Abstract
Background
The controversy surrounding Roux-en-Y (R-Y) and Billroth II with Braun (BII + B) reconstruction as an anti-bile reflux procedure after distal gastrectomy has persisted. Recent studies have demonstrated their efficacy, but the long-term outcomes and postoperative quality of life (QoL) among patients have yet to be evaluated. Therefore, we compared the short-term and long-term outcomes of the two procedures as well as QoL.
Methods
The clinical data of 151 patients who underwent total laparoscopic distal gastrectomy (TLDG) at the Gastrointestinal Surgery Department of the Second Hospital of Fujian Medical University from January 2016 to December 2019 were retrospectively analyzed. Of these, 57 cases with Roux-en-Y procedure (R-Y group) and 94 cases with Billroth II with Braun procedure were included (BII + B group). Operative and postoperative conditions, early and late complications, endoscopic outcomes at year 1 and year 3 after surgery, nutritional indicators, and quality of life scores at year 3 postoperatively were compared between the two groups.
Results
The R-Y group recorded a significantly longer operative time (194.65 ± 21.52 vs. 183.88 ± 18.02 min) and anastomotic time (36.96 ± 2.43 vs. 27.97 ± 3.74 min) compared to the BII + B group (p < 0.05). However, no other significant differences were observed in terms of perioperative variables, including blood loss (p > 0.05). Both groups showed comparable rates of early and late complications. Endoscopic findings indicated similar food residuals at years 1 and 3 post-surgery for both groups. The R-Y group had a lower occurrence of residual gastritis and bile reflux at year 1 and year 3 after surgery, with a statistically significant difference (p < 0.001). Reflux esophagitis was not significantly different between the R-Y and BII + B groups in year 1 after surgery (p = 0.820), but the R-Y group had a lower incidence than the BII + B group in year 3 after surgery (p = 0.023). Nutritional outcomes at 3 years after surgery did not differ significantly between the two groups (p > 0.05). Quality of life scores measured by the QLQ-C30 scale were not significantly different between the two groups. However, on the QLQ-STO22 scale, the reflux score was significantly lower in the R-Y group than in the BII + B group (0 [0, 0] vs. 5.56 [0, 11.11]) (p = 0.003). The rest of the scores were not significantly different (p > 0.05).
Conclusion
Both R-Y and B II + B reconstructions are equally safe and efficient for TLDG. Nevertheless, the R-Y reconstruction reduces the incidence of residual gastritis, bile reflux, and reflux esophagitis, as well as postoperative reflux symptoms, and provides a better quality of life for patients. R-Y reconstruction is superior to BII + B reconstruction for TLDG.
Similar content being viewed by others
Introduction
Quality of life (QoL) among gastric cancer patients post-surgery has become a major focus for surgeons [1]. Changes in digestive tract continuity often result in complications following distal gastrectomy, such as alkaline reflux gastritis, dumping syndrome, and delayed gastric emptying [2]. Among these complications, heartburn and abdominal pain caused by alkaline reflux gastritis heavily impact patient QoL [3]. Previously, the Billroth II procedure was reportedly accompanied by significant bile reflux [4]. The Roux-en-Y (R-Y) method has a relatively better long-term prognosis due to the superior anti-reflux effect [5]. Consequently, surgeons perform Braun anastomosis to reduce bile reflux after Billroth II. Nonetheless, earlier studies exhibited unsatisfactory outcomes [6].
Since the development and widespread use of laparoscopic distal gastrectomy (LDG), the oncologic safety and surgical security have been proven comparable to those of open surgery [7]. Currently, laparoscopic-assisted distal gastrectomy (LADG) remains the primary approach for LDG. However, with the advancement of laparoscopic techniques and linear staplers, attention has shifted toward total laparoscopic distal gastrectomy (TLDG). This minimally invasive procedure reduces postoperative pain, complications, and recovery period, in addition to enhancing the perioperative experience [8]. Nonetheless, TLDG must be performed by qualified and skilled surgeons to ensure a successful operation [9].
The R-Y and Billroth II with Braun (BII + B) reconstructions remain controversial as anti-biliary reflux procedures after distal gastrectomy. Both procedures have been compared in the literature, but most studies have emphasized short-term efficacy [10, 11]. Thus, this study compared the short- and long-term efficacy and QoL between R-Y and BII + B reconstructions.
