Abstract
Angiotensin II (Ang II), a major effector of the renin–angiotensin system, is now recognized as a pro-inflammatory mediator. This Ang II signaling, which causes transcription of pro-inflammatory genes, is regulated through nuclear factor-κB (NF-κB). At present, the molecular mechanisms underlying the effect of aging on Ang II signaling and NF-κB activation are not fully understood. The purpose of this study was to document altered molecular events involved in age-related changes in Ang II signaling and NF-κB activation. Experimentations were carried out using kidney tissues from Fischer 344 rats at 6, 12, 18, and 24 months of age, and the rat endothelial cell line, YPEN-1 for the detailed molecular work. Results show that increases in Ang II and Ang II type 1 receptor during aging were accompanied by the generation of reactive species. Increased Ang II activated NF-κB by phosphorylating IκBα and p65. Increased phosphorylation of p65 at Ser 536 was mediated by the enhanced phosphorylation of IκB kinase αβ, while phosphorylation site Ser 276 of p65 was mediated by upregulated mitogen-activated and stress-activated protein kinase-1. These altered molecular events in aged animals were partly verified by experiments using YPEN-1 cells. Collectively, our findings provide molecular insights into the pro-inflammatory actions of Ang II, actions that influence the phosphorylation of p65-mediated NF-κB activation during aging. Our study demonstrates the age-related pleiotropic nature of the physiologically important Ang II can change into a deleterious culprit that contributes to an increased incidence of many chronic diseases such as atherosclerosis, diabetes, and dementia.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Angiotensin II (Ang II), a major effector of the renin–angiotensin system (RAS), is a potent vasoconstrictor. However, recent studies have shown that it is also a potent mediator in the activation of inflammatory mechanisms during age-related vascular and renal disease (Basso et al. 2005; Diz and Lewis 2008). The use of Ang II antagonists in the treatment of these age-related diseases provides strong support for its pro-inflammatory role (de Cavanagh et al. 2003, 2004). The pro-inflammatory actions of Ang II are shown to mediate intracellular signaling pathways by binding to their specific receptor, Ang II type 1 receptor (AT1; Swanson et al. 1992; Stumpf et al. 2005). Supporting evidence for receptor mediation comes from experiments in which AT1 knockout mice protected multiple organs from oxidative damage and alleviated the aging-like phenotype associated with increased life span (Cassis et al. 2010).
The involvement of Ang II in oxidative stress was revealed in multiple ways. For instance, the interaction of Ang II and AT1 activates multiple intracellular signaling pathways involved in the production of reactive species (RS) that lead to the activation of transcription factors such as the redox-sensitive nuclear factor-κB (NF-κB). Another way relates to RS production in Ang II signaling through nicotinamide adenine dinucleotide phosphate (NADPH) oxidases, which contributes to various pro-inflammatory cascade events. In addition, evidence from Ang II infusion that generates RS and compromises endogenous antioxidant enzyme activity with disrupted redox signaling in the rat kidney further supports the pro-inflammatory action of Ang II (Ferder et al. 2006; Alvarez et al. 2004). Based on what is known about redox imbalances due to RS production and compromised antioxidative defenses, extensive alterations in cellular and molecular signaling pathways are expected in the regulation of redox-sensitive transcriptional activities such as activation of the pro-inflammatory factor NF-κB.
Reports from our laboratory on the modulation of NF-κB highlight inflammation during aging (Kim et al. 2002a, b; Chung et al. 2006). Based on our own data and those of others, we proposed a molecular inflammation hypothesis of aging (Chung et al. 2009) and described a central role for redox-sensitive NF-κB in the modulation of the gene expression of several pro-inflammatory cytokines. NF-κB is widely expressed in various mammalian tissues and can be activated by a variety of stimuli (Gilmore 2006), particularly by oxidative stress (Yu and Chung 2006). The inactive form of NF-κB, due to inhibitory subunits in the complex, is activated by at least two different pathways: (1) release of the inhibitory protein κBα (IκBα) by phosphorylation of κBα and (2) phosphorylation of another subunit, p65, of the NF-κB complex, without phosphorylation of IκBα (Chen and Greene 2004; Basseres and Baldwin 2006). Previous studies show that Ang II’s action on NF-κB activation is carried out by the phosphorylation of IκBα (Ruiz-Ortega et al. 2006; Hoffmann et al. 2002; Luo et al. 2005). However, Ang II-induced NF-κB activation by the phosphorylation of p65 is not established.
Other investigators have reported that p65 phosphorylation events occur in the cytoplasm due to the participation of various kinases. It is known that several pro-inflammatory stimuli, such as TNFα, UV light, and LPS, induce phosphorylation of p65 at the Ser 536 residue, which is triggered by IKKαβ phosphorylation in the cytoplasm. Recent studies indicate that Ang II also activates NF-κB through the phosphorylation of p65 at Ser 536, which is shown to be mediated by IKKαβ phosphorylation in various cellular models (Cui et al. 2006; Douillette et al. 2006; Wei et al. 2008). However, these findings are in contrast to earlier findings on TNFα showing Ser 276 phosphorylation by mitogen- and stress-activated protein kinase-1 (MSK-1) in the nucleus (Viatour et al. 2005; Zhong et al. 2002). TNFα phosphorylates the cytoplasmic extracellular response kinase (ERK) and p38 mitogen-activated protein kinase (MAPKs). ERK-dependent nucleic MSK-1 also undergoes phosphorylation by TNFα. However, at present, the mechanisms involving the action of Ang II on Ser 276 phosphorylation of p65 are not well delineated. In our previous studies, we reported NF-κB activation through Ser 536 phosphorylation of p65 during aging (Kim et al. 2010a, b; Lee et al. 2009), but age-related Ang II-induced molecular modulation of Ser 536 phosphorylation of p65 has not been explored.
The purpose of this study was to investigate the insight of the molecular events leading to Ang II through AT1 receptors and to explore how these molecular events are compromised by the pro-inflammatory effect of aging using kidney tissue. Thus, in the current study, we focused on aging-related changes in the molecular effects of Ang II on NF-κB activation through p65 phosphorylation.
Materials and methods
Reagents
All chemical reagents were obtained from Sigma (St. Louis, MO, USA), except where noted. Angiotensin II enzyme immunoassay kits were obtained from Phoenix Pharmaceuticals (Belmont, CA, USA). Dichlorodihydrofluorescein diacetate (DCF-DA), dihydrorhodamine 123 (DHR-123), and Antibody BeaconTM tyrosine kinase assay kits were obtained from Molecular Probes, Inc. (Eugene, OR, USA). West-zolTM Plus was obtained from iNtRON Biotechnology (Seongnam, Korea). Antibodies were obtained from Santa Cruz Biotechnology (Santa Cruz, CA, USA), Cell Signaling Technology (New England, Hertfordshire, UK), or Upstate Biotechnology (Charlottesville, VA, USA). Polyvinylidene difluoride (PVDF) membranes were obtained from Millipore Corporation (Bedford, MA, USA). Sterile plasticware for tissue culture was purchased from SPL Labware (Seoul, Korea). All other materials were obtained in the highest available grade.
