Abstract
Background
Microvascular invasion (MVI) is recognized as a risk factor for early recurrence of hepatocellular carcinoma (HCC) within the Milan criteria after curative treatment.
Methods
One hundred eleven consecutive patients with HCC within the Milan criteria who underwent hepatic resection were retrospectively reviewed. Independent preoperative predictors of MVI were identified, and a scoring system was developed using significant predictors.
Results
MVI was identified in 51 of 111 patients (46%). Multivariate analysis identified the following independent predictors of MVI: alpha-fetoprotein (AFP) of > 95 ng/mL (odds ratio [OR], 9.87; 95% confidence interval [95% CI], 2.24–56.8; P = 0.002), des-γ-carboxy prothrombin (DCP) of > 55 mAU/mL (OR, 5.50; 95% CI, 2.09–15.4; P < 0.001), tumor size of > 2.8 cm (OR, 6.10; 95% CI, 2.07–20.0; P < 0.001), and non-smooth tumor margin in the hepatobiliary phase of gadolinium-ethoxybenzyl-diethylenetriamine pentaacetic acid (Gd-EOB-DTPA)-enhanced magnetic resonance imaging (MRI) (OR, 5.34; 95% CI, 1.84–16.9; P = 0.002). A clinical scoring system was developed using these four variables. Within a total possible score of 0 to 4, the prevalence of MVI with a score of 0, 1, 2, 3, and 4 was 4.5%, 24.0%, 45.5%, 91.7%, and 100%, respectively (P < 0.001). The area under the curve of the scoring system was 0.865 based on the receiver operating characteristic curve analysis of the prediction score.
Conclusions
Our clinical scoring system, consisting of AFP, DCP, tumor size, and tumor margin in Gd-EOB-DTPA-enhanced MRI, can be valuable for predicting MVI in HCC within the Milan criteria before curative treatment.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Hepatocellular carcinoma (HCC) within the Milan criteria (i.e., a single tumor of ≤ 5 cm or three or fewer tumors of ≤ 3 cm, no macroscopic vascular invasion, and no extrahepatic involvement) is considered early-stage HCC associated with a good prognosis.1 According to the management guidelines of the European Association for the Study of the Liver and the American Association for the Study of Liver Diseases, the recommended treatment modalities for early-stage HCC include hepatic resection, radiofrequency ablation (RFA), and liver transplantation on the basis of liver function.2,3 In some countries with limited availability of the livers for transplantation, hepatic resection or RFA is the main curative treatment option for early-stage HCC. However, we have experienced some patients with HCC within the Milan criteria with early recurrence and a poor prognosis after curative treatment. Several studies have been performed to evaluate the prognostic factors in these patients with early HCC, and microvascular invasion (MVI) has been identified as a significant factor.4,5,6,7
MVI is difficult to detect by conventional imaging modalities before curative treatment, and many previous studies have revealed preoperative factors that can predict MVI.8,9,10,11 In addition to three HCC-specific tumor markers, namely alpha-fetoprotein (AFP), Lens culinaris agglutinin-reactive fraction of AFP (AFP-L3), and des-γ-carboxy prothrombin (DCP), several recent studies have shown that specific radiological findings obtained with recently established diagnostic imaging techniques are useful to predict MVI.12,13 In particular, gadolinium-ethoxybenzyl-diethylenetriamine pentaacetic acid (Gd-EOB-DTPA), which is a newly developed liver-specific contrast agent in magnetic resonance imaging (MRI), is reportedly useful in the prediction of MVI.14
Prediction of MVI is important for both predicting the prognosis in patients with early HCC and selecting appropriate treatment. According to several recent studies, RFA should be avoided for HCC with the potential of MVI or poor differentiation because of the high risk of local recurrence or intrahepatic dissemination.15,16,17 On the other hand, anatomical hepatectomy can theoretically eradicate MVI confined by tumor-bearing portal tributaries.18 Accordingly, precise evaluation of MVI before curative treatment remains an important issue in the selection of appropriate treatment modalities for HCC within the Milan criteria.
The purpose of this study was to identify preoperative predictors of MVI in HCC within the Milan criteria and to devise a scoring system for deciding adequate treatment modalities.
