Abstract
A novel class of oral glucose lowering drugs, sodium-glucose co-transporter type 2 inhibitors (SGLT2is), has shown additional beneficial effects on body weight, serum uric acid levels, blood pressure, and cardiac and renal function. Conflicting data have been published regarding the potential risk of acute kidney injury (AKI) when using SGLT2is. Aim of this manuscript was to review the current literature on this issue. SGLT2is induce a mild acute decline in estimated glomerular filtration rate, attributed to the effect of proximal tubular natriuresis on tubuloglomerular feedback through increased macula densa sodium delivery, leading to afferent arteriole vasoconstriction and reduced intraglomerular pressure. This functional effect with a subsequent rise in serum creatinine fulfills the creatinine-based criteria for AKI, as defined in clinical practice and trial settings. Other proposed potential mechanisms as to how SGLT2is lead to AKI include osmotic diuresis leading to volume depletion, increased urinary uric acid levels, intratubular oxidative stress, local inflammation and tubular injury. Despite the warning published by the US Food and Drug Administration in 2016 about a potential risk of AKI and the report of some clinical cases of AKI after treatment with SGLT2is, large observational real-life retrospective studies, randomized controlled trials and propensity-matched analyses of data from clinical practice unambiguously demonstrate that SGLT2is are safe for the kidney and do not predispose to AKI. In conclusion, while we can probably stop worrying about AKI risk when using SGLT2is, the question whether these agents should be withheld in the presence of clinical situations at high risk for AKI remains unaddressed.
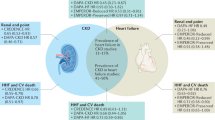
Graphical abstract

Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Diabetes mellitus (DM) is among the most common chronic conditions globally, affecting approximately 10% of the adult population with significant long-term micro- and macro-vascular complications. Diabetic nephropathy is the most common cause of chronic kidney disease (CKD), a condition listed among the top ten causes of annual mortality [1, 2]. Although angiotensin converting enzyme inhibitors (ACEis) and angiotensin receptor blockers (ARBs) have been shown to be protective against the progression of diabetic kidney disease and albuminuria, this condition still causes significant morbidity and mortality, thus requiring proper management and therapeutic alternatives [3, 4]. A novel class of oral glucose lowering drugs, sodium-glucose co-transporter type 2 inhibitors (SGLT2is), has shown additional multiple beneficial effects [5,6,7]. Conflicting data have been published regarding the potential risk of acute kidney injury (AKI) when using SGLT2is [8, 9]. The US Food and Drug Administration (FDA) reported 101 cases of AKI in patients using SGLT2is [5]. Unfortunately, this report seems vague on AKI diagnostic tools and does not provide sufficient information, thus creating a debate. The aim of this review was to evaluate the association between AKI and SGLT2i therapy and its potential pathophysiological mechanisms.
Literature search strategy
Literature search was performed according to the guidelines of the Preferred Reporting Items for Systematic Review and Meta-Analyses (PRISMA). It was performed in March 2022 on the PubMed/Medline, Web of Science, Scopus, Cochrane Library, and CINAHL databases by utilizing the listed terms or their combinations: “acute kidney injury”, “acute kidney failure”, “acute renal failure”, “nephrotoxicity”, “sodium-glucose co-transporter type 2 inhibitors”, “SGLT-2”, “SGLT-2 inhibitors”, “canagliflozin”, “dapagliflozin”, “empagliflozin”, “diabetes”, “diabetes mellitus”, “anti-diabetic drugs”, “eGFR”, and “estimated glomerular filtration rate”. We screened the abstracts and titles of the studies that were identified through the search platforms mentioned above. References of the reviews and studies were additionally screened for relevant publications. The selected studies were further investigated in full text for relevance of the specified criteria. After the preliminary selection, full texts of the selected studies were independently evaluated by two of the authors (SC and AY) (Fig. 1).
Review of the literature
Table 1 shows the 22 studies in which the risk of AKI when using SGLT2is was analyzed: 10 were retrospective cohort studies [6,7,8,9,10,11,12,13,14,15]: among them, SGLT2i users were compared with non-SGLT2i users [12, 13, 15], with dipeptidyl-peptidase-4 inhibitor (DPP-4i) users [6,7,8, 10, 11, 14], oral glucose lowering drug users [9] and GLP-1 receptor agonist (GLP-1RA) users [8]. Follow-up periods for renal adverse effects or AKI incidence varied from 6 [8, 14] to 33 months [9] with a median of 19 months [11, 13]. Most of the cohort studies indicated no relationship between SGLT2i use and AKI incidence [6, 9, 13,14,15]. Lin et al. [13] also showed a statistically significant lower incidence of estimated glomerular filtration rate (eGFR) decline as reported in two other cohorts [7, 12]. Results from several studies showed a decline in adverse renal events [11] and risk for AKI with respect to their comparators [7, 8, 10]; interestingly Zhuo et al. [8] showed a decreased risk of AKI in SGLT2i users when compared to both DPP-4i and GLP-1RA users.
Seven randomized controlled trials (RCTs) are also included in Table 1: 5 were double-blinded randomized placebo-controlled trials [16,17,18,19,20], 1 was a single-blinded randomized placebo-controlled trial [21], 1 was a phase 3 placebo-controlled trial [22]. Follow-up period ranged from 24 [22] to 50 months [16], with a median of 31.5 months [20]. Four studies showed no link between SGLT2i use and AKI incidence compared to placebo [18,19,20,21], whereas, interestingly, Cahn et al. showed a decrease in AKI with the use of SGLT2is compared to placebo [16]. Additionally, studies reported fewer serious renal adverse events [22], decreased risk of end-stage kidney disease (ESKD) [17] and statistically significant slower progression of kidney failure [19].
