Abstract
Acute lung injury (ALI) is characterized by acute respiratory failure with tachypnea and widespread alveolar infiltrates, badly affecting patients’ health. Desflurane (Des) is effective against lung injury. However, its mechanism in ALI remains unknown. BEAS-2B cells were incubated with lipopolysaccharide (LPS) to construct an ALI cell model. Cell apoptosis was evaluated using flow cytometry. Enzyme-linked immunosorbent assay (ELISA) was employed to examine the levels of inflammatory cytokines. Interactions among let-7b-5p, homeobox A9 (HOXA9), and suppressor of cytokine signaling 2 (SOCS2) were verified using Dual luciferase activity, chromatin immunoprecipitation (ChIP), and RNA pull-down analysis. All experimental data of this study were derived from three repeated experiments. Des treatment improved LPS-induced cell viability, reduced inflammatory cytokine (tumor necrosis factor-α (TNF-α), interleukin-1β (IL-1β), and interleukin-6 (IL-6)) levels, decreased cell apoptosis, down-regulated the pro-apoptotic proteins (Bcl-2-associated X protein (Bax) and cleaved caspase 3) expression, and up-regulated the anti-apoptotic protein B-cell-lymphoma-2 (Bcl-2) expression in LPS-induced BEAS-2B cells. Des treatment down-regulated let-7b-5p expression in LPS-induced BEAS-2B cells. Moreover, let-7b-5p inhibition improved LPS-induced cell injury. let-7b-5p overexpression weakened the protective effects of Des. Mechanically, let-7b-5p could negatively modulate HOXA9 expression. Furthermore, HOXA9 inhibited the NF-κB signaling by enhancing SOCS2 transcription. HOXA9 overexpression weakened the promotion of let-7b-5p mimics in LPS-induced cell injury. Des alleviated LPS-induced ALI via regulating let-7b-5p/ HOXA9/NF-κB axis.
Graphical Abstract

Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Acute lung injury (ALI) is a heterogeneous disease induced by direct or indirect factors, such as trauma, infection, and blood transfusion, resulting in diffuse interstitial and alveolar edema, which is a form of respiratory failure [1, 2]. Characteristically, ALI progression is often accompanied by severe inflammatory response. Treatment for ALI usually includes general therapy (oxygen therapy), surgery, and medications (anti-inflammatory drugs) [3]. Specifically, ventilation strategies, prone positioning, extracorporeal support, neuromuscular blockade, and corticosteroid administration are the current management recommendations for acute respiratory distress syndrome treatment [4]. Although treatment can alleviate ALI to a certain extent, the prognosis of patients is poor, and the mortality rate is still high [5]. Therefore, there is an urgent need to study the pathogenesis of ALI and find molecular targets to improve ALI.
Desflurane (Des) is a new volatile anesthetic that, compared with other inhaled anesthetics, can promote rapid recovery after surgery and allow patients to return to early normal activities [6]. Intriguingly, several studies have reported that Des poses protective effects on lung injury caused by ventilator and sepsis [7, 8]. Therefore, it can be speculated that Des may have a therapeutic effect on ALI, while some studies have identified that Des inhalation can induce or even worsen lung injury [9]. The different effects of Des on lung injury may be associated with the different preparation of animal models, such as whether lipopolysaccharide (LPS) is employed to induce rats. Des may be protective against inflammatory lung injury but may promote lung injury in rats when administered alone. So, it is meaningful to clarify the precise function and mechanism of Des in ALI for further precisely utilizing it in clinical treatment. Published reports have identified that microRNAs (miRNAs) can be the targeted genes of anesthetics in cancers [10]. For instance, Des has been found to impact cell proliferation and migration by down-regulating miR-210 and miR-138, in an ovarian cancer cell model [11]. Inhalational anesthetics such as Des or sevoflurane have been shown to regulate the miR-138, -210, and -335 expression, which in turn can restrain the glioma cell malignancy progression, in the cellular model exploration [12]. Moreover, Des has been found to exert inhibitory effects on the metastatic process of colorectal cancer cells by negatively modulating miR-34a, in an in vitro model [13]. Furthermore, miRNAs can exert modulatory effects on the ALI process, for instance, miR-23a-3p, miR-182-5p, and miR-125b-5p have repressive effects on ALI progression of cell and animal models [14, 15]. Based on the above findings, we speculated that Des may regulate ALI by controlling the expression of miRNA. Furthermore, the expression level of let-7b-5p in the bronchoalveolar lavage fluid (BALF) of rats with smoke inhalation injuries has been significantly higher than that of normal rats [16]. More importantly, our preliminary experiment found that Des could down-regulate let-7b-5p expression in lipopolysaccharide (LPS)-induced BEAS-2B cells. Thus, it was speculated that Des may regulate let-7b-5p expression to participate in ALI progression.
MiRNAs play a vital function in controlling disease progression by targeting downstream genes [17]. Homeobox (HOX) is known to exert regulatory effects on embryonic development, vascular repair, angiogenesis, and tumor progression after birth [18]. According to a previous study, it has been observed that up-regulated homeobox A9 (HOXA9) expression in mesenchymal stem cells could ameliorate endotoxemia-induced ALI [19], suggesting a potential involvement of HOXA9 in LPS-induced ALI. Moreover, TargetScan predicted that let-7b-5p harbored the binding site on HOXA9, while the interaction has not been validated yet. The suppressor of cytokine signaling 2 (SOCS2) has been evidenced to be closely associated with inflammatory processes in miscellaneous diseases, such as the nonalcoholic steatohepatitis and osteoarthritis [20, 21]. Notably, KIAA0317, a ubiquitin E3 ligase, has promoted the ubiquitination degradation of SOCS2 to exacerbate inflammation injury in mice with LPS stimulation [22], indicating SOCS2 may play a regulatory role in ALI. HOX genes are a class of highly conserved evolutionary transcription factors that can bind to DNA sequences to regulate gene expression [23]. JASPAR also predicted that HOXA9 had a potential binding site on the SOCS2 promoter. Their interaction and regulatory mechanisms in ALI are worth further investigation.
Based on the above, we hypothesize that Des negatively regulates let-7b-5p expression. let-7b-5p targets HOXA9 and inhibits the NF-κB signaling through transcriptional activation of SOCS2, thereby attenuating LPS-induced ALI. Our study may identify potential targets of Des in the treatment of ALI.
