Abstract
This study aims to assess the relationship between illness perception and disease course and symptoms in Behçet disease (BD). One hundred ten consecutive BD patients (F/M 50/60, mean age 38.5 ± 9.88 years) and 57 patients with Psoriasis as a disease control group (F/M 28/29, mean age 48.12 ± 15.52) are included in this cross-sectional study. Illness perception is evaluated using a revised version of the Illness Perception Questionnaire (IPQ-R). In IPQ-R, the identity score reflecting the number of symptoms is higher in BD patients with musculoskeletal involvement than the others (6.77 ± 2.91 vs. 5.08 ± 3.3, respectively, p = 0.007). The consequences score for musculoskeletal involvement (19.52 ± 7.03) and timeline (acute/chronic) score for eye involvement (26.67 ± 4.32) are also higher compared to patients without them (16.37 ± 5.82 and 22.09 ± 8.68) (p = 0.011 and p = 0.038), reflecting negative beliefs about the illness. The score of psychological attribution is higher in patients with psoriasis than BD (p = 0.039), whereas the other subgroup scores are lower in patients with psoriasis compared to those of BD (p < 0.05). This study provides a patient’s perspective in the disease management process of BD using the IPQ-R questionnaire. A patient’s own personal beliefs and emotional responses to their symptoms might affect the outcome measures, especially with musculoskeletal symptoms and eye involvement in BD. However, psychological attribution is found to be a prominent issue in psoriasis.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Chronic diseases are characterized by their long duration and their often incurable properties, which make them an important burden in healthcare. Since physical, psychological and social dysfunctions can be observed, patients often create their cognitive/mental representations and modify their health behaviour accordingly. Illness perception includes the description of symptoms, beliefs and expectations about the illnesses as well as perceived control of the progress [1,2,3]. Components of illness perception are identity (symptoms and illness labels), consequences (possible illness effect), control/cure, (curability of disease) timeline (expectation about the illness duration), cause (cause of illness) and emotional representation (emotional response to the disease) [2,3,4,5,6]. Since illness perceptions have been shown to influence patients’ satisfaction with the health-care, coping behaviour has been assessed in various chronic diseases such as rheumatoid arthritis [7, 8], systemic lupus erythematosus [9, 10] and vasculitis [1, 11].
Behçet’s disease (BD) as a chronic disorder is characterized by mucocutaneous, ocular, musculoskeletal, vascular, central nervous system and gastrointestinal involvement. Patients with BD are faced with unpredictable relapse patterns, tissue or organ damage and serious side effects of some treatment protocols. Although life-threatening major organ involvements can be prevented by immunosuppressive medications, a continued low disease activity can be observed in terms of both mucocutaneous and musculoskeletal involvement [12,13,14,15,16,17,18]. As predicted, fatigue [1, 11, 19], depression, anxiety [19] and unmet needs of therapies [13] may affect the emotional responses of BD patients. Similarly, emotional stress [20], shame, anger, anxiety [21], depression and internal stigma are psychological consequences of psoriasis [22], a multisystemic chronic dermatological disorder leading to an important physical and psychosocial burden. [23]. It does not affect the life span frequently, but the impact on the quality of life of the patients is quite dramatic. Patients feel themselves excluded from society because of their lesions. Therefore, the chronic disease pattern of psoriasis leads to difficulties in adjusting to treatment [24,25,26]. The data on illness perception of patients with Behçet’s disease are very sparse, and is derived from a study including groups of patients with various vasculitis [1, 11]. Since evaluation of illness perception gives critical information in the disease management, we aim to assess the relationship between illness perception and disease symptoms in BD.
Materials and methods
Patients
In this cross-sectional study, 110 consecutive BD patients (F/M 50/60, mean age 38.5 ± 9.88 years) who had been diagnosed according to the ISG criteria [27] and followed in the Behcet’s Disease Clinics of the Marmara University Medical School in Istanbul were included. Since both ISG criteria and ICBD criteria are used in the literature, we used the ISG criteria for the study design. In addition, 57 psoriasis patients were also included as a control group (F/M 28/29, mean age 48.12 ± 15.52) from the dermatology clinics of the same hospital. The clinical manifestations of the BD patients were as follows: oral ulcers (100%), genital ulcers (89.3%), cutaneous (91.8%), musculoskeletal (49.1%), ocular (33.6%), vascular (33%), neurological (2.7%) and gastrointestinal involvement (1.8%). A positive pathergy reaction was observed in 65.5% of patients. Six newly diagnosed patients (5.5%) had not received any treatment. Forty-eight patients (43.6%) were treated by colchicine (1–2 mg/day), whereas the others (n = 56, 50.9%), were treated with immune-suppressive agents.
