Abstract
Background
The novel concept of continuous intraoperative neuromonitoring (Cont-IONM) through stimulation of the vagal nerve has been used in thyroidectomies to prevent imminent injury of the recurrent laryngeal nerve (RLN). This article reports on this technology and the results of using transoral Cont-IONM in natural orifice transluminal endoscopic surgery for thyroid disease.
Methods
Cont-IONM of the RLN was achieved through automatic cyclical stimulation of the vagal nerve using a C2 monitor and delta stimulating electrode. During the operation, three vestibular incisions were made, and the stimulating electrode was transorally inserted, with its cable line lying outside the trocar. The vagal nerve was gently dissected, looped, and then enveloped by the electrode cuff. Electromyography (EMG) of the vocalis muscle was performed, and the alarm was set to activate when the EMG amplitude reduced by 50% and latency was prolonged by 10%. Demographic data and outcome variables, including incremental time required to achieve Cont-IONM, were obtained.
Results
A total of 20 patients (28 nerves at risk) undergoing a transoral endoscopic thyroidectomy vestibular approach were enrolled in this study. All Cont-IONM procedures were successfully completed. In all patients, the stimulation was set at 0.7 milliamps every 1 s, and Cont-IONM use was unassociated with any untoward neural, cardiovascular, or gastrointestinal sequelae. On average, the ipsilateral Cont-IONM procedure required 10.33 ± 2.57 min to complete. Except for one instance, no significant problems occurred with electrode displacement. In one patient, a combined EMG event occurred, which improved after releasing the thyroid retractor, and the patient had no vocal cord paralysis postoperatively.
Conclusion
Cont-IONM is feasible and safe to use during transoral endoscopic thyroidectomies and may assist in the early detection of adverse EMG changes, thereby preventing paralysis of the RLNs.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Intraoperative neuromonitoring (IONM) during thyroid surgery has gained widespread acceptance as an adjunct to the gold standard of visually identifying the recurrent laryngeal nerve (RLN) [1, 2], detecting RLN anatomic variations [3], predicting vocal cord function outcome [4, 5], and elucidating RLN injury mechanisms [6]. However, RLN injuries still occur in the time between the two nerve stimulations of intermittent IONM (Int-IONM) [7, 8]. Because most intraoperative RLN injuries occur during the combined phase of medial thyroid traction and RLN dissection [7, 8], a simple and safe procedure for the real-time monitoring of nerve function during this period is the most critical issue for surgeons. The novel concept of continuous IONM (Cont-IONM) through stimulation of the vagal nerve has been developed to provide continuous nerve integrity information and to potentially increase the level of nerve integrity scrutiny [9, 10]. It has been a useful tool for recognizing impending nerve injury and aborting the related maneuver to prevent nerve injury during traditional thyroid surgery.
Natural orifice transluminal endoscopic surgery (NOTES) for thyroid disease is a scarless operation with excellent cosmetic results [11]. However, it has some technical limitations, including an unusual vector of dissection, poor visibility, and limited surgical space, which make the identification and dissection of the RLN challenging. A MEDLINE search indicated that Cont-IONM has not been implemented in NOTES for thyroidectomies. We applied the entire Cont-IONM procedure in an animal study and subsequently in human beings. Here, we present the surgical technique and clinical results for the use of Cont-IONM in transoral endoscopic thyroidectomy in order to evaluate its feasibility and safety.
Materials and methods
From September to October 2016, we performed Cont-IONM of the vagal nerve in 20 consecutive patients undergoing transoral endoscopic thyroidectomy vestibular approach (TOETVA) at the Department of General Surgery at Chi Mei Medical Center (Tainan, Taiwan). All operations were performed by the same surgical group, with the routine implementation of transoral Cont-IONM of the vagal nerve. The surgical indications for these patients were as follows: benign solitary or multithyroid goiter, thyroid adenoma, follicular lesions (measuring ≤6.0 cm in their largest diameter, according to preoperative ultrasound evaluation), and early papillary thyroid malignancy (measuring ≤1 cm in their largest diameter, with the absence of cervical lymphadenopathy). In addition, all patients had no previous thyroid surgeries or cervical radiation history and exhibited a normally functioning RLN during a preoperative laryngoscopic examination. The study plan was reviewed and approved by our institutional ethical committee, and informed consent was obtained.
