Abstract
The endocrine nature of bones and skeletal muscles has become evident with the identification of several secreted molecules from these tissues. Cell based studies have demonstrated that conditioned media from one tissue can beneficially influence the other. Animal models of bone and muscle research have further supported the bone-muscle biochemical connection. This knowledge, in light of the tight developmental and genetic coupling of these tissues, large bivariate GWAS studies that have identified potentially pleiotropic bone-muscle genes, and the concurrence of osteoporosis and sarcopenia in older adults justifies a closer examination of the biochemical crosstalk between bones and muscles. In-depth understanding of the bone-muscle connection could pave the way to new treatments for musculoskeletal diseases.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
- Bone
- Skeletal muscle
- Bone-muscle crosstalk
- Bone-muscle connection
- Mechanical coupling
- Bone-muscle secreted factors
- Endocrine
- Osteoporosis
- Sarcopenia
- GWAS
- Genetic
Mechanical Coupling of Bones and Muscles
The musculoskeletal system is extremely complex. Contrary to the reductionist view that it is made up of only bones and muscles, the system is actually composed of bones, skeletal muscles, nerves, blood vessels, tendons, ligaments, cartilage, joints, and other connective tissues.
Historically, the association between bones and muscles has been primarily seen as a mechanical coupling where one tissue, skeletal muscle, actively applies the load and another tissue, bone, receives the load and serves as the attachment site. This physiologic association supports the locomotion, protection, and the shape/form of animals. In recent years, we have begun to appreciate that the relationship between muscle and bone goes beyond this mechanical coupling; that these two tissues also function at a higher level through crosstalk signaling that is important for their function.
The tight coupling between skeletal muscle and bone in animals begins during embryonic development with the formation of the paraxial mesoderm, which subsequently gives rise to somites that become muscles, bones, tendons, and other tissues [1]. The development of each of these tissues will be discussed later in the chapter. It is important to mention at the outset that as the skeleton develops, it has been postulated that muscle contraction in the fetus contributes to skeletal growth and development and that skeletal adaptations in early postnatal life are driven by changing mechanical forces [2, 3]. Although exercise across all ages has proven beneficial, clearly peak bone mass accrual during pre-pubertal growth is dramatically affected by exercise, or physical activity, and to a lesser extent thereafter [4]. Peak bone mass is achieved by both men and women by their third decade of life, with men having obtained more bone mass due to hormonal and other influences (i.e. diet, genetics, etc.). Human females begin to lose bone mass with a rapid loss phase occurring 2–3 years before menopause and continuing until 3–4 years after the last menses [5], then experiencing a more gradual but steady decline. Males do not experience this same dramatic decline, but rather a gradual, steady bone loss beginning in their 50s and 60s [6] (Fig. 4.1). Individuals with reduced bone mass, as seen in osteoporosis, often also develop the reduced muscle mass and function, a condition known as sarcopenia. However, declines in bone mass do not fully explain sarcopenia, nor does muscle atrophy fully explain the totality of osteoporosis. This seeming mystery may be due in part to the use of bone mass and muscle mass as the predominant measures for osteoporosis and sarcopenia. The assessments of bone quality and muscle function might better reflect the physiological basis for these diseases. However, these metrics are not in place to date, especially in the clinical arena.
Aging-related changes in bone mineral mass of the radius and muscle width in the forearm in adult men and women (From Novotny et al. [7])
The mechanical coupling of skeletal muscle and bone is visible. Bone adjusts its mass and architecture to changes in mechanical load and as contraction of skeletal muscle is essential for locomotion, it is obvious that muscle contractions apply load to the bone. This mechanical perspective implies that as muscle function declines, the result would be decreased loading of the skeleton, leading to a reduced bone mass. However, as noted above, the inability to account for totality of the changes in the musculoskeletal system based upon mechanical considerations, while important, is only a part of this major complex problem. For example, it is not possible to explain the development of osteoporosis based solely upon the presence of sarcopenia (and vice-versa). These observations imply that beyond the mechanical coupling there must also be a biochemical coupling.
As we will discuss in this chapter, it is now fully evident that muscle and bone produce factors that circulate and act on distant tissues, thus fulfilling the classical definition of endocrine action. Surprisingly, it has only been recently that the action they have on one another has begun to be under careful investigation. Perhaps this oversight derives from the bias of mechanical coupling and, until recent years, a lack of technology, testing abilities, and bioinformatics techniques. However, understanding this apparent endocrine crosstalk and biochemical coupling is an exciting new avenue of research with tremendous clinical potential.
Beyond Mechanical Coupling: Bone-Muscle Developmental and Genetic Coupling
Considering their common embryonic development while forming from somites originating from the paraxial mesoderm, the intimate relationship and close coupling between the tissues that comprise the musculoskeletal system is therefore unquestionable [3]. Bone and muscle cells share a common mesenchymal precursor and their shared experience of organogenesis occurs through a firmly orchestrated network of genes and proteins during intrauterine development. In fact, some of our own bias to accept a purely mechanical coupling between these two tissues derives from embryology. For example, it is the contraction of muscles in the developing embryo that contributes to the process of skeletal development itself and clearly to the growth of the skeleton, as well as a host of adaptations in early postnatal life that result from the changing mechanical forces [2, 4]. Furthermore, even post-development, the immediate results of muscle load can be discerned on bones, since they adjust their shape and mass to changes in load, and such load can be easily interpreted as coming from muscle contractions. We are obviously not suggesting that contracting forces do not play a major role, but rather, there are a number of additional influences to consider.
While universally accepted that bone and muscle develop embryologically as a unit, the underlying environmental cues that drive skeletal mass and other properties are regulated by a complex set of genetic factors. Heritability studies have estimated that from 40 to 80 % of the major skeletal phenotypes and muscle traits are related to genetics [8–11]. Thus, given the genetic and developmental closeness of these two tissues, it seems highly likely that there would be some degree of shared genetic components underlying some of their phenotypes. The identification of these shared (i.e., pleiotropic) genetic cues are essential to promote the discovery of the molecular/biochemical coupling that exists between muscle and bone, and serve as evidence that bone and muscle interact beyond mechanical.
Genome Wide Association Studies (GWAS)
Over the past decade, GWAS have produced several candidate gene regions that show association with variations in a number of different human bone phenotypes and muscle traits. Even limiting the focus to a small sampling of the bone muscle phenotype GWAS [12–20] and bone phenotype GWAS [21–29] reported in recent years evidence of the powerful genetic coupling between these tissues. An interesting question that arises is how mechanical forces during development interact with genetic signals. For example, do fetuses that have stronger intrauterine contractions produce genetic signaling that in turn favors the development and formation of stronger bones and muscles and a healthier musculoskeletal system? Or, are there specific genetic signals that lead to bones and muscles of higher mass and strength? Or, is it a combination of both possibilities?
Due to the development of new bioinformatics and statistical models, bivariate GWAS has been used to identify pleiotropic candidate genes/single-nucleotide polymorphisms (SNPs); regions concomitantly associated with traits in both bone and muscle [13, 30–34]. These recent bivariate GWAS based studies, including both bone and muscle phenotypes, have revealed a short list of several novel potentially-pleiotropic candidate genes such as GLYAT [13], HTR1E, COL4A2, AKAP6, SLC2A11, RYR3 and MEF2C [31], PRKCH and SCNN1B [30]; HK2, UMOD and two microRNAs MIR873 and MIR876 [34].
The MEF2C gene encodes a potent transcription factor (myocyte enhancer factor 2C) that was originally thought to be involved in cardiac and skeletal muscle development and was also used as a marker of myogenic cells in the somites [35]. Intriguing data has recently emerged with the development of the osteocyte specific mouse model of Mef2C deletion. These mice display increased bone density through a complex mechanism involving reduced Sost expression and increased osteoprotegerin (OPG) expression resulting in a reduced receptor activator of nuclear factor kB ligand (RANKL)/OPG ratio, and reduced osteoclastogenesis [36]. Therefore, the important roles of MEF2C in cardiac and skeletal muscle development, as well as in adult bone mass regulation, support the concept of shared genetic determinants in bone and muscle and in this case even beyond, since cardiac muscle is also part of this MEF2C loop.
Another of the suggestive genes that emerged from the GWAS analyses was METTL21C, which is highly expressed in muscle. Interestingly, it has been reported that there may be an association between the METTL21family of proteins and inclusion body myositis with Paget’s disease of bone [37–39]. The role of Mettl21c in myogenesis was explored using the murine skeletal muscle cell line, C2C12. By silencing the activity of Mettl21c through the process of siRNA transfection, we demonstrated a significant decrease in C2C12 myogenesis as evidenced in the reduced fusion index, smaller myotube cell area, and decreased calcium release from the sarcoplasmic reticulum when compared to negative controls (Fig. 4.2).
Partial silencing of Mettl21c reduces fusion index, myotubecell area, and calcium release from the sarcoplasmic reticulum. (a) Representative fluorescence images of DAPI‐stained nuclei (blue) and MHC antibody (green) of C2C12 at 3 days of differentiation after transfection: (a) negative control; and (b) Mettl21c‐siRNA–treated C2C12 cells. (b) Summary data show that the Fusion Index in Mettl21c‐siRNA–treated C2C12 cells decreased significantly compared to negative control (p < 0.05). (c) Summary data show that myotubecell area in Mettl21c‐siRNA–treated C2C12 cells drastically decreased compared to negative control (p < 0.0001). (d) Representative calcium transients induced by 20 mM caffeine (arrow) on C2C12 myotubes loaded with Fura‐2/AM. In Mettl21c‐siRNA–treated C2C12 myotubes at day 5 of differentiation, compared to negative control, the amplitude peak calcium response to caffeine was significantly decreased and the relaxation phase of the transient was shorter (p < 0.01). DAPI.4,6‐diamidino‐2‐phenylindole; MHC.myosin heavy chain (From Huang et al. [38])
To study the impact of Mettl21c on bone cells, the osteocyte cell line MLO-Y4 was used. We found that a partial knockdown of Mettl21c in MLO-Y4 cells led to an increased dexamethasone-induced cell death. These findings further support the concept that bones and muscles share genetic determinants, and that it is through the modulation of specific factors that lead to the phenotypic and functional effects (Fig. 4.3).
Partial knockdown of Mettl21c in MLO‐Y4 osteocytes increased cell death induced by dexamethasone. (a) Representative image of MLO‐Y4 osteocytes 24 h after transfection of All Star negative control siRNA(200 nM): (a) phase contrast image; (b) fluorescent image of tagged siRNA; both images were taken from the same area; (c) merging of (a) and (b). (b) Summary data of cell death in MLO‐Y4 cells transfected with Mettl21C siRNA, with and without Dextreatment. Cell death was detected 48 h after treatment by trypanblue exclusion assay (Dexincreased cell death under all conditions; and Mettl21c knockdown induced cell death levels higher than Dexalone, p < 0.05). (c) The nuclear fragmentation assay shows: (a) absence of nuclear blebbingin control MLO‐Y4 cells as compared with (b) enhanced blebbingin the siRNA‐treated MLO‐Y4 osteocytes; (c) the enlarged image clearly shows the blebbingprocess in siRNA‐treated MLO‐Y4 osteocytes. Dex.dexamethasone (From Huang et al. [38])
Myostatin (MSTN), or growth and differentiation factor 8 (GDF8), is a member of the TGF-β superfamily and is a muscle-derived factor (myokine) that circulates in the blood, making it an attractive candidate for muscle-bone endocrine signaling [40, 41]. The deletion and/or mutations in myostatin lead to muscle hypertrophy or “double muscling” in animal models [42–47] and in humans [48]. This is a prime example of how a mutation assumed to be restricted to one tissue can lead to altered properties in another (Fig. 4.4). In this case, the loss of myostatin not only leads to muscle doubling, but also leads to a generalized increase in bone density and strength [49]. A question that could lead to major mechanistic insights is how does myostatin exert its effects on bone? Possible explanations include direct effects of mechanical loading of bone due to the increased muscle mass, indirect action by regulating hepatic production of IGF-1 [50], or some other unknown mechanism. While the IGF-1 and GH axis is an important mechanism to be pursued due to its effects on age-related changes in bone and skeletal muscle [51], a tantalizing possibility is that larger volume muscles might release relatively larger amounts of myokines, which in turn reach the bone cells via the canalicular system, exerting anabolic effects on bone. The possibility of this endocrine-like crosstalk, along with the promise of novel and impactful therapeutic interventions, has motivated research to be conducted in this area.
Radiographs demonstrating increased shaft diameter and increased muscle attachment site at the deltoid crest in humerus (a), and the third trochanter in femur (b) in Myostatin-/-mice compared to wild type. Notice the extension of the articular surface towards the neck of the femur (b) (From Elkasrawy and Hamrick [49])
Disease Conditions with Multiple Tissue Effects
The endocrine interactions that are being discovered through the effects of bone cell secreted factors and myokines go well beyond the musculoskeletal unit. Recent findings have supported the interconnection of bone, muscle, and adipose tissue. The striking rise of chronic diseases such as diabetes, metabolic syndrome, and obesity seem to closely parallel the rise in the prevalence of sarcopenia and osteoporosis, particularly in the elderly population [52]. The musculoskeletal system is the largest organ system of the body. If we embrace the concept that bone, tendon, and muscle all produce and secrete a myriad of factors, and that they influence not only each other but also multiple organs and overall body metabolism, it makes sense that when the musculoskeletal tissues become less effective with aging, organs throughout the body would also be effected. With fewer bone-derived factors (osteokines) and fewer myokines being secreted, it is logical to expect changes in fat metabolism, as well as kidney function, and even testosterone levels; thereby translating into multiple organ effects that are normally interpreted as “aging consequences”. This new view not only helps to explain some of the multiple organ decline in function, but could also lead to new therapies related to the endocrine function of bone and muscle.
The Unique Case of Fracture Healing
An intriguing and well documented observation that cannot be ignored in the context of bone-muscle interactions is the observation that in open fractures, where muscle injury is also extensive or where muscle atrophy develops, fracture healing is significantly impaired [53–56]. Rodent models of fracture have supported the concept that muscle secretory activity aids in the process of fracture healing. For example, a significant difference (i.e., lesser healing) was found in rats with fractured femurs when their quadriceps muscles had also been paralyzed by botulin injections [57]. In mice with tibial open fracture, Harry et al., reported that when the fracture area had been covered with muscle flaps, bone repair was significantly improved [58]. The clinical significance of these findings cannot be overstated since these findings have also been reproduced in humans with open tibial fractures [59] (Fig. 4.5 [58]; Table 4.1 [59]).
Load at which failure occurred (N), through callus in the fracture groups, and un-fractured cortex in the non-trauma control group, at 28 days post fracture. Bars show standard deviations (SD) (From Hayutin et al. [128])
Taken together, these studies strongly suggest that even under conditions where substantial mechanical forces are not being produced, muscles have the intrinsic biochemical capacity to secrete factors that stimulate growth and repair. It is almost as if muscles could function as a second periosteal layer as recently proposed by Little and colleagues [76, 77]. Yet another line of evidence derives from the documented observation in humans that fracture healing is improved upon the stimulation of the affected bone with pulsed electromagnetic stimulation (PEMS) [78]. Our groups have recently demonstrated that PEMS enhances myogenesis of C2C12 myoblasts [79]. Therefore, it is possible that the improved healing observed with PEMS on bone might be attributable to direct effects on bone cells and to indirect effects of myokines. The idea of circulating factors playing a role in these processes gains further strength in light of the studies conducted by Hamrick and colleagues showing that exogenous myostatin treatment accelerates bone and muscle healing [80].
Bones and Muscles as Endocrine Organs
Anatomic proximity of the musculoskeletal system along with the physiologic roles in mechanical support and body movement has, as mentioned, defined the connection between bones and muscles historically. In fact, so physiologically reasonable is the mechanical relationship between bones and muscles that the consideration of other possible links between the tissues has in some ways been encumbered. In the 1960s, an interdisciplinary group hosted by the University of Utah began to convene annually and compiled an impressive body of evidence in support of the biomechanical relationship between bones and muscles. As a result, a new paradigm emerged that included the mechanostat model, which purported that bone strength and density was largely a function of imposed mechanical forces [81]. That model, together with the Utah paradigm continued to influence for decades research conducted on bone and muscle physiology.
However, a key aspect to the model remained nearly dormant until recent years. Even the staunchest supporters of the model admitted to the likelihood of non-mechanical agents locally and systemically affecting the skeletal architecture [81]. Nevertheless, the vast majority of investigative efforts related to the bone-muscle unit focused on the impact of mechanical loads. Basic research has experienced in recent years an explosion of technical advancements. These new techniques, equipment, cell lines and transgenic animal models provide now increased opportunities to learn more about both the mechanical and the biochemical relationship between bones and muscles. Additional experimental approaches include the study of specially created cell lines and the development of transgenic animal models. To expand the body of knowledge related to factors secreted by bones and muscles, researchers look for evidence of the impact such factors have throughout the body.
