Abstract
Objectives
Overconsumption of non-nutritive sweeteners is associated with obesity, whereas the underlying mechanisms remain controversial. This study aimed to investigate the effects of long-term consumption of nutritive or non-nutritive sweeteners with or without high fat diet on sweet taste receptor expression in nutrient-sensing tissues and energy regulation dependent on sweet-sensing.
Methods
50 Male Sprague–Dawley rats (140–160 g) were assigned to 10 groups (n = 5/group). All received fructose at 2.5% or 10%, sucralose at 0.01% or 0.015% or water with a normal chow diet or high fat diet for 12 weeks. Food and drink intake were monitored daily. Oral glucose tolerance test and intraperitoneal glucose tolerance test were performed at week 10 and 11 respectively. Serum was obtained for measurement of biochemical parameters. Tongue, duodenum, jejunum, ileum, colon and hypothalamus were rapidly removed to assess gene expression.
Results
Long-term consumption of sweeteners impaired glucose tolerance, increased calorie intake and body weight. A significant upregulation of sweet taste receptor expression was observed in all the four intestinal segments in groups fed 0.01% sucralose or 0.015% sucralose, most strikingly in the ileum, accompanied by elevated serum glucagon-like peptide-1 levels and up-regulated expression of sodium-dependent glucose cotransporter 1 and glucose transporter 2. A significant down-regulation in the tongue and hypothalamus was observed in groups fed 10% fructose or 0.015% sucralose, with alterations in hypothalamic appetite signals. The presence of high fat diet differentially modulates sweet taste perception in nutrient-sensing tissues.
Conclusions
Long-term consumption of whether nutritive sweeteners or non-nutritive sweeteners combined with high fat diet contribute to dysregulation of sweet taste receptor expression in oral, intestinal and central nervous tissues.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
In the last few decades obesity has become a major public health problem that places patients at a greater risk of obesity-related diseases and significantly decreases the quality of life [1]. Excessive sugar sweetened beverages consumption, high-fructose corn syrup in particular, is increasingly considered as a major contributor to the obesity epidemic worldwide [2]. Therefore, non-nutritive sweeteners (NNSs) emerged as sugar substitutes to assist in weight control because they provide sweet taste with negligible energy [3]. However, there is a growing body of evidence suggesting that the consumption of NNSs may be closely associated with a greater risk of the metabolic syndrome and obesity epidemic, whereas the underlying mechanisms remain elusive [4].
Sweet taste performs a critical function in nutrient sensing as well as the control of food intake [5] and is initially sensed in gustatory tissues such as the anterior and posterior tongue and palate via sweet G protein-coupled taste receptors, the heterodimeric receptor of taste receptor type 1 member 2 (T1R2) and taste receptor type 1 member 3 (T1R3) [6]. Of note, sweet taste receptors (STRs) have also been found in chemosensory cells located in extra-oral tissues, most of which play an essential role in regulating glucose homeostasis and maintaining energy balance [7], such as gastrointestinal tract [8,9,10], hypothalamus [11], pancreas [12], and adipose tissue [13]. Hypothalamus is a nodal brain structure where information on systemic energy levels as well as metabolic status is detected via hormones or nutrients and integrated for homeostatic regulation, including the stimulation or inhibition of feeding behaviors and the control of energy expenditure [14]. Recent studies have indicated that STRs may play a role in nutrient sensing, especially glucose sensing in the hypothalamic feeding center via activating the arcuate nucleus neurons [15]. Similar to the response in hypothalamus, the presence of STRs in the gastrointestinal tract could also be functionally involved in the glucose responsiveness and multiple regulatory effects independently of carbohydrate metabolism, such as the modulation of hormone secretion and glucose absorption [16].
Accumulating evidence indicates that not only nutritive sweeteners, such as sucrose and fructose, but also NNSs could selectively bind to different domains of T1R2/T1R3 [17], raising the possibilities that sweeteners may disturb sweet taste perception in multiple tissues via long-term activation of STRs and further lead to potential health risks [18]. However, little is known about the long-term effects of sweeteners on the expression levels of STRs in different tissues. Besides, while most of the published findings on sweeteners have been short-term or single-dose [19, 20], it is worthwhile to investigate the long-term effects of sweeteners at various concentrations. Further, considering that the modern diets most often comprise of a mixture of various nutrient components, what also interests us is that how the joint use of different sweeteners and a high fat diet (HFD) contribute to the dysregulation of STRs [21]. Thus, the aim of the present work was to investigate how long-term consumption of nutritive sweeteners or NNSs in the presence or absence of HFD alter mRNA expression of STRs and affect hormone secretion, glucose transport and ingestive behavior. We chose fructose and sucralose as our target sweeteners, in view of their increasing popularity worldwide and the continuing controversy over their associations with obesity and type 2 diabetes [22,23,24].
