Abstract
Several areas of medicine, mainly in surgical areas such as orthopedics are using the additive manufacturing of anatomical models and personalized implants, thus allowing accurate preoperative planning, simulation of surgeries with team training, and better communication with the patient. The first and most important step in printing objects is the acquisition of the image. Usually, it uses medical imaging such as Computer Tomography (CT), Magnetic Resonance Image (MRI), and Ultrasonography (US) in a DICOM format file. During the processing image (modeling and rendering), the 3D object is exported to the Computer-Aided Design (CAD) environment to perform the Virtual Surgical Planning (VSP). CAD programs allow us to visualize and analyze the regions with complex anatomy and simulate surgery. To perform the printing of 3D models is necessary the Computer-Aided Manufacturing (CAM) environment software for generating GCode (machine language of the printers). The Computer-Aided Engineering (CAE) software is an important resource that 3D virtual model volumes (anatomical model and implant) may be discretized and analyzed by simulation in silico using the finite elements method (FEM). According to the literature, the use of 3D printing technology in orthopedic surgery has four important areas: (1) Anatomical model printing (including medical education, pre-operative planning, and pre-operative simulation). (2) Tools, Guides, and Surgical Templates printing. (3) Implants, Prostheses, and Orthoses printing. (4) Scaffolds and Cell printing. The impact of 3D printing technology in orthopedics is rising and leaving definitive changes in the development of customized implants and surgical processes improvement.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
1 Introduction
Several areas of medicine, mainly in the surgical field such as orthopedics are using the additive manufacturing (AM) of anatomical models and personalized implants, thus allowing accurate preoperative planning, simulation of surgeries with team training, and better communication with the patient (Zheng et al. 2018a, b; Rankin et al. 2018).
The features of the 3D printing technology currently used in orthopedic surgeries allow the printing of anatomical models precisely reproducing the anatomy of the patients. These can improve the understanding of the surgeon about anatomy and fracture deviations, and in some cases, it helps to make a correct diagnostic interpretation, where it was not apparent in medical images. Besides, it helps to understand the anatomical relationships of structures and geometry of regions with complex anatomy, facilitating accurate preoperative planning. These models assist in the training of surgeons in areas of complex anatomy such as the pelvis, spine, and joint regions.
Virtual 3D planning allows the surgeon to better visualize and understand the full three-dimensional anatomy and to digitally plan, e.g., a corrective osteotomy to restore anatomy and normal function or allow better implant positioning. This planning is based on computed tomography (CT) images of the patient, in which various surgical approaches are considered. 3D planning has the potential to increase the accuracy of preoperative planning, increase the accuracy of surgical navigation, decrease postoperative complications, obtain a more economical use of operating rooms, and improve patient satisfaction. To this end, Patient-Specific surgical guides are designed to control the cut and reduction according to the surgical plan, aiming to improve the predictability of osteotomy and fracture treatment procedures (Vaishya et al. 2018; Bagaria and Chaudhary 2017).
Three-dimensional printing allows the use of personalized 3D printed tools and guides for performing osteotomies with precise implant placement to optimize surgical results. Implants, cut and drill guides, orthoses and personalized prostheses can be created according to the individualized anatomy of each patient (Vaishya et al. 2018).
In complex osteotomies and arthroplasties, the production of 3D models helps in planning the surgical procedure. It goes beyond the three-dimensional images usually reconstructed from CT and allows the surgeon to study the problem, not only seeing it in two dimensions but keeping it in his hand, ensuring a 3D perspective in real size.
The main advantages are the ability to assess bone defects, evaluate fracture patterns, guarantee the accuracy of the position of the implants and prosthesis. The printed biomodel offers the opportunity to plan the necessary instrumentation and customized implants, thus optimizing surgery. Surgeons can simulate the procedure and, if necessary, build templates, cutting and drilling guides, and personalized perforations based on the disease, anatomy, and surgeon's preferences (Bagaria and Chaudhary 2017).
The use of 3D technology in orthopedic trauma allows Virtual Surgical Planning (VSP) to provide the reduction of fragments, the choice of implants according to bone geometry. This allows the anatomical model to be printed on a full scale for a better understanding of the anatomy, performing surgical simulation with due training of the team and verification of the pre-selected implants with the possibility of preoperative modeling (bending) of these implants, as in cases where plate and screws are used, adapting the best local bone surface. Also, in orthopedic trauma surgeries, it is possible to use a 3D printing technique to print a mirror image of the bone on the unaffected side in real size (similar to the affected side) to use it in the preoperative for refinement of surgical planning and simulation and in the intraoperative approach to reference the anatomical fracture reduction (Zhang et al. 2017a, b).
2 Medical Images
2.1 Image Acquisition
The first and most important step in printing objects is the acquisition of images (Shui et al. 2017; Wong et al. 2017; Eijnateen et al. 2018). The quality of the printed model depends on the quality of the processed data (resolution of the images). Therefore, low-resolution images will result in inappropriate models and distortions in the printed object (Marro et al. 2016; Mok et al. 2016; Martelli et al. 2016; Green et al. 2016).
Bone tissue has a high contrast compared to soft tissue in CT images, which makes this type of exam the most indicated for the acquisition of data for 3D modeling (Wong et al. 2017). There is no consensus in the literature on which would be an ideal protocol for image acquisition, mainly from CT images for use in Rapid Prototyping (RP) of 3D anatomical models. Some important parameters in the acquisition of CT images were described in the literature (Eijnatten et al. 2018). Bagaria and Chaudhary (2017) in their study suggest a protocol of parameters for the CT image acquisition used in the printing of anatomical bone models (Table 14.1).
Some studies show that the width of the slices of the images CT scan also influences the quality of volumetric reconstruction of the image being one of the main limiting factors for the quality of prototyping in the medical field (Rankin et al. 2018; Eijnatten et al. 2018; Marro et al. 2016). The slices should be 0.5–2 mm depending on the anatomical region. Anatomical models of the face should have slices with 0.5–1 mm of width as models of long bones, and the pelvis can be sliced up to 2 mm according to Marro et al. (2016). Slices above 2 mm can generate distortions during volumetric reconstruction and printing of objects. Most appliances CT is limited to a slice width of at least 0.625 mm although many 3D printer companies specify a resolution of minus 0.1 mm for their machines (Eley 2017). The ROI must be established for the segmentation, to decrease the work of extracting parts that will not be useful for printing (Shui et al. 2017).
The data acquired (images) on CT scan are processed in software observing a set of standards for the treatment, storage, and transmission of information in an electronic format, structuring a protocol known as the Digital Image Communication in Medicine (DICOM format) (Shui et al. 2017; Eijnatten et al. 2018; Marro et al. 2016; Mulford et al. 2016). This format was created in the 80 s to standardize the formatting of diagnostic images such as CT, Magnetic Resonance Images (MRI), and Ultrasonography (US) used in the Picture Archiving and Communications System (PACS), a system for storing and exchanging information generated by medical equipment. The DICOM standard has a series of rules that allow medical data and information associated with images to be exchanged with diagnostic equipment that generates images and between the different equipment from different developers.
Image acquisition can be carried out by direct scanning in 3D volume. The scanned images can be exported already in the format of the STL file e.g., to be print (Li et al. 2017).
2.1.1 Computed Tomography
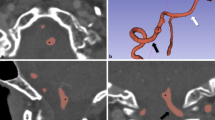
Currently, the CT data are the most used medical images in the creation of 3D anatomical models and virtual surgical simulations. Bone tissues have a high contrast compared to soft tissues in CT images, which makes this type of exam the most suitable for the acquisition of data for 3D modeling (Wong et al. 2017) (Fig. 14.1). Van den Broeck et al. (2014) conducted a study whose objective was to quantify errors in absolute dimensions between models reconstructed from CT images and MRI compared to the true model for several bone regions.
3D model images of the tibia were created from segmented CT and MRI images and compared to optical scans of real bones (considered standard). 3D reconstruction using CT images resulted in an error of 0.55 mm, corresponding to an overestimated bone model of CT compared to the real bone. The MRI resulted in an error of 0.56 mm; however, the bone model of MRI was, on average, a small underestimation in comparison with the real bone. Different regions of the bones were analyzed, indicating a difference in accuracy between the diaphysis and the epiphysis. This study shows high accuracy for CT and MRI images, supporting the feasibility of using technology imaging for 3D bone reconstruction in medical applications (Van den Broeck et al. 2014).
2.1.2 Magnetic Resonance Imaging
The most important aid of the MRI is to show the soft tissue in orthopedics images. Eley et al. (2014) and (2017) described the “Black Bone” MRI and concluded that segmentation of the “Black Bone” MRI datasets was successful with both threshold and volume rendering techniques, demonstrating considerable clinical potential as a non-ionizing alternative to CT.
According to Parthasarathy et al. (2020), bone structures require the “black bone” MRI technique for accurate evaluation. The black bone MRI technique uses a gradient echo. These authors showed that the 3D-created model from MRI with 1 mm slice acquisition is more accurate than the one created from the acquisition of 3 mm slices. The black bone sequence normally is not a routine protocol in MRI acquisition, and its specific requisition is necessary.
2.2 Processing and Postprocessing Images
2.2.1 Denoising
If the images show random noise (especially if there are metallic implants), noise cleaning should be performed to avoid artifacts in CAD models. So, the first step is the sequential reduction of the data acquired by CT. The smoothing method, which is a computer algorithm, can be used to reduce noise without losing important details and anatomical information (Bagaria and Chaudhary 2017; Green et al. 2016).
2.2.2 Segmentation
Segmentation is a process of separating an unwanted area from the desired area, that is, the region of interest (ROI) for future image processing (Bagaria and Chaudhary 2017; Shui et al. 2017; Marro et al. 2016; Green et al. 2016). The separation of the parts depends on the anatomical area and the chosen tissue to be studied (bone, muscle, vascular blood, etc.). For proper segmentation to take place, the threshold of attenuation (density) of the tissue must be chosen (Rankin et al. 2018). This is defined according to the scale of Hounsfield (HU) which is a transformation of the original measure of the coefficient of linear attenuation for a dimensionless scale in X-Ray and CT images. The Hounsfield scale is related to obtaining images from ionizing radiation like X-rays. It transforms the different shades of gray, acquired in imaging with ionizing radiation (e.g., X-ray), into numerical values.
