Abstract
Prenatal treatment with the antiepileptic drug valproic acid (VPA) is associated with a significant risk of somatic anomalies, neurodevelopmental delays, and 7–10× increase in the incidence of autism spectrum disorders (ASD) in children. Rodents exposed to VPA in pregnancy show birth defects, deficits in neurodevelopment, and cognitive/social anomalies resembling those of ASD children. Mechanisms of VPA neurobehavioral toxicity are still unclear but as VPA is a non-selective inhibitor of histone deacetylases, epigenetic modifications are likely involved. This study was aimed to evaluate the transgenerational impact of prenatal VPA exposure on mouse early behavioral development, studying F1, F2, and F3 generations after VPA challenge on gestational day (GD) 10.5. We also analyzed in brain and in peripheral blood mononuclear cells the expression levels of different endogenous retrovirus (ERV) families, potential biomarkers of derailed brain development, since human ERVs have been implicated in the pathogenesis of neurodevelopmental disorders (NDDs) such as ASD. Somatic effects of VPA were evident only in F1 generation and more markedly in the female sex. Across F1 and F2 generations, VPA delayed righting reflex, increased motor activity, and reduced ultrasonic vocalizations. The behavioral changes in F3 are milder though in the same direction. VPA increased expression of most ERVs across the three generations in brain and blood. In utero VPA induced neurodevelopmental alterations more marked in the maternal lineage that persisted also in F3, suggesting ERVs as possible downstream effectors of the VPA epigenetic alterations.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Increasing evidence supports an association between prenatal exposure to antiepileptic drugs (AEDs) and increased risk of both physical anomalies and neurodevelopmental impairment [1, 2]. Most women with epilepsy require AEDs to control seizures for the entire length of the pregnancy; AEDs are also used to treat neuropathic pain, migraines, and psychiatric disorders. Among AEDs, intake of valproic acid (VPA) during the first trimester of pregnancy is associated with a significant risk of congenital malformations (primarily neural tube defects) and neurodevelopment delay in children. Specifically, prenatal exposure to VPA has been associated to lower IQ, motor, adaptive, and emotional problems [3,4,5], and with a 7–10× increase in relative risk for autism spectrum disorders (ASD) [6, 7].
Based on this clinical evidence, prenatal exposure to VPA has been proposed as a drug-induced model of ASD [8], and it has received increasing attention with regard to behavioral outcomes and mechanisms by which an environmental factor impact on early brain development.
Rodents exposed to VPA in utero show birth defects, deficits in neurodevelopment, and cognitive/social anomalies of varying degree depending on dose and time of administration [9, 10]. A single prenatal exposure to VPA, at a range of doses comprised between 350 and 800 mg/kg and at different embryonic time points, is able to induce significant behavioral changes: they include delayed reflex development, motor stereotypies, impaired social behavior, and learning deficits [8, 11, 12]. The mechanisms by which VPA causes malformations and neurotoxicity are still unclear; several hypotheses have been drawn, including increased production of free radicals, interference with cell proliferation/migration patterns, alterations of inflammatory and immunologic markers, and altered folate metabolism [13,14,15,16]. More importantly, the role of VPA in epigenetic regulation has come to light: VPA is a non-selective inhibitor of histone deacetylase of class I and II (HDAC1 and HDAC2) expressed in the brain [17]. Changes in genome activity and expression could be implicated in the adverse effects of VPA on brain development [18, 19], as shown for other environmental stressors [20,21,22]. The potential for VPA of acting through epigenetic mechanisms is also supported by a recent study indicating that the autism-like neurobehavioral phenotype shows transgenerational epigenetic inheritance through the paternal germline in F1 and F2 VPA-treated mice [23].
The main aim of the present study was to evaluate the multigenerational impact of prenatal VPA exposure on early behavioral patterns of laboratory mice, by studying F1, F2, and F3 generations after a single injection of VPA on gestational day (GD) 10.5 in F0. We focused on the first 2 weeks of mouse postnatal life for several reasons: (i) this developmental window offers the opportunity to identify early behavioral alterations/delays (motor competences and vocal patterns) and thus to set the ground for testing of early treatment and/or interventions; (ii) a large body of clinical evidence recently points to motor abnormalities as first signs of atypical development in genetic variants and idiopathic ASD [24,25,26,27] as well as in ASD high-risk infants [28], also stressing early motor milestones as potential tools in clinical practice; (iii) early motor deficits (easily measurable in rodent models) may influence development of functions that are critical for social communication development [29,30,31].
Besides early vocal and motor patterns, we also analyzed expression of different endogenous retrovirus (ERV) families, the major subset of retrotransposons, which are the relics of ancestral retroviral infection to germline cells; they comprise about 8% of the genome in humans and over 10% in mice and are stably integrated into the host cellular DNA [32, 33]. Even if the transposition of retroelements is deemed responsible for the evolution and the genomic instability [34], the vast majority of human ERV sequences are biochemically inert and silenced by host cellular machineries. Their activity is tightly regulated during the life cycle of each individual, and the active propagation and random insertion into genomic DNA lead to gene alterations, with consequent uncontrolled expression and possible involvement in various diseases, including cancer, and autoimmune and neurological and psychiatric disorders [35].
Specifically, recent studies have found aberrant transcriptional activation of ERVs in several neurological disorders (e.g., amyotrophic lateral sclerosis, schizophrenia, and bipolar disorders) that could be, in part, the result of neurodevelopmental alterations [35,36,37,38,39,40,41]. Based on their ability to be mobilized under specific stimuli, ERVs can be seen as spanning the bridge between genetic predisposition and environmental factors. Their responsiveness to environmental conditions is an intrinsic property that places them at the frontline of the gene-environment interaction. It is likely that ERVs serve important roles as regulatory elements in brain development controlling gene networks that become dysregulated in diseases [42,43,44].
This hypothesis together with the finding of altered expression of selected ERV families in children with neurodevelopmental disorders (NDDs) such as attention deficit hyperactivity disorder and ASD [45,46,47] supports the use of ERVs as candidate biomarkers for NDDs [48]. Furthermore, in agreement with the clinical findings, we have observed a marked increase of the expression of murine ERVs from the very early phases of development till adulthood both in the BTBR T+tf/J mouse strain (a widely used model of ASD) and in mice prenatally exposed to a single injection of 500 mg/kg VPA [49].
In F1, F2, and F3 generations in parallel with the behavioral assessment, we analyzed expression of several ERVs (ETnI, ETnII-α, ETnII-β, ETnII-γ, MusD, and IAP) on postnatal day (pnd) 7, an age at which postnatal ERV expression can be fully detected in blood and brain tissues [49].
Materials and Methods
Animals
Male and female mice of the CD-1 strain purchased from Harlan (San Pietro al Natisone, UD, Italy) were housed under standard animal housing conditions and reversed light cycle, as described in [49]. All studies were carried out in accordance with the European and Italian legislation (2010/63/EU, Dl 26/2014, specific authorization 223/2011-B to GC).
VPA Exposure in F0 Mothers
After breeding, females were inspected daily for the presence of the vaginal plug (GD 0). On GD 10.5, pregnant females were randomly assigned to one of the two treatments [Vehicle (VEH) 0.9% NaCl] and VPA, 500 mg/kg in VEH by subcutaneous injection as described in [49]. Proportion of term pregnancies, gestation length, litter size, sex ratio, and neonatal mortality were also measured to exclude potential effects of the treatment on reproductive performances.
The day of birth was defined as pnd 0.
Production of F1, F2, and F3 Generations
Offspring from 20 dams (10 VEH and 10 VPA) were used for assessment of VPA effects in F1. At adulthood, male-female pairs from F1 generation were bred to generate three F2 experimental groups to evaluate the differential contribution of the two VPA parental exposures on behavioral phenotype and ERV expression profile in the following generation. To generate F2-VPA offspring via the paternal lineage (F2-VPA/PL), we crossed male F1-VPA offspring with female F1-VEH offspring. To obtain F2-VPA offspring via the maternal lineage (F2-VPA/ML), we crossed female F1-VPA offspring with male F1-VEH offspring. F1 control males and females were crossed to obtain the F2-VEH lineage (F2-VEH) (see Fig. 2(a)).
To generate the three experimental groups of F3 generation, we crossed female F2-VPA/ML with male F2-VEH (F3-VPA/ML), male F2-VPA/ML with female F2-VEH (F3-VPA/PL), and, lastly, female F2-VEH with male F2-VEH (F3-VEH) (see Fig. 2(i)).
