Abstract
Oxidative stress is a major cause of morbidity and mortality in human health and disease. In this review, we focus on the Forkhead Box (Fox) subclass O3 (FoxO3), an extensively studied transcription factor that plays a pleiotropic role in a wide range of physiological and pathological processes by regulating multiple gene regulatory networks involved in the modulation of numerous aspects of cellular metabolism, including fuel metabolism, cell death, and stress resistance. This review will also focus on regulatory mechanisms of FoxO3 expression and activity, such as crucial post-translational modifications and non-coding RNAs. Moreover, this work discusses and evidences some pathways to how this transcription factor and reactive oxygen species regulate each other, which may lead to the pathogenesis of various types of diseases. Therefore, in addition to being a promising therapeutic target, the FoxO3-regulated signaling pathways can also be used as reliable diagnostic and prognostic biomarkers and indicators for drug responsiveness.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Reduction and oxidation reactions (redox) control almost all aspects of life [1]. Oxidation is a fundamental part of aerobic life and our metabolism; thus, reactive species (RS) of oxygen (ROS), nitrogen (RNS), chlorine, bromine, iron, and sulfur are formed as by-products of this type of metabolism whose effects are counteracted by the reactions of reduction [2, 3]. Therefore, RS can be produced naturally or due to some biological dysfunction, such as during intensive physical activity, exposure to microbial infections that involve the activation of phagocytes, the action of pollutants/toxins such as cigarette smoke, alcohol, ionizing and UV radiation, pesticides, and ozone [4].
Historically, RS were believed to function exclusively as agents of cellular damage, reacting indiscriminately with lipids, proteins, and DNA [5, 6]. However, over the past two decades, there has been a growing appreciation of the role of ROS and RNS as mediators of cellular signaling, regulating numerous physiological responses [1, 2, 7]. The phenomenon termed hormesis describes a dose–response relationship to stressors, with a low-dose leading to stimulation of stress resistance mechanisms, thus enhancing the cellular capacity of preservation and repair and a high dose being detrimental, causing inhibition and cell damage [8, 9]. Therefore, biological systems present a dynamic evolutionary adaptive strategy depending on dose-time response [9]. The molecular recognition mechanisms occur at the atomic level. They operate in signaling through chemical reactions that lead to covalent modifications of proteins [10], promoting an expansion of the potential number of specific recipients [11].
The versatility of these molecules, concerning their properties and mobility within cells, is one of the significant advantages that is believed to be responsible for the evolutionary conservation of this type of signaling [12]. Moreover, as part of a highly conserved cellular signaling network, they are integrated with several signaling pathways, including the protective responses to ROS-induced oxidative stress. In this scenario, it has become apparent that moderate elevations in ROS levels (eustress) are essential for regulating processes, such as cell proliferation, apoptosis, and gene expression, through the transcription factor (TF) modulations [2, 4]. Under pathophysiological conditions, the RS production exceeds this physiological level, and only then does oxidative damage accumulate (distress), a process observed in many pathologies [1, 13]. Thus, redox homeostasis, described as “the golden mean of healthy living” [14], is indispensable for cell function and viability, so there is considerable evidence showing that oxidative damage is related to the primary or secondary pathophysiological mechanisms of various diseases [1, 13].
Regulation for such homeostasis can occur by modifying the activity of metabolic enzymes and TFs and through gene expression and epigenetic modifications [1, 15]. Therefore, this complex regulation involves a finely regulated network of redox reactions, post-translational modifications (PTMs), and their cellular outputs. This review will focus on the TF aspect of this regulation, more specifically, the Forkhead Box (Fox) subclass O3 (FoxO3), an extensively studied TF that shows a promising correlation with the redox metabolism and several pathological diseases associated with a redox disbalance [16]. Thus, this review aims to show that FoxO3 is a crucial modulator in redox metabolism by evidencing some pathways to how this TF and ROS regulate each other.
General aspects of FoxOs
The members of the FoxO family (FoxO1, 3, 4, and 6) are widely distributed throughout multiple species, ranging from yeasts to human beings [16, 17]. All four isoforms recognize and bind to the same FoxO-responsive sites, called "forkhead-responsive DNA elements" (FHRE), in the promoter region of target genes. Thus it is not surprising that FoxO isoforms have some overlapping activities, which results in a certain degree of redundancy [18]. However, there are also isoform-specific effects, as evidenced in studies with FoxO-isoform-specific knockout mice [19]. Nevertheless, there are also cell- and tissue-specific effects of the four FoxO isoforms due to differences in their expression levels and regulation [20]. FoxOs can be considered multitasking proteins as they play pleiotropic roles in a variety of physiological and pathological processes by regulating multiple gene regulatory networks involved in the modulation of numerous aspects of cellular metabolism, including fuel metabolism, cell death, and stress resistance (Fig. 1) [16, 21].
FoxOs as homeostasis regulators. Overview of FoxO transcription factors' roles in a wide range of cellular processes, which are generally regulated by external changes that disturb homeostasis, including metabolic stress (e.g., starvation) and oxidative stress, the last one being highlighted (upper right quadrant). Source: by the authors
Regarding redox homeostasis, FoxO3 is an essential TF due to its well-established role as a central mediator of cellular response to stress in different animal models [22]. Indeed, FoxO3 is a known core regulator of cellular homeostasis, stress response, and longevity, as it can modulate various stress responses upon nutrient shortage, oxidative stress, hypoxia, heat shock, and DNA damage. Therefore, we can link its role to increased lifespan by modulating stress responses upon oxidative stress, DNA damage, nutrient shortage, and caloric restriction [23].
In regard to cellular defense against oxidative stress, FoxO3 has a well-established role in regulating the expressions of many antioxidants, including catalase (CAT), Zinc and manganese superoxide dismutase (Zn- and Mn-SOD), peroxiredoxins 3, and 5 (PRDX3 and PRDX5), and glutathione peroxidase (GPx) [24,25,26,27,28]. Furthermore, the expressions of thioredoxin 2 (Trx2) and thioredoxin reductase 2 (TrxR2) were also revealed to be regulated by FoxO3 [28]. Thus, protecting cells from oxidative stress by increasing ROS scavengers contributes to extending the organismal lifespan. Moreover, FoxO3 protein can act in promoting cell growth inhibition (by enhancing the expression of various CDK inhibitors) [29,30,31,32] or apoptosis (pro-apoptotic genes are activated) [33,34,35,36,37] when upon intense oxidative stress. Hence, this demonstrates that activation of FoxO3-dependent transcription in response to oxidative stress depends on the severity of the stimulus [16] (Fig. 2).
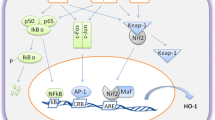
FoxO and Oxidative stress. The activity of FoxO proteins is differentially controlled in specific tissues according to oxidative stress intensity (external stimuli) through the modification of protein levels, subcellular localization, DNA-binding, and transcriptional activity of FoxO. In cases of medium oxidative stress stimuli, FoxOs proteins mediate protective cellular mechanisms by increasing the expression of ROS scavengers. On the other hand, under high oxidative stress stimuli, FoxOs promote cell growth inhibition (by enhancing the expression of various CDK inhibitors) or apoptosis (pro-apoptotic genes are activated). ATG12, autophagy related 12; BBC3, BCL-2-binding component 3 gene; BCL2L11, Bcl-2-like protein 11, commonly called BIM; Bcen1, beclin 1; BCL6, B cell lymphoma 6; BNIP3, BCL2 Interacting Protein 3; CAT, catalase; CCND1, cyclin D1; CCNG2, cyclin G2; CDKN1A, cyclin-dependent kinase inhibitor 1A; CDKN1B, cyclin-dependent kinase inhibitor 1B; CDKN2A, cyclin-dependent kinase inhibitor 2A; CDKN2B, cyclin-dependent kinase inhibitor 2B; FASLG, Fas ligand; FoxO, forkhead box O protein; GABARAPL1, GABA type A receptor associated protein like 1; GADD45A, growth arrest and DNA damage inducible alpha; GPx, glutathione peroxidase; Mn-SOD, manganese superoxide dismutase; PMAIP1, phorbol-12-myristate-13-acetate-induced protein 1; PRDX3, peroxiredoxin 3; PRDX5, peroxiredoxins 5; PTEN, induced putative kinase 1; PUMA, p53 up-regulated modulator of apoptosis; p15; p19; p21; p27; p53, up-regulated modulator of apoptosis; p130; RBL2, RB transcriptional corepressor like 2; SENP, sentrin-specific protease 1; TNF, tumor necrosis factor; TNFSF10, tumor necrosis factor superfamily member 10; TRAIL, tumor necrosis factor-related apoptosis-inducing ligand; TrxR2, mitochondrial thioredoxin reductase; Trx2, mitochondrial thioredoxin; Zn-SOD, zinc superoxide dismutase. *For a review of FOXO-regulated genes, see [38]. The authors created this figure by adapting images from Servier Medical Art Commons Attribution 3.0 Unported License (http://smart.servier.com)
Regulatory mechanisms of FoxO3 expression and activity
FoxOs are transcriptional regulators that activate gene expression in most cases. Their activities and cellular functions are regulated by various mechanisms, such as non-coding RNAs (ncRNAs), protein–protein interaction, and PTMs, such as phosphorylation, acetylation, ubiquitination, and methylation [39], as well as the oxidative modifications [40, 41].
