Abstract
This study assessed the effects of a mixed formulation containing Limosilactobacillus (L.) fermentum 139, L. fermentum 263, and L. fermentum 296 on cardiometabolic parameters, inflammatory markers, short-chain fatty acid (SCFA) fecal contents, and oxidative stress in colon, liver, heart, and kidney tissues of female rats fed a high-fat diet (HFD). Female Wistar rats were allocated into control diet (CTL, n = 6), HFD (n = 6), and HFD receiving L. fermentum formulation (HFD-LF, n = 6). L. fermentum formulation (1 × 109 CFU/mL of each strain) was administered two twice a day for 4 weeks. Administration of L. fermentum increased acetate and succinate fecal contents and reduced hyperlipidemia and hyperglycemia in rats fed a HFD (p < 0.05). Administration of L. fermentum decreased low-grade inflammation and improved antioxidant capacity along the gut, liver, heart, and kidney tissues in female rats fed a HFD (p < 0.05). Administration of L. fermentum prevented dyslipidemia, inflammation, and oxidative stress in colon, liver, heart, and kidney in female rats fed a HFD.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The high prevalence of cardiometabolic disorders, such as type 2 diabetes mellitus, dyslipidemias, arterial hypertension, and obesity, has been recognized as most important cardiovascular disease risk factors, being associated, in part, with poor food pattern, including a diet rich in calories, sugar, salt, saturated fatty acids, and cholesterol [1, 2]. Sex difference has been related to cardiometabolic disorder prevalence and evidence suggests that female hormones could have a protective effect [3].
High-fat diet (HFD) consumption, specifically diet rich in saturated and trans fats, increases the abundance of lipopolysaccharides (LPS)-expressing bacteria and provokes elevated levels of LPS in systemic circulation, characterizing a pro-inflammatory state, named metabolic endotoxemia [4, 5]. Additionally, prolonged HFD consumption increases oxidative stress and mitochondrial damage in several organs [6,7,8]. The findings suggest that interventions targeting gut microbiota and exerting anti-inflammatory and anti-oxidant properties could reduce the risk of cardiometabolic disorders provoked by HFD.
Previous investigations have suggested that gut microbiota differs between the sexes in rodents and humans. Women commonly harbor a higher ratio of Firmicutes/Bacteroidetes (F/B), enhanced lactobacilli population, and short-chain fatty acid producers in gut microbiota when compared with men [9]. The related sex differences can lead to sex-dependent changes in systemic immunity, low-grade inflammation, oxidative stress, and response to gut microbiota modulation [8, 10,11,12].
A broader range of studies carried out with male have demonstrated that administration of probiotics promoted beneficial effects on gut microbiota, inflammation, oxidative stress, and cardiometabolic functions [13,14,15,16,17]. However, the effects of probiotic administration on inflammation, oxidative stress, and cardiometabolic parameters in female have been little explored and remain to be elucidated.
An early investigation characterized three Lactobacillus fermentum (recently renamed as Limosilactobacillus fermentum) [18], namely, L. fermentum 139, L. fermentum 263, and L. fermentum 296, as potential candidates for use as probiotics in a set of functionality-related in vitro properties, such as performance regarding adhesion, aggregation, co-aggregation, antagonism, and survival to exposure to simulated gastrointestinal conditions, besides showing absence of hemolytic and mucinolytic activities and resistance to antibiotics [19]. In this study, we have evaluated the effects of a mixed formulation containing these three potentially probiotic L. fermentum strains on cardiometabolic variables, biomarkers of inflammation, caecum short-chain fatty acid production, and oxidative stress markers in gut, liver, heart, and kidney tissues of female rats fed a HFD diet.
Methods
Animals and Ethical Aspects
Female Wistar rats (Rattus norvergicus) in same estrus cycle were used in this study. Determination of the estrous cycle was carried according to previous study [20]. The animals received water and diet ad libitum and were maintained in collective polypropylene cages (03 animals/cage) under controlled temperature (22 ± 1 °C), humidity between 50 and 55% and a 12-h light–dark cycle. The experimental procedures were approved by Institutional Animal Care and Use Committee/Federal University of Paraíba (CEUA-UFPB protocol # 6,080,240,418, João Pessoa, Paraíba, Brazil) and followed the guidelines of National Council for the Control of Animal Experimentation (CONCEA) and International Principles for Biomedical Research.
Experimental Design
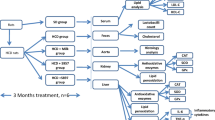
The rats were randomly assigned into control group (CTL, n = 6) receiving a control diet prepared according to the American Institute of Nutrition – AIN-93 M) [21]; HFD group receiving a high-fat diet (HFD, n = 6) purchased from Rhoster® Company (Araçoiaba da Serra, São Paulo, Brazil) and treated with placebo; and HFD group receiving a probiotic formulation containing a mix of L. fermentum 139, 263, and 296 (HFD-Lf, n = 6). Composition of CTL and HFD diets are shown in Supplemental Table 1.
In CTL and HFD groups, phosphate-buffered saline (PBS) solution was administered as placebo for 4 weeks. In HFD-Lf group, a mix formulation containing L. fermentum 139, 263, and 296 in a solution of approximately 3 × 109 CFU/mL of each strain were administered twice a day for 4 weeks. Administration of placebo or L. fermentum formulation was done by oral gavage (1 mL). Body weight were weekly measured using an appropriate scale (model AS-1000; Marte, Santa Rita, Minas Gerais, Brazil). After 4 weeks, rats were euthanized by decapitation and biochemical and cytokines were measured in serum, short-chain fatty acid (SCFA) were measured in caecum contents, and oxidative stress variables were assessed in gut, liver, heart, and kidney tissues.
Probiotic Strains and Cell Suspension Preparation
The L. fermentum 139, L. fermentum 263, and L. fermentum 296 strains were gently provided by Laboratory of Food Microbiology, Department of Nutrition, Federal University of Paraíba (João Pessoa, Paraíba, Brazil). Stocks were stored at − 20 °C in de Mann, Rogosa, and Sharpe (MRS) broth (HiMedia, Mumbai, India) containing glycerol 20% (Sigma-Aldrich, St. Louis, USA; 20 mL/100 mL).
The probiotic cell suspension was daily obtained from overnight cultures of each strain grown in MRS broth (HiMedia, Mumbai, India) anaerobically incubated (Anaerobic System Anaerogen, Oxoid Ltda., Wade Road, UK) at 37 °C, according to a previously described procedure [11, 14]. The cell suspension with viable counts of approximately 9 log CFU/mL were obtained by mixing the suspension of each probiotic strain in a ratio of 1:1:1.