Animals
Procedures for maintaining specific pathogen-free rats and chow dietary composition have been previously reported (Bertrand et al. 1999). Briefly, male Fischer 344 rats were fed a diet having the following composition: 21% soybean protein, 15% sucrose, 43.65% dextrin, 10% corn oil, 0.15% α-methionine, 0.2% choline chloride, 5% salt mix, 2% vitamin mix, and 3% Solka-Floc fed ad libitum. Rats at 6, 12, 18, and 24 months of age were killed by decapitation, and the kidneys were quickly removed and rinsed in iced-cold buffer [100 mM Tris, 1 mM ethylenediaminetetraacetic acid (EDTA), 0.2 mM PMSF, 1 μM pepstatin, 2 μM leupeptin, 80 mg/L trypsin inhibitor, 20 mM β-glycerophosphate, 20 mM NaF, 2 mM sodium orthovanadate, pH 7.4]. The tissue was immediately frozen in liquid nitrogen and stored at −80°C. The frozen kidney tissues was collected and supplied by Aging Tissue Bank. This study complied with the Guide for the Care and Use of Laboratory Animals published by the US National Institutes of Health (publication no. 85-23) and was approved by an Institutional Animal Care and Use Committee. For the current study, we chose to use kidney tissue because of its vulnerability to age-related oxidative stress and its redox-sensitive NF-κB. In addition, all components of the RAS are synthesized within the kidney (Carey and Siragy 2003; Kobori et al. 2007).
Tissue preparations
Three hundred milligrams of frozen kidney tissue was homogenized in 2 mL of hypotonic lysis buffer [buffer A: 10 mM KCl, 2 mM MgCl2, 1 mM dithiothreitol (DTT), 0.1 mM EDTA, 0.1 mM PMSF, 1 μM pepstatin, 2 μM leupeptin, 20 mM β-glycerophosphate, 20 mM NaF and 2 mM Na3VO4, 10 mM HEPES, pH 7.4] using a tissue homogenizer for 20 s. Homogenates were kept on ice for 15 min, 125 μl of 10% Nonidet P-40 (NP-40) solution was added and mixed for 15 s, and the mixture was centrifuged at 14,000×g for 2 min. The supernatants were used as the cytosol fraction. The pelleted nuclei were washed once with 400 μL of buffer A plus 25 μl of 10% NP-40, centrifuged, suspended in 200 μl of buffer C [50 mM KCl, 300 mM NaCl, 0.1 mM PMSF, 10% (v/v) glycerol, 1 μM pepstatin, 2 μM leupeptin, 20 mM β-glycerophosphate, 20 mM NaF, 2 mM Na3VO4, and 50 mM HEPES, pH 7.8], kept on ice for 30 min, and centrifuged at 14,000×g for 10 min. The supernatant (nuclear protein) was harvested and then stored at −80°C (Kim et al. 2010a, b). Protein concentration was measured by the bicinchonic acid (BCA) assay.
Cell line and culture conditions
Kidney mainly consists of endothelial cells. Thus, we chose to use rat endothelial cell line, YPEN-1. In addition, our laboratory’s extensive experiences with YPEN-1 cells were appropriated for molecular work on oxidative stress-related changes in our previous studies. YPEN-1 cells were obtained from ATCC (Manassas, VA, USA). The cells were grown in Dulbecco’s modified Eagle’s medium (Nissui, Tokyo, Japan) containing 2 mM l-glutamine, 100 mg/mL penicillin–streptomycin, 2.5 mg/L amphotericin B, and 10% heat-inactivated fetal bovine serum. Cells were maintained at 37°C in a humidified atmosphere containing 5% CO2/95% air. The medium was replaced with fresh medium after 1 day to remove non-adherent cells or cell debris.
Cell lysis
Cells were washed with phosphate-buffered saline (PBS) and then 1 ml of ice-cold PBS was added. Pellets were harvested at 1,000×g at 4°C for 5 min. The pellets were suspended in 10 mM Tris, pH 8.0, with 1.5 mM MgCl2, 1 mM DTT, 0.1% NP-40, and protease inhibitors; incubated on ice for 15 min; and then centrifuged at 14,000×g at 4°C for 15 min. The supernatants were used as the cytosolic fractions and the pellets resuspended in 10 mM Tris, pH 8.0, with 50 mM KCl, 100 mM NaCl, and protease inhibitor; incubated on ice for 30 min; then centrifuged at 14,000×g at 4°C for 30 min. The resultant supernatants were used as the nuclear fraction (Kim et al. 2010a, b). Protein concentration was measured by the BCA assay.
Quantitation of redox status
Measurement of RS
A fluorometric assay was used to determine levels of RS, which included superoxide radicals, hydroxyl radicals, and hydrogen peroxide. Non-fluorescent DCF-DA was oxidized to the highly fluorescent 2′,7′-dichlorofluorescin (DCF) in the presence of esterases and RS, including lipid peroxides. For tissue homogenates, briefly, RS generation was measured as previously described in materials utilizing a fluorescence probe. Briefly, 25 μM of 2′,7′-DCF-DA was added to homogenates to a 250-μl final volume. Changes in fluorescence intensity were measured every 5 min for 30 min on a fluorescence plate reader, GENios (Tecan Instruments, Salzburg, Austria), with excitation and emission wavelengths set at 485 and 530 nm, respectively.
Measurement of peroxynitrite
Peroxynitrite (ONOO−) generation was measured by monitoring the oxidation of DHR 123. Briefly, 10 μl homogenates was added to the rhodamine solution (50 mM sodium phosphate buffer, 90 mM sodium chloride, 5 mM diethylenetriaminepentaacetic acid, and 5 mM DHR 123). Changes in fluorescence intensity were measured every 5 min for 30 min on a fluorescence plate reader, GENios (Tecan Instruments), with excitation and emission wavelengths set at 485 and 530 nm, respectively.
Intracellular RS generation
For measurement of intracellular RS generation, cells seeded at a density of 3 × 104 cells/well in a 96-well plate were allowed to adhere overnight. Cells were then incubated in serum-free DMEM with 10 nM of Ang II and 10 μM of DCF-DA at 37°C. Changes in fluorescence intensity were measured every 5 min for 30 min on a fluorescence plate reader, GENios (Tecan Instruments), with excitation and emission wavelengths set at 485 and 530 nm, respectively.
Intracellular RS scavenging activity
Cells seeded at a density of 3 × 104 cells/well in a 96-well plate were allowed to adhere overnight. Cells were then incubated in serum-free DMEM with Ang II and/or an angiotensin receptor blocker such as losartan and telmisartan with 10 μM of 2′,7′-DCF-DA at 37°C. Trolox, a vitamin E analog, was used as a positive control. Changes in fluorescence intensity were measured every 5 min for 30 min on a fluorescence plate reader, GENios (Tecan Instruments), with excitation and emission wavelengths set at 485 and 530 nm, respectively.