Three meta-analyses [23,24,25] and 2 database analyses [26, 27] are also included in Table 1: SGLT2is were compared with placebo [23], non-SGLT2is [26, 27] or not defined [24, 25]. Results showed no association of AKI with SGLT2i use [23, 26], decrease in AKI incidence [24, 25], increasing AKI incidence [27]. These different data make it harder to interpret results and to provide precise management plans. Interestingly, Katsuhara et al. pointed out that AKI incidence was reduced with the concomitant use of ACEis or ARBs [27].
AKI risk factors in SGLT2i use are summarized in Table 2: while no additional AKI risk due to the concomitant use of ARBs or ACEis with SGLT2is was reported by Rampersad et al. [9], Pasternak et al. [11] and Katsuhara et al. [27] reported a reduction in the risk of AKI by the concomitant use of ARBs or ACEis with SGLT2is. AKI risk with SGLT2i monotherapy was found to be 0.97, whereas it was 1.19 with the concomitant use of ACEis or ARBs [10]. Similarly, Lee et al. reported a statistically significant increase in the risk of AKI with the concomitant use of ACEis (1.5 vs. 2.2) [7].The concomitant use of non-steroidal anti-inflammatory drugs (NSAIDs) and SGLT2is was reported to not increase AKI risk by Pasternak et al. [11]. Contrarily, concerns regarding the concomitant use of NSAIDs and SGLT2is were reported by Heyman et al.: their study suggested that the possible explanation for this effect could be that SGLT2is could lead to dehydration caused by osmotic diuresis and natriuresis, especially in patients treated with diuretics. It was also proposed that SGLT2is could cause an intensification of renal parenchymal hypoxia and hypoxic kidney injury. Therefore, these authors proposed avoiding the concomitant administration of NSAIDs that could lead to iatrogenic hypoxic medullary injury [28]. Furthermore, no AKI risk due to the concomitant use of SGLT2is and diuretics was found in the study by Pasternak et al. [11] or in the study by Rampersad et al. [9]. On the contrary, Iskander et al. found that the AKI risk was 0.85 without any diuretic use and 2.01 with the concomitant use of a diuretic [10]. Similarly, the AKI risk was 1.4 without any diuretic use and 6.6 with the concomitant diuretic use in the study by Lee et al. [7]. Miyoshi et al. reported that the initial decrease in eGFR was statistically significantly smaller in patients who discontinued diuretics compared with those who continued them (P = 0.004) [12].
AKI risk was shown to be higher with increasing age: incidence rates of 4.2, 5.4, and 9.3 cases per 1000 person-years were reported in age groups < 65, 65 to 75, and > 75 years, respectively (P < 0.0001) [16]. Perkovic et al. reported that SGLT2is were protective at the baseline urinary albumin-to-creatinine ratio (UACR) > 1000 mg/g; SGLT2is had no beneficial effects when the baseline UACR was ≤ 1000 mg/g [20]. AKI risk in patients aged < 80 years was 1.04% and 1.84% in patients aged ≥ 80 years in the study by Iskander et al. [10]. McMurray et al. similarly reported a slight increase in the AKI risk when comparing < 65 years with ≥ 65 years of age: 15.7 vs. 16.7 [29]. The studies by Heerspink et al. [17] and Pasternak et al. [11] found that SGLT2i were protective in all age groups. Lastly, Lee et al. showed a gender difference, i.e., AKI risk rate lower in female than in male patients (2.18 vs. 3.56%) [7].
Temporarily withholding SGLT2is along with diuretics, metformin, NSAIDs, and renin–angiotensin–aldosterone system (RAAS) blocking agents under conditions of intercurrent illness, or procedures involving contrast materials is a reasonable approach given the minimal clinical downside to discontinuing these agents for a few days until the patient is back to his/her baseline state [30]. Figure 2 summarizes the AKI risk factors when using SGLT2is, the pathophysiological mechanisms through which AKI could occur and the measures that should be taken to prevent AKI occurrence. Prevention methods shown in Fig. 2 are based on the recommendations of the best clinical practice; it must be acknowledged that clinical studies demonstrating the effectiveness of such actions are lacking.
Risk factors for acute kidney injury (AKI) related to SGLT2is and associated conditions/medications. RAAS renin–angiotensin–aldosterone system, ACEis angiotensin converting enzyme inhibitors, ARBs angiotensin II receptor blockers, NSAIDs non-steroidal anti-inflammatory drugs, SBP systolic blood pressure. (Same numbered points in different columns indicate the same entity)
Do SGLT2is predispose to AKI?
In healthy individuals the glucose filtered from the glomeruli is reabsorbed by SGLT2 located at the S1 segment of the proximal tubules (80–90%) and by SGLT1 located at the S2–S3 segment of the proximal tubules (the remaining 10–20% of the filtered glucose) [30] (Fig. 3). In contrast to the wider distribution of SGLT1 in the human body, SGLT2 is found in the cerebellum and α-cells of pancreatic Langerhans islets as well as in the proximal kidney tubules [31].
