Abstract
Background
Breast cancer patients undergoing chemotherapy encounter a significant challenge of chemoresistance because of drug efflux by ATP-binding cassette (ABC) transporters. Breast cancer cell density alters considerably throughout the early stages of primary and secondary tumor development. Although cell density in culture influences kinetics, the effects of varying cell densities on the chemoresistance of breast cancer cells remains largely unexplored.
Methods and results
We observed chemotherapeutics-induced differential gene and protein expression of ABC transporters in luminal and basal breast cancer cells cultured at low and high seeding densities. Low-density cultures depicted a significant increase in the mRNA expression of ABC transporters—ABCG2, ABCG1, ABCC4, ABCA2, ABCA3, ABCC2, ABCC3, ABCC6, ABCC7, and ABCC9 as compared with high-density cultures. Next, cells at both low and high seeding densities when pre-treated with cyclosporine A (CsA), a pan-inhibitor of ABC transporters, resulted in increased sensitization to chemotherapeutics—doxorubicin and tamoxifen at markedly low IC50 concentrations suggesting the role of ABC transporters. Finally, markedly high doxorubicin-drug accumulation, significantly increased expression of N-cadherin, and a significant decrease in chemotherapeutics-induced in vitro tumorigenesis was observed in low-density seeded breast cancer cells when pre-treated with CsA suggesting ABC transporters inhibition-mediated increased efficacy of chemotherapeutics.
Conclusion
These findings suggest that breast cancer cells grown at low seeding density imparts chemoresistance towards doxorubicin or tamoxifen by a differential increase in the expression of ABC transporters. Thus, a combinatorial treatment strategy including ABC transporter inhibitors and chemotherapeutics can be a way forward for overcoming the breast cancer chemoresistance.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Cancer is the second leading cause of mortality after heart disease, accounting for 21% of all fatalities in both men and women. In the United States alone, predictive mortality of 609,360 individuals from cancer in 2022, suggests approximately 1700 fatalities every day. Breast cancer is the most prevalent disease diagnosed in females and the main cause of cancer mortality worldwide, with 2.3 million new cases each year [1]. Although interventions like surgery, chemotherapy, and radiotherapy can control the growth of breast cancer cells but are ineffective against breast cancer stem cells (CSCs), a small fraction of cells that dwell within the tumor and migrate to distant organs forming secondary tumors and resulting in recurrence of cancer [2, 3].
Breast tumor density predicts patient responses to therapy for breast cancer cure and recurrence [4]. In individuals treated with tamoxifen as adjuvant treatment, lower breast tumor density has been linked to a lower risk of recurrence [5]. Thus, tumor density is an important factor in response to chemotherapy against breast cancer.
Cancer development can be divided into primary tumor growth and secondary metastasis. Chemotherapeutics fail to effectively eradicate dormant populations of disseminated tumor cells at the secondary tumor sites [6]. Chemoresistance in breast cancer is often due to the efflux of drugs from cells by ATP-binding cassettes (ABC) transporters that decrease intracellular drug concentration [7,8,9]. There are 49 known ABC genes in humans, which are divided into seven subfamilies (A–G) based on their amino acid sequence and their protein domains [10]. Elevated ABC transporter expression has been linked to invasive, aggressive, and chemoresistant tumors [11]. ABC transporter inhibitors in clinical settings have so far resulted in unsatisfactory therapeutic outcomes due to their drug-drug interactions, toxicity, and errors in clinical trial design [12, 13]. There is currently no evidence of the role of cancer cell density in chemoresistance. This study attempted to identify the correlation between cell density and chemoresistance in breast cancer by evaluating the expression of selected ABC transporters based on their physiological relevance.
Materials and methods
Cell culture
MCF-7, MDA-MB-468, and MDA-MB-231, breast cancer cell lines were grown in Dulbecco’s Minimum Essential Medium (DMEM) and RPMI-1640 and fortified with 10% Fetal Bovine Serum (FBS) and 1% penicillin-streptomycin at 37 °C and 5% CO2 [14]. Cells were treated with chemotherapeutic drugs doxorubicin and tamoxifen (Sigma-Aldrich, Missouri, USA).
Gene expression study
To assess the effect of doxorubicin and tamoxifen on the expression of the selected 23 ABC transporters and cell adhesion molecules, we performed the qRT-PCR-based analysis in luminal breast cancer cells, MCF-7 and basal Triple-negative breast cancer (TNBC) cells- MDA-MB-468, MDA-MB-231 at high (1 × 105 cells/well of 6-well plate) and low (1 × 103 cells/well of 6-well plate) seeding density conditions in absence or presence of chemotherapeutic drugs at their experimentally-calculated IC50 values. Cells were subjected to synchronization of the cell cycle before treatment with doxorubicin and tamoxifen for 24 h. Total RNA was extracted, and cDNA was synthesized as described previously [14]. The gene expression values of various genes (primer sequences, refer to Suppl Table, ST1) were normalized to Eukaryotic 18 S rRNA and represented as fold-change relative to the control of the high- and low-cell density group [14, 15].