The patients’ total clinical severity score was determined in BD as previously described [28]. The mean severity score in the whole group is 4.69 ± 1.54. The patients are categorized as follows: severe group: ≥ 4 points (n = 78, 70.9%), and mild group: < 4 points (n = 32, 29.1%).
The score of psoriasis area and severity index (PASI) as performed by the same dermatologist (TE) was 13.40 ± 8.28 in the group. The patients with psoriasis are categorized as follows: moderate–severe group: ≥ 10 PASI scores (n = 37, 63.8%), and mild group: < 10 PASI scores (n = 21, 36.2%).
The inclusion criteria are: being ≥ 18 years of age. The presence of other chronic conditions and mental health problems are criteria for exclusion in the study. The study was approved by the Ethics Committee of Marmara University Medical School (09.2018.122), and an informed consent was obtained from all of the involved patients.
Assessment of illness perception
The revised version of the Illness Perception Questionnaire (IPQ-R) is a quantitative and multifactorial assessment tool [6], and its Turkish version has been validated [29, 30]. The permission for the use of the questionnaire was received from Armay [30]. The questionnaire was completed by patients at the BD outpatient clinic before their visits. Trained interviewers, who were not involved in clinical practice, explained the objectives of the study, and helped patients to fill out the questionnaire.
The questionnaire consisted of three main sections. First, the Identity section relates to 14 common symptoms (Table 1). The sum of the yes-indicated items is used to calculate the total score (range 0–14 points). High scores reflect increase in the number of symptoms.
Second, Beliefs about illness section consists of 38 items with 7 subscales. Each item is rated on a five-point Likert scale, ranging from strongly disagree to strongly agree (Table 1). The scores of subscales are calculated according to the order of the questionnaire [30, 31]. The subscales of the sections are as follows: The consequences subscale represents the individual perception of the impact of the disease. The timeline (acute/chronic) represents the individual perception of the likely chronic duration of their health problems. The timeline cyclical represents the individual perception of the likely variability of the disease. The emotional representations dimension reflects the individual negative emotions experienced due to the disease. High scores for timeline, consequences, cyclic dimension and emotional representations reveal strongly held beliefs regarding the number of symptoms attributed to the illness, as well as the chronicity and the cyclical nature of the negative consequences and emotions regarding the condition. Illness coherence is used to reflect how the individual understands the disease. Personal control represents the individual’s perception of personal control, and treatment control represents the belief in a cure through treatment. High scores for the personal control, treatment control and illness coherence dimensions reflect positive beliefs regarding the illness and the understanding of the illness [2, 3, 6, 30, 31].
Third, the Cause section reflecting personal ideas is comprised of 18 possible etiologic factors in 4 dimensions such as psychological attributions, risk factors, immunity and chance [6, 30]. Each item is rated on a 5-point Likert scale, ranging from strongly disagrees to strongly agree (Table 1).
Test–Retest Reliability
External reliability is assessed by test–retest carried out on 10% of patients over a 1-month period by a single researcher (GM). Good stability is seen between the two time points (correlation coefficients ranging from 0.61 to 0.83).
Statistical analysis
The data were analysed using SPSS, version 16.0 (SPSS, Chicago, IL). Mann–Whitney U test and Spearman correlation tests were used in the analysis due to non-normal distribution of data. Internal consistency was examined by computing Cronbach’s alphas ranging from 0.704 to 0.910 in subgroups of IPQ-R, indicating good internal consistency.
Results
The IPQ-R questionnaire with three main sections regarding identity, beliefs about illness and cause is used to measure illness perception in the present study. IPQ-R scores are compared between BD and psoriasis. The score of psychological attribution is higher in patients with psoriasis than BD (p = 0.039) whereas the other subgroup scores regarding identity, timeline acute/chronic, personal control, treatment control, illness coherence and immunity are lower in patients with psoriasis compared to those of BD (p < 0.05) (Table 1).
