Abstract
Women experience greater longevity than men, but have poorer health, although sex differences vary across health measures and geographical regions. We aim to examine sex differences in Activities of Daily Living (ADL) and Instrumental Activities of Daily Living (IADL) over age across European regions in a cross-sectional setting including 51,292 men and 62,007 women aged 50+ from a pooled sample of waves 1 (2004–2005) to 6 (2015) in the Survey of Health, Ageing and Retirement in Europe. ADL and IADL were dichotomised into no limitations and at least one limitation. Binomial regression models were used to estimate absolute and relative sex differences. Women had higher risk than men of ADL limitations (RR = 1.21, 95% CI 1.16; 1.27) and IADL limitations (RR = 1.54, 95% CI 1.48; 1.60), corresponding to risk differences of 1.3% and 5.7%, respectively. When we stratified by age groups and regions, sex differences in ADL were found in all age groups in Southern Europe, in the age groups 65–79 years and 80+ years in Western and Eastern Europe, and from the age of 80 in Northern Europe. For IADL, sex differences were found in all age groups in the four European regions, except from ages 50–64 in Eastern Europe. The absolute sex differences increased with age in all European regions. In conclusion, our results lend support for the male–female health survival paradox by showing that European women have higher risk of ADL and IADL limitations than European men and that sex differences increase with advancing age.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The reduced mortality at older ages has led to an increased life expectancy and a higher proportion of the oldest people (Christensen et al. 2009; Oeppen and Vaupel 2002). At the same time, the ageing population entails a growing disease burden (Prince et al. 2015) with more people having physical limitations (Fedarko 2011). Women live longer than men (Barford et al. 2006); however, female disadvantages have been found for several measures of health: Women tend to have lower grip strength, higher prevalence of frailty and worse self-rated health than men (Ahrenfeldt et al. 2019; Crimmins et al. 2011; Herr et al. 2018; Jeune et al. 2006; Oksuzyan et al. 2010b). The phenomenon that women outlive men, but at the same time suffer from more disabilities and are physically weaker, is denoted the male–female health survival paradox (Oksuzyan et al. 2010a). Proposed explanations for this paradox are biological factors such as hormonal, autoimmune and genetic factors as well as behavioural and social factors including sex differences in health-reporting behaviour and risk-taking behaviours, such as smoking, drinking and hazardous driving, between men and women (Oksuzyan et al. 2010a; Schünemann et al. 2017).
Due to the growing proportion of elderly, it is of major interest to examine how men and women differ in terms of functional health. Activities of Daily Living (ADL) and Instrumental Activities of Daily Living (IADL) are measures of functional ability. ADLs are defined as routine everyday tasks like eating and bathing, while IADLs are defined as tasks that are considered important to lead an independent life in society, e.g. shopping and managing money (Katz et al. 1963; Lawton and Brody 1969; Noelker and Browdie 2014). Even though recent years have seen divergent trends in the prevalence of ADL and IADL limitations in Western countries (Ahrenfeldt et al. 2018a; Lin et al. 2012; Rasmussen et al. 2017), the previous studies suggest that ADL and IADL limitations increase with age (Bleijenberg et al. 2017; Lin et al. 2012). In the literature, women are generally reported to have more limitations than men (Crimmins et al. 2011; Oksuzyan et al. 2010b; Wheaton and Crimmins 2016). Explanations for sex differences in ADL and IADL are manifold and reflect a complex interplay between biological and environmental factors (Schon et al. 2011).
In general, sex differences vary across health measures, time periods and geographical regions (Crimmins et al. 2011; Oksuzyan et al. 2010a, b; Rasmussen et al. 2017). Investigation of sex differences across different populations may provide knowledge about whether differences between men and women are universal or more region-specific, and cross-country comparisons may provide useful information about the generalisability of the research findings on sex differences in health (Crimmins et al. 2011; Wheaton and Crimmins 2016). To date, little is known about the direction and magnitude of the sex differences in disability (Wheaton and Crimmins 2016), and to our knowledge, no studies have so far investigated the absolute and relative sex differences in ADL and IADL across age groups and regions in a European setting. The aim of this study is therefore to examine age-related and cross-national sex differences in ADL and IADL among middle-aged and elderly Europeans in a large, pooled cross-sectional setting of people who are participated in the Survey of Health, Ageing and Retirement in Europe (SHARE) between 2004 and 2015. We hypothesise that women have more ADL and IADL limitations than men at any given age and that sex differences will increase with age as only the strongest men survive to older ages (Austad and Fischer 2016).
