Abstract
Therapy-related acute myelogenous leukemia (t-AML) remains difficult to distinguish from de novo leukemia, and the overall incidence of t-AML is expected to increase with the successful management of other malignancies. Cytotoxic chemotherapy and radiation are causes for t-AML. Recent genetic profile data of patients with acute myelogenous leukemia (AML) at the diagnosis suggest that the field may be able to move toward a more refined genetics-based categorization of AML. This may then form the framework for an unbiased approach to the clinical management of t-AML. Cytogenetic abnormalities of t-AML mainly determine the course of disease as it does in de novo AML. Although an inferior outcome is observed in the entire population of t-AML patients, patient outcome is multifactorial. T-AML patients with favorable recurrent cytogenetic abnormalities who received a topoisomerase inhibitor 1–2 years earlier show similar responses to conventional therapy as their de novo counterparts, and patients should be encouraged to participate in clinical trials designed for de novo AML patients with similar cytogenetic abnormalities. T-AML patients who received an alkylating agent or irradiation 3–6 years earlier usually have a complex karyotype in their blast cells, and respond poorly to conventional AML therapy. Persistence of a primary malignancy, decreased organ reserve from prior therapy, and comorbidities impact clinical outcomes and limit therapeutic options for t-AML independent of genetics. Improvements in clinical outcomes in t-AML will be aided by earlier diagnosis and treatment, development of effective lower intensity treatments, post-remission strategies including investigational therapy, and pursuit of transplantation for poor-risk cytogenetic subsets.
Access provided by CONRICYT-eBooks. Download chapter PDF
Similar content being viewed by others
Keywords
- Therapy-related acute myelogenous leukemia
- Leukemia
- Cytogenetics
- Treatment
- Hematopoietic stem cell transplantation
Introduction
Individuals exposed to cytotoxic agents are at higher risk of developing myeloid disorders such as therapy-related myelodysplastic syndrome (t-MDS) , therapy-related acute myeloid leukemia (t-AML) , and therapy-related MDS/myeloproliferative neoplasms. However, all of these diseases are within the spectrum of a single disease entity, therapy-related myeloid neoplasms (t-MN) , as categorized by the WHO classification system in 2008 [1]. WHO morphologic classification system defines t-MN as MDS and myeloid leukemia, which arise following the administration of chemotherapy and/or radiation for a prior malignancy. Patients who developed myeloid disorders by environmental toxins affecting hematopoiesis are not included in this disease category. Therapy-related MDS and AML comprise the vast majority of t-MN cases. The 2008 WHO classification did not consider t-MDS and t-AML sufficiently distinctively different. However, unlike secondary AML denoting AML did not develop spontaneously or de novo, t-AML has clear history of prior chemotherapy or radiation therapy.
T-MN has become increasingly common. The fast rising incidence can be attributed to a variety of factors including longer survival of patients after treatment of their primary malignancy, intensified chemotherapy, radiation therapy, and broaden awareness of this disease category. This is a heterogeneous and poorly defined group of patients who have a shorter median survival than patients with de novo AML, MDS, or MDS/myeloproliferative neoplasia (MPN). Retrospective studies have shown that their inferior outcomes are associated with poor-risk cytogenetics, present in 50–70% of t-MDS/AML compared with 15–25% in de novo disease. Other studies have identified additional risk factors, including comorbidities from primary malignancy and therapy of the disease. Because of the poor outcome, t-AML is among the most feared long-term complication of cancer therapy these days.
Epidemiology
Therapy-related myeloid neoplasms (t-MN) account for approximately 10–20% of all cases of AML, MDS, and MDS/MPN. US Surveillance , Epidemiology, and End Results data of approximately 426,000 adults treated for an initial primary malignancy between 1975 and 2008 showed a 4.7-fold increased risk of AML compared with the incidence of AML expected in the general population. With the increasingly successful management of malignancies overall and improved cancer survivorship, the overall incidence of t-MN is expected to increase. The estimated incidence after therapy for any single prior diagnosis varies from less than 1 to 20% depending on the agents administered, therapy intensity, and survival, since the overall median latency time varies 1–5 years.
Patients with t-AML are seen among survivors of both solid tumors and hematologic malignancies. Smith et al. studied 306 patients who developed therapy-related myelodysplasia and myeloid leukemia with cytogenetic analyses [2]. In the study population, 25% of the patients had Hodgkin disease, 23% had non-Hodgkin lymphoma, and 38% had a solid tumor as the primary malignancy. Breast cancer was the most common among the 38% patients. Interestingly, 6% of patients had undergone cytotoxic chemotherapy for the management of immune disorders. Kayser et al. also showed similar patient characteristics in their study with 200 patients having t-AML. The group found that 71% of t-MN patients had a prior solid tumor and 27.5% patients had a prior hematologic malignancy. Breast cancer and non-Hodgkin lymphoma were the largest subsets in these two groups [3].
T-AML patients can present at any age. The risk associated with alkylating agents and radiation appears to increase with age, while the risk associated with topoisomerase II inhibitors appears to be constant across all ages [1]. Among those treated for breast cancer, younger age at the time of exposure, higher dose intensity of cytotoxic treatments, concomitant treatment with radiation, and adjuvant use of hematopoietic growth factors with cytotoxic therapy for accelerated white blood cell recovery are factors associated with an increased risk of t-AML [4, 5]. However, some t-AML/MDS individuals may have a DNA repair apparatus that is not as robust as normal, which also might predispose them to develop t-AML.
Etiology
T-AML appears to be a direct consequence of mutational events by therapy-induced DNA double-strand breaks, with a subsequent genomic instability [6]. Frequency of the mutations may vary between individuals as a result of genetic susceptibility. This susceptibility is usually not measurable or very subtle; a few exceptions include Fanconi anemia, and mismatch repair abnormalities.
The effects of some cytotoxic agents in the development of abnormal cytogenetics are well documented (Table 22.1). The latency period between first exposure to an agent (cytotoxic chemotherapy, radiation) and development of t-AML ranges from 1 to 5 years and varies by etiologic agent. T-AML after exposure to alkylating agents or radiation therapy typically presents after a latency period of approximately 4 years [7,8,9,10]. Most of these patients initially present with MDS. The chromosomal abnormalities seen in this category of t-AML often involve complex abnormalities such as deletion of the long arm or the entire chromosome 5 and/or 7. Topoisomerase II inhibitors are another etiologic agent of t-AML. It causes t-AML with a relatively shorter latency of 1–3 years, and the patients present with overt leukemia rather than MDS or MDS/MPN [11,12,13]. The cytogenetic alterations in this category of t-AML occur frequently with translocations including the MLL gene located at 11q23 or AML1 (RUNX1) gene at 21q22 [e.g., t(9;11), t(8;21), or t(3;21)]. However, no reliable way exists to determine the duration of the “at-risk” period for developing t-AML. The latency periods with other agents are not as clear as these two drugs. Exposure to multiple agents also makes it difficult to determine the risk, etiology, and latency period.
Alkylating agents are frequently used chemotherapeutic agents; more than 85% of patients who developed chemotherapy-related leukemia had received an alkylator [14]. Melphalan, chlorambucil, or cyclophosphamide is the offending agent in nearly 65% of patients. Therefore, different alkylating agents may be associated with varying risks of leukemogenesis. For example, one study compared the rates of mutagen-related leukemia in ovarian cancer patients treated with either melphalan or cyclophosphamide, and found that melphalan may be a more potent leukemogen than cyclophosphamide. Thus, the mutagenic potential may differ between the antineoplastic agents [15].
Alkylating agents interact with DNA in a variety of ways: monoadduct formation, inter- and intra-strand cross-links, as well as alkylation of free DNA bases. This can lead to cell death, but also can cause termination of DNA replication and chromosome loss, leading to mutagenesis and resulting in development of leukemia. Alkylation events can also change the stereometric configuration of DNA bases, causing them to mispair resulting in single-base mutations. Many of the alkylating agents have been clearly implicated in leukemogenesis.
Topoisomerase II helps mediate the relaxation of the DNA supercoil by making double-strand breaks. The breaks are repaired when homologous chromosome fragments realign. Topoisomerase II inhibitors , such as epipodophyllotoxins (etoposide and teniposide), doxorubicin, 4-epodoxorubicin, mitoxantrone, razosane, and biomolane, induce incorrect DNA repair by crossover recombination with nonhomologous end joining between the two DNA strands, which may result in the development of a balanced chromosomal translocation (Fig. 22.1). Balanced chromosomal aberrations involving the MLL, RUNX1, RARA, or NUP98 genes characterize unique genetic pathways of t-AML. The rearrangements between these genes and other partners provide gain-of-function fusion proteins. These topoisomerase II inhibitors are important components of chemotherapy regimens for many tumors, such as testicular cancer, ALL, NHL, lung cancer, and many others. Razoxane and bimolane , used in the treatment of psoriasis, have also been demonstrated to be leukemogenic. Those patients in whom t-AML develops after therapy with DNA-topoisomerase II inhibitors often have acute leukemia with no t-MDS phase [16, 17], and a short latency period, in contrast to alkylating agent-induced AML.
Formation of topoisomerase II-DNA complex is necessary to perform critical cellular functions. If the amount of complexes is elevated as a result of topoisomerase II inhibitors, DNA repair/recombination process is activated, which subsequently generates chromosomal translocations or other DNA aberrations. If the fusion protein produced by chromosomal translocation results in the cells having a growth advantage, these cells may evolve and progress into t-AML
In the Polycythemia Vera Study Group (PVSG) , 431 polycythemia vera patients were randomized to one of the three treatment groups: phlebotomy alone, P32 and phlebotomy, or chlorambucil and phlebotomy [18]. Higher number of AML cases occurred in both the P32 (9.6%) and chlorambucil (13%) treatment groups compared to phlebotomy-only group (1.5%), indicating a role of radiation and a cytotoxic agent in the development of AML in these patient groups [19]. French Polycythemia Study Group (FPSG) reported a leukemia incidence in polycythemia vera patients of 5–15% after 10 years of observation [20]. In a randomized trial in patients >65 years of age, the FPSG reported 12% AML at 10 years in patients receiving P32 alone. Hydroxyurea maintenance combined with initial P32 therapy also increased the risk of AML (21% at 10 years). In another case control study of MPN patients (68% of patients had polycythemia vera), the risk of AML/MDS development was significantly associated with high exposures of P32 and alkylators [21]. Taken together, a strong association exists of cytotoxic agents or radiation increasing the risk of development of AML in MPN patients.
Ionizing radiation clearly increases the risk of developing AML in humans and experimental animals. The incidence of leukemia after 400 cGy or less of radiation exposure from the Hiroshima nuclear explosion was approximately two cases of leukemia/106 persons/year/cGy [22]. Nearly the same incidence of leukemia was reported in patients who received 300–1500 cGy of spinal irradiation for ankylosing spondylitis. Likewise, increased rates of AML occurred in radiologists who practiced during the early years of clinical radiology before modern safety standards [23].
Animal studies confirmed the epidemiological observations in humans by showing that low-dose chronic irradiation induces leukemia in experimental animals. Half of dogs that received a daily low dose (5–10 cGy) of cobalt γ-irradiation developed AML after about 1000 days [24]. Single whole-body irradiation initiates leukemia in rodents. Myelogenous leukemia developed in 20% of mice after a single brief whole-body irradiation of 200 cGy [25]. The dose–response relationship was curvilinear; pulse irradiation of at least 300 cGy induced significantly fewer cases of leukemia than the 200 cGy dose; these doses produced marrow cell death, probably decreasing the number of cells that would otherwise have the potential to undergo malignant transformation.
Exposure to ionizing radiation can cause a DNA damage by a mechanism similar to alkylating agents. Radiation photon energy can directly lead to DNA strand breakage. Radiation is frequently used in conjunction with chemotherapy for cancer therapy, and only a few studies have specifically looked at the characteristics of myeloid neoplasms occurring after radiation alone. Recently, Nardi et al. showed that t-MDS occurring in the modern radiation therapy era, if alone, more nearly resembled de novo MDS/AML in cytogenetic characteristics and clinical behavior, and affected patients had better outcomes than patients with t-MDS secondary to chemotherapy [26].
Even though radiation therapy is leukemogenic [7, 27,28,29], studies in Hodgkin’s disease suggest that the incidence of secondary leukemia in patients receiving radiation therapy alone was low compared with those receiving chemotherapy alone [30, 31]. In one study, a total of 957 patients exclusively received radiation therapy, and none developed leukemia. By contrast, 542 patients received only chemotherapy, and 12 developed leukemia. A similar finding was reported in ovarian cancer patients who received either chemotherapy or radiation therapy [32]. In most studies, the risk of AML in patients with either Hodgkin’s disease or ovarian carcinoma treated exclusively with chemotherapy is not different from those treated with both chemotherapy and radiation therapy [7, 27,28,29, 32].