Patients and Methods
Patients
From January 2008 to December 2017, 145 patients were diagnosed with and underwent hepatic resection for primary HCC at the Department of Hepato-Biliary-Pancreatic Surgery at Kyushu Medical Center. The inclusion criteria for this study were as follows: (1) a tumor within the Milan criteria, (2) the performance of Gd-EOB-DTPA-enhanced MRI before surgery, (3) no radiological evidence of macroscopic portal or hepatic vein tumor invasion, (4) no extrahepatic metastasis, (5) no preoperative treatment, and (6) curative hepatic resection defined as the removal of all macroscopic residual tumors. Of all 145 patients, 111 met these criteria and were retrospectively included in this study. This study was conducted in accordance with the Declaration of Helsinki and the ethical guidelines for clinical studies of the Ministry of Health, Labour and Welfare in Japan. The study protocol was approved by the Ethics Committee on Clinical Investigations of Kyushu Medical Center (Approval No. 17C051).
Preoperative Clinical Evaluation
The preoperative evaluation included determination of age, sex, blood chemistry parameters, indocyanine green retention rate at 15 min, Child–Pugh classification, hepatitis virus markers (hepatitis B virus surface antigen and hepatitis C virus antibody), and three tumor markers: AFP, AFP-L3, and DCP. The serum concentrations of AFP, AFP-L3, and DCP were measured within 1 week before hepatic resection.
We generally evaluated the indications for surgery and selected the operative procedure based on the tumor extent and the hepatic reserve as assessed by the Child–Pugh score and the criteria established by Makuuchi et al.19 Anatomical resection procedures were defined based on the Brisbane 2000 classification.20
Preoperative Image Analysis
HCC lesions in each patient were preoperatively diagnosed by several imaging modalities, including Gd-EOB-DTPA-enhanced MRI, ultrasonography, and dynamic computed tomography. The final diagnosis of HCC was confirmed by pathologic examination of resected specimens. None of the patients underwent needle biopsy for preoperative diagnosis of HCC because of the risk of tumor seeding or intra-abdominal bleeding. All patients underwent Gd-EOB-DTPA-enhanced MRI at our institute within 2 weeks before hepatic resection. MRI was performed with a 1.5-T MRI system (Magnetom Symphony; Siemens Medical Systems, Erlangen, Germany and Achieva; Philips Medical Systems, Best, Netherlands) using a phased-array surface coil covering the whole liver. Contrast-enhanced MRI was performed using Gd-EOB-DTPA (Primovist; Bayer Schering Pharma, Berlin, Germany) at a dose of 0.1 mL/kg bodyweight. Hepatobiliary phase images were taken more than 15 min after contrast agent injection. Hepatobiliary phase contrast-enhanced MRI was performed using three-dimensional gradient echo sequences with fat suppression and a slice thickness of 3.0 to 3.5 mm.
The tumor margin in the hepatobiliary phase on Gd-EOB-DTPA-enhanced MRI was classified into two types: smooth and non-smooth. If the tumor was round with a distinct margin and no budding portion at the periphery, the tumor margin was considered to be smooth (Fig. 1a). If the tumor was round with a focally protruding area or lobulated with multiple nodular lesions, the tumor margin was considered to be non-smooth (Fig. 1b, c). These radiological findings were determined in each patient preoperatively by a liver surgeon with 14 years of experience (T.R.) and an abdominal radiologist with 35 years of experience (K.Y.) together, both of whom were blinded to the patients’ clinical records. In patients with multiple HCC lesions, the largest lesion was analyzed.
The tumor margin in the hepatobiliary phase on Gd-EOB-DTPA-enhanced MRI. a This round tumor shows low intensity and a distinct margin. The tumor margin was considered to be smooth. b This round tumor shows low intensity and a focally protruding area. The tumor margin was considered to be non-smooth. c This lobulated tumor shows low intensity and multiple nodular lesions. The tumor margin was considered to be non-smooth
Histopathological Diagnosis
MVI was defined as microscopic tumor invasion identified in the portal vein or hepatic vein of the surrounding liver tissue that was contiguous with the tumor. Gross classification of the nodular type and tumor differentiation were defined based on the General Rules for the Clinical and Pathological Study of Primary Liver Cancer developed by the Liver Cancer Study Group of Japan.21 When the evaluated nodule comprised two areas of different histological grades, the worse histological grade was recorded. Non-cancerous liver tissue was inspected for evidence of cirrhosis. Liver cirrhosis was defined as grade 4 fibrosis on pathologic examination of the specimen.