Post-translational modification
Of particular interest to human health, FoxO3 is under the control of the phosphatidylinositol 3-kinase (PI3K)/protein kinase B (AKT) signaling pathway, whose activation results in the phosphorylation at three conserved residues (Thr32, Ser253, and Ser315) of FoxO3 [42]. This PTM causes FoxO3 exclusion from the nucleus, and its association with the chaperone 14–3-3, ultimately blocking re-entry into the nucleus [43, 44]. Hence, contrary to PI3K/AKT, other signaling pathways can positively regulate FoxO3, for example, through stress-kinase (JNK, MST1)-mediated phosphorylation [16, 21]. This antagonistic signaling pathway occurs in response to oxidative stress. Thus, in this case, the phosphorylation of FoxO3 by MST1 or JNK at alternative PTM sites dissociates 14–3-3, promoting FoxO3’s localization to the nucleus. In other words, in the absence of AKT phosphorylation, the nuclear accumulation of FoxO3 facilitates its interaction with gene regulatory regions, inducing the expression of its target genes. However, only this subcellular localization per se presumably does not result in the total transcriptional activity of FoxO3 [45].
Other kinases, such as serum- and glucocorticoid-inducible kinase (SGK), cyclin-dependent kinases (CDKs), and mitogen-activated protein kinase (MAPK) can also phosphorylate FoxO3 [45]. For example, the mammalian MAPK family is comprised of three well-characterized subfamilies, including extracellular signal-regulated kinase (ERK) [46], which can directly phosphorylate FoxO3 at three different sites (Ser294, Ser344, and Ser425), leading to its degradation in a murine double minute 2 (MDM2)-dependent manner [47]. From this data, it is possible to observe that each kinase recognizes specific motifs within FoxO3, and thus, the phosphorylation can lead to opposing effects depending on the target residue.
Acetylation is another widely occurring dynamic PTM that modulates the functions of proteins [48]. In regards to FoxO3 role, its acetylation at Lys242 and Lys245 sites by calcium response element-binding protein (CBP)/p300 significantly reduces their DNA-binding capacity and induces their cytoplasmic localization [49]. It is noteworthy that the effect of acetylation is negatively regulated by histone deacetylases (HDACs), which remove the acetyl groups from histones and non-histone proteins through an enzymatic reaction [50]. For instance, Sirtuin 1 (SIRT1)—a subclass of HDACs with nicotinamide adenine dinucleotide-dependent deacetylation activity, was reported to maintain FoxO3 nuclear localization, following exposure to stress stimuli, by mediating its deacetylation via directly interacting with FoxO3 [51].
Protein methylation is also a reversible process that plays a crucial role in modulating protein characteristics, such as activities, translation, and localization [52]. For example, Calnan et al. demonstrated that FoxO3 methylation by the SET domain containing lysine methyltransferase 9 (Set9) at Lys270 and Lys271 resulted in the reduction of the DNA-binding activity and transactivation of FoxO3 [53]. Ubiquitination is a reversible PTM whose primary function is to mediate protein degradation via the ubiquitin–proteasome pathway [54]. In this way, ubiquitin–proteasome-mediated protein degradation plays a crucial role in regulating several cellular processes, such as cell cycle progression, transcriptional regulation, and DNA repair [55]. Thus, the interplay between molecular redox signaling and the ubiquitin–proteasome system are intertwined to pathophysiological processes in human diseases [56]. For example, constitutive photomorphogenic 1 (COP1) promotes the ubiquitination and degradation of FoxO3, decreasing the expression of its target genes [57, 58]. Another essential and complex PTM is glycosylation. This PTM plays a crucial role in regulating FOXO3 substrate structure, function, and physical properties [59]. The most common mechanisms of protein glycosylation are N-glycosylation and O-glycosylation [60]. Shin et al. demonstrated the occurrence of O-glycosylation sites in the FoxO3 transactivation domain. Additionally, they showed that the O-glycosylation at Ser284 significantly inhibited p21-mediated cancer cell growth by targeting the MDM2-p53-p21 axis [61].
Furthermore, in redox signaling, low levels of ROS can cause the oxidation of specific cysteine-thiols, which can both activate [62] or inactivate [63] proteins. This signaling is an exciting concept, as it allows the redox state-dependent regulation of TFs by introducing a covalent bond with cofactors that, under reducing conditions, would hardly interact [41]. Putker et al. demonstrated that FoxO3 forms a disulfide-dependent heterodimer with the nuclear import receptors, Importin-7 (IPO7), and Importin-8 (IPO8). These interactions are required for efficient nuclear import of FoxO3 under oxidative conditions (i.e., the interaction required for ROS-induced nuclear translocation of FoxO3). Thus, the authors proposed that ROS could directly regulate FoxO3 nuclear importation by mediating its heterodimerization in a redox-sensitive and disulfide-dependent manner through FoxO3’s cysteine oxidation [64].
Meanwhile, Hopkins et al. demonstrated that FoxO3's disulfide heterodimer with PRDX1 also influences the nuclear localization of this TF. Thus, allowing a rapid and precise regulation of FoxO3 in response to oxidative stress. The authors propose that PRDX1 constitutes an essential step for maintaining a redox signaling-dependent cytoplasmic reservoir of FoxO3 that is readily available in the face of high levels of H2O2 [65]. This observation allowed FoxO3s proteins to be classified as "Speroxiredoxinylated", a term coined to demonstrate the interaction between peroxiredoxins with redox reaction cysteines in general [66].
These examples show that FoxO3 functions are affected via distinct mechanisms. Thus, demonstrating that these PTM patterns produce specific biological effects. Therefore, as exemplified above, these reversible PTMs are dynamic and can modulate FoxO3 function by altering its subcellular localization and changing its stability and DNA-binding affinity [67]. These PTM are also affected by redox-regulatory processes (i.e., oxidative inactivation of Akt [68]), which adds another layer of complexity associated with FoxO regulation. As an example, the phosphorylation mediated by PI3K/AKT pathway is affected by ROS at several levels, including oxidative inhibition of protein tyrosine phosphatase-1B (PTB-1B), or of the lipid and protein phosphatase, PTEN, and even oxidative inactivation of AKT was described (reviewed in [68, 69].
Non‑coding RNAs influence FoxO3 regulation
According to the ENCODE (Encyclopedia of DNA Elements) project and later reports, about 80% of the human genome can be transcribed into non‑coding RNAs (ncRNAs). In general, ncRNAs are a range of RNA molecules that act on multiple biological processes, pathological or physiological, through regulating gene expression or PTM. These molecules are derived from eukaryotic transcription from different genomic regions and RNA processing that produces various ncRNA species that are grouped into different categories according to size and function, such as long ncRNAs (lncRNAs), microRNAs (miRNAs), circular RNAs (circRNAs), and others (reviewed in [70]). In the last few years, it has become clear that such molecules significantly influence the activity and expression of FOXO in different pathological conditions.
It is well established that different miRNAs can regulate FOXO transcripts in various processes due to their pleiotropic influence, such as in neurodegenerative diseases, longevity, cancer, and many others [16]. Different miRNAs targeting FOXO mRNAs are involved in tumor promotion, growth, or metastasis, such as miR-182. Under physiological conditions, miR-182 can down-regulate FOXO expression, allowing cell proliferation and cycle progression. On the other hand, when inhibition of proliferation, cell cycle arrest, or apoptosis is intended, a down-regulation of miR-182 may be required. Examples of miR-182 action occur in lung cancer [71] and melanoma [72]. Furthermore, researchers have shown that miR-182 also contributes to FOXO3 regulation in skeletal muscle during chronic diseases associated with elevated glucocorticoid production, such as diabetes and chronic kidney disease [73].