In a study of chromosomal abnormalities, only 37 of 344 patients with secondary leukemia had been treated with radiation therapy alone; the incidence of a normal karyotype was higher in patients who received only radiation than in patients who received chemotherapy either with or without radiation therapy (24.3 vs. 11.7%). Normal karyotype is associated with better response to antileukemic therapy, but with little improvement in overall survival (OS) [33]. Another study of 63 patients with either t-MDS or t-AML found that 11 of 63 had received only radiation, in most cases to ports including the pelvis or spinal bone marrow [34]. In this study, only two patients had a normal karyotype. The low risk of leukemia after currently used high-voltage irradiation may be analogous to the earlier mentioned murine model where high-dose irradiation has a lethal effect on marrow cells in contrast to lower dose exposure, which may be more likely to produce nonlethal marrow cell injury and mutations.
Although several studies examined secondary malignancies in patients with specific primary tumor types, few data have been published examining the long-term effect of pelvic radiation. Wright et al. analyzed patients with invasive tumors of the vulva, cervix, uterus, anus, and rectosigmoid treated with radiotherapy from 1973 to 2005 [35]. In a Cox proportional hazards model adjusting for other risk factors, posttreatment leukemia was increased by 72% (hazard ratio [HR], 1.72; 95% CI, 1.37–2.15) in the patients who received pelvic radiotherapy. The risk of secondary leukemia peaked at 5–10 years after primary treatment (HR, 1.85; 95% CI, 1.40–2.44) and remained elevated even 10–15 years after initial treatment (HR, 1.50; 95% CI, 1.03–2.18) [35].
Radioiodine (I-131) induces chromosomal aberrations, and theoretically can lead to leukemogenesis. However, the occurrence of t-AML after radioiodine treatment for thyrotoxicosis and thyroid cancer is infrequent. In a comprehensive meta-analysis of the currently available literature covering 16,502 patients with thyroid cancers, the relative risk of development of leukemia increased 2.5-fold in patients treated with radioiodine [36]. The latency period of t-AML associated with radiation was 5–7 years, similar to t-AML associated with alkylating agents [37].
The use of granulocyte colony-stimulating factor (G-CSF) in chemotherapy may be a risk factor for development of t-AML as shown in a meta-analysis examining data from 25 trials [38]. At a mean follow-up of 60 months, 43 t-MN cases were reported in G-CSF-treated patients, while 22 t-MN occurred in control group. G-CSF may accelerate damaged myeloid progenitors into cell cycling before repair of genetic injuries from cytotoxic therapy.
Cases of leukemic transformation in patients with severe congenital neutropenia (SCN) were prospectively studied [39]. A comprehensive analysis of the incidence of AML transformation showed that the annual risk of MDS/AML was 0.81% during the first 5 years, and 2.3% after 10 years among 374 SCN patients with G-CSF treatment. After 15 years on G-CSF, the cumulative incidence for MDS/AML was 22% in SCN, whereas none of the cyclic neutropenia patients who also received G-CSF developed MDS or AML [40]. Patients with SCN develop mutations of their G-CSF receptor, which affects the ability of the myeloid cells to differentiate.
T-MN occurring in patients with autoimmune diseases (AD) has been increasingly recognized. A large population-based study found that AD patients had significantly increased risk for AML and MDS [41], and this finding was subsequently confirmed by another study [42]. Immunosuppressive therapy may be another contributing factor for development of t-MN. Patients who received immune-suppressive agents including corticosteroids, antitumor necrosis factor (TNF) agents, sulfasalazine, and cytotoxic chemotherapeutics such as methotrexate, azathioprine, and cyclophosphamide had increased risk for hematological malignancies [43]. The development of t-APL in patients with multiple sclerosis has been reported [44, 45]. But patients receiving an antimetabolite as a single agent (e.g., fludarabine, azathioprine, and 6-thioguanine) for their autoimmune disease rarely develop t-AML [46,47,48]. Development of t-AML in AD patients who received immunosuppressive therapy other than cytotoxic agents could represent the importance of the immune-surveillance system in guarding against malignancies. Also, the underlying primary genetic defects in these individuals might increase susceptibility to AML.
Karyotypic Abnormalities in t-MDS/AML
Clonal chromosomal abnormalities can be detected in the blast cells of 80–95% of t-MDS/t-AML patients by routinely available techniques [7, 34, 49,50,51,52,53]. A hypodiploid modal number of chromosomes occur most frequently in t-MDS/t-AML patients. Hyperdiploidy, mainly trisomy 8, is rare and is often observed as an inconsistent aberration present in only a subclone of cells [52]. Chromosomes 5q and 7q probably contain critical myeloid tumor-suppressor genes in de novo and t-AML. The breakpoints for the deletions are variable, but a common chromosome region, the so-called critical region, is almost always deleted.
For chromosome 5, Le Beau et al. have narrowed down the critical region to 5q31.1, which includes the early growth response gene (EGR-1) [54]. Other genes located on the long arm of chromosome 5 include many growth factor genes, namely granulocyte-macrophage colony-stimulating factor (GM-CSF) , and interleukins-3, −4, and −5 (IL-3, −4, −5) [34, 55,56,57,58], and the growth factor receptor genes known to be present on the long arm of chromosome 5, namely macrophage colony-stimulating factor (M-CSF or FMS) receptor, platelet-derived growth factor (PDGF) receptor, glucocorticoid receptor, alpha1-adrenergic receptor, beta2-adrenergic receptor, and D1-dopamine receptor [59, 60].
The breakpoints for the deletions of 7q are variable, but a common chromosome region, the so-called critical region, is located at band 7q22 proximally with the distal breakpoint varying from q31 to q36. Potentially important genes have been mapped to 7q, including genes for EZH2, erythropoietin, p glycoprotein 1/multiple drug resistance 1 (MDR-1), and MDR-3 [61]. Abnormalities of chromosome 7q are common in myeloid malignancies. Especially, homozygous EZH2 mutations were commonly found in MDS/MPN patients [61]. However, none has yet been shown to be involved in the development of t-AML [54, 59,60,61,62].
Although most of the chromosomal abnormalities reported in t-MDS/t-AML are either complete or partial deletion of chromosome 7 or 7q [del(−7/7q)], and/or 5, or 5q del(−5/5q)], in recent years recurring unbalanced translocations that also result in loss of the long arm of 7 and/or 5 have been reported with increasing frequency. These include t(1;7)(p11;q11), t(5;7)(q11.2;p11.2), and t(7;17)(p11;p11) for chromosome 7, and t(5;7)(q11.2;p11.2) and t(5;17)(p11;p11) for chromosome 5 [63]. While the loss of function of a single gene in each of these relatively large regions is possibly responsible for the development of t-MDS/t-AML, hemizygous loss of the function of several genes in each of these regions could also contribute to the disease phenotype. Another, not mutually exclusive hypothesis is that an unknown initiating abnormality causes genomic instability leading to the deletion and rearrangement of particularly susceptible chromosome regions, such as those on chromosome 5q and 7q.
A review of 431 cases of secondary leukemia found 16 nonrandom chromosomal changes involving chromosomes 3, 5, 7, 8, 9, 11, 14, 17, and 21. These changes were dependent on the type of primary disease, previous therapy, age, and gender [64]. In another single-institution study consisting of 63 patients, additional abnormalities involving chromosomes 1, 4, 5, 7, 12, 14, and 18 occurred, with significantly increased frequency of these changes in t-AML as compared to de novo AML [34]. Abnormalities in chromosome 17, especially translocations involving bands 17p11-p13 and 17q21, occasionally are observed in t-AML, for example, t(15;17)(q22;q11–21) [65, 66]. Other chromosomes often reported to be abnormal in t-MDS/t-AML are chromosomes 21 and 11, particularly involving balanced translocations of chromosome bands 11q23 and 21q22 in t-AML [i.e., t(4;11), t(6;11), t(9;11), t(11;19), t(3;21), and t(8;21)] [52, 59, 63, 64]. These translocations are associated with previous therapy targeting DNA-topoisomerase II, primarily the epipodophyllotoxins and the anthracyclines. The 11q23 reciprocal translocations and interstitial deletions structurally interrupt a small region of the MLL (also known as HRX, ALL-1, HTRX1) gene that codes for a human homolog of the Drosophila trithorax gene [67, 68]. A fragment of the MLL gene translocates to more than 200 other chromosomal regions, resulting in the creation of a fusion protein with the partner gene [69].
The t(9;11) that results in a fusion between MLL and AF9 is a recurring chromosomal translocation in de novo AML and is one of the most common recurring chromosome translocations detected in about 50% of t-AML patients who have a MLL translocation [70]. In addition, involvement of the AF9 gene in the development of t-AML is linked to the treatment with topoisomerase inhibitors [6]. Interestingly, the unbalanced rearrangements of the same two bands, 11q23 and 21q22, were most often associated with therapy with alkylating agents alone or in combination with radiation therapy [59]. In Chinese patients treated for psoriasis with bimolane, t(15;17) has been frequently reported. Also, therapy with doxorubicin has been associated with an increased incidence of t-AML with balanced translocations at chromosome band 21q22, in particular t(3;21) [52, 64]. In addition to balanced translocations involving chromosome bands 11q23 and 21q22, other balanced aberrations such as inv (16), t(8;16), t(15;17), and t(6;9) have been observed in t-AML after previous therapy with drugs targeting DNA topoisomerase II (Table 22.2) [52, 63].
In a study of 491 t-MDS/t-AML patients with at least one balanced translocation, Rowley and Olney reported that 149 of the patients were positive for the 11q23 translocation (30.3%), followed by the 21q22 rearrangement seen in 15%, inv (16) in 9%, and t(15;17) in 8% of the patients [70]. Interestingly, no significant difference occurred in the gender distribution of patients within the subgroups, and patients in the 11q23 subgroup were of the youngest age at their primary and secondary diagnosis. Moreover, the translocation 11q23, inv (16), and t(15;17) subgroups had the shortest latency, with a median latency of 25.9 months for translocation 11q23, 22.0 months for inv (16), and 28.9 months for t(15;17) [70].
Chromosome studies have shown that when t-MDS becomes clinically diagnosable, the preleukemic clone represents a majority of the hematopoietic cells [7, 34, 49]. Additional chromosomal abnormalities occur in the original abnormal clone in 60–70% of cases as the disease evolves to frank leukemia [71, 72]. Karyotypic evolution usually involves further deletions or losses of chromosomes and a change to a lower modal chromosome number; rarely, the evolution is associated with a gain of chromosome 8. Evidence suggests that t-MDS patients who have a mixture of karyotypically normal and abnormal cells (AN) survive longer than those who have only abnormal cells (AA) [73]. Most individuals who are AN in the preleukemic phase become AA as the disease progresses [34]. Notably, Rowley and Olney observed in their study that patients presenting with a t-MDS had significantly more frequent abnormalities of chromosomes 5 and/or 7 (49%) than did patients presenting with a t-AML (16%), and that this subgroup also presented with the highest percentage of complex karyotypes (45% vs. ca. 20% for both 1 and 2 aberrations) [70].
Genetics of Therapy-Related AML
Patients who develop t-AML may be predisposed to develop AML because of defects in DNA repair or increased susceptibility to accumulation of genetic mutations [74]. Candidate single-nucleotide polymorphisms associated with either drug metabolism or DNA repair enzymes have been identified as a mechanism by which a subset of t-AML may develop [75]. The commonly found germline variants in t-AML patients are NQ01, glutathione S-transferase family of enzymes, BRCA1/2, TP53, and MDM2 [76,77,78]. Li-Fraumeni syndrome and Fanconi anemia also predispose to acute leukemia [79]. Tumor protein 53 (TP53), RUNX1, V-Ki-ras2 Kirsten rat sarcoma viral oncogene homolog (KRAS), and neuroblastoma RAS viral (v-ras) oncogene homolog (NRAS) mutations are known mutations in the development of t-MDS/AML [80].
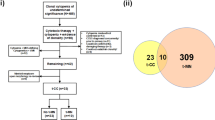
To understand the pathogenetic mechanisms underlying t-MDS/AML, Li et al. performed a prospective case-control study with patients undergoing autologous hematopoietic stem cell transplant for lymphoma. In the study, gene expression in CD34+ hematopoietic stem and progenitor cells (HSC) from patients who developed t-MDS/AML after autologous hematopoietic cell transplantation (autoHSCT) for lymphoma (n = 30) was compared with gene expression in CD34+ cells of control group. The authors demonstrated that the expression pattern of 38 genes was different long before the development of t-MDS/AML in the case group, and that this gene signature was involved in mitochondrial function, metabolism, and hematopoietic regulation in peripheral blood stem cells (PBSC) that could distinguish patients who developed t-MDS/AML post-autoHSCT from those who did not [81].