Methods
Cell culture and treatment
Human lung epithelial cells (BEAS-2B) were acquired from ATCC (USA). Cells were cultured in Dulbecco’s modified Eagle’s medium (DMEM, Thermo Fisher Scientific, USA) supplementing with 10% fetal bovine serum (Thermo Fisher Scientific) and 1% penicillin/streptomycin (Beyotime, China), in a saturated humidity incubator at 37 ℃ and 5% CO2.
For the Des and LPS administration, cells were pretreated with Des concentrations of 0.5%, 2.5%, and 5.0%, respectively, for 45 min in sealed plastic chambers as described in previous studies [24]. To control and monitor Des concentrations, the chamber contained an inlet connector coupled to an anesthesia machine and an outlet connector linked to a gas monitor (Drägerwerk AG & Co., Germany). Thereafter, BEAS-2B cells were then stimulated with LPS (2 µg/ml, 24 h) according to the established protocol to establish an acute cell injury model [25].
Cell transfection
Let-7b-5p mimics and inhibitors and negative control (mimics NC and inhibitor NC, 30 nM) were purchased from GenePharma (China). Moreover, to overexpress the HOXA9, the full-length HOXA9 cDNA was subcloned into the pcDNA3.1 vector (Invitrogen, USA) to obtain the pcDNA3.1-HOXA9 vector (40 nM, overexpression HOXA9, marked as oe-HOXA9). Cells were transfected with the above plasmids for 48 h using Lipofectamine™ 3000 (Invitrogen, USA), following the instructions.
3-(4,5-dimethylthiazol-2-yl)-2,5-diphenyltetrazolium bromide (MTT) assay
Cells were cultured overnight in 96-well plates. The cells were then treated with MTT solution (10 μl, 5 mg/ml, Beyotime, China) for 4 h. Formazan solution (100 µl) was then added and incubated for 4 h. The absorbance was read at 570 nm using a microplate reader (Thermo Fisher Scientific). The detailed experimental protocol of the MTT assay was displayed in the Supplementary Materials.
Enzyme-linked immunosorbent assay (ELISA)
Cells were collected and centrifuged to obtain the supernatant. The levels of cytokines including IL-1β, TNF-α, and IL-6 in the culture medium were determined employing the ELISA kits (Nanjing Jiancheng Bioengineering Institute, China), in keeping with the attached instructions. The precise protocol was described in the Supplementary Materials.
Flow cytometry
Collected cells were cultured with 10 µL Annexin V-FITC and 5 µL PI stain in the darkness. After incubation for 10 min, apoptotic cells were immediately analyzed utilizing flow cytometry (BD Science, China). The relevant procedure was described in the Supplementary Materials.
Western blot
The total protein of BEAS-2B cells was extracted employing the RIPA buffer (Beyotime). Then proteins were separated by SDS-PAGE and electro-transferred onto the PVDF membrane. The membranes administrated the incubation of primary antibodies including Bcl-2 (ab182858, 1:2000, Abcam, UK), cleaved caspase 3 (ab32042, 1:500), Bax (ab32503, 1:5000), HOXA9 (ab140631, 1:5000), SOCS2 (ab109245, 1:5000), p-p65 (ab76302, 1:1000), p65 (ab32536, 1:10,000), IκB-α (ab32518, 1:10,000) and p-IκB-α (ab133462, 1:10,000), and GAPDH (ab8245, 1:5000) for 12 h at 4 °C, after blocking by 5% BSA. The membrane further received the incubation of secondary antibodies conjugated with HRP. An ECL kit (Thermo Fisher Scientific) was used to react with proteins on membranes. The densitometry analysis was estimated by ImageJ (National Institutes of Health, USA). The detailed experimental procedure was described in the Supplementary Materials.
Quantitative real-time polymerase chain reaction (qRT-PCR)
The total RNA of BEAS-2B cells was extracted using the TRIzol reagent (Beyotime). The cDNA synthesis steps were carried out with the assistance of the Script Reverse Transcription Reagent Kit (TaKaRa, China). The SYBR Premix Ex Taq II Kit (TaKaRa) was utilized for the qPCR process. Detailed information regarding the primer sequences can be found in Table 1. The 2−ΔΔCt formula was employed to calculate the relative change levels of the aimed genes of interest. GAPDH and U6 acted as internal normalizing genes.
Dual luciferase activity
Dual luciferase activity analysis was carried out to validate the interaction between let-7b-5p and HOXA9. Moreover, based on the prediction of the Starbase database (http://starbase.sysu.edu.cn/), there were potential binding sites between let-7b-5p and HOXA9. The sequences containing the potential binding sites (UACCUCA) of let-7b-5p on HOXA9 3′UTR were amplified and subcloned to the psiCHECK-2 vector (Promega, USA) to conduct wild-type (WT) vectors (HOXA9-WT). Then its mutated sites (AUGGAG) of seed sequences were designed and the mutation vectors (HOXA9-MUT) were established. BEAS-2B cells were co-transfected with the above vectors, let-7b-5p mimics or mimics NC. A dual luciferase reporter kit (Promega, USA) was employed to evaluate the luciferase activity, after 48 h incubation.
Chromatin immunoprecipitation (ChIP)
ChIP analysis was conducted to verify the interaction between HOXA9 and SOCS2. BEAS-2B cells were subjected to the cross-linking reaction with 1% paraformaldehyde. Chromatin was sonicated to acquire around 200–1000 bp fragments. The fragments were incubated with the primary antibody HOXA9 (ab140631, Abcam) or IgG (ab172730, Abcam) at 4 °C for 12 h. The immunoprecipitated DNA was analyzed using agarose gel electrophoresis.
RNA pull-down
For verifying the interaction between let-7b-5p and HOXA9, RNA pull-down analysis was utilized. BEAS-2B cells were transfected with a biotin-labeled probe against let-7b-5p. Then, cells were immersed in lysis buffer after washing. The lysate was incubated with streptavidin-coated magnetic beads at 4 °C, overnight. The HOXA9 enrichment was examined by qRT-PCR.