He et al. demonstrated that MiR-25 could directly target the 3′UTR of FOXO3 mRNA, inhibiting its expression and resulting in enhanced resistance of gastric cancer cells to cisplatin [74]. A similar result was demonstrated in colorectal cancer using another miRNA, the miR153 [75]. Moreover, in another report about this later type of cancer, miR-592 promotes metastasis, in part, by targeting FOXO3 [76]. The direct bind of MiR-96 to the 3′-UTR of FOXO3 mRNA inhibits its function [77]. It can also promote, in response to collagen matrix via reducing FOXO3 and its targets (p27, p21, and Bim), the pathologically altered idiopathic pulmonary fibrosis (IPF) phenotype [78].
In regards to the lncRNAs, a recent study demonstrated that FOXO3 expression could be negatively regulated by miR-27a-3p and positively regulated by lncRNA X inactivate‑specific transcript (XIST), an RNA associated with cerebral ischemia/reperfusion ( I/R) injury that binds with miR-27a-3p to upregulate FOXO3 [79]. Wang et al. revealed that lncRNA plasmacytoma variant translocation 1 (PVT1), directly interacting with FoxO3, can modulate its transcription activity. The enhanced FoxO3 activity was achieved by the knockdown of PVT1, which considerably downregulated its phosphorylation level by facilitating SCP4-mediated FoxO3 dephosphorylation. The upregulation of FoxO3, due to PVT1 knockdown, also enabled the apoptosis of granulosa cells [80].
Moreover, overexpression of the lncRNA growth arrest-specific transcript 5 (GAS5) resulted in a significant elevation of FoxO3 protein level, which was attenuated by the addition of miR-9, demonstrating that GAS5 promoted FOXO3 expression by competitively sponging miR-9. Meanwhile, the knockdown of GAS5 significantly reduced the expression of FoxO3 protein, and the depletion of miR-9 in bEnd restored it [81]. Zhai et al. identified a new lncRNA, URRCC, as a part of a feedback loop with EGFL7/P-AKT/FoxO3 signaling. In renal cell carcinoma samples, URCC expression is upregulated, promoting clear cell renal carcinoma (ccRCC) cell proliferation, invasion, and reduced overall survival of ccRCC patients. Mechanistically, URRCC can acetylate histone H3 of EGFL7 promoter, increasing AKT signaling pathway and consequently suppressing downstream FoxO3 signaling through AKT phosphorylation, which was demonstrated to enhance cell proliferation and invasion in vitro and in vivo. On the other hand, FoxO3 can directly bind to the URRCC promoter region, downregulating its expression [82].
Lastly, studies have shown that circRNAs can be crucial modulators of FoxOs. Recently, Yu et al. demonstrated that circRNA CRIM1 overexpression significantly repressed the migration and invasion of bladder cancer cells by up-regulating FOXO3 expression via sponging miR-182, a miRNA capable of modulating FoxO3 activity. Moreover, miR-182 expression was elevated in bladder cancer tissues and cell lines, while CRIM1 and FOXO3 expressions were decreased [83].
Another layer of complexity arises from the fact that circ-FOXO3 can modulate FoxO3 activity. Du et al. presented some exciting findings about circ-FOXO3. Their study showed that in patient tumor samples and a panel of cancer cells, circ-FOXO3 was minimally expressed. However, circ-FOXO3 expression significantly increased during cancer cell apoptosis, which can be explored as the possibility of inhibiting tumor growth with the delivery of circ-FOXO3 plasmid. Moreover, silencing endogenous circ-FOXO3 contributed to cell viability, although ectopic expression of this RNA led to stress-induced apoptosis and repression of the growth of tumor xenografts. In addition, circ-FOXO3 expression elevated FoxO3 protein levels but inhibited p53 levels by promoting MDM2-induced p53 ubiquitination and degradation, leading to a decrease in p53. Due to low binding affinity to FoxO3, circ-FOXO3 avoided MDM2 from inducing FoxO3 ubiquitination and degradation, maintaining high levels of this TF that subsequently caused cell apoptosis by upregulation of its downstream target PUMA [84].
Overview of the relationship between free radicals and disease
As previously discussed, oxidative stress emerges from an imbalance of oxidative to reducing species, being also better defined as a perturbation of redox signaling [4]. The redox imbalance from chronic oxidative stress leads to significant PTM oxidative modifications in crucial biomolecules, such as lipid peroxidation, protein carbonylation, carbonyl (aldehyde/ketone) adduct formation, nitration, sulfoxidation, DNA impairment such as strand breaks, or nucleobase oxidation yielding 8-oxo-20-deoxyguanosine. Moreover, with the accumulation of these damaged biomolecules, healthy cells of the body lose their function and structure (reviewed in [85]).
In recent decades, the significance of oxidative stress has become increasingly recognized; thus, we can find stress-related diseases in virtually every organ [86]. Therefore, it is widely accepted that oxidative stress influences the establishment of multiple mechanisms by which oxidants contribute to cellular damage in various diseases, including atherosclerosis, chronic obstructive pulmonary disease (COPD), Alzheimer’s disease, and cancer [87]. In other words, it is essential to highlight the extent to which oxidative stress participates in the pathology of such diseases is quite variable. However, the effectiveness of therapeutic alternatives that increase antioxidant defense is still limited to some conditions. Thus, this section will focus on evidencing the relationships between oxidative stress and FoxO3 in different diseases.
As stated above, one of the primary mechanisms through which oxidative stress contributes to a disease involves the production of ROS (e.g., •OH, ONOO− and HOCl) that directly oxidize macromolecules, including membrane lipids, structural proteins, enzymes, and nucleic acids, leading to aberrant cell function and death. Another important mechanism of oxidative stress is aberrant redox signaling, in which non-physiological production of ROS (e.g., H2O2) can cause redox signaling to go awry [1]. Despite the role of oxidative stress in many diseases not being incompletely understood, a tentative categorization has been made: first, oxidative stress as the primary cause of pathology (e.g., atherosclerosis—oxidative stress is responsible for the conversion of LDL cholesterol into the oxidized-LDL, which has a crucial role in the development of atherosclerosis); second, oxidative stress as the secondary contributor to disease progression (such as in COPD, hypertension, and Alzheimer disease by disturbing various signaling pathways and thus, affecting multiple biological processes) (reviewed in [88]).
Additionally, in diseases caused by oxidative stress, the wide range of the pathological role of free radicals was didactically categorized, by some authors, into two major groups [89]. On one side, we have the diseases characterized by “inflammatory oxidative conditions” and enhanced activity of either NAD[P]H oxidase (leading to atherosclerosis and chronic inflammation) or xanthine oxidase-induced formation of ROS (implicated in ischemia and reperfusion injury). In this group, we can see that the reaction of the biomolecules and the free radicals will lead (directly or indirectly) to the disease, such as in the case of atherosclerosis, in which the malondialdehyde (MDA), a product of lipid peroxidation, reacts with low-density lipoproteins [90].
On the other hand, there are diseases characterized by pro-oxidants shifting the thiol/disulfide redox state and impaired glucose tolerance, also known as “mitochondrial oxidative stress” conditions (cancer and diabetes mellitus). To further exemplify, we can take cancer as a model. ROS contributes to the initiation and progression of carcinogenesis through the infliction of ROS-dependent mutations in DNA, which include base modifications to the activation of oncogenes [91].
The intrinsic relationship between the severity of different diseases and the imbalance between pro-oxidants and natural defenses suggests that antioxidant therapy represents a promising path for treatment. This strategy could be achieved by two means, through the use of natural antioxidants originating from an exogenous source, such as foods or dietary supplements (e.g., vitamins C and E) [92] or the synthesis of endogenous antioxidants, such as SOD [93]. The problem with the first option is known as the “antioxidant paradox”, which is the adverse effect resulting from the ingestion of a high concentration of antioxidants, as seen in some studies where the antioxidant treatment aggravated the oxidative damage and worsened the patient's condition (reviewed in [94]). The second alternative also presents challenges because proteins and enzymes generally make very poor drugs. Among the reasons for this “poverty”, we can cite the high cost of production, the possible immunogenicity, problems associated with purification and stability, non-availability by oral administration, and poor pharmacokinetic properties, including toxic, mutagenic effects, and possible side effects [95, 96].
