Abstract
Sulforaphane (SFN), an isothiocyanate obtained from cruciferous vegetables, exerts antioxidant, antiapoptotic, and antitumor activities in different cell types. Moreover, SFN has been viewed as an anti-inflammatory agent. Nonetheless, the mechanism underlying the ability of SFN in modulating the immune response in mammalian cells is not completely understood yet. Therefore, we investigated here whether and how SFN would be effective in preventing inflammation induced by a pro-oxidant agent (hydrogen peroxide, H2O2) in the human neuroblastoma SH-SY5Y cells. The cells were treated with SFN at 5 μM for 30 min before a challenge with H2O2 for an additional 24 h. Pretreatment with SFN reduced the secretion of interleukin-1β (IL-1β) and tumor necrosis factor-α (TNF-α), as well as decreased the levels of cyclooxygenase-2 (COX-2) in H2O2-treated cells. SFN also decreased the activity of the transcription factor nuclear factor-κB (NF-κB) and the immunocontent of the p65 NF-κB subunit in the cell nucleus. The inhibition of heme oxygenase-1 (HO-1) by ZnPP-IX at 10 μM or the silencing of the nuclear factor erythroid 2-related factor 2 (Nrf2) transcription factor by small interfering RNA targeting Nrf2 attenuated the anti-inflammatory and cytoprotective effects induced by SFN. Therefore, SFN exerted an anti-inflammatory effect in H2O2-challenged SH-SY5Y cells by a mechanism dependent on the Nrf2/HO-1 signaling pathway.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Sulforaphane (SFN; C6H11NOS2) is an isothiocyanate found in cruciferous vegetables, such as broccoli (Houghton et al. 2016). SFN has been described as an antioxidant, antiapoptotic, and antitumor agent (Tarozzi et al. 2013; Tortorella et al. 2015). Moreover, SFN induces anti-inflammatory effects, as observed in several experimental models (Carrasco-Pozo et al. 2017; Lee et al. 2017; Park et al. 2017; Yu et al. 2017). SFN is a potent activator of the nuclear factor erythroid 2-related factor 2 (Nrf2) transcription factor, which mediates cytoprotection in mammalian cells (Denzer et al. 2016; Houghton et al. 2016). After being released from the cytosolic protein complex with Kelch-like ECH-associated protein 1 (Keap1), Nrf2 migrates to the cell nucleus and modulates the expression of genes whose products present a central role in both maintenance of the redox environment homeostasis and detoxification (biotransformation) in different cell types (Nguyen et al. 2009; Ma 2013). Among these proteins, heme oxygenase-1 (HO-1) has attracted attention of several research groups due to its dual action as an antioxidant and anti-inflammatory agent (Foresti et al. 2013; Loboda et al. 2016; Son et al. 2013). HO-1 mediates the degradation of heme, generating carbon monoxide (CO), free iron, and biliverdin (Gozzelino et al. 2010). The conversion of biliverdin into bilirubin by biliverdin reductase generates a strong antioxidant exhibiting beneficial effects in several experimental models (O'Brien et al. 2015). On the other hand, CO presents anti-inflammatory, antioxidant, and antithrombotic actions and the modulation of its levels by natural compounds is an interesting strategy to modulate the negative consequences observed in neurodegeneration and cardiovascular diseases, among others (Gozzelino et al. 2010; Otterbein 2002). The modulation of HO-1 by natural compounds, including SFN, has been reported in different cell lines (Deng et al. 2012; Lee et al. 2013) and in in vivo experimental models (Hong et al. 2010; Zhou et al. 2016).
HO-1 downregulation has been related to chronic inflammation in humans. Radhakrishnan et al. (2011) have described HO-1 deficiency in a young girl presenting severe hemolysis and inflammation in a case of congenital asplenia. Moreover, Konrad et al. (2016) reported increased levels of pro-inflammatory agents in mice lacking leukocytic HO-1 submitted to lipopolysaccharide (LPS)-induced acute pulmonary inflammation. Additionally, it has been published that HO-1 would be a central point of modulation in the anti-inflammatory M2 macrophages (Naito et al. 2014). We recently demonstrated a role for the Nrf2/HO-1 signaling pathway in mediating antioxidant and anti-inflammatory effects induced by natural compounds in SH-SY5Y cells exposed to different chemical stressors (de Oliveira et al. 2017a, b, c). Neuroinflammation takes a role in a vicious cycle involving the redox homeostasis observed during the onset and progression of neurodegeneration, since redox impairment is both a cause and a consequence of inflammation in brain tissues and other organs (Mosley et al. 2006; Hulsmans and Holvoet 2010). At least in part, HO-1 attenuates inflammation by the downregulation of the nuclear factor-κB (NF-κB), the master immunomodulatory agent in mammalian cells (Alcaraz et al. 2004; Wardyn et al. 2015). Indeed, there is a growing body of evidence indicating an intricate cross talk between the Nrf2/HO-1 axis and the NF-κB-dependent signaling, and the involvement of the redox environment components (both antioxidant and pro-oxidant) would present a very important role during inflammation (Banning and Brigelius-Flohé 2005; Banning et al. 2008; Brigelius-Flohé et al. 2004).
