Abstract
The independent association of diabetes and hyperglycemia on the outcomes of sepsis remains unclear. We conducted retrospective cohort analyses of outcomes among patients with community-onset sepsis admitted to Shamir Medical Center, Israel (08-12/2016). Statistical associations were queried by Cox and logistic regressions, controlled for by matched propensity score analyses. Among 1527 patients with community-onset sepsis, 469 (30.7%) were diabetic. Diabetic patients were significantly older, with advanced complexity of comorbidities, and were more often exposed to healthcare environments. Despite statistically significant univariable associations with in-hospital and 90-day mortality, the adjusted Hazard Ratios (aHR) were 1.21 95% CI 0.8–1.71, p = 0.29 and 1.13 95% CI 0.86–1.49, p = 0.37, respectively. However, hyperglycemia at admission (i.e., above 200 mg/dl (was independently associated with: increased in-hospital mortality, aHR 1.48 95% CI 1.02–2.16, p = 0.037, 30-day mortality, aHR 1.8 95% CI 1.12–2.58, p = 0.001), and 90-day mortality, aHR 1.68 95% CI 1.24–2.27, p = 0.001. This association was more robust among diabetic patients than those without diabetes. In this study, diabetes was not associated with worse clinical outcomes in community-onset sepsis. However, high glucose levels at sepsis onset are independently associated with a worse prognosis, particularly among diabetic patients. Future trials should explore whether glycemic control could impact the outcomes and should be part of the management of sepsis, among the general adult septic population.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Increasing prevalence of obesity and aging of the population have culminated into an exponential rise in the worldwide rates of diabetes mellitus (DM), imposing a significant burden on individuals and on public health [1]. Sepsis incidence is increasing as a cause of morbidity and mortality in the population [2]. People of advanced age and patients with preexisting chronic health conditions are particularly prone to develop severe sepsis [3].
The association between DM and the risk for infections has been well established [4, 5], although the exact mechanisms are not well understood [6]. The estimated prevalence of DM among adults is 10–20%, but they comprise 20–35% of patients with sepsis [7]. Possible explanations for the higher rates of infections among DM patients are poor chronic glycemic control and/or acute hyperglycemic states, which impairs the immune system, impairs tissue perfusion, and results in gastrointestinal and urinary tract dysmotility, damaged wound healing, and increased healthcare encounters and interventions [8,9,10,11]. Comparative controlled analyses of sepsis outcomes among patients with or without DM are conflicting. In some studies, diabetes was associated with increased mortality, a longer length of stay, and higher costs [12, 13]. Other controlled studies, did not find an independent association between DM and increased mortality in sepsis [14], and some even described a protective effect [15]. Inflammatory response of patients with DM during sepsis is altered [16] hence diabetic patients may be less likely to develop adult respiratory distress syndrome (ARDS) [17] and respiratory failure [15]. Diabetic patients have reduced activity of neutrophils and reduced migration of these cells to the lungs with the result of less oxidative damage [17].
The prognostic value of blood glucose levels at admission (ABGL) on sepsis outcomes is also a matter of controversy: in some studies, elevated blood glucose levels at sepsis onset were associated with worse outcomes, [18] yet in others, the association was less established [19,20,21,22]. Our study aims were to evaluate the prognostic impact of DM and ABGL on outcomes of sepsis.
Methods
Retrospective analyses were conducted on patients admitted to Shamir (Assaf Harofeh) Medical Center from August to December 2016. The study was approved by the local ethics (Helsinki) committee prior to its initiation.
