Abstract
The number of studies on post-traumatic stress disorder after hospitalization in a pediatric intensive care unit raised since 2004. The objective of this systematic review was to summarize and critically examine the literature about risk factors for these children to develop post-traumatic stress disorder following admission to an intensive care unit. The data sources were PubMed, Cochrane, Web of Science, PsycInfo, SUDOC, Scopus, and ScienceDirect. Studies were selected if they were in English or French and published between 01/01/2004 and 31/01/2022. Studies were excluded if patients were less than 1 month old and if no post-traumatic stress disorder was found. The internal validity and risk of bias were assessed using the National Institutes of Health Study Quality Assessment Tools for observational studies and the Ottawa Scale was used for the interventional study. The search yielded 523 results and 22 articles met inclusion criteria. Three common risk factors were identified from the data: parental post-traumatic stress disorder (especially in mothers), severity of illness and delusional memories. Internalizing behavior in children, acute parent and child stress, emergency admission and sepsis are also potential risk factors that require further investigation. The prevalence of this pathology is substantial (between 14 and 36%) and increasing awareness among pediatricians and psychologists seems necessary. Prevention programs are being studied to reduce the incidence of post-traumatic stress disorder in this population. Child and adolescent psychiatry liaison should collaborate with pediatric teams to support this objective.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Psychological trauma is defined as “an intrusive phenomenon of the psyche and the overload of its defenses by related traumatic events following a distressing experience or an experience where the life or integrity (physical or psychological) of an individual involved as a victim, witness or participant is threatened.” [1].
The first studies on psychological trauma in children with life-threatening illnesses were published in 1994; these were related to cancer [2, 3]. In the same year, the fourth edition of the diagnostic and statistical manual of mental disorders (DSM-IV) identified somatic experiences as potential traumatic events if those experiences were life-threatening [4]. Since then, chronic pediatric diseases have been studied as possible cause of trauma in both parents and children. Research on psychological impact of intensive medical care began in the early 1990s with the creation of the European interdisciplinary research network for psychology and intensive care (REIRPR, Réseau Européen Interdisciplinaire de Recherche sur la Psychologie et la Réanimation) [5]. The diagnosis of post-traumatic stress disorder was first studied in adults, while its consideration in the pediatric population only appeared in 2004 [5, 6]. These studies showed that admission to a pediatric intensive care unit (PICU) is associated with a significantly higher prevalence of PTSD, and its development is associated with impaired quality of life in children. The PICU population is, therefore, at a high risk of developing PTSD. PTSD in pediatrics seems to focus on four predominant symptoms (revivification of the event, avoidance behaviors, neurovegetative overactivation, and altered cognition) appearing within three months of the trauma. According to the DSM-V, it is referred to as acute stress when these symptoms appear within the first month [1]. These symptoms can have a negative effect on the child’s social and emotional development and, if chronic, there is a risk of developing persistent anxiety and affective disorders in adulthood with social and professional implications. Therefore, it is important to consider this issue when caring for children in PICUs [7].
Recent research in adult critical care has focused on optimizing recovery and has highlighted post-ICU syndrome, in which PTSD is described as a non-physical complication of ICU admission. Research has been conducted to identify populations at risk, because psychiatric symptoms are associated with increased physical symptoms, increased functional impairment, increased health care costs, decreased adherence to treatment, and decreased quality of life [8]. Symptoms of PTSD in the adult ICU survivor population occur in one in five cases at 1-year follow-up. Risk factors for developing PTSD in this population include psychiatric comorbidity, benzodiazepine treatment, and early memories of frightening ICU experiences [9].
The National Institute of Health and Care Excellence (NICE) guidelines on intensive care recommend monitoring for psychiatric disorders as part of the care given to patients hospitalized in these units. It is recommended to refer patients with severe clinical depression, anxiety disorders, and post-traumatic stress disorder to psychiatrists [10]. The NICE guidelines on PTSD recommend that those at risk are assessed and monitored. However, this disorder may be under-diagnosed and under-evaluated due to a lack of practitioners (psychologists or psychiatrists) and a trivialization of the symptoms by the patients’ family members. This is more commonly the case in children who may develop, if left untreated, a chronic condition and this may effect social and academic functioning [11,12,13,14].
Early diagnosis and treatment improve the prognosis of the disorder. It, therefore, seems essential to study the risk factors linked to its development [13]. It has already been proven that hospitalization in a pediatric intensive care unit (PICU) is a factor in itself that can lead to post-traumatic stress disorder [5]. It appears, therefore, useful to target a “population at risk” within this unit by recognizing risk factors, so that patients can benefit from a systematic child psychiatric evaluation. The aim of this article is to conduct a systematic literature review to identify factors that increase the risk of developing PTSD after hospitalization in a PICU. We will also explore the prevalence of PTSD in the study populations as a secondary outcome.