Only behaviorally, naive offspring were used for breeding and molecular analysis, thereby avoiding possible confounds arising from using handled breeders.
Behavioral Assessment in the Neonatal Stage of F1, F2, and F3 Offspring
For each generation, one female and one male offspring from each litter (F1: VEH = 20, VPA = 20; F2: VEH = 14, VPA/PL = 14, VPA/ML = 14; F3: VEH = 10, VPA/PL = 6, VPA/ML = 12) were tested on pnd 4, 7, 10, and 12. For identification purposes, on pnd 4, pups were tattooed on the paw with animal tattoo ink (Ketchum permanent Tattoo Inks green paste, Ketchum Manufacturing Inc., Brockville, ON, Canada).
All behavioral procedures were carried out during the dark phase of the cycle between 9:00 a.m. and 2:00 p.m. under red dim lights.
Recording of Ultrasonic Vocalizations in Isolated Pups
Ultrasonic vocalizations (USVs) are an important tool to assess emotional development and communication between mother and infants, as they elicit pup retrieval by the parents and maternal licking [50, 51]. On each day of testing, a single pup was placed into an empty glass container (diameter 5 cm; height 10 cm), placed inside a sound-attenuating Styrofoam box, and USVs were assessed during a 3-min test. An ultrasound microphone (Avisoft Ultrasound Gate condenser microphone capsule CM16, Avisoft Bioacoustics, Berlin, Germany) sensitive to frequencies of 10–180 kHz was placed through a hole the cover of the Styrofoam box (about 20 cm above the pup) to record USVs, settings as in [52]. Parameters analyzed for each test day included number and duration of calls, frequency, and amplitude at the maximum of the spectrum.
Spontaneous Movements and Righting Reflex
Concomitant with the USV recording on pnd 4, 7, 10, and 12, the spontaneous movements of the pups were also assessed. Frequency and duration of each behavioral item were analyzed by using NOLDUS OBSERVER software V 10 XT (Noldus Information Technology, Wageningen, NL, USA) to score the videos. In accordance with previous studies focused on neonatal rodent behavior [53, 54], the following behavioral patterns were scored: locomotion (general translocation of the body of at least 1 cm in the glass container), head rising (a single rising of the head up and forward), face washing (forepaws moving back and forth from the ears to the snout and mouth), wall climbing (alternating forelimb placing movements on the wall of the container), and curling (roll, vigorous side-to-side rolling movements while on the back). The righting reflex was assessed by placing the pup on its back over a flat surface: the time needed to return to the natural position (all four paws on the floor) was measured using a stopwatch. The reflex was tested once in each day of assessment with a cutoff latency of 60 s.
Somatic Growth
At the end of the 3-min recording session, each pup was assessed for somatic growth from pnd 4 to 12, as previously described [52, 53]. Each pup was weighed, its body and tail length and axillary temperature recorded.
Homing Test
On pnd 11, one female and one male offspring from each litter assigned to the different treatments (unhandled siblings of pups used for sensorimotor assessment) were separated from the dam and kept for 30 min in an incubator (Elmed Ginevri 0GB 1000, Roma, Italy) at 28 ± 1 °C. Individual pups were then transferred to a Plexiglas arena (36 × 22.5 cm, walls 10 cm high) maintained at 28 ± 1 °C, with the floor subdivided by black lines in 12 quadrants. Wood shavings from the home cage were evenly spread under the wire-mesh floor on one side of the arena (14 × 22.5 cm, goal arena) and the pup was placed close to the wall on the opposite side. The time taken by the pup to reach the goal area (containing nest litter) was recorded (cut off time 3 min), as described by [55]. In addition, the pup’s overall activity during the 3-min test period was analyzed by using NOLDUS OBSERVER software V 10 XT (Noldus Information Technology, Wageningen, NL, USA) to score the time spent in the goal area and locomotor activity by square crossings.
Evaluation of ERV Expression in Brain and Blood Samples of Mice from F1, F2, and F3 generations
At pnd 7, animals of both sexes (F1: VEH = 17, VPA = 16; F2: VEH = 4, VPA/PL = 10, VPA/ML = 10; F3: VEH = 6, VPA/PL = 8, VPA/ML = 4) were euthanized by decapitation; brains were removed from the skull, immediately frozen in dry ice, and stored at − 80 °C until use. Blood samples were collected and stored at − 80 °C in heparinized tubes.
Total RNA from brain and blood samples was extracted; retro-transcribed and obtained cDNA was used to perform quantitative real-time PCR in order to evaluate the transcriptional levels of six ERV families (ETnI, ETnII-α, ETnII-β, ETnII-γ, MusD, and IAP) as described in [49].
RNA Extraction from Blood and Brain Samples
Total RNA isolation from whole blood samples was performed using NucleoSpin RNA Blood kit (Machenery-Nagel, Dueren, Germany) according to the manufacturer’s instructions and starting from 200 μl. When the volume of the sample was less than 200 μl, it was added with phosphate-buffered saline. RNA isolation from brain samples was performed using NucleoSpinTriPrep (Machenery-Nagel, Dueren, Germany) according to the manufacturer’s instructions and starting from 30 mg or less of tissue. After adding the appropriate volume (10% w/v) of lysis buffer and 1 mM of 1,4-dithiothreitol (Sigma Aldrich, St. Louis, MO, USA), samples were homogenized using the plunger of a syringe and by passing through a syringe needle. Contaminating DNA was removed by a DNase treatment and all RNA samples were stored at − 80 °C until analysis was performed.
RT (Real-Time) PCR
DNase-treated RNA obtained from blood and brain samples was reverse-transcribed into cDNA using Improm-II Reverse Transcription System (Promega, Fitchburg, Wisconsin, USA) according to the manufacturer’s protocol. For the reaction, 250 ng of RNA obtained from brain samples and an amount of RNA corresponding to 5 μl of initial blood sample were used. The transcriptional levels of six ERV families (ETnI, ETnII-α, ETnII-β, ETnII-γ, MusD, and IAP) were quantitatively assessed by real-time PCR. The assays were performed in a Bio-rad instrument (CFX96 Real-Time System, Biorad, Hercules, CA, USA) using SYBR Green chemistry (iTaq Universal SYBR green Supermix, Biorad) with specific primer pairs.
To set-up the real-time reaction, a serial dilution (10-fold) was done to calculate efficiencies and correlation coefficient, by formula [efficiency = 10 (−1/slope)] and all primer pairs used showed an efficiency ranging 0.96 to 0.97.
Real-time PCR reaction included 0.20 μl of cDNA, forward and reverse primers at 150 nM each for ERVs and 10 μl of iTaq Universal SYBR green Supermix, in a total volume of 20 μl. The reaction was conducted for 1 cycle at 95 °C for 3 min, then for 40 cycles at 95 °C for 45 s and at 60 °C for 1 min. Each sample was analyzed in triplicate and a negative control (no template reaction) was included in each experiment, to check out any possible contamination. The housekeeping glyceraldehyde 3-phosphate dehydrogenase gene (GAPDH) was used to normalize the results. Each experiment was completed with a melting curve analysis to confirm the specificity of amplification and the lack of any non-specific product and primer dimer. Quantification was performed using the threshold cycle (Ct) comparative method: the relative expression was calculated as follows: 2− [∆Ct (sample) − ∆Ct (calibrator) = 2−∆∆Ct, where ∆Ct (sample) = [Ct (target gene) − Ct (housekeeping gene)]. For the analysis in brain and blood samples, the ∆Ct (calibrator) was the mean of ∆Ct of all brain or blood samples from VEH mice at pnd 7.
Statistical Analysis
Except for homing latency data analyzed by non-parametric Mann-Whitney test, all behavioral and somatic data were analyzed by a mixed model ANOVA [56] with repeated measures with prenatal treatment as the between-litter fixed factor, sex as the within-litter fixed factor, and pnd as the repeated measures factor.
The Mann-Whitney test was used to compare the ERVs’ transcriptional levels, in brain and blood samples within each generation and across them. For paired post hocs, either Bonferroni correction for six comparisons (Mann-Whitney) or Tukey test (ANOVA main effect or interactions) was applied and considered statistically significant when p < 0.05.
