Abstract
Purpose
Endoplasmic reticulum (ER) stress is known to play key roles in the development of endothelial cell apoptosis induced by chronic intermittent hypoxia (CIH), and the angiotensin II–phospholipase C–inositol-1,4,5-triphosphate (AngII-PLC-IP3) pathway has been demonstrated to induce ER stress. To explore whether the AngII-PLC-IP3 pathway is involved in the vascular damage induced by CIH, we examined whether the AngII-PLC-IP3 pathway is involved in ER stress induced by CIH and whether losartan, a selective angiotensin II type 1 receptor (AT1R) blocker, could suppress endothelial cell apoptosis induced by CIH.
Methods
Adult male Sprague Dawley rats were subjected to 8 h/day of intermittent hypoxia/normoxia, with or without losartan, a selective AT1R blocker, and/or U73122, a selective PLC inhibitor, for 8 weeks. Endothelial cell apoptosis, ER stress markers, and levels of PLC-γ1 and IP3R expression were determined.
Results
Losartan prevented increases in PLC-γ1 and IP3R protein levels and inhibited ER stress markers induced by CIH. Addition of U73122 reproduced all the protective effects of losartan. Losartan administration before CIH significantly ameliorated CIH-induced endothelial cell apoptosis.
Conclusions
This study showed that the AngII-PLC-IP3 pathway is involved in ER stress induced by CIH and that pre-losartan administration ameliorates endothelial cell apoptosis following CIH partly via inhibition of the AngII-PLC-IP3 pathway and ER stress.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Obstructive sleep apnea syndrome (OSAS), which is characterized by chronic, repetitive short cycles of oxygen desaturation followed by rapid reoxygenation (chronic intermittent hypoxia (CIH)), has become a public health concern. CIH is the most characteristic feature in the pathophysiology of OSAS. Cardiovascular complications are the most severe clinical complications induced by CIH [1, 2], and OSAS disease severity is positively associated with the degree of cardiovascular disease [3]. Although a number of factors involved in OSAS result in cardiovascular complications, CIH causes vascular damage, such as arterial endothelial cell apoptosis, which is considered to play a key role. In our previous experiments, we demonstrated that intermittent hypoxia could induce aortic endothelial cell apoptosis via endoplasmic reticulum (ER) stress [3]. However, how CIH induces ER stress remains unclear.
Several studies have found that ER stress is closely related to the angiotensin II–phospholipase C–inositol-1,4,5-triphosphate (AngII-PLC-IP3) pathway. Circulating AngII is increased in patients with OSAS and in experimental animals exposed to CIH [4], and AngII levels are closely related to the degree of OSAS and vascular disease. Most of the physiological actions of AngII are mediated through its actions on the angiotensin II type 1 receptor (AT1R) [5]. AngII increases neonatal cardiomyocyte apoptosis, dependent on AT1R activation [6]. Increased AT1R expression results in AngII-dependent cardiac fibroblast apoptosis via the PLC signaling pathway, and PLC inhibitor prevents the effect of AngII on pro-apoptotic signal activation in AT1R-transduced cardiac fibroblasts [7]. Stimulation of the AT1 receptor activates PLC, which then cleaves phosphatidylinositol 4,5-bisphosphate into IP3 and diacylglycerol (DAG). IP3 induces Ca2+release into the cytosol from the ER. The release of Ca2+ from the ER, in turn, activates nonselective cation channels, such as transient receptor potential channels (TRPCs), at the plasma membrane, thereby promoting Ca2+ entry from extracellular and plasma membrane depolarization and subsequent elevated concentrations of intracellular Ca2+ [8–10]. In addition, DAG and IP3 production will also result in elevated cytosolic Ca2+ concentrations from intracellular sources and Ca2+ influx from the extracellular medium [11]. The subsequent loss of intracellular Ca2+ homeostasis suppresses post-translational protein modification. Consequently, misfolded proteins accumulate and trigger ER stress-response pathways [12]. An increase in intracellular Ca2+ levels due to excessive Ca2+ influx has been implicated in the activation of cell death [13]. PLC is central to the core machinery for the phosphoinositide signal transduction pathway [14]. Phosphatidylinositol (PI)-PLC consists of a family of four classes, including PLC-β, PLC-γ, PLC-δ, and PLC-ε, encoded by different genes [14, 15]. PLC-γ1 activation can induce apoptosis by Ca2+ flux and [Ca2+]i overload [16], and PLC inhibition can reduce the concentration of intracellular Ca2+ [8].