Protein expression studies
MCF-7, MDA-MB-468, and MDA-MB-231 cells were plated at high- and low-seeding density conditions, and cultured for 24 h, followed by treatment with chemotherapeutic agents for 48 h as described above. Cells were lysed for total protein extraction, SDS–PAGE was performed, and proteins were transferred onto PVDF membranes and probed with rabbit anti-ABCG2 (1:1000, #42,078, Cell Signaling Technology, USA); rabbit anti-ABCB1 (1:1000, #13,342, Cell Signaling Technology, USA); rabbit anti-ABCC1 (1:1000, #14,685, Cell Signaling Technology, USA); and/or rabbit anti-ABCC3 (1:1000, #39,909, Cell Signaling Technology, USA) antibodies. A rabbit anti-β-tubulin (1:1000, #2146, Cell Signaling Technology, USA) was used as a loading control. Following washes in TBST buffer, the membranes were incubated for 45 min at room temperature with HRP-conjugated secondary antibodies: anti-rabbit (1:5000, #7074, Cell Signaling Technology, USA). G: Box (Syngene, Maryland, USA) was used for visualization, as previously reported [14, 15].
Effect of cyclosporine a on cytotoxicity of breast cancer cell lines
MTT assay- The cytotoxicity of doxorubicin (0.001–10 µM) or tamoxifen (0.1–100 µM) in MCF-7, MDA-MB-468, and MDA-MB-231 for 24 h was evaluated using a 3-(4,5-dimethylthiazol-2-yl)-2,5-diphenyl tetrazolium bromide assay. The IC50 of the drugs was determined in breast cancer cells cultured at different cell seeding densities.
Following that, to assess the inhibition potential of cyclosporine A (pan-inhibitor of ABC transporter), breast cancer cells were cultured with varying (low density or high density) cell densities pre-conditioned with increasing concentrations of cyclosporine A (CsA) for 1 h before treatment with IC50 concentrations of doxorubicin or tamoxifen, followed by MTT assay as previously described [16, 17]. Next, to evaluate the change in IC50 of doxorubicin- or tamoxifen-treated breast cancer cell lines cultured with varying cell densities under pre-conditioning with CsA (5 µM for 1 h, Sigma-Aldrich, Missouri, USA), we performed an MTT assay as described previously [14, 16]. The IC50 values of the drugs (µM) were calculated for each group using GraphPad Prism, Version 8 (San Diego, CA, USA).
Doxorubicin-drug accumulation assay
Breast cancer cells were plated on poly-D-lysine-coated glass coverslip placed in a 6-well plate at high- and low-density seeding density conditions, cultured for 24 h, followed by treatment with doxorubicin (1 µM) in the absence or presence of CsA (5 µM) for 48 h. Cells were fixed with 4% paraformaldehyde for 15 min followed by phosphate-buffered saline wash and mounted with DAPI containing mounting medium. Images were captured using Olympus FV10i confocal microscope (Olympus) with emission bands of doxorubicin evaluated at 568 nm. Images were processed using ImageJ (NIH, Bethesda, MD) [17].
Mammosphere forming efficiency
Cells at low and high density were seeded onto poly hydroxyethyl methacrylate (pHEMA), (Sigma-Aldrich, USA) coated 24-well plates containing mammosphere medium-171 enriched with mammary epithelial growth supplement (MEGS) and B-27 (Life technologies, Auckland, New Zealand) along with either alone or combination of CsA (5 µM) and doxorubicin or tamoxifen at indicated concentrations. The suspension culture along with the treatment was incubated under 5% CO2, at 37 °C in a humidified atmosphere for 7 days. Images of the mammosphere were procured at 10 × magnification of a microscope (Olympus IX71, Japan). The size of spheres was quantified as described earlier [18, 19] using Image J software (NIH, Bethesda, USA).
Statistical analysis
Data are represented as the mean, standard error of the mean (SEM), or standard deviation (SD) of at least three independent studies. Photomicrographs depict typical experiments that have been repeated at least three times with comparable results. Statistical tests were carried out across groups and their corresponding controls, using one/two-way ANOVA subsequently followed by Dunnett’s or Tukey’s multiple comparisons analysis, with p values ≤ 0.05 considered significant.
Results
Cell density differentially regulates the expression of ABC transporters
The dose-response relationship of anti-cancer chemotherapeutic drugs often changes dramatically with tumor density and volume [20,21,22,23]. Therefore, to comprehend the effect of chemotherapeutics on the expression profile of ABC transporters in the tumor microenvironment, we exposed the breast cancer cell lines plated in varying (low and high) cell seeding densities to the chemotherapeutics against breast cancer, doxorubicin, and tamoxifen. The identified IC50 concentrations of the drugs against these breast cancer cell lines seeded at regular seeding densities (Table ST2) were used to examine the expression profile of selected ABC transporters in MCF-7 (Fig. 1 A–D), MDA-MB-468 (Fig. 2 A–D), and MDA-MB-231 (Fig. S1A–D).
