Abstract
Medical therapies are an important part of adjunctive therapy for gliomas. In this chapter we will review the chemotherapeutic and targeted agents that have been evaluated in clinical trials in grade II–IV gliomas in the last decade. A number of randomized phase III trials were completed and reported. There has been a clear success in oligodendroglial tumors and low grade glioma. Although some progress has been made in glioblastoma, considerable work involving the multidisciplinary collaboration of basic science, translational and clinical investigators needs to be done to improve the outcome of patients with anaplastic astrocytoma and glioblastoma. In addition, tailoring treatment based on molecular cytogenetic characteristics is a major focus of research into precision based medicine for glioma.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The challenges that limit the therapeutic efficacy of chemotherapy and targeted therapies in gliomas include the blood–brain barrier (BBB), active transport mechanisms of drug efflux, and high plasma protein binding of agents [1]. In addition to the difficulty of delivery of agents across the BBB, there are other challenges that limit the efficacy of these agents. Other challenges include heterogeneity of tumors, redundancy of pathway interactions, lack of accurate and reproducible biomarkers to select patients for specific therapies, and difficulty in assessing target modulation [2–4]. Intrinsic and rapidly acquired resistance further limit the efficacy of chemotherapy or targeted therapy. Chemotherapeutic approaches have demonstrated efficacy in oligodendroglioma. For several chemotherapy-refractory tumor types including glioblastoma and anaplastic astrocytoma, new approaches continue to be explored and will be reviewed. Finally, the future directions involving precision medicine approaches to optimize the therapeutic index of drug treatments for glioma will be discussed.
Low grade gliomas (WHO grade II)
Until recently, low-grade gliomas were considered to be chemotherapy resistant and there have been limited trials evaluating the utility of chemotherapy in low-grade glioma in adults. In a small Southwest Oncology Group trial, patients with incompletely excised low-grade gliomas were randomized to radiation therapy (RT) alone or combination of RT and lomustine (CCNU). The survival in both the two arms was similar [5]. Radiation Therapy Oncology Group (RTOG) study, RTOG-9802 examined the role of adjuvant chemotherapy—procarbazine, CCNU, and vincristine (PCV) for “high-risk” adults (less than total resection, age older than 40 years) with low-grade gliomas. Two hundred and fifty-one patients were randomized to RT alone or RT followed by six cycles of PCV. Progression-free survival (PFS) but not overall survival (OS) was improved in the RT and the PCV group compared to RT alone at the time of the initial data analysis [6]. At the time of that report however 65 % of the patients were still alive. A recent National Institute of Health press release on more mature results of this study reported significant improvement in OS in the PCV chemotherapy plus RT arm (13.3 years) compared to those assigned to RT alone (7.8 years) at a median follow-up of 12 years [7]. Correlative studies to establish the predictive role of molecular and cytogenetic characteristics [isocitrate dehydrogenase (IDH) mutations, loss of heterozygosity of 1p/19q, as well as methylation of methylguanine methyl transferase (MGMT) status] clinical outcome are pending.
The first results from the RTOG 0424 study demonstrated the improved 3-year OS of a regimen of concurrent and adjuvant temozolomide (TMZ) and radiotherapy in a high-risk low-grade glioma population compared to the 3 year OS rate of the high risk EORTC LGG patients reported by Pignatti et al. [8]. The 3 year OS rate was 73.1 % (95 % CI 65.3–80.8 %), significantly improved in comparison to the pre-specified historical control (p value <0.0001) [9]. There is an ongoing intergroup phase III trial to address the role of adjunctive TMZ for LGG.
Several studies have evaluated PCV and TMZ in recurrent low grade gliomas [10–21]. Approximately half the patients treated with either TMZ or PCV experienced imaging stability or improvement of neurologic symptoms in these studies. The limitations of these studies include small numbers and the varied imaging criteria used to assess response. Patients with low-grade oligodendroglial tumors with 1p/19q deletion or t(1p; 19q) have longer PFS and OS than those without [22] and consequently, 1p/19q determination is important in stratification in future clinical trials. A randomized phase III EORTC trial stratified patients with low-grade glioma by 1p status prior to randomization to RT versus TMZ alone [23]. In the first report of the trial, PFS was similar in both groups while median OS was not reached. This study showed 1p deletion as a positive prognostic factor irrespective of treatment at the time of this first analysis [PFS 0.0003; HR 0.59, 95 % CI (0.45–0.78); OS 0.002; HR 0.49, 95 % CI (0.32–0.77)].
Recent studies have identified alterations in the BRAF serine/threonine kinase gene as the likely causative mutation in childhood LGG and approaches to target this abnormality are being explored [24]. In addition, aberrant signaling in pathways including the phosphatidyl inositol-3-kinase (PI3K)/AKT/mammalian target of rapamycin (mTOR) network [25, 26] have also been identified in LGG and clinical trials are currently ongoing to target this pathway as a therapeutic approach.
In addition to the known side effects of myelosuppression from the use of alkylating agents, there may be adverse effects on the mutational landscape of tumors following this known mutagenic treatment. Johnson et al. [27] reported on a group of patients with grade II astrocytoma for whom tumor tissue was available for genomic analysis at the time of initial diagnosis and at the time of progression. They demonstrated the potential for TMZ to induce specific driver mutations that could contribute to the malignant transformation of grade II astrocytoma to glioblastoma. It is unclear which subset of patients is at specific risk for this mutagenic effect of TMZ.
Anaplastic oligodendrogliomas (WHO grade III)
Several retrospective series and phase II trials suggested chemosensitivity of oligodendrogliomas [12, 28, 29]. Two randomized prospective phase III trials evaluated the role of chemotherapy in this tumor type and patients were treated with either RT alone or RT in combination with PCV. In the RTOG-9402 trial, patients were randomized to either four cycles of intensified PCV followed by RT or immediate RT without chemotherapy. At initial report, survival in the two groups was the same and patients with 1p/19q deletions had significantly better outcomes, regardless of type of treatment [30]. A posthoc analysis showed that there was a PFS benefit from PCV that was most notable in patients with 1p/19q deletions. With over 11 years follow-up, mature data from this study showed that median survival of those with co-deleted tumors treated with PCV plus RT was twice that of patients receiving RT (14.7 vs. 7.3 years) [31]. The survival of patients with co-deleted tumors was better than those with non-co-deleted tumors regardless of treatment. The survival was not statistically significant for patients with tumors lacking 1p/19q deletion irrespective of treatment (median survival 2.6 vs. 2.7 years).