Losartan, a selective AT1R blocker, prevents CIH-induced vasodilatory impairment by preserving endothelial function [4]. Furthermore, losartan and its metabolites can suppress tumor necrosis factor (TNF)-induced endothelial cell apoptosis by activating the vascular endothelial growth factor 2/phosphatidylinositol-3-kinase/protein kinase B (VEGFR2/PI3K/Akt) pathway independently of AT1R-mediated signaling [17]. Human coronary artery endothelial cell apoptosis caused by AngII was also reduced by losartan treatment [18]. Here, we used losartan to determine whether the AngII-PLC-IP3 pathway is involved in ER stress induced by CIH. In the present work, a rodent model was used to observe the effect of losartan inhibition on CIH-damaged arterial endothelial cells in vivo.
Methods
Animal model and experimental design
Sixty-four male Sprague Dawley (SD) rats (220–250 g) were purchased from the experimental animal center of Wuhan University (Wuhan, China). Animals were maintained in a departmental animal facility on a 12-h light/12-h dark cycle under standard laboratory conditions (temperature, 25 ± 2 °C; humidity, 60 ± 5%). Rats were provided with standard rodent chow and allowed free access to water. Experimental procedures were approved by the Institutional Animal Care and Use Committee (IACUC) of Tongji Medical College at Huazhong University of Science and Technology. Rats were randomly divided into eight groups (n = 8 each): normoxia, normoxia + losartan, CIH, and CIH + losartan; normoxia + U73122, normoxia + losartan + U73122, CIH + U73122, and CIH + losartan + U73122. Rats were administered either losartan (30 mg/kg dissolved in double-distilled water) by oral gavage [4] or U73122 (30 mg/kg) by intraperitoneal injection [19] prior to exposure to intermittent hypoxia every day of the 8-week experimental period.
Chronic intermittent hypoxia exposure
CIH was performed using custom-built chambers (OxyCycler A84, BioSpherix, Redfield, NY, USA) connected to a supply of O2 and N2 gas. The CIH protocol was as follows: the O2 level was reduced from 21 to 8% over a period of 120 s, held at 8% for 120 s, returned to 21% over a period of 50 s, and held at 21% for 300 s. The rats were exposed to intermittent hypoxia for 8 h/day (during the day) for 7 days/week over 8 weeks. For the normoxic group, rats were placed in similar chambers under normoxic conditions. Within 24 h after the last exposure, rats were euthanized with 10% chloral hydrate (0.3 ml/100 g administered by intraperitoneal injection). The aortic arch was excised from each rat, perfused with cold phosphate-buffered saline (PBS), and preserved in liquid nitrogen or 10% formalin for in vitro analyses.
Measurement of AngII
AngII levels in plasma were determined using a commercial enzyme-linked immunosorbent assay (ELISA) kit (RayBiotech, Norcross, GA, USA) according to the manufacturer’s instructions.
Transferase-mediated dUTP nick end labeling assay
Aortic arches were fixed with 4% paraformaldehyde overnight at 4 °C, and 4-mm paraffin sections were obtained. Embedded tissues were sectioned (5-mm slices). The sections were washed in PBS and incubated with transferase-mediated dUTP nick end labeling (TUNEL) solution for 60 min at 37 °C using an apoptosis detection kit (Roche Applied Science, USA). After washing twice in PBS, the sections were stained with 4′,6-diamidino-2-phenylindole (DAPI, Sigma, St. Louis, MO, USA) for 5 min. The sections were analyzed using confocal microscopy (SPII2-AOBS Leica). TUNEL-positive nuclei (fragmented DNA) fluoresced bright green at 450–500 nm, whereas DAPI-positive nuclei (intact DNA) fluoresced blue at 360 nm. The ratio of TUNEL-positive nuclei to total endotheliocyte nuclei was used to determine the extent of apoptosis.
