Abstract
Osteoarthritis (OA) is a general joint disease. Cartilage damage is associated with a decrease in the density of chondrocytes. Mesenchymal stem cells (MSCs) differentiate into adipocytes, osteocytes and chondrocytes, and are an excellent source of cell therapy. Cartilage-derived extracellular matrix (ECM) promotes chondrogenesis of MSCs. However, the role of MSCs stimulated by ECM is not well known in OA. The purpose of this study is to determine the role of specific factors generated by the application of ECM and umbilical cord blood-derived mesenchymal stem cells (UCB-MSCs) in managing OA symptoms. Cartilage acellular matrix (CAM), which is a cartilage-derived ECM, was used to promote the chondrogenesis of UCB-MSCs. Induced MSCs were analyzed using chondrogenic markers (aggrecan, collagen type 2, and SOX9) and bone morphogenic protein 6 (BMP6). BMP6 is known to be involved in early chondrogenesis of MSCs. As a result, treatment with CAM significantly increased the expression of chondrogenic markers and BMP6 in UCB-MSCs. Treatment with recombinant human BMP6 also dramatically increased the levels of chondrogenic markers in UCB-MSCs. In addition, UCB-MSCs and CAM were used to evaluate OA symptom improvement in a rabbit articular cruciate ligament transection (ACLT) model. Application of UCB-MSCs and CAM enhanced not only the structure and synthesis of proteoglycan and collagen type 2 but also anti-inflammatory effects in both rabbit joint and synovial fluid. Moreover, the detection of human cells and involvement of BMP6 were confirmed in rabbit cartilage tissues. This study indicates that therapeutic potential of UCB-MSCs with CAM is mediated via BMP6 in OA.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Osteoarthritis (OA) is the most common joint disease characterized by degenerative changes in the cartilage. It is one of the major causes of limited activity in the elderly [1, 2]. OA is also caused by a decrease in chondrocyte density with a concomitant increase in enzymes (collagenase, aggrecanase, etc.) that degrade extracellular matrix (ECM) [3, 4]. In chondrocytes that are completely differentiated, ECM production gradually diminishes due to apoptosis, making it difficult to maintain normal cartilage structure. In OA, chondrocytes exhibit hypertrophy and decreased production of ECM proteins such as type 2 collagen (COL2) and aggrecan (AGG) [5,6,7]. Damaged cartilage generally has limited self-healing capacity. Systemic administration of non-steroidal anti-inflammatory drugs (NSAIDs), corticosteroids, and analgesics or intra-articular injection of hyaluronic acid (HA) have been used to prevent cartilage damage and relieve pain induced by such damage [8]. However, pharmacological therapies are unable to regenerate cartilage. Recently, stem cell therapy for protection and regeneration of cartilage has attracted significant attention [9].
Mesenchymal stem cells (MSCs) are found in various tissues, including fat [10], bone marrow [11], the umbilical cord [12], and placental tissue [13]. They are capable of differentiating into mesodermal lineage cells. Human umbilical cord blood-derived mesenchymal stem cells (UCB-MSCs) are an excellent cellular resource for the treatment of various disorders including OA [14,15,16,17,18]. Moreover, UCB-MSCs are associated with several advantages, including noninvasive collection, immunoregulation, and differentiation [19, 20]. Several studies have demonstrated the role of UCB-MSCs in promoting regeneration of damaged cartilage [21, 22]. In addition, MSC injections with platelet-rich plasma (PRP) or HA for the treatment of OA have been reported in many studies [23,24,25,26,27]. Of particular relevance for OA, extracellular matrix (ECM) derived from cartilage extract promotes chondrogenic differentiation of MSCs. Treatment with MSCs combined with cartilage extract derived ECM, regenerated cartilage damage in a rabbit articular cartilage defect (ACD) model [28].
Cartilage-derived ECM also known as cartilage acellular matrix (CAM) is complex and similar to that of natural cartilage [29]. It facilitates the regeneration of mature cartilage. The components of CAM are similar to cartilage based on collagen and proteoglycan content measurements [30]. In addition, tissue-derived ECM is biodegradable, and therefore, of interest in tissue engineering studies [31].
Bone morphogenetic proteins (BMPs) are a subfamily of the TGFβ superfamily. They are important factors during early mammalian development. They also participate in the induction of bone and cartilage formation [32, 33]. BMP6 enhances chondrogenesis of MSCs [34,35,36,37]. However, the mechanism of cartilage regeneration by MSCs is currently unknown.
We hypothesized that treatment with UCB-MSCs combined with CAM would regenerate cartilage. Thus, the purpose of this study is to determine the relevant factors via application of ECM and UCB-MSCs in the management of OA symptoms. Our results showed that CAM promoted chondrogenesis of UCB-MSCs. In addition, CAM-treated UCB-MSCs had a paracrine effect in promoting chondrogenesis of other naïve UCB-MSCs. UCB-MSCs differentiated with CAM also increased the levels of BMP6 mRNA expression. Moreover, chondrogenesis was confirmed using recombinant BMP6 protein in UCB-MSCs based on therapeutic effects in rabbit articular cruciate ligament transection (ACLT) models. Our findings suggest that combining UCB-MSCs with CAM may have a therapeutic effect via BMP6 signaling in OA. Such a combination might be therapeutically effective in OA patients.
Materials and Methods
Isolation, Culture, and Characterization of UCB-MSC
UCB-MSCs (passage 4–6, Kangstem Biotech, Seoul, Korea) were cultured in KSB-3 medium (Kangstem Biotech) supplemented with 10% fetal bovine serum (FBS, Gibco, Gaithersburg, MD, USA) and 1% GA-1000 (Lonza, Basel, Switzerland) at 37 °C with 5% CO2. Isolation, culture, and characterization of UCB-MSCs were performed according to published procedures [38].