Another study assessed the bone marrow or peripheral blood samples of 70 t-MDS/AML (including 42 t-AML) patients using a next-generation sequencing of 53 targeted genes. The mutation profile of t-AML was different from those of 428 de novo MDS/AML patients [82]. TP53 was mutated at a significantly higher rate in t-AML than de novo AML (35.7% vs. 12.8%, p = 0.002). PTPN11 mutations were observed in 11.9% of t-AML patients compared with 2.1% in de novo AML patients (p = 0.008). Mutations of NPM1 and FLT3 only occurred in 2.5% and 7.1% of t-AML patients, respectively, which was significantly lower than de novo AML patients (21.7% and 16.4%, respectively) (Table 22.3). Analysis of clonal evolution showed that TP53 mutation often occurs early in the pathogenesis of t-AML, and mutations of other genes may provide a further evolution to t-AML [83].
Lindsley et al. reported the genetics of 101 t-AML patients [84]. The goal of the study was to find a distinct mutation profile of t-AML compared with secondary or de novo AML with comprehensive sequencing. Samples obtained from patients prior to treatment were analyzed for mutations in 82 genes and the results were compared to the genetic profiles in The Cancer Genome Atlas of de novo AML. The comparative analysis demonstrated three mutually exclusive patterns of mutations that were noted in the t-AML cohort. The first group had TP53 mutations. The second group had mutations which were commonly associated with secondary AML. These “secondary” mutations at cohort included spliceosome genes (SRSF2, SF3B1, U2AF1, ZRSR2), chromatin remodeling genes (ASXL1, EZH2, BCOR), and cohesion gene (STAG2). The third group included those with de novo-type mutations (NPM1, CBF rearrangements, and MLL rearrangements). However, the authors did not find unique genetic profiles, associated with chemotherapy exposure other than the established link between exposure to topoisomerase II inhibitors and MLL rearrangements. The CR rate for t-AML patients with de novo-type mutations was less than in de novo AML patients with the same mutations, but t-AML with secondary-type mutations or TP53 mutations had remission rates similar to the older de novo AML group with the same “secondary”-type mutations. But the t-AML cohort required more cycles of induction therapy for CR. Taken together, prior chemotherapy exposure may not produce a unique “therapy-related” genetic profile, but genetic profiles may help predict outcomes of t-AML patients [84].
Next-generation sequencing could identify mutations in the leukemic transformation of Severe Congenital Neutropenia (SCN). Mutations in CSF3R-T618I, RUNX1, and ASXL1 were found only in the MDS/AML phase of SCN [85]. Another study revealed that 64.5% of patients of the study population had mutations in RUNX1 and the mutation occurred in clones with earlier acquired CSF3R mutations [86]. A sequential analysis at stages prior to leukemia development demonstrated that the RUNX1 mutations are late events in the AML development of SCN. The other mutations associated with leukemic transformation were ASXL1, SUZ12, and EP300 in less frequent rate.
Several groups have tried to identify the major genetic mutations in progression of MPN to AML by performing genotypic analyses of AML cells evolved from MPN [87,88,89,90,91,92]. The process of AML transformation is considered to arise from additional mutations outside of the JAK-STAT pathway, which is supported by the findings that the canonical JAK2V617F mutation has not been correlated with leukemic transformation. Furthermore, this mutation can be absent in the leukemic clone [93]. In these analyses, mutations affecting epigenetic regulators and transcriptional factors (ASXL1, TET2, EZH2, IDH1/IDH2, IKZF1), splicing factors (SRSF2, SF3B1, ZRSR2, U2AF1), and TP53 mutations were frequently observed in MPN-AML cells compared to MPN cells. While only 1.9% of PV patients had an IDH1/2 mutation, MPN-AML patients had a high frequency (21.6%) of this mutation [94]. Among 22 patients with post-MPN AML, 45.5% of the patients had a P53-related defect. In a study of 29 post-MPN AML samples (including 162 chronic-phase PV) using SNP arrays, changes of chromosomes 1q, 7q, 5q, 6p, 7p, 19q, 22q, and 3q were associated with post-MPN AML [88].
Clinical Presentation and Diagnosis
No specific clinical presentation demarks t-AML, but most patients have symptoms similar to patients with de novo AML including cytopenias (i.e., anemia, neutropenia, and thrombocytopenia) associated with easy fatigue, generalized malaise, infections, and/or hemorrhagic symptoms as easy bruising, nose/gingival bleeding, menorrhagia, or petechiae. Patients may have clinical manifestations of hepatomegaly, splenomegaly, lymphadenopathy, gingival hypertrophy, skin infiltration, and neurological abnormalities.
A preleukemic or myelodysplastic phase occurs in over 70% of patients in whom AML develops following chemotherapy and/or radiation therapy for another disease [7, 27, 49,50,51, 95,96,97,98], whereas about 20% of patients with de novo AML have a similar preleukemic phase. Indeed, the data suggest that a preleukemic period can be observed in nearly all patients with t-AML, when these patients are monitored closely. Exceptions are those individuals in whom t-AML develops after therapy with epipodophyllotoxins (VP16 and VM26) or other DNA-topoisomerase II inhibitors. In these patients, t-AML often develops with no preleukemic phase [16, 17]. The mean duration of the preleukemic phase is 11.2 months in typical t-AML. The preleukemic phase in individuals with de novo MDS who go on to develop AML is similar, about 14 months (Table 22.1) [95, 96, 98].
Prodromal symptoms of the emergence of t-AML may be similar. However, when a patient who has received cytotoxic agents has these symptoms, the appropriate workup to rule out t-AML should be done. The diagnostic evaluation includes a comprehensive medical history and physical examination with detailed information of exposure to cytotoxic agents (time, duration, cumulative doses). In addition, patient’s age, comorbidities, performance status, organ dysfunction, and remission status of the primary disease are important for establishing management plan. A detailed family history is essential to rule out hereditary cancer syndrome. Peripheral blood smear is an important laboratory test to rule out dysplastic changes in myeloid cells. Complete blood differential counts, and metabolic panel, as well as lactate dehydrogenase and uric acid level are required for initial laboratory tests. The diagnosis of t-AML is eventually made when evaluation of the peripheral blood and bone marrow demonstrates circulating myeloblasts in peripheral blood and/or more than 20% of myeloblasts in bone marrow. This may be buttressed by typical immunophenotypic and cytogenetic changes.
The clinical manifestation of the preleukemic phase of t-AML is marked by ineffective hematopoiesis. The bone marrow morphology is characterized by trilineage dysplasia . The degree of dysplasia is usually very prominent. Interestingly, the RAEB and RAEB-t subgroups are more frequently linked to t-MDS (73%) than in de novo MDS (53%) [99]. Prominent abnormalities are observed in the red blood cells and their precursors. Most patients show decreased red cell production with low reticulocyte counts [27]. Oval macrocytosis and nucleated red cells are often the earliest recognizable changes observed in the peripheral blood in the preleukemic phase [100]. Macrocytosis after therapy for Hodgkin’s disease was retrospectively found to be associated with a high risk of the development of leukemia [101]. Mild neutropenia is present in 75% of the individuals [27]. Neutrophils may be poorly granulated, and their nuclei can be hyposegmented (pseudo-Pelger-Hüet anomaly) [102]. Thrombocytopenia occurs in approximately 60% of patients [27], and they may be abnormally large and degranulated. Both the neutrophils and platelets can have a variety of qualitative defects. The bone marrow is often hypercellular, although hypo- and normocellular marrow can occur. Erythroid hyperplasia , megaloblastoid features, and occasionally ringed sideroblasts dominate the marrow picture [102,103,104]. Abnormalities of the marrow granulocytic and megakaryocytic series are usually more subtle. Micromegakaryocytes may be seen, particularly with monosomy 7. The percentage of immature granulocytic and megakaryocytic cells may be increased. The primary and specific granules of the granulocyte precursors occasionally are either deficient or abnormally large. Marrow fibrosis often is present during the preleukemic phase.
In summary, the development of unexplained pancytopenia and the finding of karyotypic abnormalities in the marrow cells of patients who received chemotherapy and/or radiation therapy for another disease are pathognomonic of preleukemia. Evolution to overt leukemia is universal if the preleukemic individual survives the complications of hemorrhage and infection. T-MDS can be viewed as an early phase of t-AML in which the malignant hematopoietic clone is established and becomes predominant.
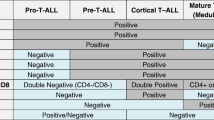
Clinical manifestations of individuals with t-AML are typical of bone marrow failure, and their clinical course is rapidly fatal often from complications of bleeding and infection. The bone marrow morphology of t-AML has been difficult to classify according to FAB criteria for AML, as most of the leukemias demonstrate trilineage involvement and appear to bridge several subtypes. Nevertheless, the blast cells of patients with t-AML most often are myeloblastic in appearance according to AML without maturation or AML with minimal differentiation in agreement with the 2008 WHO classification. A lower frequency of acute monocytic forms of leukemia has been reported in several studies as compared to de novo AML [7, 105].
Auer rods are rarely observed in the blast cells in t-AML, but are seen in blast cells of 35% of patients with de novo AML. Many of the blast cells in t-AML lack myeloperoxidase and other granulocyte-specific enzymes. In one series, only one of ten patients with secondary AML had more than 10% peroxidase-positive blast cells compared with nearly 100% peroxidase-positive blast cells in 95% of patients with de novo AML [105]. In addition, less than 20% of the t-AML patients have either greater than or equal to 10% naphthol ASD chloroacetate esterase-positive blast cells compared with 47% of patients with de novo AML. These histochemical data suggest that the leukemic cells from secondary leukemia patients are blocked at an earlier stage of differentiation than the leukemic cells from most de novo AML patients.
A patient may develop t-AML after cytotoxic treatment for a de novo myeloid neoplasm. T-AML secondary to de novo myeloid neoplasm may be identified by performing cytogenetic testing and immunophenotype evaluation at apparent t-AML development and by comparing with those at the time of primary disease diagnosis. The emergence of a distinctly different karyotype suggests, but does not prove, a therapy-related AML, rather than recurrence of the original leukemic clone.
For patients with good performance status, information about siblings is useful for establishing a management plan. HLA typing of patient can be done on final diagnosis and the identification of potential stem cell donor is the first step for matched related donor allogeneic transplant. To evaluate reserved organ function, echocardiogram, and pulmonary function tests is also required. Computed tomography/MRI or PET imaging can give information about the status of primary disease (Table 22.4).
Treatment
Effective treatment options for t-AML are often not available. The efficacy of various therapeutic modalities of t-AML has been difficult to assess because the number of reported cases is small. In addition, data for t-AML have been reported together with secondary leukemias following other hematological disorders such as MPN or de novo MDS, making the evaluation difficult. Daunorubicin in combination with cytarabine remains the standard induction chemotherapy combination for patients with AML for the last decades. All studies to date have shown that response rates, and OS, are significantly lower in whole t-AML patients compared with de novo AML. Complete remission rates in t-AML patients are reported in 40% of patients with median survivals of 6–8 months [106]. The treatment of patients with t-AML is a clinical challenge for multiple reasons. The patients have a greater number of comorbidities, decreased organ reserve from previous therapy or primary disease, and a higher incidence of unfavorable cytogenetic changes. The key prognostic factors in t-AML are patient age, performance status, and karyotype.
For all t-AML patients, the performance status is the first determinant for establishing a treatment plan. All medically fit patients should have HLA typing at initial diagnosis. Supportive care would be appropriate for patients with a poor performance status (ECOG PS >2) at initial diagnosis. Various attempts to improve survival in these patients have failed to change the course of the disease, with deaths due to infection, bleeding, or progression of the acute leukemia. Supportive therapy is, therefore, an important aspect of the medical care of these patients. No significant differences in survival have been shown between those patients who received chemotherapy and supportive care and those who received supportive care alone. Thus, supportive therapy with transfusions of red blood cells and platelets for symptomatic anemia or bleeding complications, or both, is often necessary as well as the treatment with antibiotics for infections. The goal of therapy in these individuals should be to maintain an acceptable quality of life. Clearly, innovative and radically novel approaches to this syndrome are required if these patients are to be cured.
Studies have suggested that no significant differences exist in clinical outcome between the t-AML and de novo AML in the same cytogenetic group. The therapy-related AML with favorable cytogenetic findings, such as t(8;21), t(15;17), and inv. (16), have a complete response rate, essentially the same as de novo AML with the same karyotype [63, 107, 108]. Similarly, patients who have secondary AML with unfavorable cytogenetic findings such as deletion of chromosomes 5 or 7 do poorly, similar to de novo AML individuals with the same abnormality. Therefore, though more single or complex clonal cytogenetic abnormalities are found in t-AML patients than de novo AML patients [3], the prognostic significance of karyotype in t-AML is similar to that in de novo AML.