Methods
Study population
The data in this study came from SHARE, a representative survey of Europeans aged 50 and older (Börsch-Supan et al. 2013). All data were collected in the homes of the respondents through computer-assisted personal interviews (Alcser et al. 2005). SHARE also included nursing home interviews, although they were not a part of wave 1. A proxy respondent, usually a family member, a household member, a neighbour or another person related to the social network, was allowed to answer if the respondent was unable to complete the interview due to physical or mental health limitations (Börsch-Supan et al. 2013). To compensate for dropouts and to maintain the representation of younger age cohorts, refreshment samples were drawn regularly (Börsch-Supan et al. 2013). Response rates varied considerably between the countries: In wave 1, Belgium had the lowest household response rate (40.3%) and France had the highest (97.6%) (Bergmann et al. 2017). To compensate for unequal selection probabilities between the countries, SHARE provides sampling weights (Börsch-Supan et al. 2013). For a thorough review of the SHARE study design and data collection procedures, please see Börsch-Supan et al. (2013) and the SHARE Methodology (Alcser et al. 2005).
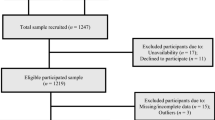
We performed a large cross-sectional analysis of men and women aged 50+ years from 20 European countries with pooled data from participants in waves 1 (2004–2005), 2 (2006–2007), 4 (2011), 5 (2013) and 6 (2015), where health data were available. Because no significant sex-by-wave interactions were found, i.e. differences between men and women did not differ by waves, we pooled all waves of SHARE. This gave us a larger sample size and enabled us to include a larger sample of the oldest people. We excluded people with missing birth dates (n = 19) and missing cross-sectional individual weights (n = 385). Participation by wave for the individual countries is shown in Supplementary Table 1.
ADL and IADL
ADL and IADL were self-reported scores of current functional limitations recorded over a period of more than 3 months. The ADL scale by Katz et al. (1963) consisted of six tasks: dressing, walking, bathing, eating, getting in or out of bed, and using the toilet. The IADL scale, which originated from Lawton and Brody (1969), covered seven instrumental activities: using a map, preparing a hot meal, shopping, using a telephone, taking medications, doing house- or garden work, and managing money. In this study, ADL and IADL were dichotomised into no limitations vs. at least one limitation.
Covariates
Age was divided into three intervals: 50–64 years, 65–79 years and 80+ years. The last interval, age 80+ years, was open ended. Based on welfare regimes as proposed by Ferrera (1996) and in line with the previous studies (Ahrenfeldt et al. 2018b, 2019; Eikemo et al. 2008; Horackova et al. 2019; Jerez-Roig et al. 2018), we grouped the 20 countries into four geographical regions: Northern Europe including Denmark and Sweden; Western Europe containing Austria, Germany, France, the Netherlands, Switzerland, Belgium, Ireland and Luxembourg; Southern Europe including Spain, Italy, Greece and Portugal; and Eastern Europe containing Czech Republic, Poland, Hungary, Slovenia, Estonia and Croatia. Educational level was assessed as the highest self-reported educational achievement through the international comparable “International Standard Classification of Education” (ISCED) classified into two levels: low (ISCED levels 0, 1 and 2) and medium/high (ISCED levels 3–6.
Statistical analysis
Sex differences in ADL and IADL were investigated using binomial regression models with robust clustered standard errors to take the non-independence of multiple observations from the same individual into account, estimating absolute (presented as percentage point differences) and relative risk differences of having any disabilities. While the absolute differences are most directly interpretable with respect to individual risk in the investigated population, we decided to also report the relative risks as these might facilitate comparisons with future studies of populations with different risk profiles. When using the term sex differences in our results, we refer to the statistically significant differences between men and women. We evaluated the fit of the model by the specification link test as well as by examining the probabilities predicted from the model and found an adequate model specification and reasonable, predicted probabilities. In all analyses, ADL and IADL were divided into no limitations and at least one limitation. The overall analyses were adjusted for age group, European region and wave. Furthermore, we carried out separate analyses for each age group and region, because significant interactions for sex by age and sex by region were found. Moreover, we investigated whether sex differences differed between age groups and European regions. To investigate whether education could explain some of the sex differences, we estimated a model also adjusting for this variable. This rationale was chosen as we wanted to explore whether education was mediating the differences between men and women in the specific regions. In all analyses, the cross-sectional individual weights supplied by SHARE were applied. Stata version 14.2 was used to analyse data.
Results
In the present study, 51,292 men (45.3%) and 62,007 (54.7%) women were included, corresponding to 244,258 observations. Mean age of the participants was 66.2 years (SD = 9.7) for men and 66.3 years (SD = 10.3) for women (Table 1). Men were slightly more dependent on help from a proxy than women (2.7% vs. 2.2%). Overall, more men than women had a medium or high education (60.9% vs. 52.7%). More women than men reported having ADL (12.8% vs. 10.4%) and IADL limitations (21.1% vs. 13.4%) with Southern and Eastern Europe having the highest proportion of limitations (Table 1).
Figure 1 and Table 2 show the absolute and relative sex differences in ADL and IADL over age groups and European regions. Furthermore, Fig. 1 shows the proportion of people with at least one ADL and IADL limitation. As demonstrated (Fig. 1a, b), the proportion of people with ADL and IADL limitations increased with age for both sexes. The proportion of ADL limitations was similar between men and women in the youngest age group (50–64 years), whereas women had more ADL limitations than men at ages 65–79 years and 80+ years. For IADL, women had more limitations than men in all age groups.