Real-time quantitative RT-PCR
Tissues from the aortic arch were used for RT-PCR. Total RNA was extracted using TRIzol according to the manufacturer’s instructions. The concentration of total RNA was measured by spectrophotometry, and the OD260/OD280 ratio was used to assess RNA purity. Total RNA was reverse transcribed into cDNA, and PCR was performed using SYBR GREEN. Gene-specific primers were designed using Premier 5.0 and were synthesized by Sangon Biological Engineering Co., Ltd. (Shanghai, China). The following primers were used: GAPDH 5′-CGCTAACATCAAATGGGGTG-3′ and 5′-TTGCTGACAATCTTGAGGGAG-3′; AGT 5′-CTGACTGGGCTCCATGAGTTC-3′ and 5′-GCGGGTTCTTTATCCAAGTCA-3′; GRP78 5′-TCGTATGTGGCCTTCACTCC-3′ and 5′-TTCTTCTGGGGCAAATGTCT-3′; CHOP 5′-CACCTCCCAAAGCCCTCG-3′ and 5′-ACCACTCTGTTTCCGTTTCCTA-3′; ATF4 5′-TCGACCCAAACCTTATGACC-3′ and 5′-CCTCGTTCTTCTTTTCTAGCTC-3′; and sXBP1 5′-GCCTGTCCTTCCTTATGTCCA-3′ and 5′-AAAATCATTCAACGGGGATGC-3′. PCR was performed using the following conditions: the cycling profile started with denaturation at 95 °C for 30 s, followed by 40 cycles of 5 s at 95 °C and 34 s at 60 °C. For each gene, “no-template” and “no-amplification” controls were used. Subsequently, a melting curve analysis was performed to measure the specificity of the amplified products by their specific melting temperatures. Melting curve analysis consisted of a denaturation step at 95 °C for 15 s, after which the reactions were decreased to 60 °C for 1 min and then increased to 95 °C for 15 s. Data for each sample were normalized against GAPDH. AGT, GRP78, CHOP, ATF4, and sXBP1 messenger RNA (mRNA) expression levels are presented according to their changes relative to the control group.
Western blot analyses
Tissues from the aortic arch were used for Western blot analysis. Proteins were extracted from the tissue using radioimmunoprecipitation assay (RIPA) lysis buffer (Beyotime, Jiangsu, China) containing a protease inhibitor cocktail to prevent protein degradation. Protein concentration was determined using a Bradford protein assay kit (Bio-Rad, Hercules, CA, USA). Samples containing 50 μg of protein were separated in a 10% SDS–PAGE gel and then transferred to 0.45-μm pore size nitrocellulose membranes (Bio-Rad). Membranes were blocked in 5% nonfat dry milk in TBST (10 mM Tris–HCl, pH 7.5, 150 mM NaCl, 0.05% Tween-20) for 1 h at room temperature. Membranes were incubated with rat monoclonal anti-AT1R, anti-IP3R, anti-GRP78, anti-CHOP, anti-caspase12, and anti-PLC-γ1 antibodies overnight at 4 °C. Both primary antibodies were diluted 1:1000 with 5% nonfat dry milk in TBST. Membranes were then incubated with the secondary antibody conjugated to horseradish peroxidase (diluted 1:3000) at room temperature for 2 h. Reactive proteins were analyzed using an ECL Western blotting detection system. All experiments were performed three or more times.
Immunohistochemistry analysis
The expression levels of ER stress-related factors GRP78 and caspase12 were evaluated immunohistochemically in rat aortic endothelial cells using a streptavidin/peroxidase kit according to the manufacturer’s instructions. First, sections were deparaffinized, rehydrated and then immersed in antigen retrieval buffer for 3 min at 95 °C. Next, sections were incubated in 3% H2O2 for 25 min at room temperature to block endogenous peroxidase activity. The sections were washed three times with PBS and then incubated with rabbit anti-rat GRP78 and caspase12 antibodies (1:100 dilution in PBS). The sections were again washed three times with PBS and then incubated with 100 μl of biotinylated goat anti-rabbit IgG (1:200 dilution in PBS). Proteins were visualized with diaminobenzidine substrate solution. As negative controls, the primary antibody was replaced with PBS. Light microscopic images were obtained. The immunoreactivity levels of caspase12 and GRP78 were analyzed using Image-Pro Plus 6.0 software.
Immunofluorescence staining
Rat aortic arch specimens were frozen in Tissue-Tek Optimal Cutting Temperature compound (O.C.T., Sakura Finetek USA, Torrance, CA, USA) with liquid nitrogen. Five-micrometer-thick sections were cut using a cryostat (Leica, Buffalo Grove, IL, USA) and were stored at −80 °C. Sections were fixed before staining with a mixture of ethanol and 0.1% trichloroacetic acid for 15 min and were then blocked with PBS-AT (500 ml PBS, 10 g bovine serum albumin (BSA) grade J and 12.5 ml of 20% Triton X-100). Sections were incubated with CHOP primary and secondary antibodies at room temperature for 1 h, with three washes in PBS between incubation steps. Mounting medium (Vectashield with DAPI; Vector Laboratories, Burlingame, CA, USA) was added to the sections after three additional washes in PBS. Images were captured using spinning disk confocal microscopy on a Nikon Eclipse TE2000-E microscope (Melville, NY, USA) and were analyzed using the IPP software.