In the EORTC 26951 trial, 368 patients received immediate RT only or RT followed by six cycles of PCV [32]. Samples from 86 % of patients were available for analysis for 1p/19q codeletion. At the time of first report, the PFS was better in the PCV group, but OS was similar. Patients with 1p/19q deletion had better outcomes, irrespective of therapy. In addition, MGMT promoter methylation was of prognostic value in this cohort [33, 34]. Long-term follow up in patients with the 1p/19q codeletion showed that the addition of PCV to RT significantly increased PFS (median 157 vs. 50 months) and there was a trend toward increase in OS (OS not reached in the RT/PCV group vs. 112 months in the RT group HR 0.56; 95 % CI 0.31–1.03) [35].
Temozolomide has produced high response rates in patients with anaplastic oligodendroglioma. In 27 newly diagnosed patients treated with TMZ prior to radiotherapy the objective response rate was 33 % and the 6-month progression rate was 10 % [36]. An international intergroup trial is being conducted in patients with newly diagnosed grade III glioma with 1p/19q status codeletion (NCT00887146). Patients are randomized to three arms, TMZ alone (phase II group); or radiotherapy with concomitant and adjuvant TMZ or radiotherapy with adjuvant procarbazine, lomustine and vincristine (PCV) (phase III).
Chemotherapy for recurrent anaplastic oligodendroglioma
Both PCV and TMZ have activity in patients that recur after radiotherapy although generally response rates are lower and the duration of disease control is shorter. The activity of TMZ was seen in a study of 48 patients with anaplastic oligodendroglioma/oligoastrocytoma who progressed on PCV [37]. The objective response rate was 44 %, including 17 % who achieved complete remission. The median PFS was 7 months and the median OS was 10 months. Although there is no direct comparison of TMZ and PCV to determine which regimen is superior in terms of efficacy, the absence of cumulative myelosuppression with TMZ makes it the preferred choice in the setting of recurrent disease.
Anaplastic astrocytoma (WHO grade III)
The role of chemotherapy in anaplastic astrocytoma is not well established. Most phase III trials have demonstrated no benefit of chemotherapy compared with radiation alone in this tumor type. Carmustine and PCV are associated with minimal improvement in survival [38]. The Glioma Meta-Analysis Trialists’ group showed a 6 % increase in 1- and 2-year survival for patients who received chemotherapy (2-year survival of 37 vs. 31 %) in a meta-analysis [39]. A large randomized trial of adjuvant PCV compared with RT alone did not show any benefit of adjuvant PCV [40]. The RTOG-9813 was a phase III study comparing radiation with BCNU or CCNU to radiation with TMZ, and the results of this study are pending.
The NOA-04 phase III trial compared the efficacy of RT followed by chemotherapy at progression, to initial chemotherapy followed by RT at progression, in newly diagnosed anaplastic gliomas [41]. Patients received conventional RT, PCV or TMZ as initial therapy. At disease progression or occurrence of unacceptable toxicity, patients in the RT arm received PCV or TMZ, whereas patients in chemotherapy arms were treated with RT. Median time to failure, PFS and OS were similar in all the treatment arms. Methylguanine DNA-methyltransferase (MGMT) promoter methylation and IDH1 mutations were included in the correlative part of the study due to their prognostic value [42–44]. Patients with hypermethylation of the MGMT promoter had prolonged PFS both in the RT and the chemotherapy arm. Hypermethylation of MGMT promoter, IDH1 mutations and oligodendroglioma histology was associated with a decreased risk of progression. The study demonstrated the prognostic value of IDH1 mutations in anaplastic gliomas, with a favorable impact that was more significant than that of 1p/19q codeletion or MGMT promoter methylation [41].
A large international trial, CATNON is being conducted in patients with newly diagnosed grade III glioma stratified by 1p/19q status. Nondeleted patients are randomized to radiation with or without TMZ; following radiotherapy there is a second randomization to adjuvant TMZ or not.
Chemotherapy for recurrent anaplastic astrocytomas
Studies of both nitrosourea-based approaches and TMZ have demonstrated efficacy in recurrent anaplastic astrocytomas. A study of TMZ in recurrent anaplastic astrocytoma demonstrated a response rate of 35 % for patients who were chemotherapy naive and 20 % for patients who had received nitrosourea-based therapy [45]. This led to accelerated approval for TMZ by the US Food and Drug Administration. Based on activity of bevacizumab in recurrent glioblastoma, it is often used in patients with recurrent anaplastic astrocytoma [46]. A retrospective study reported a 64 % radiographic response and 6-month PFS rate of 60 % in 25 patients [47].
Glioblastoma (WHO grade IV)
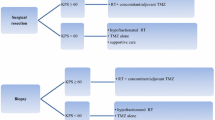
Over the last decade there were a considerable number of investigational studies performed and reported in patients with glioblastoma. In a landmark study of approximately 600 patients, patients were randomized to RT alone (60 Gy in daily 30 fractions) or in combination with concurrent TMZ (75 mg/m2 daily up to 49 days) and followed by up to six cycles of adjuvant TMZ (150–200 mg/m2 daily for 5 days, every 28 days). There was statistically significant increase in OS in the combination arm compared with RT alone [27 vs. 11 % at 1 year, hazard ratio (HR) for death 0.63] [48]. Median and 2-year survival was increased by 2.5 months and 16.1 %, respectively [48]. This study provided level 1 evidence favoring use of TMZ for patients with newly diagnosed glioblastoma (Table 1). Accompanying correlative study demonstrated that methylation of the promoter region of the MGMT gene in the tumor was associated with superior survival, regardless of treatment received, but the benefit was primarily seen in methylated patients [42]. The 2-year survival rates were 49 and 24 % with combination therapy and with RT alone, respectively, in patients with MGMT methylation. The 2-year survival rates were 15 and 2 %, respectively in those without MGMT methylation. Preclinical work suggested that different prolonged schedule of TMZ may overcome chemotherapy resistance that led to studies looking at alternative dosing of TMZ in the newly diagnosed setting and at the time of recurrence [49, 50]. A large phase III randomized international study led by the RTOG compared the standard treatment versus a 21- or 28-day adjuvant TMZ schedule [51]. Dose-dense TMZ failed to result in improved efficacy regardless of tumor methylation status but was associated with more profound lymphopenia and fatigue. Strategies to increase the therapeutic ratio of existing chemotherapies, such as the inhibition of DNA repair enzymes [i.e., poly[ADP-ribose] polymerase (PARP) or base excision repair] are being evaluated. These agents are being combined with radiation and chemotherapy to increase the cytotoxicity of the combination approach [52–54].
