Abstract
Many studies in the literature address the effect of low-power lasers in the management of pathologies related to periodontal tissues. Due to the lack of standardized information and the absence of a consensus, this review presents the current status of laser phototherapy (LPT) in periodontics and discusses its benefits and limits in the treatment of periodontal disease. The literature was searched for reviews and original research articles relating to LPT and periodontal disease. The articles were selected using either electronic search engines or manual tracing of the references cited in key papers. The literature search retrieved references on wound and bone healing, analgesia, hypersensitivity, inflammatory process and antimicrobial photodynamic therapy. Each topic is individually addressed in this review. The current literature suggests that LPT is effective in modulating different periodontal disease aspects in vitro, in animals, and in simple clinical models. Further development of this therapy is now dependent on new clinical trials with more complex study designs.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The increasing use of lasers in dentistry and medicine reflects the great advances in this technology during recent decades. In periodontics, the most commonly used are high-power lasers. CO2, Nd:YAG and Er:YAG lasers have been used for calculus removal, osseous surgery and soft-tissue management, such as gingivectomy, gingival curettage and melanin pigmentation removal [1].
The use of low-power lasers (commonly named laser phototherapy, LPT) in periodontics, on the other hand, has been claimed to be of benefit for modulating both periodontal disease aspects and therapy side effects. Several studies have shown that processes such as inflammation, soft tissue and bone healing, and side effects such as postoperative pain and posttreatment tooth hypersensitivity, can be positively influenced by LPT [2–10]. Besides that, the association of low-power lasers with photosensitizers, the so-called “antimicrobial photodynamic therapy” (aPDT), can also be used for reducing bacterial contamination of periodontal pockets [11–13].
LPT is represented by red or near-infrared light used in a low intensity range, with the consequent biological effects attributed to nonthermal cellular events [14]. LPT has been studied as adjuvant to traditional treatment of periodontal disease [8, 15–19].
Although there are different possibilities for using LPT in periodontics, many clinicians are still not familiar with this therapy. In addition, the controversial results observed in the literature are frequently related to the lack of standardization when reporting irradiation parameters and inappropriate specification of dosimetry (power, beam area, time, dose, contact or defocused irradiation mode) [20].
Therefore, a review of the literature seems to be highly necessary to put the available information together and to present its current status, as well as to contribute to an evidence-based use of low-power lasers in periodontics and to its demystification.
Materials and methods
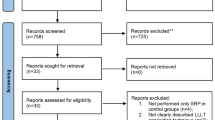
In view of the importance of low-power lasers in periodontics, a literature search was conducted. Firstly, the electronic databases searched included Medline-PUBMED and ISI Web of Knowledge search engines. Reviews of the literature and original research articles were selected. A comprehensive second search was performed by hand searching of relevant references, such as the Journal of Oral Laser Applications, the Proceedings of SPIE, and Congress Proceedings of The World Federation for Laser Dentistry (WFLD, formerly International Society for Lasers in Dentistry).
LPT in the periodontal inflammatory process
The chronic periodontal inflammatory process leads to the destruction of the periodontal ligament, and subsequently, to loss of alveolar bone. The latter is primarily mediated by osteoclasts and is triggered by the proinflammatory molecule prostaglandin E2 (PGE2) [3]. Some studies have analyzed the inflammatory aspects of periodontal tissue and have shown that patients who have undergone conventional periodontal treatment in combination with LPT show better results [21, 22]. It has been reported that LPT is able to reduce gingival inflammation and metalloproteinase 8 (MMP-8) expression when applied after scaling and root planing [8, 21, 23], as well as to reduce inflammatory cells on histology [22]. Ozawa et al. [18] showed that LPT significantly inhibits the increase in plasminogen activity induced in human periodontal ligament cells in response to mechanical tensile force. Plasminogen activity is capable of activating latent collagenase, the enzyme responsible for cleaving collagen fibres. LPT also effectively inhibits PGE2 synthesis [17, 24]. In human gingival fibroblast culture, LPT significantly inhibits PGE2 production that is stimulated by lipopolysaccharide through a reduction on COX2 gene expression in a dose-dependent manner [17]. A decrease in PGE2 levels in cultures of primary human periodontal ligament cells has also been found after cell mechanical stretching [24].
Nomura et al. [25] found that LPT significantly inhibits lipopolysaccharide-stimulated interleukin 1β (IL-1β) production in human gingival fibroblasts, and that this inhibitory effect is dependent on irradiation time. In an in vivo study, alterations in IL-1β concentrations in the periodontal pocket were not observed, although probing depth and both plaque and gingival indexes were reduced more on the laser side than on the placebo side [8]. Safavi et al. [26] evaluated the effect LPT on gene expression of IL-1β, interferon γ (IFN-γ) and growth factors (PDGF, TGF-β, bFGF) to provide an overview of the effect of LPT on their interactive role in the inflammation process. The findings of this study suggest an inhibitory effect of LPT irradiation on IL-1β and IFN-γ production and a stimulatory effect on PDGF and TGF-β. These alterations may be responsible for the antiinflammatory effects of LPT and its positive effects on wound healing.
An in vivo study conducted by Pejcic et al. [27] evaluated the effects of low-level laser irradiation treatment and conservative treatment on gingival inflammation. Authors reported a statistically significant improvement in gingival index and bleeding index after laser irradiation, especially over a longer period of time (3 and 6 months after irradiation). The results depended on the number of laser applications, and after the fifth application, a considerably antiinflammatory effect was achieved with the parameters considered. It was concluded that low-level laser irradiation (670 nm) associated with traditional periodontal therapy can be used as a successful physical adjuvant treatment, leading to better and longer-lasting therapeutic results.
The above-mentioned findings support the hypothesis that LPT can modulate the periodontal inflammatory process, especially through reducing PGE2 release. The capacity of LPT to modulate inflammation seems not to be confined to a single mechanism, since different pathways in inflammatory modulation have been described. In summary, LPT influences the expression of COX2 and IL-1β, as well as MMP-8, PDGF, TGF-β, bFGF and plasminogen. It is important to draw attention to the fact that LPT acts as a coadjuvant to traditional periodontal treatment, with no beneficial effect when used alone for this purpose [8, 10, 21–23].
LPT in wound healing
Periodontal wound healing is necessary when periodontitis and gingivitis, or trauma, have affected the composition and integrity of the periodontal structures. Therefore, several processes, including inflammation and cellular migration, proliferation, and differentiation, are necessary for a successful repair [28, 29].
Several in vitro studies have shown that LPT at certain wavelengths may stimulate fibroblast proliferation when certain combinations of exposure parameters and power densities are used [6, 30–38]. At higher energy densities, no effect [31, 33] or even decreased proliferation has been reported [38, 39]. Therefore, Karu [40] suggested a “window-specificity” at certain wavelengths and energy densities, at which the positive effects of LPT can be expected.
The range of radiation doses at which stimulation of fibroblast proliferation has been observed is wide (0.45–60 J/cm2). However, when considering studies using fibroblasts from the oral mucosa, gingival and periodontal ligament only, the range becomes narrow (0.45–7.9 J/cm2; Table 1). For wavelengths between 660–692 nm and 780–786 nm, the radiation dose is restricted to 2 J/cm2; for the range 809–830 nm, it is between 0.45 and 7.9 J/cm2; and for 2940 nm, it is 3.37 J/cm2 [6, 19, 30, 32, 34, 36–38].
Contradictory results can be found regarding the most efficient wavelength for promoting cell proliferation. However, stimulation of cell proliferation has been observed with both infrared lasers (λ = 780, 809, 812, 830, 904 nm) [30, 33, 36, 37, 39] and red lasers [19, 30, 32–37, 39]. Observation of the parameters investigated up to now shows that not only the wavelength and the energy dose but also the power density are important for cell growth stimulation [41]. Azevedo et al. [34] tested two power densities (428.57 and 142.85 mW/cm2) for the same dose (2 J/cm2, λ = 660 nm) and found that the lower power density caused higher stimulation.