Even though there is evidence pointing to an anti-inflammatory effect caused by SFN in mammalian tissues, the exact mechanism underlying this action remains to be elucidated. Therefore, we investigated here whether SFN would be able to modulate the inflammation induced by hydrogen peroxide (H2O2), a pro-oxidant agent, in the human neuroblastoma SH-SY5Y cell line. Furthermore, we analyzed whether Nrf2 and/or HO-1 would be involved in the mechanism underlying the SFN-induced anti-inflammatory effects in this experimental model.
Materials and Methods
Materials
Plastic materials used here to perform cell culture were acquired from Corning, Inc. (NY, USA) and Becton Dickinson (NJ, USA). The reagents used to maintain cultured cells have been purchased from Sigma (MO, USA). Additional chemicals and assay kits used in this work have been obtained from different manufacturers, as indicated below.
Cell Culture and Treatments
The human neuroblastoma cell line (SH-SY5Y) was purchased from the American Type Culture Collection (Manassas, VA, USA) and was maintained in Dulbecco’s modified Eagle’s medium (DMEM)/F-12 HAM nutrient medium (1:1 mixture; supplemented with 10% fetal bovine serum (FBS) and containing 2 mM l-glutamine, 1000 units/mL penicillin, 1000 μg/mL streptomycin, and 2.5 μg/mL amphotericin B) in a 5% CO2-humidified incubator at 37 °C (de Oliveira et al. 2016a, b).
We utilized H2O2 at 300 μM for 24 h in order to induce a pro-inflammatory state in SH-SY5Y cells, as previously reported (de Oliveira et al. 2017d, e). SFN (dissolved in DMSO; DMSO was utilized at a final concentration of 0.01%) at 5 μM was administrated to the cells 30 min before a challenge with H2O2 for further 24 h. In order to cause HO-1 inhibition, ZnPP IX (10 μM) was administrated to the cells for 1 h prior the exposure to SFN (Kwon et al. 2015; Wang et al. 2016; de Oliveira et al. 2017a).
Evaluation of Cell Viability and Membrane Integrity
Cell viability was evaluated by utilizing the 3-(4,5-dimethylthiazol-2-yl)-2,5-diphenyltetrazolium bromide (MTT) assay (Mosmann 1983). We performed the lactate dehydrogenase (LDH) leakage assay in order to evaluate membrane integrity according to the instructions of the manufacturer (CytoTox 96-Non-Radioactive Cytotoxicity Assay, Promega).
Quantification of the Pro-inflammatory Cytokines
The levels of IL-1β and TNF-α were determined by utilizing ELISA assay kits based on the recommendations of the manufacturer (Abcam, MA, USA).
Isolation of Cell Nucleus
The cell nucleus was isolated by utilizing a Nuclear Extraction Kit acquired from Cayman Chemical (MI, USA).
Enzyme-Linked Immunosorbent Assay to Quantify COX-2, HO-1, Nrf2, and Nuclear p65 NF-κB Subunit Immunocontents
The immunocontents of these proteins were measured by an indirect ELISA assay through the utilization of polyclonal antibodies (Abcam, MA, USA) diluted 1:1000 in phosphate-buffered saline (PBS) at pH 7.4 with 5% albumin, as previously described (de Oliveira et al. 2017d, e). The levels of the p65 NF-κB subunit were measured after nuclear isolation.
Determination of NF-κB Activity
The activity of the transcription factor NF-κB was quantified in SH-SY5Y cells through the utilization of a commercial kit based on the recommendations of the manufacturer (Abcam, MA, USA).
siRNA Transfection
Nrf2 silencing in SH-SY5Y cells was achieved by using Nrf2 siRNA following the instructions of the manufacturer (Santa Cruz, CA, USA) (Jin et al. 2015; Quesada et al. 2011).
Statistical Analyses
We performed statistical analyses by using the GraphPad 5.0 software. Data are presented as the mean ± standard error of the mean (S.E.M.) of three or five independent experiments each done in triplicate; p values were considered significant when p < 0.05. Differences between the experimental groups were checked by one-way ANOVA followed by the post hoc Tukey test.
Results
SFN Attenuated the H2O2-Induced Loss of Viability and Toxicity by HO-1-Dependent Manner in SH-SY5Y Cells
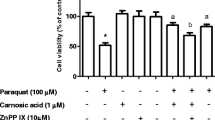
We have previously found that SFN pretreatment at 5 μM for 30 min alleviated the effects of a challenge with H2O2 at 300 μM for additional 24 h regarding the viability of SH-SY5Y cells. Therefore, we investigated in the present work whether HO-1 would be involved in the cytoprotective effects elicited by SFN. As depicted in Fig. 1a, SFN prevented loss of viability in SH-SY5Y cells exposed to H2O2 by a mechanism associated with HO-1, since the inhibition of this enzyme by ZnPP-IX abrogated the protection elicited by SFN in SH-SY5Y cells (p < 0.05). Similarly, SFN pretreatment decreased the H2O2-mediated cytotoxicity by an HO-1-dependent manner in SH-SY5Y cells (p < 0.05; Fig. 1b).