The evaluation of chemotherapy in the elderly glioblastoma patient has been the focus of several recent trials. More than half of all patients with GBM are aged 65 years or older at the time of diagnosis, and the incidence rate of GBM in patients aged over 65 years is increasing rapidly. In addition, age is a well-known prognostic factor in this disease and the median survival for elderly GBM patients is <6 months. The use of chemotherapy for elderly GBM patients remains controversial and several factors should be considered including age, MGMT methylation status, performance score, medical co-morbidities and patient preferences. Concurrent and adjuvant TMZ along with RT to 60 Gy have not been prospectively studied among patients aged over 70 years but should be considered for patients aged 65–70 years with excellent KPS [48]. Several approaches to shorten the duration of radiation (hypofractionated radiation) or to use chemotherapy alone have been evaluated. Based on recent randomized trials, testing for O6-methylguanine-DNA-methyltransferase (MGMT) promoter methylation should be performed routinely immediately after surgery to aid in adjuvant treatment decisions [55, 56]. For patients aged over 70 years with favorable KPS, or patients aged 60–70 years with borderline KPS, monotherapy utilizing standard TMZ dosing for patients with MGMT-methylated tumors, and hypofractionated RT (34 Gy in ten fractions or 40 Gy in 15 fractions) for patients with MGMT-unmethylated tumors should be considered. For elderly patients with poor KPS, reasonable options include best supportive care, TMZ alone or hypofractionated RT alone [55–57]. The role of concurrent TMZ with hypofractionated RT is being evaluated in an ongoing European Organization for Research and Treatment of Cancer/National Cancer Institute of Canada trial.
Targeted therapies for glioblastoma including anti-angiogenic approaches
The last decade has witnessed considerable progress being made in the understanding of the genetic and molecular pathogenesis of gliomas. This has in turn led to the identification of new potential therapeutic targets and the development of signaling pathway modulators.
Glioblastoma is a highly vascular tumor that is dependent on microvascular proliferation for survival and research into angiogenesis and its blockade have been among the top priorities in the last decade. The most important mediator of angiogenesis in glioblastoma is vascular endothelial growth factor (VEGF). Two trials, the BRAIN study and the NCI study showed that treatment with the anti-VEGF monoclonal antibody bevacizumab resulted in dramatic radiological responses and prolonged PFS relative to historical controls [58, 59]. Based on the response rates seen in the BRAIN study, which was a randomized noncomparative phase II study of 167 patients who were treated with bevacizumab alone or with irinotecan, and the NCI led single arm phase II study of bevacizumab alone, the US Food and Drug Administration granted accelerated approval to bevacizumab for recurrent glioblastoma in 2009 [46]. The PFS at 6 months was 43 and 50 % for bevacizumab alone and the combination arm in the BRAIN study respectively. The objective response rates were 28 and 38 % for the two arms and the OS was 9.2 and 8.7 months, respectively. The NCI study demonstrated a PFS at 6 months of 29 % and a radiographic response rate of 35 % with bevacizumab. The most common side effects associated with bevacizumab include fatigue, headache, and hypertension. A number of studies have examined whether additional chemotherapy or targeted therapy to bevacizumab translates into additional efficacy compared to bevacizumab alone. A Phase II trial (CABARET) evaluated the efficacy of adding carboplatin to bevacizumab in recurrent glioblastoma. The PFS at 6 months was 26 % and OS was 6.9 months for the combination versus 6-month PFS of 24 % and OS of 6.4 months for bevacizumab alone [60]. The addition of chemotherapy or targeted therapy has failed to show any added benefit in recurrent GBM trials with the exception of the BELOB study. In the BELOB study, a three-arm multicenter randomized phase II study, 148 recurrent glioblastoma patients received bevacizumab alone, lomustine alone or the combination of the two. OS at 9 months was 38, 43 and 59 % and the PFS-6 was 16, 13 and 41 % in the three arms respectively [61]. EORTC 26101 will assess the role of bevacizumab and lomustine versus lomustine alone in a randomized phase III trial in recurrent GBM.
The benefit of bevacizumab in recurrent glioblastoma prompted its evaluation in the treatment of newly diagnosed glioblastoma. There are several small single-arm phase II studies of the combination of bevacizumab with radiation and TMZ in the newly diagnosed setting [62]. Two large randomized trials evaluated the benefit of addition of bevacizumab to RT and TMZ. The first study, RTOG 0825 was a randomized, double-blinded, placebo controlled trial and was conducted primarily in the United States. In this study the addition of bevacizumab resulted in longer PFS that did not reach the preset level of significance (10.7 vs. 7.3 months, HR 0.79). There was no difference in OS between two arms (16.1 vs. 15.7 months, HR 1.13) [63]. The AVAglio study was an industry-sponsored, international, multicenter Phase III placebo-controlled randomized trial in newly diagnosed glioblastoma [64]. This study demonstrated that the addition of bevacizumab to RT and TMZ produced a clinically meaningful and statistically significant improvement in PFS (HR 0.64, p < 0.0001; median 10.6 vs. 6.2 months) as compared to RT and TMZ. However similar to the RTOG 0825 there was no difference in median survival (16.7 months for the placebo group; 16.8 months for the bevacizumab group. HR 0.88, p = 0.0987).
The open-label GLARIUS trial was a randomized, multicenter study of MGMT-nonmethylated GBM. The patients were randomized in a 2:1 manner to receive bevacizumab during RT that was followed by maintenance bevacizumab and irinotecan compared to standard therapy of 6 weeks of concurrent RT and TMZ followed by 6 cycles of adjuvant TMZ [65]. Preliminary results of this study demonstrated a PFS-6 rate of 71.1 % in the experimental arm compared to 26.2 % in the control arm (p < 0.0001 log rank test). Final results are pending.
