Abstract
Left ventricular remodeling appears to be a critical link between cardiac injury and the development and progression of heart failure with reduced ejection fraction (HFrEF). Several drug and device therapies that modify and reverse the remodeling process in patients with HFrEF are closely associated with improvement in clinical outcomes. Reverse remodeling, including partial or complete recovery of systolic function and structure, is possible but its determinants are incompletely understood. Methods to predict reverse remodeling in response to therapy are not well defined. Though non-invasive imaging techniques remain the most widely used methods of assessing reverse remodeling, serum biomarkers are now being investigated as more specific, mechanistically driven, and clinically useful predictors of reverse remodeling. Biomarkers that reflect myocyte stretch and stress, myocyte injury and necrosis, inflammation and fibrosis, and extracellular matrix turnover may be particularly valuable for predicting pathophysiologic changes and prognosis in individual patients. Their use may ultimately allow improved application of precision medicine in chronic HF.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
By recent estimates, chronic heart failure (HF) affects nearly 6 million adults and costs approximately $31 billion annually in the USA alone [1]. There are several evidence-based drug and device therapies that improve left ventricular (LV) systolic function and overall clinical outcomes in patients with HF with reduced ejection fraction (HFrEF), while no such therapeutic options have proven benefits in HF with preserved ejection fraction (HFpEF) [2–4]. The subset of patients with HFrEF that experiences partial or complete recovery of systolic function represents a clinical phenotype that may be distinct from that of HFrEF without recovery and will be the focus of this report [5, 6]. This phenotype is not well understood and there are limited data regarding the underlying biology, natural history, prognosis, and need for long-term therapies in patients with recovery of LV systolic function. It would be useful to define strategies to predict myocardial recovery and identify patients in whom recovery may occur. Additionally, timely identification of those who are not likely to recover may lead to earlier acceleration of therapies to optimize and ultimately alter clinical outcomes.
Definitions of Reverse Remodeling and Myocardial Recovery
HFrEF is a broad phenotypic description of cardiac dysfunction and symptoms, which describes an end result of systolic dysfunction due to a variety of etiologies. In this pathway to HF, LV remodeling appears to be a critical link between cardiac injury and the development and progression of HFrEF.
LV remodeling describes typically adverse changes in LV composition and structure that occur in response to mechanical stress or injury and neurohormonal activation, eventually leading to altered LV geometry and abnormal function. Such changes on the molecular, cellular, and interstitial levels are marked by cardiomyocyte hypertrophy, abnormal excitation-contraction coupling and contractile function, and alterations in the extracellular matrix (ECM) [7]. Therapies with the greatest impact on clinical outcomes in HF are those that modify the underlying pathophysiological process of LV remodeling; in fact, drug and device therapies with proven clinical benefit in HFrEF lead to reverse remodeling, characterized by reduction in LV volumes and mass and improvement in systolic function [2–4].
While there is no gold standard definition of reverse remodeling or myocardial recovery, Mann et al. have proposed the best used definition to date that structural recovery involving partial reversal of changes in cardiomyocyte biology and ECM composition reflects “reverse remodeling” or “myocardial remission,” while “myocardial recovery” implies the normalization of both cardiac structure and function, with freedom from clinical HF events [7, 8]. However, the term reverse remodeling is broadly used in the literature to describe any degree of cardiac structural recovery, including full myocardial recovery, and will be used as such here. Reverse remodeling appears to be a central surrogate marker of future clinical outcomes [9], and early recognition may have important implications for therapeutic decision-making.
Methods of Assessing Reverse Remodeling
The most well-established methods of assessing reverse remodeling and phenotyping HF patients are based on non-invasive imaging techniques that evaluate changes in LV geometry and function [10]. LV ejection fraction (LVEF) is the most commonly used parameter for assessment of cardiac function, and both end-systolic and end-diastolic LV volumes have been even more closely linked with response to therapy and prognosis [11]. There is no universal imaging definition of reverse remodeling, but many studies have used statistically significant increases in LVEF or decreases in LV dimensions or volumes, while others have defined cut-offs for increases in LVEF (by 5–20 %) and/or decreases in LV dimensions or volumes (by 10–20 %) with a change ≥15 % often being considered significant [12].
Currently, transthoracic echocardiography is the imaging modality of choice for assessment of LV remodeling in both clinical and research applications, primarily due to its relatively low cost, safety, and broad availability. Estimates of LVEF and LV volumes using 2-dimensional echocardiography may be subject to variability due to technical limitations and operator-dependent errors, and though contrast-enhanced echocardiography and real-time 3-dimensional echocardiography have improved accuracy and reproducibility, their use is limited by the lack of widespread availability [13, 14].
Cardiac magnetic resonance (CMR) imaging provides greater spatial and temporal resolution, and contrast-enhanced CMR with assessment of late gadolinium enhancement has been shown to predict reversibility of adverse LV remodeling [15]. On the basis of these observations and others, CMR is considered the gold standard for non-invasive measurement of functional and volumetric parameters. Its use as a research tool and in clinical practice has grown in recent years, but its general applicability remains limited by cost and availability of specialized expertise.
A major limitation of these current methods of assessing remodeling and reverse remodeling is that they rely on the identification of overt structural changes, which may occur late in the course of disease progression and potentially outside the window for therapeutic intervention; earlier recognition of these processes could significantly alter therapeutic approaches and improve clinical outcomes. Furthermore, although these imaging techniques can demonstrate changes in cardiac structure and function or identify the presence of fibrosis, neither echocardiography nor currently used CMR techniques can fully reflect the underlying biology of remodeling or reverse remodeling. It would be useful, therefore, to identify additional surrogate markers that reflect unique mechanistic pathways of remodeling or reverse remodeling earlier in the disease process.
Cardiac Biomarkers Associated with Reverse Remodeling
The clinical use of serum biomarkers in HF management, including for the identification of LV remodeling, has increased in recent years. The most clinically useful biomarkers meet the following criteria: they are easy to obtain with accuracy and precision, relatively inexpensive, easily interpreted, provide consistent and generalizable information, add knowledge beyond what is already available, and most importantly, reflect underlying biological processes [16].
Several HF biomarkers, most notably the natriuretic peptides (NPs), have demonstrated clinical utility in HF and play important roles in its diagnosis and management [17–19]. There are limited clinical data, however, regarding the use of biomarkers to predict reverse remodeling, and this is an area that is still under active investigation.
Biomarkers of particular interest are those that highlight major biological processes underlying HF pathogenesis and remodeling, such as (1) markers of myocyte stretch and stress (e.g. B-type natriuretic peptide and its amino-terminal pro-peptide equivalent); (2) indicators of myocyte injury (e.g. cardiac troponins T and I); (3) markers of inflammation and fibrosis (e.g. soluble suppression of tumorigenicity 2, galectin-3); and (4) extracellular matrix proteins (e.g. matrix metalloproteinases, tissue inhibitors of metalloproteinases, and collagen-related serum peptides).
Myocyte Stretch and Stress: Natriuretic Peptides
The NPs, B-type natriuretic peptide (BNP), and its amino-terminal pro-peptide equivalent (NT-proBNP) are secreted from cardiomyocytes in response to myocyte stretch due to increased pressure or volume. They have both been established as useful biomarkers for the diagnosis of HF, for determining prognosis, and potentially for monitoring response to and guiding therapy [20]. Concentrations of NPs decrease with proven HF treatments and lower achieved concentrations are associated with improved clinical outcomes [21].
A subgroup analysis of 116 patients with serial echocardiograms in the ProBNP Outpatient Tailored Chronic Heart Failure (PROTECT) study, a trial to evaluate the use of NT-proBNP-guided chronic HF management, explored the relationship between NT-proBNP and LV remodeling. Final achieved NT-proBNP concentration after 10 months of aggressive HF management was positively correlated with final LV end-diastolic and LV end-systolic volume indices and inversely correlated with final LVEF; in multivariable analysis, achieved log-NT-proBNP concentrations were predictive of the direction and magnitude of LV remodeling. In addition, NT-proBNP-guided therapy was associated with improvement in LVEF, LV end-diastolic volume index, E/e’, and right ventricular systolic function and pressure [22]. Furthermore, NT-proBNP non-responders (failure to achieve NT-proBNP ≤1000 pg/mL following HF therapy) often did not improve, or improved to a lesser extent than did responders, in measures of LV remodeling (Fig. 1) [23]. Cross-sectional CMR imaging studies of patients with HFrEF of ischemic etiology have similarly shown that higher NT-proBNP concentrations are associated with parameters of adverse LV remodeling and RV dysfunction, but longitudinal analyses are lacking [24, 25]. Just as neurohormonal antagonists reduce NP concentrations, there is evidence that cardiac resynchronization therapy (CRT) leads to an early and sustained reduction in NT-proBNP, which is associated with improvement in LV volumes and LVEF [26].