The inhibition of HO-1 by ZnPP IX attenuates the effects of SFN on a cell viability and b membrane integrity in SH-SY5Y cells challenged with H2O2. The cells were treated with SFN at 5 μM for 30 min prior the challenge with H2O2 at 300 μM for an additional 24 h. ZnPP IX at 10 μM was administrated to the cells for 1 h prior treatment with SFN. Data are shown as the mean ± SEM of three or five independent experiments each done in triplicate. One-way ANOVA followed by the post hoc Tukey test, *p < 0.05 different from the control group; a different from H2O2-treated group; b p < 0.05 different from H2O2 + SFN-treated cells
SFN Induced an Anti-inflammatory Effect by an HO-1-Dependent Mechanism in H2O2-Treated SH-SY5Y Cells
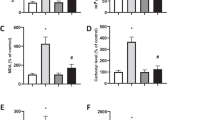
We next examined whether SFN would exert an anti-inflammatory effect in SH-SY5Y cells challenged with H2O2. As may be observed in Fig. 2a, SFN pretreatment decreased the levels of IL-1β secreted by SH-SY5Y cells exposed to H2O2 by a mechanism associated with HO-1, since ZnPP-IX partially abrogated this effect (p < 0.05). SFN also attenuated the secretion of TNF-α by H2O2-treated cells through an HO-1-dependent fashion (p < 0.05; Fig. 2b). Moreover, SFN decreased the immunocontent of COX-2 by an HO-1-dependent manner in SH-SY5Y cells exposed to H2O2 (p < 0.05; Fig. 2c). We confirmed previously reported data demonstrating that SFN upregulates HO-1 and Nrf2 in SH-SY5Y cells (Lee et al. 2013), as may be observed in Fig. S1A and Fig. S1B, respectively.
The inhibition of HO-1 by ZnPP IX alleviated the effects of SFN on the levels of a IL-1β, b TNF-α, and c COX-2 in SH-SY5Y cells challenged with H2O2. The cells were treated with SFN at 5 μM for 30 min prior to the challenge with H2O2 at 300 μM for an additional 24 h. ZnPP IX at 10 μM was administrated to the cells for 1 h prior to treatment with SFN. Data are shown as the mean ± SEM of three or five independent experiments each done in triplicate. One-way ANOVA followed by the post hoc Tukey test, *p < 0.05 different from the control group; a different from the H2O2-treated group; b p < 0.05 different from the H2O2 + SFN-treated cells
SFN Repressed the NF-κB-Mediated Signaling by a Mechanism Involving HO-1
In order to analyze the mechanism by which SFN decreased the levels of markers of inflammation in SH-SY5Y cells, we investigated whether the transcription factor NF-κB would be modulated by SFN here. Additionally, we tested whether HO-1 would be associated with the SFN-induced modulation of NF-κB in this experimental model. We observed that SFN prevented the translocation of the p65 NF-κB subunit to the nucleus of SH-SY5Y cells exposed to H2O2 by a mechanism involving HO-1, since inhibition of this enzyme partially abrogated the effects of SFN on the nuclear levels of the p65 NF-κB subunit (p < 0.05; Fig. 3a). Furthermore, we analyzed the effects of SFN on the activity of NF-κB. SFN pretreatment caused a decrease in the activity of this transcription factor by an HO-1-dependent mechanism in H2O2-challenged SH-SY5Y cells, as depicted in Fig. 3b (p < 0.05).
The inhibition of HO-1 by ZnPP IX abrogated the effects of SFN on a the levels of the p65 NF-κB subunit in the cell nucleus and on b the activity of NF-κB in SH-SY5Y cells challenged with H2O2. The cells were treated with SFN at 5 μM for 30 min prior to the challenge with H2O2 at 300 μM for an additional 24 h. ZnPP IX at 10 μM was administrated to the cells for 1 h prior to treatment with SFN. Data are shown as the mean ± SEM of three or five independent experiments each done in triplicate. One-way ANOVA followed by the post hoc Tukey test, *p < 0.05 different from the control group; a different from the H2O2-treated group; b p < 0.05 different from H2O2 + SFN-treated cells
SFN Caused an Anti-inflammatory Effect in H2O2-Treated SH-SY5Y Cells by an Nrf2-Dependent Mechanism
Based on the findings described above, we evaluated whether the transcription factor Nrf2 would be involved in the anti-inflammatory action elicited by SFN in SH-SY5Y cells. Data reported by our research group demonstrated that the Nrf2/HO-1 axis may be involved in the modulation of the anti-inflammatory effects induced by natural compounds in SH-SY5Y cells (de Oliveira et al. 2017b, c). According to Fig. 4a, silencing of Nrf2 by using siRNA targeting this transcription factor abrogated the effects of SFN on the secretion of IL-1β by SH-SY5Y cells exposed to H2O2 (p < 0.05). Additionally, silencing of Nrf2 suppressed the effects of SFN on the secretion of TNF-α in the cells challenged with H2O2 (p < 0.05). Knocking down of Nrf2 also reduced the effects of SFN on the levels of COX-2 in H2O2-treated SH-SY5Y cells, as demonstrated in Fig. 5 (p < 0.05). In order to confirm that Nrf2 would be involved in the modulation of HO-1 in SFN-treated cells, we checked whether silencing of this transcription factor would affect HO-1 levels in SH-SY5Y cells exposed to SFN. As depicted in Fig. S2A, silencing of Nrf2 suppressed the SFN-induced HO-1 upregulation (p < 0.05). Additionally, Nrf2 silencing caused a significant decrease in the levels of Nrf2 in the nucleus of SH-SY5Y cells treated with SFN (p < 0.05; Fig. S2B).