In the search for another alternative, TFs that act on energy efficiency, cell resistance to stress, and also cell repair, such as FoxO3, has been gaining prominence due to their role in the redox code. The term ‘‘Redox Code’’ is a four principles code that applies to the redox organization of cells, tissues, and organisms, ultimately extending to all living matter (extensively reviewed in [13]). This code defines the operations of genetic codes and histones in the organizational structure, differentiation, and adaptation of an organism [13]. Therefore, they act in the modulation of complex networks that control signaling and cellular metabolism, thus being a fascinating mechanism in the development of new therapeutic strategies for diseases in which oxidative stress and inflammation play an essential role [97,98,99].
The FoxO3 proteins are considered a desirable therapeutic target because of their integral ability to control cell proliferation, metabolism, and survival [100, 101]. Therefore, FoxO3 activators, such as Resveratrol, are currently gaining attention. Studies performed by Franco et al. evidence the beneficial effects of its use [102]. In this study, this polyphenolic-stilbene enhanced erythroid cell maturation and decreased red cell membrane oxidative damage and anemia in β-thalassemic mice. In addition, resveratrol upregulates the expression of antioxidant enzymes such as CAT and PRDX2 via activation of FoxO3. The results indicate that Resveratrol inhibits AKT resulting in FoxO3 activation with upregulation of cytoprotective systems allowing the erythroid precursors to survive the oxidative damage and proceed with the differentiation. Thus, considering the possibility of using this complementary tool in treating diseases with chronic stress oxidative, such as β-thalassemia [102].
Other pharmaceutical compounds approved for other uses have been shown to activate FoxO3. For example, Bepridil and Trifluoperazine could promote FoxO3 translocation to the nucleus by inhibiting AKT phosphorylation [103]. Metformin is another promising compound. This drug can induce AMPK-mediated phosphorylation and nuclear translocation of FoxO3 [104]. This metformin-induced pathway is also shown to promote Trx transcription (thru activation of FoxO3 and subsequently upregulation of Trx) and thus causes a decrease in ROS levels [105]. Hence, the AMPK-FoxO3-Trx axis may be an essential defense mechanism against excessive ROS production induced by stress and could be a therapeutic target in treating diseases.
As demonstrated in the studies above, FoxO3 plays a central role in antioxidant defense and through its activation by different drugs. Therefore, it is a promising research field for developing new therapeutic strategies to fight chronic oxidative stress in several diseases. Table 1 shows various stress-related disorders and how FoxO3 can be related to the cause or therapeutic target concerning such conditions.
Conclusion
There is considerable interest in understanding the mechanisms underlying the role of oxidative stress not only in disease development but also in life-history trade-offs, as redox signaling and oxidative damage regulate essential physiological functions [11], as stated by the “Redox signaling hypothesis of life history”. Thus, this hypothesis points to the importance of the cell-regulatory systems and how the generation of molecular oxidative damage is the mechanism that drives covariation among life history traits and self-maintenance (reviewed in detail in [158]).
Therefore, despite the challenges and limitations in targeting oxidative stress, the continuous development of this study field is essential to establishing alternative therapeutic strategies that offer meaningful ways to prevent or reduce pathology. One situation in which FoxO3 versatility highlights its importance. Recent research in human health and disease provides new insights into the molecular mechanisms underlying the role and regulation of this essential TF. In addition, comprehending the FoxO3 role as a crucial element in maintaining the equilibrium that supports life will help understand the molecular underpinning of age-associated diseases and maybe lifespan and how to deal with it.
Hence, the continuous search for identifying small pharmaceutical or nutraceutical molecules that directly or indirectly activate FoxO3 is of great interest to the aging and human wellness research field. Thus, the discovery of several other FoxO3 activators and pathways leading to its activation will occur in the coming years, leading to the expected significant development in the therapeutic field, allowing more precise pharmacological intervention with lower risks of side effects. Thus, with continued investment in this research area, the suitable FoxO3 activator for several health issues is expected to reach the general population for prophylactic use in the coming decades [159].
For this to be possible, we reinforce that studies that detail the molecular mechanism of FOXO3 gene expression modulation and its impact are required. The discovery of these action mechanisms can potentially be used in the treatment and management of many diseases, such as diabetes, cancer, neurodegeneration, and heart disease. Lastly, it can help to delay the aging process and minimize the side effects of aging.
Availability of data and materials
Not applicable.
References
Sies H, Berndt C, Jones DP (2017) Oxidative stress. Annu Rev Biochem 86:715–748. https://doi.org/10.1177/0148607111434963
Schieber M, Chandel NS (2014) ROS function in redox signaling. Curr Biol 24:453–462. https://doi.org/10.1016/j.cub.2014.03.034.ROS
Halliwell B (2006) Reactive species and antioxidants. Redox biology is a fundamental theme of aerobic life. Plant Physiol 141:312–322. https://doi.org/10.1104/pp.106.077073.312
Pisoschi AM, Pop A (2015) The role of antioxidants in the chemistry of oxidative stress: a review. Eur J Med Chem 97:55–74. https://doi.org/10.1016/j.ejmech.2015.04.040
Harman D (1956) Aging: a theory on free radical radiation chemistry. J Gerontol 11:298–300
Balaban RS, Nemoto S, Finkel T (2005) Mitochondria, oxidants, and aging. Cell 120:483–495. https://doi.org/10.1016/j.cell.2005.02.001
Ray PD, Huang B-W, Tsuji Y (2012) Reactive oxygen species (ROS) homeostasis and redox regulation in cellular signaling. Cell Signal 24:981–990. https://doi.org/10.1016/j.cellsig.2012.01.008
Schirrmacher V (2021) Less can be more: the hormesis theory of stress adaptation in the global biosphere and its implications. Biomedicines 9
Calabrese EJ (2018) Hormesis: path and progression to significance Int J Mol Sci 19. https://doi.org/10.3390/ijms19102871
Nathan C (2003) Specificity of a third kind: reactive oxygen and nitrogen intermediates in cell signaling. J Clin Invest 111:769–778. https://doi.org/10.1172/jci200318174
D’Autréaux B, Toledano MB (2007) ROS as signalling molecules: mechanisms that generate specificity in ROS homeostasis. Nat Rev Mol Cell Biol 8:813–824. https://doi.org/10.1038/nrm2256
Mittler R, Vanderauwera S, Suzuki N et al (2011) ROS signaling: the new wave? Trends Plant Sci 16:300–309. https://doi.org/10.1016/j.tplants.2011.03.007
Jones DP, Sies H (2015) The Redox Code. Antioxidants Redox. Signal 23:734–746. https://doi.org/10.1089/ars.2015.6247
Ursini F, Maiorino M, Forman HJ (2016) Redox homeostasis: The Golden Mean of healthy living. Redox Biol 8:205–215. https://doi.org/10.1016/j.redox.2016.01.010