Echocardiographic results stratified on the basis of NT-proBNP response (achieved concentration ≤1000 pg/mL) vs. non-response (achieved concentration >1000 pg/mL). Non-responders were less likely to demonstrate favorable reverse remodeling after a mean of 10 months of HF care. HF heart failure, LVEDVi left ventricular end-diastolic volume index, LVEF left ventricular ejection fraction, LVESVi left ventricular end-systolic volume index, NT-proBNP N-terminal pro-B-type natriuretic peptide. Reproduced with permission from [23]
These findings suggest that NT-proBNP concentrations might be useful non-invasive indicators of LV remodeling and cardiac function. However, in the only study to date to evaluate prediction of reverse remodeling, as defined by (1) increase in LVEF ≥15 %, OR (2) increase in LVEF ≥10 % plus decrease in LV end-systolic diameter index ≥ 20 % or in LV end-systolic volume index ≥40 %, NT-proBNP was not found to be an independent predictor [12]. In this study of 304 patients, investigators evaluated clinical characteristics and biomarkers (NT-proBNP, sST2, galectin-3 and highly sensitive cardiac troponin T), deriving and then externally validating the ST2-R2 score for the prediction of LV reverse remodeling. Though NT-proBNP is not included in this score, a close link between NPs and clinical outcomes with or without concurrent demonstration of LV remodeling is well established and it is possible that NP measurements are more sensitive than imaging techniques in reflecting response to therapy.
Myocyte Injury: Cardiac Troponins
Cardiac troponins (cTn) I and T are proteins that are specific for myocardial injury, whether it is due to obstructive coronary artery disease or to other etiologies of cardiac necrosis. Two forms of troponin assays are available, conventional (clinically widely available), and highly sensitive (clinically available in Europe, but otherwise primarily used for research purposes in the United States). When measured using a highly sensitive assay, abnormal concentrations of cTn are detectable in almost all patients with HF, even in the absence of ischemia or underlying coronary artery disease [27]. In chronic HF, elevated cTn is a marker of increased risk for progressive LV dysfunction and worse clinical outcomes with increased mortality [28–31].
Concentrations of cTn have been associated with parameters of LV remodeling in HFrEF of both ischemic and non-ischemic etiologies. In an early small study of 60 patients with idiopathic dilated cardiomyopathy, decrease in cTnT over time was associated with decrease in LV cavity size and increase in LVEF by echocardiography, as well as fewer cardiovascular (CV) events [29]. A substudy of PROTECT that included 99 patients with HFrEF of various etiologies similarly described an association between an increase in cTnI, adverse clinical outcomes, and deleterious LV remodeling based on echocardiographic parameters [32]. In another post hoc retrospective analysis of 378 patients with myocardial infarction (MI) in the Evaluation of MCC-135 for Left Ventricular Salvage in Acute Myocardial Infarction (EVOLVE) study, higher concentrations of cTnI 72 hours after percutaneous coronary intervention predicted adverse clinical outcomes, as well as large infarct size and low LVEF as measured by SPECT imaging [33]. A more recent larger registry-based study of 1307 patients with LVEF <45 % after MI found that lower peak cTnI was a significant predictor of recovery of systolic function at follow-up echocardiography [34]. A retrospective analysis of the Prediction of ICD Treatment Study (PREDICTS), multicenter international study found that in 231 patients with HFrEF after MI, higher peak cTn was an independent risk factor for persistent LV systolic dysfunction. The best-performing model to predict recovery of LVEF to (1) >35 % included peak cTn, LVEF at the time of MI, length of hospital stay, prior MI, and lateral wall motion abnormalities and (2) >50 % included peak cTn, LVEF at the time of MI, prior MI, and ventricular fibrillation and/or cardiac arrest at presentation; these models were validated in a second cohort of 236 patients [35].
Though these findings suggest a role for cTn as a potential predictor of reverse remodeling, like NT-proBNP, it was not independently associated with reverse remodeling in the ST2-R2 score mentioned above [12]. A similar caveat regarding cTn’s close link to clinical outcomes applies, however, and it may prove to be more useful in future investigations of reverse remodeling.
Inflammation and Fibrosis: sST2 and Galectin-3
Several novel biomarkers reflect interstitial processes that are important in LV remodeling and may provide useful information regarding reverse remodeling and the potential for myocardial recovery. Two such markers that reflect inflammation, fibrosis, and LV remodeling are soluble suppression of tumorigenicity 2 (ST2) and galectin-3.
Soluble ST2
ST2 is a member of the interleukin-1 receptor family with both transmembrane (ST2L) and soluble (sST2) isoforms and is expressed in cardiomyocytes, cardiac fibroblasts, and vascular endothelial cells. Cell culture and animal models have shown that sST2 is released in response to cardiomyocyte stress [36], and other cellular and in vivo experiments of LV hypertrophy and HF have shown that its secretion by endothelial cells is correlated with diastolic load, as reflected by LV end-diastolic pressure, but not with LV volumes or systolic wall stress [37].
Animal studies have suggested that paracrine interactions of ST2 and its ligand interleukin-33 (IL-33) are part of a cardioprotective signaling system involved in LV remodeling after myocardial injury and volume overload. IL-33 production is mechanically induced in cardiac fibroblasts, and its interaction with ST2L blocks pro-hypertrophic stimuli in cardiomyocytes. A murine model demonstrated that ST2-null mice had increased LV hypertrophy and fibrosis in response to pressure overload, and treatment with recombinant IL-33 was protective in wild-type mice only [38]. The same study reported that sST2 blocked the anti-hypertrophic effects of IL-33, indicating that it functions as a soluble decoy receptor that sequesters and inhibits IL-33 (Fig. 2). A subsequent study demonstrated that sST2 partially inhibited the protective effects of IL-33 against hypoxia-induced apoptosis of cardiomyocytes and confirmed in a post-MI murine model that IL-33/ST2 signaling decreases fibrosis and improves LV function [39]. These data indicate that sST2 expression is induced by cardiomyocyte stress and mitigates a cardioprotective effect of IL-33/ST2 signaling on LV remodeling.
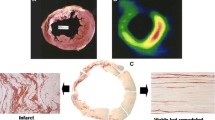
IL-33/ST2 signaling is cardioprotective in vivo. a Representative H&E and Sirius red stains and b quantitative analyses of samples from each group. ST2-null mice developed more cardiomyocyte hypertrophy and cardiac fibrosis after TAC than did WT mice. Treatment with IL-33 significantly reduced these changes in WT mice, but not in ST2-null mice. c Gross measurement of heart weight normalized to body weight was consistent with the histomorphometric analyses. d Echocardiographic analysis at 4 weeks after operation demonstrated increased LV mass, LV wall thickness, and reduced fractional shortening in ST2-null mice. Treatment with IL-33 reduced hypertrophy only in WT mice. IL-33 caused no significant change under non-stress conditions in vivo. Scale bar 10 μm. White and black bars indicate sham-operated and TAC, respectively. *P < 0.05 versus non-operated control (b, d) or sham-operated WT (c); §P < 0.05 versus the same treatment in WT; †P < 0.05 versus sham in the same group; #P < 0.05. C non-operated control, LV left ventricular, TAC transverse aortic constriction, WT wild type. Adapted with permission from [38]
Clinical studies have identified sST2 as an independent predictor of adverse clinical outcomes and mortality in patients with chronic HF [40–44] and suggested that it is particularly powerful when used in combination with NT-proBNP [43, 45]. A head-to-head comparison of sST2 and galectin-3 in a cohort of 876 patients with chronic HFrEF demonstrated that incorporation of sST2 into a model for all-cause mortality, already including clinical variables and NT-proBNP, improved risk stratification, while galectin-3 did not [46]. Cross-sectional echocardiographic analyses have demonstrated relationships between sST2 and cardiac structure and function that complement the basic science studies and clinical outcome results, identifying associations between higher sST2 concentrations and greater LV cavity size, lower LVEF, and worse RV function in diverse patient populations [47, 48].