Biochemical Analysis
Serum samples were analyzed to determine the levels of glucose, total cholesterol, high-density lipoprotein cholesterol (HDL-c), triglycerides, creatinine, urea, alanine aminotransferase (ALT), and aspartate aminotransferase (AST) using commercial kits and semi-automatic photometer HumaLyzer 3500 (HUMAN Gesellschaft für Biochemica und Diagnostica mbH, Wiesbaden, Germany). Low-density lipoprotein cholesterol (LDL-c) levels were calculated according to Friedewald formula: LDL-c (mg/dL) = [TC − HDL-c − TG]/5 [22].
Quantification of Organic Acids in Caecum Contents
Caecum sample contents were collected at the end of experiments and stored under − 80 °C. Organic acids were quantified by high-performance liquid chromatography (HPLC) using an LC 1260 Infinity system (Agilent Technologies, Santa Clara, CA, USA) coupled to a PDA detector (G1315D; Agilent Technologies) as previously described [23].
Cytokine Measurement
Cytokine levels (IL-6, IL-10, IL1β, and TNF-α) were determined using Millipore 7-plex kit (Millipore Corp., Billerica, MA, USA). Assays were performed on a 96-well plate containing a filter membrane following the manufacturer’s instructions. The concentrations of cytokines in samples were estimated from a standard curve using a third-order polynomial equation and expressed as pg/mL. Samples with values below the limit of detection were recorded as zero, while for samples with values above the quantification upper limit of standard curves were assigned the highest curve value.
Oxidative Stress Measurement in Tissues
The colon, liver, heart, and renal tissues were homogenized in a cold buffer solution with 50 mM TRIS and 1 mM EDTA, pH 7.4, 1 mM sodium orthogonadate, and 200 μg/mL phenylmethanesulfonylfluoride using an IKA RW 20 digital homogenizer, a pestle of potter–Elvehjem, and glass tubes on ice. The homogenates were centrifuged (1.180 × g, 10 min, 4 °C) [24] and protein levels were measured with Bradford protocol [25].
Assessment of Lipid Peroxidation
An aliquot (0.3 mg/mL) of homogenate of tissues was used to quantify the production of malondialdehyde (MDA) in reaction with thiobarbituric acid (TBA, 100 °C). Sequential addition of 30% (v/v) of trichloroacetic acid and Tris–HCl (3 mM) were done to the sample, followed by centrifugation (2500 × g, 10 min, 4 °C). TBA (0.8%, v/v) was added to resulting supernatant, mixed, boiled for 15 min, and after cooling, the reaction was read at 535 nm on a spectrophotometer.
Assessment of Superoxide Dismutase (SOD) Activity
Total superoxide dismutase (SOD) enzyme activity was determined according to Misra and Fridovich method. The tissue samples (0.3 mg/mL) were mixed with sodium carbonate buffer (0.05%, pH 10.2, 0.1 mmol/L EDTA, 37 °C), added of 30 mM/L of epinephrine (in 0.05% acetic acid), and SOD activity was measured by kinetics of epinephrine auto-oxidation inhibition for 1.5 min at 480 nm read on a spectrophotometer [26].
Assessment of Catalase (CAT) Activity
Catalase activity was determined by decomposition of H2O2 into O2 and H2O. A sample of tissues homogenate (0.3 mg/mL) in 50 mM phosphate buffer (pH 7.0) was added of 0.3 M H2O2. Absorbance was measured at 240 nm for 1.5 min on a spectrophotometer [27].
Assessment of Glutathione S-Transferase (GST) Activity
A sample of tissue homogenate (0.3 mg/mL) was used to quantify GST activity, as previously described [28]. Phosphate buffer (0.1 M, pH 6.5 containing 1 mM EDTA), 1 mM 1-chloro-2,4-dinitrobenzene (CDNB), and 1 mM reduced glutathione (GSH) was added to tissue homogenate samples. Absorbance was measured at 340 nm for 1.5 min on a spectrophotometer.
Assessment of Total Thiol Groups
Tissue homogenate samples (0.3 mg/mL) were incubated in extraction buffer (previously described) with 10 mM of 5,5′-dithiobis (2-nitrobenzoic acid) in a dark environment for 30 min. The absorbance of the reaction was measured at 412 nm on a spectrophotometer [29].
Statistical Analysis
Values were reported as mean ± standard deviation for parametric data or median (maximum − minimum) for non-parametric data. Kolmogorov–Smirnov and Shapiro–Wilk tests were used to assess the normality of data. Most of variables required the one-way ANOVA parametric test and Tukey post-hoc test. Non-parametric variables were compared using Kruskal–Wallis with Dunn’s post-hoc test. A Pearson’s or Spearman correlation coefficient (r) was used to evaluate the relationships among oxidative stress parameters in colon and liver, heart, and kidney tissues. The correlations were classified as bad (r ≤ 0.20), weak (0.21–0.40), moderate (0.41–0.60), good (0.61–0.80), and excellent (0.81–1.00). Statistical analysis was done with software Prism 9 (GraphPad Software, San Diego, CA, USA). The difference was considered significant when p was < 0.05.
Results
Body Weight and Biochemical Parameters
The percentage of weight gain at the end of the protocol was similar among groups (Table 1; p > 0.05). Female rats fed a HFD had increased serum levels of glucose, triglycerides, cholesterol, LDL-cholesterol, urea, ALT, and AST when compared to CTL group (Table 1; p < 0.05). Administration of L. fermentum formulation reduced serum levels of glucose (140.7 ± 14.0 vs. 207.5 ± 18.3, p < 0.05), triglycerides (94.0 ± 11.2 vs. 151.5 ± 13.1, p < 0.05), cholesterol (147.4 ± 12.1 vs. 399.5 ± 22.0, p < 0.05), LDL-cholesterol (104.9 ± 19.2 vs. 240.7 ± 27.9, p < 0.05), urea (24.4 ± 2.5 vs. 47.1 ± 7.8, p < 0.05), ALT (64.8 ± 12.0 vs. 106.3 ± 21.5, p < 0.05), and AST (122.5 ± 12.2 vs. 189.0 ± 36.7, p < 0.05) when compared to HFD group (Table 1). In addition, L. fermentum formulation increased serum levels of HDL-c (67.8 ± 6.2 vs. 45.7 ± 8.7, p < 0.05) when compared to HFD and CTL groups (Table 1).
Short-Chain Acid Fatty in Caecum Contents
Fecal contents of acetate, propionate, and succinate were similar between HFD and CTL groups (p > 0.05; Fig. 1A–C). Administration of L. fermentum formulation increased fecal contents of acetate (0.1 ± 0.01 vs. 0.03 ± 0.005 vs. 0.03 ± 0.02 g/L, p < 0.05) and succinate (1.38 ± 0.53 vs. 0.46 ± 0.30 vs. 0.78 ± 0.18 g/L, p < 0.05) when compared to CTL and HFD groups, respectively (Fig. 1A–C), but it did not change fecal contents of propionate (p > 0.05; Fig. 3B). Butyric acid contents were below the limit of detection.