Drug-induced cell density-dependent differential expression of ABC transporters in luminal breast cancer cells. Graphs depicting relative mRNA expression profile of ABC transporters in MCF-7 cells cultured in low and high seeding densities in presence of chemotherapeutic drugs at their IC50 concentrations. A ABC transporters of A, B, C, and G—subfamilies with known function as a drug efflux pump, B ABC transporters of A, B, and G—subfamilies with known physiological roles, C ABC transporters of C—subfamily with known physiological roles, and D ABC transporters of B, C, and G—subfamilies with unknown functions. (Data are represented as mean ± SEM of experiments repeated at least thrice. *p ≤ 0.05 as compared with respective controls)
Drug-induced cell density-dependent differential gene expression of ABC transporters in basal breast cancer cells. Graphs depicting relative mRNA expression profile of ABC transporters in MDA-MB-468 cells cultured in low and high seeding densities in presence of chemotherapeutic drugs at their IC50 concentrations. A ABC transporters of A, B, C, and G—subfamilies with known function as a drug efflux pump, B ABC transporters of A, B, and G—subfamilies with known physiological roles, C ABC transporters of C—subfamily with known physiological roles, and D ABC transporters of B, C, and G—subfamilies with unknown functions. (Data are represented as mean ± SEM of experiments repeated at least thrice. *p ≤ 0.05 as compared with respective controls)
The selected ABC transporters are based on their functionality such as drug efflux pumps (Fig. 1A); other physiological roles e.g., ion channels, transporters of various bio-macromolecules (Fig. 1B); ions, salts, peptides (Fig. 1C); and a few whose functions are unknown (Fig. 1D). MCF-7 at low seeding density depicted a significant increase in expression of ABCG2 (Fig. 1A) and ABCG4 (Fig. 1D) in presence of doxorubicin or tamoxifen. Doxorubicin (0.42 µM) significantly induced the expression of ABCC2 and ABCC9 (Fig. 1C) in MCF-7 cells grown at low seeding density. Similarly, tamoxifen (12.16 µM) treatment to MCF-7 cells grown at low seeding density led to significantly increased expression of ABCG1 (Fig. 1B) and ABCC5 (Fig. 1C). Interestingly, tamoxifen significantly increased the expression of ABCC11 (Fig. 1D) in MCF-7 cells grown at high seeding densities.
MDA-MB-468 cells cultured at low seeding density depicted tamoxifen (12.69 µM)-induced significantly high expression of ABCB1, ABCC1, and ABCC3 (Fig. 2A) whereas doxorubicin (0.073 µM)-induced significantly high expression of only ABCA3 (Fig. 2B). Similarly, tamoxifen-induced increased expression of ABCC7 (Fig. 2C), ABCC6, and ABCC12 (Fig. 2D) while doxorubicin-induced increased expression of ABCC6 (Fig. 2D) was observed in MDA-MB-468 cells cultured at low seeding densities. However, MDA-MB-231 cells cultured at low seeding density demonstrated a significant increase in expression of ABCA2 (Fig. S1A), and ABCC9 (Fig. S1C) in presence of doxorubicin (0.082 µM) and ABCG1 (Fig. S1B), in presence of tamoxifen (16.93 µM). A significant increase in the expression of ABCC12 was observed in MDA-MB-231 cells seeded at high density upon treatment with doxorubicin or tamoxifen.
To further corroborate the influence of seeding density on the ABC transporters, we evaluated the protein expression level of a few selected ABC transporters known for their role as drug efflux pumps, in breast cancer cell lines treated with chemotherapeutics. A differential expression of these drug efflux-associated ABC transporters (ABCG2, ABCB1, ABCC1, and ABCC3) at protein levels were observed at different seeding density of the breast cancer cells suggesting that contact inhibition influences the expression of these transporters as reported previously [24]. Low seeding density demonstrated both doxorubicin as well as a tamoxifen-induced marked increase in levels of ABCC1 and ABCC3 in MCF-7 (Fig. 3A, B). Although the mRNA expression of ABCG2 was significantly high, it did not reciprocate at the protein levels which corroborated with the earlier findings suggesting polymorphic variations or nonsense mutations of ABCG2 that decrease membrane protein expression in model cells, despite unchanged mRNA levels [25]. MDA-MB-468 cells cultured at low and high seeding densities showed a marked increase in expression levels of ABCG2 in the presence of doxorubicin whereas ABCC1 and ABCC3 in the presence of tamoxifen (Fig. 3C, D). Similarly, a high expression of ABCG2 and ABCC3 was observed in MDA-MB-231 cells cultured at low seeding density whereas ABCC1 at high seeding density in the presence of doxorubicin (Fig. 3E, F).