Serum angiotensin II measurement assay
Ang II levels were measured using a competitive enzyme immunoassay. The immunoplate in this kit is pre-coated with Ang II antibody and the nonspecific binding sites are blocked. Ang II peptide competes with peptide in standard solution or samples (Phoenix Pharmaceuticals). The absorbance was detected at a wavelength of 450 nm, respectively.
Protein tyrosine kinase activity
Protein tyrosine kinase (PTK) activity in the tissue homogenate and cell lysate was assayed with Antibody BeaconTM tyrosine kinase assay kits (Molecular Probes). To detect the tyrosine kinase activity, samples were prepared in 1× kinase buffer (100 mM Tris–HCl, pH 7.5, 20 mM MgCl2, 2 mM EGTA, 2 mM DTT 0.02%) and mixed with the Antibody Beacon detection complex plus substrate in the 96-well microplate. ATP reagent was added to the plate and continuously incubated at the reaction temperature. Fluorescence was measured at multiple time points on the GENios (Tecan Instruments) with excitation and emission wavelengths set at 485 and 535 nm, respectively.
Western blotting
Western blotting was carried out as described previously (Kim et al. 2010a, b). Homogenized samples were boiled for 5 min with a gel-loading buffer (0.125 M Tris–HCl, pH 6.8, 4% SDS, 10% 2-mercaptoethanol, and 0.2% bromophenol blue) at a 1:1 ratio. Total protein equivalents for each sample were separated by sodium dodecyl sulfate–polyacrylamide gel electrophoresis using 10% acrylamide gels as described by Laemmli (Laemmli 1970) and transferred to PVDF membranes at 15 V for 1 h in a semi-dry transfer system. The membrane was immediately placed into blocking buffer (1% nonfat milk) in 10 mM Tris, pH 7.5, 100 mM NaCl, and 0.1% Tween 20. The blot was allowed to block at room temperature for 1 h. The membrane was incubated with specific primary antibody at 25°C for 3 h, followed by a horseradish peroxidase-conjugated anti-mouse antibody (Santa Cruz, 1:10,000), an anti-rabbit antibody (Santa Cruz, 1:10,000), or an anti-goat antibody (Santa Cruz, 1:10,000) at 25°C for 1 h. Antibody labeling was detected using West-zol Plus and chemiluminescence FluorchemTMSP (Alpha Innotech Corporation, San Leandro, CA, USA). Pre-stained protein markers were used for molecular weight determinations.
Immunoprecipitation
The cell lysates were subjected to immunoprecipitation in a buffer containing 40 mM Tris, pH 7.6, 120 mM NaCl, 5 mM EDTA, 0.1% NP-40, 0.25% deoxycholic acid, protease inhibitors, and phosphatase inhibitors. Three hundred micrograms of sample was incubated with 50% slurry of protein A at 4°C for 2 h for pre-clearing. After incubation, the samples were centrifuged at 12,000×g at 4°C for 10 min. Samples were incubated overnight with the respective antibody at 4°C, followed by incubation with a 50% slurry of protein A agarose at 4°C for 3 h. After washing of the immunoprecipitates with IP buffer, immunoprecipitated proteins were analyzed by Western blotting as described previously.
Immunocytochemistry
Cells were seeded on a 60-mm cultured dish and allowed to attach for 24 h. The medium was replaced with serum-free medium to observe p-p65 (Ser 276) and p-p65 (Ser 536) translocation to the nucleus without intervention by serum. Cells were incubated with or without Ang II for 30 min and then fixed in 4% paraformaldehyde in PBS, pH 7.4, and washed with PBS. Cells were blocked in ABS/0.1% Triton X-100/3% goat serum (ABS-TS) at room temperature for 30 min and incubated with primary p-p65 (Ser 276) and p-p65 (Ser 536) antibodies (rabbit polyclonal; Santa Cruz Biotechnology; 1:500) in ABS-TS at 4°C overnight. Cells were rinsed three times in ABS-TS for 10 min per time. Cells were then washed in ABS and incubated for 3 h in the presence of anti-rabbit IgG labeled with Alexa Fluor-488. Cells were washed in ABS and 1 mg/ml of Hoechst 33342 was added to label the nucleus. Images were acquired using a Motic® AE30/31 Inverted microscope (Motic Incorporation, Seoul, Korea).
Statistical analysis
For Western blotting, one representative blot is shown from independent experiments done in triplicate. The significance between group differences was determined by one-factor analysis of variance (ANOVA) followed by the Fischer’s protected least significant difference post hoc test. Values of *p < 0.05 were considered statistically significant.
Results
Changes in serum Ang II and renal AT1 expression level during aging
To investigate age-related changes in serum Ang II levels, an enzyme-linked immunosorbent assay was used for measurement in aged rat serum. As shown in Fig. 1a, serum Ang II levels were significantly increased in aged rats compared with young rats. Next, AT1 expression levels were determined by Western blotting using anti-AT1-specific polyclonal antibody. AT1 is an important marker of the Ang II signaling-induced pro-inflammatory response. Age-related changes in AT1 expression levels in kidney were assessed (Fig. 1b) and were shown to be significantly increased with aging. Thus, the results indicate that serum Ang II levels and AT1 expressions were increased during aging.
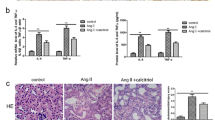
Changes in Ang II-induced redox imbalances with aging. Ang II-induced redox imbalances were measured in 6-, 12-, 18-, and 24-month-old rats. Ang II levels were measured in aged rats (a). Western blot analysis was performed to detect AT1 protein levels in aged rats. Anti-β-actin antibody was used to evaluate equal protein loading. One representative blot of each protein is shown from three experiments that yielded similar results, respectively (b). The DCF-DA method was used to determine the effect of age on RS generation in kidney homogenates (c). The DHR-123 method was used to determine the effect of age on ONOO− generation in kidney homogenates (d). Values are expressed as mean ± SE (n = 6). Results of one-factor ANOVA: *p < 0.05, **p < 0.01, ***p < 0.001 vs. 6-month-old rats. Ang II angiotensin II, AT1 angiotensin type 1 receptor, RS reactive species, DCF-DA 2′,7′-dichlorodihydrofluorescein diacetate, DHR-123 dihydrorhodamine 123, ONOO − peroxynitrite
Changes in Ang II-induced redox imbalance in aging
Ang II generates RS and oxidative stress during the inflammatory response via multiple signaling pathways. To assess overall Ang II-related oxidative stress with aging, total RS levels were measured with a DCF-DA assay. DCF-DA is oxidized to fluorescent DCF by RS including superoxide radicals and hydrogen peroxide. The data showed a gradual increase in RS with age, especially in old rats, which showed a significant increase in fluorescence intensity compared with young rats (Fig. 1c). Additionally, we determined whether increased Ang II increases ONOO− levels using a DHR-123 assay. ONOO−, a product of the reaction of nitric oxide with superoxide, is a potent and versatile oxidant that can attack a wide range of biological molecules. Ang II activates nitric oxide synthase (eNOS) to release NO, and these two radicals rapidly react with each other by forming the very reactive ONOO−. The ONOO− anion can react with DNA, proteins, and lipids under physiological conditions that lead to cellular oxidative stress. As shown in Fig 1d, ONOO− levels were increased with aging. These results indicate an age-related upregulation of Ang II effects on redox imbalances.