Perchance the easiest way to see the endocrine nature of skeletal muscles is to look to one of its major functions; which is to sequester glucose from the blood stream. Skeletal muscles are essential for the maintenance of body glucose homeostasis as demonstrated by the fact that by having a larger volume of muscles and/or being more active physically a person can help prevent diabetes type II [82–84]. While literally working as an organismal sink for glucose, skeletal muscles can simultaneously undergo catabolic reactions that lead to the release of amino acids, which travel via the blood stream to find in the liver the proper conditions for gluconeogenesis. Under certain conditions, lipids can serve as another source of energy for skeletal muscles. Lipids are also emerging as important signaling molecules; a significant point that will be discussed later in this chapter.
Bone as an Endocrine Organ
A century ago, the predominant understanding of bone physiology was that there were primarily two types of bone cells: osteoblasts and osteoclasts. At the time, it was widely accepted that skeletal homeostasis relied on the function of these two bone cells; bone formation for osteoblasts, and bone resorption for osteoclasts. The primary influences on these two bone effector cells were believed to come from hormones and dietary calcium. Although osteocytes were identified and even recognized to be the most abundant type of bone cell, they were believed to be inert, serving primarily as structural components of the bone matrix. Since then, the dynamic and crucial role of osteocytes has become known. It was in the early 1990s that support for the endocrine function of this important bone cell began to gain momentum. Osteocytes are connected to one another via gap junctions, and it was a focus on this area that provided researchers with insight into the biochemical nature of bone cells. In 1992, Marotti and his team of researchers at the University of Modena, Italy, published their findings and working hypothesis on the metabolic activity of osteocytes. Using transmission electron microscopy (TEM), they demonstrated changes in the skeletal microstructure that occur with aging, as well as evidence of osteocyte modulation of osteoblast activity [85]. Three decades earlier, Dr. Marshall Urist had demonstrated the osteogenic properties of bone by implanting a decalcified and lyophilized sample of bone into host tissue [86]. His experiments revealed that factors present in the sample of bone cells led to neovascularization and bone deposition into the host tissue. It was with the advent of technical advancements that the factors could begin to be identified and studied. Urist recommended the name Bone Morphogenic Protein (BMP) for the factor responsible for new bone formation in his trailblazing experiments. Since then, BMP has come to refer to a group of growth factors implicated in the morphogenesis of tissues throughout the body.
Klein-Nulend and her team observed that bone cells secreted prostaglandins in response to mechanical stress induced in pulsating fluid flow experiments [87]. Research findings continue to support the significant role of prostaglandins in bone homeostasis, particularly the E and F series of prostaglandins [60, 88–91].
Research performed in the early part of this century provided evidence that in addition to their function as a sensory and responsive cell, osteocytes also serve to help regulate bone density through the secretion of sclerostin, a protein that inhibits bone formation [92]. Their work tested the hypothesis that the dysregulation in bone formation resulted from phenotypes observed in osteosclerosis patients. This hypothesis was further supported through genetic testing and the development of transgenic mice with increased sclerostin production and low bone mass. Since these explorations into the biochemical nature of bone cells, continued research by a number of biomedical scientists including Bonewald, Johnson, Dallas, Karsenty, and Yamashita continue to provide evidence in support of osteoblast/osteocyte-secreted factors that impact not only bone homeostasis but also distant tissues such as the brain, heart, kidney, prostate, and muscle.
Fibroblast growth factor 23, or FGF23, is a bone-derived protein that has been identified as integral to vitamin D metabolism and the regulation of systemic phosphate levels [93]. In their 2012 review, Bonewald and Wacker discussed FGF23 expression in osteocytes and its role in cardiovascular health [94]. This has found additional support from research performed on transgenic mice phenotypes. Although the exact pathways are not fully understood, it appears that osteocyte expression of FGF23 is under the influence of molecules such as DMP1, PHEX, and MEPE [95]. Osteocalcin, which is also known as bone gamma-carboxyglutamic acid-containing protein (BGLAP) is a protein found, as the name implies, in bone and dentin. Osteocalcin helps to provide structure and has been shown to also play a part in energy metabolism, calcium ion homeostasis, and male fertility [96]. It was postulated more than 20 years ago, that bone cells are the primary source of osteocalcin [97], and recent advances in genetic engineering have helped support that idea [75, 96, 98, 99]. Osteocalcin, along with other hormone-like substances secreted by bone cells, are now thought to interact with substances from the liver and adipose tissue in a way that may predispose individuals to obesity, diabetes, non-alcoholic fatty liver disease, and osteoporosis.
The impressive list of bone derived factors continues to grow, and includes: ATP, calcium, DKK1, DMP1, FGF23, MEPE, Nitric Oxide, OPG, osteocalcin, prostaglandins (particularly PGE2), RANKl, sclerostin, and SOST. These factors represent a myriad of biochemical structures ranging from simple organic molecules to complex proteins, all of which help illustrate the diversity and far-reaching impact of bone as an endocrine organ.
Muscle as an Endocrine Organ
Skeletal muscle represents the majority of muscle tissue in the body and is so named for its functional connection and vicinity to the skeletal system. Also called striated muscle because of its appearance, skeletal muscle is under the control of the somatic nervous system and is responsible for voluntary movement, facial expressions, postural support, and respiratory expansion. Skeletal muscle develops from myogenic precursor cells and myoblasts. Myoblasts are small, mononucleated cells capable of either entering the cell cycle and proliferating, or fusing with other myoblasts to form myotubes. As myoblasts fuse and begin to form myotubes, they enlarge and take on an elongated shape (Fig. 4.6). Muscle cell proliferation and differentiation occur in the embryonic and early stages of development, and continue throughout the lifespan. Skeletal muscle is a dynamic tissue, whose cells undergo myogenesis repeatedly as muscles regenerate in response to injury [100, 101].
The process that leads to muscle contraction begins when acetylcholine (ACh) is released by a motor neuron across the synapse at the neuromuscular junction. Motor neurons originate in the central nervous system and the cell bodies of these neurons are located in the spinal cord. The neuronal fiber (axon) projects outside the spinal cord to directly or indirectly control muscles. At the muscle level, nerve-ending terminals spread and innervate each muscle fiber within a given skeletal muscle. A membrane called the sarcolemma covers each muscle fiber, and within each muscle fiber are thousands of sarcomeres, which are the functional units of contraction. The sarcomere is composed of thick myofilaments called myosin, and thin myofilaments called actin. The neuromuscular junction is a synapse with the terminal end of the motor neuron on one side and the motor end plate of a skeletal muscle fiber on the other. Release of ACh from the motor neuron causes stimulation of a muscle fiber through the exchange of sodium and potassium ions. This leads to the generation of an action potential that spreads along the sarcolemma and is transmitted into the interior of the muscle fiber by structures called transverse tubules, or T-tubules. T-tubules are juxtaposed to the calcium ion storage units, the sarcoplasmic reticulum (SR). As the action potential travels along the T-tubule, it causes the voltage-sensitive receptor named Dihydropirydine Receptor (DHPR) to change shape, and it is this allosteric modification of the DHPR that allows it to physically interact with the largest known mammalian channels, the Ryanodine Receptors (RyR) precisely located on the surface of the membrane of the SR. This DHPR-RyR contact, leads to the opening of the RyR, which brings about the release of calcium from the SR into the cytosol of the skeletal muscle cell. This rise in cytosolic calcium causes the binding sites on the actin filament to be exposed, allowing myofilaments heads to bind. The myosin filaments pull the actin filaments in, resulting in a shortening of the sarcomere. It is the shortening of sarcomere throughout the muscle fibers that causes muscle contraction. The process by which the electrical stimulation, or excitation is transferred into a mechanical contraction is called the excitation-contraction coupling (ECC) and is fundamental to skeletal muscle physiology [102–104]. The ECC is the cellular and molecular reason that we can execute from very fine controlled movements to the lifting of several hundred kilograms of weight.
The functional role of skeletal muscle to move and support the body has long been realized; it has only been recently that endocrine-like function of skeletal muscle has begun to be appreciated. Research associated with skeletal muscle secreted factors began primarily in relation to those produced in response to injury. For example, several myokines, prostaglandin, IL-6, and LIF, have been shown to enhance the myocyte differentiation after injury [105–108]. Muscle regeneration is an ongoing phenomenon throughout the life span, and provides an excellent opportunity for investigation into the endocrine function of this organ, as well as hope for targeted interventions to slow the process of muscle wasting. Two additional factors secreted by injured skeletal muscle are TGFα and TGFβ1 [106, 109]. These myokines have an inhibitory effect on muscle cell proliferation and differentiation.
In addition to raising serum levels of IL-6, exercise has been found to induce a six-fold increase in mRNA of Chemokine CXC motif ligand-1 (CXCL-1) and a 2.4-fold increase in serum CXCL-1. A functional homolog for IL-8, murine CXCL-1, belongs to a group that has gained attention for its role in inflammation, chemotaxis, angiogenesis, neuroprotective activity, and tumor growth regulation and is associated with a decrease in visceral fat [110].
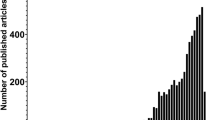
Obesity and type 2 diabetes have both reached epidemic proportions worldwide. As the body of knowledge related to myokines continues to expand, researchers are investigating the role of certain myokines, or more accurately the lack thereof, because of limited exercise and the possible connection to these chronic diseases [110]. Recently, a new myokine brought hope for the development of molecules to target fat tissue accumulation, since irisin was shown to regulate the conversion of ‘bad’ (white) fat into ‘good’ (brown) fat that is essential for thermogenesis in mice [111]. Since the original publication, 49 papers have been published on the effects of irisin. A recent study by Park [112] concluded that irisin might be directly associated with a higher risk of cardiovascular diseases and metabolic syndrome in humans, suggesting that augmented secretion of irisin by either adipocytes or muscle cells might occur to overcome an underlying irisin resistance, similar to the hyperinsulinemia seen in insulin resistance associated with obesity [112].
The list of myokines continues to grow, and includes IL-8, which has been shown to increase angiogenesis [113]; IL-5, which is an anabolic factor being investigated for its role in muscle-fat crosstalk; IL-7, which is being studied for its impact on satellite cells during myogenesis [114]; and brain-derived neurotrophic factor (BDNF) [115]. With a deeper understanding of skeletal muscle as an endocrine organ comes the promise of innovative approaches to the prevention and treatment of diseases and disorders throughout the body.
Interplay Between Bones and Muscles as Endocrine Organs
The conditions are determined in utero for the connection between bones and muscles, as they share a common mesenchymal precursor and experience organogenesis through a tightly orchestrated network of genes during intrauterine development. As mentioned, their anatomic proximity lends credence to the hypothesis that bones and muscles influence each other in a paracrine nature. Evidence of such a relationship exists as pathologic conditions are studied; specifically, some of the bone stress syndromes where inflammation localized to the muscle area underneath the periosteal region spreads into the bone itself. These situations support the paracrine relationship hypothesis, suggesting inflammatory molecules from adjacent muscle fibers may penetrate into this region of the bone. Another powerful clinical example of this paracrine relationship is the aforementioned muscle flap application to compounded bone fractures. The effect of this therapeutic approach is significantly faster healing for these fractured bones. Although the specific molecular mechanism of action is not completely understood, the introduction of muscle flaps has been used as a successful therapeutic approach to treat chronic osteomyelitis and to accelerate the healing of bone fractures [116]. These mechanisms might display further importance for bone and muscle healing after musculoskeletal injury.
Experiments performed using osteocyte and muscle cell lines have revealed that PGE2 secretion from osteocytes is more than 1000 times greater than PGE2 secretion from muscle cells. This excess amount of PGE2 from osteocytes could interplay with injured muscles, which would aid in muscle regeneration and repair. Intriguingly, recent in vitro studies have provided support for a role of osteocyte secreted PGE2 in aiding with the process of myogenesis [89]. While these studies were originally performed with the myogenic cell line C2C12, as shown in Fig. 4.7, PGE2 signaling is also a potent stimulator of myogenic differentiation in primary myoblasts/myotubes.
PGE2 signaling modulates myogenesis of primary myoblast/myotubes. Representative images following treatment with PGE2, EP4 agonist CAY10598, and EP4 inhibitor L161,982 in 5-month old mouse primary myotubes, showing the same pattern previously published in C2C12 cells in Mo et al. [89]. Ingreen, myosin heavy chain, MHC and inblue: DAPI. Unpublished results by the Brotto Lab (Mo and Brotto Unpublished Results, 2015). It is evident that PGE2 and CAY 10598 promote myogenesis while L161,982 inhibitsit. PGE2 is a major osteokine secreted by osteocytes and one of the mediators of the bone-muscle crosstalk [89] (From Mo and Brotto Unpublished Results, 2015)
Recently developed transgenic animal models provide an excellent opportunity for researchers to gain further insight into this bone-muscle crosstalk, as in the case of the myostatin-deficient mouse. Myostatin, which was discussed earlier with regard to its pleiotropic characteristics, was discovered in the late 1990s to be a potent inhibitor of muscle growth. It is expressed during development and in adult skeletal muscle, serving as an important negative regulator of skeletal muscle growth [45, 117]. Myostatin appears to decrease myoblast proliferation. The myostatin-deficient mouse model has increased muscle size and strength, with individual muscles weighing significantly more than wild type mice [118]. Hamrick used this myostatin-deficient mouse model to investigate the effects of increased muscle mass on bone mineral content and density. He and his team found that although a consistent correlation was not found in all regions of the skeletal system, there was increased cortical bone mineral density in the distal femur and an increased periosteal circumference along the humerus [49, 119–121]. Another group used the same myostatin-deficient mouse model to look at the impact of the chronic loss of myostatin on multiple organ systems and found that it appeared to preserve bone density [122]. From a contrasting perspective, Zimmers investigated the effects of myostatin overexpression in an animal model and observed a profound loss of muscle and fat, mimicking the presentation seen in chronically ill patients and commonly referred to clinically as cachexia [118]. Further research into the disruption of myostatin is a worthy direction in an effort to preserve muscle mass in patients with chronic diseases.
As mentioned in a previous section, osteocalcin serves as a splendid example of bone as an endocrine organ [123]. This osteoblast-derived factor, circulating levels of which increase with exercise, binds to the GPRC6A receptor, affecting distant adipocytes and pancreatic β cells. Interestingly, osteoblasts also naturally express the osteo-testicular phosphatase gene (Esp), which inhibits the function of osteocalcin [69]. With this information in mind, it is of specific interest to the discussion of bone-muscle crosstalk that the Gprc6a knockout mouse displays the phenotype of decreased muscle mass, while the Esp knockout mouse has increased muscle mass. Through these observations, it can be proposed that osteocalcin, a known bone cell factor, may play a role in the regulation of muscle mass. This is the type of knowledge that promises a deeper understanding of sarcopenia; as osteocalcin could be a target for the development of therapies to prevent, delay, or slow the progression of this highly prevalent disorder associated with aging. If this knowledge is useful for sarcopenia, it is possible that it may also be useful for its associated disorder, osteoporosis.
The endocrine communication that continues to be revealed through effects of factors derived from these tissues is not limited merely to a bone-muscle connection. There is a growing awareness that the factors secreted from tissues throughout the body impact the overall health of the individual. The significance of this dynamic interrelationship is becoming more apparent with the aging of the world’s population and the concomitant rise of chronic diseases such as obesity, diabetes, and metabolic syndrome. According to the Centers for Disease Control and Prevention, the prevalence of obesity in the United States among adults 65 years of age and older is nearly 35 %; translating into more than 8 million older adults [52]. The American Diabetes Association website reports that nearly 25 % of adults aged 60 and over have diabetes, and it is also becoming clear that the prevalence of metabolic syndrome increases with age [62]. Recognizing the overwhelming implications for public health posed by sarcopenia alone, a distinguished team of researchers called for increased research investigating the factors involved in the pathogenesis of sarcopenia more than a decade ago [124]. Data from many studies published around that same time began to suggest that sarcopenia influenced the development of other chronic conditions such as cardiovascular and metabolic diseases. Since then, more evidence has been uncovered that sarcopenia is often linked to dyslipidemia, insulin resistance, and hypertension as well as a decline in immunologic function [71, 125].
