Abstract
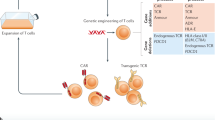
Immunotherapy is one of the most promising and innovative approaches to treat cancer, viral infections, and other immune-modulated diseases. Adoptive immunotherapy using gene-modified T cells is an exciting and rapidly evolving field. Exploiting knowledge of basic T cell biology and immune cell receptor function has fostered innovative approaches to modify immune cell function. Highly translatable clinical technologies have been developed to redirect T cell specificity by introducing designed receptors. The ability to engineer T cells to manifest desired phenotypes and functions is now a thrilling reality. In this review, we focus on outlining different varieties of genetically engineered T cells, their respective advantages and disadvantages as tools for immunotherapy, and their promise and drawbacks in the clinic.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
T cells play a central role in mediating cellular immunity. These multi-functional adaptive immune cells protect us from disease throughout our entire lives with their ability to recognize bacterial, viral, and cancer-associated antigens. T cells harbor a T cell receptor (TCR), which dictates their antigen specificity and exists as a membrane heterodimer, associated with the CD3 signaling complex. The TCR binds a ligand consisting of a peptide processed from pathogens, malignant, and normal cells presented to the T cell by the major histocompatibility complex (MHC). In this way, T cells can recognize the presence of pathogens or transformed cells, leading to target cell killing, or the secretion of pro-inflammatory cytokines that recruit and support other immune effectors.
Unfortunately, most viruses and tumors have developed various mechanisms to evade the host immune system, leading to weak or ineffective immune responses, resulting in chronic infections or malignancies. To address the issue of immune responses ineffective at eliminating cancer, many therapeutic approaches are aimed at harnessing and optimizing the anti-tumor potential of T cells. One such strategy known as adoptive cell transfer (ACT) involves the transfer of ex vivo activated and expanded antigen-reactive T cells or genetic modification to redirect their specificity prior to transfer. ACT gained its first success using lymphokine-activated killer (LAK) cells [1] and later tumor-infiltrating lymphocytes (TILs) [2, 3] or antigen-stimulated autologous peripheral blood lymphocytes (PBL) [4–7].
The most promising of these early approaches utilized TIL following harvest from tumor, and short-term ex vivo expansion was pioneered by the Rosenberg group at the Surgery Branch of the National Cancer Institute. Animal models and studies in patients with melanoma demonstrated that lymphocytes isolated from TIL maintained tumor reactivity in vitro, having the capability to lyse tumor cells and secrete cytokines, such as IL-2, IFNγ, and TNFα [8, 9]. These cells were also able to mediate objective clinical responses when grown ex vivo and infused back into patients [10].
Despite these promising but preliminary clinical results, for a variety of reasons TIL has not been a universal approach for ACT. Aside from TIL production being a logistically and technically demanding method, oftentimes primary tumors harboring TIL are previously resected as part of cancer treatment or inaccessible depending on the tumor type and location. Additionally, the time it takes or the inability to expand available TIL to therapeutic numbers calls for an alternative cell-based approach for treating cancer or chronic viral infections.
Recent technological advances have facilitated efficient expression of transgenes in T cells allowing for normal circulating peripheral lymphocytes to be redirected targeting antigens of choice. Genetic engineering of T cells with chimeric antigen receptors (CARs), TCRs, and other receptors has been shown to successfully redirect the specificity of T cells. Such strategies are the focus of this review.
However, the ability to redirect a T cell to recognize a specific antigen is not enough to ensure an effective immunotherapy. Antigen recognition needs to be coupled with efforts to ensure a T cell’s functionality specific to the target while limiting off-target or off-tumor recognition. T cells should also be able to functionally persist long term and be able to traffic to and accumulate at the target site. Additionally, optimal modified T cells should exhibit robust, multi-functional immune responses, resist mechanisms of anergy, exhaustion and immunosuppression, and be amenable to deletion on demand to diminish potential toxicity issues. While these strategies show promise at the bench and have had some clinical success at the bedside, many aspects of this type of therapy must be resolved before these effectors are good enough to become a standard treatment for patients.
Chimeric antigen receptors
CAR design
One class of antigen receptors that have been widely examined for the use of redirecting T cell specificity is CARs (Fig. 1a). A CAR is simply described as combining the antigen-binding capability of an antibody with the intracellular signaling-associated component of a TCR. This unique juxtaposition allows for high affinity, three-dimensional epitope recognition by an immunoglobulin to be linked to the helper or effector responses of a T cell. Specifically, the extracellular antigen-recognizing domain is derived from the antigen-binding fragment (Fab) of mouse monoclonal antibodies (mAbs) that have high affinity for specific antigens. Unlike the normal structure of the Fab fragment of a mAb, the Fab fragment in a CAR exists as a single-chain variable fragment (scFv). The scFv is linked via hinge and transmembrane domains to an intracellular signaling domain. This allows for antigen recognition to be coupled to immune cell signal transduction by phosphorylation of immunoreceptor tyrosine-based activation motifs (ITAMs). While the first CAR, described by Eshhar and colleagues, linked the scFv to the signaling components of the FcR γ chain [11], subsequent CARs used that of the ζ chain of the TCR/CD3 complex [12] as the CD3ζ signaling domain contains three ITAMs as opposed to FcRγ’s single ITAM. This structural configuration allows for essentially any mAb to be engineered to make a CAR. But for targets where generating conventional antibodies in mice or other species is difficult, other techniques, including phage display, have been useful in generating the antigen-binding portion of the CAR [13, 14].
CAR-mediated target cell recognition. a Structure of a second-generation CAR interacting with tumor cell. A CAR consists of a single-chain variable fragment (scFv) composed of variable light (V L) and heavy (V H) chains linked via hinge, transmembrane domains, and intracellular signaling domains containing at least the γ chain of the FcR or the ζ chain of the TCR/CD3 complex. Identity of the scFv region dictates MHC-independent recognition of a surface antigen. ITAMs of CD3ζ are denoted in blue octagons; b comparison of costimulatory domains included in first, second, or third generation of CARs. ITAMs are denoted as colored octagons
The use of a mAb or ligand receptor facilitates recognition of intact proteins, carbohydrates, and lipids and can alleviate the need for target antigens to be processed and presented by MHC molecules. However, CARs and TCR-like mAbs have also been designed to recognize conformational epitopes of pMHC [15–18]. Yet, avoiding MHC restriction would allow for CAR-mediated target recognition in spite of HLA downregulation or aberrant proteasomal antigen-processing mechanisms. This non-MHC-restricted antigen recognition also allows CAR use in patients of all HLA types, which is a distinct advantage from the use of engineered TCRs, as will be discussed. CARs are also independent of many of the signaling molecules or coreceptors required for TCR signaling and do not require association with the CD3 complex for T cell activation and function. As such, CARs contain all the minimal elements necessary to bind antigen and activate the T cell. Additionally, as a single-chain construct, CAR constructs are compact with relatively small vectors, allowing it to easily make high titer virus for transduction. Furthermore, single-chain CARs are not subject to chain pairing competition or mispairing, unlike when introducing exogenous TCRs as discussed in a later section.
However, there are some limitations to the use of CAR-engineered T cells [19]. CAR recognition only targets antigens expressed on the cell surface. Thus, they would not be effective against non-surface viral proteins that exist intracellularly and are processed and presented by MHC. Although CARs’ lack of MHC restriction avoids immune escape mechanisms including HLA downregulation, antigen loss can still limit the effectiveness of antigen-specific CARs [20, 21]. Additionally, myeloid-derived suppressor cells (MDSCs) have been shown to inhibit the efficacy of CAR-engineered T cells through engagement of PD-1 in a murine model for metastatic colorectal cancer [22]. Also, the mAb–antigen interaction is much stronger than a TCR–antigen interaction, which may impact T cell function [23], and the identity of the scFv region is thought to impact the stability and activity of CAR T cells [24]. Moreover, use of murine-derived scFv causes concern for potential immunogenicity of these chimeric receptors [25, 26], although efforts to reduce immunogenicity have been used by humanizing murine-derived scFv or generating scFv from human scFv phage display libraries [27].
Generations of CARs
Over time, the design of CARs has been refined to provide better antigen recognition and a more efficient transfer of cellular signaling for T cell function and persistence [28]. As mentioned previously, the signaling domain of FcRγ was swapped with that of CD3ζ because it included a greater number of ITAMs (Fig. 1b). Additionally, the single-chain antibody can be substituted by other receptors or a ligand of a receptor expressed on tumor cells. Such approaches include substituting the scFv region of a CAR for heregulin (a ligand for Her3 or Her4 receptors) [29], VEGF (anti-VEGFR2) [30], NKp30 (targeting B7-H6) [31], or the NKG2D receptor [32–34]. Moreover, multiple signaling domains have been added to the CD3ζ or FcRγ domains to augment activation and costimulation mimicking immunologic signal 2 during physiologic T cell activation [35].
“Second-generation” CARs (Fig. 1b) utilize an additional cytoplasmic domain of a costimulatory receptor, such as CD28, 4-1BB, DAP10, OX40, or ICOS, providing greater strength of signaling and persistence to the T cells [36–42].
A third generation of CARs (Fig. 1b) was also developed using two costimulatory domains with an activating domain, conferring an even greater potency to redirected T cells [36, 43–48]. But these more complex structures warrant further investigation as it is unclear whether the strong costimulation would always be advantageous [49]. Optimization of how many and which type of signaling domains included is necessary to determine which combination is best for augmenting activation, sustained function, and survival while minimizing anergy, premature death, and rapid exhaustion. Additionally, further efforts to examine how antigen location and density, and CAR binding moiety, affinity, and sensitivity affect its function may also help influence development of optimally designed CARs.
CAR targets
The first clinical trials using CAR targeted folate-binding protein (FBP) for patients with ovarian cancer [50] and carbonic anhydrase IX (CAIX) for patients with renal cell carcinoma (RCC) [51]. Both CARs were first generation containing the FcRγ signaling domain. In both of these trials, no objective clinical responses were seen, nor were the genetically altered T cells able to persist long term, but the potential for adverse events using CAR therapy was first evident. In the trial targeting CAIX+ RCC, the phenomenon described as “on-target, off-tumor” was clearly evident. Patients treated with the CAIX CAR gene-modified T cells experienced grade 2–4 liver toxicity because the transduced cells recognized CAIX antigen expressed on the epithelial cells of the bile duct [51].
As subsequent generations of CARs were developed and more efficient CAR targets were identified, we began to see greater clinical success with CARs. The efforts targeting pan-B cell antigen CD19 are the best examples of the proof of concept for CAR therapy of this. Initial trials targeting CD19 associated with relapsed indolent non-Hodgkin’s lymphomas (NHL) and chronic lymphocytic leukemia (CLL) [52–58] demonstrated the safety of CAR T cells and modest clinical benefit. Later, patients with B cell acute lymphoblastic leukemia (B-ALL) receiving CD19-targeted CAR T cell treatment resulted in positive clinical outcomes with robust anti-tumor efficacy in two independent trials [21, 59]. One trial utilized a second-generation CD28/CD3ζ anti-CD19 CAR and achieved rapid tumor eradication and minimal residual disease-negative complete remissions in all five patients treated [59]. Therapy was well tolerated, and steroid therapy ameliorated cytokine-mediated toxicities. The other trial used second-generation anti-CD19 CAR T cells including costimulatory cassette 4-1BB (in contrast to CD28 in the clinical study described above) to treat two children with B-ALL, achieving expansion of anti-CD19 CAR T cells and complete remission in both patients [21]. Cytokine-release syndrome developed in both patients, but was effectively reversed with etanercept and tocilizumab treatment without reducing antileukemic efficacy. However, one patient relapsed with CD19− blast cells 2 months after treatment, indicating a need to target other molecules in some patients with ALL.
The success of anti-CD19 CARs is facilitated by the near-universal expression of CD19 on B cell malignancies but limited and absent expression on B cells and bone marrow stem cells, respectively. These properties also limit the off-target potential of anti-CD19 CARs. Outcomes from this CD19 model also allowed for the observation of practical limitations of initial CAR designs and allowed for development of subsequent generations of CARs. Most recently, a clinical trial used a second-generation CD19-reactive CAR to treat both children and young adults with chemotherapy-resistant B-precursor acute lymphoblastic leukemia inducing a complete response in 70 % of patients with B-ALL and an minimal residual disease-negative complete in response in 60 % [60]. Additionally, all toxicities associated with the therapy were reversible.
Although less serious than the aforementioned “on-target, off-tumor” events, a potential drawback of the highly effective CD19 CAR campaign targeting B cell malignancies is the prolonged elimination of normal B lymphocytes and, thus, impairment of humoral immunity [52, 55, 57]. However, B cell aplasia and hypogammaglobulinemia can be easily mitigated by intravenous administration of gammaglobulin.