Statistical Analysis
Continuous variables are presented as median (range) and were compared using the Mann–Whitney U test. Categorical variables were compared using Fisher’s exact probability method or χ2 tests. A logistic regression model was used for multivariate analyses of factors related to MVI and to calculate the odds ratio (OR) and 95% confidence interval (95% CI). The cut-off value of the predictive score was calculated using a receiver operating characteristic (ROC) curve. The ROC curve is a plot of sensitivity versus 1 − specificity for all possible cut-off values. All P values were derived from two-tailed tests, and P < 0.05 was considered statistically significant. All statistical analyses were performed using the JMP 12 software package (SAS Institute Inc., Cary, NC, USA).
Results
Patient Characteristics
Table 1 shows the clinicopathological characteristics and MRI findings of the 111 patients enrolled in this study. The 111 patients included 75 men (68%), with a median age of 73 years (range, 42–88 years). The median maximum tumor size was 30.2 mm (range, 10.4–50.0); 101 patients had a single HCC lesion, 6 patients had 2 HCC lesions, and 4 patients had 3 HCC lesions. With respect to the surgical procedures, 80 patients (72%) underwent anatomical hepatectomy: 11 underwent hemihepatectomy, 26 underwent sectionectomy, and 43 underwent segmentectomy. Partial hepatectomy was performed in 31 patients (28%).
Univariate Factors Associated with MVI
Table 2 shows the clinicopathological characteristics and MRI findings submitted to univariate analysis for prediction of MVI. Of the 111 patients, 51 patients (46%) had MVI (49 with portal vein invasion, 1 with hepatic vein invasion, and 1 with portal and hepatic vein invasion). With respect to preoperative factors, univariate analysis revealed that hepatitis B virus positivity (P = 0.047), hepatitis C virus positivity (P = 0.029), the serum AFP level (P = 0.002), the serum AFP-L3 level (P = 0.043), the serum DCP level (P < 0.001), the tumor size (P < 0.001), and the tumor margin in the hepatobiliary phase on Gd-EOB-DTPA-enhanced MRI (P < 0.001) were statistically significant predictors of MVI. The serum AFP level, serum AFP-L3 level, serum DCP level, and tumor size were used to plot the ROC curve for predicting MVI (Fig. 2). The areas under the curve (AUCs) of the serum AFP level, serum AFP-L3 level, serum DCP level, and tumor size were 0.657, 0.631, 0.734, and 0.782, respectively. The best cut-off values calculated from ROC analysis were as follows: serum AFP level, 95 ng/mL; serum AFP-L3 level, 10%; serum DCP level, 55 mAU/mL; and tumor size, 2.8 cm. With respect to postoperative pathological factors, gross type (P < 0.001) and histological grade (P = 0.017) were significantly associated with MVI.
Independent Predictors of MVI According to Multivariate Analyses
Multivariate analysis of preoperative factors revealed the following independent predictive factors for MVI (Table 3): a serum AFP level of > 95 ng/mL (OR, 9.87; 95% CI, 2.24–56.8; P = 0.002), serum DCP level of > 55 mAU/mL (OR, 5.50; 95% CI, 2.09–15.4; P < 0.001), tumor size of > 2.8 cm (OR, 6.10; 95% CI, 2.07–20.0; P < 0.001), and non-smooth tumor margin in the hepatobiliary phase on Gd-EOB-DTPA-enhanced MRI (OR, 5.34; 95% CI, 1.84–16.9; P = 0.002).