Effects of a mixed formulation with Limosilactobacillus fermentum 139, 263, and 269 on short-chain fatty acid concentration in fecal samples in female rats fed a high-fat diet. Assessment of acetate (A), propionate (B), and succinate (C) in the fecal samples. Groups: control group (CTL, n = 6), high-fat diet (HFD, n = 6), and HFD receiving a mixed L. fermentum formulation (HFD-Lf, n = 6). Data are presented as mean ± standard deviation and analyzed by ANOVA one-way test with Tukey as post-hoc test
Cytokine Serum Levels
Female rats fed a HFD had increased serum levels of proinflammatory cytokines TNFα (152.8 ± 6.3 vs. 78.4 ± 6.0 pg/mL, p < 0.05) and IL-1β (159.8 ± 13.2 vs. 54.8 ± 2.1 pg/mL, p < 0.05) and decreased levels of IL-6 (38.2 ± 5.3 vs. 64.6 ± 2.9 pg/mL, p < 0.05) and IL-10 (28.1 ± 4.0 vs. 66.8 ± 4.6 pg/mL, p < 0.05) when compared with CTL group (Fig. 2A–D). HFD group receiving L. fermentum formulation had decreased serum levels of TNF-α (107.6 ± 19.5 vs. 152.8 ± 6.3 pg/mL, p < 0.05) and IL1β (107.2 ± 10.9 vs. 159.8 ± 13.2 pg/mL, p < 0.05), as well as higher IL-6 (56.1 ± 5.8 vs. 38.2 ± 5.3 pg/mL, p < 0.05) and IL-10 (41.9 ± 5.6 vs. 28.1 ± 4.0 pg/mL, p < 0.05) when compared to HFD receiving placebo treatment (Fig. 2A–D).
Effects of a mixed formulation with Limosilactobacillus fermentum 139, 263, and 269 on cytokines serum levels in female rats fed a high-fat diet. Assessment of tumoral necrosis factor alpha (TNF-α) (A), interleukin 1 beta (IL-1β) (B), interleukin 6 (IL-6) (C), and interleukin 10 (IL-10) (D). Groups: control group (CTL, n = 6), high-fat diet (HFD, n = 6), and HFD receiving a mixed L. fermentum formulation (HFD-Lf, n = 6). Data are presented as mean ± standard deviation and analyzed by ANOVA one-way test with Tukey as post-hoc test
Oxidative Stress Biomarkers in Colon Tissues
The MDA levels and sulfhydryl content in colonic mucosa were similar among groups (p > 0.05; Fig. 3A, E). Female rats fed a HFD had decreased SOD (335.7 ± 38.0 vs. 427.9 ± 21.8 U/mg protein, p < 0.05) and GST (9.2 ± 2.7 vs. 15.3 ± 3.2 U/mg protein, p < 0.05) activities in colonic mucosa when compared to CTL group (Fig. 3B, D). Administration of L. fermentum formulation although had decreased CAT activity in colonic mucosa of rats fed a HFD (p < 0.05; Fig. 3C), it caused increased SOD (408.7 ± 34.1 vs. 335.7 ± 38.0 U/mg protein, p < 0.05) and GST (15.2 ± 2.7 vs. 9.2 ± 2.7 U/mg protein, p < 0.05) activities when compared to HFD placebo treated (Fig. 3B, D).
Effects of a mixed formulation with Limosilactobacillus fermentum 139, 263, and 269 on oxidative stress parameters in colon mucosa of female rats fed a high-fat diet. Assessment of malondialdehyde levels (MDA) (A), superoxide dismutase activity (SOD) (B), catalase activity (CAT) (C), glutathione S-transferase activity (GST) (D), and total sulfhydryl content (E) in the colon mucosa. Groups: control group (CTL, n = 6), high-fat group (HFD, n = 6), and HFD receiving L. fermentum formulation (HFD-Lf, n = 6). Data are presented as mean ± standard deviation and analyzed by ANOVA one-way test with Tukey as post-hoc test
Oxidative Stress Biomarkers in Liver Tissues
The MDA level was enhanced in liver tissues of rats fed a HFD when compared to CTL group (p < 0.05; Fig. 4A). Female rats fed a HFD had decreased SOD (195.7 ± 37.1 vs. 331.0 ± 44.2 U/mg protein, p < 0.05) and CAT (7.6 ± 4.1 vs. 16.6 ± 2.2 U/mg protein, p < 0.05) activities in liver tissues when compared to CTL group (Fig. 4B, C). Administration of L. fermentum formulation although did not change CAT activity in liver of rats fed a HFD (p > 0.05; Fig. 4C), it caused increased SOD (301.8 ± 56.0 vs. 195.7 ± 37.1 U/mg protein, p < 0.05) and GST (340.8 ± 37.2 vs. 215.8 ± 20.1 U/mg protein, p < 0.05) activities and sulfhydryl content (0.10 ± 0.01 vs. 0.07 ± 0.01 μmol/mg protein, p < 0.05) when compared to HFD placebo treated (Fig. 4B, D, and E).
Effects of a mixed formulation with Limosilactobacillus fermentum 139, 263, and 269 on oxidative stress parameters in liver of female rats fed a high-fat diet. Assessment of malondialdehyde levels (MDA (A), superoxide dismutase activity (SOD) (B), catalase activity (CAT) (C), glutathione S-transferase activity (GST) (D), and total sulfhydryl content (E) in the liver. Groups: control group (CTL, n = 6), high-fat group (HFD, n = 6), and HFD receiving L. fermentum formulation (HFD-Lf, n = 6). Data are presented as mean ± standard deviation and analyzed by ANOVA one-way test with Tukey as post-hoc test
Oxidative Stress Biomarkers in Heart Tissues
The SOD and CAT activities and sulfhydryl content in heart tissues were similar between CTL and HFD groups (p > 0.05; Fig. 5B, C, and E). Female rats fed a HFD had reduced GST activity (28.6 ± 4.1 vs. 38.5 ± 4.2 U/mg protein, p < 0.05) and enhanced MDA levels (0.22 ± 0.10 vs. 0.06 ± 0.02 nmol/mg protein, p < 0.05) in heart tissues when compared to CTL group (Fig. 5C, D). Administration of L. fermentum formulation increased SOD activity (622.4 ± 55.4 vs. 374.9 ± 21.4 vs. 385.5 ± 42.6 U/mg protein, p < 0.05) and sulfhydryl content (0.35 ± 0.05 vs. 0.13 ± 0.01 vs. 0.16 ± 0.02 mmol/mg protein, p < 0.05) in heart tissues when compared to HFD and CTL group, respectively (Fig. 5B, E).