This transformation makes it possible to open windows within the grayscale obtained in the images, allowing greater differentiation between previously very similar colors (and often indistinguishable to the human eye). Visually, the air is identified as completely black area, the water as gray, and the bone as white. On that scale, the radiodensity of distilled water under standard temperature conditions and pressure is defined as zero (0) Hounsfield unit (HU), while air radiodensity in normal temperature and pressure conditions is defined as −1000 HU. The scale is commonly used between −1000 HU and 3000 HU. Some authors consider that cortical bone is reported to exhibit HU values around 150–1800. These values depend on the sex, age, and health of the bone tissue (Green et al. 2016). The segmentation can be performed manually or through algorithms created for this purpose (Chen et al. 2016). Besides this, bone segmentation can be performed using an automatic algorithm program or manually identifying bone tissue in the thresholding window using the HU. Usually, the software creates a mask to identify the segmented tissue (Fig. 14.2).
Screen image of the Invesalius v3.1.1 software showing the bone segmentation. After the segmentation process, it was created a mask that appear in green. The automatic segmentation of the bone was performed using an algorithm with the Hounsfield´s scale of 226–2014. In the same image the 3D object created from the DICOM data is shown
According to Eijnatten et al. (2018), threshold determination (thresholding) continues to be the most widely used segmentation method in the manufacture of 3D prints in the medical field. The manual threshold determination is still the best method for transforming the volume reconstruction in STL files (the most used format for manipulating 3D images) according to Rankin et al. (2018).
Van Eijnatten considers this as the most critical and most in-demand phase in the 3D printing process since the generation of low-resolution 3D images can generate low accuracy object printing (Eijnatten et al. 2018). Similarly, the segmentation and mesh generation process can generate significant accuracy between the original DICOM data, and the 3D model generated. It is important to compare the processed data from the area interest with the original images in DICOM format, at each stage to ensure that it remains a true anatomical representation according to Marro et al. (2016). Some software used to perform the segmentation of CT images are OsiriX, Horos, Invesalius and 3D Slicer.
2.2.2.1 3D File Formats
After segmentation, the surface is extracted from the volumetric data converting the voxel data into a mesh formed of a series of triangular facets (Marro et al. 2016). That is, there is a conversion of 2D images into 3D images, for the possibility of editing the three-dimensional object (Eijnatten et al. 2018; Eley 2017). At this moment, there is a three-dimensional reconstruction of the images. Currently, the most commonly used file format in medical 3D printing is Stereolithography File (with .STL extension) (Eijnatten et al. 2018). In this format, the object can be manipulated, and the necessary adjustments can be made allowing geometry editing for printing. The process of converting files in DICOM format to 3D volumetric tests templates is one of the biggest causes of inaccurate production of AM in the medical field, according to Van Eijnatten et al. (2018).
There are many types of 3D file formats to perform modeling and rendering besides STL format e.g., Additive Manufacturing File (with the .AMF extension), Wavefront 3D Object File (with the .OBJ extension), and 3D Manufacturing File (with the 0.3MF extension).
3 Computer-Aided Design (CAD)
3.1 Postprocessing Images—Modeling and Rendering
The selected volume in a 3D file format is then processed to remove unwanted parts and to improve the smoothness of the surface of the object, to make the object as close to the real situation. For this purpose, software with CAD technology is normally used. The most used programs for rendering 3D virtual objects are Mimics, Magics, Meshmixer, Meshlab, Rhinoceros 3D, Blender, and Catia. The use of these CAD software allows the rendering of the virtual bone model with the correction of imperfections and irregularities of the surface and the proper separation of the bone fragments for virtual surgery. The more accurate the segmentation, less distortion or imperfections of the object is generated with less need to correct surface irregularities in the rendering and modeling of the virtual object (Fig. 14.3).
After segmentation and modeling using the data processed within the creation of the 3D object (e.g., virtual bone model) it is possible performing surgical planning, carrying out the study of the spatial geometry of the site (anatomy), performing virtual surgery with resection of parts (e.g., in oncologic surgery), implant placement simulation (e.g., implants and prostheses) (Chen et al. 2016) and repositioning/reduction of fracture fragments (Fig. 14.4).
3.1.1 Mesh Generation
Due to the complexity of geometry and CT resolution, it is necessary to form a mesh to define the places where there are gaps so that they would be corrected with image editing methods, making the surface of the object as smooth as possible (Bagaria and Chaudhary 2017) (Fig. 14.5). The figure shows a screen image of the Meshmixer v3.5 software where a mesh was created to better understand the irregularities and flaws on the surface of the object and to facilitate the later correction of these flaws.
3.1.2 Cleaning
It is often necessary to remove artifacts that make the object irregular and with deformations on the surface created after the segmentation. Other kinds of artifacts are bridges between near surfaces and components. (e.g., connections across the joint or gap fracture) (Green et al. 2016). Some artifacts are due to metallic materials implanted on the patient’s body. The spatial smoothing method normally used is an algorithm to reduce these artifacts without losing anatomical information (Bagaria and Chaudhary 2017).
3.1.3 Smoothening
Smoothing is the process of making the surface of the object more regular and natural while trying to maintain the original geometry. Manual image smoothing and smoothing algorithms are used to improve the definition and quality of the 3D image to be printed (Bagaria and Chaudhary 2017; Favier et al. 2017). In many cases, there is a need to smooth the surface of the 3D object before printing or during the creation of cut and drilling guides and surgical simulation.
3.2 Virtual Surgical Planning (VSP)
Kim et al. (2018) in their study reports the clinical experience with the use of 3D printing techniques in orthopedic trauma, with the following applications:
-
1.
A better understanding of the fracture and anatomical relationships;
-
2.
Preoperative planning;
-
3.
Medical education;
-
4.
Training and surgical simulation.
Preoperative analysis can currently be one of the most common and important applications of useful 3D printing technology. Surgical procedures in areas of complex anatomy with a high damage risk to noble structures (vessels blood and nerves) benefit from rapid prototyping (Rankin et al. 2018). Several CAD software showed before in 14.3.1 item currently allow the performing of VSP with a better understanding of spatial geometry, anatomical relationships mainly in places of complex anatomy, and the possibility of programming less invasive surgical procedures and in the case of orthopedic trauma surgery, and the previous reduction of bone fragments simulating definitive osteosynthesis (Fadero and Shah 2014; Frizziero et al. 2021; Tappa et al. 2019) (Fig. 14.6). The figure depicts the reduction and fracture nonunion fixation with plate and screws. During VSP, it is possible to choose the best position for the implants in lateral surface of femoral condyle.
3.3 Orthopedic Implant Designing
Additive Manufacturing has great potential for customized implants in the orthopedic application. The fabrication of Patient-Specific Implants (PSI) is the most feasible example of this technology. The implants such as plates and screws, nails, prosthesis (conventional or unconventional), and endoprosthesis made with 3D printing technology are called PSI since they are personalized (custom made), and they can be used in traumatic situations, in bone loss treatment, or replacement joints in orthopedic surgeries (Tappa et al. 2019; Belvedere et al. 2019; Rathor et al. 2021). For modeling, 3D constructs (implants or prothesis) are necessary to use specific CAD software to design the project accurately. In a CAD environment is it possible to make changes and adjusting the design and make sure about the adaptation of implant or prosthesis to bone geometry (Yan et al. 2020).
The use of PSI technology is an important tool to solve complex bone destructions that require bone loss treatment in severe fractures and oncological bone resection (Tetsworth et al. 2017; Wong et al. 2015). To design PSI in orthopedics these are the currently used software e.g., SolidWorks, Creo Parametric, Autodesk Fusion 360, Autodesk Inventor, Materialise Magics. Figure 14.7 is showing an image of customized implant design (plate) using the CAE software SolidWorks.
4 Computer-Aided Engineering (CAE)
The CAE software is an important resource that 3D virtual model volumes may be discretized and analyzed by simulation in silico using the finite elements method (FEM). It is possible to perform the static and dynamic analysis, measure the forces acting in the bone, in the implant, and the bone-implant interface. Thus, it is feasible to measure the stress forces (compression and distraction) and material strain of all-system bone-implant. This kind of analysis is important to define the best mechanical and geometrical characteristics of the 3D printed personalized implant.
4.1 Finite Element Analysis (FEA)
The numerical solutions to solve structural mechanical problems are important resources in biomechanics mainly in orthopedic implant projects. Due to the advances in biomechanical studies using CAE technology, it is possible to reach a high level in correlations between computational tests and experimental mechanical assay arriving at 95% (Wieding et al. 2012). An important advantage of Finite Element Analysis (FEA) is that it can analyze the complex geometry of the model and obtain detailed data from the 3D model. During the computational simulation of the project, it is possible to measure the strain levels during different loading conditions analyzed using the FEA. This kind of analysis helps designing orthopedic implants with more mechanical effectiveness and with more accurate anatomical design (Rathor et al. 2021; Yan et al. 2020).
Some software used to perform the FEA in the orthopedics area are SolidWorks, Altair Hypermesh, Abaqus, and Ansys. Figure 14.8 is showing the FEA using the CAE software (Ansys 16.0) to analyze deformation and loads that act in the bone-implant system. During FEA performing it is possible better understanding the osteosynthesis mechanical behave. This analysis showed that the chosen implant demonstrated mechanical resistance to promote bone healing.
Images showing the FEA using the CAE software (Ansys 16.0) to analyze deformation and loads that act in the bone-implant system. During FEA performing it is possible better understanding the osteosynthesis mechanical behave. This analysis showed that the chosen implant demonstrated mechanical resistance to promote bone healing
5 Computer-Aided Manufacturing (CAM)
The bone model created through the acquisition and segmentation methods must be suitable for printing while maintaining the characteristics and dimensions of the real object. Usually, files in the STL and AMF format are then loaded into the slicing that prepares the file for printing by converting it to GCode, numerical control programming language, a universal code to send position, and extrude commands to 3D printers (Rankin et al. 2018). The printing of 3D objects of complex shapes can require different characteristics of solidity and porosity (Mulford et al. 2016).
The most used CAM environment software for generating GCode and printing 3D models with FDM technology in desktop printers are Makerbot Desktop, Cura, Slic3r, Repetier-Host.