While CD19-targeted B cell malignancies have been the poster child advocating for CAR therapy, it is important to acknowledge another CAR target that has exhibited mixed clinical results. In 2010, it was reported that the use of a third-generation CAR was based on the widely used mAb trastuzumab targeting Her-2 induced respiratory distress resulting in death in one treated patient with metastatic colon cancer [49]. It was discovered that low-level Her-2 expression on normal lung epithelium caused this fatal side effect, characterized as a much more serious “on-target, off-tumor” adverse event. Additionally, the very high dose of CAR T cells (1010 T cells) may have precluded any potential therapeutic window. With this in mind, a modified CAR-based approach targeting Her-2 led to a more successful recent trial [61]. In this report, a dose-escalation study using a second-generation Her-2-specific CAR with a different scFv was used in patients with recurrent/refractory Her-2+ sarcomas. This study also differed in that it administered lower doses of T cells (1 × 104–1 × 108/m2), and it did not use coadministration of high-dose IL-2 or lymphodepleting chemotherapy prior to transfusion. Transduced cells persisted for 6 weeks and trafficked to tumor sites without any evident toxicities. Some patients even exhibited stable disease or partial response. The stark contrast between these two trials highlights the importance of mAb selection, generation of CAR, target distribution, and host preconditioning can have on the positive and negative outcomes in CAR clinical trials.
A wide variety of other CARs have been designed to target an array of antigens showing promise as potential therapies for cancer. Other targets evaluated in vitro and in vivo include but are not limited to EGFRvIII [62] for glioblastoma, GD2 [63, 64] for neuroblastoma, GD3 [65, 66], MAGE-1 [18], and HMW-MAA [67] for melanoma, CD20 [43, 45, 68–71], CD23 [72], CD30 [73–75] and others for hematologic malignancies, PSMA [39, 76] for prostate cancer, MUC-1 [46], Her-2 [77, 78], and CEA [79–81] for breast cancer, EGP-40 [82] for colorectal cancer, VEGF-R2 [30, 83] and KDR [84] for tumor neovasculature, and MUC16 [85] for ovarian cancer. Table 1 lists a sampling of active clinical trials using CARs and their respective targets.
CAR summary
Overall, CARs provide MHC-independent recognition of a variety of extracellular target types with a compact, single-chain construct containing all the minimal elements necessary for T cell activation. For better or for worse, the design of CARs prevents any chance of receptor mispairing but circumvents the natural process of T cell activation. While documentation of “on-target, off-tumor” is well noted, “off-target” effects are not as readily seen because the antigen-binding region of CARs is derived from monoclonal antibodies that have been well characterized. However, several groups conducting clinical trials with CARs have seen other serious adverse events including tumor lysis syndrome [57] and cytokine storm [55, 86, 87]. Additionally, anti-transgene immunogenicity has been described as a potential cause of low persistence of CAR T cells post-transfer [53] and has even caused severe anaphylactic reactions in patients treated with CAR T cells [26]. Overall, the majority of CAR studies have shown much promise for their clinical use, and continuing efforts are further elucidating how to limit improve clinical outcomes while minimizing adverse events.
T cell receptors
TCR design
TCRs compose an additional class of antigen receptors used to engineer T cells. Natively, CD8+ and CD4+ T cells express a TCR as a membrane-bound αβ heterodimer, which recognizes antigenic peptide fragments bound to MHC class I or II, respectively. To date, TCRs investigated for ACT have been limited to mostly MHC-I-restricted candidates. These TCRs can recognize any intracellular antigen as it is processed and presented by MHC molecules and associate with the CD3 complex that initiates ITAM-mediated signal transduction in the T cell (Fig. 2).
TCR-mediated target cell recognition. Depicted is the structure of an MHC class I-restricted TCR interacting with tumor or virus-infected cell. TCR α and β chains are specific to both MHC and presented antigenic peptide. The TCR complexes with various CD3 components on the cell surface, and the CD8 coreceptor stabilizes the TCR–pMHC interaction while recruiting lck to facilitate TCR signaling. ITAMs are denoted as colored octagons. Lck = lymphocyte-specific protein tyrosine kinase; Zap70 = zeta-chain-associated protein kinase 70
Because TCRs recognize processed peptides presented on MHC, targeted antigens can be derived from the entire protein composition of the tumor cells, including intracellular proteins, whereas CARs can only be designed to recognize molecules expressed on the surface of target cells. This quality also allows TCRs to target a large number of non-surface antigens of virally infected cells and tumors associated with viral infection, such as hepatitis-associated hepatocellular carcinoma, papilloma virus-associated cervical cancer, and Epstein–Barr virus-related malignancies.
An important factor influencing the effectiveness of immunotherapeutic use of TCRs is the relationship between receptor affinity and cell function. Because antigen recognition depends on the interaction between the TCR and the peptide MHC (pMHC) complex, it might be predicted that T cells engineered with high-affinity TCRs are better effectors than T cells engineered with low-affinity TCRs. We and others have suggested that CD8 expression is only required for T cells with low-affinity TCRs [88–90]. The reliance on coreceptors, such as CD8, is one of the hallmarks contrasting TCRs with CARs. Various CD8-independent TCRs have been characterized that can transfer antigen recognition to CD4+ cells in an MHC-I-restricted manner [89–93]. Together, these studies suggest high-affinity TCRs allow for lower TCR transgene expression to achieve functionality, create novel populations of MHC-I-restricted CD4+ cells, and offer enhanced tumor regression. Naturally occurring high-affinity, CD8-independent TCRs are relatively rare, however, and thus difficult to find. Rather than screening for such high-affinity TCRs, various methods have been developed to affinity-enhanced already characterized TCRs, which are discussed in a later section. It is important to recognize, however, that higher-affinity TCRs hold much greater potential to undergo activation induced cell death (AICD) upon antigen encounter [94, 95], or induce “off-tumor, on-target” and “off-tumor, off-target” reactivity [96–98], counterproductive to their therapeutic intention.
It is also important to acknowledge that MHC restriction of TCRs limits the number of patients that can be treated using a single TCR, and engineered T cells would need to be HLA matched to patients. Because HLA class I expression has a tendency to be downregulated on tumor cells [99, 100], this may also serve as a barrier to effective therapy. Additionally, because TCRs require interaction with the CD3 complex, its expression and functionality are limited by available CD3 complex components. Competition for the CD3 complex with endogenous TCR limits functional transgene expression, although strategies discussed below may allow for improved surface competition for CD3 by the transgene receptor.
TCR pairing
As a heterodimer, TCRs also differ from CARs in that two chains need to be expressed rather than just one to redirect specificity, resulting in larger construct formation and potentially non-uniform chain expression. The addition of viral 2A self-cleavage peptide sequences between the α and β chains within the construct [101–103] and codon optimization of the construct [104, 105] are two examples that allow increased and more uniform TCR expression without altering the TCR sequence itself. The presence of endogenous TCR also allows for the opportunity of chain mispairing between endogenous and introduced α and β chains. These interactions reduce the level of expression of the introduced TCR [89, 106] and could lead to novel and unpredictable self-reactive TCRs with potential for serious adverse events.
Such “off-target, off-tumor” adverse events have been reported as a result of high-affinity TCR recognizing unanticipated epitopes or as a result of the phenomenon of TCR chain mispairing, generating novel self-reactive TCRs. Two recent studies demonstrate undesirable reactivity propagated from TCR mispairing between endogenous and introduced TCR α and β chains. One study observed graft-versus-host disease (GVHD) in a mouse model in five different TCR systems [107], and the other demonstrated the ability of engineered human T cells to develop MHC class I- and II-restricted allo- and auto-reactivity through mispairing [108]. However, to date, no evidence of GVHD has been seen in over 100 patients treated with this gene therapy approach [109].
The issue of TCR mispairing has been addressed in a variety of ways. One main strategic effort involves a host of modifications to the TCR construct summarized in Fig. 3. As mentioned before, codon optimization of the TCR α and β genes can help promote efficient translation and surface assembly of the introduced receptor without altering the TCR sequence itself [104, 105]. Introduction of cysteine residues in the α and β constant regions has been shown to promote inter-chain disulfide bridge formation to limit mispairing [110]. Other approaches to help improve pairing, expression, and function of the introduced TCRs include the addition of leucine zippers at the end of the intracellular tails [111] and altering the glycosylation of the TCR [112]. Substituting human constant regions with portions of or the entire mouse constant regions in the transgene also promotes proper pairing and enhanced surface expression [113–118]. It was observed that elements of the murine constant regions do not efficiently interact with the human constant regions [115]. Additionally, the murine constant region has a higher affinity for human CD3, which can favor the murinized receptor in competing for limited surface CD3 [113]. Receptors with murine constant regions were also found to mediate higher levels of cytokine secretion in vitro [113, 114], but this technique poses additional problems including evoking an immune response and possible clearance of the engineered T cells as they express potentially antigenic domains in the transgene [114].
TCR modifications to limit mispairing and improve cell surface expression and function. Modifications of wild-type TCR structure (far left) include codon optimization, introduction of a disulfide bridge, addition of leucine zipper, modification of glycosylated residues, substitution with murine constant regions, or use of single-chain Vα–Vβ–Cβ with a Cα chain
Another novel approach to alleviate mispairing was demonstrated by recent reports using single-chain TCRs. One group engineered a recombinant TCR consisting of a single-chain Vα–Vβ–Cβ and a Cα chain, which only paired with each other and not the endogenous TCR [115]. Other groups have used a stabilized Vα–Vβ single-chain TCR linked to intracellular signaling domains to elicit functional activation of T cells in the absence of coreceptors and to circumvent mispairing with endogenous TCRs [119, 120]. Efforts to limit mispairing also focus on altering the endogenous TCR by downregulation via small interfering RNA (siRNA) [121] or using designer zinc-finger nucleases [122]. All these alternate strategies share the same goal to reduce competition for the CD3 complex and allow for stable pairing of the introduced TCR.
TCR targets
More than 20 years after TCR gene-modified T cells were first used to redirect T cell specificity in mice [123], this technology was first evaluated in humans. TCR-engineered T cells’ first use in the clinic targeted HLA-A2+/MART-1+ melanoma [124, 125]. These initial clinical studies demonstrated that TCR gene-modified T cells were generally safe, well tolerated, and have the potential to be effective therapeutically in cancer patients. A later study targeting melanoma antigens MART-1 and gp100 demonstrated further clinical benefit using TCR-transduced T cells, while highlighting potential for adverse events [96]. Of note, the gp100-reactive TCR in this study was high affinity and of mouse origin, and many patients treated with this TCR exhibited toxicities in the eye and inner ear and displayed destruction of normal melanocytes. This well-characterized example of “on-target, off-tumor” effects first cautioned the use of high-affinity TCRs. Fortunately in this case such toxicities resolved naturally or with administration of topical steroids in almost all patients.
Since these early studies, identification of TCR genes encoded to recognize epitopes expressed by human tumors and improvements in TCR gene transfer technology has allowed for normal T cell antigen specificity redirection and targeting of a variety of antigens and malignancies, including carcinoembryonic antigen (CEA), cancer–testis antigen (CTA) family members, and viral protein family members.
CEA is overexpressed in many epithelial cancers, particularly in colorectal cancer. A recent clinical trial noted objective clinical response in a patient treated with high-affinity CEA-reactive T cells [98]. However, “on-target, off-tumor” adverse events, including inflammatory colitis, were documented in these patients.
The CTA family includes NY-ESO-1 and MAGE and is expressed by the normal testis and a panel of human cancers including that of breast, bladder, colon, lung, melanoma, head and neck, gastric, ovarian, thyroid, neuroblastoma, synovial cell sarcoma, and prostate. Clinical studies have shown T cells redirected to recognize NY-ESO-1 provided objective clinical response in patients with synovial cell sarcoma and melanoma without any evidence of previously reported adverse events [126].
A pair of clinical trials targeting widely expressed CTA, MAGE-A3, recorded much more mixed results. The first clinical trial used a mouse-derived, high-avidity TCR that was further modified by site-directed mutagenesis in the CDR3 region [127]. While targeting MAGE-A3, it was also reactive against MAGE-A9/A12. Although five out of nine patients experienced clinical regression of their cancers, one-third of the patients experienced neurological toxicity, and two patients died because of these adverse events. Unknown expression of MAGE-A12 in the brain is believed to be the cause of this toxicity.
Another clinical trial using an affinity-enhanced TCR targeting MAGE-A3 resulted in cardiogenic shock and death of the first two patients treated [128, 129]. While no MAGE-A3 expression was detected in cardiac tissue at autopsy, it was determined the TCR designed with affinity-enhancing mutations in the CDR2 regions exhibited an unpredicted cross-reactivity to titin, a sarcomeric protein expressed in striated muscle. Interestingly, the parental TCR from which the engineered TCR was derived from was isolated from a patient without cardiac toxicity, attributing the adverse events in the clinical trial to the intentionally induced CDR2 mutations. These mixed clinical results yield concern for use of such high-affinity receptors.
Virus-induced tumors can express members of a third family of antigens targeted by engineered T cells. Studies have engineered T cells to target antigens, such as CMV [130, 131], EBV [132–134], HIV [135–137], HCV [91–93, 138, 139], HPV [140, 141], and others. No clinical reports have yet been published testing virus-reactive TCR-transduced T cells in humans. Table 2 lists some of the active clinical trials using TCRs and their respective targets.
TCR summary
Overall, TCR-transduced T cells offer the ability to target a wide variety of self and non-self-targets through the normal biology of a T cell. Although MHC-restricted, dependent on coreceptors, and introduction of a second TCR causes potential for mispairing, great efforts are being made to better engineer high-affinity TCRs hope to enhance therapeutic efficacy while minimizing potential adverse events. Some success has been seen in clinical trials, and many are hopeful and greater objective clinical results will be observed in the future.