Klotz LO, Sánchez-Ramos C, Prieto-Arroyo I et al (2015) Redox regulation of FoxO transcription factors. Redox Biol 6:51–72. https://doi.org/10.1016/j.redox.2015.06.019
Calnan DR, Brunet A (2008) The FoxO code. Oncogene 27:2276–2288. https://doi.org/10.1038/onc.2008.21
Lehmann OJ, Sowden JC, Carlsson P et al (2003) Fox’s in development and disease. Trends Genet 19:339–344. https://doi.org/10.1016/S0168-9525(03)00111-2
Brent MM, Anand R, Marmorstein R (2008) Structural Basis for DNA Recognition by FoxO1 and its Regulation by Post-Translational Modification. Structure 16:1407–1416. https://doi.org/10.1016/j.str.2008.06.013
Hosaka T, Biggs WH, Tieu D et al (2004) Disruption of forkhead transcription factor (FOXO) family members in mice reveals their functional diversification. Proc Natl Acad Sci U S A 101:2975–2980. https://doi.org/10.1073/pnas.0400093101
Kodani N, Nakae J (2020) Tissue-specific metabolic regulation of FOXO-binding protein: FOXO Does Not Act Alone. Cells 9:702
Eijkelenboom A, Burgering BMT (2013) FOXOs: signalling integrators for homeostasis maintenance. Nat Rev Mol Cell Biol 14:83–97. https://doi.org/10.1038/nrm3507
Martins R, Lithgow GJ, Link W (2016) Long live FOXO: unraveling the role of FOXO proteins in aging and longevity. Aging Cell 15:196–207. https://doi.org/10.1111/acel.12427
Fasano C, Disciglio V, Bertora S et al (2019) Foxo3a from the nucleus to the mitochondria: a round trip in cellular stress response. Cells 8:1–28. https://doi.org/10.3390/cells8091110
Kops GJPL, Dansen TB, Polderman PE et al (2002) Forkhead transcription factor FOXO3a protects quiescent cells from oxidative stress. Nature 419:316–321. https://doi.org/10.1038/nature01036
Marinkovic D, Zhang X, Yalcin S et al (2007) Foxo3 is required for the regulation of oxidative stress in erythropoiesis. 117:2133–2144. https://doi.org/10.1172/JCI31807DS1
Nemoto S, Finkel T (2002) Redox regulation of forkhead proteins through a p66shc-dependent signaling pathway. Science (80- ) 295:2450–2452. https://doi.org/10.1126/science.1069004
Chiribau CB, Cheng L, Cucoranu IC et al (2008) FOXO3A regulates peroxiredoxin III expression in human cardiac fibroblasts. J Biol Chem 283:8211–8217. https://doi.org/10.1074/jbc.M710610200
Olmos Y, Sánchez-Gómez FJ, Wild B et al (2013) SirT1 regulation of antioxidant genes is dependent on the formation of a FoxO3a/PGC-1α complex. Antioxidants Redox Signal 19:1507–1521. https://doi.org/10.1089/ars.2012.4713
Huang H, Regan KM, Lou Z et al (2006) CDK2-dependent phosphorylation of FOXO1 as an apoptotic response to DNA damage. Science (80-) 314:294–297. https://doi.org/10.1126/science.1130512
Yuan Z, Becker EBE, Merlo P et al (2008) Activation of FOXO1 by Cdk1 in cycling cells and postmitotic neurons. Science (80-) 319:1665–1668. https://doi.org/10.1126/science.1152337
Jeong OS, Chae YC, Jung H et al (2016) Long noncoding RNA linc00598 regulates CCND2 transcription and modulates the G1 checkpoint. Sci Rep 6:1–11. https://doi.org/10.1038/srep32172
Dall’Acqua A, Sonego M, Pellizzari I et al (2017) CDK6 protects epithelial ovarian cancer from platinum‐induced death via FOXO3 regulation. EMBO Mol Med 9:1415–1433. https://doi.org/10.15252/emmm.201607012
Sunters A, Fernández De Mattos S, Stahl M et al (2003) FoxO3a transcriptional regulation of bim controls apoptosis in paclitaxel-treated breast cancer cell lines. J Biol Chem 278:49795–49805. https://doi.org/10.1074/jbc.M309523200
Essafi A, Fernández De Mattos S, Hassen YAM et al (2005) Direct transcriptional regulation of Bim by FoxO3a mediates STI571-induced apoptosis in Bcr-Abl-expressing cells. Oncogene 24:2317–2329. https://doi.org/10.1038/sj.onc.1208421
Kok S, Lin L, Hou K et al (2013) Simvastatin inhibits cysteine-rich protein 61 expression in rheumatoid arthritis synovial fibroblasts through the regulation of SIRT1/FoxO3a signaling. Arthritis Rheum 65:639–649. https://doi.org/10.1002/art
Matsuzaki H, Lee S, Maeda M et al (2016) FoxO1 regulates apoptosis induced by asbestos in the MT-2 human T-cell line. J Immunotoxicol 13:620–627. https://doi.org/10.3109/1547691X.2016.1143539
Shukla S, Sharma A, Pandey VK et al (2016) Concurrent acetylation of FoxO1/3a and p53 due to sirtuins inhibition elicit Bim/PUMA mediated mitochondrial dysfunction and apoptosis in berberine-treated HepG2 cells. Toxicol Appl Pharmacol 291:70–83. https://doi.org/10.1016/j.taap.2015.12.006
Van Der Vos KE, Coffer PJ (2011) The extending network of FOXO transcriptional target genes. Antioxidants Redox Signal 14:579–592. https://doi.org/10.1089/ars.2010.3419
Walsh CT, Garneau-Tsodikova S, Gatto GJ (2005) Protein posttranslational modifications: The chemistry of proteome diversifications. Angew Chemie - Int Ed 44:7342–7372. https://doi.org/10.1002/anie.200501023
Dickinson BC, Chang CJ (2011) Chemistry and biology of reactive oxygen species in signaling or stress responses. Nat Chem Biol 7:504–511. https://doi.org/10.1038/nchembio.607
Poole LB, Nelson KJ (2008) Discovering mechanisms of signaling-mediated cysteine oxidation. Curr Opin Chem Biol 12:18–24. https://doi.org/10.1016/j.cbpa.2008.01.021
Brunet A, Bonni A, Zigmond MJ et al (1999) Akt promotes cell survival by phosphorylating and inhibiting a forkhead transcription factor. Cell 96:857–868
Hannenhalli S, Kaestner KH (2009) The evolution of Fox genes and their role in development and disease. Nat Rev Genet 10:233–240. https://doi.org/10.1038/nrg2523
Obsilova V, Vecer J, Herman P et al (2005) 14–3-3 Protein interacts with nuclear localization sequence of forkhead transcription factor FoxO4. Biochemistry 44:11608–11617. https://doi.org/10.1021/bi050618r
Gui T, Burgering BMT (2021) FOXOs: masters of the equilibrium. FEBS J 1–22. https://doi.org/10.1111/febs.16221
García-Hernández L, García-Ortega MB, Ruiz-Alcalá G et al (2022) The p38 MAPK components and modulators as biomarkers and molecular targets in cancer. Int J Mol Sci 23. https://doi.org/10.3390/ijms23010370
Yang JY, Zong CS, Xia W et al (2008) ERK promotes tumorigenesis by inhibiting FOXO3a via MDM2-mediated degradation. Nat Cell Biol 10:138–148. https://doi.org/10.1038/ncb1676
Blasl AT, Schulze S, Qin C et al (2022) Post-translational lysine ac(et)ylation in health, ageing and disease
Matsuzaki H, Daitoku H, Hatta M et al (2005) Acetylation of Foxo1 alters its DNA-binding ability and sensitivity to phosphorylation. Proc Natl Acad Sci U S A 102:11278–11283. https://doi.org/10.1073/pnas.0502738102
Liu H (2021) The roles of histone deacetylases in kidney development and disease. Clin Exp Nephrol 25:215–223. https://doi.org/10.1007/s10157-020-01995-5
Brunet A, Sweeney LB, Sturgill JF et al (2004) Stress-dependent regulation of FOXO transcription factors by the SIRT1 deacetylase. Science 303:2011–2015. https://doi.org/10.1126/science.1094637
Di Blasi R, Blyuss O, Timms JF et al (2021) Non-histone protein methylation: biological significance and bioengineering potential. ACS Chem Biol 16:238–250. https://doi.org/10.1021/acschembio.0c00771
Calnan DR, Webb AE, White JL et al (2012) Methylation by Set9 modulates FoxO3 stability and transcriptional activity. Aging (Albany NY) 4:462–479. https://doi.org/10.18632/aging.100471
Kudriaeva AA, Belogurov AA (2019) Proteasome: a nanomachinery of creative destruction. Biochemistry (Moscow) 84(1): 159-192
Xieac Y, Wangd M, Xia M et al (2022) Ubiquitination regulation of aerobic glycolysis in cancer. Life Sci 292:120322. https://doi.org/10.1016/j.lfs.2021.119552