Cell density-dependent drug-induced protein expression of the ABC transporters in breast cancer cells. Representative images of western blot analysis demonstrating the increase in expression of selected ABC transporters: ABCG2, ABCB1, ABCC1, and ABCC3 in the presence of doxorubicin as well as tamoxifen at low and high seeding conditions of A MCF-7, C MDA-MB-468, and E MDA-MB-231. Quantification of western blot images performed in breast cancer cells B MCF-7, D MDA-MB-468, and F MDA-MB-231 with the treatment of doxorubicin and tamoxifen as compared with their respective controls at low and high seeding density. Data represented are the results of three independent experiments. (N = 3, *p ≤ 0.05 as compared with respective controls). LDC Low-density Control, LDD Low-density Doxorubicin-treated, LDT Low-density Tamoxifen-treated, HDC High-density Control, HDD High-density Doxorubicin-treated, HDT High-density Tamoxifen-treated
Thus, breast cancer cells at low cell seeding density differentially express ABC transporters that can develop chemoresistance as compared with high seeding conditions. This led us to evaluate the relative efficacies of these drugs at varying cell seeding densities.
Cell density-dependent differential efficacy of chemotherapeutic drugs
Doxorubicin or tamoxifen at low seeding conditions depicted low IC50 values, 0.068 ± 0.001 or 0.18 ± 0.025 µM, respectively as compared with high seeding density conditions (IC50 values, ≥ 100 or 75.65 ± 7.31 µM) in MCF-7 cells (Table ST3). Contrastingly, in MDA-MB-468 cells and MDA-MB-231, a lower efficacy of doxorubicin was observed at low seeding conditions with high IC50 values, 3.4 ± 0.7 µM and 0.18 ± 0.08, respectively as compared with high seeding conditions (low IC50 values, 2.144 ± 0.3 and 0.04 ± 0.001 µM) (Table ST3). Similarly, tamoxifen which has an ER-independent effect on TNBCs, MDA-MB-468, and MDA-MB-231 as reported earlier [18], also exhibited a lower efficacy against these cell types with higher IC50 values at low seeding conditions (MDA-MB-468: 49.88 ± 9.6 µM; MDA-MB-231: 15.52 ± 0.0001 µM) as compared with lower IC50 values at high seeding conditions (MDA-MB-468: 17.29 ± 1.0 µM; MDA-MB-231: 0.80 ± 0.0001 µM) (Table ST3). These findings support our plausible hypothesis that an increased expression of ABC transporters in TNBCs cultured at low seeding densities renders them comparatively more chemoresistant.
ABC transporters inhibition-mediated modulation of cell density-dependent differential efficacy of chemotherapeutic drugs
To substantiate the role of ABC transporters in imparting chemoresistance, we utilized cyclosporine A (CsA), a pan-inhibitor of ABC transporters [26] in the absence or presence of either doxorubicin or tamoxifen at their cell density-dependent IC50 concentrations. The results depicted a CsA-mediated dose-dependent inhibition of breast cancer cell growth. CsA at 5 µM concentration was optimum to induce 50% partial cell survival by the chemotherapeutics in all these cells (Fig. S2A–F). Next, we utilized CsA (5 µM) to evaluate its effect on breast cancer cell sensitization towards doxorubicin or tamoxifen. In MCF-7 at low seeding density, we observed a marked increase in the efficacy of doxorubicin (68–fold decrease in IC50: 0.001 µM) and tamoxifen (5.3–fold decrease in IC50: 0.034 µM) in presence of CsA (Table ST3). Similarly, a higher than 1000–fold decrease in IC50 values of both doxorubicin and tamoxifen was observed in MCF-7 cells at high cell seeding density (Table ST3). In MDA-MB-468 cells at both low and high seeding conditions, we observed CsA-induced marked increase in the efficacy of doxorubicin and tamoxifen with a several-fold decrease in their IC50 values (Table ST3). In MDA-MB-231 cells seeded at low and high densities we observed an increased efficacy of doxorubicin by 69.23 and 23.53–fold decrease in IC50 values, respectively in presence of CsA. CsA-induced increased efficacy of Tamoxifen was also found in MDA-MB-231 cells seeded at low (16.69–fold decrease in IC50) and high densities (13.33–fold decrease in IC50) (Table ST3). Thus, inhibition of ABC transporters sensitizes the breast cancer cells against chemotherapeutics.
Cell density potentiates the doxorubicin - drug accumulation in breast cancer cells
Furthermore, the role of cell seeding density-induced drug efflux ABC transporters expression on the chemo-sensitization of these breast cancer cells was evaluated using a doxorubicin accumulation assay in absence or presence of CsA. As observed in our study, doxorubicin-induced increased expression of drug efflux pumps - ABC transporters at a low cell seeding density correlated with the decreased fluorescence intensity of doxorubicin in the low-density seeding conditions as compared with the high-density seeding conditions, both in luminal MCF-7 (Fig. 4A), and TNBCs MDA-MB-468 (Fig. 4B) and MDA-MB-231 (Fig. 4C) cells suggesting a lower doxorubicin accumulation. Additionally, under both low and high-density cell seeding settings, pan inhibition of these drug efflux—ABC transporters using CsA markedly increased the accumulation of doxorubicin in these cells. (Fig. 4 A–C). Thus, this data confirms the role of cell density-dependent ABC transporters in mediating chemoresistance.