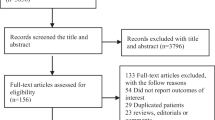
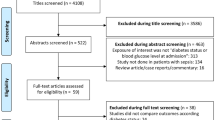
Consecutive adult patients (> 18 years) with sepsis upon admission (i.e., “community-onset” infection), as per established definition [23], were enrolled. Patients were excluded if they were directly transferred from another facility, or if they were hospitalized in the past 7 days for any reason, or in the past 30 days with the same infectious clinical syndrome. Therefore, “hospital-acquired” infections were excluded, but “community-onset” infections, consisting both of “community-acquired” and of “healthcare-associated” infections, as per established definition [24], were enrolled. The study cohort consisted of patients from whom blood cultures were drawn in the first 2 calendar days of hospitalization (including visits to, and immediate discharge from, the emergency room), who concurrently had systemic inflammatory response syndrome [25]. This screening methodology for diagnosing sepsis had displayed a sensitivity of 100% and a specificity of 99% in a prior pilot analysis [23]. Patients were excluded if they had new-onset DM (diagnosed during the index hospitalization), or if they had gestational DM. ABGL were drawn at the emergency department. For our purposes, elevated BGL were considered > 200 mg/dl, as the accepted definition for stress hyperglycemia [26,27,28,29]. Data were extracted from electronic and hard-copy records and included demographics, chronic and background co-morbidities and conditions, various exposures to healthcare, acute illness indices, and outcomes. We also analyzed and quantified multiple parameters associated with diabetes severity (e.g., duration, level of glycemic control, HbA1C, target-organ damages), for stratification purposes. Post-hospitalization mortality data were extracted from a national registry governed by the Israeli Ministry of Interior.
The index pathogen was considered a pathogen isolated from blood (except skin contaminants as determined by the US Centers for Disease Control and Prevention) [30], or from a body site associated with the patient’s clinical syndrome: e.g., a pathogen isolated from urine, of a patient with a urinary tract infection. Multi-drug resistant (MDR) phenotype were determined according to an established definition [31], and MDR organisms (MDRO) included: methicillin-resistant Staphylococcus aureus (MRSA); ampicillin- and/or vancomycin-resistant Enterococcus (VRE); penicillin and/or ceftriaxone non-susceptible Streptococcus pneumoniae; Acinetobacter baumannii; Pseudomonas aeruginosa; other inherent carbapenem non-susceptible Gram-negatives (e.g., Stenotrophomonas maltophilia, Burkholderia cepacia); and Enterobacteriaceae non-susceptible to ≥ 1 of third-generation cephalosporin (e.g., ceftriaxone, ceftazidime, cefotaxime) and/or ≥ 1 carbapenem (CRE), and/or evidence of extended-spectrum beta-lactamase (ESBL) and/or carbapenemase (CPE) production [32].
Statistical analyses
Power calculations predicted that an overall sample size of 1302 subjects (of which 977 non-diabetic patients and 325 diabetic patients) will achieve 90% power at a 0.01 significance level to detect a difference of 10% in survival between non-diabetic and diabetic patients, assuming 70% vs. 80% survival rate at 90 days for patients with vs. without diabetes given that in previous studies diabetic patients comprised 20–35% of patients with sepsis [7] and the mortality rate from sepsis in recent studies was 20–30% at 90 days [33].
All analyses were performed using SPSS software (IBM Corp. Released 2014. IBM SPSS Statistics for Windows, Version 23.0. Armonk, NY: IBM Corp). A two-tailed p < 0.05 was considered statistically significant.
Normal distribution was evaluated by histogram and Q–Q plot. Since all continuous data did not distribute normally, they are expressed as a median and interquartile range (IQR). Categorical data are expressed as frequencies and percentages and compared among groups using Chi-square tests and Fisher’s exact test. Continuous variables were compared using the Mann–Whitney test. Kaplan Meier’s curve and the log-rank test were used to describe mortality during the follow-up period comparing between diabetic and nondiabetic patients.
Multivariable logistic regression was used to study the association between of DM and morbidity outcomes while multivariable Cox regression was used to study the association of DM with survival, both while controlling for possible confounders. The multivariate regression included four blocks: In the first block DM was entered to report the crude association, in the second block, age and gender were added using enter method, in the third block clinical syndrome variables were entered and in the last block, pathogen variables were entered. The variables found to be with a p value higher than 0.1 were removed (using backward method, Wald test).
Propensity score was calculated using logistic regression as the probability of patients to have DM. DM, age, sex, CHF, CKD, dementia, malignancy, Duke’s criteria, positive culture, clinical syndrome, and bacterial growth were included in the propensity score calculation. Propensity score was divided into quintiles and then stratified Cox regression and conditional logistic regression were applied.
