Abstract
Purpose of Review
Since the nineteenth century, the surgical methods used to perform open cervical thyroidectomy have improved significantly, resulting in substantially reduced rates of mortality and morbidity. The most up-to-date techniques today now focus on the need to limit the extent of any visible scarring, which requires that surgeons make their incisions in locations which minimize their likelihood of being noticed.
Recent Findings
During the past two decades, several remote access approaches have been developed for use in the field of endoscopic and robotic thyroidectomy, and these have proved a popular alternative to open surgery because the results are much more visually appealing (Miccoli et al. J Endocrinol Investig. 22(11):849–51, 1999; Ikeda et al. Surg Endosc Other Interv Tech. 16(1):92–5, 2002; Choe et al. World J Surg. 31(3):601–6, 2007; Wang et al. Surg Endosc. 29(1):192–201, 2015). However, even with these remote techniques, it is still possible to see the scars where the incisions were made; to address this issue, the novel thyroid treatment technique of natural orifice transluminal endoscopic surgery (NOTES) has therefore been developed (Witzel et al. Surg Endosc Other Interv Tech. 22(8):1871–5, 2008; Benhidjeb Surg Endosc. 23(5):1119–20, 2009).
Summary
With this new technique, the problem of scarring is eliminated completely, but while this benefit makes the procedure very attractive, it is still considered to be an experimental form of treatment because of the limitations which applied to the earlier sublingual technique of thyroidectomy (Wilhelm et al. World J Surg. 35(3):543–51, 2011; Karakas et al. Surgery. 150(1):108–15, 2011; Wilhem et al. Transl Cancer Res. 5(7):S1531–0, 2016). The oral vestibular approach has since undergone further development, with the clinical outcomes proving to be superior to earlier techniques (Nakajo et al. Surg Endosc. 27(4):1105–10, 2013; Wang et al. Surg (United States). 155(1):33–8, 2014; Anuwong World J Surg. 40(3):491–7, 2016).
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
The Development of Minimally Invasive Thyroidectomy
The work of Ganger in 1996 [1] marked a turning point in thyroid surgery, with minimally invasive techniques thereafter gaining attention. A number of approaches were proposed in order to make improvements to endoscopic thyroidectomy procedures, and some of these proved very successful [2,3,4,5]. Their acceptance came about due to the lack of scarring on the neck—a problem which was solved by instead making the incisions at a location which was much less painful and prone to bleeding and which would also aid faster recovery times. However, for these minimally invasive thyroidectomy methods to succeed, there are certain conditions which must be taken into consideration. First of all, it is important to minimize the distance from the incision to the thyroid. Longer distances make it more likely that surgery instrument collisions will occur; shorter distances for flap dissection lower the risk of trauma caused by gaining access. The next key point is that the incisions should not be made on a readily visible part of the body; hiding the incision is one way to achieve improved cosmetic outcomes. However, when selecting the incision site, it must also be remembered that anatomical and operative visibility are critical to ensure safety; the internal jugular vein, carotid artery, or brachial plexus must not be endangered at any point during the procedure. It should also be possible to remove the specimen without disruption achieving a safe oncological outcome. Finally, the cost of the procedure must not be prohibitive, and the technique must be sufficiently straightforward that it can be quickly learned and performed by any competent and experienced surgeon.
Rationale and Development of Transoral Thyroidectomy
There are a number of different remote access approaches to thyroidectomy, but some of these, such as the BABA or axilla techniques, cannot be considered wholly non-invasive because it is necessary to dissect substantial areas of flap from the breast or axilla, extending as far as the thyroid gland [3,4,5,6]. This can lead to patients experiencing paresthesia in this area following the procedure, which can cause discomfort and a reduction in their quality of life. Moreover, the distance from the incision to the thyroid is relatively lengthy for these techniques, increasing the risk of instrument collision as mentioned earlier.