5.1 Printing Technologies
5.1.1 Fused Deposition Modeling (FDM)
The FDM uses the technique of layered deposition of a polymer heated through an extruder nozzle, layer by layer (Hoang et al. 2016), which immediately hardens after extrusion to form solid layers, making three-dimensional objects with geometric high definition. A filament of material normally thermoplastic or metal wire feeds the nozzle head extruder that heats the filament and expels it, turning it off and on, forming the successive layers (Bagaria et al. 2018).
This technique requires support for the printing of the structures (Marro et al. 2016). Print speed is low, and the print resolution is lower than the SLS technique (Wong et al. 2017; Malik et al. 2015). With FDM technology, it is necessary to consider the small amount of shrinkage that occurs with plastics when they cool to room temperature, around 0.5%, which can be surpassed by the preventive dimensioning of the model (Eley 2017). In this technique, the layer width can be up to 7 µm with an X/Y resolution of up to 2.8 µm (Hoang et al. 2016).
Currently, the most widespread use of the FDM technique in orthopedic surgeries is anatomical models (Marro et al. 2016) as depicted in Fig. 14.9. The figure presents an images of the 3D printed bone model with FDM technology in white ABS, distal femur and fragment of the lateral femoral condyle.
The main advantages of FDM for printing biomaterials with making scaffolds are high porosity due to the deposition pattern and good mechanical resistance. A challenge for FDM is the limitation for thermoplastic materials with good melt viscosity properties that have high enough viscosity to build, but low enough for extrusion (Chia and Wu 2015). The materials used in this technique are Acrylonitrile Butadiene Styrene (ABS), Polylactic Acid (PLA), Polyamide, Polycarbonate, Polypropylene, Polyester, and some types of waxes (Hoang et al. 2016).
5.1.2 Lithography-Based 3D Printing
This technique is known as vat photopolymerization technology and has three main types: Stereolithography (SLA), Digital Light Processing (DLP), and Continuous Digital Light Processing/Continuous Liquid Interface Production (CDLP/CLIP) (Pagac et al. 2021).
The SLA is a fast and very accurate technique for manufacturing 3D objects by which a computer controls a beam of ultraviolet (UV) laser for the polymerization of liquid resin from the surface to the depth forming successive layers. The polymer is contained in a container whose movement of descension, or ascension is controlled by the program printing. The photopolymer is transformed into semi-solid with heat and then it hardens (“cure”). The entire process uses the triangulated UV laser on the surface using scanning mirrors on the X and Y axis (Bagaria et al. 2018). The kinetics of the healing reactions that occur during polymerization is critical. This affects the curing time and the polymerized layer width. The kinetics can be controlled by the power of the light source, the scanning speed, and the chemistry and quantity of the monomer. Also, UV absorbers can be added to the resin to control the depth of polymerization (Chia and Wu 2015). In this technique, the width of the layer can be up to 2 µm with an X/Y resolution of up to 4 µm (Hoang et al. 2016).
The printing materials most used in resin 3D printing techniques are limited to photopolymers such as Epox and acrylic resins, which can have a high cost (Marro et al. 2016). In the DLP technique, a digital light projector is used to cure the resin, flashing images of whole layers onto the bottom of the tank. A digital light projector is used instead of a mirror to reflect a laser source used in SLA technology to cure the resin. The printing accuracy depends on projector resolution (Pagac et al. 2021).
The CDLP/CLIP technology flashes complete layers at the resin tank, employing digital projection from LEDs. Due to continuous movement of the build platform, is possible to print undisrupted prototype with high speed.
The advantages of the resin 3D printing technique are the ability to create complex shapes with internal architecture (with tubular shapes, lattices). It is possible to easily remove unpolymerized resin and obtain extremely high resolution and highly accurate models with smooth surface finishes. The main disadvantage of the 3D printing technique is the scarcity of biocompatible resins with suitable SLA, DLP, and CDLP/CLIP processing properties (Chia and Wu 2015). In the case of the DLP technique “zoomed out” effect (low accuracy printing process to print big objects) can occur.
The DLP and CDLP/CLIP techniques benefit compared to SLA is building speed, because the entire layer is flashed at once in this technology, instead of a single point in SLA technology. Currently, using this kind of technology is being used in researches in 3D bioprinting and bioinks for bone repair and regeneration (Liang et al. 2021; Luo et al. 2020).
5.1.3 Selective Laser Sintering (SLS)/Selective Laser Melting (SLM)
The SLS uses a high-quality CO2 laser power to sinter a thin layer of powder particles into layers to form the model. The laser draws the shape of the desired object merging it with the layer below; successively layers of the powder are spread over the previous ones, covering them after the laser action on each layer. It can be used to create an extremely precise representation because the precision is limited only by the laser, the powder fineness/granulation of the raw material, and layer thickness. The most used materials are thermoplastics (polycarbonate, polyamide, nylon), metals, glass, or ceramics (Hoang et al. 2016). Selective laser fusion, also known as SLM, is a subtype of SLS being used mainly for printing metals and implant manufacturing. Both SLS and SLM have high resolution and high cost (Hoang et al. 2016; Bagaria et al. 2018).
An advantage of SLS and SLM over other processes of 3D printing is that they do not require support structures during the printing of the models because the objects are supported on the powder. With other printers, support structures are sometimes necessary to prevent the model from collapsing in weak spots. These support structures can be removed manually after the model has been printed. In the SLS and SLM process, they usually leave a rough surface that may require polishing. The surface finish with SLS can be difficult, requiring more post-processing than other methods (Marro et al. 2016).
The SLM and Direct Metal Laser Sintering (DMLS) are the most popular 3D metal printing technologies. Both use a laser to scan and then selectively melt the metal dust particles that bond to each other in layers. The main difference between the two technologies is the ability to print different materials. Both techniques have less than 5% waste of raw material. Although SLM can print just a single metal, DMLS allows printing multiple alloys, just like powder with variable melting points can also fuse at the molecular level in this specific technology. The height of the layer for printing a 3D metal object varies between 20 and 50 µm and depends on the properties of the raw material, such as flow capacity, particle size, shape, and distribution. Modern metal printing standards have an accuracy of less than 100 µm, making them ideal for printing orthopedic implants that need high precision (Bagaria et al. 2018). According to Hoang, in the SLS technique, the layer width can be up to 4–6 µm with X/Y resolution of up to 30–50 µm, while using the DLMS technique layer width can be up to 0.8–1.2 µm with X/Y resolution of up to 12–16 µm (Hoang et al. 2016).
Chia and Wu (2015) in their review of advances in the use of biomaterials in 3D printing reported the use of non-metallic materials printed with the SLS technique such as previously coated ceramic thermoplastics, a mixture of polyvinyl alcohol (PVA) with hydroxyapatite (HA) and polyetheretherketone (PEEK) used for making personalized implants. In these techniques, it is possible to reuse the powder that has been used before, and it is necessary to process it again to allow a new use.
5.1.4 Electron Beam Melting (EBM)
A similar process to SLS is the EBM. In this process, what melts the dust is a laser electron beam, powered by high voltage, typically 30–60 kV. The process takes place in a high vacuum to avoid oxidation problems, as it is intended for the construction of high-precision metal parts. Other than that, the process is very similar to SLS. EBM can also process a wide range of pre-connected metals (Wong and Hernandez 2012). This AM technique allows the manufacture of personalized prostheses (such as hip or knee prostheses, endoprosthesis) of metal alloys.
5.1.5 Inkjet
In the inkjet printing technique, a print head creates droplets of a liquid binding agent, which are combined with a substrate in powder. Droplets are created using a variety of technologies, such as piezoelectric, electromagnetic, or thermal methods to be distributed on a substrate (Marro et al. 2016). Changing the applied temperature gradient, pressure, frequency of the pulse, and ink viscosity, the droplet size can be modified to different applications in the medical field (Mok et al. 2016). Like SLM, inkjet printing does not require the use of support structures. Besides, they create relatively fast, low-cost models. However, in general, parts are not as durable as those manufactured with the SLS technique. An application of inkjet technology has been used in the bioengineering of 3D printed tissue. Instead of a liquid, the head printing deposits the living cells in scaffolds (Marro et al. 2016).
According to Chia and Wu (2015), the main advantages of bioprinting are room temperature processing (if applicable), direct incorporation, and homogeneous cell distribution. The main disadvantages are stiffness limited mechanics, the critical gelling time delay, the specific correspondence of the material, and the densities of the liquid medium to preserve shapes and low print resolution.
5.2 Materials
Various compounds, including photopolymers and thermoplastics, were and are being developed for application in 3D printing technology in the medical area due to cost reduction, good resolution (20–100 µm), and easy use (Rankin et al. 2018). Various types of materials are used for 3D printing in orthopedic surgeries such as metals, natural and synthetic polymers, bioceramics, and biomaterials (Marro et al. 2016; Mok et al. 2016; Chen et al. 2016; Tang et al. 2021). Currently, the most used materials in the printing of models in orthopedic surgery are:
-
1.
Acrylonitrile Butadiene Styrene (ABS) is a rigid and lightweight thermoplastic, resistant and non-toxic, with a melting point of approximately 210 °C to 250 °C. Derived from petroleum, it is not biodegradable, it can release vapors during printing (Fadero and Shah 2014). Used in bone model printing for education, training, and surgical planning (Bagaria and Chaudhary 2017) (Fig. 14.9);
-
2.
Polylactic Acid (PLA) is a thermoplastic of vegetable origin (starch), it has a melting point of approximately 210 °C to 250 °C (Hoang et al. 2016). PLA is easy to print, is biocompatible and biodegradable, but its strength degrades over time and the print has a certain texture roughness (Bagaria et al. 2018). It is used in printing of bone models and printing of surgical guides (Mok et al. 2016). PLA is brittle and has low mechanical resistance;
-
3.
Polyetheretherketone (PEEK) is used in the manufacture of implantable medical materials because it is biocompatible and biodegradable. Devices made with such material may show greater similarity to bone strength, stiffness, and elasticity. Also, it provides better patient comfort compared to titanium, exhibiting less thermal conductivity and lower density. Radiolucency is often cited as a great benefit for the improvement of the postoperative image which is particularly valuable in cancer cases. This material is suitable for intraoperative format adjustments as it allows the removal of part of the material (Peel et al. 2017);
-
4.