Cytotoxicity Evaluation of CAM
Cartilage acellular matrix (CAM, Atems, Suwon, Korea, http://www.atems.co.kr/index_en.html) was isolated from porcine joint cartilage. CAM was prepared and verified as described previously [39]. After seeding UCB-MSCs into 24-well plates at a density of 3 × 104 cells/well, cells were treated with various concentrations (5, 10, and 20 mg/mL) of CAM for 3 days. These cells were treated with a Cell Counting Kit-8 (CCK-8, Dojindo, Tokyo, Japan) reagent for 1 h. Absorbance of incubated medium was measured at a wavelength of 450 nm to evaluate cytotoxicity.
Induction of Chondrogenic Differentiation of hUCB-MSCs
Following the attachment of UCB-MSCs (5 × 105 cells/ 5 μl) for 2 h, the chondrogenic differentiation medium (StemPro Chondrogenesis Differentiation Kit, Thermo Fisher, San Jose, CA, USA), CAM (5, 10, and 20 mg/mL) or recombinant human bone morphogenetic protein 6 (rhBMP6, 500 ng/mL, R&D System, Minneapolis, MN, USA) was added for 7 days. Cells undergoing chondrogenic induction were fixed with 4% paraformaldehyde and stained with 1% Alcian blue for 20 min.
Real-Time Polymerase Chain Reaction (RT-PCR) Analysis of Gene Expression
RNA was extracted with TRIzol® (Invitrogen, Carlsbad, CA, USA) solution and cDNA was synthesized using AccuPower RT PreMix (Bioneer, Daejeon, Korea). RT-PCR was performed with the synthesized cDNA sample as a template using PowerUp™ SYBR® Green Master Mix (Thermo Fisher, San Jose, CA, USA). Corresponding primers are shown in Table 1. The expression of target genes was normalized with RPL13a.
Co-Culture of Chondrogenic Induced UCB-MSCs by CAM with Undifferentiated UCB-MSCs
UCB-MSCs (5 × 105 cells/ 5 μl) with CAM were induced by chondrogenic medium for 7 days. After washing with PBS, cells were co-cultured in a transwell (Transwell® with 0.4 μm Pore Polycarbonate Membrane Insert, Corning, NY, USA) with undifferentiated UCB-MSCs (5 × 105 cells/5 μl) in chondrogenic medium (StemPro Chondrogenesis Differentiation Kit, Thermo Fisher, San Jose, CA, USA) for 7 days.
BMP6 Elisa
UCB-MSCs were cultured with or without CAM in 60 mm culture dishes (Thermo Fisher, San Jose, CA, USA) for 7 days. These cells were then cultured in serum-free DMEM for 3 days. Cells were then lysed with RIPA buffer. Cell culture supernatant was collected after centrifugation at 1500 rpm for 5 min. The expression of BMP6 in cell lysate or supernatant was quantified using a human BMP6 ELISA kit (R&D System, Minneapolis, MN, USA) according to the manufacturer’s protocol.
Experimental Animals
This experiment was approved by the Institutional Animal Care and Use Committee (IACUC) of Chungbuk National University Laboratory Animal Research Center and performed in accordance with the Standard Operation Procedures (SOP) of the same facility. Ten-week-old male New Zealand white (NZW) rabbits (Daehanbiolink, Eumseong, Korea) were raised until more than 12 weeks of age (marked by cessation of growth of the growth plate) until they weighed 2.8~3.2 kg, an appropriate weight for surgery. Rabbits were individually housed in rabbit cages starting from the time of receipt until the time of autopsy. The environment of the animal laboratory was controlled at a temperature of 23 ± 2 °C, a relative humidity of 55 ± 10%, a ventilation frequency of 12 times/h, lighting cycle of 12 h, and illumination of 150–300 Lux. LabDiet #5325, a pellet-type solid food (Orient Bio, Seongnam, Korea) was used as a rabbit feed. Sterile distilled water was provided without any restriction.
Establishment of Anterior Cruciate Ligament Transection (ACLT) Model
Rabbits were intramuscularly injected with Zoletil® 50 (15 mg/kg, Virbac Laboratories) and Rompum® (5 mg/kg, Bayer) to induce general anesthesia. After removing hair around the right knee, the skin was disinfected with povidone-iodine and 70% ethanol. The site for surgery was aseptically treated to initiate the procedure. After cutting the medial skin of the knee joint, fascia, and joint capsule, the anterior cruciate ligament (ACL) was exposed by moving the knee bone outward. After completely cutting medial parenchyma of the ACL and the meniscus ligament with a surgical blade, the joint capsule was closed. The subcutaneous tissue and skin were sutured and disinfected with povidone-iodine. Antibiotic Foxolin® (10 mg/kg, Samjin Pharmaceuticals, Hwasung, Korea) and analgesic Maritrol® (3 mg/kg, Jeil Pharmaceuticals) were intramuscularly administered once daily for 3 days after surgery. Foxolin® was administered once daily for an additional 3 days.
UCB-MSCs and CAM Transplantation into Cartilage Disease Models
Rabbits with ACLT were randomly distributed into five groups: normal (n = 3), ACLT (n = 5), CAM alone (n = 5), and UCB-MSCs with or without CAM (each group, n = 5). UCB-MSCs (2.5 × 106 cells) and/or CAM (20 mg/mL) in each group were suspended in 200 μl of saline, and transplanted intra-articularly using 26G 1/2 syringes (Kovax-syringe, Seoul, Korea) at 8 weeks after the ACLT surgery (Fig. 1).
Radiological and Behavioral Tests in ACLT Model
At 8 weeks after ACLT, the right knee joint was corrected in the cranio-caudal (Cr / Cd) view and radiographs were taken with a portable X-ray instrument (Genoray Seongnam, Korea). Results were scored with a modified Kellgren-Lawrence score system (KL grade). Animals were allowed to walk freely in a wide animal room. Behavioral tests for induced arthritis were then conducted and used to separate groups based on KL grade. In addition, radiological and behavioral tests were performed at 3, 5 and 7 weeks after transplantation to evaluate the degree of arthritis progression (Table S1, Fig. 1).
Visual and Histopathological Evaluation of OA in Rabbit ACLT Models
Rabbits were sacrificed at 8 weeks after transplantation in ACLT. The supracondylar portion of the femur including arthritis-induced site was then collected. Photographs of femoral condyle and tibial plateau of knee joints were taken with a digital camera. Erosion of the joint surface, changes in surface, osteophyte, and enlargement of the femoral condyle were evaluated as shown in Table S2.