No single form of post-remission therapy has been shown to be superior for t-AML. Post-remission therapy with high-dose cytarabine probably is appropriate in patients with favorable cytogenetic findings except for those t-APL patients with t(15;17). In contrast, because of their extremely poor outcome, patients with unfavorable cytogenetic findings should be encouraged to enter clinical trials. As part of the discussion of treatment options, t-AML patients with an extremely poor prognosis should probably be offered the spectrum of treatments from supportive care alone to intensive chemotherapy either with or without allogeneic hematopoietic stem cell transplantation.
Therapy-Related AML Patients with Favorable Cytogenetics
Therapy-related AML is a heterogeneous disease and cytogenetic profile remains prognostically relevant. Patients with t-AML and favorable cytogenetics including t(15;17), inv. (16), t(16;16), and t(8;21) generally have superior outcomes among patients with t-AML.
A European study identified 106 cases of t-APL in patients who received cytotoxic chemotherapy for breast cancer, non-Hodgkin’s lymphoma, and other solid tumors over a period of 10 years [109]. These t-APL patients had a short latency time (2–3 years), and exposure to topoisomerase II inhibitors or prior radiation therapy, and shared similar clinical characteristics with de novo APL [110, 111]. Yin et al. demonstrated frequent dyserythropoiesis, dysmegakaryopoiesis, FLT3 mutation (43%), and frequent additional cytogenetic abnormalities (60%) in their report of 17 t-APL patients [112]. Mounting evidence supports the practice of treating t-AML with t(15;17) as de novo disease, even when accompanied by other karyotype abnormalities [110]. They have a good response to all-trans retinoic acid (ATRA) therapy. Induction response rates appear to be equivalent to de novo APL, but induction death was more common and was attributed to impaired physiologic reserves from prior therapy. Therefore, t-APL is currently treated as de novo APL. With the use of ATRA and arsenic trioxide (ATO) in up-front therapy, anthracyclines can be eliminated for low-risk APL, which would be particularly beneficial for patients with t-APL who have had a prior anthracycline therapy for their primary malignancy [113].
T-AML with t(8;21) is not a common type of t-AML. A review article noted 26 cases and concluded that these patients had very similar hematological characteristics and treatment response as de novo AML with t(8;21) [63]. The 2002 international workshop studied 72 cases of t-AML with 21q22 (RUNX1) rearrangement and found that 44 of these cases were t(8;21) [114]. In the study, patients with t(8;21) rearrangement had a more favorable outcome than patients with other rearrangements involving 21q22. Gustafson et al. observed 13 patients with t-AML having t(8;21) karyotype in a single institute and compared them to 38 patients with de novo AML with t(8;21) and found that patients with therapy-related t(8;21) AML were older, and had a higher frequency of KIT 816D mutations, and an inferior OS than their de novo counterparts [115]. Krauth et al. showed high frequencies of additional cytogenetic and molecular lesions in AML with t(8;21) [116]. Mutations in RAS pathway, KIT and ASXL1 mutations, were the most frequent additional mutations in the study, and mutations in KIT D816 and ASXL1 were strongly associated with adverse outcomes. At the chromosomal level, −Y appeared to be associated with a good prognosis whereas trisomy 8 had an inferior prognosis. In a large series of t(8;21), 22 t-AML patients showed no differences in secondary molecular genetic events from 117 de novo AML [116]. However, a study showed that the treatment outcomes of t(8;21) t-AML were inferior to those of de novo t(8;21) AML, possibly because the t-AML cohort was older and some patients had active primary cancer.
T-AML with inv (16) was often associated with prior therapy with topoisomerase II inhibitors [117]. Response rates to intensive chemotherapy in this study were comparable to those with de novo disease. However, t-AML with inv (16) showed a significantly shorter event-free survival than de novo AML. In general, secondary chromosomal aberrations as well as gene mutations are very frequent in AML with inv (16); 80–90% patients with inv (16) AML have at least one mutation involving NRAS, KRAS, KIT, or FLT [118,119,120]. In the German-Austrian AML Study Group (AMLSG) study, 12 patients out of 176 cases (7%) were considered to be therapy related and the secondary chromosomal abnormalities/mutations were not significantly different from de novo AML [120], suggesting that the additional mutation is not the reason for shorter event-free survival in t-AML patients after intensive chemotherapy.
In summary, t-AML with favorable cytogenetics shows similar response rate to their de novo counterpart when receiving a conventional AML treatment. However, compared to de novo counterparts, t-AML with favorable cytogenetics is associated with an inferior survival. This may relate to several factors such as the status of primary disease, toxicity from prior therapy, and additional genetic mutations. Considering that additional mutations in t-AML patients with favorable karyotypes may result in poor prognosis, comprehensive genetic tests may confer an appropriate decision making, especially in patients cured of the primary malignancy and who are good candidates for allogeneic HSCT.
Non-transplant Therapeutic Options for t-AML
Few retrospective studies have evaluated the efficacy of standard chemotherapy for t-AML. The German AML Cooperative Group analyzed outcomes after remission induction chemotherapy for 1511 de novo AML and 121 t-AML patients [121]. The study demonstrated that the survival of unfavorable and intermediate cytogenetic risk groups of t-AML was similar with the same risk groups of de novo AML (6 months vs. 7 months for unfavorable, 12 months vs. 16 months for intermediate-risk group, respectively). Another study, the German–Austrian AL Study Group assessed the clinical outcomes of 200 t-AML patients treated between 1993 and 2008 [3]. The survival of t-AML patients was compared with 2653 de novo AML patients. Although response rates to induction chemotherapy were similar, OS for t-AML patients was inferior to de novo AML patients. In further analysis, patients less than 60 years old showed similar relapse rates, but their death in CR was greater, suggesting the higher toxicity of induction and post-remission therapy in this cohort. Patients older than 60 years had higher relapse rates, possibly due to lower intensity treatments, resulting in inferior survival. A retrospective study of 118 t-AML after treatment of breast cancer showed no significant difference in median OS compared with de novo AML (8.7 months vs. 10.2 months; p = 0.17) [122]. Multivariate analysis revealed cytogenetics, baseline white blood cell counts, age, and performance status as predictive factors for OS of t-AML patients.
In a prospective study of t-MDS/AML, 32 t-MDS/AML patients were treated with high-dose cytarabine and mitoxantrone induction followed by hematopoietic stem cell transplant [101]. A remarkable complete response rate of 66% was achieved. Thirteen patients who achieved CR were eventually treated with AlloHSCT for consolidation and the survival of the patients was 29% in 3 years. These studies show that patients with t-AML can achieve a comparable response with standard induction chemotherapy, and that cumulative toxicity/reserved function from prior therapy limit tolerance to induction and post-remission therapy.
T-AML patients have a higher risk of organ dysfunction due to chemotherapy and radiation-induced parenchymal and vascular toxicity, or primary malignancy. Even those with seemingly adequate organ reserves may have increased toxicity during t-AML therapy. Therefore, earlier diagnosis and treatment with less toxic therapy, while aggressively exploring transplant options, may be another critical factor in the trial of new therapeutics for t-AML. Emerging therapeutics in this area has focused on several approaches. These include novel delivery of chemotherapy as well as newer DNA-damaging agents delivered through antibody-drug conjugates, use of hypomethylating agents, and molecularly directed small molecules against specific mutations commonly occurring in t-AML.
CPX-351 is a liposomal formulation of daunorubicin and cytarabine at a fixed ratio of 5:1. The combination of these medications was developed based on in vitro data that demonstrated a synergistic effect of these two agents at the 5:1 ratio [123]. In a randomized phase II trial, CPX-351 was compared with standard daunorubicin/cytarabine in untreated patients older than the age of 60 years [124]. In a subset of secondary AML patients (n = 52), which included t-AML and AML evolving from myelodysplastic syndrome, patients treated with CPX-351 demonstrated a better OS (hazard ratio = 0.46, p = 0.01) at 24 months. Though the recovery from cytopenias was slower after CPX-351, the infection-related deaths (3.5% vs. 7.3%) or 60-day mortality (4.7% vs. 14.6%) was less than the conventional daunorubicin/cytarabine chemotherapy group. These data suggested a clinical benefit with CPX-351 in t-AML with better efficacy and tolerability.
A second approach to improving cytotoxic therapy for AML takes advantage of newer antibody-drug conjugate (ADC) technology. CD33 is a surface receptor found on more than 95% of AML cells except acute megakaryocytic leukemia. It has been a target for antibody-directed therapy. The treatment with a conjugated antibody targeting CD33 (gemtuzumab ozogamicin) as a single agent [125], and in combination with chemotherapy in untreated patients and those with relapsed AML, demonstrated clinical efficacy [126]. However, gemtuzumab ozogamicin failed to show the effectiveness in combination with standard daunorubicin/cytarabine regimen in high-risk AML patients [127]. A new ADC targeting CD33, SGN-CD33A, was developed using a novel antibody drug linkage system to a fully humanized anti-CD33 antibody. In contrast to gemtuzumab ozogamicin, SGN-CD33A exhibited a potent cytotoxicity against p53-mutated AML cells and leukemic cells with multidrug resistance-mediated drug efflux phenotypes in preclinical studies [128]. Therefore, careful clinical trials with this monoclonal antibody conjugate are appropriate for t-AML patients.
Since many cases of t-AML evolved from a preleukemic phase after being exposed to chemotherapeutics/radiation, hypomethylating agents have been evaluated as an alternative to traditional induction therapy [129]. Both azacitidine and decitabine are effective and well tolerated but the efficacy compared with cytotoxic chemotherapy is still under investigation. In a retrospective study conducted by Quintas-Cardama et al., 671 AML patients, older than 65 years, were treated with a hypomethylating agent and had a similar median survival rates with cytotoxic chemotherapy (6.5 months with hypomethylating agent and 6.7 months with chemotherapy, respectively) [130]. Moreover, a similar CR rate was observed in the subset of poor-risk cytogenetics patients carrying −5 and/or −7 (26% with hypomethylating agent vs. 28% with chemotherapy). Another retrospective study of 48 t-MDS/AML patients treated with hypomethylating agent showed 42% overall response rate including a complete response rate of 21% in a subset of patients with favorable cytogenetics, which is comparable with prospective hypomethylating agent studies for t-MDS group [131]. A phase 2 clinical trial, E1905 North American Leukemia Intergroup, studied 47 patients including 18 t-AML patients. A good response to azacitidine occurred with 46% complete hematologic response and 13 months of median OS [132]. Multivariate analyses comparing the t-MN patient with de novo MDS/AML patients treated with the same protocol showed no significant difference in complete hematologic response rate, and overall response rate between the two groups. However, another study of 54 t-MN patients (including 12 t-AML patients) treated with azacitidine demonstrated shorter 2-year OS (14%) compared with de novo MDS/AML patients (33.9%), though multivariate analysis showed that the survival was dependent on cytogenetic changes, not etiology of the AML [133].
Hypomethylating agents are frequently prescribed as an alternative to traditional AML induction chemotherapy for frail patients. They can support de novo and t-MDS/AML patients in order to receive a transplantation with less toxicity, and may be a safer option for low-blast-count t-AML. Response rates were equivalent to standard AML induction therapy in this population [131, 134], enhancing the likelihood of successful transplantations. A new hypomethylating agent, SGI-110, a metabolite of decitabine, is in clinical trials for treatment of MDS and AML [135].
An additional epigenetic modulator is the class of histone deacetylation (HDAC) inhibitors . They are often included in a combination regimen with a hypomethylating agent for MDS and AML patients. Valproic acid, vorinostat, pracinostat, and mocetinostat are the HDAC inhibitors being used in clinical trials in combination with hypomethylating agents [136,137,138,139].
P53 mutations and MLL rearrangements often occur in t-AML [140, 141]. Two agents targeting these mutations are in the drug pipeline. EPZ-5676 is a potent inhibitor of Dot1L, a histone methyl transferase which interacts with MLL oncogenic fusion protein products. In cell lines and in rat xenograft studies, EPZ-5676 significantly caused cell death and regression of MLL-rearranged leukemias [142]. It is currently in clinical trial in pediatric leukemias with MLL translocations.
Volasertib is an inhibitor of polo-like kinase (PLK). Preclinical studies demonstrated that p53-mutated cancer cells were more susceptible to PLK inhibition than p53 wild-type cancer cells [143]. In a randomized phase 2 study in untreated elderly patients with AML, volasertib, in combination with low-dose cytarabine, demonstrated a higher remission rate and improved survival compared with cytarabine alone, although median survival rates were still <1 year [144].
Hematopoietic Stem Cell Transplant for t-AML
Treatment of t-AML with conventional therapy is associated with a poor outcome. Response rate for t-AML induction therapy appears to be roughly equivalent to de novo AML when compared within their respective intermediate- and unfavorable-risk cytogenetic categories, but the responses on average are less durable, thereby justifying the use of transplantation in these patients.