The silencing of the transcription factor nuclear factor erythroid 2-related factor 2 (Nrf2) by using small interfering RNA (siRNA) targeting Nrf2 (for 48 h) attenuated the effects of SFN on the levels of a IL-1β and b TNF-α in the medium of SH-SY5Y cells exposed to H2O2. The cells were treated with SFN at 5 μM for 30 min prior to the challenge with H2O2 at 300 μM for an additional 24 h. Data are shown as the mean ± SEM of three or five independent experiments each done in triplicate. One-way ANOVA followed by the post hoc Tukey test, *p < 0.05 different from the cells transfected with scrambled control (NC) siRNA and exposed to SFN and H2O2
The silencing of the transcription factor nuclear factor erythroid 2-related factor 2 (Nrf2) by using small interfering RNA (siRNA) targeting Nrf2 (for 48 h) attenuated the effects of SFN on the immunocontents of COX-2 in SH-SY5Y cells exposed to H2O2. The cells were treated with SFN at 5 μM for 30 min prior to the challenge with H2O2 at 300 μM for additional 24 h. Data are shown as the mean ± SEM of three or five independent experiments each done in triplicate. One-way ANOVA followed by the post hoc Tukey test, *p < 0.05 different from the cells transfected with scrambled control (NC) siRNA and exposed to SFN and H2O2
SFN Inhibited NF-κB by an Nrf2-Dependent Manner
We then evaluated whether Nrf2 would be involved in the inhibition of NF-κB by SFN in this experimental model. We found that Nrf2 silencing abrogated the effects of SFN on the activity of NF-κB in the cells challenged with H2O2 (p < 0.05; Fig. 6).
The silencing of the transcription factor nuclear factor erythroid 2-related factor 2 (Nrf2) by using small interfering RNA (siRNA) targeting Nrf2 (for 48 h) attenuated the effects of SFN on the activity of NF-κB in SH-SY5Y cells exposed to H2O2. The cells were treated with SFN at 5 μM for 30 min prior to the challenge with H2O2 at 300 μM for an additional 24 h. Data are shown as the mean ± SEM of three or five independent experiments each done in triplicate. One-way ANOVA followed by the post hoc Tukey test, *p < 0.05 different from the cells transfected with scrambled control (NC) siRNA and exposed to SFN and H2O2
Nrf2 Mediated the Protection Elicited by SFN in H2O2-Treated SH-SY5Y Cells
Silencing of Nrf2 suppressed the protective effects elicited by SFN regarding the viability (p < 0.05; Fig. 7a) of the cells exposed to H2O2. Moreover, Nrf2 silencing blocked the effect of SFN on the membrane integrity in SH-SY5Y cells challenged with H2O2 (p < 0.05; Fig. 7b).
The silencing of the transcription factor nuclear factor erythroid 2-related factor 2 (Nrf2) by using small interfering RNA (siRNA) targeting Nrf2 (for 48 h) attenuated the effects of SFN on the a viability and b membrane integrity of SH-SY5Y cells exposed to H2O2. The cells were treated with SFN at 5 μM for 30 min prior to the challenge with H2O2 at 300 μM for an additional 24 h. Data are shown as the mean ± SEM of three or five independent experiments each done in triplicate. One-way ANOVA followed by the post hoc Tukey’s test, *p < 0.05 different from the cells transfected with scrambled control (NC) siRNA and exposed to SFN and H2O2
Discussion
In the herein presented work, we have found that SFN exerted an anti-inflammatory effect in H2O2-challenged SH-SY5Y cells through a mechanism associated with the Nrf2/HO-1 signaling pathway. The SFN-dependent induction of the Nrf2/HO-1 axis caused a decrease in the activity of the NF-κB transcription factor, which is a major modulator of the expression of the pro-inflammatory cytokines IL-1β and TNF-α and of the COX-2 enzyme (Lawrence 2009). Inhibition of HO-1 by ZnPP-IX or silencing of Nrf2 by siRNA abrogated the anti-inflammatory and cytoprotective effects elicited by SFN in H2O2-treated SH-SY5Y cells. This is the first work showing evidence that the Nrf2/HO-1 signaling pathway may be involved in the NF-κB-dependent modulation of inflammation in an experimental model of redox impairment. Even though it was not described here the exact mechanism by which SFN activated Nrf2, it is very likely that the Nrf2 upregulation occurred by direct interaction of SFN through its isothiocyanate functional group with the Nrf2-Keap1 complex, causing the release of Nrf2 and posterior translocation to the cell nucleus, as previously demonstrated in other works (Yao et al. 2014, 2015; Peng et al. 2015a, b, c).