Top panel: Proportion of men and women with limitations of Activities of Daily Living (ADL) and Instrumental Activities of Daily Living (IADL) by sex and age groups. Middle and bottom panels: Absolute and relative sex differences in ADL and IADL with 95% confidence intervals by age groups and European regions
When investigating sex differences in ADL in the total study population, we found that 1.3% more women than men had at least one limitation, corresponding to a risk ratio (RR) of 1.21 (95% CI 1.16, 1.27) (Table 2). When investigating risk differences (RD) in the three age groups separately, we found no differences in the youngest age group (RD = 0.001; 95% CI − 0.005, 0.007), but in the age groups 65–79 years (RD = 0.031; 95% CI 0.023, 0.039) and 80+ years (RD = 0.089; 95% CI 0.066, 0.112), respectively, 3% and 9% more women than men had at least one ADL limitation (Fig. 1c, Table 2). The absolute sex difference in ADL increased between age groups (Supplementary Table 2). The relative differences showed a similar pattern with no sex difference in the age group 50–64 years (RR = 1.00, 95% CI 0.90; 1.11), but with differences in the age groups 65–79 years (RR = 1.29; 95% CI 1.21, 1.38) and 80+ years (RR = 1.29; 95% CI 1.20, 1.38) (Fig. 1e, Table 2); however, a significant increase in the relative sex differences in ADL was only found between the youngest and middle age groups (Supplementary Table 2).
In Southern Europe, women had more limitations than men in all age groups, with the largest absolute sex difference in the age group 80+ years (RD = 0.143; 95% CI 0.104, 0.182). For Western and Eastern Europe, absolute sex differences were present at ages 65–79 years (Western: RD = 0.017; 95% CI 0.005, 0.029; Eastern: RD = 0.043; 95% CI 0.017, 0.069) and 80+ years (Western: RD = 0.056; 95% CI 0.021, 0.091; Eastern: RD = 0.098; 95% CI 0.035, 0.161), whereas in Northern Europe, women had higher risk of ADL limitations than men, but only in the oldest age group (RD = 0.040; 95% CI 0.003, 0.077) (Fig. 1c, Table 2). The absolute sex differences increased with advancing age in all regions with few exceptions. A similar pattern of sex differences in the four European regions was found for the relative differences (Fig. 1e, Table 2), but only with increasing sex differences in ADL from the youngest to the middle age group in Western and Eastern Europe (Supplementary Table 2). When testing sex differences between European regions with Northern Europe as the reference group (Supplementary Table 3), sex differences in ADL were overall significantly larger in Southern Europe both in absolute and in relative terms. In the age group 50–64 years, no cross-regional difference in ADL between men and women was found, but in the age groups 65–79 years and 80+ years, sex differences in ADL between men and women in Southern Europe were significantly larger than in Northern Europe. At ages 65–79 years, differences were found between Northern and Eastern Europe as well (Supplementary Table 3).
When examining sex differences in IADL in the total study population, results showed that 5.7% more women than men had at least one limitation, corresponding to an RR of 1.54 (95% CI 1.48, 1.60) (Table 2). When investigating absolute differences in the three age groups separately, differences were found in all age groups, demonstrating that more women than men had at least one IADL limitation, corresponding to 3.5%, 9.2% and 17.2%, respectively (Fig. 1d, Table 2). The absolute sex differences increased between age groups (Supplementary Table 2). The relative differences showed a similar pattern with sex differences at ages 50–64 years (RR = 1.55, 95% CI 1.41; 1.69), 65–79 years (RR = 1.69; 95% CI 1.60, 1.78) and 80+ years (RR = 1.43; 95% CI 1.36, 1.50) (Fig. 1f, Table 2); however, contrary to the absolute sex differences, a decrease in the relative sex differences was found between the middle and the oldest age groups (Fig. 1f, Supplementary Table 2).
When investigating sex differences in the four European regions separately, we found that women had higher risk of IADL limitations than men in all age groups in the four European regions except for Eastern Europe at ages 50–64 years (Fig. 1d, f, Table 2). The absolute sex differences increased with age in most regions with the largest sex difference in Southern Europe in the age group 80+ years, where 22% more women than men had at least one IADL limitation (RD = 0.216; 95% CI 0.177, 0.256). For the relative sex differences, a similar pattern was found with sex differences in almost all age groups in all regions (Fig. 1d, f, Table 2), but there was no consistent pattern over age. Moreover, we found that in some regions, sex differences were increasing with age, whereas in other regions they were decreasing. The cross-regional comparison of the sex differences in IADL showed overall significantly larger sex differences in Southern Europe compared with Northern Europe, corresponding to what was found for the sex differences in ADL. Also, larger sex differences in Southern than in Northern Europe were seen in the age groups 65–79 years and 80+ years, while the sex differences in Eastern Europe were significantly larger than in Northern Europe in the age group 50–64 years, also for the overall relative sex differences in IADL (Supplementary Table 3).