Sliced tissues were stained with H&E to determine the structural changes in the cartilage regeneration site. After Safranin O staining, the proteoglycan content was analyzed as an index of chondrocyte differentiation and proliferation using Image J 4.8v (NIH). In addition, ALP staining and TRAP staining were performed to determine the activities of osteoblasts and osteoclasts, respectively. Total histopathological analysis was calculated according to Table S3.
Synovial Fluid Collection and Analysis in the ACLT Model
Rabbits undergoing general anesthesia were injected intra-articularly with saline. After pumping twice with saline, joint fluid was collected. Collected fluid was treated with collagenase (400 μg/mL) and hyaluronidase (40 U/mL) at 37 °C for 10 min. The levels of inflammatory cytokines (TNF-α, IL-1β, IL-6, and IL-8) were analyzed with ELISA (TNF-αand IL-1β, R&D System, Minneapolis, MN, USA) (IL-6, IL-8, RayBiotech, Norcross, GA, USA) according to each manufacturer’s protocol.
Immunofluorescence
Tissue sections were deparaffinized and treated with antigen retrieval buffer (Dako, Glostrup, Denmark). They were then permeabilized and blocked with Triton X-100 and bovine serum albumin (BSA) in phosphate-buffered saline (PBS) followed by staining with human nuclei (Millipore, Temecula, CA, USA) and collagen type 2 (Thermo Fisher, San Jose, CA, USA). These sections were washed with PBS and then incubated with goat anti-mouse alexa 594 and 488 (Invitrogen, Carlsbad, CA, USA). Samples were counterstained with Hoechst (Invitrogen, Carlsbad, CA, USA) for nuclear staining.
Statistical Analysis
Results are expressed as mean ± SEM (standard error of the mean). Statistical significance between the means of different groups was determined using Student’s t test for two groups or one-way ANOVA with Tukey’s multiple comparison test for multiple groups. A value of p < 0.05 (*), p < 0.01 (**) and p < 0.001(***) was considered statistically significant. GraphPad Prism software (GraphPad Prism software Inc., San Diego, CA, USA) was used for all statistical analyses.
Results
CAM Promotes Chondrogenesisin UCB-MSCs
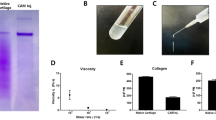
Micromass culture was used to induce chondrogenesis of UCB-MSCs. Pellet formation is one of the critical morphological changes detected during chondrogenesis of stem cells [40]. We treated with various concentrations of CAM (5, 10, and 20 mg/mL) to confirm chondrogenesis of UCB-MSCs for 7 days. None of the CAM concentrations showed any cytotoxicity (Fig. 2D). A pellet of UCB-MSCs was obtained with CAM treatment at each concentration (Fig. 2A). However, the mRNA expression of chondrogenic markers (aggrecan, type 2 collagen, and SOX9) was significantly increased by treatment with 20 mg/mL CAM (Fig. 2B) and type 1 collagen was used as a negative control. In addition, the synthesis of proteoglycan and type 2 collagen (COL2) was confirmed with Alcian blue staining (Fig. 2C) and immunostaining (Fig. 2E). Treatment with 20 mg/mL CAM increased the synthesis of proteoglycan (Fig. 2C) and protein expression of aggrecan (AGG) and COL2 (Fig. 2E). These data demonstrate that CAM promoted chondrogenic induction of UCB-MSCs.
CAM stimulates chondrogenesis of UCB-MSCs. (A) Morphological changes, (B) mRNA expression of chondrogenic markers (positive: aggrecan; AGG, type 2 collagen; COL2, SOX9, negative: type 1 collagen (COL1), (C) Proteoglycan synthesis (Alcian blue staining), (D) cytotoxicity of CAM and (E) CAM altered the expression of chondrogenic marker proteins in UCB-MSCs. Results represent means ± SEM, * p < 0.05, ** p < 0.01, *** p < 0.001. Scale bars: 500 μm in (A), 200 μm in (C, E)
Chondrogenesis of UCB-MSCs Induced by CAM Is Associated with BMP6 Expression
Co-culture was performed to determine whether CAM-treated UCB-MSCs promoted chondrogenesis of other naïve UCB-MSCs via paracrine effects (Fig. 3A). UCB-MSCs were induced for 7 days with CAM. They were co-cultured with naive UCB-MSCs using the transwell system for 7 days. As a result, co-culture with CAM-treated UCB-MSCs promoted pellet formation (Fig. 3B) and significantly increased the mRNA expression of AGG and COL2 in other naïve UCB-MSCs (Fig. 3C). Previous studies demonstrated that BMP6 accelerates chondrogenesis and mineralization in MSCs [34, 35]. CAM treatment significantly increased not only the mRNA and protein expression of BMP6 but also the secretion of BMP6 in UCB-MSCs (Fig. 3D). In addition, recombinant human BMP6 (rhBMP6) was used to treat UCB-MSCs in 500 ng/mL of induction media for 7 days. Treatment with rhBMP6 dramatically increased mRNA expression of AGG and COL2 (Fig. 3E) and also increased proteoglycan synthesis (Fig. 3F). These data indicate that CAM is associated with chondrogenesis mediated via BMP6 expression and secretion in UCB-MSCs.
Paracrine effect of CAM-treated UCB-MSCs promotes the chondrogenesis of other naïve UCB-MSCs via BMP6 expression. Chondrogenic induction was performed for 7 days (A) Paracrine effect induced by CAM. (B) Morphological changes and (C) mRNA expression analysis of chondrogenic markers. (D) Intracellular expression and secretion of BMP6 induced by CAM. (E) Changes in mRNA expression of chondrogenic markers induced by recombinant human BMP6 (rhBMP6). (F) Proteoglycan synthesis (Alcian blue staining) induced by rhBMP6 in UCB-MSCs. Results represent means ± SEM. * p < 0.05, ** p < 0.01, *** p < 0.001. Scale bars: 500 μm in (B), 1 mm (upper panel of F), 200 μm (lower panel of F).
