Abstract
The purpose of this study was to describe our clinical experience using optically-guided linear accelerator (linac)-based frameless stereotactic radiosurgery (SRS) for the treatment of brain metastases. Sixty-five patients (204 lesions) were treated between 2005 and 2008 with frameless SRS using an optically-guided bite-block system. Patients had a median of 2 lesions (range, 1–13). Prescription dose ranged from 14 to 22 Gy (median, 18 Gy) and was given in a single fraction. Clinical and radiographic evaluation occurred every 2–4 months following treatment. At a median follow-up of 6.2 months, actuarial survival at 12 months was 40% [95% confidence interval (CI), 28–52). Of 135 lesions that were evaluable for local control (LC), 119 lesions (88%) did not show evidence of progression. Actuarial 12 month LC was 76% (95% CI, 66–86). Tumors ≤2 cm in size had a better 12 month LC rate (81% vs. 36%, P = 0.017) than those >2 cm. Adverse events occurred in three patients (5%). Optically-guided linac-based frameless SRS can produce clinical outcomes that compare favorably to frame-based techniques. As this technique is convenient to use and allows for the uncomplicated delivery of hypofractionated radiotherapy, frameless SRS will likely have an increasingly important role in the management of brain metastases.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Stereotactic radiosurgery (SRS) has a well-established role for the treatment of intracranial disease and has been used specifically for the management of brain metastases in the United States since the mid 1980s [1]. The efficacy of SRS for the treatment of brain metastases has been demonstrated in several randomized trials and multi-institutional studies [2–5].
Conventionally, SRS is performed with the use of a stereotactic head frame that is affixed to the calvarium in order to provide rigid patient immobilization during planning and treatment delivery. The use of a head frame in SRS has been extensively studied and has been shown to be associated with excellent target localization during both planning and treatment delivery [6, 7]. However, although this system provides a high-degree of accuracy that is necessary when using large and highly-conformal doses, there are several disadvantages of frame-based immobilization, including patient discomfort, difficulty performing hypofractionated therapy, and additional effort required to coordinate between personnel on different services.
As an alternative to frame-based technologies, there is now a variety of frameless systems that have been devised using both CyberKnife ® (Accuray Inc., Sunnyvale, CA) and traditional linear accelerator (linac)-based platforms. These systems differ in their methods for patient tracking, as well as their ability to perform various types of modern radiotherapy advancements, such as image-guided radiotherapy (IGRT) and intensity-modulated SRS (IMSRS). However, only limited clinical data on the use of these systems for intracranial metastatic disease has been reported [8–12]. Moreover, even fewer studies have provided data specifically on linac-based frameless devices [10, 11]. As the ultimate validation of a new procedure is measured in terms of clinical outcomes, it is important to provide treatment data from actual patients prior to widespread acceptance.
In 2005, the University of California at San Diego adopted an optically-guided linac-based frameless SRS system (Varian Triology, Varian Oncology Systems, Palo Alto, CA), which has been used to treat over 200 patients with either metastatic or primary CNS disease. In this paper, we describe our clinical experience using optically-guided frameless SRS to manage brain metastases.
Materials and methods
Patient selection
All patients were treated at the University of California at San Diego in the Rebecca and John Moores Comprehensive Cancer Center between December 2005 and June 2008 using frameless SRS. Patients with intracranial metastatic disease that was histologically verified at either the primary or metastatic site were selected for treatment if they were not surgical candidates and were able to lie still and tolerate simulation. Initially, patients with greater than four metastases were offered frameless SRS only if they had refused whole-brain radiotherapy (WBRT), however we transitioned to treating patients with greater than four metastases after our initial clinical experiences were encouraging.
Patient and treatment characteristics
A total of 65 patients with 204 lesions were treated for intracranial metastatic disease. Patient characteristics are summarized in Table 1. The largest tumor diameter was measured for each lesion, and the median value was 9 mm (range, 1–35 mm). Prescription dose was 14–22 Gy (median, 18 Gy) and was given in a single fraction. Specific doses were determined by the RTOG 90-05 report [13]. Radiation therapy was delivered in rotational arc beams with circular cone collimation in 37 patients (57%) who had both small and few (three or fewer) lesions. For patients with either a large and irregular tumor or with multiple lesions (28 patients, 43%), IMSRS with a dynamic multi-leaf collimator (MLC) was used. Treatment characteristics are summarized in Table 2. Frameless SRS was performed with upfront WBRT in 10 patients (15%). Salvage therapy was offered to patients with recurrent local disease or new intracranial metastases and consisted of repeated frameless SRS, WBRT or surgery.