Longitudinal studies have provided additional insight into the utility of sST2 as a therapeutic target or as a marker of remodeling. In a cohort of 100 patients admitted with acute MI, higher serum sST2 was correlated with lower LVEF and greater infarct size at baseline and at 24-week follow-up; subsequent LV remodeling, defined as increases in LV volumes, occurred only in those patients with high baseline sST2 and was attenuated by treatment with eplerenone (though treatment did not lower sST2 concentrations) [49]. A substudy of medication effects in the 151 patients enrolled in the PROTECT study found that those patients with low sST2 treated with high-dose beta-blocker had the lowest CV event rate [50]. Further analysis of the same cohort demonstrated that more time spent with sST2 below a threshold of 35 ng/mL predicted decrease in LV end-diastolic volume index, a marker of reverse remodeling [51]. Building upon these findings, the ST2-R2 score to predict reverse remodeling ultimately included sST2 in addition to other clinical variables; the final model designated points for sST2 <48 ng/mL (3 points), non-ischemic etiology (5 points), absence of left bundle branch block (4 points), HF duration <12 months (2 points), baseline LVEF <24 % (1 point), and beta-blocker treatment (2 points), with a greater total score associated with higher likelihood of reverse remodeling [12]. The study cohort was subsequently expanded to include 569 patients from three international cohorts, in whom the ST2-R2 score appropriately predicted reverse remodeling and also provided information about mortality [52].
Galectin-3
Galectin-3 is a β-galactoside-binding lectin that is secreted by activated cardiac macrophages during phagocytosis. Its role in cardiac fibrosis was first described in a rat model of hypertensive HF, in which progression to HF was associated with increased expression of galectin-3 in hypertrophied hearts [53]. Galectin-3 was primarily found in activated myocardial macrophages, with binding sites in cardiac fibroblasts and the ECM. It induced cardiac fibroblast proliferation and reduction in LVEF in association with altered collagen production, marked by an increased ratio of collagen type I compared to type III (the two most abundant collagen components of the ECM).
In another murine model of aldosterone and high-salt-treated rats, galectin-3 overexpression was associated with increased collagen type I synthesis, vascular hypertrophy, inflammation, and fibrosis, which were reversed by treatment with spironolactone or modified citrus pectin [54]. Aldosterone treatment increased galectin-3 expression, inflammation, and collagen type I in wild-type mice but not in galectin-3-null mice; these data suggested that galectin-3 is required for vascular inflammatory and fibrotic response to aldosterone, and furthermore, may be reversed by mineralocorticoid receptor antagonist (MRA) administration. Similarly, in a mouse model of hyperaldosterone- and hypertension-induced cardiac fibrosis, BNP expression was blunted and galectin-3 expression was increased; treatment with eplerenone reversed these findings [55]. Another study found that angiotensin II infusion or transverse aortic constriction caused LV hypertrophy, fibrosis, and systolic dysfunction in wild-type mice, while galectin-3-null mice developed LV hypertrophy without fibrosis or dysfunction [56]. In the same study, pharmacologic inhibition of galectin-3 in hypertensive rats attenuated fibrosis and LV dysfunction and resulted in downregulation of collagen production (both type I and type III) and also attenuated the progression of cardiac remodeling in a mouse model of increased afterload. On the basis of these findings and other confirmatory experiments, galectin-3 has been implicated in the progression of HF via mediation of cardiac fibrosis and ECM remodeling and has also been identified as a therapeutic target or marker for the reversal of fibrosis in HF.
Several clinical trials have shown that galectin-3 is associated with adverse outcomes and mortality in patients with chronic HF [57–60], though galectin-3 is a more powerful prognostic indicator in HFpEF than in HFrEF [61], and this association appears to be attenuated in the presence of NT-proBNP [62, 63]. As noted previously, a head-to-head comparison of sST2 and galectin-3 suggested that sST2 provides additive predictive information for all-cause mortality in combination with clinical variables and NT-proBNP, while galectin-3 does not [46]. There are other data suggesting that galectin-3 concentrations predict changes in LV volumes and LVEF, but studies have been conflicting. In the PROTECT substudy, higher galectin-3 concentrations at serial measurements were associated with adverse CV events, while lower galectin-3 concentrations were associated with increase in LVEF at follow-up echocardiography at a mean of 10 months; no significant effects of medications on galectin-3 levels were observed, however [60]. Similarly, in a study of 240 patients with HF (97 % with HFrEF) who underwent serial echocardiography, lower baseline galectin-3 concentration was associated with decrease in LV end-diastolic volume at 3 months, even after adjustment for clinical risk factors [64]. These findings are in contrast, however, to an earlier study in which higher galectin-3 levels were associated with all-cause mortality in patients with chronic HFrEF, but there were no relationships between galectin-3 and echocardiographic indices including LV end-diastolic volume index and LVEF [65]. Similarly, in a cohort of 100 patients with acute MI and LV systolic dysfunction, baseline galectin-3 had no correlation with LVEF or LV volumes as measured by CMR, or with change in any of these parameters between baseline and 24 weeks [66]. Galectin-3 was not included in the recently developed ST2-R2 score for reverse remodeling, as it was not independently associated with improvement in remodeling parameters when other clinical variables and biomarkers were added to the multivariable model [12].
Importantly, there have thus far been no studies in humans demonstrating that medications associated with reverse remodeling can improve galectin-3 levels. In the CMR study mentioned above, aldosterone blockade with eplerenone was associated with a rise in galectin-3 concentration [66], and in a substudy of the Controlled Rosuvastatin Multinational Study in Heart Failure (CORONA), aldosterone antagonist use was associated with higher galectin-3 concentration [67], but both studies may be underpowered to assess for these drug effects. Most recently, a substudy of Heart Failure: A Controlled Trial Investigating Outcomes of Exercise Training (HF-ACTION) and a substudy of PROTECT both found no interaction between galectin-3 and clinical treatment effects of MRA [68, 69]. Some studies have observed that patients with elevated baseline galectin-3 were less likely to respond to medical therapy, specifically to angiotensin II receptor blockers (ARBs) and statins [58, 67]. In the context of CRT, however, data are conflicting. In a substudy of 654 patients with mildly symptomatic HF in the Multicenter Automatic Defibrillator Implantation Trial with Cardiac Resynchronization Therapy (MADIT-CRT), elevated baseline galectin-3 was an independent predictor of adverse clinical outcomes and identified patients who derived a larger benefit from CRT [70], while in another substudy of the Cardiac Resynchronization in Heart Failure (CARE-HF) trial of patients with HFrEF and cardiac dyssynchrony, elevated galectin-3 was associated with adverse long-term outcomes and increased LV end-systolic volume, but concentrations did not change over 18 months of follow-up and did not predict response to CRT [71]. In patients with advanced HF requiring mechanical circulatory support, baseline galectin-3 levels were elevated and significantly higher in those who later died, but did not decrease in response to therapy by 30 days post-implantation [72].
Before galectin-3 can be used either as a marker of clinical response or as a marker of reverse remodeling, the answer to whether or not galectin-3 concentration changes in response to therapy must be more precisely defined. Clinical trials have identified the utility of galectin-3 as a marker of increased risk, however, and elevated galectin-3 may identify a particularly high-risk phenotype that is refractory to available therapies.
Extracellular Matrix Proteins: MMP9, TIMP1, BMP1, PICP/PIIINP
ECM components are constantly deposited and degraded; imbalance in these processes can lead to abnormal LV remodeling and subsequent LV systolic dysfunction. The alterations in ECM composition are marked by dysregulated collagen homeostasis and increase in type I collagen deposition, as well as cardiac fibroblast proliferation and activation that ultimately leads to reduced cardiac compliance, chamber dilation, cardiomyocyte hypertrophy, apoptosis, and fibrosis [73]. Fibrosis occurs in response to cardiomyocyte stress, such as pressure or volume overload, neurohormonal activation, and ischemia/infarction. Some of the key enzymes and inhibitors involved in these processes have been identified as potential markers of reverse remodeling and myocardial recovery, a select group of which is described here.