Blockage of diabetes mellitus-induced hyperfiltration by SGLT2is. The decreased sodium (Na) and glucose (G) absorption through SGLT2is increases the amount of Na and chloride (Cl) delivered to macula densa. Via tubuloglomerular feedback, afferent arterioles are constricted and glomerular filtration rate (GFR) is decreased. SGLT2is also block sodium-hydrogen transporter (NHE3) and Na reabsorption
SGLT2is have been shown to reduce the progression of kidney failure by lowering glycated hemoglobin, blood pressure, body weight, and albuminuria [21, 32, 33]. The large urinary loss of glucose and sodium caused by SGLT2 transporter blockage raises the risk of hyperosmolarity and dehydration. Urine glucose may also be reabsorbed in exchange for uric acid by the glucose transporter GLUT9b, which is found in the apical membrane of proximal tubular cells. This exchange causes a 5–10% drop in serum uric acid levels, as well as increased uricosuria. A decrease in serum uric acid levels results in a decrease in systemic and glomerular hypertension in experimental animals, suggesting a relationship between uricosuria and the blood pressure lowering actions of SGLT2is [34]. On the other hand, an increase in urinary uric acid levels may be a risk factor for AKI via crystal-dependent and crystal-independent pathways. While uricosuria is a well-known cause of acute tumor lysis syndrome, evidence suggests that it may also play a role in other types of AKI, such as that caused by radiocontrast agents, rhabdomyolysis, heat stress, and, most importantly, dehydration, which is recognized as a possible cause of AKI when using SGLT2is [35]. As a result, transport of high amounts of glucose through the tubule may activate the osmolarity-sensitive gene encoding aldose reductase. Aldose reductase induction results in the production of sorbitol and fructose. Fructose is metabolized by fructokinase, which is abundant in the S3 segment, resulting in the production of uric acid, oxidative stress, release of chemokines, local tubular injury and inflammation. Furthermore, experimental models showed that this route can produce endogenous fructose in the renal cortex in type 1 DM, heat stress, or dehydration, and that it may partially cause renal damage in these conditions [34, 36] (Fig. 1).
Additionally, other intracellular organic osmolytes, such as myo-inositol and taurine are depleted at the same time in which sorbitol and fructose accumulate within the tubular cells. As a result, it could be speculated that SGLT2is may lead to tubular damage. Szelat et al. emphasized that using SGLT2i and RAAS blockers together results in a greater drop in trans-glomerular pressure, and that taking drugs like NSAIDs or radiocontrast agents together with SGLT2is can cause renal medullary hypoxic damage, which may lead to AKI [37].
SGLT2 reabsorbs glucose and sodium, which results in a reduced concentration of sodium and chloride in the tubular fluid reaching the macula densa, specialized epithelial cells located at the end of the thick ascending limb of Henle (Fig. 3). This leads to an increase in eGFR via tubuloglomerular feedback mechanisms involving the dilatation of afferent arterioles [38, 39]. On the contrary, SGLT2is induce a mild acute decline in eGFR, attributed to the effect of proximal tubular natriuresis on tubuloglomerular feedback through increased macula densa sodium delivery, leading to afferent arteriole vasoconstriction and reduced intraglomerular pressure [38, 39] (Fig. 3). Additionally, SGLT2is have also been linked to the inhibition of sodium reabsorption at the level of the proximal tubules via sodium-hydrogen transporter referred to as NHE3 (Fig. 3) [40]. Moreover, the higher amounts of electrolytes and glucose reaching the distal tubules lead to an increase in fluid volume of the distal tubule and thus to an increase in hydrostatic pressure of Bowman’s capsule that is a negative regulator of net filtration pressure at the glomerular level [41] (Fig. 3).
Lastly, the shift of energy expenditure across the nephron from the S1 segment to the S3 segment of the proximal tubule, where SGLT1 is located, and to the medullary thick ascending limb leads to a decline in partial oxygen pressure in those regions and an enhancement of hypoxia-inducible factor signaling [42, 43]. Enhanced hypoxia-inducible factor signaling results in the upregulation of erythropoietin (EPO) and hemoxygenase-1 [44, 45].
Do SGLT2is protect from AKI?
Cassis et al. provided experimental evidence of the reno-protective effects of the SGLT2i dapagliflozin, which reduced podocyte damage, glomerular lesions and proteinuria in mice with non-diabetic kidney disease [46]. In accordance with this study, SGLT2 levels were found to be increased by albumin load both in in vivo and in vitro models in an NF-kB–dependent manner; SGLT2is limited cytoskeletal remodeling mediated by albumin load in a cultured podocyte environment leading to preservation of the tubuloglomerular integrity [46, 47]. SGLT2is also interfere in a reno-protective way with non-glycemic pathways [32, 48]. Furthermore, in experimental DM models SGLT2is reduced albuminuria, mesangial expansion, matrix accumulation and interstitial fibrosis via the combined effects on glomerular hemodynamics and inhibition of renal inflammation and oxidative stress [49,50,51,52].
Another in vitro basic science study showed that the SGLT2i empagliflozin was able to reduce the levels of inflammatory and fibrotic markers [53]. Reduced metabolic requirements of blocked co-transporters also reduces the risk of ischemic-reperfusion damage or renal tubular hypoxia [54]. A reduction in AKI risk might theoretically lead to improvements in CKD progression, offering a mechanistic explanation for the favorable effect of SGLT2i on eGFR slopes in people with heart failure but no albuminuria [55,56,57,58].
Peritubular cells can produce more EPO in response to lower oxygen tension in the medulla, which could explain why hematocrit levels are higher in these individuals [59]. Because of its immunomodulatory activities, restoring EPO levels may eventually contribute to renal tissue protection [60].
Hyperglycemia causes an increase in glucose filtration, which leads to an increase in glucose reabsorption in the proximal tubule. This, in turn, increases oxygen consumption and depletes oxygen delivery to the tubular distal areas, particularly the renal medulla [38, 61]. SGLT2is may enhance oxygen availability, minimize reactive oxygen species, and improve medulla viability by lowering glucose reabsorption. This is difficult to reconcile with findings that SGLT2is boost EPO synthesis, which is often associated with renal hypoxia [62]. However, it does help to account for a rise in hematocrit, which would help oxygen supply. To explain this dilemma, it has been proposed that SGLT2is alter the production or signaling of the hypoxia-inducible factor, reduce hypoxia-inducible factor-1 activity and/or promote hypoxia-inducible factor-2 activity in the kidney, favoring a decrease in pro-inflammatory and fibrotic factors while also increasing EPO levels [63, 64].