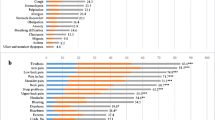
In the identity section of the questionnaire, patients were asked about symptoms attributed to their illness. Fatigue (77.3%) and pain (67.3%) are highly rated symptoms. The mean score is found to be 5.91 ± 3.29 in BD. Identity score reflecting is higher in patients with musculoskeletal involvement (6.77 ± 2.91) than without (5.08 ± 3.3) (p = 0.007). However, no significant difference was observed in identity score according to disease course and gender (p > 0.05) (Table 2). In psoriasis, identity score was lower in males (1.07 ± 1.60) compared to females (2.67 ± 2.52) (p = 0.019) (Table 3).
The scores of subgroups in beliefs about the illness are similar in both mild and severe disease course in BD (p > 0.05) (Table 2). The scores of emotional representation are higher in female patients (20.4 ± 7.32) than male patients in BD (17.22 ± 7.12) (p = 0.029) (Table 2). In BD, patients with musculoskeletal involvement (19.52 ± 7.03) had significantly higher consequences scores than those without it (16.37 ± 5.82) (p = 0.011). Similarly, the timeline (acute/chronic) score for eye involvement is higher compared to the other cases (eye involvement (+): 26.67 ± 4.32 vs eye involvement (−): 22.09 ± 8.68) (p = 0.038) (Table 1).
In psoriasis patients, the score of consequence is higher in females (19.29 ± 4.04) than males (16.28 ± 5.60) (p = 0.037). However, no significant relation is observed with the other subgroups (p > 0.05) (Table 3).
The Cause section that reflected personal ideas about aetiology of the disease, includes psychological attributions, risk factors, immunity and chance subgroups (Table 1). The scores of psychological attributions and immunity are higher in females compared to males in BD (p = 0.026 and p = 0.047, respectively) (Table 2). When the items in these subgroups are analysed according to disease course, significant differences are not observed in BD (p > 0.05). Similarly, in patients with psoriasis, there is no significant relationship between the scores of the cause section and gender and disease severity (p > 0.05) (Table 3).
In psoriasis, PASI scores are higher in males (15.88 ± 7.94) than females (10.63 ± 7.98) (p = 0.016). Similar to BD, no significant difference is observed with subscale scores of IPQ-R according to disease course in patients with psoriasis (p > 0.05) (Table 3).
Discussion
Patients’ self-management behaviour regarding their knowledge, perceptions of their condition and the treatments they are subjected to, can be explained by illness perception [1, 11, 22, 23]. In the present study, an IPQ-R questionnaire consisting of three main sections was given to patients with BD and controls with psoriasis.
As predicted, illness perception varied according to the disease nature, severity and gender. In patients with BD, poor scores are observed in identity and timeline acute/chronic reflecting negative beliefs whereas the scores of positive beliefs regarding personal control, treatment control, illness coherence and immunity are higher in BD compared to those of psoriasis. However, psychological attribution is a prominent issue in psoriasis compared to BD. This is unsurprising since Psoriasis is well-known to have a significant psychosocial impact of QoL [21,22,23, 26].
In the identity section, BD patients rate disease-specific symptoms among their commonly occurring symptoms. Fatigue and pain are highly rated symptoms. Since fatigue is commonly observed in BD as in other inflammatory diseases [1, 11, 32, 33], and pain frequently occurs [34] in musculoskeletal diseases, our results are in accordance with previous studies. In addition, the expected effects and outcomes of BD were assessed in the consequences subscale. With musculoskeletal involvement, poor consequences scores are observed. Since complete remission could not be achieved in clinical practice [13], these results could be predicted.
Patients with eye involvement are more affected by chronic duration of the disease compared to those without eye involvement according to timeline (acute/chronic) scores. The eye involvement with its recurrent nature limits patients’ lives although conventional therapies and biologic agents in resistant cases might be effective to decrease attacks and increase visual acuity. Moreover, patients with eye involvement are found to be very sensitive to anxiety and depression status associated with the relapse [35, 36]. Therefore, clinicians may emphasize the predicted course and beneficial outcomes of the treatment in managing these cases.
The emotional representation dimension reflects the patients’ negative emotional experiences due to the symptoms of BD. Emotional reactions following the start of symptoms were are more commonly observed in female patients. Moreover, the psychological and immune attributions reflecting more negative illness beliefs in the Cause section are poorer in females. A more complex emotional causal model is observed in females. Since female patients feel more psychological stress compared to men [37, 38], these results could be predicted.