Methods
Animals and diets
A total of 50 Male Sprague–Dawley rats (140–160 g) were purchased (SJA Laboratory Animal, Hunan, China) and housed in individual cages with constant temperature (25 ℃ ± 2 ℃), relative humidity (60% ± 5%), a 12 h light–dark cycle and free access to water and food. After one-week quarantine and acclimation period, rats were randomized into 10 groups (n = 5 per group), which were fed a normal control diet (NCD) or HFD (45% of energy as fat; Xietong Shengwu, Jiangsu, China) and received water or different sweeteners dissolved in water at the following concentration: fructose at 2.5% or 10% [25]; sucralose at 0.01% or 0.015% [26], and weighed daily (For more information about the composition of different diets, please see Supplementary Tables 1, 2, 3). Pre-weighed portions of food and premeasured volume of either water or the sweet taste solutions were offered to the rats. Food intake and drink consumption were monitored daily from week 1 to week 10. At the end of the 12 weeks experiment, the animals were fasted for 12 h and sacrificed by cervical dislocation after anesthetized with intraperitoneal injection of sodium pentobarbital. Blood samples were collected for serum biochemical analysis. Tongue, duodenum, jejunum, ileum, colon and hypothalamus were immediately frozen after dissection in liquid nitrogen and stored at − 80 °C. Animal use in this study was approved by the Institutional Animal Care and Use Committee, Wuhan University Center for Animal Experiment, Wuhan, China (AUP No. WP20210533).
Oral glucose tolerance test (OGTT) and intraperitoneal glucose tolerance test (IPGTT)
After feeding for 10 weeks, an oral glucose tolerance test was performed in all groups. After fasting for 14 h, all rats received 50% glucose solution via oral gavage (2 g/kg BW). Blood samples were adopted by rat tail snipping method and blood glucose levels were measured at 0 min (before gavage), 15 min, 30 min, 60 min, 90 min and 120 min via a glucometer and glucose test strips [27] (Roche, Shanghai, China).
For IPGTT, rats were fasted for 14 h after 11 weeks of diet administration and injected with a bolus of 50% glucose (2 g/kg BW) [28,29,30]. Blood glucose levels were measured at 0 min (before injection), 15 min, 30 min, 60 min, 90 min and 120 min by a glucometer.
Biochemical parameters
Serum glucose concentrations were analyzed using standard kits (Nanjing Jiancheng Bioengineering Institute, Nanjing, China) and serum insulin, glucagon-like peptide-1 (GLP-1) and leptin were determined using commercial ELISA kits (Ruixin Biotechnology, Quanzhou, China) following the manufacturers’ instructions.
Quantitative real-time PCR
Total RNA was extracted from tongue, duodenum, jejunum, ileum, colon and hypothalamus of individual rats using Biomarker Cell/Tissue Total RNA Isolation Kit (Biomarker Technologies, Beijing, China). cDNA was synthesized using BiomarkerScript II 1st Strand cDNA Synthesis Kit (Biomarker Technologies, Beijing, China). Real-time PCR was performed using the Biomarker 2X SYBR Green Fast qPCR Mix (Biomarker Technologies, Beijing, China) and Bio-Rad CFX maestro system. All manipulations were carried out according to the manufacturer’ s instructions. (All primer sequences for gene expression determination are shown in Supplementary Table 4). The β-actin gene was used as the internal control.
Statistical analysis
Shapiro–Wilk normal distribution test was used for assessing the compliance of data with the normal distribution. All data comply with normal distribution and are presented as mean ± standard deviation. Statistical analysis between multiple groups was performed using one-way ANOVA followed by Tukey’ s post-hoc test; statistical analysis between two groups was performed using Student’s t test. All the data analysis in this study were performed in GraphPad Prism 8.0 (GraphPad Software, USA); p < 0.05 was considered to be statistically significant.
Results
Body weight and changes in food intake, drink intake and calorie intake
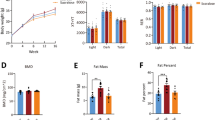
Rats fed 2.5% fructose or 10% fructose plus NCD consumed significantly less food than the control group (NCD + water). On the contrary, an evident increase in food consumption was observed in groups fed 0.015% sucralose. Food intake was significantly reduced in all groups by the presence of HFD (Fig. 1a and b). The addition of sweetener in the water significantly increased drink consumption, which was evidently reduced by the presence of HFD in all groups. Notably, rats fed 10% fructose exhibited the highest drink consumption whether in the presence of HFD or not (Fig. 1c and d). For total calorie intake, rats fed 0.015% sucralose unexpectedly showed the highest calorie intake among groups fed NCD, even higher than those fed 10% fructose. On the contrary, rats fed 2.5% fructose maintained a normal level of calorie intake. The presence of HFD significantly increased calorie intake in groups fed 2.5% fructose or 0.01% sucralose (Fig. 2a and b). Among groups fed NCD, rats fed with 10% fructose or 0.015% sucralose gained significantly more weight than those fed water, while the addition of HFD further increased body weight in all groups (Fig. 2c).