Nylon/Polyamide is a resistant and low-cost synthetic polymer, but it requires high temperature for modeling (210 °C to 250 °C) (Bagaria et al. 2018). Used in the printing of anatomical bone models for surgical programming and simulation, as well as surgical guides;
-
5.
Polycarbonate is used in the printing of bone models for education, training, and surgical planning.
As for metal printing, several materials are approved for printing implants and prostheses such as Stainless-Steel alloys (AISI 316L), Titanium alloys (Ti4ALV6), Tantalum (TA), and Chrome-Cobalt (CrCo).
6 Application of 3D Printing Technology in Orthopedic Surgery
The use of 3D printing technology is growing exponentially in various areas of medicine including orthopedic surgery. According to orthopedic literature, the biomedical use of technology 3D printing has four important uses (Bagaria et al. 2018):
-
1.
Anatomical models printing;
-
2.
Guides and Surgical Templates printing (cutting and drilling guides);
-
3.
Implants, Prostheses, and Orthoses printing;
-
4.
Scaffolds and cell printing.
In some situations, in the treatment of orthopedic problems the technology 3D printing has been used according to Bagaria et al. (2018):
-
1.
Periarticular and fractures of the hip, knee, ankle, shoulder, and elbow;
-
2.
Complex arthroplasties with bone defects;
-
3.
Complex spinal deformities;
-
4.
Deformities and fractures of the face;
-
5.
Deformities and changes due to congenital malformation;
-
6.
Planning for osteotomies.
Martelli et al. (2016) on a systematic review about the advantages and disadvantages of using 3D printing in surgeries describe them according to Table 14.2.
6.1 Biomodel Printing
The manufacture of anatomical models is currently the largest application of this type of 3D printing technology for the versatility of possibilities of use in several medical areas. One possibility of using the anatomical model includes patient-relative orientation. Regarding the communication between the medical team and the patient, some studies demonstrate the use of anatomical models to inform about the type of surgical treatment proposed, promoting a better understanding of the clinical condition of patients, surgical schedule, rehabilitation, and greater adherence to treatment, contributing to an improvement in the doctor-patient relationship (Zheng et al. 2018a, b; Bizzotto et al. 2015; Tack et al. 2016; Wilcox et al. 2017; Chen et al. 2019; Yang et al. 2016a, b).
6.1.1 Medical Education
The 3D printed anatomical models are a promising means of medical education for students in health sciences, resident doctors, and an improved form of communication with patients (Zheng et al. 2016).
Some works show the use of 3D-printed anatomical models in surgical training. A wide variety of domains including simulation accuracy, anatomical similarity, training in the use of surgical instruments use printed models for the training of surgeons (Hoang et al. 2016; Tack et al. 2016; Langridge et al. 2018). The use of 3D printing technology in the teaching process of health professionals has complemented, or even traditional teaching methods have been supplanted. Concerning the acquisition of knowledge of anatomy according to some studies as shown in the paper review by Langridge et al. (2018). This author reports that a 3D-printed anatomical model offers “feedback” that can facilitate the acquisition of surgical skills, accelerating the learning curve in some training models (Hoang et al. 2016; Zheng et al. 2016; Langridge et al. 2018).
Several studies have shown the effective application of the use of 3D printing technology in medical education and orthopedic training (Shui et al. 2017; Marro et al. 2016; Eley 2017; Mulford et al. 2016; Malik et al. 2015; Langridge et al. 2018; Bagaria et al. 2011; Cromeens et al. 2017) mainly associated with surgical procedures in complex anatomical regions. Huang et al. (2018) concluded in their study about the acetabular fracture surgical training with the aid of 3D anatomical models that the 3D printing technology was the most valuable tool for understanding this type of fracture. The data demonstrated that 3D-printed models of real fractures are an effective tool in learning the morphology of the acetabulum and promote student interest.
6.1.2 Preoperative Planning
The printing of biomodels provides additional information to conventional images with increased knowledge concerning the anatomopathology of the disease to be treated (Vaishya et al. 2018; Marro et al. 2016; Zheng et al. 2016; Bagaria et al. 2011; Zhang et al. 2017a, b).
An accurate navigation technique is essential for transferring the 3D preoperative surgical planning to the patient during surgery. Kim et al. (2018) in their study concluded that the 3D printing technique provided surgeons with a better understanding of the fracture pattern and anatomy and it was effectively used for preoperative planning, educating interns, and performing surgical simulations to improve the intraoperative technical results. Some studies have shown that 3D printing technology in planning and carrying out surgical procedures leads to a decrease in the surgical time (Bagaria and Chaudhary 2017; Malik et al. 2015; Tack et al. 2016; Zheng et al. 2016; Giannetti et al. 2017; Mobbs et al. 2018; Yang et al. 2016a, b; Ozturk et al. 2020), decreased blood loss during surgery (Bagaria and Chaudhary 2017; Mobbs et al. 2018; Yang et al. 2016a, b; Ozturk et al. 2020), decrease in time of exposure to ionizing radiation during the surgical procedure (Tack et al. 2016; Giannetti et al. 2017; Mobbs et al. 2018; Yang et al. 2016a, b; Ozturk et al. 2020), reduction of complications (Bagaria and Chaudhary 2017; Martelli et al. 2016; Kaye et al. 2016), a decrease of tourniquet time (Ozturk et al. 2020) and likely improvement in surgical results (Bagaria and Chaudhary 2017; Tack et al. 2016; Zheng et al. 2016).
Regarding the decrease in surgical time, Wilcox et al. (2017) in their systematic review reported that the reduction in surgical time was 15–20% in various scenarios of surgical procedures. The highlighted reasons given for reducing the time of surgery included a deeper understanding of pathologies, such as location and surgical approach, and the facilitation of preoperative instrumentation decisions. In a recent publication, Morgan et al. (2020) in systematic review and meta-analysis have concluded that their results suggest the use of 3D printing in pre-operative planning in orthopedic trauma reduces operative time, intraoperative blood loss, and the number of times fluoroscopy used.
One controversial point in orthopedics literature is the improvement of results using 3D printing in orthopedic surgery. Langridge et al. (2018) show in their study works suggesting that surgical planning with 3D technology leads to a better understanding of the anatomy which can lead to better surgical results.
However, there is no consensus in the orthopedics literature to improve the surgical result, in general, using 3D printing technology in orthopedic surgery and further trials are needed to highlight this aspect.
6.1.3 Preoperative Simulation
A preoperative simulation of a surgical procedure allows the prior evaluation and reproduction of complex operative stages, without suffering the time restriction of a real procedure. An effective surgical simulation requires faithful anatomical reproduction and must also behave similarly to the tissue of the patient (Rankin et al. 2018). This way 3D printing is useful in surgical simulation, surgical planning, in referencing the anatomical structures in the intraoperative step, in the preoperative choice of implants and guides to be used (Shui et al. 2017; Martelli et al. 2016; Van den Broeck et al. 2014; Zhang et al. 2017a, b; Trauner 2018) mainly regarding the understanding of geometry (distances, scales, shapes) and identification of complex anatomy (Vaishya et al. 2018; Shui et al. 2017; Marro et al. 2016; Mulford et al. 2016; Fadero and Shah 2014; Hoang et al. 2016; Wilcox et al. 2017; Langridge et al. 2018; Cromeens et al. 2017; Zhang et al. 2017a, b). Other advantages are a better choice of access to bone defects, a better understanding of the fracture pattern, and better choice in the positioning of bone implants (Zheng et al. 2018a, b; Vaishya et al. 2018; Bagaria and Chaudhary 2017; Eijnatten et al. 2018; Tetsworth et al. 2017; Karlin et al. 2017; Chana-Rodríguez et al. 2016; Huang et al. 2020; Cai et al. 2018) as depicted in Fig. 14.10.
According to Malik et al. (2015), a lot of time is spent intraoperatively to measure and bending the implant before placement during surgery to treat acetabular fractures. When performing the steps of reduction and positioning of the implant in a 3D model preoperatively, valuable time is saved during the procedure surgical, as the surgeon has more time to focus on the approach, reduction, and correction; that is, the choice of implant and preoperative bending of the implant is carried out in a free of stress environment before the procedure. In a study on osteotomy using 3D printing technique in the treatment of tibial plateau fractures malunion, Yang et al. (2016a, b) performing virtual surgical planning and using an anatomical model in scale reported an improvement in the understanding of the deformity for osteotomy programming with surgical simulation using the anatomical model (osteotomy, reduction of joint sinking and fixation with plate and screw). They report that with this technique they successfully reproduced preoperative planning with reduced surgical time, little loss of intraoperative blood, and accuracy in reducing collapse of the joint surface. These authors list the advantages of assisted surgery with 3D printing techniques compared to traditional surgery methods: Full-scale anatomical models improve understanding of the anatomy and morphology of the deformity such as details of the location, diversion, and sinking. Important details in planning the osteotomy location. Individualized surgical planning, with the possibility of less damage to soft parts due to the precise choice of surgical access and accuracy in reduction of deformity with less surgical time. The technique does not require sophisticated instruments and keeps the cost relatively low when printing the anatomical model.
The use of 3D printing technology in preoperative surgical planning has been shown to facilitate the procedure with satisfactory results, especially in complex articular fractures of the spine, pelvis, acetabulum, and sacro (Bagaria and Chaudhary 2017; Fadero and Shah 2014; Bagaria et al. 2011; Huang et al. 2020; Courvoisier et al. 2018; Zeng et al. 2016), knee (Kim et al. 2018; Bagaria et al. 2011; Giannetti et al. 2017), tibial plateau (Zheng et al. 2018a, b; Ozturk et al. 2020), tibial pilon (plafond) (Zheng et al. 2018a, b), ankle (Yang et al. 2016a, b), calcaneus (Fadero and Shah 2014; Bagaria et al. 2011), clavicle (Shon et al. 2020), shoulder and elbow (Zheng et al. 2018a, b; Kim et al. 2018) and distal radius (Bizzotto et al. 2015; Chen et al. 2019).