The mode of exposure may also play a role in optimizing the stimulation. Multiple exposures with both infrared and red lasers (λ = 809, 830 and 685 nm) have been shown to cause a significantly higher proliferation of periodontal ligament and gingival fibroblasts than a single exposure with the same energy density [6, 19, 37]. Currently, the evidence available fails to show any increase in the procollagen content and in the synthesis of collagen by human gingival fibroblasts after low-power laser irradiation [33, 42]. As regards clinical evidence, the current literature is not as extensive as it is for in vitro evidence. Clinical evidence of the effect of LPT on periodontal wound healing can be found for irradiation after scaling and root planing, gingivoplasty and gingivectomy, showing significantly better healing in the sites treated with laser, despite the different methods of measurement used [8, 16, 21, 43, 44]. In a split-mouth study in 20 patients undergoing gingivectomy bilaterally, Amorim et al. [16] measured the probing depth of the gingival sulcus before and after surgery. They observed that the laser irradiated sides (4 J/cm2, λ = 685 nm) had probing depths significantly lower than the control sides at 21 and 28 days after surgery. Another study showed that sites receiving LPT (4 J/cm2, λ = 588 nm) had significantly faster surface epithelization than control sites 3, 7 and 15 days after surgery [43]. Additionally, complete wound healing was achieved faster in sites receiving LPT (within 18–21 days) than in control sites (within 19–24 days). On the other hand, for irradiation with the same energy density (4 J/cm2) and 660 nm wavelength, Damante et al. found no significant differences when comparing irradiated and nonirradiated control sites for all histomorphometric parameters quantified. In contrast to the other above-mentioned studies, the irradiation was performed in punctal mode and used a lower output power (15 mW) [45].
After scaling and root planing, adjuvant LPT was shown to significantly reduce gingival index, probing depth and gingival crevicular fluid volume (GCF) [8]. Similar effects were observed by the same group in 2007 [21], and they also observed the importance of light coherence in the improvement in periodontal wound healing. A laser with longer coherence (HeNe laser) was clinically compared with another with shorter coherence (diode laser). For irradiations with the same power density of 100 mW/cm2, both plaque and gingival index were significantly reduced on the side treated with the HeNe laser. These results appear to show that coherence is an important parameter in light stimulation in vivo, an effect not observed in vitro [46]. Thus, further studies are needed to elucidate the exact mechanism by which each parameter influences the effects of LPT in vivo.
The use of stem cells in future tissue engineering and regenerative medicine to replace conventional therapeutic modalities has been the subject of growing interest in different areas [47–49]. These cells have self-renewing properties and are able to differentiate into one or many different specialized cell types under controlled in vitro conditions [49]. LPT is expected to significantly influence stem cell proliferation leading to improved tissue healing. Recent in vitro studies submitting stem cells to LPT using low energy densities have shown promising results [48, 50]. However, in order to determine whether this therapy can contribute to an optimal attachment and functional improvement in the cells following implantation and also reduce tissue healing time, future studies are needed to evaluate its effect on new bone formation following stem cell implantation in injured tissues.
The literature review showed several positive results of the use of LPT in improving periodontal wound healing both in vitro and in vivo [6, 8, 16, 19, 21, 26, 32, 34, 37, 38, 43, 44, 51]. In particular, the evidence from in vivo studies indicates that LPT may be beneficial in enhancing periodontal healing after gingivectomy, scaling, root planing and intrabony defect surgery [8, 21, 43, 52].
LPT in bone healing
Regenerative periodontal therapy aims to predictably restore the tooth's supporting periodontal tissues, and should result in formation of a new connective tissue attachment and new alveolar bone [53]. Preclinical models have demonstrated periodontal regeneration following treatment with barrier membranes, different types of grafting materials or their combination [54–56]. Recently, it has been suggested that LPT may be indicated in combination with regenerative methods or even alone in order to stimulate bone repair in specific bone defects [52].
Some authors have investigated the effects of LPT on growth and differentiation of human osteoblast cells [57, 58]. Stein et al. [58] reported that LPT has a biostimulatory effect on human osteoblast-like cells during the first 72 h after irradiation. Histological studies using animal experimental models [59, 60] have also demonstrated that LPT can promote an increase in collagen fibres deposition, as well as in the amount of well-organized bone trabeculae after 30 days of induced-bone defect healing. It is suggested that LPT may accelerate the process of bone repair [59, 61–63] and/or cause increases in callus volume, especially in the early stages of haematoma absorption and bone remodelling [59].
The effects of LPT on the bone healing process in surgically created bone cavities were evaluated using a biochemical assay. The results indicated that LPT acts by affecting calcium transport during new bone formation [64]. These results corroborate the findings of Khadra et al. [65], in which bone defects showed significantly more calcium, phosphorus and protein after LPT in an experimental animal model.
For the treatment of deep intrabony defects, the use of barrier membranes and different types of grafting materials are usually indicated. In a study of the effect of LPT on the healing of bone defects associated with autologous bone grafts, bone remodelling was both quantitatively and qualitatively more evident in irradiated animals than in nonirradiated animals [9]. The association of matrix protein derivative with the LPT irradiation (during and after surgery) has shown a reduction in postoperative pain, which suggests that LPT may improve the effects of matrix protein derivative by reducing postoperative complications [44]. LPT biostimulation of bone tissue attachment to implant surfaces has also been reported. It has been shown that LPT influences the expression of osteoprotegerin, receptor activator of nuclear factor κB ligand and receptor activator of nuclear factor κB, and results in the expansion of bone cells metabolic activity [66, 67].
Pinheiro and Gerbi [68] studied the photoengineering of bone repair processes and suggest that the effects of LPT on bone regeneration depends not only on the total dose of radiation, but also on the irradiation time and the irradiation mode. Studies have shown that LPT has a positive biomodulatory effect on the healing of bone defects [52, 54–56, 69], and that the positive effect of this therapy is more evident when the tissue is irradiated intraoperatively, directly to the surgical bed, and in the early stages of bone remodelling [52].
LPT in analgesia/pain reduction
Postoperative pain control is an essential part of periodontal surgery routine. Postoperative pain may be a consequence of surgical trauma and release of pain mediators [70–73], and is usually reported to be most intense during the first hours following surgery, just after cessation of local anaesthesia [74].
LPT has been suggested as an alternative method for postoperative pain control. Compared to oral analgesics and nonsteroidal antiinflammatory drugs, LPT can be advantageous because the therapeutic window for its antiinflammatory action overlaps with its ability to improve tissue repair [75]. The mechanism by which LPT reduces pain symptoms is still not clear, even though many studies have shown some physiological changes induced by the interaction of the light with different cells [2, 32, 33, 76]. Some authors describe a possible stabilization of nerve cell membranes, probably due to the more stable conformation of the lipid bilayers induced by LPT, and the associated integral proteins of the nerve cell membrane, which have already been reported in the literature [77]. The enhanced redox systems of the cell and an increase in ATP production have also been shown to restore neuronal membranes and decrease pain transmission [78].
Although some studies have indicated that LPT affects the neurophysiological processes in intact peripheral nerves in the absence of inflammation, the current literature is not conclusive [2]. Evidence of the effects of LPT on injured nerve fibres is considerably more consistent, revealing positive effects of this therapy [79, 80].
Recent reviews by Parker et al. [7] and Bjordal et al. [2] have shown that low-power lasers can significantly reduce pain. Bjordal et al. reviewed several basic and clinical studies in which LPT was used in acute pain following tissue injury. This systematic review concluded that LPT can modulate the inflammatory process in a dose-dependent manner and that it can be titrated to significantly reduce acute inflammatory pain in the clinical setting. The authors confirmed that, in acute pain, the optimal effects of LPT can be achieved when it is administered in higher energy densities during the first 72 h in order to reduce inflammation, followed by lower dosages to the target tissue during the following days with the aim of promoting tissue repair. Well-designed randomized controlled trials have also shown an effect of LPT doses well below those expected to induce biological responses [81, 82]. Thus, further clinical trials with adequate doses are still necessary to estimate the magnitude of the effect of LPT in acute pain, since high doses would be expected to be effective for pain relief but to overdose stimulatory mechanisms. On the other hand, low doses are related to biomodulation but less effective for acute pain.