Statistical analysis
The data were expressed as mean ± standard deviation (SD) and analyzed using SPSS 23.0 software (SPSS, Inc., USA). The comparison of two groups was conducted using Student’s t-test, and one-way ANOVA followed by Tukey’s test was utilized for comparing multiple groups. A significance level of p < 0.05 was considered indicative of a significant difference. All data were derived from three repeated experiments.
Results
Des alleviated LPS-induced injury of BEAS-2B cells
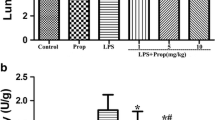
Des is an inhaled anesthetic commonly used clinically to reduce aberrant inflammation and cell injury [8]. To evaluate the effect of Des on LPS-induced lung injury, BEAS-2B cells were pretreated with different concentrations of Des (0.5%, 2.5%, 5.0%) and then stimulated with LPS (2 µg/ml). Firstly, we observed that LPS decreased cell viabilities of BEAS-2B cells using MTT assays, whereas Des pretreatment improved cell viabilities, and 2.5% Des had the best effect (Fig. 1A). Meanwhile, after LPS induction, inflammatory cytokine (IL-1β, TNF-α, and IL-6) levels were elevated, while Des significantly down-regulated the cytokine levels in BEAS-2B cells, and the greatest inhibitory effects were observed in the 2.5% Des group (Fig. 1B). Furthermore, LPS promoted cell apoptosis, which was also suppressed by Des pretreatment, especially with 2.5% Des (Fig. 1C). As anticipated, pro-apoptotic proteins including Bax and cleaved caspase 3 were increased, while the anti-apoptotic protein Bcl-2 was decreased in BEAS-2B cells with LPS stimulation, which trend was reversed by Des (Fig. 1D). Previous studies have suggested that Des may play a role in disease progression by regulating miRNA expression [26]. In this study, we studied the levels of several lung injury-related miRNAs in BEAS-2B cells, including miR-138, miR-214, miR-34a, miR-135b-5p, and let-7b-5p [27,28,29,30,31]. LPS caused a decrease in the level of miR-138 and an increase in the levels of miR-214, miR-34a, let-7b-5p, and miR-135b-5p. With the increase of Des concentration, the levels of miR-214, miR-34a, and let-7b-5p gradually decreased, among which the decrease of let-7b-5p was the most obvious (Fig. 1E). Taken together, Des could improve cell injury caused by LPS stimulation, which may be associated to let-7b-5p expression in BEAS-2B cells. Based on these results, a concentration of 2.5% Des was selected for further testing.
Des-alleviated LPS-induced injury of BEAS-2B cells. BEAS-2B cells were pretreated with different concentrations of Des (0.5%, 2.5%, 5.0%) and then received LPS stimulation. A Cell viability was evaluated using MTT. B Inflammatory cytokine levels were measured employing ELISA. C Cell apoptosis was examined by flow cytometry. D Bax, Bcl-2, and cleaved caspase 3 levels were determined using western blot. E miR-138, miR-214, miR-34a, miR-135b-5p, and let-7b-5p levels were analyzed by qRT-PCR. *p < 0.05, **p < 0.01, ***p < 0.001. All data were derived from three repeated experiments
let-7b-5p inhibition improved LPS-stimulated injury of BEAS-2B cells
Subsequently, we examined the modulatory role of let-7b-5p in LPS-induced cell injury. BEAS-2B cells were transfected with let-7b-5p inhibitor or inhibitor NC, after LPS inducement. LPS could memorably up-regulate let-7b-5p expression, while this phenomenon was abolished by let-7b-5p inhibitor transfection (Fig. 2A). Moreover, let-7b-5p silencing ameliorated the LPS-mediated decrease in cell viability by MTT assays (Fig. 2B). The silenced let-7b-5p also reversed the LPS-induced inflammatory cytokines’ increase (Fig. 2C). And let-7b-5p silencing decreased cell apoptosis which was induced by LPS (Fig. 2D). The transfection of let-7b-5p inhibitor down-regulated the Bax and cleaved caspase 3 expression and the up-regulated Bcl-2, under LPS treatment (Fig. 2E). Collectively, the let-7b-5p silencing played a protective role in the LPS-induced injury of BEAS-2B cells.
let-7b-5p inhibition improved LPS-stimulated injury of BEAS-2B cells. BEAS-2B cells were subjected to let-7b-5p inhibitor or inhibitor NC transfection and followed by LPS induction. A let-7b-5p level was analyzed by qRT-PCR. B Cell viability was evaluated using MTT. C Inflammatory cytokine levels were measured using ELISA. D Cell apoptosis was examined by flow cytometry. E Bax, Bcl-2, and cleaved caspase 3 levels were determined using western blot. *p < 0.05, **p < 0.01, ***p < 0.001. All data were derived from three repeated experiments
let-7b-5p overexpression impaired the Des-mediated protective effect on LPS-induced cell injury
To clarify whether Des affected LPS-induced cell injury by regulating let-7b-5p expression, BEAS-2B cells were transfected with let-7b-5p mimics or NC, following the Des pretreatment and LPS induction. Des markedly down-regulated let-7b-5p expression in LPS-induced BEAS-2B cells, which was reversed by let-7b-5p mimic transfection (Fig. 3A). In addition, let-7b-5p overexpression suppressed the Des-mediated improvement of cell viability under LPS via MTT assays (Fig. 3B). Under LPS induction, overexpression of let-7b-5p restrained the reduction of inflammatory factor secretion in Des-treated cells (Fig. 3C). Furthermore, the let-7b-5p overexpression reversed the Des-decreased cell apoptosis of BEAS-2B cells, under LPS stimulation (Fig. 3D). Also, Des up-regulated Bcl-2 protein expression and repressed Bax and cleaved caspase 3 expression in LPS-induced BEAS-2B cells, whereas these alterations were overturned by let-7b-5p overexpression (Fig. 3E). In summary, Des ameliorated LPS-stimulated cell injury by reducing let-7b-5p expression.