In all patients, an indirect laryngoscopic examination was performed to evaluate vocal cord motility after surgery and to check for the presence of vocal cord palsy. The primary outcome measures were the success rate and implementation time for Cont-IONM. The secondary outcome measures included whether the electromyography (EMG) signal of the vocalis muscle correlated with the operative manipulation and surgical outcomes.
Surgical technique
Anesthesia and endotracheal tubes
All operations were performed under general anesthesia with nasal endotracheal tube (ETT) insertion. A single dose of muscle relaxant was administered in the induction period only. The laryngeal electrode (Select; inomed Medizintechnik GmbH) was attached to the appropriately sized ETT, which was in contact with the true vocal cords. The position of the electrode was routinely rechecked through laryngofiberoscopy, after the neck was placed at full extension.
Establishing the IONM instrument
A C2 NerveMonitor (inomed Medizintechnik GmbH) was used for intermittent and continuous RLN neuromonitoring. A monopolar probe modified from a laparoscopic hook was used for intermittent neural stimulation. A delta electrode (inomed Medizintechnik GmbH) was used to monitor the repetitive electrical activities of the RLN and vagal nerve during TOETVA. Twisted pair needle electrodes, which were placed at the upper deltoid muscles and low anterior neck wall, played the roles of control and stimulus return, respectively. After completing the circuit of the IONM instrument, the surgeon performed a “tap test” (direct percussion of the larynx and observation of the resulting EMG wave on the screen [1]) to ensure recording of the artifact from the electrodes and confirming normal conduction across the neuromuscular junction.
Preliminary steps of TOETVA
The procedure was performed as described by Anuwong [12]. Three incisions were made in the oral vestibule, namely one 11-mm central incision for inserting the camera port and two 5-mm lateral incisions at the junction between the canine and premolar teeth for inserting the operating instruments. After creation of a premandibular space through blunt dissection and the injection of distension fluid, CO2 was insufflated, and the pressure was set at 6 mmHg. An anterior cervical subplatysmal space was created from the oral vestibule down to the sternal notch. Then, a thyroidectomy was endoscopically performed using conventional laparoscopic instruments and an ultrasonic device. First, the anterior thyroid surface was detached from the strap muscles and then the isthmus was divided. The lateral surface of the thyroid gland was also dissected, and the middle thyroid vein was divided.
Establishing the transoral Cont-IONM device (video also presented)
Step 1. Creating access to the ipsilateral carotid sheath area:
-
A.
Placement of bilateral percutaneous hanging sutures (penetraction of the contralateral sternothyroid muscle, if necessary).
-
B.
Outward retraction of ipsilateral hanging sutures and take-down of the superior thyroid lobe.
-
C.
Application of EndoGrab™ Port-Free Retractor (Virtual Ports, Ltd.) over the upper half of the thyroid (Fig. 1).
-
D.
Connection of the retractor clip to the contralateral percutaneous suture to retract the thyroid medially.
Step 2. Inserting the delta electrode (inomed Medizintechnik GmbH) into the operative field (Fig. 2):
-
A.
Insertion of the delta electrode into the operative field using forceps via the midline vestibular trocar (Fig. 2A).
-
B.
Withdrawal of the trocar from the vestibular wound (electrode not included; Fig. 2B).
-
C.
Reinsertion of the trocar (with an obstacle) so that the electrode lies outside the trocar (Fig. 2C).
-
D.
Withdrawal of the obstacle and reinsertion of the endoscope (Fig. 2D).
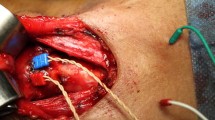
Step 3. Dissecting the vagal nerve (Fig. 3):
-
A.
Dissection of the carotid sheath for visualization of the vagal nerve.
-
B.
Dissection and identification of the vagal nerve (V1; Fig. 3A).
-
C.
360-degree dissection of the vagal nerve.
-
D.
Looping of the vagal nerve with the vessel loop (Fig. 3B).
Step 4. Positioning the delta electrode on the vagal nerve (Fig. 4):
-
A.
Lifting of the vessel loop and insertion of the delta electrode into the carotid space (Fig. 4A).
-
B.
Use of the open cuff of the delta electrode to envelop the nerve.
-
C.
Sliding of the delta electrode along the vagal nerve to secure its placement around the vagal nerve (Fig. 4B).
-
D.
Reinsertion of the delta electrode and associated vagal nerve into the carotid cavity.