It has been demonstrated that exposure of different cell types to pro-oxidant agents leads to a pro-inflammatory scenario that favors cell death, as reported in neurodegenerative and cardiovascular diseases (Hulsmans and Holvoet 2010; Biswas 2016). On the other hand, pro-inflammatory cytokines cause a redox disruption in mammalian cells, as observed in some experimental models (Yasuhara et al. 2005; Mathy-Hartert et al. 2008). Actually, inflammation may be viewed both as a cause and consequence of redox impairment (Hulsmans and Holvoet 2010). In this context, some classical antioxidant and detoxifying enzymes, such as glutathione peroxidase (GPx) and glutathione-S-transferase (GST), respectively, have been seen as anti-inflammatory agents by interacting directly with pro-inflammatory mediators, and not only by acting on potential toxic compounds (reactive species or xenobiotics, pollutants, or drugs, for example) in mammalian cells. Rao et al. (1988) have demonstrated that GPx exhibited an anti-inflammatory action in experimental lens-induced uveitis. Banning et al. (2008) have found that GPx2 downregulated the expression of COX-2 in human colon cancer cells, causing a decrease in the production of prostaglandin-E2 (PGE2). On the other hand, Xue et al. (2005) have reported that GST exhibited an anti-inflammatory effect in the RAW264.7 cell line by inhibiting the mitogen-activated protein kinases (MAPK) and the activation of NF-κB. Besides, HO-1, which produces CO during the degradation of heme, would be a major anti-inflammatory agent after signaling mediated by Nrf2 (Paine et al. 2010). Recently, Kobayashi et al. (2016) have published that Nrf2 would modulate the expression of pro-inflammatory cytokines through a non-redox, direct mechanism, suppressing the macrophage-mediated inflammatory response. Therefore, even though the inhibition of HO-1 by ZnPP-IX suppressed the anti-inflammatory effects triggered by SFN in this experimental model, a direct role for Nrf2 in modulating the expression of the pro-inflammatory cytokines studied here may not be discarded. Additionally, the involvement of the pro-oxidant and pro-inflammatory actions of COX-2 deserves further research regarding the protective effects induced by SFN, since PGE2, one of the products of the COX-2 pathway, exerts pro-oxidant and pro-inflammatory impairments in mammalian cells and has been viewed as an important pharmacological target during neurodegeneration (Andreasson 2010; Kallens et al. 2017).
In conclusion, SFN protected SH-SY5Y cells exposed to a pro-oxidant agent presenting pro-inflammatory effects by a mechanism associated with the Nrf2/HO-1 axis. Further research in in vivo experimental models would be important to evaluate whether SFN would induce such effects in brain cells, since the bioavailability of SFN may limit its effects.
References
Alcaraz MJ, Vicente AM, Araico A, Dominguez JN, Terencio MC, Ferrándiz ML (2004) Role of nuclear factor-kappaB and heme oxygenase-1 in the mechanism of action of an anti-inflammatory chalcone derivative in RAW 264.7 cells. Br J Pharmacol 142:1191–1199
Andreasson K (2010) Emerging roles of PGE2 receptors in models of neurological disease. Prostaglandins Other Lipid Mediat 91:104–112. https://doi.org/10.1016/j.prostaglandins.2009.04.003
Banning A, Brigelius-Flohé R (2005) NF-kappaB, Nrf2, and HO-1 interplay in redox-regulated VCAM-1 expression. Antioxid Redox Signal 7:889–899
Banning A, Florian S, Deubel S, Thalmann S, Müller-Schmehl K, Jacobasch G, Brigelius-Flohé R (2008) GPx2 counteracts PGE2 production by dampening COX-2 and mPGES-1 expression in human colon cancer cells. Antioxid Redox Signal 10:1491–1500. https://doi.org/10.1089/ars.2008.2047
Biswas SK (2016) Does the interdependence between oxidative stress and inflammation explain the antioxidant paradox? Oxidative Med Cell Longev 2016:5698931. https://doi.org/10.1155/2016/5698931
Brigelius-Flohé R, Banning A, Kny M, Böl GF (2004) Redox events in interleukin-1 signaling. Arch Biochem Biophys 423:66–73
Carrasco-Pozo C, Tan KN, Gotteland M, Borges K (2017) Sulforaphane protects against high cholesterol-induced mitochondrial bioenergetics impairments, inflammation, and oxidative stress and preserves pancreatic β-cells function. Oxidative Med Cell Longev 2017:3839756. https://doi.org/10.1155/2017/3839756