Frameless radiosurgery procedure
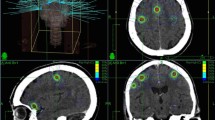
After obtaining informed consent, patients underwent contrast-enhanced T1-weighted magnetic resonance imaging (MRI) (26 cm FOV, 512 × 512 pixel size, 1.5 mm slice intervals) using a 3.0 Tesla MRI (General Electric, Fairfield, CT). Subsequently, customized immobilization was then designed for each patient and consisted of an Accuform™ (CIVCO Medical Solutions, Kalona, IA) headrest fitted to the patient’s head in neutral position, a molded thermoplastic face mask, and a customized bite block.
After the bite-block had been fashioned, the patient was taken to the treatment vault for verification. In the vault, the patient was fitted with a head band that had an attached set of reference markers. The bite-block was then removed and replaced 10 times and the positioning error was measured each time through the optical-guidance apparatus. If the variation between all 10 trials was less than 0.75 mm, the bite block was accepted for use.
Patients were then simulated supine with the thermoplastic mask, headrest, and bite block in place using non-contrast brain computed tomography (CT) (35 cm FOV, 512 × 512 pixel size, 1.25 mm slice intervals). An initial review of the CT was performed to ensure that all fiducial markers were visible and that no significant motion abnormality occurred. The MRI and CT were then transferred to the planning center and fused using a rigid auto-registration tool and subsequently manually verified.
Planning was performed using Varian FastPlan ® software for cone-based plans or Varian Eclipse™ software for IMSRS plans and was based on the enhancing tumor volume with an additional 1–2 mm margin. Single and multiple isocenter plans were constructed for one or more lesions under the guidance of the radiation oncologist, neurosurgeon, and medical physicist. The 80% isodose curve was selected for each patient planned with cone-based collimation, and approximately the 90% isodose line was selected for IMSRS patients.
On treatment day, patient setup and isocenter localization were performed with the optical-guidance system. In addition, a pair of orthogonal kilovoltage (kV) images were taken and compared to digitally reconstructed radiographs (DRRs) generated from the planning CT. These images were used for verification purposes only and were not used for repositioning. Radiation was generated from a Varian Trilogy linear accelerator (linac) using the 6MV radiosurgery mode. Treatment times were generally less than 45 min or up to 1 h if including patient setup time.
Follow-up, statistical analysis and toxicity
Patients were routinely seen 1 week following SRS for a clinical exam. Contrast-enhanced MRI and physician evaluation was performed every 3 months until 18 months, and then routine surveillance was determined on a case-by-case basis. Treatment response was analyzed by survival and local control. Local control was defined as the absence of progression; progression was defined as an increase of greater than 20% of the sum of the two largest diameters of the lesion. Intracranial status was deemed as unknown if at least one follow-up imaging exam was not performed. These patients were excluded from local control data, however they were included in survival analysis. Of those with radiographic follow-up, imaging included MRI (92%) and CT (8%). Each MRI was independently evaluated for progression by a radiologist, a radiation oncologist, and a neurosurgeon. Elsewhere-brain failure was defined as new intracranial metastatic disease occurring outside of the treatment volume on radiographic examination, and regional control was defined as the absence of elsewhere-brain failure on follow-up imaging. Survival, local failure, and regional control were estimated by the Kaplan–Meier method. All statistical analyses were performed using NCSS (originally, Number Cruncher Statistical System) (NCSS LLC, Kaysville, UT). Toxicity was graded according to the Radiation Therapy Oncology Group (RTOG) scale [14].
Results
The median follow-up for all patients was 6.2 months (range, 0.13–32.4). Sixteen were alive at the time of analysis and had a median follow-up of 18.1 months (range 7.5–32.4). The 12-month actuarial survival for the entire group was 40% [95% confidence interval (CI), 28–52%) (Fig. 1). No statistically significant difference in survival between patients treated with frameless SRS alone or combined with WBRT was detected (12-month actuarial survival 39% vs. 46%, P = 0.40).