MMP9 and TIMP1
Matrix metalloproteinases (MMPs) are a family of zinc-dependent endopeptidases that are responsible for tissue remodeling by degrading structural elements of the ECM and processing other non-ECM substrates. MMP9, first termed 92-kDa type IV collagenase or gelatinase B, is one of the family members that can cleave collagen; it is secreted by several different types of cells, including neutrophils, macrophages, and fibroblasts. It is positively regulated by multiple factors and is inhibited by tissue inhibitors of metalloproteinases (TIMPs); TIMP1 inhibits both pro-MMP9 and its active form [74].
MMP9 activity has been associated with various CV processes, including hypertension, atherosclerosis, and MI, and is increased in both ischemic and dilated cardiomyopathies [75–77]. In a cross-sectional analysis of 699 Framingham Study participants with no prior HF or MI, it was also associated with increased LV dimensions and wall thickness in men [78]. Increased MMP9 activity is associated with compensatory hypertrophy in response to hypertension and fibrosis after MI, but studies have pointed to both beneficial and deleterious effects of MMP9 on LV remodeling. In a murine model of MI, MMP9-null mice had increased expression of other MMPs and TIMP1, fewer macrophages, less collagen accumulation in the infarcted areas, and smaller increases in LV cavity dimensions [79], and in another similar model, MMP9-null mice had more neovascularization and improved LV function [80]. Surprisingly, however, transgenic overexpression of MMP9 in mouse macrophages after MI was also associated with attenuated inflammatory response and improved LVEF [81]. The conflicting results suggest that imbalances between MMPs and TIMPs may be associated with alterations in ECM degradation, contributing to LV remodeling via regulation of both pro- and anti-inflammatory phenotypes at different points in the disease process. Several neurohormonal antagonists decrease MMP9 expression and activity, including beta-blockers, ACE inhibitors, ARBs, and MRAs, indicating that its expression is modifiable and responsive to therapeutic intervention [74].
Since the balance between levels and activities of MMP9 and TIMP1 varies depending on the stage of disease or progression of HF, they may be attractive markers to track LV remodeling and reverse remodeling. Additional clinical data are needed to support their use as biomarkers for this purpose.
BMP1
Fibrillar collagens types I and III are produced by cardiac fibroblasts and are the main collagenous components of both normal and fibrotic cardiac tissues. They are secreted into the ECM as procollagen precursors and require propeptide removal before mature collagen fibrils can form and assemble. Bone morphogenetic protein 1 (BMP1) belongs to a family of tolloid-like proteinases that are involved in the maturation and assembly of fibrillar collagen by cleavage of procollagen C-terminal propeptides and were originally called procollagen C-proteinases (PCPs) [82, 83]. BMP1 has since been shown to regulate various aspects of ECM assembly, including formation of collagen cross-linking and activation of signaling molecules such as TGF-β; these actions are controlled by substrate-specific enhancer molecules in the absence of many endogenous inhibitors [84]. The crucial role of BMP1 in the processing of ECM proteins and collagen deposition has led to interest in its potential use as a therapeutic target for the prevention of fibrosis and as a biomarker of remodeling and reverse remodeling.
Several studies have linked BMP1 to cardiac fibrosis and mediators of fibrosis, but results have been conflicting. In a mouse model of MI, expression of both BMP1 and secreted frizzled related protein 2 (Sfrp2), which is proposed to enhance BMP1 activity, was increased; Sfrp2-null mice had less fibrosis and significantly improved cardiac function [85]. A similar rat model of MI also demonstrated that expression of BMP1 and collagen types I and II was upregulated in areas of infarction, consistent with the role of BMP1 in procollagen biosynthesis and maturation [86]. In a series of experiments described in the same report, however, Sfrp2 was shown to inhibit type I procollagen processing and maturation, inhibit type I collagen deposition, and eventually significantly reduce LV fibrosis and improve LV function. Studies have also shown that expression of PCP enhancers in cardiac fibroblasts is stimulated by aldosterone-induced fibrosis and blocked by the presence of spironolactone [87, 88]. Though inconclusive, these experiments provide evidence that BMP1 activity may be associated with remodeling effects, and furthermore, these effects may be modified by medical therapy.
BMP1 has the potential to be a promising marker of LV remodeling and reverse remodeling, but further understanding of its regulation in the context of cardiac fibrosis is needed and its clinical utility remain to be seen.
PICP and PIIINP
Two of the propeptides that are products of collagen processing, C-terminal propeptide of procollagen type I (PICP) and N-terminal propeptide of procollagen type III (PIIINP), are markers of collagen turnover.
In patients with dilated or ischemic cardiomyopathy, serum PIIINP was associated with collagen type III deposition and was independently associated with mortality [89]. However, in the substudy of CARE-HF mentioned above, like galectin-3, PIIINP was associated with adverse outcomes, but PIIINP concentrations were not associated with LV remodeling parameters or response to CRT and did not change over time [71]. In a small study of 65 patients with hypertension, serum PICP correlated with the extent of collagen type I deposition assessed on endomyocardial biopsy and was highest in those with HF, suggesting that it might be a useful marker of myocardial fibrosis [90]. There is also evidence that PICP may reflect LV remodeling. A recent study of 132 patients with symptomatic HFrEF demonstrated an association between PICP and BNP levels, as well as indices of LV cavity size and diastolic function [91]. In another study of 48 patients who suffered an initial acute MI, there was a sustained increase in serum PICP for up to nearly 12 months post-infarction and those patients with a greater absolute increase from baseline had evidence of adverse LV remodeling, including LV dilatation, lack of improvement in LVEF, and worse diastolic function [92].
These results suggest that PICP and PIIINP concentrations may be useful reflections of BMP1 activity and thereby complement BMP1 as markers of remodeling; as is the case for BMP1, however, additional data are needed.
Mechanical Circulatory Support
The identification of serum biomarkers for the prediction of reverse remodeling and myocardial recovery is particularly relevant in this era of mechanical support devices. As the rates of left ventricular assist device (LVAD) implantation increase, while the rates of cardiac transplantation remain relatively stable, early stratification of patients based on their likelihood of recovery might affect treatment strategy. No such serum biomarkers with prognostic value in patients with refractory cardiogenic shock requiring mechanical support have yet been identified. In a small study of 41 patients requiring support with extracorporeal membrane oxygenation, early measurements of several prognostic HF biomarkers, including NT-proBNP and cTnI, did not predict myocardial recovery [93]. In patients with chronic HFrEF requiring long-term LVAD support, however, the data are more encouraging. Several studies have demonstrated that LVAD therapy leads to decreases in concentrations of NT-proBNP and BNP from baseline, in some cases correlating with decrease in LV dimensions [94–96]. It is not clear, however, whether the reduction in NP concentrations is due primarily to pre-operative stabilization with medical therapy or whether it is a direct effect of LVAD-related hemodynamic unloading [97]. Interestingly, there are conflicting data regarding effects of LVAD therapy on markers of inflammation and fibrosis. Though one recent single-center study demonstrated a reduction in galectin-3 and ST2, along with NT-proBNP and other serum biomarkers, after LVAD therapy [94], others have found that these markers of inflammation and fibrosis remained unchanged [95, 96]. Despite these early findings, additional work is necessary to better define the role of serum biomarkers in predicting reverse remodeling or myocardial recovery after LVAD implantation; the existing data are not yet sufficient to recommend the use of any specific biomarker for this application.
