Abstract
Angiotensin II (Ang II), the central product of renin-angiotensin system, has a role in the etiology of hypertension and in pathophysiology of cardiac and renal diseases in humans. Other functions of Ang II include effects on immune response, inflammation, cell growth and proliferation, which are largely mediated by Ang II type 1 receptor (AT1). Several experimental studies have demonstrated that Ang II acts through AT1 as a mediator of normal aging processes by increasing oxidant damage to mitochondria and in consequences by affecting mitochondrial function. Recently, our group has demonstrated that the inhibition of Ang II activity by targeted disruption of the Agtr1a gene encoding Ang II type 1A receptor (AT1A) in mice translates into marked prolongation of life span. The absence of AT1A protected multiple organs from oxidative damage and the alleviation of aging-like phenotype was associated with increased number of mitochondria and upregulation of the prosurvival gene sirtuin 3. AT1 receptor antagonists have been proven safe and well-tolerated for chronic use and are used as a key component of the modern therapy for hypertension and cardiac failure, therefore Ang II/AT1 pathway represents a feasible therapeutic strategy to prolong life span in humans.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The mean life span has been increasing steadily over the course of human evolution, and in the last century, the human life expectancy in developed countries has nearly doubled as indicated by an increase from around 50 to 75–80 years [12]. Before 1950, most of the gain in life expectancy was due to marked decrease in death rates at younger ages. In the second half of the 20th century, the observed reduction in mortality at ages above 65 years could be ascribed to the delay in the onset of several age-related disorders and to the increased capacity to prevent organ damage, as a consequence of improved biomedical and nutritional conditions [47]. Therefore, ensuring disease-free survival and not merely survival per se represents an attractive and desirable goal for society as a whole. Healthy aging and longevity depend on the dynamic interaction between biological and environmental factors, including medical care, healthy diet, and lifestyle. However, emerging evidence from model organisms has indicated that several genetic factors might play a role in longevity, putting the attention on several molecular candidates involved in pathways contributing to protect organs from degeneration and diseases.
In the last 20 years, one of the main goals of our research was to find out therapeutic strategies to protect the kidney from progressive renal injury with the final aim to reduce the need of dialysis in patients. To this aim, our efforts have been devoted to identify factors implicated in the progression of chronic kidney disease, whose incidence is increasing worldwide at an alarming rate. Experimental and clinical evidence is available that blockade of the renin angiotensin system (RAS) by angiotensin converting enzyme inhibitors (ACEi) and angiotensin II receptor blockers (ARB) is effective in slowing the progression of kidney disease due to the drugs’ ability to reduce proteinuria [53]. When ACEi and ARB were given in combination to rats genetically predisposed to progressive nephropathy, reduction of glomerular sclerosis was even more evident, particularly in those glomeruli that had less severe lesion to begin with. This shows that remodeling of glomerular architecture is possible, which would imply some form of regeneration of the capillary network [53]. Recent clinical trials suggested that inhibition of RAS might actually prevent nephropathy in patients with chronic renal failure of nondiabetic origin (the Ramipril Efficacy in Nephropathy study) [57]. The effectiveness of ACEi in protecting the kidney against the development of microalbuminuria, which is a major risk factor for cardiovascular events and death, has been also documented in patients with type 2 diabetes (the Bergamo Nephrologic Diabetes Complications Trial study) [56].
Strategies able to reduce renal disease progression could translate into a decreased incidence of cardiovascular events. A tremendous body of research, both experimental and clinical, has unequivocally shown that pharmacologic blockade of RAS, beyond the renal protection, reduces cardiovascular risk more effectively than other antihypertensive treatments [54]. Inhibition of RAS prevents end-organ damage associated with aging [14], in line with evidence that angiotensin II (Ang II) promotes the onset and the progression of vascular senescence, associated with vascular, functional, and structural changes contributing to age-related vascular disease [43].
In the present review, we focus on the recent emerging data suggesting a role of Ang II in aging. In addition we highlight the mechanisms by which Ang II via AT1 could affect life span in mammals.
The renin-angiotensin system
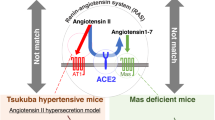
Renin-angiotensin system is considered to be the major regulator of blood pressure and fluid homeostasis. The main effector molecule of the RAS, Ang II, is produced from the substrate angiotensinogen through sequential enzymatic cleavages by renin and angiotensin converting enzyme (ACE). In particular renin cleaves angiotensinogen, forming Ang I that in turn is converted to Ang II by ACE (Fig. 1). ACE is a circulating enzyme found in the endothelial cells of the lung, vascular endothelium, and cell membranes of the kidney, heart, and brain. ACE also degrades bradykinin to inactive fragments, reducing the serum levels of endogenous vasodilators [8].