Radiological, Behavioral and Visual Evaluation in a Rabbit ACLT Model
We first confirmed the appropriate dose of UCB-MSCs in the rabbit ACD model (Fig. S1A). Four weeks after ACD, transplantation with UCB-MSCs (2.5 × 106 cells) improved the gross findings in damaged tissue (Fig. S1B). Based on the findings, UCB-MSCs (2.5 × 106 cells) along with CAM (20 mg/mL) were transplanted into intra-articular regions of a rabbit model of ACLT. The efficacy was evaluated via X-ray and behavioral analysis at 3, 5, and 7 weeks after transplantation (Fig. 4A,B). While the radiological and behavioral symptoms of OA worsened over time in the control group, no statistically significant reduction in OA symptoms was detected in all the transplantation groups. However, the group transplanted with UCB-MSCs and CAM exhibited a significant improvement in symptoms at 7 weeks (Fig. 4B). Animals were sacrificed to evaluate the damage at 8 weeks in ACLT. The cartilage tissues were visually evaluated and quantified (Fig. 4C). As a result, severe damage involving the femoral condyle, erosion, and osteophytes were found in the control group. CAM alone also triggered a damage similar to that in the ACLT group. Compared with the results of the ACLT group, a significant improvement in OA symptoms was observed in the group transplanted with UCB-MSCs combined with CAM (Fig. 4C, D).
Transplantation of UCB-MSCs along with CAM alleviated OA symptoms in rabbit ACLT model. (A) Radiological analysis (white-arrowhead, narrowed joint space; yellow-arrowhead, sharpening of tibial spine; red-arrowhead, osteophyte; green-arrowhead, deformity of medial tibia). (B) Change in radiological and behavioral scores. (C) Visual evaluation in ACLT model (yellow-arrowhead, erosion; red-arrowhead, osteophyte). (D) Gross findings of each group were analyzed. The results represent the means ± SEM, * p < 0.05.
Histopathological Evaluation of Rabbit OA Models
Histopathological analysis was performed to evaluate structural intactness, proteoglycans, osteoblasts, and osteoclast activity using H&E, Safranin O, ALP, and TRAP staining protocols. UCB-MSCs and CAM improved the histological findings associated with structure, proteoglycans, and osteoclast activity (Fig. 5A). Osteoblast activity is known to play an important role in bone regeneration. Results showed that osteoblasts were scattered in the rabbit joint tissue. However, their numbers were too few to evaluate osteoarthritis induction or efficacy (Fig. 5A). Synthesis of COL2, a component of cartilage, was significantly increased via transplantation of UCB-MSCs with or without CAM (Fig. 5B and C). Based on these histopathologic findings, the combination of UCB-MSCs and CAM significantly attenuated the histological damage (Fig. 5D).
Transplantation of UCB-MSCs along with CAM improved the histology of cartilage regeneration in the damaged joints of the ACLT model. (A, C) Tissue regeneration was analyzed with H&E, safranin O, ALP, and TRAP staining. (B, D) Expression of type 2 collagen through immuno-staining at 8 weeks after transplantation. Density of collagen type II was quantified using Image J 4.8v (NIH). Results represent means ± SEM, * p < 0.05, ** p < 0.01, *** p < 0.001. Scale bars: 200 μm in (A), 100 μm in (B)
Synovial Fluid Analysis in Rabbit OA Model
To analyze the role of cytokines as inflammatory mediators in OA progression, synovial fluid was collected at 5 and 8 weeks in the ACLT model. Inflammatory cytokines (tumor-necrosis factor-α; TNF-α, interleukin-1β; IL-1β, IL-6, IL-8) were then measured. Compared with ACLT, CAM transplantation alone significantly decreased TNF-α, IL-1β and IL-8 at 5 weeks and IL-1 β and IL-8 at 8 weeks. In addition, transplantation of UCB-MSCs with or without) CAM also significantly decreased the expression of TNF- α, IL-1β, IL-6 and IL-8 at 5 and 8 weeks (except IL-6 in UCB-MSCs combined with CAM at 8 weeks) (Fig. 6). These data showed that the transplantation of UCB-MSCs with CAM resulted in an anti-inflammatory effect in the synovial fluid of the ACLT model.
Human Cell Tracking and BMP6 Association in Rabbit ACLT Model
To confirm the detection of transplanted human UCB-MSCs, immunostaining was performed using a human-specific anti-nuclei (HuNu) antibody. The HuNu antibody did not exhibit cross-reactivity with the rabbit adipose-derived stromal cells (Fig. S2). Studies have investigated the tracking of human MSCs for 8 weeks in a rabbit ACD model [22, 28]. UCB-MSCs might be detected during transplantation of UCB-MSCs alone. However, we confirmed that HuNu-positive cells were only present in the cartilage tissues transplanted with UCB-MSCs and CAM at 8 weeks after transplantation (Fig. 7A). In addition, UCB-MSCs present in cartilage tissue were found in the lacuna and the expression of COL2 was similar to that in rabbit chondrocytes (Fig. 7B). To investigate whether BMP6 affected cartilage tissue regeneration in the ACLT model, the levels of BMP6 and COL2 expression were compared between the control group and the group treated with a combination of UCB-MSC and CAM. The expression of BMP6 was correlated with that of COL2 in the group exposed to both UCB-MSCs and CAM (Fig. 7C). Higher expression of BMP6 and COL2 was found in the group exposed to UCB-MSCs and CAM, which indicated that cartilage regeneration was accelerated by the combination therapy. These data suggest that co-transplantation with UCB-MSCs and CAM affected cartilage regeneration via BMP6 expression in the rabbit ACLT model.