Changes in NF-κB activation through IκBα phosphorylation in aging
NF-κB is a redox-sensitive transcription factor that is activated by oxidative stress. NF-κB is a well-known pro-inflammatory mediator in aging process. First, we investigated the phosphorylation levels of IκBα detected by Western blotting using an anti p-IκBα-specific monoclonal antibody. As shown in Fig 2a, the phosphorylation levels of IκBα protein in cytoplasmic extracts were increased with aging. We then determined that age-related increased IκBα phosphorylation enhances the nuclear translocation of p65 and p50. Nuclear p65 and p50 translocation levels were detected by Western blotting using anti-p65- and p50-specific polyclonal antibodies. The results clearly show that nuclear translocation of p65 and p50 was increased with aging. These results support the idea that age-related changes in Ang II increase NF-κB activation through oxidative stress.
Changes in NF-κB activation with aging. Ang II-induced NF-κB activation was measured in 6-, 12-, 18-, and 24-month-old rats. Ang II-related NF-κB activation through IκBα phosphorylation was measured by Western blot analysis using p-IKKαβ-, p-IκBα-, p50-, and p65-specific antibodies (a). Ang II-related NF-κB activation through Ser 536 phosphorylation was measured by Western blot analysis using p-IKKαβ and p-p65 (Ser 536)-specific antibodies (b). Ang II-related NF-κB activation through Ser 276 phosphorylation was measured by Western blot analysis using p-ERK-, p-MSK-1-, and p65 (Ser 276)-specific antibodies (c). Ang II-related NF-κB-dependent pro-inflammatory gene expression was measured by Western blot analysis using 5-LOX- and COX-2-specific antibodies (d). Anti-β-actin and anti-TFIIB antibodies were used to evaluate equal protein loading. One representative blot for each protein is shown from three experiments that yielded similar results. Results of one-factor ANOVA. *p < 0.05, **p < 0.01, ***p < 0.001 vs. 6-month-old rats. Ang II angiotensin II, COX-2 cyclooxygenase-2, ERK extracellular signal-regulated kinase, IκBα inhibitory κBα, IKKαβ IκB kinase αβ, 5-LOX 5-lipoxygenase, MSK-1 mitogen- and stress-activated protein kinase-1, TFIIB transcription factor II B
Change in NF-κB activation through the phosphorylation of p65 with aging
The transcriptional activity of NF-κB is stimulated upon serine residue phosphorylation of p65 by various kinases. To examine the possibility that there was increased phosphorylation of p65, we investigated typical residue sites at Ser 536 and 276. It is known that Ser 536 residue phosphorylation of p65 is triggered by IKKαβ phosphorylation. Ser 536 phosphorylation levels of p65 and phosphorylation of p65-related cellular signaling were examined by Western blotting using anti-p-p65- (Ser 536) and anti-p-IKKαβ-specific polyclonal antibodies. As shown in Fig. 2b, Ser 536 phosphorylation levels of p65 were increased with aging. We also confirmed that IKKαβ phosphorylation levels were increased with aging, which correlated with Ser 536 phosphorylation of p65. Furthermore, we elucidated the Ser 276 residue phosphorylation levels of p65 with aging. A previous study reported that Ser 276 phosphorylation of p65 is associated with ERK/MSK-1 signaling. To determine this, Ser 276 phosphorylation of p65 and its related proteins, ERK/MSK-1, were examined by Western blots using nuclear anti-p-p65 (Ser 276), anti-p-MSK-1, and cytoplasmic anti-p-ERK-specific polyclonal antibodies. The results show that Ser 276 phosphorylation levels of p65 were significantly increased with aging and that its related phosphorylation of MSK-1 and ERK was also enhanced (Fig. 2c). These results clearly indicate that aging upregulates Ang II-related NF-κB activation through the phosphorylation of p65.
Changes in NF-κB-dependent pro-inflammatory gene expression in aging
To confirm age-related changes in the NF-κB-induced inflammatory response, κB-dependent pro-inflammatory gene expression levels were investigated. To determine NF-κB-related pro-inflammatory gene expression during aging, renal COX-2 and 5-LOX protein levels were measured by Western blotting using anti-COX-2- and anti-5-LOX-specific polyclonal antibodies. These genes are known to have an NF-κB binding site in their promoter regions and controlled by NF-κB regulation. The results show that the protein expression levels of these genes were correlated with NF-κB activity (Fig. 2d). To confirm the molecular mechanisms of Ang II-induced NF-κB activation, we further investigated these findings using YPEN-1 endothelial cells.
Intracellular RS generation and PTK activity by Ang II in endothelial cells
To investigate whether Ang II induces oxidative stress, intracellular RS generation levels were measured by the DCF-DA assay in YPEN-1 cells. Cells were treated with Ang II at various concentrations. As shown in Fig. 3a, b, Ang II induced RS generation in a dose-dependent manner. It was found that under these experimental conditions, no cytokines were generated. In addition, to confirm whether Ang II induces oxidative stress, we determined intracellular RS scavenging activity using ARBs such as losartan and telmisartan. The results showed that Ang II-induced intracellular RS generation was inhibited by losartan and telmisartan compared with a positive control, trolox (Fig. 3c). These results also correlated with RS generation, suggesting an age-related increase in Ang II-generated intracellular RS. Based on the aforementioned data, to investigate Ang II-induced RS generation, we determined whether Ang II-induced ROS generation was affected by protein kinase activity.