A retrospective study of 545 t-AML patients transplanted between 1990 and 2004 found an OS of 22% at 5 years [145]. Inferior outcomes were associated with age greater than 35 years, poor-risk cytogenetics, uncontrolled disease, and use of a non-sibling-related or mismatched unrelated donor. Use of reduced-intensity chemotherapy (RIC) regimens did not decrease treatment-related mortality (TRM) , which approached 50% at 5 years, but many of these patients had received a prior autologous transplant.
The European Group for Blood and Marrow Transplantation Group also reported on 461 t-MDS/AML patients, and noted an adverse impact of abnormal cytogenetics, age greater than 40 years, and uncontrolled disease [146]. Three-year relapse-free survival and OS rates were 33% and 35%, respectively. In contrast, a study of 24 breast cancer t-MN patients who underwent allogeneic stem cell transplantation for consolidation had nearly identical clinical results as female de novo MDS/AML patients regardless of cytogenetics [147]. In general, these studies show that transplantation can be used successfully in a fraction of t-AML patients, but it is clearly less effective than when used for de novo AML patients. A busulfan/cyclophosphamide conditioning regimen appears to offer one of the best 5-year relapse-free survival (43%) and lowest non-relapse mortality (28%). Relapse rates are lower with unrelated donor transplants [145, 146, 148]. After accounting for cytogenetic classification, t-AML patients have a similar outcome as de novo AML [149].
The Italian Network reported survival for transplant recipients of 58.8 months compared with 12.1 months for the non-transplant cohort [150]. A similar benefit was seen when the German Hodgkin Study Group reported clinical outcomes of 106 patients with t-MN after therapy for Hodgkin’s lymphoma. Although the non-transplant median survival was dismal (7.2 months), the median survival for the transplanted t-MN had not been reached after a median follow-up of 41 months [151]. The survival of the patients after hematopoietic stem cell transplant at 2 years was 47% vs. 15% for the non-transplant group (p = 0.03). Although alloHSCT can provide a chance of long-term survival and cure in selected subgroups of patients with t-AML, major limitations of alloHSCT are availability of a donor and patients’ age. Alternative treatment strategies including haploidentical donor alloHSCT or nonmyeloablative HSCT, especially for older patients, should be explored for t-AML patients.
Conclusion
Therapy-related AML (t-AML) is a recognizable subgroup of AML. Alkylating agents used in primary diseases are the most frequent etiology of t-AML. The disease arises from a series of mutations in hematopoietic stem cells, and these DNA changes provide a growth advantage to the progeny of the transformed cells. The abnormal clone of cells usually has a hypodiploid modal number of chromosomes and a deletion of part or all of chromosome 5 and/or 7. T-AML remains one of the most difficult subtypes of AML to treat. Once a patient who was treated with cytotoxic agents develops cytopenias, hematopoietic cell morphologic examination, immunophenotying, and cytogenetics should be done to detect t-AML in its early phase. The patients with t-AML have more comorbidities, decreased organ reserve, and a higher incidence of unfavorable cytogenetic phenotype than de novo AML. The key prognostic factors in t-AML are patient age, performance status, and karyotype. As de novo AML, t-AML patients can be stratified based on genetics. The performance status is the first determinant for establishing a treatment plan. Supportive care at initial diagnosis would be appropriate for patients with a poor performance status (ECOG PS >2). All medically fit patients should have HLA typing at initial diagnosis. The conventional cytotoxic chemotherapy or hypomethylating agents are being used as an initial therapy. For patients in complete remission, allogeneic transplantation is the best therapeutic modality for long-term survival for the younger patients. Emerging therapeutics for AML has focused on reduced toxicity, higher efficacy, and specificity. These include novel delivery of chemotherapy in liposome as well as newer DNA-damaging agents delivered through antibody-drug conjugates, use of hypomethylating agents, and molecularly directed small molecules against specific mutations commonly occurring in t-AML.
Abbreviations
- AD:
-
Autoimmune disease
- ADC:
-
Antibody-drug conjugate
- ALL:
-
Acute lymphoblastic leukemia
- AlloHSCT:
-
Allogeneic hematopoietic stem cell transplant
- AML:
-
Acute myelogenous leukemia
- ATRA:
-
All-trans retinoic acid
- AutoHSCT:
-
Autologous hematopoietic stem cell transplant
- CLL:
-
Chronic lymphocytic leukemia
- CR:
-
Complete remission
- ECOG:
-
Eastern Cooperative Oncology Group
- EGR-1:
-
Early growth response-1
- FLT3:
-
fms-related tyrosine kinase 3
- FPSG:
-
French Polycythemia Study Group
- G-CSF:
-
Granulocyte colony-stimulating factor
- GM-CSF:
-
Granulocyte-macrophage colony-stimulating factor
- HDAC:
-
Histone deacetylation
- HLA:
-
Human leukocyte antigen
- HSC:
-
Hematopoietic stem and progenitor cells
- IL:
-
Interleukins
- LDH:
-
Lactate dehydrogenase
- M-CSF:
-
Macrophage colony-stimulating factor
- MDR:
-
Multiple drug resistance
- MF:
-
Myelofibrosis
- MLL:
-
Mixed-lineage leukemia
- MPN:
-
Myleoproliferative neoplasia
- MRI:
-
Magnetic resonance imaging
- MUGA:
-
Multigated acquisition scan
- NHL:
-
Non-Hodgkin lymphoma
- OS:
-
Overall survival
- PBSC:
-
Peripheral blood stem cells
- PDGF:
-
Platelet-derived growth factor
- PET:
-
Positron emission tomography
- PLK:
-
Polo-like kinase
- PML:
-
Promyelocytic leukemia protein
- PVSG:
-
Polycythemia Vera Study Group
- RAEB:
-
Refractory anemia with excess blasts
- RAEB-t:
-
Refractory anemia with excess blasts in transformation
- RARA:
-
Retinoic acid receptor alpha
- RIC:
-
Reduced-intensity chemotherapy
- SCN:
-
Severe congenital neutropenia
- T-AML:
-
Therapy-related acute myelogenous leukemia
- T-APL:
-
Therapy-related acute promyelocytic leukemia
- T-MDS:
-
Therapy-related myelodysplastic syndrome
- T-MN:
-
Therapy-related myeloid neoplasm
- TNF:
-
Tumor necrosis factor
- TP53:
-
Tumor protein p53
- TRM:
-
Treatment-related mortality
- WBC:
-
White blood cell
References
Vardiman JW, Thiele J, Arber DA, Brunning RD, Borowitz MJ, Porwit A, et al. The 2008 revision of the World Health Organization (WHO) classification of myeloid neoplasms and acute leukemia: rationale and important changes. Blood. 2009;114(5):937–51. PubMed PMID: 19357394
Smith SM, Le Beau MM, Huo D, Karrison T, Sobecks RM, Anastasi J, et al. Clinical-cytogenetic associations in 306 patients with therapy-related myelodysplasia and myeloid leukemia: the University of Chicago series. Blood. 2003;102(1):43–52. PubMed PMID: 12623843
Kayser S, Dohner K, Krauter J, Kohne CH, Horst HA, Held G, et al. The impact of therapy-related acute myeloid leukemia (AML) on outcome in 2853 adult patients with newly diagnosed AML. Blood. 2011;17(7):2137–45. PubMed PMID: 21127174
Le Deley MC, Suzan F, Cutuli B, Delaloge S, Shamsaldin A, Linassier C, et al. Anthracyclines, mitoxantrone, radiotherapy, and granulocyte colony-stimulating factor: risk factors for leukemia and myelodysplastic syndrome after breast cancer. J Clin Oncol. 2007;25(3):292–300. PubMed PMID: 17159192
Smith RE, Bryant J, DeCillis A, Anderson S, National Surgical Adjuvant B, Bowel Project E. Acute myeloid leukemia and myelodysplastic syndrome after doxorubicin-cyclophosphamide adjuvant therapy for operable breast cancer: the National Surgical Adjuvant Breast and Bowel Project Experience. J Clin Oncol. 2003;21(7):1195–204. PubMed PMID: 12663705
Allan JM, Travis LB. Mechanisms of therapy-related carcinogenesis. Nat Rev Cancer. 2005;5(12):943–55. PubMed PMID: 16294218
Rowley JD, Golomb HM, Vardiman JW. Nonrandom chromosome abnormalities in acute leukemia and dysmyelopoietic syndromes in patients with previously treated malignant disease. Blood. 1981;58(4):759–67. PubMed PMID: 7272506
Traweek ST, Slovak ML, Nademanee AP, Brynes RK, Niland JC, Forman SJ. Clonal karyotypic hematopoietic cell abnormalities occurring after autologous bone marrow transplantation for Hodgkin’s disease and non-Hodgkin’s lymphoma. Blood. 1994;84(3):957–63. PubMed PMID: 8043877
Kantarjian HM, Keating MJ, Walters RS, Smith TL, Cork A, McCredie KB, et al. Therapy-related leukemia and myelodysplastic syndrome: clinical, cytogenetic, and prognostic features. J Clin Oncol. 1986;4(12):1748–57. PubMed PMID: 3783201
Gundestrup M, Klarskov Andersen M, Sveinbjornsdottir E, Rafnsson V, Storm HH, Pedersen-Bjergaard J. Cytogenetics of myelodysplasia and acute myeloid leukaemia in aircrew and people treated with radiotherapy. Lancet. 2000;356(9248):2158. PubMed PMID: 11191547
Pedersen-Bjergaard J. Insights into leukemogenesis from therapy-related leukemia. N Engl J Med. 2005;352(15):1591–4. PubMed PMID: 15829541
Tebbi CK, London WB, Friedman D, Villaluna D, De Alarcon PA, Constine LS, et al. Dexrazoxane-associated risk for acute myeloid leukemia/myelodysplastic syndrome and other secondary malignancies in pediatric Hodgkin’s disease. J Clin Oncol. 2007;25(5):493–500. PubMed PMID: 17290056
Pui CH, Relling MV. Topoisomerase II inhibitor-related acute myeloid leukaemia. Br J Haematol. 2000;109(1):13–23. PubMed PMID: 10848777
Casciato DA, Scott JL. Acute leukemia following prolonged cytotoxic agent therapy. Medicine. 1979;58(1):32–47. PubMed PMID: 105227
Greene MH, Harris EL, Gershenson DM, Malkasian GD Jr, Melton LJ 3rd, Dembo AJ, et al. Melphalan may be a more potent leukemogen than cyclophosphamide. Ann Intern Med. 1986;105(3):360–7. PubMed PMID: 3740675
Pui CH, Behm FG, Raimondi SC, Dodge RK, George SL, Rivera GK, et al. Secondary acute myeloid leukemia in children treated for acute lymphoid leukemia. N Engl J Med. 1989;321(3):136–42. PubMed PMID: 2787477
Ratain MJ, Kaminer LS, Bitran JD, Larson RA, Le Beau MM, Skosey C, et al. Acute nonlymphocytic leukemia following etoposide and cisplatin combination chemotherapy for advanced non-small-cell carcinoma of the lung. Blood. 1987;70(5):1412–7. PubMed PMID: 2822173
Berk PD, Goldberg JD, Donovan PB, Fruchtman SM, Berlin NI, Wasserman LR. Therapeutic recommendations in polycythemia Vera based on polycythemia Vera Study Group protocols. Semin Hematol. 1986;23(2):132–43. PubMed PMID: 3704665
Finazzi G, Caruso V, Marchioli R, Capnist G, Chisesi T, Finelli C, et al. Acute leukemia in polycythemia vera: an analysis of 1638 patients enrolled in a prospective observational study. Blood. 2005;105(7):2664–70. PubMed PMID: 15585653
Najean Y, Rain JD. Treatment of polycythemia vera: use of 32P alone or in combination with maintenance therapy using hydroxyurea in 461 patients greater than 65 years of age. The French Polycythemia Study Group. Blood. 1997;89(7):2319–27. PubMed PMID: 9116275