Changes in food intake and drink intake. a Food intake from week 1 to week 10; b AUC for food intake; c Drink intake from week 1 to week 10; d AUC for drink intake. Data are presented as mean ± SD, n = 5 per group. Results are considered significant at p < 0.05. *p < 0.05, **p < 0.01, ***p < 0.001 compared with the control group (NCD + water); #p < 0.05, ##p < 0.01, ###p < 0.001 compared with the corresponding group fed NCD
Changes in calorie intake and body weight. a Calorie intake from week 1 to week 10; b AUC for calorie intake; c Body weight. Data are presented as mean ± SD, n = 5 per group. Results are considered significant at p < 0.05. *p < 0.05, **p < 0.01, ***p < 0.001 compared with the control group (NCD + water); #p < 0.05, ##p < 0.01, ###p < 0.001 compared with the corresponding group fed NCD
Long-term supplementation of sweeteners and HFD impaired glucose tolerance
We performed OGTT and IPGTT to test whether challenges of long-time dietary intervention were accompanied by changes in glucose homeostasis. The IPGTT bypasses the oral cavity as well as intestine and assesses peripheral glucose tolerance which depends on pancreas, muscle, liver, adipose tissue [31]. Among groups fed NCD, AUCOGTT was significantly increased in rats fed 2.5% fructose or 10% fructose (Fig. 3a and b), while rats fed 0.015% sucralose had the highest AUCIPGTT, followed by those fed 0.01% sucralose (Fig. 3c and d). The presence of HFD increased both AUCOGTT (Fig. 3a and b) and AUCIPGTT (Fig. 3c and d) in all groups, while the statistical significance was reached in rats fed 10% fructose, 0.015% sucralose or water in OGTT and rats fed water in IPGTT compared with the corresponding group fed NCD.
Long-term supplementation of sweeteners and HFD impaired glucose tolerance. a Blood glucose levels at different time points during OGTT; b AUC in OGTT; c Blood glucose levels at different time points during IPGTT; d AUC in IPGTT. Data are presented as mean ± SD, n = 5 per group. Results are considered significant at p < 0.05. *p < 0.05, **p < 0.01, ***p < 0.001 compared with the control group (NCD + water); #p < 0.05, ##p < 0.01, ###p < 0.001 compared with the corresponding group fed NCD
Biochemical parameters
Rats fed with 2.5% fructose, 10% fructose, 0.01% sucralose or 0.015% sucralose plus NCD demonstrated significantly increased fasting blood glucose levels, whereas only those fed with 2.5% fructose, 10% fructose or 0.015% sucralose developed hyperinsulinemia. The presence of HFD evidently raised fasting blood glucose in rats fed 10% fructose or water and insulin levels in groups fed 10% fructose, 0.01% sucralose, 0.015% sucralose or water (Fig. 4a and b). Fasting serum GLP-1 levels were significantly increased in all groups, while the presence of HFD further elevated serum GLP-1 levels in those fed 2.5% fructose, 10% fructose, 0.015% sucralose or water (Fig. 4c). Among groups fed NCD, rats fed 10% fructose, 0.01% sucralose or 0.015% sucralose developed hyperleptinemia. Rats fed water plus HFD also showed significantly increased serum leptin levels, while the presence of HFD further significantly increased serum leptin levels in those fed 2.5% fructose, 0.01% sucralose, 0.015% sucralose (Fig. 4d).
Biochemical parameters. a Serum blood glucose levels; b Serum insulin levels; c Serum GLP-1 levels; d Serum leptin levels. Data are presented as mean ± SD, n = 5 per group. Results are considered significant at p < 0.05. *p < 0.05, **p < 0.01, ***p < 0.001 compared with the control group (NCD + water); #p < 0.05, ##p < 0.01, ###p < 0.001 compared with the corresponding group fed NCD
STR expression along the alimentary canal
In the tongue, among groups fed NCD, rats fed 10% fructose or 0.015% sucralose showed significantly down-regulated T1R2 and T1R3 expression, while the presence of HFD evidently up-regulated T1R2 and T1R3 expression in those fed 0.01% sucralose, 0.015% sucralose or water (Fig. 5, a and b). In the duodenum, T1R2 was evidently induced by all sweeteners in groups fed NCD, while 0.015% sucralose stimulated the expression of T1R3 to a higher extent than the rest of the sweeteners, followed by 0.01% sucralose and 10% fructose (Fig. 5c and d).