Other engineering approaches
Other receptor types
While CAR and TCR engineering have been well studied, ongoing efforts to design other receptor types for T cell engineering hold merit and clinical potential as well. For example, engineering T cells to express the NKG2D receptor allow T cells acquire the reactivity of natural killer (NK) cells [32–34]. Another NK cell receptor that has been investigated for T cell engineering is NKp30, which recognizes the tumor-prone antigen B7-H6. A recent study combined the specificity of NKp30 and the signaling capability of CARs, designing a novel NKp30-based CAR replacing the scFv domain with the ligand-binding domain of NKp30 [31]. Adoptive transfer of the NKp30-CAR allowed for non-MHC-restricted recognition of B7-H6-expressing RMA, a murine lymphoma, in vivo and interestingly provided protection against subsequent challenge with wild-type RMA tumor cells. Similar efforts are being made to examine potential for CAR-related therapy replacing the scFV domain with other ligands or ligand-binding receptors described earlier.
Another unique approach being investigated engineers dual-expressing T cells. In this way, T cells can coexpress complementary CARs, TCRs or other receptors, each specific to a distinct target. This approach is thought to optimize T cell homing and tumor specificity while reducing toxic potential. In this way, it would promote selective enhancement of T cell survival in the tumor microenvironment with synergistic signaling and provide a means to combat downregulation of antigen in tumor escape mechanisms. One study validated this tactic by generating T cells coexpressing CARs reactive to MUC1 and ErbB2 targeting breast cancer in vitro [142].
Additionally, recent work has demonstrated the design of anti-specific inhibitory chimeric antigen receptors (iCARs) linked to a powerful acute inhibitory signaling domain that can recognize T cell inhibitory molecules, such as CTLA-4 and PD-1, limiting T cell responsiveness even in the present of an engaged activating receptor [143]. This dual-receptor approach provides a means to curb unwanted off-target responses.
Cytokine production
Another approach to modify or enhance potency of receptor-engineered T cells is to further genetically modify the cells to secrete pro-inflammatory or pro-proliferative cytokines. This approach not only provides autocrine support to enhance T cell function, proliferation, and/or persistence, but also favorably alters the tumor microenvironment. This would allow for innate and cognate immune effector recruitment and limitation of the systemic toxicity of exogenously delivered cytokines in therapeutic approaches. For example, engineering melanoma-reactive T cells to express IL-2 resulted in continued cell growth in the absence of exogenous IL-2, which may a viable approach to help T cell persistence post-adoptive transfer [144]. A similar tactic using T cells modified to express IL-12 have exhibited enhanced anti-tumor function and were better able to resist immunosuppression by regulatory T cells [145, 146]. Similarly, engineering T cells to secrete IL-12 allowed transformation of myeloid cell within tumors from immunosuppressive to immunosupportive [147]. This strategy was even used in a recent phase I clinical trial where IL-12 secreting MUC-16(ecto)-targeting CAR-transduced T cells were infused into patients with recurrent ovarian cancer [148].
Chemokine recognition
In addition to cytokine-engineered T cells, modifying them to express chemokine receptors can aid in migration patterns, increasing the efficiency of trafficking to and infiltration of tumors. Transferring of genes encoding CCR4, CCR2B, or CXCR2 enables T cells to home toward CCL17, CXCL1, and macrophage chemoattractant proteins [73, 149, 150]. Also, VEGFR-2-engineered T cells allowed T cells to find tumor-associated neovasculature in one study [151]. Additional efforts to improve T cell homing may include engineering T cells with certain integrins or their ligands [152] or by blocking inhibitors of migration like endothelin [153].
Ways to improve
Although in vivo studies and clinical trials have shown great promise for engineered T cells as an effective immunotherapy for cancer, many efficacy and safety issues still prevent this treatment from becoming a standard of care. Efforts to pass these hurdles aim to allow the host to be most receptive to this kind of therapy, gain a better understanding of engineered receptors’ impact on the biology of the T cell, and optimize transgene engineering and expression. Some of these strategies are discussed here.
Host conditioning
Host conditioning prior to ACT has been a point of interest to better allow long-term persistence of function of transferred cells. This evidence came from preliminary mouse studies that were followed up in the clinic by the Rosenberg group. They first noted that persistence and anti-tumor activity of transferred T cells in vivo was greatly increased with non-myeloablative lymphodepleting treatment using cyclophosphamide and fludarabine before adoptive transfer [154]. Other conditioning regimens, including fludarabine only [155], or dacarbazine [156], have also been used in studies with improved clinical responses. Lymphodepletion is thought to create space for the transferred T cells and eliminate competition for cytokines [157], remove competition at the surfaces of antigen-presenting cells [158, 159], and remove immunosuppressive regulatory T cells [160]. It is believed these changes in the host may lead to induction of a memory phenotype and enhance effector function. Systemic administration of cytokines, such as IL-2 and IFNα, post-ACT has also enhanced transferred T cell function and persistence [7, 156, 161, 162]. Post-conditioning with other cytokines including IL-15 or immunomodulatory therapies such as PD-1 and CTLA-4 blockade should also be considered. However, the type of and need for host conditioning remain controversial as numerous studies have observed clinical responses even when no host conditioning was administered [163, 164].
Suicide switch
Given the capability for “on- or off-target” toxicities and well-documented tumor lysis syndrome and cytokine storm seen with the use of engineered T cells, it would be beneficial to preserve the ability to eradicate the transferred T cells, if needed. Such strategies aim at turning off antigen receptor expression or eliminating engineered cells after transfer by incorporating certain “suicide genes” into the transgene. A long-studied approach in cell therapy investigations utilizes the herpes simplex virus thymidine kinase (HSV-tk) gene. Its incorporation into the transgene vector makes engineered T cells susceptible to ganciclovir treatment [165, 166]. However, because HSV-tk is potentially immunogenic, its expression may create unwanted immune-mediated destruction of transferred T cells and decreased persistence [167, 168]. Another common approach and non-immunogenic technique incorporate caspase 9 under an inducible promoter (iC9) to initiate apoptosis of transduced cells [169–172]. Additionally, studies incorporating CD20 [173] or EGFR [174] in transgene vectors generated transduced cell susceptible to rituximab and cetuximab treatments, respectively.
Affinity modulation
As discussed earlier, TCR affinity is known to play a significant role in determining sensitivity of a T cell to antigen recognition. Thus, it is logical to think that higher-affinity TCRs may provide a better therapeutic candidate. Altering the affinity of the TCR may better equip engineered T cells to combat immune suppression mechanisms that alter T cell function including MDSC-mediated nitration of TCR tyrosine residues which can weaken TCR-pMHC binding [175]. Additionally, high-affinity TCRs oftentimes exhibit CD8 independence, meaning T cells equipped these receptors can recognize their tumor target without CD8’s stabilization of the TCR–pMHC complex. This would allow for the generation of tumor-reactive MHC class I-restricted CD4+ T cells, allowing for production of helper cytokines upon antigen stimulation and a novel population of T cell help at the tumor site [90, 176, 177]. Moreover, a population of reactive CD4+ T cells may facilitate cross-priming or epitope spreading allowing for a broad systemic anti-tumor response.
One challenge in identifying tumor-reactive high-affinity TCRs is their inherent low frequency in patients. During T cell maturation and thymic selection, TCRs whose affinity for the host antigen/MHC is too low (death by neglect) or too high (negative selection) are eliminated from the pool of mature T cells [178]. This selection process often restricts the amount of high-affinity, self-reactive TCRs from existing in the periphery, thus limiting the discovery for high-affinity TCRs in tumor-bearing patients.
One way to identify and clone high-affinity TCRs is screening for CD8 independence against human MHC-restricted antigens in mice. It is documented that mouse CD8 does not bind to the α3 domain of human MHC class I molecules [113, 179]. Thus, in a vaccinated HLA-A2 transgenic mouse model, isolated T cell clones reactive against human tumors in vitro would likely express high-affinity TCRs. This approach has been used successfully to identify high-affinity TCRs targeting CEA [180] and p53 [181]. Additionally, TCRs have also been genetically modified to improve their biophysical properties using yeast and phage display [182–184], a technique also used in CAR design [13, 14]. Interestingly, these modified receptors can have amino acid alterations in any of three CDR regions that can contribute to enhanced TCR-pMHC affinities, not only in the CDR3 region which is responsible for the majority of TCR diversity and specificity [185].
These methods in selecting for or enhancing receptor affinity, however, may not necessarily lead to a better therapeutic. As already pointed out, it is well documented that T cells equipped with extremely high-affinity TCRs can undergo AICD, which would selectively delete the effector cells intended for therapeutic benefit [94, 95]. Additionally, two clinical trials [96, 98] and a transgenic mouse model [97] have documented autoimmunity with high-affinity TCR-engineered cells. Taken together, these observations indicate that TCR affinity can make a difference in target recognition by TCR-transduced T cells, but the question of the need to use a high-affinity TCR for effective anti-tumor immunity remains unresolved.
Conclusions
The potential for engineering T cells for immunotherapy seems limitless. Specifically targeting tumor antigens with autologous T cells is a powerful and attractive strategy for cancer therapy. While clinical trials have had initial success, there still remain many issues in optimizing efficacy and safety of this type of immunotherapy. Additionally, the design and implementation of genetically engineered T cells are often constrained by regulatory authorities in both the USA and Europe, largely influencing the feasibility of generating effective and safe CAR T cells [186–188]. Ultimately, more extensive studies are needed to determine whether this type of therapy can deliver improvements in progression-free and overall survival when compared to the standard of care.