Materials and methods
Participants
This retrospective study was conducted at the Gastrointestinal Surgery Department of the Second Affiliated Hospital of Fujian Medical University, spanning from January 2016 to December 2019. Data were collected from gastric cancer patients who underwent distal gastrectomy by a single surgical team. Patients who underwent open surgery, the Billroth I procedure, or extracorporeal anastomosis involving R-Y and BII+ B procedures were excluded from the study. In total, 176 patients underwent TLDG utilizing the R-Y and BII + B procedures (R-Y = 66, BII + B = 110). Inclusion criteria encompassed patients who underwent TLDG with R-Y and BII + B procedures and received postoperative pathological diagnoses falling within stages I to III. Exclusion criteria included combined resection, intraoperative conversion to open surgery, loss to follow-up, death, or distant tumor metastasis. The final analysis comprised 151 patients, categorized into the R-Y group (n = 57), and the BII + B group (n = 94) (refer to Fig. 1). The preference for the reconstructive method gradually shifted toward the R-Y procedure in 2019 due to severe bile reflux observed following BII + B procedure.
Surgical procedure
Gastrointestinal (GI) reconstruction after D2 lymph node dissection and distal gastrectomy.
Roux-en-Y reconstruction
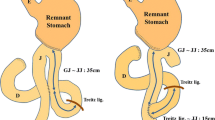
The jejunum was dissected 25 cm from the Treitz ligament. We performed a gastric-jejunal side-to-side anastomosis using a linear stapler and closed the common opening with manual sutures. Afterwards, a lateral jejuno-jejunal anastomosis was created 25 cm away from the gastrojejunal anastomosis (refer to Fig. 2).
BillrothII with Braun
A side-to-side gastrojejunal anastomosis was conducted 25 cm from the Treitz ligament, and the common gastrojejunal opening was closed using hand suturing. Additionally, a side-to-side jejuno-jejunal anastomosis was carried out 15 cm distal to the gastrojejunal anastomosis (refer to Fig. 3).
Observation indexes
Clinicopathological data and perioperative variables
Clinicopathological data:sex, age, BMI (body mass index), tumor location, tumor size, differentiation degree, neoadjuvant therapy, TNM stage, ASA score, and follow-up times. The tumor TNM staging was determined according to the 8th edition of the American Joint Committee on Cancer (AJCC) [12]. ASA score was assessed based on the American Society of Anesthesiologists Classification [13].
Perioperative variables were blood loss, anastomotic time, operation time, time to initial exhaust, time to initial liquid food, time to the removal of the abdominal drain, and postoperative hospital days.
Early complications
Obstruction, anastomotic bleeding, delayed gastric emptying, anastomosis leakage, anastomotic stricture, intra-abdominal bleeding, intra-abdominal abscess, pancreatic fistula, chylous leakage, wound morbidity, Roux stasis syndrome (RSS), and pneumonia. RSS is defined as follows: (1) postoperative symptoms of induced nausea, vomiting, and abdominal distension; (2) perfect imaging, endoscopy to exclude mechanical obstruction (anastomotic stricture), and imaging suggestive of intestinal obstruction are not included in RSS [14]. According to the Clavien-Dindo classification, early complications were graded [15].
Late complications
Dumping syndrome, anastomotic ulcer, anastomotic stricture, anastomotic ileus, and intra-abdominal hernia. Dumping syndrome is defined as palpitations, hot flashes, excessive sweating, and hypoglycemia after eating.
Endoscopic findings
Endoscopic results at 1 and 3 years postoperation. Evaluation of postoperative residue, gastritis, and bile reflux was performed according to the Kubo M endoscopic grading method [16]. Reflux esophagitis was assessed according to the Los Angeles Grading System [17].
Nutrition
Body mass index (BMI), hemoglobin, protein, and albumin to the preoperative ratio in the 3rd year of post-surgery.
Quality of life assessment (3rd year post-surgery)
Quality of life in the third year post-surgery was assessed using the Quality of Life Questionnaire-Core 30 (QLQ-C30) and the Stomach Cancer Specific Modular Scale (QLQ-STO22), both developed by the European Organization for Research and Cancer Treatment (EORTC). These evaluations were carried out through outpatient follow-ups or telephone interviews. The QLQ-C30 questionnaire, comprising 30 items, encompasses five functional scales (physical, role, cognitive, emotional, and social), three symptom scales (fatigue, pain, nausea, and vomiting), six individual items, and a Global Health Status and Quality of Life scale. On the other hand, the EORTC QLQ-STO22 includes 22 items distributed across five symptom scales (dysphagia, epigastric pain, reflux, eating restrictions, anxiety) and four individual items [18].
All scale scores were linearly transformed to 0–100 scores. Higher scores on the global health status and QoL scale and the five functional scales of the QLQ-C30 indicate a better quality of life, while elevated scores on the three symptom scales and six individual items suggest a poorer quality of life. In the STO22, higher scores indicate greater symptom severity, reflecting a lower quality of life [19].