Finally, to estimate the strength of the association between ERVs expression and behavioral outcome and to evaluate whether this association was affected by VPA across generations, we initially performed two principal component analyses (PCA) separately, either within ERVs or within behavioral responses in the overall set of mice. First, we selected ETnII-β, ETnII-γ, MusD, and IAP families, applying natural-log transformation and two behavioral items, locomotion and USVs, the measurement that resulted more sensitive to VPA across generations. PCA allowed to create variables (components of PCA) mutually unrelated within either ERVs or behavior. Scores on the first three components within ERVs and on the two components within behavioral responses were computed, and correlation between ERVs and behavioral responses in the overall group and within each generation was estimated using the Pearson linear correlation coefficient.
Subsequently, a canonical correlation analysis (CCA) [57] was performed considering three components of ERVs on one side and the two components of behavioral responses on the other side in the overall group and within each generation. Furthermore, to disentangle the contribution of either maternal or paternal lineage, the same analysis was conducted first pooling both lineages and then excluding VPA/PL mice from F2 and F3 generations.
Results
VPA Affects Somatic and Behavioral Development of F1 Offspring
VPA did not affect body weight and temperature from pnd 4 to 12 (Supplementary Fig. 4 a–b), but significantly influenced both body and tail length, an effect more marked in the female sex [treatment × sex interaction, body length F(1, 18) = 6.94, p = 0.01; tail length F(1, 18) = 6.01, p = 0.02].
VPA female pups had shorter body length than VEH female pups on pnd 4 (p < 0.05), 7, and 10 [ps < 0.01, treatment × sex × age interaction F(3, 54) = 4.18, p = 0.0098, Fig. 1(a)].
F1 generation: somatic growth and spontaneous movements shown by VPA and VEH pups at different postnatal days of testing. (a) Body length. (b) Tail length. (c) Latency to right on a surface at pnd 4: VPA females showed a deficit in righting reflex. (d) Frequency of head rising episodes (a single rising of the head up and forward, values pooled across pnd 4–12). (e) Total duration of locomotion (values pooled across pnd 4–12). f Mean number of USVs. (g) Latency in homing test on pnd 11: VPA males waited for longer before reaching the nest scented target area. All data are expressed using box plots with dots for individual data except for a and b; N: F1-VEH = 20, F1-VPA = 20; *p < 0.05, **p < 0.01
Tail length was decreased in VPA pups [F(1, 18) = 7.76, p = 0.01]. Specifically, VPA male pups had shorter tail length on pnd 12 (p < 0.01), while VPA female pups had shorter tail length on pnd 4 (p < 0.05), 7, and 10 [ps < 0.01, treatment × sex × age interaction F(3, 54) = 4.04, p = 0.01] attaining the VEH values by pnd 12 (Fig. 1(b)). All VPA exposed offspring of both sexes (20 out of 20) at weaning showed the typical “crooked tail” phenotype (first signs of this malformation were evident from pnd 12).
As for sensorimotor development, latency to righting on a surface in VPA female pups was significantly longer than in VEH female pups at pnd 4 [p < 0.01, treatment × sex × age interaction F(3, 54) = 3.01, p = 0.03 Fig. 1(c)]. The analysis of spontaneous movements indicated a main effect of VPA on selected motor responses suggesting a hyperactive profile: VPA pups spent more time in locomotion than VEH pups [F(1, 18) = 6.12, p = 0.02, Fig. 1(e)]. In addition, VPA female pups exhibited higher head rising frequency than VEH females [p < 0.01, treatment × sex F(1, 18) = 5.27, p = 0.03, Fig. 1(d)].
While displaying these spontaneous movements, VPA pups tended to emit a lower number of calls than VEH [F(1, 18) = 3.34, p = 0.08, Fig. 1(f)]. Duration of calls evidenced a significant treatment × sex × pnd interaction [F(3, 54) = 3.71 p = 0.0168] with VPA females showing shorter call duration than VEH at pnd 10 (p < 0.05, Supplementary Fig. 4c).
On pnd 11 during the homing test, VPA male pups took longer to reach the nest area, indicative of worse performance than VEH pups (p < 0.05, Fig. 1(g)).
VPA Affects Behavioral Development of F2 and F3 Offspring
No effects on somatic growth were observed in F2 and F3 generations. In F2, some behavioral alterations were found in both parental lineages, while others were specific for either the PL or ML. In detail, F2-VPA/PL showed longer latencies of righting than VEH pups [p < 0.01, main effect F(2, 18) = 3.968, p < 0.05, Fig. 2(b)] and exhibited longer duration of curling than VEH (p < 0.01) and ML offspring on pnd 4 [p < 0.05, treatment × age F(6, 54) = 1.95, p = 0.08, Fig. 2(c)]. The increased duration of curling was possibly related to the deficit in righting reflex. In line with what observed in F1 generation, both VPA/ML and VPA/PL offspring spent more time in locomotion than VEH offspring [ps < 0.01, main effect F(2, 18) = 12.05, p = 0.0005, Fig. 2(d)). Similarly, both VPA parental lineages showed increased head rising movements in comparison to controls [ps < 0.01, main effect of F(2, 18) = 6.04, p = 0.0098, Fig. 2(e)]. Pnd 7 is the age at which this effect is larger [p < 0.01, treatment × age interaction F(6, 54) = 3.62, p = 0.0043].
F2 and F3 generations: spontaneous movements shown by pups of F2- and F3-VPA/PL (paternal lineage) and VPA/ML (maternal lineage) during a 3-min session at pnd 4, 7, 10, and 12. (a) Breeding used to generate F1 and F2 (PL and ML) offspring. (b) Latency to right on surface: VPA/PL showed a deficit in righting reflex. (c) Total duration of curling (roll, vigorous side-to-side rolling movements while on the back) on pnd 4: longer duration of curling in VPA/PL is in line with increased latency to righting. (d) Total duration of locomotion. (e) Frequency of head rising episodes. (f) Total duration of wall climbing (alternating forelimb placing movements on the wall of the container). (g) Frequency of face washing episodes (forepaws moving back and forth from the ears to the snout and mouth). (h) Mean number of USVs. (i) Breeding used to generate F3 (PL and ML) offspring. (l) Total duration of locomotion. (m) Mean number of USVs. All data (values pooled across pnd 4–12 except for b) are expressed using box plots with dots for individual data; N: F2-VEH = 14, F2-VPA/PL = 14, F2-VPA/ML = 14; F3-VEH = 10, F3-VPA/PL = 6, F3-VPA/ML = 12; *p < 0.05, **p < 0.01 either PL or ML vs Veh; $p < 0.05 ML vs PL
Two behavioral responses evidenced effects of antenatal VPA/ML. Wall climbing duration was longer in VPA/ML than VEH from pnd 7 to 12 [p < 0.05, main effect F(2, 18) = 3.815, p = 0.0416, Fig. 2(f)]. Face washing frequency was higher in VPA/ML than in VPA/PL pups at pnd 10 and 12 (p < 0.05, main effect F(2, 18) = 2.792, p = 0.08, Fig. 2(g)), whereas differences between VPA/ML and VEH just missed statistical significance.
VPA/PL pups emitted a lower number of USVs than VEH [p < 0.05, main effect F(2, 18) = 4.17, p = 0.03, Fig. 2(h)]. It is worth noting that also VPA/ML tended to vocalize less than VEH pups, an effect just missing statistical significance.
In F3 offspring, differences in time spent in locomotion between VPA/ML and VEH just missed statistical significance [main effect F(2, 11) = 2.34, p = 0.14, Fig. 2(l)]. VPA/PL emitted a lower number of ultrasounds compared to VEH [p < 0.05, main effect of treatment F(2, 10) = 2.88, p = 0.10, Fig. 2(m)).
Of note, in both F2 and F3 offspring, no significant sex differences were evidenced.
ERV Expression Is Modified by VPA Exposure in Brain and Blood Samples Within Each Generation
Figure 3 shows ERV expression levels after VPA exposure in brain (left panel) and blood samples (right panel) of F1, F2, and F3 mice at pnd 7.