Abbreviations
- ACT:
-
Adoptive cell transfer
- AICD:
-
Activation-induced cell death
- B-ALL:
-
Acute B lymphoblastic leukemia
- CAIX:
-
Carbonic anhydrase IX
- CEA:
-
Carcinoembryonic antigen
- CLL:
-
Chronic lymphocytic leukemia
- CTA:
-
Cancer–testis antigen
- FBP:
-
Folate-binding protein
- HSV-tk:
-
Herpes simplex virus thymidine kinase
- iC9:
-
Inducible caspase 9
- iCAR:
-
Inhibitory chimeric antigen receptor
- NHL:
-
Non-Hodgkin lymphoma
- pMHC:
-
Peptide–major histocompatibility complex
- RCC:
-
Renal cell carcinoma
- siRNA:
-
Small interfering ribonucleic acid
References
Mule JJ, Shu S, Schwarz SL, Rosenberg SA (1984) Adoptive immunotherapy of established pulmonary metastases with LAK cells and recombinant interleukin-2. Science 225(4669):1487–1489
Dudley ME, Wunderlich JR, Robbins PF, Yang JC, Hwu P, Schwartzentruber DJ, Topalian SL, Sherry R, Restifo NP, Hubicki AM, Robinson MR, Raffeld M, Duray P, Seipp CA, Rogers-Freezer L, Morton KE, Mavroukakis SA, White DE, Rosenberg SA (2002) Cancer regression and autoimmunity in patients after clonal repopulation with antitumor lymphocytes. Science 298(5594):850–854. doi:10.1126/science.1076514
Rosenberg SA, Yannelli JR, Yang JC, Topalian SL, Schwartzentruber DJ, Weber JS, Parkinson DR, Seipp CA, Einhorn JH, White DE (1994) Treatment of patients with metastatic melanoma with autologous tumor-infiltrating lymphocytes and interleukin 2. J Natl Cancer Inst 86(15):1159–1166
Dudley ME, Wunderlich J, Nishimura MI, Yu D, Yang JC, Topalian SL, Schwartzentruber DJ, Hwu P, Marincola FM, Sherry R, Leitman SF, Rosenberg SA (2001) Adoptive transfer of cloned melanoma-reactive T lymphocytes for the treatment of patients with metastatic melanoma. J Immunother 24(4):363–373
Mackensen A, Meidenbauer N, Vogl S, Laumer M, Berger J, Andreesen R (2006) Phase I study of adoptive T-cell therapy using antigen-specific CD8+ T cells for the treatment of patients with metastatic melanoma. J Clin Oncol 24(31):5060–5069. doi:10.1200/jco.2006.07.1100
Vignard V, Lemercier B, Lim A, Pandolfino MC, Guilloux Y, Khammari A, Rabu C, Echasserieau K, Lang F, Gougeon ML, Dreno B, Jotereau F, Labarriere N (2005) Adoptive transfer of tumor-reactive Melan-A-specific CTL clones in melanoma patients is followed by increased frequencies of additional Melan-A-specific T cells. J Immunol 175(7):4797–4805
Yee C, Thompson JA, Byrd D, Riddell SR, Roche P, Celis E, Greenberg PD (2002) Adoptive T cell therapy using antigen-specific CD8+ T cell clones for the treatment of patients with metastatic melanoma: in vivo persistence, migration, and antitumor effect of transferred T cells. Proc Natl Acad Sci USA 99(25):16168–16173. doi:10.1073/pnas.242600099
Muul LM, Spiess PJ, Director EP, Rosenberg SA (1987) Identification of specific cytolytic immune responses against autologous tumor in humans bearing malignant melanoma. J Immunol 138(3):989–995
Rosenberg SA, Spiess P, Lafreniere R (1986) A new approach to the adoptive immunotherapy of cancer with tumor-infiltrating lymphocytes. Science 233(4770):1318–1321
Rosenberg SA, Packard BS, Aebersold PM, Solomon D, Topalian SL, Toy ST, Simon P, Lotze MT, Yang JC, Seipp CA et al (1988) Use of tumor-infiltrating lymphocytes and interleukin-2 in the immunotherapy of patients with metastatic melanoma. A preliminary report. N Engl J Med 319(25):1676–1680. doi:10.1056/nejm198812223192527
Gross G, Waks T, Eshhar Z (1989) Expression of immunoglobulin-T-cell receptor chimeric molecules as functional receptors with antibody-type specificity. Proc Natl Acad Sci USA 86(24):10024–10028
Letourneur F, Klausner RD (1991) T-cell and basophil activation through the cytoplasmic tail of T-cell-receptor zeta family proteins. Proc Natl Acad Sci USA 88(20):8905–8909
Hombach A, Heuser C, Sircar R, Tillmann T, Diehl V, Kruis W, Pohl C, Abken H (1997) T cell targeting of TAG72+ tumor cells by a chimeric receptor with antibody-like specificity for a carbohydrate epitope. Gastroenterology 113(4):1163–1170
Rossig C, Bollard CM, Nuchtern JG, Merchant DA, Brenner MK (2001) Targeting of G(D2)-positive tumor cells by human T lymphocytes engineered to express chimeric T-cell receptor genes. Int J Cancer 94(2):228–236
Inaguma Y, Akahori Y, Murayama Y, Shiraishi K, Tsuzuki-Iba S, Endoh A, Tsujikawa J, Demachi-Okamura A, Hiramatsu K, Saji H, Yamamoto Y, Yamamoto N, Nishimura Y, Takahashi T, Kuzushima K, Emi N, Akatsuka Y (2014) Construction and molecular characterization of a T-cell receptor-like antibody and CAR-T cells specific for minor histocompatibility antigen HA-1H. Gene Ther 21(6):575–584. doi:10.1038/gt.2014.30
Reiter Y, Di Carlo A, Fugger L, Engberg J, Pastan I (1997) Peptide-specific killing of antigen-presenting cells by a recombinant antibody-toxin fusion protein targeted to major histocompatibility complex/peptide class I complexes with T cell receptor-like specificity. Proc Natl Acad Sci USA 94(9):4631–4636
Sergeeva A, Alatrash G, He H, Ruisaard K, Lu S, Wygant J, McIntyre BW, Ma Q, Li D, St John L, Clise-Dwyer K, Molldrem JJ (2011) An anti-PR1/HLA-A2 T-cell receptor-like antibody mediates complement-dependent cytotoxicity against acute myeloid leukemia progenitor cells. Blood 117(16):4262–4272. doi:10.1182/blood-2010-07-299248
Willemsen RA, Ronteltap C, Chames P, Debets R, Bolhuis RL (2005) T cell retargeting with MHC class I-restricted antibodies: the CD28 costimulatory domain enhances antigen-specific cytotoxicity and cytokine production. J Immunol 174(12):7853–7858
Sadelain M, Brentjens R, Riviere I (2009) The promise and potential pitfalls of chimeric antigen receptors. Curr Opin Immunol 21(2):215–223. doi:10.1016/j.coi.2009.02.009
Gardner R, Wu D, Cherian S, Fang M, Hanafi LA, Finney O, Smithers H, Jensen MC, Riddell SR, Maloney DG, Turtle CJ (2016) Acquisition of a CD19 negative myeloid phenotype allows immune escape of MLL-rearranged B-ALL from CD19 CAR-T cell therapy. Blood. doi:10.1182/blood-2015-08-665547
Grupp SA, Kalos M, Barrett D, Aplenc R, Porter DL, Rheingold SR, Teachey DT, Chew A, Hauck B, Wright JF, Milone MC, Levine BL, June CH (2013) Chimeric antigen receptor-modified T cells for acute lymphoid leukemia. N Engl J Med 368(16):1509–1518. doi:10.1056/NEJMoa1215134
Burga RA, Thorn M, Point GR, Guha P, Nguyen CT, Licata LA, DeMatteo RP, Ayala A, Joseph Espat N, Junghans RP, Katz SC (2015) Liver myeloid-derived suppressor cells expand in response to liver metastases in mice and inhibit the anti-tumor efficacy of anti-CEA CAR-T. Cancer Immunol Immunother 64(7):817–829. doi:10.1007/s00262-015-1692-6
Davis MM (2004) The evolutionary and structural ‘logic’ of antigen receptor diversity. Semin Immunol 16(4):239–243. doi:10.1016/j.smim.2004.08.003
Krug C, Birkholz K, Paulus A, Schwenkert M, Schmidt P, Hoffmann N, Hombach A, Fey G, Abken H, Schuler G, Schuler-Thurner B, Dorrie J, Schaft N (2015) Stability and activity of MCSP-specific chimeric antigen receptors (CARs) depend on the scFv antigen-binding domain and the protein backbone. Cancer Immunol Immunother 64(12):1623–1635. doi:10.1007/s00262-015-1767-4
Lamers CH, Willemsen R, van Elzakker P, van Steenbergen-Langeveld S, Broertjes M, Oosterwijk-Wakka J, Oosterwijk E, Sleijfer S, Debets R, Gratama JW (2011) Immune responses to transgene and retroviral vector in patients treated with ex vivo-engineered T cells. Blood 117(1):72–82. doi:10.1182/blood-2010-07-294520
Casucci M, Hawkins RE, Dotti G, Bondanza A (2015) Overcoming the toxicity hurdles of genetically targeted T cells. Cancer Immunol Immunother 64(1):123–130. doi:10.1007/s00262-014-1641-9
Dao T, Yan S, Veomett N, Pankov D, Zhou L, Korontsvit T, Scott A, Whitten J, Maslak P, Casey E, Tan T, Liu H, Zakhaleva V, Curcio M, Doubrovina E, O’Reilly RJ, Liu C, Scheinberg DA (2013) Targeting the intracellular WT1 oncogene product with a therapeutic human antibody. Sci Transl Med 5(176):176ra133. doi:10.1126/scitranslmed.3005661
June CH, Maus MV, Plesa G, Johnson LA, Zhao Y, Levine BL, Grupp SA, Porter DL (2014) Engineered T cells for cancer therapy. Cancer Immunol Immunother 63(9):969–975. doi:10.1007/s00262-014-1568-1
Muniappan A, Banapour B, Lebkowski J, Talib S (2000) Ligand-mediated cytolysis of tumor cells: use of heregulin-zeta chimeras to redirect cytotoxic T lymphocytes. Cancer Gene Ther 7(1):128–134. doi:10.1038/sj.cgt.7700100
Niederman TM, Ghogawala Z, Carter BS, Tompkins HS, Russell MM, Mulligan RC (2002) Antitumor activity of cytotoxic T lymphocytes engineered to target vascular endothelial growth factor receptors. Proc Natl Acad Sci USA 99(10):7009–7014. doi:10.1073/pnas.092562399
Zhang T, Wu MR, Sentman CL (2012) An NKp30-based chimeric antigen receptor promotes T cell effector functions and antitumor efficacy in vivo. J Immunol 189(5):2290–2299. doi:10.4049/jimmunol.1103495
Lehner M, Gotz G, Proff J, Schaft N, Dorrie J, Full F, Ensser A, Muller YA, Cerwenka A, Abken H, Parolini O, Ambros PF, Kovar H, Holter W (2012) Redirecting T cells to Ewing’s sarcoma family of tumors by a chimeric NKG2D receptor expressed by lentiviral transduction or mRNA transfection. PLoS ONE 7(2):e31210. doi:10.1371/journal.pone.0031210
Song DG, Ye Q, Santoro S, Fang C, Best A, Powell DJ Jr (2013) Chimeric NKG2D CAR-expressing T cell-mediated attack of human ovarian cancer is enhanced by histone deacetylase inhibition. Hum Gene Ther 24(3):295–305. doi:10.1089/hum.2012.143
Zhang T, Barber A, Sentman CL (2006) Generation of antitumor responses by genetic modification of primary human T cells with a chimeric NKG2D receptor. Cancer Res 66(11):5927–5933. doi:10.1158/0008-5472.can-06-0130
Ramos CA, Dotti G (2011) Chimeric antigen receptor (CAR)-engineered lymphocytes for cancer therapy. Expert Opin Biol Ther 11(7):855–873. doi:10.1517/14712598.2011.573476
Carpenito C, Milone MC, Hassan R, Simonet JC, Lakhal M, Suhoski MM, Varela-Rohena A, Haines KM, Heitjan DF, Albelda SM, Carroll RG, Riley JL, Pastan I, June CH (2009) Control of large, established tumor xenografts with genetically retargeted human T cells containing CD28 and CD137 domains. Proc Natl Acad Sci USA 106(9):3360–3365. doi:10.1073/pnas.0813101106
Haynes NM, Trapani JA, Teng MW, Jackson JT, Cerruti L, Jane SM, Kershaw MH, Smyth MJ, Darcy PK (2002) Single-chain antigen recognition receptors that costimulate potent rejection of established experimental tumors. Blood 100(9):3155–3163. doi:10.1182/blood-2002-04-1041
Hombach A, Wieczarkowiecz A, Marquardt T, Heuser C, Usai L, Pohl C, Seliger B, Abken H (2001) Tumor-specific T cell activation by recombinant immunoreceptors: CD3 zeta signaling and CD28 costimulation are simultaneously required for efficient IL-2 secretion and can be integrated into one combined CD28/CD3 zeta signaling receptor molecule. J Immunol 167(11):6123–6131
Maher J, Brentjens RJ, Gunset G, Riviere I, Sadelain M (2002) Human T-lymphocyte cytotoxicity and proliferation directed by a single chimeric TCRzeta/CD28 receptor. Nat Biotechnol 20(1):70–75. doi:10.1038/nbt0102-70