Ang II causes increases in systemic and local blood pressure via its vasoconstrictive effect, influences renal tubuli to retain sodium and water, and stimulates aldosterone release from adrenal gland [69]. Besides being a potent vasoconstrictor, Ang II exerts several prominent nonhemodynamic effects including proliferative, proinflammatory, and profibrotic activities [58].
At the cellular level, responsiveness to Ang II is conferred by the expression of two classes of pharmacologically distinct rhodopsin-like G protein-associated receptors, the type 1 and the type 2 receptors (AT1 and AT2) [61, 69]. AT1 has been cloned in a number of species and two subtypes [59], named AT1A and AT1B, have been identified in rat and mouse. AT1A is the predominantly expressed receptor in different body districts including kidney, liver, heart, blood vessels, adrenal glands, and cardiovascular control centers in the brain [11], and is considered the closest murine homolog to the single human AT1. AT1A confers most of the classical actions of Ang II such as blood pressure increase [36], aldosterone release from the adrenal zona glomerulosa [1], salt retention in renal proximal tubuli [42], and stimulation of the sympathetic nervous system via receptors in the brain [17]. The expression of the AT1B appears to be more prominent in the anterior pituitary gland and the adrenal zona glomerulosa. AT1B regulates blood pressure when AT1A is absent [48].
The expression of the AT2 is high in the fetus, but low in adult tissues. AT2 is expressed in the adrenal medulla, uterus, ovary, vascular endothelium, and distinct brain areas [65]. AT2 interacts with and modulates actions perpetuated by the AT1, possibly antagonizing many of its effects. The binding of Ang II to the AT2 activates vasorelaxation of conduit and resistant arteries and improves resistance artery remodeling, promotes cardiovascular protection against ischemia-reperfusion injury and acute myocardial infarction, inhibits cardiac fibrosis, and protects the kidney from ischemic injury [60]. In a mouse model of renal ablation, the lack of AT2 aggravates renal injury and reduces survival [6].
Link between angiotensin II and oxidative stress
Angiotensin II is known to contribute to oxidative stress damage by stimulating the generation of both nitric oxide (NO) and NAD(P)H oxidase-derived superoxide in the cytosol of different cell types including endothelial, vascular smooth muscle, fibroblast and tubular epithelial cells [51, 55]. The interaction between NO and superoxide generates peroxynitrite, a cytotoxic anion that inhibits mitochondrial electron transport, destroys DNA and cellular proteins, leading to oxidative stress damage [52]. Furthermore, Ang II can induce endothelial nitric oxide synthase (eNOS) uncoupling, switching from NO to superoxide production [46]. Ang II stimulates both cytosolic and mitochondrial reactive oxygen species (ROS) generation [64] (Fig. 2). The direct interaction between Ang II and mitochondrial components has been suggested by the presence of Ang II in mitochondria of brain, heart, and smooth muscle cell in rodent [22]; moreover, renin, angiotensinogen, and ACE were also detected within intramitochondrial dense bodies [50].
Schematic representation of Ang II-induced oxidative stress damage. Ang II via AT1 receptor promotes oxidative stress by activating NADP(H) oxidase-derived superoxide generation and by inducing eNOS uncoupling switching from NO to superoxide production. Ang II may also have a direct action on mitochondrial ROS production, independent of AT1-receptor signaling
One of the most prominent theories to explain aging is the “free-radical theory” of aging which was initially proposed by Harman in 1950 s [30]. It postulates that the loss of cell functional capacity associated to senescence results from the accumulation of ROS-inflicted oxidative stress damage to different molecules, leading to lipid peroxidation, protein oxidation and oxidative modifications in nuclear and mitochondrial DNA [21].
Reactive oxygen species are generated in multiple compartments and by multiple enzymes within the cells, including NAD(P)H oxidases on plasma membranes, lipid metabolism within the peroxisomes, and various cytosolic enzymes such as cyclooxygenase. The majority of intracellular ROS production derives from mitochondrial matrix and the space between the inner and outer mitochondrial membrane. Mitochondria utilize more than 90% of cellular oxygen to produce energy. While most oxygen is transformed into water, 1–2% of it forms superoxide [7]. Reactive oxygen species compromise mitochondrial integrity and function, leading to a decreased mitochondrial ATP generation, with a subsequent increased release of ROS by the mitochondria themselves, initiating a vicious cycle of progressively increasing oxidative stress [23]. The aging process is frequently associated to a reduction in mitochondrial number and several changes in mitochondrial structure, such as swelling, shortening of the cristae, and matrix vacuolization [10, 31, 67].