de Oliveira MR, Ferreira GC, Schuck PF (2016a) Protective effect of carnosic acid against paraquat-induced redox impairment and mitochondrial dysfunction in SH-SY5Y cells: role for PI3K/Akt/Nrf2 pathway. Toxicol in Vitro 32:41–54. https://doi.org/10.1016/j.tiv.2015.12.005
de Oliveira MR, Peres A, Ferreira GC, Schuck PF, Bosco SM (2016b) Carnosic acid affords mitochondrial protection in chlorpyrifos-treated Sh-Sy5y cells. Neurotox Res 30:367–379. https://doi.org/10.1007/s12640-016-9620-x
de Oliveira MR, Peres A, Ferreira GC, Schuck PF, Gama CS, Bosco SMD (2017a) Carnosic acid protects mitochondria of human neuroblastoma SH-SY5Y cells exposed to paraquat through activation of the Nrf2/HO-1 axis. Mol Neurobiol 54:5961–5972. https://doi.org/10.1007/s12035-016-0100-3
de Oliveira MR, de Souza IC, Fürstenau CR (2017b) Carnosic acid induces anti-inflammatory effects in paraquat-treated SH-SY5Y cells through a mechanism involving a crosstalk between the Nrf2/HO-1 axis and NF-κB. Mol Neurobiol. https://doi.org/10.1007/s12035-017-0389-6
de Oliveira MR, da Costa FG, Brasil FB, Peres A (2017c) Pinocembrin suppresses H2O2-induced mitochondrial dysfunction by a mechanism dependent on the Nrf2/HO-1 Axis in SH-SY5Y cells. Mol Neurobiol. https://doi.org/10.1007/s12035-016-0380-7
de Oliveira MR, Fürstenau CR, de Souza ICC, da Costa Ferreira G (2017d) Tanshinone I attenuates the effects of a challenge with H2O2 on the functions of tricarboxylic acid cycle and respiratory chain in SH-SY5Y cells. Mol Neurobiol 54:7858–7868. https://doi.org/10.1007/s12035-016-0267-7
de Oliveira MR, Brasil FB, Andrade CMB (2017e) Naringenin attenuates H2O2-induced mitochondrial dysfunction by an Nrf2-dependent mechanism in SH-SY5Y cells. Neurochem Res 42:3341–3350. https://doi.org/10.1007/s11064-017-2376-8
Deng C, Tao R, Yu SZ, Jin H (2012) Sulforaphane protects against 6-hydroxydopamine-induced cytotoxicity by increasing expression of heme oxygenase-1 in a PI3K/Akt-dependent manner. Mol Med Rep 5:847–851. https://doi.org/10.3892/mmr.2011.731
Denzer I, Münch G, Friedland K (2016) Modulation of mitochondrial dysfunction in neurodegenerative diseases via activation of nuclear factor erythroid-2-related factor 2 by food-derived compounds. Pharmacol Res 103:80–94. https://doi.org/10.1016/j.phrs.2015.11.019
Foresti R, Bains SK, Pitchumony TS, de Castro Brás LE, Drago F, Dubois-Randé JL, Bucolo C, Motterlini R (2013) Small molecule activators of the Nrf2-HO-1 antioxidant axis modulate heme metabolism and inflammation in BV2 microglia cells. Pharmacol Res 76:132–148. https://doi.org/10.1016/j.phrs.2013.07.010
Gozzelino R, Jeney V, Soares MP (2010) Mechanisms of cell protection by heme oxygenase-1. Annu Rev Pharmacol Toxicol 50:323–354. https://doi.org/10.1146/annurev.pharmtox.010909.105600
Hong Y, Yan W, Chen S, Sun CR, Zhang JM (2010) The role of Nrf2 signaling in the regulation of antioxidants and detoxifying enzymes after traumatic brain injury in rats and mice. Acta Pharmacol Sin 31:1421–1430. https://doi.org/10.1038/aps.2010.101
Houghton CA, Fassett RG, Coombes JS (2016) Sulforaphane and other nutrigenomic Nrf2 activators: can the clinician’s expectation be matched by the reality? Oxidative Med Cell Longev 2016:7857186–7857117. https://doi.org/10.1155/2016/7857186
Hulsmans M, Holvoet P (2010) The vicious circle between oxidative stress and inflammation in atherosclerosis. J Cell Mol Med 14:70–78. https://doi.org/10.1111/j.1582-4934.2009.00978.x
Jin X, Liu Q, Jia L, Li M, Wang X (2015) Pinocembrin attenuates 6-OHDA-induced neuronal cell death through Nrf2/ARE pathway in SH-SY5Y cells. Cell Mol Neurobiol 35:323–333. https://doi.org/10.1007/s10571-014-0128-8
Kallens V, Tobar N, Molina J, Bidegain A, Smith PC, Porras O, Martínez J (2017) Glucose promotes a pro-oxidant and pro-inflammatory stromal microenvironment which favors motile properties in breast tumor cells. J Cell Biochem 118:994–1002. https://doi.org/10.1002/jcb.25650
Kobayashi EH, Suzuki T, Funayama R, Nagashima T, Hayashi M, Sekine H, Tanaka N, Moriguchi T, Motohashi H, Nakayama K, Yamamoto M (2016) Nrf2 suppresses macrophage inflammatory response by blocking proinflammatory cytokine transcription. Nat Commun 7:11624. https://doi.org/10.1038/ncomms11624
Konrad FM, Knausberg U, Höne R, Ngamsri KC, Reutershan J (2016) Tissue heme oxygenase-1 exerts anti-inflammatory effects on LPS-induced pulmonary inflammation. Mucosal Immunol 9:98–111. https://doi.org/10.1038/mi.2015.39