Results
Descriptive characteristics of the study’s cohort
Among 1527 patients with community-onset sepsis, 469 (30.7%) were diabetic. Diabetic patients were significantly older (75 vs. 59 years, p < 0.001), with advanced complexity of comorbidities (Charlson’s combined condition score 7 (5–8) vs. 2 (0–5), p < 0.001). They were more often exposed to healthcare environments (53.3% among diabetic vs. 36% of non-diabetics had at least one criterion of the Duke-2002 criteria for healthcare-associated infection (p < 0.001)) and to procedures- 17.6% of diabetics vs. 14.1% of non-diabetics underwent an invasive procedure in the preceding 6 months (p = 0.06). MDRO infections (15.4% vs. 8.7%; p < 0.001) and S. aureus bloodstream infections (both MRSA and MSSA, 2.3% vs. 0.9%; p = 0.02), were more common among diabetics as well as skin and soft tissue infection (19.2% vs. 12.2% p < 0.001). There were no differences in other sepsis features. Baseline characteristics of the study population are depicted in Table 1. Acute illness indices were also more severe among diabetics, including the prevalence of severe sepsis, septic shock, or multi-organ failure (40% vs. 24%; p < 0.001), need to be admitted directly to an intensive care unit (ICU, 11% vs. 7%; p = 0.01), acute kidney injury (35% vs. 17%; p < 0.001), and altered consciousness (35% vs. 20%; p < 0.001). Also, only 64.4% of patients with DM received appropriate antibiotic therapy within 48 h vs. 77.6% in non-diabetics (p = 0.002).
Patients with sepsis and hyperglycemia upon admission (both diabetics, n = 183, and non-diabetics, n = 33) were older, and had more co-morbidities compared to patients with ABGL < 200 mg/dl (Supplementary Table 1). Diabetic patients with ABGL of > 200 mg/dl were characterized by higher baseline HbA1c levels (7.83% vs. 6.5%, p < 0.001) and their glucose control regimen included more often insulin (49.2% vs. 28.3%, p < 0.001). The mean blood glucose during hospitalization was 203 mg/dl among DM with ABGL > 200 mg/dl vs. 146 mg/dl among DM patients with ABGL < 200 mg/dl (p < 0.001, Supplementary Table 2).
Sepsis outcomes among diabetic vs. nondiabetic patients
The 90 days’ survival rate was 78% in the DM group and 88% in the non-DM group (p < 0.001; Fig. 1). However, despite the significant association of DM with 90-day mortality (HR = 2.0, 95% CI 1.54–2.60; p < 0.001) (Table 2), this did not remain independently associated as per multivariable analysis (HR = 1.13, p = 0.37). Among those who survived the index hospitalization, DM was also significantly associated with worse morbidity outcomes: e.g., functional status deterioration (OR 1.95, 95% CI 1.36–2.78; p < 0.001), and discharge to a long-term care facility (LTCF) after being admitted to the index hospitalization from home (OR 1.77, 95% CI 1.05–3.00; p = 0.032). However, these associations were also not independent as per multivariable analyses (aOR = 1.13, p = 0.54, and aOR = 0.87, p = 0.6, respectively). Stratification of the cohort into PS quintiles revealed no associations between DM and the various outcomes that were queried (Table 2).
Sepsis outcomes stratified by the glucose levels upon admission to the acute-care hospital
Mortality rates were higher for patients with ABGL > 200 mg/dl (Fig. 2): i.e., in-hospital (19.4% vs. 7.6% p = 0.012, 30 days (19.9% vs. 8.3% p < 0.001) and 90 days (29.2% vs. 13.3% p < 0.001). The increment in mortality rates remained significant after multivariable regression analyses, i.e., aOR 1.48 (95% CI 1.02–2.16, p = 0.037) for in-hospital mortality, 1.8 (95% CI 1.12–2.58, p = 0.001) for 30-day mortality, and 1.68 (95% CI 1.24–2.27, p = 0.001) for 90-day mortality (Table 3). Hyperglycemia upon admission was also significantly and independently associated with worse morbidity outcomes (Supplementary Table 1).
In the subgroup of patients with diabetes, ABGL > 200 mg/dl was an independent poor prognostic factor in terms of mortality at 30 and 90 (aOR 2.13, 95% CI 1.29–3.49 p = 0.003, and 2.08 95% CI 1.39–3.11 p < 0.001, respectively). ABGL > 200 mg/dl was also associated with in-hospital mortality (OR 1.84, p = 0.014), though this association did not remain significant as per multivariable analysis (aOR = 1.56 95% CI 0.93–2.63) p = 0.09) (Table 3). In patients with DM, elevated ABGL was not associated with worse morbidity outcomes. Among the 33 non-diabetic patients, ABGL > 200 mg/dl were associated with increased 90-day mortality OR 2.34 (1.14–4.85) p = 0.02, though this association this did not remain independently associated as per multivariable analysis aOR 1.24 (0.6–2.55), p = 0.55.