Under normal physiological conditions, the capacity of Ang II to promote oxidative stress is tightly regulated [20, 27]. By contrast, in conditions associated with RAS overactivation, such as aging [3, 68, 70], the dysregulation of Ang II-dependent ROS generation may become a significant contributor to cell oxidation and tissue damage. RAS overactivation exerts deleterious effects on renal and cardiac functions documented by the increase of Ang II peptide in urines [25] and increased generation of Ang II in the heart [28] of old animals. A recent in vitro study has demonstrated that the production of ROS induced by Ang II via AT1 led to DNA damage, and consequently to accelerated aging of human vascular smooth muscle cells [32]. Cell senescence following ROS production has been proposed to be mediated by two different mechanisms of DNA damage: a telomere-independent pathway via the induction of stress induced premature senescence (SIPS) and a telomere-dependent mechanism via accelerated attrition of telomeres. This hypothesis has been confirmed by data showing that the critical DNA damage induced by AT1-mediated ROS production both increased SIPS expressions that promoted cell cycle arrest and markedly accelerated the rate of telomere loss that is associated with reduced cellular proliferation and premature cell senescence [32].
All these findings demonstrate the crucial role of oxidative stress on the aging process and strongly support the involvement of Ang II in tissue senescence by virtue of its ability to mediate the release of oxidant species.
Protective effect of inhibiting angiotensin II on aging
Angiotensin-converting enzyme inhibitors and ARBs are two widely used classes of anti-hypertensive drugs that inhibit RAS at different levels. ACEi inhibit Ang II formation by binding to the active site of the enzyme that converts Ang I into Ang II, and ARBs prevent Ang II from binding to its receptors.
In aging animals, the cardiovascular protective effects occurred after RAS inhibition was associated with an increased NOS activity [26]. Moreover, in old animals, both enalapril and losartan treatments significantly increased NO production in heart homogenate, while reduced hydrogen peroxide formation [15]. In spontaneously hypertensive rats, the inhibition of RAS was able to reverse the naturally age-related and advanced myocardial hypertrophy and fibrosis by attenuating Ang II-mediated oxidative stress, as documented by reduced expression of NAD(P)H oxidative components p22phox, p47phox, and gp91phox in old hearts [37]. Furthermore, oxygen radicals mediated the accelerated cerebral endothelial dysfunction that occurs with age, and more importantly, old mice lacking AT1 did not develop these age-related cerebral circulation damages [45].
Other studies performed in normal adult rats have clearly shown that chronic treatment with ACEi or ARB reduced kidney damage associated with age. Old animals treated with enalapril and losartan presented lower glomerular and tubulointerstitial fibrosis, reduced monocyte or macrophage infiltrates, and decreased tubular atrophy than untreated aged animals [24].
The beneficial effect of RAS inhibition involves the preservation of renal mitochondria from aging in rats. Enalapril and losartan treatments prevented the age-associated decline in the renal mitochondrial capacity for energy production and attenuated the age-associated increase in mitochondrial oxidant production [19].
A similar protective effect of RAS inhibition was also observed in the liver from old rats. In these animals the maintenance of an adequate mitochondrial function during aging was due to the enhanced transcription levels of the genes nuclear respiratory factor 1 and peroxisome proliferators activator receptor gamma coactivator-1α that are involved in mitochondrial respiration and biogenesis, respectively. These positive effects on mitochondria maintained the integrity of the hepatocyte system, and prevented liver fibrosis and the infiltration of inflammatory cells during aging [18].
The development of gene-targeting technology in mice has provided new insight into the role of RAS genes in regulating blood pressure, body fluid homeostasis, and fetal development. Mice that are unable to generate Ang II because of targeted mutation in the angiotensinogen (Agt −/−) or angiotensin-converting enzyme (Ace −/−) genes had a severe phenotype characterized by reduced survival, low blood pressure, and abnormal kidney morphology. A similar phenotype was observed in mice lacking both Ang II type 1 receptors (AT1A −/− AT1B −/−) [49].
The disruption of the gene encoding AT1A (Agtr1a)—the major mouse AT1 receptor isoform—did not cause severe postnatal mortality or the structural abnormalities seen in the kidneys of the knockout models described above. Taking advantage from this mouse model, we have recently investigated the role of the AT1 in end-stage organ damage. A prospective observational study was performed in homozygous mice deficient for the AT1A and wild-type controls. AT1A −/− mice substantially outlived their wild-type littermates by 26% (Fig. 3) and had normal body weight and physical activity as reflected by their ability to perform on a rotating system that evaluates motor coordination and vitality. Reduction in food intake of 20% and 40% in laboratory animals extends their life span by up to 50% [29]. Reduced caloric intake did not contribute to prolonged survival in AT1A −/− mice, since daily food intake was virtually identical between AT1A −/− and wild-type mice. AT1A −/− grew up normally, and the body weights increased comparably to wild-type littermates ruling out the possibility that small body size could be responsible of extended life span as previously described [9].
Aging AT1A −/− mice developed fewer aortic atherosclerotic lesions and less cardiac injury, as reflected by the reduction of myocyte size and fibrosis, with lower deposition of interstitial collagen with respect to wild-type mice [5]. These data point to a direct effect of Ang II via AT1A on atherosclerotic lesion generation and on extracellular matrix deposition by cardiac fibroblasts.