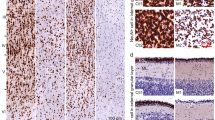
Expression levels of ERVs in brain and blood samples from VEH and VPA mice of F1, F2, and F3 generation at pnd 7. VPA prenatal exposure increased the activity of most of the ERVs in F1 (gray box plots) and F2 offspring (gray box plots, blue bold PL paternal lineage, red bold ML maternal lineage) in comparison to VEH offspring (white box plots), an increase maintained till the F3 generation (gray box plots, red PL paternal lineage, red ML maternal lineage, these are red because offspring of one F2-VPA/ML parent) both in brain and in blood tissues. Data are expressed using box plots, N: F1-VEH = 17, F1-VPA = 16; F2-VEH = 4, F2-VPA/PL = 10, F2-VPA/ML = 10; F3-VEH = 6, F3-VPA/PL = 8, F3-VPA/ML = 4
Overall, in F1, offspring VPA prenatal exposure markedly increased the transcriptional activity of all ERVs in comparison to VEH offspring both in brain (ps < 0.05) and in blood (ps < 0.05) tissue (Table 1). Interestingly within VPA offspring, females showed the highest levels of expression for most of the ERVs considered both in brain and blood samples (ps < 0.01, Supplementary Table 4), while no differences between sexes were observed in VEH mice.
In both brain and blood, F2 VPA mice (either PL or ML) showed higher levels of expression than VEH mice for all the ERVs families considered (ps < 0.05), and moreover, VPA/ML offspring showed significantly higher expression levels for most of the ERVs than VPA/PL (ps < 0.01, Table 1).
Within the VPA/ML group, females showed higher ERV expression compared to males both in brain and blood samples (ps < 0.01, Supplementary Table 4), whereas no sex differences were observed either within the VPA/PL or VEH groups.
In keeping with F1 and F2, higher levels of expression of most ERVs were found in F3-VPA/ML and VPA/PL groups both in brain and blood in comparison with VEH group (ps < 0.01, Table 1). Finally, in both brain and blood samples, VPA/ML expression levels were significantly higher than VPA/PL for all ERVs (ps < 0.01). Some differences in ERV expression levels between sexes were also identified in F2 and F3 of the VPA group (Supplementary Table 4).
ERV Expression Is Modified by VPA Exposure in Brain and Blood Samples Across Generations
Both in brain and blood, ERV expression was significantly higher in F1-VPA than in F2-VPA/PL for most of the ERVs (ps < 0.01, except for ETnI in brain), whereas F1-VPA and F2-VPA/ML values were substantially overlapping for all ERVs.
When comparing F2-VPA/ML with F3-VPA/ML, three out of the six families were significantly higher in F2 (EtnI, EtnII-β, EtnII-γ, ps < 0.01) in the blood; five out of the six families were significantly higher in F2 (EtnII-α, EtnII-β, EtnII-γ, MusD, and IAP, ps < 0.01) in the brain.
In the comparison between F2-VPA/ML and F3-VPA/PL, four out of the six families were significantly higher in F2 (EtnI, EtnII-β, MusD, IAP, ps < 0.01) in the blood; three out of the six families were significantly higher in F2 (EtnI, MusD, IAP, ps < 0.01) in the brain.
All paired comparisons are reported in Table 2.
Canonical Correlation Analysis
The CCA results are reported in Table 3. The canonical correlation between PCA components on ERVs and those on behavioral responses is moderate to strong in all generations; importantly, it improves in F2 and F3, when excluding PL. PCA data are shown in Supplementary Results and Supplementary Fig. 5.
Discussion
Gestational VPA exposure produced transgenerational changes in both behavioral development and ERV expression that last, with fading of epigenetic memories across generations, till the third one (F3). Offspring from MLs showed more marked transcriptional effects compared to PLs both in F2 and F3 generations.
Our data on early physical, sensorimotor, and behavioral screening of VPA effects in F1 are consistent with previous studies [15, 58]. Indeed, VPA treatment induced in pups of both sexes the tail malformation known as crooked tail phenotype [23, 59] together with hyperactivity previously observed in adulthood [11, 59, 60] and a weak reduction of vocalization rates [61,62,63].
Importantly, the behavioral effects by prenatal VPA upon mouse pups confirm that early motor impairments can be an important ASD feature. They now start to be considered as “core clinical feature”, potentially useful also for diagnostic purposes or phenotypic delineation [25, 64]. These impairments range from atypical righting (including inability to turn over) firstly evidenced in a retrospective study [65] to increased head turning movements [30] and laying and gait asymmetries [66, 67]. As a whole, it can be easily anticipated that such key role of motor domain will be certainly instrumental for preclinical studies in rodent models, and primarily for those interested in early phases of behavioral development because of the similarities of early motor and vocal repertoire between the two mammal species.
As our experimental design included both males and females, we could also identify sex differences in developmental effect of VPA that so far have been scarcely considered. F1-VPA female pups are delayed in somatic growth as well as in displaying a fully fledged righting reflex, indicative of a mild delay in integration between vestibular and motor systems, compensated later on [68]. In VPA female pups, head rising increased, an early sign of repetitive/stereotypic-like movements, already observed in adult female rats exposed prenatally to VPA [14]. In line with previous studies, F1-VPA male pups showed a deficit in early olfactory discrimination [11, 62, 63, 69]; a timely establishment of olfactory discrimination capabilities can be critical for development of adult social recognition, reportedly impaired in the VPA model [23, 62, 63].
In F1 generation, the direct prenatal exposure to VPA during fetal life increased expression of ERVs in both brain and blood, in agreement with our previous data [49], and in both sexes. The VPA effects, however, were significantly larger in females, in agreement with the larger epigenetic effect of prenatal VPA recently reported in female fetal brains, ascribed to sexually dimorphic trimethylation of H3K4 induced by VPA [70].
Some of the motor behavior alterations induced by VPA in F2 (both ML and PL) were already found altered in F1, namely increased locomotion and head rising. Interestingly, the magnitude of the VPA effects is comparable in both generations, and VEH values from F1 and F2 are substantially overlapping.
Besides locomotion and head rising, in F2 generation, additional behavioral patterns are influenced by VPA, with different profiles depending on whether VPA exposure came from the PL or ML. VPA effects in F2 ML offspring seem more in line with a hyperactive profile whereas those in F2 PL suggest delayed maturation of motor and vocal competences.
At the transcriptional level, VPA increased the expression of most ERVs in either F2-VPA/PL or F2-VPA/ML. VPA effects through ML resulted of greater magnitude than PL and entirely comparable to those detected in F1-VPA. The greater effectiveness of the ML in mediating VPA multigenerational effects is in agreement with the larger effects of VPA in females in F1: indeed, these same F1 females are dam breeders for F2-VPA/ML offspring and in our previous study the higher increases in ERV expression observed at pnd 7 persisted till adulthood [49].
As in F1 and F2, higher levels of ERV expression were also observed in tissues from F3-VPA offspring of both lineages, supporting a transgenerational effect of prenatal VPA exposure.
The behavioral data indicate that in F3 generation VPA influences the same domains affected in the previous generations, namely locomotion and vocalizations, inducing an increase in locomotion (in ML offspring) and a decrease in the number of USVs (in PL offspring). These F3 behavioral effects are undoubtedly milder that those observed in F2 and F1, and probably hampered by the limited sample size in these groups. However, canonical correlations of molecular and behavioral components support the view that F3 data, despite the limited number, are coherent with those from previous generations.
So far, data on transgenerational effects of VPA exposure were available for PL only and were focused on male offspring [23]: the rationale for this a priori choice was to exclude abnormal maternal nurturing behaviors in VPA-treated offspring (but such maternal behavior alterations have not been documented so far [15, 61]). By contrast, our experimental design allowed us, for the first time, to evaluate the neurotoxic effects of prenatal VPA exposure and potential effects on neurodevelopment in both sexes and throughout generations. It is worth of note that ASD prevalence in children exposed to VPA during pregnancy is characterized by an even (1:1) male to female ratio [71], so also VPA effects in females could be relevant for preclinical settings. Moreover, we were interested to evaluate the neurotoxicity and potential impact of a therapeutic agent used in reproductive age as VPA on the germline cells in both lineages, beyond the direct risk of VPA exposure for fetal neurodevelopment [72, 73].
Unexpectedly, in F1, prenatal VPA effects are larger in females than in males for somatic and motor development, as well as for ERVs expression. These results may appear in disagreement with previous data [10]; however, it is noteworthy that in most of the previous studies, only male data were reported [23, 60, 62, 63, 74,75,76]; when females were included, VPA effects were either different or of a minor extent from those of VPA males, but still significant [14, 15, 77]..Recent molecular data support a specific “vulnerability” of the female sex, as they indicate that some epigenetic effects induced by gestational VPA in offspring are greater in female than in male fetal brain [70]. For example, expression levels of androgen receptor in the developing cerebellum are more markedly altered by VPA in neonate females than in males [78].
