Abstract
Purpose of Review
Despite the important progress made in understanding the regulation of phosphate (Pi) homeostasis over the past 20 years, the mechanisms underlying the very early step leading to the regulating cascade involving multiple hormones (PTH, vitamin D, FGF23) and organs (kidney, intestine, bone, parathyroid glands) are not deciphered. Particularly, knowledge on the Pi-sensing mechanism present within or on the surface of the cell that is able to detect changes in serum or local Pi concentrations and trigger an appropriate FGF23 synthesis/secretion is limited or absent.
Recent Findings
Several molecular actors have recently been involved as potential key players in Pi sensing and Pi-dependent control of FGF23 secretion. Among them, the PiT1/Slc20a1 and PiT2/Slc20a2 proteins are standing out.
Summary
We are just beginning to accumulate in vitro and in vivo data that will provide invaluable molecular tools to explore and understand the integrated response of the body to variations of Pi concentration.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Discovered in 2000, Fibroblast growth factor 23 (FGF23) is an endocrine factor that plays a central role in Pi homeostasis in mammals [1, 2]. It is expressed mainly but not exclusively by osteoblasts and osteocytes in bone [3•] and targets the kidney to inhibit the renal reabsorption of phosphate (Pi) and the production of the active form of vitamin D, 1,25(OH)2D [4,5,6]. Accordingly, increased serum levels of active FGF23 are observed in inherited or acquired disorders of Pi homeostasis leading to renal Pi wasting and abnormal vitamin D metabolism [7,8,9]. FGF23 depends on its co-receptor αKlotho and FGFR1c to mediate this action [10]. High serum FGF23 levels are also observed during chronic kidney disease (CKD) where unregulated prolonged hyperphosphatemia resulting from renal excretion defects leads to life-threatening situations due to inappropriate deposition of calcium-Pi crystals in vessels [11, 12]. These observations illustrate the need for a tight regulation of FGF23 secretion in maintaining normal serum Pi levels.
The 1,25(OH)2 vitamin D was shown to enhance FGF23 production and FGF23 serum levels [13, 14], but the low 1,25(OH)2D serum levels during CKD [15] argues for the existence of other determinants of FGF23 secretion. Recently, FGF23 expression and/or secretion was shown to be regulated by various factors, including FGFR1 signaling [7, 16], iron deficiency [17], and pro-inflammatory stimuli [18, 19], but it remains to be determined whether these regulations have a role in Pi homeostasis regulation. Interestingly enough, while an important progress has been made in elucidating the role of FGF23 in Pi homeostasis regulation over the past 20 years, the mechanisms underlying the very early step of Pi homeostasis are still not deciphered. This first step is the ability of a cell or an organism to detect the variations of intra- and/or extracellular concentrations of Pi that will trigger the regulating cascade aimed at normalizing the Pi serum levels.
Therefore, this review will explore the possible mechanisms by which Pi could directly regulate FGF23 production and/or secretion by summarizing the interplay between FGF23 and molecules involved in Pi sensing.
Phosphate-Dependent Regulation of FGF23
Studies conducted in humans demonstrated that serum FGF23 levels are associated with dietary Pi [20,21,22], and that intravenous infusion of Pi or acute duodenal Pi load increased FGF23 levels [23]. A relationship between dietary Pi load and circulating Fgf23 levels was also illustrated in mice [24, 25]. Nevertheless, it is important to differentiate short-term (direct) changes in FGF23 levels following dietary Pi loads from long-term (indirect) changes through endocrine loops that may involve other organs than bone. For instance, we have recently showed that changes in Pi diet can influence Klotho protein expression in vivo in the kidney [26••], while another group has shown that FGFR1 mRNA expression can be regulated by extracellular Pi concentration in vitro [27], underscoring the role of these factors in the Pi-dependent regulation of FGF23. In addition, it is unclear by which mechanisms FGF23 is regulated by Pi (transcription, post-transcription, secretion, activity, and/or cleavage).
In vitro studies have been conducted in order to decipher the Pi-dependent FGF23 regulation mechanisms, but results are conflicting. Extracellular Pi concentration directly stimulates the transcription of FGF23 in some studies [28, 29] but not in others [26••, 27, 30, 31•, 32]. Undoubtedly, in vitro studies are limited by the absence of appropriate models for FGF23 secretion, since only fully differentiated osteocytes secrete significant levels of FGF23, maybe due to the importance of extracellular matrix and 3D environment that is lacking in established cell lines. Based on this observation, we recently set up an ex vivo bone shaft model in which we were able to illustrate significant Pi-dependent FGF23 secretion, together with no effect of Pi on FGF23 transcription [26••].