Cell density-dependent enhanced drug accumulation and expression of cell adhesion markers in breast cancer cells in presence of chemotherapeutics. Representative photomicrographs of A MCF-7, B MDA-MB-468, and C MDA-MB-231 cells demonstrated an increase in the doxorubicin-drug accumulation that was potentiated in presence of cyclosporine A. Graphs depicting relative mRNA expression profile of cell adhesion markers such as E-cadherin and N-cadherin in D MCF-7, E MDA-MB-468, and F MDA-MB-231. Low and high seeding conditions led to selectively upregulate the expression of N-Cad in presence of chemotherapeutic drugs at their IC50 concentrations. (Data are represented as mean ± SEM of experiments repeated at least thrice. *p ≤ 0.05 as compared with respective controls). Doxo Doxorubicin. CsA Cyclosporine A, E-Cad E cadherin, and N-Cad N cadherin
Cell density-dependent chemotherapeutics-induced expression of cell adhesion genes
Cell adhesion plays a central role in cellular communication and therefore is instrumental in tumor development and progression. Therefore, we evaluated the mRNA expression levels of E-cadherin (E-cad) and N-cadherin (N-cad) in the breast cancer cells with varying cell density conditions in absence or presence of chemotherapeutics. N-cad expression was significantly increased in MCF-7 (Fig. 4D) and MDA-MB-468 (Fig. 4E) cells in presence of tamoxifen while doxorubicin-induced significant increase in MDA-MB-468 (Fig. 4E) and MDA-MB-231 (Fig. 4F) cells at low seeding density conditions. Our observation correlates with the earlier findings which suggests that cells in confluent cultures are epithelial in nature with tight cell-cell junctions and expresses decreased levels of N-cad [27]. Interestingly, literature also suggests that chemotherapeutics treatment to breast cancer cells induce expression of epithelial-to-mesenchymal transition makers, like N-cad [11]. Thus, the expression of N-cad drives the breast cancer tumorigenesis and disease progression.
Cell density-dependent mammosphere forming efficiency of breast cancer cells
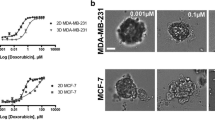
The aggressiveness of breast cancer cells is often assessed by their ability to form mammospheres in-vitro that correlate well with their in-vivo tumorigenic potential [28]. Under low-density seeding conditions, both luminal, MCF-7 (Fig. 5A–B) and TNBC, MDA-MB-468 (Fig. 5C–D) and MDA-MB-231 (Fig. 5E–F) cell lines depicted a higher percentage of sphere-forming efficiency as compared with high-density seeding conditions. However, doxorubicin, and/or tamoxifen significantly decreased the sphere-forming ability in breast cancer cells as compared to their vehicle control (Fig. 5A–F). Furthermore, CsA significantly reduced the chemotherapeutics-mediated sphere-forming efficiency in MCF-7, MDA-MB-468, and MDA-MB-231 cells in the presence of tamoxifen and doxorubicin, respectively at low-density seeding conditions (Fig. 5A–F). Interestingly, both tamoxifen and doxorubicin in presence of CsA significantly decreased the larger (> 150 μm) sphere-forming abilities in MCF-7, MDA-MB-468, and MDA-MB-231 cells, respectively (Fig. 5A–F). This data suggests that inhibition of ABC transporters improves the efficacy of these chemotherapeutics against breast tumorigenesis.
ABC transporter inhibitor increases the sensitization towards chemotherapeutics in abrogating mammosphere forming efficiency of breast cancer cells. Representative photomicrographs and quantification of mammosphere in A, B MCF-7 cells, C, D MDA-MB-468, and E, F MDA-MB-231 demonstrated cyclosporine A-induced decrease in the percent of sphere-forming ability upon treatment with chemotherapeutic drugs (doxorubicin or tamoxifen, at their cell-type specific IC50 concentrations). Statistical significance was determined from repeats of the experiment (n = 4), (Two-way ANOVA, p < 0.05 as compared to *vehicle control, #respective chemotherapeutic drug-treated group). Doxo Doxorubicin, Tam Tamoxifen, CsA Cyclosporine A, SFE Sphere forming efficiency
Discussion
Chemotherapy remains the standard treatment strategy for breast cancer patients. However, most breast cancer patients administered with conventional chemotherapeutic drugs such as doxorubicin or tamoxifen eventually develop resistance leading to metastasis and relapse [29]. Breast cancer cell density varies dramatically throughout cancer progression thereby influencing metastasis and chemoresistance [30]. While breast cancer cells are critical for breast tumor density, there are other cellular and non-cellular components in the breast tissue that influence the breast tumor progression. Tumorigenic extracellular matrix (ECM) alterations and stiffness impact the anticancer drug responses. Therapies that alleviate the ECM stiffness and breakdown, increases the drug penetration into tumor cells, and induction of cancer cell migration, invasion, and angiogenesis [31]. Several intriguing ECM-targeting therapeutics such as fibroblast activation protein (FAP), a membrane-bound serine protease expressed in tumor stroma but not in normal tissue, are being evaluated at a pre-clinical level [32]. Similarly, cellular components like lymphocytes, neutrophils, mast cells, T-reg cells, cancer-associated fibroblasts, mesenchymal stem cells, pericytes, and adipocytes as well as over-expression of various non-cellular components such as growth factors (TGFβ, PDGF, IL-1, BMP, and CXCL-1); receptors (PDGFRβ, CXCR4, EGFR, integrins, and NOTCH); transcription factors (TWIST1 and ID1); and other factor’s (PDK-1 and COX-2) also modulate tumor density [33].