Scoring System for the Prediction of MVI
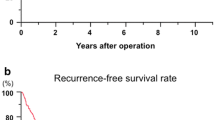
A clinical scoring system for predicting MVI before curative treatment was developed using four variables: a serum AFP level of > 95 ng/mL, a serum DCP level of > 55 mAU/mL, tumor size of > 2.8 cm, and a non-smooth tumor margin in the hepatobiliary phase on Gd-EOB-DTPA-enhanced MRI, giving a total score of 0 to 4 points. Figure 3a shows the relationship between the score and the prevalence of MVI. An increasing score was correlated with an increasing prevalence of MVI. The prevalence of MVI was 4.5% (1/22) with a score of 0, 24.0% (6/25) with a score of 1, 45.5% (15/33) with a score of 2, 91.7% (22/24) with a score of 3, and 100% (7/7) with a score of 4 (P < 0.001). The AUC of the scoring system was 0.865 based on the ROC curve analysis of the prediction score (Fig. 3b). The OR for MVI with a score of 0, 1, 2, and 3–4 was 1, 6.63 (95% CI, 1.01–131; P = 0.049), 17.5 (95% CI, 3.08–332; P < 0.001), and 304.5 (95% CI, 38.3–7336; P < 0.0001), respectively (Table 4).
Discussion
The current study revealed four independent preoperative factors for predicting MVI in patients with HCC within the Milan criteria: a serum AFP level of > 95 ng/mL, a serum DCP level of > 55 mAU/mL, tumor size of > 2.8 cm, and a non-smooth tumor margin in the hepatobiliary phase on Gd-EOB-DTPA-enhanced MRI. Based on these four predictive factors, we established a scoring system for the prediction of MVI that could enable us to more accurately diagnose the presence of MVI before curative treatment.
In various studies, the preoperative predictive factors for MVI included tumor size, tumor markers, gross type, and tumor differentiation.8,9,10,11 Tumor size was considered to be a strong predictor for MVI in several studies, while the risk of MVI continues to rise as the tumor size increases.9,22 The current study revealed that tumor size was still a significant predictor of MVI, even within the Milan criteria, with a cut-off value of 2.8 cm obtained from ROC analysis. Tumor markers for HCC, such as AFP, AFP-L3, and DCP, were assessed as predictors of MVI rather than detectors of HCC in recent studies. Additionally, we previously reported that double- or triple-positive tumor markers were associated with malignant potential and a poor prognosis in patients with HCC within the Milan criteria.23 An elevated DCP level is reportedly the strongest predictor of MVI among the three tumor markers.24,25 The present study also demonstrated that DCP is a significant predictive factor for MVI by multivariate analysis. AFP is the most widely used tumor marker for HCC; an elevated AFP is correlated with higher malignant potential of HCC as well as a higher incidence of HCC.26,27 In the present study, the AFP level itself was not associated with MVI (AUC of 0.657 for AFP). In contrast, an AFP level of > 95 ng/mL was a significant predictor of MVI. The cut-off value of 95 ng/mL was obtained by the ROC curve for predicting MVI. Mild elevation of AFP is sometimes found in patients with chronic hepatitis or liver cirrhosis, but a higher elevation of AFP (> 95 ng/mL) is highly suggestive of the presence of MVI.
Gross type was also associated with MVI in previous studies, although the gross type cannot be determined before hepatic resection.11,28 Therefore, determining the gross type by preoperative imaging is important in predicting MVI. Several recent studies have suggested that the hepatobiliary phase of Gd-EOB-DTPA-enhanced MRI is useful for evaluation of the gross type and the presence of MVI.14,29 In the present study, a non-smooth tumor margin in the hepatobiliary phase of Gd-EOB-DTPA-enhanced MRI was also found to be a significant predictive factor of MVI, which is in accordance with a previous study.14
We designed a scoring system using the serum AFP level, the serum DCP level, tumor size, and tumor margin in the hepatobiliary phase on Gd-EOB-DTPA-enhanced MRI to predict MVI before curative treatment. To maximize clinical utility, only variables known preoperatively were included. Therefore, although the gross type and histological grade were associated with MVI in the univariate analysis, they were not included in the multivariate analysis. Using this proposed scoring system, we identified a group of patients (score of 3 or 4) who certainly had MVI [91.7% (22/24) or 100% (14/14), respectively]. In contrast, few patients with 0 points had MVI [4.5% (1/22)]. The AUC of this scoring system was 0.865, which was much higher than each single predictive factor, suggesting that this scoring system can predict MVI much more precisely.