Milone MC, Fish JD, Carpenito C, Carroll RG, Binder GK, Teachey D, Samanta M, Lakhal M, Gloss B, Danet-Desnoyers G, Campana D, Riley JL, Grupp SA, June CH (2009) Chimeric receptors containing CD137 signal transduction domains mediate enhanced survival of T cells and increased antileukemic efficacy in vivo. Mol Ther 17(8):1453–1464. doi:10.1038/mt.2009.83
Moeller M, Haynes NM, Trapani JA, Teng MW, Jackson JT, Tanner JE, Cerutti L, Jane SM, Kershaw MH, Smyth MJ, Darcy PK (2004) A functional role for CD28 costimulation in tumor recognition by single-chain receptor-modified T cells. Cancer Gene Ther 11(5):371–379. doi:10.1038/sj.cgt.7700710
Yvon E, Del Vecchio M, Savoldo B, Hoyos V, Dutour A, Anichini A, Dotti G, Brenner MK (2009) Immunotherapy of metastatic melanoma using genetically engineered GD2-specific T cells. Clin Cancer Res 15(18):5852–5860. doi:10.1158/1078-0432.ccr-08-3163
Wang J, Jensen M, Lin Y, Sui X, Chen E, Lindgren CG, Till B, Raubitschek A, Forman SJ, Qian X, James S, Greenberg P, Riddell S, Press OW (2007) Optimizing adoptive polyclonal T cell immunotherapy of lymphomas, using a chimeric T cell receptor possessing CD28 and CD137 costimulatory domains. Hum Gene Ther 18(8):712–725. doi:10.1089/hum.2007.028
Liu L, Sun M, Wang Z (2012) Adoptive T-cell therapy of B-cell malignancies: conventional and physiological chimeric antigen receptors. Cancer Lett 316(1):1–5. doi:10.1016/j.canlet.2011.10.027
Wang J, Press OW, Lindgren CG, Greenberg P, Riddell S, Qian X, Laugen C, Raubitschek A, Forman SJ, Jensen MC (2004) Cellular immunotherapy for follicular lymphoma using genetically modified CD20-specific CD8+ cytotoxic T lymphocytes. Mol Ther 9(4):577–586. doi:10.1016/j.ymthe.2003.12.011
Wilkie S, Picco G, Foster J, Davies DM, Julien S, Cooper L, Arif S, Mather SJ, Taylor-Papadimitriou J, Burchell JM, Maher J (2008) Retargeting of human T cells to tumor-associated MUC1: the evolution of a chimeric antigen receptor. J Immunol 180(7):4901–4909
Zhao Y, Wang QJ, Yang S, Kochenderfer JN, Zheng Z, Zhong X, Sadelain M, Eshhar Z, Rosenberg SA, Morgan RA (2009) A herceptin-based chimeric antigen receptor with modified signaling domains leads to enhanced survival of transduced T lymphocytes and antitumor activity. J Immunol 183(9):5563–5574. doi:10.4049/jimmunol.0900447
Zhong XS, Matsushita M, Plotkin J, Riviere I, Sadelain M (2010) Chimeric antigen receptors combining 4-1BB and CD28 signaling domains augment PI3kinase/AKT/Bcl-XL activation and CD8+ T cell-mediated tumor eradication. Mol Ther 18(2):413–420. doi:10.1038/mt.2009.210
Morgan RA, Yang JC, Kitano M, Dudley ME, Laurencot CM, Rosenberg SA (2010) Case report of a serious adverse event following the administration of T cells transduced with a chimeric antigen receptor recognizing ERBB2. Mol Ther 18(4):843–851. doi:10.1038/mt.2010.24
Kershaw MH, Westwood JA, Parker LL, Wang G, Eshhar Z, Mavroukakis SA, White DE, Wunderlich JR, Canevari S, Rogers-Freezer L, Chen CC, Yang JC, Rosenberg SA, Hwu P (2006) A phase I study on adoptive immunotherapy using gene-modified T cells for ovarian cancer. Clin Cancer Res 12(20 Pt 1):6106–6115. doi:10.1158/1078-0432.ccr-06-1183
Lamers CH, Sleijfer S, Vulto AG, Kruit WH, Kliffen M, Debets R, Gratama JW, Stoter G, Oosterwijk E (2006) Treatment of metastatic renal cell carcinoma with autologous T-lymphocytes genetically retargeted against carbonic anhydrase IX: first clinical experience. J Clin Oncol 24(13):e20–e22. doi:10.1200/jco.2006.05.9964
Brentjens RJ, Riviere I, Park JH, Davila ML, Wang X, Stefanski J, Taylor C, Yeh R, Bartido S, Borquez-Ojeda O, Olszewska M, Bernal Y, Pegram H, Przybylowski M, Hollyman D, Usachenko Y, Pirraglia D, Hosey J, Santos E, Halton E, Maslak P, Scheinberg D, Jurcic J, Heaney M, Heller G, Frattini M, Sadelain M (2011) Safety and persistence of adoptively transferred autologous CD19-targeted T cells in patients with relapsed or chemotherapy refractory B-cell leukemias. Blood 118(18):4817–4828. doi:10.1182/blood-2011-04-348540
Jensen MC, Popplewell L, Cooper LJ, DiGiusto D, Kalos M, Ostberg JR, Forman SJ (2010) Antitransgene rejection responses contribute to attenuated persistence of adoptively transferred CD20/CD19-specific chimeric antigen receptor redirected T cells in humans. Biol Blood Marrow Transplant 16(9):1245–1256. doi:10.1016/j.bbmt.2010.03.014
Kalos M, Levine BL, Porter DL, Katz S, Grupp SA, Bagg A, June CH (2011) T cells with chimeric antigen receptors have potent antitumor effects and can establish memory in patients with advanced leukemia. Sci Transl Med 3(95):95ra73. doi:10.1126/scitranslmed.3002842
Kochenderfer JN, Dudley ME, Feldman SA, Wilson WH, Spaner DE, Maric I, Stetler-Stevenson M, Phan GQ, Hughes MS, Sherry RM, Yang JC, Kammula US, Devillier L, Carpenter R, Nathan DA, Morgan RA, Laurencot C, Rosenberg SA (2012) B-cell depletion and remissions of malignancy along with cytokine-associated toxicity in a clinical trial of anti-CD19 chimeric-antigen-receptor-transduced T cells. Blood 119(12):2709–2720. doi:10.1182/blood-2011-10-384388
Kochenderfer JN, Wilson WH, Janik JE, Dudley ME, Stetler-Stevenson M, Feldman SA, Maric I, Raffeld M, Nathan DA, Lanier BJ, Morgan RA, Rosenberg SA (2010) Eradication of B-lineage cells and regression of lymphoma in a patient treated with autologous T cells genetically engineered to recognize CD19. Blood 116(20):4099–4102. doi:10.1182/blood-2010-04-281931
Porter DL, Levine BL, Kalos M, Bagg A, June CH (2011) Chimeric antigen receptor-modified T cells in chronic lymphoid leukemia. N Engl J Med 365(8):725–733. doi:10.1056/NEJMoa1103849
Savoldo B, Ramos CA, Liu E, Mims MP, Keating MJ, Carrum G, Kamble RT, Bollard CM, Gee AP, Mei Z, Liu H, Grilley B, Rooney CM, Heslop HE, Brenner MK, Dotti G (2011) CD28 costimulation improves expansion and persistence of chimeric antigen receptor-modified T cells in lymphoma patients. J Clin Invest 121(5):1822–1826. doi:10.1172/jci46110
Brentjens RJ, Davila ML, Riviere I, Park J, Wang X, Cowell LG, Bartido S, Stefanski J, Taylor C, Olszewska M, Borquez-Ojeda O, Qu J, Wasielewska T, He Q, Bernal Y, Rijo IV, Hedvat C, Kobos R, Curran K, Steinherz P, Jurcic J, Rosenblat T, Maslak P, Frattini M, Sadelain M (2013) CD19-targeted T cells rapidly induce molecular remissions in adults with chemotherapy-refractory acute lymphoblastic leukemia. Sci Transl Med 5(177):177ra138. doi:10.1126/scitranslmed.3005930
Lee DW, Kochenderfer JN, Stetler-Stevenson M, Cui YK, Delbrook C, Feldman SA, Fry TJ, Orentas R, Sabatino M, Shah NN, Steinberg SM, Stroncek D, Tschernia N, Yuan C, Zhang H, Zhang L, Rosenberg SA, Wayne AS, Mackall CL (2015) T cells expressing CD19 chimeric antigen receptors for acute lymphoblastic leukaemia in children and young adults: a phase 1 dose-escalation trial. Lancet 385(9967):517–528. doi:10.1016/s0140-6736(14)61403-3
Ahmed N, Brawley VS, Hegde M, Robertson C, Ghazi A, Gerken C, Liu E, Dakhova O, Ashoori A, Corder A, Gray T, Wu MF, Liu H, Hicks J, Rainusso N, Dotti G, Mei Z, Grilley B, Gee A, Rooney CM, Brenner MK, Heslop HE, Wels WS, Wang LL, Anderson P, Gottschalk S (2015) Human Epidermal Growth Factor Receptor 2 (HER2)-Specific Chimeric Antigen Receptor-Modified T Cells for the Immunotherapy of HER2-Positive Sarcoma. J Clin Oncol 33(15):1688–1696. doi:10.1200/jco.2014.58.0225
Miao H, Choi BD, Suryadevara CM, Sanchez-Perez L, Yang S, De Leon G, Sayour EJ, McLendon R, Herndon JE II, Healy P, Archer GE, Bigner DD, Johnson LA, Sampson JH (2014) EGFRvIII-specific chimeric antigen receptor T cells migrate to and kill tumor deposits infiltrating the brain parenchyma in an invasive xenograft model of glioblastoma. PLoS ONE 9(4):e94281. doi:10.1371/journal.pone.0094281
Brentjens RJ, Latouche JB, Santos E, Marti F, Gong MC, Lyddane C, King PD, Larson S, Weiss M, Riviere I, Sadelain M (2003) Eradication of systemic B-cell tumors by genetically targeted human T lymphocytes co-stimulated by CD80 and interleukin-15. Nat Med 9(3):279–286. doi:10.1038/nm827
Rossig C, Bollard CM, Nuchtern JG, Rooney CM, Brenner MK (2002) Epstein-Barr virus-specific human T lymphocytes expressing antitumor chimeric T-cell receptors: potential for improved immunotherapy. Blood 99(6):2009–2016
Lo AS, Ma Q, Liu DL, Junghans RP (2010) Anti-GD3 chimeric sFv-CD28/T-cell receptor zeta designer T cells for treatment of metastatic melanoma and other neuroectodermal tumors. Clin Cancer Res 16(10):2769–2780. doi:10.1158/1078-0432.ccr-10-0043
Yun CO, Nolan KF, Beecham EJ, Reisfeld RA, Junghans RP (2000) Targeting of T lymphocytes to melanoma cells through chimeric anti-GD3 immunoglobulin T-cell receptors. Neoplasia (New York, NY) 2(5):449–459
Burns WR, Zhao Y, Frankel TL, Hinrichs CS, Zheng Z, Xu H, Feldman SA, Ferrone S, Rosenberg SA, Morgan RA (2010) A high molecular weight melanoma-associated antigen-specific chimeric antigen receptor redirects lymphocytes to target human melanomas. Cancer Res 70(8):3027–3033. doi:10.1158/0008-5472.can-09-2824
James SE, Greenberg PD, Jensen MC, Lin Y, Wang J, Till BG, Raubitschek AA, Forman SJ, Press OW (2008) Antigen sensitivity of CD22-specific chimeric TCR is modulated by target epitope distance from the cell membrane. J Immunol 180(10):7028–7038
Jensen MC, Cooper LJ, Wu AM, Forman SJ, Raubitschek A (2003) Engineered CD20-specific primary human cytotoxic T lymphocytes for targeting B-cell malignancy. Cytotherapy 5(2):131–138. doi:10.1080/14653240310001028
Till BG, Jensen MC, Wang J, Qian X, Gopal AK, Maloney DG, Lindgren CG, Lin Y, Pagel JM, Budde LE, Raubitschek A, Forman SJ, Greenberg PD, Riddell SR, Press OW (2012) CD20-specific adoptive immunotherapy for lymphoma using a chimeric antigen receptor with both CD28 and 4-1BB domains: pilot clinical trial results. Blood 119(17):3940–3950. doi:10.1182/blood-2011-10-387969
Yu K, Hu Y, Tan Y, Shen Z, Jiang S, Qian H, Liang B, Shan D (2008) Immunotherapy of lymphomas with T cells modified by anti-CD20 scFv/CD28/CD3zeta recombinant gene. Leuk Lymphoma 49(7):1368–1373. doi:10.1080/10428190802064958
Giordano Attianese GM, Marin V, Hoyos V, Savoldo B, Pizzitola I, Tettamanti S, Agostoni V, Parma M, Ponzoni M, Bertilaccio MT, Ghia P, Biondi A, Dotti G, Biagi E (2011) In vitro and in vivo model of a novel immunotherapy approach for chronic lymphocytic leukemia by anti-CD23 chimeric antigen receptor. Blood 117(18):4736–4745. doi:10.1182/blood-2010-10-311845
Di Stasi A, De Angelis B, Rooney CM, Zhang L, Mahendravada A, Foster AE, Heslop HE, Brenner MK, Dotti G, Savoldo B (2009) T lymphocytes coexpressing CCR4 and a chimeric antigen receptor targeting CD30 have improved homing and antitumor activity in a Hodgkin tumor model. Blood 113(25):6392–6402. doi:10.1182/blood-2009-03-209650
Hombach A, Muche JM, Gerken M, Gellrich S, Heuser C, Pohl C, Sterry W, Abken H (2001) T cells engrafted with a recombinant anti-CD30 receptor target autologous CD30(+) cutaneous lymphoma cells. Gene Ther 8(11):891–895. doi:10.1038/sj.gt.3301467
Savoldo B, Rooney CM, Di Stasi A, Abken H, Hombach A, Foster AE, Zhang L, Heslop HE, Brenner MK, Dotti G (2007) Epstein Barr virus specific cytotoxic T lymphocytes expressing the anti-CD30zeta artificial chimeric T-cell receptor for immunotherapy of Hodgkin disease. Blood 110(7):2620–2630. doi:10.1182/blood-2006-11-059139