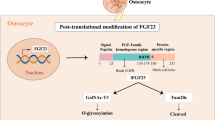
FGF23 biological action can also be regulated by intracellular cleavage of the protein, a phenomenon that is regulated by the balanced action of two molecules. Polypeptide N-acetylgalactosaminyltransferase 3 (GALNT3) protects FGF23 activity by its O-glycosylation activity at the Thr178 cleavage site providing protection of furin-mediated cleavage [33]. Another post-translational modification has more recently been involved, which is a phosphorylation of Ser180 by family with sequence similarity 20, member C (FAM20C) kinase [34•]. This phosphorylation inhibits the O-glycosylation, thus promoting FGF23 cleavage. However, GALNT3 and FAM20C regulators remain poorly described for now, except for one study showing Pi-dependent regulation of GALNT3 expression [35].
Phosphate as a Signaling Molecule
In addition to its well-known role as a component of apatite crystals, evidence of a role of Pi as a signaling molecule has slowly emerged in the scientific community. The first evidence of such a role was shown approximately 15–20 years ago owing to the work of Beck GR et al. that demonstrated the regulation of secreted phosphoprotein 1 (Spp1) expression by Pi [36, 37]. Since then, the direct effect of Pi on bone cell function and on extra-skeletal organs has been illustrated multiple times through the Pi-dependent regulation of many genes [31•, 38, 39••].
Being a “signaling” molecule implies Pi to activate a signaling pathway. Consistently, the early works of Beck GR and collaborators have described that the induction of the Spp1 gene by Pi was mediated by the activation of the ERK1/2 MAPK pathway [37]. The role of the ERK pathway in mediating the signaling function of Pi has now been confirmed by many other teams including ours [38, 40,41,42,43,44,45, 46•]. In addition to the ERK pathway, the Akt pathway has been found to be activated by Pi in adipose [4] and human bronchial cells [47], but not in HEK293 cells [44] or the chondrogenic cell line ATDC5 [43]. The PKC and proteasome were also found to be activated [37]. In contrast, several pathways have been shown not to be activated by Pi such as the P38 or JNK MAPK pathways [37, 40]. While knowledge on the signaling pathways and genes being regulated by Pi is accumulating, one key unanswered question is how Pi activates these pathways, and which pathway is relevant to the Pi-dependent FGF23 secretion.
Phosphate Sensing vs Phosphate Sensors
The mechanism by which Pi signals to the cell and activates genes or pathways is referred as Pi sensing. Although the existence of such a mechanism is now largely accepted [38, 39••, 48•], it is not known whether in mammalian organisms this involves a cell surface receptor that binds to Pi, or intracellular proteins that respond to changes in intracellular Pi concentrations (that may result from changes in the extracellular Pi). Moreover, since changes in Pi concentration occur in either compartment, both extracellular and intracellular Pi-sensing mechanisms are likely to co-exist.
Central to the sensing mechanism, the Pi sensor is thought to be a single molecule or a complex of molecules that is able to bind Pi and trigger the secondary events leading to the cellular response. A Pi sensor that detects changes in extracellular Pi concentrations would necessarily be present at the external cell surface. As such, membrane-associated proteins such as high-affinity Pi transporters or receptors represent good candidates. On the other hand, an intracellular Pi sensor could either be an intracytoplasmic protein or a membrane-associated protein with exposed intracellular regions.
Identifying a Pi sensor in higher eukaryotes is a very delicate task. An elementary difficulty relates to the definition of a Pi sensor, which, even more than the Pi-sensing mechanism, can be questionable. In addition, many processes have been proposed as part of a Pi detection mechanism, despite the lack of information on the identity of the Pi sensor itself. For instance, in yeasts, in condition of Pi starvation, the 5′-diphosphoinositol pentakisphosphate (IP7) accumulates in the cytoplasm. IP7 then binds to the SPX domain of the cyclin-dependent kinase inhibitor phosphate system positive regulatory protein (Pho81) and the Pi exporter XPR1, triggering the PHO pathway that will eventually activate Pi transporters to correct for intracellular Pi [49]. In this mechanism, in which IP7 serves as a second messenger to respond to a decrease in intracellular Pi concentration, the identity of the molecules that actually detect the intracellular Pi decrease is unknown. In mammals, IP7 is generated from IP6 by a family of IP6 kinases (IP6K1–3) [50, 51]. Early studies have identified IP6K2 as PiUS (standing for phosphate uptake stimulator), a protein characterized by its ability to enhance Pi uptake [52]. More recently, IP6K2 and IP6K3 have been identified as genetic determinants of serum Pi level regulation in humans [53], whereas PPIP5K, another enzyme responsible for the synthesis of inositol pyrophosphates, is strongly inhibited by extracellular Pi in human epithelial cells [54]. It is therefore important to design experiments to study the role of these kinases as potential intracellular Pi sensors.
Although it is expected that a Pi sensor will bind the Pi, the opposite is not necessarily true since a molecule that binds Pi does not necessarily represent a Pi sensor. This may be particularly difficult to conceptualize when considering Pi transporters at the plasma membrane. The binding of Pi on the transporter leads to a conformational change and ultimately to the transport of the Pi ion into the intracellular space, which will change the intracellular Pi concentration, triggering an adaptive cellular response. It is therefore true that a transporter participates in the sensing mechanism, but the molecule that informs the cell of a change in intracellular Pi is not necessarily the transporter itself [48•, 49]. It should be demonstrated that, independently of Pi transport, the transporter can signal to the cell (using transport-deficient transporters or non-metabolizable Pi analogues). Otherwise, it is the change in intracellular Pi itself that triggers the cellular response, via a still unknown intracellular Pi sensor.