STR expression in the tongue and duodenum. a–b T1R2 and T1R3 expression in the tongue; c–d T1R2 and T1R3 expression in the duodenum. Data are presented as mean ± SD, n = 5 per group. Results are considered significant at p < 0.05. *p < 0.05, **p < 0.01, ***p < 0.001 compared with the control group (NCD + water); #p < 0.05, ##p < 0.01, ###p < 0.001 compared with the corresponding group fed NCD
An increase in the expression of T1R2 and T1R3 in jejunum (Fig. 6a and b) and ileum (Fig. 6c and d) was also observed among groups fed NCD. By contrast, colonic expression of T1R2 and T1R3 was significantly down-regulated in rats fed 2.5% fructose plus NCD (Fig. 6e and f). In the presence of HFD, mRNA expression of T1R2 and T1R3 was significantly down-regulated in groups fed 2.5% fructose or 0.01% sucralose, but up-regulated in groups fed 0.015% sucralose or water in the jejunum (Fig. 6a and b). By contrast, in the ileum, the presence of HFD further significantly increased the expression of T1R2 and T1R3 in most of the groups with the exception of those fed 10% fructose (Fig. 6c and d). For the colon, the presence of HFD evidently up-regulated T1R2 expression in groups fed 2.5% fructose, 10% fructose or water (Fig. 6e and f).
STR expression in the jejunum, ileum and colon. a–b T1R2 and T1R3 expression in the jejunum; c–d T1R2 and T1R3 expression in the ileum; e–f T1R2 and T1R3 expression in the colon. Data are presented as mean ± SD, n = 5 per group. Results are considered significant at p < 0.05. *p < 0.05, **p < 0.01, ***p < 0.001 compared with the control group (NCD + water); #p < 0.05, ##p < 0.01, ###p < 0.001 compared with the corresponding group fed NCD
Changes in expression of glucose transporters in the duodenum, jejunum and ileum
Upon activation by the presence of sweeteners in the intestinal lumen, STRs could facilitate glucose transport capacity via sodium-dependent glucose cotransporter 1 (SGLT-1) and glucose transporter 2 (GLUT2), both of which are critical transporters for glucose absorption [32]. In the duodenum, SGLT-1 expression was significantly up-regulated in rats fed 2.5% fructose or 10% fructose among groups fed NCD. The presence of HFD up-regulated SGLT-1 expression in rats fed 0.015% sucralose or water but exhibited an opposite effect in groups fed 2.5% fructose, 10% fructose or 0.01% sucralose (Fig. 7a). SGLT-1 expression in the jejunum (Fig. 7c) followed a similar pattern. In the ileum, rats fed 2.5% fructose or 0.015% sucralose showed significantly up-regulated SGLT-1 expression, which was further evidently induced by the presence of HFD in groups fed 0.01% sucralose or water (Fig. 7e).
Changes in expression of glucose transporters in the duodenum, jejunum and ileum. a–b SGLT-1 and GLUT2 expression in the duodenum; c–d SGLT-1 and GLUT2 expression in the jejunum; e–f SGLT-1 and GLUT2 expression in the ileum. Data are presented as mean ± SD, n = 5 per group. Results are considered significant at p < 0.05. *p < 0.05, **p < 0.01, ***p < 0.001 compared with the control group (NCD + water); #p < 0.05, ##p < 0.01, ###p < 0.001 compared with the corresponding group fed NCD
The stimulating effect on jejunal and ileal GLUT2 expression by the long-term consumption of sweeteners was more evident than that on duodenal GLUT2 expression (Fig. 7b), while rats fed 2.5% fructose, 10% fructose, 0.01% sucralose or 0.015% sucralose showed significantly up-regulated GLUT2 expression both in the jejunum (Fig. 7d) and ileum among groups fed NCD. Of note, the presence of HFD also remarkably up-regulated ileal GLUT2 expression in groups fed 2.5% fructose, 0.01% sucralose or 0.015% sucralose (Fig. 7f).
Changes in expression of STR and appetite signals in the hypothalamus
Among groups fed NCD, rats fed 10% fructose or 0.015% sucralose showed significantly down-regulated T1R2 and T1R3 expression in the hypothalamus, whereas only 2.5% fructose significantly up-regulated hypothalamic STR expression compared to the control group (NCD + water). Of note, the presence of HFD down-regulated both T1R2 and T1R3 expression in all groups, while the statistical significance was reached in groups fed 0.01% sucralose, 0.015% sucralose or water (Fig. 8a and b). Agouti-related peptide (AGRP) and neuropeptide Y (NPY) were significantly down-regulated in groups fed 10% fructose, 0.01% sucralose or 0.015% sucralose, and this effect was further exacerbated by the presence of HFD (Fig. 8c and d). On the contrary, proopiomelanocortin expression was significantly up-regulated in rats fed 2.5% fructose, 10% fructose or 0.015% sucralose, while HFD further increased proopiomelanocortin expression in groups fed 0.01% sucralose, 0.015% sucralose or water (Fig. 8e).