Our data, also supported by correlational analysis, point to the importance of including females and MLs in prenatal/transgenerational VPA studies [10]. Differences between PL and ML as for transgenerational effects on neurodevelopment are still an underexplored field and they warrant further investigation [22].
Our study presents some limitations that need to be addressed in future studies. First, our experimental design, focused on ML, can be considered some-how sub-optimal for the study of PL, because of the absence of F3 offspring coming from F2-VPA/PL parents. Secondly, behavioral transmission of VPA effects through ML cannot be ruled out in the absence of systematic scoring of early maternal cares; extensive data, however, showed that maternal behavior is not altered in F0 VPA dams [15, 61], thus making it unlikely that it represents a target of VPA transgenerational effects. Finally, whether the observed early behavioral alterations are predictive of ASD-like phenotype at adulthood is not known.
Biological bases for the larger VPA effects on ERV expression in females within F1 and along MLs could include both VPA-induced downregulation of HDACs as well as other mechanisms not mediated by inhibition histone deacetylation, but by other transcription modulators (e.g., PAX6, Mecp2) [23, 79], involving early DNA damage [63] or mitochondrial DNA (mtDNA) defects [80,81,82]. To these mechanisms, the two sexes may result differently vulnerable, as it is the obvious case of mtDNA damage, to which female germline only is exposed (but see also [83]).
Furthermore, the increased expression of ERVs observed could be due to an increase in their copy number. Such intriguing hypothesis is in line with previous data showing that (i) in mice, ERVs can “cooperate” with other ERV and non-ERV elements (LINE) by a mechanism of complementation in trans, thus increasing their intrinsic capability to retrotranspose and, consequently to determine insertional mutagenesis in the germ line [84, 85]; (ii) in humans, it is known that—although the majority of ERVs are defective, fixed in the host, and ceased to proliferate millions of years ago—the most recently integrated ERV-K (HML2) continued to proliferate in the germline of our ancestors [86], inducing polymorphisms in the population [87,88,89], also with differential rate in the two sexes [90]; (iii) polymorphisms in humans were described also for ERV-H [91], that we have found highly expressed in ASD patients [45].
In our model, the ERVs copy number variations could occur in somatic as well as in germline cells, thus providing an explanation for the differences in ERVs expression between F1 and F2–F3 generations. A greater upregulated ERV expression in females could also be due to prominent rearrangement or new insertions in X rather than in Y chromosome. Further studies on copy number variations of ERVs sequences across generations and on the epigenetic status could contribute to unravel this point.
Putative pathogenic effects mediated by ERVs in neurological and psychiatric conditions in humans have been already described [92]. ERVs may alter cellular function in the developing brain by means of multiple mechanisms, including modulation of DNA stability and transcription, alteration of cell signaling pathways, and activation of immune system [93,94,95,96]. Our previous study showed in offspring directly exposed to VPA in utero, together with ERV overexpression, high levels of proinflammatory cytokines, such as IL-1β, IL-6, and TNF-α, already from intrauterine life and in the neonatal brain. A hypothesis worth to be investigated in future transgenerational in vivo studies concerns the implication of immuno-inflammatory pathways in the epigenetic effects of VPA, in line with the maternal immune activation hypothesis [22].
Proofs that ERVs are mechanistically involved in neurobehavioral alterations caused by VPA in pregnancy are still lacking. Anyhow, the substantially comparable profile of ERV expression in brain and blood tissues in pups exposed to VPA across generations, candidate ERVs blood transcriptional levels as a stable peripheral biomarker, even at early life stages, of derailed brain development.
References
Meador KJ, Baker GA, Finnell RH, Kalayjian LA, Liporace JD, Loring DW, Mawer G, Pennell PB et al (2006) In utero antiepileptic drug exposure: fetal death and malformations. Neurology 67(3):407–412. https://doi.org/10.1212/01.wnl.0000227919.81208.b2
Bromley RL, Mawer GE, Briggs M, Cheyne C, Clayton-Smith J, Garcia-Finana M, Kneen R, Lucas SB et al (2013) The prevalence of neurodevelopmental disorders in children prenatally exposed to antiepileptic drugs. J Neurol, Neurosurg,Psychiatry 84(6):637–643. https://doi.org/10.1136/jnnp-2012-304270
Baker GA, Bromley RL, Briggs M, Cheyne CP, Cohen MJ, Garcia-Finana M, Gummery A, Kneen R, Loring DW, Mawer G, Meador KJ, Shallcross R, Clayton-Smith J, Liverpool, Manchester Neurodevelopment G (2015) IQ at 6 years after in utero exposure to antiepileptic drugs: a controlled cohort study. Neurology 84 (4):382–390. doi:https://doi.org/10.1212/WNL.0000000000001182
Cohen MJ, Meador KJ, Browning N, Baker GA, Clayton-Smith J, Kalayjian LA, Kanner A, Liporace JD et al (2011) Fetal antiepileptic drug exposure: motor, adaptive, and emotional/behavioral functioning at age 3 years. Epilepsy Behav : E&B 22(2):240–246. https://doi.org/10.1016/j.yebeh.2011.06.014
Cohen MJ, Meador KJ, Browning N, May R, Baker GA, Clayton-Smith J, Kalayjian LA, Kanner A, Liporace JD, Pennell PB, Privitera M, Loring DW, group Ns (2013) Fetal antiepileptic drug exposure: adaptive and emotional/behavioral functioning at age 6 years. Epilepsy Behav : E&B 29 (2):308–315. doi:https://doi.org/10.1016/j.yebeh.2013.08.001
Christensen J, Gronborg TK, Sorensen MJ, Schendel D, Parner ET, Pedersen LH, Vestergaard M (2013) Prenatal valproate exposure and risk of autism spectrum disorders and childhood autism. Jama 309(16):1696–1703. https://doi.org/10.1001/jama.2013.2270
Ornoy A, Weinstein-Fudim L, Ergaz Z (2015) Prenatal factors associated with autism spectrum disorder (ASD). Reprod Toxicol 56:155–169. https://doi.org/10.1016/j.reprotox.2015.05.007
Wagner GC, Reuhl KR, Cheh M, McRae P, Halladay AK (2006) A new neurobehavioral model of autism in mice: pre- and postnatal exposure to sodium valproate. J Autism Dev Disord 36(6):779–793. https://doi.org/10.1007/s10803-006-0117-y
Roullet FI, Lai JK, Foster JA (2013) In utero exposure to valproic acid and autism--a current review of clinical and animal studies. Neurotoxicol Teratol 36:47–56. https://doi.org/10.1016/j.ntt.2013.01.004
Nicolini C, Fahnestock M (2017) The valproic acid-induced rodent model of autism. Exp Neurol. https://doi.org/10.1016/j.expneurol.2017.04.017
Schneider T, Przewlocki R (2005) Behavioral alterations in rats prenatally exposed to valproic acid: animal model of autism. Neuropsychopharmacology: Official Publication of the American College of Neuropsychopharmacology 30(1):80–89. https://doi.org/10.1038/sj.npp.1300518
Kataoka S, Takuma K, Hara Y, Maeda Y, Ago Y, Matsuda T (2013) Autism-like behaviours with transient histone hyperacetylation in mice treated prenatally with valproic acid. Int J Neuropsychopharmacol 16(1):91–103. https://doi.org/10.1017/S1461145711001714