The scores of causal subgroups are similar according to the disease course and gender in psoriasis. There are a few BD cases that have been attributed to microorganisms and genetics in the present study, although they are important parts of the disease aetiology [39,40,41,42,43,44,45,46]. Interestingly, change in treatment protocol is accepted as a reason for relapse in BD patients in a previous study [1].
If health professionals could understand the patient’s beliefs and opinions and pay attention to them, better clinical outcomes could be achieved in these patients [47,48,49,50]. In this condition, the Chronic Care Model (CCM) could be thought in disease management. It is a tool developed to improve self-management of patients with chronic illness. Self-management support one of the components of CCM, includes skill-based learning and empowerment of patients [51, 52]. In this perspective, patient education programs are needed for improving patient-centred care according to different organ involvement with the multidisciplinary team in BD. Similarly, they could help to overcome social stigmatism in patients with psoriasis. Finally, the implementation of the CCM into the treatment plans could change health behaviour of patients and enhance patient reported outcome measures and their self-management in BD and psoriasis.
Since a patient’s own personal beliefs and emotional responses to symptoms might affect the disease management, results of the study give important information. However, the main limitation of the study is the limited number of patient reported outcome measures used. Fatigue and pain were not evaluated by specific questionnaires according to study protocol.
In summary, this study provides a patient’s perspective in the disease management process of BD using an IPQ-R questionnaire. Patients with BD perceive more symptoms and negative opinions about musculoskeletal symptoms and eye involvement. In their causal model, female patients reveal a high level of emotional distress due to their symptoms. In this condition, patient education programs may be beneficial for patient empowerment in the disease management.
References
Grayson PC, Amudala NA, McAlear CA, Leduc RL, Shereff D, Richesson R, Fraenkel L, Merkel PA (2014) Causal attributions about disease onset and relapse in patients with systemic vasculitis. J Rheumatol 41(5):923–930. https://doi.org/10.3899/jrheum.131096
Brzoska P, Yilmaz-Aslan Y, Sultanoglu E, Sultanoglu B, Razum O (2012) The factor structure of the Turkish version of the Revised Illness Perception Questionnaire (IPQ-R) in patients with diabetes and cardiovascular disease. BMC Public Health 12:852. https://doi.org/10.1186/1471-2458-12-852
Weinman J, Petrie KJ, Moss-Morris R, Horne R (1996) The Illness Perception Questionnaire: a new method for assessing the cognitive representation of illness. Psychol Health 11(3):431–445
Figueiras MJ, Cortes MA, Marcelino D, Weinman J (2010) Lay views about medicines: the influence of the illness label for the use of generic versus brand. Psychol Health 25(9):1121–1128. https://doi.org/10.1080/08870440903137170
Leventhal H, Brissette I, Leventhal EA (2003) The common-sense model of self-regulation of health and illness. Self-regulation Health Illn Behav 1:42–65
Moss-Morris R, Weinman J, Petrie K, Horne R, Cameron L, Buick D (2002) The Revised Illness Perception Questionnaire (IPQ-R). Psychol Health 17(1):1–16
Ziarko M, Mojs E, Piasecki B, Samborski W (2014) The mediating role of dysfunctional coping in the relationship between beliefs about the disease and the level of depression in patients with rheumatoid arthritis. Sci World J 2014:585063. https://doi.org/10.1155/2014/585063