As the understanding of the role of bones and muscles as endocrine organs, and insights into bone-muscle crosstalk begin to be translated into meaningful and innovative therapeutic approaches, unprecedented advances will be achieved in the fight against chronic diseases such as obesity, diabetes, osteoporosis, and sarcopenia.
Musculoskeletal Diseases: The Special Cases of Osteoporosis and Sarcopenia
People are living longer than any time in history due to the many advances in healthcare. In 1900, the life expectancy was only 47 years. By 1930, it increased to 60 years, and by the early 2000s, the life expectancy from birth had risen to more than 75 years. As the life expectancy climbs, there is a parallel increase in the percentage of the population aged 65 and older. Again, looking just back in time to 1900, only 4 % of the population was 65 and older, but that percentage nearly tripled to 13 % by 2008, and is projected to increase to an unprecedented 22 % by 2030 [126]. This has been reported as the largest demographic shift in history by experts in fields from finance to sociology [127, 128]. Many factors have contributed to this increased life expectancy, including the development of vaccines and antibiotics, improved nutrition, and processes to better the accessibility of clean water to more of the world’s population.
Unfortunately, this trend of increasing age is accompanied by a corresponding increase in disability as aging adults experience a decline in physical functioning. The decline in functional reserve has been well documented throughout scientific and popular literature [129]. Nearly 300 diseases and injuries appear on the Global Burden of Disease (GBD) list, and a staggering 289 of those are known to cause disability. In the 2010 Global Burden of Disease (GBD) Study, researchers reported that the years lived with disability (YLD) per 100,000 people remained relatively constant over the years, until recently. With the increasing population of those who are 65 years of age and older, the YLD numbers have dramatically increased [130]. The seemingly undeniable fact of mortality is that aging is associated with the decline in function of nearly every system in the body along with the development of chronic conditions. Chronic diseases and disorders have a tremendous impact on individual health and healthcare expenditures, which has motivated much research into the prevalence of chronic conditions. Reports align and reveal that as many as 82 % of the older population in the U.S. has one or more chronic health conditions [131–133].
One of the body systems that experiences significant changes with aging is the musculoskeletal system. According to the 2010 Global Burden of Disease Study (GBD), musculoskeletal diseases are the second greatest cause of disability, affecting billions of people worldwide [130]. Disability leads to injury and a decline in function and independence. Rubenstein and Josephson reported that one in three community-dwelling older adults falls each year [134]. Fall-related injuries were responsible for more than two million Emergency Department visits and nearly 600,000 hospitalizations among older adults in 2009 [135, 136]. One of the most frightening injuries for an older adult to experience is a hip fracture. Ninety percent of hip fractures are the result of a fall, and the mortality rate 1-year post hip fracture is an astounding 25 %. It would seem the fear surrounding this injury is justified as only one in two older adults that experience a hip fracture return to their baseline level of activity [136]. There are many risk factors for falls, but primary among them is muscle weakness. The associated morbidity and mortality, especially hip fractures, is greatly increased among older adults, and is a significant health risk for those with osteoporosis. In addition to other chronic diseases and medication use, the decline in musculoskeletal health and function is a growing problem [74, 137, 138]. Loss of muscle mass and strength not only increases the individual’s risk of falls, it impacts quality of life. Depp and Jeste reported that in the majority of cases, the very definition of “successful aging” is predicated by the absence of disability [73].
The musculoskeletal changes that occur not only impact the aging individual, they create a profound economic burden. Looking at sarcopenia alone, the healthcare costs in the year 2000 were $18.5 billion, which represented 1.5 % of the nation’s total direct healthcare costs that year [139]. That percentage would translate into more than $40 billion a decade and a half later. Drawing from the 1995 Report of the National Osteoporosis Foundation [140], and adjusting for inflation and other factors to make the dollar values consistent, the same authors reported costs associated with osteoporotic fractures in the year 2000 to be $16.3 billion. Included in this price tag is the cost of inpatient care, nursing home care, outpatient care, emergency room visits, radiology services, orthopedic medical supplies, and outpatient medications. Even with all these aspects factored in, these costs may be conservative, considering that the United States Center for Disease Control and Prevention website, updated in September of 2013, reports the direct medical costs associated with fall-related injuries among the older adult population was $30 billion in 2010, and is projected to climb to nearly $55 billion by the year 2020 [141].
Osteoporosis
Osteoporosis is the most common metabolic bone disorder and is characterized by the progressive loss of bone mass. Bones are in a constant state of destruction and rebuilding, and in young, healthy individuals, the balance between bone formation and resorption is maintained. The decrease in bone density that has come to be known as osteoporosis appears to be the result of a growing imbalance of these two processes. The body of knowledge surrounding osteoporosis is growing as it is now recognized as the most common metabolic bone disease in the United States.
Evidence exists that the phenomenon of age related bone loss has afflicted mankind for centuries [142]. An English surgeon, Sir Astley Cooper was one of the first to document the changes he observed in bones of older adults: “With respect to the neck at the thigh-bone, a very principal cause of non-consolidation by bone is the advanced age at which it becomes obnoxious to fracture through that peculiar change which the part undergoes at this period of life without any apparent cause, but which renders it incapable of sustaining the superincumbent weight, and even in continuity insufficient to maintain its function; therefore it may be fairly supposed, when broken incompetent to set up a restorative action” [70]. The term, osteoporosis, is attributed to the French pathologist, Jean Lobstein, who used the term in a paper describing autopsy findings of holes in bones associated with fragility. In retrospect, it seems likely that he was actually using the term to describe osteogenesis imperfecta rather than osteoporosis [143].
Many definitions of osteoporosis have been offered over the years, with the most widely accepted being an operational definition based upon bone mineral density (BMD). And, the most widely validated measure of BMD is dual energy X-ray absorptiometry (DXA). According to the World Health Organization (WHO) criteria, osteoporosis is defined as a bone mineral density (BMD) that falls greater than or equal to 2.5 standard deviations (SD) below the average value for young healthy women [144]. In recent years, there has been a growing debate about the use of DXA scan results. This diagnostic measure has proven to have high specificity, but low sensitivity; which means that a patient with a T-score below −2.5 has a high risk of fracture, but the patient with a T-score greater than −1.0, or within normal limits, is not immune to fracture. Clinicians and researchers have learned that many factors must be considered in determining the risk of an osteoporotic fracture in the aging patient.
Women are at greater risk of osteoporosis than men. Additional risk factors for osteoporosis include increased age, Caucasian or Asian ethnicity, postmenopausal status, late menarche or early menopause, low peak bone mass, a family history of osteoporosis or low trauma fracture, low dietary calcium, vitamin D and vitamin K, low levels of physical activity, smoking, excessive alcohol intake, and the use of certain medications such as steroids, anticonvulsants, immunosuppressants and heparin [72, 145–148]. Health care providers must consider all of these as they contemplate preventive and treatment options for their aging patients.
Treatment plans for those diagnosed with osteoporosis are related to these identified risk factors. The initial approach includes lifestyle modifications such as increased physical activity if possible, smoking cessation, and decreasing alcohol intake [149]. Beyond these lifestyle changes to reduce the risk of injury, treatment goals are aimed at slowing or stopping bone loss and/or facilitating bone formation. Supplementations often recommended include calcium, vitamin D, and, in some cases, hormone replacement therapy [150]. The primary pharmacologic intervention are antiresorptives. These pharmacological approaches are reviewed in depth in Chap. 12 of this textbook.
Sarcopenia
Skeletal muscle accounts for 38 and 31 % of the total body weight in men and women, respectively, and represents the largest single organ in the human body [151]. Thus, it is reasonable that the age-related anatomical and physiologic changes in skeletal muscle have a significant impact on the overall health of the individual. Irwin Rosenberg first proposed the term ‘sarcopenia,’ in 1988 to describe age related muscle wasting [152]. The term derives from the two Greek words, sarx (flesh) and penia, (loss). Because all individuals experience muscle wasting with age, the prevalence of sarcopenia with age is essentially 100 %. However, Rosenberg and others recognized that in many, the muscle loss that accompanied aging happened at a seemingly accelerated rate and contributed significantly to disability. In 1988, a group of researchers and clinicians convened for a meeting in Albuquerque, New Mexico to discuss various measurements used to assess the health and nutritional status of the elderly population. It was in a summary report following that historic meeting that Rosenberg first coined the term, ‘sarcopenia.’ He stated at that time his motivation for coining the term was to draw attention to this all too common disabling physiologic phenomenon. With a name came an increase in research conducted into the process and effects of age-related skeletal muscle wasting. And, in a reciprocal fashion, as the body of knowledge related to sarcopenia grows and develops, so grows the acceptance of sarcopenia as a condition with specific and measureable signs and symptoms. It is now recognized that sarcopenia has significant implications for the lives of individuals, for the nation and for the world.
In the mid-1990s, the simple measurement used to identify sarcopenia among older adults was the upper-arm circumference. Even with this crude method of identification, researchers began to see a correlation between the presence of sarcopenia and the older adults’ mortality risk [153, 154]. In 1998, Baumgartner and his team suggested a modified approach to determining whether the muscle mass in an older adult was within normal limits, or whether it reflected a state of compromised health, i.e. sarcopenia. From the research he and his colleagues were conducting on older adults in New Mexico, Baumgartner defined sarcopenia as a height adjusted to muscle mass of two standard deviations (SD) or more below the mean of a young reference population. With this as his measurement, he demonstrated the increasing prevalence of sarcopenia with aging. The prevalence of sarcopenia in the New Mexico Elder Health Survey was 14 % in those 65–69 years of age, compared with greater than 50 % in those 80 years of age and older [61]. Other researchers in the field of gerontology adopted this measurement standard in their investigations of age-related loss of muscle mass. The consistent use of measurements allows for more meaningful comparisons of research findings between studies.
Nearly all of the studies conducted prior to 2005 were cross-sectional, and focused on a correlation between sarcopenia and decreased muscle mass and the associated functional impairment leading to physical disability [124, 155–158]. At least one study in the early 2000s looked at the impact of muscle size and strength over time and reported a less than 5 % change in strength attributable to a corresponding change in muscle size [159]. In an 8-year follow up to the Cardiovascular Health Study, Janssen et al. [139] reported a 27 % increased risk of developing disability with sarcopenia when compared with individuals with normal muscle mass. Interestingly, at the beginning of that same study, the reported likelihood of having disability was 79 % greater in those with severe sarcopenia than in those with normal muscle mass. The longitudinal analysis was three times smaller than the cross-sectional analysis, reported at the baseline. This underscores the importance of not drawing conclusions too early in an investigation of data, and suggests that the sarcopenia-associated risk of functional impairment and physical disability reported in cross-sectional studies of older adults in the early 2000s may have been overestimated.
Questions surrounding a universally accepted definition of sarcopenia continue as clinicians and researchers search for specific age-related musculoskeletal changes that correlate most strongly with the risk of disability. Evidence is growing that the rate at which muscles become weaker is much faster than the rate at which they become smaller [160]. Research findings are supporting that it is the loss of muscle strength, even more than the loss of muscle mass, that carries the greatest risk of disability in the aging adult [102, 160, 161].
Some researchers refer to the ‘bone-muscle unit’ in deference to observations that bones respond to varying levels of mechanical strain imposed by muscle mass and strength. The varying levels of mechanical strain appear to be modulated primarily by hormonal effects systemically, citing gender differences over time as evidence [62]. There is undeniably much evidence in support of the strong correlation between bone and muscle strength [163, 164].
A deeper understanding of the physiological relevance of these bone and muscle endocrine properties may serve to bridge the gap between the mechanical and biochemical theories of bone-muscle interaction. A feasible way of interpreting the role of these interactions is that they may serve to sense and transduce biomechanical signals such as unloading, loading, inactivity, or exercise, and even perhaps the translation of systemic hormonal stimulation into effective biochemical signals. Another way of interpreting and bridging these two theories is that one specific form of interaction could work as a priming for the other, in that, the physical effects of contraction on bone cells may prime these cells for the simultaneous, consecutive or ulterior effects of a secreted molecule. The growing evidence of a mismatch between changes in muscle mass and muscle strength that accompany muscle unloading also lends support to the biochemical communication between tissues [66]. The suggestion that in addition to mechanical force, other factors contribute to increasing muscle strength came more than three decades ago. In their work with isometric training, McDonagh and colleagues made experimental observations that led them to postulate “that the increase in the force of maximal voluntary isometric contraction must be related to factors other than the force-generating capacity of the muscle fibres themselves” [165].
In his work with the New Mexico Elder Survey, Baumgartner observed that, as many as 15 % of individuals with sarcopenia are also obese. The sarcopenic-obese older adult captured his attention because in his cross-sectional study examining older adults in the New Mexico Aging Process Study, he found this subsector of the elderly population to be at especially high risk of physical disability [166]. The decline in both lean muscle mass and bone density poses an even greater risk to independence and safety of the older adult. The appreciation of this risk has inspired research into this phenomenon. Findings of such research suggest an increase in catabolic cytokines such as interleukin-6 (IL-6), as well as inflammatory markers such as C-reactive protein and sedimentation rate [157, 167]. Interestingly, many of these same factors observed in the development of obesity are secreted by adipocytes [168, 169].
In 2004, Baumgartner and his team set out to replicate as a longitudinal study, the findings of their 2000 cross-sectional study, based upon the same cohort of individuals in New Mexico [170]. Looking at the problem over time, they found that neither sarcopenia alone nor obesity alone increased the older adult’s risk of functional impairment when compared with those with a normal body composition. Sarcopenic-obese individuals, however, had a 2.5 times greater risk of functional impairment [170]. A partial explanation for this could be related to the decreased resting metabolic rate that corresponds to the reduced skeletal muscle mass of sarcopenia [171].
Since the mid-2000s, several researchers have investigated the combination of sarcopenia and obesity, specifically concerned with the risk for physical disability. The findings of some researchers support an increased risk of physical disability in sarcopenic-obese older adults [172, 173], while the findings of other researchers do not support this notion [65, 174]. Of interest is the recognition that between research groups, and even within some research groups, conflicting results are obtained with regard to the question of sarcopenic-obesity and the increased risk for physical disability. It is possible that these conflicting results are the consequence, in part, of having no single definition of sarcopenia that is widely accepted within the research and clinical arenas. This experience should provide ample motivation to come to a consensus on the matter.
Attempts to understand the cause of an age related loss of muscle mass and strength have predominantly focused on the loss of skeletal muscle fibers, especially type II fibers. In recent years researchers have begun to delve into a wide variety of mechanisms involved in the pathophysiological mechanisms of sarcopenia including nutritional factors, activity levels, alterations in protein metabolism, and the impact of changing levels of hormones. Walrand and colleagues published a review that shed light on what many had begun to observe; suggesting that sarcopenia impacts the development of other chronic conditions such as cardiovascular and metabolic diseases [175]. Sarcopenia is beginning to be linked to dyslipidemia, insulin resistance and hypertension as well as a decline in immunologic function [71, 125].
Gaining momentum is yet another element to this issue; that age-related decreases in muscle strength result from a combination of loss of muscle mass (atrophy) and reduced muscle specific force (i.e., muscle force per unit of cross-sectional area), suggesting reduced muscle quality. Data is gathering to show that it is principally the weakness that accompanies sarcopenia, not the loss of muscle size per se that contributes to disability [62, 159, 161]. It is possible that the disproportionate loss of force and power compared to loss of muscle mass originates inside the muscle fibers themselves, due to defects on the excitation-contraction coupling (ECC) process that ultimately lead to reduced availability of calcium to be released during each cycle of contraction-relaxation [66, 102, 176]. Reflecting on the physiology behind muscle contraction, it is reasonable to postulate that factors released from distant tissues could influence the steps leading up to skeletal muscle contraction. The mismatch observed between muscle mass and strength, might at least in part, be explained by other tissue factors that influence the EC coupling, such as reduced calcium release from the sarcoplasmic reticulum (see Fig. 4.8).
Evidence for muscle atrophy, decreased contractile force, and reduced power in skeletal muscles suggested similarity from old WT and MIPKO mice. In all figures, the black bars are mature, wild type mice, the red bars are old, wild type mice, the green bars are mature MIPKO mice, and the blue bars are old, MIPKO mice. (a) Typical Toluidine blue-stained cross sections of EDL muscles from young Wt, old Wt, and mature MIPKO mice. The cross-sectional areas of old Wtand MIPKO cells are significantly reduced compared with those of the young Wt. (b) Maximal contractile force in EDL muscle for each genotype. Atrophy (decrease in muscle cross-sectional area) can explain ~1/2 of the drop in total force (note the dotted horizontal line), but does not account for the complete decrease in contractile force. (c) Data from b, except that force is normalized per cross-sectional area (N/cm2). This figure illustrates the atrophy-independent component of contractile dysfunction. (d) Maximal power in EDL muscle from all four animal models. (e) Data from panel Dwas normalized per cross sectional area of muscles. It shows that a significant drop in power is atrophy-independent. Data is the average ± SE of 24 EDL muscles from 12 mice for each genotype. * indicates a significant difference (p < 0.01) between the control muscles and a particular genotype. ** indicates a significant difference (p < 0.01) between the old MIPKO mice and the old Wtand mature MIPKO mice (FROM Romero-Suarez et al. [176])
It has also been noted that store-operated calcium entry is reduced in aged muscle cells. In a recent review, the argument is made that there is most likely a link between dysfunctional intracellular calcium homeostasis, the newly discovered modulatory genes, and biochemical factors secreted by other body tissues, which is illustrated in Fig. 4.9.