Discussion
Sepsis is a common and deadly disease, and it is more common among diabetics [7]. However, the independent association of DM with worse sepsis outcomes is less established. The isolated association of elevated blood glucose levels at the onset of sepsis (even among non-diabetics), with the outcomes of sepsis, is not established as well. Previous investigations which queried the impact or independent statistical associations of DM with sepsis outcomes (i.e., both morbidity and mortality outcomes), had not executed strict criteria to control for established confounders, [5, 34] and have displayed conflicting results.[35, 36]. Differentiating between DM (as a chronic condition), and glucose levels as a modifiable prognostic factor (either as a causative factor or as a marker for severity of illness), could impact the management of sepsis and potentially improve patients’ outcomes.
In this study, 1527 consecutive patients with community-onset sepsis upon admission to an acute-care hospital were enrolled. We included patients with ‘community-acquired’ and patients with ‘healthcare-associated’ infection [23] and excluded patients with ‘hospital-acquired’ infections since this is a distinct population with complex characteristics and features. As in previous studies [37, 38], in this large trial, diabetic patients with sepsis were much older and had more co-morbidities, with extensive exposures to healthcare settings. All these risk factors, including diabetes by itself [39], expose these patients, as indeed was evident in our cohort, to the risk of becoming MDRO carriers (Table 1). MDRO carriers are at increased risk for deleterious sepsis outcomes [40]. The detrimental impact of MDRO carriage on infectious outcomes is commonly due to delay in initiation of appropriate therapeutic management, which was also evident in this analysis (Table 1), and is considered the strongest modifiable independent mortality predictor in severe sepsis [41].
There is a complex interplay between diabetes and sepsis. During sepsis, dysregulated immune response influenced by both host and pathogen related factors is causing inflammation with a most deleterious effect [42]. Previous studies have suggested that both innate and adaptive immune systems are compromised in diabetic animals. The malfunction of neutrophils that is one of the reasons for worse outcome in diabetic patients with sepsis, may have a part in the lower incidence of ARDS, hence produce better outcomes in certain patients. The characteristics of the subpopulation of patients for whom diabetes can be a protective factor are unknown [15, 16]. This complexity can serve as an explanation for the mixing results of sepsis outcomes in diabetic patients in different studies. In this large trial, per bivariable analyses, there were significant associations between having DM and experiencing worse clinical outcomes of sepsis. However, these associations did not remain independently associated, as per multivariable analyses, with morbidity and mortality outcomes that were captured and analyzed (Table 2). The incorporation of well-controlled propensity score-matched analyses further weakened the statistical associations of diabetes per se, with worse outcomes of infections.
However, hyperglycemia (above 200 mg/dl) upon admission, was a strong independent prognostic predictor for mortality outcomes (Table 3). Stress hyperglycemia in sepsis, both among diabetics and non-diabetics, is a result of a complex interaction between counter-regulatory hormones and cytokines causing insulin resistance which leads to excess gluconeogenesis in the liver and reduced glucose uptake. The hyperglycemia itself causes inflammation and release of cytokines in a vicious cycle [29]. Stress hyperglycemia serves as a negative prognostic factor in other acute illnesses both infectious and non-infectious [43, 44]. In our cohort, elevated ABGL were associated with worse sepsis outcomes. In accordance with a previous study [45] and contrary to others [20, 37], hyperglycemia was associated with worse prognosis of sepsis more significantly in diabetics vs. non-diabetics (Table 3). This could be due to the small number of hyperglycemic non-diabetic patients in our cohort. Another explanation could be the relatively well-controlled diabetes of our diabetic patients. In previous studies, the lack of negative effect of hyperglycemia in diabetic patients was explained by the “diabetic paradox”: uncontrolled diabetic patients with elevated HbA1c levels who are used to the hyperglycemic state, as opposed to well controlled patients with diabetes or non-diabetic patients, may tolerate stress induced hyperglycemia better [28, 46]. Diabetes care has improved globally over the years [47], reflected in the proportion of patients meeting the recommended goals for diabetes care, glycemic levels, daily glucose monitoring, routine podiatric care, and an increased rate of adherence to vaccination recommendations (e.g., influenza, Streptococcus pneumoniae). This is reflected in our relatively low HbA1c levels of the cohort (Supplementary Table 2). It is possible that among our well-controlled diabetic patients, the elevated ABGL represented true stress hyperglycemia as an indicator of sepsis severity, and not a marker of the uncontrolled diabetic state. This observation was also reported in previous studies [48, 49].