Kwon SH, Ma SX, Hwang JY, Lee SY, Jang CG (2015) Involvement of the Nrf2/HO-1 signaling pathway in sulfuretin-induced protection against amyloid beta25-35 neurotoxicity. Neuroscience 304:14–28. https://doi.org/10.1016/j.neuroscience.2015.07.030
Lawrence T (2009) The nuclear factor NF-kappaB pathway in inflammation. Cold Spring Harb Perspect Biol 1:a001651. https://doi.org/10.1101/cshperspect.a001651
Lee C, Park GH, Lee SR, Jang JH (2013) Attenuation of β-amyloid-induced oxidative cell death by sulforaphane via activation of NF-E2-related factor 2. Oxidative Med Cell Longev 2013:313510–313512. https://doi.org/10.1155/2013/313510
Lee IC, Kim DY, Bae JS (2017) Sulforaphane reduces HMGB1-mediated septic responses and improves survival rate in septic mice. Am J Chin Med 45:1253–1271. https://doi.org/10.1142/S0192415X17500690
Loboda A, Damulewicz M, Pyza E, Jozkowicz A, Dulak J (2016) Role of Nrf2/HO-1 system in development, oxidative stress response and diseases: an evolutionarily conserved mechanism. Cell Mol Life Sci 73:3221–3247. https://doi.org/10.1007/s00018-016-2223-0
Ma Q (2013) Role of nrf2 in oxidative stress and toxicity. Annu Rev Pharmacol Toxicol 53:401–426. https://doi.org/10.1146/annurev-pharmtox-011112-140320
Mathy-Hartert M, Hogge L, Sanchez C, Deby-Dupont G, Crielaard JM, Henrotin Y (2008) Interleukin-1beta and interleukin-6 disturb the antioxidant enzyme system in bovine chondrocytes: a possible explanation for oxidative stress generation. Osteoarthr Cartil 16:756–763. https://doi.org/10.1016/j.joca.2007.10.009
Mosley RL, Benner EJ, Kadiu I, Thomas M, Boska MD, Hasan K, Laurie C, Gendelman HE (2006) Neuroinflammation, oxidative stress and the pathogenesis of Parkinson’s disease. Clin Neurosci Res 6:261–281. https://doi.org/10.1016/j.cnr.2006.09.006
Mosmann T (1983) Rapid colorimetric assay for cellular growth and survival: application to proliferation and cytotoxicity assays. J Immunol Methods 65:55–63
Naito Y, Takagi T, Higashimura Y (2014) Heme oxygenase-1 and anti-inflammatory M2 macrophages. Arch Biochem Biophys 564:83–88. https://doi.org/10.1016/j.abb.2014.09.005
Nguyen T, Nioi P, Pickett CB (2009) The Nrf2-antioxidant response element signaling pathway and its activation by oxidative stress. J Biol Chem 284:13291–13295. https://doi.org/10.1074/jbc.R900010200
O’Brien L, Hosick PA, John K, Stec DE, Hinds TD Jr (2015) Biliverdin reductase isozymes in metabolism. Trends Endocrinol Metab 26:212–220. https://doi.org/10.1016/j.tem.2015.02.001
Otterbein LE (2002) Carbon monoxide: innovative anti-inflammatory properties of an age-old gas molecule. Antioxid Redox Signal 4:309–319
Paine A, Eiz-Vesper B, Blasczyk R, Immenschuh S (2010) Signaling to heme oxygenase-1 and its anti-inflammatory therapeutic potential. Biochem Pharmacol 80:1895–1903. https://doi.org/10.1016/j.bcp.2010.07.014
Park YK, Ramalingam M, Kim S, Jang BC, Park JW (2017) Sulforaphane inhibits the interferon-γ-induced expression of MIG, IP-10 and I-TAC in INS-1 pancreatic β-cells through the downregulation of IRF-1, STAT-1 and PKB. Int J Mol Med 40:907–912. https://doi.org/10.3892/ijmm.2017.3054
Peng S, Zhang B, Yao J, Duan D, Fang J (2015a) Dual protection of hydroxytyrosol, an olive oil polyphenol, against oxidative damage in PC12 cells. Food Funct 6:2091–2100. https://doi.org/10.1039/c5fo00097a
Peng S, Zhang B, Meng X, Yao J, Fang J (2015b) Synthesis of piperlongumine analogues and discovery of nuclear factor erythroid 2-related factor 2 (Nrf2) activators as potential neuroprotective agents. J Med Chem 58:5242–5255. https://doi.org/10.1021/acs.jmedchem.5b00410
Peng S, Yao J, Liu Y, Duan D, Zhang X, Fang J (2015c) Activation of Nrf2 target enzymes conferring protection against oxidative stress in PC12 cells by ginger principal constituent 6-shogaol. Food Funct 6:2813–2823. https://doi.org/10.1039/c5fo00214a
Quesada A, Ogi J, Schultz J, Handforth A (2011) C-terminal mechano-growth factor induces heme oxygenase-1-mediated neuroprotection of SH-SY5Y cells via the protein kinase Cϵ/Nrf2 pathway. J Neurosci Res 89:394–405. https://doi.org/10.1002/jnr.22543
Radhakrishnan N, Yadav SP, Sachdeva A, Pruthi PK, Sawhney S, Piplani T, Wada T, Yachie A (2011) Human heme oxygenase-1 deficiency presenting with hemolysis, nephritis, and asplenia. J Pediatr Hematol Oncol 33:74–78. https://doi.org/10.1097/MPH.0b013e3181fd2aae