When taking educational level into account, we found that the results for both ADL and IADL were overall similar to the main results with some exceptions for ADL. The sex difference in Northern Europe in the oldest age group disappeared, resulting in no sex differences in any age group in this region. Also, for Western Europe, most of the sex differences in ADL disappeared with results showing higher risk for men in the youngest age group, but a higher absolute risk for women in the oldest age group (Supplementary Table 4).
Discussion
The present study of age-related sex differences in ADL and IADL demonstrated that the proportion of people with at least one ADL and IADL limitation increased with age for both sexes. In the total study population, 1.3% more women than men had at least one ADL limitation, corresponding to an RR of 1.21, whereas for IADL, 5.7% more women than men had at least one limitation, corresponding to an RR of 1.54. When stratifying by age group and region, we found significant sex differences in ADL in all age groups in Southern Europe, in age groups 65–79 and 80+ in Western and Eastern Europe and from age 80 in Northern Europe. For IADL, sex differences were present in all age groups in the four European regions, except from ages 50–64 in Eastern Europe. The absolute and relative sex differences showed overall similar patterns; however, the absolute sex differences in ADL and IADL increased with age in all European regions, whereas the relative differences remained almost constant over age groups.
The overall female disadvantage in ADL and IADL was in line with the previous studies (Crimmins et al. 2011, 2019; Murtagh and Hubert 2004; Oksuzyan et al. 2010b). A recent study by Crimmins et al. (2019) that compared results from individual-level survey data from 17 countries in Europe, North America and Asia found that the likelihood of having difficulties in IADL was about twofold higher for women than for men around the world. In contrast, sex differences in ADL limitations were found in 10 out of 17 countries with an overall OR of 1.3. We found similar results with an overall RR for IADL of 1.5 and an overall RR for ADL of 1.2. In turn, we estimated risk differences showing that 5.6% more women than men had at least one IADL limitation and that 1.3% more women than men had at least one ADL limitation. These results agree with findings from earlier studies of sex differences in physical function showing that women have lower grip strength measures, slower gait speed, take longer to rise from a sitting position and have worse balance compared with men (Ahrenfeldt et al. 2018b; Merrill et al. 1997; Oksuzyan et al. 2010b; Wheaton and Crimmins 2016). ADL and IADL require a range of physically demanding capabilities, and in addition, IADL requires cognitive capacity (Barberger-Gateau and Fabrigoule 1997; Bleijenberg et al. 2017). Thus, women’s generally weaker physique compared with men might influence sex differences in ADL and IADL (Jeune et al. 2006; Wheaton and Crimmins 2016), while a more rapid loss of cognitive function with age for women than for men (Ahrenfeldt et al. 2018b) may add to the explanation of why the gender gap is larger for IADL than for ADL in the oldest age groups.
This study showed that sex differences in ADL and IADL increased with age, thus confirming findings from other studies (Oksuzyan et al. 2010b; Serrano-Alarcón and Perelman 2017). A widening of the sex gap with increasing age may be consistent with a survival effect, which leaves the healthiest men in the sample (Austad and Fischer 2016), and this is in line with what we hypothesised based on the male–female health survival paradox. We expected this survival effect to continue into the oldest age groups, which was also the case for the absolute sex differences. The age pattern for the relative sex differences, however, was less clear. In the age groups 65–79 years and 80+ years, the relative sex difference in ADL was constant, whereas the relative difference in IADL decreased. This decrease in the risk ratio for IADL might be explained by an increasing proportion of limitations for both men and women, which may lead to a smaller relative risk even though a higher proportion of women than men had limitations in the oldest age groups (Noordzij et al. 2017).
In line with the previous studies on several health traits such as grip strength, cognitive function, comorbidity and self-rated health (Ahrenfeldt et al. 2018b, 2019; Dahlin and Härkönen 2013; Jeune et al. 2006), our results suggested a North–South gradient in health with the most pronounced sex differences in Southern Europe. In agreement with earlier studies (Chatterji et al. 2015; Jerez-Roig et al. 2018; Wahrendorf et al. 2013), we also demonstrated the highest prevalence of disability in Eastern and Southern Europe. Jerez-Roig et al. (2018), based on wave six of SHARE, found that disabled older adults in Southern Europe suffer more commonly from psychosocial and cognitive issues including low cognitive performance, isolation and low quality of life, although they had the lowest rate of hospitalisations perhaps due to greater family support in the Mediterranean countries. These studies lend support for the hypothesis that countries with less-developed social policies and more pronounced socioeconomic inequalities have higher disability levels, whereas in less-developed or more traditional societies, gender roles tend to be more pronounced (Wheaton and Crimmins 2016). Women in these societies may be less likely to smoke and drink, but, on the other hand, in societies with high inequality and traditional gender roles, women tend to have lower education (Buchmann et al. 2008) and less attachment to the labour market (Bird and Fremont 1991), and this may influence the sex differences in functional disability. This was demonstrated by Van Oyen et al. (2010) who studied the relationship between life expectancy, activity limitations and macro-level structural indicators in Europe. They found that overall in Europe, sex differences in years lived with activity limitations were associated with gross domestic product, expenditure on elderly care and income differences between men and women. In this study, controlling for education slightly reduced differences in ADL between men and women in Northern and Western Europe; however, it did not change the significance of the overall results. Earlier studies (Wheaton and Crimmins 2016; Wray and Blaum 2001) have found that controlling for education and marital status explains some, but not all, of the differences in disabilities between men and women. This suggests that there is a disadvantage in ADL and IADL for women that is unrelated to socioeconomic conditions.
