroup analysis of follow-up time in order to explore the source of heterogeneity. Nevertheless, the results should still be interpreted with caution. Thirdly, we recommend that future studies should select indicators that accurately reflect the study content, report outcome data in detail and in a standardized manner, and strictly evaluate the quality of the literature to reduce bias. Finally, the definitions of certain outcome indicators or diagnostic criteria differed across the included studies. For example, the diagnosis of seroma was based on different criteria by different authors. We established a uniform definition of seroma and included studies with a large and more stable sample size. However, the result that IPOM-plus significantly reduced the incidence of postoperative seroma should be interpreted with caution. Of the 13 included studies, seroma definition was only reported in 3 studies [14, 19, 30]. An important classification of seromas was proposed by Morales-Conde [49], who classified clinical seroma into 5 groups, ranging from 0 to IV. Types I and II would be considered an incident, while Types III and IV would be considered a complication, since a medical or invasive therapy is necessary. This new classification will provide new ideas for a closer study of seromas, however, the included studies did not adapt the proposed criteria, and we could not further classify the severity of the seroma formation in each study. In the future, global uniform evaluation criteria should be established to clarify the definition of seroma, which is crucial for understanding its true incidence.
However, we need to be aware that, for IPOM procedure, the potential risk of an intraperitoneal foreign mesh placement has not yet been solved and traumatic mesh fixation during this procedure increases the risk of adhesions, visceral damage, nerve injury, and acute and chronic pain [50].To solve this problem, a number of new technologies are emerging including MILOS (mini-or less-open sublay) [51, 52], EMILOS (endoscopic mini/less open sublay) [53], and robotic extraperitoneal mesh procedures [54]. Reinpold W et al. compared the results of the MILOS operation with the IPOM, the study concluded that the MILOS technique allows minimally invasive transhernial repair of incisional hernias using large retromuscular/preperitoneal meshes with low morbidity [52]. Schwarz et al. performed the new technique of EMILOS to put mesh outside the abdominal cavity and found that the procedure is reliable, reproducible and easily standardized [53].
Conclusion
The IPOM-plus technique has been shown to greatly reduce the occurrence of recurrence, seroma, and mesh bulging. Overall, the IPOM-plus technique is considered a safe and effective procedure. However, additional randomized controlled studies with extended follow-up periods are necessary to further evaluate the IPOM-plus technique.
Data access statement
Requests for availability of the data may be made to the corresponding author.
References
Bittner R, Bain K, Bansal VK et al (2019) Update of guidelines for laparoscopic treatment of ventral and incisional abdominal wall hernias (International Endohernia Society (IEHS))-Part A. Surg Endosc 33:3069–3139. https://doi.org/10.1007/s00464-019-06907-7
Rutkow IM (2003) Demographic and socioeconomic aspects of hernia repair in the United States in 2003. Surg Clin North Am 83:1045–vi. https://doi.org/10.1016/S0039-6109(03)00132-4
Duepree HJ, Senagore AJ, Delaney CP, Fazio VW (2003) Does means of access affect the incidence of small bowel obstruction and ventral hernia after bowel resection? Laparoscopy versus laparotomy. J Am Coll Surg 197:177–181. https://doi.org/10.1016/S1072-7515(03)00232-1
National Center for Health Statistics (1998) Vital and health statistics of the centers for disease control and prevention. Adv Data 300–307
Poulose BK, Shelton J, Phillips S, Moore D, Nealon W, Penson D, Beck W, Holzman MD (2012) Epidemiology and cost of ventral hernia repair: making the case for hernia research. Hernia 16:179–183. https://doi.org/10.1007/s10029-011-0879-9
Pauli EM, Rosen MJ (2013) Open ventral hernia repair with component separation. Surg Clin North Am 93:1111–1133. https://doi.org/10.1016/j.suc.2013.06.010