These issues can be addressed by introducing a transoral approach. There are a number of reasons why such a method might provide superior outcomes. Obtaining access via the mouth allows a much shorter distance to the thyroid than other endoscopic or robotic techniques, thus eliminating the risks associated with greater distances, and when the incision is made inside the mouth, it is hidden from the observer and thus provides the best cosmetic results. Furthermore, the surgeon is able to gain a top-down perspective which offers the advantage of being very clear anatomically, easy to get used to, and not dissimilar to an inverted view of open surgery. This makes the technique easy to learn, and there is no need for any special instruments to carry out the procedure. Moreover, the approach makes use of a midline technique with equal access to the right and left paratracheal regions, and therefore, no additional incisions are necessary even when performing a total thyroidectomy or central lymph node dissection.
Evidence for Transoral Endoscopic Thyroidectomy
Sublingual Approach
The concept of thyroid natural orifice transluminal endoscopic surgery (NOTES) was investigated by Witzel et al., who experimented with transoral endoscopic thyroidectomies by operating on two fresh cadavers and ten live pigs [7]. One initial 10-mm incision was made in the sublingual region, while two further 3.5-mm incisions were made in order to hold a pair of 3.5-mm trocars on the neck to perform the triangulation of the rigid instruments during the procedure. The procedure itself made use of an axilloscope and ultrasonic shears; there was no bleeding observed in the case of the live pigs, and no complications were reported.
Another approach, transoral partial parathyroidectomy (TOPP), was presented by Karakas et al. [8, 9]. This technique involved the use of a cervicoscope which was positioned in front of the trachea, but took a more dorsal position than in the method of Witzel et al. described above. Ten human cadavers, ten live pigs, and two live patients were involved in the experimental procedure. The two patients who participated were exhibiting cases of primary hyperparathyroidism; following the treatment, one patient was later observed to have developed a transient palsy of the right hypoglossal nerve. Karakas et al. continued to develop their approach and carried out a subsequent study in 2014 in which a total of 85 parathyroid adenoma patients were invited for treatment using the TOPP procedure. Five of these patients accepted the offer. The outcomes of the trial were not especially encouraging: in two cases, the procedure had to be switched to open surgery, and in one of those cases, the patient later developed transient recurrent laryngeal nerve (RLN) palsy. In another case, a patient suffered a transient injury to the right hypoglossal nerve. It was concluded that the technique did not appeal to patients, and the high complication rate called into question its feasibility when using the equipment and instrumentation currently available.
Combined Sublingual and Oral Vestibular Approach
Benhijeb et al. [10] provided the first technique which combined elements of the sublingual and oral vestibular approaches. In their transoral video-assisted thyroidectomy (TOVAT), they used five human cadavers to carry out their experimental surgery. The procedure involved the creation of one 5-mm incision and two 3-mm incisions in the oral vestibule and the floor of the mouth, respectively, so that trocars could be put in place. Carbon dioxide was then insufflated at a pressure of 4–6 mmHg. The cadavers were dissected once the procedure was complete so that the outcome and safety of the procedure could be evaluated.
Meanwhile, Wilhelm et al. performed an experimental procedure quite similar to TOVAT which involved a group of eight patients. The name of the technique used was endoscopic minimally invasive thyroidectomy (eMIT) [11,12,13]. The procedure required the creation of a 10-mm center port along with a 5-mm port positioned at the oral vestibule. The findings reported that in three cases, the procedure had to be switched to open surgery due to problems relating to size. In two cases, the patients subsequently developed RLN palsy, which was transient for one patient and permanent in the other. In three other cases, the patients suffered mental nerve damage. This particular research was followed by a twin-center study which enjoyed the participation of medical facilities from China and Germany [14] and focused on 96 eMIT cases. The results showed that 15 of the patients suffered mental nerve damage, six patients developed infections around the site of the sublingual incision or the neck, three patients had to undergo open surgery, one patient suffered transient RLN injury, and one suffered permanent RLN injury.
While combination approaches which make use of the sublingual route have attracted considerable attention, they have not achieved widespread acceptance because of the complexity of the techniques involved and the rather high rate of complications [15,16,17,18,19]. Although a number of researchers believe that combination approaches still have potential, the technique is rare in clinical practice [20, 21].