Cell culture and treatment
Human aortic endothelial cells were cultured in Dulbecco’s modified Eagle’s medium supplemented with 10% fetal bovine serum at 37 °C in a humidified 5% CO2 atmosphere. Cells were pre-incubated with 5 μM losartan or 2 μM U73122 under normoxic circumstances for 30 min. Cells exposed to CIH were maintained in a controlled hypoxia incubator for 4 h with a cycled O2 concentration at 5% O2 for 55 s and 21% O2 for 55 s (5% CO2; balanced N2 and water vapor; 37 °C); normoxic cells were maintained at atmospheric oxygen concentrations for 4 h (21% O2, 5% CO2; balanced N2 and water vapor; 37 °C).
Measurement of intracellular calcium ([Ca2 +]i)
Rat aortic endothelial cells were incubated in a working solution containing 10 μM Fluo-3/AM (acetoxymethyl ester form, Molecular Probes, Eugene, OR) and 0.03% Pluronic F-127 at 37 °C for 40 min. The cells were then rinsed three times with HBSS solution to remove any remaining dye. Changes in [Ca2 +]i are represented as fluorescent intensity (FI). During the experiment, the FI of Fluo-3/AM in endothelial cells was measured for 5 min using a laser scanning confocal microscope (Olympus) with excitation at 488 nm and emission at 530 nm. FI was observed in ten randomly selected cells to calculate the average FI for all cells.
Statistical analysis
All data are expressed as the means ± SD. Data were statistically analyzed using one-way analysis of variance (ANOVA) for group comparisons. Student–Newman–Keuls post hoc tests were used when appropriate. A value of P < 0.05 was considered statistically significant.
Results
Losartan significantly reduced apoptosis in CIH-induced endothelial cells in the aortic arches of rats
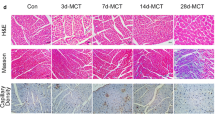
Apoptosis was significantly increased in the aortic arches of rats exposed to CIH (P < 0.05; Fig. 1 ) compared with the control rats. Treatment with losartan or U73122 effectively reduced CIH-induced endothelial apoptosis in the aortic arches of rats exposed to CIH. Addition of both losartan and U73122 had effects similar to the addition of losartan or U73122 alone.
CIH caused endothelial apoptosis in the aortic arches of rats. After 8 weeks of CIH, male SD rats showed a clear evidence of endothelial apoptosis compared with animals exposed to normal oxygen concentrations. Pre-treatment with losartan or U73122 effectively inhibited CIH-induced endothelial apoptosis. Addition of both losartan and U73122 had effects similar to the addition of losartan or U73122 alone. Representative photomicrographs of the TUNEL assay (×400). a Normoxic. b Normoxic + losartan. c Normoxic + U73122. d Normoxic + losartan + U73122. e CIH. f CIH + losartan. g CIH + U73122. h CIH + losartan + U73122. The results represent the means ± SD, with means compared using one-way ANOVA. A value of P < 0.05 is considered statistically significant. *P < 0.05 vs. normoxia; **P < 0.05 vs. CIH
Losartan reduced RAS activation induced by CIH
As shown in Fig. 2, in response to CIH, the concentration of AngII in plasma was significantly higher than in the controls (P < 0.05; Fig. 2a). AGT expression in aortic arches was assayed by real-time quantitative PCR, and CIH resulted in a significant increase in AGT levels compared with those in the controls (P < 0.05; Fig. 2b). CIH also induced a significant increase in AT1R protein levels in aortic arches compared with the controls (P < 0.05; Fig. 2c). Losartan alleviated the levels of AngII, AGT and AT1R; however, U73122 did not change AngII, AGT, and AT1R levels.
Losartan and PLC inhibition abrogated CIH-induced overexpression of ER stress factors
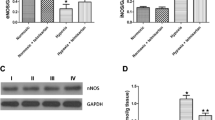
Real-time PCR analysis confirmed that the expression levels of the ER stress-related factors GRP78, CHOP, ATF4, and sXBP1 in the CIH group were increased compared with those in the normal oxygen group (P < 0.05; Fig. 3). In addition, GRP78, caspase12, and CHOP protein expression levels were significantly elevated in the aortic arch after exposure to CIH. We also used immunohistochemistry and immunofluorescence to determine the cellular localization of GRP78, CHOP, and caspase12 in aortic arches of rats. Although this method was not quantitative, we used IPP6 to analyze the integrated optical density (IOD) and found higher levels of GRP78 and caspase12 in the endothelium of the CIH group rats compared with the normal oxygen group. Pre-treatment with losartan or U73122 normalized GRP78, CHOP, ATF4, and sXBP1 mRNA levels (P < 0.05; Fig. 3). Losartan or U73122 also significantly reduced GRP78, CHOP, and caspase12 protein expression (P < 0.05; Figs. 4 and 5). Addition of both losartan and U73122 had effects similar to losartan or U73122 addition alone. The expression of ER stress markers at both the mRNA and protein levels was not modified by losartan addition in the normal oxygen group (Figs. 3, 4, and 5).