ABC transporters contribute significantly to the chemoresistance of breast cancer [34]. High expression of ABC transporters, ABCG2, ABCCB1, and ABCC1 has been often linked to poor response to chemotherapeutics such as doxorubicin, mitoxantrone, and 5-fluorouracil along with a decrease in overall survival in breast cancer. Doxorubicin resistance has also been linked to the overexpression of ABCC3 along with ABCG2 in breast cancers [35]. In addition, ABCB1 overexpression led to increased CD44 gene expression in breast cancer cells [36]. Also, ABCC3 expression and its functions as a drug resistance marker were reported to be significantly upregulated in non-small cell lung cancer [37]. ABCB1 inhibition led to an increased accumulation of doxorubicin in MDA-MB-435 S cells and induction of apoptosis [38]. Activation of Hippo signaling in pancreatic cancer cells cultured in high-density conditions led to increased mRNA expression of ABCG2, ABCA3, ABCCB4, and ABCC3, rendering them more chemoresistant [39]. The involvement of other family members of these ABC transporters has not yet been explored critically. In this effort, our study demonstrated that luminal and TNBC cells grown at low seeding density led to a differential increase in the mRNA expression of ABC transporters that may contribute to chemoresistance when treated with doxorubicin or tamoxifen. Gujral et al. also reported that differences in drug sensitivity depended on the pancreatic cancer cell density [39]. They demonstrated that pancreatic cancer cell lines grown in more crowded/dense circumstances (40–60% confluence) were substantially less susceptible to gemcitabine than cells cultured in less crowded/dense conditions (10–25% confluence). This shows the differential sensitivity towards these drugs depending upon high and low cell seeding conditions. Although these findings correlated well with our findings in the luminal breast cancer cell line, MCF-7, aggressive TNBC cells cultured at low seeding conditions were less sensitive to doxorubicin or tamoxifen. Interestingly, we also observed a differential expression profile of ABC transporters in these TNBC cells cultured at low seeding density. Corroborating these findings, we conclude that the chemotherapeutics affect differently to breast cancer cells grown in low and high density rendering them chemoresistant. Cyclosporine A, a pan-inhibitor of ABC transporters has been reported to enhance the nuclear uptake of doxorubicin and this broad-spectrum activity may contribute to its clinical efficacy [17, 26]. Similarly, our present study also showed an increased efficacy of chemotherapeutics in presence of CsA in both low and high-density conditions of breast cancer cells.
Overall, in breast cancer cells at low seeding density an increased expression of ABC transporters resulted in higher efflux of the drug or lesser drug accumulation that imparts chemoresistance along with increased expression of cell adhesion molecules. Pan inhibition of these ABC transporters results into an increased sensitization towards chemotherapeutics due to drug accumulation, and improved efficacy of these chemotherapeutics against breast tumorigenesis. In conclusion, our findings have revealed that cell density can modulate the acquisition of chemoresistance in breast cancer cells through differential expression of ABC transporters. Thus, a combinatorial treatment of potent ABC transporter inhibitor along with chemotherapeutics is the way forward to improve chemotherapy response and clinical outcomes in mitigating relapse of breast cancer.
References
Siegel RL, Miller KD, Fuchs HE, Jemal A (2022) Cancer statistics, 2022. CA Cancer J Clin 72(1):7–33. https://doi.org/10.3322/caac.21708
Waks AG, Winer EP (2019) Breast cancer treatment: a review. JAMA 321(3):288–300. https://doi.org/10.1001/jama.2018.19323
Zhou HM, Zhang JG, Zhang X, Li Q (2021) Targeting cancer stem cells for reversing therapy resistance: mechanism, signaling, and prospective agents. Sig Transduct Target Ther 6(1):62. https://doi.org/10.1038/s41392-020-00430-1
Skarping I, Förnvik D, Heide-Jørgensen U, Sartor H, Hall P, Zackrisson S, Borgquist S (2021) Mammographic density as an image-based biomarker of therapy response in neoadjuvant-treated breast cancer patients. Cancer Causes Control: CCC 32(3):251–260. https://doi.org/10.1007/s10552-020-01379-w