Oral Vestibular Approach
The first all oral vestibular procedure was conceived by Richmon and Tufano et al. [22], who carried out a transoral robotic-assisted thyroidectomy (TRAT) and central neck dissection on a cadaver with three ports (one in the midline and two at the oral commissures) and CO2 insufflation. Nakajo et al. [23] used a similar procedure called transoral video-assisted neck surgery (TOVANS) with the involvement of eight patients. In this technique, a single incision of 2.5 cm was made in the center of the oral vestibule. K-wire was used to support the skin, and the approach did not involve the use of any gas. There was only one case of RLN injury reported, but all of the patients in the study experienced paresthesia in the chin region for up to 6 months, with mental nerve damage also reported. A different vestibular technique was used by Wang et al. [24] in a study which had 12 participating patients. This technique differed insofar as three vestibular ports were employed, while carbon dioxide was the gas used for insufflation. The main complications reported were mental nerve injuries, which arose in all cases, while two of the patients also developed skin ecchymosis.
The next procedure to be developed was the transoral endoscopic thyroidectomy vestibular approach (TOETVA) which was performed by Anuwong [25] in a trial with 60 patients. The procedure required the creation of three ports at the oral vestibule. In this trial, it was noteworthy that none of the patients developed mental nerve injuries. Two patients experienced transient RLN palsy, but this was short-lived. The TOETVA procedure has since been performed in around 500 cases at the Police General Hospital in Bangkok. TOETVA has also been carried out in the USA, with Udelsman et al. [26] performing it in seven cases which included two parathyroidectomies and five thyroidectomies. These cases passed successfully without complications. Jitpratoom et al. [27] made a comparison of TOETVA with open thyroidectomies using 46 cases of the former and 49 of the latter in order to assess the overall safety levels when emphasizing the potential problem of Graves’ disease. The findings confirmed that although the operative time was longer for TOETVA, these patients benefitted from lower levels of pain experienced than the open surgery group. Other parameters which were evaluated showed no significant differences. Adding further support to these results was an Italian study by Dionigi et al. involving 15 TOETVA cases which did not report any complications [28].
Transtracheal Approach
The transtracheal approach was first described in detail by Liu et al. [29] in 2015, who carried out total transtracheal endoscopic thyroidectomy in a study involving 14 beagles and three pigs. A 4.2-mm flexible fiber optic bronchoscope was used along with endoscopic biopsy forceps and laparoscopic curved instruments; the scope was inserted close to the orotracheal tube, and then, a further incision was made in the anterior tracheal wall which thereby permitted access to the thyroid gland. Endostitch was used to seal the anterior tracheal wall upon completion of the procedure. The study involved a total of 26 thyroidectomies and 8 partial thyroidectomies, and no mortality or morbidity was reported during the initial 5 days following surgery. However, the findings in studies involving animals may not be applicable in the human context.
It is apparent from these examples that sublingual techniques are no longer actively used, while trans-tracheal techniques have not yet moved beyond practice with animals. Thyroid NOTES techniques have only been successful in the context of oral vestibular surgery, but the potential of the TOETVA approach has drawn increasing levels of interest [30,31,32,33].
Evidence for Transoral Robotic Thyroidectomy
Transoral robotic surgery offers a number of advantages, among which are the use of 3D visualization and magnification, and the flexible arm which can be operated via console. Attempts to make use of this technology have involved seeking ways to gain remote access to the thyroid via several different approaches, entering through the breast or axilla, or using the BABA or facelift techniques [34,35,36]. For example, TRAT was performed in 2011 by Richmon et al. using cadavers [22]. One midline sublingual port was used alongside two lateral vestibular ports, but the authors reported that camera movements at the sublingual port were inadequate and unsatisfactory. To address this issue, the technique was altered to use three vestibular ports; tests using a pair of cadavers showed that this improved the process [37]. The next robotic vestibular technique to be reported was transoral periosteal thyroidectomy (TOPOT), performed by Lee et al. [38]. Seven cadavers were used in the trial, along with ten live pigs, and also four human patients. One of the patients suffered a torn mental nerve while two others had their mental nerves stretched. Further research is proceeding, but to date, the most significant impediment to the success of transoral robotic thyroidectomy is the tendency for nerve injuries to result as a consequence of the robotic arm and large trocars [39, 40].