The study has several limitations. Its retrospective, chart-review based, single-center design, imposes multiple inherent confounders (such as lack of data regarding additional treatment modalities during hospitalization or socioeconomic status). However, this is a large cohort analysis, and we meticulously executed several methodologies to try and control for these confounders. We clearly isolated the independent impact of stress hyperglycemia on the outcomes of patients with community-onset sepsis. However, the pathophysiology, risk stratification, management, and therapeutic modalities of patients with sepsis and hyperglycemia, need to be further explored in future prospective controlled interventional investigations.
References
Ogurtsova K, da Rocha Fernandes JD, Huang Y, Linnenkamp U, Guariguata L, Cho NH, Cavan D, Shaw JE, Makaroff LE (2017) IDF Diabetes Atlas: global estimates for the prevalence of diabetes for 2015 and 2040. Diabetes Res Clin Pract 128:40–50. https://doi.org/10.1016/j.diabres.2017.03.024
Angus DC, Linde-Zwirble WT, Lidicker J, Clermont G, Carcillo J, Pinsky MR (2001) Epidemiology of severe sepsis in the United States: analysis of incidence, outcome, and associated costs of care. Crit Care Med 29(7):1303–1310. https://doi.org/10.1097/00003246-200107000-00002
Mayr FB, Yende S, Angus DC (2014) Epidemiology of severe sepsis. Virulence 5(1):4–11. https://doi.org/10.4161/viru.27372
Shah BR, Hux JE (2003) Quantifying the risk of infectious diseases for people with diabetes. Diabetes Care 26(2):510–513. https://doi.org/10.2337/diacare.26.2.510
Rao Kondapally Seshasai S, Kaptoge S, Thompson A, Di Angelantonio E, Gao P, Sarwar N, Whincup PH, Mukamal KJ, Gillum RF, Holme I, Njolstad I, Fletcher A, Nilsson P, Lewington S, Collins R, Gudnason V, Thompson SG, Sattar N, Selvin E, Hu FB, Danesh J, Emerging Risk Factors C (2011) Diabetes mellitus, fasting glucose, and risk of cause-specific death. N Engl J Med 364(9):829–841. https://doi.org/10.1056/NEJMoa1008862
Schuetz P, Castro P, Shapiro NI (2011) Diabetes and sepsis: preclinical findings and clinical relevance. Diabetes Care 34(3):771–778. https://doi.org/10.2337/dc10-1185
Alberti C, Brun-Buisson C, Burchardi H, Martin C, Goodman S, Artigas A, Sicignano A, Palazzo M, Moreno R, Boulme R, Lepage E, Le Gall R (2002) Epidemiology of sepsis and infection in ICU patients from an international multicentre cohort study. Intensive Care Med 28(2):108–121. https://doi.org/10.1007/s00134-001-1143-z
Kornum JB, Thomsen RW, Riis A, Lervang HH, Schonheyder HC, Sorensen HT (2008) Diabetes, glycemic control, and risk of hospitalization with pneumonia: a population-based case-control study. Diabetes Care 31(8):1541–1545. https://doi.org/10.2337/dc08-0138
Pearson-Stuttard J, Blundell S, Harris T, Cook DG, Critchley J (2016) Diabetes and infection: assessing the association with glycaemic control in population-based studies. Lancet Diabetes Endocrinol 4(2):148–158. https://doi.org/10.1016/S2213-8587(15)00379-4
Stegenga ME, van der Crabben SN, Blumer RM, Levi M, Meijers JC, Serlie MJ, Tanck MW, Sauerwein HP, van der Poll T (2008) Hyperglycemia enhances coagulation and reduces neutrophil degranulation, whereas hyperinsulinemia inhibits fibrinolysis during human endotoxemia. Blood 112(1):82–89. https://doi.org/10.1182/blood-2007-11-121723
Foss-Freitas MC, Foss NT, Donadi EA, Foss MC (2008) Effect of the glycemic control on intracellular cytokine production from peripheral blood mononuclear cells of type 1 and type 2 diabetic patients. Diabetes Res Clin Pract 82(3):329–334. https://doi.org/10.1016/j.diabres.2008.09.003