Statistical analysis
Statistical analysis was conducted using SPSS 26.0 software in this study. Data with a normal distribution are presented as the mean ± standard deviation, and the t-test was employed for group comparisons. Skewed data are described as medians with 25th and 75th percentiles, and the Mann–Whitney U test was used for group comparisons. Categorical data were analyzed using the chi-square test or Fisher’s exact test. Rank data were compared using the nonparametric rank-sum test. Statistical significance was set at p < 0.05.
Results
Clinicopathological data and perioperative variables
Clinicopathological data from 151 patients, including sex, age, BMI, tumor location, tumor size, differentiation degree, neoadjuvant therapy, TNM stage, and ASA score, were collected for this study. These parameters were comparable between the R-Y and BII + B groups (p > 0.05). The R-Y group had a median follow-up time of 45 months (range 36–66), while the BII + B group had a median follow-up time of 59 months (range 44–72) (refer to Table 1).
In terms of perioperative variables, no significant difference in blood loss was observed between the groups. However, there were statistically significant disparities in operative time (R-Y 194.65 ± 21.52 vs. BII + B 183.88 ± 18.02) and anastomotic time (R-Y 36.96 ± 2.43 vs. BII + B 27.97 ± 3.74) between the R-Y and BII + B groups (p < 0.05). Meanwhile, there were no significant differences between the postoperative conditions of both groups in terms of time to initially exhaust, time to initial liquid food, time to remove the abdominal drain, and postoperative hospital days (p > 0.05) (refer to Table 1).
Early complications
The early complication rate was 10.5% in the R-Y group and 16.0% in the BII + B group. No significant difference was found between the two groups regarding the grade of complications (p > 0.05) (refer to Table 2).
Late complications
Late complications occurred in 10.5% of the R-Y group and 12.8% of the BII + B group, but the difference between the two groups was not statistically significant (p = 0.931) (refer to Table 3).
Endoscopy findings
There was no significant difference between both groups in terms of the endoscopic findings of food residues at years 1 and 3 (p > 0.05). Conversely, the occurrence of bile reflux and residual gastritis at years 1 and 3 was lower in the R-Y group than in the BII + B group (p < 0.001). Regarding reflux esophagitis, there was no significant difference between the groups in year 1, but in year 3, the R-Y group had a lower incidence compared to the BII + B group (p = 0.023) (refer to Fig. 4).
Comparison of endoscopic findings in the remnant stomach and reflux esophagitis at 1 and 3 years post-operation. Residue, gastritis, and bile reflux were graded using the RGB score system. Reflux esophagitis was classified according to the Los Angeles (LA) classification. The x-axis represents the percentage
Nutrition
The differences in BMI, hemoglobin, protein, and albumin to preoperative ratio at 3 years post-surgery were not statistically significant (p > 0.05) (refer to Table 4).
Quality of life assessment (3rd year post-surgery)
The differences between QLQ-C30 scores in all items were not found to be statistically significant (p > 0.05) (refer to Table 5). However, on the QLQ-STO22 scale, the R-Y group had a lower epigastric pain score than the BII + B group (0 [0,0] vs. 0 [0, 11.11]), although the difference was not statistically significant (p = 0.534). Additionally, the reflux score was significantly lower in the R-Y group than in the BII + B group (0 [0, 0] vs. 5.56 [0, 11.11]) (p = 0.003). The remaining items in the QLQ-STO22 did not show significant differences (p > 0.05) (refer to Table 6).
Discussion
Currently, TLDG has become a hot topic among surgeons. Ikeda O et al. [20] demonstrated that TLDG is associated with less invasiveness, reduced blood loss, smaller incisions, and a lower incidence of postoperative infections compared to LDG. In addition, Kanaya S et al. [21] reported the application of delta anastomosis, which facilitates the Billroth I procedure in TLDG. Although the reconstruction process of the R-Y is more complex, surgeons have made modifications to make it equally easy and safe in TLDG. Takaori K et al. [22] described the use of a linear stapler in isoperistaltic anastomosis R-Y reconstruction for TLDG. Okuno K et al. [23] proposed β-type R-Y reconstruction, which avoids the need for laparoscopic suturing.