A Insertion of the delta electrode into the operative field using forceps via the midline vestibular trocar. B Withdrawal of the trocar from the vestibular wound (electrode not included). C Reinsertion of the trocar (with an obstacle), with the electrode lying outside the trocar. D Withdrawal of the obstacle and preparation for the reinsertion of the endoscope
C2 NerveMonitor setup
After the Cont-IONM device was set up on the vagal nerve, the following thyroidectomy procedures were completed under the guidance of both audio and visual information from Cont-IONM. The surgeon used the delta electrode and hand-held modified monopolar probe to receive Cont-IONM and Int-IONM signals, respectively.
Continuous neural stimulation was performed using the delta electrode device. The stimulation was set at 0.7 mA every 1 s. This enabled the ongoing assessment of stimulation waveform amplitude and latency. The reference curve (baseline) was defined as a signal of ≥500 µV to guarantee a stable and reliable EMG signal. EMG of the vocalis muscle was checked, and the alarm was set to activate when the EMG amplitude was decreased by 50% and latency was prolonged by 10% [1, 14].
Intermittent neural stimulation was performed using a monopolar probe modified from a laparoscopic hook instrument; this was inserted through the 5-mm operating port, and the curved tip was placed in contact with the target nerve. IONM was attempted in a standardized four-step (V1/R1/R2/V2) manner, as described by Chiang et al. [13].
Assessment of nerve function and follow-up
All patients received a postoperative laryngoscopic examination 1–2 weeks postoperatively to check for the presence of vocal cord palsy. In cases of dysphonia with vocal cord injury, indirect laryngoscopy was also performed 1, 3, and 6 months later. Permanent nerve palsy was defined as persistent dysfunction and clinical dysphonia lasting 6 months postoperatively.
Data collection
Data regarding age, sex, body mass index (BMI), resected thyroid gland weight, indications for thyroidectomy, thyroid pathology, delta electrode setup time, RLN identification time, operating time, and incidence of permanent or temporary RLN palsy (RLNP) were recorded. BMI was calculated as the ratio of weight (kg) divided by the square of the height (m). The delta electrode setup time was defined as the period between contralateral retraction of the thyroid gland and complete placement of the delta electrode on the vagal nerve. Identification time of the RLN was defined as the period between the beginning of the search for the nerve in the tracheoesophageal groove and its dissection up to the point where the nerve entered the larynx. Operating time was defined as the time from skin preparation to closure of the skin incisions. Measurement of the RLNP rate was based on the number of RLNs at risk (NAR).
Results
Twenty-eight nerves were monitored in 20 patients (4 men and 16 women; age, 19–63 years; mean age, 42.05 ± 10.89 years) who underwent TOETVA for various thyroid diseases [7 (35%) malignancies and 13 (65%) benign lesions]. Total thyroidectomy was performed in 8 (40%) patients and hemithyroidectomy in 12 (60%) patients, with 28 NARs. Table 1 shows the clinical characteristics of the patients analyzed in this study and the extent of surgery. The detailed data of the operative results are shown in Tables 2 and 3. All TOETVA procedures were successfully completed without conversion to an open thyroidectomy. All Cont-IONM procedures were also completed, and no signal loss was encountered in this study. All Cont-IONM procedures were successful and free of serious adverse events including injury of the carotid vessels, vagal nerve, and RLN. Furthermore, no hemodynamic instability or cardiac arrhythmia was observed. In addition, no equipment malfunction or interference occurred.
The time to establish Cont-IONM monitoring ranged from 6 to 18 min per vagal nerve, with a mean time of 10.33 ± 2.57 min. No significant problems with electrode displacement were encountered, except for one patient in whom the delta electrode became dislodged (due to inadvertent tugging on the wire coursing through the operative field) and was quickly replaced, without traumatic injury of the vagal nerve. All patients presented stable EMG signals, except for one event when >50% reduction in EMG amplitude and >10% increased nerve latency were observed. The signal improved after the release of thyroid retractor, and this patient had no vocal cord paralysis postoperatively (Fig. 5).