let-7b-5p overexpression impaired the Des-mediated protective effect on cell injury under LPS. BEAS-2B cells were transfected with let-7b-5p mimics or mimics NC and followed Des pretreatment and LPS induction. A let-7b-5p level was analyzed by qRT-PCR. B Cell viability was evaluated using MTT. C Inflammatory cytokine levels were measured using ELISA. D Cell apoptosis was examined by flow cytometry. E Bax, Bcl-2, and cleaved caspase 3 levels were determined using western blot. *p < 0.05, **p < 0.01, ***p < 0.001. All data were derived from three repeated experiments
let-7b-5p negatively regulated HOXA9 expression
Subsequently, we investigated the downstream molecules of let-7b-5p in LPS-aggravated cell injury. Bioinformatics databases (Targetscan, miRBD, Starbase, Tarbase, miRWalk) were capitalized on to predict let-7b-5p’s downstream molecules, and molecules including TRIM71, FAM118A, DUSP1, MTDH, and HOXA9 were obtained from overlap (Fig. 4A). HOXA9 and TRIM77 expressions were up-regulated, while DUSP1 was down-regulated, after the let-7b-5p silencing (Fig. 4B). As presented in Fig. 4C, let-7b-5p harbored binding sites on HOXA9. Therefore, we focused on whether Des could affect HOXA9 expression. First, LPS dramatically down-regulated HOXA9 expression, while this alteration was attenuated by Des (Fig. 4D, E). Moreover, the dual luciferase activity experiment validated that let-7b-5p mimics observably decreased the luciferase activity of the HOXA9-WT group, while it hardly influenced that in the HOXA9-MUT group (Fig. 4F). Meanwhile, RNA pull-down exhibited that Bio-let-7b-5p sense dramatically enriched HOXA9 rather than Bio-let-7b-5p anti-sense (Fig. 4G). After the overexpression of let-7b-5p, Des-up-regulated HOXA9 expression was down-regulated, while the HOXA9 overexpression overturned the trend, in LPS-induced BEAS-2B cells (Fig. 4H, I). Taken together, the let-7b-5p target negatively regulated HOXA9 expression, and this interaction was modulated by Des.
let-7b-5p negatively regulated HOXA9 expression. A Five overlapping genes (TRIM71, FAM118A, DUSP1, MTDH, and HOXA9) from five bioinformatics websites (Targetscan, miRBD, Starbase, Tarbase, miRWalk). B The levels of TRIM71, FAM118A, DUSP1, MTDH, and HOXA9 in BEAS-2B cell–transfected let-7b-5p inhibitor or inhibitor NC were determined using qRT-PCR. C The binding site between let-7b-5p and HOXA9. D, E HOXA9 expression in LPS-induced BEAS-2B cells with different concentrations of Des (0.5%, 2.5%, 5.0%) treatment was evaluated by qRT-PCR and western blot. F, G The validation of interaction between let-7b-5p and HOXA9 was conducted with a dual luciferase activity experiment and RNA pull-down. BEAS-2B cells were transfected with let-7b-5p inhibitor with/without oe-HOXA9 and followed by Des pretreatment and LPS stimulation. H, I HOXA9 expression was examined by qRT-PCR and western blot. *p < 0.05, **p < 0.01, ***p < 0.001. All data were derived from three repeated experiments
HOXA9 regulated the NF-κB pathway through transcriptional up-regulating SOCS2 expression
As previously described, SOCS2 degradation could aggravate pulmonary inflammation [22]. In the present study, we found that SOCS2 expression was down-regulated in LPS-induced BEAS-2B cells, while that was restored by Des treatment (Fig. 5A, B). In addition, as a transcription factor, HOXA9 is capable of regulating its downstream genes’ transcription [32]. As revealed in Fig. 5C, there were potential binding sites between HOXA9 and the promoter region of SOCS2. ChIP assay further validated that interaction (Fig. 5D). Then, HOXA9 expression was markedly up-regulated in the oe-HOXA9 transfected BEAS-2B cells (Fig. 5E, F). Furthermore, let-7b-5p mimics suppressed the Des-induced SOCS2 expression, whereas the inhibitory effect of let-7b-5p overexpression on SOCS2 was counteracted by the co-transfection of oe-HOXA9 and let-7b-5p mimics (Fig. 5G, H). Moreover, LPS induction significantly enhanced p-p65 and p-IκB-α expressions, which was offset by Des. However, let-7b-5p mimics eliminated Des-induced suppressing influences on p-p65 and p-IκB-α expression, which were further compromised by HOXA9 overexpression (Fig. 5H). In total, HOXA9 could inhibit the NF-κB signaling by transcriptional up-regulating SOCS2 expression.
HOXA9 regulated the NF-κB pathway through transcriptional up-regulating SOCS2 expression. A, B SOCS2 expression in LPS-induced BEAS-2B cells with different concentrations of Des (0.5%, 2.5%, 5.0%) pretreatment was evaluated by qRT-PCR and western blot. C The binding site between HOXA9 and the region of SOCS2 promoter. D The interaction between HOXA9 and SOCS2 promoter was verified by ChIP assay. E, F HOXA9 expression in BEAS-2B cells transfected with oe-NC or oe-HOXA9 was determined by qRT-PCR and western blot. BEAS-2B cells were transfected with let-7b-5p inhibitor with/without oe-HOXA9 and followed by LPS stimulation and Des treatment. G SOCS2 expression was detected using qRT-PCR. H SOCS2, p-p65, p65, IκB-α, and p-IκB-α levels were determined by western blot. *p < 0.05, **p < 0.01, ***p < 0.001. All data were derived from three repeated experiments
let-7b-5p promoted LPS-induced cell injury through silencing HOXA9 expression
Finally, we examined whether let-7b-5p played a regulatory role in LPS-induced lung injury through modulating HOXA9. After pretreatment with Des and LPS inducement, cells transfected with let-7b-5p mimic were further transfected with oe-NC or oe-HOXA9 vectors. After Des pretreatment, the overexpression of HOXA9 improved the cell viabilities of LPS-induced BEAS-2B cells, which abolished the let-7b-5p overexpression–induced viabilities’ decrease, using MTT assays (Fig. 6A). Furthermore, HOXA9 overexpression reduced the LPS-up-regulated inflammatory cytokine levels, which also reversed the effects of let-7b-5p overexpression (Fig. 6B). Moreover, HOXA9 decreased cell apoptosis, repressed Bax and cleaved caspase 3 expression, and promoted Bcl-2 in LPS-induced BEAS-2B cells with Des pretreatment, which weakened the effects of let-7b-5p overexpression (Fig. 6C, D). Thus, we concluded that let-7b-5p mimics exacerbated LPS-induced BEAS-2B cell injury by reducing HOXA9 expression.