Ideally, GI reconstruction after LDG should preserve residual gastric function, minimize long-term complications, and enhance the postoperative quality of life over the long term. The typical reconstruction involves Billroth I, Billroth II, and R-Y procedures. Billroth I procedure has the advantage of food passage in the duodenal pathway, but the risk of anastomotic fistula may be higher when the residual stomach is small; thus, this method is suitable for early-stage gastric patients [24]. In China, progressive gastric cancer is more common, and as a result, Billroth II and R-Y reconstructions more frequently performed. Billroth II reconstruction has the advantage of low tension but increases the risk of bile reflux gastritis and reflux esophagitis [25]. As a result, Braun made an anastomosis between the efferent and afferent loop at 10–15 cm from the gastrojejunal anastomosis based on Billroth II in 1892, effectively diverting partial bile and pancreatic fluid [26]. Nevertheless, this method has limitations, where studies still detected bile reflux and residual gastritis postsurgery [27]. In contrast, the R-Y method has the advantage of low-tension anastomosis. The long R-Y limb between the gastrojejunal and jejunojejunal anastomosis is beneficial for anti-bile reflux [4]. Nevertheless, previous studies indicated that RSS is often associated with nausea and vomiting post-surgery, possibly due to the disruption of intestinal electrophysiological continuity, thus affecting the patient’s QoL [28].
Surgical safety is a priority for surgeons when deciding the best reconstruction method. This study’s findings suggested that the R-Y group had significantly longer operative and anastomosis times compared to the BII + B group. Meanwhile, there was no significant difference in blood loss or postoperative recovery between the groups, which was consistent with studies by Chi F and Cui LH [11, 29]. R-Y procedure mesentery separation and jejunum dissection did not increase the risk of bleeding but prolonged the operative time. In addition, Yalikun A reported no significant difference in early postoperative complications between the R-Y (14.7%) and BII + B (7.5%) groups, which is similar to Shishegar A’s findings [30, 31]. In the present study, no significant differences were observed in the incidence of early complications (R-Y 10.5 vs. BII + B 16.0%) or late complications (R-Y 10.5 vs. BII + B 12.8%) between the two groups. Therefore, the safety of both procedures was comparable for TLDG.
RSS symptoms include stomach discomfort, bloating, and vomiting and are caused by delayed emptying in nonmechanical obstruction after the R-Y procedure, with an incidence rate of 10 to 30% [32]. The mechanism may be related to intestinal interruption, resulting in slow waves emitted by the “Y” limb that caused the limb to move retrogradely toward gastric motility [28].
However, the advancement of anastomotic devices and the modification of the traditional R-Y reconstruction by some surgeons in recent studies have significantly decreased the incidence of RSS. Gustavsson S demonstrated that an excessively long R-Y limb is a risk factor for RSS [14]. Motoyama K and An JY controlled the length of the “R-Y limb” to 25–30 cm, and none experienced RSS postoperatively [33, 34]. Additionally, our study utilized isoperistaltic R-Y reconstruction, which aligns more closely with human physiology and facilitates food emptying compared to antiperistaltic anastomosis [35]. Only one patient experienced RSS (1.8%), which was significantly lower than that in previous reports. Therefore, it was postulated that the 25-cm R-Y limb and the isoperistaltic gastrojejunal anastomosis potentially reduced RSS incidence.
Alkaline reflux gastritis caused by bile reflux is a significant factor that impacts the patient’s postoperative life [36]. Refluxed bile damage to the residual gastric mucosa results in residual gastritis, reflux esophagitis, and an increased risk of esophageal and residual gastric cancer [37, 38]. However, the effectiveness of the R-Y and BII + B procedures in preventing bile reflux remains controversial. Lee MS and Park JY reported that endoscopic findings a year after surgery exhibited significantly higher bile reflux and a higher degree of residual gastritis in the BII + B group than in the R-Y group [39, 40]. In contrast, Yalikun A indicated that a modified BII + B reconstruction with prolonged afferent and efferent loops had postoperative bile reflux and residual gastritis comparable to R-Y reconstruction but may increase the risk of afferent limb torsion and internal hernia [40].
In the current study, the endoscopic findings at years 1 and 3 post-surgery revealed significantly lower levels of residual gastritis and occurrences of bile reflux in the R-Y group compared to the BII + B group. The superiority of R-Y reconstruction in terms of anti-reflux effects can be attributed to several factors. First, the Billroth II gastrojejunal anastomosis lacks anti-reflux properties, allowing bile from the afferent loop to flow into the residual stomach along with intestinal peristalsis. Second, even with the Braun procedure diverting bile, some bile may still reflux to the residual stomach since the Braun anastomosis is positioned only 10–15 cm away from the gastrojejunostomy. In contrast, R-Y reconstruction anastomoses the proximal jejunum with the distal jejunum, preventing the direct flow of bile into the remaining stomach. Finally, the long and steep limb between the gastrojejunal and jejunojejunal anastomosis in R-Y reconstruction makes bile reflux into the residual stomach difficult.