Pizzato M, Carioli G, Rosso S, Zanetti R, La Vecchia C (2021) Mammographic breast density and characteristics of invasive breast cancer. Cancer Epidemiol 70:101879. https://doi.org/10.1016/j.canep.2020.101879
Ramamoorthi G, Kodumudi K, Gallen C, Zachariah NN, Basu A, Albert G, Czerniecki BJ (2022) Disseminated cancer cells in breast cancer: Mechanism of dissemination and dormancy and emerging insights on therapeutic opportunities. Semin Cancer Biol 78:78–89. https://doi.org/10.1016/j.semcancer.2021.02.004
Gupta SK, Singh P, Ali V, Verma M (2020) Role of membrane-embedded drug efflux ABC transporters in the cancer chemotherapy. Oncol Rev. https://doi.org/10.4081/oncol.2020.448
Chen J, Wang Z, Gao S, Wu K, Bai F, Zhang Q, Wang H, Ye Q, Xu F, Sun H, Lu Y, Liu Y (2021) Human drug efflux transporter ABCC5 confers acquired resistance to pemetrexed in breast cancer. Cancer Cell Int 21(1):136. https://doi.org/10.1186/s12935-021-01842-x
Giddings EL, Champagne DP, Wu MH, Laffin JM, Thornton TM, Valenca-Pereira F, Rincon M (2021) Mitochondrial ATP fuels ABC transporter-mediated drug efflux in cancer chemoresistance. Nat Commun 12(1):1–19. https://doi.org/10.1038/s41467-021-23071-6
Dean M, Hamon Y, Chimini G (2001) The human ATP-binding cassette (ABC) transporter superfamily. J Lipid Res 42(7):1007–1017. https://doi.org/10.1016/S0022-2275(20)31588-1
Saxena M, Stephens MA, Pathak H, Rangarajan A (2011) Transcription factors that mediate epithelial–mesenchymal transition lead to multidrug resistance by upregulating ABC transporters. Cell Death Dis 2(7):e179–e179. https://doi.org/10.1038/cddis.2011.61
Leonard GD, Fojo T, Bates SE (2003) The role of ABC transporters in clinical practice. Oncologist 8(5):411–424. https://doi.org/10.1634/theoncologist.8-5-411
Xiao H, Zheng Y, Ma L, Tian L, Sun Q (2021) Clinically-relevant ABC transporter for anti-cancer drug resistance. Front Pharmacol 12:648407. https://doi.org/10.3389/fphar.2021.648407
Manupati K, Dhoke NR, Debnath T, Yeeravalli R, Guguloth K, Saeidpour S, Das A (2017) Inhibiting epidermal growth factor receptor signalling potentiates mesenchymal–epithelial transition of breast cancer stem cells and their responsiveness to anticancer drugs. FEBS J 284(12):1830–1854. https://doi.org/10.1111/febs.14084
Yeeravalli R, Kaushik K, Das A (2021) TWIST1-mediated transcriptional activation of PDGFRβ in breast cancer stem cells promotes tumorigenesis and metastasis. Biochimica et Biophysica Acta (BBA)-Mol Basis Dis 1867(7):166141. https://doi.org/10.1016/j.bbadis.2021.166141
Reddy L, Dharmabalan ST, Manupati K, Yeeravalli R, Vijay LD, Donthiboina K, Das A (2020) Concise synthesis of 1, 1-diarylvinyl sulfones and investigations on their anti-proliferative activity via tubulin inhibition. Anticancer Agents Med Chem (Formerly Current Medicinal Chemistry-Anti-Cancer Agents) 20(12):1469–1474. https://doi.org/10.2174/1871520620666200423075630
Sampson A, Peterson BG, Tan KW, Iram SH (2019) Doxorubicin as a fluorescent reporter identifies novel MRP1 (ABCC1) inhibitors missed by calcein-based high content screening of anticancer agents. Biomed Pharmacother 118:109289. https://doi.org/10.1016/j.biopha.2019.109289
Manupati K, Debnath S, Goswami K, Bhoj PS, Chandak HS, Bahekar SP, Das A (2019) Glutathione S-transferase omega 1 inhibition activates JNK‐mediated apoptotic response in breast cancer stem cells. FEBS J 286(11):2167–2192. https://doi.org/10.1111/febs.14813
Singh D, Deshmukh RK, Das A (2021) SNAI1-mediated transcriptional regulation of epithelial-to-mesenchymal transition genes in breast cancer stem cells. Cell Signal 87:110151. https://doi.org/10.1016/j.cellsig.2021.110151
Lee HH, Bellat V, Law B (2017) Chemotherapy induces adaptive drug resistance and metastatic potentials via phenotypic CXCR4-expressing cell state transition in ovarian cancer. PLoS ONE 12(2):e0171044. https://doi.org/10.1371/journal.pone.0171044
Madden EC, Gorman AM, Logue SE, Samali A (2020) Tumour cell secretome in chemoresistance and tumour recurrence. Trends Cancer 6(6):489–505. https://doi.org/10.1016/j.trecan.2020.02.020
Muriithi W, Macharia LW, Heming CP, Echevarria JL, Nyachieo A, Niemeyer Filho P, Neto VM (2020) ABC transporters and the hallmarks of cancer: roles in cancer aggressiveness beyond multidrug resistance. Cancer Biol Med 17(2):253. https://doi.org/10.20892%2Fj.issn.2095-3941.2019.0284
Citron ML (2008) Dose-dense chemotherapy: principles, clinical results and future perspectives. Breast Care 3(4):251–255. https://doi.org/10.1159/000148914