Our proposed scoring system could be useful for selecting the appropriate treatment modalities. Several recent studies have shown that RFA is not recommended as a curative treatment for patients with HCC with the potential of MVI or poor differentiation because of the high risk of local recurrence or intrahepatic dissemination.15,16,17 Although the presence or absence of MVI could not be determined in patients with RFA, the incidence of MVI in patients with RFA would be similar to that of patients with hepatic resection.17 Patients with a score of 0 points using our scoring system could be recommended to undergo RFA because the possibility of MVI is quite low. However, patients with a score of ≥ 1 point using our scoring system should not be recommended to undergo RFA; instead, they should undergo hepatic resection. Although the prevalence of MVI was 24% with a score of 1 (i.e., either larger tumor size or elevated tumor marker levels), Imamura et al. reported that larger tumor size and elevated tumor marker levels were the surrogate markers for poor differentiation as well as MVI, while these were the risk factors of neoplastic seeding after RFA.16 In addition, poorly differentiated carcinoma itself was shown to be an independent predictor of MVI.9 Based on these findings, we recommend hepatic resection even for patients with a score of 1 point using our scoring system.
Among hepatic resection, anatomical resection for HCC with MVI was recommended with the finding that anatomical resection theoretically involved systemic removal of the segment to which the MVI might spread in several previous studies.18,30,31 Anatomical resection is recommended when a patient has good liver function, especially when they have 3 or 4 points in our scoring system, because of the extremely high prevalence of MVI. In contrast, previous retrospective cohort studies revealed that almost all areas of MVI or intrahepatic metastasis were localized within 1 cm of the tumor margin in patients with HCC of < 3 cm.26,32 When patients have inadequate liver function for anatomical resection, partial hepatectomy with a wide tumor margin of ≥ 1 cm would be permitted for relatively small HCC lesions.
There were some limitations in this study. First, this study was a retrospective study involving only patients who underwent hepatic resection, meaning that selection bias may have occurred. Second, due to the small sample size and single-institution review, we were unable to perform a validation of our prediction model. Nevertheless, we hope that our simple clinical scoring system can be informative for predicting MVI and determining the optimal therapeutic modality for patients with HCC within the Milan criteria. Future studies to validate our scoring system should be performed in other larger populations.
Conclusion
We developed a clinical scoring system consisting of the serum AFP level, serum DCP level, tumor size, and tumor margin in the hepatobiliary phase on Gd-EOB-DTPA-enhanced MRI to predict MVI before curative treatment. The proposed simple scoring system can provide more accurate preoperative diagnosis of the presence of MVI and be useful for selecting the appropriate treatment modality in patients with HCC within the Milan criteria.
References
Mazzaferro V, Regalia E, Doci R, Andrela S, Pulvirenti A, Bozzetti F, Montalto F, Ammatuna M, Morabito A, Gennari L. Liver transplantation for the treatment of small hepatocellular carcinomas in patients with cirrhosis. N Engl J Med 1996;344:693–700.
European Association for the Study of the Liver, European Organisation for Research and Treatment of Cancer. EASL-EORTC clinical practice guidelines: management of hepatocellular carcinoma. J Hepatol. 2012;56:908–943.
Bruix J, Sherman M. Management of hepatocellular carcinoma: an update. Hepatology. 2011;53:1020–1022.
Liver Cancer Study Group of Japan Primary liver cancer in Japan. Clinicopathologic features and results of surgical treatment. Ann Surg 1990;211:277–287.
Izumi R, Shimizu K, Ii T, Yagi M, Matsui O, Nonomura A, Miyazaki I. Prognostic factors of hepatocellular carcinoma in patients undergoing hepatic resection. Gastroenterology 1994;106:720–727.
Poon RT, Fan ST, Lo CM, Liu CL, Wong J. Difference in tumor invasiveness in cirrhotic patients with hepatocellular carcinoma fulfilling the Milan criteria treated by resection and transplantation. Impact on long-term survival. Ann Surg 2007;245:51–58.
Otto G, Heuschen U, Hofmann WJ, Krumm G, Hinz U, Herfarth C. Survival and recurrence after liver transplantation versus liver resection for hepatocellular carcinoma: a retrospective analysis. Ann Surg 1998;227:424–432.
Shirabe K, Itoh S, Yoshizumi T, Soejima Y, Taketomi A, Aishima S, Maehara Y. The predictors of microvascular invasion in candidates for liver transplantation with hepatocellular carcinoma: with special reference to the serum levels of des-gamma-carboxy prothrombin. J Surg Oncol 2007;95:235–240.