Despite improvement in PFS, there has been no benefit in OS with bevacizumab possibly due to resistance that can be due to intrinsic or acquired (evasive) mechanisms. Hence a number of strategies have tested combination of bevacizumab with other targeted agents, or evaluating agents that target other antiangiogenic pathways such as platelet-derived growth factor (PDGF), integrins or hepatocyte growth factor (HGF). Despite promising results in a phase II study of cediranib (AZD2171), an orally administered pan-VEGF receptor inhibitor [66], a Phase III randomized trial (REGAL) that compared the efficacy of cediranib either as monotherapy or in combination with lomustine failed to show any improvement in PFS compared to lomustine alone in recurrent GBM [67] (Table 2). VEGF Trap (aflibercept) in a phase II study showed minimal evidence of single-agent activity in unselected patients with recurrent malignant glioma [68].
Cilengitide is a cyclic pentapeptide that selectively competitively inhibits the aVb3 and aVb5 integrins and has antiangiogenic properties [69, 70]. Cilengitide showed initial promise in recurrent GBM studies that led to its evaluation in two large newly diagnosed studies [69, 70]. The CORE study evaluated the efficacy of cilgentide in the unmethylated MGMT gene promoter in a multicenter, randomized phase II trial. The study showed a median OS of 16.3 months in the cilengitide arm compared to a median OS of 13.4 months in the control-group (HR 0.69; p = 0.033). The CENTRIC study was a phase III trial that looked at the benefit of cilengitide combined with RT and TMZ for newly diagnosed glioblastoma with MGMT promoter methylation [71]. The study failed to show any additional benefit of cilengitide in this patient population [71]. Median OS was 26.3 months in both arms and median PFS was 13.5 months in the cilengitide arm and 10.7 months in the control arm (p = 0.87). This drug is not being further developed.
The other antiangiogenic agents that have undergone investigation in recurrent glioblastoma include multi-targeted tyrosine kinase inhibitors such as sunitinib, sorafenib, cabozantinib and enzastaurin, an inhibitor of protein kinase C-beta that targets VEGF, as well as the mTOR pathway [72]. The outcomes of the studies with these agents have been similar or inferior compared to those seen with bevacizumab [72–74].
The EGFR pathway can be dysregulated in up to 40 % of glioblastoma and number of phase I and II trials of erlotinib and gefitinib for recurrent high-grade gliomas evaluated the efficacy of these agents. However, the results of most of these trials were disappointing and showed limited activity for these agents [75–78]. There were reports that tumors with the variant 3 mutant (EGFRvIII), with resulting constitutive activation of EGFR tyrosine kinase activity, along with intact phosphatase and tensin analogue (PTEN) may be more responsive to EGFR inhibitors [79]. Two studies adding erlotinib to RT and TMZ for newly diagnosed glioblastoma did not show an improvement in survival [80, 81]. The cooperative group study, RTOG 0211 evaluated the benefit of RT with concurrent gefitinib and did not show an improvement in survival [82]. Irreversible EGFR inhibitor, afatinib did not show clinical benefit either alone or in combination with TMZ in patients with recurrent GBM [83]. There is an ongoing phase II study with dacomitinib, a second-generation EGFR inhibitor, in patients with recurrent glioblastoma.
Clinical trials of other targeted agents including the mTOR inhibitors everolimus and temsirolimus, and the farnesyl transferase inhibitor, tipifarnib, have shown limited efficacy in recurrent high-grade gliomas [84–88]. Studies using epigenetic modulation through histone deacetylase inhibitors and the proteasome inhibitor bortezomib have revealed minimal efficacy of these approaches [89, 90].
The future of medical treatment of gliomas
Precision medicine
As treatment for gliomas evolve in the ensuing years, studying the biological behavior of these tumors in the context of therapeutic options is increasingly important. Precision therapy that is tailor-made treatment around the molecular evolution of these tumors will require employment of high-throughput genomic technology in the clinical setting. The brain tumor centers of excellence will need to institute effective workflow that encompass tissue collection after surgery, proper as well as prompt processing, and standardization of biomaterial extraction. The tissue will require sequencing (combination of targeted capture sequencing, whole genome sequencing, and RNA sequencing), and data analysis that will lead to therapeutic recommendations for each individual will be a critical component to translate the information to the clinical management of the patient. The genomic profiling can not only inform diagnosis and but alter treatment approach as more targeted agents are available in the future.
Molecular characterization of the gliomas
The recent molecular characterization of gliomas has clarified a framework of different subtypes of these tumors and has revealed pathways that will help the development of more effective targeted therapies. The diagnosis of gliomas in the past was based on a complete clinicopathological assessment. Although this is a valuable approach that permits the distinction of different grades within categories of the same tumor type, such as astrocytomas, that may predict clinical outcome, it does not address the issue that distinct genetic subgroups may exist within each grade.
In recent years there has been extensive work in large-scale gene expression profile studies in glioblastoma to characterize the molecular subtypes of GBM that include a report of the Cancer Genome Atlas Research Network [91]. These genomic analyses provided insights underlying tumor biology that further classify different subtypes that may inform treatment plans, impact patient outcome, and improve response to treatment [92, 93]. Verhaak et al. [93] classified glioblastoma into proneural, neural, classical, and mesenchymal subtypes based on gene expression profiles of these tumors. Aberrations and differential gene expression of EGFR, NF1, and PDGFRA/IDH1 help define the various subtypes and these pathways can be targeted using novel therapies. The work in genome and transcriptome shows that glioblastoma is a heterogeneous tumor with multiple redundant pathways and distinct subtypes [94].