let-7b-5p promoted LPS-induced cell injury through silencing HOXA9 expression. BEAS-2B cells were transfected with let-7b-5p inhibitor with/without oe-HOXA9 and followed by Des pretreatment and LPS stimulation. A Cell viability was evaluated using MTT. B Inflammatory cytokine (IL-1β, TNF-α, and IL-6) levels were measured using ELISA. C Cell apoptosis was examined by flow cytometry. D Bax, Bcl-2, and cleaved caspase 3 levels were determined using western blot. *p < 0.05, **p < 0.01, ***p < 0.001. All data were derived from three repeated experiments
Discussion
ALI is a form of severe acute respiratory distress syndrome, which leads to high morbidity and mortality. Current clinical treatment strategies targeting it have limited effectiveness in remission and cure [1]. Therefore, it is essential to explore effective medications for the treatment of ALI. In this study, we demonstrated that Des has an ameliorative effect on LPS-induced ALI. Furthermore, we found for the first time that Des could alleviate LPS-induced ALI via modulating the let-7b-5p/HOXA9/SOCS2/NF-κB axis.
Inhalational agents have been contended as an effective strategy for ameliorating lung injury [33]. In particular, inhalational agents are widely utilized in the current therapies for ALI, such as inhaled corticosteroids, prostaglandins, and nitric oxide [34,35,36]. Inhalational anesthesia has shown significant therapeutic effects in cellular models of a variety of diseases, including severe bronchospasm and cardiomyocyte hypoxia/reperfusion injury [24, 37]. Koutsogiannaki et al. have found that isoflurane attenuated LTB4-mediated responses by binding to BLT1 receptors, thereby reducing sepsis-induced mice lung injury [38]. Fu et al. have also reported that sevoflurane improved LPS-induced ALI in cell or mice models [39]. Specifically, inhalational anesthetics (such as sevoflurane and Des) have been identified to exert crucial effects in controlling the progression of asthma, chronic obstructive pulmonary disease (COPD), and bronchiectasis [40,41,42]. Additionally, Des is also revealed to exert a beneficial role in the ALI recovery progression. As mentioned earlier, Des pretreatment has attenuated the sepsis-induced lung injury in rats by suppressing the STAT3 pathway [8]. And Des has down-regulated ICAM-1 expression to alleviate LPS-induced ALI, in a lung microvascular endothelial cell model [43]. In this study, BEAS-2B cells were stimulated with LPS to create a cellular model of ALI. Des pretreatment at different concentrations had a protective effect on cell injury caused by LPS. Furthermore, we observed that Des down-regulated let-7b-5p expression in LPS-induced BEAS-2B cells, indicating that let-7b-5p may be involved in the protective effect of Des.
MiRNAs are a type of non-coding RNA that plays important modulatory roles under pathological and physiological conditions [44]. Some miRNAs, such as miRNA-762, miR-132-3p, and miR-96-5p, have been found to be involved in LPS-induced ALI [45,46,47]. Previous studies have shown that drugs can modulate disease progression by altering miRNA expression [10]. We screened that LPS up-regulated let-7b-5p expression in BEAS-2B cells, whereas Des significantly down-regulated its expression. This is consistent with previous findings that let-7b-5p expression levels are increased in COPD lung tissues and LPS-induced BEAS-2B cells [48]. Furthermore, we found that LPS induction could promote let-7b-5p expression, while down-regulation of let-7b-5p ameliorated LPS-induced cell injury. More importantly, we clarified that overexpression of let-7b-5p reversed the protective effect of Des in LPS-induced BEAS-2B cells. Experimental evidence shows that let-7b-5p may be a new target for Des treatment, and interfering with let-7b-5p may have a controlling effect on the therapeutic effect of Des.
Subsequently, we investigated the downstream molecules of let-7b-5p and their effects on lung disease progression. MiRNAs can modulate their downstream target gene expression to exert regulatory effects on disease progression [49]. In an LPS-induced ALI mice model, it has been found that the enhanced HOXA9 could alleviate ALI progression [19]. Our data indicated that HOXA9 expression was observably down-regulated in LPS-induced BEAS-2B cells, and Des pretreatment raised HOXA9 expression. That suggested that HOXA9 overexpression may pose the underlying protective effects on ALI. In addition, we discovered that let-7b-5p negatively regulated HOXA9 expression and that the silencing of HOXA9 aggravated LPS-induced cell injury. Moreover, HOXA9 has been widely reported to be associated with inflammatory diseases [20]. Further, Lear et al. have revealed that ubiquitination degradation of SOCS2 expression exacerbated lung inflammatory response [22]. Consistent with this, we found that SOCS2 expression was down-regulated in LPS-stimulated cells, but this repression was reversed by Des treatment. Meanwhile, HOXA9 could up-regulate SOCS2 expression through its transcription activation. Moreover, the NF-κB signaling is known to positively regulate inflammation but is negatively regulated by SOCS2 [20, 50]. This study demonstrated that HOXA9 could inhibit the NF-κB signaling by transcriptionally up-regulating SOCS2 expression, which further strengthened the mechanism by which HOXA9 regulated inflammation. In addition, there are still several limitations of our study. Previous studies have shown that Des can aggravate or improve lung injury [8, 9], but its exact role is controversial. It is a great draw for us to explore further in this perspective. Moreover, due to the current conditions and funding constraints, there was a lack of animal-level studies. Further, it remains elusive how Des regulates the let-7b-5p expression and whether let-7b-5p affects Des’s other functions. In the future, we will conduct the intratracheal/intranasal/aerosolized administration of drugs or intravenous injection of LPS pathways to establish the ALI animal model and further verify the findings in this study, if conditions permit [51, 52]. Meanwhile, ALI is always presented as the alveolar epithelial cell and capillary endothelial cell injury triggered by injury or infection in the lung, resulting in hypoxic respiratory insufficiency caused by non-cardiogenic pulmonary edema [53]. Therefore, we can explore the effects and mechanism of Des on that injury using the pulmonary microvascular endothelial cells in the further study. If permitted, the exploration of potentially different expressed lncRNA, circRNA, and proteins in Des-treated lung epithelial cells using microarray, proteomics, and high-throughput sequencing technique pathway can be helpful to clarify the mechanism of how Des regulates let-7b-5p. Furthermore, how does Des modulate the let-7b-5p expression, whether let-7b-5p can affect other functions of Des, or whether let-7b-5p can improve Des’s therapeutic efficacy in the Agomir-let-7b-5p injected animal model? The above-involved questions greatly attract our in-depth exploration. Furthermore, there is currently no specific medicine for ALI treatment, and the conventional medicines and treatments for ALI mainly include mechanical ventilation, vasodilators (nitric oxide, prostaglandin), surfactants, antioxidants, glucocorticoids, and anti-inflammation drugs. In addition, previous studies have indicated that Des inhalation can ameliorate mechanical ventilation–induced lung injury in rats [7]. This study provides experimental evidence for the potential clinical treatment of Des in ALI. Whether inhaled anesthetics should become part of the standard treatment of ARDS requires further clinical trials.