Effect of Ang II on redox imbalances in YPEN-1 cells. Cells were treated with various doses of Ang II for 30 min. Intracellular RS levels were measured by DCF-DA using a fluorescent probe (Genious) (a). Intracellular RS levels were measured by DCF-DA using a fluorescent probe (Motic) control (a), 1 μM (b), 5 μM (c), 10 μM (d) of Ang II (b). Intracellular RS scavenging activity was measured by DCF-DA using ARBs (c). PTK activity was measured by Antibody BeaconTM tyrosine kinase assay kits (d). cSRC activation was measured using Western blot analysis to detect cSRC protein levels in aged rats. Anti-β-actin antibody was used to evaluate equal protein loading. One representative result is shown from three experiments that yielded similar results (e). Results of one-factor ANOVA: *p < 0.05, **p < 0.01, ***p < 0.001 vs. control group. # p < 0.05, ## p < 0.01, ### p < 0.001 vs. Ang II-treated group. Ang II angiotensin II, ARBs angiotensin II receptor blockers, cSrc v-src sarcoma, DCF-DA dichlorodihydrofluorescein diacetate, PTK protein tyrosine kinase, RS reactive species
PTKs are known to be activated by RS-mediated redox regulation and enhance MAPK phosphorylation. To assess whether an increase in Ang II-related RS causes PTK activation, total PTK was measured using assay kits. The results show a gradual increase in PTK activity with Ang II, especially 15 min after Ang II treatment (Fig. 3d). It is known that PTK activation directly phosphorylates tyrosine kinases such as the Src PTK family. Based on Fig. 3d results, upregulation of cSRC through its phosphorylation was determined by Western blotting using anti-p-cSRC-specific polyclonal antibody. As shown in Fig. 3e, cSRC phosphorylation levels were increased with Ang II at 15 min after treatment. This result was in accord with results shown in Fig. 3d. The results indicate that Ang II activated PTK activity and phosphorylation of cSRC by inducing RS generation. Our data support Ang II-induced ROS enhance ERK phosphorylation via cSRC phosphorylation.
NF-κB activation by Ang II through IκB phosphorylation in endothelial cell
A previous study reported that Ang II activation of NF-κB is through the phosphorylation of IκBα, which leads to ubiquitination/proteosomal degradation of IκBα. To investigate whether Ang II activates NF-κB, phosphorylation levels of IκBα were detected by Western blotting using anti-p-IκBα antibody. Cells were stimulated with 10 μM of Ang II and cytosol and nucleus fractions were separated. The reasons for the use of a pharmacological dose were based on our preliminary experiments (data not shown) that showed Ang II-induced acute RS generation and NF-κB activation response within 30 min that required a concentration of at least 10 μM of Ang II in YPEN-1 cells. As shown in Fig. 4a, IκBα was phosphorylated at 15 min after Ang II treatment, and degradation of IκBα was detected at the same time in the cytosol fraction. Phosphorylation of IκBα induced the nuclear localization of the NF-κB complex comprising the p65 and p50 subunits. Translocation levels of p65 and p50 were assessed by Western blotting using anti-p65- and anti-p50-specific polyclonal antibodies in the nuclear fraction. The results show that Ang II increased the nuclear localization of p65 and p50 at 20 min following Ang II treatment.
Effect of Ang II on NF-κB activation in YPEN-1 cells. Cells were stimulated by Ang II and incubated from 5 to 30 min. Cells lysate were analyzed by Western blot analysis using IκBα-, anti-p-IκBα-, anti-p65-, and anti-p50-specific antibodies (a). Cells lysate were analyzed by Western blot analysis using p-IKKαβ- and p-p65 (Ser 536)-specific antibodies (b). The protein–protein interaction between IKKα and phosphorylated p65 was examined by immunoprecipitation. One representative blot is shown from three experiments that yielded similar results (c). Cells lysate were analyzed by Western blot analysis using p-ERK-, p-MSK-1-, and p-p65 (Ser 276)-specific antibodies (d). Immunocytochemistry was performed using p-p65 (Ser 276)-specific polyclonal antibody. Ser 276 phosphorylation of the p65 protein was labeled with Alexa 488 fluorescence (green). Ser 276 phosphorylation of translocated p65 could be identified by nuclear staining with 1 mg/mL of Hochest 33342 (blue) for 5 min (e). Cells were stimulated by Ang II and incubated from 30 min to 24 h. Cells lysate were analyzed by Western blot analysis using COX-2- and AT1-specific antibodies (f). Anti-β-actin and anti-TFIIB antibodies were used to evaluate equal protein loading. One representative blot is shown from three experiments that yielded similar results. Results of one-factor ANOVA: *p < 0.05, **p < 0.01, ***p < 0.001 vs. control group. AT1 angiotensin II type 1 receptor, ERK extracellular signal-regulated kinase, COX-2 cyclooxygenase-2, IKKαβ IκB kinase αβ, MSK mitogen- and stress-activated protein kinase 1, TFIIB transcription factor II B
NF-κB activation by Ang II through the phosphorylation of p65 in endothelial cells
Ser 536 phosphorylation of p65 by Ang II in endothelial cells
Based on previous data (Fig. 2b), we found an age-related increase in the ability of Ang II to induce Ser 536 phosphorylation of p65. Next, we determined whether Ang II induces NF-κB activation through Ser 536 phosphorylation of p65 in YPEN-1 cells. To determine whether Ang II induced Ser 536 phosphorylation of p65, cells were treated with 10 μM Ang II and the cytosol and nuclear fractions were separated. The Ser 536 phosphorylation of p65 increased between 10 and 15 min after treatment and declined 20 min after Ang II treatment in the cytosol fraction. In addition, Ser 536 phosphorylation of p65 increased 20 min after Ang II treatment in the nuclear fraction. It was suggested that phosphorylated p65 translocates to the nucleus. In previous studies, the phosphorylation of the Ser 536 residue in p65 was triggered by IKKαβ. Ang II-induced IKKαβ phosphorylation was measured by Western blotting using an antibody against phospho-IKKαβ. Phosphorylation of IKKαβ increased with Ang II treatment in a time-dependent manner (Fig. 4b). These results indicate that Ang II induces NF-κB activation through Ser 536 phosphorylation of p65, which is mediated by IKKαβ in the cytoplasm. Moreover, it is known that IKKα approaches p65 and directly phosphorylates Ser 536 of p65 in the nucleus. Thus, to verify whether Ang II increases Ser 536 phosphorylation of p65 via IKKα in the nucleus, we examined Ang II-induced Ser 536 phosphorylation of p65 by IKKα by Western blotting using anti-IKKα and anti-p-p65 (Ser 536) antibodies. The data show that Ser 536 phosphorylation of p65 was increased by Ang II. However, the IKKα level in the nuclear fraction did not change. Immunoprecipitation experiments were undertaken to further verify whether Ang II increases protein–protein interactions between IKKα and phosphorylated p65. The use of immunoprecipitation of p65 and Western blotting of IKKα showed that Ang II induced significant increases in IKKα in nuclear extracts (Fig. 4c). Our data indicate that IKKα directly interacted with the p65 subunit of NF-κB in the nucleus, leading to the Ser 536 phosphorylation of p65.