Furthermore, aging mice lacking the AT1A showed reduced production of peroxinitrite in hearts and aortas, as compared to wild-type animals, indicating a possible role of Ang II via AT1A into the production of ROS [5]. Given the crucial role of mitochondria in producing peroxynitrite during aging processes [39], ultrastructural analysis of mitochondria was performed in proximal tubular cells of the kidney of AT1A −/− mice that possess a large number of mitochondria and are highly dependent on mitochondrial energy production for proper function [33]. The lack of AT1A protected the cells from the loss of mitochondria during aging [5], demonstrating that Ang II negatively influences mitochondrial number and function by promoting oxidative stress, and that the absence of AT1A strongly attenuated the functional and structural changes that occur in kidney mitochondria following oxidative stress increase upon age [5].
Role of sirtuins in longevity associated with AT1A −/− mice
Recent evidences have suggested that mitochondrial activity could be regulated by the expression of enzymes belonging to the Sirtuin family [16]. Sirtuins are nicotinamide adenine dinucleotide (NAD)-dependent deacetylases proteins highly conserved from Escherichia Coli to humans and associated with longevity, mitochondrial and cell cycle regulation, apoptosis, and DNA damage repair [29]. In humans and mice, there are seven different sirtuins (SIRT1-7), and three are located in the mitochondria (SIRT3, 4, and 5). Among them, SIRT3 has an apparent direct link to extended life span in humans, in fact mutations in an enhancer region of the Sirt3 gene that potentially upregulate its expression were found at a high frequency in long-lived individuals [4]. Under oxidative stress, SIRT3 overexpression protects the cardiomyocytes against Bax-mediated apoptosis by deacetylating the substrate Ku70, promoting the binding of Ku70 to Bax, and hence blocking the Bax activation [66]. Of note, SIRT3 regulates adaptive thermogenesis and decreases mitochondrial membrane potential and reactive oxygen species production, while increasing cellular respiration [62]. For these reasons SIRT3 acts as sensor of small reactive oxygen species that could lead to mitochondrial damage and activates specific cellular signaling pathway to counteract oxidative stress such as the expression of MnSOD antioxidant protein [38]. The recent identification of the two substrates such as acetyl coenzyme A synthetase and glutamate dehydrogenase as targets of SIRT3 revealed that this molecule controls a regulatory network involved in energy metabolism and in mechanisms of caloric restriction and life span determination [40, 41].
SIRT3 could exert its action only in the presence of the cosubstrate NAD+, and the concentration of NAD+ determines cell survival. In the context of nutrient restriction, mitochondria dictate cell survival through the upregulation of nicotinamide phosphoribosyltransferase (Nampt) that boosts mitochondrial NAD+ concentration [71]. Altogether these findings prompted us to study Sirt3 and Nampt survival genes in AT1A −/− mice. Transcript levels of both Nampt and Sirt3 were increased in kidneys from AT1A −/− mice with respect to wild-type animals. The finding that candesartan, an AT1 receptor antagonist, prevented Ang II-induced Nampt and Sirt3 mRNA reduction in cultured tubular epithelial cells suggested a possible biochemical link between Ang II and survival genes, which conceivably operates via the AT1A. Furthermore, experiments showing that Nampt gene silencing by siRNA limited the reduction of Sirt3 mRNA induced by Ang II would indicate a causative role of Nampt in modulating Sirt3 gene transcription in response to Ang II [5].
Caloric restriction prolongs the life span through an increase of sirtuins [29, 63]. In rodents and humans the levels of Sir2 ortholog SIRT1, that targets numerous regulatory factors affecting stress management and metabolism, increase in response to caloric restriction and this increase causes favorable changes in metabolism and stress tolerance [13].
The sirtuins are also involved in prolonged survival induced by resveratrol [2], a small molecule found in red wine which activates SIRT1 and mimics the anti-aging effect of caloric restriction. The effect of resveratrol on life span is associated with increased mitochondrial number and is dependent on the upregulation of Sir2 [35]. Moreover, resveratrol downregulates AT1 through SIRT1 activation in cultured vascular smooth muscle cells and mouse aorta implying that inhibition of the AT1 contributes to resveratrol-induced longevity [44].
In the kidney from AT1A −/− mice the levels of SIRT1 were comparable to wild-type mice, suggesting that the increased longevity of this mouse strain is independent from the SIRT1 pathway.
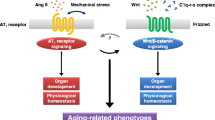
All these findings support a role of SIRT3 in the prolongation of life span, and the manipulation of the RAS system provides a remarkable beneficial effect on longevity by reducing oxidative stress and upregulating survival genes (Fig. 4).