Fan D, Beltran P, Wang Y, Bucana C, Yoon S, Deguzman A, Fidler I (1996) Cell density-dependent regulation of mdr-1 gene expression in murine colon cancer cells. Int J Oncol 9(5):865–878. https://doi.org/10.3892/ijo.9.5.865
Furukawa T, Wakabayashi K, Tamura A, Nakagawa H, Morishima Y, Osawa Y, Ishikawa T (2009) Major SNP (Q141K) variant of human ABC transporter ABCG2 undergoes lysosomal and proteasomal degradations. Pharm Res 26(2):469–479. https://doi.org/10.1007/s11095-008-9752-7
Hembruff SL, Laberge ML, Villeneuve DJ, Guo B, Veitch Z, Cecchetto M, Parissenti AM (2008) Role of drug transporters and drug accumulation in the temporal acquisition of drug resistance. BMC Cancer 8(1):1–16. https://doi.org/10.1186/1471-2407-8-318
Maeda M, Johnson KR, Wheelock MJ (2005) Cadherin switching: essential for behavioral but not morphological changes during an epithelium-to-mesenchyme transition. J Cell Sci 118(5):873–887. https://doi.org/10.1242/jcs.01634
Manupati K, Yeeravalli R, Kaushik K, Singh D, Mehra B, Gangane N, Das A (2021) Activation of CD44-Lipoprotein lipase axis in breast cancer stem cells promotes tumorigenesis. Biochim et Biophys Acta (BBA)-Mol Basis Dis 1867(11):166228. https://doi.org/10.1016/j.bbadis.2021.166228
Bai X, Ni J, Beretov J, Graham P, Li Y (2018) Cancer stem cell in breast cancer therapeutic resistance. Cancer Treat Rev 69:152–163. https://doi.org/10.1016/j.ctrv.2018.07.004
Sharif GM, Wellstein A (2015) Cell density regulates cancer metastasis via the Hippo pathway. Future Oncol 11(24):3253–3260. https://doi.org/10.2217/fon.15.268
Winkler J, Abisoye-Ogunniyan A, Metcalf KJ, Werb Z (2020) Concepts of extracellular matrix remodelling in tumour progression and metastasis. Nat Commun 11(1):1–19. https://doi.org/10.1038/s41467-020-18794
Zboralski D et al (2022) Preclinical evaluation of FAP-2286 for fibroblast activation protein targeted radionuclide imaging and therapy. Eur J Nucl Med Mol Imaging 49:3651–3667. https://doi.org/10.1007/s00259-022-05842-5
D’Andrea MR, Cereda V, Coppola L, Giordano G, Remo A, De Santis E (2021) Propensity for early metastatic spread in breast cancer: role of tumor vascularization features and tumor immune infiltrate. Cancers 13(23):5917. https://doi.org/10.3390/cancers13235917
Spitzwieser M, Pirker C, Koblmüller B, Pfeiler G, Hacker S, Berger W, Cichna-Markl M (2016) Promoter methylation patterns of ABCB1, ABCC1 and ABCG2 in human cancer cell lines, multidrug-resistant cell models and tumor, tumor-adjacent and tumor-distant tissues from breast cancer patients. Oncotarget 7(45):73347. https://doi.org/10.18632%2Foncotarget.12332
Balaji SA, Udupa N, Chamallamudi MR, Gupta V, Rangarajan A (2016) Role of the drug transporter ABCC3 in breast cancer chemoresistance. PLoS ONE 11(5):e0155013. https://doi.org/10.1371/journal.pone.0155013
Tsou SH, Chen TM, Hsiao HT, Chen YH (2015) A critical dose of doxorubicin is required to alter the gene expression profiles in MCF-7 cells acquiring multidrug resistance. PLoS ONE 10(1):e0116747. https://doi.org/10.1371/journal.pone.0116747
Zhao Y, Lu H, Yan A, Yang Y, Meng Q, Sun L, Cai L (2013) ABCC3 as a marker for multidrug resistance in non-small cell lung cancer. Sci Rep 3(1):1–6. https://doi.org/10.1038/srep03120
Sims JT, Ganguly SS, Bennett H, Friend JW, Tepe J, Plattner R (2013) Imatinib reverses doxorubicin resistance by affecting activation of STAT3-dependent NF-κB and HSP27/p38/AKT pathways and by inhibiting ABCB1. PLoS ONE 8(1):e55509. https://doi.org/10.1371/journal.pone.0055509
Gujral TS, Kirschner MW (2017) Hippo pathway mediates resistance to cytotoxic drugs. Proc Natl Acad Sci 114(18):E3729–E3738. https://doi.org/10.1073/pnas.1703096114
Acknowledgements
AD acknowledges institutional funding by CSIR-IICT. The fellowship provided by DST INSPIRE to SS is gratefully acknowledged. (Manuscript Communication number: IICT/Pubs./2022/011).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
This article does not contain any studies with human participants or animals performed by any of the authors.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Shivhare, S., Das, A. Cell density modulates chemoresistance in breast cancer cells through differential expression of ABC transporters. Mol Biol Rep 50, 215–225 (2023). https://doi.org/10.1007/s11033-022-08028-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11033-022-08028-2