Discussion
Our study demonstrates that UCB-MSCs and CAM exhibit the potential to regenerate cartilage resulting in a healing effect both in vitro and in vivo. Such effect was partly mediated via BMP6 signaling pathway (Fig. 8). Components of CAM are similar to those of natural cartilage, which consists of ECM [30, 41]. ECM components are known to facilitate constructive remodeling in various tissues [42]. Studies have shown that cartilage extracts affect chondrogenic differentiation of MSCs [43, 44]. The findings showed that CAM promoted chondrogenic effects in UCB-MSCs. MSCs exhibit paracrine effects in the microenvironment by secreting multiple molecules [45]. A previous study demonstrated that co-culture with chondrocytes induced chondrognesis of MSCs [46]. UCB-MSCs differentiating into chondrocyte-like cells by CAM also exhibit a paracrine effect to induce chondrogenesis of other naïve UCB-MSCs. However, this mechanism is currently unknown. The chondrogenesis of MSCs is mediated by many factors such as TGF β [47] and BMPs [48]. In some studies, BMP6 promoted chondrogenesis of MSCs [34,35,36,37]. CAM increased mRNA expression of BMP6 in UCB-MSCs. Intracellular BMP6 expression and secretion were also significantly increased by CAM. This study also demonstrated that the effect of BMP6 was similar to that of CAM in inducing chondrogenesis of UCB-MSCs.
Based on in vivo results, the transplantation of UCB-MSCs combined with CAM showed a therapeutic effect in the rabbit ACLT model. Surgically induced OA models have been reported in previous studies. The ACD model is widely used to investigate cartilage regeneration [49]. In addition, the ACLT model is a commonly used surgical model to induce OA [50]. We used two rabbit OA models. The rabbit ACD model was established in a preliminary study to determine the transplantation dose of UCB-MSCs. The dosage of UCB-MSCs in rabbit ACLT was determined based on the data obtained with the rabbit ACD model. As a result, transplantation of UCB-MSCs with CAM significantly improved the behavioral, radiological, and microscopic symptoms of OA in the rabbit ACLT model. It also significantly enhanced the structure and synthesis of proteoglycans and COL2 but decreased osteoclast activity. Co- (mono-) transplantation of UCB-MSCs and CAM also significantly decreased the levels of inflammatory cytokines at weeks 5 and 8 after transplantation. MSCs secrete multiple factors to reduce joint inflammation [51, 52]. A previous study demonstrated that porcine-derived ECM product contains microvesicles and exosomes [53]. Microvesicles derived from MSC promote the secretion of anti-inflammatory cytokines and modulate M1/M2 macrophage phenotype [54, 55]. The CAM used in this study consists of ECM that is similar to natural cartilage [30]. The study findings showed that the transplantation of UCB-MSCs or CAM alone results in anti-inflammatory effects. UCB-MSCs were detected after transplantation with CAM, which may be associated with sustained modulation of joint inflammation. However, we found no synergistic anti-inflammatory effect with the combination of UCB-MSCs and CAM since their suppression level was similar to that of the normal-control group. Therefore, further study is needed to determine their synergistic effect on immunosuppression in the synovial joints of OA patients.
This study demonstrates that UCB-MSCs combined with CAM represent potential therapeutic agents for structural improvement and anti-inflammatory effect in OA. Such effect might be associated with BMP6 expression as well as promotion of chondrogenesis [34, 35] in MSCs and maturation of chondrocytes [56]. Here, we found that the expression of BMP6 and COL2 was increased in the regenerated cartilage tissue after transplantation of UCB-MSCs along with CAM. However, the mechanism underlying the effect of BMP6 on cartilage regeneration or chondrogenesis of MSCs and chondrocyte is completely unknown. Further investigations are needed to determine the mechanism responsible for the effect of BMP6 on chondrogenesis in association with CAM components. In summary, the results of the present study indicate that cartilage-derived ECM materials increase the therapeutic potential of UCB-MSCs via BMP6 expression, suggesting that UCB-MSCs combined with CAM are potential therapeutic agents in OA.
Acknowlegements
We thank Seung-Hoon Choe (Kangstem Biotech) for technical assistance.
References
Verbrugge, L. M. (1995). Women, men, and osteoarthritis. Arthritis Care and Research, 8(4), 212–220. https://doi.org/10.1002/art.1790080404.
Crepaldi, G., & Punzi, L. (2003). Aging and osteoarthritis. Aging Clinical and Experimental Research, 15(5), 355–358. https://doi.org/10.1007/bf03327355.
Bijlsma, J. W., Berenbaum, F., & Lafeber, F. P. (2011). Osteoarthritis: An update with relevance for clinical practice. Lancet, 377(9783), 2115–2126. https://doi.org/10.1016/S0140-6736(11)60243-2.
Loeser, R. F., Goldring, S. R., Scanzello, C. R., & Goldring, M. B. (2012). Osteoarthritis: A disease of the joint as an organ. Arthritis and Rheumatism, 64(6), 1697–1707. https://doi.org/10.1002/art.34453.
Maldonado, M., & Nam, J. (2013). The role of changes in extracellular matrix of cartilage in the presence of inflammation on the pathology of osteoarthritis. BioMed Research International, 2013(284873), 1–10. https://doi.org/10.1155/2013/284873.
Akkiraju, H., & Nohe, A. (2015). Role of chondrocytes in cartilage formation, progression of osteoarthritis and cartilage regeneration. Journal of Developmental Biology, 3(4), 177–192. https://doi.org/10.3390/jdb3040177.
Li, Y., Wei, X., Zhou, J., & Wei, L. (2013). The age-related changes in cartilage and osteoarthritis. BioMed Research International, 2013(916530). https://doi.org/10.1155/2013/916530.
McAlindon, T. E., Bannuru, R. R., Sullivan, M. C., Arden, N. K., Berenbaum, F., Bierma-Zeinstra, S. M., et al. (2014). OARSI guidelines for the non-surgical management of knee osteoarthritis. Osteoarthritis and Cartilage, 22(3), 363–388. https://doi.org/10.1016/j.joca.2014.01.003.
Gupta, P. K., Das, A. K., Chullikana, A., & Majumdar, A. S. (2012). Mesenchymal stem cells for cartilage repair in osteoarthritis. Stem Cell Research and Therapy, 3(4), 25. https://doi.org/10.1186/scrt116.