Leysen M, Nijs J, Meeus M, Paul van Wilgen C, Struyf F, Vermandel A, Kuppens K, Roussel NA (2015) Clinimetric properties of Illness Perception Questionnaire Revised (IPQ-R) and Brief Illness Perception Questionnaire (Brief IPQ) in patients with musculoskeletal disorders: a systematic review. Man Ther 20(1):10–17. https://doi.org/10.1016/j.math.2014.05.001
Daleboudt GM, Broadbent E, Berger SP, Kaptein AA (2011) Illness perceptions in patients with systemic lupus erythematosus and proliferative lupus nephritis. Lupus 20(3):290–298. https://doi.org/10.1177/0961203310385552
Barbasio C, Vagelli R, Marengo D, Querci F, Settanni M, Tani C, Mosca M, Granieri A (2015) Illness perception in systemic lupus erythematosus patients: the roles of alexithymia and depression. Compr Psychiatry 63:88–95. https://doi.org/10.1016/j.comppsych.2015.09.004
Grayson PC, Amudala NA, McAlear CA, Leduc RL, Shereff D, Richesson R, Fraenkel L, Merkel PA (2013) Illness perceptions and fatigue in systemic vasculitis. Arthritis Care Res 65(11):1835–1843. https://doi.org/10.1002/acr.22069
Alibaz-Oner F, Karadeniz A, Ylmaz S, Balkarl A, Kimyon G, Yazc A, Cnar M, Ylmaz S, Yldz F, Bilge SY, Bilgin E, Coskun BN, Omma A, Cetin GY, Cagatay Y, Karaaslan Y, Sayarlioglu M, Pehlivan Y, Kalyoncu U, Karadag O, Kasifoglu T, Erken E, Pay S, Cefle A, Kisacik B, Onat AM, Cobankara V, Direskeneli H (2015) Behcet disease with vascular involvement: effects of different therapeutic regimens on the incidence of new relapses. Medicine 94(6):e494. https://doi.org/10.1097/MD.0000000000000494
Alibaz-Oner F, Mumcu G, Kubilay Z, Ozen G, Celik G, Karadeniz A, Can M, Oner SY, Inanc N, Atagunduz P, Ergun T, Direskeneli H (2014) Unmet need in Behcet’s disease: most patients in routine follow-up continue to have oral ulcers. Clin Rheumatol 33(12):1773–1776. https://doi.org/10.1007/s10067-014-2585-3
Merkel PA, Aydin SZ, Boers M, Cornell C, Direskeneli H, Gebhart D, Hatemi G, Luqmani R, Matteson EL, Milman N, Robson J, Seo P, Tomasson G (2014) Current status of outcome measure development in vasculitis. J Rheumatol 41(3):593–598. https://doi.org/10.3899/jrheum.131248
Hatemi G, Merkel PA, Hamuryudan V, Boers M, Direskeneli H, Aydin SZ, Yazici H (2014) Outcome measures used in clinical trials for Behcet syndrome: a systematic review. J Rheumatol 41(3):599–612. https://doi.org/10.3899/jrheum.131249
Mumcu G, Inanc N, Taze A, Ergun T, Direskeneli H (2014) A new Mucocutaneous Activity Index for Behcet’s disease. Clin Exp Rheumatol 32(4 Suppl 84):S80–S86
Hatemi G, Ozguler Y, Direskeneli H, Mahr A, Gul A, Levi V, Aydin SZ, Mumcu G, Sertel-Berk O, Stevens RM, Yazici H, Merkel PA (2015) Current Status, Goals, and Research Agenda for Outcome Measures Development in Behcet syndrome: report from OMERACT 2014. J Rheumatol 42(12):2436–2441. https://doi.org/10.3899/jrheum.141147
Emmi G, Silvestri E, Squatrito D, D’Elios MM, Ciucciarelli L, Prisco D, Emmi L (2014) Behcet’s syndrome pathophysiology and potential therapeutic targets. Intern Emerg Med 9(3):257–265. https://doi.org/10.1007/s11739-013-1036-5
Ilhan B, Can M, Alibaz-Oner F, Yilmaz-Oner S, Polat-Korkmaz O, Ozen G, Mumcu G, Maradit Kremers H, Direskeneli H (2016) Fatigue in patients with Behcet’s syndrome: relationship with quality of life, depression, anxiety, disability and disease activity. Int J Rheum Dis. https://doi.org/10.1111/1756-185x.12839
Basavaraj KH, Navya MA, Rashmi R (2011) Stress and quality of life in psoriasis: an update. Int J Dermatol 50(7):783–792. https://doi.org/10.1111/j.1365-4632.2010.04844.x
Sampogna F, Tabolli S, Abeni D, investigators IDIMPRoVE (2012) Living with psoriasis: prevalence of shame, anger, worry, and problems in daily activities and social life. Acta Derm Venereol 92(3):299–303. https://doi.org/10.2340/00015555-1273
Hayes J, Koo J (2010) Psoriasis: depression, anxiety, smoking, and drinking habits. Dermatol Ther 23(2):174–180. https://doi.org/10.1111/j.1529-8019.2010.01312.x