Scarless Thyroidectomy Conclusion
While several procedures have been described, it is only for TOETVA that significant quantities of published evidence can be provided. It is apparent that although the number of competed procedures remains limited, the level of safety and feasibility observed thus far would indicate that the technique has a positive future. It is, however, also necessary to ensure that with any novel procedure, there are clear benefits to be derived by the patients. Among these potential benefits, safety is the overriding concern, and hence, it is necessary to acquire sufficient clinical evidence to support claims that the technique is relatively risk-free before it will enter widespread use. For example, much of the research into transoral endoscopic thyroidectomies has focused upon animals or cadavers, so further work within a human context would be necessary to provide such evidence. The transoral approach does provide a number of benefits, but these are partly offset by the risk resulting from the need to make incisions in the mouth, because there is a strong possibility that bacterial infections can result, causing abscesses or compression of the airway. These potential drawbacks are the main cause of doubt regarding the suitability of transoral thyroidectomy [41]. In the case of sublingual approaches, the evidence from clinical results indicates that there is a very high rate of complications and infections, again bringing the suitability of the method into question [11, 14]. For the oral vestibular approach, however, the literature shows little evidence of infection proving problematic. For this reason, oral vestibular techniques such as TOETVA would seem to minimize complications and the risk of infection, and hence offer the potential to provide the best outcomes for patients [23,24,25, 28, 31,32,33].
However, despite this positive outlook for TOETVA, one issue concerns the removal of the specimen, since it must be extracted through a 10-mm incision made at the oral vestibule [41]. The specimen must invariably be placed in an endobag for this process. The size which would normally be expected for the thyroid is up to 40 mm, and this can be extracted using forceps and sponges by gently pushing and pulling while taking care not to rupture the thyroid capsule. When larger glands are involved, however, this technique is no longer feasible, and instead, it is necessary to make additional two or three 10-mm incisions in the thyroid capsule inside the endobag making use of endoscopic view, and avoiding the tumor. With this approach, the specimen can be removed through the midline vestibule incision, and therefore, it is suitable for benign tumors; however, occult malignancy can result on any cancer nodule [42]. If Graves’ disease is present, then cancer becomes unlikely, thus removing this particular risk in using the TOETVA procedure. However, if thyroid carcinoma has been identified prior to surgery, it would only be appropriate to perform the TOETVA procedure in the case of very small cancer nodules where the size does not exceed 20 mm, on account of the limitations of the incision size. On the other hand, the anatomical view which is available in carrying out the TOETVA procedure makes it possible to perform central lymph node dissection without difficulty. However, it will be necessary to study TOETVA further to determine whether it is likely to be beneficial to thyroid cancer patients [43].
TOETVA Surgical Technique
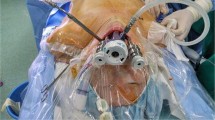
The TOETVA procedure can be described as follows [44]. In the initial stage, a nasotracheal tube is inserted and the patient placed in a supine position, with the neck slightly more extended than would be the case with conventional open thyroidectomy. The eyes and airway are protected from potential irritation using Opsite positioned from the top of the upper lip until the forehead, as shown in Fig. 1. In some situations, it would also be feasible to use orotracheal intubation, although this can restrict the movements of the lateral instruments during the procedure. It is also possible to use an intraoperative nerve monitor [45] (Fig. 2). In order to position the first camera, a 2 to 2.5-cm horizontal incision is made at the vestibule, at two thirds of the distance from the lip to the frenulum (Fig. 3). A monopolar Bovie is used to halt bleeding at the mucosa, and then, the mentalis muscle is cut. It is important to hold the Bovie at 45° to ensure that the skin is not penetrated. The dissection depth should be checked frequently by palpating around the tip of the chin; at the correct depth, it should be possible to feel the tip of the Bovie beneath the skin, along with some subcutaneous tissue. In this case, we perform hydrodissection using a Veres needle and a 500 ml NSS solution with 1 mg of adrenaline. It is normal to use 50 ml per case.