Ma Q, Safar M, Holmes E, Wang Y, Boynton AL, Junghans RP (2004) Anti-prostate specific membrane antigen designer T cells for prostate cancer therapy. Prostate 61(1):12–25. doi:10.1002/pros.20073
Moritz D, Wels W, Mattern J, Groner B (1994) Cytotoxic T lymphocytes with a grafted recognition specificity for ERBB2-expressing tumor cells. Proc Natl Acad Sci USA 91(10):4318–4322
Stancovski I, Schindler DG, Waks T, Yarden Y, Sela M, Eshhar Z (1993) Targeting of T lymphocytes to Neu/HER2-expressing cells using chimeric single chain Fv receptors. J Immunol 151(11):6577–6582
Darcy PK, Kershaw MH, Trapani JA, Smyth MJ (1998) Expression in cytotoxic T lymphocytes of a single-chain anti-carcinoembryonic antigen antibody. Redirected Fas ligand-mediated lysis of colon carcinoma. Eur J Immunol 28(5):1663–1672. doi:10.1002/(sici)1521-4141(199805)28:05<1663:aid-immu1663>3.0.co;2-l
Hombach A, Koch D, Sircar R, Heuser C, Diehl V, Kruis W, Pohl C, Abken H (1999) A chimeric receptor that selectively targets membrane-bound carcinoembryonic antigen (mCEA) in the presence of soluble CEA. Gene Ther 6(2):300–304. doi:10.1038/sj.gt.3300813
Nolan KF, Yun CO, Akamatsu Y, Murphy JC, Leung SO, Beecham EJ, Junghans RP (1999) Bypassing immunization: optimized design of “designer T cells” against carcinoembryonic antigen (CEA)-expressing tumors, and lack of suppression by soluble CEA. Clin Cancer Res 5(12):3928–3941
Daly T, Royal RE, Kershaw MH, Treisman J, Wang G, Li W, Herlyn D, Eshhar Z, Hwu P (2000) Recognition of human colon cancer by T cells transduced with a chimeric receptor gene. Cancer Gene Ther 7(2):284–291. doi:10.1038/sj.cgt.7700121
Chinnasamy D, Yu Z, Theoret MR, Zhao Y, Shrimali RK, Morgan RA, Feldman SA, Restifo NP, Rosenberg SA (2010) Gene therapy using genetically modified lymphocytes targeting VEGFR-2 inhibits the growth of vascularized syngenic tumors in mice. J Clin Invest 120(11):3953–3968. doi:10.1172/jci43490
Wang S, Yin ZF, Cui ZF, Wu ZD, Qian HH, Kang XY, Wu MC (2004) The specific cytotoxic effect of tumor infiltrating lymphocytes transfected with chimeric T cell receptor on cells which express KDR. Zhonghua Zhong Liu Za Zhi 26(2):82–84
Chekmasova AA, Rao TD, Nikhamin Y, Park KJ, Levine DA, Spriggs DR, Brentjens RJ (2010) Successful eradication of established peritoneal ovarian tumors in SCID-Beige mice following adoptive transfer of T cells genetically targeted to the MUC16 antigen. Clin Cancer Res 16(14):3594–3606. doi:10.1158/1078-0432.ccr-10-0192
Brentjens R, Yeh R, Bernal Y, Riviere I, Sadelain M (2010) Treatment of chronic lymphocytic leukemia with genetically targeted autologous T cells: case report of an unforeseen adverse event in a phase I clinical trial. Mol Ther 18(4):666–668. doi:10.1038/mt.2010.31
Xu XJ, Tang YM (2014) Cytokine release syndrome in cancer immunotherapy with chimeric antigen receptor engineered T cells. Cancer Lett 343(2):172–178. doi:10.1016/j.canlet.2013.10.004
Clay TM, Custer MC, Sachs J, Hwu P, Rosenberg SA, Nishimura MI (1999) Efficient transfer of a tumor antigen-reactive TCR to human peripheral blood lymphocytes confers anti-tumor reactivity. J Immunol 163(1):507–513
Cole DJ, Weil DP, Shilyansky J, Custer M, Kawakami Y, Rosenberg SA, Nishimura MI (1995) Characterization of the functional specificity of a cloned T-cell receptor heterodimer recognizing the MART-1 melanoma antigen. Cancer Res 55(4):748–752
Roszkowski JJ, Lyons GE, Kast WM, Yee C, Van Besien K, Nishimura MI (2005) Simultaneous generation of CD8+ and CD4+ melanoma-reactive T cells by retroviral-mediated transfer of a single T-cell receptor. Cancer Res 65(4):1570–1576. doi:10.1158/0008-5472.can-04-2076
Callender GG, Rosen HR, Roszkowski JJ, Lyons GE, Li M, Moore T, Brasic N, McKee MD, Nishimura MI (2006) Identification of a hepatitis C virus-reactive T cell receptor that does not require CD8 for target cell recognition. Hepatology 43(5):973–981. doi:10.1002/hep.21157
Spear TT, Callender GG, Roszkowski JJ, Moxley KM, Simms PE, Foley KC, Murray DC, Scurti GM, Li M, Thomas JT, Langerman A, Garrett-Mayer E, Zhang Y, Nishimura MI (2016) TCR gene-modified T cells can efficiently treat established hepatitis C-associated hepatocellular carcinoma tumors. Cancer Immunol Immunother 65(3):293–304. doi:10.1007/s00262-016-1800-2
Zhang Y, Liu Y, Moxley KM, Golden-Mason L, Hughes MG, Liu T, Heemskerk MH, Rosen HR, Nishimura MI (2010) Transduction of human T cells with a novel T-cell receptor confers anti-HCV reactivity. PLoS Pathog 6(7):e1001018. doi:10.1371/journal.ppat.1001018
Combadiere B, Reis e Sousa C, Trageser C, Zheng LX, Kim CR, Lenardo MJ (1998) Differential TCR signaling regulates apoptosis and immunopathology during antigen responses in vivo. Immunity 9(3):305–313
Lenardo MJ, Boehme S, Chen L, Combadiere B, Fisher G, Freedman M, McFarland H, Pelfrey C, Zheng L (1995) Autocrine feedback death and the regulation of mature T lymphocyte antigen responses. Int Rev Immunol 13(2):115–134
Johnson LA, Morgan RA, Dudley ME, Cassard L, Yang JC, Hughes MS, Kammula US, Royal RE, Sherry RM, Wunderlich JR, Lee CC, Restifo NP, Schwarz SL, Cogdill AP, Bishop RJ, Kim H, Brewer CC, Rudy SF, VanWaes C, Davis JL, Mathur A, Ripley RT, Nathan DA, Laurencot CM, Rosenberg SA (2009) Gene therapy with human and mouse T-cell receptors mediates cancer regression and targets normal tissues expressing cognate antigen. Blood 114(3):535–546. doi:10.1182/blood-2009-03-211714
Mehrotra S, Al-Khami AA, Klarquist J, Husain S, Naga O, Eby JM, Murali AK, Lyons GE, Li M, Spivey ND, Norell H, Martins da Palma T, Onicescu G, Diaz-Montero CM, Garrett-Mayer E, Cole DJ, Le Poole IC, Nishimura MI (2012) A coreceptor-independent transgenic human TCR mediates anti-tumor and anti-self immunity in mice. J Immunol 189(4):1627–1638. doi:10.4049/jimmunol.1103271
Parkhurst MR, Yang JC, Langan RC, Dudley ME, Nathan DA, Feldman SA, Davis JL, Morgan RA, Merino MJ, Sherry RM, Hughes MS, Kammula US, Phan GQ, Lim RM, Wank SA, Restifo NP, Robbins PF, Laurencot CM, Rosenberg SA (2011) T cells targeting carcinoembryonic antigen can mediate regression of metastatic colorectal cancer but induce severe transient colitis. Mol Ther 19(3):620–626. doi:10.1038/mt.2010.272
Bicknell DC, Rowan A, Bodmer WF (1994) Beta 2-microglobulin gene mutations: a study of established colorectal cell lines and fresh tumors. Proc Natl Acad Sci USA 91(11):4751–4755
Hicklin DJ, Marincola FM, Ferrone S (1999) HLA class I antigen downregulation in human cancers: T-cell immunotherapy revives an old story. Mol Med Today 5(4):178–186
Leisegang M, Engels B, Meyerhuber P, Kieback E, Sommermeyer D, Xue SA, Reuss S, Stauss H, Uckert W (2008) Enhanced functionality of T cell receptor-redirected T cells is defined by the transgene cassette. J Mol Med (Berl) 86(5):573–583. doi:10.1007/s00109-008-0317-3
Scholten KB, Kramer D, Kueter EW, Graf M, Schoedl T, Meijer CJ, Schreurs MW, Hooijberg E (2006) Codon modification of T cell receptors allows enhanced functional expression in transgenic human T cells. Clin Immunol 119(2):135–145. doi:10.1016/j.clim.2005.12.009
Yang S, Cohen CJ, Peng PD, Zhao Y, Cassard L, Yu Z, Zheng Z, Jones S, Restifo NP, Rosenberg SA, Morgan RA (2008) Development of optimal bicistronic lentiviral vectors facilitates high-level TCR gene expression and robust tumor cell recognition. Gene Ther 15(21):1411–1423. doi:10.1038/gt.2008.90
Leisegang M, Turqueti-Neves A, Engels B, Blankenstein T, Schendel DJ, Uckert W, Noessner E (2010) T-cell receptor gene-modified T cells with shared renal cell carcinoma specificity for adoptive T-cell therapy. Clin Cancer Res 16(8):2333–2343. doi:10.1158/1078-0432.ccr-09-2897
Meyerhuber P, Conrad H, Starck L, Leisegang M, Busch DH, Uckert W, Bernhard H (2010) Targeting the epidermal growth factor receptor (HER) family by T cell receptor gene-modified T lymphocytes. J Mol Med (Berl) 88(11):1113–1121. doi:10.1007/s00109-010-0660-z
Hart DP, Xue SA, Thomas S, Cesco-Gaspere M, Tranter A, Willcox B, Lee SP, Steven N, Morris EC, Stauss HJ (2008) Retroviral transfer of a dominant TCR prevents surface expression of a large proportion of the endogenous TCR repertoire in human T cells. Gene Ther 15(8):625–631. doi:10.1038/sj.gt.3303078
Bendle GM, Linnemann C, Hooijkaas AI, Bies L, de Witte MA, Jorritsma A, Kaiser AD, Pouw N, Debets R, Kieback E, Uckert W, Song JY, Haanen JB, Schumacher TN (2010) Lethal graft-versus-host disease in mouse models of T cell receptor gene therapy. Nat Med 16(5):565–570. doi:10.1038/nm.2128
van Loenen MM, de Boer R, Amir AL, Hagedoorn RS, Volbeda GL, Willemze R, van Rood JJ, Falkenburg JH, Heemskerk MH (2010) Mixed T cell receptor dimers harbor potentially harmful neoreactivity. Proc Natl Acad Sci USA 107(24):10972–10977. doi:10.1073/pnas.1005802107
Rosenberg SA (2010) Of mice, not men: no evidence for graft-versus-host disease in humans receiving T-cell receptor-transduced autologous T cells. Mol Ther 18(10):1744–1745. doi:10.1038/mt.2010.195
Kuball J, Dossett ML, Wolfl M, Ho WY, Voss RH, Fowler C, Greenberg PD (2007) Facilitating matched pairing and expression of TCR chains introduced into human T cells. Blood 109(6):2331–2338. doi:10.1182/blood-2006-05-023069
Chang HC, Bao Z, Yao Y, Tse AG, Goyarts EC, Madsen M, Kawasaki E, Brauer PP, Sacchettini JC, Nathenson SG et al (1994) A general method for facilitating heterodimeric pairing between two proteins: application to expression of alpha and beta T-cell receptor extracellular segments. Proc Natl Acad Sci USA 91(24):11408–11412
Kuball J, Hauptrock B, Malina V, Antunes E, Voss RH, Wolfl M, Strong R, Theobald M, Greenberg PD (2009) Increasing functional avidity of TCR-redirected T cells by removing defined N-glycosylation sites in the TCR constant domain. J Exp Med 206(2):463–475. doi:10.1084/jem.20082487
Cohen CJ, Zhao Y, Zheng Z, Rosenberg SA, Morgan RA (2006) Enhanced antitumor activity of murine-human hybrid T-cell receptor (TCR) in human lymphocytes is associated with improved pairing and TCR/CD3 stability. Cancer Res 66(17):8878–8886. doi:10.1158/0008-5472.can-06-1450
Sommermeyer D, Uckert W (2010) Minimal amino acid exchange in human TCR constant regions fosters improved function of TCR gene-modified T cells. J Immunol 184(11):6223–6231. doi:10.4049/jimmunol.0902055
Voss RH, Thomas S, Pfirschke C, Hauptrock B, Klobuch S, Kuball J, Grabowski M, Engel R, Guillaume P, Romero P, Huber C, Beckhove P, Theobald M (2010) Coexpression of the T-cell receptor constant alpha domain triggers tumor reactivity of single-chain TCR-transduced human T cells. Blood 115(25):5154–5163. doi:10.1182/blood-2009-11-254078
Blank U, Boitel B, Mege D, Ermonval M, Acuto O (1993) Analysis of tetanus toxin peptide/DR recognition by human T cell receptors reconstituted into a murine T cell hybridoma. Eur J Immunol 23(12):3057–3065. doi:10.1002/eji.1830231203
Hastings AE, Hurley CK, Robinson ED, Salerno K, Hernandez E, Richert JR (1996) Molecular interactions between transfected human TCR, immunodominant myelin basic protein peptide 152-165, and HLA-DR13. J Immunol 157(8):3460–3471