Manent JB, Jorquera I, Mazzucchelli I, Depaulis A, Perucca E, Ben-Ari Y, Represa A (2007) Fetal exposure to GABA-acting antiepileptic drugs generates hippocampal and cortical dysplasias. Epilepsia 48(4):684–693. https://doi.org/10.1111/j.1528-1167.2007.01056.x
Schneider T, Roman A, Basta-Kaim A, Kubera M, Budziszewska B, Schneider K, Przewlocki R (2008) Gender-specific behavioral and immunological alterations in an animal model of autism induced by prenatal exposure to valproic acid. Psychoneuroendocrinology 33(6):728–740. https://doi.org/10.1016/j.psyneuen.2008.02.011
Kazlauskas N, Campolongo M, Lucchina L, Zappala C, Depino AM (2016) Postnatal behavioral and inflammatory alterations in female pups prenatally exposed to valproic acid. Psychoneuroendocrinology 72:11–21. https://doi.org/10.1016/j.psyneuen.2016.06.001
Kolozsi E, Mackenzie RN, Roullet FI, deCatanzaro D, Foster JA (2009) Prenatal exposure to valproic acid leads to reduced expression of synaptic adhesion molecule neuroligin 3 in mice. Neuroscience 163(4):1201–1210. https://doi.org/10.1016/j.neuroscience.2009.07.021
Fukuchi M, Nii T, Ishimaru N, Minamino A, Hara D, Takasaki I, Tabuchi A, Tsuda M (2009) Valproic acid induces up- or down-regulation of gene expression responsible for the neuronal excitation and inhibition in rat cortical neurons through its epigenetic actions. Neurosci Res 65(1):35–43. https://doi.org/10.1016/j.neures.2009.05.002
Tung EW, Winn LM (2010) Epigenetic modifications in valproic acid-induced teratogenesis. Toxicol Appl Pharmacol 248(3):201–209. https://doi.org/10.1016/j.taap.2010.08.001
Kawanai T, Ago Y, Watanabe R, Inoue A, Taruta A, Onaka Y, Hasebe S, Hashimoto H, Matsuda T, Takuma K (2016) Prenatal exposure to histone deacetylase inhibitors affects gene expression of autism-related molecules and delays neuronal maturation. Neurochem Res 41 (10):2574–2584. doi:https://doi.org/10.1007/s11064-016-1969-y
Rodgers AB, Morgan CP, Leu NA, Bale TL (2015) Transgenerational epigenetic programming via sperm microRNA recapitulates effects of paternal stress. Proc Natl Acad Sci USA 112(44):13699–13704. https://doi.org/10.1073/pnas.1508347112
Vassoler FM, White SL, Schmidt HD, Sadri-Vakili G, Pierce RC (2013) Epigenetic inheritance of a cocaine-resistance phenotype. Nat Neurosci 16(1):42–47. https://doi.org/10.1038/nn.3280
Weber-Stadlbauer U, Richetto J, Labouesse MA, Bohacek J, Mansuy IM, Meyer U (2017) Transgenerational transmission and modification of pathological traits induced by prenatal immune activation. Mol Psychiatry 22(1):102–112. https://doi.org/10.1038/mp.2016.41
Choi CS, Gonzales EL, Kim KC, Yang SM, Kim JW, Mabunga DF, Cheong JH, Han SH et al (2016) The transgenerational inheritance of autism-like phenotypes in mice exposed to valproic acid during pregnancy. Sci Rep 6:36250. https://doi.org/10.1038/srep36250
Bishop SL, Farmer C, Bal V, Robinson EB, Willsey AJ, Werling DM, Havdahl KA, Sanders SJ, Thurm A (2017) Identification of developmental and behavioral markers associated with genetic abnormalities in autism spectrum disorder. Am J Psychiatry 174 (6):576–585. doi:https://doi.org/10.1176/appi.ajp.2017.16101115
Wilson RB, Enticott PG, Rinehart NJ (2018) Motor development and delay: advances in assessment of motor skills in autism spectrum disorders. Curr Opin Neurol 31(2):134–139. https://doi.org/10.1097/WCO.0000000000000541
Buja A, Volfovsky N, Krieger AM, Lord C, Lash AE, Wigler M, Iossifov I (2018) Damaging de novo mutations diminish motor skills in children on the autism spectrum. Proc Natl Acad Sci USA 115(8):E1859–E1866. https://doi.org/10.1073/pnas.1715427115
Craig F, Lorenzo A, Lucarelli E, Russo L, Fanizza I, Trabacca A (2018) Motor competency and social communication skills in preschool children with autism spectrum disorder. Autism Res : Off J Int Soc Autism Res. https://doi.org/10.1002/aur.1939
Varcin KJ, Jeste SS (2017) The emergence of autism spectrum disorder: insights gained from studies of brain and behaviour in high-risk infants. Curr Opin Psychiatry 30(2):85–91. https://doi.org/10.1097/YCO.0000000000000312
LeBarton ES, Iverson JM (2016) Associations between gross motor and communicative development in at-risk infants. Infant Behav Dev 44:59–67. https://doi.org/10.1016/j.infbeh.2016.05.003
Martin KB, Hammal Z, Ren G, Cohn JF, Cassell J, Ogihara M, Britton JC, Gutierrez A et al (2018) Objective measurement of head movement differences in children with and without autism spectrum disorder. Mol Autism 9:14. https://doi.org/10.1186/s13229-018-0198-4
Harris SR (2017) Early motor delays as diagnostic clues in autism spectrum disorder. Eur J Pediatr 176(9):1259–1262. https://doi.org/10.1007/s00431-017-2951-7
Lander ES, Linton LM, Birren B, Nusbaum C, Zody MC, Baldwin J et al (2001) Initial sequencing and analysis of the human genome. Nature 409(6822):860–921. https://doi.org/10.1038/35057062
Waterston RH, Lindblad-Toh K, Birney E, Rogers J, Abril JF, Agarwal P et al (2002) Initial sequencing and comparative analysis of the mouse genome. Nature 420(6915):520–562. https://doi.org/10.1038/nature01262
Gorbunova V, Boeke JD, Helfand SL, Sedivy JM (2014) Human genomics. Sleeping dogs of the genome. Science 346 (6214):1187–1188. doi:https://doi.org/10.1126/science.aaa3177
Kury P, Nath A, Creange A, Dolei A, Marche P, Gold J, Giovannoni G, Hartung HP, Perron H (2018) Human endogenous retroviruses in neurological diseases. Trends Mol Med 24 (4):379–394. doi:https://doi.org/10.1016/j.molmed.2018.02.007
Brattås PL, Jönsson ME, Fasching L, Nelander Wahlestedt J, Shahsavani M, Falk R, Falk A, Jern P, Parmar M, Jakobsson J (2017) TRIM28 Controls a gene regulatory network based on endogenous retroviruses in human neural progenitor cells. Cell Rep 18 (1):1–11. doi:https://doi.org/10.1016/j.celrep.2016.12.010
Manghera M, Ferguson J, Douville R (2014) Endogenous retrovirus-K and nervous system diseases. Curr Neurol Neurosci Rep 14(10):488. https://doi.org/10.1007/s11910-014-0488-y
Perron H, Hamdani N, Faucard R, Lajnef M, Jamain S, Daban-Huard C, Sarrazin S, LeGuen E, Houenou J, Delavest M, Moins-Teisserenc H, Bengoufa D, Yolken R, Madeira A, Garcia-Montojo M, Gehin N, Burgelin I, Ollagnier G, Bernard C, Dumaine A, Henrion A, Gombert A, Le Dudal K, Charron D, Krishnamoorthy R, Tamouza R, Leboyer M (2012) Molecular characteristics of human endogenous retrovirus type-W in schizophrenia and bipolar disorder. Transl Psychiatry 2:e201. doi:https://doi.org/10.1038/tp.2012.125
Slokar G, Hasler G (2015) Human endogenous retroviruses as pathogenic factors in the development of schizophrenia. Front Psychiatry 6:183. doi:https://doi.org/10.3389/fpsyt.2015.00183
Douville R, Liu J, Rothstein J, Nath A (2011) Identification of active loci of a human endogenous retrovirus in neurons of patients with amyotrophic lateral sclerosis. Ann Neurol 69(1):141–151. https://doi.org/10.1002/ana.22149
Douville RN, Nath A (2017) Human endogenous retrovirus-K and TDP-43 expression bridges ALS and HIV neuropathology. Front Microbiol 8:1986. doi:https://doi.org/10.3389/fmicb.2017.01986
Douville RN, Nath A (2014) Human endogenous retroviruses and the nervous system. Handb Clin Neurol 123:465–485. https://doi.org/10.1016/B978-0-444-53488-0.00022-5
Hurst TP, Magiorkinis G (2015) Activation of the innate immune response by endogenous retroviruses. J Gen Virol 96(Pt 6):1207–1218. https://doi.org/10.1099/jgv.0.000017