Antimicrobial photodynamic therapy
The presence of bacteria in the gingival sulcus and periodontal connective tissues is a determinant factor in the development of periodontitis [83]. In areas of difficult access such as furcations, invaginations and concavities, the use of manual curettes or ultrasound is not enough to ensure the eradication of periodontal pathogenic bacteria. Likewise, antibiotic-resistant strains may also damage the efficacy of conventional periodontal treatment [84]. Based on these facts, alternative methods are being studied with the aim of achieving a more efficient therapy such as antimicrobial phytochemicals and light-activated killing [85].
The development of laser technology and the discovery of its significant antimicrobial effects have introduced this treatment modality as a possible coadjuvant to the treatment of periodontitis. Differently from high-power lasers, low-power lasers do not increase tissue temperature [86]. Thus, when used alone, the same antimicrobial effect as that of high-power lasers in periodontitis active sites cannot be expected [87]. The antimicrobial effect of low-power lasers is achieved by association with extrinsic photosensitizers, which results in the production of highly reactive oxygen species [88] that cause damage to membranes, mitochondria and DNA, culminating in the death of the microorganisms [89–91]. This is the process of aPDT, and its use is being increasingly studied with the aim of complementing the microbial reduction achieved by conventional mechanical periodontal therapy.
For the effective treatment of bacterial infectious diseases, it is paramount to have an adequate light source and a photosensitizer capable of binding to the targeted pathogen, so that photosensitization may occur in either subgingival or superficial oral tissues. Different light sources have been studied, such as light emitting diodes [92, 93], conventional light [94, 95] and low-power lasers [96]. There are several photosensitizers available for aPDT, but disinfection related to periodontopathogens generally indicates the use of cationic charged photosensitizers, such as toluidine blue, methylene blue and poly-l-lysine-chlorin-e6 conjugates [97, 98]. Plaque disclosure agents such as erythrosine and malachite green have also been addressed in in vitro studies as potential photosensitizers in aPDT [96, 99]. The interaction between the photosensitizer and microorganisms occurs within a few minutes, and this period (incubation or preirradiation time) must be respected before laser irradiation [88, 98].
Several in vitro studies have demonstrated that microorganisms related to periodontal disease such as Porphyromonas gingivalis, Aggregatibacter actinomycetemcomitans (previously Actinobacillus actinomycetemcomitans), Fusobacterium nucleatum, Prevotella intermedia and Streptococcus sanguis are significantly suppressed by aPDT under different environmental conditions (pure cultures, pure or multispecies biofilms) [11, 13, 96, 100, 101]. Key virulence factors (lipopolysaccharide and proteases) present after the destruction of bacteria are also reduced by photosensitization [90, 102]. Moreover, some periodontal bacteria are capable of producing intrinsic photosensitizer (protoporphyrin IX) [85]. The so-called black-pigmented bacteria have been shown to be more susceptible to lethal photosensitization, even without the use of extrinsic photosensitizers [103–105].
More recently, in vivo studies have shown a decrease in bone loss and reduction of periodontal signs of redness and bleeding on probing after aPDT for the treatment of periodontitis [12, 106–108] and periimplantitis [109–112] in rat and dog models. These studies included healthy [12, 106–108], diabetic [113] and even immunosuppressed animals [114]. Clinical trials have shown the efficacy of this therapy as coadjuvant in the treatment of chronic [10, 115–117] and aggressive [118, 119] periodontitis and periimplantitis [120, 121], and even in treatment maintenance at follow-up session [122]. The photosensitization process is dependent on photosensitizer concentration, laser irradiation parameters and the microorganism species involved [11].
Antimicrobial PDT is considered a safe coadjuvant in nonsurgical treatment of periodontitis, as it has been proved to reduce the signs of inflammation and microbial infection without any harmful effects on adjacent periodontal tissues [12, 106, 123]. Its potential effect in improving wound healing has also been reported [98, 124]. The topical application of aPDT allows a local and specific action in the disease active site, with no effects on the microflora at other sites of the oral cavity, and reduced probability of side effects that are associated with the systemic administration of antimicrobial agents [11]. Additionally, the increasing bacterial resistance to antibiotics that frequently occurs in conventional therapy is highly unlikely to occur with aPDT, since it suppresses microorganisms in a short time by producing reactive oxygen species that interact with various cell structures and targets [89, 90]. Thus, repeated photosensitization of both antibiotic-resistant and antibiotic-susceptible bacteria seemed not to induce the selection of resistant strains [125].
Controlled clinical studies are still needed to better embed the use of aPDT in periodontists’ clinical routine [126]. However, the in vitro and in vivo studies present in the literature indicate that aPDT may potentially become a successful antiinfectious procedure to be associated with conventional therapy in the management of periodontal disease [98, 127–129].
LPT in the treatment of dentin hypersensitivity
In periodontology, the removal of enamel or denudation of the root surface by loss of cementum and periodontal tissues following nonsurgical periodontal treatment are often associated with increased levels of dentin hypersensitivity (DH) [130–132]. Studies suggest that periodontal diseases play a role in the aetiology of this condition [133–135]. Numerous desensitizing agents have been clinically tested in an effort to find a means to alleviate the discomfort experienced by patients undergoing periodontal treatment [136]. The results have been variable and inconclusive due to the different methodologies employed, the variability in the subjective response and the influence of the placebo effect.
The advent of dental lasers has raised another possibility for the treatment for DH, and has become the object of research interest in recent decades. The effect of LPT on DH depends on many variables, such as the type of equipment used (low- or high-power lasers), wavelength and selection of parameters. However, contradictory results have been reported in the literature due to the lack of information related to the irradiation protocol used and the subjectivity of the evaluation of DH. The effect of high-power lasers in the treatment of DH has already been described. CO2, Nd:YAG and Er:YAG are suitable lasers for the management of DH [5]. Their mechanism of action is related to the increase in tooth surface temperature. Following their use, it is possible to notice the complete or partial closure of dentinal tubules after recrystallization of dentinal surface.
Several mechanisms are proposed to explain the decrease in pain after LPT in DH. The positive effects are mainly attributed to the formation of tertiary dentin and the reduction in sensory nerve activity [137]. Although information on the neurophysiological mechanism is not yet conclusive, it is postulated that LPT mediates an analgesic effect related to the depolarization of C-fibre afferents. This interference in the polarity of cell membranes by increasing the amplitude of its potential action is capable of blocking the transmission of pain stimuli in hypersensitive dentin. Histological studies have shown that the formation of hard tissue is enhanced as a reaction of the dental pulp to laser irradiation [138, 139]. Matsui et al. [140] showed that hydroxyl generated by laser irradiation activates cell-signalling molecules such as G-protein, thereby promoting the formation of hard tissue by human dental pulp cells.
The promising results observed in in vitro studies stimulated the evaluation of LPT for the treatment of DH in vivo. Wakabayashi et al. [141] showed that a low-power diode laser was effective in 61 out of 66 patients. The results of Gerschman et al. [142] were also satisfactory and corroborated those of Wakabayashi et al. [141]. Groth [4] reported that the results with the low-power laser were significantly better, and established an irradiation protocol of three sessions with an interval of 72 hours between them. As these studies were performed with low-power lasers in the infrared spectrum, Ladalardo et al. [143] studied the influence of different wavelengths on pain reduction, and observed that the 660 nm red diode laser was more effective than the 830 nm infrared diode laser. Marsilio et al. [144] observed positive clinical results using a low-power laser in the red spectrum, with 86.53% and 88.88% pain reduction for 3 and 5 J/cm2, respectively. Corona et al. [145] compared this same wavelength with fluoride varnish frequently used in the treatment of DH, and obtained better results with LPT. Also, it should be born in mind that the evaluation of treatments for DH is not a simple procedure due to the interference of the placebo effect, which is easily observed in clinical trials [146].