Methods
Research approach
This review follows the 2019 PRISMA statements for performing a systematic review [15]. As a first step, studies treating PTSD and hospitalization in pediatric intensive care unit were identified using an online search in PubMed, Cochrane, Web of Science, SUDOC, SCOPUS, ScienceDirect, and PsycInfo using the following keywords in French “état de stress post traumatique” and “réanimation pédiatrique” and in English “stress disorder, post traumatic” AND “intensive care unit, pediatric”. To increase the number of articles analyzed and thus avoid selection bias, the term “risk factor” was voluntarily removed from the research equation. The MeSH terms selected for the search criteria were (PTSD OR stress disorder, post traumatic OR chronic post traumatic OR stress disorder, post-traumatic OR stress disorder, post-traumatic) AND (PICU OR intensive care unit, pediatric OR intensive care units, pediatric OR (intensive care unit AND children) OR (critical care AND children)). These MeSH terms were selected from the HeTOP database. In the PsycInfo database, the keywords selected were: “post-traumatic stress disorder or ptsd or posttraumatic stress disorder or post-traumatic stress disorder” AND “picu or pediatric intensive care unit or pediatric critical care.” Bibliographic references and sources were managed using Zotero software. Duplicates were checked digitally and manually to remove duplicates that could have been missed by the software.
To avoid publication bias, the grey literature was analyzed using the Open Grey and the Grey Literature Report databases but no results were found.
A search for ongoing studies was conducted using the “International Clinical Trials Registry Platform” database but no results were found.
Study selection
Articles selected had to be written in English or French and published between 01/01/2004 and 31/01/2022. In addition, the articles had to meet the following inclusion criteria to be included: be medical or psychological articles, a qualitative or quantitative study, observational or interventional, evaluating at least one risk factor related to developing PTSD following admission to intensive care as the primary or secondary objective, and the age of the children had to be between 1 month and 18 years (thus excluding articles related to neonatology).
Articles were excluded if they were not written in English or French, if they were literature reviews, or if no link to post-traumatic stress disorder was found.
Studies evaluating post-traumatic stress disorder in families were selected by reading the abstract and were included if the trauma experienced by the child was assessed.
The inclusion of articles was determined by first by first reading the title, then the abstract and then the entire article to ensure that it fulfilled all inclusion criteria. To strengthen the literature review, it was decided to include all articles, including the less valid studies. This will be taken into account when interpreting the results.
A second reading was carried out by an independent researcher and resulted in a consensus of articles to be included. Cohen’s kappa coefficient, which measures the interrater reliability, was 0.82. This corresponds to a near perfect agreement level between the two readers [16].
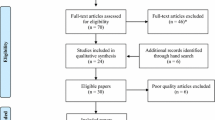
The PRISMA flow diagram of this bibliographic search is shown in Fig. 1.
Data analysis
We created a table to facilitate data extraction containing the author, country and year of publication, type of study, primary and secondary objectives, inclusion criteria, questionnaires on PTSD or risk factors, the quality score of the study and results (risk factors and other key results, including prevalence of PTSD if researched). This table is available in Annex.
The quality score was defined using the NIH Quality Assessment Tool for Observational Cohort and Cross-Sectional Studies (QATOCCS) for descriptive studies and a modified version of the Jadad scale for clinical trials (the “Oxford Quality Score”) [17, 18]. Each observational study was assessed by the QATOCCS to be assigned a quality level defined by “high”, “fair” or “poor” quality corresponding to the risk of bias. This quality score relates to the principal aim of the studies.
The data synthesis was conducted using descriptive methods. Both the level of evidence and the biases that were analyzed for each article were considered when interpreting the results.
Results
Reference selection and analysis
Five hundred twenty-three articles were identified through the various databases selected. The process of selecting references is described below in the flowchart using the PRISMA criteria (Fig. 1). Twenty-two articles from these databases were eligible for selection. One article was found through the analysis of bibliographies and subsequent Google Scholar searches, and was included in the final qualitative analysis. In fact, when analyzed in the study, the MeSH terms in this article did not include post-traumatic stress disorder or any synonyms [19]. In the end, 22 articles met the inclusion criteria and were included. These articles were almost all descriptive studies, so their methodological quality was analyzed using the QATOCCS. Only one study was a clinical trial and was analyzed using the Jadad scale.
Table 1 summarizes the risk factors sought in the included studies, the significance of the results and the quality of the study.
Annex 1 presents the articles included in the review and describes the primary objective, the results regarding PTSD, and the other results found. The results of the quality analysis of each article are provided.
Results analysis
Primary outcome: risk factor of developing PTSD in children admitted in PICU
Child’s environment and behavior (Table 1A)
Parents experiencing PTSD. Post-traumatic stress disorder in children following hospitalization in pediatric intensive care appears to correlate with the PTSD experienced by parents. A study targeting a population hospitalized for meningococcal infection assessed the risk of developing post-traumatic stress disorder (PTSD) using the self-assessment Impact of Event Scale. PTSD was only observed in children hospitalized in pediatric intensive care. There was a correlation between the mother and child self-assessment scores (p = 0.035). However, there is a selection bias to take into account here as the study only included children with meningococcal infection. Furthermore, the cohort was small with only four patients at risk of developing PTSD [20]. In another study, both the correlation between PTSD in children and their mother and in children with their father were assessed separately. The results indicated a correlation between PTSD presented by the mother and child at 3 and 9 months after hospitalization. The same link was not found between the father and child [21]. The correlation between the risk of PTSD in parents and their child was found in other studies, which validates these results [6, 22]. It would appear that it is the parent’s subjective perception of the severity of the illness and the threat to the child’s life that is a risk factor for PTSD in both the parent and the child [6]. There was only one study that did not support this result. While a correlation between PTSD experienced by parents and children was found at 3 months, no correlation was found 1 year on from hospitalization. Indeed, the disorder improved significantly in the parent, while it remained relatively unchanged in the child. Various factors would, therefore, influence the development and especially the maintenance of the disorder in these children [22].
