Abstract
Purpose
Few comparative studies assessed the current concept of individualised alignment for total knee arthroplasty (TKA) and their outcomes at mid-term. This study aimed to evaluate the functional outcomes at 1 year of primary TKA performed with a functional positioning technique based on an image-based robotic-assisted system, compared to conventional TKA performed with a restricted kinematic alignment technique.
Methods
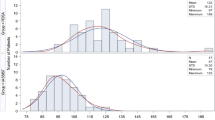
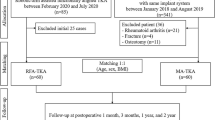
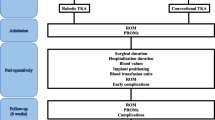
This retrospective comparative study included 100 primary TKAs performed with functional positioning principles using an image-based robotic-assisted system. A control group included 100 primary TKAs with the same posterior-stabilised implant as the robotic group but performed with manual instrumentation and restricted kinematic alignment technique. In the robotic group, the mean age was 69.2 years old ± 7.9; the mean body mass index was 29.7 kg/m2 ± 4.6. The demographic characteristics were similar between both groups. Kujala score, Forgotten Joint Score (FJS), Knee Society Score (KSS) knee and KSS function were collected 12 months postoperatively. Normally distributed continuous variables were compared using the Student t test. For non-normally distributed continuous variables, the Mann–Whitney test was used.
Results
FJS was significantly higher in the robotic group (76.3 ± 13 vs. 68.6 ± 16.9 in the conventional group; p = 0.026). At a 1-year follow-up, there was no significant difference in the KSS knee and KSS function scores and the Kujala score between both groups. The mean KSS knee score was 90.8 ± 11.4 in the robotic group versus 89.4 ± 9.6 in the conventional group (p = 0.082). The mean KSS function score was 91.4 ± 12.3 versus 91.3 ± 12.6, respectively (p = 0.778).
Conclusion
Functional positioning principles using an image-based robotic-assisted system achieved a higher Forgotten Joint Score 1 year after TKA compared to restricted kinematic alignment. Personalised alignment and implant positioning are interesting paths to improve the functional outcomes after TKA.
Level of evidence
III.





Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.References
Batailler C, Fernandez A, Swan J, Servien E, Haddad FS, Catani F et al (2021) MAKO CT-based robotic arm-assisted system is a reliable procedure for total knee arthroplasty: a systematic review. Knee Surg Sports Traumatol Arthrosc 29:3585–3598
Batailler C, Lording T, De Massari D, Witvoet-Braam S, Bini S, Lustig S (2021) Predictive models for clinical outcomes in total knee arthroplasty: a systematic analysis. Arthroplast Today 9:1–15
Batailler C, Swan J, Sappey Marinier E, Servien E, Lustig S (2020) New technologies in knee arthroplasty: current concepts. J Clin Med
Behrend H, Giesinger K, Giesinger JM, Kuster MS (2012) The “forgotten joint” as the ultimate goal in joint arthroplasty: validation of a new patient-reported outcome measure. J Arthroplasty 27(430–436):e431
Canovas F, Dagneaux L (2018) Quality of life after total knee arthroplasty. Orthop Traumatol Surg Res 104:S41–S46
Choi BS, Kim SE, Yang M, Ro DH, Han HS (2023) Correction to: Functional alignment with robotic-arm assisted total knee arthroplasty demonstrated better patient-reported outcomes than mechanical alignment with manual total knee arthroplasty. Knee Surg Sports Traumatol Arthrosc 31:1081
Clark GW, Steer RA, Khan RN, Collopy DM, Wood D (2023) Maintaining joint line obliquity optimizes outcomes of functional alignment in total knee arthroplasty in patients with constitutionally varus knees. J Arthroplasty 38(7 Suppl 2):S239–S244. https://doi.org/10.1016/j.arth.2023.04.004
Cotter EJ, Wang J, Illgen RL (2020) Comparative cost analysis of robotic-assisted and jig-based manual primary total knee arthroplasty. J Knee Surg. https://doi.org/10.1055/s-0040-1713895