The utilization of the 3D anatomical model in preoperative planning allows the study and better understanding of anatomy, especially in articular and periarticular joints; improved visualization of specific fracture details confirming the pattern of fractures; better determining the displacement/deviation and the number of fracture fragments; better confirming the collapse and comminute condition of the joint surface; better checking the potential presence of bone defects; better determining whether the graft is needed. This type of virtual planning allows fracture fragments reduced in the best possible way and the most appropriate implants chosen and used, in addition to the possibility of the best choice of approach surgery at the injury site (Fadero and Shah 2014; Zheng et al. 2018a, b). VSP combined with 3D printing technology allows the surgeon to view the entire preoperative reduction process and guide intraoperative reduction, making the reduction less time-consuming and more precise (Giannetti et al. 2017; Ma et al. 2017) with less chance of surgical complications (Zheng et al. 2018a, b) (Fig. 14.11). It also allows adequate planning of percutaneous fixings in situations of irregular bone fractures (Fadero and Shah 2014).
Complete surgical wound healing after 3 weeks postoperative and the motion range of the right knee joint close to normal (a, b, c). One-year postoperative X-ray images showing nonunion healing with anatomical reduction and restored articular surface. The implant positioning performed during the surgery was according to preoperative VSP (Fig. 14.9) and the preoperative surgical simulation (Fig. 14.10) (d, e)
The 3D anatomical models of complex joint fractures increase considerably the number of important information needed for the appropriate treatment compared to radiographic and CT images. This one benefit that 3D printing favors are also dependent on the experience of the surgeon according to Bagaria and Chaudhary (2017). For the treatment of unilateral severe fractures of the lower limbs, Zhang et al. (2017a, b) described a technique for mirroring CT images of long bones for programming fracture reduction and programming of the implants to be used.
In his study on the use of 3D technology in the treatment of humeral intercondylar fractures, Zheng et al. (2018a, b) made a comparison between the group control that was submitted to conventional treatment and the group submitted to surgical treatment using 3D technology in preoperative planning (virtual surgery and anatomical model printing) and found a statistically significant difference in the following aspects: duration of surgery, blood loss, fluoroscopy time. The group submitted to treatment with the use of 3D technology showed a lower index in these three aspects with a value of p < 0.001. However, there was no statistical difference regarding the length of consolidation and clinical results.
In a randomized, single-blinded, prospective clinical trial conducted to evaluate the efficacy of using 3D printing in the treatment of distal radius fracture Chen et al. (2019) concluded in their study that 3D printing models effectively help the doctors plan and perform the surgery and provide more effective communication between doctors and patients, but cannot improve postoperative function compared with routine treatment.
Considering the anatomical complexity of acetabular fractures, several studies have reported the benefits of 3D printed models with preoperative planning (Bagaria and Chaudhary 2017; Kim et al. 2018; Fadero and Shah 2014; Malik et al. 2015; Bagaria et al. 2011, Courvoisier et al. 2018; Zeng et al. 2016). The use of technology of AM in the treatment of acetabular fractures provides the study of accurate fracture morphology; performing VSP; allows for a better choice surgical approach; pre-bent (pre-contoured) of implants with greater accuracy in their positioning (Courvoisier et al. 2018; Maini et al. 2018). Huang et al. (2020) in their study described a minimally invasive technique with an anterior approach combined with 3D printing for anterior plate fixation of the sacral fracture using VSP and preoperative simulation surgery for pre-bent implants. This author described that the postoperative x-Rays images have shown that the sacral fractures of all cases (12 patients) were successfully reduced and internally fixated.
Some authors have described the use of AM technology in the treatment of fractures of the tibial plateau. Giannetti et al. conducted a study whose proposal was to compare the surgical time, intraoperative blood loss, and postoperative clinical and radiographic results in the treatment of complex tibial plateau fractures operated with and without the pre and intraoperative use of real anatomical models of fractures printed in 3D. They concluded that patients operated with the aid of anatomical models printed with the 3D technology have seen a significant reduction in the time of surgery. However, in surgeries of patients operated without the use of anatomical models, there was an increased time of exposure to ionizing radiation (Giannetti et al. 2017). Huang et al. (2018) in a series of 6 cases submitted to surgical treatment of tibial plateau fracture performed preoperative planning with fracture reduction and positioning of the plate and screws, and 3D surgical guides were printed (PSI) according to the planning for positioning the screws and the board. Deviations in the positioning of the screws were evaluated before and after surgery comparing size, entry point, and direction of screws. They reported that there was no statistical difference in terms of size, entrance, and the projection of the ideal and real angle of the direction (trajectory) of the screw. They concluded that this technology increases the accuracy and efficiency of internal fixation using PSI. In their study, Ozturk et al. (2020) concluded that the use of the 3D life-size anatomical models assisting surgical planning maximized the possibility of ideal anatomical reduction and provided individualized information concerning tibial plateau fractures.
Zheng et al. (2018a, b) in their study on the feasibility of 3D printing in the treatment of tibial pilon (plafond) fracture and its effect on doctor-patient communication carried out a prospective study (100 patients) randomized into two groups: one group undergoing conventional treatment and another group undergoing treatment with the use of 3D printing technology. The latter group was subjected to virtual planning and virtual simulation of fracture reduction with mirroring of the contralateral side. The printing of the anatomical model and surgical simulation using an anatomical model printed in full scale for choosing and modeling of implants was also used. The statistical analysis of data was of the double-blind type. This study concluded that the 3D printing technology is safe and effective for treating adults with fractures tibial plateau with significantly shorter surgical time, less intraoperative blood loss, fewer fluoroscopy times, higher rate of anatomical reduction, and better results compared to the group that did not use these resources, finding any statistic differences regarding the complication rate comparing the groups. They also concluded that 3D printing can help doctors improve their theoretical knowledge and practical skills, reduce the learning curves, improve surgical quality, and provide better communication between doctors and patients.
6.2 Surgical Guides and Surgical Tools Printing
The cutting, drilling, and reduction guides made with 3D printing technology are called Patient-Specific Instrument (PSI) since they are customized and used in various situations in orthopedic surgeries.
These guides are personalized molds that fit the bone of the patient, with cutting guides and screw hole guides to position directly previously planned surgical instruments (Caiti et al. 2018) with bone graft removal cut guides and cutting and drilling guides in osteotomy and arthroplasty (Vaishya et al. 2018; Hoang et al. 2016; Tack et al. 2016; Zheng et al. 2016; Nam 2015; Woo et al. 2020). In addition to this minor or percutaneous surgical approaches are possible using this technique (Bagaria et al. 2018).
The PSI has been developed as an alternative to navigation systems. PSI was originally developed for Total Knee Arthroplasty (TKA). Other applications have been used as the insertion of pedicle screws in spine surgeries, Total Hip Arthroplasty (THA), and corrective osteotomy. The PSI technology has been adapted for tumor surgery bones: the customized cutting guides are designed with smooth surfaces specific to fit the bone in a unique position to direct the desired resection plans (Gouin et al. 2014).
Possible benefits of PSI printing are preoperative surgical planning reproducibility, reduced surgical time, and optimized efficiency and cost-effectiveness. Despite the proposed benefits, it is not yet proven to be better than standard techniques. In 2014 in Australia, this technique was used in 6.8% of all TKA according to Mulford et al. (2016).
In oncological surgeries, preoperative planning associated with PSI may result in greater surgical accuracy concerning resection of free margins and precision in bone cuts (Gouin et al. 2014).
Studies show that the use of PSI in bone tumor resections in the pelvis, simplify the surgical procedure (Sallent et al. 2017). In the same way the use of the combination of 3D models associated with computerized navigation results in increased surgical accuracy in tumor resection (Fadero and Shah 2014; Zhang et al. 2017a, b). Jentzsch et al. (2016) reported in a series of cases the use of cutting guides in performing osteotomies in surgeries for hemipelvectomy in the treatment of pelvic tumors. They concluded that the virtual surgical planning associated with intraoperative use of 3D models and PSI anatomical assist in visualizing the anatomy and surgical accuracy.
Cutting guides for block osteotomies assist in the adequate resection of the injury with safety margins (Jentzsch et al. 2016). The use of 3D image modeling has led to an improvement in the design of various instruments (cutting and drilling guides) and implants used in orthopedic surgery, mainly in those whose realization occurs in places of complex anatomy such as pelvis, spine, and scapular waist (Mok et al. 2016; Malik et al. 2015; Zhang et al. 2017a, b). PSI prototyping has become a technological advance with an impact on TKA and THA, oncological surgery, and spine surgery (Chen et al. 2016; Malik et al. 2015; Trauner et al. 2018).
The use of PSI in spine surgery allows planning the screw trajectories reducing the risk of deviations out of the body and the vertebral pedicle reducing the risk of vascular and nerve damage, in addition to making custom implants according to Mobbs et al. (2018). Intraoperative guides, created with specific patient data, in spine surgeries may have the ability to decrease the risks associated with these procedures according to Wilcox et al. (2017). In their systematic review, numerous studies have shown that guides help shorten operations, suggesting that this may decrease complications related to operative time (e.g., infection). Other benefits include decreased intraoperative radiation; simplicity of use; elimination of subjectivity of the procedure; improved preoperative planning; and moderate cost compared to other techniques.
In the same way as deformity correction planning in orthopedic trauma, the making of personalized surgical instruments is one of the great benefits of 3D printing technology (Fadero and Shah 2014). For the treatment of malunion fracture, Hoekstra et al. (2016) described a long bone corrective osteotomy technique using specific individualized guides printed with 3D technology. This process is summarized in:
-
1.
Image acquisition of the segment that has vicious consolidation in CT. It is necessary to acquire the contralateral limb to perform the technique;
-
2.
Creation of the 3D virtual model and realization of the mirroring of the contralateral side to define the variables to be corrected (rotation, angulation, and length);
-
3.
Choosing of osteotomy position and orientation (addition wedge or subtraction e.g.) and determining the corrected position of the bone, the location of the implants is defined. This one step is performing virtual surgical planning (VSP);
-
4.
Printing of the cut and drill guide (PSI) and the anatomical model;
-
5.
Performing surgery with exposure of the osteotomy site, positioning of the guide, and provisional fixation of the guide with Kirschner’s wire; In this step, the holes of the definitive screws can be pre-drilled;
-
6.
Performing the osteotomy with the cutting guide according to the VSP;
-
7.
Performing osteotomy reduction to the corrected site. Kirschner's wires can be used to perform the reduction;
-
8.