Seventeen patients were excluded from local control and regional control analysis owing to unknown intracranial status at the time of death. Of the 48 remaining patients with 135 lesions who were radiographically evaluable for local control, 37 patients (77%) and 119 lesions (88%) did not show evidence of progression. Actuarial 12 month local control was 76% (95% CI, 66–86%) (Fig. 2). Tumors ≤2 cm in size had a better 12 month local control rate than those >2 cm (81% vs. 36%, P = 0.017) (Fig. 3). No statistically significant difference was observed between lesions treated with and without WBRT (P = 0.31).
Elsewhere-brain failures were detected in 23 patients (48%). Actuarial 12 month regional control was 46% (95% CI, 30–62%) (Fig. 4). No statistically significant difference in regional control was observed between patients treated with and without WBRT (P = 0.83). Salvage therapy was performed for patients with local failures or new intracranial metastatic disease and consisted of repeat SRS (nine patients, 14%), WBRT (seven patients, 11%), repeat SRS and WBRT (three patients, 5%), and surgery (two patients, 3%). Of patients treated with repeat SRS, nine patients received a single re-treatment, two patients received two re-treatments, and one patient received four re-treatments.
Nine patients (14%) had grade 2 toxicities; one patient had a single seizure, one patient had transient mild ataxia, and seven had edema-associated symptoms that resolved with steroids. Grade 3 or higher toxicities occurred in three patients (5%); one patient developed aphasia, one patient with metastatic melanoma developed hemorrhage in a treated lesion, and one patient developed hemiparesis secondary to radionecrosis and required surgery.
Discussion
Frameless SRS is a relatively new treatment that avoids the use of invasive head frames for patient immobilization and provides several distinct advantages over frame-based techniques. Although several systems are currently in use, limited clinical data exist to demonstrate the safety and efficacy of frameless devices, and data are especially lacking on systems that employ conventional linac-based platforms. In this study, we present encouraging clinical outcomes on a series of patients treated with optically-guided frameless linac-based SRS for the management of brain metastases.
Local control was selected as a primary endpoint, as it is a sensitive clinical outcome for assessing targeting accuracy. Frame-based SRS has been shown to produce 12-month actuarial local-control rates ranging from 64 to 89% (Table 3) [4, 15–21]. Our actuarial local control rate was 76% at 12 months, which compares favorably to frame-based, as well as other frameless SRS techniques (Table 3). Furthermore, a unique advantage of the present series of patients is that the majority of our patients (82%) did not receive upfront WBRT or surgery, and therefore the influence of WBRT and other initial therapies on our local control rate was minimized. In contrast, other frameless studies have reported only 26–40% [10, 11] of patients treated with frameless SRS alone.
Survival was also analyzed as an endpoint. Frame-based SRS 12-month actuarial survival rates range from 23 to 54% (Table 3). Our experience with frameless SRS resulted in a 12 month actuarial survival rate of 40%, which also compares favorably to both frame-based, as well as other frameless SRS techniques (Table 3).
Frameless techniques have several advantages over frame-based approaches, including added patient comfort, convenience of use, and improved ability to perform hypofractionated therapy for large lesions. Generally, SRS is recommended for lesions less than 3 cm [22]. However, research has suggested that patients may benefit from hypofractionated SRS for larger tumors [9, 23]. Although hypofractionation is possible with frame-based systems, frameless systems can offer improved patient comfort and less complicated delivery of therapy.
Clinical outcomes have now been reported on each of the frameless radiosurgery systems currently available. CyberKnife ® offers a frameless system that employs a compact linac mounted on a robotic-arm that acquires X-ray based images for precise target localization [24]. Novalis™ (BrainLab Inc, Chicago, IL) offers a system that uses both optical-guidance of reflective fiducials placed over the patient’s mask for initial positioning and orthogonal kilovoltage images for added image-guidance [11]. RadioCameras (Zmed, Ashland, MA) provides a linac-based system that employs an optically-guided bite-block [10], which was later adapted by Varian and combined with the Trilogy™ machine to allow for high-output delivery along with IGRT and IMSRS. Clinical outcomes reported by these systems are similar (Table 3), and the advantages of each technique depend on various institutional preferences.