Bernardo VS, Torres FF, Zucão ACA, da Silva DGH (2021) The interplay between molecular redox signaling and the ubiquitin-proteasome system: relevant aspects related to pathophysiological processes in human diseases. In: DUNCAN LT (ed) Advances in Health and Diseases, 44th ed. Nova Science Publishers, Inc, New York, pp 1–67
Fu W, Ma Q, Chen L et al (2009) MDM2 acts downstream of p53 as an E3 ligase to promote FOXO ubiquitination and degradation. J Biol Chem 284:13987–14000. https://doi.org/10.1074/jbc.M901758200
Choi HH, Zou S, Wu JL et al (2020) EGF relays signals to COP1 and facilitates FOXO4 degradation to promote tumorigenesis. Adv Sci 7:1–17. https://doi.org/10.1002/advs.202000681
Liu Y, Ao X, Jia Y et al (2022) The FOXO family of transcription factors: key molecular players in gastric cancer. J Mol Med 100:997–1015. https://doi.org/10.1007/s00109-022-02219-x
Pirillo A, Svecla M, Catapano AL et al (2021) Impact of protein glycosylation on lipoprotein metabolism and atherosclerosis. Cardiovasc Res 117:1033–1045. https://doi.org/10.1093/cvr/cvaa252
Shin H, Cha HJ, Na K et al (2018) O-GlcN acylation of the tumor suppressor FOXO3 triggers aberrant cancer cell growth. Cancer Res 78:1214–1224. https://doi.org/10.1158/0008-5472.CAN-17-3512
Guo Z, Kozlov S, Lavin MF et al (2010) ATM activation by oxidative stress. Science (80-) 330:517–521. https://doi.org/10.1126/science.1192912
Anastasiou D, Poulogiannis G, Asara JM et al (2012) Inhibition of pyruvate kinase M2 by reactive oxygen species contributes to cellular antioxidant responses. Science (80-) 334:1278–1283. https://doi.org/10.1126/science.1211485.Inhibition
Putker M, Vos HR, Van Dorenmalen K et al (2015) Evolutionary acquisition of cysteines determines FOXO paralog-specific redox signaling. Antioxidants Redox Signal 22:15–28. https://doi.org/10.1089/ars.2014.6056
Hopkins BL, Nadler M, Skoko JJ et al (2018) A peroxidase peroxiredoxin 1-specific redox regulation of the novel FOXO3 microRNA target let-7. Antioxidants Redox Signal 28:62–77. https://doi.org/10.1089/ars.2016.6871
van Dam L, Pagès-Gallego M, Polderman PE et al (2021) The human 2-cys peroxiredoxins form widespread, cysteine-dependent-and isoform-specific protein-protein interactions. Antioxidants 10. https://doi.org/10.3390/antiox10040627
Ao X, Ding W, Zhang Y et al (2020) TCF21: a critical transcription factor in health and cancer. J Mol Med 98:1055–1068. https://doi.org/10.1007/s00109-020-01934-7
Klotz LO, Steinbrenner H (2017) Cellular adaptation to xenobiotics: Interplay between xenosensors, reactive oxygen species and FOXO transcription factors. Redox Biol 13:646–654. https://doi.org/10.1016/j.redox.2017.07.015
Tauber S, Steinbrenner H, Klotz L-O (2020) FoxO transcription factors in the control of redox homeostasis and fuel metabolism. Elsevier Inc
Zhang P, Wu W, Chen Q, Chen M (2019) Non-Coding RNAs and their Integrated Networks. J Integr Bioinform 16:1–12. https://doi.org/10.1515/jib-2019-0027
Yang WB, Chen PH, Hsu TI et al (2014) Sp1-mediated microRNA-182 expression regulates lung cancer progression. Oncotarget 5:740–753. https://doi.org/10.18632/oncotarget.1608
Segura MF, Hanniford D, Menendez S et al (2009) Aberrant miR-182 expression promotes melanoma metastasis by repressing FOXO3 and microphthalmia-associated transcription factor. Proc Natl Acad Sci U S A 106:1814–1819. https://doi.org/10.1073/pnas.0808263106
Hudson MB, Rahnert JA, Zheng B et al (2014) miR-182 attenuates atrophy-related gene expression by targeting FoxO3 in skeletal muscle. Am J Physiol - Cell Physiol 307:314–319. https://doi.org/10.1152/ajpcell.00395.2013
He J, Qi H, Chen F, Cao C (2017) MicroRNA-25 contributes to cisplatin resistance in gastric cancer cells by inhibiting forkhead box O3a. Oncol Lett 14:6097–6102. https://doi.org/10.3892/ol.2017.6982
Zhang L, Pickard K, Jenei V et al (2013) MiR-153 supports colorectal cancer progression via pleiotropic effects that enhance invasion and chemotherapeutic resistance. Cancer Res 73:6435–6447. https://doi.org/10.1158/0008-5472.CAN-12-3308
Fu Q, Du Y, Yang C et al (2016) An oncogenic role of miR-592 in tumorigenesis of human colorectal cancer by targeting Forkhead Box O3A (FoxO3A). Expert Opin Ther Targets 20:771–782. https://doi.org/10.1080/14728222.2016.1181753
Lin H, Dai T, Xiong H et al (2010) Unregulated miR-96 induces cell proliferation in human breast cancer by downregulating transcriptional factor FOXO3a. PLoS ONE 5:e15797. https://doi.org/10.1371/journal.pone.0015797
Nho RS, Im J, Ho YY, Hergert P (2014) MicroRNA-96 inhibits Foxo3a function in IPF fibroblasts on type I collagen matrix. Am J Physiol - Lung Cell Mol Physiol 307:L632–L642. https://doi.org/10.1152/ajplung.00127.2014
Zhang H, Xia J, Hu Q et al (2021) Long non-coding RNA XIST promotes cerebral ischemia/reperfusion injury by modulating miR-27a-3p/FOXO3 signaling. Mol Med Rep 24. https://doi.org/10.3892/mmr.2021.12205
Wang F, Chen X, Sun B et al (2021) Hypermethylation-mediated downregulation of lncRNA PVT1 promotes granulosa cell apoptosis in premature ovarian insufficiency via interacting with Foxo3a. J Cell Physiol 236:5162–5175. https://doi.org/10.1002/jcp.30222
Wang L, Niu Y, He G, Wang J (2019) Down-regulation of lncRNA GAS5 attenuates neuronal cell injury through regulating miR-9/FOXO3 axis in cerebral ischemic stroke. RSC Adv 9:16158–16166. https://doi.org/10.1039/c9ra01544b
Zhai W, Zhu R, Ma J et al (2019) A positive feed-forward loop between LncRNA-URRCC and EGFL7/P-AKT/FOXO3 signaling promotes proliferation and metastasis of clear cell renal cell carcinoma. Mol Cancer 18:1–15. https://doi.org/10.1186/s12943-019-0998-y
Yu XY, Ma CQ, Sheng YH (2022) circRNA CRIM1 regulates the migration and invasion of bladder cancer by targeting miR182/Foxo3a axis. Clin Transl Oncol 24:1195–1203. https://doi.org/10.1007/s12094-021-02768-6
Du WW, Fang L, Yang W et al (2017) Induction of tumor apoptosis through a circular RNA enhancing Foxo3 activity. Cell Death Differ 24:357–370. https://doi.org/10.1038/cdd.2016.133
Pisoschi AM, Pop A, Iordache F et al (2020) Oxidative stress mitigation by antioxidants - An overview on their chemistry and influences on health status. Eur J Med Chem 209:112891. https://doi.org/10.1016/j.ejmech.2020.112891
Pala FS, Gürkan H (2008) The role of free radicals in ethiopathogenesis of diseases. Adv Mol Biol 1:1–9
Valko M, Leibfritz D, Moncol J et al (2007) Free radicals and antioxidants in normal physiological functions and human disease. Int J Biochem Cell Biol 39:44–84. https://doi.org/10.1016/j.biocel.2006.07.001
Forman HJ, Zhang H (2021) Targeting oxidative stress in disease: promise and limitations of antioxidant therapy. Nat Rev Drug Discov 20:689–709. https://doi.org/10.1038/s41573-021-00233-1
Sharma N (2014) Free radicals, antioxidants and disease. Biol Med 6:1–6. https://doi.org/10.4172/0974-8369.1000214
Slatter DA, Bolton CH, Bailey AJ (2000) The importance of lipid-derived malondialdehyde in diabetes mellitus. Diabetologia 43:550–557. https://doi.org/10.1007/s001250051342
Waris G, Ahsan H (2006) Reactive oxygen species: role in the development of cancer and various chronic conditions. J Carcinog 5:1–8. https://doi.org/10.1186/1477-3163-5-14
Carlsen MH, Halvorsen BL, Holte K et al (2010) The total antioxidant content of more than 3100 foods, beverages, spices, herbs and supplements used worldwide. Nutr J 9:1–11. https://doi.org/10.1186/1475-2891-9-3