Bjorkholm M, Derolf AR, Hultcrantz M, Kristinsson SY, Ekstrand C, Goldin LR, et al. Treatment-related risk factors for transformation to acute myeloid leukemia and myelodysplastic syndromes in myeloproliferative neoplasms. J Clin Oncol. 2011;29(17):2410–5. PubMed PMID: 21537037. Pubmed Central PMCID: 3107755
Bizzozero OJ Jr, Johnson KG, Ciocco A. Radiation-related leukemia in Hiroshima and Nagasaki, 1946–1964. I. Distribution, incidence and appearance time. N Engl J Med. 1966;274(20):1095–101. PubMed PMID: 5932020
Ginevan ME. Nonlymphatic leukemias and adult exposure to diagnostic X-rays: the evidence reconsidered. Health Phys. 1980;38(2):129–38. PubMed PMID: 7372480
Seed TM, Tolle DV, Fritz TE, Devine RL, Poole CM, Norris WP. Irradiation-induced erythroleukemia and myelogenous leukemia in the beagle dog: hematology and ultrastructure. Blood. 1977;50(6):1061–79. PubMed PMID: 270374
Coltman CA Jr, Dixon DO. Second malignancies complicating Hodgkin’s disease: a Southwest Oncology Group 10-year followup. Cancer Treat Rep. 1982;66(4):1023–33. PubMed PMID: 7074630
Nardi V, Winkfield KM, Ok CY, Niemierko A, Kluk MJ, Attar EC, et al. Acute myeloid leukemia and myelodysplastic syndromes after radiation therapy are similar to de novo disease and differ from other therapy-related myeloid neoplasms. J Clin Oncol. 2012;30(19):2340–7. PubMed PMID: 22585703
Pedersen-Bjergaard J, Philip P, Mortensen BT, Ersboll J, Jensen G, Panduro J, et al. Acute nonlymphocytic leukemia, preleukemia, and acute myeloproliferative syndrome secondary to treatment of other malignant diseases. Clinical and cytogenetic characteristics and results of in vitro culture of bone marrow and HLA typing. Blood. 1981;57(4):712–23. PubMed PMID: 7470622
Cadman EC, Capizzi RL, Bertino JR. Acute nonlymphocytic leukemia: a delayed complication of Hodgkin’s disease therapy: analysis of 109 cases. Cancer. 1977;40(3):1280–96. PubMed PMID: 409479
Coleman CN, Williams CJ, Flint A, Glatstein EJ, Rosenberg SA, Kaplan HS. Hematologic neoplasia in patients treated for Hodgkin’s disease. N Engl J Med. 1977;297(23):1249–52. PubMed PMID: 917069
Valagussa P, Santoro A, Fossati Bellani F, Franchi F, Banfi A, Bonadonna G. Absence of treatment-induced second neoplasms after ABVD in Hodgkin’s disease. Blood. 1982;59(3):488–94. PubMed PMID: 6174160
Pedersen-Bjergaard J, Larsen SO. Incidence of acute nonlymphocytic leukemia, preleukemia, and acute myeloproliferative syndrome up to 10 years after treatment of Hodgkin’s disease. N Engl J Med. 1982;307(16):965–71. PubMed PMID: 7110299
Greene MH, Boice JD Jr, Greer BE, Blessing JA, Dembo AJ. Acute nonlymphocytic leukemia after therapy with alkylating agents for ovarian cancer: a study of five randomized clinical trials. N Engl J Med. 1982;307(23):1416–21. PubMed PMID: 6752720
De Braekeleer M. Cytogenetic studies in secondary leukemia: statistical analysis. Oncology. 1986;43(6):358–63. PubMed PMID: 3808568
Le Beau MM, Albain KS, Larson RA, Vardiman JW, Davis EM, Blough RR, et al. Clinical and cytogenetic correlations in 63 patients with therapy-related myelodysplastic syndromes and acute nonlymphocytic leukemia: further evidence for characteristic abnormalities of chromosomes no. 5 and 7. J Clin Oncol. 1986;4(3):325–45. PubMed PMID: 3950675
Wright JD, St Clair CM, Deutsch I, Burke WM, Gorrochurn P, Sun X, et al. Pelvic radiotherapy and the risk of secondary leukemia and multiple myeloma. Cancer. 2010;116(10):2486–92. PubMed PMID: 20209618
Sawka AM, Thabane L, Parlea L, Ibrahim-Zada I, Tsang RW, Brierley JD, et al. Second primary malignancy risk after radioactive iodine treatment for thyroid cancer: a systematic review and meta-analysis. Thyroid. 2009;19(5):451–7. PubMed PMID: 19281429
Dohner H, Estey EH, Amadori S, Appelbaum FR, Buchner T, Burnett AK, et al. Diagnosis and management of acute myeloid leukemia in adults: recommendations from an international expert panel, on behalf of the European LeukemiaNet. Blood. 2010;115(3):453–74. PubMed PMID: 19880497
Lyman GH, Dale DC, Wolff DA, Culakova E, Poniewierski MS, Kuderer NM, et al. Acute myeloid leukemia or myelodysplastic syndrome in randomized controlled clinical trials of cancer chemotherapy with granulocyte colony-stimulating factor: a systematic review. J Clin Oncol. 2010;28(17):2914–24. PubMed PMID: 20385991
Rosenberg PS, Alter BP, Bolyard AA, Bonilla MA, Boxer LA, Cham B, et al. The incidence of leukemia and mortality from sepsis in patients with severe congenital neutropenia receiving long-term G-CSF therapy. Blood. 2006;107(12):4628–35. PubMed PMID: 16497969. Pubmed Central PMCID: 1895804
Rosenberg PS, Zeidler C, Bolyard AA, Alter BP, Bonilla MA, Boxer LA, et al. Stable long-term risk of leukaemia in patients with severe congenital neutropenia maintained on G-CSF therapy. Br J Haematol. 2010;150(2):196–9. PubMed PMID: 20456363. Pubmed Central PMCID: 2906693
Anderson LA, Pfeiffer RM, Landgren O, Gadalla S, Berndt SI, Engels EA. Risks of myeloid malignancies in patients with autoimmune conditions. Br J Cancer. 2009;100(5):822–8. PubMed PMID: 19259097. Pubmed Central PMCID: 2653768
Kristinsson SY, Bjorkholm M, Hultcrantz M, Derolf AR, Landgren O, Goldin LR. Chronic immune stimulation might act as a trigger for the development of acute myeloid leukemia or myelodysplastic syndromes. J Clin Oncol. 2011;29(21):2897–903. PubMed PMID: 21690473. Pubmed Central PMCID: 3138717
Bernatsky S, Clarke AE, Suissa S. Hematologic malignant neoplasms after drug exposure in rheumatoid arthritis. Arch Intern Med. 2008;168(4):378–81. PubMed PMID: 18299492
Ramkumar B, Chadha MK, Barcos M, Sait SN, Heyman MR, Baer MR. Acute promyelocytic leukemia after mitoxantrone therapy for multiple sclerosis. Cancer Genet Cytogenet. 2008;182(2):126–9. PubMed PMID: 18406875
Ammatuna E, Montesinos P, Hasan SK, Ramadan SM, Esteve J, Hubmann M, et al. Presenting features and treatment outcome of acute promyelocytic leukemia arising after multiple sclerosis. Haematologica. 2011;96(4):621–5. PubMed PMID: 21193421. Pubmed Central PMCID: 3069242
Leleu X, Soumerai J, Roccaro A, Hatjiharissi E, Hunter ZR, Manning R, et al. Increased incidence of transformation and myelodysplasia/acute leukemia in patients with Waldenstrom macroglobulinemia treated with nucleoside analogs. J Clin Oncol. 2009;27(2):250–5. PubMed PMID: 19064987
Coso D, Costello R, Cohen-Valensi R, Sainty D, Nezri M, Gastaut JA, et al. Acute myeloid leukemia and myelodysplasia in patients with chronic lymphocytic leukemia receiving fludarabine as initial therapy. Ann Oncol. 1999;10(3):362–3. PubMed PMID: 10355587
Morrison VA, Rai KR, Peterson BL, Kolitz JE, Elias L, Appelbaum FR, et al. Therapy-related myeloid leukemias are observed in patients with chronic lymphocytic leukemia after treatment with fludarabine and chlorambucil: results of an intergroup study, cancer and leukemia group B 9011. J Clin Oncol. 2002;20(18):3878–84. PubMed PMID: 12228208
Anderson RL, Bagby GC Jr, Richert-Boe K, Magenis RE, Koler RD. Therapy-related preleukemic syndrome. Cancer. 1981;47(7):1867–71. PubMed PMID: 7226081
Kapadia SB, Krause JR, Ellis LD, Pan SF, Wald N. Induced acute non-lymphocytic leukemia following long-term chemotherapy: a study of 20 cases. Cancer. 1980;45(6):1315–21. PubMed PMID: 6928396
Papa G, Alimena G, Annino L, Anselmo AP, Ciccone F, De Luca AM, et al. Acute non lymphoid leukaemia following Hodgkin’s disease. Clinical, biological and cytogenetic aspects of 3 cases. Scand J Haematol. 1979;23(4):339–47. PubMed PMID: 295150
Pedersen-Bjergaard J, Rowley JD. The balanced and the unbalanced chromosome aberrations of acute myeloid leukemia may develop in different ways and may contribute differently to malignant transformation. Blood. 1994;83(10):2780–6. PubMed PMID: 8180374
Chromosomes in acute non-lymphocytic leukaemia. First International Workshop on Chromosomes in Leukaemia. Br J Haematol. 1978;39(3):311–6. PubMed PMID: 698112
Le Beau MM, Espinosa R 3rd, Neuman WL, Stock W, Roulston D, Larson RA, et al. Cytogenetic and molecular delineation of the smallest commonly deleted region of chromosome 5 in malignant myeloid diseases. Proc Natl Acad Sci U S A. 1993;90(12):5484–8. PubMed PMID: 8516290. Pubmed Central PMCID: 46745
Le Beau MM, Epstein ND, O’Brien SJ, Nienhuis AW, Yang YC, Clark SC, et al. The interleukin 3 gene is located on human chromosome 5 and is deleted in myeloid leukemias with a deletion of 5q. Proc Natl Acad Sci U S A. 1987;84(16):5913–7. PubMed PMID: 3497400. Pubmed Central PMCID: 298973
Le Beau MM, Lemons RS, Espinosa R 3rd, Larson RA, Arai N, Rowley JD. Interleukin-4 and interleukin-5 map to human chromosome 5 in a region encoding growth factors and receptors and are deleted in myeloid leukemias with a del(5q). Blood. 1989;73(3):647–50. PubMed PMID: 2783863
Nienhuis AW, Bunn HF, Turner PH, Gopal TV, Nash WG, O’Brien SJ, et al. Expression of the human c-fms proto-oncogene in hematopoietic cells and its deletion in the 5q- syndrome. Cell. 1985;42(2):421–8. PubMed PMID: 4028159
Le Beau MM, Westbrook CA, Diaz MO, Larson RA, Rowley JD, Gasson JC, et al. Evidence for the involvement of GM-CSF and FMS in the deletion (5q) in myeloid disorders. Science. 1986;231(4741):984–7. PubMed PMID: 3484837
Levine EG, Bloomfield CD. Leukemias and myelodysplastic syndromes secondary to drug, radiation, and environmental exposure. Semin Oncol. 1992;19(1):47–84. PubMed PMID: 1736370
List AF, Jacobs A. Biology and pathogenesis of the myelodysplastic syndromes. Semin Oncol. 1992;19(1):14–24. PubMed PMID: 1736366
Tsui LC, Farrall M, Donis-Keller H. Report of the committee on the genetic constitution of chromosomes 7 and 8. Cytogenet Cell Genet. 1989;51(1–4):166–201. PubMed PMID: 2676369
Kere J, Donis-Keller H, Ruutu T, de la Chapelle A. Chromosome 7 long-arm deletions in myeloid disorders: terminal DNA sequences are commonly conserved and breakpoints vary. Cytogenet Cell Genet. 1989;50(4):226–9. PubMed PMID: 2805820
Quesnel B, Kantarjian H, Bjergaard JP, Brault P, Estey E, Lai JL, et al. Therapy-related acute myeloid leukemia with t(8;21), inv (16), and t(8;16): a report on 25 cases and review of the literature. J Clin Oncol. 1993;11(12):2370–9. PubMed PMID: 8246025
Pedersen-Bjergaard J, Johansson B, Philip P. Translocation (3;21)(q26;q22) in therapy-related myelodysplasia following drugs targeting DNA-topoisomerase II combined with alkylating agents, and in myeloproliferative disorders undergoing spontaneous leukemic transformation. Cancer Genet Cytogenet. 1994;76(1):50–5. PubMed PMID: 8076352
Pedersen-Bjergaard J, Philip P, Larsen SO, Jensen G, Byrsting K. Chromosome aberrations and prognostic factors in therapy-related myelodysplasia and acute nonlymphocytic leukemia. Blood. 1990;76(6):1083–91. PubMed PMID: 2400804