Chung JH’s endoscopic findings at 6–32 months demonstrated that the proportion of grade 2 and 3 residual gastritis increased from 73.0 to 86.1% in the BII + B group, and the incidence of reflux esophagitis rose from 1 to 15.7% [41]. Similarly, Choi C’s endoscopic findings at year 2 postoperatively showed increased bile reflux and an aggravated degree of residual gastritis in the BII + B group compared to year 1, with significantly higher reflux esophagitis compared to the R-Y group [42]. In the current study, the proportion of grade 2 and 3 residual gastritis increased in the BII + B group at year 3 postoperatively by 86.2% compared with 74.5% at year 1. Conversely, there was no significant change in the R-Y group. Furthermore, there was no significant difference in the degree of reflux esophagitis between the two groups in year 1, but in year 3, the occurrence was significantly lower in the R-Y group than in the BII + B group (p = 0.023). These findings suggest that the degree of residual gastritis and reflux esophagitis due to bile reflux may worsen over time, indicating that the R-Y group has a better long-term prognosis.
Moreover, when the residual stomach is smaller, the distance between the gastrojejunal anastomosis and the cardia is reduced. This shortened distance increases the likelihood of bile damaging the esophageal mucosa, leading to reflux esophagitis. Therefore, the R-Y method is advantageous when the patient’s residual stomach is small. Additionally, the two groups had no significant differences in BMI, hemoglobin, protein, or albumin to the preoperative ratio at year 3 post-surgery. Likewise, Lee MS and Park JY also reported similar results [39, 40].
Gastric surgery alters digestive structure and function, leading to post-gastrectomy symptoms such as restricted eating, appetite loss, and reflux, significantly impacting long-term quality of life. Lee MS’s study suggested that R-Y procedure reduces bile reflux, but at 6 and 12 months post-surgery, the Gastrointestinal Quality of Life Index scores, including symptoms, physical, emotional, and social functions, showed no significant difference compared to Billroth I and BII + B methods [39]. Cui L compared R-Y and BII + B groups at 6 months post-surgery and found no significant differences in gastrointestinal symptom scores [29]. However, Chan DC et al. indicated that R-Y reconstruction can reduce bile reflux-related abdominal pain and heartburn, enhancing quality of life after surgery [43].
The combined use of EORTC QLQ-30 and STO22 questionnaires allows a comprehensive evaluation of post-gastrectomy Qol from physical, and mental health, and specific gastric cancer-related symptoms. Smolskas E’s study revealed no significant differences in QLQ-30 scores 1 year after surgery among the Billroth I, Billroth II, and R-Y groups. However, specific gastric cancer symptoms were not assessed using STO22 [44]. Yang K’s research demonstrated that R-Y reconstruction reduces reflux, leading to a better long-term quality of life compared to Billroth I [45]. This study’s results indicate that 3 years after surgery, R-Y and BII + B groups show no significant differences in the QLQ-30 scales. However, in the STO22 scale, the R-Y group had lower scores for epigastric pain and reflux symptoms compared to the BII_B group, indicating a better postoperative quality of life.
However, this study has limitations. It is a single-center retrospective study with small sample size. Preoperative QOL was not assessed, making it impossible to establish a baseline. Additionally, postoperative QoL was evaluated at a single time point, which does not capture the dynamic changes in QoL over time. Future research will involve large-scale, multicenter prospective studies to address these limitations. Furthermore, we have collated findings from prior studies focusing on surgical and endoscopic outcomes, nutrition, and quality of life, to offer a comparative perspective with the results of our current research (refer to Table 7).
Conclusion
The anastomotic time of R-Y reconstruction in TLDG is longer than that of BII + B reconstruction. However, there is no increased risk of bleeding associated with R-Y reconstruction. Postoperative recovery and surgical safety were comparable in both groups. Nonetheless, R-Y reconstruction exhibits a superior anti-biliary reflux effect, reducing residual gastritis and reflux esophagitis in comparison to BII + B reconstruction. Furthermore, R-Y reconstruction diminishes postoperative reflux symptoms and enhances the QoL. Both procedures demonstrate safety and feasibility, but the R-Y surpasses the BII + B procedure for TLDG. Future prospective studies should be conducted involving multiple centers and a larger sample size to further validate the results of this study.
Availability of data and materials
The original anonymous dataset is available on request from the corresponding author at e5179518qihe9323@163.com.