Ser 276 phosphorylation of p65 by Ang II in endothelial cells
Based on the aforementioned data, we investigated whether Ang II induces NF-κB activation through another p65 phosphorylation residue. Cells were exposed to Ang II, and Ser 276 phosphorylation of p65 was determined by Western blotting using the Ser 276 phospho-p65 antibody. The results show that Ser 276 phosphorylation of p65 in the nuclear fraction significantly increased 20 min after Ang II treatment. It is known that Ser 276 phosphorylation of p65 is associated with ERK/MSK-1 signaling. We assessed upstream signaling for Ser 276 phosphorylation of p65. As shown in Fig. 4d, Ang II phosphorylated ERK in the cytosol fraction. ERK-dependent MSK-1, which is a downstream target of ERK, also increased with Ang II treatment in the nuclear fraction. These results suggest that Ang II is associated with Ser 276 phosphorylation of p65 by enhancing ERK and MSK-1 phosphorylation. Ang II-associated Ser 276 phosphorylation of p65 was also confirmed by immunocytochemistry using the Ser 276 phospho-p65 antibody. Cells were stimulated by Ang II from 5 to 30 min. As shown in Fig. 4e, Ser 276 phosphorylation of p65 expression increased 20 min after Ang II treatment. This result strongly supports previous results. These results therefore suggest a close association between Ang II-induced NF-κB activation and Ser 276 phosphorylation of p65.
Changes in NF-κB-dependent gene expression due to Ang II in endothelial cells
To elucidate whether Ang II induces the expression of pro-inflammatory genes that have an NF-κB binding site in their promoter regions, Western blotting was done on Ang II-treated YPEN-1 cells. Ang II upregulates the expression of cyclooxygenase-2 (COX-2) which is known to have an NF-κB binding site in their promoter regions and to be controlled by NF-κB regulation (Umezawa et al. 2000; Jaimes et al. 2005). Ang II-induced COX-2 gene expression regenerated RS and elevated glomerular endothelium damage (Jaimes et al. 2010). The results show that COX-2 and 5-lipoxygenase were increased 6 h after Ang II treatment. As shown in Fig. 4f, NF-κB-dependent AT1 expression also increased 6 h following Ang II treatment. These results indicate that Ang II induces NF-κB activation and NF-κB-dependent expression of pro-inflammatory genes.
Discussion
Aging is characterized by the deleterious effects from many physiological mediators that deviate from their normal functions during aging. Aging affects the function and structure of arteries, the risk of cardiovascular diseases, and contributes to increased hypertension (Seals et al. 2008). In addition, altered renal expression of AT1 precedes the development of renal fibrosis in aging rats (Schulman et al. 2010). Ang II, an important vascular constrictor, is recognized as a potent pro-inflammatory mediator that participates in vascular inflammatory responses (Ferrario and Strawn 2006; Muller et al. 2000; Ruiz-Ortega et al. 2000). It seems clear that the production of RS and the activation of transcription factor NF-κB play major roles in the intracellular signaling pathways involved in RAS and Ang II-induced inflammation (Ungvari et al. 2006). Recent studies have suggested their potential role in the activation of inflammatory mechanisms associated with age-related vascular and renal damage. For one thing, Ang II signaling increases with aging (Basso et al. 2005; Diz and Lewis 2008). For another, suppression of Ang II signaling attenuates the development of age-related vascular diseases. Based on this rationale, the current study proposed that Ang II plays a role in age-related pro-inflammatory responses through its enhancing effect of oxidative stress, which triggers NF-κB-activated inflammatory pathways during aging.
First, we examined age-related Ang II-induced oxidative stress using rat kidney and YPEN-1 cells. Several studies have demonstrated that the pro-inflammatory actions of Ang II are promoted through AT1, which enhances inflammatory gene expression. Ang II-modulated NADPH oxidase-dependent ROS production leads to oxidative stress by several intracellular pathways (Touyz et al. 2003; Garrido and Griendling 2009; Hitomi et al. 2007). For aging, increased ROS have been proposed as the exacerbating agents underlying aging and age-related inflammation due to oxidative stress (Chung et al. 2006). Modrick et al. (2009) showed that in the absence of AT1, endothelial dysfunction did not occur in old mice, suggesting a novel and fundamental role for Ang II in age-related vascular dysfunction. While it is well established that Ang II produces oxidative stress in various tissues (Higashi et al. 2005; Lassegue et al. 2001; Seshiah et al. 2002), the relative importance of Ang II and its ability to induce signaling that leads to vascular dysfunction with aging has been less well explored.
According to a previous study of Khan et al. (2008), Ang II and AT1 interactions influenced NF-κB activation via ROS production, stimulating the nuclear translocation of the p65 subunit, DNA binding, the transcription of a NF-κB reporter gene, and IκB degradation. Our data suggest that increases in a redox-sensitive transcription factor, NF-κB and NF-κB activation in aged rat kidney, were likely due to Ang II-induced redox disturbances during aging. Studies in cultured cells (Mehta and Griendling 2007; Chai and Danser 2005) or in animal models (Atkinson et al. 1980; Zhuo et al. 1993) of Ang II-induced tissue injury further support an important role for NF-κB in mediating the detrimental effects of Ang II. Ang II is known to induce target organ damage in cardiovascular, hypertensive, and renal diseases by activating a number of pro-inflammatory cytokines, chemokines, and growth factors (Wolf et al. 2000; Endemann and Schiffrin 2004). Furthermore, the Ang II-induced pro-inflammatory response has been shown clinically and experimentally to affect the onset, progression, and outcome of age-related vascular diseases such as atherosclerosis (Wolf et al. 2002; Manjunath et al. 2003).
One interesting finding generated from the current study is that age-related upregulation ability of Ang II to activate NF-κB occurs by a different pathway in the kidney by causing enhanced Ser 536 and Ser 276 phosphorylation of p65. Although previous reports from our laboratory show that NF-κB activation through Ser 536 phosphorylation of p65 occurs during aging, the age-related molecular mechanism of Ser 536 phosphorylation of p65 has not been reported (Kim et al. 2010a, b; Lee et al. 2009). Our investigation into Ang II-induced cytoplasmic Ser 536 phosphorylation of p65 by IKKαβ phosphorylation during aging indicates that phosphorylation of Ser 536 on p65 occurred by p65 directly interacting with IKKα in the nucleus. Our evidence for Ser 276 phosphorylation of p65 increasing with age is of importance because of the lack of data that Ser 276 phosphorylation of p65 is involved in aging-induced changes in Ang II signaling. Our expectation that ERK/MSK-1 signaling is involved was confirmed by data in Fig 4 on age-related increases in ERK/MSK-1 signaling. Our data seem to indicate that Ang II modulated p65 signaling by phosphorylation at the Ser 276 site, which was not known before. However, whether the ERK/MSK-1 pathway in fact mediates Ang II-induced Ser 276 phosphorylation of p65 requires further clarification using specific inhibitors of ERK activation.