Conclusion
Serum biomarkers are promising tools for the prediction of reverse remodeling in chronic HFrEF, and their potential application to myocardial recovery is of specific clinical relevance given its association with improved clinical outcomes. Many serum biomarkers, including those reflecting myocyte stretch and stress, myocyte injury and necrosis, inflammation and fibrosis, and extracellular matrix turnover, have been studied in both preclinical and clinical settings. Several of these markers are associated with prognosis in HFrEF, and a smaller number have been linked to LV remodeling and reverse remodeling in studies to date. The relative strength of evidence linking each subgroup of biomarkers to clinical outcomes, LV remodeling, and reverse remodeling is depicted in Table 1. Based on the data currently available, sST2 appears to be the most promising of the biomarkers described here, specifically in terms of its link to LV reverse remodeling demonstrated in imaging studies; due to their close associations with clinical outcomes, however, NPs and cTn may also prove to be of use in the future. Additional work is necessary to better define the utility of these and other novel candidate biomarkers. The biomarkers that reflect mechanistic processes of myocardial recovery are particularly important because they may allow improved application of precision medicine, with tailoring of therapeutic decisions to individuals based on their underlying biology. This is an approach already routinely used in other fields such as oncology, but has only recently begun to take hold in HF, and is likely to form the basis of future applications of therapeutic strategies and targeted research.
References
Mozaffarian D, Benjamin EJ, Go AS, Arnett DK, Blaha MJ, Cushman M, et al. Heart disease and stroke statistics—2016 update: a report from the American Heart Association. Circulation. 2016;133(4):e38–360. doi:10.1161/CIR.0000000000000350.
Udelson JE, Konstam MA. Relation between left ventricular remodeling and clinical outcomes in heart failure patients with left ventricular systolic dysfunction. J Card Fail. 2002;8(6 Suppl):S465–71. doi:10.1054/jcaf.2002.129289.
Goldfinger JZ, Nair AP. Myocardial recovery and the failing heart: medical, device and mechanical methods. Ann Glob Health. 2014;80(1):55–60. doi:10.1016/j.aogh.2013.12.006.
Mancini GB, Howlett JG, Borer J, Liu PP, Mehra MR, Pfeffer M, et al. Pharmacologic options for the management of systolic heart failure: examining underlying mechanisms. Can J Cardiol. 2015;31(10):1282–92. doi:10.1016/j.cjca.2015.02.013.
Punnoose LR, Givertz MM, Lewis EF, Pratibhu P, Stevenson LW, Desai AS. Heart failure with recovered ejection fraction: a distinct clinical entity. J Card Fail. 2011;17(7):527–32. doi:10.1016/j.cardfail.2011.03.005.
Basuray A, French B, Ky B, Vorovich E, Olt C, Sweitzer NK, et al. Heart failure with recovered ejection fraction: clinical description, biomarkers, and outcomes. Circulation. 2014;129(23):2380–7. doi:10.1161/CIRCULATIONAHA.113.006855.
Mann DL, Barger PM, Burkhoff D. Myocardial recovery and the failing heart: myth, magic, or molecular target? J Am Coll Cardiol. 2012;60(24):2465–72. doi:10.1016/j.jacc.2012.06.062.
Mann DL, Burkhoff D. Is myocardial recovery possible and how do you measure it? Curr Cardiol Rep. 2012;14(3):293–8. doi:10.1007/s11886-012-0264-z.
Konstam MA. Reliability of ventricular remodeling as a surrogate for use in conjunction with clinical outcomes in heart failure. Am J Cardiol. 2005;96(6):867–71. doi:10.1016/j.amjcard.2005.05.037.
Konstam MA, Kramer DG, Patel AR, Maron MS, Udelson JE. Left ventricular remodeling in heart failure: current concepts in clinical significance and assessment. J Am Coll Cardiol Img. 2011;4(1):98–108. doi:10.1016/j.jcmg.2010.10.008.
White HD, Norris RM, Brown MA, Brandt PW, Whitlock RM, Wild CJ. Left ventricular end-systolic volume as the major determinant of survival after recovery from myocardial infarction. Circulation. 1987;76(1):44–51.
Lupon J, Gaggin HK, de Antonio M, Domingo M, Galan A, Zamora E, et al. Biomarker-assist score for reverse remodeling prediction in heart failure: the ST2-R2 score. Int J Cardiol. 2015;184:337–43. doi:10.1016/j.ijcard.2015.02.019.
Mulvagh SL, DeMaria AN, Feinstein SB, Burns PN, Kaul S, Miller JG, et al. Contrast echocardiography: current and future applications. J Am Soc Echocardiogr Off Publ Am Soc Echocardiogr. 2000;13(4):331–42.
Jenkins C, Bricknell K, Hanekom L, Marwick TH. Reproducibility and accuracy of echocardiographic measurements of left ventricular parameters using real-time three-dimensional echocardiography. J Am Coll Cardiol. 2004;44(4):878–86. doi:10.1016/j.jacc.2004.05.050.
Kim RJ, Wu E, Rafael A, Chen EL, Parker MA, Simonetti O, et al. The use of contrast-enhanced magnetic resonance imaging to identify reversible myocardial dysfunction. N Engl J Med. 2000;343(20):1445–53. doi:10.1056/NEJM200011163432003.
Heil B, Tang WH. Biomarkers: their potential in the diagnosis and treatment of heart failure. Cleve Clin J Med. 2015;82(12 Suppl 2):S28–35. doi:10.3949/ccjm.82.s2.05.
Writing Committee M, Yancy CW, Jessup M, Bozkurt B, Butler J, Casey Jr DE, et al. 2013 ACCF/AHA guideline for the management of heart failure: a report of the American College of Cardiology Foundation/American Heart Association Task Force on practice guidelines. Circulation. 2013;128(16):e240–327. doi:10.1161/CIR.0b013e31829e8776.
McMurray JJ, Adamopoulos S, Anker SD, Auricchio A, Bohm M, Dickstein K, et al. ESC guidelines for the diagnosis and treatment of acute and chronic heart failure 2012: the task force for the diagnosis and treatment of acute and chronic heart failure 2012 of the European Society of Cardiology. Developed in collaboration with the Heart Failure Association (HFA) of the ESC. Eur Heart J. 2012;33(14):1787–847. doi:10.1093/eurheartj/ehs104.
Moe GW, Ezekowitz JA, O’Meara E, Lepage S, Howlett JG, Fremes S, et al. The 2014 Canadian Cardiovascular Society heart failure management guidelines focus update: anemia, biomarkers, and recent therapeutic trial implications. Can J Cardiol. 2015;31(1):3–16. doi:10.1016/j.cjca.2014.10.022.
Motiwala SR, Januzzi Jr JL. The role of natriuretic peptides as biomarkers for guiding the management of chronic heart failure. Clin Pharmacol Ther. 2013;93(1):57–67. doi:10.1038/clpt.2012.187.
Masson S, Latini R, Anand IS, Barlera S, Angelici L, Vago T, et al. Prognostic value of changes in N-terminal pro-brain natriuretic peptide in Val-HeFT (Valsartan Heart Failure Trial). J Am Coll Cardiol. 2008;52(12):997–1003. doi:10.1016/j.jacc.2008.04.069.
Weiner RB, Baggish AL, Chen-Tournoux A, Marshall JE, Gaggin HK, Bhardwaj A, et al. Improvement in structural and functional echocardiographic parameters during chronic heart failure therapy guided by natriuretic peptides: mechanistic insights from the ProBNP Outpatient Tailored Chronic Heart Failure (PROTECT) study. Eur J Heart Fail. 2013;15(3):342–51. doi:10.1093/eurjhf/hfs180.
Gaggin HK, Truong QA, Rehman SU, Mohammed AA, Bhardwaj A, Parks KA, et al. Characterization and prediction of natriuretic peptide “nonresponse” during heart failure management: results from the ProBNP Outpatient Tailored Chronic Heart Failure (PROTECT) and the NT-proBNP-Assisted Treatment to Lessen Serial Cardiac Readmissions and Death (BATTLESCARRED) study. Congest Heart Fail. 2013;19(3):135–42. doi:10.1111/chf.12016.
Krittayaphong R, Boonyasirinant T, Saiviroonporn P, Thanapiboonpol P, Nakyen S, Udompunturak S. Correlation between NT-pro BNP levels and left ventricular wall stress, sphericity index and extent of myocardial damage: a magnetic resonance imaging study. J Card Fail. 2008;14(8):687–94. doi:10.1016/j.cardfail.2008.05.002.