Effects of a mixed formulation with Limosilactobacillus fermentum 139, 263, and 269 on oxidative stress parameters in heart tissue of female rats fed a high-fat diet. Assessment of malondialdehyde levels (MDA) (A), superoxide dismutase activity (SOD) (B), catalase activity (CAT) (C), glutathione S-transferase activity (GST) (D), and total sulfhydryl content (E) in the heart tissue. Groups: control group (CTL, n = 6), high-fat group (HFD, n = 6), and HFD receiving L. fermentum formulation (HFD-Lf, n = 6). Data are presented as mean ± standard deviation and analyzed by ANOVA one-way test with Tukey as post-hoc test
Oxidative Stress Biomarkers in Renal Cortex
MDA levels, SOD and CAT activities, and sulfhydryl content in renal cortex were similar between CTL and HFD groups (p > 0.05; Fig. 6A, B, C, and E). Female rats fed a HFD had reduced GST activity (30.0 ± 9.1 vs. 49.2 ± 6.8 U/mg protein, p < 0.05) in renal cortex when compared to CTL group (Fig. 6C, D). Administration of L. fermentum formulation increased SOD (380.4 ± 116.5 vs. 211.1 ± 35.4 U/mg protein, p < 0.05) and GST activities (53.6 ± 17.8 vs. 30.0 ± 9.1 U/mg protein, p < 0.05) in renal cortex when compared to HFD group (Fig. 6B, D), but did not change MDA levels, CAT activity, and sulfhydryl content (p > 0.05; Fig. 6A, C, and E).
Effects of a mixed formulation with Limosilactobacillus fermentum 139, 263, and 269 on oxidative stress parameters in renal cortex of female rats fed a high-fat diet. Assessment of malondialdehyde levels (MDA) (A), superoxide dismutase activity (SOD) (B), catalase activity (CAT) (C), glutathione S-transferase activity (GST) (D), and total sulfhydryl content (E) in the renal cortex. Groups: control group (CTL, n = 6), high-fat group (HFD, n = 6), and HFD receiving L. fermentum formulation (HFD-Lf, n = 6). Data are presented as mean ± standard deviation and analyzed by ANOVA one-way test with Tukey as post-hoc test
The relationship between antioxidant enzyme activities in colon, liver, heart, and kidney tissues was demonstrated as a hierarchical heat map (Fig. 7), which showed distinct clusters of associations based on antioxidant enzyme activities found in CTL, HFD, and HFD-LF groups (Fig. 7). In addition, we have carried correlation analysis between oxidative stress biomarkers in colon with oxidative stress biomarkers in liver, heart, and renal cortex (Table 2). SOD activity in colon correlated positively with SOD activity in liver (r = 0.708, p = 0.001), but not with SOD activity in heart (r = 0.234, p = 0.349) and renal cortex (r = 0.199, p = 0.428). Similarly, CAT activity in colon correlated positively with CAT activity in liver (r = 0.641, p = 0.004), but not with CAT activity in heart and renal cortex (p > 0.05; Table 2). GST activity in colon also correlated positively with GST activity in liver (r = 0.0.566, p = 0.014), but not with GST activity in heart and renal cortex (p > 0.05; Table 2). TBARS and sulfhydryl contents in colon had not correlation with liver, heart, and renal cortex (p > 0.05; Table 2).
Effects of a mixed formulation with Limosilactobacillus fermentum 139, 263, and 269 on antioxidant enzyme activities. Heatmap showing antioxidant enzyme activities in colon, liver, heart, and kidney tissues in female rats. Groups: control group (CTL, n = 6), high-fat group (HFD, n = 6), and HFD receiving L. fermentum formulation (HFD-LF, n = 6)
Discussion
In recent years, our research group has isolated and characterized potentially probiotic fruit-derived strains. The strains of L. fermentum 139, L. fermentum 296, and L. fermentum 263 were recovered from Brazilian fruit by-products [19, 30]. L. fermentum 139 was isolated from Mangifera indica L. (mango), L. fermentum 263 was isolated from Ananas comosus (pineapple), and L. fermentum 296 was isolated from Fragaria vesca L. (strawberry). All the three strains displayed potential for use as probiotics in terms of a set of functionalities related in vitro properties, such as auto-aggregation, co-aggregation, survival during exposure to simulated gastrointestinal conditions, and pathogen antagonism, in addition to showing the absence of hemolytic and mucolytic activities and resistance to antibiotics [19]. Such findings indicated that these L. fermentum fruit-derived strains could be potential candidates for use as novel probiotics. Using those strains, we have demonstrated for the first time that administration of a mixed formulation containing three potentially probiotic L. fermentum strains, twice a day for 4 weeks, increased fecal acetate and succinate contents, reduced glycemia, dyslipidemia, systemic low-grade inflammation, and oxidative stress in colonic mucosa, liver, heart, and kidney tissues of female rats fed a HFD.
In agreement with previous studies, HFD consumption provoked hyperglycemia and hyperlipemia [14, 31, 32]. Here, administration of mixed L. fermentum formulation prevented increases of glucose, triglycerides, urea, ALT, AST, and cholesterol serum levels, as well increased serum levels of HDL-cholesterol in female rats, indicating to occur relevant hypoglycemic and hypolipidemic effects and reduced serum indicators of hepatic injury. The use of different L. fermentum strain types have also caused hypolipidemic and hypoglycemic findings, as well reduced hepatic injury indicators in rodents and humans in early investigations [13, 33,34,35,36]. For example, in female rats, administration of L. fermentum MCC2759 and MCC2760 alleviated inflammation and improved intestinal function in high‑fat diet‑fed and streptozotocin‑induced diabetic [36].
For us, the results of the present study reinforce that L. fermentum 139, L. fermentum 263, and L. fermentum 296 strains has great potential to act as novel anti-dyslipidemia and anti-diabetes biotherapeutic products due to their ability to attenuate lipid-glucose metabolism disorders and further translational studies should be carried out [11, 14].
The SCFAs, primarily are acetate, propionate, and butyrate, can be generated in the colon as end products of bacterial fermentation [37]. In the present study, butyrate contents were below the analytical detection limit. Administration of mixed L. fermentum formulation although had no significant effect on propionate fecal contents, it effectively increased acetate and succinate fecal contents in female rats fed a HFD, indicating heterofermentative properties of L. fermentum strains used in this formulation and a stimulatory effect on gut microbiota. In the colon, SCFAs play a key role in maintenance of epithelial integrity, energy source of colonocytes, fluid absorption, and important anti-inflammatory effect [37]. Acetate has been found as prevalent SCFA concentration in colon and early studies have demonstrated acetate as a relevant suppressor of colonic inflammation via G-protein coupled receptor 43 (GPR43) signaling [37, 38]. If L. fermentum exert a suppressor effect of colonic inflammation remain to be elucidated.