Kaibori M, Ishizaki M, Matsui K, Kwon AH. Predictors of microvascular invasion before hepatectomy for hepatocellular carcinoma. J Surg Oncol 2010;102:462–468.
Sakata J, Shirai Y, Wakai T, Kaneko K, Nagahashi M, Hatakeyama K. Preoperative predictors of vascular invasion in hepatocellular carcinoma. Eur J Surg Oncol 2008;34:900–905.
Sumie S, Kuromatsu R, Okuda K, Ando E, Takata A, Fukushima N, Watanabe Y, Kojiro M, Sata M. Microvascular invasion in patients with hepatocellular carcinoma and its predictable clinicopathological factors. Ann Surg Oncol 2008;15:1375–1382.
Kim H, Park MS, Choi JY, Park YN, Kim MJ, Kim KS, Choi JS, Han KH, Kim EJ, Kim KW. Can microvessel invasion of hepatocellular carcinoma be predicted by pre-operative MRI? Eur Radiol 2009;19:1744–1751.
Nishie A, Yoshimitsu K, Asayama Y, Irie H, Tajima T, Hirakawa M, Ishigami K, Nakayama T, Kakihara D, Nishihara Y, Taketomi A, Honda H. Radiologic detectability of minute portal venous invasion in hepatocellular carinoma. Am J Roentgenol 2008;190:81–87.
Ariizumi S, Kitagawa K, Kotera Y, Takahashi Y, Katagiri S, Kuwatsuru R, Yamamoto M. A non-smooth tumor margin in the hepatobiliary phase of gadoxetic acid disodium (Gd-EOB-DTPA)-enhanced magnetic resonance imaging predicts microscopic portal vein invasion, intrahepatic metastasis, and early recurrence after hepatectomy in patients with hepatocellular carcinoma. J Hepatobiliary Pancreat Sci 2011;18:575–585.
Yu HC, Cheng JS, Lai KH, Lin CP, Lo GH, Lin CK, Hsu PI, Chan HH, Lo CC, Tsai WL, Chen WC. Factors for early tumor recurrence of single small hepatocellular carcinoma after percutaneous radiofrequency ablation therapy. World J Gastroenterol 2005;11:1439–1444.
Imamura J, Tateishi R, Shiina S, Goto E, Sato T, Ohki T, Masuzaki R, Goto T, Yoshida H, Kanai F, Hamamura K, Obi S, Yoshida H, Omata M. Neoplastic seeding after radiofrequency ablation for hepatocellular carcinoma. Am J Gastroenterol 2008;103:3057–3062.
Ueno M, Hayami S, Shigekawa Y, Kawai M, Hirono S, Okada K, Tamai H, Shingaki N, Mori Y, Ichinose M, Yamaue H. Prognostic impact of surgery and radiofrequency ablation on single nodular HCC ≤5 cm: Cohort study based on serum HCC markers. J Hepatol 2015;65:1352–1359.
Hasegawa K, Kokudo N, Imamura H, Matsuyama Y, Aoki T, Minagawa M, Sano K, Sugawara Y, Takayama T, Makuuchi M. Prognostic impact of anatomic resection for hepatocellular carcinoma. Ann Surg 2005;242:252–259.
Makuuchi M, Kosuge T, Takayama T, Yamazaki S, Kakazu T, Miyagawa S, Kawasaki S. Surgery for small liver cancers. Semin Surg Oncol 1993;9:298–304.
Belghiti J, Clavien PA, Gadzijev E, Garden JO, Lau WY, Makuuchi M, Strong RW et al. The Brisbane 2000 terminology of liver anatomy and resections. HBP 2000;2:333–339.
Liver Cancer Study Group of Japan. General Rules for the Clinical and Pathological Study of Primary Liver Cancer, 3rd English edn. Tokyo: Kanehara Shuppan, 2010.
Hirokawa F, Hayashi M, Miyamoto Y, Asakuma M, Shimizu T, Komeda K, Inoue Y, Uchiyama K. Outcomes and predictors of microvascular invasion of solitary hepatocellular carcinoma. Hepatol Res 2014;44: 846–853.