Although these results are promising, our analysis has several limitations. First, this is a retrospective study and thus suffers from the inherent limitations of such an analysis. Second, not all patients underwent follow-up imaging to document local control, and therefore, local failures may have been missed. Unfortunately, this is a common problem with research on brain metastases, as many patients die within a few months of treatment.
In conclusion, we report on our clinical experience using an optically-guided linac-based frameless SRS system for the treatment of brain metastases. Our results show encouraging clinical outcomes that compare favorably to traditional frame-based as well as other frameless technologies and support the continued role of frameless SRS in the management of patients with brain metastases.
References
Lunsford LD, Flickinger J, Lindner G, Maitz A (1989) Stereotactic radiosurgery of the brain using the first United States 201 cobalt-60 source gamma knife. Neurosurgery 24:151–159
Kondziolka D, Patel A, Lunsford LD, Kassam A, Flickinger JC (1999) Stereotactic radiosurgery plus whole brain radiotherapy versus radiotherapy alone for patients with multiple brain metastases. Int J Radiat Oncol Biol Phys 45:427–434
Andrews DW, Scott CB, Sperduto PW, Flanders AE, Gaspar LE, Schell MC, Werner-Wasik M, Demas W, Ryu J, Bahary JP, Souhami L, Rotman M, Mehta MP, Curran WJ Jr (2004) Whole brain radiation therapy with or without stereotactic radiosurgery boost for patients with one to three brain metastases: phase III results of the RTOG 9508 randomised trial. Lancet 363:1665–1672
Sneed PK, Suh JH, Goetsch SJ, Sanghavi SN, Chappell R, Buatti JM, Regine WF, Weltman E, King VJ, Breneman JC, Sperduto PW, Mehta MP (2002) A multi-institutional review of radiosurgery alone vs. radiosurgery with whole brain radiotherapy as the initial management of brain metastases. Int J Radiat Oncol Biol Phys 53:519–526
Aoyama H, Shirato H, Tago M, Nakagawa K, Toyoda T, Hatano K, Kenjyo M, Oya N, Hirota S, Shioura H, Kunieda E, Inomata T, Hayakawa K, Katoh N, Kobashi G (2006) Stereotactic radiosurgery plus whole-brain radiation therapy vs stereotactic radiosurgery alone for treatment of brain metastases: a randomized controlled trial. JAMA 295:2483–2491
Yeung D, Palta J, Fontanesi J, Kun L (1994) Systematic analysis of errors in target localization and treatment delivery in stereotactic radiosurgery (SRS). Int J Radiat Oncol Biol Phys 28:493–498
Kitchen ND, Lemieux L, Thomas DG (1993) Accuracy in frame-based and frameless stereotaxy. Stereotact Funct Neurosurg 61:195–206
Shimamoto S, Inoue T, Shiomi H, Sumida I, Yamada Y, Tanaka E (2002) CyberKnife stereotactic irradiation for metastatic brain tumors. Radiat Med 20:299–304
Nishizaki T, Saito K, Jimi Y, Harada N, Kajiwara K, Nomura S, Ishihara H, Yoshikawa K, Yoneda H, Suzuki M, Gibbs IC (2006) The role of cyberknife radiosurgery/radiotherapy for brain metastases of multiple or large-size tumors. Minim Invasive Neurosurg 49:203–209
Kamath R, Ryken TC, Meeks SL, Pennington EC, Ritchie J, Buatti JM (2005) Initial clinical experience with frameless radiosurgery for patients with intracranial metastases. Int J Radiat Oncol Biol Phys 61:1467–1472
Breneman JC, Steinmetz R, Smith A, Lamba M, Warnick RE (2009) Frameless image-guided intracranial stereotactic radiosurgery: clinical outcomes for brain metastases. Int J Radiat Oncol Biol Phys
Furuse M, Aoki T, Takagi T, Takahashi JA, Ishikawa M (2008) Frameless stereotactic radiosurgery with a bite-plate: our experience with brain metastases. Minim Invasive Neurosurg 51:333–335
Shaw E, Scott C, Souhami L, Dinapoli R, Kline R, Loeffler J, Farnan N (2000) Single dose radiosurgical treatment of recurrent previously irradiated primary brain tumors and brain metastases: final report of RTOG protocol 90-05. Int J Radiat Oncol Biol Phys 47:291–298