Pre-admission characteristics. Other studies have also examined elements concerning the child’s environment before and after hospitalization that could make the child susceptible to the development of PTSD. Research on family functioning indicates that there is no correlation [23].
In addition, the child’s behavioral history was studied. It was found that a child with preadmission internalizing behavior, such as withdrawal or lack of communication, was at risk of developing chronic symptoms of PTSD (OR = 5.02 (1.51–16.70)) [24].
Conditions and etiologies of admission (Table 1B)
Condition of admission. One high validity study with the principal aim of researching PTSD risk factors found that emergency admission was a statistically significant risk factor (p = 0.002) [25]. This result is similar to the study by Colville and Pierce, which investigated this risk factor by creating three subgroups in the study population: scheduled admissions (post-surgery), head trauma, and other admission etiologies. Unscheduled admission was found to be a significant risk factor for developing PTSD. However, the primary objective of this study was to evaluate the quality of life in children hospitalized in pediatric intensive care units, so the p-value was not calculated. Additionally, one of the biases of this study is the significant number of patients lost to follow-up in the other admission etiologies group. This bias has not been explained [26]. This risk factor is found in another study, but the study population appears to be the same as the previous one (at the same location and on similar dates) [25]. Emergency admission, therefore, appears to be a risk factor for developing PTSD.
Severity of illness. The severity of the disease was primarily assessed using two tools: the PRISM (Pediatric Risk of Mortality Score) and the PIM (Pediatric Index of Mortality) or PIM 2. These scores enable the evaluation of the severity of the disease based on different physiological parameters on admission to pediatric intensive care. One study established an association with the number of invasive procedures using the IPS (Invasive Procedure Score) to define a high-risk group (with a high level of disease severity). As expected, high-risk children were more likely to develop post-traumatic stress disorder (validity remained stable over time at 6 weeks and 6 months). However, the severity of the disorder appeared to be the risk factor for developing the disorder at 6 weeks in the multivariate analysis, while the number of invasive procedures was the risk factor for developing the disorder at 6 months. The multivariate analysis in this study is unclear and the interpretation of the results is inconsistent with the statistical data presented in the tables. It should be noted that the decrease in post-traumatic symptoms is far greater in the low-risk group than in the high-risk group [19]. However, one other study found a correlation between elevated PIM 2 and PTSD development. This study has a high score on the quality assessment. PIM2 and the rate of intubation, considered to be an invasive procedure, was both independently associated with significant risk to develop elevated PTS symptoms (PIM2 p = 0.014, intubation rate p = 0.012) [24]. Other previously referenced studies have identified disease severity as a significant risk factor for developing post-traumatic stress disorder with fair and high-quality assessment [19, 25]. Another of these studies found that the effect of this risk factor remained stable over time (similar at the 1 year assessment) [22]. However, another study did not present significant results at 1 year, but the cohort was small which may have led to a results bias [26]. Multiple studies contradicted these results and did not identify disease severity at admission as a risk factor, including studies with a high level of quality according to QATOCC assessment [20, 21, 23, 27,28,29].
Etiologies of admission. Several studies have identified sepsis as a risk factor for developing PTSD in children hospitalized in pediatric intensive care units. However, for a large proportion of the studies included, the targeted population were children admitted to pediatric intensive care units at St Mary’s Hospital and Great Ormond Street Hospital in London from March 2007 to March 2010. Nevertheless, the cohorts were not identical due to different inclusion criteria [27, 30,31,32]. In the Corbet et al. study, the result was not significant in the multivariate analysis, as the cohort was probably insufficient [32]. The Caspani et al. study investigated the correlation between the various biological markers of inflammation and PTSD. CRP levels were the only identifiable risk factor in the sepsis group. No results were found for the other admission etiologies [27].
In terms of the reasons for admission, another study attempted to identify potential risk factors for the development of post-traumatic stress disorder in a cohort of 102 patients. Head trauma and sepsis did not increase the risk of developing this disorder (p-value equal to 0.24 and 0.51, respectively) [25]. According to Bronner et al. reasons for admission are not a risk factor but as they were not detailed, it is impossible to determine if the sepsis was actually isolated or not [21]. Lastly, two populations enabled the assessment of the role of sepsis in the development of PTSD, but further studies are required due to opposing results.
Head trauma represented an exclusion criterion for many authors. They suspected that it could influence the onset of PTSD due to memory loss on admission, acting as either a protective or aggravating factor. However, Colville et al. 2008 explore head trauma as potential risk factor and did not identify it as a risk factor for developing PTSD after hospitalization in PICU despite recording a decrease in memories on admission in 77% of patients [25].