Considerable research in genetic alterations in WHO grade II astrocytoma in adults has shown the role of inactivation of the TP53 tumor suppressor gene, heterozygous point mutations of the IDH1, and loss of chromosome 22q in these tumors. TP53 on chromosome 17p encodes the p53 protein that has an important role in a numerous cellular processes, including apoptosis, cell cycle arrest, and response to DNA damage [95]. Somatic mutations in IDH1 are present in 50–80 % of WHO grade II and III astrocytic tumors and oligodendroglial tumors in adults and up to 5 % of the secondary glioblastomas [44, 96]. These mutations lead to conversion of α-ketoglutarate into D-2-hydroxyglutarate, an oncometabolite that drives the oncogenic activity of IDH mutations [97]. Patient with tumors with IDH mutations have better outcomes than do IDH-wild-type gliomas of the same histological grade [98, 99]. Recent discoveries of pathogenic mutations in IDH1 [97], IDH2, ATRX [100], CIC [101], and FUBP1 [101], have helped genomic characterization of low grade gliomas. These mutations form the framework of molecular pathogenesis of these tumors and offers robust markers that not only enhance classification but also guide treatment. Common cytogenetic alteration in oligodendroglial histology consists of an unbalanced t(1;19)(q10;p10) translocation that results in combined loss of chromosomal arms 1p/19q and leads to the loss of one hybrid chromosome and thus loss of heterozygosity [22]. Tumors with 1p/19q-codeletions have a better prognosis than do histologically identical tumors of the same grade that do not harbor this codeletion [102]. The key to successful treatment of these tumors will lie in the realization that these molecularly defined subsets are different disease entities and it is likely that specific targeted therapies aimed at the driver mutations will be more likely to be efficacious. In the future, the molecular classification of these tumors will be performed routinely and be defined in clinically relevant terms based on the identification of markers that define subsets and guide therapeutic options.
The next 10 years
The advances in imaging, improved targeted therapeutic options, and routine availability of molecular characterization of tumors will enhance glioma management in the next decade. A great deal of progress has been made in the last decade in the understanding of the molecular mechanisms of gliomas. The continuation of these efforts may further classify the subtypes of tumors of the same grade and warrant different therapeutic options for the patients. Accelerated developments of new drugs will likely aid improvements in therapeutic outcomes in the next 10 years. Given the complex network of pathways involved, one approach would be the use of multitargeted therapy that simultaneously aims at different constitutive pathways driving the malignancy. Further developments in drug delivery will play a key role in translating this into improved patient outcomes. While the next decade appears to be promising, considerable work involving the multidisciplinary collaboration of basic science, translational and clinical investigators will need to be done to improve the outcome of patients with gliomas.
References
Muldoon LL, Soussain C, Jahnke K et al (2007) Chemotherapy delivery issues in central nervous system malignancy: a reality check. J Clin Oncol 25:2295–2305
Omuro AM, Faivre S, Raymond E (2007) Lessons learned in the development of targeted therapy for malignant gliomas. Mol Cancer Ther 6:1909–1919
Chang SM, Lamborn KR, Kuhn JG et al (2008) Neurooncology clinical trial design for targeted therapies: lessons learned from the North American brain tumor consortium. Neuro-Oncology 10:631–642
Huang TT, Sarkaria SM, Cloughesy TF, Mischel PS (2009) Targeted therapy for malignant glioma patients: lessons learned and the road ahead. Neurotherapeutics 6:500–512
Shaw EG, Wisoff JH (2003) Prospective clinical trials of intracranial low-grade glioma in adults and children. Neuro-Oncology 5:153–160
Shaw EG, Wang M, Coons SW et al (2012) Randomized trial of radiation therapy plus procarbazine, lomustine, and vincristine chemotherapy for supratentorial adult low-grade glioma: initial results of RTOG 9802. J Clin Oncol 30:3065–3070
Buckner JC, Pugh SL, Shaw EG (2014) Phase III study of radiation therapy (RT) with or without procarbazine, CCNU, and vincristine (PCV) in low grade gliomas: RTOG 9802 with Alliance, ECOG, and SWOG. ASCO meeting abstracts 32:2001
Pignatti F, van den Bent M, Curran D et al (2002) Prognostic factors for survival in adult patients with cerebral low-grade glioma. J Clin Oncol 20:2076–2084
Fisher BJ, Lui J, Macdonald DR et al (2013) A phase II study of a temozolomide-based chemoradiotherapy regimen for high-risk low-grade gliomas: preliminary results of RTOG 0424. ASCO meeting abstracts 31:2008
Hoang-Xuan K, Capelle L, Kujas M et al (2004) Temozolomide as initial treatment for adults with low-grade oligodendrogliomas or oligoastrocytomas and correlation with chromosome 1p deletions. J Clin Oncol 22:3133–3138
Quinn JA, Reardon DA, Friedman AH et al (2003) Phase II trial of temozolomide in patients with progressive low-grade glioma. J Clin Oncol 21:646–651
van den Bent MJ, Taphoorn MJ, Brandes AA et al (2003) Phase II study of first-line chemotherapy with temozolomide in recurrent oligodendroglial tumors: the European Organization for Research and Treatment of Cancer Brain Tumor Group Study 26971. J Clin Oncol 21:2525–2528
Pace A, Vidiri A, Galie E et al (2003) Temozolomide chemotherapy for progressive low-grade glioma: clinical benefits and radiological response. Ann Oncol 14:1722–1726
Soffietti R, Ruda R, Bradac GB, Schiffer D (1998) PCV chemotherapy for recurrent oligodendrogliomas and oligoastrocytomas. Neurosurgery 43:1066–1073