Finally, while PHEX and DMP1 are involved in the regulation of Pi homeostasis through complex regulatory loops involving FGF23 secretion [9], it has recently been shown that mutations in these genes alter the responsiveness to extracellular Pi [55, 56] that may involve FGFR1 [7].
Candidate Molecules as Pi Sensors Involved in the Control of FGF23 Secretion
When considering the above definitions, candidate intracellular or membrane-bound proteins capable of binding Pi and acting as mediator of the Pi-dependent regulation of FGF23 are rare. The best candidates for mediating the Pi-dependent FGF23 regulation are presently the PiT/Slc20 proteins. PiT1/Slc20a1 and PiT2/Slc20a2 are high-affinity Na+-dependent Pi transporters [57, 58] that were originally identified as retrovirus receptors [59,60,61]. Unlike the other high-affinity Na+-Pi co-transporters described in mammals and which belong to the Slc34 family [62], PiT proteins are widely expressed, including in the main organs involved in the regulation of Pi homeostasis [63]. PiT1 expression was shown to be regulated by extracellular Pi concentration [32, 64,65,66]. Notably, PiT1 is involved in the Pi-dependent activation of the ERK1/2 pathway in numerous cell types [43,44,45, 46•]. The PiT1 paralog PiT2, although less studied, has also been suggested to be involved in Pi signaling.
We recently demonstrated that the Pi-dependent activation of ERK1/2 pathway requires both PiT1 and PiT2, and that Pi-dependent/PiT-mediated ERK1/2 phosphorylation does not require Pi transport through the PiT proteins [46•]. Although this was the first time that PiT2 was demonstrated to play a role in Pi signaling, Pi-independent function of PiT1 on ERK signaling has also been shown earlier [45, 67]. We also showed that PiT1 and PiT2 were able to form low-abundant heterodimers in addition to high-abundant homodimers and that the heterodimerization was enhanced by increased extracellular Pi. Importantly, we showed that the heterodimerization was dependent upon the binding of Pi to the PiTs, but not the transport of Pi. Early studies have also suggested a homodimerization of PiT2 in response to extracellular Pi variations that was independent of its transport function [68, 69]. These results reinforce the idea that PiT protein dimers are strong Pi sensor candidates mediating extracellular Pi variations. However, the cell-specificity of the redundancy or non-redundancy of PiT1 and PiT2 in mediating Pi effects and the physiological relevance of these findings are both unknown. As a first step to illustrate a physiological role for PiTs in Pi sensing, we recently illustrated in vitro, ex vivo in bone shafts culture, and in vivo in mice that lack of PiT2 blunted the Pi-dependent regulation of FGF23 secretion [26••]. Importantly, we also showed in this model that the ERK1/2 pathway was not involved in the Pi-dependent FGF23 secretion, despite a normal expression of FGFR1, suggesting that mechanistic links other than the ERK1/2 pathway may be at work between PiT2 and FGF23 secretion. Despite this observation, a role for FGFR1 in mediating the effect of Pi and PiTs on FGF23 secretion should still be considered. Indeed, the osteocyte-specific deletion of Fgfr1 partially restored the overproduction of FGF23 seen in Hyp mice [16]. Moreover, exogenous over-expression of FGFR1 in HEK cells rescued the decrease in the Pi-induced phosphorylation of ERK1/2 in PiT1-deficient cells [70], suggesting that FGFR1 may be a molecular link between PiT1 and the Raf/MEK/ERK pathway. Clearly, further studies are therefore necessary to decipher the link between PiT1/PiT2, FGFR1, and the ERK pathway in regulating FGF23 secretion.
A contribution in the sensing of extracellular Pi variations may involve the calcium-sensing receptor (CaSR). Not surprisingly, the CaSR was identified in a genome-wide association study as a genetic determinant of serum Pi concentration [53]. More intriguingly, the recent crystal structure of the receptor revealed multiple binding sites for PO43− ions in the extracellular domain of CaSR [71••]. Although no functional studies have been performed and the role of CaSR in the detection of Pi has not been tested, the authors suggest that binding Pi may modify the conformation of CaSR, which could modify the binding properties of Ca2+ to the receptor and have indirect consequences on the regulation of Pi homeostasis through Pi sensing.
Since the deletion of the intestinal high-affinity Na+-Pi co-transporter Npt2b/Slc34a2 leads to a decrease in Fgf23 serum levels [72] and that serum Pi levels have been shown to be regulated through an intestine-kidney axis [73, 74], the involvement of Npt2b in Pi sensing was suggested [75]. Although a role of Npt2b in regulating Pi concentration is consistent with the current observations, Npt2b expression is not regulated by Pi [76] and no study has yet been conducted to determine whether Npt2b could represent a Pi sensor. Particularly, it remains to be established whether its possible involvement in a Pi-sensing mechanism relates to its sole transport function, whereby Npt2b-mediated Pi entry in the cell would be detected by a yet unknown intracellular Pi sensor triggering the cell’s response.