However, in spite of being speculative, the mechanisms proposed for the effects of LPT on DH reduction require serious consideration and new experiments may elucidate the cellular events involved in this process. Still, the positive results and the lack of serious side effects reported in the literature allow the statement that low-power lasers are an effective method for the treatment of DH, being a predictable, reliable and simple approach.
Final considerations
LPT has been increasingly studied due to its clinical effects including analgesia, modulation of inflammation and biomodulation. Although a few studies mention the possible placebo effect of LPT [146], several in vitro and in vivo studies have shown its efficacy when used as coadjuvant in traditional periodontal treatment. The clinical applications of LPT include periodontal inflammation modulation, improvement in wound and bone healing processes, control of postoperative pain and posttreatment tooth hypersensitivity, and microbial reduction when associated with an extrinsic photosensitizer. Despite the clinical observations, additional clinical trials are still needed to better elucidate these events and to provide the clinical outcomes of LPT in periodontics with a solid scientific basis.
The optimal laser parameters and the irradiation protocols are not fully described in the literature. The main factors hindering their precise definition are the lack of standardization in the reporting of laser parameters and the great variety of research methodologies used. However, considering the high number of positive reports currently available in the literature, new in vitro investigations should no longer seek to confirm the effectiveness of LPT, but to determine its precise mechanism and to identify the ideal set of parameters and protocols for different clinical situations.
Although LPT seems to enhance clinical outcomes in periodontology, it is only reasonable to perform it in a decontaminated and calculus-free periodontium. This means that conventional periodontal treatment should not be discarded. LPT must be considered an adjuvant therapy, which may have additional benefit for a previously well-treated periodontal tissue.
References
Ishikawa I, Sasaki KM, Aoki A, Watanabe H (2003) Effects of Er:YAG laser on periodontal therapy. J Int Acad Periodontol 5(1):23–28
Bjordal JM, Johnson MI, Iversen V, Aimbire F, Lopes-Martins RA (2006) Photoradiation in acute pain: a systematic review of possible mechanisms of action and clinical effects in randomized placebo-controlled trials. Photomed Laser Surg 24(2):158–168. doi:10.1089/pho.2006.24.158
Choi BK, Moon SY, Cha JH, Kim KW, Yoo YJ (2005) Prostaglandin E(2) is a main mediator in receptor activator of nuclear factor-kappaB ligand-dependent osteoclastogenesis induced by Porphyromonas gingivalis, Treponema denticola, and Treponema socranskii. J Periodontol 76(5):813–820. doi:10.1902/jop.2005.76.5.813
Groth EB (1995) Treatment of dentin hypersensitivity with low power laser of GaAlAs (abstract). J Dent Res 74(3):794
Kimura Y, Wilder-Smith P, Yonaga K, Matsumoto K (2000) Treatment of dentine hypersensitivity by lasers: a review. J Clin Periodontol 27(10):715–721
Kreisler M, Christoffers AB, Willershausen B, d'Hoedt B (2003) Effect of low-level GaAlAs laser irradiation on the proliferation rate of human periodontal ligament fibroblasts: an in vitro study. J Clin Periodontol 30(4):353–358
Parker J, Dowdy D, Harkness E (2000) The effects of laser therapy on tissue repair and pain control. A meta analysis of the literature (abstract). Proceedings of the Third Congress of the World Association for Laser Therapy, Athens, Greece, p 77
Qadri T, Miranda L, Tuner J, Gustafsson A (2005) The short-term effects of low-level lasers as adjunct therapy in the treatment of periodontal inflammation. J Clin Periodontol 32(7):714–719. doi:10.1111/j.1600-051X.2005.00749.x
Weber JB, Pinheiro AL, de Oliveira MG, Oliveira FA, Ramalho LM (2006) Laser therapy improves healing of bone defects submitted to autologous bone graft. Photomed Laser Surg 24(1):38–44. doi:10.1089/pho.2006.24.38
Yilmaz S, Kuru B, Kuru L, Noyan U, Argun D, Kadir T (2002) Effect of gallium arsenide diode laser on human periodontal disease: a microbiological and clinical study. Lasers Surg Med 30(1):60–66. doi:10.1002/lsm.10010
Chan Y, Lai CH (2003) Bactericidal effects of different laser wavelengths on periodontopathic germs in photodynamic therapy. Lasers Med Sci 18(1):51–55. doi:10.1007/s10103-002-0243-5
Qin YL, Luan XL, Bi LJ, Sheng YQ, Zhou CN, Zhang ZG (2008) Comparison of toluidine blue-mediated photodynamic therapy and conventional scaling treatment for periodontitis in rats. J Periodontal Res 43(2):162–167. doi:10.1111/j.1600-0765.2007.01007.x
O'Neill JF, Hope CK, Wilson M (2002) Oral bacteria in multi-species biofilms can be killed by red light in the presence of toluidine blue. Lasers Surg Med 31(2):86–90. doi:10.1002/lsm.10087
Lanzafame RJ, Stadler I, Coleman J, Haerum B, Oskoui P, Whittaker M, Zhang RY (2004) Temperature-controlled 830-nm low-level laser therapy of experimental pressure ulcers. Photomed Laser Surg 22(6):483–488. doi:10.1089/pho.2004.22.483
Crespi R, Romanos GE, Barone A, Sculean A, Covani U (2005) Er:YAG laser in defocused mode for scaling of periodontally involved root surfaces: an in vitro pilot study. J Periodontol 76(5):686–690. doi:10.1902/jop.2005.76.5.686
Amorim JC, de Sousa GR, de Barros Silveira L, Prates RA, Pinotti M, Ribeiro MS (2006) Clinical study of the gingiva healing after gingivectomy and low-level laser therapy. Photomed Laser Surg 24(5):588–594. doi:10.1089/pho.2006.24.588
Sakurai Y, Yamaguchi M, Abiko Y (2000) Inhibitory effect of low-level laser irradiation on LPS-stimulated prostaglandin E2 production and cyclooxygenase-2 in human gingival fibroblasts. Eur J Oral Sci 108(1):29–34
Ozawa Y, Shimizu N, Abiko Y (1997) Low-energy diode laser irradiation reduced plasminogen activator activity in human periodontal ligament cells. Lasers Surg Med 21(5):456–463
Saygun I, Karacay S, Serdar M, Ural AU, Sencimen M, Kurtis B (2008) Effects of laser irradiation on the release of basic fibroblast growth factor (bFGF), insulin like growth factor-1 (IGF-1), and receptor of IGF-1 (IGFBP3) from gingival fibroblasts. Lasers Med Sci 23(2):211–215. doi:10.1007/s10103-007-0477-3
Tunér J, Hode L (1998) It's all in the parameters: a critical analysis of some well-known negative studies on low-level laser therapy. J Clin Laser Med Surg 16(5):245–248
Qadri T, Bohdanecka P, Tuner J, Miranda L, Altamash M, Gustafsson A (2007) The importance of coherence length in laser phototherapy of gingival inflammation: a pilot study. Lasers Med Sci 22(4):245–251. doi:10.1007/s10103-006-0439-1