Stege EM, Kros JM, de Bruin HG et al (2005) Successful treatment of low-grade oligodendroglial tumors with a chemotherapy regimen of procarbazine, lomustine, and vincristine. Cancer 103:802–809
Lebrun C, Fontaine D, Bourg V et al (2007) Treatment of newly diagnosed symptomatic pure low-grade oligodendrogliomas with PCV chemotherapy. Eur J Neurol 14:391–398
Buckner JC, Gesme D Jr, O’Fallon JR et al (2003) Phase II trial of procarbazine, lomustine, and vincristine as initial therapy for patients with low-grade oligodendroglioma or oligoastrocytoma: efficacy and associations with chromosomal abnormalities. J Clin Oncol 21:251–255
van den Bent MJ, Chinot O, Boogerd W et al (2003) Second-line chemotherapy with temozolomide in recurrent oligodendroglioma after PCV (procarbazine, lomustine and vincristine) chemotherapy: EORTC Brain Tumor Group phase II study 26972. Ann Oncol 14:599–602
Brada M, Viviers L, Abson C et al (2003) Phase II study of primary temozolomide chemotherapy in patients with WHO grade II gliomas. Ann Oncol 14:1715–1721
Murphy PS, Viviers L, Abson C et al (2004) Monitoring temozolomide treatment of low-grade glioma with proton magnetic resonance spectroscopy. Br J Cancer 90:781–786
Pouratian N, Gasco J, Sherman JH, Shaffrey ME, Schiff D (2007) Toxicity and efficacy of protracted low dose temozolomide for the treatment of low grade gliomas. J Neurooncol 82:281–288
Jenkins RB, Blair H, Ballman KV et al (2006) A t(1;19)(q10;p10) mediates the combined deletions of 1p/19q and predicts a better prognosis of patients with oligodendroglioma. Cancer Res 66:9852–9861
Baumert BG, Mason WP, Ryan G et al (2013) Temozolomide chemotherapy versus radiotherapy in molecularly characterized (1p loss) low-grade glioma: a randomized phase III intergroup study by the EORTC/NCIC-CTG/TROG/MRC-CTU (EORTC 22033-26033). ASCO meeting abstracts 31:2007
Chen YH, Gutmann DH (2014) The molecular and cell biology of pediatric low-grade gliomas. Oncogene 33:2019–2026
Wiencke JK, Zheng S, Jelluma N et al (2007) Methylation of the PTEN promoter defines low-grade gliomas and secondary glioblastoma. Neuro-Oncology 9:271–279
McBride SM, Perez DA, Polley MY et al (2010) Activation of PI3K/mTOR pathway occurs in most adult low-grade gliomas and predicts patient survival. J Neurooncol 97:33–40
Johnson BE, Mazor T, Hong C et al (2014) Mutational analysis reveals the origin and therapy-driven evolution of recurrent glioma. Science 343:189–193
Cairncross JG, Macdonald DR (1988) Successful chemotherapy for recurrent malignant oligodendroglioma. Ann Neurol 23:360–364
Cairncross G, Macdonald D, Ludwin S et al (1994) Chemotherapy for anaplastic oligodendroglioma. National Cancer Institute of Canada Clinical Trials Group. J Clin Oncol 12:2013–2021
Cairncross G, Berkey B, Shaw E et al (2006) Phase III trial of chemotherapy plus radiotherapy compared with radiotherapy alone for pure and mixed anaplastic oligodendroglioma: intergroup radiation therapy oncology group trial 9402. J Clin Oncol 24:2707–2714
Cairncross G, Wang M, Shaw E et al (2013) Phase III trial of chemoradiotherapy for anaplastic oligodendroglioma: long-term results of RTOG 9402. J Clin Oncol 31:337–343
van den Bent MJ, Carpentier AF, Brandes AA et al (2006) Adjuvant procarbazine, lomustine, and vincristine improves progression-free survival but not overall survival in newly diagnosed anaplastic oligodendrogliomas and oligoastrocytomas: a randomized European Organisation for Research and Treatment of Cancer phase III trial. J Clin Oncol 24:2715–2722
van den Bent MJ, Dubbink HJ, Sanson M et al (2009) MGMT promoter methylation is prognostic but not predictive for outcome to adjuvant PCV chemotherapy in anaplastic oligodendroglial tumors: a report from EORTC Brain Tumor Group Study 26951. J Clin Oncol 27:5881–5886
Kouwenhoven MC, Gorlia T, Kros JM et al (2009) Molecular analysis of anaplastic oligodendroglial tumors in a prospective randomized study: a report from EORTC study 26951. Neuro-Oncology 11:737–746
van den Bent MJ, Brandes AA, Taphoorn MJ et al (2013) Adjuvant procarbazine, lomustine, and vincristine chemotherapy in newly diagnosed anaplastic oligodendroglioma: long-term follow-up of EORTC brain tumor group study 26951. J Clin Oncol 31:344–350
Vogelbaum MA, Berkey B, Peereboom D et al (2009) Phase II trial of preirradiation and concurrent temozolomide in patients with newly diagnosed anaplastic oligodendrogliomas and mixed anaplastic oligoastrocytomas: RTOG BR0131. Neuro-Oncology 11:167–175
Chinot OL, Honore S, Dufour H et al (2001) Safety and efficacy of temozolomide in patients with recurrent anaplastic oligodendrogliomas after standard radiotherapy and chemotherapy. J Clin Oncol 19:2449–2455
Prados MD, Scott C, Curran WJ Jr, Nelson DF, Leibel S, Kramer S (1999) Procarbazine, lomustine, and vincristine (PCV) chemotherapy for anaplastic astrocytoma: a retrospective review of radiation therapy oncology group protocols comparing survival with carmustine or PCV adjuvant chemotherapy. J Clin Oncol 17:3389–3395
Stewart LA (2002) Chemotherapy in adult high-grade glioma: a systematic review and meta-analysis of individual patient data from 12 randomised trials. Lancet 359:1011–1018
(2001) Randomized trial of procarbazine, lomustine, and vincristine in the adjuvant treatment of high-grade astrocytoma: a Medical Research Council trial. J Clin Oncol 19:509–518
Wick W, Hartmann C, Engel C et al (2009) NOA-04 randomized phase III trial of sequential radiochemotherapy of anaplastic glioma with procarbazine, lomustine, and vincristine or temozolomide. J Clin Oncol 27:5874–5880
Hegi ME, Diserens AC, Gorlia T et al (2005) MGMT gene silencing and benefit from temozolomide in glioblastoma. N Engl J Med 352:997–1003