Two recent SHARE studies have investigated sex differences in health based on the same study population as in this study. The most recent study based on the Comorbidity Index and the Frailty Phenotype (Ahrenfeldt et al. 2019) found that women are more frail and have slightly more comorbidity than men with the most pronounced sex differences in Southern and Eastern Europe. The other study (Ahrenfeldt et al. 2018b) found higher cognitive scores and grip strength measures in Northern than in Southern Europe, but with contrasting directions of sex differences in cognition between North and South. Women had better cognitive function than men in most age groups in Northern Europe, but worse cognitive function in Southern Europe in line with the previous literature (Weber et al. 2014). The gender gap in cognitive function was to some extent explained by differences in education, height and chronic diseases (Ahrenfeldt et al. 2018b). Although sex differences in life expectancy are larger in Southern than in Northern Europe (Ahrenfeldt et al. 2019; Van Oyen et al. 2010), e.g. due to the higher prevalence of smokers among men than among women (Eurostat 2019), which may result in a selection effect with the strongest men surviving to the oldest ages, it is likely that several other factors such as frailty, comorbidity, lower physical strength and worse cognitive function among women in Southern Europe also influence ADL and IADL.
Two hypotheses: differential “exposure” and differential “vulnerability” have been stated to explain the role of social factors in gender–health associations (Kaneda et al. 2009). The differential exposure hypothesis suggests that due to the different access to material resources and other social conditions of life, men and women are exposed to different levels of risk, resulting in different health outcomes (Arber and Cooper 1999; Denton et al. 2004; Ross and Bird 1994). In a large study based on the Canadian National Population Health Survey from 1994 to 1995, Denton et al. found that although women on average have more social support than men, they are generally more likely to live alone or as single parents, to carry a double day (i.e. working full- or part-time and caring for a family), to work in the home for taking care of the family and to work in lower status occupations (Denton et al. 2004). Furthermore, they found important gender differences in the psychosocial variables, with women experiencing more stressful life events and more chronic stress at the domains of, for example, child and family health, which may translate into poorer functioning and greater disability. On the other hand, men were more likely to smoke and drink and to be overweight compared with women (Denton et al. 2004). However, gender differences in health were only slightly reduced by controlling for structural, behavioural and psychosocial determinants of health lending more support for the differential vulnerability hypothesis (Denton et al. 2004), which states that men and women react differently to various conditions of life and therefore differs in their vulnerability to risk factors (McDonough and Walters 2001). Some evidence shows that the association between BMI and mobility difficulty is worse for women than for men (Wray and Blaum 2001) and that a higher proportion of women with arthritis developed an ADL or IADL disability compared with men with this disease (Peek and Coward 1999) supporting the differential vulnerability hypothesis (Denton et al. 2004). In agreement, our findings of consistently greater disabilities among women than among men in all European regions may support the vulnerability hypothesis, although the cross-regional differences with the largest female disadvantage in ADL and IADL in Southern Europe may also lend support for the differential exposure hypothesis.
This study has several strengths. It included 113,299 individuals corresponding to 244,258 interviews providing great power to the statistical analyses, which included both absolute and relative sex differences. Moreover, the strict data collection procedures in SHARE with an ex ante harmonised design permit cross-country comparisons (Börsch-Supan et al. 2013). Finally, we included elderly and very old individuals for whom data are sparser (Christensen et al. 2013).
A limitation in SHARE is the low participation rates, potentially leading to selection bias. However, the calibrated weights in SHARE are designed to account for this problem (Börsch-Supan et al. 2013). Another limitation in SHARE is the self-reporting, which could potentially result in response bias. Although self-reports generally agree with objective measures of common medical conditions (Bergmann et al. 1998; Okura et al. 2004), sex differences in ADL and IADL may be affected by gender-specific reporting attitudes if more health-conscious women overstate their health deficits, while more status-concerned men underreport them (Schünemann et al. 2017), resulting in an overestimation of sex differences in self-reported measures. Among the IADL items are activities that are traditionally regarded as either male tasks (i.e. using a map) or female tasks (i.e. cooking). Sheehan and Tucker-Drob (2017) found that males were more likely not to do the IADL activities for reasons unrelated to health limitations, while Light and Thigpen (2017) found that males’ perception of a given IADL item was correlated with their performance of that activity. This could indicate that males may underreport certain tasks not because of actual limitations but due to a negative perception of the task leading to an overestimation of the sex differences in IADL. However, Case and Paxson (2005) showed that differences in self-assessed health between men and women can be explained by differences in the distribution of the health conditions that they face, indicating no gender bias in reporting. Moreover, a recent study showed overall similar findings across both self-reported and objective measures, suggesting that sex differences are not explained by reporting differences (Wheaton and Crimmins 2016). Due to the large amount of missing information on mortality in SHARE, longitudinal analyses would not be reliable, and thus, it was not possible to show the longitudinal trajectories of ADL and IADL. Future studies with the possibilities of taking mortality into account would help to better explain the increasing sex gap with age. However, this study contributes to our understanding of sex differences in ADL and IADL as it is, we believe, the largest cross-sectional study of age-related sex differences to date with inclusion of multiple countries and very old participants.