The retrovirus receptor XPR1 [77] has recently been described as the only known Pi exporter in mammalian cells [78••]. XPR1 contains an N-terminal SPX (Syg1/Pho81/Xpr1) domain that is not required for Pi export function [78••], suggesting a potential role in another function. Consistently, the SPX domain is described in yeasts and plants as a domain that could mediate signal transmission from variations of extracellular Pi concentration [79, 80]. Recently, as outlined above, it was reported that the SPX domain binds inositol polyphosphates (IP), particularly IP7 [81••], the concentration of which changes upon Pi availability, suggesting that, as in yeasts, IP concentration participates to the Pi-sensing mechanism in mammals. The role of IP kinases may therefore be central to the regulation of intracellular Pi, while their role in regulating FGF23 secretion is totally unknown. A recent study illustrated that conditional deletion in mice of Xpr1 in the renal tubule resulted in renal Fanconi-like syndrome with impaired renal Pi reabsorption and impaired bone mineralization [82]. In addition to these Pi-related effects, these mice excrete massive amounts of glucose, amino acids, and albumin, indicating severe kidney damage and suggesting an important role for XPR1 in the kidney that may extend beyond the export or sensing of Pi. Although XPR1 is a promising candidate for controlling intracellular Pi concentration, further studies are needed to establish a link between its expression in the kidney or bone and the regulation of FGF23 synthesis or secretion.
Conclusion and Unresolved Questions
Although the regulation of Pi homeostasis by FGF23 has been extensively studied, the feedback loop by which Pi modulates FGF23 is much less known. Recent efforts have been made to identify the molecular actors involved in the detection of Pi and their role in triggering the expression or secretion of FGF23 (Fig. 1). Important molecules include the PiTs and XPR1 proteins, but also perhaps FGFR1 and CaSR. However, many questions remain. What is the respective role of PiT1 and PiT2 in controlling FGF23 secretion? What are the molecules connecting the PiT proteins to the ERK, Akt, or PKC signaling pathways? Since extracellular and intracellular Pi concentrations are closely related, what is the functional relationship between PiTs and XPR1, and do they function together in a coordinated manner to control FGF23 secretion? Is the sensing of Pi controlling FGF23 secretion limited to bone, or is there a coordination between the intestine, kidneys, bone, and parathyroid glands to integrate the response to variations in serum Pi levels? Finally, if Pi-sensing controlling serum Pi levels proves to be a universal mechanism widely distributed in the body’s cells, how can therapeutic strategies be devised to control it? These and many other questions remain challenges for researchers and clinicians and will require in-depth in vivo studies to decipher and understand them.
Schematic view of putative Pi-sensing pathways involved in FGF23 secretion. Upon Pi binding to the PiT1-PiT2 heterodimer, the ERK1/2 MAPK pathway is activated within few minutes, whereas FGF23 secretion is observed within few hours. However, the use of a MEK inhibitor did not block Pi-dependent PiT-mediated secretion of FGF23 indicating that other signaling pathways are involved. Upon stimulation by Pi, FGFR1 has been implicated in FGF23 regulation at the transcription level, a phenomenon that involves the ERK pathway. Since Pi was not demonstrated to bind FGFR1, a functional link between this receptor and the PiT proteins has been suggested. The regulation of intracellular Pi concentration may involve a coordinated control of Pi uptake through the PiTs and Pi efflux through XPR1. The IP6K2 kinase may represent an intracellular Pi sensor by modulating the concentration of IP7 that binds the SPX domain of XPR1 and controls Pi efflux. The role of the binding of Pi to CaSR and the transport of Pi by Npt2b in controlling FGF23 synthesis or secretion requires more investigation but may modulate the above phenomenon
References
Papers of particular interest, published recently, have been highlighted as: • Of importance •• Of major importance
ADHR Consortium. Autosomal dominant hypophosphataemic rickets is associated with mutations in FGF23. Nat Genet. 2000;26:345–8.
Yamashita T, Yoshioka M, Itoh N. Identification of a novel fibroblast growth factor, FGF-23, preferentially expressed in the ventrolateral thalamic nucleus of the brain. Biochem Biophys Res Commun. 2000;277:494–8.
• Richter B, Faul C. FGF23 actions on target tissues-with and without Klotho. Front Endocrinol (Lausanne). 2018;9:189. Extensive and up-to-date review on the roles of FGF23 not restricted to its role on Pi homeostasis.
Kawai M, Kinoshita S, Ozono K, Michigami T. Inorganic phosphate activates the AKT/mTORC1 pathway and shortens the life span of an α-Klotho-deficient model. J Am Soc Nephrol. 2016;27:2810–24.
Erben RG. Update on FGF23 and Klotho signaling. Mol Cell Endocrinol. Elsevier Ireland Ltd. 2016;432:56–65.