Gao B, Flores SC, Leff JA et al (2003) Synthesis and anti-inflammatory activity of a chimeric recombinant superoxide dismutase: SOD2/3. Am J Physiol - Lung Cell Mol Physiol 284:917–925. https://doi.org/10.1152/ajplung.00374.2002
Halliwell B (2000) The antioxidant paradox. Lancet 355:1179–1180. https://doi.org/10.1016/S0140-6736(00)02075-4
Halliwell B (1991) Drug antioxidant effect. A Basis for Drug Selection? Drugs 42:569–605. https://doi.org/10.1097/00003643-199603000-00035
Augustyniak A, Bartosz G, Čipak A et al (2010) Natural and synthetic antioxidants: An updated overview. Free Radic Res 44:1216–1262. https://doi.org/10.3109/10715762.2010.508495
Levonen A-L, Hill BG, Kansanen E et al (2014) Redox regulation of antioxidants, autophagy, and the response to stress: implications for electrophile therapeutics. Free Radic Biol Med 71:196–207. https://doi.org/10.1038/s41395-018-0061-4
Groeger AL, Freeman BA (2010) Signaling actions of electrophiles: Anti-inflammatory therapeutic candidates. Mol Interv 10:39–50. https://doi.org/10.1124/mi.10.1.7
Yates MS, Kensler TW (2007) Chemopreventive promise of targeting the Nrf2 pathway. Drug News Perspect 20:109–117. https://doi.org/10.1358/dnp.2007.20.2.108343
Orea-Soufi A, Paik J, Bragança J et al (2022) FOXO transcription factors as therapeutic targets in human diseases. Trends Pharmacol Sci 43:1070–1084. https://doi.org/10.1016/j.tips.2022.09.010
Calissi G, Lam EWF, Link W (2021) Therapeutic strategies targeting FOXO transcription factors. Nat Rev Drug Discov 20:21–38. https://doi.org/10.1038/s41573-020-0088-2
Franco SS, De FL, Ghaffari S et al (2014) Resveratrol accelerates erythroid maturation by activation of FoxO3 and ameliorates anemia in beta-thalassemic mice. Haematologica 99:267–275. https://doi.org/10.3324/haematol.2013.090076
Park SH, Chung YM, Ma J et al (2016) Pharmacological activation of FOXO3 suppresses triple-negative breast cancer in vitro and in vivo. Oncotarget 7:42110–42125. https://doi.org/10.18632/oncotarget.9881
Sato A, Sunayama J, Okada M et al (2012) Glioma-Initiating Cell Elimination by Metformin Activation of FOXO3 via AMPK. Stem Cells Transl Med 1:811–824. https://doi.org/10.5966/sctm.2012-0058
Hou X, Song J, Li XN et al (2010) Metformin reduces intracellular reactive oxygen species levels by upregulating expression of the antioxidant thioredoxin via the AMPK-FOXO3 pathway. Biochem Biophys Res Commun 396:199–205. https://doi.org/10.1016/j.bbrc.2010.04.017
Yu W, Gao B, Li N et al (2017) Sirt3 deficiency exacerbates diabetic cardiac dysfunction: Role of Foxo3A- Parkin-mediated mitophagy. BBA - Mol Basis Dis 1863:1973–1983. https://doi.org/10.1016/j.bbadis.2016.10.021
Wu Z, Huang A, Yan J et al (2017) Resveratrol ameliorates cardiac dysfunction by inhibiting apoptosis via the PI3K/Akt/FoxO3a pathway in a rat model of diabetic cardiomyopathy. J Cardiovasc Pharmacol 70:184–193. https://doi.org/10.1097/FJC.0000000000000504
Asadi S, Rahimi Z, Saidijam M et al (2018) Effects of Resveratrol on FOXO1 and FOXO3a genes expression in adipose tissue, serum insulin, insulin resistance and serum SOD activity in type 2 diabetic rats. Int J Mol Cell Med 7:176–184
Zhang Y, Cao Y, Chen J et al (2019) A new possible mechanism by which punicalagin protects against liver injury induced by type 2 diabetes mellitus: upregulation of autophagy via the Akt/FoxO3a signaling pathway. J Agric Food Chem 67:13948–13959. https://doi.org/10.1021/acs.jafc.9b05910
Schinner S, Scherbaum WA, Bornstein SR, Barthel A (2005) Molecular mechanisms of insulin resistance. Diabet Med 22:674–682
Teumer A, Qi Q, Nethander M et al (2016) Genomewide meta-analysis identifies loci associated with IGF-I and IGFBP-3 levels with impact on age-related traits. Aging Cell 15:811–824. https://doi.org/10.1111/acel.12490
Luong N, Davies CR, Wessells RJ et al (2006) Activated FOXO-mediated insulin resistance is blocked by reduction of TOR activity. Cell Metab 4:133–142. https://doi.org/10.1016/j.cmet.2006.05.013
Su B, Liu H, Wang X et al (2009) Ectopic localization of FOXO3a protein in Lewy bodies in Lewy body dementia and Parkinson’s disease. Mol Neurodegener 4:1–5. https://doi.org/10.1186/1750-1326-4-32
Pino E, Amamoto R, Zheng L et al (2014) FOXO3 determines the accumulation α-synuclein and controls the fate of dopaminergic neurons in the substantia nigra. Hum Mol Genet 23:1435–1452
Wong HKA, Veremeyko T, Patel N et al (2013) De-repression of FOXO3a death axis by microRNA-132 and -212 causes neuronal apoptosis in Alzheimer’s disease. Hum Mol Genet 22:3077–3092. https://doi.org/10.1093/hmg/ddt164
Qin W, Zhao W, Ho L et al (2008) Regulation of forkhead transcription factor foxo3a contributes to calorie restriction-induced prevention of Alzheimer ’ s disease-type amyloid neuropathology and spatial memory. Ann N Y Acad Sci 1147:335–347. https://doi.org/10.1196/annals.1427.024
Bellinger FP, He Q, Bellinger MT et al (2008) Association of Selenoprotein P with Alzheimer’s Pathology in Human Cortex. J Alzheimers Dis 15:465–472
Wang H, Quirion R, Little PJ et al (2015) Forkhead box O transcription factors as possible mediators in the development of major depression. Neuropharmacology 99:527–537. https://doi.org/10.1016/j.neuropharm.2015.08.020
Polter A, Yang S, Zmijewska AA et al (2009) Forkhead Box, Class O transcription factors in brain: regulation and behavioral manifestation. Biol Psychiatry 65:150–159. https://doi.org/10.1016/j.biopsych.2008.08.005
Steinman L (2009) A molecular trio in relapse and remission in multiple sclerosis. Nat Rev Immunol 9:440–447. https://doi.org/10.1038/nri2548
Hur EM, Youssef S, Haws ME et al (2007) Osteopontin-induced relapse and progression of autoimmune brain disease through enhanced survival of activated T cells. Nat Immunol 8:74–83. https://doi.org/10.1038/ni1415
Chung HW, Lim JH, Kim MY et al (2012) High-fat diet-induced renal cell apoptosis and oxidative stress in spontaneously hypertensive rat are ameliorated by fenofibrate through the PPAR a – FoxO3a – PGC-1 a pathway. Nephrol Dial Transpl 27:2213–2225. https://doi.org/10.1093/ndt/gfr613
Liu DF, Li S, Zhu Q, Jiang W (2018) The involvement of miR-155 in blood pressure regulation in pregnant hypertension rat via targeting FOXO3a. Eur Rev Med Pharmacol Sci 22:6591–6598
Lin J, Zheng Y, Zhang Z et al (2018) Suppression of endothelial-to-mesenchymal transition by SIRT (Sirtuin) 3 alleviated the development of hypertensive renal injury. Hypertension 72:350–360. https://doi.org/10.1161/HYPERTENSIONAHA.118.10482
Tsuchiya K, Westerterp M, Murphy AJ et al (2013) Expanded granulocyte/monocyte compartment in myeloid- specific triple FoxO knockout increases oxidative stress and accelerates atherosclerosis in mice. Circ Res 112:992–1003. https://doi.org/10.1161/CIRCRESAHA.112.300749
Tucka J, Yu H, Gray K et al (2014) Akt1 regulates vascular smooth muscle cell apoptosis through FoxO3a and Apaf1 and protects against arterial remodeling and atherosclerosis. Arterioscler Thromb Vasc Biol 34:2421–2428. https://doi.org/10.1161/ATVBAHA.114.304284
Yu H, Fellows A, Foote K et al (2018) FOXO3a (Forkhead transcription factor o subfamily member 3a) links vascular smooth muscle cell apoptosis, matrix breakdown, atherosclerosis, and vascular remodeling through a novel pathway involving MMP13 (Matrix metalloproteinase 13). Arterioscler Thromb Vasc Biol 38:555–565. https://doi.org/10.1161/ATVBAHA.117.310502