Gut microbiota can also produce important amounts of succinate, an intermediary microbial product especially derived from fermentation of fibers and oligosaccharides [39, 40]. Early investigations have reported enhanced succinate cecal contents and improved glycemic control in mice fed a fiber-rich diet [40, 41]. The role and tolerance level of succinate gut-derived is still unclear, but it has been suggested that succinate acting in GPR91 exert an important function in modulation of intestinal inflammation [39] and against colonization and growth of exogenous pathogens [42].
In agreement to results of early studies, HFD consumption provoked diabetic dyslipidemia phenotype [43] and a low-grade inflammation condition in female rats [44, 45], which was linked to increased serum levels of pro-inflammatory cytokines TNFα and IL1β and reduced anti-inflammatory cytokine IL-10. Pro- and anti-inflammatory properties have been reported as potential functions of cytokine IL-6 [46]. Although reduced serum levels of IL6 have been found in female rats fed a HFD, the result set of measured cytokines could indicate a metabolic endotoxemia condition.
Strain- and sex-specific immunological effects have been found in probiotic bacteria [47]. Regarding anti-inflammatory properties of L. fermentum CECT5716, preceding studies have reported a significant reduction in pro-inflammatory cytokines TNFα and IL-1β in inflamed tissue of rats displaying colitis [48, 49]. Additionally, it has been reported that L. fermentum CECT5716 [50] and L. fermentum UCO-979C [51] can modulate the host immune system by increasing regulatory T cells (Treg) leading to enhanced IL-10 production in serum and intestine of female mice. The results of this study indicate for first time that administration of potentially probiotic L. fermentum promoted an important immune modulation in female rats fed a HFD, as indicated by induction of increased levels of IL-10 and IL-6 and decreased levels of IL-1β and TNF-α.
In physiological condition, reactive oxygen species (ROS) are found at low concentration into normal cells due to an efficient enzymatic and non-enzymatic anti-oxidant system [52]. However, it has been broadly reported that during nutritional stress (e.g., HFD consumption) excessive ROS production or down-regulation of anti-oxidant response can provoke oxidative stress, damage cells, and development of chronic diseases [7, 53]. Available evidence has suggested that powerful oxidative stress inducers may be associated with gut dysbiosis and pro-inflammatory processes [54,55,56]. In the present study, HFD consumption increased systemic low-grade inflammation and damaged the anti-oxidant system in colon mucosa, liver, heart, and kidney tissues of female rats.
Many beneficial effects of probiotics on oxidative stress tolerance and antioxidant capacity have been reported [13, 16, 35]. In the present study, a mixed L. fermentum formulation promoted increased antioxidant enzyme activities in colonic mucosa, liver, heart, and kidney tissues of rats fed a HFD, suggesting a direct and broad antioxidant effect. Probiotic strains with antioxidant properties have been growing explored [16] and studies have reported a relevant anti-oxidant capacity in other L. fermentum strains. Administration of L. fermentum CECT5716 [57] and L. fermentum MTCC: 5898 [13] has shown to reduce oxidative stress in cardiometabolic disorders.
Although underlying mechanism by which mixed L. fermentum formulation increased SOD and GST activities in colonic mucosa, liver, heart, and kidney tissues were not explored, MnSODs enzyme activity has been reported for some lactic acid bacteria [16]. Additionally, it has been demonstrated that L. fermentum strains could have a fully functional GSH system composed of GSH peroxidase and GSH reductase capable of protecting cells against oxidative stress [58].
We have postulated that tissue oxidative damage provoked by HFD consumption, in part, could be due to increased oxidative stress in colon. Here, we have reported that antioxidant enzyme activities in colon were correlated positively with antioxidant enzyme activities in liver, but not in heart and renal cortex. Our findings suggest that L. fermentum formulation might modulate oxidative stress biomarkers through gut-liver axis [59], but the modulation of oxidative stress biomarkers in gut-heart axis and gut-kidney axis was not demonstrated.
Early investigation has suggested that gut-heart axis and gut-kidney axis could be considered as novel areas for therapeutic research to prevent and reduce the risk of cardiovascular disease [60, 61] and renal disease [8, 62]. For us, further studies using probiotic therapy are needed to investigate the potentiality of gut-heart axis and gut-kidney axis as therapeutic strategy.
The lack of gut microbiota composition analysis could be described as a main limitation of this study, although we have previously documented enhanced Lactobacillus counts in feces from rats treated with L. fermentum strains with claimed probiotic properties [11, 14].
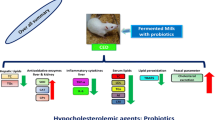
In conclusion, administration of a mixed formulation containing three potentially probiotic L. fermentum strains prevented diabetic dyslipidemia, low-grade inflammation, and oxidative stress along the gut, liver, heart, and kidney tissues in female rats fed a HFD (Fig. 8). Additionally, the mixed L. fermentum formulation was effective to increase acetate and succinate fecal contents. These results encourage the development of future clinical trials to assess the effects of examined L. fermentum formulation in subjects with dyslipidemias.
Schematic drawing showing the impact of the high-fat diet receiving placebo (HFD) or a mixed of Limosilactobacillus fermentum 139, 263, and 296 (HFD-Lf, 3 × 109 CFU, twice a day, 4 weeks) on short-chain fatty acid, biochemical, inflammatory variables, and oxidative stress along the gut, liver, heart, and kidney tissues in female rats. ALT alanine aminotransferase, AST aspartate aminotransferase, CAT catalase, CTL control group, FG fasting glucose, GST glutathione S-transferase, HFD high-fat diet, IL interleukins, MDA malondialdehyde, SOD superoxide dismutase, SULF sulfhydryl content, TNF-α tumoral necrosis factor alpha, TC total cholesterol, TG triglycerides, U urea
Data Availability
The data that support the findings of this study are available on request from the corresponding author. The data are not publicly available due to privacy or ethical restrictions.