Characteristics of the hospitalization (Table 1C)
Length of hospitalization. One study found that hospitalization in pediatric intensive care exceeding 48 h was a risk factor for the development of post-traumatic stress disorder [33]. However, a significant selection bias was found, as the patients included were only children hospitalized for cardiac surgery. Furthermore, with reference to disease severity, an adjustment variable has not been tested. In fact, another study found that the length of hospitalization was related to the severity of the disease [20]. Two other studies found that the length of hospitalization was a risk factor for developing PTSD [30, 34]. One of them identified it as a risk factor with a significant result in univariate analysis but negative in multivariate analysis. The authors indicate that this is caused by the inclusion of sepsis in the multivariate analysis, which represents a confounding factor [30]. Indeed, another study found greater disease severity and length of hospitalization in the sepsis group compared to groups of patients presenting other admission etiologies [27].
None of the other studies demonstrated a correlation between the length of hospitalization and the development of post-traumatic stress disorder outside of hospitalization in a pediatric intensive care unit [23, 26, 28, 35]. One study analyzed the characteristics of patients with PTSD in this population, although the primary objective was not to assess risk factors for developing PTSD after hospitalization in pediatric intensive care. The length of hospitalization was not a characteristic that differed between the group that developed PTSD and the group that did not [28]. Finally, length of stay was investigated in a more recent good quality study and was not found to be a significant factor associated with PTSD [23]. This strengthens the results found in the Stowman et al. study, which would be of limited significance due to the low quality of the study. (QATOCC: poor quality level) [35].
Quality of memories during hospitalization. Given that delirium is found as a risk factor for developing PTSD after hospitalization in pediatric intensive care, the influence of the length of hospitalization on the manifestation of delusions was also studied. It turned out that this timeline was positively correlated with the risk of having delusional memories of hospitalization. However, this result no longer stands in the logistic regression when the duration of benzodiazepine and opiate treatment is considered. Indeed, the longer the period of hospitalization, the more likely the prescription of these drugs is to last. Therefore, it is not a question of the length of hospitalization in itself that leads to a risk of hallucinations, but rather the length of time the drug treatment has been administered [25].
Dow et al. explored the link between children’s memories and experience of PICU admission and hospitalization with developing post-traumatic stress symptoms (PTSS). It was found that experiencing confusion during hospitalization was associated with more acute PTSS (p < 0.05) [36]. In fact, there is a correlation between the risk of hallucinations and developing post-traumatic stress disorder following hospitalization in pediatric intensive care units.
Drugs use. In the study by Colville et al., it was found that the risk of hallucinating is five times higher if opiates and benzodiazepines are prescribed for longer than 48 h. No direct correlation has been found between the prescription of benzodiazepines/opioids and the development of post-traumatic stress disorder in this study (p = 0.45) [25]. However, Long et al. explored the association between medical treatment factors and the development of children’s PTSS in the 12 months following PICU discharge in a large sample of patients (n = 265). The study showed that exposure to midazolam was associated with elevated post-traumatic stress symptoms at 1 month after PICU discharge (p = 0.024) with no significant difference at 3 months, 6 months and 1 year after discharge. The use of other drugs explored in this study were not associated with significant higher PTSS at any time after discharge [34]. Watson et al. conducted a comparative study evaluating the effectiveness of using the RESTORE sedation protocol during mechanical ventilation to decrease the level of sedation. Decreasing the level of sedation did not show a significant difference in the incidence of PTSD at 6 months after discharge from the PICU [37].
Expected factors not found: age, cortisol, physical after effects (Table 1D)
Age does not seem to be a risk factor for developing PTSD after hospitalization in pediatric intensive care units. Indeed, multiple studies of varying methodological quality have investigated this factor and have not identified it as something that aggravates the disorder [21, 25, 28, 33, 34]. However, the assessment age is a selection bias in most of these studies. Due to the use of self-assessment questionnaires, children from the age of seven were included, except for two studies. One was based on a structured interview and thus included children from the age of 5 [33]. The other one assessed children from the age of 2 [34]. Only one other study showed that younger age was a risk factor for the development of PTSD, but the study was rated as poor using the QATOCC [36].
In the study by Als et al., high salivary cortisol levels measured 12 h after waking up at 3 to 6 months after hospitalization in pediatric intensive care units were identified as a risk factor for PTSD. However, it was missing in the multivariate analysis when gender and age were used as covariates [31].
Board and Dai sought to evaluate the following five risk factors for developing PTSD: parental stress levels, child anxiety, disease severity, invasive procedures, and neuroendocrine stress response as calculated by salivary cortisol assay. None of these five factors were identified but the cohort was too small (only eight patients included). The only relevant finding was a decrease in salivary cortisol levels depending on the severity of the PTSD [38].
The study by Shears et al. investigated the impact of physical sequels on the risk of developing PTSD after hospitalization in pediatric intensive care. In this study, six children had significant physical sequels (two had an amputation, three had a skin graft and one had a left sided transient regression in muscle strength) but these were not correlated with the development of PTSD [20].
Finally, Rosenberg et al. and Watson et al. evaluated the use of propranolol as a protective factor for PTSD in children in PICU for burn injuries. These studies quality was high and fair and the propranolol was not associated with a lower rate of PTSD [37, 39].