Tula E, Ergun T, Seckin D, Ozgen Z, Avsar E (2017) Psoriasis and the liver: problems, causes and course. Australas J Dermatol 58(3):194–199. https://doi.org/10.1111/ajd.12460
Lin TY, See LC, Shen YM, Liang CY, Chang HN, Lin YK (2011) Quality of life in patients with psoriasis in northern Taiwan. Chang Gung Med J 34(2):186–196
Tang MM, Chang CC, Chan LC, Heng A (2013) Quality of life and cost of illness in patients with psoriasis in Malaysia: a multicenter study. Int J Dermatol 52(3):314–322. https://doi.org/10.1111/j.1365-4632.2011.05340.x
Alpsoy E, Polat M, FettahlioGlu-Karaman B, Karadag AS, Kartal-Durmazlar P, YalCin B, Emre S, Didar-Balci D, Bilgic-Temel A, Arca E, Koca R, Gunduz K, Borlu M, Ergun T, Dogruk-Kacar S, Cordan-Yazici A, Dursun P, Bilgi CO, Gunes-Bilgili S, Sendur N, Baysal O, Halil-Yavuz I, Yagcioglu G, Yilmaz E, Kavuzlu U, Senol Y (2017) Internalized stigma in psoriasis: a multicenter study. J Dermatol 44(8):885–891. https://doi.org/10.1111/1346-8138.13841
International Study Group for Behcet’s Disease (1990) Criteria for diagnosis of Behcet’s disease. Lancet 335(8697):1078–1080
Krause I, Mader R, Sulkes J, Paul M, Uziel Y, Adawi M, Weinberger A (2001) Behcet’s disease in Israel: the influence of ethnic origin on disease expression and severity. J Rheumatol 28(5):1033–1036
Kocaman N, Özkan M, Armay Z, Özkan S (2007) Hastalik Algisi Ölçeginin Türkçe uyarlamasinin geçerlilik ve güvenilirlik çalismasi [Reliability and validity study of the Turkish adaptation of the revised Illness Perception Questionnaire]. Anadolu Psikiyatri Dergisi 8:271–280
http://www.uib.no/ipq/. Accessed 10 Oct 2018
Ashley L, Smith AB, Keding A, Jones H, Velikova G, Wright P (2013) Psychometric evaluation of the revised Illness Perception Questionnaire (IPQ-R) in cancer patients: confirmatory factor analysis and Rasch analysis. J Psychosom Res 75(6):556–562. https://doi.org/10.1016/j.jpsychores.2013.08.005
Buyuktas D, Hatemi G, Yuksel-Findikoglu S, Ugurlu S, Yazici H, Yurdakul S (2015) Fatigue is correlated with disease activity but not with the type of organ involvement in Behcet’s syndrome: a comparative clinical survey. Clin Exp Rheumatol 33(6 Suppl 94):S107–S112
Melikoglu M, Melikoglu MA (2014) What affects the quality of life in patients with Behcet’s disease? Acta Reumatol Port 39(1):46–53
Backman CL, Kennedy SM, Chalmers A, Singer J (2004) Participation in paid and unpaid work by adults with rheumatoid arthritis. J Rheumatol 31(1):47–56
Hatemi G, Seyahi E, Fresko I, Talarico R, Hamuryudan V (2015) Behcet’s syndrome: a critical digest of the 2014-2015 literature. Clin Exp Rheumatol 33(6 Suppl 94):S3–S14
Tanriverdi N, Taskintuna Duru C, Ozdal P, Ortac S, Firat E (2003) Health-related quality of life in Behcet patients with ocular involvement. Jpn J Ophthalmol 47(1):85–92
Trovato GM, Pace P, Cangemi E, Martines GF, Trovato FM, Catalano D (2012) Gender, lifestyles, illness perception and stress in stable atrial fibrillation. Clin Ter 163(4):281–286
Fabiani C, Vitale A, Orlando I, Sota J, Capozzoli M, Franceschini R, Galeazzi M, Tosi GM, Frediani B, Cantarini L (2017) Quality of life impairment in Behcet’s disease and relationship with disease activity: a prospective study. Intern Emerg Med 12(7):947–955. https://doi.org/10.1007/s11739-017-1691-z
Karacayli U, Mumcu G, Simsek I, Pay S, Kose O, Erdem H, Direskeneli H, Gunaydin Y, Dinc A (2009) The close association between dental and periodontal treatments and oral ulcer course in behcet’s disease: a prospective clinical study. J Oral Pathol Med 38(5):410–415. https://doi.org/10.1111/j.1600-0714.2009.00765.x
Mumcu G, Ergun T, Inanc N, Fresko I, Atalay T, Hayran O, Direskeneli H (2004) Oral health is impaired in Behcet’s disease and is associated with disease severity. Rheumatology (Oxford) 43(8):1028–1033. https://doi.org/10.1093/rheumatology/keh236