Krittayaphong R, Boonyasirinant T, Saiviroonporn P, Udompunturak S. NT-proBNP levels in the evaluation of right ventricular dysfunction in patients with coronary artery disease and abnormal left ventricular wall motion: a magnetic resonance imaging study. Coron Artery Dis. 2008;19(7):481–7. doi:10.1097/MCA.0b013e32830b4d0e.
Fruhwald FM, Fahrleitner-Pammer A, Berger R, Leyva F, Freemantle N, Erdmann E, et al. Early and sustained effects of cardiac resynchronization therapy on N-terminal pro-B-type natriuretic peptide in patients with moderate to severe heart failure and cardiac dyssynchrony. Eur Heart J. 2007;28(13):1592–7. doi:10.1093/eurheartj/ehl505.
Januzzi Jr JL, Filippatos G, Nieminen M, Gheorghiade M. Troponin elevation in patients with heart failure: on behalf of the third universal definition of Myocardial Infarction Global Task Force: Heart Failure Section. Eur Heart J. 2012;33(18):2265–71. doi:10.1093/eurheartj/ehs191.
Hudson MP, O’Connor CM, Gattis WA, Tasissa G, Hasselblad V, Holleman CM, et al. Implications of elevated cardiac troponin T in ambulatory patients with heart failure: a prospective analysis. Am Heart J. 2004;147(3):546–52. doi:10.1016/j.ahj.2003.10.014.
Sato Y, Yamada T, Taniguchi R, Nagai K, Makiyama T, Okada H, et al. Persistently increased serum concentrations of cardiac troponin t in patients with idiopathic dilated cardiomyopathy are predictive of adverse outcomes. Circulation. 2001;103(3):369–74.
Horwich TB, Patel J, MacLellan WR, Fonarow GC. Cardiac troponin I is associated with impaired hemodynamics, progressive left ventricular dysfunction, and increased mortality rates in advanced heart failure. Circulation. 2003;108(7):833–8. doi:10.1161/01.CIR.0000084543.79097.34.
Setsuta K, Seino Y, Takahashi N, Ogawa T, Sasaki K, Harada A, et al. Clinical significance of elevated levels of cardiac troponin T in patients with chronic heart failure. Am J Cardiol. 1999;84(5):608–11. A9.
Motiwala SR, Gaggin HK, Gandhi PU, Belcher A, Weiner RB, Baggish AL, et al. Concentrations of highly sensitive cardiac troponin-I predict poor cardiovascular outcomes and adverse remodeling in chronic heart failure. J Cardiovasc Transl Res. 2015;8(3):164–72. doi:10.1007/s12265-015-9618-4.
Chia S, Senatore F, Raffel OC, Lee H, Wackers FJ, Jang IK. Utility of cardiac biomarkers in predicting infarct size, left ventricular function, and clinical outcome after primary percutaneous coronary intervention for ST-segment elevation myocardial infarction. J Am Coll Cardiol Intv. 2008;1(4):415–23. doi:10.1016/j.jcin.2008.04.010.
Oh PC, Choi IS, Ahn T, Moon J, Park Y, Seo JG, et al. Predictors of recovery of left ventricular systolic dysfunction after acute myocardial infarction: from the korean acute myocardial infarction registry and korean myocardial infarction registry. Korean Circ J. 2013;43(8):527–33. doi:10.4070/kcj.2013.43.8.527.
Brooks GC, Lee BK, Rao R, Lin F, Morin DP, Zweibel SL, et al. Predicting persistent left ventricular dysfunction following myocardial infarction: the PREDICTS study. J Am Coll Cardiol. 2016;67(10):1186–96. doi:10.1016/j.jacc.2015.12.042.
Weinberg EO, Shimpo M, De Keulenaer GW, MacGillivray C, Tominaga S, Solomon SD, et al. Expression and regulation of ST2, an interleukin-1 receptor family member, in cardiomyocytes and myocardial infarction. Circulation. 2002;106(23):2961–6.
Bartunek J, Delrue L, Van Durme F, Muller O, Casselman F, De Wiest B, et al. Nonmyocardial production of ST2 protein in human hypertrophy and failure is related to diastolic load. J Am Coll Cardiol. 2008;52(25):2166–74. doi:10.1016/j.jacc.2008.09.027.
Sanada S, Hakuno D, Higgins LJ, Schreiter ER, McKenzie AN, Lee RT. IL-33 and ST2 comprise a critical biomechanically induced and cardioprotective signaling system. J Clin Invest. 2007;117(6):1538–49. doi:10.1172/JCI30634.
Seki K, Sanada S, Kudinova AY, Steinhauser ML, Handa V, Gannon J, et al. Interleukin-33 prevents apoptosis and improves survival after experimental myocardial infarction through ST2 signaling. Circ Heart Fail. 2009;2(6):684–91. doi:10.1161/CIRCHEARTFAILURE.109.873240.
Weinberg EO, Shimpo M, Hurwitz S, Tominaga S, Rouleau JL, Lee RT. Identification of serum soluble ST2 receptor as a novel heart failure biomarker. Circulation. 2003;107(5):721–6.
Pascual-Figal DA, Ordonez-Llanos J, Tornel PL, Vazquez R, Puig T, Valdes M, et al. Soluble ST2 for predicting sudden cardiac death in patients with chronic heart failure and left ventricular systolic dysfunction. J Am Coll Cardiol. 2009;54(23):2174–9. doi:10.1016/j.jacc.2009.07.041.
Bayes-Genis A, Pascual-Figal D, Januzzi JL, Maisel A, Casas T, Valdes Chavarri M, et al. Soluble ST2 monitoring provides additional risk stratification for outpatients with decompensated heart failure. Rev Esp Cardiol. 2010;63(10):1171–8.
Ky B, French B, McCloskey K, Rame JE, McIntosh E, Shahi P, et al. High-sensitivity ST2 for prediction of adverse outcomes in chronic heart failure. Circ Heart Fail. 2011;4(2):180–7. doi:10.1161/CIRCHEARTFAILURE.110.958223.
Broch K, Ueland T, Nymo SH, Kjekshus J, Hulthe J, Muntendam P, et al. Soluble ST2 is associated with adverse outcome in patients with heart failure of ischaemic aetiology. Eur J Heart Fail. 2012;14(3):268–77. doi:10.1093/eurjhf/hfs006.
Bayes-Genis A, de Antonio M, Galan A, Sanz H, Urrutia A, Cabanes R, et al. Combined use of high-sensitivity ST2 and NTproBNP to improve the prediction of death in heart failure. Eur J Heart Fail. 2012;14(1):32–8. doi:10.1093/eurjhf/hfr156.
Bayes-Genis A, de Antonio M, Vila J, Penafiel J, Galan A, Barallat J, et al. Head-to-head comparison of 2 myocardial fibrosis biomarkers for long-term heart failure risk stratification: ST2 versus galectin-3. J Am Coll Cardiol. 2014;63(2):158–66. doi:10.1016/j.jacc.2013.07.087.
Shah RV, Chen-Tournoux AA, Picard MH, van Kimmenade RR, Januzzi JL. Serum levels of the interleukin-1 receptor family member ST2, cardiac structure and function, and long-term mortality in patients with acute dyspnea. Circ Heart Fail. 2009;2(4):311–9. doi:10.1161/CIRCHEARTFAILURE.108.833707.
Daniels LB, Clopton P, Iqbal N, Tran K, Maisel AS. Association of ST2 levels with cardiac structure and function and mortality in outpatients. Am Heart J. 2010;160(4):721–8. doi:10.1016/j.ahj.2010.06.033.
Weir RA, Miller AM, Murphy GE, Clements S, Steedman T, Connell JM, et al. Serum soluble ST2: a potential novel mediator in left ventricular and infarct remodeling after acute myocardial infarction. J Am Coll Cardiol. 2010;55(3):243–50. doi:10.1016/j.jacc.2009.08.047.
Gaggin HK, Motiwala S, Bhardwaj A, Parks KA, Januzzi Jr JL. Soluble concentrations of the interleukin receptor family member ST2 and beta-blocker therapy in chronic heart failure. Circ Heart Fail. 2013;6(6):1206–13. doi:10.1161/CIRCHEARTFAILURE.113.000457.