LeBlanc KA, Booth WV (1993) Laparoscopic repair of incisional abdominal hernias using expanded polytetrafluoroethylene:preliminary findings. Surg Laparosc Endosc 3:39–41
Misiakos EP, Machairas A, Patapis P, Liakakos T (2008) Laparoscopic ventral hernia repair: pros and cons compared with open hernia repair. JSLS 12:117–125
Parker SG, Halligan S, Liang MK et al (2020) International classification of abdominal wall planes (ICAP) to describe mesh insertion for ventral hernia repair. Br J Surg 107:209–217. https://doi.org/10.1002/bjs.11400
Van Hoef S, Tollens T (2019) Primary non-complicated midline ventral hernia: is laparoscopic IPOM still a reasonable approach? Hernia 23:915–925. https://doi.org/10.1007/s10029-019-02031-6
Su J, Liu B, He H, Ma C, Wei B, Li M, Li J, Wang F, Sun J, Liu K, Zhang H (2022) Engineering high strength and super-toughness of unfolded structural proteins and their extraordinary anti-adhesion performance for abdominal hernia repair. Adv Mater 34:e2200842. https://doi.org/10.1002/adma.202200842
Tryliskyy Y, Wong CS, Demykhova I, Tyselskyi V, Kebkalo A, Poylin V, Pournaras DJ (2022) Fascial defect closure versus bridged repair in laparoscopic ventral hernia mesh repair: a systematic review and meta-analysis of randomized controlled trials. Hernia 26:1473–1481. https://doi.org/10.1007/s10029-021-02533-2
Ali F, Wallin G, Fathalla B, Sandblom G (2020) Peritoneal bridging versus fascia closure in laparoscopic intraperitoneal onlay ventral hernia mesh repair: a randomized clinical trial. BJS Open 4:587–592. https://doi.org/10.1002/bjs5.50305
Ahonen-Siirtola M, Nevala T, Vironen J, Kössi J, Pinta T, Niemeläinen S, Keränen U, Ward J, Vento P, Karvonen J, Ohtonen P, Mäkelä J, Rautio T (2018) Laparoscopic versus hybrid approach for treatment of incisional ventral hernia: a prospective randomized multicenter study of 1-month follow-up results. Hernia 22:1015–1022. https://doi.org/10.1007/s10029-018-1784-2
Moher D, Shamseer L, Clarke M, Ghersi D, Liberati A, Petticrew M, Shekelle P, Stewart LA (2015) Preferred reporting items for systematic review and meta-analysis protocols (PRISMA-P) 2015 statement. Syst Rev 4:1. https://doi.org/10.1186/2046-4053-4-1
Higgins JPT, Savović J, Page MJ, Elbers RG, Sterne JAC (2020) Chapter 8: assessing risk of bias in a randomized trial. In: Higgins JPT, Thomas J, Chandler J, Cumpston M, Li T, Page MJ, Welch VA (eds) Cochrane handbook for systematic reviews of interventions version 6.1 (updated September 2020). Cochrane. http://www.training.cochrane.org/handbook. Accessed 28 Nov 2020
Wells GA, Shea B, O’Connell D, Peterson J, Welch V, Losos M et al (2000) The Newcastle–Ottawa Scale (NOS) for assessing the quality of nonrandomised studies in meta-analyses. Oxford
Bernardi K, Olavarria OA, Holihan JL, Kao LS, Ko TC, Roth JS, Tsuda S, Vaziri K, Liang MK (2020) Primary fascial closure during laparoscopic ventral hernia repair improves patient quality of life: a multicenter, blinded randomized controlled trial. Ann Surg 271:434–439. https://doi.org/10.1097/SLA.0000000000003505
Christoffersen MW, Westen M, Rosenberg J, Helgstrand F, Bisgaard T (2020) Closure of the fascial defect during laparoscopic umbilical hernia repair: a randomized clinical trial. Br J Surg 107:200–208. https://doi.org/10.1002/bjs.11490
Banerjee A, Beck C, Narula VK, Linn J, Noria S, Zagol B, Mikami D (2012) Laparoscopic ventral hernia repair: does primary repair in addition to placement of mesh decrease recurrence? Surg Endosc 26:1264–1268. https://doi.org/10.1002/bjs.11490
Basukala S, Tamang A, Rawal SB, Malla S, Bhusal U, Dhakal S, Sharma S (2022) Comparison of outcomes of laparoscopic hernioplasty with and without fascial repair [IPOM-plus vs IPOM] for ventral hernia: a retrospective cohort study. Ann Med Surg 80:104297. https://doi.org/10.1016/j.amsu.2022.104297
Zeichen MS, Lujan HJ, Mata WN, Maciel VH, Lee D, Jorge I, Plasencia G, Gomez E, Hernandez AM (2013) Closure versus non-closure of hernia defect during laparoscopic ventral hernia repair with mesh. Hernia 17:589–596. https://doi.org/10.1007/s10029-013-1115-6