Daffara V, Zambianchi F, Bazzan G, Matveitchouk N, Berni A, Piacentini L, Cuoghi Costantini R, Catani F (2023) No difference in clinical outcomes between functionally aligned cruciate-retaining and posterior-stabilized robotic-assisted total knee arthroplasty. Int Orthop 47(3):711–717. https://doi.org/10.1007/s00264-023-05693-1
Debette C, Parratte S, Maucort-Boulch D, Blanc G, Pauly V, Lustig S et al (2014) French adaptation of the new Knee Society Scoring System for total knee arthroplasty. Orthop Traumatol Surg Res 100:531–534
Fontalis A, Kayani B, Asokan A, Haddad IC, Tahmassebi J, Konan S et al (2022) Inflammatory response in robotic-arm-assisted versus conventional jig-based TKA and the correlation with early functional outcomes: results of a prospective randomized controlled trial. J Bone Joint Surg Am 104:1905–1914
Gunaratne R, Pratt DN, Banda J, Fick DP, Khan RJK, Robertson BW (2017) Patient dissatisfaction following total knee arthroplasty: a systematic review of the literature. J Arthroplasty 32:3854–3860
Kayani B, Konan S, Huq SS, Tahmassebi J, Haddad FS (2019) Robotic-arm assisted total knee arthroplasty has a learning curve of seven cases for integration into the surgical workflow but no learning curve effect for accuracy of implant positioning. Knee Surg Sports Traumatol Arthrosc 27:1132–1141
Kayani B, Konan S, Tahmassebi J, Pietrzak JRT, Haddad FS (2018) Robotic-arm assisted total knee arthroplasty is associated with improved early functional recovery and reduced time to hospital discharge compared with conventional jig-based total knee arthroplasty: a prospective cohort study. Bone Joint J 100-B:930–937
Kayani B, Tahmassebi J, Ayuob A, Konan S, Oussedik S, Haddad FS (2021) A prospective randomized controlled trial comparing the systemic inflammatory response in conventional jig-based total knee arthroplasty versus robotic-arm assisted total knee arthroplasty. Bone Joint J 103-B:113–122
Kim YH, Yoon SH, Park JW (2020) Does robotic-assisted TKA result in better outcome scores or long-term survivorship than conventional TKA? A randomized, controlled trial. Clin Orthop Relat Res 478:266–275
Kort N, Stirling P, Pilot P, Muller JH (2022) Robot-assisted knee arthroplasty improves component positioning and alignment, but results are inconclusive on whether it improves clinical scores or reduces complications and revisions: a systematic overview of meta-analyses. Knee Surg Sports Traumatol Arthrosc 30:2639–2653
Mahoney O, Kinsey T, Sodhi N, Mont MA, Chen AF, Orozco F et al (2022) Improved component placement accuracy with robotic-arm assisted total knee arthroplasty. J Knee Surg 35:337–344
Mancuso CA, Sculco TP, Wickiewicz TL, Jones EC, Robbins L, Warren RF et al (2001) Patients’ expectations of knee surgery. J Bone Joint Surg Am 83:1005–1012
Marchand KB, Moody R, Scholl LY, Bhowmik-Stoker M, Taylor KB, Mont MA et al (2023) Results of robotic-assisted versus manual total knee arthroplasty at 2-year follow-up. J Knee Surg 36:159–166. https://doi.org/10.1055/s-0041-1731349
Marchand RC, Sodhi N, Anis HK, Ehiorobo J, Newman JM, Taylor K et al (2019) One-year patient outcomes for robotic-arm-assisted versus manual total knee arthroplasty. J Knee Surg 32:1063–1068
Marchand RC, Sodhi N, Khlopas A, Sultan AA, Harwin SF, Malkani AL et al (2017) Patient satisfaction outcomes after robotic arm-assisted total knee arthroplasty: a short-term evaluation. J Knee Surg 30:849–853
McCormick BP, Rigor P, Trent SM, Lee JW, Tefera E, Mistretta KL, Boucher HR (2022) Short-term outcomes following cemented versus cementless robotic-assisted total knee arthroplasty. Cureus 14(10):e30667. https://doi.org/10.7759/cureus.30667
Mitchell J, Wang J, Bukowski B, Greiner J, Wolford B, Oyer M et al (2021) Relative clinical outcomes comparing manual and robotic-assisted total knee arthroplasty at minimum 1-year follow-up. HSS J 17:267–273
Moser LB, Hess S, Amsler F, Behrend H, Hirschmann MT (2019) Native non-osteoarthritic knees have a highly variable coronal alignment: a systematic review. Knee Surg Sports Traumatol Arthrosc 27:1359–1367