Changes in expression of STR and appetite signals in the hypothalamus. a–b T1R2 and T1R3 expression in the hypothalamus; c–e AGRP, NPY and POMC expression in the hypothalamus. Data are presented as mean ± SD, n = 5 per group. Results are considered significant at p < 0.05. *p < 0.05, **p < 0.01, ***p < 0.001 compared with the control group (NCD + water); #p < 0.05, ##p < 0.01, ###p < 0.001 compared with the corresponding group fed NCD
Discussion
Our investigation started with exploring the effect of long-term consumption of sweeteners, in the presence or absence of HFD, on glucose homeostasis and obesity-related parameters. We found that persistent consumption of sweeteners, particularly 10% fructose and 0.015% sucralose, resulted in increased body weight, AUCOGTT, AUCIPGTT and higher blood glucose levels, which were further exacerbated in the presence of HFD. It is well recognized that the gastrointestinal tract is a major determinant of postprandial glycemic control, responsible for glucose transport and the release of diverse peptide hormones and neurotransmitters [33]. Our results demonstrated that rats fed NCD in combination with either fructose or sucralose showed an overall increased mRNA expression of T1R2 and T1R3 in the duodenum, jejunum and mainly in the ileum. However, colonic expression of T1R2 and T1R3 was significantly up-regulated only in rats fed 0.01% sucralose or 0.015% sucralose among groups fed NCD. While a potential role of high fat diet in modulating intestinal STR expression has been indicated [25], in our study, the combination of HFD and sweetener had the most striking effect on the ileal STR expression. It is important to note that rats fed 0.01% sucralose or 0.015% sucralose plus HFD showed significantly up-regulated mRNA expression of T1R2 and T1R3 in all the four intestine segments. Evidence in rodents [34, 35], human cells and tissues [36, 37] strongly supports the functional role of STR, mainly expressed in gastrointestinal enteroendocrine cells, as an upstream sensor regulating GLP-1 secretion and the expression of glucose transporters, SGLT-1 and GLUT2 in the intestine. For example, GLP-1 secretion from the human L cell line NCI-H716 was promoted by sugars and sucralose but blocked by the sweet receptor antagonist lactisole or siRNA for α-gustducin [38]. Besides, in knockout mice lacking T1R3 or α-gustducin, mRNA expression and protein abundance of SGLT-1 were not increased in response to dietary sugar and NNS supplementation, as occurred in wild-type mice [39]. Our study showed that intestinal STR dysregulation was accompanied by elevated fasting serum GLP-1 levels and STR-dependent gains in mRNA expression of SGLT-1 and GLUT2 mainly in the ileum. We moreover noted that GLUT2 was stimulated to a higher extent than SGLT-1 by long-term consumption of fructose or sucralose whether in the presence or absence of HFD, suggesting an enhanced intestinal absorptive capacity especially when lumenal glucose concentration is high after a meal, which further results in an increase in postprandial excursions [40], as shown in OGTT.
Evidence has been provided that different metabolic states could influence lingual and hypothalamic sweet responses through modifying the expression of STRs, which further contributes to changes in feeding motivation and food intake [41, 42]. In our study, among groups fed NCD, rats fed 0.015% sucralose surprisingly ingested the most calories, even higher than those fed 10% fructose, while rats fed 2.5% fructose or 0.01% sucralose consumed equivalent energy to the control group (NCD + water), indicating that those fed 2.5% fructose compensated for the ingested liquid calories by reducing the ingestion of NCD. The presence of HFD increased energy intake in most of the groups, and rats fed 10% fructose consumed the most calories, followed by those fed 2.5% fructose or 0.015% sucralose. It has been previously revealed that impaired sweet taste sensitivity would promote obesity because a down-regulation in STRs could result in a different threshold for glucose and other sweet tastants both in the tongue and hypothalamus and increase food intake to compensate for the reduced sensitivity [41]. In line with these findings, we found that groups fed 10% fructose or 0.015% sucralose plus NCD showed significantly down-regulated STR expression both in the tongue and hypothalamus. Besides, our data indicated a potential role of HFD in modulating sweet taste perception in different nutrient-sensing tissues, since the presence of HFD exhibited opposite effects on lingual and hypothalamic STR expression in rats fed 0.01% sucralose, 0.015% sucralose or water.