The first infiltration is made at the tip of the chin; if this is done correctly, it begins to weal up (Fig. 4). The fingers can then be used to raise the skin while pushing the Veress down to a sternal notch, allowing the solution to infiltrate all over the anterior neck, and between the two sides of the sternocleidomastoid muscles. Once this has been done, a Kelly clamp can be put in place to create a dilated tract around the chin. When the clamp fulcrum sits at the tip of the chin, it will ensure that the end of the Kelly clamp is located just above the cricoid cartilage (Fig. 5).
The tract must be sufficiently dilated to allow the insertion of a 10-mm port, but before the port is put in place, a dilator should be used to dissect the subplatysmal plane in three directions, around the region in which the fluid had previously been injected (Fig. 6). The fingers should be used to act against the force exerted at the rim of the mandible, while the palm of the hand is used to ensure that the dissection is not too deep in the area below the clavicles.
When the dissection is complete, a 10-mm port is inserted and an insufflation unit connected. A 2/0 silk sling is used to hold up the skin and the subcutaneous tissue, placed 1 cm below the outside end of the camera port (Fig. 7). This benefit of doing this is that it ensures that the overhanging edge of the skin does not obstruct the port, thus making it easier to subsequently dissect the tissue in front of the port when required.
It is then necessary to make a lateral working port, taking into consideration the presence of two important elements: a mental nerve and a canine tooth. The ideal ergonomic port position, which will reduce the risk of mental nerve damage, should be located at the end of the imaginary line which runs perpendicular from the incisor towards the top of the inside portion of the lower lip.
A superficial vertical incision is then made only to the mucosa, followed once again by hydrodissection, but on this occasion, the needle is pushed to the edge of a mandible and a 5-mm port inserted. Maintaining awareness of the depth of the skin, this procedure is repeated on the other side of the mouth, resulting in the creation of three carefully aligned ports (Fig. 8).
The pressure is then set to 6 mmHg and the flow to 15–25 l/min. Upon insertion of a 30° scope, three holes of the subplatysmal plane become visible (Fig. 9). A Bovie or a vascular sealing tool can then be used to clear away the tissue surrounding the port so that the flap dissection can be completed. The boundary of this flap dissection runs down to the clavicle and the medial border of the sides of the sternocleidomastoid muscles.
The midline of the strap muscles can then be carefully opened, layer by layer, until the thyroid gland is reached, as far as the level of the cricoid cartilage (Fig. 10). The gland from the strap muscles can be further mobilized laterally until a carotid artery is reached. The 2/0 silk is used to construct a lateral hanging stitch from the outside, and the strap muscle is then wrapped to the greatest extent possible (Fig. 11).
Once the lateral mobilization is complete, the cricoid cartilage must be located. A grasper is used to raise a pyramidal lobe, revealing an avascular pre-tracheal fascia. A vascular sealing device is then used to carry out an isthmectomy from this fascia, moving downwards along the trachea to reach the end of the thyroid gland (Fig. 12).
Upon completion of the isthmectomy, a Joll’s space (or cricothyroid space) is approached while using the grasper to hold and raise the superior pole towards the contralateral side (Fig. 13). The bottom of this space houses the external branch of superior laryngeal nerve (EBSL). An energy device is then used to cut the superior thyroid vessels, and the thyroid is pushed to the contralateral side. The parathyroid is located just below the thyroid (Fig. 14). The parathyroid gland is then medially dissected with great care in order to maintain its blood supply and is then pushed down, away from the plane of dissection.
The recurrent laryngeal nerve must then be identified, typically dorsal to the inferior parathyroid gland or ventral to the superior one (Fig. 15). It is located at the insertion at the anterolateral part of the cricothyroid cartilage. This nerve is then pushed down, and the rest of Berry’s ligament is dissected (Fig. 16). An endobag is employed for the removal of the specimen via the 2-cm central incision. After going inside the endoscopic view once again to halt the bleeding, the strap muscles can be re-approximated using an absorbable barbed or plain suture (Fig. 17). Finally, the mentalis muscle and oral mucosa are closed using 4/0 absorbable suture material (Fig. 18).