The messenger RNA (mRNA) levels of GRP78, sXBP1, ATF4, and CHOP in aortic arch endothelial cells were increased in rats exposed to CIH compared with those in rats exposed to normal oxygen concentrations. Treatment with losartan or U73122 significantly reduced the mRNA expression levels of GRP78, sXBP1, ATF4, and CHOP in aortic arch endothelial cells. Addition of both losartan and U73122 had effects similar to the addition of losartan or U73122 alone. The results represent the means ± SD, with means compared using one-way ANOVA. A value of P < 0.05 is considered statistically significant. *P < 0.05 vs. normoxia; **P < 0.05 vs. CIH
GRP78 and sXBP1 expression in aortic arch endothelial cells was detected with immunohistochemistry. CHOP expression was detected with immunofluorescence. Representative photomicrographs and quantified data are shown. GRP78, caspase12, and CHOP protein expression levels were increased in rats exposed to CIH compared with those in rats exposed to normal oxygen concentrations. Treatment with losartan or U73122 significantly reduced GRP78, caspase12, and CHOP expression in the aortic arches of rats. Addition of both losartan and U73122 had effects similar to the addition of losartan or U73122 alone. a Normoxic. b Normoxic + losartan. c Normoxic + U73122. d Normoxic + losartan + U73122. e CIH. f CIH + losartan. g CIH + U73122. h CIH + losartan + U73122. The results represent the means ± SD, with means compared using one-way ANOVA. A value of P < 0.05 is considered statistically significant. *P < 0.05 vs. normoxia; **P < 0.05 vs. CIH
Quantitative analysis of GRP78, caspase12, and CHOP proteins by Western blot analyses. a Western blot from a representative experiment. b Representative photomicrographs and quantified data are shown. GRP78, caspase12, and CHOP protein expression levels were increased in rats exposed to CIH compared with those in rats exposed to normal oxygen concentrations. Treatment with losartan or U73122 suppressed GRP78, caspase12, and CHOP overexpression induced by CIH. Addition of both losartan and U73122 had effects similar to losartan or U73122 addition alone. The results represent the means ± SD, with means compared using one-way ANOVA. A value of P < 0.05 is considered statistically significant. *P < 0.05 vs. normoxia; **P < 0.05 vs. CIH
Losartan and PLC inhibition suppressed CIH-induced PLC-γ1 and IP3R overexpression
Several studies have demonstrated that the PLC-IP3 pathway can regulate ER stress, which is involved in [Ca2+]i elevation. To further explore the signaling pathway involved in CIH-stimulated ER stress and the effect of losartan, IP3R and PLC-γ1 protein expression levels were examined in the aortic arches of rats. We observed that PLC-γ1 and IP3R protein expression levels were increased in response to CIH compared with those in the controls. Treatment with either losartan or U73122 significantly reduced PLC-γ1 and IP3R levels. Addition of both losartan and U73122 had effects similar to losartan or U73122 addition alone (P < 0.05; Fig. 6).
Effects of CIH and losartan on PLC-γ1 and IP3R expression. PLC-γ1 and IP3R expression levels were significantly increased by CIH. Pre-treatment with losartan or U73122 could reduce PLC-γ1 and IP3R expression. Addition of both losartan and U73122 had effects similar to losartan or U73122 addition alone. The results represent the means ± SD, with means compared using one-way ANOVA. A value of P < 0.05 is considered statistically significant. *P < 0.05 vs. normoxia; **P < 0.05 vs. CIH
Losartan and PLC inhibition protect calcium homeostasis of human aortic endothelial cells from CIH
Calcium signaling plays an important role in regulating nuclear functions, including cell growth and death. Our results revealed that CIH stimulation increased [Ca2+]i. When pretreated with losartan and U73122, CIH did not effectively increase [Ca2+]i, and addition of both losartan and U73122 had effects similar to losartan or U73122 addition alone (P < 0.05; Fig. 7). These results indicated that losartan downregulated the [Ca2+]i elevation induced by CIH by inhibiting the PLC-γ1/IP3/Ca2+ pathway.