Fixating of osteotomy as planned with plate and screw;
-
9.
Performing postoperative CT.
Caiti et al. (2018) showed in their study on radio osteotomy that the positioning error of the PSI (cutting guides) depends on the mounting location. That must be carefully considered when using 3D printing during surgery, recommending the use of extended guides, as it increases the accuracy of surgical navigation. Several studies cite that despite the creation of personalized guides for angular correction surgery with osteotomy the cutting guide and plate positioning may lead to unsatisfactory surgical procedures (Hoekstra et al. 2016; de Muinck Keizer et al. 2017; Rosseels et al. 2019).
According to Rosseels et al. (2019) in their study on the use of guides printed with 3D technology (PSI) to perform osteotomies found four big traps using the 3D printing technique. They are:
-
1.
Careful placement of the planned guide is mandatory since that the sub-optimal positioning of the guide is the main cause of the incomplete correction;
-
2.
The use of screw holes (pre-drilled) does not guarantee the proper screw placement;
-
3.
The translation of bone fragments over the osteotomy planes in an oblique osteotomy is a potential risk;
-
4.
The depth of the osteotomy is difficult to estimate and can lead to cartilage lesions in peri-articular regions.
Tack et al. (2016) in their systematic review regarding the use of 3D technology in the medical field report that many recent studies mention that there is no difference in clinical outcomes between TKA surgeries that used standardized cuts compared to surgeries that used cutting guides obtained through 3D printing technology. This same author claims that recent studies showing the cost–benefit assessment of the use of custom cut guides suggest that 3D printing technology does not offer advantages to cover the cost associated with using these personalized cut guides. Besides, Tack mentions that some studies show an increased time in preparing and discussing surgical planning with the use of 3D technology. The use of customized cutting guides in TKA requires a long period of programming the surgery that is much longer than the reduction of time in the TKA surgical procedure. These studies suggest that surgical planning is more accurate when performed by an orthopedist compared to other professionals.
6.3 Orthopedics Implants Printing
A major advantage of using AM technology is the ability to make personalized implants—PSI (Mobbs et al. 2018) being a resource increasingly used in orthopedic surgeries (Bagaria and Chaudhary 2017; Eijnatten et al. 2018; Chen et al. 2016; Tack et al. 2016; Kaye et al. 2016; Sallent et al. 2017; Rosseels et al. 2019). The use of PSI is an effective method with great reproduction accuracy of preoperative planning (Malik et al. 2015; Caiti et al. 2018; Sallent et al. 2017). Besides the accuracy, these printed materials must have two other important characteristics: they must have mechanical resistance and be sterilizable (Rankin et al. 2018).
The possibility of printing personalized implants as mentioned by Ma et al. where a 3D printed titanium mesh tray was used in the treatment of a complex comminuted mandibular fracture can provide more predictable aesthetic and functional results. In this study, Ma et al. described a case where virtual surgery was performed to simulate the process reduction of the displaced fragments in the preoperative. The team conducted a study on the morphology of fractured sites to be reduced. The tray fabric was manufactured by 3D printing technology based on the anatomic model serving as an intraoperative template. All of these factors led to a reduction in the time of surgery and better results (Ma et al. 2017).
Regarding the use of customized implants used in spinal surgery, Wilcox et al. (2017) described in their systematic review that the cases performed so far are limited anatomically to rare pathologies and challenging in which an individualized solution to restore a patient’s anatomy specificity is a key prognostic factor. Also, most custom prostheses were made of titanium alloy (TiV6Al4) due to their biocompatibility and ability to improve bone healing by porosity optimization to match the trabecular bone structure.
In a retrospective study of a series of cases, Li et al. (2016) described the use of acetabular components printed with 3D printing technology in THA revision surgeries with severe bone loss. This study concluded that the use of custom acetabular components using prototyping technology and 3D printing seems to provide stable fixation and good short-term functionalities in this series of cases. As further improvements in the design and the manufacturing process are made, future studies should evaluate groups with larger numbers of patients for longer and ideally compare this approach with other alternative approaches for treating this type of complex bone defect in THA reviews.
Wong et al. (2015) reported a clinical case of partial resection of the acetabulum in a patient with pelvic chondrosarcoma and performed a reconstruction with a personalized pelvic implant. Bone resection was virtually planned, and an implant was designed using CAD software to fill in the bone defect. The implant was evaluated biomechanically and made with titanium 3D printing technology (Ti6Al4V) with the SLM technique. A cutting guide (PSI) was used to reproduce the planned resection (osteotomy in VSP) to suit the custom implant. The accuracy of free margin resection was validated by comparing the obtained resection and the implant position with that planned. There was no recurrence of the injury or loosening of the implanted material in an 11-month postoperative follow-up.
Liang et al. (2017) described a reconstruction technique for treating tumors in the pelvis using modular pelvic endoprosthesis printed with 3D printing technology in titanium alloy by EBM technique. Based on their report of a series of 35 patients, the study concluded that the use of prostheses pelvic floor using 3D printing technology for reconstruction of defect bone after excision of pelvic tumors is possible and safe with good functional results in a 30-month follow-up.
With the development of AM technology, it was possible to make structures to replace complex bone defects and even whole bones. Tetsworth et al. (2017) described a reconstruction technique for bone defects with the use of a printed implant with 3D technology for the treatment of massive segmental defects of long bones. They performed virtual planning (VSP) and constructed the customized metal structure (PSI) titanium lattice type. Based on mirroring of the contralateral limb, the titanium lattice was made according to the original bone geometry. The truss design was defined according to the implants used to fixate the bone-implant set. Imanishi and Choong (2015) described a clinical case of using a calcaneus prosthesis printed with 3D technology after total calcanectomy. The patient had calcaneus chondrosarcoma that was completely resected, and a heel prosthesis was placed. The VSP was performed using the mirroring technique on the contralateral side, and a prosthesis of the calcaneus with EBM titanium technology was made. The articular surface was submitted to polishing treatment. Tendon and ligament reinsertion were performed in the prosthesis for stabilization. With a 5-month follow-up, the patient did not present surgical complications nor pain. This was the first case of calcaneus prosthesis created with AM technology. Xie et al. (2018) described reconstructive surgery for the treatment of Kienböck disease in stage IIIC, using a metallic prosthesis 3D printed semilunar bone. The shape and size of the prosthesis were determined by mirroring the contralateral side based on CT images. In this case, the author does not mention the technology for printing the prosthesis, nor the material used in printing. Choy et al. (2017) described a clinical case of treatment of primary bone tumor in the spine undergoing reconstruction after vertebrectomy. The T9 body was printed with 3D technology in titanium restoring the local anatomy, with a good result in a 6-month follow-up.
In a systematic review concerning the technique of 3D printing in the medical field, Tack et al. (2016) report that the most commonly used materials in making custom implants are titanium (Ti), PEEK, hydroxyapatite (HA), PMMA. Researches are being carried out concerning the manufacturing of customized meshes using biodegradable materials such as HA and PLA (Ma et al. 2017). Qiao et al. (2015) described the use of AM technology in the printing of a customized external fixator to aid in reducing the fracture, reporting advantages such as easy handling, accurate reduction, and minimally invasive procedure.
Other possibilities for using AM technology are e.g., the printing of surgical instruments for hand fractures surgery as described by Fuller et al. (2014) and the making of hand prostheses printed with 3D technology for the treatment of children who suffered hand amputation due to traumatic or malformation, as described by Burn et al. (2016).
6.4 Scaffold and Cell Printing
With the progressive technological advancements, a new frontier was reached in health research with the establishment of the “State of the Art” in medical science with the structuring of two new areas of knowledge: regenerative medicine (RM) and tissue engineering (TE). RM combines the principles of engineering and biology for the production of structures that can restore or strengthen the functions of human organs and tissues (Arealis and Nikolaou 2015). TE is a transdisciplinary and translational field that aims to combine knowledge about cells and tissues, biomaterials, biochemical factors, and biomechanics to create biological structures to replace and/or regenerate tissues (Wong et al. 2017).
Bioprinting is a rapid prototyping technology for the printing of biologically active cells and cellular matrices. The development of culture media and cell growth systems allowed for the direct printing of biological materials in scaffolds (3D structures that serve as frameworks used for transplantation with or without cells). The scaffolds are critical to providing structure for infiltration and cell proliferation, space for extracellular matrix generation, and remodeling providing biochemical signals to direct cellular behavior and physical connections to injured tissue. According to Chia and Wu (2015). when printing scaffolds, it is necessary to evaluate the architecture at the macro, micro, and nano-level to provide structural conditions, nutrient transport, and cell–matrix interaction. Macro architecture is the general form of the structure that can be complex (e.g., patient and organ specificities, anatomical features). Microarchitecture reflects fabric architecture (e.g., pore size, shape, porosity, spatial distribution, and pore interconnection). Nanoarchitecture is the modification of the surface (e.g., fixation of biomolecules for adhesion, proliferation, and cell differentiation). It is possible to print scaffolds, fabrics, or even biologically active organs through various methodologies including constructions of biodegradable materials associated with cell seeding, bio-jet printing ink, microextrusion bioprinting, or laser-assisted bioprinting (Rankin et al. 2018). Tang et al. (2021) described the specific features that ideal scaffolds material should present:
-
1.
Excellent biocompatibility to support the adhesion and proliferation of bone-forming cells;
-
2.
High mechanical properties for load bearing;
-
3.
Suitable pore interconnectivity and size for transport of nutrients and oxygen.
-
4.
Tailored biodegradation or bioresorbability to provide growth space of new bone tissue;
-
5.
Allowable incorporation of biological cues and signals for cell adhesion, proliferation, metabolism, and differentiation.
Bone Tissue Engineering (BTE) in the field of RM develops alternative treatment options for treating bone defects. According to Arealis and Nikolaou (2015), BTE has four methods for creating bone grafts in vitro:
-
1.
Printing a scaffold in which all other components will be loaded. Ideally, it should imitate the bone structure, reabsorb the fee that allows the native bone to fill the defect and at the same time protect and provide nutrients to the cellular components of the graft (osteoconduction);
-
2.
The second component is the cells. They can be osteoblasts or pluripotent progenitor cells that differ from osteoblasts bone producers with osteogenic function;
-
3.