Gonzalez AM, Romero RJ, Seetharamaiah R, Gallas M, Lamoureux J, Rabaza JR (2015) Laparoscopic ventral hernia repair with primary closure versus no primary closure of the defect: potential benefits of the robotic technology. Int J Med Robot 11:120–125. https://doi.org/10.1002/rcs.1605
Light D, Bawa S (2016) Trans-fascial closure in laparoscopic ventral hernia repair. Surg Endosc 30:5228–5231. https://doi.org/10.1007/s00464-016-4868-z
Mitura K, Skolimowska-Rzewuska M, Garnysz K (2017) Outcomes of bridging versus mesh augmentation in laparoscopic repair of small and medium midline ventral hernias. Surg Endosc 31:382–388. https://doi.org/10.1007/s00464-016-4984-9
Nguyen D, Szomstein S, Ordonez A, Dip F, Rajan M, Menzo EL, Rosenthal RJ (2016) Unidirectional barbed sutures as a novel technique for laparoscopic ventral hernia repair. Surg Endosc 30:764–769. https://doi.org/10.1007/s00464-015-4275-x
Sharma D, Jindal V, Pathania OP, Thomas S (2010) Novel technique for closure of defect in laparoscopic ventral hernia repair. J Minim Access Surg 6:86–88. https://doi.org/10.4103/0972-9941.68580
Suwa K, Okamoto T, Yanaga K Is fascial defect closure with intraperitoneal onlay mesh superior to standard intraperitoneal onlay mesh for laparoscopic repair of large incisional hernia? Asian J Endosc Surg 11:378–384. https://doi.org/10.4103/0972-9941.68580
Wennergren JE, Askenasy EP, Greenberg JA, Holihan J, Keith J, Liang MK, Martindale RG, Trott S, Plymale M, Roth JS (2016) Laparoscopic ventral hernia repair with primary fascial closure versus bridged repair: a risk-adjusted comparative study. Surg Endosc 30:3231–3238. https://doi.org/10.1007/s00464-015-4644-5
Clapp ML, Hicks SC, Awad SS, Liang MK (2013) Trans-cutaneous Closure of Central Defects (TCCD) in laparoscopic ventral hernia repairs (LVHR). World J Surg 37:42–51. https://doi.org/10.1007/s00268-012-1810-y
Moreau PE, Helmy N, Vons C (2012) Laparoscopic treatment of incisional hernia. State of the art in 2012. J Visc Surg 149:e40–e48. https://doi.org/10.1016/j.jviscsurg.2012.09.001
Burger JW, Luijendijk RW, Hop WC, Halm JA, Verdaasdonk EG, Jeekel J (2004) Long-term follow-up of a randomized controlled trial of suture versus mesh repair of incisional hernia. Ann Surg 240:578–583. https://doi.org/10.1097/01.sla.0000141193.08524.e7
Chelala E, Baraké H, Estievenart J, Dessily M, Charara F, Allé JL (2016) Long-term outcomes of 1326 laparoscopic incisional and ventral hernia repair with the routine suturing concept: a single instit ution experience. Hernia 20:101–110. https://doi.org/10.1007/s10029-015-1397-y
Bittner R, Bingener-Casey J, Dietz U et al (2014) International Endohernia Society [IEHS]. Guidelines for laparoscopic treatment of ventral and incisional abdominal wall hernias [International Endohernia Society [IEHS]-part 1. Surg Endosc 28:2–29. https://doi.org/10.1007/s00464-013-3170-6
Lambrecht JR, Vaktskjold A, Trondsen E, Øyen OM, Reiertsen O (2015) Laparoscopic ventral hernia repair: outcomes in primary versus incisional hernias: no effect of defect closure. Hernia 19:479–486. https://doi.org/10.1007/s10029-015-1345-x
Suwa K, Okamoto T, Yanaga K (2016) Closure versus non-closure of fascial defects in laparoscopic ventral and incisional hernia repairs: a review of the literature. Surg Today 46:764–773. https://doi.org/10.1007/s00595-015-1219-y
Toffolo Pasquini M, Medina P, Arrechea Antelo R, Cerutti R, Porto EA, Pirchi DE (2023) Ring closure outcome for laparoscopic ventral hernia repair (IPOM plus) in medium and large defects. Long-term follow-up. Surg Endosc 37:2078–2084. https://doi.org/10.1007/s00464-022-09738-1
Holihan JL, Nguyen DH, Nguyen MT, Mo J, Kao LS, Liang MK (2016) Mesh location in open ventral hernia repair: a systematic review and network meta-analysis. World J Surg 40:89–99. https://doi.org/10.1007/s00268-015-3252-9
Tandon A, Pathak S, Lyons NJ, Nunes QM, Daniels IR, Smart NJ (2016) Meta-analysis of closure of the fascial defect during laparoscopic incisional and ventral hernia repair. Br J Surg 103:1598–1607. https://doi.org/10.1002/bjs.10268
Parker HH 3rd, Nottingham JM, Bynoe RP, Yost MJ (2002) Laparoscopic repair of large incisional hernias. Am Surg 68:530–533
Perrone JM, Soper NJ, Eagon JC, Klingensmith ME, Aft RL, Frisella MM, Brunt LM (2005) Perioperative outcomes and complications of laparoscopic ventral hernia repair. Surgery 138:708–715. https://doi.org/10.1016/j.surg.2005.06.054