Balss J, Meyer J, Mueller W, Korshunov A, Hartmann C, von Deimling A (2008) Analysis of the IDH1 codon 132 mutation in brain tumors. Acta Neuropathol 116:597–602
Yan H, Parsons DW, Jin G et al (2009) IDH1 and IDH2 mutations in gliomas. N Engl J Med 360:765–773
Yung WK, Prados MD, Yaya-Tur R et al (1999) Multicenter phase II trial of temozolomide in patients with anaplastic astrocytoma or anaplastic oligoastrocytoma at first relapse. Temodal Brain Tumor Group. J Clin Oncol 17:2762–2771
Friedman HS, Prados MD, Wen PY et al (2009) Bevacizumab alone and in combination with irinotecan in recurrent glioblastoma. J Clin Oncol 27:4733–4740
Chamberlain MC, Johnston S (2009) Salvage chemotherapy with bevacizumab for recurrent alkylator-refractory anaplastic astrocytoma. J Neurooncol 91:359–367
Stupp R, Mason WP, van den Bent MJ et al (2005) Radiotherapy plus concomitant and adjuvant temozolomide for glioblastoma. N Engl J Med 352:987–996
Clarke JL, Iwamoto FM, Sul J et al (2009) Randomized phase II trial of chemoradiotherapy followed by either dose-dense or metronomic temozolomide for newly diagnosed glioblastoma. J Clin Oncol 27:3861–3867
Perry JR, Belanger K, Mason WP et al (2010) Phase II trial of continuous dose-intense temozolomide in recurrent malignant glioma: RESCUE study. J Clin Oncol 28:2051–2057
Gilbert MR, Wang M, Aldape KD et al (2013) Dose-dense temozolomide for newly diagnosed glioblastoma: a randomized phase III clinical trial. J Clin Oncol 31:4085–4091
Chalmers AJ (2009) The potential role and application of PARP inhibitors in cancer treatment. Br Med Bull 89:23–40
Dungey FA, Loser DA, Chalmers AJ (2008) Replication-dependent radiosensitization of human glioma cells by inhibition of poly(ADP-ribose) polymerase: mechanisms and therapeutic potential. Int J Radiat Oncol Biol Phys 72:1188–1197
Sandhu SK, Yap TA, de Bono JS (2010) Poly(ADP-ribose) polymerase inhibitors in cancer treatment: a clinical perspective. Eur J Cancer 46:9–20
Malmstrom A, Gronberg BH, Marosi C et al (2012) Temozolomide versus standard 6-week radiotherapy versus hypofractionated radiotherapy in patients older than 60 years with glioblastoma: the Nordic randomised, phase III trial. Lancet Oncol 13:916–926
Wick W, Platten M, Meisner C et al (2012) Temozolomide chemotherapy alone versus radiotherapy alone for malignant astrocytoma in the elderly: the NOA-08 randomised, phase III trial. Lancet Oncol 13:707–715
Arvold ND, Reardon DA (2014) Treatment options and outcomes for glioblastoma in the elderly patient. Clin Interv Aging 9:357–367
Vredenburgh JJ, Desjardins A, Herndon JE 2nd et al (2007) Phase II trial of bevacizumab and irinotecan in recurrent malignant glioma. Clin Cancer Res 13:1253–1259
Kreisl TN, Kim L, Moore K et al (2009) Phase II trial of single-agent bevacizumab followed by bevacizumab plus irinotecan at tumor progression in recurrent glioblastoma. J Clin Oncol 27:740–745
Field KM, Simes J, Wheeler H et al (2013) A randomized phase II study of carboplatin and bevacizumab in recurrent glioblastoma multiforme (CABARET). ASCO meeting abstracts 31:2017
Taal W, Oosterkamp HM, Walenkamp AME et al (2013) A randomized phase II study of bevacizumab versus bevacizumab plus lomustine versus lomustine single agent in recurrent glioblastoma: The Dutch BELOB study. ASCO meeting abstracts2013 31:2001
Lai A, Filka E, McGibbon B et al (2008) Phase II pilot study of bevacizumab in combination with temozolomide and regional radiation therapy for up-front treatment of patients with newly diagnosed glioblastoma multiforme: interim analysis of safety and tolerability. Int J Radiat Oncol Biol Phys 71:1372–1380
Gilbert MR, Dignam JJ, Armstrong TS et al (2014) A randomized trial of bevacizumab for newly diagnosed glioblastoma. N Engl J Med 370:699–708
Chinot OL, Wick W, Mason W et al (2014) Bevacizumab plus radiotherapy-temozolomide for newly diagnosed glioblastoma. N Engl J Med 370:709–722
Herrlinger U, Schaefer N, Steinbach JP et al (2013) Bevacizumab, irinotecan, and radiotherapy versus standard temozolomide and radiotherapy in newly diagnosed, MGMT-nonmethylated glioblastoma patients: first results from the randomized multicenter GLARIUS trial. ASCO meeting abstracts 31:LBA2000
Batchelor TT, Sorensen AG, di Tomaso E et al (2007) AZD2171, a pan-VEGF receptor tyrosine kinase inhibitor, normalizes tumor vasculature and alleviates edema in glioblastoma patients. Cancer Cell 11:83–95
Batchelor TT, Mulholland P, Neyns B et al (2013) Phase III randomized trial comparing the efficacy of cediranib as monotherapy, and in combination with lomustine, versus lomustine alone in patients with recurrent glioblastoma. J Clin Oncol 31:3212–3218
de Groot JF, Lamborn KR, Chang SM et al (2011) Phase II study of aflibercept in recurrent malignant glioma: a North American Brain Tumor Consortium study. J Clin Oncol 29:2689–2695
Reardon DA, Fink KL, Mikkelsen T et al (2008) Randomized phase II study of cilengitide, an integrin-targeting arginine-glycine-aspartic acid peptide, in recurrent glioblastoma multiforme. J Clin Oncol 26:5610–5617
Stupp R, Hegi ME, Neyns B et al (2010) Phase I/IIa study of cilengitide and temozolomide with concomitant radiotherapy followed by cilengitide and temozolomide maintenance therapy in patients with newly diagnosed glioblastoma. J Clin Oncol 28:2712–2718
Stupp R, Hegi ME, Gorlia T et al (2013) Cilengitide combined with standard treatment for patients with newly diagnosed glioblastoma and methylated O6-methylguanine-DNA methyltransferase (MGMT) gene promoter: key results of the multicenter, randomized, open-label, controlled, phase III CENTRIC study. ASCO meeting abstracts 31:LBA2009
Wick W, Puduvalli VK, Chamberlain MC et al (2010) Phase III study of enzastaurin compared with lomustine in the treatment of recurrent intracranial glioblastoma. J Clin Oncol 28:1168–1174