In conclusion, the present study first clarified that Des alleviated LPS-induced BEAS-2B cell injury by targeting the let-7b-5p/HOXA9/SOCS2 axis to inhibit the NF-κB signaling (Graphical abstract). Our findings revealed the function and mechanism of the let-7b-5p/HOXA9/SOCS2 axis in the Des treatment for ALI and provided the potential molecular target for the ALI. Precisely, let-7b-5p may be utilized as an underlying target for early diagnosis and supportive treatment of ALI.
Data availability
No datasets were generated or analysed during the current study.
Abbreviations
- ALI:
-
Acute lung injury
- Des:
-
Desflurane
- MiRNAs:
-
MicroRNAs
- BALF:
-
Bronchoalveolar lavage fluid
- LPS:
-
Lipopolysaccharide
- HOX:
-
Homeobox
- HOXA9:
-
Homeobox A9
- SOCS2:
-
Suppressor of cytokine signaling 2
- ELISA:
-
Enzyme-linked immunosorbent assay
- ChIP:
-
Chromatin immunoprecipitation
- SD:
-
Standard deviation
References
Long ME, Mallampalli RK, Horowitz JC. Pathogenesis of pneumonia and acute lung injury. Clin Sci (Lond). 2022;136(10):747–69. https://doi.org/10.1042/cs20210879.
Mowery NT, Terzian WTH, Nelson AC. Acute lung injury. Curr Probl Surg. 2020;57(5): 100777. https://doi.org/10.1016/j.cpsurg.2020.100777.
Chen X, Wang H, Jia K, Wang H, Ren T. Anti-Semaphorin-7A single chain antibody demonstrates beneficial effects on pulmonary inflammation during acute lung injury. Exp Ther Med. 2018;15(3):2356–64. https://doi.org/10.3892/etm.2018.5724.
Gorman EA, O’Kane CM, McAuley DF. Acute respiratory distress syndrome in adults: diagnosis, outcomes, long-term sequelae, and management. Lancet. 2022;400(10358):1157–70. https://doi.org/10.1016/S0140-6736(22)01439-8.
Goligher EC, Costa ELV, Yarnell CJ, Brochard LJ, Stewart TE, Tomlinson G, et al. Effect of lowering Vt on mortality in acute respiratory distress syndrome varies with respiratory system elastance. Am J Respir Crit Care Med. 2021;203(11):1378–85. https://doi.org/10.1164/rccm.202009-3536OC.
Woo JH, Baik HJ, Kim CH, Chung RK, Kim DY, Lee GY, et al. Effect of propofol and desflurane on immune cell populations in breast cancer patients: a randomized trial. J Korean Med Sci. 2015;30(10):1503–8. https://doi.org/10.3346/jkms.2015.30.10.1503.
Lin X, Ju YN, Gao W, Li DM, Guo CC. Desflurane attenuates ventilator-induced lung injury in rats with acute respiratory distress syndrome. Biomed Res Int. 2018;2018:7507314. https://doi.org/10.1155/2018/7507314.
Wang C, Liu N, Yang HT. Desflurane pretreatment can reduce sepsis-evoked lung injury in rats via inhibiting STAT3 pathway. J Biol Regul Homeost Agents. 2020;34(3):935–42. https://doi.org/10.23812/20-173-a-48.
Tosun M, Olmez H, Unver E, Arslan YK, Cimen FK, Ozcicek A et al. Oxidative and pro-inflammatory lung injury induced by desflurane inhalation in rats and the protective effect of rutin. Adv Clin Exp Med. 2021;30(9):941–8. https://doi.org/10.17219/acem/136194.
Tabnak P, Masrouri S, Geraylow KR, Zarei M, Esmailpoor ZH. Targeting miRNAs with anesthetics in cancer: Current understanding and future perspectives. Biomed Pharmacother. 2021;144: 112309. https://doi.org/10.1016/j.biopha.2021.112309.
Ishikawa M, Iwasaki M, Zhao H, Saito J, Hu C, Sun Q, et al. Sevoflurane and desflurane exposure enhanced cell proliferation and migration in ovarian cancer cells via miR-210 and miR-138 downregulation. Int J Mol Sci. 2021;22(4):1826. https://doi.org/10.3390/ijms22041826.
Ishikawa M, Iwasaki M, Zhao H, Saito J, Hu C, Sun Q, et al. Inhalational anesthetics inhibit neuroglioma cell proliferation and migration via miR-138, -210 and -335. Int J Mol Sci. 2021;22(9):4355. https://doi.org/10.3390/ijms22094355.
Ren J, Wang X, Wei G, Meng Y. Exposure to desflurane anesthesia confers colorectal cancer cells metastatic capacity through deregulation of miR-34a/LOXL3. Eur J Cancer Prev. 2021;30(2):143–53. https://doi.org/10.1097/CEJ.0000000000000608.
Xiao K, He W, Guan W, Hou F, Yan P, Xu J, et al. Mesenchymal stem cells reverse EMT process through blocking the activation of NF-kappaB and Hedgehog pathways in LPS-induced acute lung injury. Cell Death Dis. 2020;11(10):863. https://doi.org/10.1038/s41419-020-03034-3.