Gaggin HK, Szymonifka J, Bhardwaj A, Belcher A, De Berardinis B, Motiwala S, et al. Head-to-head comparison of serial soluble ST2, growth differentiation factor-15, and Highly-sensitive troponin T measurements in patients with chronic heart failure. JACC Heart Fail. 2014;2(1):65–72. doi:10.1016/j.jchf.2013.10.005.
Lupon J, Sanders-van Wijk S, Januzzi JL, de Antonio M, Gaggin HK, Pfisterer M, et al. Prediction of survival and magnitude of reverse remodeling using the ST2-R2 score in heart failure: a multicenter study. Int J Cardiol. 2016;204:242–7. doi:10.1016/j.ijcard.2015.11.163.
Sharma UC, Pokharel S, van Brakel TJ, van Berlo JH, Cleutjens JP, Schroen B, et al. Galectin-3 marks activated macrophages in failure-prone hypertrophied hearts and contributes to cardiac dysfunction. Circulation. 2004;110(19):3121–8. doi:10.1161/01.CIR.0000147181.65298.4D.
Calvier L, Miana M, Reboul P, Cachofeiro V, Martinez-Martinez E, de Boer RA, et al. Galectin-3 mediates aldosterone-induced vascular fibrosis. Arterioscler Thromb Vasc Biol. 2013;33(1):67–75. doi:10.1161/ATVBAHA.112.300569.
Azibani F, Benard L, Schlossarek S, Merval R, Tournoux F, Fazal L, et al. Aldosterone inhibits antifibrotic factors in mouse hypertensive heart. Hypertension. 2012;59(6):1179–87. doi:10.1161/HYPERTENSIONAHA.111.190512.
Yu L, Ruifrok WP, Meissner M, Bos EM, van Goor H, Sanjabi B, et al. Genetic and pharmacological inhibition of galectin-3 prevents cardiac remodeling by interfering with myocardial fibrogenesis. Circ Heart Fail. 2013;6(1):107–17. doi:10.1161/CIRCHEARTFAILURE.112.971168.
van der Velde AR, Gullestad L, Ueland T, Aukrust P, Guo Y, Adourian A, et al. Prognostic value of changes in galectin-3 levels over time in patients with heart failure: data from CORONA and COACH. Circ Heart Fail. 2013;6(2):219–26. doi:10.1161/CIRCHEARTFAILURE.112.000129.
Anand IS, Rector TS, Kuskowski M, Adourian A, Muntendam P, Cohn JN. Baseline and serial measurements of galectin-3 in patients with heart failure: relationship to prognosis and effect of treatment with valsartan in the Val-HeFT. Eur J Heart Fail. 2013;15(5):511–8. doi:10.1093/eurjhf/hfs205.
Lok DJ, Van Der Meer P, de la Porte PW, Lipsic E, Van Wijngaarden J, Hillege HL, et al. Prognostic value of galectin-3, a novel marker of fibrosis, in patients with chronic heart failure: data from the DEAL-HF study. Clin Res Cardiol: Off J Ger Card Soc. 2010;99(5):323–8. doi:10.1007/s00392-010-0125-y.
Motiwala SR, Szymonifka J, Belcher A, Weiner RB, Baggish AL, Sluss P, et al. Serial measurement of galectin-3 in patients with chronic heart failure: results from the ProBNP Outpatient Tailored Chronic Heart Failure Therapy (PROTECT) study. Eur J Heart Fail. 2013;15(10):1157–63. doi:10.1093/eurjhf/hft075.
de Boer RA, Lok DJ, Jaarsma T, van der Meer P, Voors AA, Hillege HL, et al. Predictive value of plasma galectin-3 levels in heart failure with reduced and preserved ejection fraction. Ann Med. 2011;43(1):60–8. doi:10.3109/07853890.2010.538080.
Gullestad L, Ueland T, Kjekshus J, Nymo SH, Hulthe J, Muntendam P, et al. The predictive value of galectin-3 for mortality and cardiovascular events in the Controlled Rosuvastatin Multinational Trial in Heart Failure (CORONA). Am Heart J. 2012;164(6):878–83. doi:10.1016/j.ahj.2012.08.021.
Felker GM, Fiuzat M, Shaw LK, Clare R, Whellan DJ, Bettari L, et al. Galectin-3 in ambulatory patients with heart failure: results from the HF-ACTION study. Circ Heart Fail. 2012;5(1):72–8. doi:10.1161/CIRCHEARTFAILURE.111.963637.
Lok DJ, Lok SI, Bruggink-Andre de la Porte PW, Badings E, Lipsic E, van Wijngaarden J, et al. Galectin-3 is an independent marker for ventricular remodeling and mortality in patients with chronic heart failure. Clin Res Cardiol: Off J Ger Card Soc. 2013;102(2):103–10. doi:10.1007/s00392-012-0500-y.
Tang WH, Shrestha K, Shao Z, Borowski AG, Troughton RW, Thomas JD, et al. Usefulness of plasma galectin-3 levels in systolic heart failure to predict renal insufficiency and survival. Am J Cardiol. 2011;108(3):385–90. doi:10.1016/j.amjcard.2011.03.056.
Weir RA, Petrie CJ, Murphy CA, Clements S, Steedman T, Miller AM, et al. Galectin-3 and cardiac function in survivors of acute myocardial infarction. Circ Heart Fail. 2013;6(3):492–8. doi:10.1161/CIRCHEARTFAILURE.112.000146.
Gullestad L, Ueland T, Kjekshus J, Nymo SH, Hulthe J, Muntendam P, et al. Galectin-3 predicts response to statin therapy in the Controlled Rosuvastatin Multinational Trial in Heart Failure (CORONA). Eur Heart J. 2012;33(18):2290–6. doi:10.1093/eurheartj/ehs077.
Fiuzat M, Schulte PJ, Felker M, Ahmad T, Neely M, Adams KF, et al. Relationship between galectin-3 levels and mineralocorticoid receptor antagonist use in heart failure: analysis from HF-ACTION. J Card Fail. 2014;20(1):38–44. doi:10.1016/j.cardfail.2013.11.011.
Gandhi PU, Motiwala SR, Belcher AM, Gaggin HK, Weiner RB, Baggish AL, et al. Galectin-3 and mineralocorticoid receptor antagonist use in patients with chronic heart failure due to left ventricular systolic dysfunction. Am Heart J. 2015;169(3):404–11. doi:10.1016/j.ahj.2014.12.012. e3.
Stolen CM, Adourian A, Meyer TE, Stein KM, Solomon SD. Plasma galectin-3 and heart failure outcomes in MADIT-CRT (multicenter automatic defibrillator implantation trial with cardiac resynchronization therapy). J Card Fail. 2014;20(11):793–9. doi:10.1016/j.cardfail.2014.07.018.
Lopez-Andres N, Rossignol P, Iraqi W, Fay R, Nuee J, Ghio S, et al. Association of galectin-3 and fibrosis markers with long-term cardiovascular outcomes in patients with heart failure, left ventricular dysfunction, and dyssynchrony: insights from the CARE-HF (Cardiac Resynchronization in Heart Failure) trial. Eur J Heart Fail. 2012;14(1):74–81. doi:10.1093/eurjhf/hfr151.
Milting H, Ellinghaus P, Seewald M, Cakar H, Bohms B, Kassner A, et al. Plasma biomarkers of myocardial fibrosis and remodeling in terminal heart failure patients supported by mechanical circulatory support devices. J Heart Lung Transplant Off Publ Int Soc Heart Transplant. 2008;27(6):589–96. doi:10.1016/j.healun.2008.02.018.
Travers JG, Kamal FA, Robbins J, Yutzey KE, Blaxall BC. Cardiac fibrosis: the fibroblast awakens. Circ Res. 2016;118(6):1021–40. doi:10.1161/CIRCRESAHA.115.306565.
Yabluchanskiy A, Ma Y, Iyer RP, Hall ME, Lindsey ML. Matrix metalloproteinase-9: many shades of function in cardiovascular disease. Physiology. 2013;28(6):391–403. doi:10.1152/physiol.00029.2013.
Thomas CV, Coker ML, Zellner JL, Handy JR, Crumbley 3rd AJ, Spinale FG. Increased matrix metalloproteinase activity and selective upregulation in LV myocardium from patients with end-stage dilated cardiomyopathy. Circulation. 1998;97(17):1708–15.