Schematic drawing of the triad junction, the chief site of the E-C coupling process in skeletal muscles. The predicted localization of the four genes/proteins emphasized in this review article is shown and they are represented in different colors along with the Dihydropyridine Receptor (DHPR), the Ryanodine Receptortype1 (RyR1) and Calsequestrin (CSQ). In youngmusclesE-C coupling is effectively maintained through coordinated actions of the E-C coupling machinery and the optimal participation of MG29, MTMR14, SAR, and KLF15. Their concentration and/or effectiveness is reduced with aging, which associates with structural changes of the triad junction itself. Together these biochemical and morphological changes contribute to the reduced coupling between depolarization of the sarcolemma and contraction due to the reduced calcium release capacity of aged muscles. In summary, “E-C coupling quality” is reduced in aged muscles, and becomes a key factor to reduced muscle quality during aging. The steps of the E-C coupling process are described in detail in the text. In skeletal muscles, depolarization of the sarcolemma and its invaginations (t-tubules) represented by the lightning bolt in yellow color alters the configuration of the DHPR, which modifies its interaction with RyR1, leading to the dominant type of calcium release in skeletal muscle (depolarization-induced calcium release, DICR). This initial release phase can be further amplified by a secondary mechanism, calcium-induced calcium release (CICR), the main release mechanism in cardiac muscles. The structural deformation as well as the lack of organized triads is a hallmark of aged muscles and also common in other diseases covered in this article. Not detailed in this figure is the process of calcium entry or re-entry, store-operated calcium entry (SOCE), responsible for continual refilling of the sarcoplasmic reticulum (SR). SOCE is also reduced with aging, which we have postulated contributes to sarcopenia and to the un-matching between muscle mass and muscle contractile force during aging, since force/power decrease significantly more than the observed decrease in muscle mass. We foresee that new generations of drugs could be developed to specifically target the different steps of E-C coupling in disease states to increase efficiency of Ca2+ handling. F. Altered Ca + 2 homeostasis is present in muscle fibers from old Wtand MIPKO mice. Original traces representative of caffeine-induced Fura-2 Ca + 2 transients in mature Wt (black trace), old Wt (red trace), and mature MIPKO FDB muscle fibers (blue trace). Examples shown are representative of 6–12 muscle fibers from 3 mice, and data were normalized to the intracellular Ca + 2 concentrations in nM (From Manring et al. [102], doi:10.3389/fphys.2014.00037. eCollection 2014. Review)
Additional health risks experienced by sarcopenic older adults include insulin resistance and the development of type 2 diabetes mellitus. Srikanthan, Hevener, and Karlamangla conducted a study to investigate the relationship between sarcopenia, obesity and age-related insulin resistance. In their cross-sectional analysis of the National Health and Nutrition Examination Survey III (NANES III), they concluded that sarcopenia, independent of obesity, is associated with compromised glucose metabolism [177]. In support of that analysis, another study conducted around the same time concurred that type 2 diabetes was associated with an increased risk of sarcopenia [178]. A relationship between diabetes and sarcopenia certainly makes physiologic sense from the perspective that skeletal muscle represents the largest target tissue for insulin-mediated glucose uptake. A decline in muscle mass with aging is, therefore, associated with a decrease in sites for glucose uptake, which would be further exacerbated by a decline in physical activity. Along with this, data supports an increase in triglycerides with aging, which have been indicted both in age-related mitochondrial damage and with blocking of ability of insulin to facilitate glucose entry into the muscle cell. All of these phenomena contribute to an increase in blood glucose. Insulin is a potent anabolic hormone that impacts glucose, protein and lipid metabolism, and may play a significant role in all of this as well. It facilitates glucose uptake, inhibits hepatic glucose uptake and triglyceride production, inhibits skeletal muscle protein synthesis and inhibits adipose tissue lipolysis [179]. Recognizing this relationship, research conducted by Lee et al. provided data supporting a direct relationship between insulin resistance, the loss of lean muscle mass and the gain of fat mass in men aged 65 and older [180]. The chronic complications of diabetes mellitus affect systems throughout the body; including bones. Individuals with type 1 diabetes mellitus have lower bone mass density, with impaired bone formation believed to be the primary cause [181]. Patients with type 1- or type 2-diabetic patients experience hypercalciuria during times of glycosuria. This increased loss of calcium has been hypothesized to contribute to impaired bone quality observed with diabetes, although the direct effects of this loss of calcium on skeletal muscle function remains elusive. As more is understood about these chronic conditions, the connections between them are becoming undeniable. Recognizing these connections and conducting research from this multifactorial perspective will deepen understanding and further the development of meaningful interventions (Fig. 4.10).
Bone-muscle crosstalk, interactions with other tissues, and impact on chronic diseases. This original drawing illustrates the concept that interactions among different tissues throughout the organism are abundant and much more complex than previously realized. In this larger context, bone–muscle cross talk remains both physiologically and pathologically relevant but is also seen as being affected by other tissues of the body. At the center of this figure is the outline of an individual, the patient. The smaller circle, closest to the patient, lists cells discussed in the text, along with factors they are known to secrete. The dashed line connecting these cells indicates that they are connected biochemically through the impact that their secreted factors have on one another. The larger circle surrounding the patient lists a number of conditions and diseases impacted by the biochemical interactions between cells listed and others. Special significance for multi-tissue/organ cross talk is revealed by pathological conditions such as obesity, diabetes, and metabolic syndrome. The dotted line of this larger circle indicates the developing understanding that these conditions and diseases impact one another. These conditions seem to directly influence sarcopenia and osteoporosisasdetailed in the text (From Isaacson and Brotto [182])
The Role of Cartilage, Ligaments, and Tendons in Bone-Muscle Crosstalk
Crosstalk in MSK Development
As previously mentioned in this chapter, tissues of the musculoskeletal (MSK) system have been traditionally studied as individual and autonomous entities, in spite of being functionally intimately associated. This is especially true for bones, muscles, and tendons, which are commonly referred to as the musculoskeletal unit. This interrelationship is more noticeably characterized by a biomechanical interdependence, which is essential for body movement. Tendons, in most cases, connect muscles to bones, as muscles contract and shorten, they pull tendons, which in their turn pull bones, resulting in movement. This way, a weakness in any component should imply in loss of functionality of the whole unit. In addition to bones, muscles, and tendons, other tissues are also part of the MSK system, such as ligaments, which are responsible for bone to bone connection and essential for joint stability, and cartilaginous tissues. At the articular ends of bones, hyaline cartilage is closely associated with bone tissue as they form cartilaginous joints.
Tissue interactions required for tendon progenitor induction in vertebrate embryos. Induction of tendon progenitors, identified as Scx-expressing cells, depends on a unique set of tissue interactions in different parts of the embryo. Each panel shows tendon progenitor distributionby whole-mount in situ hybridization (ISH) with an Scxprobe. The line across each upper image shows the orientation of the section schematized beneath, which highlights the relevant tissue interactions (with tendon progenitors shown in green; muscle progenitors in red; cartilage in yellow). (a) Whole-mount ScxISH on E10.5 mouse embryo and a schematic of a frontal trunk section, showing somite pairs (squares) and the neural tube (gray). Skeletal tissue derives from the sclerotome(Sc) of somites, whereas the musculature arises from the myotome(m). The tendon progenitors are found in the syndetome(S, green), a stripe of sclerotomecells at the junction between two adjacent myotomes. Scxexpression in syndetomecells is induced by FGFs secreted from the adjacent myotomes (arrows). (b) Whole-mount ScxISH on E10.5 mouse limb bud and a schematized sagittal section through the limb bud. In the early limb bud, Scxis expressed in mesodermal cells directly under the dorsal and ventral ectoderm. Scxexpression at this stage depends on ectoderm (curved arrows) and not on a signal from the myoblasts or from pre-chondrogeniccells. (c) Whole mount ScxISH on E12.5 mouse limb and a schematized sagittal section through the autopod. In the differentiating autopod, Scxis expressed in subectodermalmesoderm along the differentiating skeletal elements. Scxexpression along the differentiating digits can be induced by a signal from the skeletal condensations (straight arrow), and the sub-ectodermal position of the tendon progenitors suggests a role for the ectoderm (curved arrows) in tendon induction as well. A anterior, D distal, P posterior, Pr proximal, nt neural tube (From Schweitzer et al. [183])
More recently, the concept that the communication between MSK tissues may extend beyond their biomechanical relationship has been gaining momentum as novel evidence in this direction is acquired through new research. In this case, MSK tissues would talk by exchanging chemical factors, in a paracrine or even endocrine way, that is, factors produced by one tissue would exert a determined effect on another tissue of the MSK system. Earlier in the chapter, we presented evidence about this biochemical crosstalk between bones and muscles. However, what about other tissues of the MSK system? Is it reasonable to expect that they also communicate via chemical factors? Or, alternatively, do they merely fulfill an essentially mechanical function?
In order to answer these intriguing questions, first we turn our attention to the development of the MSK system, where the importance of a crosstalk, biomechanical and biochemical, has been demonstrated. The events that characterize MSK embryologic development are quite complex and the objective of this section is not to present a comprehensive review of the topic, rather we will solely focus on findings that point to a biochemical crosstalk between tissues of the MSK system during development. Furthermore, we will restrict our discussion to vertebrates, more specifically using limb development as a model [184]. Muscles, tendons, and bones progenitor cells originate from different somites (i.e., divisions) of the mesoderm, respectively, the myotome, the syndetome, and the sclerotome. Two regions critical for the development of the MSK unit (muscle-tendon-bone): the myotendinous junction and the entheses, are specialized regions representing the muscle-tendon and tendon-bone interfaces, respectively. Correct assembly of these regions, which requires close interactions between these tissues, is crucial for the proper functioning of the MSK system.
Experimental evidence has shown that, in addition to the most flagrant role of mechanical load, the biochemical communication between bone, tendon, and muscle is crucial to their proper development. For example, scleraxis (Scx), a tendon marker, regulates the genetic expression of bone morphogenic protein-4 (Bmp4) in tendon cells. When Bmp4 expression was blocked in mice, it led to a partial loss of bone ridges [183], suggesting a role of factors secreted by tendon on bone ridge formation. In addition, syndetome-induction, which will initiate tendon formation in mouse embryos, is associated with fibroblast growth factors (FGFs), FGF-4 and FGF-6 in mice, and FGF-8 in chicken [64, 185], only expressed in the myotome. This induction is a consequence of the activation of Scx expression and other tendon markers [64, 186] (Fig. 4.11). Down-regulation of these tendon markers in muscle-less and aneural conditions was reverted by the administration of exogenous FGF4, demonstrating an unequivocal biochemical dependence of tendon formation from muscle [187]. On the other hand, muscle development, initially characterized by increased proliferation of myogenic cells with later adjustment to normal morphology, happens because of controlled cell death modulated by local apoptotic factor(s). Interestingly, only muscle fibers that are not part of a stable myotendinous junction are affected, suggesting a role for tendon in muscle that belies morphogenesis. Retinoic acid, produced by both tendon and muscle, has been suggested as a potential apoptotic factor with an important role in mediating muscle apoptosis and muscle-tendon assembly [188].
Bone-Cartilage Crosstalk
Like other interactions between contiguous tissues of the MSK system, mechanical load is an integral part of their relationship and biomechanical crosstalk is indisputable. In this way, defective bone remodeling affects its mechanical properties, and, consequently, modifies how load is transmitted to cartilage, which ultimately results in altered local strains, and cartilage weakening and disease. Several studies have shown that initiation of osteoarthritis (OA) is preceded by increased osteoclastic activity and subchondral bone resorption [68], but it is not clear if it happens only because of mechanical causes or if other factors are also involved. Despite this almost ubiquitous mechanical influence and the difficulty of removing the mechanical influence in this relationship, there is evidence that also points to a biochemical crosstalk between subchondral bone and cartilage in OA. In mice, over-expression of the EPHB4 receptor in osteoblasts was able to protect against OA induced by medial meniscus destabilization. In this case, OA was not initially related to a previously altered mechanical environment, and molecular changes in bone were able to deter OA development, which clearly suggests a role for factor(s) produced by bone in this process, and a bone-cartilage crosstalk [189]. There is also evidence that the hepatocyte growth-factor (HGF) may be part of the bone-cartilage crosstalk in OA. HGF expression and production in human subchondral osteoblasts are increased in OA, while the protein, but not the gene, can be detected in the articular cartilage, suggesting that subchondral bone could be the origin of that HGF. Other potential players in the bone-cartilage crosstalk are RANK ligand (RANKL) and osteoprotegerin (OPG). Interestingly, though both molecules are produced by bone and cartilage cells, RANK receptor is expressed only in human OA chondrocytes [190]. How does this crosstalk happen? First, there is evidence that small molecules can easily diffuse between the bone marrow and the articular space, suggesting that, at least for small molecules, a direct exchange of biochemical factors between subchondral bone and articular cartilage is possible in a paracrine fashion [189, 191]. Second, during the pathogenesis of OA, vascular penetration in cartilage would expose the chondrocytes to cytokines and growth factors, such as VEGF, NGF, IL-1, IL-6, HGF, or IGF-1, from subchondral bone [192]. Overall, the demonstration of the bone-cartilage crosstalk indicates that targeting subchondral bone is a viable therapeutic approach in the OA treatment [193].
Tendon-Muscle Crosstalk
We have mentioned that during development there is strong evidence pointing to a biochemical crosstalk between muscle and tendon. Is there similar evidence post-development? Although the crosstalk between MSK tissues is a recently new research topic and the factors supposedly responsible for the crosstalk are yet to be identified, there are subtle but unquestionable indications that the relationship between muscles and tendons go beyond their biomechanical dependence.
Tendinopathies are common overuse injuries in sports and are often associated with aging. Tendons are difficult to heal, and most of the time the mechanical properties of the tissue are poorer when compared to the normal tissue. Clinicians have known for quite a long time that eccentric (i.e. lengthening contraction), not concentric (i.e. shortening contraction), training is the most effective conservative treatment to promote healing of tendon diseases, including Achilles and patellar tendinopathies [63, 194]. In eccentric training muscle contraction occurs at the same time that the muscles and tendons are stretching or remain stretched [63]. Despite overwhelming clinical evidence, the mechanisms of how eccentric contraction improves tendon healing remain unknown. The answer may be in how the expression of growth factors, such as TGFβ-1 and IGF-1, respond to eccentric and concentric training in tendons and muscles. Heinemeier et al. exposed rats to short-term strength training consisting of pure shortening (concentric), lengthening (eccentric), or static plantar extensors contraction. Strength training in the Achilles tendon, regardless of the type of contraction, increased the expression of TGFβ-1 and IGF-1, even though the force produced was higher during the eccentric contractions. In the gastrocnemius muscle, there was similar upregulation of growth factors; however, the effect of lengthening was significantly greater than the effect of shortening [195]. The fact that muscle, but not tendon, responded differently depending on the type of strength training strongly suggests that if eccentric contractions have superior effect on tendon healing, it may be caused by one or more muscle factors produced during eccentric but not concentric contraction.
Transgenic mice are useful models to study the role of specific cytokines in different tissues. The mdx mouse is the classical animal model for Duchenne muscular dystrophy. Dystrophin is a cytoplasmatic protein that forms a complex that connects the cytoskeleton of the muscle fiber to the surrounding extracellular matrix. Without the dystrophin-complex, the sarcolemma becomes fragile and as the muscle fibers contract the muscle is damaged. As a result, mdx skeletal muscles are ~20 % weaker than normal muscles. Rizzuto et al. found that in dystrophin-deficient (mdx) mice, tendons are also affected by an increase in the number of dead cells, more energy dissipation during dynamic loading, and a significant loss of the elastic properties of the tissue. Furthermore, these functional changes suggest that mdx tendon experience similar alterations to those found in mdx muscles (reduction of viable cells and higher inflammatory response). It could be argued that a weaker muscle would cause a loss in tendon mechanical properties, but the similarity in response to missing dystrophin could also mean that either the protein has a role in tendon homeostasis or that there is a paracrine communication between muscles and tendons [196].