Shimada T, Hasegawa H, Yamazaki Y, Muto T, Hino R, Takeuchi Y, et al. FGF-23 is a potent regulator of vitamin D metabolism and phosphate homeostasis. J Bone Miner Res. 2004;19:429–35.
Martin A, Liu S, David V, Li H, Karydis A, Feng JQ, et al. Bone proteins PHEX and DMP1 regulate fibroblastic growth factor Fgf23 expression in osteocytes through a common pathway involving FGF receptor (FGFR) signaling. FASEB J. 2011;25:2551–62.
Christov M, Jüppner H. Insights from genetic disorders of phosphate homeostasis. Semin Nephrol. 2013;33:143–57.
Goldsweig BK, Carpenter TO. Hypophosphatemic rickets: lessons from disrupted FGF23 control of phosphorus homeostasis. Curr Osteoporos Rep. 2015;13:88–97.
Urakawa I, Yamazaki Y, Shimada T, Iijima K, Hasegawa H, Okawa K, et al. Klotho converts canonical FGF receptor into a specific receptor for FGF23. Nature. 2006;444:770–4.
Razzaque MS. Phosphate toxicity: new insights into an old problem. Clin Sci. 2011;120:91–7.
Lau WL, Pai A, Moe SM, Giachelli CM. Direct effects of phosphate on vascular cell function. Adv Chronic Kidney Dis. Elsevier Ltd. 2011;18:105–12.
Ito N, Fukumoto S, Takeuchi Y, Takeda S, Suzuki H, Yamashita T, et al. Effect of acute changes of serum phosphate on fibroblast growth factor (FGF)23 levels in humans. J Bone Miner Metab. 2007;25:419–22.
Kolek OI. 1α,25-Dihydroxyvitamin D3 upregulates FGF23 gene expression in bone: the final link in a renal-gastrointestinal-skeletal axis that controls phosphate transport. Am J Physiol Gastrointest Liver Physiol. 2005;289:G1036–42.
Shigematsu T, Kazama JJ, Yamashita T, Fukumoto S, Hosoya T, Gejyo F, et al. Possible involvement of circulating fibroblast growth factor 23 in the development of secondary hyperparathyroidism associated with renal insufficiency. Am J Kidney Dis. 2004;44:250–6.
Xiao Z, Huang J, Cao L, Liang Y, Han X, Quarles LD. Osteocyte-specific deletion of Fgfr1 suppresses FGF23. PLoS One. 2014;9:e104154.
Wolf M, White KE. Coupling fibroblast growth factor 23 production and cleavage. Curr Opin Nephrol Hypertens. 2014;23:411–9.
David V, Martin A, Isakova T, Spaulding C, Qi L, Ramirez V, et al. Inflammation and functional iron deficiency regulate fibroblast growth factor 23 production. Kidney Int, Nature Publishing Group. 2015;1–12.
Ito N, Wijenayaka AR, Prideaux M, Kogawa M, Ormsby RT, Evdokiou A, et al. Molecular and cellular endocrinology. Mol Cell Endocrinol. Elsevier Ireland Ltd. 2015;399:208–18.
Ferrari SL, Bonjour J-P, Rizzoli R. Fibroblast growth factor-23 relationship to dietary phosphate and renal phosphate handling in healthy young men. J Clin Endocrinol Metab. 2005;90:1519–24.
Burnett SAM, Gunawardene SC, Bringhurst FR, Jüppner H, Lee H, Finkelstein JS. Regulation of C-terminal and intact FGF-23 by dietary phosphate in men and women. J Bone Miner Res. 2006;21:1187–96.
Antoniucci DM, Yamashita T, Portale AA. Dietary phosphorus regulates serum fibroblast growth factor-23 concentrations in healthy men. J Clin Endocrinol Metab. 2006 ed. 2006;91:3144–9.
Scanni R, von Rotz M, Jehle S, Hulter HN, Krapf R. The human response to acute enteral and parenteral phosphate loads. J Am Soc Nephrol. 2014;25:2730–9.
Saito H, Maeda A, Ohtomo S-I, Hirata M, Kusano K, Kato S, et al. Circulating FGF-23 is regulated by 1alpha,25-dihydroxyvitamin D3 and phosphorus in vivo. J Biol Chem. 2005;280:2543–9.
Perwad F, Azam N, Zhang MYH, Yamashita T, Tenenhouse HS, Portale AA. Dietary and serum phosphorus regulate fibroblast growth factor 23 expression and 1,25-dihydroxyvitamin D metabolism in mice. Endocrinology. 2005;146:5358–64.
•• Bon N, Frangi G, Sourice S, Guicheux J, Beck-Cormier S, Beck L. Phosphate-dependent FGF23 secretion is modulated by PiT2/Slc20a2. Mol Metab. 2018;2018:1–8. First demonstration, in vitro, ex vivo, and in vivo of a direct role of PiT2 in Pi-dependent FGF23 secretion.
Nishino J, Yamazaki M, Kawai M, Tachikawa K, Yamamoto K, Miyagawa K, et al. Extracellular phosphate induces the expression of dentin matrix protein 1 through the FGF receptor in osteoblasts. J Cell Biochem. 2017;118:1151–63.