Roszkowski JJ, Yu DC, Rubinstein MP, McKee MD, Cole DJ, Nishimura MI (2003) CD8-independent tumor cell recognition is a property of the T cell receptor and not the T cell. J Immunol 170(5):2582–2589
Aggen DH, Chervin AS, Schmitt TM, Engels B, Stone JD, Richman SA, Piepenbrink KH, Baker BM, Greenberg PD, Schreiber H, Kranz DM (2012) Single-chain ValphaVbeta T-cell receptors function without mispairing with endogenous TCR chains. Gene Ther 19(4):365–374. doi:10.1038/gt.2011.104
Stone JD, Harris DT, Soto CM, Chervin AS, Aggen DH, Roy EJ, Kranz DM (2014) A novel T cell receptor single-chain signaling complex mediates antigen-specific T cell activity and tumor control. Cancer Immunol Immunother 63(11):1163–1176. doi:10.1007/s00262-014-1586-z
Okamoto S, Mineno J, Ikeda H, Fujiwara H, Yasukawa M, Shiku H, Kato I (2009) Improved expression and reactivity of transduced tumor-specific TCRs in human lymphocytes by specific silencing of endogenous TCR. Cancer Res 69(23):9003–9011. doi:10.1158/0008-5472.can-09-1450
Provasi E, Genovese P, Lombardo A, Magnani Z, Liu PQ, Reik A, Chu V, Paschon DE, Zhang L, Kuball J, Camisa B, Bondanza A, Casorati G, Ponzoni M, Ciceri F, Bordignon C, Greenberg PD, Holmes MC, Gregory PD, Naldini L, Bonini C (2012) Editing T cell specificity towards leukemia by zinc finger nucleases and lentiviral gene transfer. Nat Med 18(5):807–815. doi:10.1038/nm.2700
Dembic Z, Haas W, Weiss S, McCubrey J, Kiefer H, von Boehmer H, Steinmetz M (1986) Transfer of specificity by murine alpha and beta T-cell receptor genes. Nature 320(6059):232–238. doi:10.1038/320232a0
Duval L, Schmidt H, Kaltoft K, Fode K, Jensen JJ, Sorensen SM, Nishimura MI, von der Maase H (2006) Adoptive transfer of allogeneic cytotoxic T lymphocytes equipped with a HLA-A2 restricted MART-1 T-cell receptor: a phase I trial in metastatic melanoma. Clin Cancer Res 12(4):1229–1236. doi:10.1158/1078-0432.ccr-05-1485
Morgan RA, Dudley ME, Wunderlich JR, Hughes MS, Yang JC, Sherry RM, Royal RE, Topalian SL, Kammula US, Restifo NP, Zheng Z, Nahvi A, de Vries CR, Rogers-Freezer LJ, Mavroukakis SA, Rosenberg SA (2006) Cancer regression in patients after transfer of genetically engineered lymphocytes. Science 314(5796):126–129. doi:10.1126/science.1129003
Robbins PF, Morgan RA, Feldman SA, Yang JC, Sherry RM, Dudley ME, Wunderlich JR, Nahvi AV, Helman LJ, Mackall CL, Kammula US, Hughes MS, Restifo NP, Raffeld M, Lee CC, Levy CL, Li YF, El-Gamil M, Schwarz SL, Laurencot C, Rosenberg SA (2011) Tumor regression in patients with metastatic synovial cell sarcoma and melanoma using genetically engineered lymphocytes reactive with NY-ESO-1. J Clin Oncol 29(7):917–924. doi:10.1200/jco.2010.32.2537
Morgan RA, Chinnasamy N, Abate-Daga D, Gros A, Robbins PF, Zheng Z, Dudley ME, Feldman SA, Yang JC, Sherry RM, Phan GQ, Hughes MS, Kammula US, Miller AD, Hessman CJ, Stewart AA, Restifo NP, Quezado MM, Alimchandani M, Rosenberg AZ, Nath A, Wang T, Bielekova B, Wuest SC, Akula N, McMahon FJ, Wilde S, Mosetter B, Schendel DJ, Laurencot CM, Rosenberg SA (2013) Cancer regression and neurological toxicity following anti-MAGE-A3 TCR gene therapy. J Immunother 36(2):133–151. doi:10.1097/CJI.0b013e3182829903
Cameron BJ, Gerry AB, Dukes J, Harper JV, Kannan V, Bianchi FC, Grand F, Brewer JE, Gupta M, Plesa G, Bossi G, Vuidepot A, Powlesland AS, Legg A, Adams KJ, Bennett AD, Pumphrey NJ, Williams DD, Binder-Scholl G, Kulikovskaya I, Levine BL, Riley JL, Varela-Rohena A, Stadtmauer EA, Rapoport AP, Linette GP, June CH, Hassan NJ, Kalos M, Jakobsen BK (2013) Identification of a Titin-derived HLA-A1-presented peptide as a cross-reactive target for engineered MAGE A3-directed T cells. Sci Transl Med 5(197):197ra103. doi:10.1126/scitranslmed.3006034
Linette GP, Stadtmauer EA, Maus MV, Rapoport AP, Levine BL, Emery L, Litzky L, Bagg A, Carreno BM, Cimino PJ, Binder-Scholl GK, Smethurst DP, Gerry AB, Pumphrey NJ, Bennett AD, Brewer JE, Dukes J, Harper J, Tayton-Martin HK, Jakobsen BK, Hassan NJ, Kalos M, June CH (2013) Cardiovascular toxicity and titin cross-reactivity of affinity-enhanced T cells in myeloma and melanoma. Blood 122(6):863–871. doi:10.1182/blood-2013-03-490565
Schub A, Schuster IG, Hammerschmidt W, Moosmann A (2009) CMV-specific TCR-transgenic T cells for immunotherapy. J Immunol 183(10):6819–6830. doi:10.4049/jimmunol.0902233
van Lent AU, Nagasawa M, van Loenen MM, Schotte R, Schumacher TN, Heemskerk MH, Spits H, Legrand N (2007) Functional human antigen-specific T cells produced in vitro using retroviral T cell receptor transfer into hematopoietic progenitors. J Immunol 179(8):4959–4968
Orentas RJ, Roskopf SJ, Nolan GP, Nishimura MI (2001) Retroviral transduction of a T cell receptor specific for an Epstein-Barr virus-encoded peptide. Clin Immunol 98(2):220–228. doi:10.1006/clim.2000.4977
Yang D, Shao Q, Sun H, Mu X, Gao Y, Jiang R, Hou J, Yao K, Chen Y, Sun B (2011) Evaluation of Epstein-Barr virus latent membrane protein 2 specific T-cell receptors driven by T-cell specific promoters using lentiviral vector. Clin Dev Immunol 2011:716926. doi:10.1155/2011/716926
Zheng Y, Parsonage G, Zhuang X, Machado LR, James CH, Salman A, Searle PF, Hui EP, Chan AT, Lee SP (2015) Human leukocyte antigen (HLA) A*1101-restricted Epstein-Barr virus-specific T-cell receptor gene transfer to target nasopharyngeal carcinoma. Cancer Immunol Res 3(10):1138–1147. doi:10.1158/2326-6066.cir-14-0203-T
Hofmann C, Hofflin S, Huckelhoven A, Bergmann S, Harrer E, Schuler G, Dorrie J, Schaft N, Harrer T (2011) Human T cells expressing two additional receptors (TETARs) specific for HIV-1 recognize both epitopes. Blood 118(19):5174–5177. doi:10.1182/blood-2011-04-347005
Ueno T, Fujiwara M, Tomiyama H, Onodera M, Takiguchi M (2004) Reconstitution of anti-HIV effector functions of primary human CD8 T lymphocytes by transfer of HIV-specific alphabeta TCR genes. Eur J Immunol 34(12):3379–3388. doi:10.1002/eji.200425568
Varela-Rohena A, Molloy PE, Dunn SM, Li Y, Suhoski MM, Carroll RG, Milicic A, Mahon T, Sutton DH, Laugel B, Moysey R, Cameron BJ, Vuidepot A, Purbhoo MA, Cole DK, Phillips RE, June CH, Jakobsen BK, Sewell AK, Riley JL (2008) Control of HIV-1 immune escape by CD8 T cells expressing enhanced T-cell receptor. Nat Med 14(12):1390–1395. doi:10.1038/nm.1779
Pasetto A, Frelin L, Aleman S, Holmstrom F, Brass A, Ahlen G, Brenndorfer ED, Lohmann V, Bartenschlager R, Sallberg M, Bertoletti A, Chen M (2012) TCR-redirected human T cells inhibit hepatitis C virus replication: hepatotoxic potential is linked to antigen specificity and functional avidity. J Immunol 189(9):4510–4519. doi:10.4049/jimmunol.1201613
Spear TT, Riley TP, Lyons GE, Callender GG, Roszkowski JJ, Wang Y, Simms PE, Scurti GM, Foley KC, Murray DC, Hellman LM, McMahan RH, Iwashima M, Garrett-Mayer E, Rosen HR, Baker BM, Nishimura MI (2016) Hepatitis C virus-cross-reactive TCR gene-modified T cells: a model for immunotherapy against diseases with genomic instability. J Leukoc Biol. doi:10.1189/jlb.2A1215-561R
Scholten KB, Turksma AW, Ruizendaal JJ, van den Hende M, van der Burg SH, Heemskerk MH, Meijer CJ, Hooijberg E (2011) Generating HPV specific T helper cells for the treatment of HPV induced malignancies using TCR gene transfer. J Transl Med 9:147. doi:10.1186/1479-5876-9-147
Lyons GE, Roszkowski JJ, Man S, Yee C, Kast WM, Nishimura MI (2006) T-cell receptor tetramer binding or the lack there of does not necessitate antigen reactivity in T-cell receptor transduced T cells. Cancer Immunol Immunother 55(9):1142–1150. doi:10.1007/s00262-005-0103-9
Wilkie S, van Schalkwyk MC, Hobbs S, Davies DM, van der Stegen SJ, Pereira AC, Burbridge SE, Box C, Eccles SA, Maher J (2012) Dual targeting of ErbB2 and MUC1 in breast cancer using chimeric antigen receptors engineered to provide complementary signaling. J Clin Immunol 32(5):1059–1070. doi:10.1007/s10875-012-9689-9
Fedorov VD, Themeli M, Sadelain M (2013) PD-1- and CTLA-4-based inhibitory chimeric antigen receptors (iCARs) divert off-target immunotherapy responses. Sci Transl Med 5(215):215ra172. doi:10.1126/scitranslmed.3006597
Liu K, Rosenberg SA (2001) Transduction of an IL-2 gene into human melanoma-reactive lymphocytes results in their continued growth in the absence of exogenous IL-2 and maintenance of specific antitumor activity. J Immunol 167(11):6356–6365
Kerkar SP, Muranski P, Kaiser A, Boni A, Sanchez-Perez L, Yu Z, Palmer DC, Reger RN, Borman ZA, Zhang L, Morgan RA, Gattinoni L, Rosenberg SA, Trinchieri G, Restifo NP (2010) Tumor-specific CD8+ T cells expressing interleukin-12 eradicate established cancers in lymphodepleted hosts. Cancer Res 70(17):6725–6734. doi:10.1158/0008-5472.can-10-0735
Spear P, Barber A, Rynda-Apple A, Sentman CL (2012) Chimeric antigen receptor T cells shape myeloid cell function within the tumor microenvironment through IFN-gamma and GM-CSF. J Immunol 188(12):6389–6398. doi:10.4049/jimmunol.1103019
Kerkar SP, Goldszmid RS, Muranski P, Chinnasamy D, Yu Z, Reger RN, Leonardi AJ, Morgan RA, Wang E, Marincola FM, Trinchieri G, Rosenberg SA, Restifo NP (2011) IL-12 triggers a programmatic change in dysfunctional myeloid-derived cells within mouse tumors. J Clin Invest 121(12):4746–4757. doi:10.1172/jci58814
Koneru M, O’Cearbhaill R, Pendharkar S, Spriggs DR, Brentjens RJ (2015) A phase I clinical trial of adoptive T cell therapy using IL-12 secreting MUC-16(ecto) directed chimeric antigen receptors for recurrent ovarian cancer. J Transl Med 13:102. doi:10.1186/s12967-015-0460-x
Craddock JA, Lu A, Bear A, Pule M, Brenner MK, Rooney CM, Foster AE (2010) Enhanced tumor trafficking of GD2 chimeric antigen receptor T cells by expression of the chemokine receptor CCR2b. J Immunother 33(8):780–788. doi:10.1097/CJI.0b013e3181ee6675
Kershaw MH, Wang G, Westwood JA, Pachynski RK, Tiffany HL, Marincola FM, Wang E, Young HA, Murphy PM, Hwu P (2002) Redirecting migration of T cells to chemokine secreted from tumors by genetic modification with CXCR2. Hum Gene Ther 13(16):1971–1980. doi:10.1089/10430340260355374
Chinnasamy D, Yu Z, Kerkar SP, Zhang L, Morgan RA, Restifo NP, Rosenberg SA (2012) Local delivery of interleukin-12 using T cells targeting VEGF receptor-2 eradicates multiple vascularized tumors in mice. Clin Cancer Res 18(6):1672–1683. doi:10.1158/1078-0432.ccr-11-3050
Legler DF, Johnson-Leger C, Wiedle G, Bron C, Imhof BA (2004) The alpha v beta 3 integrin as a tumor homing ligand for lymphocytes. Eur J Immunol 34(6):1608–1616. doi:10.1002/eji.200424938
Buckanovich RJ, Facciabene A, Kim S, Benencia F, Sasaroli D, Balint K, Katsaros D, O’Brien-Jenkins A, Gimotty PA, Coukos G (2008) Endothelin B receptor mediates the endothelial barrier to T cell homing to tumors and disables immune therapy. Nat Med 14(1):28–36. doi:10.1038/nm1699
Dudley ME, Yang JC, Sherry R, Hughes MS, Royal R, Kammula U, Robbins PF, Huang J, Citrin DE, Leitman SF, Wunderlich J, Restifo NP, Thomasian A, Downey SG, Smith FO, Klapper J, Morton K, Laurencot C, White DE, Rosenberg SA (2008) Adoptive cell therapy for patients with metastatic melanoma: evaluation of intensive myeloablative chemoradiation preparative regimens. J Clin Oncol 26(32):5233–5239. doi:10.1200/jco.2008.16.5449