Secondary outcome: prevalence of PTSD in the studied populations
When the prevalence of PTSD was investigated, it varied from 21 to 36% in the traditional PICU population [6, 21, 22, 25, 27, 28, 30, 31, 35, 37, 38]. Two studies found lower prevalence. Connolly et al. reported a prevalence of 12% in a PICU population following planned cardiac surgery [33]. Prevalence of PTSD was 15% in the study by Rosenberg et al. in which the population studied consisted of children with burn injuries who arrived in the unit after initially receiving care in a generalist unit [39].
Discussion
This literature review highlights several potential risk factors for developing PTSD. Parental PTSD seems to be the main risk factor regarding the child and their environment. Severity of the illness seems to have a significant impact on the development of PTSD in children admitted to the intensive care unit. Finally, some risk factors are associated with hospitalization and are therefore modifiable, such as intensive care delirium and the use of sedative drugs. It is important to point out that the potential risk factor of age was not found in any study that attempted to make this link. These risk factors are the most significant ones found in several trials. Other risk factors have been studied and reported in this review. They should be considered, although their impact has yet to be studied.
The strengths of this study include meeting the PRISMA criteria in 22 of the 27 items, resulting in 81% study validity. It also included all relevant studies but took into account the quality, the risks of bias, and the inclusion criteria of the studies when interpreting the results. Searching different databases and using broad search terms resulted in the inclusion of a significant number of articles [40]. However, one study limitation was the exclusion of the Google Scholar database as the search terms yielded over 8000 results. A selection bias of the study was also the selection of articles that were only in English and French. Consequently, the country of origin for the studies are limited to Canada, the United States, England, the Netherlands, and Australia. It is also worth noting that no study of this nature has been conducted in France. Another limitation of our study is that we included studies in which the exploration of risk factors for developing PTSD after a PICU stay was either the primary or secondary aim. The quality assessment of these studies focused on the primary objective. Some studies, despite their high study quality, may not have sufficient power to determine the presence of risk factors if looking for the risk factor in question was not the primary objective. Finally, the heterogeneity of the included studies regarding populations, risk factors studied, design, and quality affect the analysis of the results.
Interpretation bias in the assessment of studies must be considered. The method used in this study is based on the NIH Quality Assessment Tool for Cohort Studies and the Jadad scale. The NIH Quality Assessment Tool for Cohort Studies is a checklist that aims to reduce the subjectivity of the assessment.
Post-traumatic stress disorders in parents as a risk factor for the child developing PTSD had the most powerful proof level. However, definition for the term “parent” differed depending on the study. Some studies only included mothers while others included anyone who took care of the child. Some studies also assessed the reactions of both the father and the mother as well. Where this differentiation was made, a correlation was found between the post-traumatic stress disorder symptoms in the mother and child but not in the father and child. Indeed, attachment theory and particularly caregiving (the function of caring by meeting the child’s attachment needs) may explain this difference [41]. It is thought that maternal caregiving is more closely related to the child’s emotional development than paternal caregiving [42, 43]. However, it should be noted that cultural representations play a key part in the representation of maternal caregiving (and therefore of the maternal “role”) [44]. Protection by parent(s) from the traumatic impact of an event is very important, allowing them to understand and adapt to the traumatic episode. Thus, it is assumed that a parent with avoidance symptoms would not be able to help their child adapt.
It seems that PTSD improves more in the parent than the child. Since the child is the patient experiencing the risk factors for developing PTSD, it is reasonable to consider that it is more likely to affect the child over time. Moreover, some children will not readily talk about their sources of anxiety, which may lead to a prolongation of the disorder [45]. Indeed, it is possible that there may be a correlation between the progression of PTSD symptoms and the child’s preadmission internalizing behavior for both the chronic and recovery trajectories [24]. This is, therefore, a risk factor of interest to be studied in the future.
Emergency admission is a risk factor that has been studied with good external consistency and a good quality study finding a significant result [25]. However, it has been studied in few trials, so further research would be of interest. Indeed, during emergency admission, psychological disruption could lead to an increased risk of developing PTSD.
Head injuries are the most likely to result in memory loss at admission. However, they have been an exclusion criterion in many studies. It therefore seems important to include children admitted for head injury in PICUs in future studies.
The results for sepsis are heterogeneous, even within the good quality studies. However, the effects of sepsis, including delusions and cerebral toxicity, make it a potential cause of psychological sequelae. It would, therefore, be of interest to consider it in future studies.
The severity of the disease is a common risk factor found in several good- and fair-quality studies. It is, therefore, a risk factor identified by this review. Beyond the objective severity, it is possible that the subjective perception of the disease is a risk factor more often in parents than in their children. Further studies could allow us to highlight this aspect.
Regarding the elements of hospitalization, it seems that hallucinations are a risk factor for post-traumatic stress disorder in these children. The main risk factor for these hallucinations is the prescription of benzodiazepines for more than 48 h (fivefold risk) [34]. This finding may be related to the delusional effect of midazolam. This is a well-documented risk factor in the adult population. To reduce the risk of delirious episodes in non-pediatric ICU patients, maintaining low levels of sedation with minimal use of benzodiazepines is recommended [46]. In addition, the use of morphine for pain control has been shown to reduce post-traumatic stress disorder [47].