Pejcic A, Zivkvic V (2007) Histological examination of gingiva treated with low-level laser in periodontal therapy. J Oral Laser Appl 71(1):37–43
Ribeiro IW, Sbrana MC, Esper LA, Almeida AL (2008) Evaluation of the effect of the GaAlAs laser on subgingival scaling and root planing. Photomed Laser Surg 26(4):387–391. doi:10.1089/pho.2007.2152
Shimizu N, Yamaguchi M, Goseki T, Shibata Y, Takiguchi H, Iwasawa T, Abiko Y (1995) Inhibition of prostaglandin e2 and interleukin 1-beta production by low-power laser irradiation in stretched human periodontal ligament cells. J Dent Res 74(7):1382–1388
Nomura K, Yamaguchi M, Abiko Y (2001) Inhibition of interleukin-1beta production and gene expression in human gingival fibroblasts by low-energy laser irradiation. Lasers Med Sci 16(3):218–223
Safavi SM, Kazemi B, Esmaeili M, Fallah A, Modarresi A, Mir M (2008) Effects of low-level He-Ne laser irradiation on the gene expression of IL-1beta, TNF-alpha, IFN-gamma, TGF-beta, bFGF, and PDGF in rat's gingiva. Lasers Med Sci 23(3):331–335. doi:10.1007/s10103-007-0491-5
Pejcic A, Kojovic D, Kesic L, Obradovic R (2010) The effects of low level laser irradiation on gingival inflammation. Photomed Laser Surg 28 (1):69–74. doi:10.1089/pho.2008.2301
Grzesik WJ, Narayanan AS (2002) Cementum and periodontal wound healing and regeneration. Crit Rev Oral Biol Med 13(6):474–484
Pitaru S, McCulloch CA, Narayanan SA (1994) Cellular origins and differentiation control mechanisms during periodontal development and wound healing. J Periodontal Res 29(2):81–94
Loevschall H, Arenholt-Bindslev D (1994) Effect of low level diode laser irradiation of human oral mucosa fibroblasts in vitro. Lasers Surg Med 14(4):347–354
Yu W, Naim JO, Lanzafame RJ (1994) The effect of laser irradiation on the release of bFGF from 3T3 fibroblasts. Photochem Photobiol 59(2):167–170
Almeida-Lopes L, Rigau J, Zangaro RA, Guidugli-Neto J, Jaeger MM (2001) Comparison of the low level laser therapy effects on cultured human gingival fibroblasts proliferation using different irradiance and same fluence. Lasers Surg Med 29(2):179–184. doi:10.1002/lsm.1107
Pereira AN, Eduardo Cde P, Matson E, Marques MM (2002) Effect of low-power laser irradiation on cell growth and procollagen synthesis of cultured fibroblasts. Lasers Surg Med 31(4):263–267. doi:10.1002/lsm.10107
Azevedo LH, de Paula Eduardo F, Moreira MS, de Paula Eduardo C, Marques MM (2006) Influence of different power densities of LILT on cultured human fibroblast growth: a pilot study. Lasers Med Sci 21(2):86–89. doi:10.1007/s10103-006-0379-9
Moore P, Ridgway TD, Higbee RG, Howard EW, Lucroy MD (2005) Effect of wavelength on low-intensity laser irradiation-stimulated cell proliferation in vitro. Lasers Surg Med 36(1):8–12. doi:10.1002/lsm.20117
Kreisler M, Christoffers AB, Al-Haj H, Willershausen B, d'Hoedt B (2002) Low level 809-nm diode laser-induced in vitro stimulation of the proliferation of human gingival fibroblasts. Lasers Surg Med 30(5):365–369. doi:10.1002/lsm.10060
Khadra M, Lyngstadaas SP, Haanaes HR, Mustafa K (2005) Determining optimal dose of laser therapy for attachment and proliferation of human oral fibroblasts cultured on titanium implant material. J Biomed Mater Res A 73(1):55–62. doi:10.1002/jbm.a.30270
Pourzarandian A, Watanabe H, Ruwanpura SM, Aoki A, Ishikawa I (2005) Effect of low-level Er:YAG laser irradiation on cultured human gingival fibroblasts. J Periodontol 76(2):187–193. doi:10.1902/jop.2005.76.2.187
Lubart R, Wollman Y, Friedmann H, Rochkind S, Laulicht I (1992) Effects of visible and near-infrared lasers on cell cultures. J Photochem Photobiol B 12(3):305–310. doi:1011-1344(92)85032-P
Karu TI (1990) Effects of visible radiation on cultured cells. Photochem Photobiol 52(6):1089–1098
van Breugel HH, Bar PR (1992) Power density and exposure time of He-Ne laser irradiation are more important than total energy dose in photo-biomodulation of human fibroblasts in vitro. Lasers Surg Med 12(5):528–537
Marques MM, Pereira AN, Fujihara NA, Nogueira FN, Eduardo CP (2004) Effect of low-power laser irradiation on protein synthesis and ultrastructure of human gingival fibroblasts. Lasers Surg Med 34(3):260–265. doi:10.1002/lsm.20008
Ozcelik O, Cenk Haytac M, Kunin A, Seydaoglu G (2008) Improved wound healing by low-level laser irradiation after gingivectomy operations: a controlled clinical pilot study. J Clin Periodontol 35(3):250–254. doi:10.1111/j.1600-051X.2007.01194.x
Ozcelik O, Cenk Haytac M, Seydaoglu G (2008) Enamel matrix derivative and low-level laser therapy in the treatment of intra-bony defects: a randomized placebo-controlled clinical trial. J Clin Periodontol 35(2):147–156. doi:10.1111/j.1600-051X.2007.01176.x
Damante CA, Greghi SL, Sant'Ana AC, Passanezi E, Taga R (2004) Histomorphometric study of the healing of human oral mucosa after gingivoplasty and low-level laser therapy. Lasers Surg Med 35(5):377–384. doi:10.1002/lsm.20111
Karu T, Kalenko GS, Letokhov VS, Lobko VV (1982) Biological action of low-intensity visible light on HeLa cells as a function of the coherence, dose, wavelength, and irradiation regime. Sov J Quantum Electron 12(9):1134–1138
Kerkis I, Kerkis A, Dozortsev D, Stukart-Parsons GC, Gomes Massironi SM, Pereira LV, Caplan AI, Cerruti HF (2006) Isolation and characterization of a population of immature dental pulp stem cells expressing OCT-4 and other embryonic stem cell markers. Cells Tissues Organs 184(3–4):105–116. doi:10.1159/000099617
Tuby H, Maltz L, Oron U (2007) Low-level laser irradiation (LLLI) promotes proliferation of mesenchymal and cardiac stem cells in culture. Lasers Surg Med 39(4):373–378. doi:10.1002/lsm.20492
Vieira NM, Brandalise V, Zucconi E, Jazedje T, Secco M, Nunes VA, Strauss BE, Vainzof M, Zatz M (2008) Human multipotent adipose-derived stem cells restore dystrophin expression of Duchenne skeletal-muscle cells in vitro. Biol Cell 100(4):231–241. doi:10.1042/BC20070102
Eduardo Fde P, Bueno DF, de Freitas PM, Marques MM, Passos-Bueno MR, Eduardo Cde P, Zatz M (2008) Stem cell proliferation under low intensity laser irradiation: A preliminary study. Lasers Surg Med 40(6):433–438. doi:10.1002/lsm.20646
Soares LP, Oliveira MG, Pinheiro AL, Fronza BR, Maciel ME (2008) Effects of laser therapy on experimental wound healing using oxidized regenerated cellulose hemostat. Photomed Laser Surg 26(1):10–13. doi:10.1089/pho.2007.2115
Torres CS, dos Santos JN, Monteiro JS, Amorim PG, Pinheiro AL (2008) Does the use of laser photobiomodulation, bone morphogenetic proteins, and guided bone regeneration improve the outcome of autologous bone grafts? An in vivo study in a rodent model. Photomed Laser Surg 26(4):371–377. doi:10.1089/pho.2007.2172