Bertoni AG, Saydah S, Brancati FL (2001) Diabetes and the risk of infection-related mortality in the U.S. Diabetes Care 24(6):1044–1049. https://doi.org/10.2337/diacare.24.6.1044
Kabeya Y, Shimada A, Tsukada N, Atsumi Y, Higaki M (2016) Diabetes affects length of stay and hospital costs for elderly patients with pneumonia: an analysis of a hospital administrative database. Tokai J Exp Clin Med 41(4):203–209
van Vught LA, Holman R, de Jonge E, de Keizer NF, van der Poll T (2017) Diabetes is not associated with increased 90-day mortality risk in critically ill patients with sepsis. Crit Care Med 45(10):e1026–e1035. https://doi.org/10.1097/CCM.0000000000002590
Esper AM, Moss M, Martin GS (2009) The effect of diabetes mellitus on organ dysfunction with sepsis: an epidemiological study. Crit Care 13(1):R18. https://doi.org/10.1186/cc7717
Trevelin SC, Carlos D, Beretta M, da Silva JS, Cunha FQ (2017) Diabetes mellitus and sepsis: a challenging association. Shock 47(3):276–287. https://doi.org/10.1097/SHK.0000000000000778
Moss M, Guidot DM, Steinberg KP, Duhon GF, Treece P, Wolken R, Hudson LD, Parsons PE (2000) Diabetic patients have a decreased incidence of acute respiratory distress syndrome. Crit Care Med 28(7):2187–2192. https://doi.org/10.1097/00003246-200007000-00001
Kang L, Han J, Yang QC, Huang HL, Hao N (2015) Effects of different blood glucose levels on critically ill patients in an intensive care unit. J Mol Microbiol Biotechnol 25(6):388–393. https://doi.org/10.1159/000441655
Koyfman L, Brotfain E, Erblat A, Kovalenko I, Reina YY, Bichovsky Y, Borer A, Friger M, Frenkel A, Klein M (2018) The impact of the blood glucose levels of non-diabetic critically ill patients on their clinical outcome. Anaesthesiol Intensive Ther 50(1):20–26. https://doi.org/10.5603/AIT.2018.0004
Akirov A, Elis A (2016) The prognostic significance of admission blood glucose levels in patients with urinary tract infection. Diabetes Res Clin Pract 115:99–105. https://doi.org/10.1016/j.diabres.2016.01.025
Furukawa M, Kinoshita K, Yamaguchi J, Hori S, Sakurai A (2019) Sepsis patients with complication of hypoglycemia and hypoalbuminemia are an early and easy identification of high mortality risk. Intern Emerg Med 14(4):539–548. https://doi.org/10.1007/s11739-019-02034-2
Falcone M, Tiseo G, Russo A, Giordo L, Manzini E, Bertazzoni G, Palange P, Taliani G, Cangemi R, Farcomeni A, Vullo V, Violi F, Venditti M (2016) Hospitalization for pneumonia is associated with decreased 1-year survival in patients with type 2 diabetes: results from a prospective cohort study. Medicine (Baltimore) 95(5):e2531. https://doi.org/10.1097/MD.0000000000002531
Friedman ND, Levit D, Taleb E, Marcus G, Michaeli L, Broide M, Mengesha B, Zaidenstein R, Lazarovitch T, Dadon M, Kaye KS, Marchaim D (2018) Towards a definition for health care-associated infection. Open Forum Infect Dis 5(6):ofy116. https://doi.org/10.1093/ofid/ofy116
Friedman ND, Kaye KS, Stout JE, McGarry SA, Trivette SL, Briggs JP, Lamm W, Clark C, MacFarquhar J, Walton AL, Reller LB, Sexton DJ (2002) Health care–associated bloodstream infections in adults: a reason to change the accepted definition of community-acquired infections. Ann Intern Med 137(10):791–797. https://doi.org/10.7326/0003-4819-137-10-200211190-00007
Singer M, Deutschman CS, Seymour CW, Shankar-Hari M, Annane D, Bauer M, Bellomo R, Bernard GR, Chiche JD, Coopersmith CM, Hotchkiss RS, Levy MM, Marshall JC, Martin GS, Opal SM, Rubenfeld GD, van der Poll T, Vincent JL, Angus DC (2016) The third international consensus definitions for sepsis and septic shock (Sepsis-3). JAMA 315(8):801–810. https://doi.org/10.1001/jama.2016.0287