Ingestive behavior is regulated by two major populations of neurons in the arcuate nucleus of hypothalamus: NPY and AgRP-coexpression neurons stimulate food intake; proopiomelanocortin-expression neurons decrease food intake [43]. In our study, in addition to significantly down-regulated STR expression, long term supplementation of 10% fructose or 0.015% sucralose resulted in an evident increase in proopiomelanocortin expression but a decrease in AGRP/NPY expression whether in the presence of NCD or HFD, which is consistent with hypothalamic neuropeptide expression in animals exhibiting hyperphagia induced by palatable food [44, 45]. While the leptin-mediated inhibition of NPY and AgRP may partially explain the reduction of these orexigenic neuropeptides [45], our study also indicated a role for STR since activation of hypothalamic STR in the arcuate nucleus contributes to the increased firing of glucose-excitatory neurons, including proopiomelanocortin-expression neurons [15, 46], and decreased STR expression could therefore result in a high activation threshold of glucose-excitatory neurons and consequently weaken of the satiation effects of glucose. However, further studies will be needed to fully elucidate the relationship between the dysregulation of STR and alteration in ingestive behavior.
In conclusion, NNSs, typically considered to be metabolically inert, are actually not functionally inert and could result in disturbance in sweet taste perception in not only oral but also intestinal and central nervous tissues and further exert negative influence on global glycemic control, fuel utilization and energy homeostasis in a STR-dependent manner. It has to be pointed out that the difference between T1R2 and T1R3 expression may be due to the fact that T1R3 is also associated with umami sensing and could operate in a homomeric form [7]. We also investigate a new possibility that the combination of HFD may also influence sweet taste sensation and exacerbate the effects of different sweeteners. Alteration in protein levels and tissue-specific ablation of STRs will be further required to elucidate the specific downstream signaling, by which STRs perform multiple functions and play a role in the development of obesity.
Data availability
The datasets used and analysed in this current study are available from the corresponding author upon reasonable request.
Abbreviations
- AGRP:
-
Agouti-related peptide
- AUC:
-
Area under the curve
- GLP-1:
-
Glucagon-like peptide-1
- GLUT2:
-
Glucose transporter 2
- HFD:
-
High-fat diet
- IPGTT:
-
Intraperitoneal glucose tolerance test
- NCD:
-
Normal control diet
- NNS:
-
Non-nutritive sweetener
- NPY:
-
Neuropeptide Y
- OGTT:
-
Oral glucose tolerance test
- SGLT-1:
-
Sodium-dependent glucose cotransporter 1
- STR:
-
Sweet taste receptor
- T1R2:
-
Taste receptor type 1 member 2
- T1R3:
-
Taste receptor type 1 member 3
References
Bluher M (2019) Obesity: global epidemiology and pathogenesis. Nat Rev Endocrinol 15:288–298. https://doi.org/10.1038/s41574-019-0176-8
Febbraio MA, Karin M (2021) “Sweet death”: fructose as a metabolic toxin that targets the gut-liver axis. Cell Metab 33:2316–2328. https://doi.org/10.1016/j.cmet.2021.09.004
Hunter SR, Reister EJ, Cheon E et al (2019) Low calorie sweeteners differ in their physiological effects in humans. Nutrients. https://doi.org/10.3390/nu11112717
Pearlman M, Obert J, Casey L (2017) The association between artificial sweeteners and obesity. Curr Gastroenterol Rep 19:64. https://doi.org/10.1007/s11894-017-0602-9
Liem DG, Russell CG (2019) The influence of taste liking on the consumption of nutrient rich and nutrient poor foods. Front Nutr 6:174. https://doi.org/10.3389/fnut.2019.00174
Treesukosol Y, Smith KR, Spector AC (2011) The functional role of the t1r family of receptors in sweet taste and feeding. Physiol Behav 105:14–26. https://doi.org/10.1016/j.physbeh.2011.02.030
von Molitor E, Riedel K, Krohn M et al (2021) Sweet taste is complex: signaling cascades and circuits involved in sweet sensation. Front Hum Neurosci 15:667709–10. https://doi.org/10.3389/fnhum.2021.667709
Young RL, Sutherland K, Pezos N et al (2009) Expression of taste molecules in the upper gastrointestinal tract in humans with and without type 2 diabetes. Gut 58:337–346. https://doi.org/10.1136/gut.2008.148932
Hass N, Schwarzenbacher K, Breer H (2010) T1r3 is expressed in brush cells and ghrelin-producing cells of murine stomach. Cell Tissue Res 339:493–504. https://doi.org/10.1007/s00441-009-0907-6