Effects of CIH and losartan on intracellular calcium. Human aortic endothelial cells were pre-treated with losartan (5 μM) or U73122 (2 μM) for 30 min and were then exposed to CIH. Intracellular calcium was detected using confocal laser scanning microscopy after Fluo-3/AM staining 1 h after CIH. a Normoxic. b Normoxic + losartan. c Normoxic + U73122. d Normoxic + losartan + U73122. e CIH. f CIH + losartan. g CIH + U73122. h CIH + losartan + U73122. Measurements were performed in triplicate, and values are expressed as the means ± SD (n = 3). *P < 0.05 vs. normoxia; **P < 0.05 vs. CIH
Discussion
Cardiovascular damage is the most common complication of OSAS. However, the pathophysiological mechanisms involved in OSAS-induced cardiovascular damage are poorly understood. Endothelial cell apoptosis constitutes an early and critical element in cardiovascular damage induced by CIH. In the current study, we used a rodent model of CIH to demonstrate that the PLC-IP3-Ca2+ pathway was involved in pathophysiological endothelial apoptosis induced by CIH, and we provide the first evidence that RAS inhibition by losartan preserves the endothelial apoptosis induced by CIH.
AngII, a multifunctional peptide with pleiotropic actions, modulates vasomotor tone, cell growth, apoptosis/anoikis, and cell migration. In a previous study, anoxia-reoxygenation resulted in apoptosis in human coronary artery endothelial cells, and the addition of either AngII or TNF-α significantly increased apoptosis [20]. The intracellular signal transduction pathway triggered by AT1R includes PLC activation and the generation of IP3 and DAG [20], which subsequently leads to the activation of protein kinase C and Ca2+ mobilization from intracellular stores [21]. AngII/AT1R stimulates the PLC-IP3 pathway, resulting in Ca2+ mobilization and consequent contraction [22]. AngII stimulates Ca2+ activity via AT1R-mediated tyrosine phosphorylation of the PLC-γ1 isoform [23]. In this study, we showed that losartan alleviated the levels of AngII, AGT, and AT1R increased by CIH, and for the first time, we described that PLC-γ1 expression in endothelial cells was significantly increased by CIH. Treatment by losartan reduced PLC-γ1 levels in the same manner as the PLC inhibitor U73122, supporting our hypothesis of a direct effect of losartan on the PLC-Ca2 + pathway.
CIH-activated PLC generates IP3, which induces the release of intracellular calcium from the ER via IP3 receptors. We observed that endothelial cells exposed to CIH overexpress IP3R at the protein level, and losartan prevents IP3R overexpression. [Ca2+]i was significantly elevated in rat aortic endothelial cells stimulated by CIH, but it was attenuated by losartan. PLC inhibition mimics the effects of losartan on Ca2+ homeostasis, reinforcing our hypothesis that losartan inhibits the PLC-IP3-Ca2+ pathway.
The ER is a highly dynamic organelle in which newly synthesized secretory and transmembrane proteins are assembled and folded into their correct tertiary structures and thereby plays a critical role in controlling cell fate. The ER is a highly dynamic organelle responsible for multiple cellular functions. However, the ER is highly sensitive to alterations in its homeostasis. Multiple disturbances can cause unfolded protein accumulation in the ER. Aberration of Ca2+ regulation in the ER also contributes to protein unfolding problems due to the Ca2+-dependent nature of chaperones, such as GRP78, GRP94, and calreticulin [24]; these issues trigger an evolutionarily conserved response termed the unfolded protein response (UPR) [25]. The initial intent of the UPR is to re-establish homeostasis and normal ER function. When the adaptive mechanisms put into motion by the UPR fail to compensate—for instance, when the primary stimulus-causing protein unfolding in the ER is protracted or excessive—cell death is induced, typically by apoptosis. ER stress has been implicated in the activation of various death effectors, such as mitochondria [26], caspase12, CHOP, and GADD34. In this study, we showed that the expression levels of ER-associated pro-apoptotic effectors, CHOP and caspase12, were significantly increased, and chronic exposure of rats to CIH resulted in significant ER stress responses, such as the activation of IRE1α/XBP-1, PERK/ATF4, and GRP78/ATF6 pathways. Losartan, by inhibiting AT1R activation, counteracted CIH-induced ER stress, and PLC inhibition would have been sufficient to inhibit ER stress. Various studies have shown that ER stress inhibitors are able to protect endothelial cell apoptosis due to CIH [27]. We show here that losartan and PLC inhibition abrogated ER stress induced by CIH.
Ca2+ homeostasis and ER-regulated functions are essential for appropriate, integrated endothelial cell functions. In our study, we show that both Ca2+ homeostasis and ER function are misregulated in the cases of CIH, resulting in endothelial cell apoptosis. CIH-activated RAS and PLC-IP3-Ca2+ pathways, and the intracellular Ca2+ imbalance induced ER stress and endothelial cell impairment.