Schoenmaeckers EJ, Wassenaar EB, Raymakers JT, Rakic S (2010) Bulging of the mesh after laparoscopi repair of ventral and incisional hernias. JSLS 14:541–546. https://doi.org/10.4293/108680810X12924466008240
Parker SG, Mallett S, Quinn L, Wood CPJ, Boulton RW, Jamshaid S, Erotocrito M, Gowda S, Collier W, Plumb AAO, Windsor ACJ, Archer L, Halligan S (2021) Identifying predictors of ventral hernia recurrence: systematic review and meta-analysis. BJS Open 5:zraa071. https://doi.org/10.1093/bjsopen/zraa071
Lau B, Kim H, Haigh PI, Tejirian T (2012) Obesity increases the odds of acquiring and incarcerating noninguinal abdominal wall hernias. Am Surg 78:1118–1121
Frezza EE, Shebani KO, Robertson J, Wachtel MS (2007) Morbid obesity causes hcronic increase of intraabdominal pressure. DigDis Sci 52:1038–1041. https://doi.org/10.1007/s10620-006-9203-4
Ching SS, Sarela AI, Dexter SP, Hayden JD, McMahon MJ (2008) Comparison of early outcomes for laparoscopic ventral hernia repair between nonobese and morbidly obese patient populations. World J Surg 22:2244–2250. https://doi.org/10.1007/s00464-008-0039-1
Pawlak M, Hilgers RD, Bury K, Lehmann A, Owczuk R, Smietanski M (2015) Comparison of two different concepts of mesh and fixation technique in laparoscopic ventral hernia repair: a randomized controlled trial. Surg Endosc 30(3):1188–1197. https://doi.org/10.1007/s00464-015-4329-0
Staarink M, van Veen RN, Hop WC, Weidema WF (2008) A 10-year repair follow-up study on endoscopic total extraperito-neal repair of primary and recurrent inguinal hernia. Surg Endosc 22:1803–1806. https://doi.org/10.1007/s00464-008-9917-9
Morales-Conde S (2012) A new classification for seroma after laparoscopic ventral hernia repair. Hernia 16:261–267. https://doi.org/10.1007/s10029-012-0911-8
Bittner R, Bingener-Casey J, Dietz U et al (2014) Guidelines for laparoscopic treatment of ventral and incisional abdominal wall hernias (International Endohernia Society [IEHS])—PartIII. Surg Endosc 28:380–404. https://doi.org/10.1007/s00464-013-3172-4
Reinpold W (2015) Endoskopisch total extraperitonealer transhernialer sublay Bauchwand-Hernienverschluss in singleport-technik. In: Schumpelick V, Arlt G, Conze J, Junge K (eds) Hernien, 5th edn. Thieme, Stuttgart, pp 301–304
Reinpold W, Schröder M, Berger C, Nehls J, Schröder A, Hukauf M, Köckerling F, Bittner R (2019) Mini- or less-open sublay operation (MILOS): a new minimally invasive technique for the extraperitoneal mesh repair of incisional hernias. Ann Surg 269:748–755. https://doi.org/10.1097/SLA.0000000000002661
Schwarz J, Reinpold W, Bittner R (2017) Endoscopic mini/less open sublay technique (EMILOS)-a new technique for ventral hernia repair. Langenbecks Arch Surg 402:173–180. https://doi.org/10.1007/s00423-016-1522-0
Kudsi OY, Gokcal F, Chang K (2020) Robotic intraperitoneal onlay versus totally extraperitoneal (TEP) retromuscular mesh ventral hernia repair: a propensity score matching analysis of short-term outcomes. Am J Surg 220:837–844. https://doi.org/10.1016/j.amjsurg.2020.01.003
Funding
This research did not receive any specific Grant funding.
Author information
Authors and Affiliations
Contributions
All authors were involved in the conception, design, material preparation, data collection and analysis of the study. The first draft of the manuscript was written by XH, and JL revised the manuscript several times and checked the quality of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
All authors declare that they have no conflict of interest.
Ethical approval
This article did not require ethical approval of any kind.
Informed consent
This article is a meta-analysis and does not involve informed consent.
Human and animal rights'
This article does not contain human participants or animals.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Huang, X., Shao, X., Cheng, T. et al. Laparoscopic intraperitoneal onlay mesh (IPOM) with fascial repair (IPOM-plus) for ventral and incisional hernia: a systematic review and meta-analysis. Hernia 28, 385–400 (2024). https://doi.org/10.1007/s10029-024-02983-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10029-024-02983-4