McGrade P, Yang S, Nugent K (2019) The association between admission glucose levels and outcomes in adults admitted to a tertiary care hospital. J Community Hosp Intern Med Perspect 9(3):195–202. https://doi.org/10.1080/20009666.2019.1611318
Sotello D, Yang S, Nugent K (2019) Glucose and lactate levels at admission as predictors of in-hospital mortality. Cureus 11(10):e6027. https://doi.org/10.7759/cureus.6027
Kutz A, Struja T, Hausfater P, Amin D, Amin A, Haubitz S, Bernard M, Huber A, Mueller B, Schuetz P, group Ts (2017) The association of admission hyperglycaemia and adverse clinical outcome in medical emergencies: the multinational, prospective, observational TRIAGE study. Diabet Med 34(7):973–982. https://doi.org/10.1111/dme.13325
Dungan KM, Braithwaite SS, Preiser JC (2009) Stress hyperglycaemia. Lancet 373(9677):1798–1807. https://doi.org/10.1016/S0140-6736(09)60553-5
https://www.cdc.gov/nhsn/xls/master-organism-com-commensals-lists.xlsx. Accessed Jan 2020
Magiorakos AP, Srinivasan A, Carey RB, Carmeli Y, Falagas ME, Giske CG, Harbarth S, Hindler JF, Kahlmeter G, Olsson-Liljequist B, Paterson DL, Rice LB, Stelling J, Struelens MJ, Vatopoulos A, Weber JT, Monnet DL (2012) Multidrug-resistant, extensively drug-resistant and pandrug-resistant bacteria: an international expert proposal for interim standard definitions for acquired resistance. Clin Microbiol Infect 18(3):268–281. https://doi.org/10.1111/j.1469-0691.2011.03570.x
Leclercq R, Canton R, Brown DF, Giske CG, Heisig P, MacGowan AP, Mouton JW, Nordmann P, Rodloff AC, Rossolini GM, Soussy CJ, Steinbakk M, Winstanley TG, Kahlmeter G (2013) EUCAST expert rules in antimicrobial susceptibility testing. Clin Microbiol Infect 19(2):141–160. https://doi.org/10.1111/j.1469-0691.2011.03703.x
Cecconi M, Evans L, Levy M, Rhodes A (2018) Sepsis and septic shock. Lancet 392(10141):75–87. https://doi.org/10.1016/S0140-6736(18)30696-2
Huang ES, Laiteerapong N, Liu JY, John PM, Moffet HH, Karter AJ (2014) Rates of complications and mortality in older patients with diabetes mellitus: the diabetes and aging study. JAMA Intern Med 174(2):251–258. https://doi.org/10.1001/jamainternmed.2013.12956
Kanafani ZA, Kourany WM, Fowler VG Jr, Levine DP, Vigliani GA, Campion M, Katz DE, Corey GR, Boucher HW (2009) Clinical characteristics and outcomes of diabetic patients with Staphylococcus aureus bacteremia and endocarditis. Eur J Clin Microbiol Infect Dis 28(12):1477–1482. https://doi.org/10.1007/s10096-009-0808-3
Torres A, Peetermans WE, Viegi G, Blasi F (2013) Risk factors for community-acquired pneumonia in adults in Europe: a literature review. Thorax 68(11):1057–1065. https://doi.org/10.1136/thoraxjnl-2013-204282
Chao HY, Liu PH, Lin SC, Chen CK, Chen JC, Chan YL, Wu CC, Blaney GN, Liu ZY, Wu CJ, Chen KF (2017) Association of in-hospital mortality and dysglycemia in septic patients. PLoS ONE 12(1):e0170408. https://doi.org/10.1371/journal.pone.0170408
Schuetz P, Jones AE, Howell MD, Trzeciak S, Ngo L, Younger JG, Aird W, Shapiro NI (2011) Diabetes is not associated with increased mortality in emergency department patients with sepsis. Ann Emerg Med 58(5):438–444. https://doi.org/10.1016/j.annemergmed.2011.03.052
Michalopoulos A, Falagas ME, Karatza DC, Alexandropoulou P, Papadakis E, Gregorakos L, Chalevelakis G, Pappas G (2011) Epidemiologic, clinical characteristics, and risk factors for adverse outcome in multiresistant gram-negative primary bacteremia of critically ill patients. Am J Infect Control 39(5):396–400. https://doi.org/10.1016/j.ajic.2010.06.017