Hurst TP, Magiorkinis G (2017) Epigenetic control of human endogenous retrovirus expression: focus on regulation of long-terminal repeats (LTRs). Viruses 9 (6). doi:https://doi.org/10.3390/v9060130
Balestrieri E, Arpino C, Matteucci C, Sorrentino R, Pica F, Alessandrelli R, Coniglio A, Curatolo P, Rezza G, Macciardi F, Garaci E, Gaudi S, Sinibaldi-Vallebona P (2012) HERVs expression in autism spectrum disorders. PloS one 7 (11):e48831. doi:https://doi.org/10.1371/journal.pone.0048831
Balestrieri E, Pitzianti M, Matteucci C, D'Agati E, Sorrentino R, Baratta A, Caterina R, Zenobi R et al (2014) Human endogenous retroviruses and ADHD. World J Biol Psychiatry 15(6):499–504. https://doi.org/10.3109/15622975.2013.862345
Balestrieri E, Cipriani C, Matteucci C, Capodicasa N, Pilika A, Korca I, Sorrentino R, Argaw-Denboba A et al (2016) Transcriptional activity of human endogenous retrovirus in Albanian children with autism spectrum disorders. New Microbiol 39(3):228–231
Nadeau MJ, Manghera M, Douville RN (2015) Inside the envelope: endogenous retrovirus-K ENV as a biomarker and therapeutic target. Front Microbiol 6:1244. doi:https://doi.org/10.3389/fmicb.2015.01244
Cipriani C, Ricceri L, Matteucci C, De Felice A, Tartaglione AM, Argaw-Denboba A, Pica F, Grelli S, Calamandrei G, Sinibaldi Vallebona P, Balestrieri E (2018) High expression of endogenous retroviruses from intrauterine life to adulthood in two mouse models of autism spectrum disorders. Sci Rep 8 (1):629. doi:https://doi.org/10.1038/s41598-017-19035-w
Brunelli SA, Hofer MA (2007) Selective breeding for infant rat separation-induced ultrasonic vocalizations: developmental precursors of passive and active coping styles. Behav Brain Res 182(2):193–207. https://doi.org/10.1016/j.bbr.2007.04.014
Zimmerberg B, Rosenthal AJ, Stark AC (2003) Neonatal social isolation alters both maternal and pup behaviors in rats. Dev Psychobiol 42(1):52–63. https://doi.org/10.1002/dev.10086
Scattoni ML, Gandhy SU, Ricceri L, Crawley JN (2008) Unusual repertoire of vocalizations in the BTBR T+tf/J mouse model of autism. PloS one 3(8):e3067. https://doi.org/10.1371/journal.pone.0003067
De Felice A, Scattoni ML, Ricceri L, Calamandrei G (2015) Prenatal exposure to a common organophosphate insecticide delays motor development in a mouse model of idiopathic autism. PloS one 10(3):e0121663. https://doi.org/10.1371/journal.pone.0121663
De Filippis B, Ricceri L, Laviola G (2010) Early postnatal behavioral changes in the Mecp2-308 truncation mouse model of Rett syndrome. Genes, Brain, Behav 9(2):213–223. https://doi.org/10.1111/j.1601-183X.2009.00551.x
Ricceri L, Markina N, Valanzano A, Fortuna S, Cometa MF, Meneguz A, Calamandrei G (2003) Developmental exposure to chlorpyrifos alters reactivity to environmental and social cues in adolescent mice. Toxicol Appl Pharmacol 191(3):189–201
Chiarotti F, Alleva E, Bignami G (1987) Problems of test choice and data analysis in behavioral teratology: the case of prenatal benzodiazepines. Neurotoxicol Teratol 9(2):179–186
Misic B, Sporns O (2016) From regions to connections and networks: new bridges between brain and behavior. Curr Opin Neurobiol 40:1–7. https://doi.org/10.1016/j.conb.2016.05.003
Podgorac J, Pesic V, Pavkovic Z, Martac L, Kanazir S, Filipovic L, Sekulic S (2016) Early physical and motor development of mouse offspring exposed to valproic acid throughout intrauterine development. Behav Brain Res 311:99–109. https://doi.org/10.1016/j.bbr.2016.05.023
Kim P, Park JH, Kwon KJ, Kim KC, Kim HJ, Lee JM, Kim HY, Han SH et al (2013) Effects of Korean red ginseng extracts on neural tube defects and impairment of social interaction induced by prenatal exposure to valproic acid. Food Chem Toxy: Int J Publ Br Ind Biol Res Assoc 51:288–296. https://doi.org/10.1016/j.fct.2012.10.011
Kim JW, Seung H, Kwon KJ, Ko MJ, Lee EJ, Oh HA, Choi CS, Kim KC et al (2014) Subchronic treatment of donepezil rescues impaired social, hyperactive, and stereotypic behavior in valproic acid-induced animal model of autism. PloS one 9(8):e104927. https://doi.org/10.1371/journal.pone.0104927
Barrett CE, Hennessey TM, Gordon KM, Ryan SJ, McNair ML, Ressler KJ, Rainnie DG (2017) Developmental disruption of amygdala transcriptome and socioemotional behavior in rats exposed to valproic acid prenatally. Mol Autism 8:42. https://doi.org/10.1186/s13229-017-0160-x
Servadio M, Melancia F, Manduca A, di Masi A, Schiavi S, Cartocci V, Pallottini V, Campolongo P et al (2016) Targeting anandamide metabolism rescues core and associated autistic-like symptoms in rats prenatally exposed to valproic acid. Transl Psychiatry 6(9):e902. https://doi.org/10.1038/tp.2016.182
Servadio M, Manduca A, Melancia F, Leboffe L, Schiavi S, Campolongo P, Palmery M, Ascenzi P et al (2017) Impaired repair of DNA damage is associated with autistic-like traits in rats prenatally exposed to valproic acid. Eur Neuropsychopharmacol: J Eur Coll Neuropsychopharmacol. https://doi.org/10.1016/j.euroneuro.2017.11.014
May T, Cornish K, Rinehart NJ (2016) Gender profiles of behavioral attention in children with autism spectrum disorder. J Atten Disord 20 (7):627–635. doi:https://doi.org/10.1177/1087054712455502
Teitelbaum P, Teitelbaum O, Nye J, Fryman J, Maurer RG (1998) Movement analysis in infancy may be useful for early diagnosis of autism. Proc Natl Acad Sci USA 95(23):13982–13987
Esposito G, Venuti P, Maestro S, Muratori F (2009) An exploration of symmetry in early autism spectrum disorders: analysis of lying. Brain Dev 31(2):131–138. https://doi.org/10.1016/j.braindev.2008.04.005
Eggleston JD, Harry JR, Hickman RA, Dufek JS (2017) Analysis of gait symmetry during over-ground walking in children with autism spectrum disorder. Gait Posture 55:162–166. https://doi.org/10.1016/j.gaitpost.2017.04.026
Fox WM (1965) Reflex-ontogeny and behavioural development of the mouse. Anim Behav 13(2):234–241
Roullet FI, Wollaston L, Decatanzaro D, Foster JA (2010) Behavioral and molecular changes in the mouse in response to prenatal exposure to the anti-epileptic drug valproic acid. Neuroscience 170(2):514–522. https://doi.org/10.1016/j.neuroscience.2010.06.069
Konopko MA, Densmore AL, Krueger BK (2017) Sexually dimorphic epigenetic regulation of brain-derived neurotrophic factor in fetal brain in the valproic acid model of autism spectrum disorder. Dev Neurosci. https://doi.org/10.1159/000481134
Rasalam AD, Hailey H, Williams JH, Moore SJ, Turnpenny PD, Lloyd DJ, Dean JC (2005) Characteristics of fetal anticonvulsant syndrome associated autistic disorder. Dev Med Child Neurol 47(8):551–555
Fujimura K, Mitsuhashi T, Takahashi T (2017) Adverse effects of prenatal and early postnatal exposure to antiepileptic drugs: validation from clinical and basic researches. Brain Dev 39 (8):635–643. doi:https://doi.org/10.1016/j.braindev.2017.03.026
Gotlib D, Ramaswamy R, Kurlander JE, DeRiggi A, Riba M (2017) Valproic acid in women and girls of childbearing age. Curr Psychiatry Rep 19 (9):58. doi:https://doi.org/10.1007/s11920-017-0809-3
Moldrich RX, Leanage G, She D, Dolan-Evans E, Nelson M, Reza N, Reutens DC (2013) Inhibition of histone deacetylase in utero causes sociability deficits in postnatal mice. Behav Brain Res 257:253–264. https://doi.org/10.1016/j.bbr.2013.09.049