Abbreviations
- QoL:
-
Quality of Life
- R-Y:
-
Roux-en-Y
- LDG:
-
Laparoscopic distal gastrectomy
- LADG:
-
Laparoscopic-assisted distal gastrectomy
- TLDG:
-
Total laparoscopic distal gastrectomy
- BII + B:
-
Billroth II with Braun
- BMI:
-
Body mass index
- RSS:
-
Roux stasis syndrome
References
Wang FH, Zhang XT, Li YF, Tang L, Qu XJ, Ying JE, Zhang J, Sun LY, Lin RB, Qiu H, et al. The Chinese Society of Clinical Oncology (CSCO): clinical guidelines for the diagnosis and treatment of gastric cancer, 2021. Cancer Commun (Lond). 2021;41:747–95.
Wang Q, Ni Q, Yang K, Ji S, Fan Y, Wang C, Zhang W, Yan S, Ma Q, Wei Q, et al. Laparoscopic uncut Roux-en-Y for radical distal gastrectomy: the study protocol for a multirandomized controlled trial. Cancer Manag Res. 2019;11:1697–704.
Ritchie WP Jr. Alkaline reflux gastritis. An objective assessment of its diagnosis and treatment. Ann Surg. 1980;192:288–98.
Kojima K, Yamada H, Inokuchi M, Kawano T, Sugihara K. A comparison of Roux-en-Y and Billroth-I reconstruction after laparoscopy-assisted distal gastrectomy. Ann Surg. 2008;247:962–7.
Hoya Y, Mitsumori N, Yanaga K. The advantages and disadvantages of a Roux-en-Y reconstruction after a distal gastrectomy for gastric cancer. Surg Today. 2009;39:647–51.
Vogel SB, Drane WE, Woodward ER. Clinical and radionuclide evaluation of bile diversion by Braun enteroenterostomy: prevention and treatment of alkaline reflux gastritis. An alternative to Roux-en-Y diversion. Ann Surg. 1994;219:458–65 discussion 465-456.
Huang C, Liu H, Hu Y, Sun Y, Su X, Cao H, Hu J, Wang K, Suo J, Tao K, et al. Laparoscopic vs open distal gastrectomy for locally advanced gastric cancer: five-year outcomes from the CLASS-01 randomized clinical trial. JAMA Surg. 2022;157:9–17.
Jin HE, Kim MS, Lee CM, Park JH, Choi CI, Lee HH, Min JS, Jee YS, Oh J, Chae H, et al. Meta-analysis and systematic review on laparoscopic-assisted distal gastrectomy (LADG) and totally laparoscopic distal gastrectomy (TLDG) for gastric cancer: preliminary study for a multicenter prospective KLASS07 trial. Eur J Surg Oncol. 2019;45:2231–40.
Tang T, Peng W, Zhang L, Zuo Z, Cao D, Huang J, Duan L. Effectiveness and safety of total laparoscopic distal gastrectomy versus laparoscopy-assisted distal gastrectomy for gastric cancer: a retrospective cohort study. Am J Surg. 2018;216:528–33.
Shim JH, Oh SI, Yoo HM, Jeon HM, Park CH, Song KY. Roux-en-Y gastrojejunostomy after totally laparoscopic distal gastrectomy: comparison with Billorth II reconstruction. Surg Laparosc Endosc Percutan Tech. 2014;24:448–51.
Chi F, Lan Y, Bi T, Zhou S. Billroth-II with Braun versus Roux-en-Y reconstruction in totally laparoscopic distal gastrectomy for gastric cancer. Wideochir Inne Tech Maloinwazyjne. 2021;16:664–8.
Liao X, Zhang D. The 8th Edition American Joint Committee on cancer staging for hepato-pancreato-biliary cancer: a review and update. Arch Pathol Lab Med. 2021;145:543–53.
Horvath B, Kloesel B, Todd MM, Cole DJ, Prielipp RC. The evolution, current value, and future of the American Society of Anesthesiologists Physical Status Classification System. Anesthesiology. 2021;135:904–19.
Gustavsson S, Ilstrup DM, Morrison P, Kelly KA. Roux-Y stasis syndrome after gastrectomy. Am J Surg. 1988;155:490–4.
Rassweiler JJ, Rassweiler MC, Michel MS. Classification of complications: is the Clavien-Dindo classification the gold standard? Eur Urol. 2012;62:256–8 discussion 259-260.
Kubo M, Sasako M, Gotoda T, Ono H, Fujishiro M, Saito D, Sano T, Katai H. Endoscopic evaluation of the remnant stomach after gastrectomy: proposal for a new classification. Gastric Cancer. 2002;5:83–9.
Armstrong D, Bennett JR, Blum AL, Dent J, De Dombal FT, Galmiche JP, Lundell L, Margulies M, Richter JE, Spechler SJ, et al. The endoscopic assessment of esophagitis: a progress report on observer agreement. Gastroenterology. 1996;111:85–92.