Dyer J, Salmon KS, Zibrik L et al (2005) Expression of sweet taste receptors of the t1r family in the intestinal tract and enteroendocrine cells. Biochem Soc Trans 33:302–305. https://doi.org/10.1042/BST0330302
Ren X, Zhou L, Terwilliger R et al (2009) Sweet taste signaling functions as a hypothalamic glucose sensor. Front Integr Neurosci 3:12. https://doi.org/10.3389/neuro.07.012.2009
Medina A, Nakagawa Y, Ma J et al (2014) Expression of the glucose-sensing receptor t1r3 in pancreatic islet: changes in the expression levels in various nutritional and metabolic states. Endocr J 61:797–805. https://doi.org/10.1507/endocrj.ej14-0221
Masubuchi Y, Nakagawa Y, Ma J et al (2013) A novel regulatory function of sweet taste-sensing receptor in adipogenic differentiation of 3t3-l1 cells. Plos One 8:e54500. https://doi.org/10.1371/journal.pone.0054500
Hao S, Yang Y, Helmy M et al (2020) Neural regulation of feeding behavior. Adv Exp Med Biol 1284:23–33. https://doi.org/10.1007/978-981-15-7086-5_3
Kohno D (2017) Sweet taste receptor in the hypothalamus: a potential new player in glucose sensing in the hypothalamus. J Physiol Sci 67:459–465. https://doi.org/10.1007/s12576-017-0535-y
Steinert RE, Gerspach AC, Gutmann H et al (2011) The functional involvement of gut-expressed sweet taste receptors in glucose-stimulated secretion of glucagon-like peptide-1 (glp-1) and peptide yy (pyy). Clin Nutr 30:524–532. https://doi.org/10.1016/j.clnu.2011.01.007
DuBois GE (2016) Molecular mechanism of sweetness sensation. Physiol Behav 164:453–463. https://doi.org/10.1016/j.physbeh.2016.03.015
Laffitte A, Neiers F, Briand L (2014) Functional roles of the sweet taste receptor in oral and extraoral tissues. Curr Opin Clin Nutr Metab Care 17:379–385. https://doi.org/10.1097/MCO.0000000000000058
Thomson P, Santibanez R, Aguirre C et al (2019) Short-term impact of sucralose consumption on the metabolic response and gut microbiome of healthy adults. Br J Nutr 122:856–862. https://doi.org/10.1017/S0007114519001570
Morales-Rios EI, Garcia-Machorro J, Briones-Aranda A et al (2022) Effect of long-term intake of nutritive and non-nutritive sweeteners on metabolic health and cognition in adult male rats. J Med Food. https://doi.org/10.1089/jmf.2022.0016
Khan AS, Murtaza B, Hichami A et al (2019) A cross-talk between fat and bitter taste modalities. Biochimie 159:3–8. https://doi.org/10.1016/j.biochi.2018.06.013
Khorshidian N, Shadnoush M, Zabihzadeh KM et al (2021) Fructose and high fructose corn syrup: are they a two-edged sword? Int J Food Sci Nutr 72:592–614. https://doi.org/10.1080/09637486.2020.1862068
Martyn D, Darch M, Roberts A et al (2018) Low-/no-calorie sweeteners: a review of global intakes. Nutrients. https://doi.org/10.3390/nu10030357
Walbolt J, Koh Y (2020) Non-nutritive sweeteners and their associations with obesity and type 2 diabetes. J Obes Metab Syndr 29:114–123. https://doi.org/10.7570/jomes19079
Sanchez-Tapia M, Martinez-Medina J, Tovar AR et al (2019) Natural and artificial sweeteners and high fat diet modify differential taste receptors, insulin, and tlr4-mediated inflammatory pathways in adipose tissues of rats. Nutrients. https://doi.org/10.3390/nu11040880
Loney GC, Torregrossa AM, Smith JC et al (2011) Rats display a robust bimodal preference profile for sucralose. Chem Senses 36:733–745. https://doi.org/10.1093/chemse/bjr048
Boye A, Acheampong DO, Gyamerah EO et al (2020) Glucose lowering and pancreato-protective effects of Abrus precatorius (L.) leaf extract in normoglycemic and STZ/nicotinamide—induced diabetic rats. J Ethnopharmacol 258:112918. https://doi.org/10.1016/j.jep.2020.112918
Kim JY, Choi MJ, So B et al (2015) The preventive effects of 8 weeks of resistance training on glucose tolerance and muscle fiber type composition in zucker rats. Diabetes Metab J 39:424–433. https://doi.org/10.4093/dmj.2015.39.5.424
Zhang R, Zhou J, Li M et al (2014) Ameliorating effect and potential mechanism of Rehmannia glutinosa oligosaccharides on the impaired glucose metabolism in chronic stress rats fed with high-fat diet. Phytomedicine 21:607–614. https://doi.org/10.1016/j.phymed.2013.11.008
Shu Q, Chen L, Wu S et al (2020) Acupuncture targeting sirt1 in the hypothalamic arcuate nucleus can improve obesity in high-fat-diet-induced rats with insulin resistance via an anorectic effect. Obes Facts 13:40–57. https://doi.org/10.1159/000503752