Sculean A, Nikolidakis D, Schwarz F (2008) Regeneration of periodontal tissues: combinations of barrier membranes and grafting materials – biological foundation and preclinical evidence: a systematic review. J Clin Periodontol 35(8 Suppl):106–116. doi:10.1111/j.1600-051X.2008.01263.x
Aboelsaad NS, Soory M, Gadalla LM, Ragab LI, Dunne S, Zalata KR, Louca C (2009) Effect of soft laser and bioactive glass on bone regeneration in the treatment of infra-bony defects (a clinical study). Lasers Med Sci 24(4):527–533. doi:10.1007/s10103-008-0576-9
Pinheiro AL, Martinez Gerbi ME, Carneiro Ponzi EA, Pedreira Ramalho LM, Marques AM, Carvalho CM, Santos Rde C, Oliveira PC, Noia M (2008) Infrared laser light further improves bone healing when associated with bone morphogenetic proteins and guided bone regeneration: an in vivo study in a rodent model. Photomed Laser Surg 26(2):167–174. doi:10.1089/pho.2007.7027
Pinheiro AL, Martinez Gerbi ME, de Assis LF Jr, Carneiro Ponzi EA, Marques AM, Carvalho CM, de Carneiro Santos R, Oliveira PC, Noia M, Ramalho LM (2009) Bone repair following bone grafting hydroxyapatite guided bone regeneration and infra-red laser photobiomodulation: a histological study in a rodent model. Lasers Med Sci 24(4):234–240. doi:10.1007/s10103-008-0556-0
Fujihara NA, Hiraki KR, Marques MM (2006) Irradiation at 780 nm increases proliferation rate of osteoblasts independently of dexamethasone presence. Lasers Surg Med 38(4):332–336. doi:10.1002/lsm.20298
Stein E, Koehn J, Sutter W, Wendtlandt G, Wanschitz F, Thurnher D, Baghestanian M, Turhani D (2008) Initial effects of low-level laser therapy on growth and differentiation of human osteoblast-like cells. Wien Klin Wochenschr 120(3–4):112–117. doi:10.1007/s00508-008-0932-6
Liu X, Lyon R, Meier HT, Thometz J, Haworth ST (2007) Effect of lower-level laser therapy on rabbit tibial fracture. Photomed Laser Surg 25(6):487–494. doi:10.1089/pho.2006.2075
Gerbi ME, Marques AM, Ramalho LM, Ponzi EA, Carvalho CM, Santos Rde C, Oliveira PC, Noia M, Pinheiro AL (2008) Infrared laser light further improves bone healing when associated with bone morphogenic proteins: an in vivo study in a rodent model. Photomed Laser Surg 26(1):55–60. doi:10.1089/pho.2007.2026
Guzzardella GA, Fini M, Torricelli P, Giavaresi G, Giardino R (2002) Laser stimulation on bone defect healing: an in vitro study. Lasers Med Sci 17(3):216–220. doi:10.1007/s101030200031
Miloro M, Miller JJ, Stoner JA (2007) Low-level laser effect on mandibular distraction osteogenesis. J Oral Maxillofac Surg 65(2):168–176. doi:10.1016/j.joms.2006.10.002
Lirani-Galvao AP, Jorgetti V, da Silva OL (2006) Comparative study of how low-level laser therapy and low-intensity pulsed ultrasound affect bone repair in rats. Photomed Laser Surg 24(6):735–740. doi:10.1089/pho.2006.24.735
Nissan J, Assif D, Gross MD, Yaffe A, Binderman I (2006) Effect of low intensity laser irradiation on surgically created bony defects in rats. J Oral Rehabil 33(8):619–924. doi:10.1111/j.1365-2842.2006.01601.x
Khadra M, Kasem N, Haanaes HR, Ellingsen JE, Lyngstadaas SP (2004) Enhancement of bone formation in rat calvarial bone defects using low-level laser therapy. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 97(6):693–700. doi:10.1016/S1079210403006851
Kim YD, Kim SS, Hwang DS, Kim SG, Kwon YH, Shin SH, Kim UK, Kim JR, Chung IK (2007) Effect of low-level laser treatment after installation of dental titanium implant – immunohistochemical study of RANKL, RANK, OPG: an experimental study in rats. Lasers Surg Med 39(5):441–450. doi:10.1002/lsm.20508
Lopes CB, Pinheiro AL, Sathaiah S, da Silva NS, Salgado MA (2007) Infrared laser photobiomodulation (lambda 830 nm) on bone tissue around dental implants: a Raman spectroscopy and scanning electronic microscopy study in rabbits. Photomed Laser Surg 25(2):96–101. doi:10.1089/pho.2006.2030
Pinheiro AL, Gerbi ME (2006) Photoengineering of bone repair processes. Photomed Laser Surg 24(2):169–178. doi:10.1089/pho.2006.24.169
Blaya DS, Guimaraes MB, Pozza DH, Weber JB, de Oliveira MG (2008) Histologic study of the effect of laser therapy on bone repair. J Contemp Dent Pract 9(6):41–48. doi:1526-3711-545
Horton EW (1963) Action of prostaglandin E1 on tissues which respond to bradykinin. Nature 200:892–893
Seymour RA, Walton JG (1984) Pain control after third molar surgery. Int J Oral Surg 13(6):457–485
Dinarello CA, Savage N (1989) Interleukin-1 and its receptor. Crit Rev Immunol 9(1):1–20
Shapiro RD, Cohen BH (1992) Perioperative pain control. Oral Maxillofac Surg Clin North Am 4:663–674
Fisher SE, Frame JW, Rout PG, McEntegart DJ (1988) Factors affecting the onset and severity of pain following the surgical removal of unilateral impacted mandibular third molar teeth. Br Dent J 164(11):351–354
Basford JR (1995) Low intensity laser therapy: still not an established clinical tool. Lasers Surg Med 16(4):331–342
Karu T (1989) Laser biostimulation: a photobiological phenomenon. J Photochem Photobiol B 3(4):638–640
Iijima K, Shimoyama N, Shimoyama M, Mizuguchi T (1993) Effect of low-power He-Ne laser on deformability of stored human erythrocytes. J Clin Laser Med Surg 11(4):185–189
Passarella S, Casamassima E, Molinari S, Pastore D, Quagliariello E, Catalano IM, Cingolani A (1984) Increase of proton electrochemical potential and ATP synthesis in rat liver mitochondria irradiated in vitro by helium-neon laser. FEBS Lett 175(1):95–99. doi:0014-5793(84)80577-3
Moore A, Moore O, McQuay H, Gavaghan D (1997) Deriving dichotomous outcome measures from continuous data in randomised controlled trials of analgesics: use of pain intensity and visual analogue scales. Pain 69(3):311–315. doi:S0304-3959(96)03306-4
Barden J, Edwards JE, McQuay HJ, Andrew Moore R (2004) Pain and analgesic response after third molar extraction and other postsurgical pain. Pain 107(1–2):86–90. doi:S0304395903004032
Irvine J, Chong SL, Amirjani N, Chan KM (2004) Double-blind randomized controlled trial of low-level laser therapy in carpal tunnel syndrome. Muscle Nerve 30(2):182–187. doi:10.1002/mus.20095
Brosseau L, Wells G, Marchand S, Gaboury I, Stokes B, Morin M, Casimiro L, Yonge K, Tugwell P (2005) Randomized controlled trial on low level laser therapy (LLLT) in the treatment of osteoarthritis (OA) of the hand. Lasers Surg Med 36(3):210–219. doi:10.1002/lsm.20137
Tanner AC, Socransky SS, Goodson JM (1984) Microbiota of periodontal pockets losing crestal alveolar bone. J Periodontal Res 19(3):279–291
Adriaens PA, Edwards CA, de Boever JA, Loesche WJ (1988) Ultrastructural observations on bacterial invasion in cementum and radicular dentin of periodontally diseased human teeth. J Periodontol 59(8):493–503