Conclusions
Chronic activation of RAS plays an important role in the promotion of end-stage organ damage associated with aging by increasing tissue and mitochondrial oxidative stress. Therapies targeting RAS (ACEi and ARBs) reduce age-associated cardiovascular and renal damage and preserve the number and the function of mitochondria. A stronger protective effect, demonstrated by a significant prolongation of life span, was observed in genetically modified mice, which lack the AT1A gene. In these mice, the longevity is the consequence of reduced mitochondrial damage due to the attenuation of oxidative stress and the upregulation of Nampt and Sirt3 survival genes.
The extension of the life span observed in AT1A −/− mice is comparable to that of mice lacking the insulin growth factor-1 (IGF-1) receptor [34]. However the manipulation of the latter pathway in humans is not imminently feasible. In contrast, Ang II type 1 receptor antagonists have been proven safe, well-tolerated for chronic use and represent a key component of the modern therapy for hypertension and cardiac failure. Thus, the inhibition of AT1 could represent a possible therapeutic strategy for diseases of aging and possibly for extending the life span. Further studies are necessary to deepen the role of AT1 in humans and to understand whether the receptor function is similar to that found in animals.
Abbreviations
- RAS:
-
renin-angiotensin system
- Ang II:
-
angiotensin II
- ACE:
-
angiotensin converting enzyme
- AT1 :
-
Ang II type 1 receptor
- AT2 :
-
Ang II type 2 receptor
- NO:
-
nitric oxide
- eNOS:
-
endothelial nitric oxide synthase
- ROS:
-
reactive oxygen species
- ACEi:
-
angiotensin-converting enzyme inhibitors
- ARBs:
-
angiotensin II receptor blockers
- SIRT:
-
sirtuin
- Nampt:
-
nicotinamide phosphoribosyltransferase
- IGF-1:
-
insulin growth factor-1
References
Aguilera G (1992) Role of angiotensin II receptor subtypes on the regulation of aldosterone secretion in the adrenal glomerulosa zone in the rat. Mol Cell Endocrinol 90:53–60
Baur JA, Pearson KJ, Price NL, Jamieson HA, Lerin C, Kalra A, Prabhu VV, Allard JS, Lopez-Lluch G, Lewis K, Pistell PJ, Poosala S, Becker KG, Boss O, Gwinn D, Wang M, Ramaswamy S, Fishbein KW, Spencer RG, Lakatta EG, Le Couteur D, Shaw RJ, Navas P, Puigserver P, Ingram DK, de Cabo R, Sinclair DA (2006) Resveratrol improves health and survival of mice on a high-calorie diet. Nature 444:337–342
Baylis C, Engels K, Hymel A, Navar LG (1997) Plasma renin activity and metabolic clearance rate of angiotensin II in the unstressed aging rat. Mech Ageing Dev 97:163–172
Bellizzi D, Rose G, Cavalcante P, Covello G, Dato S, De Rango F, Greco V, Maggiolini M, Feraco E, Mari V, Franceschi C, Passarino G, De Benedictis G (2005) A novel VNTR enhancer within the SIRT3 gene, a human homologue of SIR2, is associated with survival at oldest ages. Genomics 85:258–263
Benigni A, Corna D, Zoja C, Sonzogni A, Latini R, Salio M, Conti S, Rottoli D, Longaretti L, Cassis P, Morigi M, Coffman TM, Remuzzi G (2009) Disruption of the Ang II type 1 receptor promotes longevity in mice. J Clin Invest 119:524–530
Benndorf RA, Krebs C, Hirsch-Hoffmann B, Schwedhelm E, Cieslar G, Schmidt-Haupt R, Steinmetz OM, Meyer-Schwesinger C, Thaiss F, Haddad M, Fehr S, Heilmann A, Helmchen U, Hein L, Ehmke H, Stahl RA, Boger RH, Wenzel UO (2009) Angiotensin II type 2 receptor deficiency aggravates renal injury and reduces survival in chronic kidney disease in mice. Kidney Int 75:1039–1049
Boveris A, Chance B (1973) The mitochondrial generation of hydrogen peroxide. General properties and effect of hyperbaric oxygen. Biochem J 134:707–716
Brewster UC, Perazella MA (2004) The renin-angiotensin-aldosterone system and the kidney: effects on kidney disease. Am J Med 116:263–272
Brown-Borg HM, Borg KE, Meliska CJ, Bartke A (1996) Dwarf mice and the ageing process. Nature 384:33
Burns EM, Kruckeberg TW, Comerford LE, Buschmann MT (1979) Thinning of capillary walls and declining numbers of endothelial mitochondria in the cerebral cortex of the aging primate, Macaca nemestrina. J Gerontol 34:642–650