Discussion
The importance of both the anatomic and physiologic preservation of RLN function cannot be overestimated in thyroid surgery. Two mechanisms of RLNP exist: transection injury and nontransection injuries such as heat, stretch, and compression injuries. Most RLNP events are reversible and occur as a result of nontransection injuries [15,16,17]. For 50 years, IONM underwent development to prevent RLNP, with significant improvements in this technology during the past decade [14, 18,19,20]. Two IONM techniques have been established, namely the intermittent and continuous variants [9, 21]. Int-IONM is performed using a hand-held stimulating probe to stimulate the RLN or vagal nerve intermittently. By contrast, Cont-IONM is performed using a temporary implantable electrode to automatically stimulate the vagal nerve cyclically. Unlike Int-IONM, in which injury may occur between stimulations, Cont-IONM provides real-time surveillance of RLN function during thyroid mobilization and RLN dissection, and it may aid in the early detection of nontransection RLNP [9, 10, 18,19,20, 22].
The Cont-IONM technique has been refined by several studies focusing on improving its implementation in endoscopic thyroid surgery [9, 10]. However, these studies did not consider the NOTES approach. During an endoscopic thyroidectomy, several essential procedures are required for the use of Cont-IONM technology, including the creation of an access to the carotid sheath, 360-degree circumferential dissection of the vagal nerve, and implantation of the electrode on the vagal nerve [22]. All these procedures are more technically difficult to perform in NOTES for thyroid disease because of the problems of an unusual vector of dissection, poor visibility, and limited surgical space. In this article, we describe the first clinical experience of using Cont-IONM in transoral thyroidectomy. Our clinical results demonstrate the feasibility and safety of using Cont-IONM during transoral endoscopic thyroidectomies. This technique is noninvasive and does not require additional oral, vestibular, or cervical cutaneous trocar incision. However, various surgical techniques and commercially available devices are required to facilitate its success. All these requirements can be summarized as follows:
-
1.
Modified EndoGrab™ Port-Free Retractor (Virtual Ports, Ltd.): this retractor is composed of two daughter retractors, and each one is linked by a steel wire. We divided the wire and placed the two clips over both ends of the smaller component of the retractor to catch the upper part of the thyroid and the contralateral percutaneous anchoring suture. The ipsilateral thyroid was effectively retracted medially, especially after the contralateral retraction of the anchoring suture. This method is almost atraumatic and can steadily maintain the open access to the carotid sheath.
-
2.
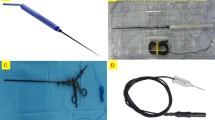
Delta electrode (inomed Medizintechnik GmbH; Fig. 6): it is (17 × 4.5 × 4.5 mm) sufficiently small to be easily delivered through the midline transoral trocar and placed into the space of the carotid sheath. It has the optimal shape of a partially closed mouth (<360°), which facilitates the envelopment of the target nerve more easily than does using an electrode with a closed mouth. In addition, the electrode is elastic in consistency and can be easily dislodged from the target nerve. The delta electrode was set up through vestibular incision, and its cable line was placed outside the trocar. Through this manipulation, the occurrence of inadvertent traction to the cable line was significantly decreased, resulting in less dislodgement of the electrode during surgical dissection.
-
3.
C2 monitoring system: it provides automatic cyclical stimulation to the vagal nerve and produces visual free-running EMG signals. The system is not only useful for comparison and analysis but also has the advantages of synchronization with surgical maneuvers. An audible and visual alert can be set when the threshold values exceeded to aid the surgeon in identifying risky maneuvers. It also has an auto switch function between the complementary use of the Int-IONM and Cont-IONM modes.
Clinical benefits of transoral Cont-IONM
Cont-IONM has more specific benefits than does Int-IONM, which are as follows:
-
1.
Provides continuous real-time information and immediate alerts regarding RLN injury.
-
2.
Elucidates the stress mechanism and prevents RLN failure through the synchronization of surgical maneuvers.
-
3.
Demonstrates the intraoperative information of functional nerve recovery.
Our experience revealed that the restitution of EMG amplitudes of ≥50% of the initial baseline allows the continuation of the resection in the contralateral side.
All these benefits were especially useful during transoral thyroidectomy, in which the anatomical view is not as clear as that in other procedures; therefore, this procedure requires more thyroid traction for surgical exposure in order to facilitate early corrective action before permanent damage to the nerve occurs.
Potential drawbacks
The use of Cont-IONM in TOVETVA may have the following drawbacks:
-
1.
Setup time: incorporation of this additional process of nerve monitoring requires an average of 10 min per monitored nerve. However, this may be prolonged in patients with a high BMI or in cases of bilateral usage.