Tsuchiya K, Tanaka J, Shuiqing Y et al (2012) FoxOs integrate pleiotropic actions of insulin in vascular endothelium to protect mice from atherosclerosis. Cell Metab 15:372–381. https://doi.org/10.1016/j.cmet.2012.01.018
Sun G, Shen J, Wei X, Qi G (2021) Circular RNA Foxo3 Relieves Myocardial Ischemia / Reperfusion Injury by Suppressing Autophagy via Inhibiting HMGB1 by Repressing KAT7 in Myocardial Infarction. J Inflamm Res 14:6397–6407
Lv W, Jiang J, Li Y et al (2020) MiR-302a-3p aggravates myocardial ischemia-reperfusion injury by suppressing mitophagy via targeting FOXO3. Exp Mol Pathol 117:1–9. https://doi.org/10.1016/j.yexmp.2020.104522
Boal F, Roumegoux J, Alfarano C et al (2015) Apelin regulates FoxO3 translocation to mediate cardioprotective responses to myocardial injury and obesity. Sci Rep 5:1–17. https://doi.org/10.1038/srep16104
Zheng T, Lu Y (2011) Changes in SIRT1 expression and its downstream pathways in age-related cataract in humans. Curr Eye Res 36:449–455. https://doi.org/10.3109/02713683.2011.559301
Li J, Sun Q, Qiu X et al (2022) Downregulation of AMPK dependent FOXO3 and TFEB involves in the inhibition of autophagy in diabetic cataract. Curr Eye Res 47:555–564. https://doi.org/10.1080/02713683.2021.2009516
Kadiri M, Charbonneau M, Lalanne C et al (2022) 14-3-3 η promotes invadosome formation via the FOXO3 – snail axis in rheumatoid arthritis fibroblast-like synoviocytes. Int J Mol Sci 23:1–17
Liu N, Feng X, Wang W et al (2017) Paeonol protects against TNF-α-induced proliferation and cytokine release of rheumatoid arthritis fibroblast-like synoviocytes by upregulating FOXO3 through inhibition of miR-155 expression. Inflamm Res 66:603–610. https://doi.org/10.1007/s00011-017-1041-7
Manda G, Isvoranu G, Comanescu MV et al (2015) The redox biology network in cancer pathophysiology and therapeutics. Redox Biol 5:347–357. https://doi.org/10.1016/j.redox.2015.06.014
Yadava RK, Chauhana AS, Zhuanga L, Gan B (2018) FoxO transcription factors in cancer metabolism. Semin Cancer Biol 50:65–76. https://doi.org/10.1016/j.semcancer.2018.01.004
Hornsveld M, Smits LMM, Meerlo M et al (2018) FOXO transcription factors both suppress and support breast cancer progression. Cancer Res 78:2356–2369. https://doi.org/10.1158/0008-5472.CAN-17-2511
Alasiri G, Fan LY, Zona S et al (2017) ER stress and cancer: The FOXO forkhead transcription factor link. Mol Cell Endocrinol 462:67–81. https://doi.org/10.1016/j.mce.2017.05.027
Xiao Z, Han L, Lee H et al (2017) Energy stress-induced lncRNA FILNC1 represses c-Myc-mediated energy metabolism and inhibits renal tumor development. Nat Commun 8:1–13. https://doi.org/10.1038/s41467-017-00902-z
Liu H, Yin J, Wang H et al (2015) FOXO3a modulates WNT/β -catenin signaling and suppresses epithelial-to-mesenchymal transition in prostate cancer cells. Cell Signal 27:510–518. https://doi.org/10.1016/j.cellsig.2015.01.001
Hwang J, Rajendrasozhan S, Yao H et al (2011) FOXO3 deficiency leads to increased susceptibility to cigarette smoke-induced inflammation, airspace enlargement, and chronic obstructive pulmonary disease. J Immunol 187:987–998. https://doi.org/10.4049/jimmunol.1001861
Ganesan S, Unger BL, Comstock AT et al (2013) Aberrantly activated EGFR contributes to enhanced IL-8 expression in COPD airways epithelial cells via regulation of nuclear FoxO3A. Thorax 68:131–141. https://doi.org/10.1136/thoraxjnl-2012-201719
Barkund S, Shah T, Ambatkar N et al (2015) FOXO3a gene polymorphism associated with asthma in indian population. Mol Biol Int 2015:1–7
Liu B, Sun H, Wang J et al (2021) Potential role for EZH2 in promotion of asthma through suppression of miR-34b transcription by inhibition of FOXO3. Lab Investig 101:998–1010. https://doi.org/10.1038/s41374-021-00585-7
Liu B, Wang J, Ren Z (2021) SKP2-promoted ubiquitination of FOXO3 promotes the development of asthma. J Immunol 206:2366–2375. https://doi.org/10.4049/jimmunol.2000387
Imraish A, Abu-Thiab T, Zihlif M (2021) IL-13 and FOXO3 genes polymorphisms regulate IgE levels in asthmatic patients. Biomed Rep 14:1–7. https://doi.org/10.3892/br.2021.1431
Li L, Kang H, Zhang Q et al (2019) FoxO3 activation in hypoxic tubules prevents chronic kidney disease. J Clin Invest 129:2374–2389
Lin F (2020) Molecular regulation and function of FoxO3 in chronic kidney disease. Curr Opin Nephrol Hypertens 29:439–445. https://doi.org/10.1097/MNH.0000000000000616
Nlandu-khodo S, Osaki Y, Scarfe L et al (2020) Tubular β -catenin and FoxO3 interactions protect in chronic kidney disease. JCI Insight 5:1–17
Tothova Z, Kollipara R, Huntly BJ et al (2007) FoxOs are critical mediators of hematopoietic stem cell resistance to physiologic oxidative stress. Cell 128:325–339. https://doi.org/10.1016/j.cell.2007.01.003
Menon V, Ghaffari S (2018) Transcription factors FOXO in the regulation of homeostatic hematopoiesis. Curr Opin Hematol 1–9. https://doi.org/10.1097/MOH.0000000000000441
Zhang Y, Chang A, Sumazin P, Sheehan V (2017) Piceatannol induces fetal hemoglobin in erythroid progenitor cells from patients with sickle cell disease. Blood 130:2221. https://doi.org/10.1182/blood.V130.Suppl
Zhang Y, Paikari A, Sumazin P et al (2018) Metformin induces FOXO3-dependent fetal hemoglobin production in human primary erythroid cells. Blood 132:321–333. https://doi.org/10.1182/blood-2017-11-814335
Simões V, Felix F, Alves N et al (2020) Relationship of polymorphism rs3800231 in FOXO3 gene and clinical severity with oxidative stress markers in sickle cell disease. Meta Gene 24:100660. https://doi.org/10.1016/j.mgene.2020.100660
Thanuthanakhun N, Nuntakarn L, Sampattavanich S et al (2017) Investigation of FoxO3 dynamics during erythroblast development in β -thalassemia major. PLoS ONE 12:1–13. https://doi.org/10.1371/journal.pone.0187610November
Zhang X, Campreciós G, Rimmelé P et al (2015) FOXO3-mTOR Metabolic Cooperation in the Regulation of Erythroid Cell Maturation and Homeostasis. 89:954–963. https://doi.org/10.1002/ajh.23786.FOXO3-mTOR
Costantini D (2019) Understanding diversity in oxidative status and oxidative stress: The opportunities and challenges ahead. J Exp Biol 222. https://doi.org/10.1242/jeb.194688
McIntyre RL, Liu YJ, Hu M et al (2022) Pharmaceutical and nutraceutical activation of FOXO3 for healthy longevity. Ageing Res Rev 78:101621. https://doi.org/10.1016/j.arr.2022.101621
Funding
This work was supported by Conselho Nacional de Desenvolvimento Científico e Tecnológico (CNPq, Grant number 406700/2021–4), and by the Coordenação de Aperfeiçoamento de Pessoal de Nível Superior–Brasil (CAPES)–Finance Code 001.
Author information
Authors and Affiliations
Contributions
VSB and FFT conceived, reviewed the literature, and wrote the manuscript. DGHS reviewed and edited the manuscript. All authors were involved in reading and approving the final manuscript. The authors declare that all data were generated in-house and that no paper mill was used.
Corresponding author
Ethics declarations
Ethics approval and consent to participate
Not applicable
Competing interests
The authors declare that they have no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Bernardo, V.S., Torres, F.F. & da Silva, D.G.H. FoxO3 and oxidative stress: a multifaceted role in cellular adaptation. J Mol Med 101, 83–99 (2023). https://doi.org/10.1007/s00109-022-02281-5
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00109-022-02281-5