References
Benziger CP, Roth GA, Moran AE (2016) The global burden of disease study and the preventable burden of NCD. Glob Heart 11(4):393–397. https://doi.org/10.1016/j.gheart.2016.10.024
Ravera A, Carubelli 2, Sciatti E, Bonadei I, Gorga E, Cani D, Vizzardi E, Metra M, Lombardi C (2016) Nutrition and cardiovascular disease: finding the perfect recipe for cardiovascular health Nutrients 8(6):1-27. https://doi.org/10.3390/nu8060363
Regitz-Zagrosek V, Kararigas G (2017) Mechanistic pathways of sex differences in cardiovascular disease. Physiol Rev 97(1):1–37. https://doi.org/10.1152/physrev.00021.2015
Zmora N, Suez J, Elinav E (2019) You are what you eat: diet, health and the gut microbiota. Nat Rev Gastroenterol Hepatol 16(1):35–56. https://doi.org/10.1038/s41575-018-0061-2
Tremaroli V, Bäckhed F (2012) Functional interactions between the gut microbiota and host metabolism. Nature 489(7415):242–249. https://doi.org/10.1038/nature11552
Ballal K, Wilson CR, Harmancey R, Taegtmeyer H (2010) Obesogenic high fat western diet induces oxidative stress and apoptosis in rat heart. Mol Cell Biochem 344:221–230. https://doi.org/10.1007/s11010-010-0546-y
Tan BL, Norhaizan ME, Liew WPP (2018) Nutrients and oxidative stress: friend or foe? Oxid Med Cell Longev 9719584:1–24. https://doi.org/10.1155/2018/9719584
do Nascimento LCP, Cruz Neto JPR, Braga VA, Lagranha CJ, de Brito Alves JL, (2020) Maternal exposure to high-fat and high-cholesterol diet induces arterial hypertension and oxidative stress along the gut-kidney axis in rat offspring. Life Sci 261:118367. https://doi.org/10.1016/j.lfs.2020.118367
Razavi AC, Potts KS, Kelly TN, Bazzano LA (2019) Sex, gut microbiome, and cardiovascular disease risk. Biol Sex Differ 10(29):1–14. https://doi.org/10.1186/s13293-019-0240-z
Bouman A, Heineman MJ, Faas MM (2005) Sex hormones and the immune response in humans. Hum Reprod Update 11(4):411–423. https://doi.org/10.1093/humupd/dmi008
Oliveira Y, Cavalcante RGS, Cavalcanti Neto MP, Magnani M, Braga VA, Souza EL, de Brito Alves JL (2020) Oral administration of Lactobacillus fermentum post-weaning improves the lipid profile and autonomic dysfunction in rat offspring exposed to maternal dyslipidemia. Food Funct 11(6):5581–5594. https://doi.org/10.1039/d0fo00514b
Vemuri R, Sylvia KE, Klein SL, Forster SC, Plebanski M, Eri R, Flanagan KL (2019) The microgenderome revealed: sex differences in bidirectional interactions between the microbiota, hormones, immunity and disease susceptibility. Semin Immunopathol 41(2):265–275. https://doi.org/10.1007/s00281-018-0716-7
Yadav R, Khan SH, Mada SB, Meena S, Kapila R, Kapila S (2019) Consumption of probiotic Lactobacillus fermentum MTCC: 5898-fermented milk attenuates dyslipidemia, oxidative stress, and inflammation in male rats fed on cholesterol-enriched diet. Probiotics Antimicrob Proteins 11(2):509–518. https://doi.org/10.1007/s12602-018-9429-4
Cavalcante RGS, Albuquerque TMR, Luna Freire MO, Ferreira GAH, Santos LAC, Magnani M, Cruz JC, Braga VA, Souza EL, de Brito Alves JL (2019) The probiotic Lactobacillus fermentum 296 attenuates cardiometabolic disorders in high fat diet-treated rats. Nutr Metab Cardiovasc Dis 29(12):1408–1417. https://doi.org/10.1016/j.numecd.2019.08.003
Romão da Silva LF, de Oliveira Y, Souza EL, Luna Freire MO, Braga VA, Magnani M, de Brito Alves JL (2019) Effects of probiotic therapy on cardio-metabolic parameters and autonomic modulation in hypertensive women: a randomized, triple-blind, placebo-controlled trial. Food Funct 11(8):7152–7163. https://doi.org/10.1039/d0fo01661f
Feng T, Wang J (2020) Oxidative stress tolerance and antioxidant capacity of lactic acid bacteria as probiotic: a systematic review. Gut Microbes 12(1):1801944. https://doi.org/10.1080/19490976.2020.1801944
Cavalcanti-Neto MP, Aquino JS, Romão da Silva LF, Silva RO, Guimarães KSL, de Oliveira Y, Souza MM, Vidal H, de Brito Alves JL (2018) Gut microbiota and probiotics intervention: a potential therapeutic target for management of cardiometabolic disorders and chronic kidney disease? Pharmacol Res 130:152–163. https://doi.org/10.1016/j.phrs.2018.01.020
Zheng J, Wittouck S, Salvetti E, Franz CMAP, Harris HMB, Mattarelli P, O’Toole PW, Pot B, Vandamme P, Walter J, Watanabe K, Wuyts S, Felis GE, Gänzle MG, Lebeer S (2020) A taxonomic note on the genus Lactobacillus: description of 23 novel genera, emended description of the genus Lactobacillus Beijerinck 1901, and union of Lactobacillaceae and Leuconostocaceae. Int J Syst Evol Microbiol 70(4):2782–2858. https://doi.org/10.1099/ijsem.0.004107
Albuquerque TMR, Garcia EF, Araújo AO, Magnani M, Saarela M, Souza EL (2018) In vitro characterization of Lactobacillus strains isolated from fruit processing by-products as potential probiotics. Probiotics Antimicrob Proteins 10(4):704–716. https://doi.org/10.1007/s12602-017-9318-2
Marcondes FK, Bianchi FJ, Tanno AP (2002) Determination of the estrous cycle phases of rats: some helpful considerations. Braz J Biol 62(4A):609–614. https://doi.org/10.1590/s1519-69842002000400008
Reeves PG, Nielsen FH, Fahey GC Jr (1993) AIN-93 purified diets for laboratory rodents: final report of the American institute of nutrition ad hoc writing committee on the reformulation of the AIN-76A rodent diet. J Nutr 123(11):1939–1951. https://doi.org/10.1093/jn/123.11.1939
Friedewald WT, Levy RI, Fredrickson DS (1972) Estimation of the concentration of low-density lipoprotein cholesterol in plasma, without use of the preparative ultracentrifuge. Clin Chem 18(6):499–502
Luna Freire MO, do Nascimento LCP, de Oliveira KAR, Oliveira AM, Napoleão TH, Dos Santos Lima M, Lagranha CJ, Souza EL, de Brito Alves JL (2021) Effects of a mixed Limosilactobacillus fermentum formulation with claimed probiotic properties on cardiometabolic variables, biomarkers of inflammation and oxidative stress in male rats fed a high-fat diet. Foods 10(9):2202. https://doi.org/10.3390/foods10092202