Naziri Q, Cusson BC, Chaudhri M, Shah NV, Sastry A (2019) Making the transition from traditional to robotic-arm assisted TKA: What to expect? A single-surgeon comparative-analysis of the first-40 consecutive cases. J Orthop 16:364–368
Nickel BT, Carroll KM, Pearle AD, Kleeblad LJ, Burger J, Mayman DJ et al (2021) The accuracy and clinical success of robotic-assisted total knee arthroplasty. HSS J 17:261–266
Parvizi J, Mui A, Purtill JJ, Sharkey PF, Hozack WJ, Rothman RH (2007) Total joint arthroplasty: when do fatal or near-fatal complications occur? J Bone Joint Surg Am 89:27–32
Ruangsomboon P, Ruangsomboon O, Pornrattanamaneewong C, Narkbunnam R, Chareancholvanich K (2023) Clinical and radiological outcomes of robotic-assisted versus conventional total knee arthroplasty: a systematic review and meta-analysis of randomized controlled trials. Acta Orthop 94:60–79
Shatrov J, Batailler C, Sappey-Marinier E, Gunst S, Servien E, Lustig S (2022) Correction Notice to: Functional Alignment Philosophy in Total Knee Arthroplasty - Rationale and technique for the varus morphotype using a CT based robotic platform and individualized planning. SICOT J 8:18
Sires JD, Wilson CJ (2021) CT validation of intraoperative implant position and knee alignment as determined by the MAKO total knee arthroplasty system. J Knee Surg 34:1133–1137
Sires JD, Wilson CJ (2020) CT validation of intraoperative implant position and knee alignment as determined by the MAKO total knee arthroplasty system. J Knee Surg. https://doi.org/10.1055/s-0040-1701447
Smith AF, Eccles CJ, Bhimani SJ, Denehy KM, Bhimani RB, Smith LS, et al. (2019) Improved patient satisfaction following robotic-assisted total knee arthroplasty. J Knee Surg. https://doi.org/10.1055/s-0039-1700837
Vendittoli PA, Martinov S, Blakeney WG (2021) Restricted kinematic alignment, the fundamentals, and clinical applications. Front Surg 8:697020
Vermue H, Batailler C, Monk P, Haddad F, Luyckx T, Lustig S (2023) The evolution of robotic systems for total knee arthroplasty, each system must be assessed for its own value: a systematic review of clinical evidence and meta-analysis. Arch Orthop Trauma Surg 143:3369–3381
Funding
No funding.
Author information
Authors and Affiliations
Contributions
MK: study design, data collection, statistical analysis, literature review and manuscript writing. CB: study design, statistical analysis, literature review, manuscript editing and supervision. JS: literature review and manuscript editing. JAJ: data collection and manuscript editing. JF: data collection and manuscript editing. ES: study design and manuscript editing. SL: study design, supervision, literature review and manuscript editing. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
MK, CB, JS, JAJ, JF declare that they have no conflict of interest. ES: Consultant for Corin. SL: Consultant for Stryker, Smith Nephew, Heraeus, Depuy Synthes; institutional research support from Groupe Lepine, Amplitude; Editorial Board for Journal of Bone and Joint Surgery (Am).
Ethical approval
All procedures performed in studies involving human participants followed the ethical standards of the institutional and/or national research committees and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards. For this type of study, formal consent is not required. Data collection and analysis were carried out in accordance with MR004 Reference Methodology from the Commission Nationale de l'Informatique et des Libertés (Ref. 2226075) obtained the 19 April 2022. The study was registered and filed on the Health Data Hub website.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Kafelov, M., Batailler, C., Shatrov, J. et al. Functional positioning principles for image-based robotic-assisted TKA achieved a higher Forgotten Joint Score at 1 year compared to conventional TKA with restricted kinematic alignment. Knee Surg Sports Traumatol Arthrosc 31, 5591–5602 (2023). https://doi.org/10.1007/s00167-023-07609-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00167-023-07609-3