Zuk, P. A., Zhu, M., Ashjian, P., De Ugarte, D. A., Huang, J. I., Mizuno, H., et al. (2002). Human adipose tissue is a source of multipotent stem cells. Molecular Biology of the Cell, 13(12), 4279–4295. https://doi.org/10.1091/mbc.e02-02-0105.
Colter, D. C., Class, R., DiGirolamo, C. M., & Prockop, D. J. (2000). Rapid expansion of recycling stem cells in cultures of plastic-adherent cells from human bone marrow. Proceedings of the National Academy of Sciences of the United States of America, 97(7), 3213–3218. https://doi.org/10.1073/pnas.070034097.
Miranda, J. P., Filipe, E., Fernandes, A. S., Almeida, J. M., Martins, J. P., De la Fuente, A., et al. (2015). The human umbilical cord tissue-derived MSC population UCX((R)) promotes early Motogenic effects on keratinocytes and fibroblasts and G-CSF-mediated mobilization of BM-MSCs when transplanted in vivo. Cell Transplantation, 24(5), 865–877. https://doi.org/10.3727/096368913X676231.
Parolini, O., Alviano, F., Bagnara, G. P., Bilic, G., Buhring, H. J., Evangelista, M., . . . & Strom, S. C. (2008). Concise review: Isolation and characterization of cells from human term placenta: Outcome of the first international workshop on placenta derived stem cells. Stem Cells, 26(2), 300–311. doi:https://doi.org/10.1634/stemcells.2007-0594.
Lee, B. C., Shin, N., Lee, J. Y., Kang, I., Kim, J. J., Lee, S. E., et al. (2018). MIS416 enhances therapeutic functions of human umbilical cord blood-derived Mesenchymal stem cells against experimental colitis by modulating systemic immune milieu. Frontiers in Immunology, 28(9), 1078. https://doi.org/10.3389/fimmu.2018.01078.
Lee, Y. S., Sah, S. K., Lee, J. H., Seo, K. W., Kang, K. S., & Kim, T. Y. (2017). Human umbilical cord blood-derived mesenchymal stem cells ameliorate psoriasis-like skin inflammation in mice. Biochemistry and Biophysics Reports, 8(9), 281–288. https://doi.org/10.1016/j.bbrep.2016.10.002.
Park, E. H., Lim, H. S., Lee, S., Roh, K., Seo, K. W., Kang, K. S., & Shin, K. (2018). Intravenous infusion of umbilical cord blood-derived Mesenchymal stem cells in rheumatoid arthritis: A phase Ia clinical trial. Stem Cells Translational Medicine, 7(9), 636–642. https://doi.org/10.1002/sctm.18-0031.
Kim, H. S., Yun, J. W., Shin, T. H., Lee, S. H., Lee, B. C., Yu, K. R., et al. (2015). Human umbilical cord blood mesenchymal stem cell-derived PGE2 and TGF-beta1 alleviate atopic dermatitis by reducing mast cell degranulation. Stem Cells, 33(4), 1254–1266. https://doi.org/10.1002/stem.1913.
Sun, B., Jeong, Y. H., Jung, J. W., Seo, K., Lee, Y. S., & Kang, K. S. (2007). Regulation of human umbilical cord blood-derived multi-potent stem cells by autogenic osteoclast-based niche-like structure. Biochemical and Biophysical Research Communications, 357(1), 92–98. https://doi.org/10.1016/j.bbrc.2007.03.072.
Wang, M., Yang, Y., Yang, D., Luo, F., Liang, W., Guo, S., & Xu, J. (2009). The immunomodulatory activity of human umbilical cord blood-derived mesenchymal stem cells in vitro. Immunology, 126(2), 220–232. https://doi.org/10.1111/j.1365-2567.2008.02891.x.
Bieback, K., Kern, S., Kluter, H., & Eichler, H. (2004). Critical parameters for the isolation of mesenchymal stem cells from umbilical cord blood. Stem Cells, 22(4), 625–634. https://doi.org/10.1634/stemcells.22-4-625.
Jeong, S. Y., Kim, D. H., Ha, J., Jin, H. J., Kwon, S. J., Chang, J. W., Choi, S. J., Oh, W., Yang, Y. S., Kim, G., Kim, J. S., Yoon, J. R., Cho, D. H., & Jeon, H. B. (2013). Thrombospondin-2 secreted by human umbilical cord blood-derived mesenchymal stem cells promotes chondrogenic differentiation. Stem Cells, 31(10), 2136–2148. https://doi.org/10.1002/stem.1471.
Park, Y. B., Ha, C. W., Kim, J. A., Han, W. J., Rhim, J. H., Lee, H. J., Kim, K. J., Park, Y. G., & Chung, J. Y. (2017). Single-stage cell-based cartilage repair in a rabbit model: Cell tracking and in vivo chondrogenesis of human umbilical cord blood-derived mesenchymal stem cells and hyaluronic acid hydrogel composite. Osteoarthritis and Cartilage, 25(4), 570–580. https://doi.org/10.1016/j.joca.2016.10.012.
Mifune, Y., Matsumoto, T., Takayama, K., Ota, S., Li, H., Meszaros, L. B., et al. (2013). The effect of platelet-rich plasma on the regenerative therapy of muscle derived stem cells for articular cartilage repair. Osteoarthritis and Cartilage, 21(1), 175–185. https://doi.org/10.1016/j.joca.2012.09.018.
Hermeto, L. C., DeRossi, R., Oliveira, R. J., Pesarini, J. R., Antoniolli-Silva, A. C., Jardim, P. H., Santana, A. E., Deffune, E., Rinaldi, J. C., & Justulin, L. A. (2016). Effects of intra-articular injection of mesenchymal stem cells associated with platelet-rich plasma in a rabbit model of osteoarthritis. Genetics and Molecular Research, 15(3). https://doi.org/10.4238/gmr.15038569.
Yun, S., Ku, S. K., & Kwon, Y. S. (2016). Adipose-derived mesenchymal stem cells and platelet-rich plasma synergistically ameliorate the surgical-induced osteoarthritis in beagle dogs. Journal of Orthopaedic Surgery and Research, 11(9), 1–12. https://doi.org/10.1186/s13018-016-0342-9.