Shen K, Wang X, Wang Y, Jia Y, Zhang Y, Wang K, et al. miR-125b-5p in adipose derived stem cells exosome alleviates pulmonary microvascular endothelial cells ferroptosis via Keap1/Nrf2/GPX4 in sepsis lung injury. Redox Biol. 2023;62: 102655. https://doi.org/10.1016/j.redox.2023.102655.
Xiao P, Sun S, Cao J, Wang J, Li H, Hou S, et al. Expression profile of microRNAs in bronchoalveolar lavage fluid of rats as predictors for smoke inhalation injury. Burns. 2018;44(8):2042–50. https://doi.org/10.1016/j.burns.2018.07.009.
Wu CY, Ghule SS, Liaw CC, Achudhan D, Fang SY, Liu PI, et al. Ugonin P inhibits lung cancer motility by suppressing DPP-4 expression via promoting the synthesis of miR-130b-5p. Biomed Pharmacother. 2023;167: 115483. https://doi.org/10.1016/j.biopha.2023.115483.
Tang L, Peng L, Tan C, Liu H, Chen P, Wang H. Role of HOXA9 in solid tumors: mechanistic insights and therapeutic potential. Cancer Cell Int. 2022;22(1):349. https://doi.org/10.1186/s12935-022-02767-9.
Xin X, Yan L, Guangfa Z, Yan H, Keng L, Chunting W. Mesenchymal stem cells promoted lung wound repair through Hox A9 during endotoxemia-induced acute lung injury. Stem Cells Int. 2017;2017:3648020. https://doi.org/10.1155/2017/3648020.
Li S, Han S, Jin K, Yu T, Chen H, Zhou X, et al. SOCS2 suppresses inflammation and apoptosis during NASH progression through limiting NF-κB activation in macrophages. Int J Biol Sci. 2021;17(15):4165–75. https://doi.org/10.7150/ijbs.63889.
Shi L, Hu H, Sun P, Li Z, Ji L, Liu S, et al. RPL38 knockdown inhibits the inflammation and apoptosis in chondrocytes through regulating METTL3-mediated SOCS2 m6A modification in osteoarthritis. Inflamm Res. 2022;71(7–8):977–89. https://doi.org/10.1007/s00011-022-01579-x.
Lear TB, McKelvey AC, Evankovich JW, Rajbhandari S, Coon TA, Dunn SR, et al. KIAA0317 regulates pulmonary inflammation through SOCS2 degradation. JCI Insight. 2019;4(19):e129110. https://doi.org/10.1172/jci.insight.129110.
Zhou X, Lu R. HOXA9/MEIS1 targets in leukemia: reinforced signaling networks and therapeutic opportunities. Haematologica. 2023;108(5):1205–7. https://doi.org/10.3324/haematol.2022.281779.
Adi O, Apoo FN, Fong CP, Ahmad AH, Roslan NL, Khan FA et al. Inhaled volatile anesthetic gas for severe bronchospasm in the emergency department. Am J Emerg Med. 2023;68:213.e5-.e9. https://doi.org/10.1016/j.ajem.2023.04.032.
Li P, Gu L, Bian Q, Jiao D, Xu Z, Wang L. Long non-coding RNA MALAT1 enhances the protective effect of dexmedetomidine on acute lung injury by sponging miR-135a-5p to downregulate the ratio of X-box binding proteins XBP-1S/XBP-1U. Bioengineered. 2021;12(1):6377–89. https://doi.org/10.1080/21655979.2021.1967579.
Yu Y, Zhang Y. Desflurane accelerates neuronal cytotoxicity of Aβ by downregulating miR-214. Neurosci Lett. 2013;554:28–33. https://doi.org/10.1016/j.neulet.2013.08.063.
Chen S, Ding R, Hu Z, Yin X, Xiao F, Zhang W, et al. MicroRNA-34a inhibition alleviates lung injury in cecal ligation and puncture induced septic mice. Front Immunol. 2020;11:1829. https://doi.org/10.3389/fimmu.2020.01829.
He K, Han S, An L, Zhang J. Inhibition of microRNA-214 alleviates lung injury and inflammation via increasing FGFR1 expression in ventilator-induced lung injury. Lung. 2021;199(1):63–72. https://doi.org/10.1007/s00408-020-00415-5.
Li Z, Yu Y, Liu C, Chen G, Gong W, Luo J, et al. Identification of the key ferroptosis-related genes involved in sepsis progression and experimental validation in vivo. Front Pharmacol. 2022;13: 940261. https://doi.org/10.3389/fphar.2022.940261.
Liu F, Yang Y, Peng W, Zhao N, Chen J, Xu Z, et al. Mitophagy-promoting miR-138-5p promoter demethylation inhibits pyroptosis in sepsis-associated acute lung injury. Inflamm Res. 2023;72(2):329–46. https://doi.org/10.1007/s00011-022-01675-y.
Zang BB, Li H, Yang Y, Xie H, Xu XT. [The role of miR-135b-5p in inhibiting mice acute lung injury (ALI) induced by sepsis and its mechanism]. Zhongguo Ying Yong Sheng Li Xue Za Zhi. 2022;38(4):366–72. https://doi.org/10.12047/j.cjap.6263.2022.069.
Lambert M, Alioui M, Jambon S, Depauw S, Van Seuningen I, David-Cordonnier MH. Direct and indirect targeting of HOXA9 transcription factor in acute myeloid leukemia. Cancers (Basel). 2019;11(6):837. https://doi.org/10.3390/cancers11060837.
Zhao R, Wang L, Wang T, Xian P, Wang H, Long Q. Inhalation of MSC-EVs is a noninvasive strategy for ameliorating acute lung injury. J Control Release. 2022;345:214–30. https://doi.org/10.1016/j.jconrel.2022.03.025.
Zhuang C, Kang M, Lee M. Delivery systems of therapeutic nucleic acids for the treatment of acute lung injury/acute respiratory distress syndrome. J Control Release. 2023;360:1–14. https://doi.org/10.1016/j.jconrel.2023.06.018.
Fuller BM, Mohr NM, Skrupky L, Fowler S, Kollef MH, Carpenter CR. The use of inhaled prostaglandins in patients with ARDS: a systematic review and meta-analysis. Chest. 2015;147(6):1510–22. https://doi.org/10.1378/chest.14-3161.