Allaker RP, Douglas CW (2009) Novel anti-microbial therapies for dental plaque-related diseases. Int J Antimicrob Agents 33(1):8–13. doi:10.1016/j.ijantimicag.2008.07.014
Dickers B, Lamard L, Peremans A, Geerts S, Lamy M, Limme M, Rompen E, de Moor RJ, Mahler P, Rocca JP, Nammour S (2009) Temperature rise during photo-activated disinfection of root canals. Lasers Med Sci 24(1):81–85. doi:10.1007/s10103-007-0526-y
Ishikawa I, Aoki A, Takasaki AA (2004) Potential applications of Erbium:YAG laser in periodontics. J Periodontal Res 39(4):275–285. doi:10.1111/j.1600-0765.2004.00738.xJRE738
Wainwright M (1998) Photodynamic antimicrobial chemotherapy (PACT). J Antimicrob Chemother 42(1):13–28
Bhatti M, MacRobert A, Meghji S, Henderson B, Wilson M (1998) A study of the uptake of toluidine blue O by Porphyromonas gingivalis and the mechanism of lethal photosensitization. Photochem Photobiol 68(3):370–376
Bhatti M, Nair SP, Macrobert AJ, Henderson B, Shepherd P, Cridland J, Wilson M (2001) Identification of photolabile outer membrane proteins of Porphyromonas gingivalis. Curr Microbiol 43(2):96–99. doi:10.1007/s002840010268
Harris F, Chatfield LK, Phoenix DA (2005) Phenothiazinium based photosensitisers – photodynamic agents with a multiplicity of cellular targets and clinical applications. Curr Drug Targets 6(5):615–627
Bevilacqua IM, Nicolau RA, Khouri S, Brugnera A Jr, Teodoro GR, Zangaro RA, Pacheco MT (2007) The impact of photodynamic therapy on the viability of Streptococcus mutans in a planktonic culture. Photomed Laser Surg 25(6):513–518. doi:10.1089/pho.2007.2109
Soukos NS, Ximenez-Fyvie LA, Hamblin MR, Socransky SS, Hasan T (1998) Targeted antimicrobial photochemotherapy. Antimicrob Agents Chemother 42(10):2595–2601
Wood S, Nattress B, Kirkham J, Shore R, Brookes S, Griffiths J, Robinson C (1999) An in vitro study of the use of photodynamic therapy for the treatment of natural oral plaque biofilms formed in vivo. J Photochem Photobiol B 50(1):1–7. doi:10.1016/S1011-1344(99)00056-1
Matevski D, Weersink R, Tenenbaum HC, Wilson B, Ellen RP, Lepine G (2003) Lethal photosensitization of periodontal pathogens by a red-filtered xenon lamp in vitro. J Periodontal Res 38(4):428–435
Prates RA, Yamada AM Jr, Suzuki LC, Eiko Hashimoto MC, Cai S, Gouw-Soares S, Gomes L, Ribeiro MS (2007) Bactericidal effect of malachite green and red laser on Actinobacillus actinomycetemcomitans. J Photochem Photobiol B 86(1):70–76. doi:10.1016/j.jphotobiol.2006.07.010
Soukos NS, Hamblin MR, Hasan T (1997) The effect of charge on cellular uptake and phototoxicity of polylysine chlorin(e6) conjugates. Photochem Photobiol 65(4):723–729
Jori G, Fabris C, Soncin M, Ferro S, Coppellotti O, Dei D, Fantetti L, Chiti G, Roncucci G (2006) Photodynamic therapy in the treatment of microbial infections: Basic principles and perspective applications. Lasers Surg Med 38(5):468–481. doi:10.1002/lsm.20361
Wood S, Metcalf D, Devine D, Robinson C (2006) Erythrosine is a potential photosensitizer for the photodynamic therapy of oral plaque biofilms. J Antimicrob Chemother 57(4):680–684. doi:10.1093/jac/dkl021
Qin Y, Luan X, Bi L, He G, Bai X, Zhou C, Zhang Z (2008) Toluidine blue-mediated photoinactivation of periodontal pathogens from supragingival plaques. Lasers Med Sci 23(1):49–54. doi:10.1007/s10103-007-0454-x
Pfitzner A, Sigusch BW, Albrecht V, Glockmann E (2004) Killing of periodontopathogenic bacteria by photodynamic therapy. J Periodontol 75(10):1343–1349
Komerik N, Wilson M, Poole S (2000) The effect of photodynamic action on two virulence factors of gram-negative bacteria. Photochem Photobiol 72(5):676–680
Soukos NS, Som S, Abernethy AD, Ruggiero K, Dunham J, Lee C, Doukas AG, Goodson JM (2005) Phototargeting oral black-pigmented bacteria. Antimicrob Agents Chemother 49(4):1391–1396. doi:10.1128/AAC.49.4.1391-1396.2005
Konig K, Teschke M, Sigusch B, Glockmann E, Eick S, Pfister W (2000) Red light kills bacteria via photodynamic action. Cell Mol Biol 46(7):1297–1303
Sarkar S, Wilson M (1993) Lethal photosensitization of bacteria in subgingival plaque from patients with chronic periodontitis. J Periodontal Res 28(3):204–210
Komerik N, Nakanishi H, MacRobert AJ, Henderson B, Speight P, Wilson M (2003) In vivo killing of Porphyromonas gingivalis by toluidine blue-mediated photosensitization in an animal model. Antimicrob Agents Chemother 47(3):932–940
de Almeida JM, Theodoro LH, Bosco AF, Nagata MJ, Oshiiwa M, Garcia VG (2007) Influence of photodynamic therapy on the development of ligature-induced periodontitis in rats. J Periodontol 78(3):566–575. doi:10.1902/jop.2007.060214
de Almeida JM, Theodoro LH, Bosco AF, Nagata MJ, Oshiiwa M, Garcia VG (2008) In vivo effect of photodynamic therapy on periodontal bone loss in dental furcations. J Periodontol 79(6):1081–1088. doi:10.1902/jop.2008.070456
Sigusch BW, Pfitzner A, Albrecht V, Glockmann E (2005) Efficacy of photodynamic therapy on inflammatory signs and two selected periodontopathogenic species in a beagle dog model. J Periodontol 76(7):1100–1105. doi:10.1902/jop.2005.76.7.1100
Shibli JA, Martins MC, Nociti FH Jr, Garcia VG, Marcantonio E Jr (2003) Treatment of ligature-induced peri-implantitis by lethal photosensitization and guided bone regeneration: a preliminary histologic study in dogs. J Periodontol 74(3):338–345
Shibli JA, Martins MC, Ribeiro FS, Garcia VG, Nociti FH Jr, Marcantonio E Jr (2006) Lethal photosensitization and guided bone regeneration in treatment of peri-implantitis: an experimental study in dogs. Clin Oral Implants Res 17(3):273–281. doi:10.1111/j.1600-0501.2005.01167.x
Hayek RR, Araujo NS, Gioso MA, Ferreira J, Baptista-Sobrinho CA, Yamada AM, Ribeiro MS (2005) Comparative study between the effects of photodynamic therapy and conventional therapy on microbial reduction in ligature-induced peri-implantitis in dogs. J Periodontol 76(8):1275–1281. doi:10.1902/jop.2005.76.8.1275
de Almeida JM, Theodoro LH, Bosco AF, Nagata MJ, Bonfante S, Garcia VG (2008) Treatment of experimental periodontal disease by photodynamic therapy in rats with diabetes. J Periodontol 79(11):2156–2165. doi:10.1902/jop.2008.080103
Fernandes LA, de Almeida JM, Theodoro LH, Bosco AF, Nagata MJ, Martins TM, Okamoto T, Garcia VG (2009) Treatment of experimental periodontal disease by photodynamic therapy in immunosuppressed rats. J Clin Periodontol 36(3):219–228. doi:10.1111/j.1600-051X.2008.01355.x
Braun A, Dehn C, Krause F, Jepsen S (2008) Short-term clinical effects of adjunctive antimicrobial photodynamic therapy in periodontal treatment: a randomized clinical trial. J Clin Periodontol 35(10):877–884. doi:10.1111/j.1600-051X.2008.01303.x