Aaronson NK, Ahmedzai S, Bergman B, Bullinger M, Cull A, Duez NJ, Filiberti A, Flechtner H, Fleishman SB, de Haes JC, et al. The European Organization for Research and Treatment of cancer QLQ-C30: a quality-of-life instrument for use in international clinical trials in oncology. J Natl Cancer Inst. 1993;85:365–76.
Vickery CW, Blazeby JM, Conroy T, Arraras J, Sezer O, Koller M, Rosemeyer D, Johnson CD, Alderson D. Development of an EORTC disease-specific quality of life module for use in patients with gastric cancer. Eur J Cancer. 2001;37:966–71.
Ikeda O, Sakaguchi Y, Aoki Y, Harimoto N, Taomoto J, Masuda T, Ohga T, Adachi E, Toh Y, Okamura T, Baba H. Advantages of totally laparoscopic distal gastrectomy over laparoscopically assisted distal gastrectomy for gastric cancer. Surg Endosc. 2009;23:2374–9.
Kanaya S, Kawamura Y, Kawada H, Iwasaki H, Gomi T, Satoh S, Uyama I. The delta-shaped anastomosis in laparoscopic distal gastrectomy: analysis of the initial 100 consecutive procedures of intracorporeal gastroduodenostomy. Gastric Cancer. 2011;14:365–71.
Takaori K, Nomura E, Mabuchi H, Lee SW, Agui T, Miyamoto Y, Iwamoto M, Watanabe H, Tanigawa N. A secure technique of intracorporeal Roux-Y reconstruction after laparoscopic distal gastrectomy. Am J Surg. 2005;189:178–83.
Okuno K, Nakagawa M, Kojima K, Kanemoto E, Gokita K, Tanioka T, Inokuchi M. Long-term functional outcomes of Roux-en-Y versus Billroth I reconstructions after laparoscopic distal gastrectomy for gastric cancer: a propensity-score matching analysis. Surg Endosc. 2018;32:4465–71.
Ren Z, Wang WX. Comparison of Billroth I, Billroth II, and Roux-en-Y reconstruction after totally laparoscopic distal gastrectomy: a randomized controlled study. Adv Ther. 2019;36:2997–3006.
Csendes A, Burgos AM, Smok G, Burdiles P, Braghetto I, Díaz JC. Latest results (12–21 years) of a prospective randomized study comparing Billroth II and Roux-en-Y anastomosis after a partial gastrectomy plus vagotomy in patients with duodenal ulcers. Ann Surg. 2009;249:189–94.
Huang MQ, Li M, Mao JY, Tian BL. Braun enteroenterostomy reduces delayed gastric emptying: a systematic review and meta-analysis. Int J Surg. 2015;23:75–81.
Yan Y, Wang D, Liu Y, Lu L, Wang X, Zhao Z, Li C, Liu J, Li W, Fu W. Optimal reconstruction after laparoscopic distal gastrectomy: a single-center retrospective study. Cancer Control. 2022;29:10732748221087059.
Herbella FA, Silva LC, Vicentine FP, Patti MG. Roux-en-Y limb motility after total gastrectomy. J Gastrointest Surg. 2014;18:906–10.
Cui LH, Son SY, Shin HJ, Byun C, Hur H, Han SU, Cho YK. Billroth II with Braun enteroenterostomy is a good alternative reconstruction to Roux-en-Y Gastrojejunostomy in laparoscopic distal gastrectomy. Gastroenterol Res Pract. 2017;2017:1803851.
Yalikun A, Aikemu B, Li S, Zhang T, Ma J, Zheng M, Zang L. A modified Billroth-II with Braun anastomosis in totally laparoscopic distal gastrectomy: initial experience compared with Roux-en-Y anastomosis. Ann Surg Oncol. 2022;29:2359–67.
Shishegar A, Vahedi M, Kamani F, Kazerouni MF, Pasha MA, Fathi F. Comparison between Roux-en-Y gastrojejunostomy and Billroth-II with Braun anastomosis following partial gastrectomy: a randomized controlled trial. Ann Med Surg (Lond). 2022;76:103544.
Woodward A, Sillin LF, Bortoff A. Migrating myoelectric complex and jejunal slow-wave propagation after Roux gastrectomy in dogs. Dig Dis Sci. 1993;38:1073–8.
Motoyama K, Kojima K, Hayashi M, Kato K, Inokuchi M, Sugihara K. β-Shaped intracorporeal Roux-en-Y reconstruction after totally laparoscopic distal gastrectomy. Gastric Cancer. 2014;17:588–93.