In summary, our results confirm that European women have higher risk of ADL and IADL limitations than European men. Despite the cross-regional differences in ADL and IADL with the largest sex differences in Southern Europe, our results show a clear pattern of a female disadvantage that is increasing with advancing age in all European regions, in agreement with what we expected based on the male–female health survival paradox.
References
Ahrenfeldt LJ, Lindahl-Jacobsen R, Rizzi S, Thinggaard M, Christensen K, Vaupel JW (2018a) Comparison of cognitive and physical functioning of Europeans in 2004–2005 and 2013. Int J Epidemiol. https://doi.org/10.1093/ije/dyy094
Ahrenfeldt LJ, Scheel-Hincke LL, Kjaergaard S, Möller S, Christensen K, Lindahl-Jacobsen R (2018b) Gender differences in cognitive function and grip strength: a cross-national comparison of four European regions. Eur J Public Health. https://doi.org/10.1093/eurpub/cky266
Ahrenfeldt LJ, Möller S, Thinggaard M, Christensen K, Lindahl-Jacobsen R (2019) Sex differences in comorbidity and frailty in Europe. Int J Public Health 64(7):1025–1036. https://doi.org/10.1007/s00038-019-01270-9
Alcser KH et al (2005) The survey of health, aging, and retirement in europe—methodology. Mannheim Mannheim Research Institute for the Economics of Aging (MEA), Mannheim
Arber S, Cooper H (1999) Gender differences in health in later life: the new paradox? Soc Sci Med 48:61–76
Austad SN, Fischer KE (2016) Sex differences in lifespan. Cell Metab 23:1022–1033. https://doi.org/10.1016/j.cmet.2016.05.019
Barberger-Gateau P, Fabrigoule C (1997) Disability and cognitive impairment in the elderly. Disabil Rehabil 19:175–193. https://doi.org/10.3109/09638289709166525
Barford A, Dorling D, Smith GD, Shaw M (2006) Life expectancy: women now on top everywhere: during 2006, even in the poorest countries, women can expect to outlive men. BMJ 332:808. https://doi.org/10.1136/bmj.332.7545.808
Bergmann MM, Byers T, Freedman DS, Mokdad A (1998) Validity of self-reported diagnoses leading to hospitalization: a comparison of self-reports with hospital records in a prospective study of American adults. Am J Epidemiol 147:969–977. https://doi.org/10.1093/oxfordjournals.aje.a009387
Bergmann M, Kneip T, De Luca G, Scherpenzeel A (2017) Survey participation in the Survey of Health, Ageing and Retirement in Europe (SHARE), Wave 1-6. SHARE Working Paper Series 31-2017. Munich Center for the Economics of Aging (MEA), Munich
Bird CE, Fremont AM (1991) Gender, time use, and health. J Health Soc Behav 32:114–129
Bleijenberg N, Zuithoff NPA, Smith AK, de Wit NJ, Schuurmans MJ (2017) Disability in the individual ADL, IADL, and mobility among older adults: a prospective cohort study. J Nutr Health Aging 21:897–903. https://doi.org/10.1007/s12603-017-0891-6
Börsch-Supan A et al (2013) Data resource profile: the survey of health, ageing and retirement in Europe (SHARE). Int J Epidemiol 42:992–1001. https://doi.org/10.1093/ije/dyt088
Buchmann C, DiPrete TA, McDaniel A (2008) Gender inequalities in education. Annu Rev Sociol 34:319–337. https://doi.org/10.1146/annurev.soc.34.040507.134719
Case A, Paxson C (2005) Sex differences in morbidity and mortality. Demography 42:189–214. https://doi.org/10.1353/dem.2005.0011
Chatterji S, Byles J, Cutler D, Seeman T, Verdes E (2015) Health, functioning, and disability in older adults–present status and future implications. Lancet 385:563–575. https://doi.org/10.1016/S0140-6736(14)61462-8
Christensen K, Doblhammer G, Rau R, Vaupel JW (2009) Ageing populations: the challenges ahead. Lancet 374:1196–1208. https://doi.org/10.1016/s0140-6736(09)61460-4
Christensen K et al (2013) Physical and cognitive functioning of people older than 90 years: a comparison of two Danish cohorts born 10 years apart. Lancet 382:1507–1513. https://doi.org/10.1016/s0140-6736(13)60777-1
Crimmins EM, Kim JK, Solé-Auró A (2011) Gender differences in health: results from SHARE, ELSA and HRS. Eur J Public Health 21:81–91. https://doi.org/10.1093/eurpub/ckq022
Crimmins EM, Shim H, Zhang YS, Kim JK (2019) Differences between men and women in mortality and the health dimensions of the morbidity process. Clin Chem 65:135–145. https://doi.org/10.1373/clinchem.2018.288332