Lastly, various alternative pathways for SGLT2i renal protection have been suggested. The capacity to reduce blood pressure without increasing heart rate results in a decrease in sympathetic activity [65]. SGLT2is also reduce venous congestion and backpressure against renal venous drainage by reducing heart failure [66].
Dekkers et al. showed that dapagliflozin reduced albuminuria by 43.9% and eGFR by 5.1% compared to placebo. Dapagliflozin had no effect on glomerular charge or size selectivity index and reduced urinary excretion of IgG, IgG4, IL-6 and KIM-1; no changes in NGAL, LFABP, or MCP-1 were observed. Changes in albuminuria were shown to be linked to changes in eGFR and KIM-1. Finally, the albuminuria-lowering impact of dapagliflozin therapy for 6 weeks could be due to a reduction in intraglomerular pressure or tubular cell damage [67, 68].
It may be speculated that AKI can occur in the early phases, but due to inadequate measurements within 1–2 weeks of SGLT2i use, it might not be detected by clinicians. If not progressive, a slight initial reduction in GFR due to hemodynamic effects should be expected and tolerated [69]. Herrington et al. showed a small reversible reduction in eGFR in the first 4 weeks compared to placebo, followed by a significant reduction in the rate of chronic eGFR fall over time [70].
Five large scale RCTs have investigated the effects of SGLT2is on renal outcomes: the EMPA-REG outcome trial, the CANVAS program, CREDENCE, DAPA-CKD and EMPA-Kidney [17, 20, 21, 33, 70]. The EMPA-REG outcome trial investigated primarily the cardiovascular effects and secondarily renal outcomes of empagliflozin therapy for 192 weeks in 6185 participants with type-2 DM and high cardiovascular disease risk and eGFR > 30 mL/min/1.73 m2. This trial reported an initial decline in eGFR in the empagliflozin group compared to the placebo group at 4-week follow-up (weekly decline of 0.62 ± 0.04 and 0.82 ± 0.04 mL/min/1.73 m2 with 10 mg/day and 25 mg/day of empagliflozin, respectively); an increase of 0.01 ± 0.04 mL/min/1.73 m2 was observed in the placebo group. The risk for incident or worsening nephropathy (12.7% vs. 18.8%), progression of macroalbuminuria (11.2% vs. 16.2%), doubling of serum creatinine (1.5% vs. 2.6%), and need for renal replacement therapy (0.3% vs. 0.6%) were lower in a statistically significant way in the empagliflozin group. No statistically significant change was observed in incident albuminuria (51.5% vs. 51.2%) [33, 71]. The CANVAS program included two RCTs with a total of 10,142 participants with a mean follow-up period of 188.2 weeks and investigated primarily the cardiovascular outcomes of canagliflozin therapy. The latter reduced the risk for albuminuria progression (89.4 vs. 128.7 participants with an event/1000 patient-years), the need for renal replacement therapy, death due to renal causes and eGFR decline in a statistically significant way compared to placebo [21]. Few other small scale studies investigated the renal outcomes associated with SGLT2is and reported contradictory findings. The limitation of such studies are the low number of participants and the short follow-up periods [72,73,74,75,76,77,78].
Therefore, the latest research has shown beneficial renal protective effects of SGLT2is, while the initial concerns raised by the US FDA Adverse Event Reporting System (FAERS) in 2016 with the announcement of 101 cases of SGLT2i-associated AKI in the first month following the initiation of therapy are mostly overcome by the growing literature [79]. Initial decline in eGFR and elevation in serum creatinine in diabetic patients are not caused by tubular or glomerular injury, and thus, do not impose additional risks for AKI. Figure 4 summarizes the mentioned pathophysiological mechanisms through which SGLT2is protect kidney function, as shown by the latest clinical and pre-clinical studies.
Conclusions
We can probably stop worrying about AKI risk when using SGLT2is. Despite the warning published by the US FDA in 2016 about a potential AKI risk and the report of some clinical cases of AKI when prescribing SGLT2is, large observational real-life retrospective studies, RCTs and propensity-matched analyses of data from clinical practice unambiguously demonstrate that SGLT2is are safe for the kidney and do not predispose to AKI. However, the question whether these agents should be withheld in the presence of high-risk clinical situations remains unaddressed.
References
Gheith O, Farouk N, Nampoory N, Halim MA, Al-Otaibi T (2015) Diabetic kidney disease: world wide difference of prevalence and risk factors. J Nephropharmacol 5:49–56
Hill NR, Fatoba ST, Oke JL, Hirst JA, O’Callaghan CA, Lasserson DS, Hobbs FD (2016) Global prevalence of chronic kidney disease—a systematic review and meta-analysis. PLoS One 11:e0158765
Lewis EJ, Hunsicker LG, Bain RP, Rohde RD (1993) The effect of angiotensin-converting-enzyme inhibition on diabetic nephropathy. The Collaborative Study Group. N Engl J Med 329:1456–1462
Brenner BM, Cooper ME, de Zeeuw D, Keane WF, Mitch WE, Parving HH, Remuzzi G, Snapinn SM, Zhang Z, Shahinfar S (2001) Effects of losartan on renal and cardiovascular outcomes in patients with type 2 diabetes and nephropathy. N Engl J Med 345:861–869
FDA Drug Safety Communication: FDA strengthens kidney warnings for diabetes medicines canagliflozin (Invokana, Invokamet) and dapagliflozin (Farxiga, Xigduo XR). U.S. Food and Drug Administration; 2016.