Cox JD, Stetz J, Pajak TF (1995) Toxicity criteria of the radiation therapy oncology group (RTOG) and the European organization for research and treatment of cancer (EORTC). Int J Radiat Oncol Biol Phys 31:1341–1346
Becker G, Jeremic B, Engel C, Buchgeister M, Paulsen F, Duffner F, Meisner C, Bamberg M (2002) Radiosurgery for brain metastases: the Tuebingen experience. Radiother Oncol 62:233–237
Chitapanarux I, Goss B, Vongtama R, Frighetto L, De Salles A, Selch M, Duick M, Solberg T, Wallace R, Cabatan-Awang C, Ford J (2003) Prospective study of stereotactic radiosurgery without whole brain radiotherapy in patients with four or less brain metastases: incidence of intracranial progression and salvage radiotherapy. J Neurooncol 61:143–149
Datta R, Jawahar A, Ampil FL, Shi R, Nanda A, D’Agostino H (2004) Survival in relation to radiotherapeutic modality for brain metastasis: whole brain irradiation vs. gamma knife radiosurgery. Am J Clin Oncol 27:420–424
Rades D, Bohlen G, Pluemer A, Veninga T, Hanssens P, Dunst J, Schild SE (2007) Stereotactic radiosurgery alone versus resection plus whole-brain radiotherapy for 1 or 2 brain metastases in recursive partitioning analysis class 1 and 2 patients. Cancer 109:2515–2521
Schomas DA, Roeske JC, MacDonald RL, Sweeney PJ, Mehta N, Mundt AJ (2005) Predictors of tumor control in patients treated with linac-based stereotactic radiosurgery for metastatic disease to the brain. Am J Clin Oncol 28:180–187
Bhatnagar AK, Flickinger JC, Kondziolka D, Lunsford LD (2006) Stereotactic radiosurgery for four or more intracranial metastases. Int J Radiat Oncol Biol Phys 64:898–903
Serizawa T, Yamamoto M, Nagano O, Higuchi Y, Matsuda S, Ono J, Iwadate Y, Saeki N (2008) Gamma Knife surgery for metastatic brain tumors. J Neurosurg 109(Suppl):118–121
Alexander EIII, Moriarty TM, Davis RB, Wen PY, Fine HA, Black PM, Kooy HM, Loeffler JS (1995) Stereotactic radiosurgery for the definitive, noninvasive treatment of brain metastases. J Natl Cancer Inst 87:34–40
Davey P, Schwartz ML, Scora D, Gardner S, O’Brien PF (2007) Fractionated (split dose) radiosurgery in patients with recurrent brain metastases: implications for survival. Br J Neurosurg 21:491–495
Adler JR Jr, Chang SD, Murphy MJ, Doty J, Geis P, Hancock SL (1997) The Cyberknife: a frameless robotic system for radiosurgery. Stereotact Funct Neurosurg 69:124–128
Acknowledgments
This research was supported by an NIH T32 training grant (RR023254). Conflicts of interest statement A.J.M and K.T.M have received honorariums from Varian Medical Systems for giving lectures on varying topics in radiotherapy. The Center for Advanced Radiotherapy Technologies receives funding from Varian Medical Systems for research unrelated to the current project.
Open Access
This article is distributed under the terms of the Creative Commons Attribution Noncommercial License which permits any noncommercial use, distribution, and reproduction in any medium, provided the original author(s) and source are credited.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
Open Access This is an open access article distributed under the terms of the Creative Commons Attribution Noncommercial License (https://creativecommons.org/licenses/by-nc/2.0), which permits any noncommercial use, distribution, and reproduction in any medium, provided the original author(s) and source are credited.
About this article
Cite this article
Nath, S.K., Lawson, J.D., Wang, JZ. et al. Optically-guided frameless linac-based radiosurgery for brain metastases: clinical experience. J Neurooncol 97, 67–72 (2010). https://doi.org/10.1007/s11060-009-9989-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11060-009-9989-y