Once the procedure has been completed, the chin should be supported using a pressure dressing or a jaw bra for the subsequent 24-h period (Fig. 19). The patient should have commenced a liquid diet from the day of surgery, progressing to a soft diet on the first day following the operation.
Conclusion
On the basis of evidence provided directly by the author, and from examination of the literature, it is clear that TOETVA is a safe procedure which has successfully passed its experimental phase and should therefore be deemed suitable for clinical practice. The outcomes offered by the practice are superior to the alternatives in terms of cosmetic appeal and oncological efficacy. The procedure can be performed on suitable candidates with minimal risk of complications and thus represents an attractive alternative to the conventional approach of open thyroidectomy.
References
Papers of particular interest, published recently, have been highlighted as: •• Of major importance
Gagner M. Endoscopic subtotal parathyroidectomy in patients with primary hyperparathyroidism. Br J Surg. 1996;83(6):875.
Miccoli P, Berti P, Conte M, Bendinelli C, Marcocci C. Minimally invasive surgery for thyroid small nodules: preliminary report. J Endocrinol Investig. 1999;22(11):849–51.
Ikeda Y, Takami H, Niimi M, Kan S, Sasaki Y, Takayama J. Endoscopic thyroidectomy and parathyroidectomy by the axillary approach: a preliminary report. Surg Endosc Other Interv Tech. 2002;16(1):92–5.
Choe JH, Kim SW, Chung KW, Park KS, Han W, Noh DY, et al. Endoscopic thyroidectomy using a new bilateral axillo-breast approach. World J Surg. 2007;31(3):601–6.
Wang C, Feng Z, Li J, Yang W, Zhai H, Choi N, et al. Endoscopic thyroidectomy via areola approach: summary of 1,250 cases in a single institution. Surg Endosc. 2015;29(1):192–201.
Lee KE, Kim E, Koo DH, Choi JY, Kim KH, Youn YK. Robotic thyroidectomy by bilateral axillo-breast approach: review of 1026 cases and surgical completeness. Surg Endosc. 2013;27(8):2955–62.
Witzel K, Von Rahden BHA, Kaminski C, Stein HJ. Transoral access for endoscopic thyroid resection. Surg Endosc Other Interv Tech. 2008;22(8):1871–5.
Karakas E, Steinfeldt T, Gockel A, Schlosshauer T, Dietz C, Jäger J, et al. Transoral thyroid and parathyroid surgery—development of a new transoral technique. Surgery. 2011;150(1):108–15.
Karakas E, Steinfeldt T, Gockel A, Westermann R, Kiefer A, Bartsch DK. Transoral thyroid and parathyroid surgery. Surg Endosc. 2010;24(6):1261–7.
Benhidjeb T, Wilhelm T, Harlaar J, Kleinrensink GJ, Schneider TAJ, Stark M. Natural orifice surgery on thyroid gland: totally transoral video-assisted thyroidectomy (TOVAT): report of first experimental results of a new surgical method. Surg Endosc. 2009;23(5):1119–20.
Wilhelm T, Metzig A. Endoscopic minimally invasive thyroidectomy (eMIT): a prospective proof-of-concept study in humans. World J Surg. 2011;35(3):543–51.
Karakas E, Steinfeldt T, Gockel A, Mangalo A, Sesterhenn A, Bartsch DK. Transoral parathyroid surgery—a new alternative or nonsense? Langenbeck's Arch Surg. 2014;399(6):741–5.
Wilhelm T, Metzig A. Video. Endoscopic minimally invasive thyroidectomy: first clinical experience. Surg Endosc. 2010;24(7):1757–8.
Wilhem T, Wu G, Teymoortash A, Güldner C, Günzel THS. Transoral endoscopic thyroidectomy: current state of the art—a systematic literature review and results of a bi-center study. Transl Cancer Res. 2016;5(7):S1531–0.