For cells to proliferate and differentiate into osteoblasts, morphogenic or osteoinductive signs are needed. Protein bone morphogenetic (BMP) and similar inducing molecules are the third components required;
-
4.
For the graft to develop and be incorporated in vivo, sufficient vascularization to meet the growing metabolic tissue is needed.
Therefore, a possibility of using scaffolds is their use on bone defect treatments (post-traumatic, congenital, or post-arthroplasty), with osteoconductive function. Currently, bioceramics such as HA and calcium phosphate—or even bioactive glass—are biomaterials for manufacturing porous structures, as they are highly biocompatible and biodegradable. However, the low mechanical strength is a major challenge, and most scaffolds are used only in unloaded regions (Wong et al. 2017). For reconstructing bone defects that require mechanical support such as long bone (femur, tibia) metal materials are used in scaffolds. The two more used are Ti alloy and tantalum (Ta) as bone trabecular metal to create a biomimetic structure that occupies the bone defect and allows scaffold cellularization (Tang et al. 2021).
Currently, research is underway to develop other types of natural and synthetic polymers, composites, and biomaterials used in 3D printed scaffolds for the treatment of bone defects. In the last years, scholars have made important progress in BTE technology concerning biomaterial development, bioprinting cells, and using of the bone bioreactor to promote viable substitutes to bone regeneration (Liang et al. 2021; Luo et al. 2020).
References
Arealis G, Nikolaou VS (2015) Bone printing: new frontiers in the treatment of bone defects. Injury 46(8):S20–S22
Bagaria V, Bhansali R, Pawar P (2018) 3D printing creating a blueprint for the future of orthopedics: current concept review and the road ahead! J Clin Orthop Trauma 9(3):207–212
Bagaria V, Chaudhary K (2017) A paradigm shift in surgical planning and simulation using 3Dgraphy: experience of first 50 surgeries done using 3D-printed biomodels. Injury 48(11):2501–2508
Bagaria V, Deshpande S, Rasalkar DD, Kuthe A, Paunipagar BK (2011) Use of rapid prototyping and three-dimensional reconstruction modeling in the management of complex fractures. Eur J Radiol 80(3):814–820
Belvedere C, Siegler S, Fortunato A, Caravaggi P, Liverani E, Durante S (2019) New comprehensive procedure for custom-made total ankle replacements: medical imaging, joint modeling, prosthesis design, and 3D printing. J Orthop Res 37(3):760–768
Bizzotto N, Tami I, Santucci A, Romani D, Cosentino A (2015) 3D Printed replica of articular fractures for surgical planning and patient consent: a 3 years multi-centric experience. 3D Print Med, 2(1):2
Burn MB, Ta A, Gogola GR (2016) Three-dimensional printing of prosthetic hands for children. J Hand Surg Am 41(5):e103–e109
Cai L, Zhang Y, Chen C, Lou Y, Guo X, Wang J (2018) 3D printing-based minimally invasive cannulated screw treatment of unstable pelvic fracture. J Orthop Surg Res 13(1):71
Caiti G, Dobbe JGG, Strijkers GJ, Strackee SD, Streekstra GJ, Caiti BG (2018) Positioning error of custom 3D-printed surgical guides for the radius: influence of fitting location and guide design. Int J Comput Assist Radiol Surg 13(4):507–518
Chana-Rodríguez F, Mañanes RP, Rojo-Manaute J, Gil P, Martínez-Gómiz JM, Vaquero-Martín J (2016) 3D surgical printing and pre contoured plates for acetabular fractures. Injury 47(11):2507–2511
Chen C, Cai L, Zheng W, Wang J, Guo X, Chen H (2019) The efficacy of using 3D printing models in the treatment of fractures: A randomised clinical trial. BMC Musculoskelet Disord 20(1):65
Chen X, Xu L, Wang W, Li X, Sun Y, Politis C (2016) Computer-aided design and manufacturing of surgical templates and their clinical applications: a review. Expert Rev Med Devices 13(9):853–864
Chia HN, Wu BM (2015) Recent advances in 3D printing of biomaterials. J Biol Eng 9(1):4
Choy WJ, Mobbs RJ, Wilcox B, Phan S, Phan K, Sutterlin III CE (2017) Reconstruction of the thoracic spine using a personalized 3D-printed vertebral body in an adolescent with a T9 primary bone tumour: case report. World Neurosurg 105:1032e13–1032e17
Courvoisier A, Boudissa M, Chabanas M, Tonetti J (2018) Computer assisted surgery in preoperative planning of acetabular fracture surgery: state of the art. Expert Rev Med Devices 15(1):81–89
Cromeens BP, Ray WC, Hoehne B, Abayneh F, Adler B, Besner GE (2017) Facilitating surgeon understanding of complex anatomy using a three-dimensional printed model. J Surg Res 216:18–25
de Muinck Keizer RJO, Lechner KM, Mulders MAM, Schep NWL, Eygendaal D, Goslings JC (2017) Three-dimensional virtual planning of corrective osteotomies of distal radius malunions: a systematic review and meta-analysis. Strateg Trauma Limb Reconstr 12(2):77–89
van Eijnatten M, van Dijk R, Dobbe J, Streekstra G, Koivisto J, Wolff J (2018) CT image segmentation methods for bone used in medical additive manufacturing. Med Eng Phys 51:6–16
Eley KA, Watt-Smith SR, Sheerin F, Golding SJ (2014) “Black Bone” MRI: a potential alternative to CT with three-dimensional reconstruction of the craniofacial skeleton in the diagnosis of craniosynostosis. Eur Radiol 24(10):2417–2426
Eley KA, Watt-smith SR, Golding SJ (2017) “Black Bone” MRI: a novel imaging technique for 3D printing. Dentomaxillofacial Radiol 46(3):20160407
Eley KA (2017) Centralised 3D printing in the NHS: a radiological review. Clin Radiol 72(4):269–275
Fadero PE, Shah M (2014) Three dimensional (3D) modelling and surgical planning in trauma and orthopaedics. Surgeon 12(6):328–333
Favier V, Zemiti N, Mora OC, Subsol G, Captier G, Lebrun R et al (2017) Geometric and mechanical evaluation of 3D-printing materials for skull base anatomical education and endoscopic surgery simulation—a first step to create reliable customized simulators. PLoS ONE 12(12):e0189486
Frizziero L, Pagliari C, Donnici G, Liverani A, Santi GM, Papaleo P et al (2021) Effectiveness assessment of CAD simulation in complex orthopedic surgery practices. Symmetry (basel) 13(5):850
Fuller SM, Butz DR, Vevang CB, Makhlouf MV (2014) Application of 3-dimensional printing in hand surgery for production of a novel bone reduction clamp. J Hand Surg Am 39(9):1840–1845
Giannetti S, Bizzotto N, Stancati A, Santucci A (2017) Minimally invasive fixation in tibial plateau fractures using an pre-operative and intra-operative real size 3D printing. Injury 48(3):784–788
Gouin F, Paul L, Odri GA, Cartiaux O (2014) Computer-assisted planning and patient-specific instruments for bone tumor resection within the pelvis: a series of 11 patients. Sarcoma 2014:842709
Green N, Glatt V, Tetsworth K, Wilson LJ, Grant CA (2016) A practical guide to image processing in the creation of 3D models for orthopedics. Tech Orthop 31(3):153–163
Hoang D, Perrault D, Stevanovic M, Ghiassi A (2016) Surgical applications of three-dimensional printing: a review of the current literature & how to get started. Ann Transl Med 4(23):456
Hoekstra H, Rosseels W, Sermon A, Nijs S (2016) Corrective limb osteotomy using patient specific 3D-printed guides: a technical note. Injury 47(10):2375–2380
Huang H, Xing W, Zeng C, Huang W (2020) Pararectus approach combined with three-dimensional printing for anterior plate fixation of sacral fractures. Injury 52(10):2719–2724
Huang Z, Song W, Zhang Y, Zhang Q, Zhou D, Zhou X et al (2018) Three-dimensional printing model improves morphological understanding in acetabular fracture learning: a multicenter, randomized, controlled study. PLoS ONE 13(1):e0191328
Imanishi J, Choong PFM (2015) Three-dimensional printed calcaneal prosthesis following total calcanectomy. Int J Surg Case Rep 10:83–87
Jentzsch T, Vlachopoulos L, Fürnstahl P, Müller DA, Fuchs B (2016) Tumor resection at the pelvis using three-dimensional planning and patient-specific instruments: a case series. World J Surg Oncol 14(1):249
Karlin L, Weinstock P, Hedequist D, Prabhu SP (2017) The surgical treatment of spinal deformity in children with myelomeningocele: the role of personalized three-dimensional printed models. J Pediatr Orthop B 26(4):375–382
Kaye R, Goldstein T, Zeltsman D, Grande DA, Smith LP (2016) Three dimensional printing: a review on the utility within medicine and otolaryngology. Int J Pediatr Otorhinolaryngol 89:145–148
Kim JW, Lee Y, Seo J, Park JH, Seo YM, Kim SS et al (2018) Clinical experience with three-dimensional printing techniques in orthopedic trauma. J Orthop Sci 23(2):383–388
Langridge B, Momin S, Coumbe B, Woin E, Griffin M, Butler P (2018) Systematic review of the use of 3-Dimensional printing in surgical teaching and assessment. J Surg Educ 75(1):209–221
Li H, Qu X, Mao Y, Dai K, Zhu Z (2016) Custom acetabular cages offer stable fixation and improved hip scores for revision THA with severe bone defects. Clin Orthop Relat Res 474(3):731–740
Li L, Yu F, Shi J, Shen S, Teng H, Yang J et al (2017) In situ repair of bone and cartilage defects using 3D scanning and 3D printing. Sci Rep 7(1):9416
Liang H, Ji T, Zhang Y, Wang Y, Guo W (2017) Reconstruction with 3D-printed pelvic endoprostheses after resection of a pelvic tumour. Bone Joint J 99-B(2):267–275