Alkabbani W, Zongo A, Minhas-Sandhu JK, Eurich DT, Shah BR, Alsabbagh MW, Gamble JM (2021) Renal effectiveness and safety of the sodium-glucose cotransporter-2 inhibitors: a population-based cohort study. BMJ Open Diabetes Res Care 9:e002496
Lee YT, Hsu CN, Fu CM, Wang SW, Huang CC, Li LC (2021) Comparison of adverse kidney outcomes with empagliflozin and linagliptin use in patients with type 2 diabetic patients in a real-world setting. Front Pharmacol 12:781379
Zhuo M, Paik JM, Wexler DJ, Bonventre JV, Kim SC, Patorno E (2022) SGLT2 inhibitors and the risk of acute kidney injury in older adults with type 2 diabetes. Am J Kidney Dis 79:858–867
Rampersad C, Kraut E, Whitlock RH, Komenda P, Woo V, Rigatto C, Tangri N (2020) Acute kidney injury events in patients with type 2 diabetes using SGLT2 inhibitors versus other glucose-lowering drugs: a retrospective cohort study. Am J Kidney Dis 76:471-479.e471
Iskander C, Cherney DZ, Clemens KK, Dixon SN, Harel Z, Jeyakumar N, McArthur E, Muanda FT, Parikh CR, Paterson JM, Tangri N, Udell JA, Wald R, Garg AX (2020) Use of sodium-glucose cotransporter-2 inhibitors and risk of acute kidney injury in older adults with diabetes: a population-based cohort study. CMAJ 192:E351-e360
Pasternak B, Wintzell V, Melbye M, Eliasson B, Svensson AM, Franzén S, Gudbjörnsdottir S, Hveem K, Jonasson C, Svanström H, Ueda P (2020) Use of sodium-glucose co-transporter 2 inhibitors and risk of serious renal events: Scandinavian cohort study. BMJ 369:m1186
Miyoshi H, Kameda H, Yamashita K, Nakamura A, Kurihara Y (2019) Protective effect of sodium-glucose cotransporter 2 inhibitors in patients with rapid renal function decline, stage G3 or G4 chronic kidney disease and type 2 diabetes. J Diabetes Investig 10:1510–1517
Lin YH, Huang YY, Hsieh SH, Sun JH, Chen ST, Lin CH (2019) Renal and glucose-lowering effects of empagliflozin and dapagliflozin in different chronic kidney disease stages. Front Endocrinol (Lausanne) 10:820
Cahn A, Melzer-Cohen C, Pollack R, Chodick G, Shalev V (2019) Acute renal outcomes with sodium-glucose co-transporter-2 inhibitors: real-world data analysis. Diabetes Obes Metab 21:340–348
Nadkarni GN, Ferrandino R, Chang A, Surapaneni A, Chauhan K, Poojary P, Saha A, Ferket B, Grams ME, Coca SG (2017) Acute kidney injury in patients on SGLT2 inhibitors: a propensity-matched analysis. Diabetes Care 40:1479–1485
Cahn A, Mosenzon O, Wiviott SD, Rozenberg A, Yanuv I, Goodrich EL, Murphy SA, Bhatt DL, Leiter LA, McGuire DK, Wilding JPH, Gause-Nilsson IAM, Fredriksson M, Johansson PA, Langkilde AM, Sabatine MS, Raz I (2020) Efficacy and safety of dapagliflozin in the elderly: analysis from the DECLARE-TIMI 58 study. Diabetes Care 43:468–475
Heerspink HJL, Stefánsson BV, Correa-Rotter R, Chertow GM, Greene T, Hou FF, Mann JFE, McMurray JJV, Lindberg M, Rossing P, Sjöström CD, Toto RD, Langkilde AM, Wheeler DC (2020) Dapagliflozin in patients with chronic kidney disease. N Engl J Med 383:1436–1446
Cannon CP, Pratley R, Dagogo-Jack S, Mancuso J, Huyck S, Masiukiewicz U, Charbonnel B, Frederich R, Gallo S, Cosentino F, Shih WJ, Gantz I, Terra SG, Cherney DZI, McGuire DK (2020) Cardiovascular Outcomes with ertugliflozin in type 2 diabetes. N Engl J Med 383:1425–1435
Bakris G, Oshima M, Mahaffey KW, Agarwal R, Cannon CP, Capuano G, Charytan DM, de Zeeuw D, Edwards R, Greene T, Heerspink HJL, Levin A, Neal B, Oh R, Pollock C, Rosenthal N, Wheeler DC, Zhang H, Zinman B, Jardine MJ, Perkovic V (2020) Effects of Canagliflozin in patients with baseline eGFR <30 ml/min per 1.73 m(2): subgroup analysis of the randomized CREDENCE trial. Clin J Am Soc Nephrol 15:1705–1714
Perkovic V, Jardine MJ, Neal B, Bompoint S, Heerspink HJL, Charytan DM, Edwards R, Agarwal R, Bakris G, Bull S, Cannon CP, Capuano G, Chu PL, de Zeeuw D, Greene T, Levin A, Pollock C, Wheeler DC, Yavin Y, Zhang H, Zinman B, Meininger G, Brenner BM, Mahaffey KW (2019) Canagliflozin and renal outcomes in type 2 diabetes and nephropathy. N Engl J Med 380:2295–2306
Neal B, Perkovic V, Mahaffey KW, de Zeeuw D, Fulcher G, Erondu N, Shaw W, Law G, Desai M, Matthews DR (2017) Canagliflozin and cardiovascular and renal events in type 2 diabetes. N Engl J Med 377:644–657
McMurray JJV, Solomon SD, Inzucchi SE, Køber L, Kosiborod MN, Martinez FA, Ponikowski P, Sabatine MS, Anand IS, Bělohlávek J, Böhm M, Chiang CE, Chopra VK, de Boer RA, Desai AS, Diez M, Drozdz J, Dukát A, Ge J, Howlett JG, Katova T, Kitakaze M, Ljungman CEA, Merkely B, Nicolau JC, O’Meara E, Petrie MC, Vinh PN, Schou M, Tereshchenko S, Verma S, Held C, DeMets DL, Docherty KF, Jhund PS, Bengtsson O, Sjöstrand M, Langkilde AM (2019) Dapagliflozin in patients with heart failure and reduced ejection fraction. N Engl J Med 381:1995–2008