Dionigi G, Rovera F, Boni L. Commentary on transoral access for endoscopic thyroid resection: WWWitzel K, von Rahden BH, Kaminski C, Stein HJ (2008) Transoral access for endoscopic thyroid resection. Surg Endosc 22(8):1871–1875. Surg Endosc. 2009;23(2):454–5.
Miccoli P, Materazzi G, Berti P. Natural orifice surgery on the thyroid gland using totally transoral video-assisted thyroidectomy: report of the first experimental results for a new surgical method: are we going in the right direction? Surg Endosc. 2010;24(4):957–8.
Benhidjeb T, Witzel K, Stark M, Mann O. Transoral thyroid and parathyroid surgery: still experimental! Surg Endosc. 2011;25(7):2411–3.
Benhidjeb T. Transoral video-assisted thyroidectomy and its clinical implementation. J Laparoendosc Adv Surg Tech A. 2015;25(6):514–5.
Benhidjeb T. Transoral endoscopic thyroidectomy with central neck dissection. Chin Med J. 2015;128(13):1838.
Guo PY, Tang ZP, Ding ZH, Chu GL, Yao HS, Pan T, et al. Transoral endoscopic thyroidectomy with central neck dissection: experimental studies on human cadavers. Chin Med J. 2014;127(6):1067–70.
Woo SH. Endoscope-assisted transoral thyroidectomy using a frenotomy incision. J Laparoendosc Adv Surg Tech A. 2014;24(5):345–9 Available from: http://www.ncbi.nlm.nih.gov/pubmed/24809786.
Richmon JD, Pattani KM BT. Transoral robotic-assisted thyroidectomy: a preclinical feasibility study in 2 cadavers. Head Neck 2011;33(3):330–3.
Nakajo A, Arima H, Hirata M, Mizoguchi T, Kijima Y, Mori S, et al. Trans-oral video-assisted neck surgery (TOVANS). A new transoral technique of endoscopic thyroidectomy with gasless premandible approach. Surg Endosc. 2013;27(4):1105–10.
Wang C, Zhai H, Liu W, Li J, Yang J, Hu Y, et al. Thyroidectomy: a novel endoscopic oral vestibular approach. Surg (United States). 2014;155(1):33–8. Available from: https://doi.org/10.1016/j.surg.2013.06.010
•• Anuwong A. Transoral endoscopic thyroidectomy vestibular approach: a series of the first 60 human cases. World J Surg. 2016;40(3):491–7. This was the first successful series of TOETVA, which was demonstrated the feasiblity and safty of this technique to a clinical practice.
Udelsman R, Anuwong A, Oprea AD, Rhodes A, Prasad M, Sansone M, et al. Trans-oral vestibular endocrine surgery: a new technique in the United States. Ann Surg. 2016;264(6):e13–6.
Jitpratoom P, Ketwong K, Sasanakietkul T, Anuwong A. Transoral endoscopic thyroidectomy vestibular approach (TOETVA) for Graves’ disease: a comparison of surgical results with open thyroidectomy. Gland Surg. 2016;5(6):546–52 Available from: http://gs.amegroups.com/article/view/12529/13326.
Dionigi G, Bacuzzi A, Lavazza M, Inversini D, Boni L, Rausei S, et al. Transoral endoscopic thyroidectomy: preliminary experience in Italy. Updat Surg. 2017;69(2):225–34.
Liu E, Qadir Khan A, Niu J, Xu Z, Peng C. Natural orifice total transtracheal endoscopic thyroidectomy surgery: first reported experiment. J Laparoendosc Adv Surg Tech A. 2015;25(7):586–91.
Pai VM, Muthukumar P, Prathap A, Leo J, A. R. Transoral endoscopic thyroidectomy: a case report. Int J Surg Case Rep. 2015;12:99–101. Available from: https://doi.org/10.1016/j.ijscr.2015.04.010
Wang Y, Yu X, Wang P, Miao C, Xie Q, Yan H, et al. Implementation of intraoperative neuromonitoring for transoral endoscopic thyroid surgery: a preliminary report. J Laparoendosc Adv Surg Tech. 2016;26(12):965–71 Available from: http://online.liebertpub.com/doi/10.1089/lap.2016.0291.