Rao NA, Romero JL, Sevanian A, Fernandez MA, Wong C, Ward PA, Marak GE Jr (1988) Anti-inflammatory effect of glutathione peroxidase on experimental lens-induced uveitis. Ophthalmic Res 20:213–219
Son Y, Lee JH, Chung HT, Pae HO (2013) Therapeutic roles of heme oxygenase-1 in metabolic diseases: curcumin and resveratrol analogues as possible inducers of heme oxygenase-1. Oxidative Med Cell Longev 2013:639541–639512. https://doi.org/10.1155/2013/639541
Tarozzi A, Angeloni C, Malaguti M, Morroni F, Hrelia S, Hrelia P (2013) Sulforaphane as a potential protective phytochemical against neurodegenerative diseases. Oxidative Med Cell Longev 2013:415078–415010. https://doi.org/10.1155/2013/415078
Tortorella SM, Royce SG, Licciardi PV, Karagiannis TC (2015) Dietary sulforaphane in cancer chemoprevention: the role of epigenetic regulation and HDAC inhibition. Antioxid Redox Signal 22:1382–1424. https://doi.org/10.1089/ars.2014.6097
Wang Y, Miao Y, Mir AZ, Cheng L, Wang L, Zhao L, Cui Q, Zhao W, Wang H (2016) Inhibition of beta-amyloid-induced neurotoxicity by pinocembrin through Nrf2/HO-1 pathway in SH-SY5Y cells. J Neurol Sci 368:223–230. https://doi.org/10.1016/j.jns.2016.07.010
Wardyn JD, Ponsford AH, Sanderson CM (2015) Dissecting molecular cross-talk between Nrf2 and NF-κB response pathways. Biochem Soc Trans 43:621–626. https://doi.org/10.1042/BST20150014
Xue B, Wu Y, Yin Z, Zhang H, Sun S, Yi T, Luo L (2005) Regulation of lipopolysaccharide-induced inflammatory response by glutathione S-transferase P1 in RAW264.7 cells. FEBS Lett 579:4081–4087
Yao J, Ge C, Duan D, Zhang B, Cui X, Peng S, Liu Y, Fang J (2014) Activation of the phase II enzymes for neuroprotection by ginger active constituent 6-dehydrogingerdione in PC12 cells. J Agric Food Chem 62:5507–5518. https://doi.org/10.1021/jf405553v
Yao J, Zhang B, Ge C, Peng S, Fang J (2015) Xanthohumol, a polyphenol chalcone present in hops, activating Nrf2 enzymes to confer protection against oxidative damage in PC12 cells. J Agric Food Chem 63:1521–1531. https://doi.org/10.1021/jf505075n
Yasuhara R, Miyamoto Y, Akaike T, Akuta T, Nakamura M, Takami M, Morimura N, Yasu K, Kamijo R (2005) Interleukin-1beta induces death in chondrocyte-like ATDC5 cells through mitochondrial dysfunction and energy depletion in a reactive nitrogen and oxygen species-dependent manner. Biochem J 389:315–323
Yu C, He Q, Zheng J, Li LY, Hou YH, Song FZ (2017) Sulforaphane improves outcomes and slows cerebral ischemic/reperfusion injury via inhibition of NLRP3 inflammasome activation in rats. Int Immunopharmacol 45:74–78. https://doi.org/10.1016/j.intimp.2017.01.034
Zhou Q, Chen B, Wang X, Wu L, Yang Y, Cheng X, Hu Z, Cai X, Yang J, Sun X, Lu W, Yan H, Chen J, Ye J, Shen J, Cao P (2016) Sulforaphane protects against rotenone-induced neurotoxicity in vivo: involvement of the mTOR, Nrf2, and autophagy pathways. Sci Rep 6:32206. https://doi.org/10.1038/srep32206
Acknowledgements
This work was supported by CNPq and FOPESQ/UFF.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no conflict of interest.
Electronic supplementary material
Figure S1
The effects of a treatment with SFN at 5 μM for different periods on (A) the levels of heme oxygenase-1 (HO-1) and on (B) the nuclear content of Nrf2 in SH-SY5Y cells. Data are shown as the mean ± SEM of three or five independent experiments each done in triplicate. One-way ANOVA followed by the post hoc Tukey’s test, *p < 0.05 different from the control group. (PDF 84 kb).
Figure S2
The silencing of the transcription factor nuclear factor erythroid 2-related factor 2 (Nrf2) by using small interfering RNA (siRNA) targeting Nrf2 (for 48 h) attenuated the effects of SFN on (A) the levels of heme oxygenase-1 (HO-1) and on (B) the levels of Nrf2 in the nucleus of SH-SY5Y cells exposed to SFN at 5 μM for 6 h and 3 h, respectively. * p < 0.05 different from the control cells transfected with scrambled control (NC) siRNA; ** p < 0.05 different from the cells transfected with scrambled control (NC) siRNA and exposed to SFN. (PDF 84 kb).
Rights and permissions
About this article
Cite this article
de Oliveira, M.R., Brasil, F.B. & Fürstenau, C.R. Sulforaphane Attenuated the Pro-Inflammatory State Induced by Hydrogen Peroxide in SH-SY5Y Cells Through the Nrf2/HO-1 Signaling Pathway. Neurotox Res 34, 241–249 (2018). https://doi.org/10.1007/s12640-018-9881-7
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12640-018-9881-7