Wen PY, Prados M, Schiff D et al (2010) Phase II study of XL184 (BMS 907351), an inhibitor of MET, VEGFR2, and RET, in patients (pts) with progressive glioblastoma (GB). ASCO meeting abstracts 28:2006
Wick W, Steinbach JP, Platten M et al (2013) Enzastaurin before and concomitant with radiation therapy, followed by enzastaurin maintenance therapy, in patients with newly diagnosed glioblastoma without MGMT promoter hypermethylation. Neuro-Oncology 15:1405–1412
Prados MD, Yung WK, Jaeckle KA et al (2004) Phase I trial of irinotecan (CPT-11) in patients with recurrent malignant glioma: a North American Brain Tumor Consortium study. Neuro-Oncology 6:44–54
Krishnan S, Brown PD, Ballman KV et al (2006) Phase I trial of erlotinib with radiation therapy in patients with glioblastoma multiforme: results of North Central Cancer Treatment Group protocol N0177. Int J Radiat Oncol Biol Phys 65:1192–1199
Rich JN, Reardon DA, Peery T et al (2004) Phase II trial of gefitinib in recurrent glioblastoma. J Clin Oncol 22:133–142
van den Bent MJ, Brandes AA, Rampling R et al (2009) Randomized phase II trial of erlotinib versus temozolomide or carmustine in recurrent glioblastoma: EORTC brain tumor group study 26034. J Clin Oncol 27:1268–1274
Mellinghoff IK, Wang MY, Vivanco I et al (2005) Molecular determinants of the response of glioblastomas to EGFR kinase inhibitors. N Engl J Med 353:2012–2024
Prados MD, Chang SM, Butowski N et al (2009) Phase II study of erlotinib plus temozolomide during and after radiation therapy in patients with newly diagnosed glioblastoma multiforme or gliosarcoma. J Clin Oncol 27:579–584
Brown PD, Krishnan S, Sarkaria JN et al (2008) Phase I/II trial of erlotinib and temozolomide with radiation therapy in the treatment of newly diagnosed glioblastoma multiforme: North Central Cancer Treatment Group Study N0177. J Clin Oncol 26:5603–5609
Chakravarti A, Wang M, Robins HI et al (2013) RTOG 0211: a phase I/II study of radiation therapy with concurrent gefitinib for newly diagnosed glioblastoma patients. Int J Radiat Oncol Biol Phys 85:1206–1211
Eisenstat DD, Nabors LB, Mason WP et al (2011) A phase II study of daily afatinib (BIBW 2992) with or without temozolomide (21/28 days) in the treatment of patients with recurrent glioblastoma. ASCO meeting abstracts 29:2010
Chang SM, Wen P, Cloughesy T et al (2005) Phase II study of CCI-779 in patients with recurrent glioblastoma multiforme. Invest New Drugs 23:357–361
Cloughesy TF, Wen PY, Robins HI et al (2006) Phase II trial of tipifarnib in patients with recurrent malignant glioma either receiving or not receiving enzyme-inducing antiepileptic drugs: a North American Brain Tumor Consortium Study. J Clin Oncol 24:3651–3656
Doherty L, Gigas DC, Kesari S et al (2006) Pilot study of the combination of EGFR and mTOR inhibitors in recurrent malignant gliomas. Neurology 67:156–158
Galanis E, Buckner JC, Maurer MJ et al (2005) Phase II trial of temsirolimus (CCI-779) in recurrent glioblastoma multiforme: a North Central Cancer Treatment Group Study. J Clin Oncol 23:5294–5304
Reardon DA, Desjardins A, Vredenburgh JJ et al (2010) Phase II trial of erlotinib plus sirolimus in adults with recurrent glioblastoma. J Neurooncol 96:219–230
Galanis E, Jaeckle KA, Maurer MJ et al (2009) Phase II trial of vorinostat in recurrent glioblastoma multiforme: a north central cancer treatment group study. J Clin Oncol 27:2052–2058
Kubicek GJ, Werner-Wasik M, Machtay M et al (2009) Phase I trial using proteasome inhibitor bortezomib and concurrent temozolomide and radiotherapy for central nervous system malignancies. Int J Radiat Oncol Biol Phys 74:433–439
Parsons DW, Jones S, Zhang X et al (2008) An integrated genomic analysis of human glioblastoma multiforme. Science 321:1807–1812
Phillips HS, Kharbanda S, Chen R et al (2006) Molecular subclasses of high-grade glioma predict prognosis, delineate a pattern of disease progression, and resemble stages in neurogenesis. Cancer Cell 9:157–173
Verhaak RG, Hoadley KA, Purdom E et al (2010) Integrated genomic analysis identifies clinically relevant subtypes of glioblastoma characterized by abnormalities in PDGFRA, IDH1, EGFR, and NF1. Cancer Cell 17:98–110
Dunn GP, Rinne ML, Wykosky J et al (2012) Emerging insights into the molecular and cellular basis of glioblastoma. Genes Dev 26:756–784
Louis DN (2006) Molecular pathology of malignant gliomas. Annu Rev Pathol 1:97–117
Yan H, Bigner DD, Velculescu V, Parsons DW (2009) Mutant metabolic enzymes are at the origin of gliomas. Cancer Res 69:9157–9159
Choi C, Ganji SK, DeBerardinis RJ et al (2012) 2-Hydroxyglutarate detection by magnetic resonance spectroscopy in IDH-mutated patients with gliomas. Nat Med 18:624–629
Sanson M, Marie Y, Paris S et al (2009) Isocitrate dehydrogenase 1 codon 132 mutation is an important prognostic biomarker in gliomas. J Clin Oncol 27:4150–4154
Leu S, von Felten S, Frank S et al (2013) IDH/MGMT-driven molecular classification of low-grade glioma is a strong predictor for long-term survival. Neuro-Oncology 15:469–479
Heaphy CM, de Wilde RF, Jiao Y et al (2011) Altered telomeres in tumors with ATRX and DAXX mutations. Science 333:425
Bettegowda C, Agrawal N, Jiao Y et al (2011) Mutations in CIC and FUBP1 contribute to human oligodendroglioma. Science 333:1453–1455
Weiler M, Wick W (2012) Molecular predictors of outcome in low-grade glioma. Curr Opin Neurol 25:767–773
Conflict of interest
M.S.A. has received research support from Novartis, Boehringer Ingelheim. M.S.A. has served on advisory board for Genentech/Roche. S.M.C. has received research support from Novartis/Schering.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Ahluwalia, M.S., Chang, S.M. Medical therapy of gliomas. J Neurooncol 119, 503–512 (2014). https://doi.org/10.1007/s11060-014-1495-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11060-014-1495-1