Inabnet WB, Suh H, Fernandez-Ranvier G. Transoral endoscopic thyroidectomy vestibular approach with intraoperative nerve monitoring. Surg Endosc. 2017;31(7):3030.
Park J-O, Kim M-R, Kim DH, Lee DK. Transoral endoscopic thyroidectomy via the trivestibular route. Ann Surg Treat Res. 2016;91(5):269 Available from: https://synapse.koreamed.org/DOIx.php?id=10.4174/astr.2016.91.5.269.
Lobe TE, Wright SKIM. Novel uses of surgical robotics in head and neck surgery. J Laparoendosc Adv Surg Tech A. 2005;15(6):647–52.
Berber E, Bernet V, Fahey TJ, Kebebew E, Shaha A, Stack BC, et al. American Thyroid Association statement on remote-access thyroid surgery. Thyroid. 2016;26(3):331–7 Available from: http://online.liebertpub.com/doi/10.1089/thy.2015.0407.
Terris DJ, Singer MC, Seybt MW. Robotic facelift thyroidectomy: II. Clinical feasibility and safety. Laryngoscope. 2011;121(8):1636–41.
Richmon JD, Holsinger FC, Kandil E, Moore MW, Garcia JA, Tufano RP. Transoral robotic-assisted thyroidectomy with central neck dissection: preclinical cadaver feasibility study and proposed surgical technique. J Robot Surg. 2011;5(4):279–82.
Lee HY, You JY, Woo SU, Son GS, Lee JB, Bae JW, et al. Transoral periosteal thyroidectomy: cadaver to human. Surg Endosc. 2015;29(4):898–904.
Clark JH, Kim HY, Richmon JD. Transoral robotic thyroid surgery. Gland Surg. 2015;4(5):429–34 Available from: http://www.pubmedcentral.nih.gov/articlerender.fcgi?artid=4561656&tool=pmcentrez&rendertype=abstract.
Article O. Early experience of transoral thyroidectomy: comparison of robotic and endoscopic procedures. 2018;(September):17–24.
Livhits MJYM. Transoral endoscopic thyroidectomy is a novel experimental technique. Clin Thyroidol. 2017;29(1):19–21.
Jongekkasit I, Jitpratoom P. Transoral endoscopic thyroidectomy for thyroid cancer. Endocrinol Metab Clin NA. 2019;48(1):165–180. Available from: https://doi.org/10.1016/j.ecl.2018.11.009
•• Kim HK, Chai YJ, Dionigi G, Berber E. Transoral robotic thyroidectomy for papillary thyroid carcinoma: perioperative out comes of 100 consecutive patients. World J Surg. 2018;43(4):1038–46. https://doi.org/10.1007/s00268-018-04877-w. This study provides a safety and good outcomes for Transoral robotic thyroidectomy for papillary thyroid cancer.
Anuwong A, Sasanakietkul T, Jitpratoom P, Ketwong K, Kim HY, Dionigi G, et al. Transoral endoscopic thyroidectomy vestibular approach (TOETVA): indications, techniques and results. Surg Endosc. 2018;32(1):456–65.
Chen HCC, Lin KWY, Uen KLY. Application of transoral continuous intraoperative neuromonitoring in natural orifice transluminal endoscopic surgery for thyroid disease: a preliminary study. Surg Endosc. 2018;32(1):517–25.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no conflict of interest.
Human and Animal Rights and Informed Consent
This article does not contain any studies with human or animal subjects performed by any of the authors.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This article is part of the Topical Collection on Transoral Thyroid and Parathyroid Surgery
Rights and permissions
About this article
Cite this article
Jamikorn, T., Anuwong, A. Transoral Endoscopic Thyroidectomy (TOETVA). Curr Otorhinolaryngol Rep 7, 209–218 (2019). https://doi.org/10.1007/s40136-019-00250-0
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40136-019-00250-0