Pedroza A, Ferreira DS, Santana DF, Silva PT, Aguiar Júnior FCA, Sellitti DF, Lagranha CJ (2019) A maternal low-protein diet and neonatal overnutrition result in similar changes to glomerular morphology and renal cortical oxidative stress measures in male Wistar rats. Appl Physiol Nutr Metab 44(2):164–171. https://doi.org/10.1139/apnm-2018-0288
Bradford MM (1976) A rapid and sensitive method for the quantitation of microgram quantities of protein utilizing the principle of protein-dye binding. Anal Biochem 72:248–254. https://doi.org/10.1006/abio.1976.9999
Misra HP, Fridovich l (1972) The role of superoxide anion in the autoxidation of epinephrine and a simple assay for superoxide dismutase. J Biol Chem 247(10):3170–3175
Aebi H (1984) Catalase in vitro. Methods Enzymol 105:121–126. https://doi.org/10.1016/s0076-6879(84)05016-3
Habig WH, Pabst MJ, Jakoby WB (1974) Glutathione S-transferases: the first enzymatic step in mercapturic acid formation. J Biol Chem 249(22):7130–7139. https://doi.org/10.1016/S0021-9258(19)42083-8
Ellman GL (1959) Tissue sulfhydryl groups. Arch Biochem Biophys 82(1):70–77. https://doi.org/10.1016/0003-9861(59)90090-6
Garcia EF, Luciano WA, Xavier DE, Costa WCA, Oliveira KS, Franco OL, de Morais Júnior MA, Lucena BTL, Picão RC, Magnani M, Saarela M, Souza EL (2016) Identification of lactic acid bacteria in fruit pulp processing byproducts and potential probiotic properties of selected Lactobacillus strains. Front Microbiol 7:1–11. https://doi.org/10.3389/fmicb.2016.01371
Udomkasemsab A, Prangthip P (2019) High fat diet for induced dyslipidemia and cardiac pathological alterations in Wistar rats compared to Sprague Dawley rats. Clin Investig Arterioscler 31(2):56–62. https://doi.org/10.1016/j.arteri.2018.09.004
Gheibi S, Kashfi K, Ghasemi A (2017) A practical guide for induction of type-2 diabetes in rat: incorporating a high-fat diet and streptozotocin. Biomed Pharmacother 95:605–613. https://doi.org/10.1016/j.biopha.2017.08.098
Kullisaar T, Zilmer K, Salum T, Rehema A, Zilmer M (2016) The use of probiotic L. fermentum ME-3 containing Reg'Activ cholesterol supplement for 4 weeks has a positive influence on blood lipoprotein profiles and inflammatory cytokines: an open-label preliminary study. Nutr J 15(93):1–6. https://doi.org/10.1186/s12937-016-0213-6
Lye HS, Kato T, Low WY, Taylor TD, Prakash T, Lew LC, Ohno H, Liong MT (2017) Lactobacillus fermentum FTDC 8312 combats hypercholesterolemia via alteration of gut microbiota. J Biotechnol 262:75–83. https://doi.org/10.1016/j.jbiotec.2017.09.007
Wu Y, Li X, Tan F, Zhou X, Mu J, Zhao X (2021) Lactobacillus fermentum CQPC07 attenuates obesity, inflammation and dyslipidemia by modulating the antioxidant capacity and lipid metabolism in high-fat diet induced obese mice. J Inflamm (Lond) 18(5):1–11. https://doi.org/10.1186/s12950-021-00272-w
Archer AC, Muthukumar SP, Halami PM (2021) Lactobacillus fermentum MCC2759 and MCC2760 alleviate inflammation and intestinal function in high-fat diet-fed and streptozotocin-induced diabetic rats. Probiotics Antimicrob Proteins 13(4):1068–1080. https://doi.org/10.1007/s12602-021-09744-0
Venegas DP, De la Fuente MK, Landskron G, González MJ, Quera R, Dijkstra G, Harmsen HJM, Faber KN, Hermoso MA (2019) Short chain fatty acids (SCFAs)-mediated gut epithelial and immune regulation and its relevance for inflammatory bowel diseases. Front Immunol 10(277):1–16. https://doi.org/10.3389/fimmu.2019.00277
Xu M, Jiang Z, Wang C, Li N, Bo L, Zha Y, Bian J, Zhang Y, Deng X (2019) Acetate attenuates inflammasome activation through GPR43-mediated Ca2+-dependent NLRP3 ubiquitination. Exp Mol Med 51(7):1–13. https://doi.org/10.1038/s12276-019-0276-5
de Vadder F, Mithieux G (2018) Gut-brain signaling in energy homeostasis: the unexpected role of microbiota-derived succinate. J Endocrinol 236(2):R105–R108. https://doi.org/10.1530/JOE-17-0542
Zhong Y, Marungruang N, Fåk F, Nyman M (2015) Effects of two whole-grain barley varieties on caecal SCFA, gut microbiota and plasma inflammatory markers in rats consuming low- and high-fat diets. Br J Nutr 113(10):1558–1570. https://doi.org/10.1017/S0007114515000793
De Vadder F, Kovatcheva-Datchary P, Zitoun C, Duchampt A, Bäckhed F, Mithieux G (2016) Microbiota-produced succinate improves glucose homeostasis via intestinal gluconeogenesis. Cell Metab 24(1):151–157. https://doi.org/10.1016/j.cmet.2016.06.013
Kim YG, Sakamoto K, Seo SU, Pickard JM, Gillilland MG, Pudlo NA, Hoostal M, Li X, Wang TD, Feehley T, Stefka AT, Schmidt TM, Martens EC, Fukuda S, Inohara N, Nagler CR, Núñez G (2017) Neonatal acquisition of Clostridia species protects against colonization by bacterial pathogens. Science 356(6335):315–319. https://doi.org/10.1126/science.aag2029
Wu L, Parhofer KG (2014) Diabetic dyslipidemia. Metabolism 63(12):1469–1479. https://doi.org/10.1016/j.metabol.2014.08.010
Libby P (2002) Inflammation in atherosclerosis. Nature 420(6917):868–874. https://doi.org/10.1038/nature01323
Moreira APB, Texeira TFS, Ferreira AB, Peluzio MCG, Alfenas RCG (2012) Influence of a high-fat diet on gut microbiota, intestinal permeability and metabolic endotoxaemia. Br J Nutr 108(5):801–809. https://doi.org/10.1017/S0007114512001213
Scheller J, Chalaris A, Schmidt-Arras D (1813) Rose-John S (2011) The pro- and anti-inflammatory properties of the cytokine interleukin-6. Biochim Biophys Acta 5:878–888. https://doi.org/10.1016/j.bbamcr.2011.01.034
Lee J, Yang W, Hostetler A, Schultz N, Suckow MA, Stewart KL, Kim DD, Kim HS (2016) Characterization of the anti-inflammatory Lactobacillus reuteri BM36301 and its probiotic benefits on aged mice. BMC Microbiol 16(69):1–13. https://doi.org/10.1186/s12866-016-0686-7