Johansson B, Mertens F, Heim S, Kristoffersson U, Mitelman F. Cytogenetics of secondary myelodysplasia (sMDS) and acute nonlymphocytic leukemia (sANLL). Eur J Haematol. 1991;47(1):17–27. PubMed PMID: 1868912
Cimino G, Moir DT, Canaani O, Williams K, Crist WM, Katzav S, et al. Cloning of ALL-1, the locus involved in leukemias with the t(4;11)(q21;q23), t(9;11)(p22;q23), and t(11;19)(q23;p13) chromosome translocations. Cancer Res. 1991;51(24):6712–4. PubMed PMID: 1835902
Ziemin-van der Poel S, NR MC, Gill HJ, Espinosa R 3rd, Patel Y, Harden A, et al. Identification of a gene, MLL, that spans the breakpoint in 11q23 translocations associated with human leukemias. Proc Natl Acad Sci U S A. 1991;88(23):10735–9. PubMed PMID: 1720549. Pubmed Central PMCID: 53005
Marschalek R. Systematic classification of mixed-lineage leukemia fusion partners predicts additional cancer pathways. Ann Lab Med. 2016;36(2):85–100. PubMed PMID: 26709255. Pubmed Central PMCID: 4713862
Rowley JD, Olney HJ. International workshop on the relationship of prior therapy to balanced chromosome aberrations in therapy-related myelodysplastic syndromes and acute leukemia: overview report. Genes Chromosomes Cancer. 2002;33(4):331–45. PubMed PMID: 11921269
Baccarani M, Bosi A, Papa G. Second malignancy in patients treated by Hodgkin’s disease. Cancer. 1980;46(8):1735–40. PubMed PMID: 6932997
Bernstein ML, Vekemans MJ. Chromosomal changes in secondary leukemias of childhood and young adulthood. Crit Rev Oncol Hematol. 1986;5(4):325–60. PubMed PMID: 3533293
Aksoy M, Erdem S. Followup study on the mortality and the development of leukemia in 44 pancytopenic patients with chronic exposure to benzene. Blood. 1978;52(2):285–92. PubMed PMID: 667356
Seedhouse C, Faulkner R, Ashraf N, Das-Gupta E, Russell N. Polymorphisms in genes involved in homologous recombination repair interact to increase the risk of developing acute myeloid leukemia. Clin Cancer Res. 2004;10(8):2675–80. PubMed PMID: 15102670
Knight JA, Skol AD, Shinde A, Hastings D, Walgren RA, Shao J, et al. Genome-wide association study to identify novel loci associated with therapy-related myeloid leukemia susceptibility. Blood. 2009;113(22):5575–82. PubMed PMID: 19299336. Pubmed Central PMCID: 2689055
Larson RA, Wang Y, Banerjee M, Wiemels J, Hartford C, Le Beau MM, et al. Prevalence of the inactivating 609C-->T polymorphism in the NAD(P)H:quinone oxidoreductase (NQO1) gene in patients with primary and therapy-related myeloid leukemia. Blood. 1999;94(2):803–7. PubMed PMID: 10397748
Allan JM, Wild CP, Rollinson S, Willett EV, Moorman AV, Dovey GJ, et al. Polymorphism in glutathione S-transferase P1 is associated with susceptibility to chemotherapy-induced leukemia. Proc Natl Acad Sci U S A. 2001;98(20):11592–7. PubMed PMID: 11553769. Pubmed Central PMCID: 58774
Ellis NA, Huo D, Yildiz O, Worrillow LJ, Banerjee M, Le Beau MM, et al. MDM2 SNP309 and TP53 Arg72Pro interact to alter therapy-related acute myeloid leukemia susceptibility. Blood. 2008;112(3):741–9. PubMed PMID: 18426989. Pubmed Central PMCID: 2481552
Voso MT, Fabiani E, Zang Z, Fianchi L, Falconi G, Padella A, et al. Fanconi anemia gene variants in therapy-related myeloid neoplasms. Blood Cancer J. 2015;5:e323. PubMed PMID: 26140431. Pubmed Central PMCID: 4526773
Pedersen-Bjergaard J, Andersen MT, Andersen MK. Genetic pathways in the pathogenesis of therapy-related myelodysplasia and acute myeloid leukemia. Hematology. 2007:392–7. PubMed PMID: 18024656
Li L, Li M, Sun C, Francisco L, Chakraborty S, Sabado M, et al. Altered hematopoietic cell gene expression precedes development of therapy-related myelodysplasia/acute myeloid leukemia and identifies patients at risk. Cancer Cell. 2011;20(5):591–605. PubMed PMID: 22094254. Pubmed Central PMCID: 3220884
Ok CY, Patel KP, Garcia-Manero G, Routbort MJ, Fu B, Tang G, et al. Mutational profiling of therapy-related myelodysplastic syndromes and acute myeloid leukemia by next generation sequencing, a comparison with de novo diseases. Leuk Res. 2015;39(3):348–54. PubMed PMID: 25573287
Wong TN, Ramsingh G, Young AL, Miller CA, Touma W, Welch JS, et al. Role of TP53 mutations in the origin and evolution of therapy-related acute myeloid leukaemia. Nature. 2015;518(7540):552–5. PubMed PMID: 25487151. Pubmed Central PMCID: 4403236
Lindsley RC, Mar BG, Mazzola E, Grauman PV, Shareef S, Allen SL, et al. Acute myeloid leukemia ontogeny is defined by distinct somatic mutations. Blood. 2015;125(9):1367–76. PubMed PMID: 25550361. Pubmed Central PMCID: 4342352
Link DC, Kunter G, Kasai Y, Zhao Y, Miner T, McLellan MD, et al. Distinct patterns of mutations occurring in de novo AML versus AML arising in the setting of severe congenital neutropenia. Blood. 2007;110(5):1648–55. PubMed PMID: 17494858. Pubmed Central PMCID: 1975847
Skokowa J, Steinemann D, Katsman-Kuipers JE, Zeidler C, Klimenkova O, Klimiankou M, et al. Cooperativity of RUNX1 and CSF3R mutations in severe congenital neutropenia: a unique pathway in myeloid leukemogenesis. Blood. 2014;123(14):2229–37. PubMed PMID: 24523240
Vainchenker W, Delhommeau F, Constantinescu SN, Bernard OA. New mutations and pathogenesis of myeloproliferative neoplasms. Blood. 2011;118(7):1723–35. PubMed PMID: 21653328
Klampfl T, Harutyunyan A, Berg T, Gisslinger B, Schalling M, Bagienski K, et al. Genome integrity of myeloproliferative neoplasms in chronic phase and during disease progression. Blood. 2011;118(1):167–76. PubMed PMID: 21531982
Campbell PJ, Baxter EJ, Beer PA, Scott LM, Bench AJ, Huntly BJ, et al. Mutation of JAK2 in the myeloproliferative disorders: timing, clonality studies, cytogenetic associations, and role in leukemic transformation. Blood. 2006;108(10):3548–55. PubMed PMID: 16873677
Thoennissen NH, Krug UO, Lee DH, Kawamata N, Iwanski GB, Lasho T, et al. Prevalence and prognostic impact of allelic imbalances associated with leukemic transformation of Philadelphia chromosome-negative myeloproliferative neoplasms. Blood. 2010;115(14):2882–90. PubMed PMID: 20068225. Pubmed Central PMCID: 2854432
Vannucchi AM, Lasho TL, Guglielmelli P, Biamonte F, Pardanani A, Pereira A, et al. Mutations and prognosis in primary myelofibrosis. Leukemia. 2013;27(9):1861–9. PubMed PMID: 23619563
Zhang SJ, Rampal R, Manshouri T, Patel J, Mensah N, Kayserian A, et al. Genetic analysis of patients with leukemic transformation of myeloproliferative neoplasms shows recurrent SRSF2 mutations that are associated with adverse outcome. Blood. 2012;119(19):4480–5. PubMed PMID: 22431577. Pubmed Central PMCID: 3362363
Theocharides A, Boissinot M, Girodon F, Garand R, Teo SS, Lippert E, et al. Leukemic blasts in transformed JAK2-V617F-positive myeloproliferative disorders are frequently negative for the JAK2-V617F mutation. Blood. 2007;110(1):375–9. PubMed PMID: 17363731
Tefferi A, Lasho TL, Abdel-Wahab O, Guglielmelli P, Patel J, Caramazza D, et al. IDH1 and IDH2 mutation studies in 1473 patients with chronic-, fibrotic- or blast-phase essential thrombocythemia, polycythemia vera or myelofibrosis. Leukemia. 2010;24(7):1302–9. PubMed PMID: 20508616. Pubmed Central PMCID: 3035975
Dreyfus B. Preleukemic states. I. Definition and classification. II. Refractory anemia with an excess of myeloblasts in the bone marrow (smoldering acute leukemia). Nouvelle revue francaise d’hematologie. Blood Cells. 1976;17(1–2):33–55. PubMed PMID: 1005106
Koeffler HP, Golde DW. Human myeloid leukemia cell lines: a review. Blood. 1980;56(3):344–50. PubMed PMID: 6996765
Rowley JD, Alimena G, Garson OM, Hagemeijer A, Mitelman F, Prigogina EL. A collaborative study of the relationship of the morphological type of acute nonlymphocytic leukemia with patient age and karyotype. Blood. 1982;59(5):1013–22. PubMed PMID: 6951613
Saarni MI, Linman JW. Preleukemia. The hematologic syndrome preceding acute leukemia. Am J Med. 1973;55(1):38–48. PubMed PMID: 4515079
Kantarjian HM, Estey EH, Keating MJ. Treatment of therapy-related leukemia and myelodysplastic syndrome. Hematol Oncol Clin N Am. 1993;7(1):81–107. PubMed PMID: 7680643
Dohy H, Genot JY, Imbert M, D’Agay MF, Sultan C. Myelodysplasia and leukaemia related to chemotherapy and/or radiotherapy--a haematological study of 13 cases. Value of macrocytosis as an early sign of bone marrow injury. Clin Lab Haematol. 1980;2(2):111–9. PubMed PMID: 6931004
Ballen KK, Antin JH. Treatment of therapy-related acute myelogenous leukemia and myelodysplastic syndromes. Hematol Oncol Clin N Am. 1993;7(2):477–93. PubMed PMID: 8468276
Vardiman JW, Golomb HM, Rowley JD, Variakojis D. Acute nonlymphocytic leukemia in malignant lymphoma: a morphologic study. Cancer. 1978;42(1):229–42. PubMed PMID: 276415
Khaleeli M, Keane WM, Lee GR. Sideroblastic anemia in multiple myeloma: a preleukemic change. Blood. 1973;41(1):17–25. PubMed PMID: 4118108
Maldonado JE, Maigne J, Lecoq D. Comparative electron-microscopic study of the erythrocytic line in refractory anemia (preleukemia) and myelomonocytic leukemia. Nouvelle revue francaise d’hematologie. Blood Cells. 1976;17(1–2):167–85. PubMed PMID: 1069972
Vardiman JW, Coelho A, Golomb HM, Rowley J. Morphologic and cytochemical observations on the overt leukemic phase of therapy-related leukemia. Am J Clin Pathol. 1983;79(5):525–30. PubMed PMID: 6188364
Churpek JE, Larson RA. The evolving challenge of therapy-related myeloid neoplasms. Best Pract Res Clin Haematol. 2013;26(4):309–17. PubMed PMID: 24507808. Pubmed Central PMCID: 3920194
Fenaux P, Lucidarme D, Lai JL, Bauters F. Favorable cytogenetic abnormalities in secondary leukemia. Cancer. 1989;63(12):2505–8. PubMed PMID: 2720600
Lee EJ, George SL, Caligiuri M, Szatrowski TP, Powell BL, Lemke S, et al. Parallel phase I studies of daunorubicin given with cytarabine and etoposide with or without the multidrug resistance modulator PSC-833 in previously untreated patients 60 years of age or older with acute myeloid leukemia: results of cancer and leukemia group B study 9420. J Clin Oncol. 1999;17(9):2831–9. PubMed PMID: 10561359
Beaumont M, Sanz M, Carli PM, Maloisel F, Thomas X, Detourmignies L, et al. Therapy-related acute promyelocytic leukemia. J Clin Oncol. 2003;21(11):2123–37. PubMed PMID: 12775738
Duffield AS, Aoki J, Levis M, Cowan K, Gocke CD, Burns KH, et al. Clinical and pathologic features of secondary acute promyelocytic leukemia. Am J Clin Pathol. 2012;137(3):395–402. PubMed PMID: 22338051. Pubmed Central PMCID: 3578661
Ottone T, Cicconi L, Hasan SK, Lavorgna S, Divona M, Voso MT, et al. Comparative molecular analysis of therapy-related and de novo acute promyelocytic leukemia. Leuk Res. 2012;36(4):474–8. PubMed PMID: 22071137
Yin CC, Glassman AB, Lin P, Valbuena JR, Jones D, Luthra R, et al. Morphologic, cytogenetic, and molecular abnormalities in therapy-related acute promyelocytic leukemia. Am J Clin Pathol. 2005;123(6):840–8. PubMed PMID: 15899774