Wallen H, Thompson JA, Reilly JZ, Rodmyre RM, Cao J, Yee C (2009) Fludarabine modulates immune response and extends in vivo survival of adoptively transferred CD8 T cells in patients with metastatic melanoma. PLoS ONE 4(3):e4749. doi:10.1371/journal.pone.0004749
Khammari A, Labarriere N, Vignard V, Nguyen JM, Pandolfino MC, Knol AC, Quereux G, Saiagh S, Brocard A, Jotereau F, Dreno B (2009) Treatment of metastatic melanoma with autologous Melan-A/MART-1-specific cytotoxic T lymphocyte clones. J Invest Dermatol 129(12):2835–2842. doi:10.1038/jid.2009.144
Gattinoni L, Finkelstein SE, Klebanoff CA, Antony PA, Palmer DC, Spiess PJ, Hwang LN, Yu Z, Wrzesinski C, Heimann DM, Surh CD, Rosenberg SA, Restifo NP (2005) Removal of homeostatic cytokine sinks by lymphodepletion enhances the efficacy of adoptively transferred tumor-specific CD8+ T cells. J Exp Med 202(7):907–912. doi:10.1084/jem.20050732
Cho BK, Rao VP, Ge Q, Eisen HN, Chen J (2000) Homeostasis-stimulated proliferation drives naive T cells to differentiate directly into memory T cells. J Exp Med 192(4):549–556
Kedl RM, Rees WA, Hildeman DA, Schaefer B, Mitchell T, Kappler J, Marrack P (2000) T cells compete for access to antigen-bearing antigen-presenting cells. J Exp Med 192(8):1105–1113
Antony PA, Piccirillo CA, Akpinarli A, Finkelstein SE, Speiss PJ, Surman DR, Palmer DC, Chan CC, Klebanoff CA, Overwijk WW, Rosenberg SA, Restifo NP (2005) CD8+ T cell immunity against a tumor/self-antigen is augmented by CD4+ T helper cells and hindered by naturally occurring T regulatory cells. J Immunol 174(5):2591–2601
Besser MJ, Shapira-Frommer R, Itzhaki O, Treves AJ, Zippel DB, Levy D, Kubi A, Shoshani N, Zikich D, Ohayon Y, Ohayon D, Shalmon B, Markel G, Yerushalmi R, Apter S, Ben-Nun A, Ben-Ami E, Shimoni A, Nagler A, Schachter J (2013) Adoptive transfer of tumor-infiltrating lymphocytes in patients with metastatic melanoma: intent-to-treat analysis and efficacy after failure to prior immunotherapies. Clin Cancer Res 19(17):4792–4800. doi:10.1158/1078-0432.ccr-13-0380
Ellebaek E, Iversen TZ, Junker N, Donia M, Engell-Noerregaard L, Met O, Holmich LR, Andersen RS, Hadrup SR, Andersen MH, thor Straten P, Svane IM (2012) Adoptive cell therapy with autologous tumor infiltrating lymphocytes and low-dose Interleukin-2 in metastatic melanoma patients. J Transl Med 10:169. doi:10.1186/1479-5876-10-169
Butler MO, Friedlander P, Milstein MI, Mooney MM, Metzler G, Murray AP, Tanaka M, Berezovskaya A, Imataki O, Drury L, Brennan L, Flavin M, Neuberg D, Stevenson K, Lawrence D, Hodi FS, Velazquez EF, Jaklitsch MT, Russell SE, Mihm M, Nadler LM, Hirano N (2011) Establishment of antitumor memory in humans using in vitro-educated CD8+ T cells. Sci Transl Med 3(80):80ra34. doi:10.1126/scitranslmed.3002207
Hunder NN, Wallen H, Cao J, Hendricks DW, Reilly JZ, Rodmyre R, Jungbluth A, Gnjatic S, Thompson JA, Yee C (2008) Treatment of metastatic melanoma with autologous CD4+ T cells against NY-ESO-1. N Engl J Med 358(25):2698–2703. doi:10.1056/NEJMoa0800251
Ciceri F, Bonini C, Stanghellini MT, Bondanza A, Traversari C, Salomoni M, Turchetto L, Colombi S, Bernardi M, Peccatori J, Pescarollo A, Servida P, Magnani Z, Perna SK, Valtolina V, Crippa F, Callegaro L, Spoldi E, Crocchiolo R, Fleischhauer K, Ponzoni M, Vago L, Rossini S, Santoro A, Todisco E, Apperley J, Olavarria E, Slavin S, Weissinger EM, Ganser A, Stadler M, Yannaki E, Fassas A, Anagnostopoulos A, Bregni M, Stampino CG, Bruzzi P, Bordignon C (2009) Infusion of suicide-gene-engineered donor lymphocytes after family haploidentical haemopoietic stem-cell transplantation for leukaemia (the TK007 trial): a non-randomised phase I-II study. Lancet Oncol 10(5):489–500. doi:10.1016/s1470-2045(09)70074-9
Recchia A, Bonini C, Magnani Z, Urbinati F, Sartori D, Muraro S, Tagliafico E, Bondanza A, Stanghellini MT, Bernardi M, Pescarollo A, Ciceri F, Bordignon C, Mavilio F (2006) Retroviral vector integration deregulates gene expression but has no consequence on the biology and function of transplanted T cells. Proc Natl Acad Sci USA 103(5):1457–1462. doi:10.1073/pnas.0507496103
Berger C, Flowers ME, Warren EH, Riddell SR (2006) Analysis of transgene-specific immune responses that limit the in vivo persistence of adoptively transferred HSV-TK-modified donor T cells after allogeneic hematopoietic cell transplantation. Blood 107(6):2294–2302. doi:10.1182/blood-2005-08-3503
Riddell SR, Elliott M, Lewinsohn DA, Gilbert MJ, Wilson L, Manley SA, Lupton SD, Overell RW, Reynolds TC, Corey L, Greenberg PD (1996) T-cell mediated rejection of gene-modified HIV-specific cytotoxic T lymphocytes in HIV-infected patients. Nat Med 2(2):216–223
Budde LE, Berger C, Lin Y, Wang J, Lin X, Frayo SE, Brouns SA, Spencer DM, Till BG, Jensen MC, Riddell SR, Press OW (2013) Combining a CD20 chimeric antigen receptor and an inducible caspase 9 suicide switch to improve the efficacy and safety of T cell adoptive immunotherapy for lymphoma. PLoS ONE 8(12):e82742. doi:10.1371/journal.pone.0082742
Di Stasi A, Tey SK, Dotti G, Fujita Y, Kennedy-Nasser A, Martinez C, Straathof K, Liu E, Durett AG, Grilley B, Liu H, Cruz CR, Savoldo B, Gee AP, Schindler J, Krance RA, Heslop HE, Spencer DM, Rooney CM, Brenner MK (2011) Inducible apoptosis as a safety switch for adoptive cell therapy. N Engl J Med 365(18):1673–1683. doi:10.1056/NEJMoa1106152
Hoyos V, Savoldo B, Quintarelli C, Mahendravada A, Zhang M, Vera J, Heslop HE, Rooney CM, Brenner MK, Dotti G (2010) Engineering CD19-specific T lymphocytes with interleukin-15 and a suicide gene to enhance their anti-lymphoma/leukemia effects and safety. Leukemia 24(6):1160–1170. doi:10.1038/leu.2010.75
Straathof KC, Pule MA, Yotnda P, Dotti G, Vanin EF, Brenner MK, Heslop HE, Spencer DM, Rooney CM (2005) An inducible caspase 9 safety switch for T-cell therapy. Blood 105(11):4247–4254. doi:10.1182/blood-2004-11-4564
Griffioen M, van Egmond EH, Kester MG, Willemze R, Falkenburg JH, Heemskerk MH (2009) Retroviral transfer of human CD20 as a suicide gene for adoptive T-cell therapy. Haematologica 94(9):1316–1320. doi:10.3324/haematol.2008.001677
Wang X, Chang WC, Wong CW, Colcher D, Sherman M, Ostberg JR, Forman SJ, Riddell SR, Jensen MC (2011) A transgene-encoded cell surface polypeptide for selection, in vivo tracking, and ablation of engineered cells. Blood 118(5):1255–1263. doi:10.1182/blood-2011-02-337360
Nagaraj S, Gupta K, Pisarev V, Kinarsky L, Sherman S, Kang L, Herber DL, Schneck J, Gabrilovich DI (2007) Altered recognition of antigen is a mechanism of CD8+ T cell tolerance in cancer. Nat Med 13(7):828–835. doi:10.1038/nm1609
Chhabra A, Yang L, Wang P, Comin-Anduix B, Das R, Chakraborty NG, Ray S, Mehrotra S, Yang H, Hardee CL, Hollis R, Dorsky DI, Koya R, Kohn DB, Ribas A, Economou JS, Baltimore D, Mukherji B (2008) CD4+ CD25− T cells transduced to express MHC class I-restricted epitope-specific TCR synthesize Th1 cytokines and exhibit MHC class I-restricted cytolytic effector function in a human melanoma model. J Immunol 181(2):1063–1070
Ray S, Chhabra A, Chakraborty NG, Hegde U, Dorsky DI, Chodon T, von Euw E, Comin-Anduix B, Koya RC, Ribas A, Economou JS, Rosenberg SA, Mukherji B (2010) MHC-I-restricted melanoma antigen specific TCR-engineered human CD4+ T cells exhibit multifunctional effector and helper responses, in vitro. Clin Immunol 136(3):338–347. doi:10.1016/j.clim.2010.04.013
Eisen HN, Sykulev Y, Tsomides TJ (1996) Antigen-specific T-cell receptors and their reactions with complexes formed by peptides with major histocompatibility complex proteins. Adv Protein Chem 49:1–56
Vitiello A, Marchesini D, Furze J, Sherman LA, Chesnut RW (1991) Analysis of the HLA-restricted influenza-specific cytotoxic T lymphocyte response in transgenic mice carrying a chimeric human-mouse class I major histocompatibility complex. J Exp Med 173(4):1007–1015
Parkhurst MR, Joo J, Riley JP, Yu Z, Li Y, Robbins PF, Rosenberg SA (2009) Characterization of genetically modified T-cell receptors that recognize the CEA:691-699 peptide in the context of HLA-A2.1 on human colorectal cancer cells. Clin Cancer Res 15(1):169–180. doi:10.1158/1078-0432.ccr-08-1638
Kuball J, Schmitz FW, Voss RH, Ferreira EA, Engel R, Guillaume P, Strand S, Romero P, Huber C, Sherman LA, Theobald M (2005) Cooperation of human tumor-reactive CD4+ and CD8+ T cells after redirection of their specificity by a high-affinity p53A2.1-specific TCR. Immunity 22(1):117–129. doi:10.1016/j.immuni.2004.12.005
Holler PD, Holman PO, Shusta EV, O’Herrin S, Wittrup KD, Kranz DM (2000) In vitro evolution of a T cell receptor with high affinity for peptide/MHC. Proc Natl Acad Sci USA 97(10):5387–5392. doi:10.1073/pnas.080078297
Li Y, Moysey R, Molloy PE, Vuidepot AL, Mahon T, Baston E, Dunn S, Liddy N, Jacob J, Jakobsen BK, Boulter JM (2005) Directed evolution of human T-cell receptors with picomolar affinities by phage display. Nat Biotechnol 23(3):349–354. doi:10.1038/nbt1070
Zhao Y, Bennett AD, Zheng Z, Wang QJ, Robbins PF, Yu LY, Li Y, Molloy PE, Dunn SM, Jakobsen BK, Rosenberg SA, Morgan RA (2007) High-affinity TCRs generated by phage display provide CD4+ T cells with the ability to recognize and kill tumor cell lines. J Immunol 179(9):5845–5854
Chlewicki LK, Holler PD, Monti BC, Clutter MR, Kranz DM (2005) High-affinity, peptide-specific T cell receptors can be generated by mutations in CDR1, CDR2 or CDR3. J Mol Biol 346(1):223–239. doi:10.1016/j.jmb.2004.11.057
de Witte MA, Kierkels GJ, Straetemans T, Britten CM, Kuball J (2015) Orchestrating an immune response against cancer with engineered immune cells expressing alphabetaTCRs, CARs, and innate immune receptors: an immunological and regulatory challenge. Cancer Immunol Immunother 64(7):893–902. doi:10.1007/s00262-015-1710-8
Guest RD, Kirillova N, Mowbray S, Gornall H, Rothwell DG, Cheadle EJ, Austin E, Smith K, Watt SM, Kuhlcke K, Westwood N, Thistlethwaite F, Hawkins RE, Gilham DE (2014) Definition and application of good manufacturing process-compliant production of CEA-specific chimeric antigen receptor expressing T-cells for phase I/II clinical trial. Cancer Immunol Immunother 63(2):133–145. doi:10.1007/s00262-013-1492-9
Krug C, Wiesinger M, Abken H, Schuler-Thurner B, Schuler G, Dorrie J, Schaft N (2014) A GMP-compliant protocol to expand and transfect cancer patient T cells with mRNA encoding a tumor-specific chimeric antigen receptor. Cancer Immunol Immunother 63(10):999–1008. doi:10.1007/s00262-014-1572-5
Acknowledgments
The authors would like to acknowledge funding kindly provided by the National Cancer Institute of the National Institutes of Health. These include Grants P01 CA154778 (Nishimura) and F30 CA180731 (Spear).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Spear, T.T., Nagato, K. & Nishimura, M.I. Strategies to genetically engineer T cells for cancer immunotherapy. Cancer Immunol Immunother 65, 631–649 (2016). https://doi.org/10.1007/s00262-016-1842-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00262-016-1842-5