Yang EJ, Ahn S, Lee K, Mahmood U, Kim HS (2016) Early behavioral abnormalities and perinatal alterations of PTEN/AKT pathway in valproic acid autism model mice. PloS one 11 (4):e0153298. doi:https://doi.org/10.1371/journal.pone.0153298
Zhang R, Zhou J, Ren J, Sun S, Di Y, Wang H, An X, Zhang K et al (2018) Transcriptional and splicing dysregulation in the prefrontal cortex in valproic acid rat model of autism. Reprod Toxicol 77:53–61. https://doi.org/10.1016/j.reprotox.2018.01.008
Anshu K, Nair AK, Kumaresan UD, Kutty BM, Srinath S, Laxmi TR (2017) Altered attentional processing in male and female rats in a prenatal valproic acid exposure model of autism spectrum disorder. Autism Res: Off J Int Soc Autism Res 10(12):1929–1944. https://doi.org/10.1002/aur.1852
Perez-Pouchoulen M, Miquel M, Saft P, Brug B, Toledo R, Hernandez ME, Manzo J (2016) Prenatal exposure to sodium valproate alters androgen receptor expression in the developing cerebellum in a region and age specific manner in male and female rats. Int J Dev Neurosci: Off J Int Soc Dev Neurosci 53:46–52. https://doi.org/10.1016/j.ijdevneu.2016.07.001
Kim KC, Choi CS, Kim JW, Han SH, Cheong JH, Ryu JH, Shin CY (2016) MeCP2 modulates sex differences in the postsynaptic development of the valproate animal model of autism. Mol Neurobiol 53 (1):40–56. doi:https://doi.org/10.1007/s12035-014-8987-z
Finsterer J, Scorza FA (2017) Effects of antiepileptic drugs on mitochondrial functions, morphology, kinetics, biogenesis, and survival. Epilepsy Res 136:5–11. https://doi.org/10.1016/j.eplepsyres.2017.07.003
Chen H, Dzitoyeva S, Manev H (2012) Effect of valproic acid on mitochondrial epigenetics. Eur J Pharmacol 690(1–3):51–59. https://doi.org/10.1016/j.ejphar.2012.06.019
Komulainen T, Lodge T, Hinttala R, Bolszak M, Pietila M, Koivunen P, Hakkola J, Poulton J et al (2015) Sodium valproate induces mitochondrial respiration dysfunction in HepG2 in vitro cell model. Toxicology 331:47–56. https://doi.org/10.1016/j.tox.2015.03.001
Pei L, Wallace DC. Mitochondrial etiology of neuropsychiatric disorders. Biological Psychiatry 83 (9):722–730. doi:https://doi.org/10.1016/j.biopsych.2017.11.018
Maksakova IA, Romanish MT, Gagnier L, Dunn CA, van de Lagemaat LN, Mager DL (2006) Retroviral elements and their hosts: insertional mutagenesis in the mouse germ line. PLoS genetics 2(1):e2. https://doi.org/10.1371/journal.pgen.0020002
Zhang Y, Maksakova IA, Gagnier L, van de Lagemaat LN, Mager DL (2008) Genome-wide assessments reveal extremely high levels of polymorphism of two active families of mouse endogenous retroviral elements. PLoS genetics 4(2):e1000007. https://doi.org/10.1371/journal.pgen.1000007
Bannert N, Kurth R (2006) The evolutionary dynamics of human endogenous retroviral families. Ann Rev Genomics Hum Genet 7:149–173. https://doi.org/10.1146/annurev.genom.7.080505.115700
Marchi E, Kanapin A, Magiorkinis G, Belshaw R (2014) Unfixed endogenous retroviral insertions in the human population. J Virol 88(17):9529–9537. https://doi.org/10.1128/JVI.00919-14
Wildschutte JH, Williams ZH, Montesion M, Subramanian RP, Kidd JM, Coffin JM (2016) Discovery of unfixed endogenous retrovirus insertions in diverse human populations. Proc Nat Acad Sci USAm 113(16):E2326–E2334. https://doi.org/10.1073/pnas.1602336113
Burmeister T, Ebert AD, Pritze W, Loddenkemper C, Schwartz S, Thiel E (2004) Insertional polymorphisms of endogenous HERV-K113 and HERV-K115 retroviruses in breast cancer patients and age-matched controls. AIDS Res Hum Retrovir 20(11):1223–1229. https://doi.org/10.1089/aid.2004.20.1223
Cakmak Guner B, Karlik E, Marakli S, Gozukirmizi N (2018) Detection of HERV-K6 and HERV-K11 transpositions in the human genome. Biomed Rep 9(1):53–59. https://doi.org/10.3892/br.2018.1096
Guliyev M, Yilmaz S, Sahin K, Marakli S, Gozukirmizi N (2013) Human endogenous retrovirus-H insertion screening. Mol Med Rep 7(4):1305–1309. https://doi.org/10.3892/mmr.2013.1295
Lucchina L, Depino AM (2014) Altered peripheral and central inflammatory responses in a mouse model of autism. Autism Res: Off J Int Soc Autism Res 7(2):273–289. https://doi.org/10.1002/aur.1338
Tai AK, Lin M, Chang F, Chen G, Hsiao F, Sutkowski N, Huber BT (2006) Murine Vbeta3+ and Vbeta7+ T cell subsets are specific targets for the HERV-K18 Env superantigen. J Immunol 177(5):3178–3184
Perron H, Dougier-Reynaud HL, Lomparski C, Popa I, Firouzi R, Bertrand JB, Marusic S, Portoukalian J et al (2013) Human endogenous retrovirus protein activates innate immunity and promotes experimental allergic encephalomyelitis in mice. PloS one 8(12):e80128. https://doi.org/10.1371/journal.pone.0080128
Firouzi R, Rolland A, Michel M, Jouvin-Marche E, Hauw JJ, Malcus-Vocanson C, Lazarini F, Gebuhrer L et al (2003) Multiple sclerosis-associated retrovirus particles cause T lymphocyte-dependent death with brain hemorrhage in humanized SCID mice model. J Neurovirol 9(1):79–93. https://doi.org/10.1080/13550280390173328
Perron H, Jouvin-Marche E, Michel M, Ounanian-Paraz A, Camelo S, Dumon A, Jolivet-Reynaud C, Marcel F et al (2001) Multiple sclerosis retrovirus particles and recombinant envelope trigger an abnormal immune response in vitro, by inducing polyclonal Vbeta16 T-lymphocyte activation. Virology 287(2):321–332. https://doi.org/10.1006/viro.2001.1045
Acknowledgements
The authors thank Luigia Cancemi for expert animal care and Cosimo Curianò for his assistance in graphical editing. This work was supported by ISS 13/cal 508 “Identification of early markers in mouse models of autism spectrum disorders: role of endogenous retroviruses.”
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
All studies were carried out in accordance with the European and Italian legislation (2010/63/EU, Dl 26/2014, specific authorization 223/2011-B to GC).
Conflict of Interest
The authors declare that they have no conflict of interest.
Electronic Supplementary Material
ESM 1
(DOCX 25 kb)
Supplementary Fig. 4
F1 generation: a) body weight and b) body temperature shown by VPA- and VEH pups at different postnatal days of testing; c) Mean duration of USVs: VPA females showed shorter duration of calls than VEH at pnd 10. (PDF 882 kb)
Supplementary Fig. 5
Left panel: Scatterplots of first component obtained by PCA from two behavioral variables, locomotion and USVs (1st PCA comp Behaviour, y axis) and first component obtained by PCA from four ERV families, ETnII-β, ETnII-γ, MusD and IAP (1st PCA comp ERVs, x axis) across generations when all data are included in the analysis (i.e. both ML and PL datasets for F2 and F3); Right panel: Scatterplots of the same behavioural and ERV PCA components across generations after excluding PL datasets (from both F2 and F3 generations). Note how PL values were those closer to VEH ones: excluding them it makes treatment groups more distinguishable. (PDF 55 kb)
ESM 2
(PDF 5 kb)
Rights and permissions
About this article
Cite this article
Tartaglione, A.M., Cipriani, C., Chiarotti, F. et al. Early Behavioral Alterations and Increased Expression of Endogenous Retroviruses Are Inherited Across Generations in Mice Prenatally Exposed to Valproic Acid. Mol Neurobiol 56, 3736–3750 (2019). https://doi.org/10.1007/s12035-018-1328-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12035-018-1328-x