Elliott MA, Letendre L, Tefferi A, Hogan WJ, Hook C, Kaufmann SH, et al. Therapy-related acute promyelocytic leukemia: observations relating to APL pathogenesis and therapy. Eur J Haematol. 2012;88(3):237–43. PubMed PMID: 22023492
Slovak ML, Bedell V, Popplewell L, Arber DA, Schoch C, Slater R. 21q22 balanced chromosome aberrations in therapy-related hematopoietic disorders: report from an international workshop. Genes Chromosomes Cancer. 2002;33(4):379–94. PubMed PMID: 11921272
Gustafson SA, Lin P, Chen SS, Chen L, Abruzzo LV, Luthra R, et al. Therapy-related acute myeloid leukemia with t(8;21) (q22;q22) shares many features with de novo acute myeloid leukemia with t(8;21)(q22;q22) but does not have a favorable outcome. Am J Clin Pathol. 2009;131(5):647–55. PubMed PMID: 19369623
Krauth MT, Eder C, Alpermann T, Bacher U, Nadarajah N, Kern W, et al. High number of additional genetic lesions in acute myeloid leukemia with t(8;21)/RUNX1-RUNX1T1: frequency and impact on clinical outcome. Leukemia. 2014;28(7):1449–58. PubMed PMID: 24402164
Andersen MK, Larson RA, Mauritzson N, Schnittger S, Jhanwar SC, Pedersen-Bjergaard J. Balanced chromosome abnormalities inv (16) and t(15;17) in therapy-related myelodysplastic syndromes and acute leukemia: report from an international workshop. Genes Chromosomes Cancer. 2002;33(4):395–400. PubMed PMID: 11921273
Goemans BF, Zwaan CM, Miller M, Zimmermann M, Harlow A, Meshinchi S, et al. Mutations in KIT and RAS are frequent events in pediatric core-binding factor acute myeloid leukemia. Leukemia. 2005;19(9):1536–42. PubMed PMID: 16015387
Haferlach C, Dicker F, Kohlmann A, Schindela S, Weiss T, Kern W, et al. AML with CBFB-MYH11 rearrangement demonstrate RAS pathway alterations in 92% of all cases including a high frequency of NF1 deletions. Leukemia. 2010;24(5):1065–9. PubMed PMID: 20164853
Paschka P, Du J, Schlenk RF, Gaidzik VI, Bullinger L, Corbacioglu A, et al. Secondary genetic lesions in acute myeloid leukemia with inv (16) or t(16;16): a study of the German-Austrian AML Study Group (AMLSG). Blood. 2013;121(1):170–7. PubMed PMID: 23115274
Kern W, Haferlach T, Schnittger S, Hiddemann W, Schoch C. Prognosis in therapy-related acute myeloid leukemia and impact of karyotype. J Clin Oncol. 2004;22(12):2510–1. PubMed PMID: 15197216
Chen Y, Estrov Z, Pierce S, Qiao W, Borthakur G, Ravandi F, et al. Myeloid neoplasms after breast cancer: "therapy-related" not an independent poor prognostic factor. Leuk Lymphoma. 2015;56(4):1012–9. PubMed PMID: 25048874. Pubmed Central PMCID: 4326620
Kim HP, Gerhard B, Harasym TO, Mayer LD, Hogge DE. Liposomal encapsulation of a synergistic molar ratio of cytarabine and daunorubicin enhances selective toxicity for acute myeloid leukemia progenitors as compared to analogous normal hematopoietic cells. Exp Hematol. 2011;39(7):741–50. PubMed PMID: 21530609
Lancet JE, Cortes JE, Hogge DE, Tallman MS, Kovacsovics TJ, Damon LE, et al. Phase 2 trial of CPX-351, a fixed 5:1 molar ratio of cytarabine/daunorubicin, vs cytarabine/daunorubicin in older adults with untreated AML. Blood. 2014;123(21):3239–46. PubMed PMID: 24687088. Pubmed Central PMCID: 4624448
Sievers EL, Larson RA, Stadtmauer EA, Estey E, Lowenberg B, Dombret H, et al. Efficacy and safety of gemtuzumab ozogamicin in patients with CD33-positive acute myeloid leukemia in first relapse. J Clin Oncol. 2001;19(13):3244–54. PubMed PMID: 11432892
Kharfan-Dabaja MA, Hamadani M, Reljic T, Pyngolil R, Komrokji RS, Lancet JE, et al. Gemtuzumab ozogamicin for treatment of newly diagnosed acute myeloid leukaemia: a systematic review and meta-analysis. Br J Haematol. 2013;163(3):315–25. PubMed PMID: 24033280
Burnett AK, Hills RK, Milligan D, Kjeldsen L, Kell J, Russell NH, et al. Identification of patients with acute myeloblastic leukemia who benefit from the addition of gemtuzumab ozogamicin: results of the MRC AML15 trial. J Clin Oncol. 2011;29(4):369–77. PubMed PMID: 21172891
Kung Sutherland MS, Walter RB, Jeffrey SC, Burke PJ, Yu C, Kostner H, et al. SGN-CD33A: a novel CD33-targeting antibody-drug conjugate using a pyrrolobenzodiazepine dimer is active in models of drug-resistant AML. Blood. 2013;122(8):1455–63. PubMed PMID: 23770776
Tawfik B, Sliesoraitis S, Lyerly S, Klepin HD, Lawrence J, Isom S, et al. Efficacy of the hypomethylating agents as frontline, salvage, or consolidation therapy in adults with acute myeloid leukemia (AML). Ann Hematol. 2014;93(1):47–55. PubMed PMID: 24149914. Pubmed Central PMCID: 3879720
Quintas-Cardama A, Ravandi F, Liu-Dumlao T, Brandt M, Faderl S, Pierce S, et al. Epigenetic therapy is associated with similar survival compared with intensive chemotherapy in older patients with newly diagnosed acute myeloid leukemia. Blood. 2012;120(24):4840–5. PubMed PMID: 23071272. Pubmed Central PMCID: 3952725
Fianchi L, Criscuolo M, Lunghi M, Gaidano G, Breccia M, Levis A, et al. Outcome of therapy-related myeloid neoplasms treated with azacitidine. J Hematol Oncol. 2012;5:44. PubMed PMID: 22853048. Pubmed Central PMCID: 3419605
Prebet T, Sun Z, Ketterling RP, Zeidan A, Greenberg P, Herman J, et al. Azacitidine with or without Entinostat for the treatment of therapy-related myeloid neoplasm: further results of the E1905 North American leukemia intergroup study. Br J Haematol. 2016;172(3):384–91. PubMed PMID: 26577691. Pubmed Central PMCID: 4794257
Bally C, Thepot S, Quesnel B, Vey N, Dreyfus F, Fadlallah J, et al. Azacitidine in the treatment of therapy related myelodysplastic syndrome and acute myeloid leukemia (tMDS/AML): a report on 54 patients by the Groupe francophone des Myelodysplasies (GFM). Leuk Res. 2013;37(6):637–40. PubMed PMID: 23499498
Klimek VM, Dolezal EK, Tees MT, Devlin SM, Stein K, Romero A, et al. Efficacy of hypomethylating agents in therapy-related myelodysplastic syndromes. Leuk Res. 2012;36(9):1093–7. PubMed PMID: 22608310
Montalban-Bravo G, Garcia-Manero G. Novel drugs for older patients with acute myeloid leukemia. Leukemia. 2015;29(4):760–9. PubMed PMID: 25142817
Kuendgen A, Bug G, Ottmann OG, Haase D, Schanz J, Hildebrandt B, et al. Treatment of poor-risk myelodysplastic syndromes and acute myeloid leukemia with a combination of 5-azacytidine and valproic acid. Clin Epigenetics. 2011;2(2):389–99. PubMed PMID: 22704349. Pubmed Central PMCID: 3365387
Gore SD, Hermes-DeSantis ER. Future directions in myelodysplastic syndrome: newer agents and the role of combination approaches. Cancer Control. 2008;15(Suppl):40–9. PubMed PMID: 18813208. Pubmed Central PMCID: 2727156
Bose P, Grant S. Orphan drug designation for pracinostat, volasertib and alvocidib in AML. Leuk Res. 2014;38(8):862–5. PubMed PMID: 24996975
Boumber Y, Younes A, Garcia-Manero G. Mocetinostat (MGCD0103): a review of an isotype-specific histone deacetylase inhibitor. Expert Opin Invest Drugs. 2011;20(6):823–9. PubMed PMID: 21554162
Shih AH, Chung SS, Dolezal EK, Zhang SJ, Abdel-Wahab OI, Park CY, et al. Mutational analysis of therapy-related myelodysplastic syndromes and acute myelogenous leukemia. Haematologica. 2013;98(6):908–12. PubMed PMID: 23349305. Pubmed Central PMCID: 3669447
Pedersen-Bjergaard J, Andersen MK, Andersen MT, Christiansen DH. Genetics of therapy-related myelodysplasia and acute myeloid leukemia. Leukemia. 2008;22(2):240–8. PubMed PMID: 18200041
Daigle SR, Olhava EJ, Therkelsen CA, Basavapathruni A, Jin L, Boriack-Sjodin PA, et al. Potent inhibition of DOT1L as treatment of MLL-fusion leukemia. Blood. 2013;122(6):1017–25. PubMed PMID: 23801631. Pubmed Central PMCID: 3739029
Degenhardt Y, Greshock J, Laquerre S, Gilmartin AG, Jing J, Richter M, et al. Sensitivity of cancer cells to Plk1 inhibitor GSK461364A is associated with loss of p53 function and chromosome instability. Mol Cancer Ther. 2010;9(7):2079–89. PubMed PMID: 20571075
Dohner H, Lubbert M, Fiedler W, Fouillard L, Haaland A, Brandwein JM, et al. Randomized, phase 2 trial of low-dose cytarabine with or without volasertib in AML patients not suitable for induction therapy. Blood. 2014;124(9):1426–33. PubMed PMID: 25006120. Pubmed Central PMCID: 4148765
Litzow MR, Tarima S, Perez WS, Bolwell BJ, Cairo MS, Camitta BM, et al. Allogeneic transplantation for therapy-related myelodysplastic syndrome and acute myeloid leukemia. Blood. 2010;115(9):1850–7. PubMed PMID: 20032503. Pubmed Central PMCID: 2832815
Kroger N, Brand R, van Biezen A, Zander A, Dierlamm J, Niederwieser D, et al. Risk factors for therapy-related myelodysplastic syndrome and acute myeloid leukemia treated with allogeneic stem cell transplantation. Haematologica. 2009;94(4):542–9. PubMed PMID: 19278968. Pubmed Central PMCID: 2663618
Armand P, Kim HT, Mayer E, Cutler CS, Ho VT, Koreth J, et al. Outcome of allo-SCT for women with MDS or AML occurring after breast cancer therapy. Bone Marrow Transplant. 2010;45(11):1611–7. PubMed PMID: 20154738. Pubmed Central PMCID: 2889243
Witherspoon RP, Deeg HJ, Storer B, Anasetti C, Storb R, Appelbaum FR. Hematopoietic stem-cell transplantation for treatment-related leukemia or myelodysplasia. J Clin Oncol. 2001;19(8):2134–41. PubMed PMID: 11304765
Armand P, Kim HT, DeAngelo DJ, Ho VT, Cutler CS, Stone RM, et al. Impact of cytogenetics on outcome of de novo and therapy-related AML and MDS after allogeneic transplantation. Biol Blood Marrow Transplant. 2007;13(6):655–64. PubMed PMID: 17531775. Pubmed Central PMCID: 2743535
Fianchi L, Pagano L, Piciocchi A, Candoni A, Gaidano G, Breccia M, et al. Characteristics and outcome of therapy-related myeloid neoplasms: report from the Italian network on secondary leukemias. Am J Hematol. 2015;90(5):E80–5. PubMed PMID: 25653205
Eichenauer DA, Thielen I, Haverkamp H, Franklin J, Behringer K, Halbsguth T, et al. Therapy-related acute myeloid leukemia and myelodysplastic syndromes in patients with Hodgkin lymphoma: a report from the German Hodgkin Study Group. Blood. 2014;123(11):1658–64. PubMed PMID: 24478403
Acknowledgments
H.C.S. is supported by John C. Hall Memorial Research Grant of Tower Cancer Research Foundation. H.P.K. is the holder of the Mark Goodson endowed Chair in Oncology Research at Cedars Sinai and a member of the Jonsson Comprehensive Cancer Center and Molecular Biology Institute at UCLA, as well as the Cancer Science Institute of Singapore, and is supported by the A*STaR award from the National University of Singapore and NIH RO-1 grant.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2018 Springer International Publishing AG, part of Springer Nature
About this chapter
Cite this chapter
Suh, H.C., Koeffler, H.P. (2018). Therapy-Related Acute Myelogenous Leukemia. In: Wiernik, P., Dutcher, J., Gertz, M. (eds) Neoplastic Diseases of the Blood. Springer, Cham. https://doi.org/10.1007/978-3-319-64263-5_22
Download citation
DOI: https://doi.org/10.1007/978-3-319-64263-5_22
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-319-64262-8
Online ISBN: 978-3-319-64263-5
eBook Packages: MedicineMedicine (R0)