Thus, we now propose a new pathway by which Ang II leads to increases in pro-inflammatory signaling with aging: it occurs through the phosphorylation of p65. In the current study, we presented data showing that Ang II plays a role in aging through its enhancement of oxidative stress and expression of inflammatory pathways through NF-κB activation. Our data show that Ang II-induced NF-κB activation is related to the phosphorylation of p65 at serine 536 and 276 residues in the senescent kidney and in endothelial YPEN-1 cells. The significance of our study is that it documents the deleterious role of renal Ang II and AT1 during aging, a role that includes upregulating their activities and eliciting pro-inflammatory changes via NF-κB activation. Our study presents strong experimental evidence that the increased NF-κB activation observed in aged rat kidney is due to increases in Ang II and AT1 levels and that these increases may play a key role in the development of age-related inflammatory renal diseases such as glomerulonephritis.
References
Alvarez A, Cerda-Nicolas M, Naim Abu Nabah Y, Mata M, Issekutz A, Panes J, Lobb R, Sanz M (2004) Direct evidence of leukocyte adhesion in arterioles by angiotensin II. Blood 104:402–408
Atkinson A, Brown J, Fraser R, Lever A, Morton J, Riegger A, Robertson J (1980) Angiotensin II and renal hypertension in dog, rat and man: effect of converting enzyme inhibition. Clin Exp Hypertens 2:499–524
Basseres D, Baldwin A (2006) Nuclear factor-kappaB and inhibitor of kappaB kinase pathways in oncogenic initiation and progression. Oncogene 25:6817–6830
Basso N, Paglia N, Stella I, de Cavanagh E, Ferder L, del Rosario Lores Arnaiz M, Inserra F (2005) Protective effect of the inhibition of the renin–angiotensin system on aging. Regul Pept 128:247–252
Bertrand V, Guessous F, Le Roy AL, Viossat B, Fessi H, El Abbouyi A, Giroud JP, Roch-Arveiller M (1999) Copper-indomethacinate associated with zwitterionic phospholipids prevents enteropathy in rats: effect on inducible NO synthase. Dig Dis Sci 44(5):991–999
Carey R, Siragy H (2003) Newly recognized components of the renin-angiotensin system: potential roles in cardiovascular and renal regulation. Endocr Rev 24:261–271
Cassis P, Conti S, Remuzzi G, Benigni A (2010) Angiotensin receptors as determinants of life span. Pflugers Arch 459:325–332
Chai W, Danser A (2005) Is angiotensin II made inside or outside of the cell? Curr Hypertens Rep 2:124–127
Chen L, Greene W (2004) Shaping the nuclear action of NF-κB. Nat Rev Mol Cell Biol 5:392–401
Chung H, Kim H, Kim J, Yu B (2006) The inflammation hypothesis of aging. Ann NY Acad Sci 928:327–335
Chung HY, Cesari M, Anton S, Marzetti E, Giovannini S, Seo AY, Carter C, Yu BP, Leeuwenburgh C (2009) Molecular inflammation: underpinnings of aging and age-related diseases. Ageing Res Rev 1:18–30
Cui R, Tieu B, Recinos A, Tilton R, Brasier A (2006) RhoA mediates angiotensin II-induced phospho-Ser536 nuclear factor kappa B/RelA subunit exchange on the interleukin-6 promoter in VSMCs. Circ Res 99:723
de Cavanagh E, Piotrkowski B, Basso N, Stella I, Inserra F, Ferder L, Fraga C (2003) Enalapril and losartan attenuate mitochondrial dysfunction in aged rats. FASEB J 9:1096–1098
de Cavanagh E, Piotrkowski B, Fraga C (2004) Concerted action of the renin–angiotensin system, mitochondria, and antioxidant defenses in aging. Mol Aspects Med 25:27–36
Diz D, Lewis K (2008) Dahl memorial lecture: the renin–angiotensin system and aging. Hypertension 52:37–43
Douillette A, Bibeau-Poirier A, Gravel S, Clement J, Chenard V, Moreau P, Servant M (2006) The proinflammatory actions of angiotensin II are dependent on p65 phosphorylation by the IκB kinase complex. J Biol Chem 19:13275–13284
Endemann D, Schiffrin E (2004) Endothelial dysfunction. J Am Soc Nephrol 15(8):1983–1992
Ferder L, Inserra F, Martinez-Maldonado M (2006) Inflammation and the metabolic syndrome: role of angiotensin II and oxidative stress. Curr Hypertens Rep 8:191–198
Ferrario C, Strawn W (2006) Role of the renin–angiotensin–aldosterone system and proinflammatory mediators in cardiovascular disease. Am J Cardiol 98:121–128
Garrido A, Griendling K (2009) NADPH oxidases and angiotensin II receptor signaling. Mol Cell Endocrinol 302:148–158
Gilmore T (2006) Introduction to NF-κB: players, pathways, perspectives. Oncogene 25:6680–6684
Higashi Y, Chayama K, Yoshizumi M (2005) Angiotensin II type I receptor blocker and endothelial function in humans: role of nitric oxide and oxidative stress. Curr Med Chem Cardiovasc Hematol Agents 3:133–148
Hitomi H, Kiyomoto H, Nishiyama A (2007) Angiotensin II and oxidative stress. Curr Opin Cardiol 4:311–315
Hoffmann A, Levchenko A, Scott M, Baltimore D (2002) The IκB-NF-κB signaling module: temporal control and selective gene activation. Science 298:1241–1245
Jaimes E, Tian R, Pearse D, Raij L (2005) Up-regulation of glomerular COX-2 by angiotensin II: role of reactive oxygen species. Kidney Int 5:2143–2153
Jaimes E, Hua P, Tian R, Raij L (2010) Human glomerular endothelium: interplay among glucose, free fatty acids, angiotensin II, and oxidative stress. Am J Physiol Renal Physiol 298:F125–F132
Khan N, Hemmelgarn B, Herman R, Rabkin S, McAlister F, Bell C, Touyz R, Padwal R, Leiter L, Mahon J, Hill M, Larochelle P, Feldman R, Schiffrin E, Campbell N, Arnold M, Moe G, Campbell T, Milot A, Stone J, Jones C, Ogilvie R, Hamet P, Fodor G, Carruthers G, Burns K, Ruzicka M, dechamplain J, Pylypchuk G, Petrella R, Boulanger J, Trudeau L, Hegele R, Woo V, McFarlane P, Vallée M, Howlett J, Katzmarzyk P, Tobe S, Lewanczuk R (2008) The 2008 Canadian Hypertension Education Program recommendations for the management of hypertension: part 2—therapy. Can J Cardiol 6:465–475
Kim J, Jung J, Yu P, Cho G, Choi S, Chung Y (2002a) Modulation of redox-sensitive transcription factors by calorie restriction during aging. Mech Ageing Dev 12:1589–1595