The existence of a crosstalk between tissues of the MSK system, in development and adult life, are crucial for a better understanding of the biology of theses tissues and may open the door to strategies that would improve the regeneration of these tissues, especially those that are difficult to heal.
Concluding Remarks and Future Directions
In the year 2000, United Nations member states signed the United Nations Millennium Declaration agreeing to work toward the achievement of eight Millennium Development Goals (MDGs) by the year 2030. Among these are the goals to improve health and combat disease. While major issues related to health care education and access, such as proper diet, exercise levels, and a host of social factors remain critical to be addressed, if humanity is to achieve the WHO health goals, all of us must do more. Even in face of all these challenges, however, humans are living longer due in large part to basic improvements in health conditions and reductions in absolute levels of poverty or misery.
Life expectancy in Japan has reached almost 83 years and the oldest human on record has lived to 122 years of age. Very simple metabolic and telomerase estimations give us the clue that humans could live to 125 years of age. This increasing life expectancy poses a unique set of challenges. On the one hand, there is the desire to live a longer and healthier life, but the cost seems quite high since morbidities and co-morbidities combine to afflict in particular older adults. Musculoskeletal diseases alone affect almost 2 billion humans in the planet and the large majority of them are older persons. The puzzle that is facing us is that while living a long life is desirable; it is really the quality of such life that matters the most.
As MSK scientists are trying to put the pieces of this puzzle together, they have come across some very interesting new ideas. There is no doubt that bones-tendons-muscles come together in a unit of mechanical coupling where physical forces are constantly shaping the relationships between these tissues. What is relatively new is the “kine”; the endocrine-like role that these tissues play. It seems that the human body is significantly more endocrine than we had ever anticipated and the MSK players are no different from other parts of the body.
Thus, in this complex interaction of physical forces and secreted factors (myokines, osteokines, tenokines), these tissues interact both physically and biochemically in ways about which we are still learning. However, it is even more complex. Behind these interactions, there are complex genetic signaling pathways apparently shared among these tissues, and this pleiotropy might itself influence the way these tissues respond to physical and biochemical forces and factors.
In a world filled with uncertainty, there is one certainty; the MSK field is poised to bring many new developments and advancements as we improve our understanding of the MSK system and how different tissues interact and prime other in heath and disease. If we learn for example to control or modulate the secretion or to mimic the effects of the “kines”, many MSK conditions could be treated or improved, including the twin diseases of aging, osteoporosis and sarcopenia. One last and very positive aspect of this field is that its basic research is continuing to push new boundaries of cell biological understanding, thus facilitating the development of new technologies that will benefit science and humankind in general.
References
Pourquie O. Vertebrate somitogenesis. Annu Rev Cell Dev Biol. 2001;17:311–50. doi:10.1146/annurev.cellbio.17.1.311.
Land C, Schoenau E. Fetal and postnatal bone development: reviewing the role of mechanical stimuli and nutrition. Best Pract Res Clin Endocrinol Metab. 2008;22(1):107–18. doi:10.1016/j.beem.2007.09.005.
Rauch F, Schoenau E. The developing bone: slave or master of its cells and molecules? Pediatr Res. 2001;50(3):309–14. doi:10.1203/00006450-200109000-00003.
Gunter KB, Almstedt HC, Janz KF. Physical activity in childhood may be the key to optimizing lifespan skeletal health. Exerc Sport Sci Rev. 2012;40(1):13–21. doi:10.1097/JES.0b013e318236e5ee.
Recker R, Lappe J, Davies K, Heaney R. Characterization of perimenopausal bone loss: a prospective study. J Bone Miner Res Off J Am Soc Bone Miner Res. 2000;15(10):1965–73. doi:10.1359/jbmr.2000.15.10.1965.
Hu MC, Shiizaki K, Kuro-o M, Moe OW. Fibroblast growth factor 23 and Klotho: physiology and pathophysiology of an endocrine network of mineral metabolism. Annu Rev Physiol. 2013;75:503–33. doi:10.1146/annurev-physiol-030212-183727.
Novotny SA, Warren GL, Hamrick MW. Aging and the muscle-bone relationship. Physiology. 2015;30:8–16.
Arden NK, Spector TD. Genetic influences on muscle strength, lean body mass, and bone mineral density: a twin study. J Bone Miner Res Off J Am Soc Bone Miner Res. 1997;12(12):2076–81. doi:10.1359/jbmr.1997.12.12.2076.
Costa AM, Breitenfeld L, Silva AJ, Pereira A, Izquierdo M, Marques MC. Genetic inheritance effects on endurance and muscle strength: an update. Sports Med. 2012;42(6):449–58. doi:10.2165/11650560-000000000-00000.
Prior SJ, Roth SM, Wang X, Kammerer C, Miljkovic-Gacic I, Bunker CH, Wheeler VW, Patrick AL, Zmuda JM. Genetic and environmental influences on skeletal muscle phenotypes as a function of age and sex in large, multigenerational families of African heritage. J Appl Physiol. 2007;103(4):1121–7. doi:10.1152/japplphysiol.00120.2007.
Silventoinen K, Magnusson PK, Tynelius P, Kaprio J, Rasmussen F. Heritability of body size and muscle strength in young adulthood: a study of one million Swedish men. Genet Epidemiol. 2008;32(4):341–9. doi:10.1002/gepi.20308.
Cheng Y, Rachagani S, Canovas A, Mayes MS, Tait Jr RG, Dekkers JC, Reecy JM. Body composition and gene expression QTL mapping in mice reveals imprinting and interaction effects. BMC Genet. 2013;14:103. doi:10.1186/1471-2156-14-103.
Guo YF, Zhang LS, Liu YJ, Hu HG, Li J, Tian Q, Yu P, Zhang F, Yang TL, Guo Y, Peng XL, Dai M, Chen W, Deng HW. Suggestion of GLYAT gene underlying variation of bone size and body lean mass as revealed by a bivariate genome-wide association study. Hum Genet. 2013;132(2):189–99. doi:10.1007/s00439-012-1236-5.
Hai R, Pei YF, Shen H, Zhang L, Liu XG, Lin Y, Ran S, Pan F, Tan LJ, Lei SF, Yang TL, Zhang Y, Zhu XZ, Zhao LJ, Deng HW. Genome-wide association study of copy number variation identified gremlin1 as a candidate gene for lean body mass. J Hum Genet. 2012;57(1):33–7. doi:10.1038/jhg.2011.125.
Keildson S, Fadista J, Ladenvall C, Hedman AK, Elgzyri T, Small KS, Grundberg E, Nica AC, Glass D, Richards JB, Barrett A, Nisbet J, Zheng HF, Ronn T, Strom K, Eriksson KF, Prokopenko I, Consortium M, Consortium D, Mu TC, Spector TD, Dermitzakis ET, Deloukas P, McCarthy MI, Rung J, Groop L, Franks PW, Lindgren CM, Hansson O. Expression of phosphofructokinase in skeletal muscle is influenced by genetic variation and associated with insulin sensitivity. Diabetes. 2014;63(3):1154–65. doi:10.2337/db13-1301.
Kuo T, Lew MJ, Mayba O, Harris CA, Speed TP, Wang JC. Genome-wide analysis of glucocorticoid receptor-binding sites in myotubes identifies gene networks modulating insulin signaling. Proc Natl Acad Sci U S A. 2012;109(28):11160–5. doi:10.1073/pnas.1111334109.
Liu XG, Tan LJ, Lei SF, Liu YJ, Shen H, Wang L, Yan H, Guo YF, Xiong DH, Chen XD, Pan F, Yang TL, Zhang YP, Guo Y, Tang NL, Zhu XZ, Deng HY, Levy S, Recker RR, Papasian CJ, Deng HW. Genome-wide association and replication studies identified TRHR as an important gene for lean body mass. Am J Hum Genet. 2009;84(3):418–23. doi:10.1016/j.ajhg.2009.02.004.
Perusse L, Rankinen T, Rauramaa R, Rivera MA, Wolfarth B, Bouchard C. The human gene map for performance and health-related fitness phenotypes: the 2002 update. Med Sci Sports Exerc. 2003;35(8):1248–64. doi:10.1249/01.MSS.0000078938.84161.22.
Thomis MA, De Mars G, Windelinckx A, Peeters MW, Huygens W, Aerssens J, Beunen GP. Genome-wide linkage scan for resistance to muscle fatigue. Scand J Med Sci Sports. 2011;21(4):580–8. doi:10.1111/j.1600-0838.2009.01082.x.
Windelinckx A, De Mars G, Huygens W, Peeters MW, Vincent B, Wijmenga C, Lambrechts D, Delecluse C, Roth SM, Metter EJ, Ferrucci L, Aerssens J, Vlietinck R, Beunen GP, Thomis MA. Comprehensive fine mapping of chr12q12-14 and follow-up replication identify activin receptor 1B (ACVR1B) as a muscle strength gene. Eur J Hum Genet EJHG. 2011;19(2):208–15. doi:10.1038/ejhg.2010.173.
Duncan EL, Danoy P, Kemp JP, Leo PJ, McCloskey E, Nicholson GC, Eastell R, Prince RL, Eisman JA, Jones G, Sambrook PN, Reid IR, Dennison EM, Wark J, Richards JB, Uitterlinden AG, Spector TD, Esapa C, Cox RD, Brown SD, Thakker RV, Addison KA, Bradbury LA, Center JR, Cooper C, Cremin C, Estrada K, Felsenberg D, Gluer CC, Hadler J, Henry MJ, Hofman A, Kotowicz MA, Makovey J, Nguyen SC, Nguyen TV, Pasco JA, Pryce K, Reid DM, Rivadeneira F, Roux C, Stefansson K, Styrkarsdottir U, Thorleifsson G, Tichawangana R, Evans DM, Brown MA. Genome-wide association study using extreme truncate selection identifies novel genes affecting bone mineral density and fracture risk. PLoS Genet. 2011;7(4):e1001372. doi:10.1371/journal.pgen.1001372.
Estrada K, Styrkarsdottir U, Evangelou E, Hsu YH, Duncan EL, Ntzani EE, Oei L, Albagha OM, Amin N, Kemp JP, Koller DL, Li G, Liu CT, Minster RL, Moayyeri A, Vandenput L, Willner D, Xiao SM, Yerges-Armstrong LM, Zheng HF, Alonso N, Eriksson J, Kammerer CM, Kaptoge SK, Leo PJ, Thorleifsson G, Wilson SG, Wilson JF, Aalto V, Alen M, Aragaki AK, Aspelund T, Center JR, Dailiana Z, Duggan DJ, Garcia M, Garcia-Giralt N, Giroux S, Hallmans G, Hocking LJ, Husted LB, Jameson KA, Khusainova R, Kim GS, Kooperberg C, Koromila T, Kruk M, Laaksonen M, Lacroix AZ, Lee SH, Leung PC, Lewis JR, Masi L, Mencej-Bedrac S, Nguyen TV, Nogues X, Patel MS, Prezelj J, Rose LM, Scollen S, Siggeirsdottir K, Smith AV, Svensson O, Trompet S, Trummer O, van Schoor NM, Woo J, Zhu K, Balcells S, Brandi ML, Buckley BM, Cheng S, Christiansen C, Cooper C, Dedoussis G, Ford I, Frost M, Goltzman D, Gonzalez-Macias J, Kahonen M, Karlsson M, Khusnutdinova E, Koh JM, Kollia P, Langdahl BL, Leslie WD, Lips P, Ljunggren O, Lorenc RS, Marc J, Mellstrom D, Obermayer-Pietsch B, Olmos JM, Pettersson-Kymmer U, Reid DM, Riancho JA, Ridker PM, Rousseau F, Slagboom PE, Tang NL, Urreizti R, Van Hul W, Viikari J, Zarrabeitia MT, Aulchenko YS, Castano-Betancourt M, Grundberg E, Herrera L, Ingvarsson T, Johannsdottir H, Kwan T, Li R, Luben R, Medina-Gomez C, Palsson ST, Reppe S, Rotter JI, Sigurdsson G, van Meurs JB, Verlaan D, Williams FM, Wood AR, Zhou Y, Gautvik KM, Pastinen T, Raychaudhuri S, Cauley JA, Chasman DI, Clark GR, Cummings SR, Danoy P, Dennison EM, Eastell R, Eisman JA, Gudnason V, Hofman A, Jackson RD, Jones G, Jukema JW, Khaw KT, Lehtimaki T, Liu Y, Lorentzon M, McCloskey E, Mitchell BD, Nandakumar K, Nicholson GC, Oostra BA, Peacock M, Pols HA, Prince RL, Raitakari O, Reid IR, Robbins J, Sambrook PN, Sham PC, Shuldiner AR, Tylavsky FA, van Duijn CM, Wareham NJ, Cupples LA, Econs MJ, Evans DM, Harris TB, Kung AW, Psaty BM, Reeve J, Spector TD, Streeten EA, Zillikens MC, Thorsteinsdottir U, Ohlsson C, Karasik D, Richards JB, Brown MA, Stefansson K, Uitterlinden AG, Ralston SH, Ioannidis JP, Kiel DP, Rivadeneira F. Genome-wide meta-analysis identifies 56 bone mineral density loci and reveals 14 loci associated with risk of fracture. Nat Genet. 2012;44(5):491–501. doi:10.1038/ng.2249.
Karasik D, Hsu YH, Zhou Y, Cupples LA, Kiel DP, Demissie S. Genome-wide pleiotropy of osteoporosis-related phenotypes: the Framingham Study. J Bone Miner Res Off J Am Soc Bone Miner Res. 2010;25(7):1555–63. doi:10.1002/jbmr.38.
Lee YH, Choi SJ, Ji JD, Song GG. Pathway analysis of genome-wide association study for bone mineral density. Mol Biol Rep. 2012;39(8):8099–106. doi:10.1007/s11033-012-1657-1.
Oei L, Hsu YH, Styrkarsdottir U, Eussen BH, de Klein A, Peters MJ, Halldorsson B, Liu CT, Alonso N, Kaptoge SK, Thorleifsson G, Hallmans G, Hocking LJ, Husted LB, Jameson KA, Kruk M, Lewis JR, Patel MS, Scollen S, Svensson O, Trompet S, van Schoor NM, Zhu K, Buckley BM, Cooper C, Ford I, Goltzman D, Gonzalez-Macias J, Langdahl BL, Leslie WD, Lips P, Lorenc RS, Olmos JM, Pettersson-Kymmer U, Reid DM, Riancho JA, Slagboom PE, Garcia-Ibarbia C, Ingvarsson T, Johannsdottir H, Luben R, Medina-Gomez C, Arp P, Nandakumar K, Palsson ST, Sigurdsson G, van Meurs JB, Zhou Y, Hofman A, Jukema JW, Pols HA, Prince RL, Cupples LA, Marshall CR, Pinto D, Sato D, Scherer SW, Reeve J, Thorsteinsdottir U, Karasik D, Richards JB, Stefansson K, Uitterlinden AG, Ralston SH, Ioannidis JP, Kiel DP, Rivadeneira F, Estrada K. A genome-wide copy number association study of osteoporotic fractures points to the 6p25.1 locus. J Med Genet. 2014;51(2):122–31. doi:10.1136/jmedgenet-2013-102064.
Ran S, Pei YF, Liu YJ, Zhang L, Han YY, Hai R, Tian Q, Lin Y, Yang TL, Guo YF, Shen H, Thethi IS, Zhu XZ, Deng HW. Bivariate genome-wide association analyses identified genes with pleiotropic effects for femoral neck bone geometry and age at menarche. PLoS One. 2013;8(4):e60362. doi:10.1371/journal.pone.0060362.
Rivadeneira F, Styrkarsdottir U, Estrada K, Halldorsson BV, Hsu YH, Richards JB, Zillikens MC, Kavvoura FK, Amin N, Aulchenko YS, Cupples LA, Deloukas P, Demissie S, Grundberg E, Hofman A, Kong A, Karasik D, van Meurs JB, Oostra B, Pastinen T, Pols HA, Sigurdsson G, Soranzo N, Thorleifsson G, Thorsteinsdottir U, Williams FM, Wilson SG, Zhou Y, Ralston SH, van Duijn CM, Spector T, Kiel DP, Stefansson K, Ioannidis JP, Uitterlinden AG, Genetic Factors for Osteoporosis C. Twenty bone-mineral-density loci identified by large-scale meta-analysis of genome-wide association studies. Nat Genet. 2009;41(11):1199–206. doi:10.1038/ng.446.