Previous articles have shown that age and gender are risk factors for the development of PTSD after a traumatic event in the general population [48]. No study has found significant results in the PICU population. However, age was a major selection bias of the studies in this review. Due to the self-report questionnaire, most studies included children from the age of 7. More recently, several studies have included children from the age of 2 using the parent assessment questionnaire. Only two studies were based on semi-structured interviews. No significant results were found for any of the assessment methods used. Therefore, age cannot be considered as a factor modifying the incidence of PTSD for an individual.
As a secondary outcome, the prevalence of PTSD was reported as somewhere between 1/4 and 1/3 of patients in an unplanned admission PICU population. Psycho-educational programs for parents have been developed to prevent the development of PTSD in children who have been hospitalized in PICUs. However, these programs have experienced a lack of adherence (only 1/4 to 1/3 of families used the program) [49]. Follow-up programs after PICU discharge are being developed with pediatric post-ICU syndrome assessments, including PTSD. [50, 51]. Knowledge of the risk factors for the development of PTSD after PICU hospitalization may enable targeting of at-risk populations to improve adherence.
Follow-up of these at-risk populations would allow early treatment to be provided to facilitate the evolution of the disorder before any complications occur [13]. Currently, psychotherapies have been shown to be the most effective treatment for PTSD in children. Cognitive behavioral therapies with trauma exposure have been shown to be effective [52, 53]. In the absence of sufficient evidence for other types of psychotherapy, NICE currently recommends cognitive behavioral therapy (CBT) over 6–12 sessions for children aged 5 to 17. It also recommends involving parents in therapy sessions where possible. EMDR (Eye Movement Desensitization and Reprocessing) also appears to be effective, but is only indicated as a second-line treatment for children aged 7 to 17 if CBT is ineffective [54, 55]. Few studies have looked at the potential benefits of psychodynamic psychotherapy (using play) for this disorder, so it is not currently recommended [53]. However, a study comparing it with CBT treatment found results that support psychodynamic therapy but for short-term assessment only [56].
Conclusion
This systematic review of the literature highlighted several risk factors to be considered during the emergence of PTSD following hospitalization in a PICU. These include the development of PTSD in the parent, severity of illness, onset of intensive care delirium, and use of benzodiazepines.
Other factors such as child internalizing behavior, acute parent and child stress, emergency admission, and sepsis are potential risk factors that still require investigation. Finally, age and sex are not significantly associated with PTSD in this population.
As this disorder affects at least one in four children in PICU, it seemed important to raise awareness among caregivers in these units of the risk factors for developing this disorder. The aim of this literature review was to improve the current understanding of children at risk of developing PTSD. Recognizing the populations at risk would make it possible to direct patients and their families toward appropriate care to prevent the disorder from becoming chronic.
References
Association, Pull-Erpelding M-C (2015) A psychiatric. DSM-5®. Elsevier Masson, Issy-les-Moulineaux
Stuber ML, Shemesh E (2006) Post-traumatic stress response to life-threatening illnesses in children and their parents. Child Adolesc Psychiatr Clin N Am Juill 15:597–609
Walker AM, Harris G, Baker A et al (1999) Post-traumatic stress responses following liver transplantation in older children. J Child Psychol Psychiatry 40:363–374
Association, Crocq M-A, Guelfi J-D (2004) A psychiatric. DSM-IV-TR. Masson, Issy-les-Moulineaux
Davydow DS, Gifford JM, Desai SV et al (2008) Posttraumatic stress disorder in general intensive care unit survivors: a systematic review. Gen Hosp Psychiatry 30:421–434. https://doi.org/10.1016/j.genhosppsych.2008.05.006
Rees G, Gledhill J, Garralda ME, Nadel S (2004) Psychiatric outcome following paediatric intensive care unit (PICU) admission: a cohort study. Intensive Care Med 30:1607–1614
Camisasca E (2011) Post-traumatic stress related to pediatric illness and injury. Post-traumatic syndromes in childhood and adolescence. John Wiley & Sons Ltd, Hoboken, pp 91–110
Prince E, Gerstenblith TA, Davydow D, Bienvenu OJ (2018) Psychiatric morbidity after critical illness. Crit Care Clin 34:599–608. https://doi.org/10.1016/j.ccc.2018.06.006
Parker AM, Sricharoenchai T, Raparla S et al (2015) Posttraumatic stress disorder in critical illness survivors: a metaanalysis. Crit Care Med 43:1121–1129. https://doi.org/10.1097/CCM.0000000000000882
National Institute for Health and care Excellence. Rehabilitation after critical illness in adults | Guidance and guidelines | NICE Internet. 25 March 2009. National Institute for, London
Ziegler MF (2005) Posttraumatic stress responses in children: Awareness and practice among a sample of pediatric emergency care providers. Pediatrics 115:1261–1267
Bolton D, O’Ryan D, Udwin O et al (2000) The long-term psychological effects of a disaster experienced in adolescence: II: general psychopathology. J Child Psychol Psychiatry 41:513–523. https://doi.org/10.1111/1469-7610.00636
Hiller RM, Meiser-Stedman R, Fearon P et al (2016) Research review: changes in the prevalence and symptom severity of child post-traumatic stress disorder in the year following trauma–a meta-analytic study. J Child Psychol Psychiatry 57:884–898. https://doi.org/10.1111/jcpp.12566
Copeland WE, Keeler G, Angold A, Costello EJ (2007) Traumatic events and posttraumatic stress in childhood. Arch Gen Psychiatry 64:577–584. https://doi.org/10.1001/archpsyc.64.5.577
Gedda M (2015) Traduction française des lignes directrices PRISMA pour l’écriture et la lecture des revues systématiques et des méta-analyses. Kinésithérapie Rev 15:39–44
Cohen J (1960) A Coefficient of agreement for nominal scales. Educ Psychol Meas 20(37):46
Study Quality Assessment Tools | NHLBI, NIH. https://www.nhlbi.nih.gov/health-topics/study-quality-assessment-tools. Accessed 20 Mar 2022.