An JY, Cho I, Choi YY, Kim YM, Noh SH. Totally laparoscopic Roux-en-Y gastrojejunostomy after laparoscopic distal gastrectomy: analysis of initial 50 consecutive cases of single surgeon in comparison with totally laparoscopic Billroth I reconstruction. Yonsei Med J. 2014;55:162–9.
Lee Y, Lee CM, Park S, Kim JH, Park SH. Comparison of the clinical outcomes between isoperistaltic and antiperistaltic anastomoses after laparoscopic distal gastrectomy for patients with gastric cancer. Front Oncol. 2020;10:1237.
Zobolas B, Sakorafas GH, Kouroukli I, Glynatsis M, Peros G, Bramis J. Alkaline reflux gastritis: early and late results of surgery. World J Surg. 2006;30:1043–9.
Ohira M, Toyokawa T, Sakurai K, Kubo N, Tanaka H, Muguruma K, Yashiro M, Onoda N, Hirakawa K. Current status in remnant gastric cancer after distal gastrectomy. World J Gastroenterol. 2016;22:2424–33.
Greene CL, Worrell SG, DeMeester TR. Rat reflux model of esophageal cancer and its implication in human disease. Ann Surg. 2015;262:910–24.
Lee MS, Ahn SH, Lee JH, Park DJ, Lee HJ, Kim HH, Yang HK, Kim N, Lee WW. What is the best reconstruction method after distal gastrectomy for gastric cancer? Surg Endosc. 2012;26:1539–47.
Park JY, Kim YJ. Uncut Roux-en-Y reconstruction after laparoscopic distal gastrectomy can be a favorable method in terms of gastritis, bile reflux, and gastric residue. J Gastric Cancer. 2014;14:229–37.
Chung JH, Im DW, Choi CW, Kim SJ, Hwang SH, Lee SH. A 3-year follow-up study of uncut Roux-en-Y reconstruction: clinical results and outcomes. Surg Endosc. 2022;36:7588–96.
In Choi C, Baek DH, Lee SH, Hwang SH, Kim DH, Kim KH, Jeon TY, Kim DH. Comparison between Billroth-II with Braun and Roux-en-Y reconstruction after laparoscopic distal gastrectomy. J Gastrointest Surg. 2016;20:1083–90.
Chan DC, Fan YM, Lin CK, Chen CJ, Chen CY, Chao YC. Roux-en-Y reconstruction after distal gastrectomy to reduce enterogastric reflux and helicobacter pylori infection. J Gastrointest Surg. 2007;11:1732–40.
Smolskas E, Lunevicius R, Samalavicius NE. Quality of life after subtotal gastrectomy for gastric cancer: does restoration method matter? - a retrospective cohort study. Ann Med Surg (Lond). 2015;4:371–5.
Yang K, Zhang W, Chen Z, Chen X, Liu K, Zhao L, Hu J. Comparison of long-term quality of life between Billroth-I and Roux-en-Y anastomosis after distal gastrectomy for gastric cancer: a randomized controlled trial. Chin Med J (Engl). 2023;136:1074–81.
Acknowledgements
Not applicable.
Funding
Supported by Key Clinical Specialty Discipline Construction Program of Fujian, PRC (Fujian Health Medicine and Politics [2022]884).
Author information
Authors and Affiliations
Contributions
Writing—Original Draft: Yan-xin Chen. Acquisition of Data: Qiao-zhen Huang, Peng-cheng Wang. Analysis and Interpretation: Yue-Jia Zhu, Li-quan Chen, Chu-ying Wu, Jin-tian Wang, Jun-xing Chen. Study Concept and Design: Kai Ye. All authors have read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethics approval and consent to participate
This study was approved by the Ethics Committee of the Second Hospital of Fujian Medical University ((2023) Ethical Examination No. (23) of the Second Hospital of Fujian Medical University). The patients’ and their families’ consent was obtained before the study.
Consent for publication
All the authors have consented to publication.
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/. The Creative Commons Public Domain Dedication waiver (http://creativecommons.org/publicdomain/zero/1.0/) applies to the data made available in this article, unless otherwise stated in a credit line to the data.
About this article
Cite this article
Chen, Yx., Huang, Qz., Wang, Pc. et al. Short- and long-term outcomes of Roux-en-Y and Billroth II with Braun reconstruction in total laparoscopic distal gastrectomy: a retrospective analysis. World J Surg Onc 21, 361 (2023). https://doi.org/10.1186/s12957-023-03249-6
Received:
Accepted:
Published:
DOI: https://doi.org/10.1186/s12957-023-03249-6