Donnan JR, Grandy CA, Chibrikov E, Marra CA, Aubrey-Bassler K, Johnston K, Swab M, Hache J, Curnew D, Nguyen H, Gamble JM (2019) Comparative safety of the sodium glucose co-transporter 2 (SGLT2) inhibitors: a systematic review and meta-analysis. BMJ Open 9:e022577
Menne J, Dumann E, Haller H, Schmidt BMW (2019) Acute kidney injury and adverse renal events in patients receiving SGLT2-inhibitors: a systematic review and meta-analysis. PLoS Med 16:e1002983
Gilbert RE, Thorpe KE (2019) Acute kidney injury with sodium-glucose co-transporter-2 inhibitors: a meta-analysis of cardiovascular outcome trials. Diabetes Obes Metab 21:1996–2000
Katsuhara Y, Ogawa T (2020) Acute renal failure, ketoacidosis, and urogenital tract infections with SGLT2 inhibitors: signal detection using a Japanese spontaneous reporting database. Clin Drug Investig 40:645–652
Katsuhara Y, Ikeda S (2021) Correlations between SGLT-2 inhibitors and acute renal failure by signal detection using FAERS: stratified analysis for reporting country and concomitant drugs. Clin Drug Investig 41:235–243
Heyman SN, Khamaisi M, Rosen S, Rosenberger C, Abassi Z (2017) Potential hypoxic renal injury in patients with diabetes on SGLT2 inhibitors: caution regarding concomitant use of NSAIDs and iodinated contrast media. Diabetes Care 40:e40–e41
McMurray JJ, Solomon SD, Inzucchi SE, Køber L, Kosiborod MN, Martinez FA, Ponikowski P, Sabatine MS, Anand IS, Bělohlávek J (2019) Dapagliflozin in patients with heart failure and reduced ejection fraction. N Engl J Med 381:1995–2008
DeFronzo RA, Norton L, Abdul-Ghani M (2017) Renal, metabolic and cardiovascular considerations of SGLT2 inhibition. Nat Rev Nephrol 13:11–26
Wright EM, Loo DD, Hirayama BA (2011) Biology of human sodium glucose transporters. Physiol Rev 91:733–794
Heerspink HJ, Desai M, Jardine M, Balis D, Meininger G, Perkovic V (2017) Canagliflozin slows progression of renal function decline independently of glycemic effects. J Am Soc Nephrol 28:368–375
Wanner C, Inzucchi SE, Lachin JM, Fitchett D, von Eynatten M, Mattheus M, Johansen OE, Woerle HJ, Broedl UC, Zinman B (2016) Empagliflozin and progression of kidney disease in type 2 diabetes. N Engl J Med 375:323–334
Hahn K, Ejaz AA, Kanbay M, Lanaspa MA, Johnson RJ (2016) Acute kidney injury from SGLT2 inhibitors: potential mechanisms. Nat Rev Nephrol 12:711–712
Hahn K, Kanbay M, Lanaspa MA, Johnson RJ, Ejaz AA (2017) Serum uric acid and acute kidney injury: a mini review. J Adv Res 8:529–536
Bjornstad P, Lanaspa MA, Ishimoto T, Kosugi T, Kume S, Jalal D, Maahs DM, Snell-Bergeon JK, Johnson RJ, Nakagawa T (2015) Fructose and uric acid in diabetic nephropathy. Diabetologia 58:1993–2002
Szalat A, Perlman A, Muszkat M, Khamaisi M, Abassi Z, Heyman SN (2018) Can SGLT2 inhibitors cause acute renal failure? Plausible role for altered glomerular hemodynamics and medullary hypoxia. Drug Saf 41:239–252
Vallon V, Thomson SC (2020) The tubular hypothesis of nephron filtration and diabetic kidney disease. Nat Rev Nephrol 16:317–336
Wilcox CS (1998) Role of macula densa NOS in tubuloglomerular feedback. Curr Opin Nephrol Hypertens 7:443–449
Vallon V, Thomson SC (2017) Targeting renal glucose reabsorption to treat hyperglycaemia: the pleiotropic effects of SGLT2 inhibition. Diabetologia 60:215–225
Vallon V, Richter K, Blantz RC, Thomson S, Osswald H (1999) Glomerular hyperfiltration in experimental diabetes mellitus: potential role of tubular reabsorption. J Am Soc Nephrol 10:2569–2576
Layton AT, Vallon V, Edwards A (2016) Predicted consequences of diabetes and SGLT inhibition on transport and oxygen consumption along a rat nephron. Am J Physiol Renal Physiol 310:F1269-1283
O’Neill J, Fasching A, Pihl L, Patinha D, Franzén S, Palm F (2015) Acute SGLT inhibition normalizes O2 tension in the renal cortex but causes hypoxia in the renal medulla in anaesthetized control and diabetic rats. Am J Physiol Renal Physiol 309:F227-234
Vallon V, Rose M, Gerasimova M, Satriano J, Platt KA, Koepsell H, Cunard R, Sharma K, Thomson SC, Rieg T (2013) Knockout of Na-glucose transporter SGLT2 attenuates hyperglycemia and glomerular hyperfiltration but not kidney growth or injury in diabetes mellitus. Am J Physiol Renal Physiol 304:F156-167
Layton AT, Vallon V (2018) SGLT2 inhibition in a kidney with reduced nephron number: modeling and analysis of solute transport and metabolism. Am J Physiol Renal Physiol 314:F969-f984
Cassis P, Locatelli M, Cerullo D, Corna D, Buelli S, Zanchi C, Villa S, Morigi M, Remuzzi G, Benigni A, Zoja C (2018) SGLT2 inhibitor dapagliflozin limits podocyte damage in proteinuric nondiabetic nephropathy. JCI Insight 3(15):e98720