Gerlier J (2002) L’échelle de Jadad pour approcher la qualité d’un ECR. Acupuncture et moxibustion 1:66–67
Rennick JE, Morin I, Kim D et al (2004) Identifying children at high risk for psychological sequelae after pediatric intensive care unit hospitalization*. Pediatr Crit Care Med 5:358–363. https://doi.org/10.1097/01.PCC.0000128603.20501.0D
Shears D, Nadel S, Gledhill J, Garralda ME (2005) Short-term psychiatric adjustment of children and their parents following meningococcal disease. Pediatr Crit Care Med 6:39–43. https://doi.org/10.1097/01.PCC.0000144705.81825.EE
Bronner MB, Knoester H, Bos AP et al (2008) Posttraumatic stress disorder (PTSD) in children after paediatric intensive care treatment compared to children who survived a major fire disaster. Child Adolesc Psychiatry Ment Health 2:9. https://doi.org/10.1186/1753-2000-2-9
Colville G, Pierce C (2012) Patterns of post-traumatic stress symptoms in families after paediatric intensive care. Intensive Care Med 38:1523–1531. https://doi.org/10.1007/s00134-012-2612-2
Nelson LP, Lachman SE, Li SW, Gold JI (2019) The effects of family functioning on the development of posttraumatic stress in children and their parents following admission to the PICU. Pediatr Crit Care Med J Soc Crit Care Med World Fed Pediatr Intensive Crit Care Soc 20:e208–e215. https://doi.org/10.1097/PCC.0000000000001894
Le Brocque RM, Dow BL, McMahon H et al (2020) The course of posttraumatic stress in children: examination of symptom trajectories and predictive factors following admission to pediatric intensive care. Pediatr Crit Care Med J Soc Crit Care Med World Fed Pediatr Intensive Crit Care Soc 21:e399–e406. https://doi.org/10.1097/PCC.0000000000002316
Colville G, Kerry S, Pierce C (2008) Children’s factual and delusional memories of intensive care. Am J Respir Crit Care Med 177:976–982. https://doi.org/10.1164/rccm.200706-857OC
Colville GA, Pierce CM (2013) Children’s self-reported quality of life after intensive care treatment. Pediatr Crit Care Med J Soc Crit Care Med World Fed Pediatr Intensive Crit Care Soc 14:e85-92. https://doi.org/10.1097/PCC.0b013e3182712997
Caspani G, Corbet Burcher G, Garralda ME et al (2018) Inflammation and psychopathology in children following PICU admission: an exploratory study. Evid Based Ment Health 21:139–144. https://doi.org/10.1136/ebmental-2018-300027
Dow BL, Kenardy JA, Le Brocque RM, Long DA (2012) The utility of the children’s revised impact of event scale in screening for concurrent PTSD following admission to intensive care. J Trauma Stress 25:602–605. https://doi.org/10.1002/jts.21742
Vermunt LC, Buysse CMP, Joosten KFM et al (2008) Behavioural, emotional, and post-traumatic stress problems in children and adolescents, long term after septic shock caused by Neisseria meningitidis. Br J Clin Psychol 47:251–263
Als LC, Picouto MD, Hau S-M et al (2015) Mental and physical well-being following admission to pediatric intensive care. Pediatr Crit Care Med J Soc Crit Care Med World Fed Pediatr Intensive Crit Care Soc 16:e141-149. https://doi.org/10.1097/PCC.0000000000000424
Als LC, Picouto MD, O’Donnell KJ et al (2017) Stress hormones and posttraumatic stress symptoms following paediatric critical illness: an exploratory study. Eur Child Adolesc Psychiatry 26:511–519. https://doi.org/10.1007/s00787-016-0933-3
Corbet Burcher G, Picouto MD, Als LC et al (2018) Post-traumatic stress after PICU and corticosteroid use. Arch Dis Child 103:887–889. https://doi.org/10.1136/archdischild-2017-314157
Connolly D, McClowry S, Hayman L et al (2004) Posttraumatic stress disorder in children after cardiac surgery. J Pediatr 144:480–484. https://doi.org/10.1016/j.jpeds.2003.12.048
Long D, Gibbons K, Le Brocque R et al (2021) Midazolam exposure in the paediatric intensive care unit predicts acute post-traumatic stress symptoms in children. Aust Crit Care. https://doi.org/10.1016/j.aucc.2021.06.004
Stowman S, Kearney CA, Daphtary K (2015) Mediators of initial acute and later posttraumatic stress in youth in a PICU. Pediatr Crit Care Med J Soc Crit Care Med World Fed Pediatr Intensive Crit Care Soc 16:e113-118. https://doi.org/10.1097/PCC.0b013e31822f1916
Dow BL, Kenardy JA, Long DA, Le Brocque RM (2019) Cognitive/affective factors are associated with children’s acute posttraumatic stress following pediatric intensive care. Psychol Trauma Theory Res Pract Policy 11:55–63. https://doi.org/10.1037/tra0000349