Ryu T, Takami Y, Wada Y, Tateishi M, Matsushima H, Mikagi K, Saitsu H. Double- and triple-positive tumor markers predict early recurrence and poor survival in patients with hepatocellular carcinoma within the Milan criteria and Child-Pugh Class A. J Gastrointest Surg 2017;21:957–966.
Koike Y, Shiratori Y, Sato S, Obi S, Teratani T, Imamura M, Yoshida H, Shiina S, Omata M. Des-γ-carboxy prothrombin as a useful predisposing factor for the development of portal venous invasion in patients with hepatocellular carcinoma: a prospective analysis of 227 patients. Cancer 2001;91:561–569.
Pote N, Cauchy F, Albuquerque M, Voitot H, Belghiti J, Castera L, Puy H, Bedossa P, Paradis V. Performance of PIVKA-II for early hepatocellular carcinoma diagnosis and prediction of microvascular invasion. J Hepatol 2015;62:848–854.
Di Bisceglie AM, Sterling RK, Chung RT, Everhart JE, Dienstag JL, Bonkovsky HL, Wright EC, Everson GT, Lindsay KL, Lok AS, Lee WM, Morgan TR, Ghany MG, Gretch DR, HALT-C Trial Group: Serum alpha-fetoprotein levels in patients with advanced hepatitis C: results from the HALT-C Trial. J Hepatol 2005;43:434–441.
Marrero JA, Feng Z, Wang Y, Nguyen MH, Befeler AS, Roberts LR, Reddy KR, Harnois D, Llovet JM, Normolle D, Dalhgren J, Chia D, Lok AS, Wagner PD, Srivastava S, Schwartz M. Alpha-fetoprotein, des-gamma carboxyprothrombin, and lectin-bound alpha-fetoprotein in early hepatocellular carcinoma. Gastroenterology. 2009;137:110–118.
Nakashima Y, Nakashima O, Tanaka M, Okuda K, Nakashima M, Kojiro M. Portal vein invasion and intrahepatic micrometastasis in small hepatocellular carcinoma by gross type. Hepatol Res 2003;26:142–147.
Fujinaga Y, Kadoya M, Kozaka K, Shinmura R, Matsui O, Takayama T, Yamamoto M, Kokudo N, Kawasaki S, Arii S. Prediction of macroscopic findings of hepatocellular carcinoma on hepatobiliary phase of gadolinium-ethoxybenzyl-diethylenetriamine pentaacetic acid-enhanced magnetic resonance imaging:correlation with pathology. Hepatol Res. 2013;43:488–494.
Ueno S, Kubo F, Sakoda M, Hiwatashi K, Tateno T, Mataki Y, Maemura K, Shinchi H, Natsugoe S, Aikou T. Efficacy of anatomic resection vs. nonanatomic resection for small nodular hepatocellular carcinoma based on gross classification. J Hepatobiliary Pancreat Sci 2008;15:493–500.
Agrawal S, Belghiti J. Oncologic resection for malignant tumors of the liver. Ann Surg 2011;253:656–665.
Fukutomi S, Nomura Y, Nakashima O, Yano H, Tanaka H, Akagi Y, Okuda K. Evaluation of hepatocellular carcinoma spread via the portal system by 3-dimensional mapping. HPB 2017;19:1119–1125.
Acknowledgements
We thank Angela Morben, DVM, ELS, from Edanz Group (www.edanzediting.com/ac), for editing a draft of this manuscript.
Funding
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Author information
Authors and Affiliations
Contributions
Study conception and design: Ryu, Saitsu, and Okuda.
Acquisition of data: Ryu, Wada, Tateishi, Hara, Yoshitomi, Momosaki, and Yasumori.
Analysis and interpretation of data: Ryu, Takami, Yasumori, Momosaki, Saitsu, and Okuda.
Drafting of manuscript: Ryu.
Critical revision: Takami, Saitsu, and Okuda.
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no conflicts of interest.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Ryu, T., Takami, Y., Wada, Y. et al. A Clinical Scoring System for Predicting Microvascular Invasion in Patients with Hepatocellular Carcinoma Within the Milan Criteria. J Gastrointest Surg 23, 779–787 (2019). https://doi.org/10.1007/s11605-019-04134-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11605-019-04134-y