Smith KR, Hussain T, Karimian AE et al (2016) Disruption of the sugar-sensing receptor t1r2 attenuates metabolic derangements associated with diet-induced obesity. Am J Physiol Endocrinol Metab 310:E688–E698. https://doi.org/10.1152/ajpendo.00484.2015
Young RL (2011) Sensing via intestinal sweet taste pathways. Front Neurosci 5:23. https://doi.org/10.3389/fnins.2011.00023
Kreuch D, Keating DJ, Wu T et al (2018) Gut mechanisms linking intestinal sweet sensing to glycemic control. Front Endocrinol (Lausanne) 9:741. https://doi.org/10.3389/fendo.2018.00741
Qian C, Qi YC, Feng RL et al (2021) Sucralose can improve glucose tolerance and upregulate expression of sweet taste receptors and glucose transporters in an obese rat model. Eur J Nutr 60:1809–1817. https://doi.org/10.1007/s00394-020-02375-1
Song X, Wang F, Xu H et al (2019) 3-deoxyglucosone induces glucagon-like peptide-1 secretion from stc-1 cells via upregulating sweet taste receptor expression under basal conditions. Int J Endocrinol 2019:4959646. https://doi.org/10.1155/2019/4959646
Ohtsu Y, Nakagawa Y, Nagasawa M et al (2014) Diverse signaling systems activated by the sweet taste receptor in human glp-1-secreting cells. Mol Cell Endocrinol 394:70–79. https://doi.org/10.1016/j.mce.2014.07.004
Nguyen NQ, Debreceni TL, Bambrick JE et al (2015) Accelerated intestinal glucose absorption in morbidly obese humans: relationship to glucose transporters, incretin hormones, and glycemia. J Clin Endocrinol Metab 100:968–976. https://doi.org/10.1210/jc.2014-3144
Jang HJ, Kokrashvili Z, Theodorakis MJ et al (2007) Gut-expressed gustducin and taste receptors regulate secretion of glucagon-like peptide-1. Proc Natl Acad Sci USA 104:15069–15074. https://doi.org/10.1073/pnas.0706890104
Margolskee RF, Dyer J, Kokrashvili Z et al (2007) T1r3 and gustducin in gut sense sugars to regulate expression of na+-glucose cotransporter 1. Proc Natl Acad Sci USA 104:15075–15080. https://doi.org/10.1073/pnas.0706678104
Kellett GL, Brot-Laroche E (2005) Apical glut2—a major pathway of intestinal sugar absorption. Diabetes 54:3056–3062. https://doi.org/10.2337/diabetes.54.10.3056
Herrera MCD, Argmann C, Van Eijk M et al (2016) Impact of obesity on taste receptor expression in extra-oral tissues: emphasis on hypothalamus and brainstem. Sci Rep 6:29094. https://doi.org/10.1038/srep29094
Zhao X, Yan J, Chen K et al (2018) Effects of saccharin supplementation on body weight, sweet receptor mRNA expression and appetite signals regulation in post-weanling rats. Peptides 107:32–38. https://doi.org/10.1016/j.peptides.2018.07.006
Schneeberger M, Gomis R, Claret M (2014) Hypothalamic and brainstem neuronal circuits controlling homeostatic energy balance. J Endocrinol 220:T25–T46. https://doi.org/10.1530/JOE-13-0398
la Fleur SE, van Rozen AJ, Luijendijk MC et al (2010) A free-choice high-fat high-sugar diet induces changes in arcuate neuropeptide expression that support hyperphagia. Int J Obes (Lond) 34:537–546. https://doi.org/10.1038/ijo.2009.257
Guerra-Cantera S, Frago LM, Collado-Perez R et al (2021) Sex differences in metabolic recuperation after weight loss in high fat diet-induced obese mice. Front Endocrinol (Lausanne) 12:796661–8. https://doi.org/10.3389/fendo.2021.796661
Kohno D, Koike M, Ninomiya Y et al (2016) Sweet taste receptor serves to activate glucose- and leptin-responsive neurons in the hypothalamic arcuate nucleus and participates in glucose responsiveness. Front Neurosci 10:502. https://doi.org/10.3389/fnins.2016.00502
Funding
No.
Author information
Authors and Affiliations
Contributions
The authors’ responsibilities were as followed. YZ and HD designed research; YZ, LC, JG, YC, FL, XB conducted research; YZ and HD analyzed data; YZ wrote the paper; YZ and HD had primary responsibility for the final content. All authors read and approved the final version of the paper.
Corresponding author
Ethics declarations
Conflict of interest
Y. Zhang, L. Chen, J. Gao, Y. Cheng, F. Luo, X. Bai, H. Ding, no conflicts of interest.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Zhang, Y., Chen, L., Gao, J. et al. Nutritive/non-nutritive sweeteners and high fat diet contribute to dysregulation of sweet taste receptors and metabolic derangements in oral, intestinal and central nervous tissues. Eur J Nutr 62, 3149–3159 (2023). https://doi.org/10.1007/s00394-023-03187-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00394-023-03187-9