Kim J, Lee E, Park G, Kim M, Yokozawa T, Yu B, Chung H (2002b) Morin modulates the oxidative stress-induced NF-kappaB pathway through its anti-oxidant activity. Free Radic Res 4:454–461
Kim M, Lee K, Kim H, Yu P, Chung H (2010a) Kaempferol modulates pro-inflammatory NF-kappaB activation by suppressing advanced glycation endproducts-induced NADPH oxidase. Age 2:197–208
Kim M, Chung S, Kim D, Kim J, Lee E, Kim J, Ha Y, Kim Y, No J, Chung H, Park K, Rhee S, Choi J, Yu B, Yokozawa T, Kim Y, Chung H (2010b) Modulation of age-related NF-kappaB activation by dietary zingerone via MAPK pathway. Exp Gerontol 6:419–426
Kobori H, Nangaku M, Navar LG, Nishiyama A (2007) The intrarenal renin–angiotensin system: from physiology to the pathobiology of hypertension and kidney disease. Pharmacol Rev 3:251–287
Laemmli U (1970) Cleavage of structural proteins during the assembly of the head of bacteriophage T4. Nature 227:680–685
Lassegue B, Sorescu D, Szocs K, Yin Q, Akers M, Zhang Y, Grant S, Lambeth J, Griendling K (2001) Novel gp91phox homologues in vascular smooth muscle cells: nox1 mediates angiotensin II-induced superoxide formation and redox-sensitive signaling pathways. Circ Res 9:888–894
Lee E, Chung S, Kim J, Kim J, Heo H, Lim H, Kim M, Anton S, Yokozawa T, Chung H (2009) Allylmethylsulfide down-regulates X-ray irradiation-induced nuclear factor-kappaB signaling in C57/BL6 mouse kidney. J Med Food 3:542–551
Luo J, Kamata H, Karin M (2005) IKK/NF-κB signaling: balancing life and death—a new approach to cancer therapy. J Clin Invest 10:2625–2632
Manjunath G, Tighiouart H, Coresh J, Macleod B, Salem D, Griffith J, Levey A, Sarnak M (2003) Level of kidney function as a risk factor for cardiovascular outcomes in the elderly. Kidney Int 63:1121–1129
Mehta P, Griendling K (2007) Angiotensin II cell signaling: physiological and pathological effects in the cardiovascular system. Am J Physiol Cell Physiol 1:C82–C97
Modrick M, Didion SP, Sigmund C, Faraci F (2009) Role of hydrogen peroxide and the impact of glutathione peroxidase-1 in regulation of cerebral vascular tone. Am J Physiol Heart Circ Physiol 6:H1914–H1919
Muller D, Dechend R, Mervaala E, Park J, Schmidt F, Fiebeler A, Theuer J, Breu V, Ganten D, Haller H (2000) NF-{kappa} B inhibition ameliorates angiotensin II-induced inflammatory damage in rats. Hypertension 35:193–201
Ruiz-Ortega M, Lorenzo O, Ruperez M, Konig S, Wittig B, Egido J (2000) Angiotensin II activates nuclear transcription factor kappaB through AT (1) and AT (2) in vascular smooth muscle cells: molecular mechanisms. Circ Res 12:1266–1272
Ruiz-Ortega M, Ruperez M, Esteban V, Rodriguez-Vita J, Sanchez-Lopez E, Carvajal G, Egido J (2006) Angiotensin II: a key factor in the inflammatory and fibrotic response in kidney diseases. Nephrol Dial Transplant 1:16–20
Schulman I, Zhou M, Treuer A, Chadipiralla K, Hare J, Raij L (2010) Altered renal expression of angiotensin II receptors, renin receptor, and ACE-2 precede the development of renal fibrosis in aging rats. Am J Nephrol 3:249–261
Seals D, DeSouza C, Donato A, Tanaka H (2008) Habitual exercise and arterial aging. J Appl Physiol 4:1323–1332
Seshiah P, Weber D, Rocic P, Valppu L, Taniyama Y, Griendling K (2002) Angiotensin II stimulation of NAD(P)H oxidase activity: upstream mediators. Circ Res 5:406–413
Stumpf C, John S, Jukic J, Yilmaz A, Raaz D, Schmieder R, Daniel W, Garlichs C (2005) Enhanced levels of platelet P-selectin and circulating cytokines in young patients with mild arterial hypertension. J Hypertens 5:995–1000
Swanson G, Hanesworth J, Sardinia M, Coleman J, Wright J, Hall K, Miller-Wing A, Stobb J, Cook V, Harding E (1992) Discovery of a distinct binding site for angiotensin II (3-8), a putative angiotensin IV receptor. Regulatorypeptides 40:409–419
Touyz R, Yao G, Schiffrin E (2003) c-Src induces phosphorylation and translocation of p47phox: role in superoxide generation by angiotensin II in human vascular smooth muscle cells. Arterioscler Thromb Vasc Biol 6:981–987
Umezawa K, Ariga A, Matsumoto N (2000) Naturally occurring and synthetic inhibitors of NF-kappaB functions. Anticancer Drug Des 4:239–244
Ungvari Z, Wolin M, Csiszar A (2006) Mechanosensitive production of reactive oxygen species in endothelial and smooth muscle cells: role in microvascular remodeling? Antioxid Redox Signal 8:1121–1129
Viatour P, Merville M, Bours V, Chariot A (2005) Phosphorylation of NF-[kappa] B and I [kappa] B proteins: implications in cancer and inflammation. Trends Biochem Sci 1:43–52
Wei Y, Sowers J, Clark S, Li W, Ferrario C, Stump C (2008) Angiotensin II-induced skeletal muscle insulin resistance mediated by NF-kappaB activation via NADPH oxidase. Am J Physiol Endocrinol Metab 2:E345–E351
Wolf G, Butzmann U, Wenzel U (2000) The renin–angiotensin system and progression of renal disease: from hemodynamics to cell biology. Nephron Physiol 93:p3–p13
Wolf G, Wenzel U, Burns K, Harris R, Stahl R, Thaiss F (2002) Angiotensin II activates nuclear transcription factor-κB through AT1 and AT2 receptors. Kidney Int 61:1986–1995
Yu BP, Chung HY (2006) Adaptive mechanisms to oxidative stress during aging. Mech Ageing Dev 5:436–443
Zhong H, May M, Jimi E, Ghosh S (2002) The phosphorylation status of nuclear NF-[kappa] B determines its association with CBP/p300 or HDAC-1. Mol Cell 9:625–636
Zhuo J, Alcorn D, Harris PJ (1993) Localization and properties of angiotensin II receptors in rat kidney. Mendelsohn FAKidney Int Suppl 42:S40–S46
Acknowledgments
This work was supported by a National Research Foundation of Korea (NRF) grant funded by the Korean government (MEST, No.2009-0083538).
Author information
Authors and Affiliations
Corresponding author
About this article
Cite this article
Kim, J.M., Heo, HS., Ha, Y.M. et al. Mechanism of Ang II involvement in activation of NF-κB through phosphorylation of p65 during aging. AGE 34, 11–25 (2012). https://doi.org/10.1007/s11357-011-9207-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11357-011-9207-7