Savage SA, Mirabello L, Wang Z, Gastier-Foster JM, Gorlick R, Khanna C, Flanagan AM, Tirabosco R, Andrulis IL, Wunder JS, Gokgoz N, Patino-Garcia A, Sierrasesumaga L, Lecanda F, Kurucu N, Ilhan IE, Sari N, Serra M, Hattinger C, Picci P, Spector LG, Barkauskas DA, Marina N, de Toledo SR, Petrilli AS, Amary MF, Halai D, Thomas DM, Douglass C, Meltzer PS, Jacobs K, Chung CC, Berndt SI, Purdue MP, Caporaso NE, Tucker M, Rothman N, Landi MT, Silverman DT, Kraft P, Hunter DJ, Malats N, Kogevinas M, Wacholder S, Troisi R, Helman L, Fraumeni Jr JF, Yeager M, Hoover RN, Chanock SJ. Genome-wide association study identifies two susceptibility loci for osteosarcoma. Nat Genet. 2013;45(7):799–803. doi:10.1038/ng.2645.
Zhang L, Choi HJ, Estrada K, Leo PJ, Li J, Pei YF, Zhang Y, Lin Y, Shen H, Liu YZ, Liu Y, Zhao Y, Zhang JG, Tian Q, Wang YP, Han Y, Ran S, Hai R, Zhu XZ, Wu S, Yan H, Liu X, Yang TL, Guo Y, Zhang F, Guo YF, Chen Y, Chen X, Tan L, Zhang L, Deng FY, Deng H, Rivadeneira F, Duncan EL, Lee JY, Han BG, Cho NH, Nicholson GC, McCloskey E, Eastell R, Prince RL, Eisman JA, Jones G, Reid IR, Sambrook PN, Dennison EM, Danoy P, Yerges-Armstrong LM, Streeten EA, Hu T, Xiang S, Papasian CJ, Brown MA, Shin CS, Uitterlinden AG, Deng HW. Multistage genome-wide association meta-analyses identified two new loci for bone mineral density. Hum Mol Genet. 2014;23(7):1923–33. doi:10.1093/hmg/ddt575.
Gupta M, Cheung CL, Hsu YH, Demissie S, Cupples LA, Kiel DP, Karasik D. Identification of homogeneous genetic architecture of multiple genetically correlated traits by block clustering of genome-wide associations. J Bone Miner Res Off J Am Soc Bone Miner Res. 2011;26(6):1261–71. doi:10.1002/jbmr.333.
Karasik D, Cohen-Zinder M. Osteoporosis genetics: year 2011 in review. Bonekey Rep. 2012;1:114. doi:10.1038/bonekey.2012.114.
Karasik D, Kiel DP. Evidence for pleiotropic factors in genetics of the musculoskeletal system. Bone. 2010;46(5):1226–37. doi:10.1016/j.bone.2010.01.382.
Karasik D, Zhou Y, Cupples LA, Hannan MT, Kiel DP, Demissie S. Bivariate genome-wide linkage analysis of femoral bone traits and leg lean mass: Framingham study. J Bone Miner Res Off J Am Soc Bone Miner Res. 2009;24(4):710–8. doi:10.1359/jbmr.081222.
Sun L, Tan LJ, Lei SF, Chen XD, Li X, Pan R, Yin F, Liu QW, Yan XF, Papasian CJ, Deng HW. Bivariate genome-wide association analyses of femoral neck bone geometry and appendicular lean mass. PLoS One. 2011;6(11):e27325. doi:10.1371/journal.pone.0027325.
Edmondson DG, Lyons GE, Martin JF, Olson EN. Mef2 gene expression marks the cardiac and skeletal muscle lineages during mouse embryogenesis. Development. 1994;120(5):1251–63.
Kramer I, Baertschi S, Halleux C, Keller H, Kneissel M. Mef2c deletion in osteocytes results in increased bone mass. J Bone Miner Res Off J Am Soc Bone Miner Res. 2012;27(2):360–73. doi:10.1002/jbmr.1492.
Cloutier P, Lavallee-Adam M, Faubert D, Blanchette M, Coulombe B. A newly uncovered group of distantly related lysine methyltransferases preferentially interact with molecular chaperones to regulate their activity. PLoS Genet. 2013;9(1):e1003210. doi:10.1371/journal.pgen.1003210.
Huang J, Hsu YH, Mo C, Abreu E, Kiel DP, Bonewald LF, Brotto M, Karasik D. METTL21C is a potential pleiotropic gene for osteoporosis and sarcopenia acting through the modulation of the NF-kappaB signaling pathway. J Bone Miner Res Off J Am Soc Bone Miner Res. 2014;29(7):1531–40. doi:10.1002/jbmr.2200.
Kimonis VE, Fulchiero E, Vesa J, Watts G. VCP disease associated with myopathy, Paget disease of bone and frontotemporal dementia: review of a unique disorder. Biochim Biophys Acta. 2008;1782(12):744–8. doi:10.1016/j.bbadis.2008.09.003.
McPherron AC, Lawler AM, Lee SJ. Regulation of skeletal muscle mass in mice by a new TGF-beta superfamily member. Nature. 1997;387(6628):83–90. doi:10.1038/387083a0.
Pedersen BK, Febbraio MA. Muscles, exercise and obesity: skeletal muscle as a secretory organ. Nat Rev Endocrinol. 2012;8(8):457–65. doi:10.1038/nrendo.2012.49.
Clop A, Marcq F, Takeda H, Pirottin D, Tordoir X, Bibe B, Bouix J, Caiment F, Elsen JM, Eychenne F, Larzul C, Laville E, Meish F, Milenkovic D, Tobin J, Charlier C, Georges M. A mutation creating a potential illegitimate microRNA target site in the myostatin gene affects muscularity in sheep. Nat Genet. 2006;38(7):813–8. doi:10.1038/ng1810.
Grobet L, Martin LJ, Poncelet D, Pirottin D, Brouwers B, Riquet J, Schoeberlein A, Dunner S, Menissier F, Massabanda J, Fries R, Hanset R, Georges M. A deletion in the bovine myostatin gene causes the double-muscled phenotype in cattle. Nat Genet. 1997;17(1):71–4. doi:10.1038/ng0997-71.
Kambadur R, Sharma M, Smith TP, Bass JJ. Mutations in myostatin (GDF8) in double-muscled Belgian Blue and Piedmontese cattle. Genome Res. 1997;7(9):910–6.
McPherron AC, Lee SJ. Double muscling in cattle due to mutations in the myostatin gene. Proc Natl Acad Sci U S A. 1997;94(23):12457–61.
Mosher DS, Quignon P, Bustamante CD, Sutter NB, Mellersh CS, Parker HG, Ostrander EA. A mutation in the myostatin gene increases muscle mass and enhances racing performance in heterozygote dogs. PLoS Genet. 2007;3(5), e79. doi:10.1371/journal.pgen.0030079.
Zhang GX, Zhao XH, Wang JY, Ding FX, Zhang L. Effect of an exon 1 mutation in the myostatin gene on the growth traits of the Bian chicken. Anim Genet. 2012;43(4):458–9. doi:10.1111/j.1365-2052.2011.02274.x.
Williams MS. Myostatin mutation associated with gross muscle hypertrophy in a child. N Engl J Med. 2004;351(10):1030–1; author reply 1030–1.
Elkasrawy MN, Hamrick MW. Myostatin (GDF-8) as a key factor linking muscle mass and bone structure. J Musculoskelet Neuronal Interact. 2010;10(1):56–63.
Williams NG, Interlichia JP, Jackson MF, Hwang D, Cohen P, Rodgers BD. Endocrine actions of myostatin: systemic regulation of the IGF and IGF binding protein axis. Endocrinology. 2011;152(1):172–80. doi:10.1210/en.2010-0488.
Perrini S, Laviola L, Carreira MC, Cignarelli A, Natalicchio A, Giorgino F. The GH/IGF1 axis and signaling pathways in the muscle and bone: mechanisms underlying age-related skeletal muscle wasting and osteoporosis. J Endocrinol. 2010;205(3):201–10. doi:10.1677/JOE-09-0431.
Fakhouri TH, Ogden CL, Carroll MD, Kit BK, Flegal KM. Prevalence of obesity among older adults in the United States, 2007–2010. NCHS Data Brief. 2012;106:1–8.
Landry PS, Marino AA, Sadasivan KK, Albright JA. Effect of soft-tissue trauma on the early periosteal response of bone to injury. J Trauma. 2000;48(3):479–83.
Stein H, Perren SM, Cordey J, Kenwright J, Mosheiff R, Francis MJ. The muscle bed–a crucial factor for fracture healing: a physiological concept. Orthopedics. 2002;25(12):1379–83.
Utvag SE, Iversen KB, Grundnes O, Reikeras O. Poor muscle coverage delays fracture healing in rats. Acta Orthop Scand. 2002;73(4):471–4. doi:10.1080/00016470216315.
Zacks SI, Sheff MF. Periosteal and metaplastic bone formation in mouse minced muscle regeneration. Lab Invest J Tech Methods Pathol. 1982;46(4):405–12.
Aydin A, Memisoglu K, Cengiz A, Atmaca H, Muezzinoglu B, Muezzinoglu US. Effects of botulinum toxin A on fracture healing in rats: an experimental study. J Orthop Sci Off J Jpn Orthop Assoc. 2012;17(6):796–801. doi:10.1007/s00776-012-0269-x.
Harry LE, Sandison A, Paleolog EM, Hansen U, Pearse MF, Nanchahal J. Comparison of the healing of open tibial fractures covered with either muscle or fasciocutaneous tissue in a murine model. J Orthop Res Off Publ Orthop Res Soc. 2008;26(9):1238–44. doi:10.1002/jor.20649.
Reverte MM, Dimitriou R, Kanakaris NK, Giannoudis PV. What is the effect of compartment syndrome and fasciotomies on fracture healing in tibial fractures? Injury. 2011;42(12):1402–7. doi:10.1016/j.injury.2011.09.007.
Agas D, Marchetti L, Hurley MM, Sabbieti MG. Prostaglandin F2alpha: a bone remodeling mediator. J Cell Physiol. 2013;228(1):25–9. doi:10.1002/jcp.24117.
Baumgartner RN, Koehler KM, Gallagher D, Romero L, Heymsfield SB, Ross RR, Garry PJ, Lindeman RD. Epidemiology of sarcopenia among the elderly in New Mexico. Am J Epidemiol. 1998;147(8):755–63.
Beltran-Sanchez H, Harhay MO, Harhay MM, McElligott S. Prevalence and trends of metabolic syndrome in the adult U.S. population, 1999–2010. J Am Coll Cardiol. 2013;62(8):697–703. doi:10.1016/j.jacc.2013.05.064.
Camargo PR, Alburquerque-Sendin F, Salvini TF. Eccentric training as a new approach for rotator cuff tendinopathy: review and perspectives. World J Orthop. 2014;5(5):634–44. doi:10.5312/wjo.v5.i5.634.
Charvet B, Ruggiero F, Le Guellec D. The development of the myotendinous junction. A review. Muscles Ligaments Tendons J. 2012;2(2):53–63.
Choquette S, Bouchard DR, Doyon CY, Senechal M, Brochu M, Dionne IJ. Relative strength as a determinant of mobility in elders 67–84 years of age. A nuage study: nutrition as a determinant of successful aging. J Nutr Health Aging. 2010;14(3):190–5.
Clark BC, Fernhall B, Ploutz-Snyder LL. Adaptations in human neuromuscular function following prolonged unweighting: I. Skeletal muscle contractile properties and applied ischemia efficacy. J Appl Physiol. 2006;101(1):256–63. doi:10.1152/japplphysiol.01402.2005.
Clark BC, Manini TM. Sarcopenia =/= dynapenia. J Gerontol A Biol Sci Med Sci. 2008;63(8):829–34.
Cohen-Solal M, Funck-Brentano T, Hay E. Animal models of osteoarthritis for the understanding of the bone contribution. Bonekey Rep. 2013;2:422. doi:10.1038/bonekey.2013.156.
Coiro V, Volpi R, Cataldo S, Magotti MG, Maffei ML, Giumelli C, Araldi A, Volpi L, Chiodera P. Effect of physiological exercise on osteocalcin levels in subjects with adrenal incidentaloma. J Endocrinol Invest. 2012;35(4):357–8.
Cooper A. A treatise on dislocations, and on fractures of the joints. Philadelphia: Lea and Blanchard; 1844.
Cosqueric G, Sebag A, Ducolombier C, Thomas C, Piette F, Weill-Engerer S. Sarcopenia is predictive of nosocomial infection in care of the elderly. Br J Nutr. 2006;96(5):895–901.
Cummings SR, Black DM, Nevitt MC, Browner W, Cauley J, Ensrud K, Genant HK, Palermo L, Scott J, Vogt TM. Bone density at various sites for prediction of hip fractures. The Study of Osteoporotic Fractures Research Group. Lancet. 1993;341(8837):72–5.
Depp CA, Jeste DV. Definitions and predictors of successful aging: a comprehensive review of larger quantitative studies. Am J Geriatr Psychiatry Off J Am Assoc Geriatric Psychiatry. 2006;14(1):6–20. doi:10.1097/01.JGP.0000192501.03069.bc.
Di Monaco M, Vallero F, Di Monaco R, Tappero R. Prevalence of sarcopenia and its association with osteoporosis in 313 older women following a hip fracture. Arch Gerontol Geriatr. 2011;52(1):71–4. doi:10.1016/j.archger.2010.02.002.
Ducy P, Desbois C, Boyce B, Pinero G, Story B, Dunstan C, Smith E, Bonadio J, Goldstein S, Gundberg C, Bradley A, Karsenty G. Increased bone formation in osteocalcin-deficient mice. Nature. 1996;382(6590):448–52.
Liu R, Schindeler A, Little DG. The potential role of muscle in bone repair. J Musculoskelet Neuronal Interact. 2010;10(1):71–6.
Schindeler A, Liu R, Little DG. The contribution of different cell lineages to bone repair: exploring a role for muscle stem cells. Differ Res Biol Divers. 2009;77(1):12–8. doi:10.1016/j.diff.2008.09.007.
Griffin XL, Costa ML, Parsons N, Smith N. Electromagnetic field stimulation for treating delayed union or non-union of long bone fractures in adults. Cochrane Database Syst Rev. 2011;4:CD008471. doi:10.1002/14651858.CD008471.pub2.
Leon-Salas WD, Rizk H, Mo C, Weisleder N, Brotto L, Abreu E, Brotto M. A dual mode pulsed electro-magnetic cell stimulator produces acceleration of myogenic differentiation. Recent Pat Biotechnol. 2013;7(1):71–81.
Elkasrawy M, Immel D, Wen X, Liu X, Liang LF, Hamrick MW. Immunolocalization of myostatin (GDF-8) following musculoskeletal injury and the effects of exogenous myostatin on muscle and bone healing. J Histochem Cytochem Off J Histochem Soc. 2012;60(1):22–30. doi:10.1369/0022155411425389.
Frost HM. Perspectives: a proposed general model of the “mechanostat” (suggestions from a new skeletal-biologic paradigm). Anat Rec. 1996;244(2):139–47. doi:10.1002/(SICI)1097-0185(199602)244:2<139::AID-AR1>3.0.CO;2-X.
Toledo FG, Goodpaster BH. The role of weight loss and exercise in correcting skeletal muscle mitochondrial abnormalities in obesity, diabetes and aging. Mol Cell Endocrinol. 2013;379(1–2):30–4. doi:10.1016/j.mce.2013.06.018.
Toledo FG, Menshikova EV, Ritov VB, Azuma K, Radikova Z, DeLany J, Kelley DE. Effects of physical activity and weight loss on skeletal muscle mitochondria and relationship with glucose control in type 2 diabetes. Diabetes. 2007;56(8):2142–7. doi:10.2337/db07-0141.
Yang J. Enhanced skeletal muscle for effective glucose homeostasis. Prog Mol Biol Transl Sci. 2014;121:133–63. doi:10.1016/B978-0-12-800101-1.00005-3.
Marotti G, Ferretti M, Muglia MA, Palumbo C, Palazzini S. A quantitative evaluation of osteoblast-osteocyte relationships on growing endosteal surface of rabbit tibiae. Bone. 1992;13(5):363–8.
Urist MR. Bone: formation by autoinduction. Science. 1965;150(3698):893–9.
Klein-Nulend J, Burger EH, Semeins CM, Raisz LG, Pilbeam CC. Pulsating fluid flow stimulates prostaglandin release and inducible prostaglandin G/H synthase mRNA expression in primary mouse bone cells. J Bone Miner Res Off J Am Soc Bone Miner Res. 1997;12(1):45–51. doi:10.1359/jbmr.1997.12.1.45.