Burson JM, Aguilera G, Gross KW, Sigmund CD (1994) Differential expression of angiotensin receptor 1A and 1B in mouse. Am J Physiol 267:E260–E267
Christensen K, Johnson TE, Vaupel JW (2006) The quest for genetic determinants of human longevity: challenges and insights. Nat Rev Genet 7:436–448
Cohen HY, Miller C, Bitterman KJ, Wall NR, Hekking B, Kessler B, Howitz KT, Gorospe M, de Cabo R, Sinclair DA (2004) Calorie restriction promotes mammalian cell survival by inducing the SIRT1 deacetylase. Science 305:390–392
Cohn JN, Goldman JM (2008) Establishing a new option for target-organ protection: rationale for ARB plus ACE inhibitor combination therapy. Am J Hypertens 21:248–256
Costa LE, La-Padula P, Lores-Arnaiz S, D’Amico G, Boveris A, Kurnjek ML, Basso N (2002) Long-term angiotensin II inhibition increases mitochondrial nitric oxide synthase and not antioxidant enzyme activities in rat heart. J Hypertens 20:2487–2494
Dali-Youcef N, Lagouge M, Froelich S, Koehl C, Schoonjans K, Auwerx J (2007) Sirtuins: the ‘magnificent seven’, function, metabolism and longevity. Ann Med 39:335–345
Davisson RL, Oliverio MI, Coffman TM, Sigmund CD (2000) Divergent functions of angiotensin II receptor isoforms in the brain. J Clin Invest 106:103–106
de Cavanagh EM, Flores I, Ferder M, Inserra F, Ferder L (2008) Renin-angiotensin system inhibitors protect against age-related changes in rat liver mitochondrial DNA content and gene expression. Exp Gerontol 43:919–928
de Cavanagh EM, Piotrkowski B, Basso N, Stella I, Inserra F, Ferder L, Fraga CG (2003) Enalapril and losartan attenuate mitochondrial dysfunction in aged rats. FASEB J 17:1096–1098
de Cavanagh EM, Piotrkowski B, Fraga CG (2004) Concerted action of the renin-angiotensin system, mitochondria, and antioxidant defenses in aging. Mol Aspects Med 25:27–36
Droge W, Schipper HM (2007) Oxidative stress and aberrant signaling in aging and cognitive decline. Aging Cell 6:361–370
Erdmann B, Fuxe K, Ganten D (1996) Subcellular localization of angiotensin II immunoreactivity in the rat cerebellar cortex. Hypertension 28:818–824
Esposito LA, Melov S, Panov A, Cottrell BA, Wallace DC (1999) Mitochondrial disease in mouse results in increased oxidative stress. Proc Natl Acad Sci U S A 96:4820–4825
Ferder LF, Inserra F, Basso N (2002) Advances in our understanding of aging: role of the renin-angiotensin system. Curr Opin Pharmacol 2:189–194
Gilliam-Davis S, Payne VS, Kasper SO, Tommasi EN, Robbins ME, Diz DI (2007) Long-term AT1 receptor blockade improves metabolic function and provides renoprotection in Fischer-344 rats. Am J Physiol Heart Circ Physiol 293:H1327–H1333
Gonzalez Bosc LV, Kurnjek ML, Muller A, Terragno NA, Basso N (2001) Effect of chronic angiotensin II inhibition on the nitric oxide synthase in the normal rat during aging. J Hypertens 19:1403–1409
Griendling KK, Minieri CA, Ollerenshaw JD, Alexander RW (1994) Angiotensin II stimulates NADH and NADPH oxidase activity in cultured vascular smooth muscle cells. Circ Res 74:1141–1148
Groban L, Pailes NA, Bennett CD, Carter CS, Chappell MC, Kitzman DW, Sonntag WE (2006) Growth hormone replacement attenuates diastolic dysfunction and cardiac angiotensin II expression in senescent rats. J Gerontol A Biol Sci Med Sci 61:28–35
Guarente L (2006) Sirtuins as potential targets for metabolic syndrome. Nature 444:868–874
Harman D (1956) Aging: a theory based on free radical and radiation chemistry. J Gerontol 11:298–300
Herbener GH (1976) A morphometric study of age-dependent changes in mitochondrial population of mouse liver and heart. J Gerontol 31:8–12
Herbert KE, Mistry Y, Hastings R, Poolman T, Niklason L, Williams B (2008) Angiotensin II-mediated oxidative DNA damage accelerates cellular senescence in cultured human vascular smooth muscle cells via telomere-dependent and -independent pathways. Circ Res 102:201–208
Heudes D, Michel O, Chevalier J, Scalbert E, Ezan E, Bariety J, Zimmerman A, Corman B (1994) Effect of chronic ANG I-converting enzyme inhibition on aging processes. I. Kidney structure and function. Am J Physiol 266:R1038–R1051