For the first time, we demonstrated that losartan directly reduced PLC expression in endothelial cells in the same manner as the selective PLC inhibitor U73122. Losartan reduced endothelial apoptosis partly through the AT1R-PLC-IP3-Ca2+ pathway by preserving the Ca2+ balance and by limiting the ER overactivity induced by CIH.
In summary, this study provided the first evidence that the AngII-PLC-IP3-Ca2+ pathway was involved in ER stress caused by CIH and that losartan could attenuate CIH-induced endothelial apoptosis in part by inhibiting the AngII-PLC-IP3-Ca2+ pathway. The present findings provide novel insights into the mechanisms through which OSAS induces cardiovascular complications. The results of this study may contribute to the development of future therapeutic strategies for OSAS-induced cardiovascular complications. However, it should be noted that our study had some limitations. The use of a PLC agonist would help to clarify the role of PLC-IP3 in contributing to endothelial cell damage in this setting.
References
Gottlieb DJ, Yenokyan G, Newman AB, O’Connor GT, Punjabi NM, Quan SF, Redline S, Resnick HE, Tong EK, Diener-West M, Shahar E (2010) Prospective study of obstructive sleep apnea and incident coronary heart disease and heart failure: the sleep heart health study. Circulation 122:352–360. doi:10.1161/CIRCULATIONAHA.109.901801
Peppard PE, Young T, Palta M, Skatrud J (2000) Prospective study of the association between sleep-disordered breathing and hypertension. N Engl J Med 342:1378–1384. doi:10.1056/NEJM200005113421901
Jean-Philippe Baguet GBRT (2012) Mechanisms of cardiac dysfunction. Cardiology 9:679–688
Marcus NJ, Philippi NR, Bird CE, Li YL, Schultz HD, Morgan BJ (2012) Effect of AT1 receptor blockade on intermittent hypoxia-induced endothelial dysfunction. Respir Physiol Neurobiol 183:67–74. doi:10.1016/j.resp.2012.05.025
de Gasparo M, Catt KJ, Inagami T, Wright JW, Unger T (2000) International union of pharmacology. XXIII. The angiotensin II receptors. Pharmacol Rev 52:415–472
Goldenberg I, Grossman E, Jacobson KA, Shneyvays V, Shainberg A (2001) Angiotensin II-induced apoptosis in rat cardiomyocyte culture: a possible role of AT1 and AT2 receptors. J Hypertens 19:1681–1689. doi:10.1097/00004872-200109000-00022
Vivar R, Soto C, Copaja M, Mateluna F, Aranguiz P, Muñoz JP, Chiong M, Garcia L, Letelier A, Thomas WG, Lavandero S, Díaz-Araya G (2008) Phospholipase C/protein kinase C pathway mediates angiotensin II-dependent apoptosis in neonatal rat cardiac fibroblasts expressing AT1 receptor. J Cardiovasc Pharmacol 52:184–190. doi:10.1097/FJC.0b013e318181fadd
Deliu E, Brailoiu GC, Eguchi S, Hoffman NE, Rabinowitz JE, Tilley DG, Madesh M, Koch WJ, Brailoiu E (2014) Direct evidence of intracrine angiotensin II signaling in neurons. Am J Physiol Cell Physiol 306:C736–C744. doi:10.1152/ajpcell.00131.2013
Zhao Y, Zhang X, Li J, Bian Y, Sheng M, Liu B, Fu Z, Zhang Y, Yang B (2016) Jujuboside B reduces vascular tension by increasing Ca2+ influx and activating endothelial nitric oxide synthase. PLoS One 11:e149386. doi:10.1371/journal.pone.0149386
Rosado JA, Sage SO (2001) Activation of store-mediated calcium entry by secretion-like coupling between the inositol 1,4,5-trisphosphate receptor type II and human transient receptor potential (hTrp1) channels in human platelets. Biochem J 356:191–198
Dietrich A, Kalwa H, Gudermann T (2010) TRPC channels in vascular cell function. Thromb Haemost 103:262–270. doi:10.1160/TH09-08-0517
Jain A, Olovsson M, Burton GJ, Yung HW (2012) Endothelin-1 induces endoplasmic reticulum stress by activating the PLC-IP(3) pathway: implications for placental pathophysiology in preeclampsia. Am J Pathol 180:2309–2320. doi:10.1016/j.ajpath.2012.03.005
Bascands JL, Girolami JP, Troly M, Escargueil-Blanc I, Nazzal D, Salvayre R, Blaes N (2001) Angiotensin II induces phenotype-dependent apoptosis in vascular smooth muscle cells. Hypertension 38:1294–1299. doi:10.1161/hy1201.096540