Rodríguez-Nogales A, Algieri F, Vezza T, Garrido-Mesa N, Olivares M, Comalada M, Riccardi C, Utrilla MP, Rodríguez-Cabezas ME, Galvez J (2015) The viability of Lactobacillus fermentum CECT5716 is not essential to exert intestinal anti-inflammatory properties. Food Funct 6(4):1176–1184. https://doi.org/10.1039/c4fo00938j
Peran L, Camuesco D, Mnica Comalada M, Nieto A, Concha A, Adrio JL, Olivares M, Xaus J, Zarzuelo A, Galvez J (2006) Lactobacillus fermentum, a probiotic capable to release glutathione, prevents colonic inflammation in the TNBS model of rat colitis. Int J Colorectal Dis 21(8):737–746. https://doi.org/10.1007/s00384-005-0773-y
Pérez-Cano FJ, Dong H, Yaqoob P (2010) In vitro immunomodulatory activity of Lactobacillus fermentum CECT5716 and Lactobacillus salivarius CECT5713: two probiotic strains isolated from human breast milk. Immunobiology 215(12):996–1004. https://doi.org/10.1016/j.imbio.2010.01.004
Garcia-Castillo V, Komatsu R, Clua P, Indo Y, Takagi M, Salva S, Islam MA, Alvarez S, Takahashi H, Garcia-Cancino A, Kitazawa H, Villena J (2019) Evaluation of the immunomodulatory activities of the probiotic strain Lactobacillus fermentum UCO-979C. Front Immunol 10(1376):1–14. https://doi.org/10.3389/fimmu.2019.01376
Rahal A, Kumar A, Singh V, Yadav B, Tiwari R, Chakraborty S, Dhama K (2014) Oxidative stress, prooxidants, and antioxidants: the interplay. Biomed Res Int 2014:761264. https://doi.org/10.1155/2014/761264
Fernández-Sánchez A, Madrigal-Santillán E, Bautista M, Esquivel-Soto J, Morales-González A, Csar Esquivel-Chirino C, Durante-Montiel I, Sánchez-Rivera G, Valadez-Veja C, Morales-González JA (2011) Inflammation, oxidative stress, and obesity. Int J Mol Sci 12(5):3117–3132. https://doi.org/10.3390/ijms12053117
Rohr MW, Narasimhulu CA, Rudeski-Rohr TA, Parthasarathy S (2020) Negative effects of a high-fat diet on intestinal permeability: a review. Adv Nutr 11(1):77–91. https://doi.org/10.1093/advances/nmz061
Gulhane M, Murray L, Lourie R, Tong H, Sheng YH, Wang R, Kang A, Schreiber V, Wong KY, Magor G, Denman S, Begun J, Florin TH, Perkins A, Cuív PÓ, McGuckin MA, Hasnain SZ (2016) High fat diets induce colonic epithelial cell stress and inflammation that is reversed by IL-22. Sci Rep 6:28990. https://doi.org/10.1038/srep28990
Feillet-Coudray C, Fouret G, Vigor C, Bonafos B, Jover B, Blachnio-Zabielska A, Rieusset J, Casas F, Gaillet S, Landrier JF, Durand T, Coudray C (2019) Long-term measures of dyslipidemia, inflammation, and oxidative stress in rats fed a high-fat/high-fructose diet. Lipids 54(1):81–97. https://doi.org/10.1002/lipd.12128
Molina-Tijeras JA, Diez-Echave P, Vezza T, Hidalgo-García L, Ruiz-Malagón AJ, Rodríguez-Sojo MJ, Romero M, Robles-Vera I, García F, Plaza-Diaz J, Olivares M, Duarte J, Rodríguez-Cabezas ME, Rodríguez-Nogales A, Gálvez J (2021) Lactobacillus fermentum CECT5716 ameliorates high fat diet-induced obesity in mice through modulation of gut microbiota dysbiosis. Pharmacol Res 167:105471. https://doi.org/10.1016/j.phrs.2021.105471
Mikelsaar M, Zilmer M (2009) Lactobacillus fermentum ME-3 — an antimicrobial and antioxidative probiotic. Microb Ecol Health Dis 21(1):1–27. https://doi.org/10.1080/08910600902815561
Paolella G, Mandato C, Pierri L, Poeta M, Di Stasi M, Vajro P (2014) Gut-liver axis and probiotics: their role in non-alcoholic fatty liver disease. World J Gastroenterol 20(42):15518–15531. https://doi.org/10.3748/wjg.v20.i42.15518
Smolgovsky s, Ibeh u, Tamayo TP, Alcaide P (2021) Adding insult to injury — inflammation at the heart of cardiac fibrosis. Cell Signal 77:109828. https://doi.org/10.1016/j.cellsig.2020.109828
Trøseid M, Andersen GØ, Broch K, Hov JR (2020) The gut microbiome in coronary artery disease and heart failure: current knowledge and future directions. EBioMedicine 52:102649. https://doi.org/10.1016/j.ebiom.2020.102649
Han C, Jiang YH, Li W, Liu Y (2021) Astragalus membranaceus and Salvia miltiorrhiza ameliorates cyclosporin A-induced chronic nephrotoxicity through the “gut-kidney axis.” J Ethnopharmacol 269:113768. https://doi.org/10.1016/j.jep.2020.113768
Acknowledgements
The authors are grateful to the Coordenação de Aperfeiçoamento de Pessoal de nível Superior (CAPES, Brazil—Finance code 001) for the scholarships awarded to M.O. de Luna Freire (MSc student). The authors are also grateful to the CAPES for the scholarships awarded to K.Á.R. de Oliveira (post-doctoral). The authors are grateful to the Fundação de Apoio à Pesquisa do Estado da Paraíba (FAPESQ, Brazil) for the scholarships awarded to L.C.P. do Nascimento (PhD student). Additionally, the authors give thanks for the research productivity fellowship granted by the Brazilian National Council for Scientific and Technological Development (CNPq) to J.L. de Brito Alves.
Author information
Authors and Affiliations
Contributions
J.L. de Brito Alves designed the study. M.O. de Luna Freire, L.C.P. Nascimento, K.A.R. de Oliveira, A.M. Oliveira, and M.S. Lima conducted the experiments. M.O. de Luna Freire, L.C.P. Nascimento, and J.L. de Brito Alves analyzed the data. J.L. de Brito Alves prepared the manuscript. C.J. Lagranha, J.H. da Costa-Silva, and E.L. de Souza reviewed critically the manuscript.
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
de Luna Freire, M.O., do Nascimento, L.C.P., de Oliveira, K.Á.R. et al. Limosilactobacillus fermentum Strains with Claimed Probiotic Properties Exert Anti-oxidant and Anti-inflammatory Properties and Prevent Cardiometabolic Disorder in Female Rats Fed a High-Fat Diet. Probiotics & Antimicro. Prot. 15, 601–613 (2023). https://doi.org/10.1007/s12602-021-09878-1
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12602-021-09878-1