Watson RS, Asaro LA, Hertzog JH et al (2018) Long-term outcomes after protocolized sedation versus usual care in ventilated pediatric patients. Am J Respir Crit Care Med 197:1457–1467
Board R, Dai J (2011) Effects of five parent-and-child risk factors on salivary cortisol levels and symptoms of posttraumatic stress disorder in school-age, critically ill children: pilot study. Heart Lung J Crit Care 40:236–246. https://doi.org/10.1016/j.hrtlng.2010.05.051
Rosenberg L, Rosenberg M, Sharp S et al (2018) Does Acute propranolol treatment prevent posttraumatic stress disorder, anxiety, and depression in children with burns? J Child Adolesc Psychopharmacol 28:117–123
Lopes-Júnior LC, de Rosa MADRP, de Lima RAG (2018) Psychological and psychiatric outcomes following PICU admission: a systematic review of cohort studies. Pediatr Crit Care Med J Soc Crit Care Med World Fed Pediatr Intensive Crit Care Soc 19:e58–e67. https://doi.org/10.1097/PCC.0000000000001390
Bowlby J (1988) A secure base: parent-child attachment and healthy human development. Basic Books, New York
Steele H, Steele M, Fonagy P (1996) Associations among attachment classifications of mothers, fathers, and their infants. Child Dev 67:541–555. https://doi.org/10.1111/j.1467-8624.1996.tb01750.x
Steele H, Steele M (2005) Understanding and Resolving emotional conflict: The London parent-child project. Attachment from infancy to adulthood: the major longitudinal studies. Guilford Publications, New York, NY, US, pp 137–164
Sagi A, van IJzendoorn M, Scharf M et al (1997) Ecological constraints for intergenerational transmission of attachment. Int J Behav Dev 20(2):287–299. https://doi.org/10.1080/016502597385342
Traiter les psychotraumatismes, Gérard Lopez, Dunod, Les Ateliers Du Praticien, 16th July 2020
Piva S, McCreadie VA, Latronico N (2015) Neuroinflammation in sepsis: sepsis associated delirium. Cardiovasc Hematol Disord Drug Targets 15:10–18
Sheridan RL, Stoddard FJ, Kazis LE et al (2014) Long-term posttraumatic stress symptoms vary inversely with early opiate dosing in children recovering from serious burns: effects durable at 4 years. J Trauma Acute Care Surg 76:828–832. https://doi.org/10.1097/TA.0b013e3182ab111c
Bokszczanin A (2007) PTSD symptoms in children and adolescents 28 months after a flood: age and gender differences. J Trauma Stress 20:347–351. https://doi.org/10.1002/jts.20220
Baker SC, Gledhill JA (2017) Systematic review of interventions to reduce psychiatric morbidity in parents and children after Picu admissions*. Pediatr Crit Care Med 18:343–348. https://doi.org/10.1097/PCC.0000000000001096
NCT04961697 (2021) Family and Patient Outcomes After Pediatric Intensive Care (FOREVER). https://clinicaltrials.gov/show/NCT04961697. https://doi.org/10.1002/central/CN-02290377. Accessed Jan 2022
Hartman ME, Williams CN, Hall TA et al (2020) Post-intensive-care syndrome for the pediatric neurologist. Pediatr Neurol 108:47–53. https://doi.org/10.1016/j.pediatrneurol.2020.02.003
Morina N, Koerssen R, Pollet TV (2016) Interventions for children and adolescents with posttraumatic stress disorder: a meta-analysis of comparative outcome studies. Clin Psychol Rev 47:41–54. https://doi.org/10.1016/j.cpr.2016.05.006
Gillies D, Maiocchi L, Bhandari AP et al (2016) Psychological therapies for children and adolescents exposed to trauma. Cochrane Database Syst Rev. https://doi.org/10.1002/14651858.CD012371
National Collaborating Centre for Mental Health (UK) (2005) Post-traumatic stress disorder: the management of PTSD in adults and children in primary and secondary care. Gaskell, Leicester (UK)
National Institute for Health and care Excellence (2018) Post-traumatic stress disorder | Guidance and guidelines |. National Institute for Health and care Excellence, London
Schottelkorb AA, Doumas DM, Garcia R (2012) Treatment for childhood refugee trauma: a randomized, controlled trial. Int J Play Ther 21:57–73. https://doi.org/10.1037/a0027430
Funding
None.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
None.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
de Pellegars, A., Cariou, C., Le Floch, M. et al. Risk factors of post-traumatic stress disorder after hospitalization in a pediatric intensive care unit: a systematic literature review. Eur Child Adolesc Psychiatry (2023). https://doi.org/10.1007/s00787-023-02141-8
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00787-023-02141-8