Mumcu G, Inanc N, Aydin SZ, Ergun T, Direskeneli H (2009) Association of salivary S. mutans colonisation and mannose-binding lectin deficiency with gender in Behcet’s disease. Clin Exp Rheumatol 27(2 Suppl 53):S32–36
Kaneko F, Oyama N, Nishibu A (1997) Streptococcal infection in the pathogenesis of Behcet’s disease and clinical effects of minocycline on the disease symptoms. Yonsei Med J 38(6):444–454
Kaneko F, Oyama N, Yanagihori H, Isogai E, Yokota K, Oguma K (2008) The role of streptococcal hypersensitivity in the pathogenesis of Behcet’s disease. Eur J Dermatol 18(5):489–498. https://doi.org/10.1684/ejd.2008.0484
Ognenovski M, Renauer P, Gensterblum E, Kotter I, Xenitidis T, Henes JC, Casali B, Salvarani C, Direskeneli H, Kaufman KM, Sawalha AH (2015) Whole exome sequencing identifies rare protein-coding variants in Behcet’s disease. Arthritis Rheumatol. 1:2–5. https://doi.org/10.1002/art.39545
Hughes T, Ture-Ozdemir F, Alibaz-Oner F, Coit P, Direskeneli H, Sawalha AH (2014) Epigenome-wide scan identifies a treatment-responsive pattern of altered DNA methylation among cytoskeletal remodeling genes in monocytes and CD4 + T cells from patients with Behcet’s disease. Arthritis Rheumatol 66(6):1648–1658. https://doi.org/10.1002/art.38409
Direskeneli H, Mumcu G (2010) A possible decline in the incidence and severity of Behcet’s disease: implications for an infectious etiology and oral health. Clin Exp Rheumatol 28(4 Suppl 60):S86–S90
Mumcu G, Lehimci F, Fidan O, Guk H, Alpar U, Unal AU, Erturk Z, Alibaz Oner F, Inanc GN, Ergun SAT, Direskeneli RH (2017) The assessment of work productivity and activity impairment in Behcet’s disease. Turk J Med Sci 47(2):535–541. https://doi.org/10.3906/sag-1603-161
Mumcu G, Alibaz-Oner F, Oner SY, Ozen G, Atagunduz P, Inanc N, Koksal L, Ergun T, Direskeneli H (2017) Oral ulcer activity in Behcet’s disease: poor medication adherence is an underestimated risk factor. Eur J Rheumatol 4(2):109–112. https://doi.org/10.5152/eurjrheum.2017.160094
Yilmaz-Oner S, Ilhan B, Can M, Alibaz-Oner F, Polat-Korkmaz O, Ozen G, Mumcu G, Kremers HM, Tuglular S, Direskeneli H (2017) Fatigue in systemic lupus erythematosus: association with disease activity, quality of life and psychosocial factors. Z Rheumatol 76(10):913–919. https://doi.org/10.1007/s00393-016-0185-0
Sreih AG, Alibaz-Oner F, Easley E, Davis T, Mumcu G, Milman N, Robson J, Direskeneli H, Merkel PA, Cronholm P (2018) Health-related outcomes of importance to patients with Takayasu’s arteritis. Clin Exp Rheumatol 36(111 Suppl 2):51–57
Wagner EH, Austin BT, Davis C, Hindmarsh M, Schaefer J, Bonomi A (2001) Improving chronic illness care: translating evidence into action. Health Aff (Millwood) 20(6):64–78. https://doi.org/10.1377/hlthaff.20.6.64
Wagner EH, Davis C, Schaefer J, Von Korff M, Austin B (1999) A survey of leading chronic disease management programs: are they consistent with the literature? Manag Care Q 7(3):56–66
Acknowledgements
There is no financial support and conflict of interests of each author in the manuscript.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
There were no financial support and conflict of interest.
Statement of human and animal rights
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study
Additional information
This article is part of the topical collection “Behcet Disease”.
Rights and permissions
About this article
Cite this article
Mumcu, G., Yağar, F., Alibaz-Öner, F. et al. Does illness perception associate with disease symptoms in Behçet’s disease?. Intern Emerg Med 14, 691–697 (2019). https://doi.org/10.1007/s11739-018-1983-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11739-018-1983-y