Rhee SG (2001) Regulation of phosphoinositide-specific phospholipase C. Annu Rev Biochem 70:281–312. doi:10.1146/annurev.biochem.70.1.281
Rebecchi MJ, Pentyala SN (2000) Structure, function, and control of phosphoinositide-specific phospholipase C. Physiol Rev 80:1291–1335
Baumann S, Fas SC, Giaisi M, Müller WW, Merling A, Gülow K, Edler L, Krammer PH, Li-Weber M (2008) Wogonin preferentially kills malignant lymphocytes and suppresses T-cell tumor growth by inducing PLCgamma1- and Ca2+-dependent apoptosis. Blood 111:2354–2363. doi:10.1182/blood-2007-06-096198
Watanabe T, Suzuki J, Yamawaki H, Sharma VK, Sheu SS, Berk BC (2005) Losartan metabolite EXP3179 activates Akt and endothelial nitric oxide synthase via vascular endothelial growth factor receptor-2 in endothelial cells: angiotensin II type 1 receptor-independent effects of EXP3179. Circulation 112:1798–1805. doi:10.1161/CIRCULATIONAHA.104.509760
Li D, Yang B, Philips MI, Mehta JL (1999) Proapoptotic effects of ANG II in human coronary artery endothelial cells: role of AT1 receptor and PKC activation. Am J Phys 276:H786–H792
Hou C, Kirchner T, Singer M, Matheis M, Argentieri D, Cavender D (2004) In vivo activity of a phospholipase C inhibitor, 1-(6-((17beta-3-methoxyestra-1,3,5(10)-trien-17-yl)amino)hexyl)-1H-pyrrole-2,5-dione (U73122), in acute and chronic inflammatory reactions. J Pharmacol Exp Ther 309:697–704. doi:10.1124/jpet.103.060574
Kathy K, Griendling SERT, Michael A, JARW G (1986) Sustained diacylglycerol formation from inositol phospholipids in angiotensin 11-stimulated vascular smooth muscle cells. J Biol Chem 261:5901–5906
Catt KJ, Balla T, Baukal AJ, Hausdorff WP, Aguilera G (1988) Control of glomerulosa cell function by angiotensin II: transduction by G-proteins and inositol polyphosphates. Clin Exp Pharmacol Physiol 15:501–515. doi:10.1111/j.1440-1681.1988.tb01108.x
Touyz RM (2005) Intracellular mechanisms involved in vascular remodelling of resistance arteries in hypertension: role of angiotensin II. Exp Physiol 90:449–455. doi:10.1113/expphysiol.2005.030080
Lea JP, Jin SG, Roberts BR, Shuler MS, Marrero MB, Tumlin JA (2002) Angiotensin II stimulates calcineurin activity in proximal tubule epithelia through AT-1 receptor-mediated tyrosine phosphorylation of the PLC-gamma1 isoform. J Am Soc Nephrol 13:1750–1756. doi:10.1097/01.ASN.0000022029.50356.2C
Ma Y, Hendershot LM (2004) ER chaperone functions during normal and stress conditions. J Chem Neuroanat 28:51–65. doi:10.1016/j.jchemneu.2003.08.007
Ron D, Walter P (2007) Signal integration in the endoplasmic reticulum unfolded protein response. Nat Rev Mol Cell Biol 8:519–529. doi:10.1038/nrm2199
Wei MC, Zong WX, Cheng EH, Lindsten T, Panoutsakopoulou V, Ross AJ, Roth KA, MacGregor GR, Thompson CB, Korsmeyer SJ (2001) Proapoptotic BAX and BAK: a requisite gateway to mitochondrial dysfunction and death. Science 292:727–730. doi:10.1126/science.1059108
Yang YY, Shang J, Liu HG (2013) Role of endoplasmic reticular stress in aortic endothelial apoptosis induced by intermittent/persistent hypoxia. Chin Med J Peking 126:4517–4523. doi:10.3760/cma.j.issn.0366-6999.20130602
Acknowledgements
This study was funded by the National Natural Science Foundation of China (grants 81570080 and 81370185).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethical standards
The manuscript does not contain clinical studies or patient data.
Conflict of interest
The authors declare that they have no competing interests.
Ethical approval
All applicable international, national, and/or institutional guidelines for the care and use of animals were followed.
Rights and permissions
About this article
Cite this article
Ren, J., Liu, W., Deng, Y. et al. Losartan attenuates aortic endothelial apoptosis induced by chronic intermittent hypoxia partly via the phospholipase C pathway. Sleep Breath 21, 679–689 (2017). https://doi.org/10.1007/s11325-017-1479-4
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11325-017-1479-4