Redaelli S, Pozzi M, Giani M, Magliocca A, Fumagalli R, Foti G, et al. Inhaled nitric oxide in acute respiratory distress syndrome subsets: rationale and clinical applications. J Aerosol Med Pulm Drug Deliv. 2023;36(3):112–26. https://doi.org/10.1089/jamp.2022.0058.
An L, Zhong Y, Tan J, Liu Y, Li A, Yang T, et al. Sevoflurane exerts protection against myocardial ischemia-reperfusion injury and pyroptosis through the circular RNA PAN3/microRNA-29b-3p/stromal cell-derived factor 4 axis. Int Immunopharmacol. 2023;120: 110219. https://doi.org/10.1016/j.intimp.2023.110219.
Koutsogiannaki S, Okuno T, Kobayashi Y, Ogawa N, Yuki K. Isoflurane attenuates sepsis-associated lung injury. Biochem Biophys Res Commun. 2022;599:127–33. https://doi.org/10.1016/j.bbrc.2022.02.028.
Fu Z, Wu X, Zheng F, Zhang Y. Sevoflurane anesthesia ameliorates LPS-induced acute lung injury (ALI) by modulating a novel LncRNA LINC00839/miR-223/NLRP3 axis. BMC Pulm Med. 2022;22(1):159. https://doi.org/10.1186/s12890-022-01957-5.
Schutte D, Zwitserloot AM, Houmes R, de Hoog M, Draaisma JM, Lemson J. Sevoflurane therapy for life-threatening asthma in children. Br J Anaesth. 2013;111(6):967–70. https://doi.org/10.1093/bja/aet257.
Karacaer F, Biricik E, Ilginel M, Lafli Tunay D, Baydar O, Avci A, et al. Effects of ketamine infusion on oxygenation in patients with chronic obstructive pulmonary disease undergoing lung cancer surgery. Turk J Anaesthesiol Reanim. 2023;51(1):16–23. https://doi.org/10.5152/TJAR.
Antoniu SA. Investigational inhaled therapies for non-CF bronchiectasis. Expert Opin Investig Drugs. 2018;27(2):139–46. https://doi.org/10.1080/13543784.2018.1427728.
Luo X, Miao CH, Ge BX, Jiang H. Effects of isoflurane, sevoflurane and desflurane on expression of ICAM-1 and VCAM-1 in LPS-induced rat lung microvascular endothelial cells. Zhejiang Da Xue Xue Bao Yi Xue Ban. 2010;39(5):464–9. https://doi.org/10.3785/j.issn.1008-9292.2010.05.004.
Cui Y, Qi Y, Ding L, Ding S, Han Z, Wang Y, et al. miRNA dosage control in development and human disease. Trends Cell Biol. 2023;34(1):31–47. https://doi.org/10.1016/j.tcb.2023.05.009.
Li C, Liu JH, Su J, Lin WJ, Zhao JQ, Zhang ZH, et al. LncRNA XIST knockdown alleviates LPS-induced acute lung injury by inactivation of XIST/miR-132-3p/MAPK14 pathway: XIST promotes ALI via miR-132-3p/MAPK14 axis. Mol Cell Biochem. 2021;476(12):4217–29. https://doi.org/10.1007/s11010-021-04234-x.
Wu W, Zhong W, Xu Q, Yan J. Silencing of long non-coding RNA ZFAS1 alleviates LPS-induced acute lung injury by mediating the miR-96-5p/OXSR1 axis in sepsis. Am J Med Sci. 2022;364(1):66–75. https://doi.org/10.1016/j.amjms.2022.03.008.
Zhang XL, An J, Deng YZ, Fang XZ, Xu CY, Liu XF, et al. A novel miRNA-762/NFIX pathway modulates LPS-induced acute lung injury. Int Immunopharmacol. 2021;100: 108066. https://doi.org/10.1016/j.intimp.2021.108066.
Wang Y, Chen J, Chen W, Liu L, Dong M, Ji J, et al. LINC00987 ameliorates COPD by regulating LPS-induced cell apoptosis, oxidative stress, inflammation and autophagy through let-7b-5p/SIRT1 axis. Int J Chron Obstruct Pulmon Dis. 2020;15:3213–25. https://doi.org/10.2147/copd.S276429.
Li P, Hao X, Liu J, Zhang Q, Liang Z, Li X, et al. miR-29a-3p regulates autophagy by targeting Akt3-mediated mTOR in SiO2-induced lung fibrosis. Int J Mol Sci. 2023;24(14):11440. https://doi.org/10.3390/ijms241411440.
Yu H, Lin L, Zhang Z, Zhang H, Hu H. Targeting NF-κB pathway for the therapy of diseases: mechanism and clinical study. Signal Transduct Target Ther. 2020;5(1):209. https://doi.org/10.1038/s41392-020-00312-6.
Kuhar E, Chander N, Stewart DJ, Jahandideh F, Zhang H, Kristof AS, et al. A preclinical systematic review and meta-analysis assessing the effect of biological sex in lipopolysaccharide-induced acute lung injury. Am J Physiol Lung Cell Mol Physiol. 2024. https://doi.org/10.1152/ajplung.00336.2023.
Yang C, Song C, Liu Y, Qu J, Li H, Xiao W, et al. Re-Du-Ning injection ameliorates LPS-induced lung injury through inhibiting neutrophil extracellular traps formation. Phytomedicine. 2021;90: 153635. https://doi.org/10.1016/j.phymed.2021.153635.
Hsieh PC, Wu YK, Yang MC, Su WL, Kuo CY, Lan CC. Deciphering the role of damage-associated molecular patterns and inflammatory responses in acute lung injury. Life Sci. 2022;305: 120782. https://doi.org/10.1016/j.lfs.2022.120782.
Acknowledgements
This work was supported by Young Scholar Project of the First Affiliated Hospital of Nanchang University (YFYPY202215).
Author information
Authors and Affiliations
Contributions
Xiaoyun Shi and Xiuhong Wang wrote the main manuscript text and Yundie Li, Shibiao Chen, and Huaping Xu prepared figures. All authors reviewed the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Shi, X., Li, Y., Chen, S. et al. Desflurane alleviates LPS-induced acute lung injury by modulating let-7b-5p/HOXA9 axis. Immunol Res 72, 683–696 (2024). https://doi.org/10.1007/s12026-024-09474-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12026-024-09474-9