Hori M, Kinoshita Y, Taguchi M, Fukumoto S. Phosphate enhances Fgf23 expression through reactive oxygen species in UMR-106 cells. J Bone Miner Metab. 2015;34:132–9.
Ito N, Findlay DM, Anderson PH, Bonewald LF, Atkins GJ. Extracellular phosphate modulates the effect of 1α,25-dihydroxy vitamin D3 (1,25D) on osteocyte like cells. J Steroid Biochem Mol Biol. 2013;136:183–6.
Liu S, Tang W, Fang J, Ren J, Li H, Xiao Z, et al. Novel regulators of Fgf23 expression and mineralization in Hyp bone. Mol Endocrinol. 2009;23:1505–18.
• Camalier CE, Yi M, Yu L-R, Hood BL, Conrads KA, Lee YJ, et al. An integrated understanding of the physiological response to elevated extracellular phosphate. J Cell Physiol. 2013;228:1536–50. Extensive study on the Pi-dependent signaling pathways and gene expression in a pre-osteoblastic cell line.
Miyagawa K, Yamazaki M, Kawai M, Nishino J, Koshimizu T, Ohata Y, et al. Dysregulated gene expression in the primary osteoblasts and osteocytes isolated from hypophosphatemic Hyp mice. PLoS One. 2014;9:e93840.
Kato K, Jeanneau C, Tarp MA, Benet-Pagès A, Lorenz-Depiereux B, Bennett EP, et al. Polypeptide GalNAc-transferase T3 and familial tumoral calcinosis. Secretion of fibroblast growth factor 23 requires O-glycosylation. J Biol Chem. 2006;281:18370–7.
• Tagliabracci VS, Engel JL, Wiley SE, Xiao J, Gonzalez DJ, Nidumanda Appaiah H, et al. Dynamic regulation of FGF23 by Fam20C phosphorylation, GalNAc-T3 glycosylation, and furin proteolysis. Proc Natl Acad Sci U S A. 2014;111:5520–4. Elegant paper on the post-translational regulation of FGF23.
Chefetz I, Kohno K, Izumi H, Uitto J, Richard G, Sprecher E. GALNT3, a gene associated with hyperphosphatemic familial tumoral calcinosis, is transcriptionally regulated by extracellular phosphate and modulates matrix metalloproteinase activity. Biochim Biophys Acta. 2008 ed. 2009;1792:61–7.
Beck G, Zerler B, Moran E. Phosphate is a specific signal for induction of osteopontin gene expression. Proc Natl Acad Sci U S A. 2000;97:8352–7.
Beck G, Moran E, Knecht N. Inorganic phosphate regulates multiple genes during osteoblast differentiation, including Nrf2. Exp Cell Res. 2003;288:288–300.
Khoshniat S, Bourgine A, Julien M, Weiss P, Guicheux J, Beck L. The emergence of phosphate as a specific signaling molecule in bone and other cell types in mammals. Cell Mol Life Sci. 2011;68:205–18.
•• Michigami T, Kawai M, Yamazaki M, Ozono K. Phosphate as a signaling molecule and its sensing mechanism. Physiol Rev. 2018;98:2317–48. Most up-to-date and comprehensive review on Pi sensing and Pi sensors in mammals and other species.
Julien M, Magne D, Masson M, Rolli-Derkinderen M, Chassande O, Cario-Toumaniantz C, et al. Phosphate stimulates matrix Gla protein expression in chondrocytes through the extracellular signal regulated kinase signaling pathway. Endocrinology. 2007;148:530–7.
Julien M, Khoshniat S, Lacreusette A, Gatius M, Bozec A, Wagner EF, et al. Phosphate-dependent regulation of MGP in osteoblasts: role of ERK1/2 and Fra-1. J Bone Miner Res. 2009;24:1856–68.
Khoshniat S, Bourgine A, Julien M, Petit M, Pilet P, Rouillon T, et al. Phosphate-dependent stimulation of MGP and OPN expression in osteoblasts via the ERK1/2 pathway is modulated by calcium. Bone. Elsevier Inc. 2011;48:894–902.
Kimata M, Michigami T, Tachikawa K, Okada T, Koshimizu T, Yamazaki M, et al. Signaling of extracellular inorganic phosphate up-regulates cyclin D1 expression in proliferating chondrocytes via the Na(+)/Pi cotransporter Pit-1 and Raf/MEK/ERK pathway. Bone. 2010;47:938–47.
Yamazaki M, Ozonoa K, Okada T, Tachikawa K, Kondou H, Ohata Y, et al. Both FGF23 and extracellular phosphate activate Raf/MEK/ERK pathway via FGF receptors in HEK293 cells. J Cell Biochem. 2010;111:1210–21.
Chavkin NW, Chia JJ, Crouthamel MH, Giachelli CM. Phosphate uptake-independent signaling functions of the type III sodium-dependent phosphate transporter, PiT-1, in vascular smooth muscle cells. Exp Cell Res. Elsevier. 2015;333:39–48.