Dahlin J, Härkönen J (2013) Cross-national differences in the gender gap in subjective health in Europe: Does country-level gender equality matter? Soc Sci Med 98:24–28. https://doi.org/10.1016/j.socscimed.2013.08.028
Denton M, Prus S, Walters V (2004) Gender differences in health: a Canadian study of the psychosocial, structural and behavioural determinants of health. Soc Sci Med 58:2585–2600. https://doi.org/10.1016/j.socscimed.2003.09.008
Eikemo TA, Huisman M, Bambra C, Kunst AE (2008) Health inequalities according to educational level in different welfare regimes: a comparison of 23 European countries. Sociol Health Illn 30:565–582. https://doi.org/10.1111/j.1467-9566.2007.01073.x
Eurostat (2019) Tobacco consumption statistics. Eurostat. https://ec.europa.eu/eurostat/statistics-explained/index.php?title=Tobacco_consumption_statistics#Context. Accessed 6 June 2019
Fedarko NS (2011) The biology of aging and frailty. Clin Geriatr Med 27:27–37. https://doi.org/10.1016/j.cger.2010.08.006
Ferrera M (1996) The ‘Southern Model’ of welfare in social Europe. J Eur Soc Policy 6:17–37. https://doi.org/10.1177/095892879600600102
Herr M et al (2018) Frailty and associated factors among centenarians in the 5-COOP countries. Gerontology. https://doi.org/10.1159/000489955
Horackova K, Kopecek M, Machu V, Kagstrom A, Aarsland D, Motlova LB, Cermakova P (2019) Prevalence of late-life depression and gap in mental health service use across European regions. Eur Psychiatry 57:19–25. https://doi.org/10.1016/j.eurpsy.2018.12.002
Jerez-Roig J, Bosque-Prous M, Gine-Garriga M, Bagur-Calafat C, Bezerra de Souza DL, Teixido-Compano E, Espelt A (2018) Regional differences in the profile of disabled community-dwelling older adults: a European population-based cross-sectional study. PLoS ONE 13:e0208946. https://doi.org/10.1371/journal.pone.0208946
Jeune B et al (2006) Handgrip strength among nonagenarians and centenarians in three european regions. J Gerontol Ser A 61:707–712
Kaneda T, Zimmer Z, Fang X, Tang Z (2009) Gender differences in functional health and mortality among the chinese elderly: testing an exposure versus vulnerability hypothesis. Res Aging 31:361–388. https://doi.org/10.1177/0164027508330725
Katz S, Ford AB, Moskowitz RW, Jackson BA, Jaffe MW (1963) Studies of illness in the aged. The index of ADL: a standardized measure of biologic and psychologic function. JAMA 185:94–99
Lawton MP, Brody EM (1969) Assessment of older people: self-maintaining and instrumental activities of daily living. Gerontologist 9:179–186
Light KE, Thigpen MT (2017) Perception of physical capacity and IADL performance in older men. OAJ Gerontol Geriatr Med 2:1–12. https://doi.org/10.19080/OAJGGM.2017.02.555583
Lin SF, Beck AN, Finch BK, Hummer RA, Masters RK (2012) Trends in US older adult disability: exploring age, period, and cohort effects. Am J Public Health 102:2157–2163. https://doi.org/10.2105/ajph.2011.300602
McDonough P, Walters V (2001) Gender and health: reassessing patterns and explanations. Soc Sci Med 52:547–559
Merrill SS, Seeman TE, Kasl SV, Berkman LF (1997) Gender differences in the comparison of self-reported disability and performance measures. J Gerontol A Biol Sci Med Sci 52:M19–M26. https://doi.org/10.1093/gerona/52a.1.m19
Murtagh KN, Hubert HB (2004) Gender differences in physical disability among an elderly cohort. Am J Public Health 94:1406–1411. https://doi.org/10.1007/s10654-010-9460-6
Noelker LS, Browdie R, Sidney Katz MD (2014) A new paradigm for chronic illness and long-term care. Gerontologist 54:13–20. https://doi.org/10.1093/geront/gnt086
Noordzij M, van Diepen M, Caskey FC, Jager KJ (2017) Relative risk versus absolute risk: one cannot be interpreted without the other. Nephrol Dial Transplant 32:ii13–ii18. https://doi.org/10.1186/s12939-017-0673-0
Oeppen J, Vaupel JW (2002) Demography. Broken limits to life expectancy. Science 296:1029–1031. https://doi.org/10.1126/science.1069675
Oksuzyan A, Bronnum-Hansen H, Jeune B (2010a) Gender gap in health expectancy. Eur J Ageing 7:213–218. https://doi.org/10.1007/s10433-010-0170-4
Oksuzyan A, Crimmins E, Saito Y, O’Rand A, Vaupel JW, Christensen K (2010b) Cross-national comparison of sex differences in health and mortality in Denmark, Japan and the US. Eur J Epidemiol 25:471–480. https://doi.org/10.1007/s10654-010-9460-6