Liang R, Gu Y, Wu Y, Bunpetch V, Zhang S (2021) Lithography-Based 3D bioprinting and bioinks for bone repair and regeneration. ACS Biomater Sci Eng 7(3):806–816
Luo Y, Pan H, Jiang J, Zhao C, Zhang J, Chen P et al (2020) Desktop-stereolithography 3D printing of a polyporous extracellular matrix bioink for bone defect regeneration. Front Bioeng Biotechnol 8:589094
Ma J, Ma L, Wang Z, Zhu X, Wang W (2017) The use of 3D-printed titanium mesh tray in treating complex comminuted mandibular fractures A case report. Medicine (baltimore) 96(27):e7250
Maini L, Verma T, Sharma A, Sharma A, Mishra A, Jha S (2018) Evaluation of accuracy of virtual surgical planning for patient-specific pre-contoured plate in acetabular fracture fixation. Arch Orthop Trauma Surg 138(4):495–504
Malik HH, Darwood ARJ, Shaunak S, Kulatilake P, El-Hilly AA, Mulki O et al (2015) Three-dimensional printing in surgery: a review of current surgical applications. J Surg Res 199(2):512–522
Marro A, Bandukwala T, Mak W (2016) Three-dimensional printing and medical imaging: a review of the methods and applications. Curr Probl Diagn Radiol 45(1):2–9
Martelli N, Serrano C, van den Brink H, Pineau J, Prognon P, Borget I et al (2016) Advantages and disadvantages of 3-dimensional printing in surgery: a systematic review. Surgery 159(6):1485–1500
Mobbs RJ, Choy WJ, Wilson P, McEvoy A, Phan K, Parr WCH (2018) L5 En-bloc vertebrectomy with customized reconstructive implant: comparison of patient-specific versus off-the-shelf implant. World Neurosurg 112:94–100
Mok S-W, Nizak R, Fu S-C, Ho K-WK, Qin L, Saris DBF et al (2016) From the printer: potential of three-dimensional printing for orthopaedic applications. J Orthop Transl 6:42–49
Morgan C, Khatri C, Hanna SA, Ashrafian H, Sarraf KM (2020) Use of three-dimensional printing in preoperative planning in orthopaedic trauma surgery: a systematic review and meta-analysis. World J Orthop 11(1):57–67
Mulford JS, Babazadeh S, Mackay N (2016) Three-dimensional printing in orthopaedic surgery: review of current and future applications. ANZ J Surg 86(9):648–653
Nam D (2015) Patient-specific instrumentation (PSI) in total knee arthroplasty (TKA) [Internet]. In: Surgical techniques in total knee arthroplasty (TKA) and alternative procedures. Woodhead Publishing Limited, pp 207–227
Ozturk AM, Suer O, Derin O, Ozer MA, Govsa F, Aktuglu K (2020) Surgical advantages of using 3D patient-specific models in high-energy tibial plateau fractures. Eur J Trauma Emerg Surg 46(5):1183–1194
Pagac M, Hajnys J, Ma Q, Jancar L, Jansa J, Stefek P et al (2021) A review of vat photopolymerization technology: materials, applications, challenges, and future trends of 3D printing. Polymers (basel) 13(4):598
Parthasarathy J, Krishnamurthy R, Ostendorf A, Shinoka T, Krishnamurthy R (2020) 3D printing with MRI in pediatric applications. J Magn Reson Imaging 51(6):1641–1658
Peel S, Bhatia S, Eggbeer D, Morris DS, Hayhurst C (2017) Evolution of design considerations in complex craniofacial reconstruction using patient-specific implants. Proc Inst Mech Eng H 231(6):509–524
Qiao F, Li D, Jin Z, Gao Y, Zhou T, He J et al (2015) Application of 3D printed customized external fixator in fracture reduction. Injury 46(6):1150–1155
Rankin TM, Wormer BA, Miller JD, Giovinco NA, Al Kassis S, Armstrong DG (2018) Image once, print thrice? Three-dimensional printing of replacement parts. Br J Radiol 91(1083):20170374
Rathor S, Jena J, Uddanwadikar R, Apte A (2021) Finite element analysis of type I and type II fracture with PFN implant—a comparative study. In: Kalamkar V, Monkova K (eds) Advances in mechanical engineering. Lecture notes in mechanical engineering. Springer, Singapore, pp 243–251
Rosseels W, Herteleer M, Sermon A, Nijs S, Hoekstra H (2019) Corrective osteotomies using patient-specific 3D-printed guides: a critical appraisal. Eur J Trauma Emerg Sur 45(2):299–307
Sallent A, Vicente M, Reverté MM, Lopez A, Rodríguez-Baeza A, Pérz-Domínguez M et al (2017) How 3D patient-specific instruments improve accuracy of pelvic bone tumour resection in a cadaveric study. Bone Joint Res 6(10):577–583
Shon HC, Bang JY, Lee Y, Koh KH, Kim JW (2020) Optimal plate position in minimally invasive plate osteosynthesis for mid-shaft clavicle fractures: simulation using 3D-printed models of actual clinical cases. Eur J Trauma Emerg Surg 1–7
Shui W, Zhou M, Chen S, Pan Z, Deng Q, Yao Y et al (2017) The production of digital and printed resources from multiple modalities using visualization and three-dimensional printing techniques. Int J Comput Assist Radiol Surg 12(1):13–23
Tack P, Victor J, Gemmel P, Annemans L (2016) 3D-printing techniques in a medical setting: a systematic literature review. Biomed Eng Online 15(1):115
Tang G, Liu Z, Liu Y, Yu J, Wang X, Tan Z et al (2021) Recent trends in the development of bone regenerative biomaterials. Front Cell Dev Biol 9:665813
Tappa K, Jammalamadaka U, Weisman JA, Ballard DH, Wolford DD, Pascual-Garrido C et al (2019) 3D printing custom bioactive and absorbable surgical screws, pins, and bone plates for localized drug delivery. J Funct Biomater 10(2):17
Tetsworth K, Block S, Glatt V (2017) Putting 3D modelling and 3D printing into practice: virtual surgery and preoperative planning to reconstruct complex post-traumatic skeletal deformities and defects. SICOT J 3:16
Trauner KB (2018) The emerging role of 3D printing in arthroplasty and orthopedics. J Arthroplasty 33(8):2352–2354
Vaishya R, Patralekh MK, Vaish A, Agarwal AK, Vijay V (2018) Publication trends and knowledge mapping in 3D printing in orthopaedics. J Clin Orthop Trauma 9(3):194–201
Van den Broeck J, Vereecke E, Wirix-Speetjens R, Vander Sloten J (2014) Segmentation accuracy of long bones. Med Eng Phys 36(7):949–953
Wieding J, Souffrant R, Fritsche A, Mittelmeier W, Bader R (2012) Finite element analysis of osteosynthesis screw fixation in the bone stock: an appropriate method for automatic screw modelling. PLoS ONE 7(3):e33776
Wilcox B, Mobbs RJ, Wu A-M, Phan K (2017) Systematic review of 3D printing in spinal surgery: the current state of play. J Spine Surg 3(3):433–443
Wong KC, Kumta SM, Gee NVL, Demol J (2015) One-step reconstruction with a 3D-printed, biomechanically evaluated custom implant after complex pelvic tumor resection. Comput Aided Surg 20(1):14–23
Wong KV, Hernandez A (2012) A review of additive manufacturing. ISRN Mech Eng 2012:208760
Wong TM, Jin J, Lau TW, Fang C, Yan CH, Yeung K et al (2017) The use of three-dimensional printing technology in orthopaedic surgery: a review. J Orthop Surg (hong Kong) 25(1):2309499016684077
Woo S-H, Sung M-J, Park K-S, Yoon T-R (2020) Three-dimensional-printing technology in hip and pelvic surgery: current landscape. Hip Pelvis 32(1):1–10
Xie M, Tang K, Yuan C (2018) 3D printing lunate prosthesis for stage IIIc Kienböck’s disease: a case report. Arch Orthop Trauma Surg 138(4):447–451
Yan L, Lim JL, Lee JW, Tia CSH, O’Neill GK, Chong DYR (2020) Finite element analysis of bone and implant stresses for customized 3D-printed orthopaedic implants in fracture fixation. Med Biol Eng Comput 58(5):921–931
Yang L, Shang XW, Fan JN, He ZX, Wang JJ, Liu M et al (2016a) Application of 3D printing in the surgical planning of trimalleolar fracture and doctor-patient communication. Biomed Res Int 2016:2482086
Yang P, Du D, Zhou Z, Lu N, Fu Q, Ma J et al (2016b) 3D printing-assisted osteotomy treatment for the malunion of lateral tibial plateau fracture. Injury 47(12):2816–2821
Zeng C, Xing W, Wu Z, Huang H, Huang W (2016) A combination of three-dimensional printing and computer-assisted virtual surgical procedure for preoperative planning of acetabular fracture reduction. Injury 47(10):2223–2227
Zhang W, Ji Y, Wang X, Liu J, Li D (2017a) Can the recovery of lower limb fractures be achieved by use of 3D printing mirror model? Injury 48(11):2485–2495
Zhang Y, Wen L, Zhang J, Yan G, Zhou Y, Huang B (2017b) Three-dimensional printing and computer navigation assisted hemipelvectomy for en bloc resection of osteochondroma. Medicine (baltimore) 96(12):e6414
Zheng YX, Yu DF, Zhao JG, Wu YL, Zheng B (2016) 3D printout models vs. 3D-rendered images: which is better for preoperative planning? J Surg Educ 73(3):518–523
Zheng W, Chen C, Zhang C, Tao Z, Cai L (2018a) The feasibility of 3D printing technology on the treatment of Pilon fracture and its effect on doctor-patient communication. Biomed Res Int 2018:8054698
Zheng W, Su J, Cai L, Lou Y, Wang J, Guo X et al (2018b) Application of 3D printing technology in the treatment of humeral intercondylar fractures. Orthop Traumatol Surg Res 104(1):83–88
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2022 The Author(s), under exclusive license to Springer Nature Switzerland AG
About this chapter
Cite this chapter
Mendonça, C.J.A., Setti, J.A.P. (2022). 3D Printing in Orthopedic Surgery. In: Canciglieri Junior, O., Trajanovic, M.D. (eds) Personalized Orthopedics. Springer, Cham. https://doi.org/10.1007/978-3-030-98279-9_14
Download citation
DOI: https://doi.org/10.1007/978-3-030-98279-9_14
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-030-98278-2
Online ISBN: 978-3-030-98279-9
eBook Packages: EngineeringEngineering (R0)