• Bon N, Couasnay G, Bourgine A, Sourice S, Beck-Cormier S, Guicheux J, et al. Phosphate (Pi)-regulated heterodimerization of the high-affinity sodium-dependent Pi transporters PiT1/Slc20a1 and PiT2/Slc20a2 underlies extracellular Pi sensing independently of Pi uptake. J Biol Chem. 2018;293:2102–14. First demonstration that Pi-dependent ERK signaling depends both on PiT1 and PiT2, and that low-abundant PiT1-PiT2 heterodimers are Pi-responsive.
Chang S, Yu K, Lee Y, An G, Beck G, Colburn N, et al. Elevated inorganic phosphate stimulates Akt-ERK1/2-Mnk1 signaling in human lung cells. Am J Respir Cell Mol Biol. 2006;35:528–39.
• Chande S, Bergwitz C. Role of phosphate sensing in bone and mineral metabolism. Nat Rev Endocrinol. 2018:1–19. Extended review on Pi sensing with a strong focus on clinical aspects.
Qi W, Baldwin SA, Muench SP, Baker A. Pi sensing and signalling: from prokaryotic to eukaryotic cells. Biochem Soc Trans. 2016;44:766–73.
Saiardi A, Erdjument-Bromage H, Snowman AM, Tempst P, Snyder SH. Synthesis of diphosphoinositol pentakisphosphate by a newly identified family of higher inositol polyphosphate kinases. Curr Biol. 1999;9:1323–6.
Saiardi A, Nagata E, Luo HR, Snowman AM, Snyder SH. Identification and characterization of a novel inositol hexakisphosphate kinase. J Biol Chem. 2001;276:39179–85.
Norbis F, Boll M, Stange G, Markovich D, Verrey F, Biber J, et al. Identification of a cDNA/protein leading to an increased Pi-uptake in Xenopus laevis oocytes. J Membr Biol. 1997;156:19–24.
Kestenbaum B, Glazer NL, Köttgen A, Felix JF, Hwang S-J, Liu Y, et al. Common genetic variants associate with serum phosphorus concentration. J Am Soc Nephrol. 2010;21:1223–32.
Gu C, Nguyen H-N, Hofer A, Jessen HJ, Dai X, Wang H, et al. The significance of the bifunctional kinase/phosphatase activities of diphosphoinositol pentakisphosphate kinases (PPIP5Ks) for coupling inositol pyrophosphate cell signaling to cellular phosphate homeostasis. J Biol Chem. 2017;292:4544–55.
Ichikawa S, Austin AM, Gray AK, Econs MJ. A Phex mutation in a murine model of X-linked hypophosphatemia alters phosphate responsiveness of bone cells. J Bone Miner Res. 2012;27:453–60.
Ichikawa S, Gerard-O’Riley RL, Acton D, McQueen AK, Strobel IE, Witcher PC, et al. A mutation in the Dmp1 gene alters phosphate responsiveness in mice. Endocrinology. 2017;158:470–6.
Kavanaugh MP, Miller DG, Zhang W, Law W, Kozak SL, Kabat D, et al. Cell-surface receptors for gibbon ape leukemia virus and amphotropic murine retrovirus are inducible sodium-dependent phosphate symporters. Proc Natl Acad Sci U S A. 1994;91:7071–5.
Miller DG, Miller AD. A family of retroviruses that utilize related phosphate transporters for cell entry. J Virol. 1994;68:8270–6.
O’Hara B, Johann SV, Klinger HP, Blair DG, Rubinson H, Dunn KJ, et al. Characterization of a human gene conferring sensitivity to infection by gibbon ape leukemia virus. Cell Growth Differ. 1990;1:119–27.
Van Zeijl M, Johann SV, Closs E, Cunningham J, Eddy R, Shows TB, et al. A human amphotropic retrovirus receptor is a second member of the gibbon ape leukemia virus receptor family. Proc Natl Acad Sci U S A. 1994;91:1168–72.
Miller DG, Edwards RH, Miller AD. Cloning of the cellular receptor for amphotropic murine retroviruses reveals homology to that for gibbon ape leukemia virus. Proc Natl Acad Sci U S A. 1994;91:78–82.
Wagner CA, Hernando N, Forster IC, Biber J. The SLC34 family of sodium-dependent phosphate transporters. Pflugers Arch. 2013;466:139–53.
Forster IC, Hernando N, Biber J, Murer H. Molecular aspects of medicine. Mol Asp Med. 2013 ed. 2013;34:386–95.
Miyamoto K, Tatsumi S, Segawa H, Morita K, Nii T, Fujioka A, et al. Regulation of PiT-1, a sodium-dependent phosphate co-transporter in rat parathyroid glands. Nephrol Dial Transplant. 1999;14(Suppl 1):73–5.
Miyamoto K, Ito M, Segawa H, Kuwahata M. Secondary hyperparathyroidism and phosphate sensing in parathyroid glands. J Med Investig. 2000;47:118–22.