Okura Y, Urban LH, Mahoney DW, Jacobsen SJ, Rodeheffer RJ (2004) Agreement between self-report questionnaires and medical record data was substantial for diabetes, hypertension, myocardial infarction and stroke but not for heart failure. J Clin Epidemiol 57:1096–1103. https://doi.org/10.1016/j.jclinepi.2004.04.005
Peek MK, Coward RT (1999) Gender differences in the risk of developing disability among older adults with arthritis. J Aging Health 11:131–150. https://doi.org/10.1177/089826439901100201
Prince MJ, Wu F, Guo Y, Gutierrez Robledo LM, O’Donnell M, Sullivan R, Yusuf S (2015) The burden of disease in older people and implications for health policy and practice. Lancet 385:549–562. https://doi.org/10.1016/S0140-6736(14)61347-7
Rasmussen SH, Thinggaard M, Hojgaard MB, Jeune B, Christensen K, Andersen-Ranberg K (2017) Improvement in activities of daily living among danish centenarians? J Gerontol A Biol Sci Med Sci. https://doi.org/10.1093/gerona/glx113
Ross CE, Bird CE (1994) Sex stratification and health lifestyle: consequences for men’s and women’s perceived health. J Health Soc Behav 35:161–178. https://doi.org/10.2307/2137363
Schon P, Parker MG, Kareholt I, Thorslund M (2011) Gender differences in associations between ADL and other health indicators in 1992 and 2002. Aging Clin Exp Res 23:91–98
Schünemann J, Strulik H, Trimborn T (2017) The gender gap in mortality: How much is explained by behavior? J Health Econ 54:79–90. https://doi.org/10.1016/j.jhealeco.2017.04.002
Serrano-Alarcón M, Perelman J (2017) Ageing under unequal circumstances: a cross-sectional analysis of the gender and socioeconomic patterning of functional limitations among the Southern European elderly. Int J Equity Health 16:175. https://doi.org/10.1186/s12939-017-0673-0
Sheehan CM, Tucker-Drob EM (2017) Gendered expectations distort male–female differences in instrumental activities of daily living in later adulthood. J Gerontol B Psychol Sci Soc Sci. https://doi.org/10.1093/geronb/gbw209
Van Oyen H, Cox B, Jagger C, Cambois E, Nusselder W, Gilles C, Robine J-M (2010) Gender gaps in life expectancy and expected years with activity limitations at age 50 in the European Union: associations with macro-level structural indicators. Eur J Ageing 7:229–237. https://doi.org/10.1007/s10433-010-0172-2
Wahrendorf M, Reinhardt JD, Siegrist J (2013) Relationships of disability with age among adults aged 50–85: evidence from the United States, England and continental europe. PLoS ONE 8:e71893. https://doi.org/10.1371/journal.pone.0071893
Weber D, Skirbekk V, Freund I, Herlitz A (2014) The changing face of cognitive gender differences in Europe. Proc Natl Acad Sci 111:11673–11678. https://doi.org/10.1073/pnas.1319538111
Wheaton FV, Crimmins EM (2016) Female disability disadvantage: a global perspective on sex differences in physical function and disability. Ageing Soc 36:1136–1156. https://doi.org/10.1017/S0144686X15000227
Wray LA, Blaum CS (2001) Explaining the role of sex on disability: a population-based study. Gerontologist 41:499–510. https://doi.org/10.1093/geront/41.4.499
Acknowledgements
This paper uses data from SHARE waves 1, 2, 4, 5 and 6, see Börsch-Supan et al. (2013) for methodological details (Börsch-Supan et al. 2013). The SHARE data collection has been primarily funded by the European Commission through FP5 (QLK6-CT-2001-00360), FP6 (SHARE-I3: RII-CT-2006-062193, COMPARE: CIT5-CT-2005-028857, SHARELIFE: CIT4-CT-2006-028812) and FP7 (SHARE-PREP: No. 211909, SHARE-LEAP: No. 227822, SHARE M4: No. 261982). Additional funding from the German Ministry of Education and Research, the Max Planck Society for the Advancement of Science, the U.S. National Institute on Aging (U01_AG09740-13S2, P01_AG005842, P01_AG08291, P30_AG12815, R21_AG025169, Y1-AG-4553-01, IAG_BSR06-11, OGHA_04-064, HHSN271201300071C) and from various national funding sources is gratefully acknowledged.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Responsible editor: Susanne Iwarsson.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Scheel-Hincke, L.L., Möller, S., Lindahl-Jacobsen, R. et al. Cross-national comparison of sex differences in ADL and IADL in Europe: findings from SHARE. Eur J Ageing 17, 69–79 (2020). https://doi.org/10.1007/s10433-019-00524-y
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10433-019-00524-y