Christodoulides N, Nikolidakis D, Chondros P, Becker J, Schwarz F, Rossler R, Sculean A (2008) Photodynamic therapy as an adjunct to non-surgical periodontal treatment: a randomized, controlled clinical trial. J Periodontol 79(9):1638–1644. doi:10.1902/jop.2008.070652
Andersen R, Loebel N, Hammond D, Wilson M (2007) Treatment of periodontal disease by photodisinfection compared to scaling and root planing. J Clin Dent 18(2):34–38
de Oliveira RR, Schwartz-Filho HO, Novaes AB Jr, Taba M Jr (2007) Antimicrobial photodynamic therapy in the non-surgical treatment of aggressive periodontitis: a preliminary randomized controlled clinical study. J Periodontol 78(6):965–973. doi:10.1902/jop.2007.060494
de Oliveira RR, Schwartz-Filho HO, Novaes AB, Garlet GP, de Souza RF, Taba M, Scombatti de Souza SL, Ribeiro FJ (2009) Antimicrobial photodynamic therapy in the non-surgical treatment of aggressive periodontitis: cytokine profile in gingival crevicular fluid, preliminary results. J Periodontol 80(1):98–105. doi:10.1902/jop.2009.070465
Haas R, Baron M, Dortbudak O, Watzek G (2000) Lethal photosensitization, autogenous bone, and e-PTFE membrane for the treatment of peri-implantitis: preliminary results. Int J Oral Maxillofac Implants 15(3):374–382
Dortbudak O, Haas R, Bernhart T, Mailath-Pokorny G (2001) Lethal photosensitization for decontamination of implant surfaces in the treatment of peri-implantitis. Clin Oral Implants Res 12(2):104–108
Chondros P, Nikolidakis D, Christodoulides N, Rossler R, Gutknecht N, Sculean A (2008) Photodynamic therapy as adjunct to non-surgical periodontal treatment in patients on periodontal maintenance: a randomized controlled clinical trial. Lasers Med Sci 24(5):681–688. doi:10.1007/s10103-008-0565-z
Luan XL, Qin YL, Bi LJ, Hu CY, Zhang ZG, Lin J, Zhou CN (2009) Histological evaluation of the safety of toluidine blue-mediated photosensitization to periodontal tissues in mice. Lasers Med Sci 24(2):162–166. doi:10.1007/s10103-007-0513-3
Gad F, Zahra T, Francis KP, Hasan T, Hamblin MR (2004) Targeted photodynamic therapy of established soft-tissue infections in mice. Photochem Photobiol Sci 3(5):451–458. doi:10.1039/b311901g
Lauro FM, Pretto P, Covolo L, Jori G, Bertoloni G (2002) Photoinactivation of bacterial strains involved in periodontal diseases sensitized by porphycene-polylysine conjugates. Photochem Photobiol Sci 1(7):468–470
Gutknecht N (2006) Proceedings of the 1st International Workshop of Evidence Based Dentistry on Lasers in Dentistry. Quintessence, New Malden UK
Jori G (2006) Photodynamic therapy of microbial infections: state of the art and perspectives. J Environ Pathol Toxicol Oncol 25(1–2):505–519. doi:5d84548f012e18bf,70ad294f57d6fc57
Komerik N, MacRobert AJ (2006) Photodynamic therapy as an alternative antimicrobial modality for oral infections. J Environ Pathol Toxicol Oncol 25(1–2):487–504
Meisel P, Kocher T (2005) Photodynamic therapy for periodontal diseases: State of the art. J Photochem Photobiol B 79(2):159–170. doi:10.1016/j.jphotobiol.2004.11.023
Baker P (2002) The management of gingival recession. Dent Update 29(3):114–120, 122–124, 126
Uchida A, Wakano Y, Fukuyama O, Miki T, Iwayama Y, Okada H (1980) Controlled clinical evaluation of a 10% strontium chloride dentifrice in treatment of dentin hypersensitivity following periodontal surgery. J Periodontol 51(10):578–581
Nishida M, Katamsi D, Ucheda A (1976) Hypersensitivity of the exposed root surfaces after surgical periodontal treatment. J Osaka Univ Dent Soc 16:73–77
Chabanski MB, Gillam DG, Bulman JS, Newman HN (1997) Clinical evaluation of cervical dentine sensitivity in a population of patients referred to a specialist periodontology department: a pilot study. J Oral Rehabil 24(9):666–672
Chabanski MB, Gillam DG, Bulman JS, Newman HN (1996) Prevalence of cervical dentine sensitivity in a population of patients referred to a specialist periodontology department. J Clin Periodontol 23(11):989–992
Taani SD, Awartani F (2002) Clinical evaluation of cervical dentin sensitivity (CDS) in patients attending general dental clinics (GDC) and periodontal specialty clinics (PSC). J Clin Periodontol 29(2):118–122
Ling TY, Gillam DG (1996) The effectiveness of desensitizing agents for the treatment of cervical dentine sensitivity (CDS) – a review. J West Soc Periodontol Periodontal Abstr 44(1):5–12
Tate Y, Yoshiba K, Yoshiba N, Iwaku M, Okiji T, Ohshima H (2006) Odontoblast responses to GaAlAs laser irradiation in rat molars: an experimental study using heat-shock protein-25 immunohistochemistry. Eur J Oral Sci 114(1):50–57. doi:10.1111/j.1600-0722.2006.00261.x
Melcer J, Chaumette MT, Melcer F (1987) Dental pulp exposed to the CO2 laser beam. Lasers Surg Med 7(4):347–352
Ferreira AN, Silveira L, Genovese WJ, de Araujo VC, Frigo L, de Mesquita RA, Guedes E (2006) Effect of GaAlAs laser on reactional dentinogenesis induction in human teeth. Photomed Laser Surg 24(3):358–365. doi:10.1089/pho.2006.24.358
Matsui S, Tsujimoto Y, Matsushima K (2007) Stimulatory effects of hydroxyl radical generation by Ga-Al-As laser irradiation on mineralization ability of human dental pulp cells. Biol Pharm Bull 30(1):27–31. doi:JST.JSTAGE/bpb/30.27
Wakabayashi H, Matsumoto K (1988) Treatment of dentin hypersensitivity by GaAlAs laser irradiation (abstract). J Dent Res 67:182
Gerschman JA, Ruben J, Gebart-Eaglemont J (1994) Low level laser therapy for dentinal tooth hypersensitivity. Aust Dent J 39(6):353–357
Ladalardo TC, Pinheiro A, Campos RA, Brugnera Junior A, Zanin F, Albernaz PL, Weckx LL (2004) Laser therapy in the treatment of dentine hypersensitivity. Braz Dent J 15(2):144–150
Marsilio AL, Rodrigues JR, Borges AB (2003) Effect of the clinical application of the GaAlAs laser in the treatment of dentine hypersensitivity. J Clin Laser Med Surg 21(5):291–296. doi:10.1089/104454703322564505
Corona SA, Nascimento TN, Catirse AB, Lizarelli RF, Dinelli W, Palma-Dibb RG (2003) Clinical evaluation of low-level laser therapy and fluoride varnish for treating cervical dentinal hypersensitivity. J Oral Rehabil 30(12):1183–1189
Aranha AC, Pimenta LA, Marchi GM (2009) Clinical evaluation of desensitizing treatments for cervical dentin hypersensitivity. Braz Oral Res 23(3):333–339. doi:S1806-83242009000300018
Acknowledgments
The authors wish to express their gratitude to the Special Laboratory of Lasers in Dentistry (LELO), University of São Paulo (Brazil), and to CNPq (303798/2005-0 and 305574/2008-6) and FAPESP (CEPID – 98/14270-8) for financial support.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
de Paula Eduardo, C., de Freitas, P.M., Esteves-Oliveira, M. et al. Laser phototherapy in the treatment of periodontal disease. A review. Lasers Med Sci 25, 781–792 (2010). https://doi.org/10.1007/s10103-010-0812-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10103-010-0812-y