Pogue JM, Kaye KS, Cohen DA, Marchaim D (2015) Appropriate antimicrobial therapy in the era of multidrug-resistant human pathogens. Clin Microbiol Infect 21(4):302–312. https://doi.org/10.1016/j.cmi.2014.12.025
Paul M, Shani V, Muchtar E, Kariv G, Robenshtok E, Leibovici L (2010) Systematic review and meta-analysis of the efficacy of appropriate empiric antibiotic therapy for sepsis. Antimicrob Agents Chemother 54(11):4851–4863. https://doi.org/10.1128/AAC.00627-10
Grondman I, Pirvu A, Riza A, Ioana M, Netea MG (2020) Biomarkers of inflammation and the etiology of sepsis. Biochem Soc Trans 48(1):1–14. https://doi.org/10.1042/BST20190029
Hadjadj S, Coisne D, Mauco G, Ragot S, Duengler F, Sosner P, Torremocha F, Herpin D, Marechaud R (2004) Prognostic value of admission plasma glucose and HbA in acute myocardial infarction. Diabet Med 21(4):305–310. https://doi.org/10.1111/j.1464-5491.2004.01112.x
Di Carlo A, Lamassa M, Franceschini M, Bovis F, Cecconi L, Pournajaf S, Paravati S, Biggeri A, Inzitari D, Ferro S, Italian Study Group on Implementation of Stroke C (2018) Impact of acute-phase complications and interventions on 6-month survival after stroke. A prospective observational study. PLoS ONE 13(3):e0194786. https://doi.org/10.1371/journal.pone.0194786
van Vught LA, Wiewel MA, Klein Klouwenberg PM, Hoogendijk AJ, Scicluna BP, Ong DS, Cremer OL, Horn J, Bonten MM, Schultz MJ, van der Poll T, Molecular D, Risk Stratification of Sepsis C (2016) Admission hyperglycemia in critically ill sepsis patients: association with outcome and host response. Crit Care Med 44(7):1338–1346. https://doi.org/10.1097/CCM.0000000000001650
Hoang QN, Pisani MA, Inzucchi S, Hu B, Honiden S (2014) The prevalence of undiagnosed diabetes mellitus and the association of baseline glycemic control on mortality in the intensive care unit: a prospective observational study. J Crit Care 29(6):1052–1056. https://doi.org/10.1016/j.jcrc.2014.06.007
Ali MK, Bullard KM, Saaddine JB, Cowie CC, Imperatore G, Gregg EW (2013) Achievement of goals in U.S. diabetes care, 1999–2010. N Engl J Med 368(17):1613–1624. https://doi.org/10.1056/NEJMsa1213829
Plummer MP, Bellomo R, Cousins CE, Annink CE, Sundararajan K, Reddi BA, Raj JP, Chapman MJ, Horowitz M, Deane AM (2014) Dysglycaemia in the critically ill and the interaction of chronic and acute glycaemia with mortality. Intensive Care Med 40(7):973–980. https://doi.org/10.1007/s00134-014-3287-7
Egi M, Bellomo R, Stachowski E, French CJ, Hart GK, Taori G, Hegarty C, Bailey M (2011) The interaction of chronic and acute glycemia with mortality in critically ill patients with diabetes. Crit Care Med 39(1):105–111. https://doi.org/10.1097/CCM.0b013e3181feb5ea
Elixhauser A, Steiner C, Harris DR, Coffey RM (1998) Comorbidity measures for use with administrative data. Med Care 36(1):8–27
Funding
The authors received no funding.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors have nothing to declare.
Ethical approval
The study was approved by the local ethics (Helsinki) committee prior to its initiation.
Consent to participate
Due to its retrospective nature no consent was necessary.
Consent for publication
All authors give their consent for publication.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Zohar, Y., Zilberman Itskovich, S., Koren, S. et al. The association of diabetes and hyperglycemia with sepsis outcomes: a population-based cohort analysis. Intern Emerg Med 16, 719–728 (2021). https://doi.org/10.1007/s11739-020-02507-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11739-020-02507-9