-
2.
Extra cost: in addition to the cost of the delta stimulating electrode used in Cont-IONM, there are the expenses of the ETT (with the surface electrode) and the monitoring system.
-
3.
Partial replacement of Int-IONM function: Cont-IONM cannot completely replace Int-IONM because of the limitations in identification, mapping, and direct confirmation of the RLN. Cont-IONM should be used to complement Int-IONM.
Potential pitfalls
The use of Cont-IONM in TOVETVA may have the following pitfalls:
-
1.
Increase in the risk of injury to the internal jugular vein, carotid artery, and vagal nerve; although these complications did not occur in the present study, the vagal nerve should be carefully and gently isolated and mobilized to avoid nerve devascularization [20, 23].
-
2.
Adverse events such as cardiac arrhythmia, a complication related to the increase in parasympathetic tone, maybe caused by the vagal stimulation [20, 23].
-
3.
False positive/negative error due to etiologies including incorrect intubation, incorrect dosage and timing of the muscle relaxant, and instability of the electrode. The preventive methods for this error include the following:
-
a.
Initial vagal stimulation prior to the Cont-IONM electrode placement to test the integrity and function of the nerve.
-
b.
Appropriate frequency and intensity of stimulation.
-
c.
System calibration with the highest achievable amplitude.
-
a.
Further study
In the present study, we demonstrated the feasibility and safety of transoral Cont-IONM in TOETVA for achieving high success rates. However, this procedure is technically demanding and presents a learning curve for setting up the transoral Cont-IONM instrument. The transoral Cont-IONM device should be set up in a standardized manner. An ongoing controversy exists regarding the cost-effectiveness and risk–benefit ratio of Cont-IONM. This new technique should be carefully assessed using relevant data regarding the cost-effectiveness and risk–benefit ratio.
Conclusion
The present study demonstrated that transoral Cont-IONM use in NOTES for thyroid disease is feasible and safe and may assist in the early detection of adverse EMG changes, thereby preventing RLN paralysis. Our surgical technique for the implementation of the delta electrode on the vagal nerve is noninvasive and require no additional oral, vestibular, or cervical cutaneous trocar incision.
References
Randolph GW, Dralle H, Abdullah H, Barczynski M, Bellantone R, Brauckhoff M, Carnaille B, Cherenko S, Chiang FY, Dionigi G, Finck C, Hartl D, Kamani D, Lorenz K, Miccolli P, Mihai R, Miyauchi A, Orloff L, Perrier N, Poveda MD, Romanchishen A, Serpell J, Sitges-Serra A, Sloan T, Van Slycke S, Snyder S, Takami H, Volpi E, Woodson G (2011) Electrophysiologic recurrent laryngeal nerve monitoring during thyroid and parathyroid surgery: international standards guideline statement. Laryngoscope 121(Suppl 1):S1–S16
Shedd DP, Burget GC (1966) Identification of the recurrent laryngeal nerve. Arch Surg 92:861–864
Ghani U, Assad S (2016) Role of intraoperative nerve monitoring during parathyroidectomy to prevent recurrent laryngeal nerve injury. Cureus 8:e880
Hermann M, Hellebart C, Freissmuth M (2004) Neuromonitoring in thyroid surgery: prospective evaluation of intraoperative electrophysiological responses for the prediction of recurrent laryngeal nerve injury. Ann Surg 240:9–17
Caragacianu D, Kamani D, Randolph GW (2013) Intraoperative monitoring: normative range associated with normal postoperative glottic function. Laryngoscope 123:3026–3031
Snyder SK, Lairmore TC, Hendricks JC, Roberts JW (2008) Elucidating mechanisms of recurrent laryngeal nerve injury during thyroidectomy and parathyroidectomy. J Am Coll Surg 206:123–130
Liu XL, Wu CW, Zhao YS, Wang T, Chen P, Xin JW, Li SJ, Zhang DQ, Zhang G, Fu YT, Zhao LN, Zhou L, Dionigi G, Chiang FY, Sun H (2016) Exclusive real-time monitoring during recurrent laryngeal nerve dissection in conventional monitored thyroidectomy. Kaohsiung J Med Sci 32:135–141