Vallon V, Komers R (2011) Pathophysiology of the diabetic kidney. Compr Physiol 1:1175–1232
Rajasekeran H, Cherney DZ, Lovshin JA (2017) Do effects of sodium-glucose cotransporter-2 inhibitors in patients with diabetes give insight into potential use in non-diabetic kidney disease? Curr Opin Nephrol Hypertens 26:358–367
Vallon V, Gerasimova M, Rose MA, Masuda T, Satriano J, Mayoux E, Koepsell H, Thomson SC, Rieg T (2014) SGLT2 inhibitor empagliflozin reduces renal growth and albuminuria in proportion to hyperglycemia and prevents glomerular hyperfiltration in diabetic Akita mice. Am J Physiol Renal Physiol 306:F194-204
Gembardt F, Bartaun C, Jarzebska N, Mayoux E, Todorov VT, Hohenstein B, Hugo C (2014) The SGLT2 inhibitor empagliflozin ameliorates early features of diabetic nephropathy in BTBR ob/ob type 2 diabetic mice with and without hypertension. Am J Physiol Renal Physiol 307:F317-325
Terami N, Ogawa D, Tachibana H, Hatanaka T, Wada J, Nakatsuka A, Eguchi J, Horiguchi CS, Nishii N, Yamada H, Takei K, Makino H (2014) Long-term treatment with the sodium glucose cotransporter 2 inhibitor, dapagliflozin, ameliorates glucose homeostasis and diabetic nephropathy in db/db mice. PLoS One 9:e100777
Wang XX, Levi J, Luo Y, Myakala K, Herman-Edelstein M, Qiu L, Wang D, Peng Y, Grenz A, Lucia S, Dobrinskikh E, D’Agati VD, Koepsell H, Kopp JB, Rosenberg AZ, Levi M (2017) SGLT2 protein expression is increased in human diabetic nephropathy: SGLT2 protein inhibition decreases renal lipid accumulation, inflammation, and the development of nephropathy in diabetic mice. J Biol Chem 292:5335–5348
Panchapakesan U, Pegg K, Gross S, Komala MG, Mudaliar H, Forbes J, Pollock C, Mather A (2013) Effects of SGLT2 inhibition in human kidney proximal tubular cells–renoprotection in diabetic nephropathy? PLoS One 8:e54442
Sridhar VS, Tuttle KR, Cherney DZI (2020) We can finally stop worrying about SGLT2 inhibitors and acute kidney injury. Am J Kidney Dis 76:454–456
Packer M, Anker SD, Butler J, Filippatos G, Pocock SJ, Carson P, Januzzi J, Verma S, Tsutsui H, Brueckmann M, Jamal W, Kimura K, Schnee J, Zeller C, Cotton D, Bocchi E, Böhm M, Choi DJ, Chopra V, Chuquiure E, Giannetti N, Janssens S, Zhang J, Gonzalez Juanatey JR, Kaul S, Brunner-La Rocca HP, Merkely B, Nicholls SJ, Perrone S, Pina I, Ponikowski P, Sattar N, Senni M, Seronde MF, Spinar J, Squire I, Taddei S, Wanner C, Zannad F (2020) Cardiovascular and renal outcomes with empagliflozin in heart failure. N Engl J Med 383:1413–1424
Zannad F, Ferreira JP, Pocock SJ, Zeller C, Anker SD, Butler J, Filippatos G, Hauske SJ, Brueckmann M, Pfarr E, Schnee J, Wanner C, Packer M (2021) Cardiac and kidney benefits of empagliflozin in heart failure across the spectrum of kidney function: insights from EMPEROR-reduced. Circulation 143:310–321
Jhund PS, Solomon SD, Docherty KF, Heerspink HJL, Anand IS, Böhm M, Chopra V, de Boer RA, Desai AS, Ge J, Kitakaze M, Merkley B, O’Meara E, Shou M, Tereshchenko S, Verma S, Vinh PN, Inzucchi SE, Køber L, Kosiborod MN, Martinez FA, Ponikowski P, Sabatine MS, Bengtsson O, Langkilde AM, Sjöstrand M, McMurray JJV (2021) Efficacy of dapagliflozin on renal function and outcomes in patients with heart failure with reduced ejection fraction: results of DAPA-HF. Circulation 143:298–309
Basile DP, Bonventre JV, Mehta R, Nangaku M, Unwin R, Rosner MH, Kellum JA, Ronco C (2016) Progression after AKI: understanding maladaptive repair processes to predict and identify therapeutic treatments. J Am Soc Nephrol 27:687–697
Sano M, Goto S (2019) Possible mechanism of hematocrit elevation by sodium glucose cotransporter 2 inhibitors and associated beneficial renal and cardiovascular effects. Circulation 139:1985–1987
Cantarelli C, Angeletti A, Cravedi P (2019) Erythropoietin, a multifaceted protein with innate and adaptive immune modulatory activity. Am J Transplant 19:2407–2414
Feng YZ, Ye YJ, Cheng ZY, Hu JJ, Zhang CB, Qian L, Lu XH, Cai XR (2020) Non-invasive assessment of early stage diabetic nephropathy by DTI and BOLD MRI. Br J Radiol 93:20190562
Mazer CD, Hare GMT, Connelly PW, Gilbert RE, Shehata N, Quan A, Teoh H, Leiter LA, Zinman B, Jüni P, Zuo F, Mistry N, Thorpe KE, Goldenberg RM, Yan AT, Connelly KA, Verma S (2020) Effect of empagliflozin on erythropoietin levels, iron stores, and red blood cell morphology in patients with type 2 diabetes mellitus and coronary artery disease. Circulation 141:704–707
Packer M (2021) Mechanisms leading to differential hypoxia-inducible factor signaling in the diabetic kidney: modulation by SGLT2 inhibitors and hypoxia mimetics. Am J Kidney Dis 77:280–286