Holzenberger M, Dupont J, Ducos B, Leneuve P, Geloen A, Even PC, Cervera P, Le Bouc Y (2003) IGF-1 receptor regulates lifespan and resistance to oxidative stress in mice. Nature 421:182–187
Howitz KT, Bitterman KJ, Cohen HY, Lamming DW, Lavu S, Wood JG, Zipkin RE, Chung P, Kisielewski A, Zhang LL, Scherer B, Sinclair DA (2003) Small molecule activators of sirtuins extend Saccharomyces cerevisiae lifespan. Nature 425:191–196
Ito M, Oliverio MI, Mannon PJ, Best CF, Maeda N, Smithies O, Coffman TM (1995) Regulation of blood pressure by the type 1A angiotensin II receptor gene. Proc Natl Acad Sci U S A 92:3521–3525
Ito N, Ohishi M, Yamamoto K, Tatara Y, Shiota A, Hayashi N, Komai N, Yanagitani Y, Rakugi H, Ogihara T (2007) Renin-angiotensin inhibition reverses advanced cardiac remodeling in aging spontaneously hypertensive rats. Am J Hypertens 20:792–799
Jacobs KM, Pennington JD, Bisht KS, Aykin-Burns N, Kim HS, Mishra M, Sun L, Nguyen P, Ahn BH, Leclerc J, Deng CX, Spitz DR, Gius D (2008) SIRT3 interacts with the daf-16 homolog FOXO3a in the mitochondria, as well as increases FOXO3a dependent gene expression. Int J Biol Sci 4:291–299
Krishnan KJ, Greaves LC, Reeve AK, Turnbull DM (2007) Mitochondrial DNA mutations and aging. Ann N Y Acad Sci 1100:227–240
Law IK, Liu L, Xu A, Lam KS, Vanhoutte PM, Che CM, Leung PT, Wang Y (2009) Identification and characterization of proteins interacting with SIRT1 and SIRT3: implications in the anti-aging and metabolic effects of sirtuins. Proteomics 9:2444–2456
Lombard DB, Alt FW, Cheng HL, Bunkenborg J, Streeper RS, Mostoslavsky R, Kim J, Yancopoulos G, Valenzuela D, Murphy A, Yang Y, Chen Y, Hirschey MD, Bronson RT, Haigis M, Guarente LP, Farese RV Jr, Weissman S, Verdin E, Schwer B (2007) Mammalian Sir2 homolog SIRT3 regulates global mitochondrial lysine acetylation. Mol Cell Biol 27:8807–8814
Masilamani S, Kim GH, Mitchell C, Wade JB, Knepper MA (1999) Aldosterone-mediated regulation of ENaC alpha, beta, and gamma subunit proteins in rat kidney. J Clin Invest 104:R19–R23
Min LJ, Mogi M, Iwai M, Horiuchi M (2009) Signaling mechanisms of angiotensin II in regulating vascular senescence. Ageing Res Rev 8:113–121
Miyazaki R, Ichiki T, Hashimoto T, Inanaga K, Imayama I, Sadoshima J, Sunagawa K (2008) SIRT1, a longevity gene, downregulates angiotensin II type 1 receptor expression in vascular smooth muscle cells. Arterioscler Thromb Vasc Biol 28:1263–1269
Modrick ML, Didion SP, Sigmund CD, Faraci FM (2009) Role of oxidative stress and AT1 receptors in cerebral vascular dysfunction with aging. Am J Physiol Heart Circ Physiol 296:H1914–H1919
Mollnau H, Wendt M, Szocs K, Lassegue B, Schulz E, Oelze M, Li H, Bodenschatz M, August M, Kleschyov AL, Tsilimingas N, Walter U, Forstermann U, Meinertz T, Griendling K, Munzel T (2002) Effects of angiotensin II infusion on the expression and function of NAD(P)H oxidase and components of nitric oxide/cGMP signaling. Circ Res 90:E58–E65
Morris BJ (2005) A forkhead in the road to longevity: the molecular basis of lifespan becomes clearer. J Hypertens 23:1285–1309
Oliverio MI, Coffman TM (2000) Angiotensin II receptor physiology using gene targeting. News Physiol Sci 15:171–175
Oliverio MI, Kim HS, Ito M, Le T, Audoly L, Best CF, Hiller S, Kluckman K, Maeda N, Smithies O, Coffman TM (1998) Reduced growth, abnormal kidney structure, and type 2 (AT2) angiotensin receptor-mediated blood pressure regulation in mice lacking both AT1A and AT1B receptors for angiotensin II. Proc Natl Acad Sci U S A 95:15496–15501
Peters J, Kranzlin B, Schaeffer S, Zimmer J, Resch S, Bachmann S, Gretz N, Hackenthal E (1996) Presence of renin within intramitochondrial dense bodies of the rat adrenal cortex. Am J Physiol 271:E439–E450
Pueyo ME, Arnal JF, Rami J, Michel JB (1998) Angiotensin II stimulates the production of NO and peroxynitrite in endothelial cells. Am J Physiol 274:C214–C220
Radi R, Beckman JS, Bush KM, Freeman BA (1991) Peroxynitrite-induced membrane lipid peroxidation: the cytotoxic potential of superoxide and nitric oxide. Arch Biochem Biophys 288:481–487