Chiang FY, Lu IC, Chang PY, Sun H, Wang P, Lu XB, Chen HC, Chen HY, Kim HY, Dionigi G, Wu CW (2015) Stimulating dissecting instruments during neuromonitoring of RLN in thyroid surgery. Laryngoscope 125:2832–2837
Lamade W, Meyding-Lamade U, Buchhold C, Brauer M, Brandner R, Uttenweiler V, Motsch J, Klar E, Herfarth C (2000) First continuous nerve monitoring in thyroid gland surgery. Der Chirurg; Zeitschrift fur alle Gebiete der operativen Medizen 71:551–557
Lorincz BB, Mockelmann N, Busch CJ, Hezel M, Knecht R (2016) Automatic periodic stimulation of the vagus nerve during single-incision transaxillary robotic thyroidectomy: feasibility, safety, and first cases. Head Neck 38:482–485
Witzel K, von Rahden BH, Kaminski C, Stein HJ (2008) Transoral access for endoscopic thyroid resection. Surg Endosc 22:1871–1875
Anuwong A (2016) Transoral endoscopic thyroidectomy vestibular approach: a series of the first 60 human cases. World J Surg 40:491–497
Chiang FY, Lee KW, Chen HC, Chen HY, Lu IC, Kuo WR, Hsieh MC, Wu CW (2010) Standardization of intraoperative neuromonitoring of recurrent laryngeal nerve in thyroid operation. World J Surg 34:223–229
Schneider R, Randolph GW, Sekulla C, Phelan E, Thanh PN, Bucher M, Machens A, Dralle H, Lorenz K (2013) Continuous intraoperative vagus nerve stimulation for identification of imminent recurrent laryngeal nerve injury. Head Neck 35:1591–1598
Mattsson P, Hydman J, Svensson M (2015) Recovery of laryngeal function after intraoperative injury to the recurrent laryngeal nerve. Gland Surg 4:27–35
Paniello RC, Rich JT, Debnath NL (2015) Laryngeal adductor function in experimental models of recurrent laryngeal nerve injury. Laryngoscope 125:E67–E72
Chiang FY, Lu IC, Kuo WR, Lee KW, Chang NC, Wu CW (2008) The mechanism of recurrent laryngeal nerve injury during thyroid surgery–the application of intraoperative neuromonitoring. Surgery 143:743–749
Lamade W, Ulmer C, Seimer A, Molnar V, Meyding-Lamade U, Thon KP, Koch KP (2007) A new system for continuous recurrent laryngeal nerve monitoring. Minim Invasive Ther Allied Technol 16:149–154
Schneider R, Przybyl J, Pliquett U, Hermann M, Wehner M, Pietsch UC, Konig F, Hauss J, Jonas S, Leinung S (2010) A new vagal anchor electrode for real-time monitoring of the recurrent laryngeal nerve. Am J Surg 199:507–514
Lamade W, Ulmer C, Rieber F, Friedrich C, Koch KP, Thon KP (2011) New backstrap vagus electrode for continuous intraoperative neuromonitoring in thyroid surgery. Surg Innov 18:206–213
Lipton RJ, McCaffrey TV, Litchy WJ (1988) Intraoperative electrophysiologic monitoring of laryngeal muscle during thyroid surgery. Laryngoscope 98:1292–1296
Dionigi G, Donatini G, Boni L, Rausei S, Rovera F, Tanda ML, Kim HY, Chiang FY, Wu CW, Mangano A, Rulli F, Alesina PF, Dionigi R (2013) Continuous monitoring of the recurrent laryngeal nerve in thyroid surgery: a critical appraisal. Int J Surg 11(Suppl 1):S44–S46
Friedrich C, Ulmer C, Rieber F, Kern E, Kohler A, Schymik K, Thon KP, Lamade W (2012) Safety analysis of vagal nerve stimulation for continuous nerve monitoring during thyroid surgery. Laryngoscope 122:1979–1987
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosure
All authors, Drs. Han-Kun Chen, Chun-Liang Chen, Yi-Feng Lin, Kai-Yuan Lin, Yih-Huei Uen, and Mr. Kuo-Shan Wen have no conflicts of interest or financial ties to disclose.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Chen, HK., Chen, CL., Wen, KS. et al. Application of transoral continuous intraoperative neuromonitoring in natural orifice transluminal endoscopic surgery for thyroid disease: a preliminary study. Surg Endosc 32, 517–525 (2018). https://doi.org/10.1007/s00464-017-5656-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-017-5656-0