Cai T, Ke Q, Fang Y, Wen P, Chen H, Yuan Q, Luo J, Zhang Y, Sun Q, Lv Y, Zen K, Jiang L, Zhou Y, Yang J (2020) Sodium-glucose cotransporter 2 inhibition suppresses HIF-1α-mediated metabolic switch from lipid oxidation to glycolysis in kidney tubule cells of diabetic mice. Cell Death Dis 11:390
Scheen AJ (2019) Effect of SGLT2 inhibitors on the sympathetic nervous system and blood pressure. Curr Cardiol Rep 21:70
Bailey CJ, Day C, Bellary S (2022) Renal protection with SGLT2 inhibitors: effects in acute and chronic kidney disease. Curr Diab Rep 22:39–52
Dekkers CC, Petrykiv S, Laverman GD, Cherney DZ, Gansevoort RT, Heerspink HJ (2018) Effects of the SGLT-2 inhibitor dapagliflozin on glomerular and tubular injury markers. Diabetes Obes Metab 20:1988–1993
Satirapoj B, Korkiatpitak P, Supasyndh O (2019) Effect of sodium-glucose cotransporter 2 inhibitor on proximal tubular function and injury in patients with type 2 diabetes: a randomized controlled trial. Clin Kidney J 12:326–332
Ryan R, Choo S, Willows J, Walker J, Prasad K, Tez D (2021) Acute interstitial nephritis due to sodium-glucose co-transporter 2 inhibitor empagliflozin. Clin Kidney J 14:1020–1022
Herrington WG, Preiss D, Haynes R, von Eynatten M, Staplin N, Hauske SJ, George JT, Green JB, Landray MJ, Baigent C, Wanner C (2018) The potential for improving cardio-renal outcomes by sodium-glucose co-transporter-2 inhibition in people with chronic kidney disease: a rationale for the EMPA-KIDNEY study. Clin Kidney J 11:749–761
Zinman B, Wanner C, Lachin JM, Fitchett D, Bluhmki E, Hantel S, Mattheus M, Devins T, Johansen OE, Woerle HJ, Broedl UC, Inzucchi SE (2015) Empagliflozin, cardiovascular outcomes, and mortality in type 2 diabetes. N Engl J Med 373:2117–2128
Bailey CJ, Gross JL, Hennicken D, Iqbal N, Mansfield TA, List JF (2013) Dapagliflozin add-on to metformin in type 2 diabetes inadequately controlled with metformin: a randomized, double-blind, placebo-controlled 102-week trial. BMC Med 11:43
Bailey CJ, Iqbal N, T’Joen C, List JF (2012) Dapagliflozin monotherapy in drug-naïve patients with diabetes: a randomized-controlled trial of low-dose range. Diabetes Obes Metab 14:951–959
Cefalu WT, Leiter LA, de Bruin TW, Gause-Nilsson I, Sugg J, Parikh SJ (2015) Dapagliflozin’s effects on glycemia and cardiovascular risk factors in high-risk patients with type 2 diabetes: a 24-week, multicenter, randomized, double-blind, placebo-controlled study with a 28-week extension. Diabetes Care 38:1218–1227
Kohan DE, Fioretto P, Tang W, List JF (2014) Long-term study of patients with type 2 diabetes and moderate renal impairment shows that dapagliflozin reduces weight and blood pressure but does not improve glycemic control. Kidney Int 85:962–971
Leiter LA, Yoon KH, Arias P, Langslet G, Xie J, Balis DA, Millington D, Vercruysse F, Canovatchel W, Meininger G (2015) Canagliflozin provides durable glycemic improvements and body weight reduction over 104 weeks versus glimepiride in patients with type 2 diabetes on metformin: a randomized, double-blind, phase 3 study. Diabetes Care 38:355–364
Maldonado-Lutomirsky M, Softeland E, Meier J, Vangen B, Toorawa R, Woerle H-J, Broedl U. Empagliflozin (EMPA) as add-on to linagliptin (LINA) and metformin in patients with type 2 diabetes (T2DM): a 24-week randomised, double-blind, parallel-group trial. Diabetologia. New York: Springer; 2016. p. S93.
Søfteland E, Meier JJ, Vangen B, Toorawa R, Maldonado-Lutomirsky M, Broedl UC (2017) Empagliflozin as add-on therapy in patients with type 2 diabetes inadequately controlled with linagliptin and metformin: a 24-week randomized, double-blind, parallel-group trial. Diabetes Care 40:201–209
Nespoux J, Vallon V (2018) SGLT2 inhibition and kidney protection. Clin Sci (Lond) 132:1329–1339
Funding
No funding agency granted the present study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosure of potential conflicts of interest
The authors declare that they have no conflict of interest.
Research involving human participants and/or animals
This article does not contain any studies with human participants or animals performed by any of the authors.
Informed consent
No verbal and written informed consent was necessary for this study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Copur, S., Yildiz, A., Basile, C. et al. Is there any robust evidence showing that SGLT2 inhibitor use predisposes to acute kidney injury?. J Nephrol 36, 31–43 (2023). https://doi.org/10.1007/s40620-022-01422-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40620-022-01422-w