Hartke JR, Lundy MW. Bone anabolic therapy with selective prostaglandin analogs. J Musculoskelet Neuronal Interact. 2001;2(1):25–31.
Mo C, Romero-Suarez S, Bonewald L, Johnson M, Brotto M. Prostaglandin E2: from clinical applications to its potential role in bone- muscle crosstalk and myogenic differentiation. Recent Pat Biotechnol. 2012;6(3):223–9.
Raisz LG. Prostaglandins and bone: physiology and pathophysiology. Osteoarthritis Cartilage/OARS Osteoarthritis Res Soc. 1999;7(4):419–21. doi:10.1053/joca.1998.0230.
Yoshida K, Oida H, Kobayashi T, Maruyama T, Tanaka M, Katayama T, Yamaguchi K, Segi E, Tsuboyama T, Matsushita M, Ito K, Ito Y, Sugimoto Y, Ushikubi F, Ohuchida S, Kondo K, Nakamura T, Narumiya S. Stimulation of bone formation and prevention of bone loss by prostaglandin E EP4 receptor activation. Proc Natl Acad Sci U S A. 2002;99(7):4580–5. doi:10.1073/pnas.062053399.
Winkler DG, Sutherland MK, Geoghegan JC, Yu C, Hayes T, Skonier JE, Shpektor D, Jonas M, Kovacevich BR, Staehling-Hampton K, Appleby M, Brunkow ME, Latham JA. Osteocyte control of bone formation via sclerostin, a novel BMP antagonist. EMBO J. 2003;22(23):6267–76. doi:10.1093/emboj/cdg599.
Shimada T, Kakitani M, Yamazaki Y, Hasegawa H, Takeuchi Y, Fujita T, Fukumoto S, Tomizuka K, Yamashita T. Targeted ablation of Fgf23 demonstrates an essential physiological role of FGF23 in phosphate and vitamin D metabolism. J Clin Invest. 2004;113(4):561–8. doi:10.1172/JCI19081.
Bonewald LF, Wacker MJ. FGF23 production by osteocytes. Pediatr Nephrol. 2013;28(4):563–8. doi:10.1007/s00467-012-2309-3.
Martin A, Liu S, David V, Li H, Karydis A, Feng JQ, Quarles LD. Bone proteins PHEX and DMP1 regulate fibroblastic growth factor Fgf23 expression in osteocytes through a common pathway involving FGF receptor (FGFR) signaling. FASEB J Off Publ Feder Am Soc Exp Biol. 2011;25(8):2551–62. doi:10.1096/fj.10-177816.
Karsenty G, Wagner EF. Reaching a genetic and molecular understanding of skeletal development. Dev Cell. 2002;2(4):389–406.
Lajeunesse D, Kiebzak GM, Frondoza C, Sacktor B. Regulation of osteocalcin secretion by human primary bone cells and by the human osteosarcoma cell line MG-63. Bone Miner. 1991;14(3):237–50.
Ducy P, Zhang R, Geoffroy V, Ridall AL, Karsenty G. Osf2/Cbfa1: a transcriptional activator of osteoblast differentiation. Cell. 1997;89(5):747–54.
Lee NK, Sowa H, Hinoi E, Ferron M, Ahn JD, Confavreux C, Dacquin R, Mee PJ, McKee MD, Jung DY, Zhang Z, Kim JK, Mauvais-Jarvis F, Ducy P, Karsenty G. Endocrine regulation of energy metabolism by the skeleton. Cell. 2007;130(3):456–69.
Nag AC, Foster JD. Myogenesis in adult mammalian skeletal muscle in vitro. J Anat. 1981;132(Pt 1):1–18.
Shefer G, Van de Mark DP, Richardson JB, Yablonka-Reuveni Z. Satellite-cell pool size does matter: defining the myogenic potency of aging skeletal muscle. Dev Biol. 2006;294(1):50–66. doi:10.1016/j.ydbio.2006.02.022.
Manring H, Abreu E, Brotto L, Weisleder N, Brotto M. Novel excitation- contraction coupling related genes reveal aspects of muscle weakness beyond atrophy – new hopes for treatment of musculoskeletal diseases. Front Physiol. 2014;5(37).
Pan Z, Brotto M, Ma J. Store-operated Ca2+ entry in muscle physiology and diseases. BMB Rep. 2014;47(2):69–79.
Rios E, Pizarro G, Stefani E. Charge movement and the nature of signal transduction in skeletal muscle excitation-contraction coupling. Annu Rev Physiol. 1992;54:109–33. doi:10.1146/annurev.ph.54.030192.000545.
Goldspink DF, Goldspink G. The role of passive stretch in retarding muscle atrophy. In: Nix WA, Vrbová G, editors. Electrical stimulation and neuromuscular disorders. Berlin Heidelberg: Springer; 1986. p. 91–100. doi:10.1007/978-3-642-71337-8_10.
Kurek JB, Bower JJ, Romanella M, Koentgen F, Murphy M, Austin L. The role of leukemia inhibitory factor in skeletal muscle regeneration. Muscle Nerve. 1997;20(7):815–22.
Pedersen BK, Febbraio MA. Muscle as an endocrine organ: focus on muscle-derived interleukin-6. Physiol Rev. 2008;88(4):1379–406. doi:10.1152/physrev.90100.2007.
Pedersen BK, Steensberg A, Fischer C, Keller C, Keller P, Plomgaard P, Febbraio M, Saltin B. Searching for the exercise factor: is IL-6 a candidate? J Muscle Res Cell Motil. 2003;24(2–3):113–9.
Li Y, Huard J. Differentiation of muscle-derived cells into myofibroblasts in injured skeletal muscle. Am J Pathol. 2002;161(3):895–907. doi:10.1016/S0002-9440(10)64250-2.
Pedersen L, Olsen CH, Pedersen BK, Hojman P. Muscle-derived expression of the chemokine CXCL1 attenuates diet-induced obesity and improves fatty acid oxidation in the muscle. Am J Physiol Endocrinol Metab. 2012;302(7):E831–40. doi:10.1152/ajpendo.00339.2011.
Seale P, Bjork B, Yang W, Kajimura S, Chin S, Kuang S, Scime A, Devarakonda S, Conroe HM, Erdjument-Bromage H, Tempst P, Rudnicki MA, Beier DR, Spiegelman BM. PRDM16 controls a brown fat/skeletal muscle switch. Nature. 2008;454(7207):961–7. doi:10.1038/nature07182.
Park KH, Zaichenko L, Brinkoetter M, Thakkar B, Sahin-Efe A, Joung KE, Tsoukas MA, Geladari EV, Huh JY, Dincer F, Davis CR, Crowell JA, Mantzoros CS. Circulating irisin in relation to insulin resistance and the metabolic syndrome. J Clin Endocrinol Metab. 2013;98(12):4899–907. doi:10.1210/jc.2013-2373.
Nielsen AR, Pedersen BK. The biological roles of exercise-induced cytokines: IL-6, IL-8, and IL-15. Appl Physiol Nutr Metab = Physiologie appliquee, nutrition et metabolisme. 2007;32(5):833–9. doi:10.1139/H07-054.
Pedersen BK, Akerstrom TC, Nielsen AR, Fischer CP. Role of myokines in exercise and metabolism. J Appl Physiol. 2007;103(3):1093–8. doi:10.1152/japplphysiol.00080.2007.
Matthews VB, Astrom MB, Chan MH, Bruce CR, Krabbe KS, Prelovsek O, Akerstrom T, Yfanti C, Broholm C, Mortensen OH, Penkowa M, Hojman P, Zankari A, Watt MJ, Bruunsgaard H, Pedersen BK, Febbraio MA. Brain-derived neurotrophic factor is produced by skeletal muscle cells in response to contraction and enhances fat oxidation via activation of AMP-activated protein kinase. Diabetologia. 2009;52(7):1409–18. doi:10.1007/s00125-009-1364-1.
Chan JK, Harry L, Williams G, Nanchahal J. Soft-tissue reconstruction of open fractures of the lower limb: muscle versus fasciocutaneous flaps. Plast Reconstr Surg. 2012;130(2):284e–95. doi:10.1097/PRS.0b013e3182589e63.
Joulia-Ekaza D, Cabello G. The myostatin gene: physiology and pharmacological relevance. Curr Opin Pharmacol. 2007;7(3):310–5. doi:10.1016/j.coph.2006.11.011.
Zimmers TA, Davies MV, Koniaris LG, Haynes P, Esquela AF, Tomkinson KN, McPherron AC, Wolfman NM, Lee SJ. Induction of cachexia in mice by systemically administered myostatin. Science. 2002;296(5572):1486–8. doi:10.1126/science.1069525.
Hamrick MW. Increased bone mineral density in the femora of GDF8 knockout mice. The Anatomical Record. 2003;272A(1):388–91. doi:10.1002/ar.a.10044.
Hamrick MW, McPherron AC, Lovejoy CO. Bone mineral content and density in the humerus of adult myostatin-deficient mice. Calcified Tissue International. 2002;71(1):63–8. doi:10.1007/s00223-001-1109-8.
Hamrick MW, Samaddar T, Pennington C, McCormick J. Increased muscle mass with myostatin deficiency improves gains in bone strength with exercise. Journal of Bone and Mineral Research. 2005;21(3):477–83. doi:10.1359/JBMR.051203.
Morissette MR, Stricker JC, Rosenberg MA, Buranasombati C, Levitan EB, Mittleman MA, Rosenzweig A. Effects of myostatin deletion in aging mice. Aging Cell. 2009;8(5):573–83. doi:10.1111/j.1474-9726.2009.00508.x.
Karsenty G, Ferron M. The contribution of bone to whole-organism physiology. Nature. 2012;481(7381):314–20. doi:10.1038/nature10763.
Morley JE, Baumgartner RN, Roubenoff R, Mayer J, Nair KS. Sarcopenia. J Lab Clin Med. 2001;137(4):231–43. doi:10.1067/mlc.2001.113504.
Karakelides H, Nair KS. Sarcopenia of aging and its metabolic impact. Curr Top Dev Biol. 2005;68:123–48. doi:10.1016/S0070-2153(05)68005-2.
Haber D. Health promotion and aging. 5th ed. New York: Springer Publishing Company; 2013.
Bloom DE, Canning D. Booms, busts, and echoes. International Monetary Fund. 2006. http://www.imf.org/external/pubs/ft/fandd/2006/09/bloom.htm. Accessed 3 43.
Hayutin A, Beals M, Borges E. The aging workforce: a Chartbook of demographic shifts. Stanford center of longevity. 2013. http://longevity3.stanford.edu/wp-content/uploads/2013/09/The_Aging_U.S.-Workforce.pdf.
Muravchick S. Preoperative assessment of the elderly patient. Anesthesiol Clin North America. 2000;18(1):71–89. vi.
Vos T, Flaxman AD, Naghavi M, Lozano R, Michaud C, Ezzati M, Shibuya K, Salomon JA, Abdalla S, Aboyans V, Abraham J, Ackerman I, Aggarwal R, Ahn SY, Ali MK, Alvarado M, Anderson HR, Anderson LM, Andrews KG, Atkinson C, Baddour LM, Bahalim AN, Barker-Collo S, Barrero LH, Bartels DH, Basanez MG, Baxter A, Bell ML, Benjamin EJ, Bennett D, Bernabe E, Bhalla K, Bhandari B, Bikbov B, Bin Abdulhak A, Birbeck G, Black JA, Blencowe H, Blore JD, Blyth F, Bolliger I, Bonaventure A, Boufous S, Bourne R, Boussinesq M, Braithwaite T, Brayne C, Bridgett L, Brooker S, Brooks P, Brugha TS, Bryan-Hancock C, Bucello C, Buchbinder R, Buckle G, Budke CM, Burch M, Burney P, Burstein R, Calabria B, Campbell B, Canter CE, Carabin H, Carapetis J, Carmona L, Cella C, Charlson F, Chen H, Cheng AT, Chou D, Chugh SS, Coffeng LE, Colan SD, Colquhoun S, Colson KE, Condon J, Connor MD, Cooper LT, Corriere M, Cortinovis M, de Vaccaro KC, Couser W, Cowie BC, Criqui MH, Cross M, Dabhadkar KC, Dahiya M, Dahodwala N, Damsere-Derry J, Danaei G, Davis A, De Leo D, Degenhardt L, Dellavalle R, Delossantos A, Denenberg J, Derrett S, Des Jarlais DC, Dharmaratne SD, Dherani M, Diaz-Torne C, Dolk H, Dorsey ER, Driscoll T, Duber H, Ebel B, Edmond K, Elbaz A, Ali SE, Erskine H, Erwin PJ, Espindola P, Ewoigbokhan SE, Farzadfar F, Feigin V, Felson DT, Ferrari A, Ferri CP, Fevre EM, Finucane MM, Flaxman S, Flood L, Foreman K, Forouzanfar MH, Fowkes FG, Franklin R, Fransen M, Freeman MK, Gabbe BJ, Gabriel SE, Gakidou E, Ganatra HA, Garcia B, Gaspari F, Gillum RF, Gmel G, Gosselin R, Grainger R, Groeger J, Guillemin F, Gunnell D, Gupta R, Haagsma J, Hagan H, Halasa YA, Hall W, Haring D, Haro JM, Harrison JE, Havmoeller R, Hay RJ, Higashi H, Hill C, Hoen B, Hoffman H, Hotez PJ, Hoy D, Huang JJ, Ibeanusi SE, Jacobsen KH, James SL, Jarvis D, Jasrasaria R, Jayaraman S, Johns N, Jonas JB, Karthikeyan G, Kassebaum N, Kawakami N, Keren A, Khoo JP, King CH, Knowlton LM, Kobusingye O, Koranteng A, Krishnamurthi R, Lalloo R, Laslett LL, Lathlean T, Leasher JL, Lee YY, Leigh J, Lim SS, Limb E, Lin JK, Lipnick M, Lipshultz SE, Liu W, Loane M, Ohno SL, Lyons R, Ma J, Mabweijano J, MacIntyre MF, Malekzadeh R, Mallinger L, Manivannan S, Marcenes W, March L, Margolis DJ, Marks GB, Marks R, Matsumori A, Matzopoulos R, Mayosi BM, McAnulty JH, McDermott MM, McGill N, McGrath J, Medina-Mora ME, Meltzer M, Mensah GA, Merriman TR, Meyer AC, Miglioli V, Miller M, Miller TR, Mitchell PB, Mocumbi AO, Moffitt TE, Mokdad AA, Monasta L, Montico M, Moradi-Lakeh M, Moran A, Morawska L, Mori R, Murdoch ME, Mwaniki MK, Naidoo K, Nair MN, Naldi L, Narayan KM, Nelson PK, Nelson RG, Nevitt MC, Newton CR, Nolte S, Norman P, Norman R, O’Donnell M, O’Hanlon S, Olives C, Omer SB, Ortblad K, Osborne R, Ozgediz D, Page A, Pahari B, Pandian JD, Rivero AP, Patten SB, Pearce N, Padilla RP, Perez-Ruiz F, Perico N, Pesudovs K, Phillips D, Phillips MR, Pierce K, Pion S, Polanczyk GV, Polinder S, Pope 3rd CA, Popova S, Porrini E, Pourmalek F, Prince M, Pullan RL, Ramaiah KD, Ranganathan D, Razavi H, Regan M, Rehm JT, Rein DB, Remuzzi G, Richardson K, Rivara FP, Roberts T, Robinson C, De Leon FR, Ronfani L, Room R, Rosenfeld LC, Rushton L, Sacco RL, Saha S, Sampson U, Sanchez-Riera L, Sanman E, Schwebel DC, Scott JG, Segui-Gomez M, Shahraz S, Shepard DS, Shin H, Shivakoti R, Singh D, Singh GM, Singh JA, Singleton J, Sleet DA, Sliwa K, Smith E, Smith JL, Stapelberg NJ, Steer A, Steiner T, Stolk WA, Stovner LJ, Sudfeld C, Syed S, Tamburlini G, Tavakkoli M, Taylor HR, Taylor JA, Taylor WJ, Thomas B, Thomson WM, Thurston GD, Tleyjeh IM, Tonelli M, Towbin JA, Truelsen T, Tsilimbaris MK, Ubeda C, Undurraga EA, van der Werf MJ, van Os J, Vavilala MS, Venketasubramanian N, Wang M, Wang W, Watt K, Weatherall DJ, Weinstock MA, Weintraub R, Weisskopf MG, Weissman MM, White RA, Whiteford H, Wiersma ST, Wilkinson JD, Williams HC, Williams SR, Witt E, Wolfe F, Woolf AD, Wulf S, Yeh PH, Zaidi AK, Zheng ZJ, Zonies D, Lopez AD, Murray CJ, AlMazroa MA, Memish ZA. Years lived with disability (YLDs) for 1160 sequelae of 289 diseases and injuries 1990–2010: a systematic analysis for the Global Burden of Disease Study 2010. Lancet. 2012;380(9859):2163–96. doi:10.1016/S0140-6736(12)61729-2.