Coker ML, Thomas CV, Clair MJ, Hendrick JW, Krombach RS, Galis ZS, et al. Myocardial matrix metalloproteinase activity and abundance with congestive heart failure. Am J Phys. 1998;274(5 Pt 2):H1516–23.
Polyakova V, Loeffler I, Hein S, Miyagawa S, Piotrowska I, Dammer S, et al. Fibrosis in endstage human heart failure: severe changes in collagen metabolism and MMP/TIMP profiles. Int J Cardiol. 2011;151(1):18–33. doi:10.1016/j.ijcard.2010.04.053.
Sundstrom J, Evans JC, Benjamin EJ, Levy D, Larson MG, Sawyer DB, et al. Relations of plasma matrix metalloproteinase-9 to clinical cardiovascular risk factors and echocardiographic left ventricular measures: the Framingham Heart Study. Circulation. 2004;109(23):2850–6. doi:10.1161/01.CIR.0000129318.79570.84.
Ducharme A, Frantz S, Aikawa M, Rabkin E, Lindsey M, Rohde LE, et al. Targeted deletion of matrix metalloproteinase-9 attenuates left ventricular enlargement and collagen accumulation after experimental myocardial infarction. J Clin Invest. 2000;106(1):55–62. doi:10.1172/JCI8768.
Lindsey ML, Escobar GP, Dobrucki LW, Goshorn DK, Bouges S, Mingoia JT, et al. Matrix metalloproteinase-9 gene deletion facilitates angiogenesis after myocardial infarction. Am J Phys Heart Circ Phys. 2006;290(1):H232–9. doi:10.1152/ajpheart.00457.2005.
Zamilpa R, Ibarra J, de Castro Bras LE, Ramirez TA, Nguyen N, Halade GV, et al. Transgenic overexpression of matrix metalloproteinase-9 in macrophages attenuates the inflammatory response and improves left ventricular function post-myocardial infarction. J Mol Cell Cardiol. 2012;53(5):599–608. doi:10.1016/j.yjmcc.2012.07.017.
Li SW, Sieron AL, Fertala A, Hojima Y, Arnold WV, Prockop DJ. The C-proteinase that processes procollagens to fibrillar collagens is identical to the protein previously identified as bone morphogenic protein-1. Proc Natl Acad Sci U S A. 1996;93(10):5127–30.
Kessler E, Takahara K, Biniaminov L, Brusel M, Greenspan DS. Bone morphogenetic protein-1: the type I procollagen C-proteinase. Science. 1996;271(5247):360–2.
Vadon-Le Goff S, Hulmes DJ, Moali C. BMP-1/tolloid-like proteinases synchronize matrix assembly with growth factor activation to promote morphogenesis and tissue remodeling. Matrix Biol J Int Soc Matrix Biol. 2015;44–46:14–23. doi:10.1016/j.matbio.2015.02.006.
Kobayashi K, Luo M, Zhang Y, Wilkes DC, Ge G, Grieskamp T, et al. Secreted frizzled-related protein 2 is a procollagen C proteinase enhancer with a role in fibrosis associated with myocardial infarction. Nat Cell Biol. 2009;11(1):46–55. doi:10.1038/ncb1811.
He W, Zhang L, Ni A, Zhang Z, Mirotsou M, Mao L, et al. Exogenously administered secreted frizzled related protein 2 (Sfrp2) reduces fibrosis and improves cardiac function in a rat model of myocardial infarction. Proc Natl Acad Sci U S A. 2010;107(49):21110–5. doi:10.1073/pnas.1004708107.
Shalitin N, Schlesinger H, Levy MJ, Kessler E, Kessler-Icekson G. Expression of procollagen C-proteinase enhancer in cultured rat heart fibroblasts: evidence for co-regulation with type I collagen. J Cell Biochem. 2003;90(2):397–407. doi:10.1002/jcb.10646.
Kessler-Icekson G, Schlesinger H, Freimann S, Kessler E. Expression of procollagen C-proteinase enhancer-1 in the remodeling rat heart is stimulated by aldosterone. Int J Biochem Cell Biol. 2006;38(3):358–65. doi:10.1016/j.biocel.2005.10.007.
Klappacher G, Franzen P, Haab D, Mehrabi M, Binder M, Plesch K, et al. Measuring extracellular matrix turnover in the serum of patients with idiopathic or ischemic dilated cardiomyopathy and impact on diagnosis and prognosis. Am J Cardiol. 1995;75(14):913–8.
Querejeta R, Lopez B, Gonzalez A, Sanchez E, Larman M, Martinez Ubago JL, et al. Increased collagen type I synthesis in patients with heart failure of hypertensive origin: relation to myocardial fibrosis. Circulation. 2004;110(10):1263–8. doi:10.1161/01.CIR.0000140973.60992.9A.
Lofsjogard J, Kahan T, Diez J, Lopez B, Gonzalez A, Edner M, et al. Biomarkers of collagen type I metabolism are related to B-type natriuretic peptide, left ventricular size, and diastolic function in heart failure. J Cardiovasc Med. 2014;15(6):463–9. doi:10.2459/01.JCM.0000435617.86180.0b.
Poulsen SH, Host NB, Egstrup K. Long-term changes in collagen formation expressed by serum carboxyterminal propeptide of type-I procollagen and relation to left ventricular function after acute myocardial infarction. Cardiology. 2001;96(1):45–50.
Luyt CE, Landivier A, Leprince P, Bernard M, Pavie A, Chastre J, et al. Usefulness of cardiac biomarkers to predict cardiac recovery in patients on extracorporeal membrane oxygenation support for refractory cardiogenic shock. J Crit Care. 2012;27(5):524 e7–14. doi:10.1016/j.jcrc.2011.12.009.
Ahmad T, Wang T, O’Brien EC, Samsky MD, Pura JA, Lokhnygina Y, et al. Effects of left ventricular assist device support on biomarkers of cardiovascular stress, fibrosis, fluid homeostasis, inflammation, and renal injury. JACC Heart Fail. 2015;3(1):30–9. doi:10.1016/j.jchf.2014.06.013.
Lok SI, Nous FM, van Kuik J, van der Weide P, Winkens B, Kemperman H, et al. Myocardial fibrosis and pro-fibrotic markers in end-stage heart failure patients during continuous-flow left ventricular assist device support. Eur J Cardiothorac Surg Off J Eur Assoc Cardiothorac Surg. 2015;48(3):407–15. doi:10.1093/ejcts/ezu539.
Grosman-Rimon L, Jacobs I, Tumiati LC, McDonald MA, Bar-Ziv SP, Fuks A, et al. Longitudinal assessment of inflammation in recipients of continuous-flow left ventricular assist devices. Can J Cardiol. 2015;31(3):348–56. doi:10.1016/j.cjca.2014.12.006.
Hasin T, Kushwaha SS, Lesnick TG, Kremers W, Boilson BA, Schirger JA, et al. Early trends in N-terminal pro-brain natriuretic peptide values after left ventricular assist device implantation for chronic heart failure. Am J Cardiol. 2014;114(8):1257–63. doi:10.1016/j.amjcard.2014.07.056.
Acknowledgments
Dr. Gaggin is supported in part by the Clark Fund for Cardiac Research Innovation.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
Hanna K. Gaggin reports the following disclosures: 1) Roche Diagnostics: research grant, consultancy; 2) Portola: research grant; 3) Amgen: consultancy; 4) American Regent: consultancy; 5) Boston Heart Diagnostics: consultancy; 6) Critical Diagnostics: consultancy; 7) Ortho Clinical: consultancy; 8) EchoSense, Radiometer: clinical endpoint committee.
Dr. Motiwala does not have any disclosures.
Human and Animal Rights and Informed Consent
This article does not contain any studies with human or animal subjects performed by any of the authors.
Additional information
This article is part of the Topical Collection on Biomarkers of Heart Failure
Rights and permissions
About this article
Cite this article
Motiwala, S.R., Gaggin, H.K. Biomarkers to Predict Reverse Remodeling and Myocardial Recovery in Heart Failure. Curr Heart Fail Rep 13, 207–218 (2016). https://doi.org/10.1007/s11897-016-0303-y
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11897-016-0303-y