Lv, X., He, J., Zhang, X., Luo, X., He, N., Sun, Z., Xia, H., Liu, V., Zhang, L., Lin, X., Lin, L., Yin, H., Jiang, D., Cao, W., Wang, R., Zhou, G., & Wang, W. (2018). Comparative efficacy of autologous stromal vascular fraction and autologous adipose-derived Mesenchymal stem cells combined with hyaluronic acid for the treatment of sheep osteoarthritis. Cell Transplantation, 27(7), 1111–1125. https://doi.org/10.1177/0963689718773333.
Chiang, E. R., Ma, H. L., Wang, J. P., Liu, C. L., Chen, T. H., & Hung, S. C. (2016). Allogeneic Mesenchymal stem cells in combination with hyaluronic acid for the treatment of osteoarthritis in rabbits. PLoS One, 11(2), e0149835. https://doi.org/10.1371/journal.pone.0149835.
Yin, H., Wang, Y., Sun, Z., Sun, X., Xu, Y., Li, P., et al. (2016). Induction of mesenchymal stem cell chondrogenic differentiation and functional cartilage microtissue formation for in vivo cartilage regeneration by cartilage extracellular matrix-derived particles. Acta Biomaterialia, 33, 96–109. https://doi.org/10.1016/j.actbio.2016.01.024.
Baek, J. H., Kim, K., Yang, S. S., Park, S. H., Song, B. R., Yun, H. W., . . . & Kim, M. S. (2016). Preparation of Extracellular Matrix Developed Using Porcine Articular Cartilage and In Vitro Feasibility Study of Porcine Articular Cartilage as an Anti-Adhesive Film. Materials (Basel), 9(1), pii: E49. doi:10.3390/ma9010049.
Kim, H. J., Lee, S., Yun, H. W., Yin, X. Y., Kimm, S. H., Choi, B. H., et al. (2016). In vivo degradation profile of porcine cartilage-derived extracellular matrix powder scaffolds using a non-invasive fluorescence imaging method. Journal of Biomaterials Science, Polymer Edition, 27(2), 177–190. https://doi.org/10.1080/09205063.2015.1120262.
Benders, K. E., van Weeren, P. R., Badylak, S. F., Saris, D. B., Dhert, W. J., & Malda, J. (2013). Extracellular matrix scaffolds for cartilage and bone regeneration. Trends in Biotechnology, 31(3), 169–176. https://doi.org/10.1016/j.tibtech.2012.12.004.
Bragdon, B., Moseychuk, O., Saldanha, S., King, D., Julian, J., & Nohe, A. (2011). Bone morphogenetic proteins: A critical review. Cellular Signalling, 23(4), 609–620. https://doi.org/10.1016/j.cellsig.2010.10.003.
Sekiya, I., Vuoristo, J. T., Larson, B. L., & Prockop, D. J. (2002). In vitro cartilage formation by human adult stem cells from bone marrow stroma defines the sequence of cellular and molecular events during chondrogenesis. Proceedings of National Academy of Science of the United States of America, 99(7), 4397–4402. https://doi.org/10.1073/pnas.052716199.
Sekiya, I., Colter, D. C., & Prockop, D. J. (2001). BMP-6 enhances chondrogenesis in a subpopulation of human marrow stromal cells. Biochemedical and Biophysical Research Communications, 284(2), 411–418. https://doi.org/10.1006/bbrc.2001.4898.
Boskey, A. L., Paschalis, E. P., Binderman, I., & Doty, S. B. (2002). BMP-6 accelerates both chondrogenesis and mineral maturation in differentiating chick limb-bud mesenchymal cell cultures. Journal of Cellular Biochemistry, 84(3), 509–519.
Hildner, F., Peterbauer, A., Wolbank, S., Nurnberger, S., Marlovits, S., Redl, H., . . . & Gabriel, C. (2010). FGF-2 abolishes the chondrogenic effect of combined BMP-6 and TGF-beta in human adipose derived stem cells. Journal of Biomedical Materials Research. Part A, 94(3), 978–987. doi:https://doi.org/10.1002/jbm.a.32761.
Diekman, B. O., Estes, B. T., & Guilak, F. (2010). The effects of BMP6 overexpression on adipose stem cell chondrogenesis: Interactions with dexamethasone and exogenous growth factors. Journal of Biomedical Materials Research. Part A, 93(3), 994–1003. doi:https://doi.org/10.1002/jbm.a.32589.
Seo, Y., Yang, S. R., Jee, M. K., Joo, E. K., Roh, K. H., Seo, M. S., Han, T. H., Lee, S. Y., Ryu, P. D., Jung, J. W., Seo, K. W., Kang, S. K., & Kang, K. S. (2011). Human umbilical cord blood-derived mesenchymal stem cells protect against neuronal cell death and ameliorate motor deficits in Niemann pick type C1 mice. Cell Transplantation, 20(7), 1033–1047. https://doi.org/10.3727/096368910X545086.
Kwon, J. S., Yoon, S. M., Shim, S. W., Park, J. H., Min, K. J., Oh, H. J., Kim, J. H., Kim, Y. J., Yoon, J. J., Choi, B. H., & Kim, M. S. (2013). Injectable extracellular matrix hydrogel developed using porcine articular cartilage. International Journal of Pharmaceutics, 454(1), 183–191. https://doi.org/10.1016/j.ijpharm.2013.06.023.
Hamid, A. A., Idrus, R. B., Saim, A. B., Sathappan, S., & Chua, K. H. (2012). Characterization of human adipose-derived stem cells and expression of chondrogenic genes during induction of cartilage differentiation. Clinics (São Paulo, Brazil), 67(2), 99–106. https://doi.org/10.6061/clinics/2012(02)03.
Jin, C. Z., Park, S. R., Choi, B. H., Park, K., & Min, B. H. (2007). In vivo cartilage tissue engineering using a cell-derived extracellular matrix scaffold. Artificial Organs, 31(3), 183–192. https://doi.org/10.1111/j.1525-1594.2007.00363.x.