Tatsumi S, Segawa H, Morita K, Haga H, Kouda T, Yamamoto H, et al. Molecular cloning and hormonal regulation of PiT-1, a sodium-dependent phosphate cotransporter from rat parathyroid glands. Endocrinology. 1998;139:1692–9.
Bourgine A, Colombeix C, Couasnay G, Masson M, Weiss P, Beck-Cormier S, et al. Involvement of PiT1 and PiT2 in the phosphate sensing in osteoblastic cells. Bone. 2012;50:S70.
Salaün C, Gyan E, Rodrigues P, Heard JM. Pit2 assemblies at the cell surface are modulated by extracellular inorganic phosphate concentration. J Virol. 2002;76:4304–11.
Salaün C, Maréchal V, Heard JM. Transport-deficient Pit2 phosphate transporters still modify cell surface oligomers structure in response to inorganic phosphate. J Mol Biol. 2004;340:39–47.
Yamasaki S, Yagishita N, Tsuchimochi K, Kato Y, Sasaki T, Amano T, et al. Resistance to endoplasmic reticulum stress is an acquired cellular characteristic of rheumatoid synovial cells. Int J Mol Med. 2006;18:113–7.
•• Geng Y, Mosyak L, Kurinov I, Zuo H, Sturchler E, Cheng TC, et al. Structural mechanism of ligand activation in human calcium-sensing receptor. Elife. 2016;5:e13662 First demonstration of the presence of PO 4 binding sites on the CaSR that may play a role either on Pi sensing or Pi homeostasis.
Sabbagh Y, O’Brien SP, Song W, Boulanger JH, Stockmann A, Arbeeny C, et al. Intestinal npt2b plays a major role in phosphate absorption and homeostasis. J Am Soc Nephrol. 2009;20:2348–58.
Berndt T, Thomas L, Craig T, Sommer S, Li X, Bergstralh E, et al. Evidence for a signaling axis by which intestinal phosphate rapidly modulates renal phosphate reabsorption. Proc Natl Acad Sci U S A. 2007;104:11085–90.
Kumar R. Phosphate sensing. Curr Opin Nephrol Hypertens. 2009;18:281–4.
Sabbagh Y, Schiavi SC. Role of NPT2b in health and chronic kidney disease. Curr Opin Nephrol Hypertens. 2014;23:377–84.
Tenenhouse HS, Martel J, Gauthier C, Zhang M, Portale AA. Renal expression of the sodium/phosphate cotransporter gene, Npt2, is not required for regulation of renal 1α-hydroxylase by phosphate. Endocrinology. Endocrine Soc. 2001;142:1124–9.
Battini JL, Rasko JE, Miller AD. A human cell-surface receptor for xenotropic and polytropic murine leukemia viruses: possible role in G protein-coupled signal transduction. Proc Natl Acad Sci U S A. 1999;96:1385–90.
•• Giovannini D, Touhami J, Charnet P, Sitbon M, Battini J-L. Inorganic phosphate export by the retrovirus receptor XPR1 in metazoans. Cell Rep. The Authors. 2013;3:1866–73. Identification and characterization of the first Pi exporter in mammals.
Ghillebert R, Swinnen E, De Snijder P, Smets B, Winderickx J. Differential roles for the low-affinity phosphate transporters Pho87 and Pho90 in Saccharomyces cerevisiae. Biochem J. 2011;434:243–51.
Hürlimann HC, Pinson B, Stadler-Waibel M, Zeeman SC, Freimoser FM. The SPX domain of the yeast low-affinity phosphate transporter Pho90 regulates transport activity. EMBO Rep. 2009;10:1003–8.
•• Wild R, Gerasimaite R, Jung JY, Truffault V, Pavlovic I, Schmidt A, et al. Control of eukaryotic phosphate homeostasis by inositol polyphosphate sensor domains. Science. 2016;352:986–90. Essential role of intracellular inositol polyphosphates in controlling intracelluar Pi homeostasis.
Ansermet C, Moor MB, Centeno G, Auberson M, Hu DZ, Baron R, et al. Renal Fanconi syndrome and hypophosphatemic rickets in the absence of xenotropic and polytropic retroviral receptor in the nephron. J Am Soc Nephrol. 2017;28:1073–8.
Funding
This work was supported by grants from Institut National de la Santé et de la Recherche Médicale (INSERM), Région des Pays de la Loire (grants “Nouvelle Equipe/Nouvelle Thématique”, “Senseo,” and “Adipos”).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
Nina Bon, Sarah Beck-Cormier, and Laurent Beck each declare no potential conflicts of interest.
Human and Animal Rights and Informed Consent
This article does not contain any studies with human or animal subjects performed by any of the authors.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This article is part of the Topical Collection on Molecular Control of Phosphorus Homeostasis
Rights and permissions
About this article
Cite this article
Bon, N., Beck-Cormier, S. & Beck, L. Interplay Between FGF23, Phosphate, and Molecules Involved in Phosphate Sensing. Curr Mol Bio Rep 5, 1–7 (2019). https://doi.org/10.1007/s40610-019-0109-2
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40610-019-0109-2