McLaughlin SJ, Connell CM, Heeringa SG, Li LW, Roberts JS. Successful aging in the United States: prevalence estimates from a national sample of older adults. J Gerontol B Psychol Sci Soc Sci. 2010;65B(2):216–26. doi:10.1093/geronb/gbp101.
Wolff JL, Starfield B, Anderson G. Prevalence, expenditures, and complications of multiple chronic conditions in the elderly. Arch Intern Med. 2002;162(20):2269–76.
Wu SY, Green A. Projection of chronic illness prevalence and cost inflation. National Centers for Health Statistics. 2000. http://www.nationalhealthcouncil.org.
Rubenstein LZ, Josephson KR. Falls and their prevention in elderly people: what does the evidence show? Med Clin North Am. 2006;90(5):807–24. doi:10.1016/j.mcna.2006.05.013.
Auron-Gomez M, Michota F. Medical management of hip fracture. Clin Geriatr Med. 2008;24(4):701–719, ix. doi:10.1016/j.cger.2008.07.002.
Bradley SM. Falls in older adults. Mount Sinai J Med, New York. 2011;78(4):590–595. doi:10.1002/msj.20280.
Scott D, Blizzard L, Fell J, Jones G. The epidemiology of sarcopenia in community living older adults: what role does lifestyle play? J Cachex Sarcopenia Muscle. 2011;2(3):125–34. doi:10.1007/s13539-011-0036-4.
Walsh MC, Hunter GR, Livingstone MB. Sarcopenia in premenopausal and postmenopausal women with osteopenia, osteoporosis and normal bone mineral density. Osteoporos Int J Establ Result Cooper Between Eur Found Osteoporosional Osteoporos Found USA. 2006;17(1):61–7. doi:10.1007/s00198-005-1900-x.
Janssen I, Shepard DS, Katzmarzyk PT, Roubenoff R. The healthcare costs of sarcopenia in the United States. J Am Geriatr Soc. 2004;52(1):80–5.
Ray NF, Chan JK, Thamer M, Melton 3rd LJ. Medical expenditures for the treatment of osteoporotic fractures in the United States in 1995: report from the National Osteoporosis Foundation. J Bone Miner Res Off J Am Soc Bone Miner Res. 1997;12(1):24–35. doi:10.1359/jbmr.1997.12.1.24.
CDC. National Vital Statistics Report. 2013. http://www.cdc.gov/nchs/nvss.htm.
Zaki ME, Hussein FH, Banna RAE-SE. Osteoporosis among ancient Egyptians. Int J Osteoarchaeol. 2009;19(1):78–89. doi:10.1002/oa.978.
Schapira D, Schapira C. Osteoporosis: the evolution of a scientific term. Osteoporos Int J Establ Result Cooper Between Eur Found Osteoporose Natl Osteoporos Found USA. 1992;2(4):164–7.
WHO. Assessment of fracture risk and its application to screening for postmenopausal osteoporosis, WHO Technical Report Series, No. 843 edn. Geneve: World Health Organization; 1994.
Schwartz AV, Nevitt MC, Brown Jr BW, Kelsey JL. Increased falling as a risk factor for fracture among older women: the study of osteoporotic fractures. Am J Epidemiol. 2005;161(2):180–5. doi:10.1093/aje/kwi023.
Taylor BC, Schreiner PJ, Stone KL, Fink HA, Cummings SR, Nevitt MC, Bowman PJ, Ensrud KE. Long-term prediction of incident hip fracture risk in elderly white women: study of osteoporotic fractures. J Am Geriatr Soc. 2004;52(9):1479–86. doi:10.1111/j.1532-5415.2004.52410.x.
Vermeer C, Knapen MH, Schurgers LJ. Vitamin K and metabolic bone disease. J Clin Pathol. 1998;51(6):424–6.
Versluis RG, Papapoulos SE, de Bock GH, Zwinderman AH, Petri H, van de Ven CM, Springer MP. Clinical risk factors as predictors of postmenopausal osteoporosis in general practice. Br J Gen Pract J Royal Coll Gen Pract. 2001;51(471):806–10.
Body JJ, Bergmann P, Boonen S, Boutsen Y, Bruyere O, Devogelaer JP, Goemaere S, Hollevoet N, Kaufman JM, Milisen K, Rozenberg S, Reginster JY. Non-pharmacological management of osteoporosis: a consensus of the Belgian Bone Club. Osteoporos Int J Establ Result Cooper Between Eur Foundation for Osteoporos Natl Osteoporos Found USA. 2011;22(11):2769–88. doi:10.1007/s00198-011-1545-x.
Rizzoli R, Boonen S, Brandi ML, Burlet N, Delmas P, Reginster JY. The role of calcium and vitamin D in the management of osteoporosis. Bone. 2008;42(2):246–9. doi:10.1016/j.bone.2007.10.005.
Janssen I, Ross R. Linking age-related changes in skeletal muscle mass and composition with metabolism and disease. J Nutr Health Aging. 2005;9(6):408–19.
Rosemberg I. Summary comments: epidemiological and methodological problems in determining nutritional status of older persons. Am J Clin Nutr. 1989;50:1231–3.
Muhlethaler R, Stuck AE, Minder CE, Frey BM. The prognostic significance of protein-energy malnutrition in geriatric patients. Age Ageing. 1995;24(3):193–7.
Prothro JW, Rosenbloom CA. Body measurements of black and white elderly persons with emphasis on body composition. Gerontology. 1995;41(1):22–38.
Janssen I, Heymsfield SB, Ross R. Low relative skeletal muscle mass (sarcopenia) in older persons is associated with functional impairment and physical disability. J Am Geriatr Soc. 2002;50(5):889–96.
Newman AB, Kupelian V, Visser M, Simonsick E, Goodpaster B, Nevitt M, Kritchevsky SB, Tylavsky FA, Rubin SM, Harris TB, Health ABCSI. Sarcopenia: alternative definitions and associations with lower extremity function. J Am Geriatr Soc. 2003;51(11):1602–9.
Roubenoff R. Physical activity, inflammation, and muscle loss. Nutr Rev. 2007;65(12):S208–12.
Vandervoort AA, Symons TB. Functional and metabolic consequences of sarcopenia. Can J Appl Physiol. 2001;26(1):90–101.
Hughes VA, Frontera WR, Wood M, Evans WJ, Dallal GE, Roubenoff R, Fiatarone Singh MA. Longitudinal muscle strength changes in older adults: influence of muscle mass, physical activity, and health. J Gerontol A Biol Sci Med Sci. 2001;56(5):B209–17.
Mitchell WK, Williams J, Atherton P, Larvin M, Lund J, Narici M. Sarcopenia, dynapenia, and the impact of advancing age on human skeletal muscle size and strength; a quantitative review. Front Physiol. 2012;3:260. doi:10.3389/fphys.2012.00260.
Goodpaster BH, Park SW, Harris TB, Kritchevsky SB, Nevitt M, Schwartz AV, Simonsick EM, Tylavsky FA, Visser M, Newman AB. The loss of skeletal muscle strength, mass, and quality in older adults: the health, aging and body composition study. J Gerontol A Biol Sci Med Sci. 2006;61(10):1059–64.
Lang TF. The bone-muscle relationship in men and women. J Osteoporos. 2011;2011:702735. doi:10.4061/2011/702735.
Wang Q, Alen M, Nicholson P, Suominen H, Koistinen A, Kroger H, Cheng S. Weight-bearing, muscle loading and bone mineral accrual in pubertal girls–a 2-year longitudinal study. Bone. 2007;40(5):1196–202. doi:10.1016/j.bone.2006.12.054.
Zanchetta JR, Plotkin H, Alvarez Filgueira ML. Bone mass in children: normative values for the 2–20-year-old population. Bone. 1995;16(4 Suppl):393S–9.
McDonagh MJ, Hayward CM, Davies CT. Isometric training in human elbow flexor muscles. The effects on voluntary and electrically evoked forces. J Bone Joint Surg. 1983;65(3):355–8.
Baumgartner RN. Body composition in healthy aging. Ann N Y Acad Sci. 2000;904:437–48.
Roubenoff R, Hughes VA. Sarcopenia: current concepts. J Gerontol A Biol Sci Med Sci. 2000;55(12):M716–24.
Roubenoff R. Excess baggage: sarcopenia, obesity, and cancer outcomes. Lancet Oncol. 2008;9(7):605–7. doi:10.1016/S1470-2045(08)70160-8.
Schrager MA, Metter EJ, Simonsick E, Ble A, Bandinelli S, Lauretani F, Ferrucci L. Sarcopenic obesity and inflammation in the InCHIANTI study. J Appl Physiol. 2007;102(3):919–25. doi:10.1152/japplphysiol.00627.2006.
Baumgartner RN, Wayne SJ, Waters DL, Janssen I, Gallagher D, Morley JE. Sarcopenic obesity predicts instrumental activities of daily living disability in the elderly. Obes Res. 2004;12(12):1995–2004. doi:10.1038/oby.2004.250.
Lammes E, Akner G. Resting metabolic rate in elderly nursing home patients with multiple diagnoses. J Nutr Health Aging. 2006;10(4):263–70.
Bouchard DR, Janssen I. Dynapenic-obesity and physical function in older adults. J Gerontol A Biol Sci Med Sci. 2010;65(1):71–7. doi:10.1093/gerona/glp159.
Janssen I. Morbidity and mortality risk associated with an overweight BMI in older men and women. Obesity. 2007;15(7):1827–40. doi:10.1038/oby.2007.217.
Bouchard DR, Dionne IJ, Brochu M. Sarcopenic/obesity and physical capacity in older men and women: data from the Nutrition as a Determinant of Successful Aging (NuAge)-the Quebec longitudinal Study. Obesity. 2009;17(11):2082–8. doi:10.1038/oby.2009.109.
Walrand S, Guillet C, Salles J, Cano N, Boirie Y. Physiopathological mechanism of sarcopenia. Clin Geriatr Med. 2011;27(3):365–85. doi:10.1016/j.cger.2011.03.005.
Romero-Suarez S, Shen J, Brotto L, Hall T, Mo C, Valdivia HH, Andresen J, Wacker M, Nosek TM, Qu CK, Brotto M. Muscle-specific inositide phosphatase (MIP/MTMR14) is reduced with age and its loss accelerates skeletal muscle aging process by altering calcium homeostasis. Aging. 2010;2(8):504–13.
Srikanthan P, Hevener AL, Karlamangla AS. Sarcopenia exacerbates obesity-associated insulin resistance and dysglycemia: findings from the National Health and Nutrition Examination Survey III. PLoS One. 2010;5(5):e10805. doi:10.1371/journal.pone.0010805.
Kim TN, Park MS, Yang SJ, Yoo HJ, Kang HJ, Song W, Seo JA, Kim SG, Kim NH, Baik SH, Choi DS, Choi KM. Prevalence and determinant factors of sarcopenia in patients with type 2 diabetes: the Korean Sarcopenic Obesity Study (KSOS). Diabetes Care. 2010;33(7):1497–9. doi:10.2337/dc09-2310.
Magkos F, Wang X, Mittendorfer B. Metabolic actions of insulin in men and women. Nutrition. 2010;26(7–8):686–93. doi:10.1016/j.nut.2009.10.013.
Lee CG, Boyko EJ, Strotmeyer ES, Lewis CE, Cawthon PM, Hoffman AR, Everson-Rose SA, Barrett-Connor E, Orwoll ES, Osteoporotic Fractures in Men Study Research G. Association between insulin resistance and lean mass loss and fat mass gain in older men without diabetes mellitus. J Am Geriatr Soc. 2011;59(7):1217–24. doi:10.1111/j.1532-5415.2011.03472.x.
Hofbauer LC, Brueck CC, Singh SK, Dobnig H. Osteoporosis in patients with diabetes mellitus. J Bone Miner Res Off J Am Soc Bone Miner Res. 2007;22(9):1317–28. doi:10.1359/jbmr.070510.
Isaacson J, Brotto M. Physiology of Mechanotransduction: How Do Muscle and Bone “Talk” to One Another? Clinical Reviews in Bone and Mineral Metabolism. 2014;12(2):77–85.
Schweitzer R, Zelzer E, Volk T. Connecting muscles to tendons: tendons and musculoskeletal development in flies and vertebrates. Development. 2010;137(17):2807–17. doi:10.1242/dev.047498.
Pineault KM, Wellik DM. Hox genes and limb musculoskeletal development. Curr Osteoporos Rep. 2014;12(4):420–7. doi:10.1007/s11914-014-0241-0.
Blitz E, Viukov S, Sharir A, Shwartz Y, Galloway JL, Pryce BA, Johnson RL, Tabin CJ, Schweitzer R, Zelzer E. Bone ridge patterning during musculoskeletal assembly is mediated through SCX regulation of Bmp4 at the tendon-skeleton junction. Dev Cell. 2009;17(6):861–73. doi:10.1016/j.devcel.2009.10.010.
Edom-Vovard F, Duprez D. Signals regulating tendon formation during chick embryonic development. Dev Dyn Off Publ Am Assoc Anat. 2004;229(3):449–57. doi:10.1002/dvdy.10481.
Edom-Vovard F, Schuler B, Bonnin MA, Teillet MA, Duprez D. Fgf4 positively regulates scleraxis and tenascin expression in chick limb tendons. Dev Biol. 2002;247(2):351–66.
Rodriguez-Guzman M, Montero JA, Santesteban E, Ganan Y, Macias D, Hurle JM. Tendon-muscle crosstalk controls muscle bellies morphogenesis, which is mediated by cell death and retinoic acid signaling. Dev Biol. 2007;302(1):267–80. doi:10.1016/j.ydbio.2006.09.034.
Findlay DM, Atkins GJ. Osteoblast-chondrocyte interactions in osteoarthritis. Curr Osteoporos Rep. 2014;12(1):127–34. doi:10.1007/s11914-014-0192-5.
Funck-Brentano T, Cohen-Solal M. Crosstalk between cartilage and bone: when bone cytokines matter. Cytokine Growth Factor Rev. 2011;22(2):91–7. doi:10.1016/j.cytogfr.2011.04.003.
Pan J, Zhou X, Li W, Novotny JE, Doty SB, Wang L. In situ measurement of transport between subchondral bone and articular cartilage. J Orthop Res Off Publ Orthop Res Soc. 2009;27(10):1347–52. doi:10.1002/jor.20883.
Yuan XL, Meng HY, Wang YC, Peng J, Guo QY, Wang AY, Lu SB. Bone-cartilage interface crosstalk in osteoarthritis: potential pathways and future therapeutic strategies. Osteoarthritis Cartilage/OARS Osteoarthritis Res Soc. 2014;22(8):1077–89. doi:10.1016/j.joca.2014.05.023.
Tat SK, Lajeunesse D, Pelletier J-P, Martel-Pelletier J. Targeting subchondral bone for treating osteoarthritis: what is the evidence? Best Pract Res Clin Rheumatol. 2010;24:51–70.
Loppini M, Maffulli N. Conservative management of tendinopathy: an evidence-based approach. Muscles Ligaments Tendons J. 2011;1(4):134–7.
Heinemeier KM, Olesen JL, Haddad F, Langberg H, Kjaer M, Baldwin KM, Schjerling P. Expression of collagen and related growth factors in rat tendon and skeletal muscle in response to specific contraction types. J Physiol. 2007;582(Pt 3):1303–16. doi:10.1113/jphysiol.2007.127639.
Rizzuto E, Musaro A, Catizone A, Del Prete Z. Measuring tendon properties in mdx mice: cell viability and viscoelastic characteristics. J Biomech. 2009;42(14):2243–8. doi:10.1016/j.jbiomech.2009.06.041.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2016 Springer International Publishing Switzerland
About this chapter
Cite this chapter
Brotto, M., Isaacson, J., Abreu, E.L. (2016). The Muscle-Bone Connection. In: Duque, G., Kiel, D. (eds) Osteoporosis in Older Persons. Springer, Cham. https://doi.org/10.1007/978-3-319-25976-5_4
Download citation
DOI: https://doi.org/10.1007/978-3-319-25976-5_4
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-319-25974-1
Online ISBN: 978-3-319-25976-5
eBook Packages: MedicineMedicine (R0)