Badylak, S. F., Freytes, D. O., & Gilbert, T. W. (2009). Extracellular matrix as a biological scaffold material: Structure and function. Acta Biomaterialia, 5(1), 1–13. https://doi.org/10.1016/j.actbio.2008.09.013.
Talakoob, S., Joghataei, M. T., Parivar, K., Bananej, M., & Sanadgol, N. (2015). Capability of cartilage extract to in vitro differentiation of rat Mesenchymal stem cells (MSCs) to chondrocyte lineage. International Journal of Molecular and Cellular Medicine, 4(1), 9–21.
Xue, J. X., Gong, Y. Y., Zhou, G. D., Liu, W., Cao, Y., & Zhang, W. J. (2012). Chondrogenic differentiation of bone marrow-derived mesenchymal stem cells induced by acellular cartilage sheets. Biomaterials, 33(24), 5832–5840. https://doi.org/10.1016/j.biomaterials.2012.04.054.
Park, W. S., Ahn, S. Y., Sung, S. I., Ahn, J. Y., & Chang, Y. S. (2018). Strategies to enhance paracrine potency of transplanted mesenchymal stem cells in intractable neonatal disorders. Pediatric Research, 83(1–2), 214–222. https://doi.org/10.1038/pr.2017.249.
Meretoja, V. V., Dahlin, R. L., Kasper, F. K., & Mikos, A. G. (2012). Enhanced chondrogenesis in co-cultures with articular chondrocytes and mesenchymal stem cells. Biomaterials, 33(27), 6362–6369. https://doi.org/10.1016/j.biomaterials.2012.05.042.
Lee, S. Y., Nakagawa, T., & Reddi, A. H. (2008). Induction of chondrogenesis and expression of superficial zone protein (SZP)/lubricin by mesenchymal progenitors in the infrapatellar fat pad of the knee joint treated with TGF-beta1 and BMP-7. Biochemedical and Biophysical Research Communications, 376(1), 148–153. https://doi.org/10.1016/j.bbrc.2008.08.138.
Yoon, B. S., & Lyons, K. M. (2004). Multiple functions of BMPs in chondrogenesis. Journal of Cellular Biochemistry, 93(1), 93–103. https://doi.org/10.1002/jcb.20211.
Chu, C. R., Szczodry, M., & Bruno, S. (2010). Animal models for cartilage regeneration and repair. Tissue Engineering. Part B. Reviews, 16(1), 105–115. doi:https://doi.org/10.1089/ten.TEB.2009.0452.
Kuyinu, E. L., Narayanan, G., Nair, L. S., & Laurencin, C. T. (2016). Animal models of osteoarthritis: Classification, update, and measurement of outcomes. Journal of Orthopaedic Surgery and Research, 11, 19. https://doi.org/10.1186/s13018-016-0346-5.
van Buul, G. M., Villafuertes, E., Bos, P. K., Waarsing, J. H., Kops, N., Narcisi, R., et al. (2012). Mesenchymal stem cells secrete factors that inhibit inflammatory processes in short-term osteoarthritic synovium and cartilage explant culture. Osteoarthritis and Cartilage, 20(10), 1186–1196. https://doi.org/10.1016/j.joca.2012.06.003.
Kehoe, O., Cartwright, A., Askari, A., El Haj, A. J., & Middleton, J. (2014). Intra-articular injection of mesenchymal stem cells leads to reduced inflammation and cartilage damage in murine antigen-induced arthritis. Journal of Translational Medicine, 12, 157. https://doi.org/10.1186/1479-5876-12-157.
Huleihel, L., Hussey, G. S., Naranjo, J. D., Zhang, L., Dziki, J. L., Turner, N. J., Stolz, D. B., & Badylak, S. F. (2016). Matrix-bound nanovesicles within ECM bioscaffolds. Science Advances, 2(6), e1600502. https://doi.org/10.1126/sciadv.1600502.
Zhang, B., Yin, Y., Lai, R. C., Tan, S. S., Choo, A. B., & Lim, S. K. (2014). Mesenchymal stem cells secrete immunologically active exosomes. Stem Cells and Development, 23(11), 1233–1244. https://doi.org/10.1089/scd.2013.0479.
Mokarizadeh, A., Delirezh, N., Morshedi, A., Mosayebi, G., Farshid, A. A., & Mardani, K. (2012). Microvesicles derived from mesenchymal stem cells: Potent organelles for induction of tolerogenic signaling. Immunology Letters, 147(1–2), 47–54. https://doi.org/10.1016/j.imlet.2012.06.001.
Grimsrud, C. D., Romano, P. R., D'Souza, M., Puzas, J. E., Schwarz, E. M., Reynolds, P. R., et al. (2001). BMP signaling stimulates chondrocyte maturation and the expression of Indian hedgehog. Journal of Orthopaedic Research, 19(1), 18–25. https://doi.org/10.1016/S0736-0266(00)00017-6.
Author information
Authors and Affiliations
Contributions
Conception and design of the study, KWS, YBK, KSK; acquisition of data, HJJ, KAY, ESA, TWK, YBS; analysis and interpretation of data, HJJ, SHL, EKC, JCA; drafting the manuscript, HJJ, JCA; All authors read and approved the final manuscript.
Corresponding authors
Ethics declarations
Conflict of Interest
The authors declare that they have no conflict of interest.
Funding
This study received no specific grant from any funding agency in the public, commercial or not-for-profit sectors.
Ethical Approval
This experiment was approved by the Institutional Animal Care and Use Committee (IACUC) of Chungbuk National University Laboratory Animal Research Center and performed in accordance with the Standard Operation Procedures (SOP) of the same facility.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Jeon, HJ., Yoon, KA., An, E.S. et al. Therapeutic Effects of Human Umbilical Cord Blood-Derived Mesenchymal Stem Cells Combined with Cartilage Acellular Matrix Mediated Via Bone Morphogenic Protein 6 in a Rabbit Model of Articular Cruciate Ligament Transection. Stem Cell Rev and Rep 16, 596–611 (2020). https://doi.org/10.1007/s12015-020-09958-9
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12015-020-09958-9