Remuzzi G, Benigni A, Remuzzi A (2006) Mechanisms of progression and regression of renal lesions of chronic nephropathies and diabetes. J Clin Invest 116:288–296
Remuzzi G, Perico N, Macia M, Ruggenenti P (2005) The role of renin-angiotensin-aldosterone system in the progression of chronic kidney disease. Kidney Int Suppl 99:S57–S65
Rueckschloss U, Quinn MT, Holtz J, Morawietz H (2002) Dose-dependent regulation of NAD(P)H oxidase expression by angiotensin II in human endothelial cells: protective effect of angiotensin II type 1 receptor blockade in patients with coronary artery disease. Arterioscler Thromb Vasc Biol 22:1845–1851
Ruggenenti P, Fassi A, Ilieva AP, Bruno S, Iliev IP, Brusegan V, Rubis N, Gherardi G, Arnoldi F, Ganeva M, Ene-Iordache B, Gaspari F, Perna A, Bossi A, Trevisan R, Dodesini AR, Remuzzi G (2004) Preventing microalbuminuria in type 2 diabetes. N Engl J Med 351:1941–1951
Ruggenenti P, Perna A, Gherardi G, Garini G, Zoccali C, Salvadori M, Scolari F, Schena FP, Remuzzi G (1999) Renoprotective properties of ACE-inhibition in non-diabetic nephropathies with non-nephrotic proteinuria. Lancet 354:359–364
Ruster C, Wolf G (2006) Renin-angiotensin-aldosterone system and progression of renal disease. J Am Soc Nephrol 17:2985–2991
Sasaki K, Yamano Y, Bardhan S, Iwai N, Murray JJ, Hasegawa M, Matsuda Y, Inagami T (1991) Cloning and expression of a complementary DNA encoding a bovine adrenal angiotensin II type-1 receptor. Nature 351:230–233
Schulman IH, Raij L (2008) The angiotensin II type 2 receptor: what is its clinical significance? Curr Hypertens Rep 10:188–193
Shanmugam S, Sandberg K (1996) Ontogeny of angiotensin II receptors. Cell Biol Int 20:169–176
Shi T, Wang F, Stieren E, Tong Q (2005) SIRT3, a mitochondrial sirtuin deacetylase, regulates mitochondrial function and thermogenesis in brown adipocytes. J Biol Chem 280:13560–13567
Sinclair DA (2005) Toward a unified theory of caloric restriction and longevity regulation. Mech Ageing Dev 126:987–1002
Sorescu D, Griendling KK (2002) Reactive oxygen species, mitochondria, and NAD(P)H oxidases in the development and progression of heart failure. Congest Heart Fail 8:132–140
Steckelings UM, Kaschina E, Unger T (2005) The AT2 receptor–a matter of love and hate. Peptides 26:1401–1409
Sundaresan NR, Samant SA, Pillai VB, Rajamohan SB, Gupta MP (2008) SIRT3 is a stress-responsive deacetylase in cardiomyocytes that protects cells from stress-mediated cell death by deacetylation of Ku70. Mol Cell Biol 28:6384–6401
Tauchi H, Sato T (1968) Age changes in size and number of mitochondria of human hepatic cells. J Gerontol 23:454–461
Thompson MM, Oyama TT, Kelly FJ, Kennefick TM, Anderson S (2000) Activity and responsiveness of the renin-angiotensin system in the aging rat. Am J Physiol Regul Integr Comp Physiol 279:R1787–R1794
Timmermans PB, Wong PC, Chiu AT, Herblin WF, Benfield P, Carini DJ, Lee RJ, Wexler RR, Saye JA, Smith RD (1993) Angiotensin II receptors and angiotensin II receptor antagonists. Pharmacol Rev 45:205–251
Wang M, Takagi G, Asai K, Resuello RG, Natividad FF, Vatner DE, Vatner SF, Lakatta EG (2003) Aging increases aortic MMP-2 activity and angiotensin II in nonhuman primates. Hypertension 41:1308–1316
Yang H, Yang T, Baur JA, Perez E, Matsui T, Carmona JJ, Lamming DW, Souza-Pinto NC, Bohr VA, Rosenzweig A, de Cabo R, Sauve AA, Sinclair DA (2007) Nutrient-sensitive mitochondrial NAD + levels dictate cell survival. Cell 130:1095–1107
Acknowledgements
Paola Cassis is a recipient of a fellowship from Associazione Ricerca Trapianti (ART), Milan, Italy, and Sara Conti is a recipient of a fellowship from Fondazione Aiuti per la Ricerca sulle Malattie Rare (ARMR) in memory of Lidia D’Arcangelo, Bergamo, Italy. The research was partially supported by the European Commission within the EuReGene project (LSHG-CT-2004–005085).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Cassis, P., Conti, S., Remuzzi, G. et al. Angiotensin receptors as determinants of life span. Pflugers Arch - Eur J Physiol 459, 325–332 (2010). https://doi.org/10.1007/s00424-009-0725-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00424-009-0725-4